Parenteral Nutrition and Intestinal Failure
Abstract
:1. Introduction
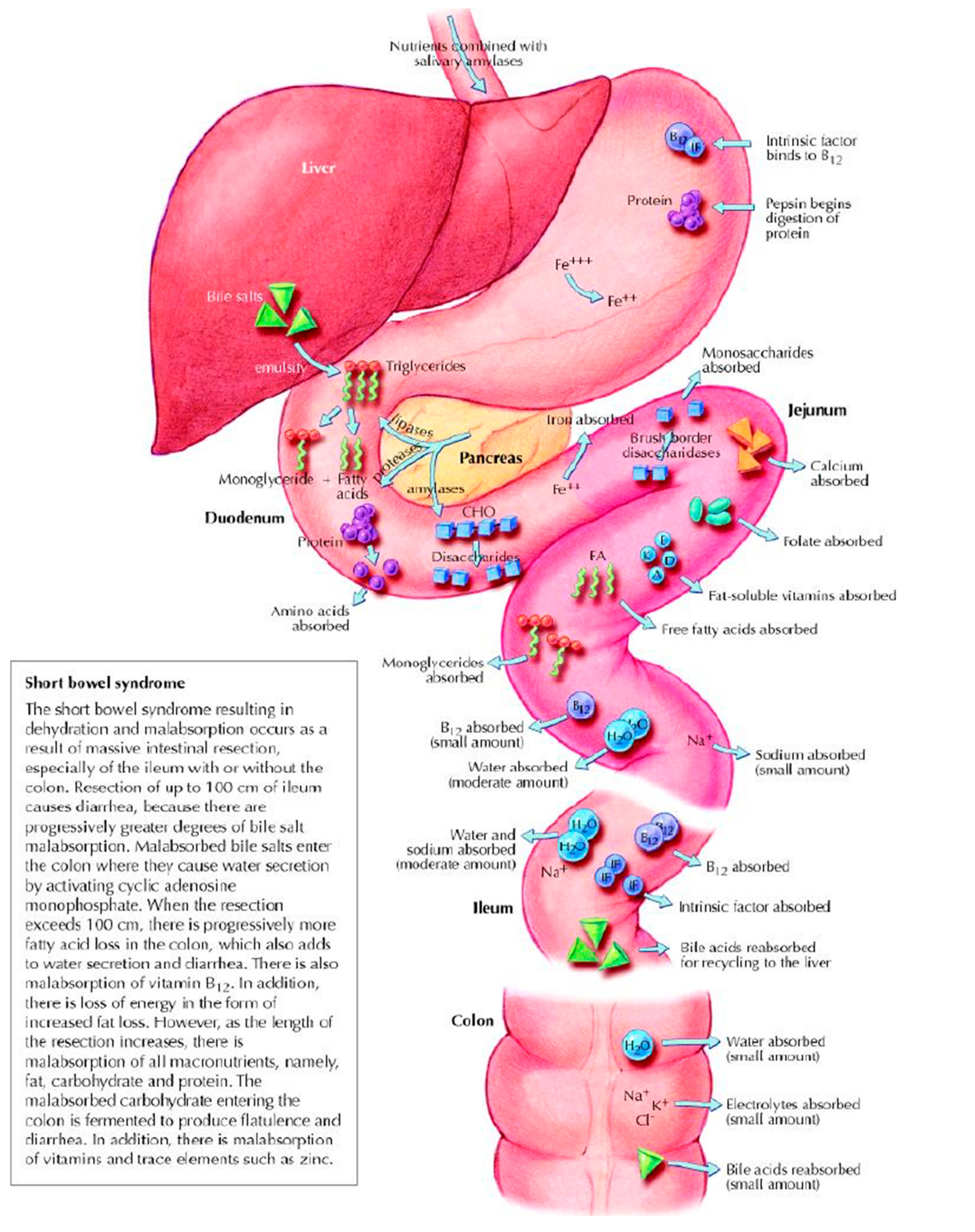
2. Short Bowel Syndrome
2.1. Mechanisms of Malabsorption
2.2. Management
2.2.1. Diet and Micronutrient Supplementation
2.2.2. Pharmacologic Therapy
2.2.3. Surgical Options
3. Home Parenteral Nutrition
3.1. HPN Initiation
3.2. Monitoring
3.3. Complications of Long-Term PN
3.3.1. Venous Access Related Complications
3.3.2. Intestinal Failure Associated Liver Disease (IFALD)
3.3.3. Other Metabolic Complications
3.4. Outcomes of Home Parenteral Nutrition
3.5. The Future of HPN Research
4. Conclusions
Conflicts of Interest
References
- O’Keefe, S.J.; Buchman, A.L.; Fishbein, T.M.; Jeejeebhoy, K.N.; Jeppesen, P.B.; Shaffer, J. Short bowel syndrome and intestinal failure: Consensus definitions and overview. Clin. Gastroenterol. Hepatol. 2006, 4, 6–10. [Google Scholar] [CrossRef] [PubMed]
- Lal, S.; Teubner, A.; Shaffer, J.L. Review article: Intestinal failure. Aliment. Pharmacol. Ther. 2006, 24, 19–31. [Google Scholar] [CrossRef] [PubMed]
- Dibb, M.; Teubner, A.; Theis, V.; Shaffer, J.; Lal, S. Review article: The management of long-term parenteral nutrition. Aliment. Pharmacol. Ther. 2013, 37, 587–603. [Google Scholar] [CrossRef] [PubMed]
- Pironi, L.; Arends, J.; Bozzetti, F.; Cuerda, C.; Gillanders, L.; Jeppesen, P.B.; Joly, F.; Kelly, D.; Lal, S.; Staun, M.; et al. Espen guidelines on chronic intestinal failure in adults. Clin. Nutr. 2016, 35, 247–307. [Google Scholar] [CrossRef] [PubMed]
- Booth, C.C. The metabolic effects of intestinal resection in man. Postgrad. Med. J. 1961, 37, 725–739. [Google Scholar] [CrossRef] [PubMed]
- Booth, C.C.; Alldis, D.; Read, A.E. Studies on the site of fat absorption: 2 fat balances after resection of varying amounts of the small intestine in man. Gut 1961, 2, 168–174. [Google Scholar] [CrossRef] [PubMed]
- Nightingale, J.M.; Kamm, M.A.; van der Sijp, J.R.; Ghatei, M.A.; Bloom, S.R.; Lennard-Jones, J.E. Gastrointestinal hormones in short bowel syndrome. Peptide yy may be the ‘colonic brake’ to gastric emptying. Gut 1996, 39, 267–272. [Google Scholar] [CrossRef] [PubMed]
- Dibaise, J.K.; Young, R.J.; Vanderhoof, J.A. Enteric microbial flora, bacterial overgrowth, and short-bowel syndrome. Clin. Gastroenterol. Hepatol. 2006, 4, 11–20. [Google Scholar] [CrossRef] [PubMed]
- Debongnie, J.C.; Phillips, S.F. Capacity of the human colon to absorb fluid. Gastroenterology 1978, 74, 698–703. [Google Scholar] [PubMed]
- Jeppesen, P.B.; Mortensen, P.B. Significance of a preserved colon for parenteral energy requirements in patients receiving home parenteral nutrition. Scand. J. Gastroenterol. 1998, 33, 1175–1179. [Google Scholar] [PubMed]
- Pape, U.F.; Maasberg, S.; Pascher, A. Pharmacological strategies to enhance adaptation in intestinal failure. Curr. Opin. Organ. Transplant 2016, 21, 147–152. [Google Scholar] [CrossRef] [PubMed]
- Tappenden, K.A. Intestinal adaptation following resection. JPEN J. Parenter. Enteral. Nutr. 2014, 38, 23S–31S. [Google Scholar] [CrossRef] [PubMed]
- Messing, B.; Crenn, P.; Beau, P.; Boutron-Ruault, M.C.; Rambaud, J.C.; Matuchansky, C. Long-term survival and parenteral nutrition dependence in adult patients with the short bowel syndrome. Gastroenterology 1999, 117, 1043–1050. [Google Scholar] [CrossRef]
- Williams, N.S.; Evans, P.; King, R.F. Gastric acid secretion and gastrin production in the short bowel syndrome. Gut 1985, 26, 914–919. [Google Scholar] [CrossRef] [PubMed]
- Griffin, G.E.; Fagan, E.F.; Hodgson, H.J.; Chadwick, V.S. Enteral therapy in the management of massive gut resection complicated by chronic fluid and electrolyte depletion. Dig. Dis. Sci. 1982, 27, 902–908. [Google Scholar] [CrossRef] [PubMed]
- Wall, E.A. An overview of short bowel syndrome management: Adherence, adaptation, and practical recommendations. J. Acad. Nutr. Diet. 2013, 113, 1200–1208. [Google Scholar] [CrossRef] [PubMed]
- Nightingale, J.; Woodward, J.M.; Small, B.; Small Bowel and Nutrition Committee of the British Society of Gastroenterology. Guidelines for management of patients with a short bowel. Gut 2006, 55, iv1–iv12. [Google Scholar] [CrossRef] [PubMed]
- Higham, S.E.; Read, N.W. The effect of ingestion of guar gum on ileostomy effluent. Br. J. Nutr. 1992, 67, 115–122. [Google Scholar] [CrossRef] [PubMed]
- Abdalian, R.; Fernandes, G.; Duerksen, D.; Jeejeebhoy, K.N.; Whittaker, S.; Gramlich, L.; Allard, J.P. Prescription of trace elements in adults on home parenteral nutrition: Current practice based on the canadian home parenteral nutrition registry. JPEN J. Parenter. Enteral. Nutr. 2013, 37, 410–415. [Google Scholar] [CrossRef] [PubMed]
- Kumar, P.R.; Fenton, T.R.; Shaheen, A.A.; Raman, M. Prevalence of vitamin D deficiency and response to oral vitamin d supplementation in patients receiving home parenteral nutrition. JPEN J. Parenter. Enteral. Nutr. 2012, 36, 463–469. [Google Scholar] [CrossRef] [PubMed]
- Uzzan, M.; Kirchgesner, J.; Poupon, J.; Corcos, O.; Pingenot, I.; Joly, F. Antioxidant trace elements serum levels in long-term parenteral nutrition (PN): Prevalence and infectious risk associated with deficiencies, a retrospective study from a tertiary home-pn center. Clin. Nutr. 2016. [Google Scholar] [CrossRef] [PubMed]
- Btaiche, I.F.; Carver, P.L.; Welch, K.B. Dosing and monitoring of trace elements in long-term home parenteral nutrition patients. JPEN J. Parenter. Enteral. Nutr. 2011, 35, 736–747. [Google Scholar] [CrossRef] [PubMed]
- King, R.F.; Norton, T.; Hill, G.L. A double-blind crossover study of the effect of loperamide hydrochloride and codeine phosphate on ileostomy output. ANZ J. Surg. 1982, 52, 121–124. [Google Scholar] [CrossRef]
- Jeppesen, P.B.; Staun, M.; Tjellesen, L.; Mortensen, P.B. Effect of intravenous ranitidine and omeprazole on intestinal absorption of water, sodium, and macronutrients in patients with intestinal resection. Gut 1998, 43, 763–769. [Google Scholar] [CrossRef] [PubMed]
- O’Keefe, S.J.; Peterson, M.E.; Fleming, C.R. Octreotide as an adjunct to home parenteral nutrition in the management of permanent end-jejunostomy syndrome. JPEN J. Parenter. Enteral. Nutr. 1994, 18, 26–34. [Google Scholar] [PubMed]
- Murphy, M.S. Growth factors and the gastrointestinal tract. Nutrition 1998, 14, 771–774. [Google Scholar] [CrossRef]
- Jeppesen, P.B.; Hartmann, B.; Thulesen, J.; Graff, J.; Lohmann, J.; Hansen, B.S.; Tofteng, F.; Poulsen, S.S.; Madsen, J.L.; Holst, J.J.; et al. Glucagon-like peptide 2 improves nutrient absorption and nutritional status in short-bowel patients with no colon. Gastroenterology 2001, 120, 806–815. [Google Scholar] [CrossRef] [PubMed]
- Jeppesen, P.B.; Gilroy, R.; Pertkiewicz, M.; Allard, J.P.; Messing, B.; O’Keefe, S.J. Randomised placebo-controlled trial of teduglutide in reducing parenteral nutrition and/or intravenous fluid requirements in patients with short bowel syndrome. Gut 2011, 60, 902–914. [Google Scholar] [CrossRef] [PubMed]
- O’Keefe, S.J.; Jeppesen, P.B.; Gilroy, R.; Pertkiewicz, M.; Allard, J.P.; Messing, B. Safety and efficacy of teduglutide after 52 weeks of treatment in patients with short bowel intestinal failure. Clin. Gastroenterol. Hepatol. 2013, 11, 815–823. [Google Scholar] [CrossRef] [PubMed]
- DiBaise, J.K. Short bowel syndrome and small bowel transplantation. Curr. Opin. Gastroenterol. 2014, 30, 128–133. [Google Scholar] [CrossRef] [PubMed]
- Pakarinen, M.P.; Kurvinen, A.; Koivusalo, A.I.; Iber, T.; Rintala, R.J. Long-term controlled outcomes after autologous intestinal reconstruction surgery in treatment of severe short bowel syndrome. J. Pediatr. Surg. 2013, 48, 339–344. [Google Scholar] [CrossRef] [PubMed]
- Hommel, M.J.; van Baren, R.; Haveman, J.W. Surgical management and autologous intestinal reconstruction in short bowel syndrome. Best Pract. Res. Clin. Gastroenterol. 2016, 30, 263–280. [Google Scholar] [CrossRef] [PubMed]
- Rege, A.; Sudan, D. Intestinal transplantation. Best Pract. Res. Clin. Gastroenterol. 2016, 30, 319–335. [Google Scholar] [CrossRef] [PubMed]
- Grant, D.; Abu-Elmagd, K.; Mazariegos, G.; Vianna, R.; Langnas, A.; Mangus, R.; Farmer, D.G.; Lacaille, F.; Iyer, K.; Fishbein, T.; et al. Intestinal transplant registry report: Global activity and trends. Am. J. Transplant. 2015, 15, 210–219. [Google Scholar] [CrossRef] [PubMed]
- Hortencio, T.D.; Arendt, B.M.; Teterina, A.; Jeejeebhoy, K.N.; Gramlich, L.M.; Whittaker, J.S.; Armstrong, D.; Raman, M.; Nogueira, R.J.; Allard, J.P.; et al. Changes in home parenteral nutrition practice based on the canadian home parenteral nutrition patient registry. JPEN J. Parenter. Enteral. Nutr. 2015. [Google Scholar] [CrossRef] [PubMed]
- Frankenfield, D.C.; Rowe, W.A.; Smith, J.S.; Cooney, R.N. Validation of several established equations for resting metabolic rate in obese and nonobese people. J. Am. Diet. Assoc. 2003, 103, 1152–1159. [Google Scholar] [CrossRef]
- Anderegg, B.A.; Worrall, C.; Barbour, E.; Simpson, K.N.; Delegge, M. Comparison of resting energy expenditure prediction methods with measured resting energy expenditure in obese, hospitalized adults. JPEN J. Parenter. Enteral. Nutr. 2009, 33, 168–175. [Google Scholar] [CrossRef] [PubMed]
- Klein, S. A primer of nutritional support for gastroenterologists. Gastroenterology 2002, 122, 1677–1687. [Google Scholar] [CrossRef] [PubMed]
- Staun, M.; Pironi, L.; Bozzetti, F.; Baxter, J.; Forbes, A.; Joly, F.; Jeppesen, P.; Moreno, J.; Hebuterne, X.; Pertkiewicz, M.; et al. Espen guidelines on parenteral nutrition: Home parenteral nutrition (Hpn) in adult patients. Clin. Nutr. 2009, 28, 467–479. [Google Scholar] [CrossRef] [PubMed]
- Van Gossum, A.; Cabre, E.; Hebuterne, X.; Jeppesen, P.; Krznaric, Z.; Messing, B.; Powell-Tuck, J.; Staun, M.; Nightingale, J. Espen guidelines on parenteral nutrition: Gastroenterology. Clin. Nutr. 2009, 28, 415–427. [Google Scholar] [CrossRef] [PubMed]
- Wanten, G.; Calder, P.C.; Forbes, A. Managing adult patients who need home parenteral nutrition. BMJ 2011, 342, d1447. [Google Scholar] [CrossRef] [PubMed]
- Duerksen, D.R.; Papineau, N.; Siemens, J.; Yaffe, C. Peripherally inserted central catheters for parenteral nutrition: A comparison with centrally inserted catheters. JPEN J. Parenter. Enteral. Nutr. 1999, 23, 85–89. [Google Scholar] [CrossRef] [PubMed]
- Mullady, D.K.; O’Keefe, S.J. Treatment of intestinal failure: Home parenteral nutrition. Nat. Clin. Pract. Gastroenterol. Hepatol. 2006, 3, 492–504. [Google Scholar] [CrossRef] [PubMed]
- Zurcher, M.; Tramer, M.R.; Walder, B. Colonization and bloodstream infection with single- versus multi-lumen central venous catheters: A quantitative systematic review. Anesth. Analg. 2004, 99, 177–182. [Google Scholar] [CrossRef] [PubMed]
- Asplin, J.R. The management of patients with enteric hyperoxaluria. Urolithiasis 2016, 44, 33–43. [Google Scholar] [CrossRef] [PubMed]
- Dibb, M.J.; Abraham, A.; Chadwick, P.R.; Shaffer, J.L.; Teubner, A.; Carlson, G.L.; Lal, S. Central venous catheter salvage in home parenteral nutrition catheter-related bloodstream infections: Long-term safety and efficacy data. JPEN J. Parenter. Enteral. Nutr. 2016, 40, 699–704. [Google Scholar] [CrossRef] [PubMed]
- Buchman, A.L.; Opilla, M.; Kwasny, M.; Diamantidis, T.G.; Okamoto, R. Risk factors for the development of catheter-related bloodstream infections in patients receiving home parenteral nutrition. JPEN J. Parenter. Enteral. Nutr. 2014, 38, 744–749. [Google Scholar] [CrossRef] [PubMed]
- Dreesen, M.; Foulon, V.; Spriet, I.; Goossens, G.A.; Hiele, M.; De Pourcq, L.; Willems, L. Epidemiology of catheter-related infections in adult patients receiving home parenteral nutrition: A systematic review. Clin. Nutr. 2013, 32, 16–26. [Google Scholar] [CrossRef] [PubMed]
- Elfassy, S.; Kassam, Z.; Amin, F.; Khan, K.J.; Haider, S.; Armstrong, D. Epidemiology and risk factors for bloodstream infections in a home parenteral nutrition program. JPEN J. Parenter. Enteral. Nutr. 2015, 39, 147–153. [Google Scholar] [CrossRef] [PubMed]
- Bisseling, T.M.; Willems, M.C.; Versleijen, M.W.; Hendriks, J.C.; Vissers, R.K.; Wanten, G.J. Taurolidine lock is highly effective in preventing catheter-related bloodstream infections in patients on home parenteral nutrition: A heparin-controlled prospective trial. Clin. Nutr. 2010, 29, 464–468. [Google Scholar] [CrossRef] [PubMed]
- Richards, D.M.; Deeks, J.J.; Sheldon, T.A.; Shaffer, J.L. Home parenteral nutrition: A systematic review. Health Technol. Assess. 1997, 1, 1–59. [Google Scholar]
- Messing, B.; Joly, F. Guidelines for management of home parenteral support in adult chronic intestinal failure patients. Gastroenterology 2006, 130, S43–S51. [Google Scholar] [CrossRef] [PubMed]
- Christensen, L.D.; Vinter-Jensen, L.; Rasmussen, H.H.; Kristensen, S.R.; Larsen, T.B. Rivaroxaban as anticoagulant therapy in short bowel syndrome. Report of three cases. Thromb. Res. 2015, 135, 568–570. [Google Scholar] [CrossRef] [PubMed]
- Salvino, R.; Ghanta, R.; Seidner, D.L.; Mascha, E.; Xu, Y.; Steiger, E. Liver failure is uncommon in adults receiving long-term parenteral nutrition. JPEN J. Parenter. Enteral. Nutr. 2006, 30, 202–208. [Google Scholar] [CrossRef] [PubMed]
- Lee, W.S.; Sokol, R.J. Intestinal microbiota, lipids, and the pathogenesis of intestinal failure-associated liver disease. J. Pediatr. 2015, 167, 519–526. [Google Scholar] [CrossRef] [PubMed]
- Cavicchi, M.; Beau, P.; Crenn, P.; Degott, C.; Messing, B. Prevalence of liver disease and contributing factors in patients receiving home parenteral nutrition for permanent intestinal failure. Ann. Intern. Med. 2000, 132, 525–532. [Google Scholar] [CrossRef] [PubMed]
- Dray, X.; Joly, F.; Reijasse, D.; Attar, A.; Alves, A.; Panis, Y.; Valleur, P.; Messing, B. Incidence, risk factors, and complications of cholelithiasis in patients with home parenteral nutrition. J. Am. Coll. Surg. 2007, 204, 13–21. [Google Scholar] [CrossRef] [PubMed]
- Reimund, J.M.; Duclos, B.; Arondel, Y.; Baumann, R. Persistent inflammation and immune activation contribute to cholestasis in patients receiving home parenteral nutrition. Nutrition 2001, 17, 300–304. [Google Scholar] [CrossRef]
- Clayton, P.T.; Whitfield, P.; Iyer, K. The role of phytosterols in the pathogenesis of liver complications of pediatric parenteral nutrition. Nutrition 1998, 14, 158–164. [Google Scholar] [CrossRef]
- Alemmari, A.; Miller, G.G.; Bertolo, R.F.; Dinesh, C.; Brunton, J.A.; Arnold, C.J.; Zello, G.A. Reduced aluminum contamination decreases parenteral nutrition associated liver injury. J. Pediatr. Surg. 2012, 47, 889–894. [Google Scholar] [CrossRef] [PubMed]
- Blaszyk, H.; Wild, P.J.; Oliveira, A.; Kelly, D.G.; Burgart, L.J. Hepatic copper in patients receiving long-term total parenteral nutrition. J. Clin. Gastroenterol. 2005, 39, 318–320. [Google Scholar] [CrossRef] [PubMed]
- Fell, J.M.; Reynolds, A.P.; Meadows, N.; Khan, K.; Long, S.G.; Quaghebeur, G.; Taylor, W.J.; Milla, P.J. Manganese toxicity in children receiving long-term parenteral nutrition. Lancet 1996, 347, 1218–1221. [Google Scholar] [CrossRef]
- Buchman, A.L.; Ament, M.E.; Sohel, M.; Dubin, M.; Jenden, D.J.; Roch, M.; Pownall, H.; Farley, W.; Awal, M.; Ahn, C. Choline deficiency causes reversible hepatic abnormalities in patients receiving parenteral nutrition: Proof of a human choline requirement: A placebo-controlled trial. JPEN J. Parenter. Enteral. Nutr. 2001, 25, 260–268. [Google Scholar] [CrossRef] [PubMed]
- Spencer, A.U.; Yu, S.; Tracy, T.F.; Aouthmany, M.M.; Llanos, A.; Brown, M.B.; Brown, M.; Shulman, R.J.; Hirschl, R.B.; Derusso, P.A.; et al. Parenteral nutrition-associated cholestasis in neonates: Multivariate analysis of the potential protective effect of taurine. JPEN J. Parenter. Enteral. Nutr. 2005, 29, 337–343, discussion 343–334. [Google Scholar] [CrossRef] [PubMed]
- Harris, J.K.; El Kasmi, K.C.; Anderson, A.L.; Devereaux, M.W.; Fillon, S.A.; Robertson, C.E.; Wagner, B.D.; Stevens, M.J.; Pace, N.R.; Sokol, R.J. Specific microbiome changes in a mouse model of parenteral nutrition associated liver injury and intestinal inflammation. PLoS ONE 2014, 9, e110396. [Google Scholar] [CrossRef] [PubMed]
- Capron, J.P.; Gineston, J.L.; Herve, M.A.; Braillon, A. Metronidazole in prevention of cholestasis associated with total parenteral nutrition. Lancet 1983, 1, 446–447. [Google Scholar] [CrossRef]
- McClure, R.J.; Newell, S.J. Randomised controlled study of clinical outcome following trophic feeding. Arch. Dis. Child. Fetal. Neonatal. Ed. 2000, 82, F29–F33. [Google Scholar] [CrossRef] [PubMed]
- Hwang, T.L.; Lue, M.C.; Chen, L.L. Early use of cyclic tpn prevents further deterioration of liver functions for the tpn patients with impaired liver function. Hepatogastroenterology 2000, 47, 1347–1350. [Google Scholar] [PubMed]
- Beau, P.; Labat-Labourdette, J.; Ingrand, P.; Beauchant, M. Is ursodeoxycholic acid an effective therapy for total parenteral nutrition-related liver disease? J. Hepatol. 1994, 20, 240–244. [Google Scholar] [CrossRef]
- Lauverjat, M.; Hadj Aissa, A.; Vanhems, P.; Bouletreau, P.; Fouque, D.; Chambrier, C. Chronic dehydration may impair renal function in patients with chronic intestinal failure on long-term parenteral nutrition. Clin. Nutr. 2006, 25, 75–81. [Google Scholar] [CrossRef] [PubMed]
- Smith, L.H.; Fromm, H.; Hofmann, A.F. Acquired hyperoxaluria, nephrolithiasis, and intestinal disease. Description of a syndrome. N. Engl. J. Med. 1972, 286, 1371–1375. [Google Scholar] [CrossRef] [PubMed]
- Amiot, A.; Messing, B.; Corcos, O.; Panis, Y.; Joly, F. Determinants of home parenteral nutrition dependence and survival of 268 patients with non-malignant short bowel syndrome. Clin. Nutr. 2013, 32, 368–374. [Google Scholar] [CrossRef] [PubMed]
- Jeppesen, P.B.; Langholz, E.; Mortensen, P.B. Quality of life in patients receiving home parenteral nutrition. Gut 1999, 44, 844–852. [Google Scholar] [CrossRef] [PubMed]
- Huisman-de Waal, G.; Schoonhoven, L.; Jansen, J.; Wanten, G.; van Achterberg, T. The impact of home parenteral nutrition on daily life-a review. Clin. Nutr. 2007, 26, 275–288. [Google Scholar] [CrossRef] [PubMed]
- Lawinski, M.; Kot-Mielczarska, E.; Gradowska, A. Quality of life of patients on chronic parenteral nutrition before and after gastrointestinal tract continuity restoration. Pol. Przegl. Chir. 2015, 87, 153–159. [Google Scholar] [PubMed]
- Girke, J.; Seipt, C.; Markowski, A.; Luettig, B.; Schettler, A.; Momma, M.; Schneider, A.S. Quality of life and nutrition condition of patients improve under home parenteral nutrition: An exploratory study. Nutr. Clin. Pract. 2016, 31, 659–665. [Google Scholar] [CrossRef] [PubMed]
- Saqui, O.; Fernandes, G.; Allard, J.P. Quality of life analysis during transition from stationary to portable infusion pump in home parenteral nutrition patients: A canadian experience. Nutr. Clin. Pract. 2014, 29, 131–141. [Google Scholar] [CrossRef] [PubMed]
- Baxter, J.P.; Fayers, P.M.; McKinlay, A.W. A review of the quality of life of adult patients treated with long-term parenteral nutrition. Clin. Nutr. 2006, 25, 543–553. [Google Scholar] [CrossRef] [PubMed]
- Scolapio, J.S.; Fleming, C.R.; Kelly, D.G.; Wick, D.M.; Zinsmeister, A.R. Survival of home parenteral nutrition-treated patients: 20 years of experience at the mayo clinic. Mayo Clin. Proc. 1999, 74, 217–222. [Google Scholar] [CrossRef] [PubMed]
- Pironi, L.; Goulet, O.; Buchman, A.; Messing, B.; Gabe, S.; Candusso, M.; Bond, G.; Gupte, G.; Pertkiewicz, M.; Steiger, E.; et al. Outcome on home parenteral nutrition for benign intestinal failure: A review of the literature and benchmarking with the european prospective survey of espen. Clin. Nutr. 2012, 31, 831–845. [Google Scholar] [CrossRef] [PubMed]
- Harrison, E.; Allan, P.; Ramu, A.; Vaidya, A.; Travis, S.; Lal, S. Management of intestinal failure in inflammatory bowel disease: Small intestinal transplantation or home parenteral nutrition? World J. Gastroenterol. 2014, 20, 3153–3163. [Google Scholar] [CrossRef] [PubMed]
- Raman, M.; Aghdassi, E.; Baun, M.; Yeung, M.; Fairholm, L.; Saqui, O.; Allard, J.P. Metabolic bone disease in patients receiving home parenteral nutrition: A canadian study and review. JPEN J. Parenter. Enteral. Nutr. 2006, 30, 492–496. [Google Scholar] [CrossRef] [PubMed]
- Saqui, O.; Raman, M.; Chang, A.; Allard, J.P. Catheter-related infections in a Canadian home total parenteral nutrition program: A prospective study using U.S. Centers for disease control and prevention criteria. J. Assoc. Vasc. Access 2007, 12, 85–88. [Google Scholar] [CrossRef]
- Aljarallah, B.; Fernandes, G.; Jeejeebhoy, K.N.; Gramlich, L.M.; Whittaker, J.S.; Armstrong, D.; Duerksen, D.R.; Allard, J.P. The canadian home total parenteral nutrition (HTPN) registry: Vitamin K supplementation and bone mineral density. JPEN J. Parenter. Enteral. Nutr. 2012, 36, 415–420. [Google Scholar] [CrossRef] [PubMed]
- Jawa, H.; Fernandes, G.; Saqui, O.; Allard, J.P. Home parenteral nutrition in patients with systemic sclerosis: A retrospective review of 12 cases. J. Rheumatol. 2012, 39, 1004–1007. [Google Scholar] [CrossRef] [PubMed]
- Abdalian, R.; Saqui, O.; Fernandes, G.; Allard, J.P. Effects of manganese from a commercial multi-trace element supplement in a population sample of canadian patients on long-term parenteral nutrition. JPEN J. Parenter. Enteral. Nutr. 2013, 37, 538–543. [Google Scholar] [CrossRef] [PubMed]
© 2017 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Bielawska, B.; Allard, J.P. Parenteral Nutrition and Intestinal Failure. Nutrients 2017, 9, 466. https://doi.org/10.3390/nu9050466
Bielawska B, Allard JP. Parenteral Nutrition and Intestinal Failure. Nutrients. 2017; 9(5):466. https://doi.org/10.3390/nu9050466
Chicago/Turabian StyleBielawska, Barbara, and Johane P. Allard. 2017. "Parenteral Nutrition and Intestinal Failure" Nutrients 9, no. 5: 466. https://doi.org/10.3390/nu9050466
APA StyleBielawska, B., & Allard, J. P. (2017). Parenteral Nutrition and Intestinal Failure. Nutrients, 9(5), 466. https://doi.org/10.3390/nu9050466



