Activities, Participation and Quality of Life Concepts in Children and Adolescents with Celiac Disease: A Scoping Review
Abstract
1. Introduction
2. Materials and Methods
2.1. Identifying the Research Question
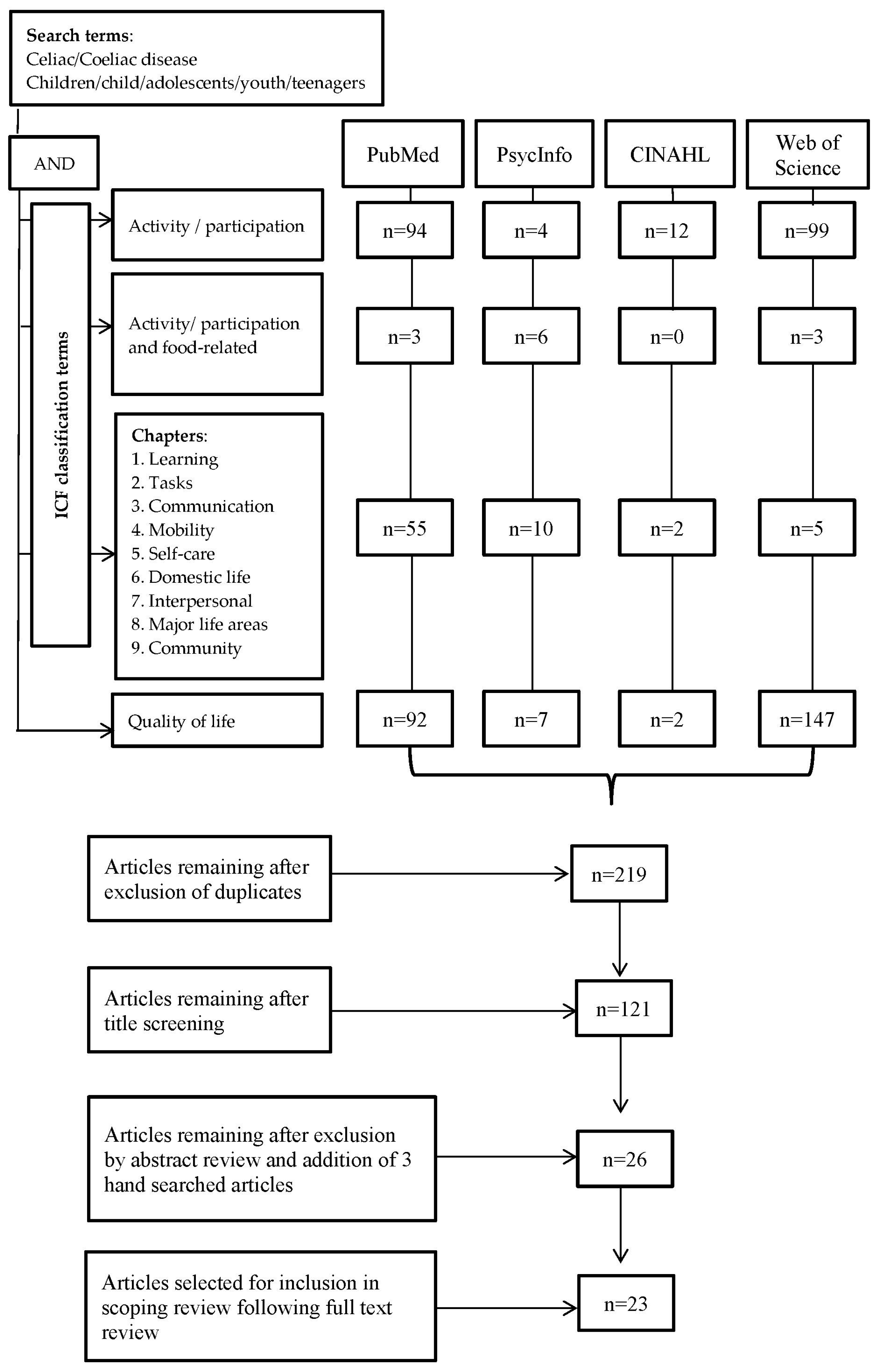
2.2. Identifying Relevant Studies and Study Selection
2.3. Study Selection
2.4. Charting the Data
3. Results
3.1. Study Populations
3.2. Study Objectives
3.3. Study Methods and Tools
3.4. Activities and Participation in Food-Related Activities
3.4.1. Community, Social, and Civic life
3.4.2. Major Life Areas
3.4.3. Self-Care
3.4.4. Communication
3.4.5. Domestic Life, Interpersonal Interactions, and Relationships and General Tasks and Demands
4. Discussion
5. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Green, P.H.R.; Cellier, C. Celiac disease. N. Engl. J. Med. 2007, 357, 1731–1743. [Google Scholar] [CrossRef] [PubMed]
- Byass, P.; Kahn, K.; Ivarsson, A. The global burden of childhood coeliac disease: A neglected component of diarrhoeal mortality? PLoS ONE 2011, 6, e22774. [Google Scholar] [CrossRef] [PubMed]
- Ciccocioppo, R.; Kruzliak, P.; Cangemi, G.C.; Pohanka, M.; Betti, E.; Lauret, E.; Rodrigo, L. The spectrum of differences between childhood and adulthood celiac disease. Nutrients 2015, 7, 8733–8751. [Google Scholar] [CrossRef] [PubMed]
- Newton, K.P.; Singer, S.A. Celiac disease in children and adolescents: Special considerations. Semin. Immunol. 2012, 34, 479–496. [Google Scholar] [CrossRef] [PubMed]
- Haines, M.; Anderson, R.; Gibson, P. Systematic review: The evidence base for long-term management of coeliac disease. Aliment. Pharmacol. Ther. 2008, 28, 1042–1066. [Google Scholar] [CrossRef] [PubMed]
- Ludvigsson, J.F.; Agreus, L.; Ciacci, C.; Crowe, S.E.; Geller, M.G.; Green, P.H.; Hill, I.; Hungin, A.P.; Koletzko, S.; Koltai, T.; et al. Transition from childhood to adulthood in coeliac disease: The Prague consensus report. Gut 2016, 65, 1242–1251. [Google Scholar] [CrossRef] [PubMed]
- Errichiello, S.; Esposito, O.; Di Mase, R.; Camarca, M.E.; Natale, C.; Limongelli, M.G.; Marano, C.; Coruzzo, A.; Lombardo, M.; Strisciuglio, P.; Greco, L. Celiac disease: Predictors of compliance with a gluten-free diet in adolescents and young adults. J. Pediatr. Gastroenterol. Nutr. 2010, 50, 54–60. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. International Classification of Functioning, Disability, and Health: ICF; World Health Organization: Geneva, Switzerland, 2001. [Google Scholar]
- World Health Organization. International Classification of Functioning, Disability and Health: Children & Youth Version: ICF-CY; World Health Organization: Geneva, Switzerland, 2007. [Google Scholar]
- McDougall, J.; Wright, V.; Schmidt, J.; Miller, L.; Lowry, K. Applying the ICF framework to study changes in quality-of-life for youth with chronic conditions. Dev. Neurorehabil. 2011, 14, 41–53. [Google Scholar] [CrossRef] [PubMed]
- Anaby, D.; Law, M. The role of participation in the lives of children and young people with neurological and developmental conditions. In Life Quality Outcomes in Children and Young People with Neurological and Developmental Conditions; Ronen, G., Rosenbaum, P., Eds.; Mac Keith Press: London, UK, 2013; pp. 51–64. [Google Scholar]
- Cieza, A.; Fayed, N.; Bickenbach, J.; Prodinger, B. Refinements of the ICF Linking Rules to strengthen their potential for establishing comparability of health information. Disabil. Rehabil. 2016. [Google Scholar] [CrossRef] [PubMed]
- Meyer, S.; Rosenblum, S. Children with celiac disease: Health-related quality of life and leisure participation. Am. J. Occup. Ther. 2016, 70, 7006220010p1–7006220010p8. [Google Scholar] [CrossRef] [PubMed]
- Fayers, P.M.; Machin, D. Developing and validating instruments for assessing quality of life and patient-reported outcomes. In Quality of Life: The Assessment, Analysis and Reporting of Patient-Reported Outcomes; Fayers, P.M., Machin, D., Eds.; John Wiley & Sons: Chichester, UK, 2016; pp. 3–34. [Google Scholar]
- Renwick, R. Quality of life for young people with neurological and developmental conditions: Issues and challenges. In Life Quality Outcomes in Children and Young People with Neurological and Developmental Conditions; Ronen, G., Rosenbaum, P., Eds.; Mac Keith Press: London, UK, 2013; pp. 22–35. [Google Scholar]
- Van Doorn, R.K.; Winkler, L.M.; Zwinderman, K.H.; Mearin, M.L.; Koopman, H.M. CDDUX: A disease-specific health-related quality-of-life questionnaire for children with celiac disease. J. Pediatr. Gastroenterol. Nutr. 2008, 47, 147–152. [Google Scholar] [CrossRef] [PubMed]
- Byström, I.M.; Hollén, E.; Fälth-Magnusson, K.; Johansson, A.K. Health-related quality of life in children and adolescents with celiac disease: From the perspectives of children and parents. Gastroenterol. Res. Pract. 2012. [Google Scholar] [CrossRef] [PubMed]
- Biagetti, C.; Naspi, G.; Catassi, C. Health-related quality of life in children with celiac disease: A study based on the critical incident technique. Nutrients 2013, 5, 4476–4485. [Google Scholar] [CrossRef] [PubMed]
- Jordan, N.E.; Li, Y.; Magrini, D.; Simpson, S.; Reilly, N.R.; Defelice, A.R.; Sockolow, R.; Green, P.H.R. Development and validation of a celiac disease quality of life instrument for North American children. J. Pediatr. Gastroenterol. Nutr. 2013, 57, 477–486. [Google Scholar] [CrossRef] [PubMed]
- Cieza, A.; Stucki, G. The international classification of functioning disability and health: Its development process and content validity. Eur. J. Phys. Rehabil. Med. 2008, 44, 303–313. [Google Scholar] [PubMed]
- White, L.; Bannerman, E.; Gillett, P. Coeliac disease and the gluten-free diet: A review of the burdens; factors associated with adherence and impact on health-related quality of life, with specific focus on adolescence. J. Hum. Nutr. Diet. 2016, 29, 593–606. [Google Scholar] [CrossRef] [PubMed]
- Howard, R.A.; Urquhart-Law, G. Psychological well-being of children and young people with coeliac disease. In Paediatric Gastrointestinal Disorders: A Psychosocial Perspective; Martin, C., Dovey, T., Eds.; Radcliffe Publishing Ltd.: London, UK, 2014; pp. 186–207. [Google Scholar]
- Colquhoun, H.L.; Levac, D.; O’Brien, K.K.; Straus, S.; Tricco, A.C.; Perrier, L.; Kastner, M.; Moher, D. Scoping reviews: Time for clarity in definition, methods, and reporting. J. Clin. Epidemiol. 2014, 67, 1291–1294. [Google Scholar] [CrossRef] [PubMed]
- Levac, D.; Colquhoun, H.; O′Brien, K.K. Scoping studies: Advancing the methodology. Implement. Sci. 2010, 5, 69. [Google Scholar] [CrossRef] [PubMed]
- Bacigalupe, G.; Plocha, A. Celiac is a social disease: Family challenges and strategies. Fam. Syst. Health 2015, 33, 46–54. [Google Scholar] [CrossRef] [PubMed]
- Barrio, J.; Roman, E.; Cilleruelo, M.; Marquez, M.; Mearin, M.L.; Fernandez, C. Health-related quality of life in Spanish children with coeliac disease. J. Pediatr. Gastroenterol. Nutr. 2016, 62, 603–608. [Google Scholar] [CrossRef] [PubMed]
- Biagetti, C.; Gesuita, R.; Gatti, S.; Catassi, C. Quality of life in children with celiac disease: A paediatric cross-sectional study. Dig. Liver Dis. 2015, 47, 927–932. [Google Scholar] [CrossRef] [PubMed]
- Chauhan, J.C.; Kumar, P.; Dutta, A.K.; Basu, S.; Kumar, A. Assessment of dietary compliance to gluten free diet and psychosocial problems in Indian children with celiac disease. Indian J. Pediatr. 2010, 77, 649–654. [Google Scholar] [CrossRef] [PubMed]
- De Lorenzo, C.M.; Xikota, J.C.; Wayhs, M.C.; Nassar, S.M.; de Souza Pires, M.M. Evaluation of the quality of life of children with celiac disease and their parents: A case–control study. Qual. Life Res. 2012, 21, 77–85. [Google Scholar] [CrossRef] [PubMed]
- MacCulloch, K.; Rashid, M. Factors affecting adherence to a gluten-free diet in children with celiac disease. Paediatr. Child Health 2014, 19, 305–309. [Google Scholar] [CrossRef] [PubMed]
- Pico, M.; Spirito, M.F. Implementation of a health-related quality of life questionnaire for children and adolescents with celiac disease. Arch. Argent. Pediatr. 2014, 112, 19–25. [Google Scholar] [PubMed]
- Rosén, A.; Ivarsson, A.; Nordyke, K.; Karlsson, E.; Carlsson, A.; Danielsson, L.; Högberg, L.; Emmelin, M. Balancing health benefits and social sacrifices: A qualitative study of how screening-detected celiac disease impacts adolescents′ quality of life. BMC Pediatr. 2011, 11, 1–10. [Google Scholar] [CrossRef] [PubMed]
- Skjerning, H.; Mahony, R.O.; Husby, S.; DunnGalvin, A. Health-related quality of life in children and adolescents with celiac disease: Patient-driven data from focus group interviews. Qual. Life Res. 2014, 23, 1883–1894. [Google Scholar] [CrossRef] [PubMed]
- Veen, M.; te Molder, H.; Gremmen, B.; van Woerkum, C. If you can′t eat what you like, like what you can: How coeliac disease patients and their families construct dietary restrictions as a matter of choice. Sociol. Health Illn. 2013, 35, 592–609. [Google Scholar] [CrossRef] [PubMed]
- Altobelli, E.; Paduano, R.; Gentile, T.; Caloisi, C.; Marziliano, C.; Necozione, S.; di Orio, F. Health-related quality of life in children and adolescents with celiac disease: Survey of a population from central Italy. Health Qual. Life Outcomes 2013, 11, 204. [Google Scholar] [CrossRef] [PubMed]
- Bellini, A.; Zanchi, C.; Martelossi, S.; Di Leo, G.; Not, T.; Ventura, A. Compliance with the gluten-free diet: The role of locus of control in celiac disease. J. Pediatr. 2011, 158, 463–466. [Google Scholar] [CrossRef] [PubMed]
- Bongiovanni, T.R.; Clark, A.L.; Garnett, E.A.; Wojcicki, J.M.; Heyman, M.B. Impact of gluten-free camp on quality of life of children and adolescents with celiac disease. Pediatrics 2010, 125, e525–e529. [Google Scholar] [CrossRef] [PubMed]
- Olsson, C.; Lyon, P.; Hornell, A.; Ivarsson, A.; Sydner, Y.M. Food that makes you different: The stigma experienced by adolescents with celiac disease. Qual. Health Res. 2009, 19, 976–984. [Google Scholar] [CrossRef] [PubMed]
- Roma, E.; Roubani, A.; Kolia, E.; Panayiotou, J.; Zellos, A.; Syriopoulou, V.P. Dietary compliance and life style of children with coeliac disease. J. Hum. Nutr. Diet. 2010, 23, 176–182. [Google Scholar] [CrossRef] [PubMed]
- Cederborg, A.; Hultman, E.; Magnusson, K. Living with children who have coeliac disease: A parental perspective. Child Care Health Dev. 2012, 38, 484–489. [Google Scholar] [CrossRef] [PubMed]
- Arnone, J.; Fitzsimons, V. Adolescents with celiac disease: A literature review of the impact developmental tasks have on adherence with a gluten-free diet. Gastroenterol. Nurs. 2012, 35, 248–254. [Google Scholar] [CrossRef] [PubMed]
- Lins, M.T.C.; Tassitano, R.M.; Brandt, K.G.; de Castro Antunes, M.M.; da Silva, G.A.P. Translation, cultural adaptation, and validation of the celiac disease DUX (CDDUX). J. Pediatr. 2015, 91, 448–454. [Google Scholar] [CrossRef] [PubMed]
- Olsson, C.; Hörnell, A.; Ivarsson, A.; Sydner, Y.M. The everyday life of adolescent Coeliacs: Issues of importance for compliance with the gluten-free diet. J. Hum. Nutr. Diet. 2008, 21, 359–367. [Google Scholar] [CrossRef] [PubMed]
- Simeonsson, R.T.; Lollar, D.; Leonardi, R.J.S.M.; Bjorck-Akesson, E.; Hollenweger, J.; Martinuzzi, A. Applying the International Classification of Functioning, Disability and Health (ICF) to measure childhood disability. Disabil. Rehabil. 2003, 25, 602–610. [Google Scholar] [CrossRef] [PubMed]
- Kurppa, K.; Collin, P.; Maki, M.; Kaukinen, K. Celiac disease and health-related quality of life. Expert Rev. Gastroenterol. Hepatol. 2011, 5, 83–90. [Google Scholar] [CrossRef] [PubMed]
- Coster, W.; Khetani, M.A. Measuring participation of children with disabilities: Issues and challenges. Disabil. Rehabil. 2008, 30, 639–648. [Google Scholar] [CrossRef] [PubMed]
- Barrio Torres, J.; Cilleruelo-Pascual, M.L.; Riechmann, E.R.; Fernandez, C.; Mearin, L. Health related quality of life: Cross-cultural differences. In Proceedings of the 50th ESPGHAN Annual Meeting of the European Society for Paediatric Gastroenterology, Hepatology and Nutrition, Prague, Czech Republic, 10–13 May 2017; ESPGHAN: Vienna, Austria, 2017; p. 181. [Google Scholar]
- Varni, J.W.; Limbers, C.A.; Newman, D.A. Using factor analysis to confirm the validity of children’s self-reported health-related quality of life across different modes of administration. Clin. Trials 2009, 6, 185–195. [Google Scholar] [CrossRef] [PubMed]
- Sisk, C. Promoting children′s health-related quality of life. Pediatr. Nurs. 2016, 42, 86–88. [Google Scholar] [PubMed]
- Imms, C.; Adair, B.; Keen, D.; Ullenhag, A.; Rosenbaum, P.; Granlund, M. ‘Participation’: A systematic review of language, definitions, and constructs used in intervention research with children with disabilities. Dev. Med. Child Neurol. 2016, 28, 29–38. [Google Scholar] [CrossRef] [PubMed]
- Adolfsson, M.; Granlund, M.; Pless, M. Professionals′ views of children′s everyday life situations and the relation to participation. Disabil. Rehabil. 2012, 34, 581–592. [Google Scholar] [CrossRef] [PubMed]
- Chapparo, C.; Lowe, S. School: Participating in more than just the classroom. In Kids Can Be Kids: A Childhood Occupations Approach; Lane, S.J., Bundy, A.C., Eds.; FA Davis Company: Philadelphia, PA, USA, 2012; pp. 83–101. [Google Scholar]
- American Occupational Therapy Association. Occupational therapy practice framework: Domain and process (3rd Edition). Am. J. Occup. Ther. 2014, 68, S1–S48. [Google Scholar]
- Grootenhuis, M.; Koopman, H.; Verrips, E.; Vogels, A.; Last, B. Health-related quality of life problems of children aged 8–11 years with a chronic disease. Dev. Neurorehabil. 2007, 10, 27–33. [Google Scholar] [CrossRef] [PubMed]
| Author/s | Key Words | Participants | Ages in Years | Type of Study | Constructs Measured |
|---|---|---|---|---|---|
| Altobelli et al., 2013 [35] | N/A | n = 140 | 10–18 | Quantitative | CD specific questions-frequency of negative feelings (e.g., feel angry, bad, embarrassed), |
| Arnone and Fitzsimons, 2012 [41] | N/A | Adolescence | Review | Psychological aspects of CD | |
| Bacigalupe and Plocha, 2015 [25] | adherence; CD; family rituals; GFD; social support | n = 10 (children and parents) | 6–12 | Qualitative interviews | Family challenges and strategies |
| Barrio Torres et al., 2016 [26] | disease-specific questionnaire; outcome health; transcultural adaptation | n = 214 (parents only), n = 214 (parents and children), n = 52 (children only) | 10–18 | Quantitative | HRQOL |
| Bellini et al., 2011 [36] | N/A | n = 156 (CD), n = 353 (healthy controls) | 6–16 | Quantitative | QOL scale (e.g., feeling embarrassed; feeling unhappy giving up some group activities due to temptation not to follow the GFD) |
| Biagetti et al., 2013 [18] | QOL; CD; GFD; children; lived experiences; psycho-social aspects | N = 76 >8 years (children) <8 years (parents) | 2–18 | Qualitative open ended questions | Emotional impact of GFD on everyday life |
| Biagetti et al., 2015 [27] | Child; GFD; HRQOL | n = 76 (CD); n = 143 (non-CD) | 2–18 | Quantitative | QOL; impact of GFD on social life |
| Bongiovanni et al., 2010 [37] | Pediatric; sprue; QOL | n = 77 | 7–17 | Quantitative | General well-being; emotional outlook; self-perception (e.g., difficulty doing) |
| Cederborg et al., 2011 [40] | adaption process; children; coeliac disease; parental perspective | n = 20 (children and parents) | 3–5; 16–17 | Qualitative interviews | Parental perspective of living with CD |
| Chauhan et al., 2010 [28] | CD; GFD; compliance; QOL | n = 70 | 2–17 | Interview consisted of a self-administered questionnaire | Effect of CD on child′s feeling |
| de Lorenzo et al., 2012 [29] | CD; QOL; child; parents | n = 33 (CD), n = 63 (non-CD), n = 96 (parents) | 5–12 | Quantitative | Leisure |
| Jordan et al., 2013 [19] | CD; children; focus groups, GFD; HRQOL | N = 181 | 8–18 | Quantitative | HRQOL |
| Lins et al., 2015 [42] | QoL; Cross-cultural adaptation; CD | n = 33 (children and parents) | 8–18 | Quantitative | HRQOL |
| MacCulloch and Rashid, 2014 [30] * | Adherence; CD; compliance; GFD | n = 126 | 2–18 | Quantitative | HRQOL |
| Meyer and Rosenblum, 2016 [13] * | CD; child; leisure activities; parents; QOL; self-report | n = 34 (CD), n = 34 (healthy controls) | 8–15 | Quantitative | HRQOL, Leisure |
| Olsson et al., 2008 [43] | Adolescent; CD; focus groups; GFD; patient compliance | n = 57 | 15–18 | Qualitative focus groups | Views of everyday life with coeliac disease and a prescription of a GFD |
| Olsson et al., 2009 [38] | Adolescent; chronic illness; focus groups; lived experiences; social constructionism; stigma | n = 57 | 15–18 | Qualitative focus groups | The GFD can produce stigma experiences in adolescence |
| Pico and Spirito, 2014 [31] | QOL, children/adolescents, CD, CDDUX, sensitivity to change | n = 118 (children and parents) | 8–18 | Quantitative | HRQOL |
| Roma et al., 2010 [39] | Children; CD; compliance; GFD; life style | n = 73 (self-report and parents) | 5–14.5 | Quantitative | HRQOL |
| Rosén et al., 2011 [32] | N/A | n = 101 (adolescents) n = 125 (parents) | 13.9–15.4 | Qualitative interviews | |
| Skjerning et al., 2014 [33] | CD; HRQOL; Children; Adolescents/youth; Coping; focus groups; illness and disease; chronic | n = 23 (children/adolescents) n = 3 (parents) | 8–18 | Qualitative focus group interviews | HRQOL |
| van Doorn et al., 2008 [16] | CD; QOL; disease specific questionnaire; proxy | n = 530 | 8–18 | Quantitative | HRQOL |
| Veen et al., 2012 [34] * | Discursive psychology, coeliac disease, family mealtime, discourse analysis, experience of illness | n = 7 | 2–20 | Qualitative | Conversation about the food during meals |
| ICF Classification | Food-Related Activities | n |
|---|---|---|
| d9 Community, social, and civic life | ||
| Eating at restaurants | 8 [13,19,30,33,35,36,38,40] |
| Parties/birthday parties | 7 [25,27,28,29,32,38,43] | |
| Social functions/events | 7 [19,25,28,33,37,38,40] | |
| Eating/dining out with friends | 6 [28,32,33,38,41,43] | |
| Travelling | 4 [28,30,35,43] | |
| Eating at a friend’s house | 3 [19,36,38] | |
| Vacations | 2 [29,33] | |
| Once each: Picnics; visiting people/family [13]; activities at friends; bringing GF food when traveling [35]; group activities [37]; meals outside the home with peers; social engagement outside the home; communal meals with peers [41]; sleep overs [25]; eating meals outside home [18]; eating GF food in public [38]; travelling abroad; bringing GF food to a meal; spontaneous social life with friends [40] | 1 | |
| Summer camp | 2 [25,43] |
| Sports camp | 1 [43] | |
| d8 Major life areas-education | ||
| Food situations/activities/events at school | 7 [18,25,29,35,38,39,41] |
| Given gluten foods at school | 5 [13,16,26,31,42] | |
| Eating at school cafeteria/canteen | 4 [27,32,38,39] | |
| Meals/eating at school/daycare | 4 [30,40,43] | |
| Eating with friends at school | 2 [19,29] | |
| Once each: school parties; after-school activities [19]; unexpected snack in class; play games with food in class [33]; eating pastries in class [43]; home economic classes [38] | 1 | |
| d5 Self-care | ||
| Not being able to eat anything/ Paying attention to what I eat/ not eating what others eat/ frustrated about not eating something you want | 6 [13,16,26,31,37,42] |
| Following a lifelong diet/ following a diet for my CD/angry about having to follow a special diet | 6 [13,16,26,31,37,42] | |
| thinking of gluten food | 5 [13,16,26,31,42] | |
| Offered gluten food | 5 [13,16,26,31,42] | |
| Having CD | 5 [13,16,26,31,42] | |
| Once each: meals at home [18]; knowing what to eat; making sure there is GF food before visiting friends [40] | 1 | |
| Eating with the family | 2 [19,29] |
| Having meals | 1 [29] | |
| d3 Communication | ||
| Talking about CD | 5 [13,16,26,31,42] |
| Explaining about CD | 5 [13,16,26,31,42] | |
| Talking about CD to friends | 5 [13,16,26,31,42] | |
| d6 Domestic life | ||
| Determining if food is GF or not from the food label | 2 [19,35] |
| Finding GF food in stores | 1 [35] | |
| d7 Interpersonal interactions and relationships | ||
| Feel teachers do not understand | 2 [28,35] |
| Talking to school staff | 1 [40] | |
| d2 General tasks and demands | ||
| Once each: eating at home [40]; cooking at home [43] | 1 |
© 2017 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Meyer, S.; Rosenblum, S. Activities, Participation and Quality of Life Concepts in Children and Adolescents with Celiac Disease: A Scoping Review. Nutrients 2017, 9, 929. https://doi.org/10.3390/nu9090929
Meyer S, Rosenblum S. Activities, Participation and Quality of Life Concepts in Children and Adolescents with Celiac Disease: A Scoping Review. Nutrients. 2017; 9(9):929. https://doi.org/10.3390/nu9090929
Chicago/Turabian StyleMeyer, Sonya, and Sara Rosenblum. 2017. "Activities, Participation and Quality of Life Concepts in Children and Adolescents with Celiac Disease: A Scoping Review" Nutrients 9, no. 9: 929. https://doi.org/10.3390/nu9090929
APA StyleMeyer, S., & Rosenblum, S. (2017). Activities, Participation and Quality of Life Concepts in Children and Adolescents with Celiac Disease: A Scoping Review. Nutrients, 9(9), 929. https://doi.org/10.3390/nu9090929






