Association between Milk Consumption and Metabolic Syndrome among Korean Adults: Results from the Health Examinees Study
Abstract
1. Introduction
2. Subjects and Methods
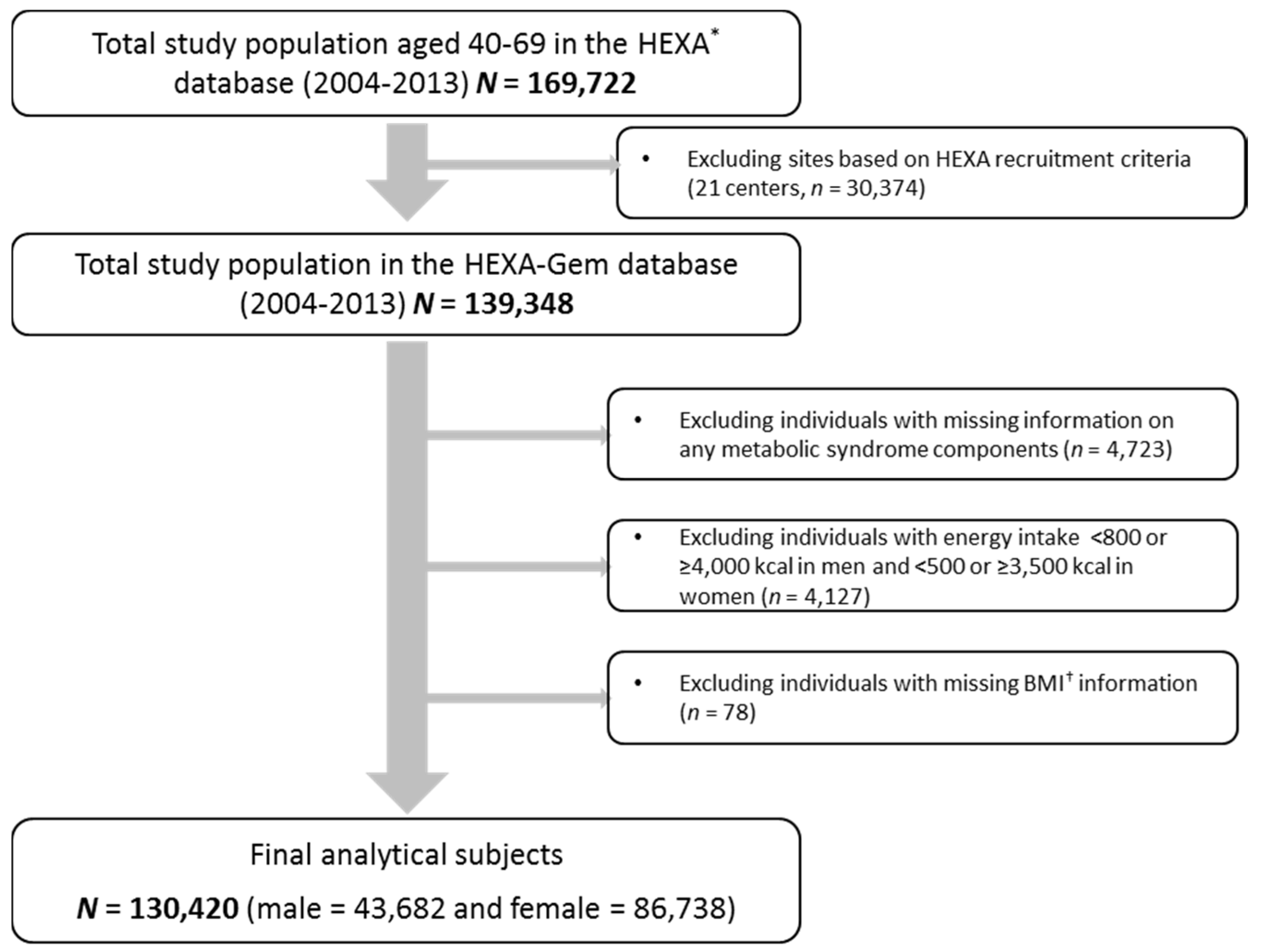
2.1. Study Population
2.2. Assessment of Milk and Dairy Food Consumption
2.3. Definition of Metabolic Syndrome
2.4. Covariates
2.5. Statistical Analysis
3. Results
4. Discussion
5. Conclusions
Supplementary Materials
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Grundy, S.M.; Hansen, B.; Smith, S.C., Jr.; Cleeman, J.I.; Kahn, R.A. Clinical management of metabolic syndrome: Report of the American Heart Association/National Heart, Lung, and Blood Institute/American Diabetes Association conference on scientific issues related to management. Circulation 2004, 109, 551–556. [Google Scholar] [CrossRef] [PubMed]
- Esposito, K.; Chiodini, P.; Colao, A.; Lenzi, A.; Giugliano, D. Metabolic Syndrome and Risk of Cancer A systematic review and meta-analysis. Diabetes Care 2012, 35, 2402–2411. [Google Scholar] [CrossRef] [PubMed]
- Grundy, S.M. Metabolic syndrome pandemic. Arterioscler. Thromb. Vasc. Biol. 2008, 28, 629–636. [Google Scholar] [CrossRef] [PubMed]
- Oh, S.W. Obesity and metabolic syndrome in Korea. Diabetes Metab. J. 2011, 35, 561–566. [Google Scholar] [CrossRef] [PubMed]
- Poulsen, P.; Vaag, A.; Kyvik, K.; Beck-Nielsen, H. Genetic versus environmental aetiology of the metabolic syndrome among male and female twins. Diabetologia 2001, 44, 537–543. [Google Scholar] [CrossRef] [PubMed]
- Azadbakht, L.; Mirmiran, P.; Esmaillzadeh, A.; Azizi, F. Dairy consumption is inversely associated with the prevalence of the metabolic syndrome in Tehranian adults. Am. J. Clin. Nutr. 2005, 82, 523–530. [Google Scholar] [PubMed]
- Pereira, M.A.; Jacobs, D.R.; Van Horn, L.; Slattery, M.L.; Kartashov, A.I.; Ludwig, D.S. Dairy consumption, obesity, and the insulin resistance syndrome in young adults—The CARDIA study. Jama J. Am. Med. Assoc. 2002, 287, 2081–2089. [Google Scholar] [CrossRef]
- Tong, X.; Dong, J.Y.; Wu, Z.W.; Li, W.; Qin, L.Q. Dairy consumption and risk of type 2 diabetes mellitus: A meta-analysis of cohort studies. Eur. J. Clin. Nutr. 2011, 65, 1027–1031. [Google Scholar] [CrossRef] [PubMed]
- Toledo, E.; Delgado-Rodriguez, M.; Estruch, R.; Salas-Salvado, J.; Corella, D.; Gomez-Gracia, E.; Fiol, M.; Lamuela-Raventos, R.M.; Schroder, H.; Aros, F.; et al. Low-fat dairy products and blood pressure: Follow-up of 2290 older persons at high cardiovascular risk participating in the PREDIMED study. Br. J. Nutr. 2009, 101, 59–67. [Google Scholar] [CrossRef] [PubMed]
- Wang, H.; Troy, L.M.; Rogers, G.T.; Fox, C.S.; McKeown, N.M.; Meigs, J.B.; Jacques, P.F. Longitudinal association between dairy consumption and changes of body weight and waist circumference: The Framingham Heart Study. Int. J. Obes. 2014, 38, 299–305. [Google Scholar] [CrossRef] [PubMed]
- Kris-Etherton, P.M.; Grieger, J.A.; Hilpert, K.F.; West, S.G. Milk products, dietary patterns and blood pressure management. J. Am. Coll. Nutr. 2009, 28 (Suppl. 1), 103S–119S. [Google Scholar] [CrossRef] [PubMed]
- Pfeuffer, M.; Schrezenmeir, J. Milk and the metabolic syndrome. Obes. Rev. 2007, 8, 109–118. [Google Scholar] [CrossRef] [PubMed]
- Tremblay, A.; Gilbert, J.A. Milk products, insulin resistance syndrome and type 2 diabetes. J. Am. Coll. Nutr. 2009, 28 (Suppl. 1), 91S–102S. [Google Scholar] [CrossRef] [PubMed]
- Fumeron, F.; Lamri, A.; Khalil, C.A.; Jaziri, R.; Porchay-Balderelli, I.; Lantieri, O.; Vol, S.; Balkau, B.; Marre, M.; Insulin, D.E.S. Dairy Consumption and the Incidence of Hyperglycemia and the Metabolic Syndrome Results from a French prospective study, Data from the Epidemiological Study on the Insulin Resistance Syndrome (DESIR). Diabetes Care 2011, 34, 813–817. [Google Scholar] [CrossRef] [PubMed]
- Kirii, K.; Mizoue, T.; Iso, H.; Takahashi, Y.; Kato, M.; Inoue, M.; Noda, M.; Tsugane, S.; Japan Public Health Center-based Prospective Study Group. Calcium, vitamin D and dairy intake in relation to type 2 diabetes risk in a Japanese cohort. Diabetologia 2009, 52, 2542–2550. [Google Scholar] [CrossRef] [PubMed]
- Zong, G.; Sun, Q.; Yu, D.; Zhu, J.; Sun, L.; Ye, X.; Li, H.; Jin, Q.; Zheng, H.; Hu, F.B.; et al. Dairy consumption, type 2 diabetes, and changes in cardiometabolic traits: A prospective cohort study of middle-aged and older Chinese in Beijing and Shanghai. Diabetes Care 2014, 37, 56–63. [Google Scholar] [CrossRef] [PubMed]
- Kim, Y.; Je, Y. Dairy consumption and risk of metabolic syndrome: A meta-analysis. Diabet. Med. 2016, 33, 428–440. [Google Scholar] [CrossRef] [PubMed]
- Louie, J.C.Y.; Flood, V.M.; Rangan, A.M.; Burlutsky, G.; Gill, T.P.; Gopinath, B.; Mitchell, P. Higher regular fat dairy consumption is associated with lower incidence of metabolic syndrome but not type 2 diabetes. Nutr. Metab. Cardiovas. 2013, 23, 816–821. [Google Scholar] [CrossRef] [PubMed]
- Beydoun, M.A.; Gary, T.L.; Caballero, B.H.; Lawrence, R.S.; Cheskin, L.J.; Wang, Y.F. Ethnic differences in dairy and related nutrient consumption among US adults and their association with obesity, central obesity, and the metabolic syndrome. Am. J. Clin. Nutr. 2008, 87, 1914–1925. [Google Scholar] [PubMed]
- Kim, J. Dairy food consumption is inversely associated with the risk of the metabolic syndrome in Korean adults. J. Hum. Nutr. Diet 2013, 26, 171–179. [Google Scholar] [CrossRef] [PubMed]
- Lee, K.W.; Cho, W. The Consumption of Dairy Products Is Associated with Reduced Risks of Obesity and Metabolic Syndrome in Korean Women but not in Men. Nutrients 2017, 9, 630. [Google Scholar] [CrossRef] [PubMed]
- Kim, D.; Kim, J. Dairy consumption is associated with a lower incidence of the metabolic syndrome in middle-aged and older Korean adults: The Korean Genome and Epidemiology Study (KoGES). Br. J. Nutr. 2017, 117, 148–160. [Google Scholar] [CrossRef] [PubMed]
- Lim, S.; Shin, H.; Song, J.H.; Kwak, S.H.; Kang, S.M.; Won Yoon, J.; Choi, S.H.; Cho, S.I.; Park, K.S.; Lee, H.K.; et al. Increasing prevalence of metabolic syndrome in Korea: The Korean National Health and Nutrition Examination Survey for 1998–2007. Diabetes Care 2011, 34, 1323–1328. [Google Scholar] [CrossRef] [PubMed]
- Kim, Y.; Han, B.G.; The KoGES Group. Cohort Profile: The Korean Genome and Epidemiology Study (KoGES) Consortium. Int. J. Epidemiol. 2016, 46, e20. [Google Scholar]
- Health Examinees Study Group. The Health Examinees (HEXA) study: Rationale, study design and baseline characteristics. Asian Pac. J. Cancer Prev. APJCP 2015, 16, 1591–1597. [Google Scholar]
- National Institute of Agricultural Sciences. Korean Standard Food Composition Tables, 8th ed.; Hye Kyung Chun: Seoul, Korea, 2013.
- Ahn, Y.; Kwon, E.; Shim, J.E.; Park, M.K.; Joo, Y.; Kimm, K.; Park, C.; Kim, D.H. Validation and reproducibility of food frequency questionnaire for Korean genome epidemiologic study. Eur. J. Clin. Nutr. 2007, 61, 1435–1441. [Google Scholar] [CrossRef] [PubMed]
- Grundy, S.M.; Becker, D.; Clark, L.T.; Cooper, R.S.; Denke, M.A.; Howard, W.J.; Hunninghake, D.B.; Illingworth, R.; Luepker, R.V.; McBride, P.; et al. Third Report of the National Cholesterol Education Program (NCEP) Expert Panel on Detection, Evaluation, and Treatment of High Blood Cholesterol in Adults (Adult Treatment Panel III) Final Report. Circulation 2002, 106, 3143–3421. [Google Scholar]
- Yang, J.J.; Song, M.; Yoon, H.S.; Lee, H.W.; Lee, Y.; Lee, S.A.; Choi, J.Y.; Lee, J.K.; Kang, D. What Are the Major Determinants in the Success of Smoking Cessation: Results from the Health Examinees Study. PLoS ONE 2015, 10. [Google Scholar] [CrossRef] [PubMed]
- Elwood, P.C.; Pickering, J.E.; Fehily, A.M. Milk and dairy consumption, diabetes and the metabolic syndrome: The Caerphilly prospective study. J. Epidemiol. Commun. H 2007, 61, 695–698. [Google Scholar] [CrossRef] [PubMed]
- Martins, M.L.B.; Kac, G.; Silva, R.A.; Bettiol, H.; Barbieri, M.A.; Cardoso, V.C.; Silva, A.A.M. Dairy consumption is associated with a lower prevalence of metabolic syndrome among young adults from Ribeirao Preto, Brazil. Nutrition 2015, 31, 716–721. [Google Scholar] [CrossRef] [PubMed]
- Lawlor, D.A.; Ebrahim, S.; Timpson, N.; Smith, G.D. Avoiding milk is associated with a reduced risk of insulin resistance and the metabolic syndrome: Findings from the British Women’s Heart and Health Study. Diabet. Med. 2005, 22, 808–811. [Google Scholar] [CrossRef] [PubMed]
- Snijder, M.B.; van der Heijden, A.A.W.A.; van Dam, R.M.; Stehouwer, C.D.A.; Hiddink, G.J.; Nijlels, G.; Heine, R.J.; Bouter, L.M.; Dekker, J.M. Is higher dairy consumption associated with lower body weight and fewer metabolic disturbances? The Hoorn Study. Am. J. Clin. Nutr. 2007, 85, 989–995. [Google Scholar] [PubMed]
- de Oliveira, E.P.; McLellan, K.C.P.; Silveira, L.V.D.; Burini, R.C. Dietary factors associated with metabolic syndrome in Brazilian adults. Nutr. J. 2012, 11. [Google Scholar] [CrossRef] [PubMed]
- Boon, N.; Hul, G.B.J.; Stegen, J.H.C.H.; Sluijsmans, W.E.M.; Valle, C.; Langin, D.; Viguerie, N.; Saris, W.H.M. An intervention study of the effects of calcium intake on faecal fat excretion, energy metabolism and adipose tissue mRNA expression of lipid-metabolism related proteins. Int. J. Obes. 2007, 31, 1704–1712. [Google Scholar] [CrossRef] [PubMed]
- Reid, I.R.; Mason, B.; Horne, A.; Ames, R.; Clearwater, J.; Bava, U.; Orr-Walker, B.; Wu, F.; Evans, M.C.; Gamble, G.D. Effects of calcium supplementation on serum lipid concentrations in normal older women: A randomized controlled trial. Am. J. Med. 2002, 112, 343–347. [Google Scholar] [CrossRef]
- Lorenzen, J.K.; Nielsen, S.; Holst, J.J.; Tetens, I.; Rehfeld, J.F.; Astrup, A. Effect of dairy calcium or supplementary calcium intake on postprandial fat metabolism, appetite, and subsequent energy intake. Am. J. Clin. Nutr. 2007, 85, 678–687. [Google Scholar] [PubMed]
- Zemel, M.B. Calcium modulation of hypertension and obesity: mechanisms and implications. J. Am. Coll. Nutr. 2001, 20, 428S–435S. [Google Scholar] [CrossRef] [PubMed]
- Bjornshave, A.; Hermansen, K. Effects of dairy protein and fat on the metabolic syndrome and type 2 diabetes. Rev. Diabet. Stud. 2014, 11, 153–166. [Google Scholar] [CrossRef] [PubMed]
- Rice, B.H.; Cifelli, C.J.; Pikosky, M.A.; Miller, G.D. Dairy Components and Risk Factors for Cardiometabolic Syndrome: Recent Evidence and Opportunities for Future Research. Adv. Nutr. 2011, 2, 396–407. [Google Scholar] [CrossRef] [PubMed]
- Pal, S.; Ellis, V.; Dhaliwal, S. Effects of whey protein isolate on body composition, lipids, insulin and glucose in overweight and obese individuals. Br. J. Nutr. 2010, 104, 716–723. [Google Scholar] [CrossRef] [PubMed]
- Zemel, M.B. The role of dairy foods in weight management. J. Am. Coll. Nutr. 2005, 24, 537s–546s. [Google Scholar] [CrossRef] [PubMed]
- Huth, P.J.; DiRienzo, D.B.; Miller, G.D. Major scientific advances with dairy foods in nutrition and health. J. Dairy Sci. 2006, 89, 1207–1221. [Google Scholar] [CrossRef]
- Dougkas, A.; Reynolds, C.K.; Givens, I.D.; Elwood, P.C.; Minihane, A.M. Associations between dairy consumption and body weight: A review of the evidence and underlying mechanisms. Nutr. Res. Rev. 2011, 24, 72–95. [Google Scholar] [CrossRef] [PubMed]
- Capriotti, A.L.; Cavaliere, C.; Piovesana, S.; Samperi, R.; Lagana, A. Recent trends in the analysis of bioactive peptides in milk and dairy products. Anal. Bioanal. Chem. 2016, 408, 2677–2685. [Google Scholar] [CrossRef] [PubMed]
- Pal, S.; Ellis, V. The chronic effects of whey proteins on blood pressure, vascular function, and inflammatory markers in overweight individuals. Obesity 2010, 18, 1354–1359. [Google Scholar] [CrossRef] [PubMed]
- Rego, O.A.; Portugal, P.V.; Sousa, M.B.; Rosa, H.J.D.; Vouzela, C.M.; Borba, A.E.S.; Bessa, R.J.B. Effect of diet on the fatty acid pattern of milk from dairy cows. Anim. Res. 2004, 53, 213–220. [Google Scholar] [CrossRef]
- Han, J.R.; Hamilton, J.A.; Kirkland, J.L.; Corkey, B.E.; Guo, W. Medium-chain oil reduces fat mass and down-regulates expression of adipogenic genes in rats. Obes. Res. 2003, 11, 734–744. [Google Scholar] [CrossRef] [PubMed]
- Gillingham, L.G.; Harris-Janz, S.; Jones, P.J. Dietary monounsaturated fatty acids are protective against metabolic syndrome and cardiovascular disease risk factors. Lipids 2011, 46, 209–228. [Google Scholar] [CrossRef] [PubMed]
- Cheema, S.K.; Agarwal-Mawal, A.; Murray, C.M.; Tucker, S. Lack of stimulation of cholesteryl ester transfer protein by cholesterol in the presence of a high-fat diet. J. Lipid Res. 2005, 46, 2356–2366. [Google Scholar] [CrossRef] [PubMed]
- Willett, W.C.; Howe, G.R.; Kushi, L.H. Adjustment for total energy intake in epidemiologic studies. Am. J. Clin. Nutr. 1997, 65, 1220–1228. [Google Scholar]
- Kautzky-Willer, A.; Harreiter, J.; Pacini, G. Sex and Gender Differences in Risk, Pathophysiology and Complications of Type 2 Diabetes Mellitus. Endocr. Rev. 2016, 37, 278–316. [Google Scholar] [CrossRef] [PubMed]
- Abreu, S.; Moreira, P.; Moreira, C.; Mota, J.; Moreira-Silva, I.; Santos, P.C.; Santos, R. Intake of milk, but not total dairy, yogurt, or cheese, is negatively associated with the clustering of cardiometabolic risk factors in adolescents. Nutr. Res. 2014, 34, 48–57. [Google Scholar] [CrossRef] [PubMed]
- Cade, J.; Thompson, R.; Burley, V.; Warm, D. Development, validation and utilisation of food-frequency questionnaires—A review. Public Health Nutr. 2002, 5, 567–587. [Google Scholar] [CrossRef] [PubMed]
- Dhurandhar, N.V.; Schoeller, D.; Brown, A.W.; Heymsfield, S.B.; Thomas, D.; Sorensen, T.I.; Speakman, J.R.; Jeansonne, M.; Allison, D.B.; Energy Balance Measurement Working Group. Energy balance measurement: When something is not better than nothing. Int. J. Obes. 2015, 39, 1109–1113. [Google Scholar] [CrossRef] [PubMed]
| Milk Consumption | p-Value † | |||||
|---|---|---|---|---|---|---|
| Non or Rarely | ≤2/Week | 3–6/Week | ≥1/Day | |||
| Men (N = 43,786) | 18,972 | 11,588 | 5936 | 7186 | ||
| Age (years) | 54.2 ± 8.2 | 52.7 ± 8.4 | 53.0 ± 8.4 | 53.9 ± 8.6 | <0.0001 | |
| BMI (kg/m2) | 24.4 ± 2.8 | 24.5 ± 2.7 | 24.4 ± 2.7 | 24.3 ± 2.7 | 0.0006 | |
| ≥College or above, n (%) | 6352 (34.0) | 4495 (39.2) | 2376 (40.6) | 2764 (38.9) | <0.0001 | |
| Current smokers, n (%) | 6257 (33.1) | 3660 (31.7) | 1736 (29.4) | 2055 (28.7) | <0.0001 | |
| Current drinkers, n (%) | 13,679 (72.2) | 8606 (74.4) | 4371 (73.8) | 5101 (71.2) | 0.5511 | |
| Regular exercisers, n (%) | 10,152 (53.6) | 6698 (57.9) | 3584 (60.6) | 4477 (62.4) | <0.0001 | |
| Dietary Intake | ||||||
| Energy (kcal) | 1730.8 ± 437.3 | 1835.1 ± 449.6 | 1960.5 ± 468.3 | 2054.2 ± 492.8 | <0.0001 | |
| Carbohydrate (g) | 312.8 ± 75.0 | 324.4 ± 76.5 | 338.3 ± 78.8 | 348.1 ± 83.3 | <0.0001 | |
| Protein (g) | 56.6 ± 20.5 | 61.5 ± 20.6 | 68.3 ± 21.8 | 73.8 ± 23.1 | <0.0001 | |
| Fat (g) | 25.5 ± 14.3 | 29.8 ± 14.5 | 34.9 ± 15.4 | 39.0 ± 16.0 | <0.0001 | |
| Calcium (mg) | 325.2 ± 169.7 | 380.7 ± 167.6 | 509.3 ± 183.1 | 666.0 ± 234.9 | <0.0001 | |
| Grain (g) | 643.9 ± 207.0 | 611.8 ± 192.3 | 572.9 ± 188.3 | 545.2 ± 189.1 | <0.0001 | |
| Vegetable (g) | 129.3 ± 102.0 | 129.3 ± 92.6 | 137.9 ± 95.3 | 138.3 ± 97.1 | <0.0001 | |
| Fruit (g) | 141.5 ± 144.0 | 140.6 ± 126.8 | 151.8 ± 132.0 | 160.7 ± 137.6 | <0.0001 | |
| Meat (g) | 41.0 ± 34.9 | 43.5 ± 31.6 | 42.1 ± 31.1 | 38.2 ± 30.7 | <0.0001 | |
| Non or Rarely | ≤2/Week | 3–6/Week | 1/Day | ≥2/Day | ||
| Women (N = 86,738) | 30,025 | 21,970 | 14,529 | 17,608 | 2606 | |
| Age, years | 53.1 ± 7.9 | 51.3 ± 7.7 | 51.5 ± 7.6 | 52.9 ± 7.7 | 52.2 ± 7.5 | <0.0001 |
| BMI, kg/m2 | 23.7 ± 3.0 | 23.6 ± 3.0 | 23.5 ± 2.8 | 23.6 ± 2.9 | 23.5 ± 2.8 | <0.0001 |
| ≥ College or above, n (%) | 4799 (16.2) | 4578 (21.1) | 3239 (22.6) | 3639 (20.9) | 585 (22.8) | <0.0001 |
| Current smokers, n (%) | 744 (2.5) | 424 (1.9) | 272 (1.9) | 369 (2.1) | 62 (2.4) | 0.0291 |
| Current drinkers, n (%) | 8376 (28.0) | 7144 (32.6) | 4762 (33.0) | 5368 (30.6) | 787 (30.4) | <0.0001 |
| Regular exercisers, n (%) | 13,814 (46.1) | 11,018 (50.2) | 7949 (54.8) | 9929 (56.5) | 1565 (60.3) | <0.0001 |
| Dietary Intake | ||||||
| Energy (kcal) | 1556.4 ± 456.2 | 1635.9 ± 466.3 | 1758.4 ± 484.5 | 1838.2 ± 489.5 | 2093.8 ± 555.7 | <0.0001 |
| Carbohydrate (g) | 287.8 ± 81.9 | 295.9 ± 83.4 | 309.4 ± 85.4 | 318.1 ± 85.9 | 342.0 ± 95.7 | <0.0001 |
| Protein (g) | 50.5 ± 20.0 | 54.2 ± 20.0 | 61.0 ± 21.3 | 65.7 ± 21.7 | 80.6 ± 27.3 | <0.0001 |
| Fat (g) | 20.7 ± 12.8 | 24.4 ± 13.3 | 29.3 ± 14.3 | 32.6 ± 14.3 | 44.8 ± 17.1 | <0.0001 |
| Calcium (mg) | 329.0 ± 184.2 | 380.2 ± 182.7 | 508.0 ± 194.4 | 633.5 ± 206.4 | 1053.1 ± 383.2 | <0.0001 |
| Grain (g) | 572.4 ± 216.6 | 536.9 ± 201.8 | 497.0 ± 189.9 | 470.6 ± 184.9 | 387.8 ± 181.0 | <0.0001 |
| Vegetable (g) | 150.7 ± 117.7 | 151.3 ± 110.9 | 158.9 ± 109.0 | 160.8 ± 109.4 | 181.0 ± 139.6 | <0.0001 |
| Fruit (g) | 197.9 ± 184.1 | 202.8 ± 180.9 | 210.3 ± 171.1 | 219.5 ± 169.9 | 223.7 ± 190.7 | <0.0001 |
| Meat (g) | 30.2 ± 30.2 | 33.5 ± 29.3 | 33.0 ± 28.7 | 30.4 ± 27.2 | 26.0 ± 24.5 | <0.0001 |
| Metabolic Syndrome and Components | Milk Consumption | p-Trend † | ||||
|---|---|---|---|---|---|---|
| Non or Rarely | ≤2/Week | 3–6/Week | ≥1/Day | |||
| Men (N = 43,682) | 18,972 | 11,588 | 5936 | 7186 | ||
| MetS ‡ | 5715 (30.1) § | 3345 (28.9) | 1671 (28.2) | 1970 (27.4) | ||
| Ref. | 0.94 (0.89–1.00) | 0.93 (0.86–1.00) | 0.92 (0.86–0.99) | 0.0160 | ||
| WC ≥ 90 cm | 5607 (29.6) | 3453 (29.8) | 1703 (28.7) | 2005 (27.9) | ||
| Ref. | 0.97 (0.91–1.04) | 0.9 (0.82–0.98) | 0.91 (0.84–0.99) | 0.0098 | ||
| Serum TG ≥ 150 mg/dL | 7765 (40.9) | 4555 (39.3) | 2241 (37.8) | 2586 (36.0) | ||
| Ref. | 0.91 (0.87–0.96) | 0.87 (0.82–0.93) | 0.84 (0.79–0.89) | <0.0001 | ||
| Serum HDL-C ≤ 40 mg/dL | 4622 (24.4) | 2676 (23.1) | 1279 (21.5) | 1492 (20.8) | ||
| Ref. | 0.95 (0.90–1.01) | 0.88 (0.82–0.94) | 0.83 (0.78–0.89) | <0.0001 | ||
| BP ≥ 130/85 mmHg | 10,192 (53.7) | 5959 (51.4) | 3060 (51.5) | 3776 (52.5) | ||
| Ref. | 0.94 (0.89–0.98) | 0.94 (0.89–1.00) | 0.99 (0.93–1.05) | 0.7007 | ||
| FB ≥ 100 mg/dL | 6604 (34.8) | 3946 (34.1) | 2040 (34.4) | 2559 (35.6) | ||
| Ref. | 0.98 (0.93–1.04) | 1.05 (0.97–1.14) | 1.07 (0.99–1.16) | 0.0500 | ||
| Non or Rarely | ≤2/Week | 3–6/Week | 1/Day | ≥2/Day | ||
| Women (N = 86,738) | 30,025 | 21,970 | 14,529 | 17,608 | 2606 | |
| MetS | 7053 (23.5) | 6368 (29.0) | 3203 (22.0) | 4212 (23.9) | 502 (19.3) | |
| Ref. | 0.88 (0.84–0.92) | 0.86 (0.82–0.91) | 0.85 (0.81–0.90) | 0.68 (0.60–0.76) | <0.0001 | |
| WC ≥ 80 cm | 13,168 (43.9) | 8964 (40.8) | 5635 (38.8) | 7259 (41.2) | 979 (37.6) | |
| Ref. | 0.97 (0.92–1.02) | 0.91 (0.86–0.96) | 0.94 (0.89–0.99) | 0.79 (0.71–0.89) | 0.0126 | |
| Serum TG ≥ 150 mg/dL | 7579 (25.2) | 4858 (22.1) | 3051 (21.0) | 3899 (22.1) | 508 (19.5) | |
| Ref. | 0.93 (0.89–0.97) | 0.87 (0.83–0.92) | 0.86 (0.82–0.90) | 0.76 (0.69–0.85) | <0.0001 | |
| Serum HDL-C ≤ 50 mg/dL | 11,976 (39.9) | 7667 (34.9) | 4765 (32.8) | 5884 (33.4) | 724 (27.8) | |
| Ref. | 0.87 (0.84–0.91) | 0.81 (0.77–0.84) | 0.78 (0.75–0.81) | 0.61 (0.56–0.67) | <0.0001 | |
| BP ≥ 130/85 mmHg | 11,912 (39.7) | 7702 (35.1) | 5104 (35.1) | 6677 (37.9) | 893 (34.3) | |
| Ref. | 0.95 (0.90–0.99) | 0.96 (0.91–1.02) | 1.01 (0.96–1.07) | 0.96 (0.86–1.08) | 0.3906 | |
| FB ≥ 100 mg/dL | 6139 (20.4) | 4035 (18.4) | 2689 (18.5) | 3614 (20.5) | 495 (19.0) | |
| Ref. | 0.97 (0.93–1.01) | 1.01 (0.96–1.06) | 1.07 (1.02–1.12) | 1.04 (0.93–1.15) | 0.0021 | |
© 2017 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Shin, S.; Lee, H.-W.; Kim, C.E.; Lim, J.; Lee, J.-k.; Kang, D. Association between Milk Consumption and Metabolic Syndrome among Korean Adults: Results from the Health Examinees Study. Nutrients 2017, 9, 1102. https://doi.org/10.3390/nu9101102
Shin S, Lee H-W, Kim CE, Lim J, Lee J-k, Kang D. Association between Milk Consumption and Metabolic Syndrome among Korean Adults: Results from the Health Examinees Study. Nutrients. 2017; 9(10):1102. https://doi.org/10.3390/nu9101102
Chicago/Turabian StyleShin, Sangah, Hwi-Won Lee, Claire E. Kim, Jiyeon Lim, Jong-koo Lee, and Daehee Kang. 2017. "Association between Milk Consumption and Metabolic Syndrome among Korean Adults: Results from the Health Examinees Study" Nutrients 9, no. 10: 1102. https://doi.org/10.3390/nu9101102
APA StyleShin, S., Lee, H.-W., Kim, C. E., Lim, J., Lee, J.-k., & Kang, D. (2017). Association between Milk Consumption and Metabolic Syndrome among Korean Adults: Results from the Health Examinees Study. Nutrients, 9(10), 1102. https://doi.org/10.3390/nu9101102






