Adherence to a Vegetarian Diet and Diabetes Risk: A Systematic Review and Meta-Analysis of Observational Studies
Abstract
:1. Introduction
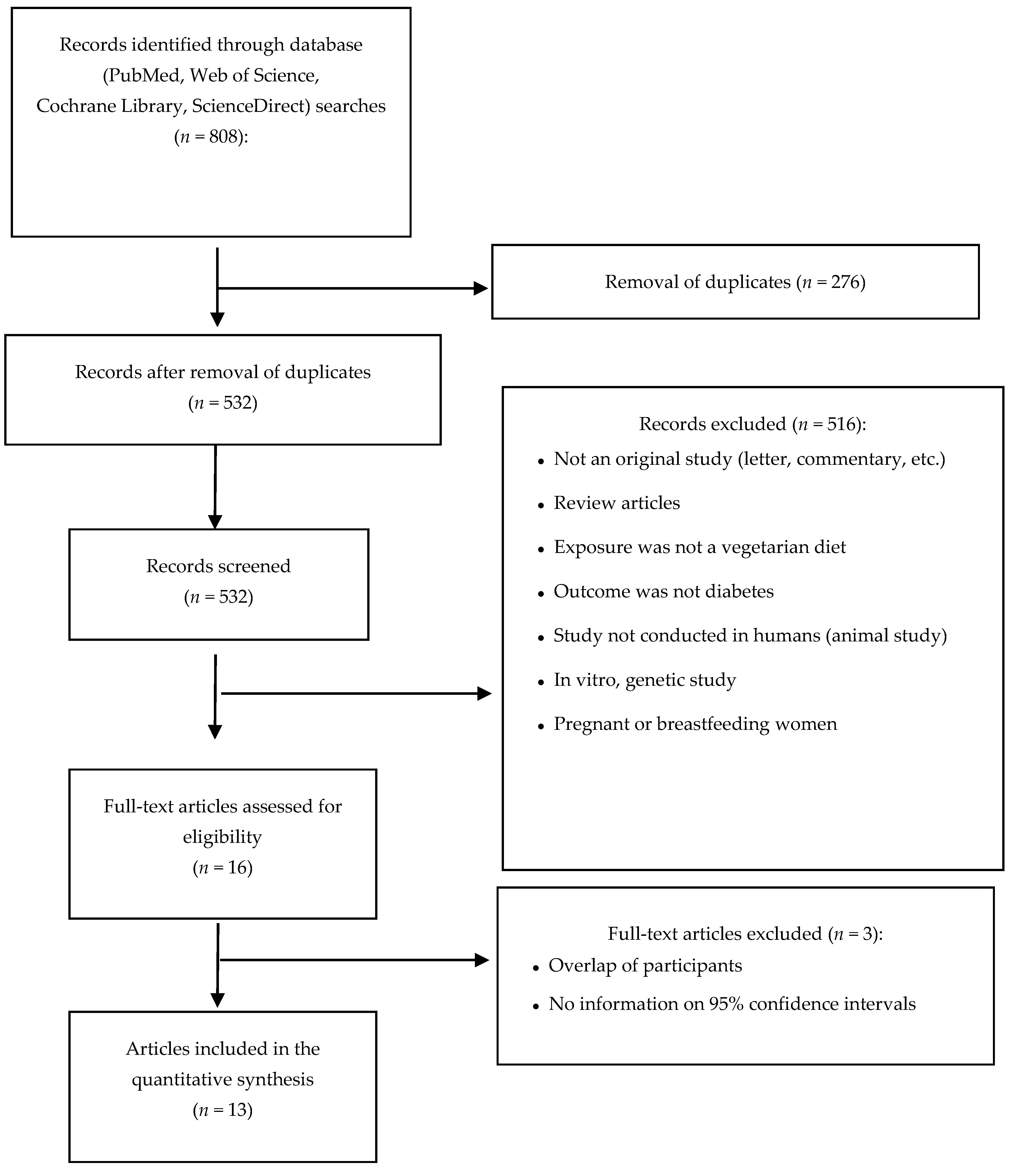
2. Materials and Methods
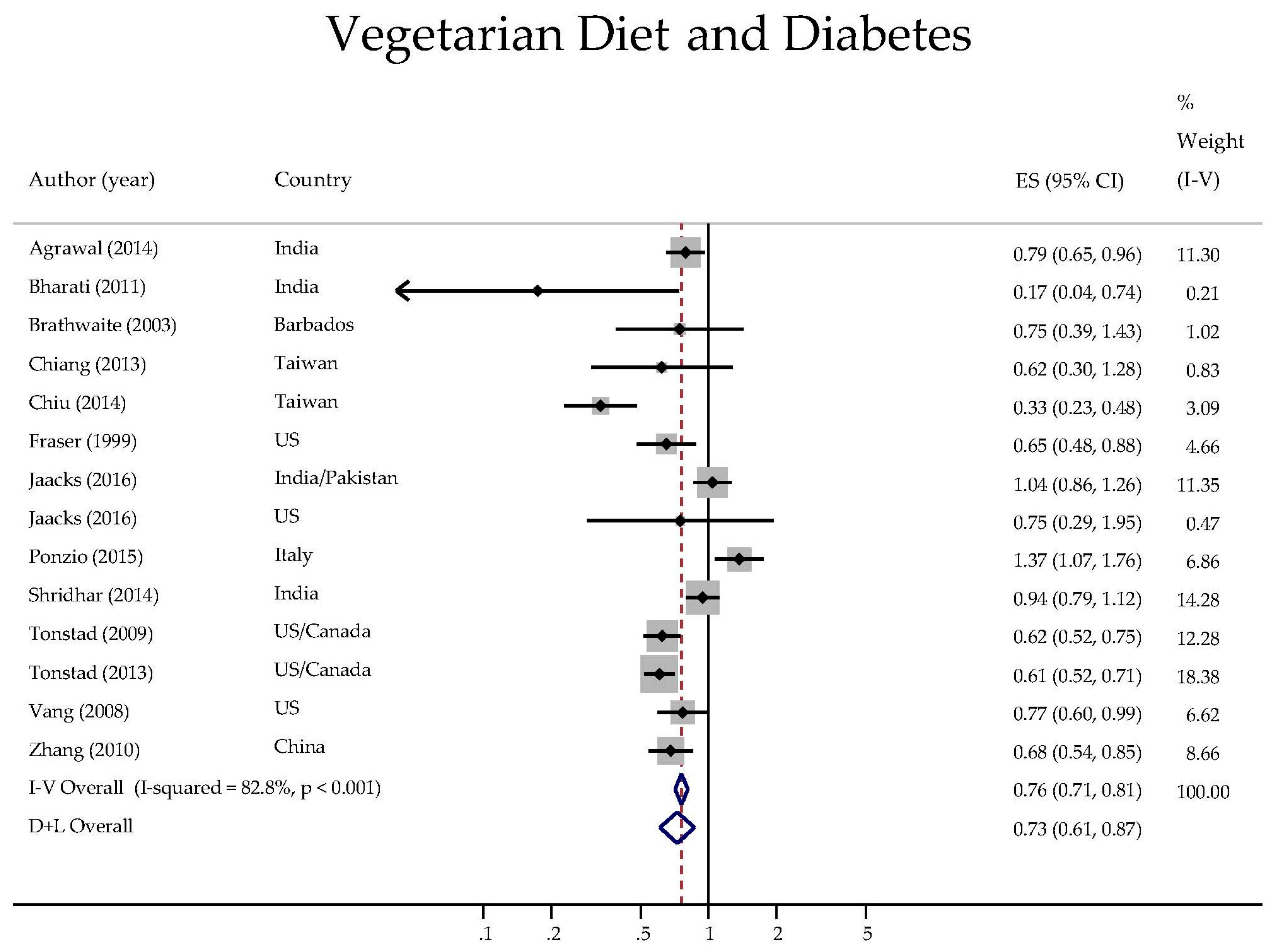
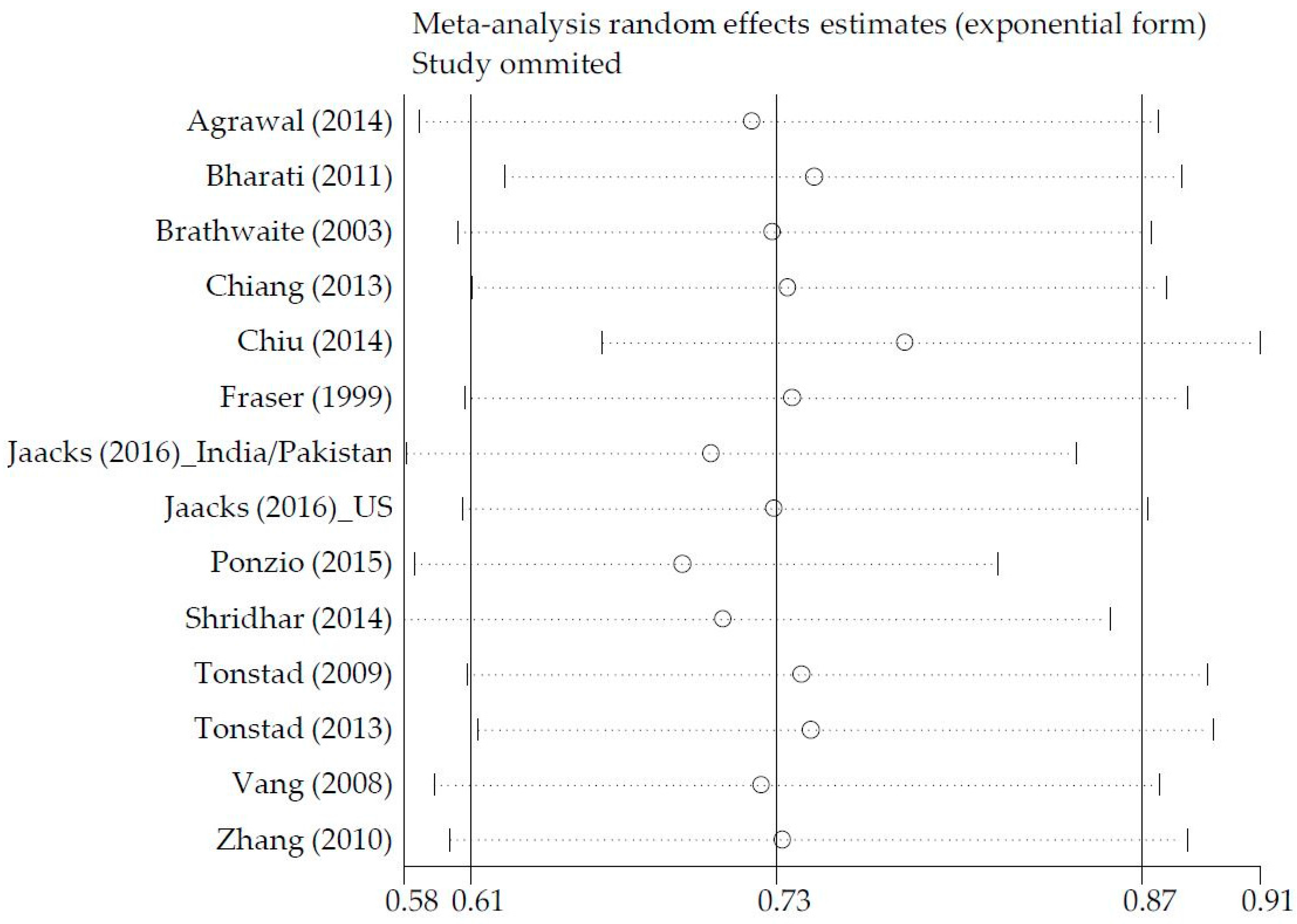
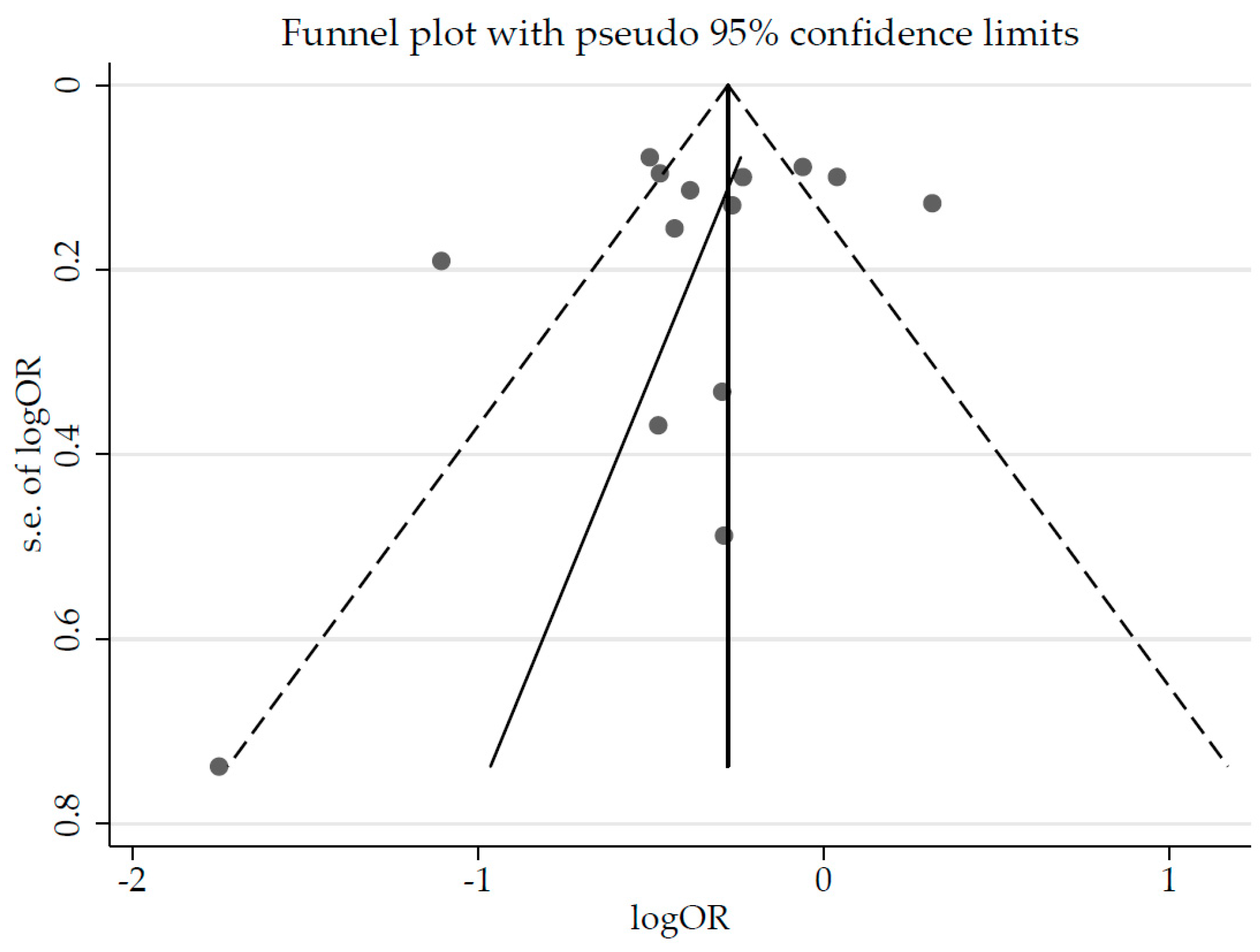
3. Results
4. Discussion
5. Conclusions
Supplementary Materials
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Federation, I.D. Idf Diabetes Atlas—Seventh ed. Available online: http://www.diabetesatlas.org (accessed on 15 December 2016).
- Fox, C.S.; Golden, S.H.; Anderson, C.; Bray, G.A.; Burke, L.E.; de Boer, I.H.; Deedwania, P.; Eckel, R.H.; Ershow, A.G.; Fradkin, J.; et al. Update on prevention of cardiovascular disease in adults with type 2 diabetes mellitus in light of recent evidence: A scientific statement from the american heart association and the american diabetes association. Diabetes Care 2015, 38, 1777–1803. [Google Scholar] [CrossRef] [PubMed]
- Schwingshackl, L.; Hoffmann, G.; Lampousi, A.M.; Knuppel, S.; Iqbal, K.; Schwedhelm, C.; Bechthold, A.; Schlesinger, S.; Boeing, H. Food groups and risk of type 2 diabetes mellitus: A systematic review and meta-analysis of prospective studies. Eur. J. Epidemiol. 2017. [Google Scholar] [CrossRef] [PubMed]
- Ley, S.H.; Hamdy, O.; Mohan, V.; Hu, F.B. Prevention and management of type 2 diabetes: Dietary components and nutritional strategies. Lancet 2014, 383, 1999–2007. [Google Scholar] [CrossRef]
- Appleby, P.N.; Key, T.J. The long-term health of vegetarians and vegans. Proc. Nutr. Soc. 2016, 75, 287–293. [Google Scholar] [CrossRef] [PubMed]
- Agrawal, S.; Millett, C.J.; Dhillon, P.K.; Subramanian, S.V.; Ebrahim, S. Type of vegetarian diet, obesity and diabetes in adult Indian population. Nutr. J. 2014, 13, 89. [Google Scholar] [CrossRef] [PubMed]
- Brathwaite, N.; Fraser, H.S.; Modeste, N.; Broome, H.; King, R. For the patient. Are vegetarians at less risk for obesity, diabetes, and hypertension? Obesity, diabetes, hypertension, and vegetarian status among seventh-day adventists in barbados: Preliminary results. Ethn. Dis. 2003, 13, 148. [Google Scholar] [PubMed]
- Chiang, J.K.; Lin, Y.L.; Chen, C.L.; Ouyang, C.M.; Wu, Y.T.; Chi, Y.C.; Huang, K.C.; Yang, W.S. Reduced risk for metabolic syndrome and insulin resistance associated with ovo-lacto-vegetarian behavior in female buddhists: A case-control study. PLoS ONE 2013, 8, e71799. [Google Scholar] [CrossRef] [PubMed]
- Chiu, T.H.; Huang, H.Y.; Chiu, Y.F.; Pan, W.H.; Kao, H.Y.; Chiu, J.P.; Lin, M.N.; Lin, C.L. Taiwanese vegetarians and omnivores: Dietary composition, prevalence of diabetes and ifg. PLoS ONE 2014, 9, e88547. [Google Scholar] [CrossRef] [PubMed]
- Fraser, G.E. Associations between diet and cancer, ischemic heart disease, and all-cause mortality in non-hispanic white California seventh-day adventists. Am. J. Clin. Nutr. 1999, 70, 532S–538S. [Google Scholar] [PubMed]
- Jaacks, L.M.; Kapoor, D.; Singh, K.; Narayan, K.M.V.; Ali, M.K.; Kadir, M.M.; Mohan, V.; Tandon, N.; Prabhakaran, D. Vegetarianism and cardiometabolic disease risk factors: Differences between south Asian and US adults. Nutrition 2016, 32, 975–984. [Google Scholar] [CrossRef] [PubMed]
- Davey, G.K.; Spencer, E.A.; Appleby, P.N.; Allen, N.E.; Knox, K.H.; Key, T.J. Epic-oxford: Lifestyle characteristics and nutrient intakes in a cohort of 33 883 meat-eaters and 31 546 non meat-eaters in the UK. Public Health Nutr. 2003, 6, 259–269. [Google Scholar] [CrossRef] [PubMed]
- Tonstad, S.; Butler, T.; Yan, R.; Fraser, G.E. Type of vegetarian diet, body weight, and prevalence of type 2 diabetes. Diabetes Care 2009, 32, 791–796. [Google Scholar] [CrossRef] [PubMed]
- Jayanthi, V. Vegetarianism in India. Perit. Dial. Int. 2001, 21, S322–S325. [Google Scholar] [PubMed]
- Lee, H.Y.; Woo, J.; Chen, Z.Y.; Leung, S.F.; Peng, X.H. Serum fatty acid, lipid profile and dietary intake of Hong Kong Chinese omnivores and vegetarians. Eur. J. Clin. Nutr. 2000, 54, 768–773. [Google Scholar] [CrossRef] [PubMed]
- Yokoyama, Y.; Barnard, N.D.; Levin, S.M.; Watanabe, M. Vegetarian diets and glycemic control in diabetes: A systematic review and meta-analysis. Cardiovasc. Diagn. Ther. 2014, 4, 373–382. [Google Scholar] [PubMed]
- Ajala, O.; English, P.; Pinkney, J. Systematic review and meta-analysis of different dietary approaches to the management of type 2 diabetes. Am. J. Clin. Nutr. 2013, 97, 505–516. [Google Scholar] [CrossRef] [PubMed]
- Barnard, N.D.; Katcher, H.I.; Jenkins, D.J.; Cohen, J.; Turner-McGrievy, G. Vegetarian and vegan diets in type 2 diabetes management. Nutr. Rev. 2009, 67, 255–263. [Google Scholar] [CrossRef] [PubMed]
- American Diabetes Association. Diagnosis and classification of diabetes mellitus. Diabetes Care 2011, 34, S62–S69. [Google Scholar]
- Higgins, J.P.; Thompson, S.G.; Deeks, J.J.; Altman, D.G. Measuring inconsistency in meta-analyses. BMJ 2003, 327, 557–560. [Google Scholar] [CrossRef] [PubMed]
- Higgins, J.; Green, S. (Eds.) Cochrane Handbook for Systematic Reviews of Interventions; The Cochrane Collaboration: London, UK, 2011. [Google Scholar]
- Tonstad, S.; Stewart, K.; Oda, K.; Batech, M.; Herring, R.P.; Fraser, G.E. Vegetarian diets and incidence of diabetes in the adventist health study-2. Nutr. Metab. Cardiovasc. Dis. 2013, 23, 292–299. [Google Scholar] [CrossRef] [PubMed]
- Vang, A.; Singh, P.N.; Lee, J.W.; Haddad, E.H.; Brinegar, C.H. Meats, processed meats, obesity, weight gain and occurrence of diabetes among adults: Findings from adventist health studies. Ann. Nutr. Metab. 2008, 52, 96–104. [Google Scholar] [CrossRef] [PubMed]
- Bharati, D.R.; Pal, R.; Rekha, R.; Yamuna, T.V. Evaluation of the burden of type 2 diabetes mellitus in population of puducherry, South India. Diabetes Metab. Syndr. 2011, 5, 12–16. [Google Scholar] [CrossRef] [PubMed]
- Brathwaite, N.; Fraser, H.S.; Modeste, N.; Broome, H.; King, R. Obesity, diabetes, hypertension, and vegetarian status among seventh-day adventists in barbados: Preliminary results. Ethn. Dis. 2003, 13, 34–39. [Google Scholar] [PubMed]
- Ponzio, E.; Mazzarini, G.; Gasperi, G.; Bottoni, M.C.; Vallorani, S. The vegetarian habit in Italy: Prevalence and characteristics of consumers. Ecol. Food Nutr. 2015, 54, 370–379. [Google Scholar] [CrossRef] [PubMed]
- Shridhar, K.; Dhillon, P.K.; Bowen, L.; Kinra, S.; Bharathi, A.V.; Prabhakaran, D.; Reddy, K.S.; Ebrahim, S. The association between a vegetarian diet and cardiovascular disease (cvd) risk factors in India: The Indian migration study. BMJ Open 2014, 9, e110586. [Google Scholar] [CrossRef] [PubMed]
- Zhang, L.; Qin, L.Q.; Liu, A.P.; Wang, P.Y. Prevalence of risk factors for cardiovascular disease and their associations with diet and physical activity in suburban Beijing, China. J. Epidemiol. Jpn. Epidemiol. Assoc. 2010, 20, 237–243. [Google Scholar] [CrossRef]
- Kuo, C.S.; Lai, N.S.; Ho, L.T.; Lin, C.L. Insulin sensitivity in Chinese ovo-lactovegetarians compared with omnivores. Eur. J. Clin. Nutr. 2004, 58, 312–316. [Google Scholar] [CrossRef] [PubMed]
- Hung, C.J.; Huang, P.C.; Li, Y.H.; Lu, S.C.; Ho, L.T.; Chou, H.F. Taiwanese vegetarians have higher insulin sensitivity than omnivores. Br. J. Nutr. 2006, 95, 129–135. [Google Scholar] [CrossRef] [PubMed]
- Goff, L.M.; Bell, J.D.; So, P.W.; Dornhorst, A.; Frost, G.S. Veganism and its relationship with insulin resistance and intramyocellular lipid. Eur. J. Clin. Nutr. 2005, 59, 291–298. [Google Scholar] [CrossRef] [PubMed]
- Aune, D.; Norat, T.; Romundstad, P.; Vatten, L.J. Whole grain and refined grain consumption and the risk of type 2 diabetes: A systematic review and dose-response meta-analysis of cohort studies. Eur. J. Epidemiol. 2013, 28, 845–858. [Google Scholar] [CrossRef] [PubMed]
- Jaacks, L.M.; Siegel, K.R.; Gujral, U.P.; Narayan, K.M. Type 2 diabetes: A 21st century epidemic. Best Pract. Res. Clin. Endocrinol. Metab. 2016, 30, 331–343. [Google Scholar] [CrossRef] [PubMed]
- Schulze, M.B.; Schulz, M.; Heidemann, C.; Schienkiewitz, A.; Hoffmann, K.; Boeing, H. Fiber and magnesium intake and incidence of type 2 diabetes: A prospective study and meta-analysis. Arch. Intern. Med. 2007, 167, 956–965. [Google Scholar] [CrossRef] [PubMed]
- Fang, X.; Han, H.; Li, M.; Liang, C.; Fan, Z.; Aaseth, J.; He, J.; Montgomery, S.; Cao, Y. Dose-response relationship between dietary magnesium intake and risk of type 2 diabetes mellitus: A systematic review and meta-regression analysis of prospective cohort studies. Nutrients 2016, 8, 739. [Google Scholar] [CrossRef] [PubMed]
- Micha, R.; Wallace, S.K.; Mozaffarian, D. Red and processed meat consumption and risk of incident coronary heart disease, stroke, and diabetes mellitus: A systematic review and meta-analysis. Circulation 2010, 121, 2271–2283. [Google Scholar] [CrossRef] [PubMed]
- Kim, Y.; Keogh, J.; Clifton, P. A review of potential metabolic etiologies of the observed association between red meat consumption and development of type 2 diabetes mellitus. Metab. Clin. Exp. 2015, 64, 768–779. [Google Scholar] [CrossRef] [PubMed]
- Micha, R.; Michas, G.; Mozaffarian, D. Unprocessed red and processed meats and risk of coronary artery disease and type 2 diabetes—An updated review of the evidence. Curr. Atheroscler. Rep. 2012, 14, 515–524. [Google Scholar] [CrossRef] [PubMed]
- Wu, J.H.; Micha, R.; Imamura, F.; Pan, A.; Biggs, M.L.; Ajaz, O.; Djousse, L.; Hu, F.B.; Mozaffarian, D. Omega-3 fatty acids and incident type 2 diabetes: A systematic review and meta-analysis. Br. J. Nutr. 2012, 107, S214–S227. [Google Scholar] [CrossRef] [PubMed]
- Sabate, J.; Ratzin-Turner, R.A.; Brown, J.E. Vegetarian diets: Description and trends. In Vegetarian Nutrition; Sabate, J., Ed.; CRC Press LLC: Boca Raton, FL, USA, 2001; p. 5. [Google Scholar]
- Newby, P.K.; Tucker, K.L.; Wolk, A. Risk of overweight and obesity among semivegetarian, lactovegetarian, and vegan women. Am. J. Clin. Nutr. 2005, 81, 1267–1274. [Google Scholar] [PubMed]
- Cade, J.E.; Burley, V.J.; Greenwood, D.C. The UK women’s cohort study: Comparison of vegetarians, fish-eaters and meat-eaters. Public Health Nutr. 2004, 7, 871–878. [Google Scholar] [CrossRef] [PubMed]
- Le, L.T.; Sabate, J. Beyond meatless, the health effects of vegan diets: Findings from the adventist cohorts. Nutrients 2014, 6, 2131–2147. [Google Scholar] [CrossRef] [PubMed]
- Leitzmann, C.; Keller, M. Vegetarishe Ernaehrung, 2nd ed.; Verlag Eugen Ulmer KG: Stuttgart, Germany, 2010. [Google Scholar]
- Radnitz, C.; Beezhold, B.; DiMatteo, J. Investigation of lifestyle choices of individuals following a vegan diet for health and ethical reasons. Appetite 2015, 90, 31–36. [Google Scholar] [CrossRef] [PubMed]
- Singh, P.N.; Arthur, K.N.; Orlich, M.J.; James, W.; Purty, A.; Job, J.S.; Rajaram, S.; Sabate, J. Global epidemiology of obesity, vegetarian dietary patterns, and noncommunicable disease in Asian Indians. Am. J. Clin. Nutr. 2014, 100, 359s–364s. [Google Scholar] [CrossRef] [PubMed]
- Szeto, Y.T.; Kwok, T.C.; Benzie, I.F. Effects of a long-term vegetarian diet on biomarkers of antioxidant status and cardiovascular disease risk. Nutrition 2004, 20, 863–866. [Google Scholar] [CrossRef] [PubMed]
- Piccoli, G.B.; Vigotti, F.N.; Leone, F.; Capizzi, I.; Daidola, G.; Cabiddu, G.; Avagnina, P. Low-protein diets in ckd: How can we achieve them? A narrative, pragmatic review. Clin. Kidney J. 2015, 8, 61–70. [Google Scholar] [CrossRef] [PubMed]
| Study | No. of Studies | Odds Ratio (95% CI) | Heterogeneity | ||
|---|---|---|---|---|---|
| p | I2 (%) | ||||
| Sex | |||||
| Men | 3 | 0.614 | (0.527, 0.716) | 0.719 | 0.0 |
| Women | 4 | 0.569 | (0.298, 1.086) | <0.001 | 86.0 |
| Overall | 7 | 0.584 | (0.439, 0.778) | 0.001 | 73.6 |
| Study design | |||||
| Prospective cohort | 2 | 0.644 | (0.565, 0.735) | 0.116 | 59.5 |
| Cross-sectional | 12 | 0.733 | (0.595, 0.904) | <0.001 | 83.1 |
| Overall | 14 | 0.726 | (0.608, 0.867) | <0.001 | 82.8 |
| Region of study | |||||
| Southeast Asia | 4 | 0.888 | (0.718, 1.099) | 0.03 | 66.4 |
| Western Pacific | 3 | 0.514 | (0.304, 0.871) | 0.005 | 81.1 |
| Europe & North America | 7 | 0.756 | (0.589, 0.971) | <0.001 | 81.9 |
| Overall | 14 | 0.726 | (0.608, 0.867) | <0.001 | 82.8 |
| Vegetarian type | |||||
| Vegan | 4 | 0.593 | (0.386, 0.911) | 0.017 | 70.5 |
| Lacto-vegetarian | 3 | 0.762 | (0.613, 0.949) | 0.016 | 75.7 |
| Lacto-ovo-vegetarian | 4 | 0.564 | (0.517, 0.616) | 0.301 | 17.9 |
| Pesco-vegetarian | 4 | 0.867 | (0.636, 1.180) | 0.008 | 74.9 |
| Semi-vegetarian | 9 | 0.799 | (0.667, 0.956) | 0.002 | 67.3 |
| Overall | 24 | 0.735 | (0.654, 0.826) | <0.001 | 78.8 |
© 2017 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lee, Y.; Park, K. Adherence to a Vegetarian Diet and Diabetes Risk: A Systematic Review and Meta-Analysis of Observational Studies. Nutrients 2017, 9, 603. https://doi.org/10.3390/nu9060603
Lee Y, Park K. Adherence to a Vegetarian Diet and Diabetes Risk: A Systematic Review and Meta-Analysis of Observational Studies. Nutrients. 2017; 9(6):603. https://doi.org/10.3390/nu9060603
Chicago/Turabian StyleLee, Yujin, and Kyong Park. 2017. "Adherence to a Vegetarian Diet and Diabetes Risk: A Systematic Review and Meta-Analysis of Observational Studies" Nutrients 9, no. 6: 603. https://doi.org/10.3390/nu9060603
APA StyleLee, Y., & Park, K. (2017). Adherence to a Vegetarian Diet and Diabetes Risk: A Systematic Review and Meta-Analysis of Observational Studies. Nutrients, 9(6), 603. https://doi.org/10.3390/nu9060603






