Dietary Magnesium and Incident Frailty in Older People at Risk for Knee Osteoarthritis: An Eight-Year Longitudinal Study
Abstract
1. Introduction
2. Materials and Methods
2.1. Data Source and Subjects
2.2. Baseline Dietary Magnesium Intake (Exposure)
2.3. Incident Frailty (Outcome)
2.4. Covariates
2.5. Statistical Analyses
3. Results
3.1. Sample Selection
3.2. Descriptive Characteristics
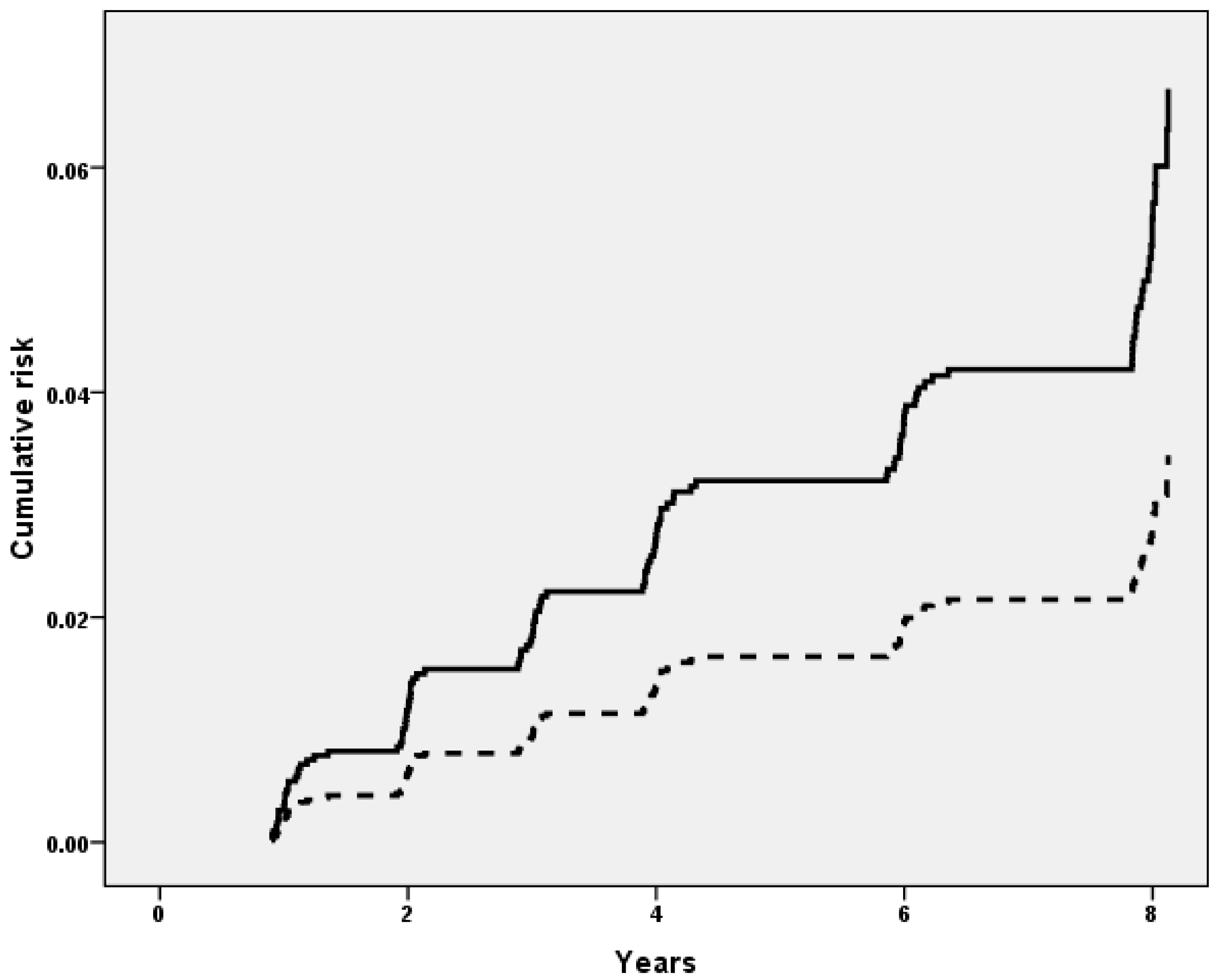
3.3. Dietary Magnesium Intake and Incident Frailty
4. Discussion
5. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Morley, J.E. Frailty and sarcopenia: The new geriatric giants. Revista de Investigacion Clinica Organo del Hospital de Enfermedades de la Nutricion 2016, 68, 59–67. [Google Scholar] [PubMed]
- Collard, R.M.; Boter, H.; Schoevers, R.A.; Oude Voshaar, R.C. Prevalence of frailty in community-dwelling older persons: A systematic review. J. Am. Geriatr. Soc. 2012, 60, 1487–1492. [Google Scholar] [CrossRef] [PubMed]
- Kojima, G. Prevalence of frailty in nursing homes: A systematic review and meta-analysis. J. Am. Med. Dir. Assoc. 2015, 16, 940–945. [Google Scholar] [CrossRef] [PubMed]
- Clegg, A.; Young, J.; Iliffe, S.; Rikkert, M.O.; Rockwood, K. Frailty in elderly people. Lancet (Lond. Engl.) 2013, 381, 752–762. [Google Scholar] [CrossRef]
- Veronese, N.; Stubbs, B.; Fontana, L.; Trevisan, C.; Bolzetta, F.; De Rui, M.; Sartori, L.; Musacchio, E.; Zambon, S.; Maggi, S.; et al. Frailty is associated with an increased risk of incident type 2 diabetes in the elderly. J. Am. Med. Dir. Assoc. 2016. [Google Scholar] [CrossRef] [PubMed]
- Soysal, P.; Veronese, N.; Thompson, T.; Kahl, K.G.; Fernandes, B.S.; Prina, A.M.; Solmi, M.; Schofield, P.; Koyanagi, A.; Tseng, P.T.; et al. Relationship between depression and frailty in older adults: A systematic review and meta-analysis. Ageing Res. Rev. 2017, 36, 78–87. [Google Scholar] [CrossRef] [PubMed]
- Veronese, N.; Cereda, E.; Stubbs, B.; Solmi, M.; Luchini, C.; Manzato, E.; Sergi, G.; Manu, P.; Harris, T.; Fontana, L.; et al. Risk of cardiovascular disease morbidity and mortality in frail and pre-frail older adults: Results from a meta-analysis and exploratory meta-regression analysis. Ageing Res. Rev. 2017. [Google Scholar] [CrossRef] [PubMed]
- Morley, J.E.; Vellas, B.; van Kan, G.A.; Anker, S.D.; Bauer, J.M.; Bernabei, R.; Cesari, M.; Chumlea, W.C.; Doehner, W.; Evans, J.; et al. Frailty consensus: A call to action. J. Am. Med. Dir. Assoc. 2013, 14, 392–397. [Google Scholar] [CrossRef] [PubMed]
- Artaza-Artabe, I.; Saez-Lopez, P.; Sanchez-Hernandez, N.; Fernandez-Gutierrez, N.; Malafarina, V. The relationship between nutrition and frailty: Effects of protein intake, nutritional supplementation, vitamin d and exercise on muscle metabolism in the elderly. A systematic review. Maturitas 2016, 93, 89–99. [Google Scholar] [CrossRef] [PubMed]
- Bartali, B.; Frongillo, E.A.; Bandinelli, S.; Lauretani, F.; Semba, R.D.; Fried, L.P.; Ferrucci, L. Low nutrient intake is an essential component of frailty in older persons. J. Gerontol. Ser. A Biol. Sci. Med. Sci. 2006, 61, 589–593. [Google Scholar] [CrossRef]
- Arnaud, M.J. Update on the assessment of magnesium status. Br. J. Nutr. 2008, 99 (Suppl. 3), S24–S36. [Google Scholar] [CrossRef]
- Dominguez, L.J.; Barbagallo, M.; Lauretani, F.; Bandinelli, S.; Bos, A.; Corsi, A.M.; Simonsick, E.M.; Ferrucci, L. Magnesium and muscle performance in older persons: The inchianti study. Am. J. Clin. Nutr. 2006, 84, 419–426. [Google Scholar] [PubMed]
- Welch, A.A.; Kelaiditi, E.; Jennings, A.; Steves, C.J.; Spector, T.D.; MacGregor, A. Dietary magnesium is positively associated with skeletal muscle power and indices of muscle mass and may attenuate the association between circulating c-reactive protein and muscle mass in women. J. Bone Miner. Res. 2016, 31, 317–325. [Google Scholar] [CrossRef] [PubMed]
- Hasebe, N. Oxidative stress and magnesium. Clin. Calcium 2005, 15, 194–202. [Google Scholar] [PubMed]
- Barbagallo, M. Role of magnesium in insulin action, diabetes and cardio-metabolic syndrome x. Mol. Asp. Med. 2003, 24, 39–52. [Google Scholar] [CrossRef]
- Veronese, N.; Watutantrige-Fernando, S.; Luchini, C.; Solmi, M.; Sartore, G.; Sergi, G.; Manzato, E.; Barbagallo, M.; Maggi, S.; Stubbs, B. Effect of magnesium supplementation on glucose metabolism in people with or at risk of diabetes: A systematic review and meta-analysis of double-blind randomized controlled trials. Eur. J. Clin. Nutr. 2016, 70, 1463. [Google Scholar] [CrossRef] [PubMed]
- Veronese, N.; Berton, L.; Carraro, S.; Bolzetta, F.; De Rui, M.; Perissinotto, E.; Toffanello, E.D.; Bano, G.; Pizzato, S.; Miotto, F.; et al. Effect of oral magnesium supplementation on physical performance in healthy elderly women involved in a weekly exercise program: A randomized controlled trial. Am. J. Clin. Nutr. 2014, 100, 974–981. [Google Scholar] [CrossRef] [PubMed]
- Peterfy, C.G.; Schneider, E.; Nevitt, M. The osteoarthritis initiative: Report on the design rationale for the magnetic resonance imaging protocol for the knee. Osteoarthr. Cartil. 2008, 16, 1433–1441. [Google Scholar] [CrossRef] [PubMed]
- Veronese, N.; Stubbs, B.; Solmi, M.; Noale, M.; Vaona, A.; Demurtas, J.; Maggi, S. Dietary magnesium intake and fracture risk: Data from a large prospective study. Br. J. Nutr. 2017, 117, 1570–1576. [Google Scholar] [CrossRef] [PubMed]
- Institute of Medicine; Food and Nutrition Board; Standing Committee on the Scientific Evaluation of Dietary Reference Intakes. Dietary Reference Intakes for Calcium, Phosphorus, Magnesium, Vitamin D, and Fluoride; The National Academies Press: Washington, DC, USA, 1997; p. 432. [Google Scholar]
- Ensrud, K.E.; Ewing, S.K.; Taylor, B.C.; Fink, H.A.; Stone, K.L.; Cauley, J.A.; Tracy, J.K.; Hochberg, M.C.; Rodondi, N.; Cawthon, P.M.; et al. Frailty and risk of falls, fracture, and mortality in older women: The study of osteoporotic fractures. J. Gerontol. Ser. A Biol. Sci. Med. Sci. 2007, 62, 744–751. [Google Scholar] [CrossRef]
- Misra, D.; Felson, D.T.; Silliman, R.A.; Nevitt, M.; Lewis, C.E.; Torner, J.; Neogi, T. Knee osteoarthritis and frailty: Findings from the multicenter osteoarthritis study and osteoarthritis initiative. J. Gerontol. Ser. A Biol. Sci. Med. Sci. 2015, 70, 339–344. [Google Scholar] [CrossRef] [PubMed]
- Veronese, N.; Stubbs, B.; Noale, M.; Solmi, M.; Pilotto, A.; Vaona, A.; Demurtas, J.; Mueller, C.; Huntley, J.; Crepaldi, G.; et al. Polypharmacy is associated with higher frailty risk in older people: An 8-year longitudinal cohort study. J. Am. Med. Dir. Assoc. 2017. [Google Scholar] [CrossRef] [PubMed]
- Veronese, N.; Stubbs, B.; Noale, M.; Solmi, M.; Rizzoli, R.; Vaona, A.; Demurtas, J.; Crepaldi, G.; Maggi, S. Adherence to a Mediterranean diet is associated with lower incidence of frailty: A longitudinal cohort study. Clin. Nutr. (Edinb. Scotl.) 2017. [Google Scholar] [CrossRef] [PubMed]
- Shivappa, N.; Stubbs, B.; Hebert, J.R.; Cesari, M.; Schofield, P.; Soysal, P.; Maggi, S.; Veronese, N. The relationship between the dietary inflammatory index and incident frailty: A longitudinal cohort study. J. Am. Med. Dir. Assoc. 2017. [Google Scholar] [CrossRef] [PubMed]
- Washburn, R.A.; McAuley, E.; Katula, J.; Mihalko, S.L.; Boileau, R.A. The physical activity scale for the elderly (pase): Evidence for validity. J. Clin. Epidemiol. 1999, 52, 643–651. [Google Scholar] [CrossRef]
- Radloff, L.S. The CES-D scale: A self-report depression scale for research in the general population. Appl. Psychol. Meas. 1977, 1, 385–401. [Google Scholar] [CrossRef]
- Katz, J.N.; Chang, L.C.; Sangha, O.; Fossel, A.H.; Bates, D.W. Can comorbidity be measured by questionnaire rather than medical record review? Med. Care 1996, 34, 73–84. [Google Scholar] [CrossRef] [PubMed]
- Grambsch, P.M.; Therneau, T.M. Proportional hazards tests and diagnostics based on weighted residuals. Biometrika 1994, 81, 515–526. [Google Scholar] [CrossRef]
- Bailey, R.L.; Fulgoni, V.L., III; Keast, D.R.; Dwyer, J.T. Dietary supplement use is associated with higher intakes of minerals from food sources. Am. J. Clin. Nutr. 2011, 94, 1376–1381. [Google Scholar] [CrossRef] [PubMed]
- Rosanoff, A.; Weaver, C.M.; Rude, R.K. Suboptimal magnesium status in the united states: Are the health consequences underestimated? Nutr. Rev. 2012, 70, 153–164. [Google Scholar] [CrossRef] [PubMed]
- Veronese, N.; Stubbs, B.; Noale, M.; Solmi, M.; Vaona, A.; Demurtas, J.; Nicetto, D.; Crepaldi, G.; Schofield, P.; Koyanagi, A.; et al. Fried potato consumption is associated with elevated mortality: An 8-year longitudinal cohort study. Am. J. Clin. Nutr. 2017. [Google Scholar] [CrossRef] [PubMed]
- Cruz-Jentoft, A.J.; Kiesswetter, E.; Drey, M.; Sieber, C.C. Nutrition, frailty, and sarcopenia. Aging Clin. Exp. Res. 2017, 29, 43–48. [Google Scholar] [CrossRef] [PubMed]
- Bohl, C.H.; Volpe, S.L. Magnesium and exercise. Crit. Rev. Food Sci. Nutr. 2002, 42, 533–563. [Google Scholar] [CrossRef] [PubMed]
- Hubbard, R.E. Sex differences in frailty. In Frailty in Aging; Karger Publishers: Basel, Switzerland, 2015; Voloume 41, pp. 41–53. [Google Scholar]
- Alexandre, T.D.S.; Corona, L.P.; Brito, T.R.P.; Santos, J.L.F.; Duarte, Y.A.O.; Lebrão, M.L. Gender differences in the incidence and determinants of components of the frailty phenotype among older adults. J. Aging Health 2016. [Google Scholar] [CrossRef] [PubMed]
- Walker, A.F.; Marakis, G.; Christie, S.; Byng, M. Mg citrate found more bioavailable than other Mg preparations in a randomised, double-blind study. Magnes. Res. 2003, 16, 183–191. [Google Scholar] [PubMed]
- Veronese, N.; Zanforlini, B.M.; Manzato, E.; Sergi, G. Magnesium and healthy aging. Magnes. Res. 2015, 28, 112–115. [Google Scholar] [PubMed]
- Swaminathan, R. Magnesium metabolism and its disorders. Clin. Biochem. Rev./Aust. Assoc. Clin. Biochem. 2003, 24, 47–66. [Google Scholar]
| Men | Women | |||||
|---|---|---|---|---|---|---|
| Greater Than/Equal to RDA (n = 233) | Less than RDA (n = 1624) | p-Value a | Greater Than/Equal to RDA (n = 586) | Less than RDA (n = 1978) | p-Value a | |
| General characteristics | ||||||
| Age (years) | 61.5 (9.0) | 60.9 (9.5) | 0.37 | 62.0 (8.8) | 61.4 (9.0) | 0.13 |
| Energy intake (kcal/day) | 2313 (701) | 1488 (523) | <0.0001 | 1760 (553) | 1143 (376) | <0.0001 |
| PASE (points) | 187 (96) | 174 (86) | 0.03 | 156 (80) | 149 (75) | 0.03 |
| White race (n, %) | 193 (82.8) | 1388 (85.6) | 0.28 | 456 (77.9) | 1516 (76.6) | 0.54 |
| Smoking (previous/current) (n, %) | 116 (50.2) | 805 (49.8) | 0.94 | 262 (44.9) | 894 (45.4) | 0.85 |
| Graduate degree (n, %) | 87 (37.3) | 596 (36.8) | 0.89 | 146 (24.9) | 517 (26.2) | 0.59 |
| Yearly income (>US$50,000) | 79 (33.9) | 478 (29.4) | 0.17 | 292 (50.2) | 953 (48.2) | 0.40 |
| Medical conditions | ||||||
| BMI (kg/m2) | 28.2 (4.2) | 28.9 (4.1) | 0.08 | 28.5 (5.1) | 28.6 (5.3) | 0.67 |
| CES-D (points) | 6.3 (6.7) | 5.9 (6.4) | 0.35 | 6.9 (6.9) | 7.0 (7.2) | 0.61 |
| Charlson co-morbidity index (points) | 0.5 (1.1) | 0.4 (0.9) | 0.22 | 0.4 (0.8) | 0.4 (0.8) | 0.94 |
| Frailty items | ||||||
| Poor physical performance (n, %) | 25 (10.8) | 146 (9.0) | 0.40 | 68 (11.6) | 251 (12.7) | 0.52 |
| Poor chair stand time (n, %) | 2 (0.9) | 10 (0.6) | 0.66 | 7 (1.2) | 13 (0.7) | 0.19 |
| Weight loss (n, %) | 3 (1.3) | 11 (0.7) | 0.40 | 23 (3.9) | 62 (3.1) | 0.36 |
| Incidence (95% CI) for 1000 Persons-Year | Basic Adjusted a HR (95% CI) | p Value | Fully Adjusted b HR (95% CI) | p Value | |
|---|---|---|---|---|---|
| Men | |||||
| Greater than the RDA | 10 (8–12) | 1 (reference) | 1 (reference) | ||
| Greater than/equal to the RDA | 6 (3–12) | 0.70 (0.38–0.95) | 0.03 | 0.51 (0.26–0.93) | 0.03 |
| Women | |||||
| Less than the RDA | 14 (12–16) | 1 (reference) | 1 (reference) | ||
| Greater than/equal to the RDA | 16 (12–20) | 1.13 (0.84–1.51) | 0.43 | 1.02 (0.71–1.46) | 0.92 |
© 2017 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Veronese, N.; Stubbs, B.; Maggi, S.; Notarnicola, M.; Barbagallo, M.; Firth, J.; Dominguez, L.J.; Caruso, M.G. Dietary Magnesium and Incident Frailty in Older People at Risk for Knee Osteoarthritis: An Eight-Year Longitudinal Study. Nutrients 2017, 9, 1253. https://doi.org/10.3390/nu9111253
Veronese N, Stubbs B, Maggi S, Notarnicola M, Barbagallo M, Firth J, Dominguez LJ, Caruso MG. Dietary Magnesium and Incident Frailty in Older People at Risk for Knee Osteoarthritis: An Eight-Year Longitudinal Study. Nutrients. 2017; 9(11):1253. https://doi.org/10.3390/nu9111253
Chicago/Turabian StyleVeronese, Nicola, Brendon Stubbs, Stefania Maggi, Maria Notarnicola, Mario Barbagallo, Joseph Firth, Ligia J. Dominguez, and Maria Gabriella Caruso. 2017. "Dietary Magnesium and Incident Frailty in Older People at Risk for Knee Osteoarthritis: An Eight-Year Longitudinal Study" Nutrients 9, no. 11: 1253. https://doi.org/10.3390/nu9111253
APA StyleVeronese, N., Stubbs, B., Maggi, S., Notarnicola, M., Barbagallo, M., Firth, J., Dominguez, L. J., & Caruso, M. G. (2017). Dietary Magnesium and Incident Frailty in Older People at Risk for Knee Osteoarthritis: An Eight-Year Longitudinal Study. Nutrients, 9(11), 1253. https://doi.org/10.3390/nu9111253







