Differences in Dialysis Efficacy Have Limited Effects on Protein-Bound Uremic Toxins Plasma Levels over Time
Abstract
:1. Introduction
2. Results
2.1. Treatment Effects on Study End-Points
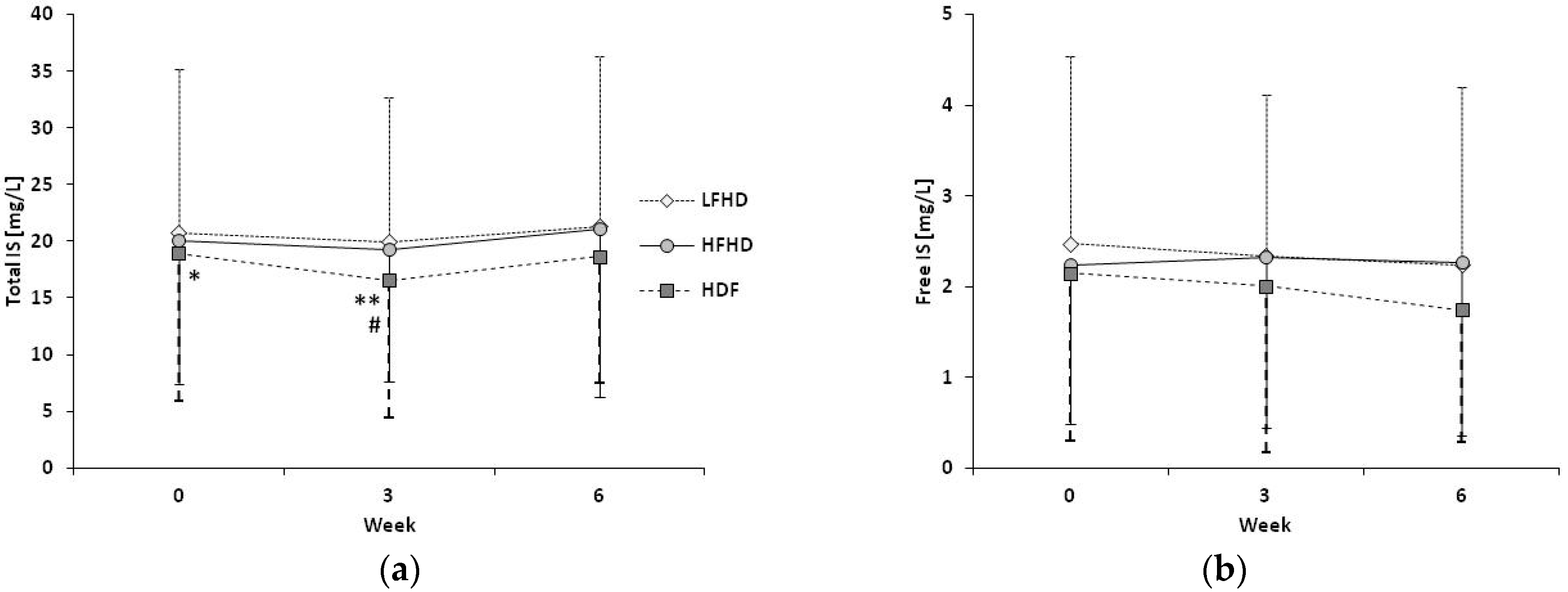
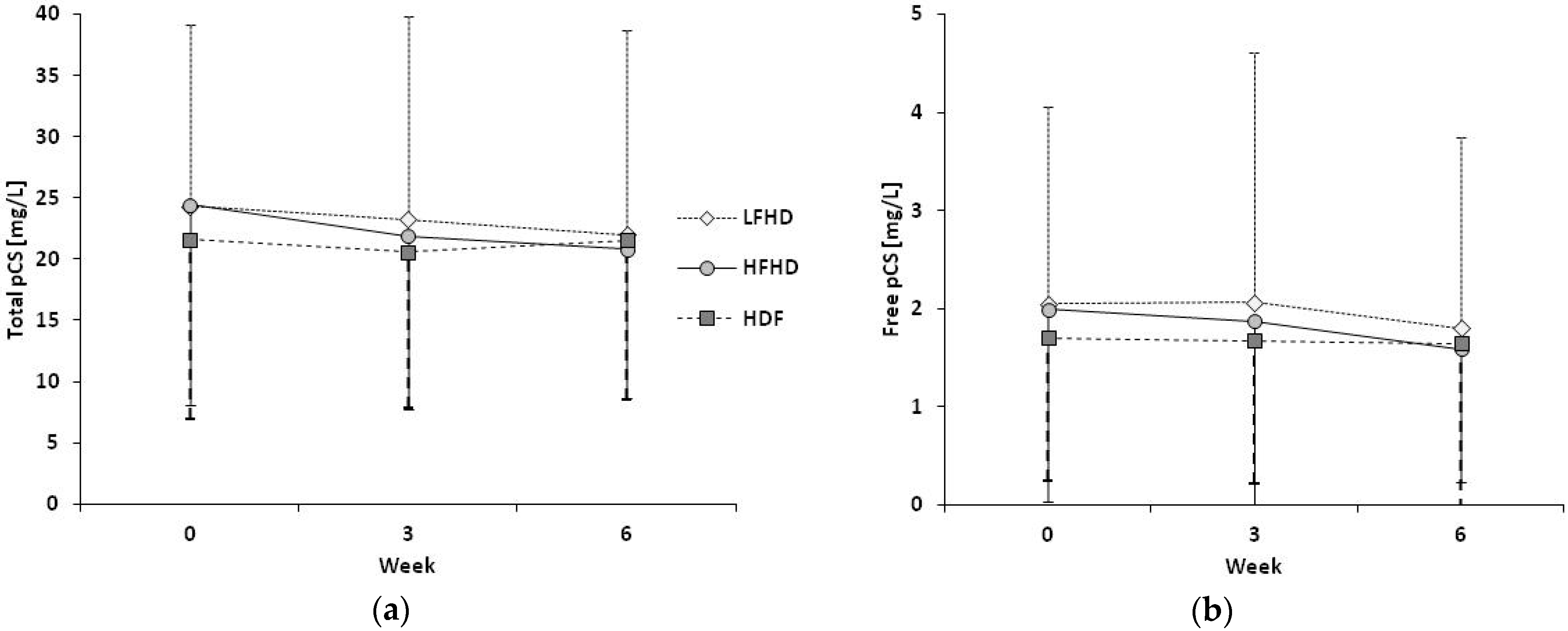
2.1.1. Plasma Concentrations of Toxins over Time
2.1.2. Instantaneous Treatment Efficacy
2.1.3. Other Laboratory Parameters
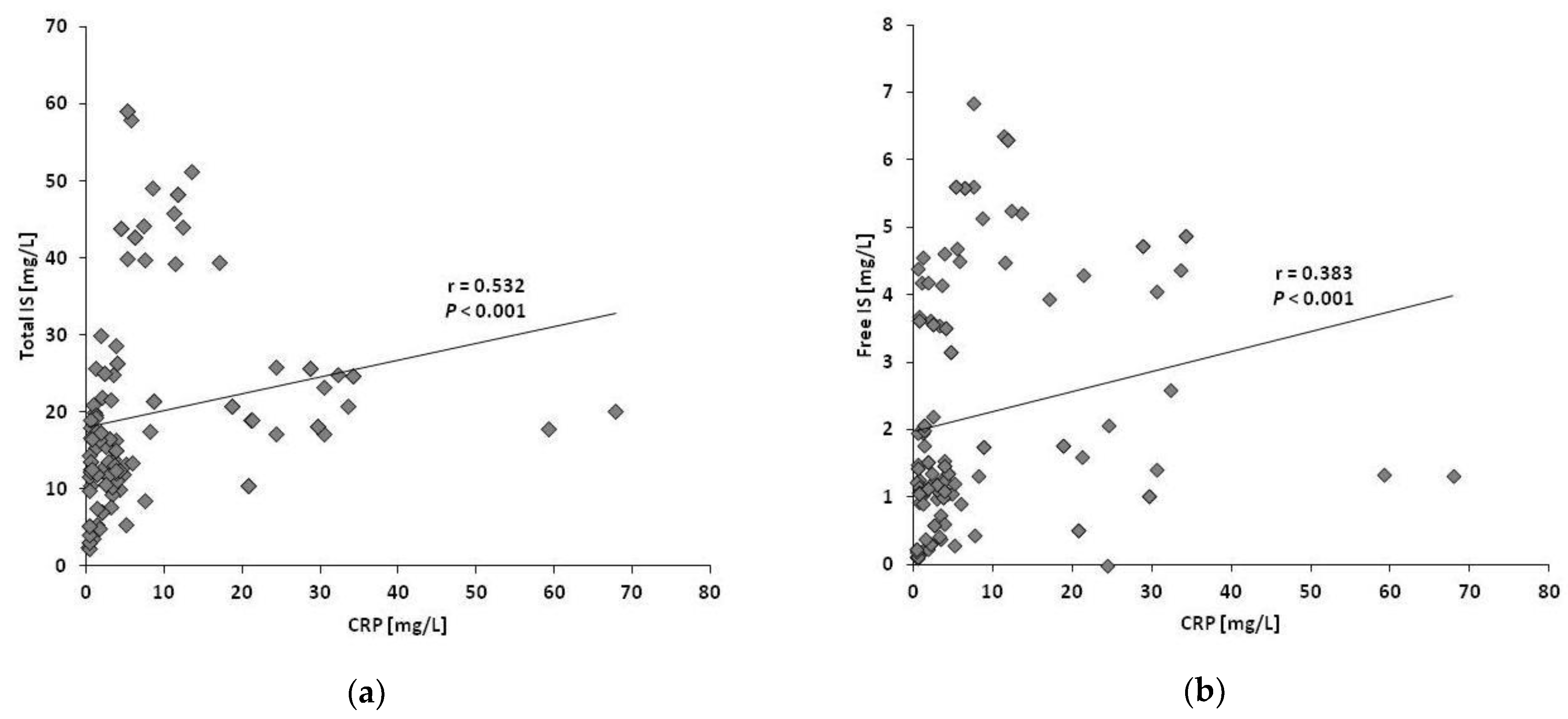
2.1.4. Associations between Parameters
3. Discussion
4. Conclusions
5. Materials and Methods
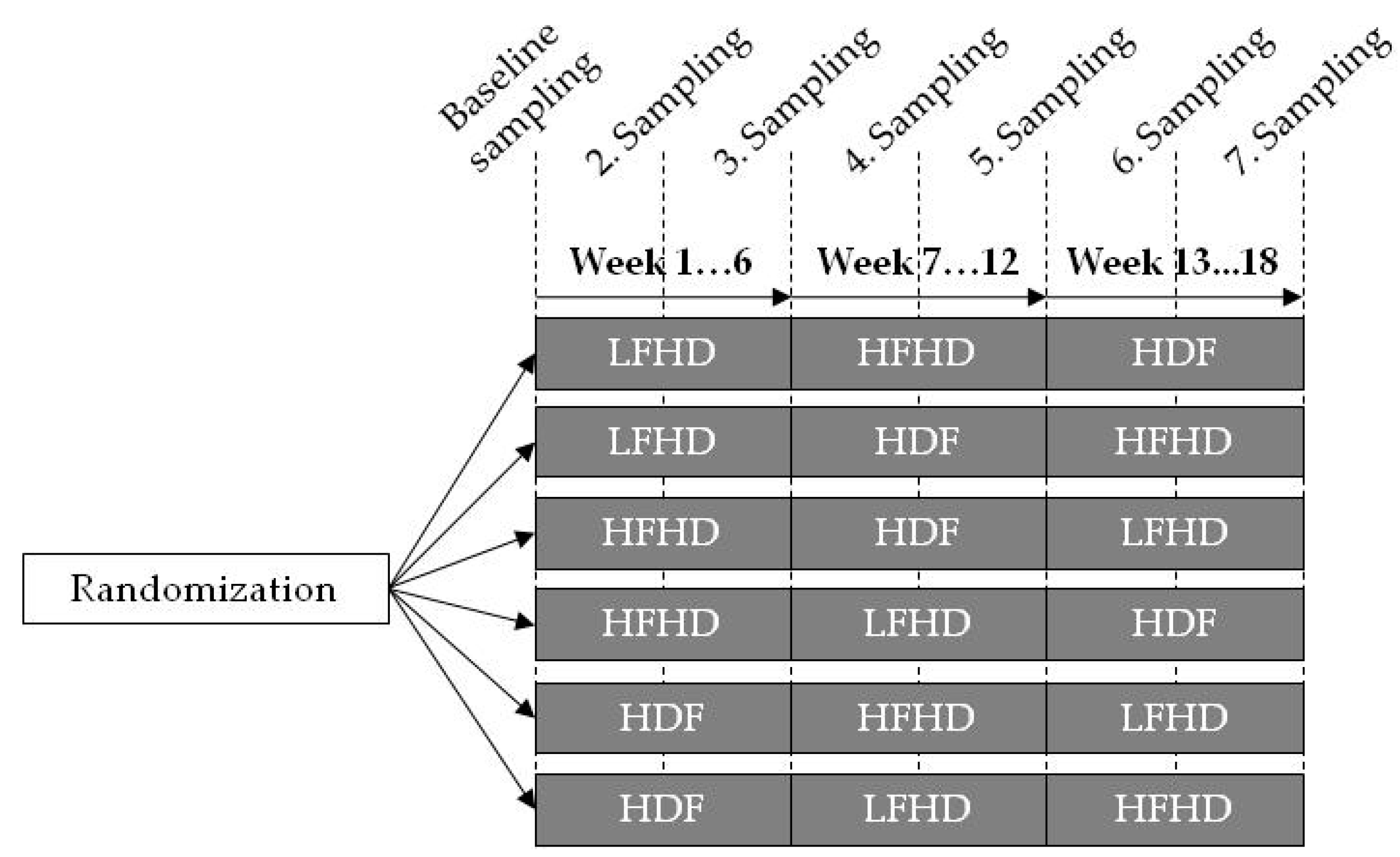
5.1. Study Design
5.2. Monitoring of Treatment Effects
5.3. Analytical Methods
5.4. Data Analysis
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Vanholder, R.; Fouque, D.; Glorieux, G.; Heine, G.H.; Kanbay, M.; Mallamaci, F.; Massy, Z.A.; Ortiz, A.; Rossignol, P.; Wiecek, A.; et al. European Renal Association European Dialysis; Transplant Association (ERA-EDTA) European Renal; Cardiovascular Medicine (EURECA-m) working group. Clinical management of the uraemic syndrome in chronic kidney disease. Lancet Diabetes Endocrinol. 2016, 4, 360–373. [Google Scholar] [CrossRef]
- Vanholder, R.; Pletinck, A.; Schepers, E.; Glorieux, G. Biochemical and Clinical Impact of Organic Uremic Retention Solutes: A Comprehensive Update. Toxins (Basel) 2018, 10, E33. [Google Scholar] [CrossRef] [PubMed]
- Böhringer, F.; Jankowski, V.; Gajjala, P.R.; Zidek, W.; Jankowski, J. Release of uremic retention solutes from protein binding by hypertonic predilution hemodiafiltration. ASAIO J. 2015, 61, 55–60. [Google Scholar] [CrossRef] [PubMed]
- Krieter, D.H.; Devine, E.; Körner, T.; Rüth, M.; Wanner, C.; Raine, M.; Jankowski, J.; Lemke, H.D. Haemodiafiltration at increased plasma ionic strength for improved protein-bound toxin removal. Acta Physiol. 2017, 219, 510–520. [Google Scholar] [CrossRef] [PubMed]
- Pavlenko, D.; van Geffen, E.; van Steenbergen, M.J.; Glorieux, G.; Vanholder, R.; Gerritsen, K.G.; Stamatialis, D. New low-flux mixed matrix membranes that offer superior removal of protein-bound toxins from human plasma. Sci. Rep. 2016, 6, 34429. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Sandeman, S.R.; Zheng, Y.; Ingavle, G.C.; Howell, C.A.; Mikhalovsky, S.V.; Basnayake, K.; Boyd, O.; Davenport, A.; Beaton, N.; Davies, N. A haemocompatible and scalable nanoporous adsorbent monolith synthesised using a novel lignin binder route to augment the adsorption of poorly removed uraemic toxins in haemodialysis. Biomed. Mater. 2017, 12, 035001. [Google Scholar] [CrossRef] [Green Version]
- Yamamoto, S.; Sato, M.; Sato, Y.; Wakamatsu, T.; Takahashi, Y.; Iguchi, A.; Omori, K.; Suzuki, Y.; Ei, I.; Kaneko, Y.; et al. Adsorption of protein-bound uremic toxins through direct hemoperfusion with hexadecyl-immobilized cellulose beads in patients undergoing hemodialysis. Artif. Organs 2018, 42, 88–93. [Google Scholar] [CrossRef]
- Luo, F.J.; Patel, K.P.; Marquez, I.O.; Plummer, N.S.; Hostetter, T.H.; Meyer, T.W. Effect of increasing dialyzer mass transfer area coefficient and dialysate flow on clearance of protein-bound solutes: A pilot crossover trial. Am. J. Kidney Dis. 2009, 53, 1042–1049. [Google Scholar] [CrossRef]
- Cornelis, T.; Eloot, S.; Vanholder, R.; Glorieux, G.; van der Sande, F.M.; Scheijen, J.L.; Leunissen, K.M.; Kooman, J.P.; Schalkwijk, C.G. Protein-bound uraemic toxins, dicarbonyl stress and advanced glycation end products in conventional and extended haemodialysis and haemodiafiltration. Nephrol. Dial. Transplant. 2015, 30, 1395–1402. [Google Scholar] [CrossRef] [Green Version]
- Camacho, O.; Rosales, M.C.; Shafi, T.; Fullman, J.; Plummer, N.S.; Meyer, T.W.; Sirich, T.L. Effect of a sustained difference in hemodialytic clearance on the plasma levels of p-cresol sulfate and indoxyl sulfate. Nephrol. Dial. Transplant. 2016, 31, 1335–1341. [Google Scholar] [CrossRef] [Green Version]
- Abad, S.; Vega, A.; Quiroga, B.; Arroyo, D.; Panizo, N.; Reque, J.E.; López-Gómez, J.M. Protein-bound toxins: Added value in their removal with high convective volumes. Nefrologia 2016, 36, 637–642. [Google Scholar] [CrossRef] [PubMed]
- Lin, C.J.; Wu, V.; Wu, P.C.; Wu, C.J. Meta-Analysis of the Associations of p-Cresyl Sulfate (PCS) and Indoxyl Sulfate (IS) with Cardiovascular Events and All-Cause Mortality in Patients with Chronic Renal Failure. PLoS ONE 2015, 10, e0132589. [Google Scholar] [CrossRef]
- Meert, N.; Waterloos, M.A.; Van Landschoot, M.; Dhondt, A.; Ledebo, I.; Glorieux, G.; Goeman, J.; Van der Eycken, J.; Vanholder, R. Prospective evaluation of the change of predialysis protein-bound uremic solute concentration with postdilution online hemodiafiltration. Artif. Organs 2010, 34, 580–585. [Google Scholar] [CrossRef] [PubMed]
- Panichi, V.; Rocchetti, M.T.; Scatena, A.; Rosati, A.; Migliori, M.; Pizzarelli, F.; Gesualdo, L.; REDERT Study group. Long term variation of serum levels of uremic toxins in patients treated by post-dilution high volume on-line hemodiafiltration in comparison to standard low-flux bicarbonate dialysis: Results from the REDERT study. J. Nephrol. 2017, 30, 583–591. [Google Scholar] [CrossRef]
- Canaud, B.; Vienken, J.; Ash, S.; Ward, R.A.; Kidney Health Initiative HDF Workgroup. Hemodiafiltration to address unmet medical needs ESKD Patients. Clin. J. Am. Soc. Nephrol. 2018, 13, 1435–1443. [Google Scholar] [CrossRef] [PubMed]
- Bammens, B.; Evenepoel, P.; Verbeke, K.; Vanrenterghem, Y. Removal of the protein-bound solute p-cresol by convective transport: A randomized crossover study. Am. J. Kidney Dis. 2004, 44, 278–285. [Google Scholar] [CrossRef] [PubMed]
- Meert, N.; Beerenhout, C.; Schepers, E.; Glorieux, G.; Kooman, J.; Vanholder, R. Evolution of protein-bound uraemic solutes during predilution haemofiltration. J. Nephrol. 2009, 22, 352–357. [Google Scholar]
- Grooteman, M.P.; van den Dorpel, M.A.; Bots, M.L.; Penne, E.L.; van der Weerd, N.C.; Mazairac, A.H.; den Hoedt, C.H.; van der Tweel, I.; Lévesque, R.; Nubé, M.J.; et al. Effect of online hemodiafiltration on all-cause mortality and cardiovascular outcomes. J. Am. Soc. Nephrol. 2012, 23, 1087–1096. [Google Scholar] [CrossRef]
- Jean, G.; Hurot, J.M.; Deleaval, P.; Mayor, B.; Lorriaux, C. Online-haemodiafiltration vs. conventional haemodialysis: A cross-over study. BMC Nephrol. 2015, 16, 70. [Google Scholar] [CrossRef]
- Eloot, S.; van Biesen, W.; Glorieux, G.; Neirynck, N.; Dhondt, A.; Vanholder, R. Does the adequacy parameter Kt/V(urea) reflect uremic toxin concentrations in hemodialysis patients? PLoS ONE 2013, 13, e76838. [Google Scholar] [CrossRef]
- Kandouz, S.; Mohamed, A.S.; Zheng, Y.; Sandeman, S.; Davenport, A. Reduced protein bound uraemic toxins in vegetarian kidney failure patients treated by haemodiafiltration. Hemodial Int. 2016, 20, 610–617. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Eloot, S.; Van Biesen, W.; Roels, S.; Delrue, W.; Schepers, E.; Dhondt, A.; Vanholder, R.; Glorieux, G. Spontaneous variability of pre-dialysis concentrations of uremic toxins over time in stable hemodialysis patients. PLoS ONE 2017, 12, e0186010. [Google Scholar] [CrossRef]
- Smith, J.R.; Zimmer, N.; Bell, E.; Francq, B.G.; McConnachie, A.; Mactier, R. A Randomized, Single-Blind, Crossover Trial of Recovery Time in High-Flux Hemodialysis and Hemodiafiltration. Am. J. Kidney Dis. 2017, 69, 762–770. [Google Scholar] [CrossRef]
- Viaene, L.; Annaert, P.; de Loor, H.; Poesen, R.; Evenepoel, P.; Meijers, B. Albumin is the main plasma binding protein for indoxyl sulfate and p-cresyl sulfate. Biopharm. Drug Dispos. 2013, 34, 165–175. [Google Scholar] [CrossRef]
- Rippe, B.; Öberg, C.M. Albumin turnover in peritoneal and hemodialysis. Semin. Dial. 2016, 29, 458–462. [Google Scholar] [CrossRef] [PubMed]
- Hsu, H.J.; Yen, C.H.; Wu, I.W.; Hsu, K.H.; Chen, C.K.; Sun, C.Y.; Chou, C.C.; Chen, C.Y.; Tsai, C.J.; Wu, M.S.; et al. The association of uremic toxins and inflammation in hemodialysis patients. PLoS ONE 2014, 9, e102691. [Google Scholar] [CrossRef] [PubMed]
- Velasquez, M.T.; Centron, P.; Barrows, I.; Dwivedi, R.; Raj, D.S. Gut microbiota and cardiovascular uremic toxicities. Toxins (Basel) 2018, 10, E287. [Google Scholar] [CrossRef] [PubMed]
- Mair, R.D.; Sirich, T.L.; Meyer, T.W. Uremic toxin clearance and cardiovascular toxicities. Toxins (Basel) 2018, 10, E226. [Google Scholar] [CrossRef]
- Saito, A.; Sawada, K.; Fujimura, S.; Suzuki, H.; Hirukawa, T.; Tatsumi, R.; Kanai, G.; Takahashi, H.; Miyakogawa, T.; Sanechika, N.; et al. Evaluation of bioartificial renal tubule device prepared with lifespan-extended human renal proximal tubular epithelial cells. Nephrol. Dial. Transplant. 2012, 27, 3091–3099. [Google Scholar] [CrossRef] [Green Version]
- Yamamoto, S.; Kazama, J.J.; Omori, K.; Matsuo, K.; Takahashi, Y.; Kawamura, K.; Matsuto, T.; Watanabe, H.; Maruyama, T.; Narita, I. Continuous Reduction of protein-bound uraemic toxins with improved oxidative stress by using the oral charcoal adsorbent AST-120 in haemodialysis patients. Sci. Rep. 2015, 5, 14381. [Google Scholar] [CrossRef]
- Daugirdas, J.T. Second generation logarithmic estimates of single-pool variable volume Kt/V: An analysis of error. J. Am. Soc. Nephrol. 1993, 4, 1205–1213. [Google Scholar] [PubMed]
- Krieter, D.H.; Hackl, A.; Rodriguez, A.; Chenine, L.; Moragues, H.L.; Lemke, H.D.; Wanner, C.; Canaud, B. Protein-bound uraemic toxin removal in haemodialysis and post-dilution haemodiafiltration. Nephrol. Dial. Transplant. 2010, 25, 212–218. [Google Scholar] [CrossRef] [PubMed]
| Characteristic | Result |
|---|---|
| Age—years | 67.7 ± 12.0 |
| Female sex—no. (%) | 4 (28.6) |
| Renal disease—no. (%) | |
| Glomerulonephritis | 4 (28.6) |
| Diabetic nephropathy | 4 (28.6) |
| Hypertensive nephropathy | 2 (14.3) |
| Urate nephropathy | 1 (7.1) |
| Tubulo-interstitial nephritis | 1 (7.1) |
| Renal ischemia | 1 (7.1) |
| Unknown | 1 (7.1) |
| Dialysis vintage—months | 84.6 ± 28.0 |
| Smoker—no. (%) | 3 (21.4) |
| Residual renal function—no. (%) | 5 (35.7) |
| Diabetes mellitus—no. (%) | 5 (35.7) |
| History of cardiovascular disease—no. (%) | |
| Myocardial infarction | 2 (14.3) |
| Coronary heart disease | 3 (21.4) |
| Congestive heart failure | 1 (7.1) |
| Cardiac valve disorder | 1 (7.1) |
| Peripheral vascular disease | 8 (57.1) |
| Stroke or transient ischemic attack | 2 (14.3) |
| Body weight—kg | 79.5 ± 6.4 |
| Hemoglobin—g/dl | 11.4 ± 0.7 |
| Albumin—g/L | 34.7 ± 2.7 |
| C-reactive protein—mg/L | 6.4 ± 8.9 |
| Calcium—mmol/L | 2.34 ± 0.17 |
| Phosphate—mmol/L | 1.41 ± 0.41 |
| CRP [mg/L] | Albumin [g/L] | b2M [mg/L] | |||||||
|---|---|---|---|---|---|---|---|---|---|
| Week 0 | Week 3 | Week 6 | Week 0 | Week 3 | Week 6 | Week 0 | Week 3 | Week 6 | |
| LFHD | 7.1 ± 9.0 | 7.9 ± 9.9 | 11.4 ± 19.2 | 36.0 ± 4.0 | 35.8 ± 3.8 1 | 38.2 ± 4.9 2 | 23.7 ± 7.4 | 34.0 ± 13.5 4 | 35.7 ± 14.4 4 |
| HFHD | 7.1 ± 8.8 | 9.7 ± 16.5 | 7.7 ± 10.4 | 35.5 ± 3.3 | 34.9 ± 3.4 1 | 37.1 ± 4.3 | 27.1 ± 11.9 | 23.8 ± 7.7 | 24.5 ± 7.4 |
| HDF | 7.1 ± 10.8 | 7.5 ± 9.2 | 5.1 ± 7.2 | 35.5 ± 4.7 | 33.8 ± 3.8 3 | 36.7 ± 4.7 | 28.7 ± 13.1 | 22.2 ± 6.4 2 | 22.4 ± 6.2 2 |
| Parameter | LFHD | HFHD | HDF | |||
|---|---|---|---|---|---|---|
| Week 0 | Week 3 | Week 0 | Week 3 | Week 0 | Week 3 | |
| Reduction Ratio [%] | ||||||
| total IS | 36.5 ± 10.7 | 34.3 ± 8.2 | 35.9 ± 8.7 | 37.0 ± 10.5 | 48.1 ± 9.6 1 | 46.0 ± 18.3 1 |
| free IS | 48.3 ± 11.6 | 44.0 ± 16.1 | 49.8 ± 12.7 | 49.4 ± 20.0 | 60.8 ± 10.4 1 | 56.3 ± 23.1 2 |
| total pCS | 30.7 ± 11.9 | 29.4 ± 7.3 | 29.7 ± 10.8 | 30.8 ± 10.6 | 42.8 ± 10.0 1 | 39.1 ± 20.6 1 |
| free pCS | 43.5 ± 13.9 | 40.0 ± 16.4 | 47.1 ± 13.6 | 47.8 ± 18.6 | 58.9 ± 10.6 1 | 52.3 ± 25.9 2 |
| b2M | −1.9 ± 8.0 | −0.3 ± 6.7 | 60.6 ± 6.0 3 | 60.6 ± 6.0 3 | 77.9 ± 4.9 1 | 78.4 ± 5.1 1 |
| Dialytic Clearance [mL/min] | ||||||
| total IS | 20 ± 16 | 21 ± 14 | 25 ± 18 4 | 26 ± 24 | 30 ± 23 4 | 23 ± 23 |
| total pCS | 18 ± 16 | 18 ± 16 | 24 ± 19 | 23 ± 21 | 26 ± 18 4 | 25 ± 19 |
| b2M | 8 ± 0 | 8 ± 1 | 33 ± 19 3 | 33 ± 20 3 | 52 ± 27 1 | 49 ± 24 1 |
| Mass in Dialysate [mg] | ||||||
| total IS | 73 ± 64 | 76 ± 57 | 93 ± 72 | 97 ± 97 | 110 ± 91 | 89 ± 90 |
| total pCS | 70 ± 65 | 70 ± 66 | 92 ± 80 | 87 ± 84 | 96 ± 72 | 92 ± 76 |
| b2M | 30 ± 2 | 30 ± 2 | 124 ± 78 3 | 121 ± 78 2 | 190 ± 108 1 | 174 ± 87 2 |
| spKt/V | ||||||
| urea | 1.53 ± 0.31 | 1.59 ± 0.29 | 1.69 ± 0.27 3 | 1.68 ± 0.35 | 2.01 ± 0.35 1 | 2.03 ± 0.33 1 |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Krieter, D.H.; Kerwagen, S.; Rüth, M.; Lemke, H.-D.; Wanner, C. Differences in Dialysis Efficacy Have Limited Effects on Protein-Bound Uremic Toxins Plasma Levels over Time. Toxins 2019, 11, 47. https://doi.org/10.3390/toxins11010047
Krieter DH, Kerwagen S, Rüth M, Lemke H-D, Wanner C. Differences in Dialysis Efficacy Have Limited Effects on Protein-Bound Uremic Toxins Plasma Levels over Time. Toxins. 2019; 11(1):47. https://doi.org/10.3390/toxins11010047
Chicago/Turabian StyleKrieter, Detlef H., Simon Kerwagen, Marieke Rüth, Horst-Dieter Lemke, and Christoph Wanner. 2019. "Differences in Dialysis Efficacy Have Limited Effects on Protein-Bound Uremic Toxins Plasma Levels over Time" Toxins 11, no. 1: 47. https://doi.org/10.3390/toxins11010047
APA StyleKrieter, D. H., Kerwagen, S., Rüth, M., Lemke, H.-D., & Wanner, C. (2019). Differences in Dialysis Efficacy Have Limited Effects on Protein-Bound Uremic Toxins Plasma Levels over Time. Toxins, 11(1), 47. https://doi.org/10.3390/toxins11010047





