Dietary Factors and Female Breast Cancer Risk: A Prospective Cohort Study
Abstract
:1. Introduction
2. Materials and Methods
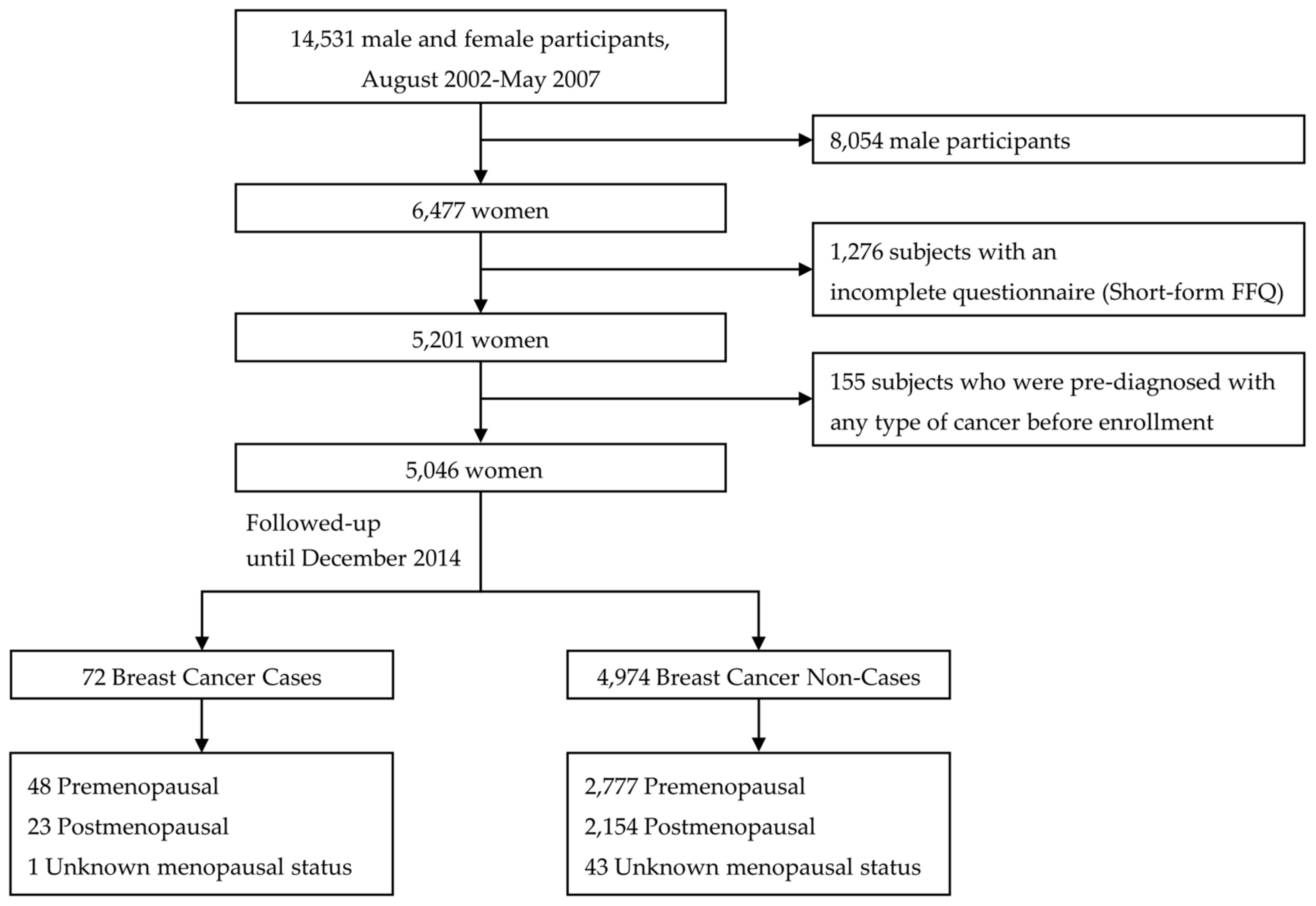
2.1. Study Population
2.2. Data Collection and Management
2.3. Statistical Analysis
3. Results
4. Discussion
5. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
Appendix A
| Food list for the 16 food groups in the short-form FFQ: | |
| Food group | Food list |
| Cereals | Rice, bread, noodles, potatoes, sweet potatoes |
| Salted vegetables and seafood | Kimchi, salted fermented seafood, food boiled in soya with spices |
| Light-colored vegetables | Bean sprouts, cucumbers, radishes, onions, bellflower |
| Green-yellow vegetables | Carrots, spinach, sesame leaf, lettuce, zucchini, dropwort |
| Seaweed | Laver, brown seaweed, tangle |
| Fruit | Apples, tangerines, grapes, watermelon, strawberries, peaches, pears, fruit juice |
| Grilled meat | Grilled ribs, barbecue |
| Healthy protein foods | Lean meat, fish, legumes, soy foods (e.g., soybean curd), egg whites |
| Dairy foods | Yogurt, cheese, milk |
| Bony fish | Anchovies, dried whitebait |
| Fried foods | Deep-fried food, stir-fried food |
| High-cholesterol foods | Egg yolks, seafood (eel, shrimp, squid), organ meats (from fish or other animals) |
| Animal fat-rich foods | High-fat red meat (beef, pork), processed food (ham, sausage), butter |
| Sweet foods | Bread, cookies, chocolate, honey, candy, ice cream |
| Fast foods | Pizza, chicken, processed food |
| Caffeinated drinks | Coffee, black tea, cocoa, coke |
References
- Ferlay, J.; Soerjomataram, I.; Dikshit, R.; Eser, S.; Mathers, C.; Rebelo, M.; Parkin, D.M.; Forman, D.; Bray, F. Cancer incidence and mortality worldwide: Sources, methods and major patterns in GLOBOCAN 2012. Int. J. Cancer 2015, 136, E359–E386. [Google Scholar]
- Siegel, R.L.; Miller, K.D.; Jemal, A. Cancer statistics, 2017. CA Cancer J. Clin. 2017, 67, 7–30. [Google Scholar] [CrossRef]
- Oh, C.M.; Won, Y.J.; Jung, K.W.; Kong, H.J.; Cho, H.; Lee, J.K.; Lee, D.H.; Lee, K.H. Cancer statistics in Korea: incidence, mortality, survival, and prevalence in 2013. Cancer Res. Treat. 2016, 48, 436–450. [Google Scholar] [CrossRef]
- Park, S.K.; Kim, Y.; Kang, D.; Jung, E.J.; Yoo, K.Y. Risk factors and control strategies for the rapidly rising rate of breast cancer in Korea. J. Breast Cancer 2011, 14, 79–87. [Google Scholar] [CrossRef]
- Doll, R.; Peto, R. The causes of cancer: Quantitative estimates of avoidable risks of cancer in the United States today. J. Natl. Cancer Inst. 1981, 66, 1192–1308. [Google Scholar] [CrossRef]
- Kotepui, M. Diet and risk of breast cancer. Contemp. Oncol. 2016, 20, 13–19. [Google Scholar]
- Michels, K.B.; Mohllajee, A.P.; Roset-Bahmanyar, E.; Beehler, G.P.; Moysich, K.B. Diet and breast cancer. Cancer 2007, 109, 2712–2749. [Google Scholar] [CrossRef]
- Guo, J.; Wei, W.; Zhan, L. Red and processed meat intake and risk of breast cancer: A meta-analysis of prospective studies. Breast Cancer Res. Treat. 2015, 151, 191–198. [Google Scholar] [CrossRef] [PubMed]
- Park, B.; Park, S.; Shin, H.R.; Shin, A.; Yeo, Y.; Choi, J.Y.; Jung, K.W.; Kim, B.G.; Kim, Y.M.; Noh, D.Y. Population attributable risks of modifiable reproductive factors for breast and ovarian cancers in Korea. BMC Cancer 2016, 16, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Kim, Z.; Min, S.Y.; Yoon, C.S.; Lee, H.J.; Lee, J.S.; Youn, H.J.; Park, H.K.; Noh, D.Y.; Hur, M.H. The basic facts of Korean breast cancer in 2011: Results of a nationwide survey and breast cancer registry database. J. Breast Cancer 2014, 17, 99–106. [Google Scholar] [CrossRef]
- Lee, S.K.; Sobal, J. Socio-economic, dietary, activity, nutrition and body weight transitions in South Korea. Public Health Nutr. 2003, 6, 665–674. [Google Scholar] [CrossRef] [PubMed]
- Paik, N.S. Current status of breast cancer in Korea. Ewha Med. J. 2014, 37, 69–74. [Google Scholar] [CrossRef]
- Kim, S.; Moon, S.; Popkin, B.M. The nutrition transition in South Korea. Am. J. Clin. Nutr. 2000, 71, 44–53. [Google Scholar] [PubMed]
- Lee, M.J.; Popkin, B.M.; Kim, S. The unique aspects of the nutrition transition in South Korea: The retention of healthful elements in their traditional diet. Public Health Nutr. 2002, 5, 197–203. [Google Scholar] [CrossRef] [PubMed]
- Jun, S.; Ha, K.; Chung, S.; Joung, H. Meat and milk intake in the rice-based Korean diet: Impact on cancer and metabolic syndrome. Proc. Nutr. Soc. 2016, 75, 374–384. [Google Scholar] [CrossRef] [PubMed]
- Woo, H.D.; Kim, J. Nutritional epidemiology of cancer in Korea: Recent accomplishments and future directions. Asian Pac. J. Cancer Prev. 2011, 12, 2377–2383. [Google Scholar] [PubMed]
- Park, M.K.; Paik, H.Y.; Lee, Y. Intake Trends of red meat, alcohol, and fruits and vegetables as cancer-related dietary factors from 1998 to 2009. Osong Public Health Res. Perspect. 2016, 7, 180–189. [Google Scholar] [CrossRef] [PubMed]
- Chen, W.Y.; Rosner, B.; Hankinson, S.E.; Colditz, G.A.; Willett, W.C. Moderate alcohol consumption during adult life, drinking patterns, and breast cancer risk. JAMA 2011, 306, 1884–1890. [Google Scholar] [CrossRef] [PubMed]
- Taylor, E.; Burley, V.; Greenwood, D.; Cade, J. Meat consumption and risk of breast cancer in the UK Women’s Cohort Study. Br. J. Cancer 2007, 96, 1139–1146. [Google Scholar] [CrossRef] [PubMed]
- Kruk, J.; Marchlewicz, M. Dietary fat and physical activity in relation to breast cancer among Polish women. Asian Pac. J. Cancer Prev. 2013, 14, 2495–2502. [Google Scholar] [CrossRef] [PubMed]
- Kallianpur, A.R.; Lee, S.A.; Gao, Y.T.; Lu, W.; Zheng, Y.; Ruan, Z.X.; Dai, Q.; Gu, K.; Shu, X.O.; Zheng, W. Dietary animal-derived iron and fat intake and breast cancer risk in the Shanghai Breast Cancer Study. Breast Cancer Res. Treat. 2008, 107, 123–132. [Google Scholar] [CrossRef] [PubMed]
- Masala, G.; Assedi, M.; Bendinelli, B.; Ermini, I.; Sieri, S.; Grioni, S.; Sacerdote, C.; Ricceri, F.; Panico, S.; Mattiello, A.; et al. Fruit and vegetables consumption and breast cancer risk: The EPIC Italy study. Breast Cancer Res. Treat. 2012, 132, 1127–1136. [Google Scholar] [CrossRef] [PubMed]
- Ferrari, P.; Rinaldi, S.; Jenab, M.; Lukanova, A.; Olsen, A.; Tjønneland, A.; Overvad, K.; Clavel-Chapelon, F.; Fagherazzi, G.; Touillaud, M.; et al. Dietary fiber intake and risk of hormonal receptor–defined breast cancer in the European Prospective Investigation into cancer and nutrition study. Am. J. Clin. Nutr. 2013, 97, 344–353. [Google Scholar] [CrossRef] [PubMed]
- Brennan, S.F.; Cantwell, M.M.; Cardwell, C.R.; Velentzis, L.S.; Woodside, J.V. Dietary patterns and breast cancer risk: A systematic review and meta-analysis. Am. J. Clin. Nutr. 2010, 91, 1294–1302. [Google Scholar] [CrossRef] [PubMed]
- Romieu, I. Diet and breast cancer. Salud Publica Mexico 2011, 53, 430–439. [Google Scholar]
- WCRF/AICR. Food, Nutrition, Physical Activity, and the Prevention of Cancer: A Global Perspective; AICR: Washington, DC, USA, 2007. [Google Scholar]
- Hu, F.B. Dietary pattern analysis: A new direction in nutritional epidemiology. Curr. Opin. Lipidol. 2002, 13, 3–9. [Google Scholar] [CrossRef] [PubMed]
- Wie, G.A.; Cho, Y.A.; Kang, H.H.; Ryu, K.A.; Yoo, M.K.; Kim, Y.A.; Jung, K.W.; Kim, J.; Lee, J.H.; Joung, H.J. Red meat consumption is associated with an increased overall cancer risk: A prospective cohort study in Korea. Br. J. Nutr. 2014, 112, 238–247. [Google Scholar] [CrossRef] [PubMed]
- Woo, H.D.; Park, S.; Oh, K.; Kim, H.J.; Shin, H.R.; Moon, H.K.; Kim, J. Diet and cancer risk in the Korean population: A meta-analysis. Asian Pac. J. Cancer Prev. 2014, 15, 8509–8519. [Google Scholar] [CrossRef] [PubMed]
- Shin, A.; Lim, S.Y.; Sung, J.; Shin, H.R.; Kim, J. Dietary intake, eating habits, and metabolic syndrome in Korean men. J. Am. Diet. Assoc. 2009, 109, 633–640. [Google Scholar] [CrossRef] [PubMed]
- Shin, A.; Lim, S.; Sung, J.; Myung, S.; Kim, J. Dietary habit and bone mineral density in Korean postmenopausal women. Osteoporos. Int. 2010, 21, 947–955. [Google Scholar] [CrossRef] [PubMed]
- Cho, Y.A.; Kim, J.; Cho, E.R.; Shin, A. Dietary patterns and the prevalence of metabolic syndrome in Korean women. Nutr. Metab. Cardiovasc. Dis. 2011, 21, 893–900. [Google Scholar] [CrossRef] [PubMed]
- Cho, E.R.; Shin, A.; Lim, S.Y.; Kim, J. Dietary patterns and their associations with health behaviours in Korea. Public Health Nutr. 2011, 14, 356–364. [Google Scholar] [CrossRef] [PubMed]
- Farvid, M.S.; Cho, E.; Eliassen, A.H.; Chen, W.Y.; Willett, W.C. Lifetime grain consumption and breast cancer risk. Breast Cancer Res. Treat. 2016, 159, 335–345. [Google Scholar] [CrossRef] [PubMed]
- Reeves, G.K.; Pirie, K.; Green, J.; Bull, D.; Beral, V. Reproductive factors and specific histological types of breast cancer: Prospective study and meta-analysis. Br. J. Cancer 2009, 100, 538–544. [Google Scholar] [CrossRef] [PubMed]
- Abid, Z.; Cross, A.J.; Sinha, R. Meat, dairy, and cancer. Am. J. Clin. Nutr. 2014, 100, 386S–393S. [Google Scholar] [CrossRef] [PubMed]
- Knize, M.G.; Salmon, C.P.; Pais, P.; Felton, J.S. Food heating and the formation of heterocyclic aromatic amine and polycyclic aromatic hydrocarbon mutagens/carcinogens. Adv. Exp. Med. Biol. 1999, 459, 179–194. [Google Scholar] [PubMed]
- Jägerstad, M.; Skog, K. Formation of meat mutagens. Adv. Exp. Med. Biol. 1991, 289, 83–105. [Google Scholar] [PubMed]
- Phillips, D.H. Polycyclic aromatic hydrocarbons in the diet. Mutat. Res. Genet. Toxicol. Environ. Mutagen. 1999, 443, 139–147. [Google Scholar] [CrossRef]
- White, A.J.; Bradshaw, P.T.; Herring, A.H.; Teitelbaum, S.L.; Beyea, J.; Stellman, S.D.; Steck, S.E.; Mordukhovich, I.; Eng, S.M.; Engel, L.S.; et al. Exposure to multiple sources of polycyclic aromatic hydrocarbons and breast cancer incidence. Environ. Int. 2016, 89, 185–192. [Google Scholar] [CrossRef] [PubMed]
- Mourouti, N.; Kontogianni, M.D.; Papavagelis, C.; Plytzanopoulou, P.; Vassilakou, T.; Psaltopoulou, T.; Malamos, N.; Linos, A.; Panagiotakos, D.B. Meat consumption and breast cancer: A case–control study in women. Meat Sci. 2015, 100, 195–201. [Google Scholar] [CrossRef] [PubMed]
- Kabat, G.C.; Cross, A.J.; Park, Y.; Schatzkin, A.; Hollenbeck, A.R.; Rohan, T.E.; Sinha, R. Meat intake and meat preparation in relation to risk of postmenopausal breast cancer in the NIH-AARP diet and health study. Int. J. Cancer 2009, 124, 2430–2435. [Google Scholar] [CrossRef] [PubMed]
- Fu, Z.; Deming, S.L.; Fair, A.M.; Shrubsole, M.J.; Wujcik, D.M.; Shu, X.O.; Kelley, M.; Zheng, W. Well-done meat intake and meat-derived mutagen exposures in relation to breast cancer risk: The Nashville Breast Health Study. Breast Cancer Res. Treat. 2011, 129, 919–928. [Google Scholar] [CrossRef] [PubMed]
- Dai, Q.; Shu, X.O.; Jin, F.; Gao, Y.T.; Ruan, Z.X.; Zheng, W. Consumption of animal foods, cooking methods, and risk of breast cancer. Cancer Epidemiol. Biomark. Prev. 2002, 11, 801–808. [Google Scholar]
- Ferrucci, L.; Cross, A.; Graubard, B.; Brinton, L.; McCarty, C.; Ziegler, R.; Ma, X.; Mayne, S.; Sinha, R. Intake of meat, meat mutagens, and iron and the risk of breast cancer in the Prostate, Lung, Colorectal, and Ovarian Cancer Screening Trial. Br. J. Cancer 2009, 101, 178–184. [Google Scholar] [CrossRef] [PubMed]
- Steck, S.E.; Gaudet, M.M.; Eng, S.M.; Britton, J.A.; Teitelbaum, S.L.; Neugut, A.I.; Santella, R.M.; Gammon, M.D. Cooked meat and risk of breast cancer—Lifetime versus recent dietary intake. Epidemiology 2007, 18, 373–382. [Google Scholar] [CrossRef] [PubMed]
- Siiteri, P.K. Adipose tissue as a source of hormones. Am. J. Clin. Nutr. 1987, 45, 277–282. [Google Scholar] [PubMed]
- Clemons, M.; Goss, P. Estrogen and the risk of breast cancer. N. Engl. J. Med. 2001, 344, 276–285. [Google Scholar] [CrossRef] [PubMed]
- Cleary, M.P.; Grossmann, M.E. Obesity and breast cancer: The estrogen connection. Endocrinology 2009, 150, 2537–2542. [Google Scholar] [CrossRef] [PubMed]
- Balogh, Z.; Gray, J.; Gomaa, E.; Booren, A. Formation and inhibition of heterocyclic aromatic amines in fried ground beef patties. Food Chem. Toxicol. 2000, 38, 395–401. [Google Scholar] [CrossRef]
- Uribarri, J.; Woodruff, S.; Goodman, S.; Cai, W.; Chen, X.; Pyzik, R.; Yong, A.; Striker, G.E.; Vlassara, H. Advanced glycation end products in foods and a practical guide to their reduction in the diet. J. Am. Diet. Assoc. 2010, 110, 911–916. [Google Scholar] [CrossRef] [PubMed]
- Turner, D. Chapter One-The role of advanced glycation end-products in cancer disparity. Adv. Cancer Res. 2017, 133, 1–22. [Google Scholar] [PubMed]
- Jiao, L.; Stolzenberg-Solomon, R.; Zimmerman, T.P.; Duan, Z.; Chen, L.; Kahle, L.; Risch, A.; Subar, A.F.; Cross, A.J.; Hollenbeck, A.; et al. Dietary consumption of advanced glycation end products and pancreatic cancer in the prospective NIH-AARP Diet and Health Study. Am. J. Clin. Nutr. 2015, 101, 126–134. [Google Scholar] [CrossRef] [PubMed]
- Perrone, L.; Grant, W.B. Observational and ecological studies of dietary advanced glycation end products in national diets and Alzheimer’s disease incidence and prevalence. J. Alzheimers Dis. 2015, 45, 965–979. [Google Scholar] [PubMed]
- Jiao, L.; Kramer, J.R.; Chen, L.; Rugge, M.; Parente, P.; Verstovsek, G.; Alsarraj, A.; El-Serag, H.B. Dietary consumption of meat, fat, animal products and advanced glycation end-products and the risk of Barrett’s oesophagus. Aliment. Pharmacol. Ther. 2013, 38, 817–824. [Google Scholar] [CrossRef] [PubMed]
- Tesarova, P.; Zima, T.; Kubena, A.A.; Kalousova, M. Polymorphisms of the receptor for advanced glycation end products and glyoxalase I and long-term outcome in patients with breast cancer. Tumour Biol. 2017, 39. [Google Scholar] [CrossRef] [PubMed]
- Nankali, M.; Karimi, J.; Goodarzi, M.T.; Saidijam, M.; Khodadadi, I.; Razavi, A.N.E.; Rahimi, F. Increased expression of the receptor for advanced glycation end-products (RAGE) is associated with advanced breast cancer stage. Oncol. Res. Treat. 2016, 39, 622–628. [Google Scholar] [CrossRef] [PubMed]
- Nass, N.; Ignatov, A.; Andreas, L.; Weißenborn, C.; Kalinski, T.; Sel, S. Accumulation of the advanced glycation end product carboxymethyl lysine in breast cancer is positively associated with estrogen receptor expression and unfavorable prognosis in estrogen receptor-negative cases. Histochem. Cell Biol. 2017, 147, 625–634. [Google Scholar] [CrossRef] [PubMed]
- Danilo, C.; Frank, P.G. Cholesterol and breast cancer development. Curr. Opin. Pharmacol. 2012, 12, 677–682. [Google Scholar] [CrossRef] [PubMed]
- Ronco, A.L.; De Stéfani, E.; Stoll, M. Hormonal and metabolic modulation through nutrition: Towards a primary prevention of breast cancer. Breast 2010, 19, 322–332. [Google Scholar] [CrossRef] [PubMed]
- Nelson, E.R.; Chang, C.-Y.; McDonnell, D.P. Cholesterol and breast cancer pathophysiology. Trends Endocrinol. Metab. 2014, 25, 649–655. [Google Scholar] [CrossRef] [PubMed]
- De Stefani, E.; Deneo Pellegrini, H.; Mendilaharsu, M.; Ronco, A. Essential fatty acids and breast cancer: A case-control study in Uruguay. Int. J. Cancer 1998, 76, 491–494. [Google Scholar] [CrossRef]
- Hu, J.; La Vecchia, C.; de Groh, M.; Negri, E.; Morrison, H.; Mery, L. Dietary cholesterol intake and cancer. Ann. Oncol. 2012, 23, 491–500. [Google Scholar] [CrossRef] [PubMed]
- Al Othaimeen, A.; Ezzat, A.; Mohamed, G.; Muammar, T.; Al Madouj, A. Dietary fat and breast cancer in Saudi Arabia: A case-control study. East Mediterr. Health J. 2004, 10, 879–886. [Google Scholar]
- Farvid, M.S.; Cho, E.; Chen, W.Y.; Eliassen, A.H.; Willett, W.C. Premenopausal dietary fat in relation to pre-and post-menopausal breast cancer. Breast Cancer Res. Treat. 2014, 145, 255–265. [Google Scholar] [CrossRef] [PubMed]
- Boeke, C.E.; Eliassen, A.H.; Chen, W.Y.; Cho, E.; Holmes, M.D.; Rosner, B.; Willett, W.C.; Tamimi, R.M. Dietary fat intake in relation to lethal breast cancer in two large prospective cohort studies. Breast Cancer Res. Treat. 2014, 146, 383–392. [Google Scholar] [CrossRef] [PubMed]
- Jones, D.Y.; Schatzkin, A.; Green, S.B.; Block, G.; Brinton, L.A.; Ziegler, R.G.; Hoover, R.; Taylor, P.R. Dietary fat and breast cancer in the National Health and Nutrition Examination Survey I epidemiologic follow-up study. J. Natl. Cancer Inst. 1987, 79, 465–471. [Google Scholar] [CrossRef]
- Knekt, P.; Albanes, D.; Seppänen, R.; Aromaa, A.; Järvinen, R.; Hyvönen, L.; Teppo, L.; Pukkala, E. Dietary fat and risk of breast cancer. Am. J. Clin. Nutr. 1990, 52, 903–908. [Google Scholar] [PubMed]
- Kushi, L.H.; Sellers, T.A.; Potter, J.D.; Nelson, C.L.; Munger, R.G.; Kaye, S.A.; Folsom, A.R. Dietary fat and postmenopausal breast cancer. J. Natl. Cancer Inst. 1992, 84, 1092–1099. [Google Scholar] [CrossRef] [PubMed]
- Van den Brandt, P.A.; van’t Veer, P.; Goldbohm, R.A.; Dorant, E.; Volovics, A.; Hermus, R.J.; Sturmans, F. A prospective cohort study on dietary fat and the risk of postmenopausal breast cancer. Cancer Res. 1993, 53, 75–82. [Google Scholar] [PubMed]
- Li, C.; Yang, L.; Zhang, D.; Jiang, W. Systematic review and meta-analysis suggest that dietary cholesterol intake increases risk of breast cancer. Nutr. Res. 2016, 36, 627–635. [Google Scholar] [CrossRef] [PubMed]
- Inoue Choi, M.; Sinha, R.; Gierach, G.L.; Ward, M.H. Red and processed meat, nitrite, and heme iron intakes and postmenopausal breast cancer risk in the NIH-AARP diet and health study. Int. J. Cancer 2016, 138, 1609–1618. [Google Scholar] [CrossRef] [PubMed]
- Pala, V.; Krogh, V.; Berrino, F.; Sieri, S.; Grioni, S.; Tjønneland, A.; Olsen, A.; Jakobsen, M.U.; Overvad, K.; Clavel-Chapelon, F.; et al. Meat, eggs, dairy products, and risk of breast cancer in the European Prospective Investigation into Cancer and Nutrition (EPIC) cohort. Am. J. Clin. Nutr. 2009, 90, 602–612. [Google Scholar] [CrossRef] [PubMed]
- Egeberg, R.; Olsen, A.; Autrup, H.; Christensen, J.; Stripp, C.; Tetens, I.; Overvad, K.; Tjønneland, A. Meat consumption, N-acetyl transferase 1 and 2 polymorphism and risk of breast cancer in Danish postmenopausal women. Eur. J. Cancer Prev. 2008, 17, 39–47. [Google Scholar] [CrossRef] [PubMed]
- Hu, J.; La Vecchia, C.; Morrison, H.; Negri, E.; Mery, L. Salt, processed meat and the risk of cancer. Eur. J. Cancer Prev. 2011, 20, 132–139. [Google Scholar] [CrossRef] [PubMed]
- Cross, A.J.; Leitzmann, M.F.; Gail, M.H.; Hollenbeck, A.R.; Schatzkin, A.; Sinha, R. A prospective study of red and processed meat intake in relation to cancer risk. PLoS Med. 2007, 4, e325. [Google Scholar] [CrossRef] [PubMed]
- Wu, K.; Sinha, R.; Holmes, M.D.; Giovannucci, E.; Willett, W.; Cho, E. Meat mutagens and breast cancer in postmenopausal women—A cohort analysis. Cancer Epidemiol. Biomark. Prev. 2010, 19, 1301–1310. [Google Scholar] [CrossRef] [PubMed]
- Genkinger, J.M.; Makambi, K.H.; Palmer, J.R.; Rosenberg, L.; Adams-Campbell, L.L. Consumption of dairy and meat in relation to breast cancer risk in the Black Women’s Health Study. Cancer Causes Control 2013, 24, 675–684. [Google Scholar] [CrossRef] [PubMed]
- Holmes, M.D.; Colditz, G.A.; Hunter, D.J.; Hankinson, S.E.; Rosner, B.; Speizer, F.E.; Willett, W.C. Meat, fish and egg intake and risk of breast cancer. Int. J. Cancer 2003, 104, 221–227. [Google Scholar] [CrossRef] [PubMed]
- Gandini, S.; Merzenich, H.; Robertson, C.; Boyle, P. Meta-analysis of studies on breast cancer risk and diet: The role of fruit and vegetable consumption and the intake of associated micronutrients. Eur. J. Cancer 2000, 36, 636–646. [Google Scholar] [CrossRef]
- Yu, H.; Hwang, J.Y.; Ro, J.; Kim, J.; Chang, N. Vegetables, but not pickled vegetables, are negatively associated with the risk of breast cancer. Nutr. Cancer 2010, 62, 443–453. [Google Scholar] [CrossRef] [PubMed]
- Cho, Y.A.; Kim, J.; Shin, A.; Park, K.-S.; Ro, J. Dietary patterns and breast cancer risk in Korean women. Nutr. Cancer 2010, 62, 1161–1169. [Google Scholar] [CrossRef] [PubMed]
- Nicodemus, K.K.; Jacobs, D.R.; Folsom, A.R. Whole and refined grain intake and risk of incident postmenopausal breast cancer (United States). Cancer Causes Control 2001, 12, 917–925. [Google Scholar] [CrossRef] [PubMed]
- Egeberg, R.; Olsen, A.; Loft, S.; Christensen, J.; Johnsen, N.F.; Overvad, K.; Tjønneland, A. Intake of whole grain products and risk of breast cancer by hormone receptor status and histology among postmenopausal women. Int. J. Cancer 2009, 124, 745–750. [Google Scholar] [CrossRef] [PubMed]
- Franceschi, S.; La Vecchia, C.; Russo, A.; Negri, E.; Favero, A.; Decarli, A. Low-risk diet for breast cancer in Italy. Cancer Epidemiol. Biomark. Prev. 1997, 6, 875–879. [Google Scholar]
- Potischman, N.; Coates, R.J.; Swanson, C.A.; Carroll, R.J.; Daling, J.R.; Brogan, D.R.; Gammon, M.D.; Midthune, D.; Curtin, J.; Brinton, L.A. Increased risk of early-stage breast cancer related to consumption of sweet foods among women less than age 45 in the United States. Cancer Causes Control 2002, 13, 937–946. [Google Scholar] [CrossRef] [PubMed]
- Tavani, A.; Giordano, L.; Gallus, S.; Talamini, R.; Franceschi, S.; Giacosa, A.; Montella, M.; La Vecchia, C. Consumption of sweet foods and breast cancer risk in Italy. Annal. Oncol. 2006, 17, 341–345. [Google Scholar] [CrossRef] [PubMed]
- Dong, J.Y.; Zhang, L.; He, K.; Qin, L.Q. Dairy consumption and risk of breast cancer: A meta-analysis of prospective cohort studies. Breast Cancer Res. Treat. 2011, 127, 23–31. [Google Scholar] [CrossRef] [PubMed]
- Ganmaa, D.; Willett, W.C.; Li, T.Y.; Feskanich, D.; van Dam, R.M.; Lopez-Garcia, E.; Hunter, D.J.; Holmes, M.D. Coffee, tea, caffeine and risk of breast cancer: A 22-year follow-up. Int. J. Cancer 2008, 122, 2071–2076. [Google Scholar] [CrossRef] [PubMed]
- Marinac, C.R.; Sears, D.D.; Natarajan, L.; Gallo, L.C.; Breen, C.I.; Patterson, R.E. Frequency and circadian timing of eating may influence biomarkers of inflammation and insulin resistance associated with breast cancer risk. PLoS ONE 2015, 10, e0136240. [Google Scholar] [CrossRef] [PubMed]
- Mahoney, M.C.; Bevers, T.; Linos, E.; Willett, W.C. Opportunities and strategies for breast cancer prevention through risk reduction. CA Cancer J. Clin. 2008, 58, 347–371. [Google Scholar] [CrossRef] [PubMed]
| Characteristics | Total (n = 5046) | Premenopausal (n = 2825) | Postmenopausal (n = 2177) | ||||||
|---|---|---|---|---|---|---|---|---|---|
| Non-Cases (n = 4974) | Cases (n = 72) | p Value | Non-Cases (n = 2777) | Cases (n = 48) | p Value | Non-Cases (n = 2154) | Cases (n = 23) | p Value | |
| Age (years) | |||||||||
| <40 | 1025 (20.6) | 10 (13.9) | 0.06 | 1000 (36.0) | 10 (20.8) | 0.09 | 15 (0.7) | 0 (0.0) | 0.33 |
| 40–49 | 1951 (39.2) | 39 (54.2) | 1599 (57.6) | 34 (70.8) | 336 (15.6) | 5 (21.7) | |||
| 50–59 | 1390 (28.0) | 14 (19.4) | 177 (6.4) | 4 (8.3) | 1201 (55.8) | 9 (39.1) | |||
| 60+ | 608 (12.2) | 9 (12.5) | 1 (0.0) | 0 (0.0) | 602 (28.0) | 9 (39.1) | |||
| BMI (kg/m2) | |||||||||
| <23.0 | 2692 (54.1) | 41 (56.9) | 0.89 | 1771 (63.8) | 32 (66.7) | 0.50 | 897 (41.6) | 9 (39.1) | 0.30 |
| 23.0–<25.0 | 1170 (23.5) | 16 (22.2) | 547 (19.7) | 11 (22.9) | 614 (28.5) | 4 (17.4) | |||
| ≥25.0 | 1112 (22.4) | 15 (20.8) | 459 (16.5) | 5 (10.4) | 643 (29.9) | 10 (43.5) | |||
| Body fat (%) | 29.21 ± 5.35 | 29.03 ± 5.73 | 0.78 | 27.88 ± 5.17 | 27.91 ± 5.52 | 0.99 | 30.88 ± 5.09 | 31.36 ± 5.67 | 0.66 |
| Education level | |||||||||
| lementary school or less | 529 (10.6) | 3 (4.2) | 0.01 | 79 (2.8) | 0 (0.0) | 0.42 | 449 (20.8) | 3 (13.0) | 0.04 |
| Middle school | 443 (8.9) | 5 (6.9) | 158 (5.7) | 3 (6.3) | 282 (13.1) | 2 (8.7) | |||
| High school | 1957 (39.3) | 21 (29.2) | 1146 (41.3) | 16 (33.3) | 794 (36.9) | 5 (21.7) | |||
| College or higher | 1962 (39.5) | 42 (58.3) | 1365 (49.2) | 29 (60.4) | 581 (27.0) | 13 (56.5) | |||
| Occupation | |||||||||
| Housewife | 3045 (61.2) | 40 (55.6) | 0.33 | 1584 (57.0) | 27 (56.3) | 0.56 | 1443 (67.0) | 13 (56.5) | 0.37 |
| Professional, office worker | 740 (14.9) | 16 (22.2) | 537 (19.3) | 12 (25.0) | 192 (8.9) | 4 (17.4) | |||
| Sales, service | 592 (11.9) | 7 (9.7) | 381 (13.7) | 4 (8.3) | 208 (9.7) | 3 (13.0) | |||
| Agriculture, labor, unemployed, other | 463 (9.3) | 8 (11.1) | 223 (8.0) | 5 (10.4) | 236 (11.0) | 3 (13.0) | |||
| Household income (10,000 won/month) | |||||||||
| <200 | 768 (15.4) | 6 (8.3) | 0.06 | 270 (9.7) | 3 (6.3) | 0.10 | 494 (22.9) | 3 (13.0) | 0.42 |
| 200–<400 | 1386 (27.9) | 16 (22.2) | 807 (29.1) | 8 (16.7) | 569 (26.4) | 8 (34.8) | |||
| ≥400 | 2226 (44.8) | 41 (56.9) | 1439 (51.8) | 31 (64.6) | 766 (35.6) | 10 (43.5) | |||
| Marital status | |||||||||
| Unmarried | 165 (3.3) | 3 (4.2) | 0.90 | 147 (5.3) | 2 (4.2) | 0.93 | 17 (0.8) | 1 (4.4) | 0.06 |
| Married | 4378 (88.0) | 62 (86.1) | 2499 (90.0) | 45 (93.8) | 1847 (85.8) | 17 (73.9) | |||
| Divorced/widowed | 384 (7.7) | 6 (8.3) | 112 (4.0) | 1 (2.1) | 267 (12.4) | 5 (21.7) | |||
| Family history of breast cancer (Yes) | 168 (3.4) | 4 (5.6) | 0.31 | 91 (3.3) | 2 (4.2) | 0.67 | 76 (3.5) | 2 (8.7) | 0.21 |
| Smoking status | |||||||||
| Current smokers | 267 (5.4) | 9 (12.5) | <0.001 | 196 (7.1) | 7 (14.6) | <0.001 | 68 (3.2) | 2 (8.7) | 0.21 |
| Ex-smokers | 117 (2.4) | 7 (9.7) | 70 (2.5) | 6 (12.5) | 45 (2.1) | 1 (4.4) | |||
| Non-smokers | 3847 (77.3) | 48 (66.7) | 2199 (79.2) | 28 (58.3) | 1617 (75.1) | 19 (82.6) | |||
| Total pack-years | 0.7 ± 3.5 | 1.4 ± 4.2 | 0.22 | 0.7 ± 3.3 | 2.1 ± 5.2 | 0.13 | 0.6 ± 3.8 | 0.2 ± 0.7 | 0.03 |
| Alcohol consumption | |||||||||
| Current drinkers | 2300 (46.2) | 36 (50.0) | 0.80 | 1524 (54.9) | 26 (54.2) | 0.98 | 757 (35.1) | 9 (39.1) | 0.62 |
| Ex-drinkers | 188 (3.8) | 2 (2.8) | 108 (3.9) | 2 (4.2) | 79 (3.7) | 0 (0.0) | |||
| Non-drinkers | 2224 (44.7) | 31 (43.1) | 1048 (37.7) | 19 (39.6) | 1157 (53.7) | 12 (52.2) | |||
| Total alcohol consumption (g/day) | 17 ± 64 | 18 ± 49 | 0.93 | 22 ± 66 | 20 ± 55 | 0.86 | 11 ± 60 | 14 ± 35 | 0.78 |
| Physical activity (Yes) | 2242 (45.1) | 35 (48.6) | 0.86 | 1210 (43.6) | 24 (50.0) | 0.52 | 1011 (46.9) | 11 (47.8) | >0.99 |
| Age at menarche (years) | |||||||||
| ≤13 | 981 (19.7) | 13 (18.1) | 0.88 | 749 (27.0) | 10 (20.8) | 0.66 | 228 (10.6) | 3 (13.0) | 0.67 |
| 14 | 963 (19.4) | 16 (22.2) | 631 (22.7) | 14 (29.2) | 325 (15.1) | 2 (8.7) | |||
| 15 | 1111 (22.3) | 14 (19.4) | 651 (23.4) | 11 (22.9) | 450 (20.9) | 3 (13.0) | |||
| ≥16 | 1587 (31.9) | 22 (30.6) | 625 (22.5) | 10 (20.8) | 955 (44.3) | 12 (52.2) | |||
| Parity | |||||||||
| 0 | 328 (6.6) | 7 (9.7) | 0.20 | 257 (9.3) | 5 (10.4) | 0.96 | 69 (3.2) | 2 (8.7) | 0.10 |
| 1 | 467 (9.4) | 7 (9.7) | 353 (12.7) | 6 (12.5) | 110 (5.1) | 1 (4.4) | |||
| 2 | 2587 (52.0) | 43 (59.7) | 1686 (60.7) | 30 (62.5) | 885 (41.1) | 13 (56.5) | |||
| ≥3 | 1592 (32.0) | 15 (20.8) | 481 (17.3) | 7 (14.6) | 1090 (50.6) | 7 (30.4) | |||
| Lactation (Yes) | 2903 (58.4) | 43 (59.7) | 0.84 | 1472 (53.0) | 27 (56.3) | >0.99 | 1412 (65.6) | 16 (69.6) | 0.25 |
| Oral contraceptive use (Yes) | 864 (17.4) | 12 (16.7) | 0.91 | 403 (14.5) | 7 (14.6) | >0.99 | 455 (21.1) | 5 (21.7) | >0.99 |
| Benign breast tumor history (Yes) | 186 (3.7) | 7 (9.7) | 0.02 | 113 (4.1) | 2 (4.2) | 0.67 | 71 (3.3) | 5 (21.7) | 0.001 |
| Menopausal status (Yes) b | 2154 (43.3) | 23 (31.9) | 0.07 | - | - | - | - | - | - |
| Postmenopausal hormone use (yes) c | - | - | - | - | - | - | 613 (28.5) | 9 (39.1) | 0.31 |
| Age at menopause (years) c | - | - | - | - | - | - | |||
| <46 | - | - | - | - | - | - | 380 (17.6) | 4 (17.4) | 0.53 |
| 46–<49 | - | - | - | - | - | - | 330 (15.3) | 2 (8.7) | |
| 49–<52 | - | - | - | - | - | - | 321 (14.9) | 6 (26.1) | |
| ≥52 | - | - | - | - | - | - | 488 (22.7) | 5 (21.7) | |
| Type of menopause c | - | - | - | - | - | - | |||
| Natural | - | - | - | - | - | - | 1485 (68.9) | 17 (73.9) | 0.84 |
| Surgical, other | - | - | - | - | - | - | 642 (29.8) | 6 (26.1) | |
| Food Group | Consumption Frequency a | All Women | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| All (n = 5046) | Case (n = 72) | Person Years | Age-Adjusted | Multivariate 1 b | Multivariate 2 c | |||||||
| N | % | n | % | HR | 95% CI | HR | 95% CI | HR | 95% CI | |||
| Cereals | Low | 1738 | 34.4 | 26 | 36.1 | 16,876 | 1.00 | 1.00 | 1.00 | |||
| High | 3308 | 65.6 | 46 | 63.9 | 30,837 | 0.96 | 0.59–1.55 | 0.86 | 0.52–1.40 | 0.95 | 0.58–1.57 | |
| Salted vegetables and seafood | Low | 2838 | 56.2 | 41 | 56.9 | 27,009 | 1.00 | 1.00 | 1.00 | |||
| High | 2208 | 43.8 | 31 | 43.1 | 20,704 | 0.98 | 0.62–1.57 | 0.99 | 0.62–1.58 | 0.98 | 0.61–1.58 | |
| Light-colored vegetables | Low | 2083 | 41.3 | 32 | 44.4 | 19,610 | 1.00 | 1.00 | 1.00 | |||
| High | 2963 | 58.7 | 40 | 55.6 | 28,103 | 0.88 | 0.55–1.40 | 0.86 | 0.54–1.37 | 0.87 | 0.54–1.38 | |
| Green-yellow vegetables | Low | 3101 | 61.5 | 38 | 52.8 | 29,564 | 1.00 | 1.00 | 1.00 | |||
| High | 1945 | 38.6 | 34 | 47.2 | 18,149 | 1.46 | 0.92–2.32 | 1.38 | 0.87–2.20 | 1.46 | 0.91–2.33 | |
| Seaweed | Low | 1746 | 34.6 | 25 | 34.7 | 16,777 | 1.00 | 1.00 | 1.00 | |||
| High | 3300 | 65.4 | 47 | 65.3 | 30,936 | 1.01 | 0.62–1.64 | 0.96 | 0.59–1.57 | 1.06 | 0.65–1.73 | |
| Fruit | Low | 2554 | 50.6 | 35 | 48.6 | 24,168 | 1.00 | 1.00 | 1.00 | |||
| High | 2492 | 49.4 | 37 | 51.4 | 23,545 | 1.09 | 0.69–1.73 | 1.05 | 0.65–1.70 | 1.22 | 0.76–1.97 | |
| Grilled meat | Low | 2908 | 57.6 | 31 | 43.1 | 27,398 | 1.00 | 1.00 | 1.00 | |||
| High | 2138 | 42.4 | 41 | 56.9 | 20,315 | 1.80 | 1.12–2.91 | 1.66 | 1.03–2.68 | 1.77 | 1.09–2.85 | |
| Healthy protein foods | Low | 2885 | 57.2 | 35 | 48.6 | 27,391 | 1.00 | 1.00 | 1.00 | |||
| High | 2161 | 42.8 | 37 | 51.4 | 20,322 | 1.42 | 0.89–2.25 | 1.25 | 0.78–2.00 | 1.46 | 0.91–2.34 | |
| Dairy foods | Low | 2864 | 56.8 | 36 | 50.0 | 27,142 | 1.00 | 1.00 | 1.00 | |||
| High | 2182 | 43.2 | 36 | 50.0 | 20,571 | 1.33 | 0.83–2.10 | 1.24 | 0.78–1.97 | 1.32 | 0.83–2.11 | |
| Bony fish | Low | 2293 | 45.4 | 31 | 43.1 | 21,766 | 1.00 | 1.00 | 1.00 | |||
| High | 2753 | 54.6 | 41 | 56.9 | 25,947 | 1.12 | 0.70–1.80 | 1.10 | 0.69–1.78 | 1.14 | 0.71–1.83 | |
| Fried foods | Low | 2599 | 51.5 | 34 | 47.2 | 24,588 | 1.00 | 1.00 | 1.00 | |||
| High | 2447 | 48.5 | 38 | 52.8 | 23,125 | 1.18 | 0.73–1.89 | 1.06 | 0.66–1.71 | 1.19 | 0.74–1.92 | |
| High-cholesterol foods | Low | 2153 | 42.7 | 22 | 30.6 | 20,527 | 1.00 | 1.00 | 1.00 | |||
| High | 2893 | 57.3 | 50 | 69.4 | 27,186 | 1.71 | 1.03–2.85 | 1.48 | 0.88–2.48 | 1.69 | 1.01–2.82 | |
| Animal fat-rich foods | Low | 3143 | 62.3 | 43 | 59.7 | 29,641 | 1.00 | 1.00 | 1.00 | |||
| High | 1903 | 37.7 | 29 | 40.3 | 18,072 | 1.09 | 0.68–1.77 | 1.03 | 0.63–1.67 | 1.05 | 0.64–1.71 | |
| Sweet foods | Low | 2180 | 43.2 | 32 | 44.4 | 20,395 | 1.00 | 1.00 | 1.00 | |||
| High | 2866 | 56.8 | 40 | 55.6 | 27,318 | 0.92 | 0.57–1.47 | 0.82 | 0.51–1.33 | 0.90 | 0.56–1.45 | |
| Fast-foods | Low | 3152 | 62.5 | 42 | 58.3 | 29,741 | 1.00 | 1.00 | 1.00 | |||
| High | 1894 | 37.5 | 30 | 41.7 | 17,972 | 1.17 | 0.71-1.94 | 1.03 | 0.62-1.70 | 1.16 | 0.70-1.90 | |
| Caffeinated drinks | Low | 2128 | 42.2 | 30 | 41.7 | 20,133 | 1.00 | 1.00 | 1.00 | |||
| High | 2918 | 57.8 | 42 | 58.3 | 27,580 | 1.01 | 0.63-1.62 | 0.88 | 0.55-1.42 | 0.90 | 0.55-1.46 | |
| Food Group | Consumption Frequency a | Premenopausal Women | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| All (n = 2825) | Case (n = 48) | Person Years | Age-Adjusted | Multivariate 1 b | Multivariate 2 c | |||||||
| N | % | n | % | HR | 95% CI | HR | 95% CI | HR | 95% CI | |||
| Cereals | Low | 929 | 32.9 | 15 | 31.3 | 9054 | 1.00 | 1.00 | 1.00 | |||
| High | 1896 | 67.1 | 33 | 68.8 | 17,666 | 1.15 | 0.63–2.13 | 1.19 | 0.64–2.20 | 1.15 | 0.61–2.17 | |
| Salted vegetables and seafood | Low | 1560 | 55.2 | 25 | 52.1 | 14,877 | 1.00 | 1.00 | 1.00 | |||
| High | 1265 | 44.8 | 23 | 47.9 | 11,843 | 1.17 | 0.66–2.06 | 1.21 | 0.68–2.13 | 1.17 | 0.65–2.09 | |
| Light-colored vegetables | Low | 1168 | 41.4 | 25 | 52.1 | 10,971 | 1.00 | 1.00 | 1.00 | |||
| High | 1657 | 58.7 | 23 | 47.9 | 15,749 | 0.63 | 0.36–1.10 | 0.64 | 0.36–1.12 | 0.61 | 0.35–1.09 | |
| Green-yellow vegetables | Low | 1792 | 63.4 | 27 | 56.3 | 17,071 | 1.00 | 1.00 | 1.00 | |||
| High | 1033 | 36.6 | 21 | 43.8 | 9649 | 1.36 | 0.77–2.41 | 1.38 | 0.78–2.44 | 1.33 | 0.75–2.36 | |
| Seaweed | Low | 940 | 33.3 | 19 | 39.6 | 9054 | 1.00 | 1.00 | 1.00 | |||
| High | 1885 | 66.7 | 29 | 60.4 | 17,666 | 0.78 | 0.44–1.40 | 0.81 | 0.45–1.44 | 0.76 | 0.42–1.38 | |
| Fruit | Low | 1497 | 53.0 | 24 | 50.0 | 14,108 | 1.00 | 1.00 | 1.00 | |||
| High | 1328 | 47.0 | 24 | 50.0 | 12,612 | 1.10 | 0.62–1.94 | 1.25 | 0.71–2.22 | 1.23 | 0.69–2.20 | |
| Grilled meat | Low | 1413 | 50.0 | 21 | 43.8 | 13,287 | 1.00 | 1.00 | 1.00 | |||
| High | 1412 | 50.0 | 27 | 56.3 | 13,433 | 1.36 | 0.77–2.42 | 1.33 | 0.75–2.36 | 1.36 | 0.77–2.43 | |
| Healthy protein foods | Low | 1582 | 56.0 | 26 | 54.2 | 15,028 | 1.00 | 1.00 | 1.00 | |||
| High | 1243 | 44.0 | 22 | 45.8 | 11,692 | 1.08 | 0.61–1.91 | 1.12 | 0.63–1.97 | 1.12 | 0.63–2.00 | |
| Dairy food | Low | 1666 | 59.0 | 26 | 54.2 | 15,786 | 1.00 | 1.00 | 1.00 | |||
| High | 1159 | 41.0 | 22 | 45.8 | 10,934 | 1.21 | 0.69–2.14 | 1.22 | 0.69–2.16 | 1.20 | 0.67–2.13 | |
| Bony fish | Low | 1391 | 49.2 | 24 | 50.0 | 13,246 | 1.00 | 1.00 | 1.00 | |||
| High | 1434 | 50.8 | 24 | 50.0 | 13,474 | 0.92 | 0.52–1.63 | 0.96 | 0.54–1.70 | 0.95 | 0.53–1.69 | |
| Fried foods | Low | 1222 | 43.3 | 22 | 45.8 | 11,554 | 1.00 | 1.00 | 1.00 | |||
| High | 1603 | 56.7 | 26 | 54.2 | 15,166 | 0.97 | 0.55–1.73 | 1.00 | 0.56–1.78 | 1.00 | 0.56–1.79 | |
| High-cholesterol foods | Low | 1014 | 35.9 | 14 | 29.2 | 9707 | 1.00 | 1.00 | 1.00 | |||
| High | 1811 | 64.1 | 34 | 70.8 | 17,013 | 1.45 | 0.78–2.70 | 1.46 | 0.78–2.73 | 1.42 | 0.75–2.67 | |
| Animal fat-rich foods | Low | 1519 | 53.8 | 27 | 56.3 | 14,284 | 1.00 | 1.00 | 1.00 | |||
| High | 1306 | 46.2 | 21 | 43.8 | 12,436 | 0.94 | 0.53–1.67 | 0.93 | 0.52–1.64 | 0.93 | 0.52–1.67 | |
| Sweet foods | Low | 1036 | 36.7 | 18 | 37.5 | 9633 | 1.00 | 1.00 | 1.00 | |||
| High | 1789 | 63.3 | 30 | 62.5 | 17,087 | 1.01 | 0.56–1.82 | 1.07 | 0.59–1.94 | 1.02 | 0.56–1.86 | |
| Fast-foods | Low | 1422 | 50.3 | 25 | 52.1 | 13,376 | 1.00 | 1.00 | 1.00 | |||
| High | 1403 | 49.7 | 23 | 47.9 | 13,344 | 1.03 | 0.58–1.85 | 1.07 | 0.60–1.92 | 1.05 | 0.58–1.89 | |
| Caffeinated drinks | Low | 995 | 35.2 | 16 | 33.3 | 9373 | 1.00 | 1.00 | 1.00 | |||
| High | 1830 | 64.8 | 32 | 66.7 | 17,347 | 1.08 | 0.59–1.97 | 1.06 | 0.58–1.93 | 1.07 | 0.58–1.96 | |
| Food Group | Consumption Frequency a | Postmenopausal Women | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| All (n = 2177) | Case (n = 23) | Person Years | Age-Adjusted | Multivariate 1 b | Multivariate 2 c | |||||||
| N | % | n | % | HR | 95% CI | HR | 95% CI | HR | 95% CI | |||
| Cereals | Low | 786 | 36.1 | 11 | 47.8 | 7593 | 1.00 | 1.00 | 1.00 | |||
| High | 1391 | 63.9 | 12 | 52.2 | 12,986 | 0.62 | 0.28–1.41 | 0.54 | 0.24–1.23 | 0.53 | 0.22–1.25 | |
| Salted vegetables and seafood | Low | 1254 | 57.6 | 16 | 69.6 | 11,894 | 1.00 | 1.00 | 1.00 | |||
| High | 923 | 42.4 | 7 | 30.4 | 8685 | 0.59 | 0.24–1.44 | 0.59 | 0.24–1.42 | 0.45 | 0.18–1.14 | |
| Light-colored vegetables | Low | 894 | 41.1 | 7 | 30.4 | 8437 | 1.00 | 1.00 | 1.00 | |||
| High | 1283 | 58.9 | 16 | 69.6 | 12,142 | 1.59 | 0.65–3.86 | 1.38 | 0.56–3.36 | 1.37 | 0.55–3.39 | |
| Green-yellow vegetables | Low | 1280 | 58.8 | 11 | 47.8 | 12,215 | 1.00 | 1.00 | 1.00 | |||
| High | 897 | 41.2 | 12 | 52.2 | 8364 | 1.58 | 0.70–3.57 | 1.34 | 0.59–3.07 | 1.42 | 0.62–3.30 | |
| Seaweed | Low | 790 | 36.3 | 6 | 26.1 | 7566 | 1.00 | 1.00 | 1.00 | |||
| High | 1387 | 63.7 | 17 | 73.9 | 13,013 | 1.63 | 0.64–4.15 | 1.40 | 0.55–3.59 | 1.73 | 0.67–4.50 | |
| Fruit | Low | 1035 | 47.5 | 10 | 43.5 | 9859 | 1.00 | 1.00 | 1.00 | |||
| High | 1142 | 52.5 | 13 | 56.5 | 10,720 | 1.18 | 0.52–2.70 | 0.86 | 0.36–2.03 | 1.22 | 0.51–2.92 | |
| Grilled meat | Low | 1475 | 67.8 | 10 | 43.5 | 13,912 | 1.00 | 1.00 | 1.00 | |||
| High | 702 | 32.3 | 13 | 56.5 | 6667 | 2.80 | 1.22–6.41 | 2.41 | 1.05–5.54 | 3.06 | 1.31–7.15 | |
| Healthy protein foods | Low | 1275 | 58.6 | 9 | 39.1 | 12,093 | 1.00 | 1.00 | 1.00 | |||
| High | 902 | 41.4 | 14 | 60.9 | 8486 | 2.23 | 0.96–5.15 | 1.77 | 0.74–4.20 | 2.28 | 0.94–5.52 | |
| Dairy foods | Low | 1175 | 54.0 | 10 | 43.5 | 11,130 | 1.00 | 1.00 | 1.00 | |||
| High | 1002 | 46.0 | 13 | 56.5 | 9449 | 1.53 | 0.67–3.49 | 1.31 | 0.57–3.01 | 1.56 | 0.67–3.65 | |
| Bony fish | Low | 882 | 40.5 | 7 | 30.4 | 8324 | 1.00 | 1.00 | 1.00 | |||
| High | 1295 | 59.5 | 16 | 69.6 | 12,255 | 1.53 | 0.63–3.72 | 1.34 | 0.54–3.29 | 1.38 | 0.55–3.46 | |
| Fried foods | Low | 1351 | 62.1 | 11 | 47.8 | 12,790 | 1.00 | 1.00 | 1.00 | |||
| High | 826 | 37.9 | 12 | 52.2 | 7789 | 1.84 | 0.81–4.17 | 1.47 | 0.64–3.38 | 1.78 | 0.75–4.21 | |
| High-cholesterol foods | Low | 1124 | 51.6 | 8 | 34.8 | 10,677 | 1.00 | 1.00 | 1.00 | |||
| High | 1053 | 48.4 | 15 | 65.2 | 9902 | 2.06 | 0.87–4.88 | 1.59 | 0.66–3.82 | 1.97 | 0.81–4.80 | |
| Animal fat-rich foods | Low | 1595 | 73.3 | 16 | 69.6 | 15,080 | 1.00 | 1.00 | 1.00 | |||
| High | 582 | 26.7 | 7 | 30.4 | 5499 | 1.25 | 0.51–3.07 | 1.11 | 0.45–2.70 | 1.18 | 0.47–2.99 | |
| Sweet foods | Low | 1121 | 51.5 | 13 | 56.5 | 10,552 | 1.00 | 1.00 | 1.00 | |||
| High | 1056 | 48.5 | 10 | 43.5 | 10,027 | 0.83 | 0.36–1.90 | 0.69 | 0.30–1.60 | 0.66 | 0.27–1.57 | |
| Fast-foods | Low | 1699 | 78.0 | 16 | 69.6 | 16,078 | 1.00 | 1.00 | 1.00 | |||
| High | 478 | 22.0 | 7 | 30.4 | 4501 | 1.68 | 0.68–4.14 | 1.29 | 0.52–3.20 | 1.47 | 0.58–3.71 | |
| Caffeinated drinks | Low | 1118 | 51.4 | 14 | 60.9 | 10,617 | 1.00 | 1.00 | 1.00 | |||
| High | 1059 | 48.6 | 9 | 39.1 | 9962 | 0.70 | 0.30–1.64 | 0.61 | 0.26–1.42 | 0.56 | 0.23–1.35 | |
| Dietary Habit | Frequency | All Women | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| All (n = 5046) | Case (n = 72) | Person Years | Age-Adjusted | Multivariate 1 b | Multivariate 2 c | |||||||
| N | % | n | % | HR | 95% CI | HR | 95% CI | HR | 95% CI | |||
| Meal frequency | 3 times/day | 3285 | 65.1 | 37 | 51.4 | 31,174 | 1.00 | 1.00 | 1.00 | |||
| 2 times/day | 1110 | 22.0 | 18 | 25.0 | 10,327 | 1.49 | 0.84–2.63 | 1.37 | 0.77–2.44 | 1.36 | 0.76–2.42 | |
| Irregular a | 616 | 12.2 | 17 | 23.6 | 5896 | 2.47 | 1.38–4.41 | 2.37 | 1.31–4.27 | 2.19 | 1.20–3.98 | |
| p for trend | 0.003 | 0.006 | 0.01 | |||||||||
| Breakfast frequency | Always | 2792 | 55.3 | 31 | 43.1 | 26,361 | 1.00 | 1.00 | 1.00 | |||
| Often | 1579 | 31.3 | 29 | 40.3 | 14,992 | 1.67 | 1.00–2.80 | 1.55 | 0.92–2.60 | 1.56 | 0.93–2.63 | |
| Not at all | 657 | 13.0 | 12 | 16.7 | 6193 | 1.68 | 0.85–3.33 | 1.41 | 0.71–2.84 | 1.43 | 0.71–2.90 | |
| p for trend | 0.06 | 0.18 | 0.17 | |||||||||
| Meal time regularity | Regular | 1969 | 39.0 | 36 | 50.0 | 18,474 | 1.00 | 1.00 | 1.00 | |||
| Often | 2549 | 50.5 | 25 | 34.7 | 24,404 | 0.52 | 0.31–0.87 | 0.53 | 0.32–0.90 | 0.52 | 0.31–0.88 | |
| Irregular | 510 | 10.1 | 11 | 15.3 | 4661 | 1.18 | 0.59–2.34 | 1.24 | 0.62–2.51 | 1.02 | 0.50–2.06 | |
| p for trend | 0.40 | 0.48 | 0.29 | |||||||||
| Meal speed | Slow | 557 | 11.0 | 7 | 9.7 | 5240 | 1.00 | 1.00 | 1.00 | |||
| Average | 2634 | 52.2 | 40 | 55.6 | 24,817 | 1.22 | 0.55–2.72 | 1.41 | 0.63–3.16 | 1.35 | 0.60–3.04 | |
| Fast | 1850 | 36.7 | 25 | 34.7 | 17,611 | 1.07 | 0.47–2.49 | 1.27 | 0.55–2.95 | 1.17 | 0.50–2.74 | |
| p for trend | 0.91 | 0.81 | 0.99 | |||||||||
| Overeating | Less than once a week | 1686 | 33.4 | 19 | 26.4 | 15,817 | 1.00 | 1.00 | 1.00 | |||
| 2–3 times a week | 2864 | 56.8 | 43 | 59.7 | 27,211 | 1.26 | 0.74–2.14 | 1.22 | 0.72–2.08 | 1.24 | 0.72–2.12 | |
| More than 4 times a week | 479 | 9.5 | 9 | 12.5 | 4525 | 1.58 | 0.72–3.48 | 1.57 | 0.71–3.48 | 1.46 | 0.64–3.31 | |
| p for trend | 0.20 | 0.22 | 0.26 | |||||||||
| Added spices | Often | 598 | 11.9 | 10 | 13.9 | 5701 | 1.00 | 1.00 | 1.00 | |||
| Sometimes | 2684 | 53.2 | 47 | 65.3 | 25,530 | 1.08 | 0.54–2.13 | 1.04 | 0.52–2.06 | 1.06 | 0.53–2.12 | |
| Never | 1745 | 34.6 | 15 | 20.8 | 16,305 | 0.53 | 0.24–1.19 | 0.50 | 0.22–1.11 | 0.54 | 0.24–1.20 | |
| p for trend | 0.04 | 0.03 | 0.045 | |||||||||
| Dietary Habit | Frequency | Premenopausal Women | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| All (n = 2825) | Case (n = 48) | Person Years | Age-Adjusted | Multivariate 1 b | Multivariate 2 c | |||||||
| N | % | n | % | HR | 95% CI | HR | 95% CI | HR | 95% CI | |||
| Meal frequency | 3 times/day | 1705 | 60.4 | 23 | 47.9 | 16,191 | 1.00 | 1.00 | 1.00 | |||
| 2 times/day | 702 | 24.9 | 13 | 27.1 | 6527 | 1.50 | 0.76–2.96 | 1.31 | 0.66–2.61 | 1.34 | 0.67–2.68 | |
| Irregular a | 400 | 14.2 | 12 | 25.0 | 3838 | 2.34 | 1.16–4.71 | 2.15 | 1.06–4.40 | 2.35 | 1.13–4.91 | |
| p for trend | 0.02 | 0.044 | 0.03 | |||||||||
| Breakfast frequency | Always | 1340 | 47.4 | 20 | 41.7 | 12,623 | 1.00 | 1.00 | 1.00 | |||
| Often | 1011 | 35.8 | 18 | 37.5 | 9604 | 1.25 | 0.66–2.36 | 1.16 | 0.61–2.20 | 1.17 | 0.62–2.24 | |
| Not at all | 466 | 16.5 | 10 | 20.8 | 4414 | 1.57 | 0.73–3.38 | 1.33 | 0.61–2.92 | 1.37 | 0.62–3.05 | |
| p for trend | 0.24 | 0.47 | 0.45 | |||||||||
| Meal time regularity | Regular | 981 | 34.7 | 23 | 47.9 | 9162 | 1.00 | 1.00 | 1.00 | |||
| Often | 1487 | 52.6 | 18 | 37.5 | 14,284 | 0.53 | 0.28–0.98 | 0.51 | 0.27–0.94 | 0.52 | 0.28–0.98 | |
| Irregular | 348 | 12.3 | 7 | 14.6 | 3187 | 0.93 | 0.40–2.17 | 0.76 | 0.32–1.79 | 0.76 | 0.31–1.83 | |
| p for trend | 0.30 | 0.17 | 0.19 | |||||||||
| Meal speed | Slow | 317 | 11.2 | 2 | 4.2 | 3025 | 1.00 | 1.00 | 1.00 | |||
| Average | 1501 | 53.1 | 29 | 60.4 | 14,138 | 3.03 | 0.72–12.71 | 3.28 | 0.78–13.77 | 3.28 | 0.78–13.84 | |
| Fast | 1005 | 35.6 | 17 | 35.4 | 9536 | 2.62 | 0.61–11.35 | 2.75 | 0.63–11.93 | 2.94 | 0.67–12.86 | |
| p for trend | 0.49 | 0.49 | 0.38 | |||||||||
| Overeating | Less than once a week | 884 | 31.3 | 13 | 27.1 | 8257 | 1.00 | 1.00 | 1.00 | |||
| 2–3 times a week | 1627 | 57.6 | 28 | 58.3 | 15,466 | 1.18 | 0.61–2.27 | 1.12 | 0.58–2.17 | 1.18 | 0.61–2.30 | |
| More than 4 times a week | 304 | 10.8 | 7 | 14.6 | 2895 | 1.61 | 0.64–4.04 | 1.37 | 0.54–3.47 | 1.60 | 0.62–4.15 | |
| p for trend | 0.35 | 0.54 | 0.37 | |||||||||
| Added spices | Often | 304 | 10.8 | 8 | 16.7 | 2854 | 1.00 | 1.00 | 1.00 | |||
| Sometimes | 1479 | 52.4 | 29 | 60.4 | 14,101 | 0.75 | 0.34–1.63 | 0.82 | 0.37–1.80 | 0.78 | 0.35–1.74 | |
| Never | 1037 | 36.7 | 11 | 22.9 | 9719 | 0.41 | 0.16–1.01 | 0.46 | 0.19–1.16 | 0.43 | 0.17–1.08 | |
| p for trend | 0.03 | 0.06 | 0.045 | |||||||||
| Dietary Habit | Frequency | Postmenopausal Women | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| All (n = 2177) | Case (n = 23) | Person Years | Age-Adjusted | Multivariate 1 b | Multivariate 2 c | |||||||
| N | % | n | % | HR | 95% CI | HR | 95% CI | HR | 95% CI | |||
| Meal frequency | 3 times/day | 1558 | 71.6 | 14 | 60.9 | 14,767 | 1.00 | 1.00 | 1.00 | |||
| 2 times/day | 394 | 18.1 | 5 | 21.7 | 3668 | 1.51 | 0.54–4.24 | 1.71 | 0.60–4.81 | 1.65 | 0.57–4.76 | |
| Irregular a | 208 | 9.6 | 4 | 17.4 | 1992 | 2.22 | 0.73–6.78 | 1.95 | 0.64–5.98 | 1.73 | 0.53–5.70 | |
| p for trend | 0.15 | 0.18 | 0.28 | |||||||||
| Breakfast frequency | Always | 1428 | 65.6 | 10 | 43.5 | 13,511 | 1.00 | 1.00 | 1.00 | |||
| Often | 554 | 25.5 | 11 | 47.8 | 5257 | 3.05 | 1.28–7.25 | 2.86 | 1.20–6.79 | 2.98 | 1.21–7.33 | |
| Not at all | 186 | 8.5 | 2 | 8.7 | 1732 | 1.75 | 0.38–8.14 | 1.58 | 0.34–7.35 | 1.83 | 0.36–9.21 | |
| p for trend | 0.07 | 0.10 | 0.07 | |||||||||
| Meal time regularity | Regular | 967 | 44.4 | 12 | 52.2 | 9118 | 1.00 | 1.00 | 1.00 | |||
| Often | 1043 | 47.9 | 7 | 30.4 | 9932 | 0.56 | 0.22–1.44 | 0.62 | 0.24–1.60 | 0.60 | 0.23–1.58 | |
| Irregular | 158 | 7.3 | 4 | 17.4 | 1442 | 2.20 | 0.70–6.94 | 3.10 | 0.96–9.99 | 2.28 | 0.64–8.10 | |
| p for trend | 0.76 | 0.49 | 0.70 | |||||||||
| Meal speed | Slow | 238 | 10.9 | 5 | 21.7 | 2195 | 1.00 | 1.00 | 1.00 | |||
| Average | 1116 | 51.3 | 10 | 43.5 | 10,533 | 0.43 | 0.15–1.24 | 0.52 | 0.18–1.54 | 0.46 | 0.15–1.42 | |
| Fast | 820 | 37.7 | 8 | 34.8 | 7827 | 0.46 | 0.15–1.41 | 0.56 | 0.18–1.72 | 0.45 | 0.13–1.54 | |
| p for trend | 0.30 | 0.42 | 0.30 | |||||||||
| Overeating | Less than once a week | 793 | 36.4 | 6 | 26.1 | 7477 | 1.00 | 1.00 | 1.00 | |||
| 2–3 times a week | 1203 | 55.3 | 14 | 60.9 | 11,426 | 1.38 | 0.55–3.46 | 1.34 | 0.54–3.37 | 1.23 | 0.47–3.24 | |
| More than 4 times a week | 174 | 8.0 | 2 | 8.7 | 1618 | 1.40 | 0.29–6.83 | 1.47 | 0.30–7.14 | 1.11 | 0.21–5.92 | |
| p for trend | 0.38 | 0.36 | 0.52 | |||||||||
| Added spices | Often | 289 | 13.3 | 2 | 8.7 | 2797 | 1.00 | 1.00 | 1.00 | |||
| Sometimes | 1182 | 54.3 | 17 | 73.9 | 11,214 | 2.20 | 0.51–9.52 | 1.93 | 0.44–8.49 | 2.47 | 0.54–11.28 | |
| Never | 692 | 31.8 | 4 | 17.4 | 6437 | 0.91 | 0.17–4.95 | 0.79 | 0.14–4.40 | 1.14 | 0.20–6.60 | |
| p for trend | 0.50 | 0.41 | 0.73 | |||||||||
© 2017 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Kim, J.H.; Lee, J.; Jung, S.-Y.; Kim, J. Dietary Factors and Female Breast Cancer Risk: A Prospective Cohort Study. Nutrients 2017, 9, 1331. https://doi.org/10.3390/nu9121331
Kim JH, Lee J, Jung S-Y, Kim J. Dietary Factors and Female Breast Cancer Risk: A Prospective Cohort Study. Nutrients. 2017; 9(12):1331. https://doi.org/10.3390/nu9121331
Chicago/Turabian StyleKim, Ji Hyun, Jeonghee Lee, So-Youn Jung, and Jeongseon Kim. 2017. "Dietary Factors and Female Breast Cancer Risk: A Prospective Cohort Study" Nutrients 9, no. 12: 1331. https://doi.org/10.3390/nu9121331
APA StyleKim, J. H., Lee, J., Jung, S.-Y., & Kim, J. (2017). Dietary Factors and Female Breast Cancer Risk: A Prospective Cohort Study. Nutrients, 9(12), 1331. https://doi.org/10.3390/nu9121331





