Efficacy and Safety of the Radiotherapy for Liver Cancer: Assessment of Local Controllability and Its Role in Multidisciplinary Therapy
Simple Summary
Abstract
1. Introduction
2. Methods
2.1. Patients
2.2. Evaluation of Antitumor Effects
2.3. Evaluation of Safety
2.4. Statistical Analysis
3. Results
3.1. Patient Characteristics
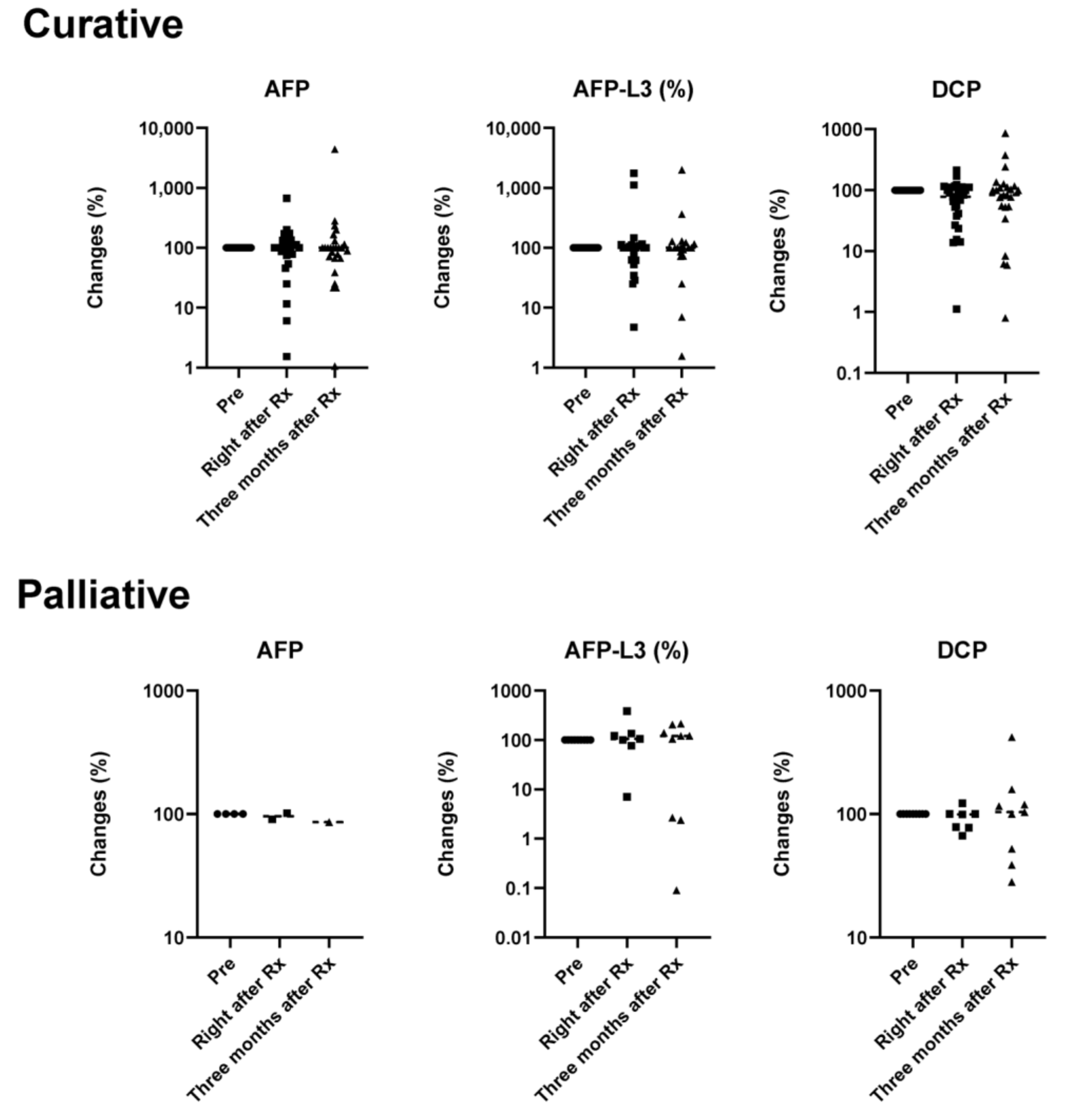
3.2. Efficacy
3.2.1. Curative Radiation
3.2.2. Palliative Radiation
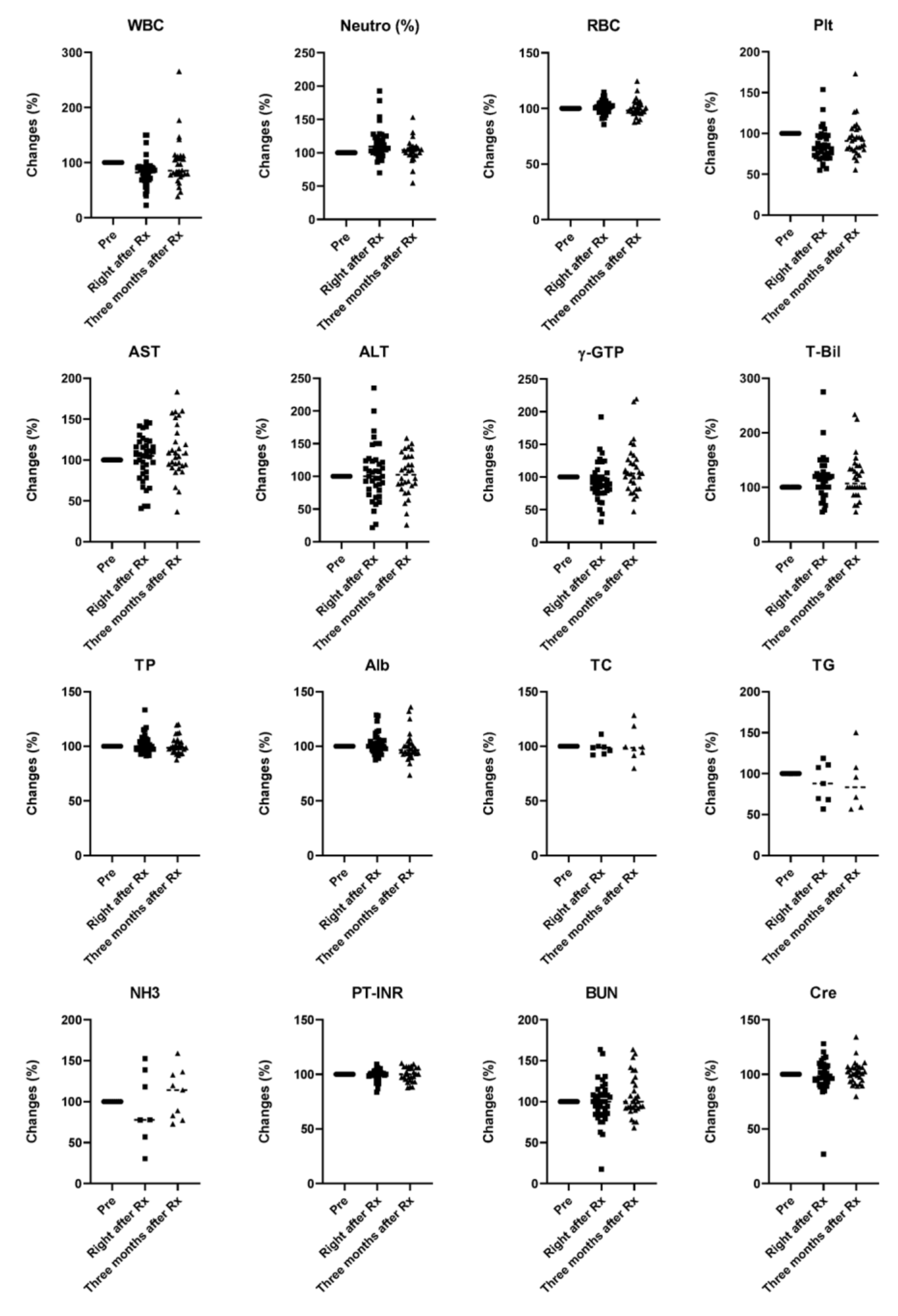
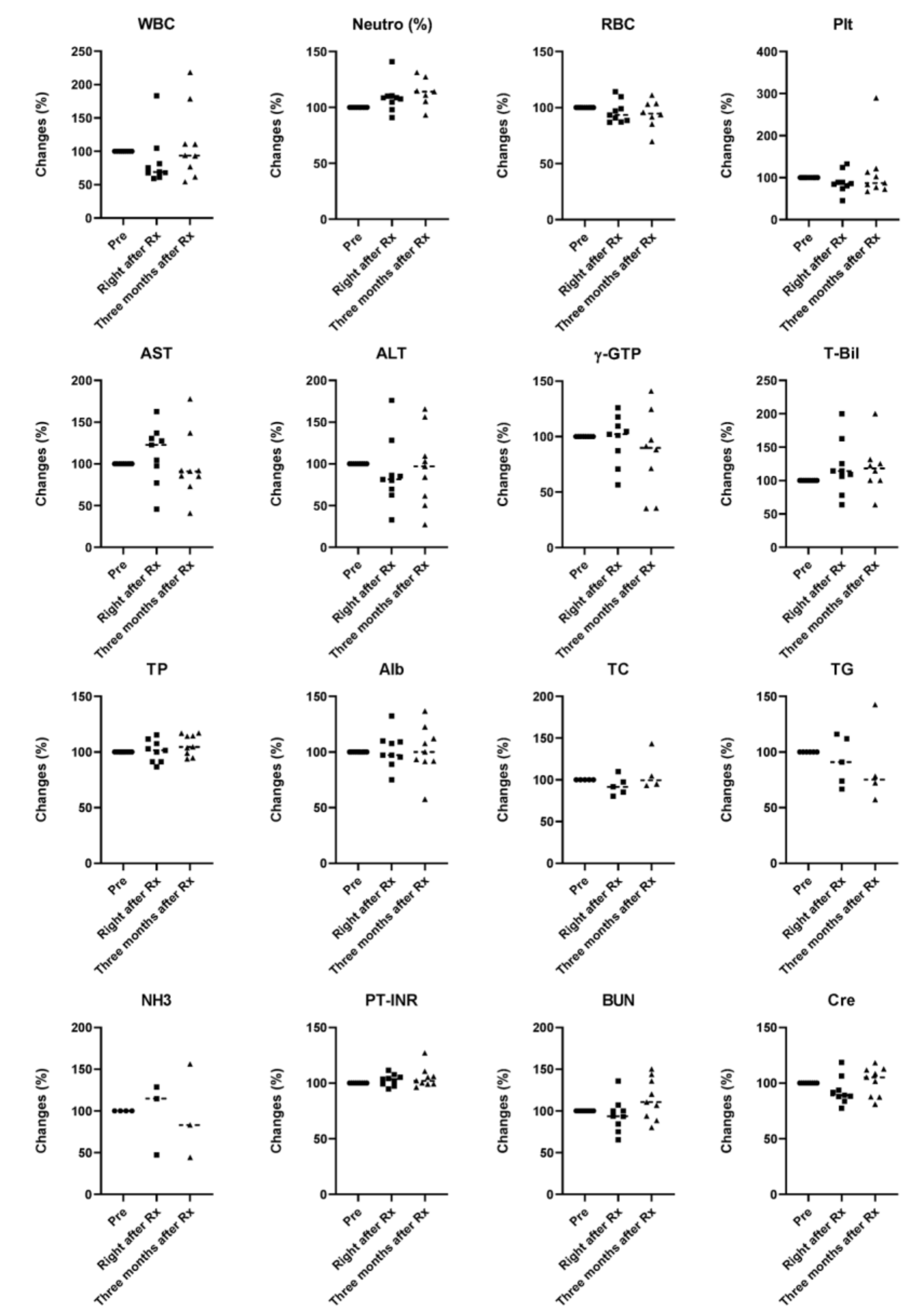
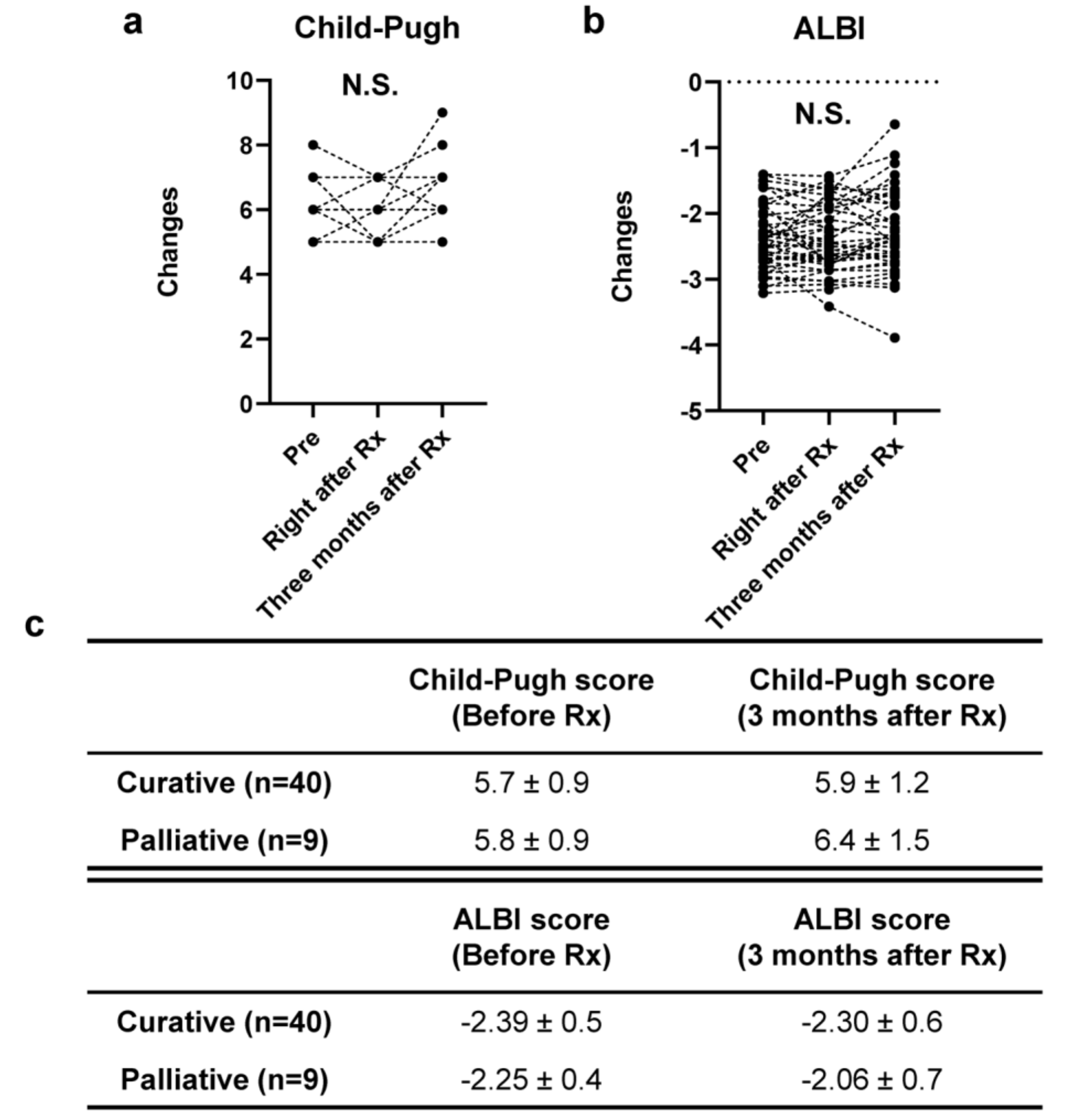
3.3. Safety
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- European Association for the Study of the Liver. EASL Clinical practice guidelines: Management of hepatocellular carcinoma. J. Hepatol. 2018, 69, 182–236. [Google Scholar] [CrossRef] [PubMed]
- Fonseca, A.Z.; Santin, S.; Gomes, L.G.; Waisberg, J.; Ribeiro, M.A., Jr. Complications of radiofrequency ablation of hepatic tumors: Frequency and risk factors. World J. Hepatol. 2014, 6, 107–113. [Google Scholar] [CrossRef] [PubMed]
- Keane, F.K.; Hong, T.S.; Zhu, A.X. Evolving systemic therapy in hepatocellular carcinoma: Current management and opportunities for integration with radiotherapy. Semin. Radiat. Oncol. 2018, 28, 332–341. [Google Scholar] [CrossRef] [PubMed]
- Kim, N.; Kim, H.J.; Won, J.Y.; Kim, D.Y.; Han, K.H.; Jung, I.; Seong, J. Retrospective analysis of stereotactic body radiation therapy efficacy over radiofrequency ablation for hepatocellular carcinoma. Radiother. Oncol. 2019, 131, 81–87. [Google Scholar] [CrossRef]
- Rim, C.H.; Kim, H.J.; Seong, J. Clinical feasibility and efficacy of stereotactic body radiotherapy for hepatocellular carcinoma: A systematic review and meta-analysis of observational studies. Radiother. Oncol. 2019, 131, 135–144. [Google Scholar] [CrossRef]
- Kong, V.C.; Velec, M. Stereotactic body radiation therapy for liver cancer: A review of the technology. J. Med. Imaging Radiat. Sci. 2015, 46, 343–350. [Google Scholar] [CrossRef]
- Shibuya, K.; Ohno, T.; Terashima, K.; Toyama, S.; Yasuda, S.; Tsuji, H.; Okimoto, T.; Shioyama, Y.; Nemoto, K.; Kamada, T.; et al. Short-course carbon-ion radiotherapy for hepatocellular carcinoma: A multi- institutional retrospective study. Liver Int. 2018, 38, 2239–2247. [Google Scholar] [CrossRef]
- Mathew, A.S.; Atenafu, E.G.; Owen, D.; Maurino, C.; Brade, A.; Brierley, J.; Dinniwell, R.; Kim, J.; Cho, C.; Ringash, J.; et al. Long term outcomes of stereotactic body radiation therapy for hepatocellular carcinoma without macrovascular invasion. Eur. J. Cancer 2020, 134, 41–51. [Google Scholar] [CrossRef]
- Hara, K.; Takeda, A.; Tsurugai, Y.; Saigusa, Y.; Sanuki, N.; Eriguchi, T.; Maeda, S.; Tanaka, K.; Numata, K. Radiotherapy for hepatocellular carcinoma results in comparable survival to radiofrequency ablation: A propensity score analysis. Hepatology 2019, 69, 2533–2545. [Google Scholar] [CrossRef]
- Wong, T.C.; Chiang, C.L.; Lee, A.S.; Lee, V.H.; Yeung, C.S.; Ho, C.H.; Cheung, T.T.; Ng, K.K.; Chok, S.H.; Chan, A.C.; et al. Better survival after stereotactic body radiation therapy following transarterial chemoembolization in nonresectable hepatocellular carcinoma: A propensity score matched analysis. J. Surg. Oncol. 2019, 28, 228–235. [Google Scholar] [CrossRef]
- Kloeckner, R.; Galle, P.R.; Bruix, J. Local and regional therapies for hepatocellular carcinoma. Hepatology 2020. [Google Scholar] [CrossRef] [PubMed]
- Song, M.J.; Bae, S.H.; Lee, J.S.; Lee, S.W.; Song, D.S.; You, C.R.; Choi, J.Y.; Yoon, S.K. Combination transarterial chemoembolization and radiofrequency ablation therapy for early hepatocellular carcinoma. Korean J. Intern. Med. 2016, 31, 242–252. [Google Scholar] [CrossRef] [PubMed]
- Fu, Y.; Xi, M.; Pan, Y.; Chen, J.; Wang, J.; Liu, S.; Xu, L.; Zhou, Z.; Liu, M.; Chen, M.; et al. Stereotactic body radiotherapy as a salvage therapy after incomplete radiofrequency ablation for hepatocellular carcinoma: A retrospective cohort study. J. Oncol. 2020, 2020, 4835653. [Google Scholar] [CrossRef] [PubMed]
- Bettinger, D.; Pinato, D.J.; Schultheiss, M.; Sharma, R.; Rimassa, L.; Pressiani, T.; Burlone, M.E.; Pirisi, M.; Kudo, M.; Park, J.W.; et al. Stereotactic body radiation therapy as an alternative treatment for patients with hepatocellular carcinoma compared to sorafenib: A propensity score analysis. Liver Cancer 2019, 8, 281–294. [Google Scholar] [CrossRef] [PubMed]
- Kishi, N.; Kanayama, N.; Hirata, T.; Ohira, S.; Wada, K.; Kawaguchi, Y.; Konishi, K.; Nagata, S.; Nakatsuka, S.I.; Marubashi, S.; et al. Preoperative stereotactic body radiotherapy to portal vein tumour thrombus in hepatocellular carcinoma: Clinical and pathological analysis. Sci. Rep. 2020, 10, 4105. [Google Scholar] [CrossRef] [PubMed]
- Que, J.; Wu, H.C.; Lin, C.H.; Huang, C.I.; Li, L.C.; Ho, C.H. Comparison of stereotactic body radiation therapy with and without sorafenib as treatment for hepatocellular carcinoma with portal vein tumor thrombosis. Medicine 2020, 99, e19660. [Google Scholar] [CrossRef]
- Chu, H.H.; Kim, J.H.; Shim, J.H.; Yoon, S.M.; Kim, P.H.; Alrashidi, I. Chemoembolization plus radiotherapy versus chemoembolization plus sorafenib for the treatment of hepatocellular carcinoma invading the portal vein: A propensity score matching analysis. Cancers 2020, 12, 1116. [Google Scholar] [CrossRef]
- Luo, J.; Guo, R.P.; Lai, E.C.; Zhang, Y.J.; Lau, W.Y.; Chen, M.S.; Shi, M. Transarterial chemoembolization for unresectable hepatocellular carcinoma with portal vein tumor thrombosis: A prospective comparative study. Ann. Surg. Oncol. 2011, 18, 413–420. [Google Scholar] [CrossRef]
- Bruix, J.; Raoul, J.L.; Sherman, M.; Mazzaferro, V.; Bolondi, L.; Craxi, A.; Galle, P.R.; Santoro, A.; Beaugrand, M.; Sangiovanni, A.; et al. Efficacy and safety of sorafenib in patients with advanced hepatocellular carcinoma: Subanalyses of a phase III trial. J. Hepatol. 2012, 57, 821–829. [Google Scholar] [CrossRef]
- Tanaka, O.; Kojima, T.; Ohbora, A.; Makita, C.; Taniguchi, T.; Ono, K.; Matsuo, M.; Nagata, Y. Scores of Child-Pugh classification impact overall survival after stereotactic body radiation therapy for primary and metastatic liver tumors. J. Clin. Exp. Hepatol. 2020, 10, 101–105. [Google Scholar] [CrossRef]
- Tang, Q.H.; Li, A.J.; Yang, G.M.; Lai, E.C.; Zhou, W.P.; Jiang, Z.H.; Lau, W.Y.; Wu, M.C. Surgical resection versus conformal radiotherapy combined with TACE for resectable hepatocellular carcinoma with portal vein tumor thrombus: A comparative study. World J. Surg. 2013, 37, 1362–1370. [Google Scholar] [CrossRef] [PubMed]
- Wei, X.; Jiang, Y.; Zhang, X.; Feng, S.; Zhou, B.; Ye, X.; Xing, H.; Xu, Y.; Shi, J.; Guo, W.; et al. Neoadjuvant three-dimensional conformal radiotherapy for resectable hepatocellular carcinoma with portal vein tumor thrombus: A randomized, open-label, multicenter controlled study. J. Clin. Oncol. 2019, 37, 2141–2151. [Google Scholar] [CrossRef] [PubMed]
- Koay, E.J.; Owen, D.; Das, P. Radiation-induced liver disease and modern radiotherapy. Semin. Radiat. Oncol. 2018, 28, 321–331. [Google Scholar] [CrossRef] [PubMed]
- Munoz-Schuffenegger, P.; Ng, S.; Dawson, L.A. Radiation-induced liver toxicity. Semin. Radiat. Oncol. 2017, 27, 350–357. [Google Scholar] [CrossRef]
- Shanker, M.D.; Liu, H.Y.; Lee, Y.Y.; Stuart, K.A.; Powell, E.E.; Wigg, A.; Pryor, D.I. Stereotactic radiotherapy for hepatocellular carcinoma: Expanding the multidisciplinary armamentarium. J. Gastroenterol. Hepatol. 2020. [Google Scholar] [CrossRef] [PubMed]
- Chapman, T.R.; Bowen, S.R.; Schaub, S.K.; Yeung, R.H.; Kwan, S.W.; Park, J.O.; Yu, L.; Harris, W.P.; Johnson, G.E.; Liou, I.W.; et al. Toward consensus reporting of radiation-induced liver toxicity in the treatment of primary liver malignancies: Defining clinically relevant endpoints. Pract. Radiat. Oncol. 2018, 8, 157–166. [Google Scholar] [CrossRef]
- Johnson, P.J.; Berhane, S.; Kagebayashi, C.; Satomura, S.; Teng, M.; Reeves, H.L.; O’Beirne, J.; Fox, R.; Skowronska, A.; Palmer, D.; et al. Assessment of liver function in patients with hepatocellular carcinoma: A new evidence-based approach―the ALBI grade. J. Clin. Oncol. 2015, 33, 550–558. [Google Scholar] [CrossRef]
- Hiraoka, A.; Kumada, T.; Michitaka, K.; Toyoda, H.; Tada, T.; Ueki, H.; Kaneto, M.; Aibiki, T.; Okudaira, T.; Kawakami, T.; et al. Usefulness of albumin-bilirubin (ALBI) grade for evaluation of prognosis of 2584 Japanese patients with hepatocellular carcinoma. J. Gastroenterol. Hepatol. 2015, 31, 1031–1036. [Google Scholar] [CrossRef]
- Su, T.S.; Yang, H.M.; Zhou, Y.; Huang, Y.; Liang, P.; Cheng, T.; Chen, L.; Li, L.Q.; Liang, S.X. Albumin-bilirubin (ALBI) versus Child-Turcotte-Pugh (CTP) in prognosis of HCC after stereotactic body radiation therapy. Radiat. Oncol. 2019, 14, 50. [Google Scholar] [CrossRef]
- Kudo, M. Systemic Therapy for Hepatocellular Carcinoma: Latest Advances. Cancers 2018, 10, 412. [Google Scholar] [CrossRef]
- Bruix, J.; da Fonseca, L.G.; Reig, M. Insights into the success and failure of systemic therapy for hepatocellular carcinoma. Nat. Rev. Gastroenterol. Hepatol. 2019, 16, 617–630. [Google Scholar] [CrossRef] [PubMed]
- Gadsden, M.M.; Kaplan, D.E. Multidisciplinary approach to HCC management: How can this be done? Dig. Dis. Sci. 2019, 64, 968–975. [Google Scholar] [CrossRef] [PubMed]
- Finn, R.S.; Qin, S.; Ikeda, M.; Galle, P.R.; Ducreux, M.; Kim, T.Y.; Kudo, M.; Breder, V.; Merle, P.; Kaseb, A.O.; et al. IMbrave150 Investigators. Atezolizumab plus Bevacizumab in unresectable hepatocellular carcinoma. N. Engl. J. Med. 2020, 382, 1894–1905. [Google Scholar] [CrossRef] [PubMed]
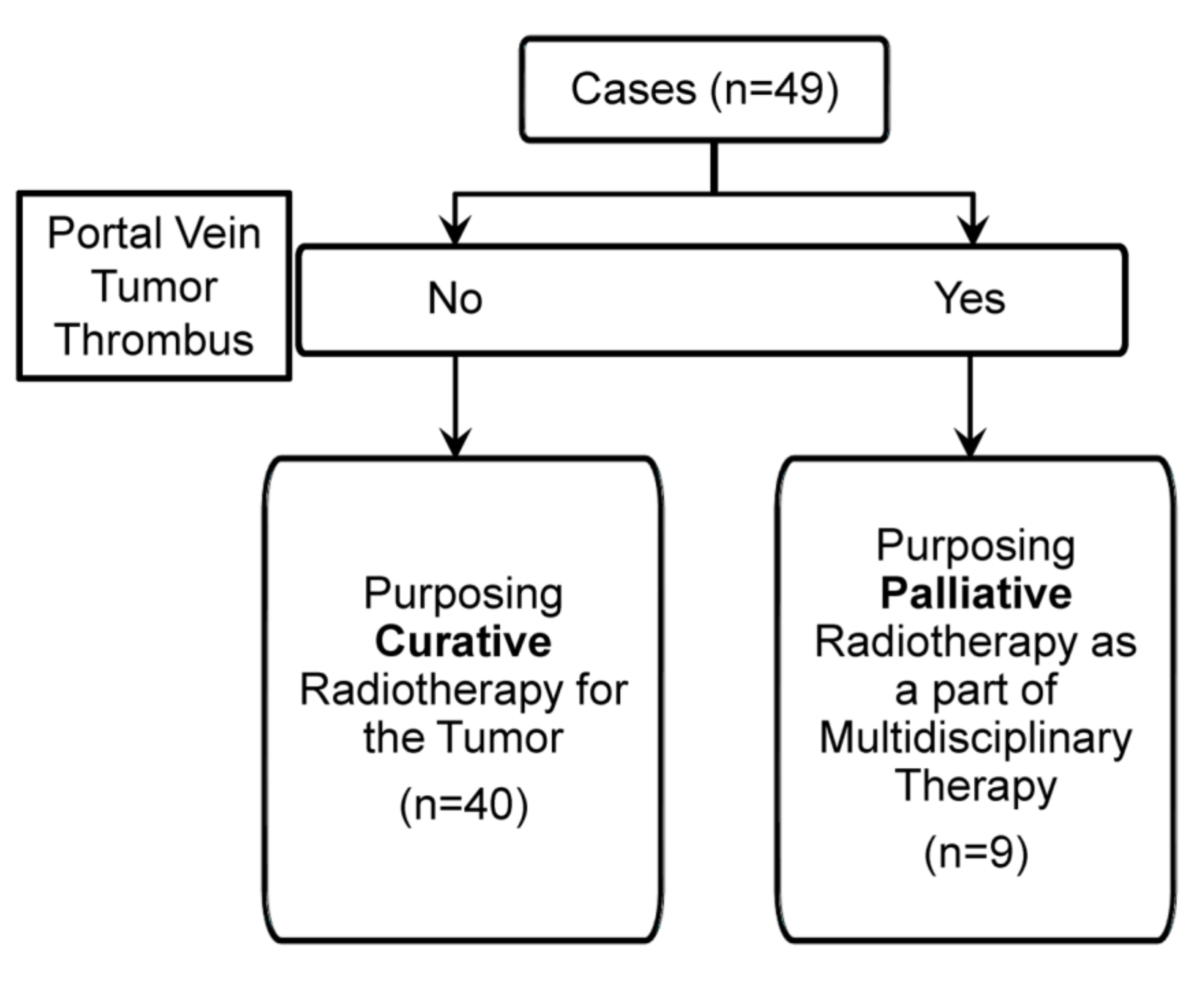
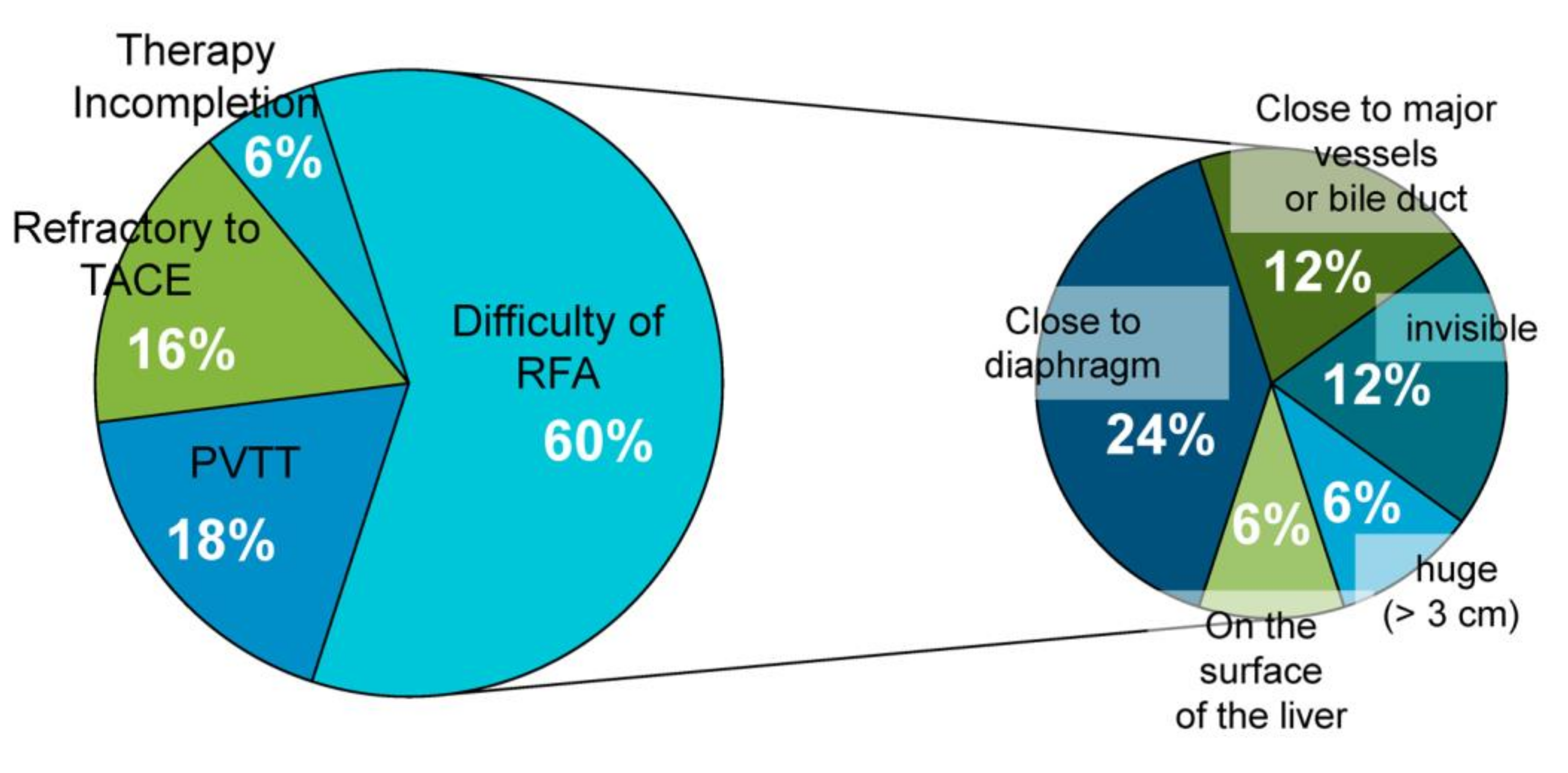
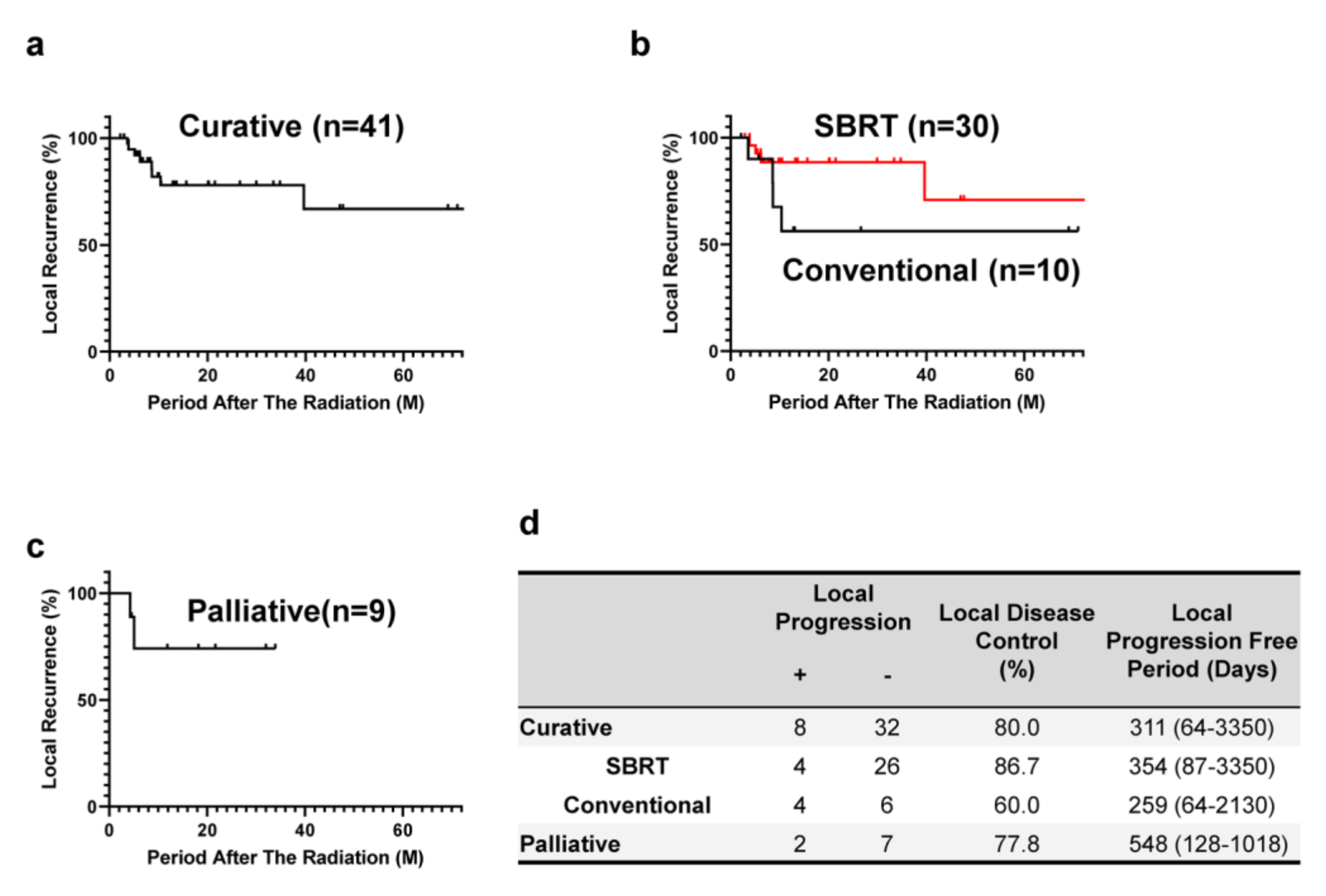
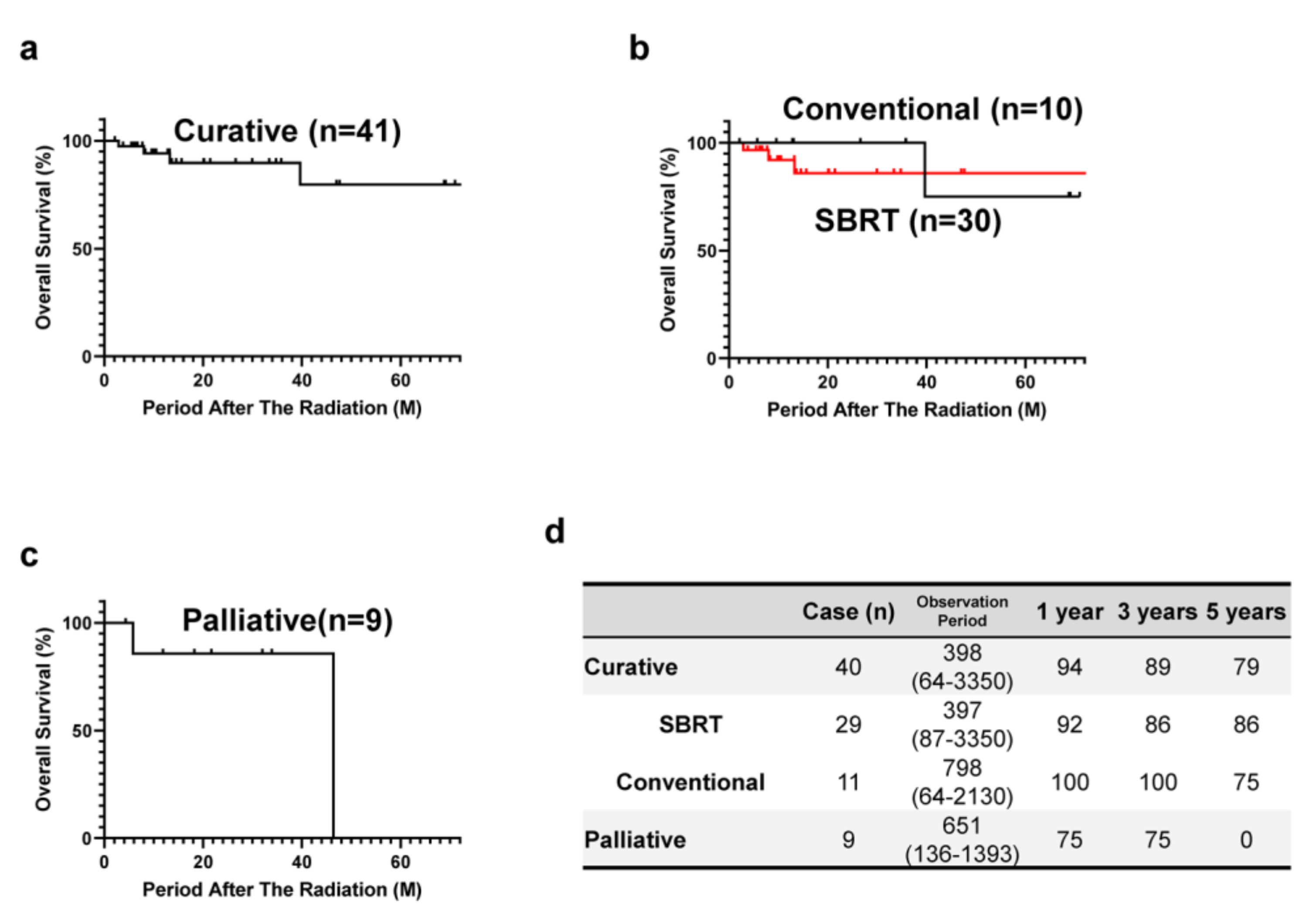
| Characteristic | Curative Group | Palliative Group |
|---|---|---|
| Number of patients | 40 | 9 |
| Age (yr) | 71 (44–86) | 71 (50–84) |
| Gender (M:F) | 30:10 | 6:3 |
| Etiology (HBV, HCV, NBNC) | 3, 18, 19 | 4, 2, 3 |
| Child–Pugh (A, B, C) | 33, 7, 0 | 8, 1, 0 |
| ALBI score | −2.39 (−3.21 to −1.50) | −2.25 (−2.90 to −1.50) |
| BCLC staging (0, A, B, C) | 6, 26, 8, 0 | 0, 0, 0, 9 |
| Recurrence (Yes/No) | 16/24 | 3/6 |
| Types of radiotherapy | ||
| SBRT | 29 | 0 |
| Conventional | 11 | 9 |
| Total dose (Gy) | SBRT 51 (44–60) Conventional 50 (30–50) | 48 (30–50) |
| Dose per fraction (Gy) | SBRT 3 (2–11) Conventional 2 (2–3 Gy) | 2 (2–3) |
| BED to the PTV | SBRT 78.0 (60.0–92.4) Conventional 60.0 (39.0–66.3) | 55.2 (39.0–60.0) |
| EQD2 to the PTV | SBRT 65.0 (50.0–77.0) Conventional 50.0 (32.5–77.0) | 46.0 (32.5–50.0) |
| Mean liver dose (Gy) | SBRT 11.7 (3.3–19.3) Conventional 14.7 (4.1–21.9) | 12.6 (8.2–18.7) |
| V30Gy of the liver | SBRT 11.4 (3.5–28.4) Conventional 18.0 (1.4–40.4) | 19.7 (12.3–34.0) |
| Pre-treatment | ||
| TACE | 17 | 4 |
| RFA | 5 | 0 |
| MTA | 0 | 2 |
| Post-treatment | ||
| TACE | 16 | 6 |
| RFA | 1 | 0 |
| MTA | 6 | 5 |
| Case Number | TACE (Times) | MTA |
|---|---|---|
| 1 | 1 | SOR |
| 2 | 3 | SOR |
| 3 | 1 | LEN |
| 4 | 6 | LEN |
| 5 | 1 | SOR |
| 6 | 2 | - |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Ohkoshi-Yamada, M.; Kamimura, K.; Shibata, O.; Morita, S.; Kaidu, M.; Nakano, T.; Maruyama, K.; Ota, A.; Saito, H.; Yamana, N.; et al. Efficacy and Safety of the Radiotherapy for Liver Cancer: Assessment of Local Controllability and Its Role in Multidisciplinary Therapy. Cancers 2020, 12, 2955. https://doi.org/10.3390/cancers12102955
Ohkoshi-Yamada M, Kamimura K, Shibata O, Morita S, Kaidu M, Nakano T, Maruyama K, Ota A, Saito H, Yamana N, et al. Efficacy and Safety of the Radiotherapy for Liver Cancer: Assessment of Local Controllability and Its Role in Multidisciplinary Therapy. Cancers. 2020; 12(10):2955. https://doi.org/10.3390/cancers12102955
Chicago/Turabian StyleOhkoshi-Yamada, Marina, Kenya Kamimura, Osamu Shibata, Shinichi Morita, Motoki Kaidu, Toshimichi Nakano, Katsuya Maruyama, Atsushi Ota, Hirotake Saito, Nobuko Yamana, and et al. 2020. "Efficacy and Safety of the Radiotherapy for Liver Cancer: Assessment of Local Controllability and Its Role in Multidisciplinary Therapy" Cancers 12, no. 10: 2955. https://doi.org/10.3390/cancers12102955
APA StyleOhkoshi-Yamada, M., Kamimura, K., Shibata, O., Morita, S., Kaidu, M., Nakano, T., Maruyama, K., Ota, A., Saito, H., Yamana, N., Oshikane, T., Goto, Y., Yoshimura, N., Tanabe, S., Nakano, H., Sakai, M., Tanaka, Y., Koseki, Y., Arao, Y., ... Terai, S. (2020). Efficacy and Safety of the Radiotherapy for Liver Cancer: Assessment of Local Controllability and Its Role in Multidisciplinary Therapy. Cancers, 12(10), 2955. https://doi.org/10.3390/cancers12102955






