High Prevalence of Vitamin D Deficiency in Pregnant Korean Women: The First Trimester and the Winter Season as Risk Factors for Vitamin D Deficiency
Abstract
:1. Introduction
2. Methods
2.1. Ethics Statement
2.2. Study Population
2.3. Data Collection
2.4. Definitions of Adverse Pregnancy Outcomes
2.5. Laboratory Analyses
2.6. Statistical Analysis
3. Results
3.1. General Characteristics
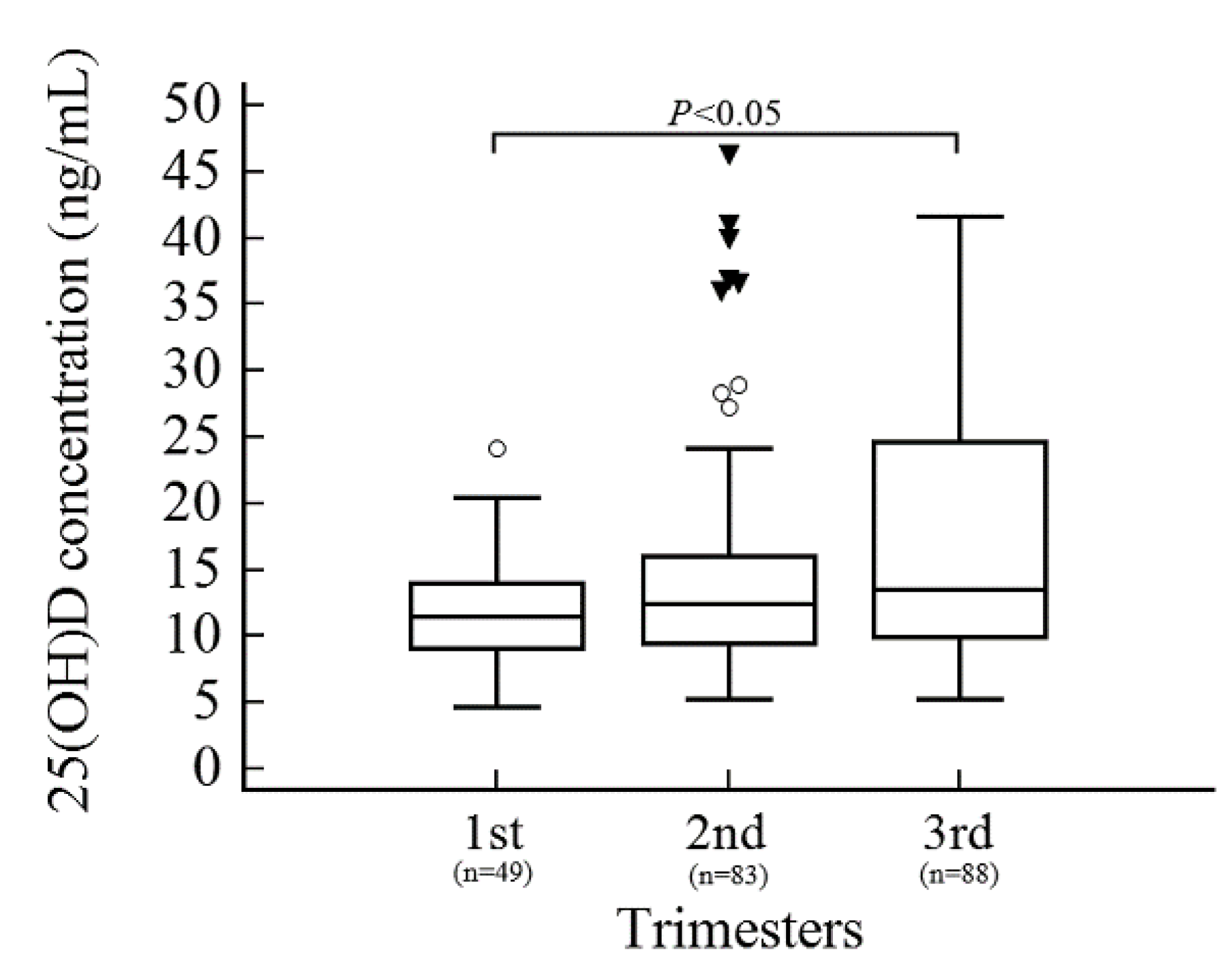
3.2. Serum 25(OH)D Levels in Pregnant Korean Women
3.3. Prevalences of Vitamin D Deficiency and Insufficiency in Pregnant Women
| Parameter | Total (n = 220) | First Trimester (n = 49) | Second Trimester (n = 83) | Third Trimester (n = 88) | p | ||||
|---|---|---|---|---|---|---|---|---|---|
| Median | Range | Median | Range | Median | Range | Median | Range | ||
| Age, years | 32.0 | 24.0–43.9 | 31.0 | 24.0–41.3 | 32.0 | 26.0–43.9 | 32.0 | 25.0–39.0 | 0.72 |
| Prepregnant BMI (kg/m2) | 20.2 | 16.0–28.5 | 20.3 | 16.0–26.3 | 20.8 | 16.3–28.5 | 19.8 | 16.0–27.5 | 0.21 |
| Prepregnant BMI * | n | % | n | % | n | % | n | % | 0.84 |
| Underweight (BMI < 18.0) | 27 | 12.3 | 6 | 12.2 | 10 | 10.0 | 11 | 12.5 | |
| Healthy normal (BMI 18.0–23.9) | 169 | 76.8 | 38 | 77.6 | 63 | 75.9 | 68 | 77.3 | |
| Overweight (BMI 24.0–26.9) | 20 | 9.1 | 5 | 10.2 | 7 | 8.4 | 8 | 9.1 | |
| Obese (BMI ≥ 27.0) | 4 | 1.8 | 0 | 0.0 | 3 | 3.6 | 1 | 1.2 | |
| Season † | 0.10 | ||||||||
| Spring | 98 | 44.5 | 20 | 40.8 | 35 | 42.2 | 43 | 48.9 | |
| Summer | 22 | 10.0 | 5 | 10.2 | 7 | 8.4 | 10 | 11.4 | |
| Fall | 87 | 39.5 | 18 | 39.7 | 34 | 40.9 | 35 | 39.8 | |
| Winter | 13 | 5.9 | 6 | 12.2 | 7 | 8.4 | 0 | 0.0 | |
| Education level ‡ | 0.53 | ||||||||
| Low | 12 | 5.5 | 3 | 6.1 | 6 | 7.2 | 3 | 3.4 | |
| High | 208 | 94.5 | 46 | 93.9 | 77 | 92.8 | 85 | 96.6 | |
| Job | 0.66 | ||||||||
| Any job | 70 | 31.8 | 35 | 71.4 | 58 | 69.9 | 57 | 64.8 | |
| Homemaker | 150 | 68.2 | 14 | 28.6 | 25 | 30.1 | 31 | 35.2 | |
| Type of current pregnancy | 0.56 | ||||||||
| Spontaneous pregnancy | 213 | 96.8 | 48 | 98.0 | 79 | 95.2 | 86 | 97.7 | |
| Artificial pregnancy | 7 | 3.2 | 1 | 2.0 | 4 | 4.8 | 2 | 2.3 | |
| Single or multiple pregnancy | 0.90 | ||||||||
| Singleton | 217 | 98.6 | 48 | 98.0 | 82 | 98.8 | 87 | 98.9 | |
| Twins | 3 | 1.4 | 1 | 2.0 | 1 | 1.2 | 1 | 1.1 | |
| Gravida | 0.57 | ||||||||
| Primigravida | 142 | 64.5 | 29 | 59.2 | 53 | 63.9 | 60 | 68.2 | |
| Multigravida | 78 | 35.5 | 20 | 40.8 | 30 | 36.1 | 28 | 31.8 | |
| n | % | n | % | n | % | n | % | ||
| Parity | 0.36 | ||||||||
| 0 (nullipara) | 136 | 61.8 | 27 | 55.1 | 50 | 60.2 | 59 | 67.0 | |
| ≥1 | 84 | 38.2 | 22 | 44.9 | 33 | 39.8 | 29 | 33.0 | |
| Previous or concurrent medical history | 0.30 | ||||||||
| Yes | 68 | 30.9 | 17 | 34.7 | 29 | 34.9 | 22 | 25.0 | |
| No | 152 | 69.1 | 32 | 65.3 | 54 | 65.1 | 66 | 75.0 | |
| Gynecological disease history | 0.88 | ||||||||
| Yes | 44 | 20.0 | 9 | 18.4 | 16 | 19.3 | 19 | 21.6 | |
| No | 176 | 80.0 | 40 | 81.6 | 67 | 80.7 | 69 | 78.4 | |
| 25(OH)D (ng/mL) | Healthy Nonpregnant Women * (n = 500) | All Pregnant Women (n = 220) | First Trimester (n = 49) | Second Trimester (n = 83) | Third Trimester (n = 88) |
|---|---|---|---|---|---|
| Median †,‡ | 15.4 | 12.6 | 11.5 | 12.5 | 13.6 |
| IQR | 12.7–19.7 | 9.7–17.3 | 9.1–14.0 | 9.5–16.0 | 9.9–24.7 |
| 95% CI | 14.8–15.8 | 11.9–13.3 | 10.0–13.0 | 11.1–13.4 | 12.1–16.6 |
| Range | 5.8–40.4 | 4.7–46.3 | 4.7–24.2 | 5.3–46.3 | 5.3–41.6 |
| % <10 ng/mL †,§,¶,|| | 7.2 | 28.6 | 32.7 | 28.9 | 26.1 |
| % <20 ng/mL § | 79.2 | 77.3 | 91.8 | 80.7 | 65.9 |
| % <30 ng/mL †,§ | 98.0 | 91.4 | 100.0 | 92.8 | 85.2 |

| Vitamin D Cutoff | Total | Deficiency | Suboptimal | Optimal | p | ||||
|---|---|---|---|---|---|---|---|---|---|
| <20 ng/mL | 20–29 ng/mL | 30–100 ng/mL | |||||||
| n | % | n | % | n | % | n | % | ||
| All women | 220 | 100.0 | 170 | 77.3 | 31 | 14.1 | 19 | 8.6 | |
| Prepregnant BMI * | >1 | ||||||||
| Underweight (BMI < 18.0) | 27 | 12.3 | 21 | 77.8 | 5 | 18.5 | 1 | 3.7 | |
| Healthy normal (BMI 18.0–23.9) | 169 | 76.8 | 129 | 76.3 | 25 | 14.8 | 15 | 8.9 | |
| Overweight (BMI 24.0–26.9) | 20 | 9.1 | 17 | 85.0 | 1 | 5.0 | 2 | 10.0 | |
| Obese (BMI ≥ 27.0) | 4 | 1.9 | 3 | 75.0 | 0 | 0.0 | 1 | 25.0 | |
| Age | 0.53 | ||||||||
| <30 years | 56 | 25.5 | 46 | 82.1 | 8 | 14.3 | 2 | 3.6 | |
| 30–35 years | 119 | 54.1 | 86 | 72.3 | 19 | 16.0 | 14 | 11.8 | |
| 35–40 years | 45 | 20.5 | 38 | 84.4 | 4 | 8.9 | 3 | 6.7 | |
| Trimester | 0.012 | ||||||||
| First trimester | 49 | 22.3 | 45 | 91.8 | 4 | 8.2 | 0 | 0.0 | |
| Second trimester | 83 | 37.7 | 67 | 80.7 | 10 | 12.0 | 6 | 7.2 | |
| Third trimester | 88 | 40.0 | 58 | 65.9 | 17 | 19.3 | 13 | 14.8 | |
| Season † | 0.007 | ||||||||
| Spring | 98 | 44.5 | 82 | 83.7 | 9 | 9.2 | 7 | 7.1 | |
| Summer | 22 | 10.0 | 10 | 45.5 | 8 | 36.4 | 4 | 18.2 | |
| Fall | 87 | 39.5 | 65 | 74.7 | 14 | 16.1 | 8 | 9.2 | |
| Winter | 13 | 5.9 | 13 | 100.0 | 0 | 0.0 | 0 | 0.0 | |
| Education level | 0.84 | ||||||||
| ≤12 years | 12 | 5.5 | 11 | 91.7 | 1 | 8.3 | 0 | 0.0 | |
| >12 years | 208 | 94.5 | 159 | 76.4 | 30 | 14.4 | 19 | 9.1 | |
| Job | 0.61 | ||||||||
| Any job | 150 | 68.2 | 119 | 79.3 | 21 | 14.0 | 10 | 6.7 | |
| Homemaker | 70 | 31.8 | 51 | 72.9 | 10 | 14.3 | 9 | 12.9 | |
| Type of current pregnancy | 0.13 | ||||||||
| Spontaneous | 213 | 96.8 | 167 | 78.4 | 29 | 13.6 | 17 | 8.0 | |
| Artificial insemination | 7 | 3.2 | 3 | 42.9 | 2 | 28.6 | 2 | 28.6 | |
| Single or multiple pregnancy | 0.31 | ||||||||
| Singleton | 217 | 98.6 | 169 | 77.9 | 30 | 13.8 | 18 | 8.3 | |
| Twins | 3 | 1.4 | 1 | 33.3 | 1 | 33.3 | 1 | 33.3 | |
| Gravity | >1 | ||||||||
| Primigravida | 142 | 64.5 | 107 | 75.4 | 21 | 14.8 | 14 | 9.9 | |
| Multigravida | 78 | 35.5 | 63 | 80.8 | 10 | 12.8 | 5 | 6.4 | |
| Parity | 0.96 | ||||||||
| 0 (nullipara) | 136 | 61.8 | 102 | 75.0 | 20 | 14.7 | 14 | 10.3 | |
| ≥1 | 84 | 38.2 | 68 | 81.0 | 11 | 13.1 | 5 | 6.0 | |
| Previous or concurrent medical history | 0.69 | ||||||||
| Yes | 152 | 69.1 | 120 | 78.9 | 18 | 11.8 | 14 | 9.2 | |
| No | 68 | 30.9 | 50 | 73.5 | 13 | 19.1 | 5 | 7.4 | |
| Gynecological disease history | 0.18 | ||||||||
| Yes | 176 | 80.0 | 131 | 74.4 | 29 | 16.5 | 16 | 9.1 | |
| No | 44 | 20.0 | 39 | 88.6 | 2 | 4.5 | 3 | 6.8 | |
| Risk of Vitamin D Deficiency | Number of Subjects | VitD-Deficient Subjects (<20 ng/mL) | Unadjusted Odds Ratio | 95% CI | p | Adjusted Odds Ratio | 95% CI | p | |||
|---|---|---|---|---|---|---|---|---|---|---|---|
| n | % | Lower | Upper | Lower | Upper | ||||||
| Age | 0.16 | 0.27 | |||||||||
| <30 years | 56 | 46 | 82.1 | Reference | Reference | ||||||
| 30–35 years | 119 | 86 | 72.3 | 0.567 | 0.229 | 1.403 | 0.523 | 0.186 | 1.475 | ||
| 35–40 years | 45 | 38 | 84.4 | 1.180 | 0.352 | 3.953 | 0.926 | 0.242 | 3.553 | ||
| Prepregnant BMI * | 0.86 | 0.74 | |||||||||
| Underweight (BMI < 18.0) | 27 | 21 | 77.8 | 1.085 | 0.330 | 3.567 | 0.628 | 0.168 | 2.345 | ||
| Healthy normal (BMI 18.0–23.9) | 169 | 129 | 76.3 | Reference | Reference | ||||||
| Overweight (BMI 24.0–26.9) | 20 | 17 | 85.0 | 1.757 | 0.369 | 8.3670 | 0.789 | 0.148 | 4.217 | ||
| Obese (BMI ≥ 27.0) | 4 | 3 | 75.0 | 0.930 | 0.058 | 15.271 | 0.326 | 0.010 | 11.007 | ||
| Trimester | 0.003 | 0.023 | |||||||||
| First trimester | 49 | 45 | 91.8 | 5.819 | 1.629 | 20.792 | 4.274 | 1.205 | 15.159 | ||
| Second trimester | 83 | 67 | 80.7 | 2.166 | 0.971 | 4.830 | 2.013 | 0.818 | 4.957 | ||
| Third trimester | 88 | 58 | 65.9 | Reference | Reference | ||||||
| Season † | 0.002 | 0.003 | |||||||||
| Spring | 98 | 82 | 83.7 | 5.952 | 1.770 | 20.018 | 8.026 | 1.973 | 32.650 | ||
| Summer | 22 | 10 | 45.5 | Reference | Reference | ||||||
| Fall | 87 | 65 | 74.7 | 3.465 | 1.063 | 11.296 | 4.346 | 1.113 | 16.970 | ||
| Winter | 13 | 13 | 100.0 | 32.157 | 0.777 | 1330.6 | 26.322 | 0.596 | 1161.7 | ||
| Education level | 0.25 | 0.40 | |||||||||
| ≤12 years | 12 | 11 | 91.7 | Reference | Reference | ||||||
| >12 years | 208 | 159 | 76.4 | 0.295 | 0.037 | 2.343 | 0.446 | 0.067 | 2.969 | ||
| Job | 0.29 | 0.10 | |||||||||
| Any job | 150 | 119 | 79.3 | 1.430 | 0.740 | 2.763 | 1.932 | 0.880 | 4.242 | ||
| Homemaker | 70 | 51 | 72.9 | Reference | Reference | ||||||
| Type of current pregnancy | 0.044 | 0.11 | |||||||||
| Spontaneous | 213 | 167 | 78.4 | Reference | Reference | ||||||
| Artificial insemination | 7 | 3 | 42.9 | 0.207 | 0.045 | 0.956 | 0.127 | 0.010 | 1.610 | ||
| Single or multiple pregnancy | 0.11 | 0.78 | |||||||||
| Singleton | 217 | 169 | 77.9 | Reference | Reference | ||||||
| Twins | 3 | 1 | 33.3 | 0.142 | 0.013 | 1.601 | 0.559 | 0.009 | 35.596 | ||
| Gravity ‡ | 0.72 | ||||||||||
| Primigravida | 142 | 107 | 75.4 | Reference | |||||||
| Multigravida | 78 | 63 | 80.8 | 1.374 | 0.631 | 2.991 | |||||
| Parity | 0.62 | 0.27 | |||||||||
| 0 (nullipara) | 136 | 102 | 75.0 | Reference | Reference | ||||||
| ≥1 | 84 | 68 | 81.0 | 1.417 | 0.659 | 3.0436 | 1.586 | 0.702 | 3.580 | ||
| Previous or concurrent medical history | 0.38 | 0.36 | |||||||||
| Yes | 152 | 120 | 78.9 | 0.741 | 0.381 | 1.4400 | 0.698 | 0.324 | 1.503 | ||
| No | 68 | 50 | 73.5 | Reference | Reference | ||||||
| Gynecological disease history | 0.05 | 0.027 | |||||||||
| Yes | 176 | 131 | 74.4 | 2.679 | 0.995 | 7.2150 | 3.466 | 1.155 | 10.399 | ||
| No | 44 | 39 | 88.6 | Reference | Reference | ||||||
3.4. Factors Associated with Vitamin D Deficiency during Pregnancy
3.5. Associations between Vitamin D Deficiency and Pregnancy Outcomes
| Outcomes | Preterm | SGA | ||||
|---|---|---|---|---|---|---|
| Preterm (−) | Preterm (+) | p | SGA (−) | SGA (+) | p | |
| Number of subjects | 211 | 9 | 196 | 24 | ||
| Number with VitD deficiency * | 163 | 7 | 155 | 15 | ||
| % with VitD deficiency * | 77.3 | 77.8 | 79.1 | 62.5 | ||
| Unadjusted OR (95% CI) | Reference | 1.030 (0.207–5.124) | 0.97 | Reference | 0.441 (0.180–1.079) | 0.07 |
| Adjusted OR (95% CI) | Reference | 0.699 (0.144–3.402) | 0.66 | Reference | 0.448 (0.149–1.351) | 0.15 |
4. Discussion
| Ref. | Region | Lat. (°N) * | N of Preg | GA at Blood Sampling | 25(OH)D Concentration | % <20 ng/mL § (% <50 nmol/L) | Pregnancy and Birth Outcome | Significant Association (p < 0.05) | Method | ||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Presented as | Reported Value | Units † | Converted to ng/mL ‡ | ||||||||||
| Asia | |||||||||||||
| This study | South Korea | 36 | 220 | First, Second, Third trimesters | median (IQR) | 12.6 (9.65–17.30) | ng/mL | 12.6 | 77.3% | PROM, preterm delivery, SGA | No | LC-MS/MS | |
| [16] | Tokai, Japan | 35.3 | 93 ¶ | 30 weeks | mean ± SD | 14.5 ± 5.0 | ng/mL | 14.5 | 89.5% | premature delivery | premature delivery | RIA | |
| [17] | Beijing, China ** | 39.9 | 125 | 15–20 weeks | mean ± SD | 28.4 ± 9.5 | nmol/L | 11.42 | 96.8% | NA | ELISA | ||
| [19] | Guiyang, China | NA * | 311 | Second and third trimesters | mean ± SD | 14.69 ± 6.81 | ng/mL | 14.69 | 83.6% | NA | LC-MS/MS | ||
| [17] | Beijing, China | 39.9 | 70 | Prior to labor | mean ± SE | 28.64 ± 1.41 | nmol/L | 11.47 | 90.2% | birth weight, birth length, HC | birth weight, birth length | ELISA | |
| [15]. | Nanjing, China | 31 | 152 | 24–28 weeks | mean ± SD | 10.9 ± 4.78 | ng/mL | 10.9 | in winter 96.1% in summer 94.7% | NA | ELISA | ||
| [18] | Chengdu, China | 30.7 | 77 | Before labor | mean ± SD | 35.95 ± 19.7 | nmol/L | 14.40 | NA | NA | EIA | ||
| Studies at regions near 36°N | |||||||||||||
| [21] | Tehran, Iran ** | NA * | 552 | Delivery | mean ± 2 SD | 27.8 ± 21.71 | nmol/L | 11.1 | NA | birth height, weight, HC, post. & ant. fontanel diameter, Apgar score | No | RIA | |
| [20] | USA | NA * | 928 | First, second, third trimesters | mean (95% CI) | 65 (61–68) | nmol/L | 26.0 | 33.8% | NA | RIA | ||
| [23] | Almeria, Spain | 36 | 502 | 11–14 weeks | median (IQR) | 27.4 (20.9–32.8) | ng/mL | 27.4 | 22.7% | NA | ECLIA | ||
| [3] | Almeria, Spain ‡‡ | 36 | 466 | First, third trimesters | NA | NA | ng/mL | NA | 23.4% | §§ PROM, preterm delivery, SGA, etc. | No | ECLIA | |
| [22] | Athens, Greece | NA * | 123 | Delivery | median (IQR) | 16.4 (11–21.1) | ng/mL | 16.4 | NA | NA | CLIA | ||
| [4] | Izmir, Turkey | 38.25 | 300 | ≥37 weeks | mean ± SD | 11.5 ± 5.4 | ng/mL | 11.5 | 90.3% | NA | CLIA | ||
| [24] | Ankara, Turkey ** | 40 | 79 | Third trimester | mean ± SD | 11.95 + 7.20 | ng/mL | 11.95 | NA | birth height, weight, HC, post. & ant. fontanel diameter, MUAC, Apgar score | No | HPLC | |
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Holick, M.F. Vitamin D deficiency. New Engl. J. Med. 2007, 357, 266–281. [Google Scholar] [CrossRef] [PubMed]
- Stepman, H.C.; Vanderroost, A.; van Uytfanghe, K.; Thienpont, L.M. Candidate reference measurement procedures for serum 25-hydroxyvitamin D3 and 25-hydroxyvitamin D2 by using isotope-dilution liquid chromatography-tandem mass spectrometry. Clin. Chem. 2011, 57, 441–448. [Google Scholar] [CrossRef] [PubMed]
- Fernandez-Alonso, A.M.; Dionis-Sanchez, E.C.; Gonzalez-Salmeron, M.D.; Perez-Lopez, F.R.; Chedraui, P. First-trimester maternal serum 25-hydroxyvitamin D(3) status and pregnancy outcome. Int. J. Gynaecol. Obstet. 2012, 116, 6–9. [Google Scholar] [CrossRef] [PubMed]
- Thorne-Lyman, A.; Fawzi, W.W. Vitamin D during pregnancy and maternal, neonatal and infant health outcomes: A systematic review and meta-analysis. Paediatr. Perinat. Epidemiol. 2012, 26 (Suppl. 1), 75–90. [Google Scholar] [CrossRef] [PubMed]
- Aghajafari, F.; Nagulesapillai, T.; Ronksley, P.E.; Tough, S.C.; O’Beirne, M.; Rabi, D.M. Association between maternal serum 25-hydroxyvitamin D level and pregnancy and neonatal outcomes: Systematic review and meta-analysis of observational studies. BMJ Clin. Res. Ed. 2013, 346, f1169. [Google Scholar] [CrossRef]
- Bener, A.; Al-Hamaq, A.O.; Saleh, N.M. Association between vitamin D insufficiency and adverse pregnancy outcome: Global comparisons. Int. J. Womens Health 2013, 5, 523–531. [Google Scholar] [CrossRef] [PubMed]
- Bedner, M.; Lippa, K.A.; Tai, S.S. An assessment of 25-hydroxyvitamin D measurements in comparability studies conducted by the vitamin D metabolites quality assurance program. Clin. Chim. Acta 2013, 426, 6–11. [Google Scholar] [CrossRef] [PubMed]
- Heijboer, A.C.; Blankenstein, M.A.; Kema, I.P.; Buijs, M.M. Accuracy of 6 routine 25-hydroxyvitamin D assays: Influence of vitamin d binding protein concentration. Clin. Chem. 2012, 58, 543–548. [Google Scholar] [CrossRef] [PubMed]
- Farrell, C.J.; Herrmann, M. Determination of vitamin D and its metabolites. Best Pract. Res. Clin. Endocrinol. Metab. 2013, 27, 675–688. [Google Scholar] [CrossRef] [PubMed]
- Karras, S.N.; Shah, I.; Petroczi, A.; Goulis, D.G.; Bili, H.; Papadopoulou, F.; Harizopoulou, V.; Tarlatzis, B.C.; Naughton, D.P. An observational study reveals that neonatal vitamin D is primarily determined by maternal contributions: Implications of a new assay on the roles of vitamin d forms. Nutr. J. 2013, 12, 77. [Google Scholar] [CrossRef] [PubMed]
- Simoens, C.; Goffin, F.; Simon, P.; Barlow, P.; Antoine, J.; Foidart, J.M.; Arbyn, M. Adverse obstetrical outcomes after treatment of precancerous cervical lesions: A belgian multicentre study. BJOG Int. J. Obstet. Gynaecol. 2012, 119, 1247–1255. [Google Scholar] [CrossRef]
- Wildman, R.P.; Gu, D.; Reynolds, K.; Duan, X.; He, J. Appropriate body mass index and waist circumference cutoffs for categorization of overweight and central adiposity among chinese adults. Am. J. Clin. Nutr. 2004, 80, 1129–1136. [Google Scholar] [PubMed]
- Institute of Medicine. Dietary Reference Intakes for Calcium and Vitamin; Ross, A.C., Taylor, C.L., Eds.; The National Academies Press: Washington, DC, USA, 2011. [Google Scholar]
- Mulligan, M.L.; Felton, S.K.; Riek, A.E.; Bernal-Mizrachi, C. Implications of vitamin D deficiency in pregnancy and lactation. Am. J. Obstet. Gynecol. 2010, 202, 429.e1–429.e9. [Google Scholar] [CrossRef] [PubMed]
- Jiang, L.; Xu, J.; Pan, S.; Xie, E.; Hu, Z.; Shen, H. High prevalence of hypovitaminosis D among pregnant women in southeast China. Acta Paediatr. 2012, 101, e192–e194. [Google Scholar] [CrossRef] [PubMed]
- Shibata, M.; Suzuki, A.; Sekiya, T.; Sekiguchi, S.; Asano, S.; Udagawa, Y.; Itoh, M. High prevalence of hypovitaminosis D in pregnant Japanese women with threatened premature delivery. J. Bone Miner. Metab. 2011, 29, 615–620. [Google Scholar] [CrossRef] [PubMed]
- Song, S.J.; Zhou, L.; Si, S.; Liu, J.; Zhou, J.; Feng, K.; Wu, J.; Zhang, W. The high prevalence of vitamin D deficiency and its related maternal factors in pregnant women in Beijing. PloS ONE 2013, 8, e85081. [Google Scholar] [CrossRef] [PubMed]
- Wang, J.; Yang, F.; Mao, M.; Liu, D.H.; Yang, H.M.; Yang, S.F. High prevalence of vitamin D and calcium deficiency among pregnant women and their newborns in Chengdu, China. World J. Pediatr. WJP 2010, 6, 265–267. [Google Scholar] [CrossRef]
- Xiang, F.; Jiang, J.; Li, H.; Yuan, J.; Yang, R.; Wang, Q.; Zhang, Y. High prevalence of vitamin D insufficiency in pregnant women working indoors and residing in Guiyang, China. J. Endocrinol. Investig. 2013, 36, 503–507. [Google Scholar]
- Ginde, A.A.; Sullivan, A.F.; Mansbach, J.M.; Camargo, C.A., Jr. Vitamin D insufficiency in pregnant and nonpregnant women of childbearing age in the United States. Am. J. Obstet. Gynecol. 2010, 202, 436.e1–436.e8. [Google Scholar] [CrossRef] [PubMed]
- Maghbooli, Z.; Hossein-Nezhad, A.; Shafaei, A.R.; Karimi, F.; Madani, F.S.; Larijani, B. Vitamin D status in mothers and their newborns in Iran. BMC Pregnancy Childbirth 2007, 7, 1. [Google Scholar] [CrossRef] [PubMed]
- Nicolaidou, P.; Hatzistamatiou, Z.; Papadopoulou, A.; Kaleyias, J.; Floropoulou, E.; Lagona, E.; Tsagris, V.; Costalos, C.; Antsaklis, A. Low vitamin D status in mother-newborn pairs in Greece. Calcif. Tissue Int. 2006, 78, 337–342. [Google Scholar] [CrossRef] [PubMed]
- Perez-Lopez, F.R.; Fernandez-Alonso, A.M.; Ferrando-Marco, P.; Gonzalez-Salmeron, M.D.; Dionis-Sanchez, E.C.; Fiol-Ruiz, G.; Chedraui, P. First trimester serum 25-hydroxyvitamin D status and factors related to lower levels in gravids living in the Spanish Mediterranean coast. Reprod. Sci. 2011, 18, 730–736. [Google Scholar] [CrossRef] [PubMed]
- Ustuner, I.; Keskin, H.L.; Tas, E.E.; Neselioglu, S.; Sengul, O.; Avsar, A.F. Maternal serum 25(OH) D levels in the third trimester of pregnancy during the winter season. J. Matern. Fetal Neonatal Med. 2011, 24, 1421–1426. [Google Scholar] [CrossRef] [PubMed]
- Brannon, P.M.; Picciano, M.F. Vitamin D in pregnancy and lactation in humans. Annu. Rev. Nutr. 2011, 31, 89–115. [Google Scholar] [CrossRef] [PubMed]
- Charatcharoenwitthaya, N.; Nanthakomon, T.; Somprasit, C.; Chanthasenanont, A.; Chailurkit, L.O.; Pattaraarchachai, J.; Ongphiphadhanakul, B. Maternal vitamin D status, its associated factors and the course of pregnancy in Thai women. Clin. Endocrinol. 2013, 78, 126–133. [Google Scholar] [CrossRef]
- Marwaha, R.K.; Tandon, N.; Chopra, S.; Agarwal, N.; Garg, M.K.; Sharma, B.; Kanwar, R.S.; Bhadra, K.; Singh, S.; Mani, K.; et al. Vitamin D status in pregnant indian women across trimesters and different seasons and its correlation with neonatal serum 25-hydroxyvitamin D levels. Br. J. Nutr. 2011, 106, 1383–1389. [Google Scholar] [CrossRef] [PubMed]
- Paffoni, A.; Somigliana, E.; Vigano, P.; Benaglia, L.; Cardellicchio, L.; Pagliardini, L.; Papaleo, E.; Candiani, M.; Fedele, L. Vitamin D status in women with uterine leiomyomas. J. Clin. Endocrinol. Metab. 2013, 98, E1374–E1378. [Google Scholar] [CrossRef] [PubMed]
- Sayegh, L.; Fuleihan Gel, H.; Nassar, A.H. Vitamin D in endometriosis: A causative or confounding factor? Metab. Clin. Exp. 2014, 63, 32–41. [Google Scholar] [CrossRef] [PubMed]
- Hensel, K.J.; Randis, T.M.; Gelber, S.E.; Ratner, A.J. Pregnancy-specific association of vitamin D deficiency and bacterial vaginosis. Am. J. Obstet. Gynecol. 2011, 204, 41.e1–41.e9. [Google Scholar] [CrossRef] [PubMed]
- Holick, M.F.; Binkley, N.C.; Bischoff-Ferrari, H.A.; Gordon, C.M.; Hanley, D.A.; Heaney, R.P.; Murad, M.H.; Weaver, C.M. Evaluation, treatment, and prevention of vitamin D deficiency: An endocrine society clinical practice guideline. J. Clin. Endocrinol. Metab. 2011, 96, 1911–1930. [Google Scholar] [CrossRef] [PubMed]
- Dawodu, A.; Saadi, H.F.; Bekdache, G.; Javed, Y.; Altaye, M.; Hollis, B.W. Randomized controlled trial (RCT) of vitamin D supplementation in pregnancy in a population with endemic vitamin D deficiency. J. Clin. Endocrinol. Metab. 2013, 98, 2337–2346. [Google Scholar] [CrossRef] [PubMed]
- Hill, A.B. The environment and disease: Association or causation? Proc. R. Soc. Med. 1965, 58, 295–300. [Google Scholar] [PubMed]
- Wei, S.Q.; Qi, H.P.; Luo, Z.C.; Fraser, W.D. Maternal vitamin D status and adverse pregnancy outcomes: A systematic review and meta-analysis. J. Matern. Fetal Neonatal Med. 2013, 26, 889–899. [Google Scholar] [CrossRef] [PubMed]
© 2015 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Choi, R.; Kim, S.; Yoo, H.; Cho, Y.Y.; Kim, S.W.; Chung, J.H.; Oh, S.-y.; Lee, S.-Y. High Prevalence of Vitamin D Deficiency in Pregnant Korean Women: The First Trimester and the Winter Season as Risk Factors for Vitamin D Deficiency. Nutrients 2015, 7, 3427-3448. https://doi.org/10.3390/nu7053427
Choi R, Kim S, Yoo H, Cho YY, Kim SW, Chung JH, Oh S-y, Lee S-Y. High Prevalence of Vitamin D Deficiency in Pregnant Korean Women: The First Trimester and the Winter Season as Risk Factors for Vitamin D Deficiency. Nutrients. 2015; 7(5):3427-3448. https://doi.org/10.3390/nu7053427
Chicago/Turabian StyleChoi, Rihwa, Seonwoo Kim, Heejin Yoo, Yoon Young Cho, Sun Wook Kim, Jae Hoon Chung, Soo-young Oh, and Soo-Youn Lee. 2015. "High Prevalence of Vitamin D Deficiency in Pregnant Korean Women: The First Trimester and the Winter Season as Risk Factors for Vitamin D Deficiency" Nutrients 7, no. 5: 3427-3448. https://doi.org/10.3390/nu7053427
APA StyleChoi, R., Kim, S., Yoo, H., Cho, Y. Y., Kim, S. W., Chung, J. H., Oh, S.-y., & Lee, S.-Y. (2015). High Prevalence of Vitamin D Deficiency in Pregnant Korean Women: The First Trimester and the Winter Season as Risk Factors for Vitamin D Deficiency. Nutrients, 7(5), 3427-3448. https://doi.org/10.3390/nu7053427





