Association between Nutritional Awareness and Diet Quality: Evidence from the Observation of Cardiovascular Risk Factors in Luxembourg (ORISCAV-LUX) Study
Abstract
:1. Introduction
2. Material and Methods
2.1. Study Design and Participants
2.2. Dietary Intake
2.3. Outcome Variables: Diet Quality Indicators
2.4. Explanatory Variable: Nutritional Awareness
2.5. Covariates
2.6. Statistical Analysis
3. Results
3.1. Characteristics of the ORISCAV-LUX Participants
3.2. Nutrition Awareness and Diet Quality
| Participant’s characteristics | Nutritional Awareness | Total Sample | p-value | ||
|---|---|---|---|---|---|
| High Importance | Moderate Importance | Little Importance | |||
| N (%) | N (%) | N (%) | N (%) | ||
| n | 700 (51) | 570 (42.2) | 81(6.0) | 1351 | |
| Sex, % | |||||
| Men | 293 (41.9) | 310 (54.4) | 53 (65.4) | 656 (48.6) | <0.0001 |
| Women | 407 (58.1) | 260 (45.6) | 28 (34.6) | 695 (51.4) | |
| Country of birth, % | <0.0001 | ||||
| Luxembourg | 373 (53.3) | 391 (68.6) | 58 (71.6) | 822 (60.8) | |
| Portugal | 112 (16.0) | 47 (8.2) | 3 (3.7) | 162 (12.0) | |
| Other European | 159 (22.7) | 118 (20.7) | 15 (18.5) | 292 (21.6) | |
| Non-European | 56 (8.0) | 14 (2.5) | 5 (6.2) | 75 (5.6) | |
| Education level, % | 0.27 | ||||
| Primary | 195 (28.3) | 133 (23.5) | 22 (27.2) | 350 (26.2) | |
| Secondary | 312 (45.2) | 278 (49.1) | 42 (51.9) | 632 (47.3) | |
| Tertiary | 183 (26.5) | 155 (27.4) | 17 (21.0) | 355 (26.6) | |
| Poverty threshold, | 0.006 | ||||
| Above | 475 (78.4) | 405 (80.8) | 42 (63.6) | 922 (78.6) | |
| Below | 131 (21.6) | 96 (19.2) | 24 (36.4) | 251 (21.4) | |
| Mean (SD) | Mean (SD) | Mean (SD) | |||
| Age, year | 44.9 (13.0) | 44.4 (12.8) | 38.6 (13.6) | 44.23 (13.1) | <0.0001 |
| BMI, kg/m2 | 26.1 (4.7) | 27.2 (5.2) | 26.5 (5.1) | 26.55 (5) | <0.0001 |
| Total energy intake, kcal/day | 2322.1 (851.6) | 2460 (951.8) | 2975 (1255.1) | 2419 (935) | <0.0001 |
| Diet quality variables | |||||
| Energy density (EDS) | 99.1 (26.2) | 103.5 (25.8) | 115 (35.2) | 101.9 (26.9) | <0.0001 |
| Food diversity (DDS) | 15.3 (3.2) | 14.8 (3.3) | 13.4 (3.9) | 15.9 (2.6) | <0.0001 |
| Recommendation Compliance Index (RCI) | 7.2 (2.3) | 6.5 (2.2) | 5.3 (2.0) | 6.8 (2.3) | <0.0001 |
| Diet quality scores | Nutrition Awareness | p-value | ||
|---|---|---|---|---|
| High Importance | Moderate Importance | Little Importance | ||
| β (SE) | β (SE) | β (SE) | ||
| Energy density (EDS) | ||||
| Model I | −11.8 (3.1) | −8.3 (3.1) | Ref. | <0.0001 |
| Model II | −11.4 (3.1) | −7.5 (3.1) | Ref. | <0.0001 |
| Model III | −7.6 (3.4) | −4.4 (3.4) | Ref. | 0.024 |
| Model IV | −7.4 (3.4) | −3.9 (3.3) | Ref. | 0.020 |
| Dietary diversity (DDS) * | ||||
| Model I | 2.8 (0.4) | 2.2 (0.4) | Ref. | <0.0001 |
| Model II | 2.7 (0.4) | 2.2 (0.4) | Ref. | <0.0001 |
| Model III | 2.5 (0.4) | 1.9 (0.4) | Ref. | <0.0001 |
| Model IV | 2.6 (0.4) | 2.0 (0.4) | Ref. | <0.0001 |
| Recommendation Compliance Index (RCI) * | ||||
| Model I | 1.4 (0.3) | 0.8 (0.3) | Ref. | <0.0001 |
| Model II | 1.4 (0.3) | 0.8 (0.3) | Ref. | <0.0001 |
| Model III | 1.3 (0.3) | 0.7 (0.3) | Ref. | <0.0001 |
| Model IV | 1.4 (0.3) | 0.8 (0.3) | Ref. | <0.0001 |
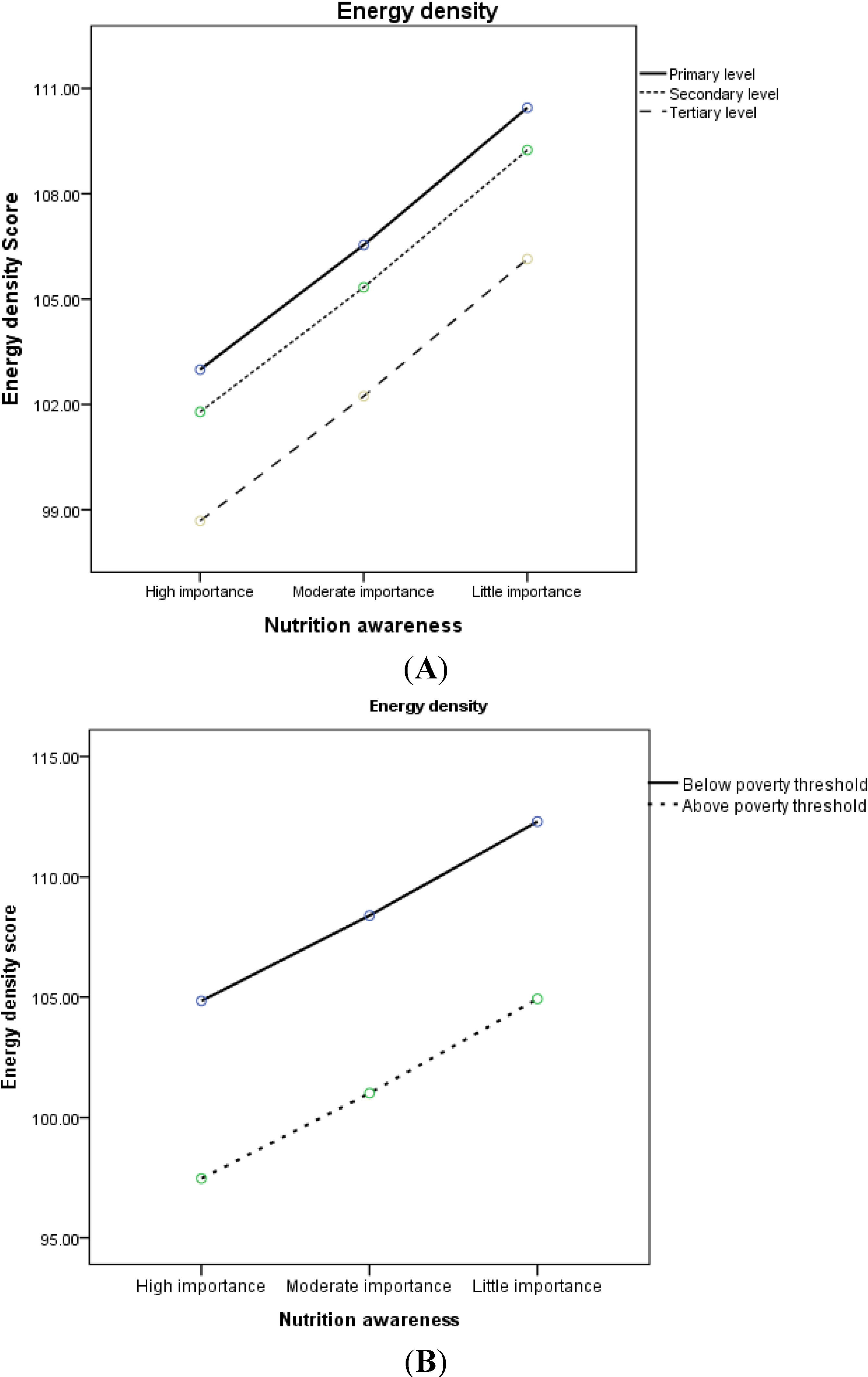
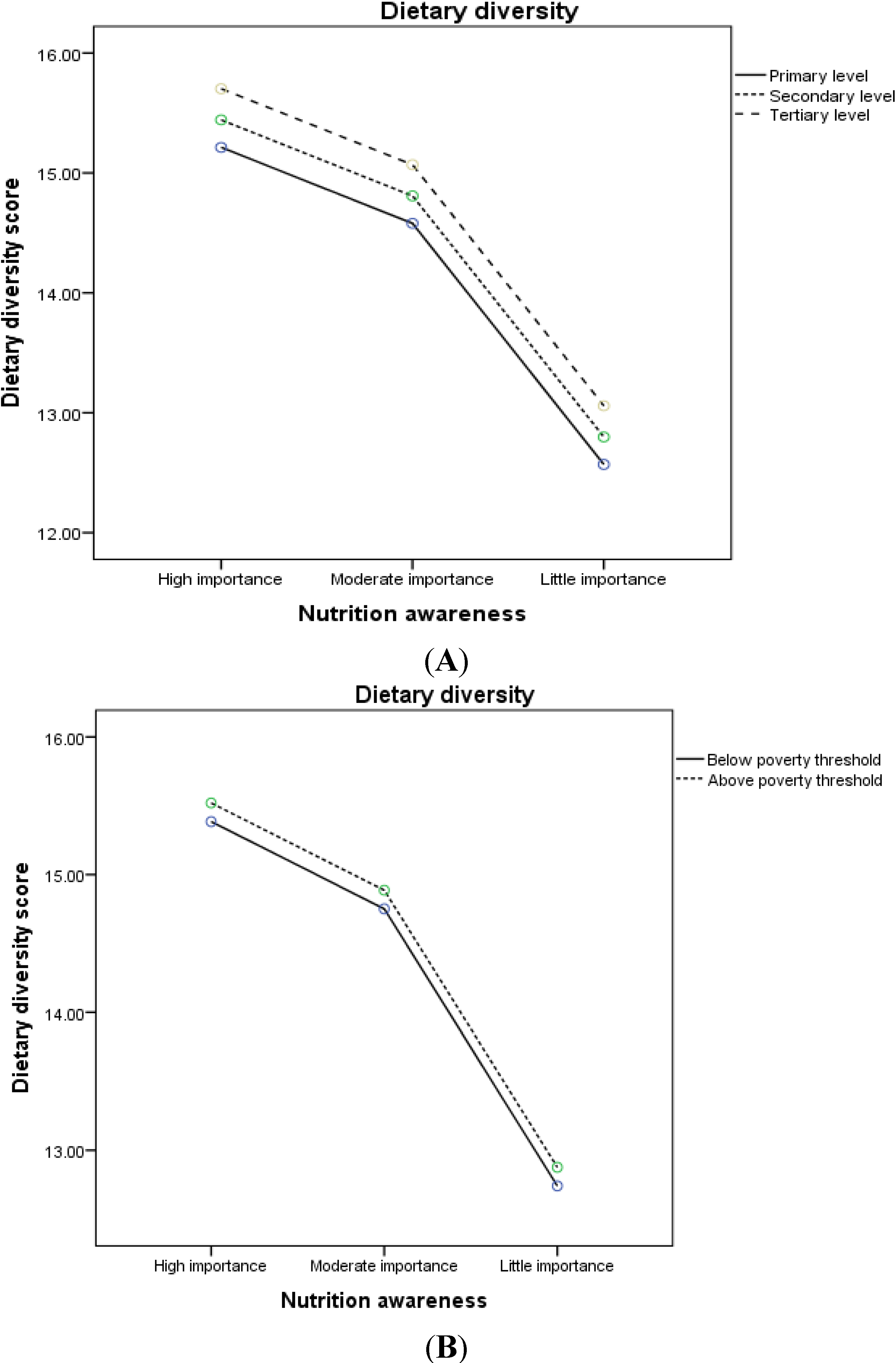
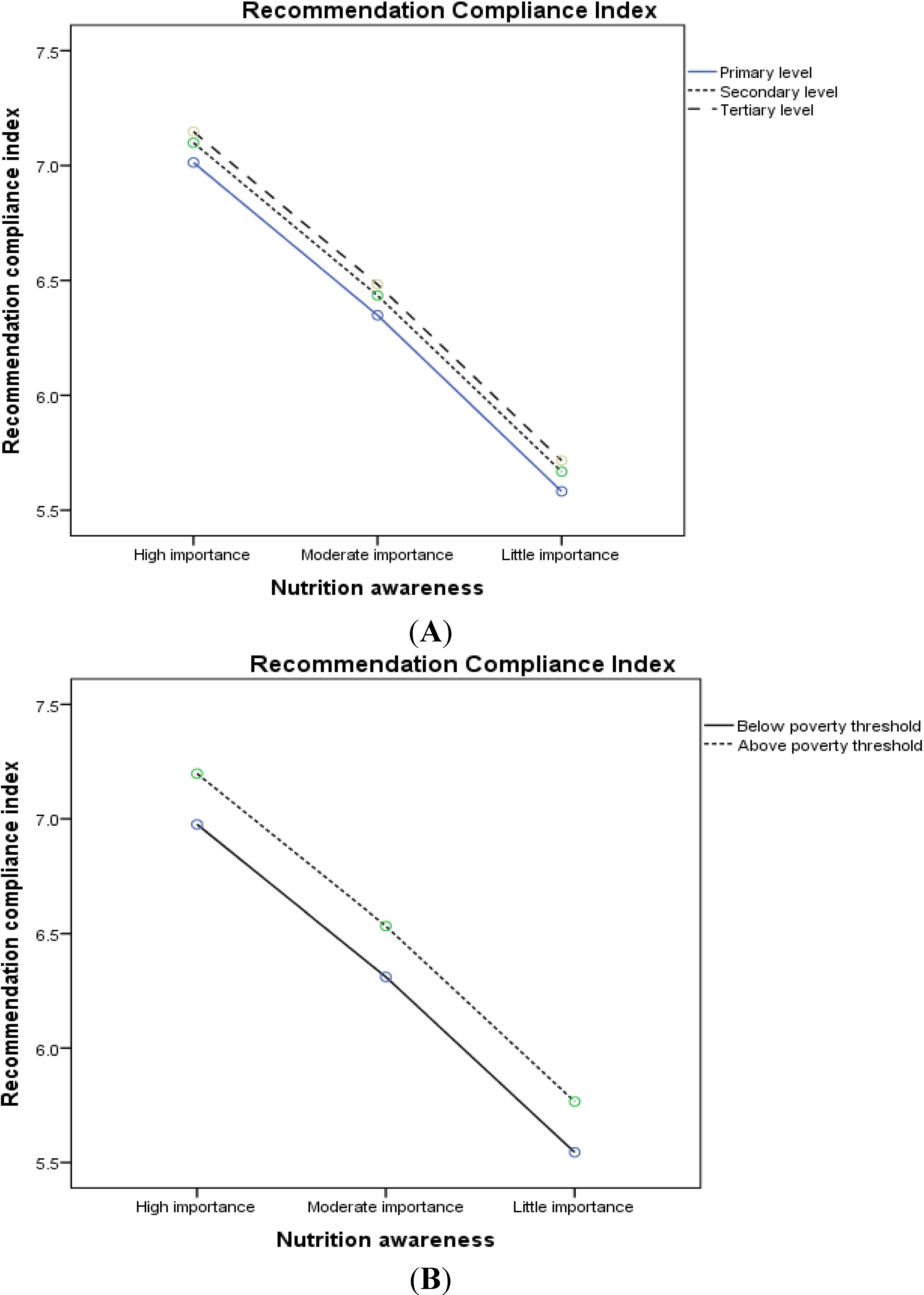
4. Discussion
5. Conclusions
Supplementary Files
Supplementary File 1Acknowledgments
Author Contributions
Conflicts of Interest
References
- WHO. Diet, nutrition and the prevention of chronic diseases: Report of a joint WHO/FAO expert consultation; WHO: Geneva, Switzerland, 2003. [Google Scholar]
- Graham, I.M. Guidelines on cardiovascular disease prevention in clinical practice: The European perspective. Curr. Opin. Cardiol. 2005, 20, 430–439. [Google Scholar] [CrossRef] [PubMed]
- Lin, J.S.; O’Connor, E.; Whitlock, E.P.; Beil, T.L.; Zuber, S.P.; Perdue, L.A.; Plaut, D.; Lutz, K. Behavioral counseling to promote physical activity and a healthful diet to prevent cardiovascular disease in adults: A systematic review for the U.S. Preventive Services Task Force. Ann. Intern Med. 2010, 153, 736–750. [Google Scholar]
- Gaskins, N.D.; Sloane, P.D.; Mitchell, C.M.; Ammerman, A.; Ickes, S.B.; Williams, C.S. Poor nutritional habits: A modifiable predecessor of chronic illness? A North Carolina Family Medicine Research Network (NC-FM-RN) study. J. Am. Board Fam. Med. 2007, 20, 124–134. [Google Scholar]
- Bowman, S.A.; Vinyard, B.T. Fast food consumption of U.S. adults: Impact on energy and nutrient intakes and overweight status. J. Am. Coll. Nutr. 2004, 23, 163–168. [Google Scholar]
- Poti, J.M.; Duffey, K.; Popkin, B.M. The association of fast food consumption with poor dietary outcomes and obesity among children. Am. J. Clin. Nutr. 2014, 4, 162–171. [Google Scholar] [CrossRef]
- Darmon, N.; Drewnowski, A. Does social class predict diet quality? Am. J. Clin. Nutr. 2008, 87, 1107–1117. [Google Scholar] [PubMed]
- Groth, M.V.; Fagt, S.; Brondsted, L. Social determinants of dietary habits in Denmark. Eur. J. Clin. Nutr. 2001, 55, 959–966. [Google Scholar] [CrossRef] [PubMed]
- Franchini, B.; Poinhos, R.; Klepp, K.I.; vaz de Almeida, M.D. Fruit and vegetables: Intake and sociodemographic determinants among Portuguese mothers. Ann. Nutr. Metab. 2013, 63, 131–138. [Google Scholar] [CrossRef] [PubMed]
- Shannon, J.; Shikany, J.M.; Barrett-Connor, E.; Marshall, L.M.; Bunker, C.H.; Chan, J.M.; Stone, K.L.; Orwoll, E.; Osteoporotic Fractures in Men (MrOS) Research Group. Demographic factors associated with the diet quality of older US men: Baseline data from the Osteoporotic Fractures in Men (MrOS) study. Public Health Nutr. 2007, 10, 810–818. [Google Scholar]
- Dallongeville, J.; Marecaux, N.; Cottel, D.; Bingham, A.; Amouyel, P. Association between nutrition knowledge and nutritional intake in middle-aged men from Northern France. Public Health Nutr. 2001, 4, 27–33. [Google Scholar] [CrossRef] [PubMed]
- Gates, G.; McDonald, M. Comparison of dietary risk factors for cardiovascular disease in African-American and white women. J. Am. Diet. Assoc. 1997, 97, 1394–1400. [Google Scholar] [CrossRef] [PubMed]
- Furst, T.; Connors, M.; Bisogni, C.A.; Sobal, J.; Falk, L.W. Food choice: A conceptual model of the process. Appetite 1996, 26, 247–265. [Google Scholar] [CrossRef] [PubMed]
- Paquette, M.C. Perceptions of healthy eating: State of knowledge and research gaps. Can. J. Public Health 2005, 96 (Suppl. 3), S15–S21. [Google Scholar] [PubMed]
- Alkerwi, A.; Sauvageot, N.; Donneau, A.F.; Lair, M.-L.; Couffignal, S.; Beissel, J.; Delagardelle, C.; Wagener, Y.; Albert, A.; Guillaume, M. First nationwide survey on cardiovascular risk factors in Grand-Duchy of Luxembourg (ORISCAV-LUX). BMC Public Health 2010, 10, 468. [Google Scholar] [CrossRef] [PubMed]
- Alkerwi, A.; Sauvageot, N.; Couffignal, S.; Albert, A.; Lair, M.-L.; Guillaume, M. Comparison of participants and non-participants to the ORISCAV-LUX population-based study on cardiovascular risk factors in Luxembourg. BMC Med. Res. Methodol. 2010, 10, 80. [Google Scholar] [CrossRef] [PubMed]
- Alkerwi, A.; Donneau, A.F.; Sauvageot, N.; Lair, M.L.; Albert, A.; Guillaume, M. Dietary, behavioural and socio-economic determinants of the metabolic syndrome among adults in Luxembourg: Findings from the ORISCAV-LUX study. Public Health Nutr. 2012, 15, 849–859. [Google Scholar] [CrossRef] [PubMed]
- Sauvageot, N.; Alkerwi, A.; Albert, A.; Guillaume, M. Use of food frequency questionnaire to assess relationships between dietary habits and cardiovascular risk factors in NESCAV study: Validation with biomarkers. Nutr. J. 2013, 12, 143. [Google Scholar] [CrossRef]
- Sauvageot, N.; Alkerwi, A.; Adelin, A.; Guillaume, M. Validation of the food frequency questionnaire used to assess the association between dietary habits and cardiovascular risk factors in the NESCAV Study. J. Nutr. Food Sci. 2013, 3, 208. [Google Scholar] [CrossRef]
- Fransen, H.P.; Ocke, M.C. Indices of diet quality. Curr. Opin. Clin. Nutr. Metab. Care 2008, 11, 559–565. [Google Scholar] [CrossRef] [PubMed]
- Maillot, M.; Darmon, N.; Vieux, F.; Drewnowski, A. Low energy density and high nutritional quality are each associated with higher diet costs in French adults. Am. J. Clin. Nutr. 2007, 86, 690–696. [Google Scholar] [PubMed]
- Ledikwe, J.H.; Blanck, H.M.; Khan, L.K.; Serdula, M.K.; Seymour, J.D.; Tohill, B.C.; Rolls, B.J. Low-energy-density diets are associated with high diet quality in adults in the United States. J. Am. Diet. Assoc. 2006, 106, 1172–1180. [Google Scholar] [CrossRef] [PubMed]
- Aggarwal, A.; Monsivais, P.; Cook, A.J.; Serdula, M.K.; Seymour, J.D.; Tohill, B.C.; Rolls, B.J. Does diet cost mediate the relation between socioeconomic position and diet quality? Eur. J. Clin. Nutr. 2011, 65, 1059–1066. [Google Scholar] [CrossRef] [PubMed]
- Kim, S.; Haines, P.S.; Siega-Riz, A.M.; Popkin, B.M. The Diet Quality Index-International (DQI-I) provides an effective tool for cross-national comparison of diet quality as illustrated by China and the United States. J. Nutr. 2003, 133, 3476–3484. [Google Scholar] [PubMed]
- Alkerwi, A.; Sauvageot, N.; Nau, A.; Lair, M.L.; Donneau, A.F.; Albert, A.; Guillaume, M. Population compliance with national dietary recommendations and its determinants: Findings from the ORISCAV-LUX study. Br. J. Nutr. 2012, 108, 2083–2092. [Google Scholar] [CrossRef] [PubMed]
- Patterson, R.E.; Haines, P.S.; Popkin, B.M. Diet quality index: Capturing a multidimensional behavior. J. Am. Diet. Assoc. 1994, 94, 57–64. [Google Scholar] [CrossRef] [PubMed]
- Krebs-Smith, S.M.; Smiciklas-Wright, H.; Guthrie, H.A.; Krebs-Smith, J. The effects of variety in food choices on dietary quality. J. Am. Diet. Assoc. 1987, 87, 897–903. [Google Scholar] [PubMed]
- Murphy, S.P.; Foote, J.A.; Wilkens, L.R.; Basiotis, P.P.; Carlson, A.; White, K.K.; Yonemori, K.M. Simple measures of dietary variety are associated with improved dietary quality. J. Am. Diet. Assoc. 2006, 106, 425–429. [Google Scholar] [CrossRef] [PubMed]
- Ruel, M.T. Operationalizing dietary diversity: A review of measurement issues and research priorities. J. Nutr. 2003, 133, 3911S–3926S. [Google Scholar] [PubMed]
- Moursi, M.M.; Arimond, M.; Dewey, K.G.; Trèche, S.; Ruel, M.T.; Delpeuch, F. Dietary diversity is a good predictor of the micronutrient density of the diet of 6- to 23-month-old children in Madagascar. J. Nutr. 2008, 138, 2448–2453. [Google Scholar] [CrossRef] [PubMed]
- Azadbakht, L.; Haghighatdoost, F.; Esmaillzadeh, A. Dietary energy density is inversely associated with the diet quality indices among Iranian young adults. J. Nutr. Sci. Vitaminol. (Tokyo) 2012, 58, 29–35. [Google Scholar] [CrossRef]
- Arimond, M.; Ruel, M.T. Dietary diversity is associated with child nutritional status: Evidence from 11 demographic and health surveys. J. Nutr. 2004, 134, 2579–2585. [Google Scholar] [PubMed]
- Beydoun, M.A.; Wang, Y. Do nutrition knowledge and beliefs modify the association of socio-economic factors and diet quality among US adults? Prev. Med. 2008, 46, 145–153. [Google Scholar] [CrossRef] [PubMed]
- McLeod, E.R.; Campbell, K.J.; Hesketh, K.D. Nutrition knowledge: A mediator between socioeconomic position and diet quality in Australian first-time mothers. J. Am. Diet. Assoc. 2011, 111, 696–704. [Google Scholar] [CrossRef] [PubMed]
- Marmot, M.; Friel, S.; Bell, R.; Houweling, T.A.; Taylor, S.; Commission on Social Determinants of Health. Closing the gap in a generation: Health equity through action on the social determinants of health. Lancet 2008, 372, 1661–1669. [Google Scholar]
- Spronk, I.; Kullen, C.; Burdon, C.; O’Connor, H. Relationship between nutrition knowledge and dietary intake. Br. J. Nutr. 2014, 111, 1713–1726. [Google Scholar] [CrossRef] [PubMed]
- Drewnowski, A.; Specter, S.E. Poverty and obesity: The role of energy density and energy costs. Am. J. Clin. Nutr. 2004, 79, 6–16. [Google Scholar] [PubMed]
- Darmon, N.; Briend, A.; Drewnowski, A. Energy-dense diets are associated with lower diet costs: A community study of French adults. Public Health Nutr. 2004, 7, 21–27. [Google Scholar] [CrossRef] [PubMed]
- Kristal, A.R.; Peters, U.; Potter, J.D. Is it time to abandon the food frequency questionnaire? Cancer Epidemiol. Biomark. Prev. 2005, 14, 2826–2828. [Google Scholar] [CrossRef]
- Schatzkin, A.; Kipnis, V.; Carroll, R.J.; Midthune, D.; Subar, A.F.; Bingham, S.; Schoeller, D.A.; Troiano, R.P.; Freedman, L.S. A comparison of a food frequency questionnaire with a 24-hour recall for use in an epidemiological cohort study: Results from the biomarker-based Observing Protein and Energy Nutrition (OPEN) study. Int. J. Epidemiol. 2003, 32, 1054–1062. [Google Scholar] [CrossRef] [PubMed]
- Hebert, J.R.; Clemow, L.; Pbert, L.; Ockene, I.S.; Ockene, J.K. Social desirability bias in dietary self-report may compromise the validity of dietary intake measures. Int. J. Epidemiol. 1995, 24, 389–398. [Google Scholar] [CrossRef] [PubMed]
© 2015 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Alkerwi, A.; Sauvageot, N.; Malan, L.; Shivappa, N.; Hébert, J.R. Association between Nutritional Awareness and Diet Quality: Evidence from the Observation of Cardiovascular Risk Factors in Luxembourg (ORISCAV-LUX) Study. Nutrients 2015, 7, 2823-2838. https://doi.org/10.3390/nu7042823
Alkerwi A, Sauvageot N, Malan L, Shivappa N, Hébert JR. Association between Nutritional Awareness and Diet Quality: Evidence from the Observation of Cardiovascular Risk Factors in Luxembourg (ORISCAV-LUX) Study. Nutrients. 2015; 7(4):2823-2838. https://doi.org/10.3390/nu7042823
Chicago/Turabian StyleAlkerwi, Ala'a, Nicolas Sauvageot, Leoné Malan, Nitin Shivappa, and James R. Hébert. 2015. "Association between Nutritional Awareness and Diet Quality: Evidence from the Observation of Cardiovascular Risk Factors in Luxembourg (ORISCAV-LUX) Study" Nutrients 7, no. 4: 2823-2838. https://doi.org/10.3390/nu7042823
APA StyleAlkerwi, A., Sauvageot, N., Malan, L., Shivappa, N., & Hébert, J. R. (2015). Association between Nutritional Awareness and Diet Quality: Evidence from the Observation of Cardiovascular Risk Factors in Luxembourg (ORISCAV-LUX) Study. Nutrients, 7(4), 2823-2838. https://doi.org/10.3390/nu7042823





