A Randomized Controlled Trial Investigating the Effects of a Special Extract of Bacopa monnieri (CDRI 08) on Hyperactivity and Inattention in Male Children and Adolescents: BACHI Study Protocol (ANZCTRN12612000827831)
Abstract
:1. Introduction
1.1. Background & Rationale
1.2. What is the Significance of Clinical and Sub-Clinical Symptoms of ADHD?
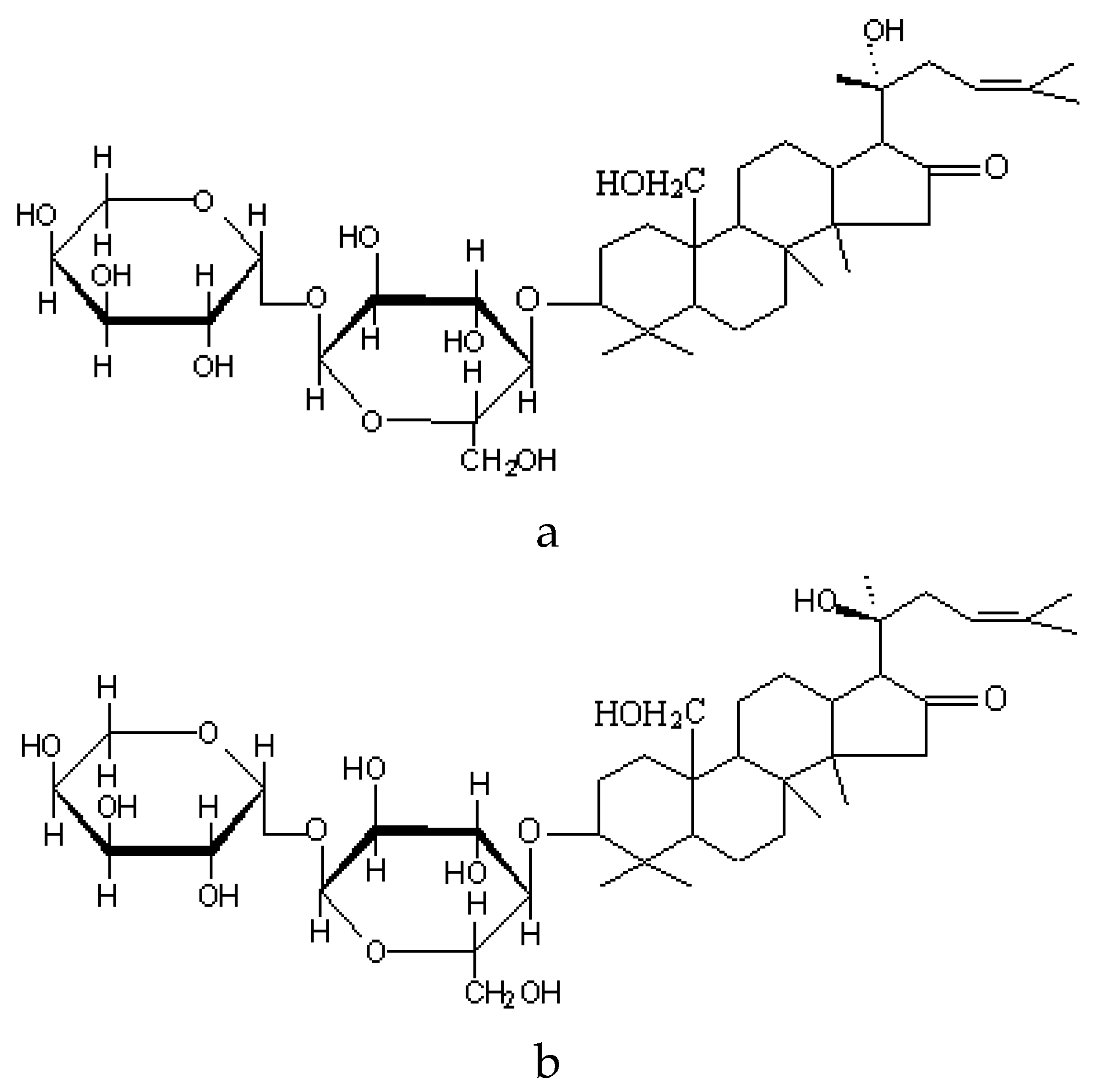
1.3. Bacopa Monnieri (“Brahmi”)
1.4. CDRI 08
2. Experimental Section
2.1. Design
2.2. Study Aims and Hypotheses
2.3. Participants
2.4. Centre
2.5. Procedure
| Behavioural, Demographic & Genetic Measures | V1 Screening Weeks 0 | V2 Baseline Weeks 1 | V3 Follow-up 1 Weeks 8 | V4 Follow-up 2 Weeks 15 | V5 Final Visit Weeks 16 |
| Administer 1 week dose of placebo to all participants | Give randomized treatment | Continue to take randomized treatment | Give 1 week placebo run out | Return any remaining capsules | |
| Structured interview (DSM ADHD rating) | X | ||||
| Wechsler Intelligence Scale for Children Short Form (4th Revision) | X | ||||
| Conners’ Parent Rating Scale | X | X | X | X | X |
| Global Clinical Impression Scale | X | X | X | ||
| Current Health & Medical Questionnaire | X | X | X | X | X |
| Demographics Questionnaire | X | ||||
| OraGene Genetic Sample | X | ||||
| Cognitive & Mood Measures | V1 Practice Week 0 | V2 Baseline Week 1 | V3 Follow-up 1 Weeks 8 | V4 Follow-up 2 Weeks 15 | V5 Final Visit Weeks 16 |
| Neurophysiology (EEG) resting states | X | X | X | ||
| CNS Vital Signs (CNSVS) | X | X | X | X | X |
| Test of Variables of Attention (TOVA) | X | X | X | X | X |
| Hick Reaction Time Paradigm (Jensen’s Box) | X | X | X | X | X |
| Child Depression Inventory (CDI) | X | X | X | X | X |
| Paediatric Sleep Problems Survey Instrument (PSPSI) | X | X | X | X | X |
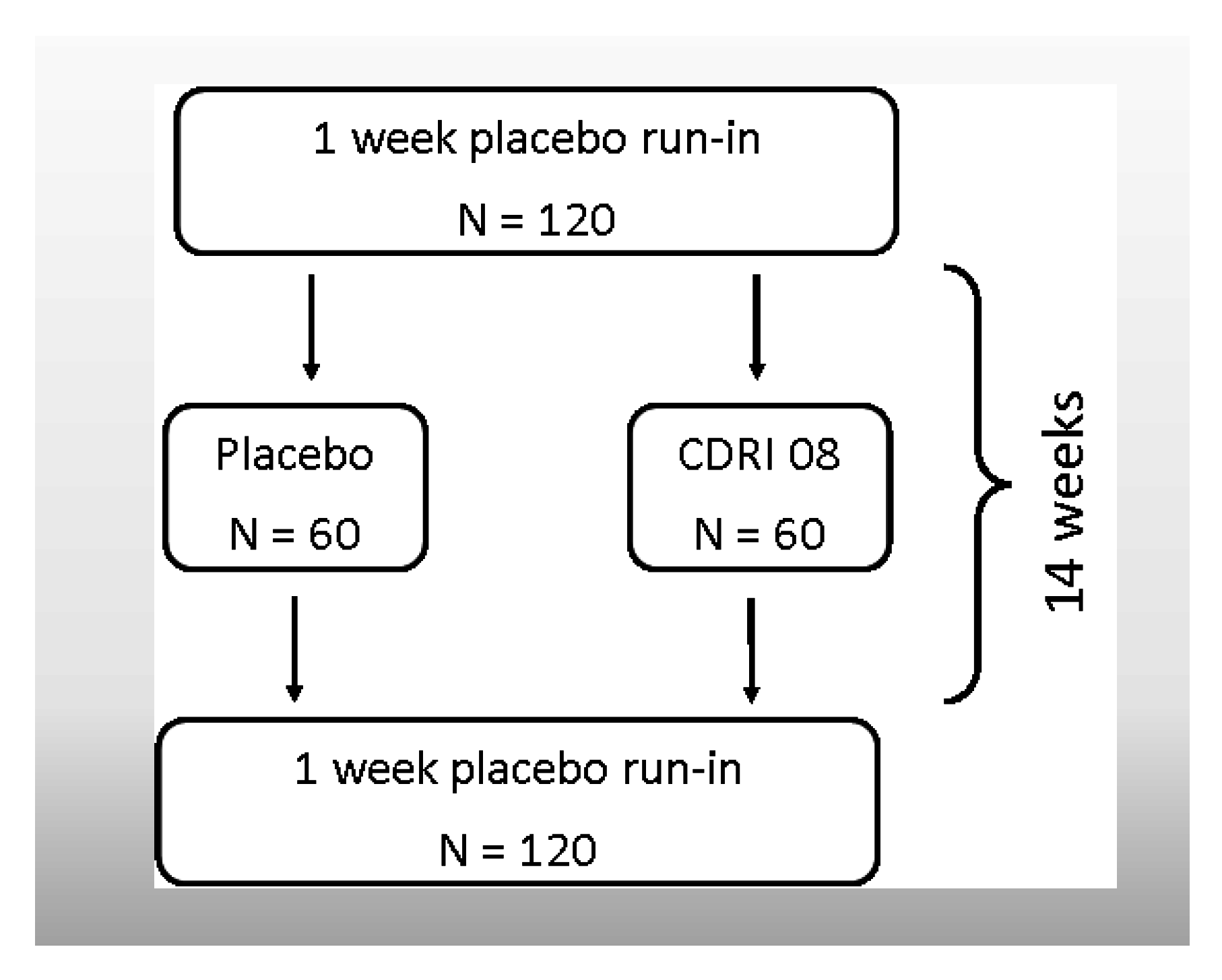
2.6. Randomization & Blinding
2.7. Primary Outcome
2.8. Secondary Outcomes
2.8.1. Cognition
| CNSVS | TOVA | Jensen Box |
|---|---|---|
| Verbal Memory Test | Errors of omission (attention) | Simple Decision Time |
| Visual Memory Test | Errors of commission (inhibition) | Simple Movement Time |
| Finger Tapping Test | Response Time | 2 Choice Decision Time |
| Symbol Digit Coding | 2 Choice Movement Time | |
| Stroop Paradigm | 4 Choice Decision Time | |
| Shifting Attention Test | 4 Choice Movement Time | |
| Continuous Performance Test | 8 Choice Decision Time | |
| Verbal Memory Test 2 | 8 Choice Movement Time | |
| Visual Memory Test 2 | ||
| Paediatric Symptom Checklist |
2.8.2. Mood
2.8.3. Sleep
2.8.4. Global Clinical Impression Scale (GCI)
2.8.5. Neurophysiology (EEG Resting States)
2.8.6. Genetic Material (OraGene Saliva Kits)
2.8.7. Wechsler Intelligence Scale for Children Short Form (WISC-IV-SF)
2.8.8. Compliance, Health & Medical Assessments
2.9. Power Analysis
2.10. Statistical Analysis
3. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Palmer, E.D.; Finger, S. An early description of adhd (inattentive subtype): Dr alexander crichton and “mental restlessness“ (1798). Child Adolesc. Ment. Health 2001, 6, 66–73. [Google Scholar] [CrossRef]
- Lange, K.; Reichl, S.; Lange, K.; Tucha, L.; Tucha, O. The history of attention deficit hyperactivity disorder. ADHD Atten. Deficit Hyperact. Disord. 2010, 2, 241–255. [Google Scholar] [CrossRef] [PubMed]
- Goldman, L.S.; Genel, M.; Bezman, R.J.; Slanetz, P.J.; Karlan, M.S.; Davis, R.M.; Altman, R.D.; Deitchman, S.D.; Howe, J.P., III; Nielsen, N.H.; et al. Diagnosis and treatment of attention-deficit/hyperactivity disorder in children and adolescents. J. Am. Med. Assoc. 1998, 279, 1100–1107. [Google Scholar] [CrossRef]
- Biederman, J. Attention-deficit/hyperactivity disorder: A selective overview. Biol. Psychiatry 2005, 57, 1215–1220. [Google Scholar] [CrossRef] [PubMed]
- Wolraich, M.L. Attention deficit hyperactivity disorder: The most studied and yet most controversial diagnosis. Ment. Retard. Dev. Disabil. Res. Rev. 1999, 5, 163–168. [Google Scholar] [CrossRef]
- Smelter, R.W.; Rasch, B.W.; Fleming, J.; Nazos, P.; Baranowski, S. Is attention deficit disorder becoming a desired diagnosis? Phi Delta Kappan 1996, 78, 429–432. [Google Scholar]
- Sciutto, M.J.; Eisenberg, M. Evaluating the evidence for and against the overdiagnosis of ADHD. J. Atten. Disord. 2007, 11, 106–113. [Google Scholar] [CrossRef] [PubMed]
- Bruchmüller, K.; Margraf, J.; Schneider, S. Is adhd diagnosed in accord with diagnostic criteria? Overdiagnosis and influence of client gender on diagnosis. J. Consult. Clin. Psychol. 2012, 80, 128–138. [Google Scholar] [CrossRef] [PubMed]
- Cotuono, A.J. The diagnosis of attention deficit hyperactivity disorder (ADHD) in community mental health centers: Where and when. Psychol. Sch. 1993, 30, 338–344. [Google Scholar] [CrossRef]
- Meijer, W.M.; Faber, A.; Van Den Ban, E.; Tobi, H. Current issues around the pharmacotherapy of ADHD in children and adults. Pharm. World Sci. 2009, 31, 509–516. [Google Scholar] [CrossRef] [PubMed]
- McNamara, R.K.; Carlson, S.E. Role of omega-3 fatty acids in brain development and function: Potential implications for the pathogenesis and prevention of psychopathology. Prostaglandins Leukot. Essent. Fatty Acids 2006, 75, 329–349. [Google Scholar] [CrossRef] [PubMed]
- Miller, E.K.; Cohen, J.D. An integrative theory of prefrontal cortex function. Annu. Rev. Neurosci. 2001, 24, 167–202. [Google Scholar] [CrossRef] [PubMed]
- McGough, J.J.; McCracken, J.T.; Loo, S.K.; Manganiello, M.; Leung, M.C.; Tietjens, J.R.; Trinh, T.; Baweja, S.; Suddath, R.; Smalley, S.L.; et al. A candidate gene analysis of methylphenidate response in attention-deficit/hyperactivity disorder. J. Am. Acad. Child Adolesc. Psychiatry 2009, 48, 1155–1164. [Google Scholar] [CrossRef] [PubMed]
- Schweren, L.J.; de Zeeuw, P.; Durston, S. MR imaging of the effects of methylphenidate on brain structure and function in attention-deficit/hyperactivity disorder. Eur. Neuropsychopharmacol. 2013, 23, 1151–1164. [Google Scholar] [CrossRef] [PubMed]
- Adler, L.D.; Nierenberg, A.A. Review of medication adherence in children and adults with ADHD. Postgrad. Med. 2010, 122, 184–191. [Google Scholar] [CrossRef] [PubMed]
- Rucklidge, J.J.; Johnstone, J.; Kaplan, B.J. Nutrient supplementation approaches in the treatment of ADHD. Expert Rev. Neurother. 2009, 9, 461–476. [Google Scholar] [CrossRef] [PubMed]
- Pataki, C.S.; Carlson, G.A.; Kelly, K.L.; Rapport, M.D.; Biancaniello, T.M. Side effects of methylphenidate and desipramine alone and in combination in children. J. Am. Acad. Child Adolesc. Psychiatry 1993, 32, 1065–1072. [Google Scholar] [CrossRef] [PubMed]
- Sarris, J.; Kean, J.; Schweitzer, I.; Lake, J. Complementary medicines (herbal and nutritional products) in the treatment of attention deficit hyperactivity disorder (ADHD): A systematic review of the evidence. Complement. Ther. Med. 2011, 19, 216–227. [Google Scholar] [CrossRef] [PubMed]
- Chan, E. The role of complementary and alternative medicine in attention-deficit hyperactivity disorder. Dev. Behav. Pediatry 2002, 23, S37–S45. [Google Scholar] [CrossRef]
- American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders dsm-iv-tr, 4th ed.; American Psychiatric Publishing: Washington, DC, USA, 2000. [Google Scholar]
- Wolraich, M.L.; Wibbelsman, C.J.; Brown, T.E.; Evans, S.W.; Gotlieb, E.M.; Knight, J.R.; Ross, E.C.; Shubiner, H.H.; Wender, E.H.; Wilens, T. Attention-deficit/hyperactivity disorder among adolescents: A review of the diagnosis, treatment, and clinical implications. Pediatrics 2005, 115, 1734–1746. [Google Scholar] [CrossRef] [PubMed]
- Biederman, J.; Faraone, S.V. Attention-deficit hyperactivity disorder. Lancet 2005, 366, 237–248. [Google Scholar] [CrossRef]
- American Psychiatric, A.; American Psychiatric, A.; Force, D.S.M.T. Diagnostic and Statistical Manual of Mental Disorders: DSM-5. Available online: http://dsm.psychiatryonline.org/book.aspx?bookid=556 (accessed on 13 May 2015).
- Chabot, R.J.; Serfontein, G. Quantitative electroencephalographic profiles of children with attention deficit disorder. Biol. Psychiatry 1996, 40, 951–963. [Google Scholar] [CrossRef]
- Clarke, A.R.; Barry, R.J.; McCarthy, R.; Selikowitz, M. Electroencephalogram differences in two subtypes of attention-deficit/hyperactivity disorder. Psychophysiology 2001, 38, 212–221. [Google Scholar] [CrossRef] [PubMed]
- Lazzaro, I.; Gordon, E.; Whitmont, S.; Plahn, M.; Li, W.; Clarke, S.; Dosen, A.; Meares, R. Quantified eeg activity in adolescent attention deficit hyperactivity disorder. Clin. EEG Electroencephalogr. 1998, 29, 37–42. [Google Scholar] [CrossRef]
- Chabot, R.J.; di Michele, F.; Prichep, L. The role of quantitative electroencephalography in child and adolescent psychiatric disorders. Child Adolesc. Psychiatry Clin. N. Am. 2005, 14, 21–53. [Google Scholar] [CrossRef] [PubMed]
- Chabot, R.J.; di Michele, F.; Prichep, L.; John, E.R. The clinical role of computerized eeg in the evaluation and treatment of learning and attention disorders in children and adolescents. J. Neuropsychiatry Clin. Neurosci. 2001, 13, 171–186. [Google Scholar] [CrossRef] [PubMed]
- El-Sayed, E.; Larsson, J.O.; Persson, H.E.; Santosh, P.J.; Rydelius, P.A. “Maturational lag“ hypothesis of attention deficit hyperactivity disorder: An update. Acta Paediatr. Int. J. Paediatry 2003, 92, 776–784. [Google Scholar] [CrossRef]
- Chabot, R.J.; Merkin, H.; Wood, L.M.; Davenport, T.L.; Serfontein, G. Sensitivity and specificity of qeeg in children with attention deficit or specific developmental learning disorders. Clin. EEG Electroencephalogr. 1996, 27, 26–33. [Google Scholar] [CrossRef]
- Surwillo, W.W. Changes in the electroencephalogram accompanying the use of stimulant drugs (methylphenidate and dextroamphetamine) in hyperactive children. Biol. Psychiatr. 1977, 12, 787–799. [Google Scholar]
- Bertha, E.; Balázs, J. Subthreshold depression in adolescence: A systematic review. Eur. Child Adolesc. Psychiatry 2013, 22, 589–603. [Google Scholar] [CrossRef] [PubMed]
- Balázs, J.; Keresztény, Á. Subthreshold attention deficit hyperactivity in children and adolescents: A systematic review. Eur. Child Adolesc. Psychiatry 2014, 23, 393–408. [Google Scholar] [CrossRef] [PubMed]
- Gohil, K.J.; Patel, J.J. A review on bacopa monniera: Current research and future prospects. Int. J. Green Pharm. 2010, 4, 1–9. [Google Scholar] [CrossRef]
- Russo, A.; Borrelli, F. Bacopa monniera, a reputed nootropic plant: An overview. Phytomedicine 2005, 12, 305–317. [Google Scholar] [CrossRef] [PubMed]
- Malhotra, C.L.; Das, P.K. Pharmacological studies of herpestis monniera, Linn., (Brahmi). Indian J. Med. Res. 1959, 47, 294–305. [Google Scholar] [PubMed]
- Singh, H.K.; Dhawan, B.N. Neuropsychopharmacological effects of the ayurvedic nootropic bacopa monniera Linn.(Brahmi). Indian J. Pharmacol. 1997, 29, S359–S365. [Google Scholar]
- Bacopin. Chemical Constituents. Available online: http://bacopin.com/chemical.htm (accessed on 18 March 2015).
- Singh, H.K.; Rastogi, R.P.; Srimal, R.C.; Dhawan, B.N. Effect of bacosides a and b on avoidance responses in rats. Phytother. Res. 1988, 2, 70–75. [Google Scholar] [CrossRef]
- Uabundit, N.; Wattanathorn, J.; Mucimapura, S.; Ingkaninan, K. Cognitive enhancement and neuroprotective effects of bacopa monnieri in Alzheimer’s disease model. J. Ethnopharmacol. 2010, 127, 26–31. [Google Scholar] [CrossRef] [PubMed]
- Bhattacharya, S.K.; Kumar, A.; Ghosal, S. Effect of bacopa monniera on animal models of alzheimer’s disease and perturbed central cholinergic markers of cognition in rats. Res. Commun. Pharmacol. Toxicol. 1999, 4, 1–12. [Google Scholar]
- Holcomb, L.A.; Dhanasekaran, M.; Hitt, A.R. Bacopa monniera extract reduces amyloid levels in PSAPP mice. J. Alzheimer's Disease 2006, 9, 243–251. [Google Scholar]
- Bhattacharya, S.K.; Bhattacharya, A.; Kumar, A.; Ghosal, S. Antioxidant activity of bacopa monniera in rat frontal cortex, striatum and hippocampus. Phytother. Res. 2000, 14, 174–179. [Google Scholar] [CrossRef]
- Russo, A.; Izzo, A.A.; Borrelli, F. Free radical scavenging capacity and protective effect of bacopa monniera L. On DNA damage. Phytother. Res. 2003, 17, 870–875. [Google Scholar] [CrossRef] [PubMed]
- Kapoor, R.; Srivastava, S.; Kakkar, P. Bacopa monnieri modulates antioxidant responses in brain and kidney of diabetic rats. Environ. Toxicol. Pharmacol. 2009, 27, 62–69. [Google Scholar] [CrossRef] [PubMed]
- Dhanasekaran, M.; Tharakan, B.; Holcomb, L.A. Neuroprotective mechanisms of ayurvedic antidementia botanical bacopa monniera. Phytother. Res. 2007, 21, 965–969. [Google Scholar] [CrossRef] [PubMed]
- Stough, C.; Lloyd, J.; Clarke, J.; Downey, L.A.; Hutchison, C.W.; Rodgers, T.; Nathan, P.J. The chronic effects of an extract of bacopa monniera (Brahmi) on cognitive function in healthy human subjects. Psychopharmacology 2001, 156, 481–484. [Google Scholar] [CrossRef] [PubMed]
- Nathan, P.J.; Tanner, S.; Lloyd, J.; Harrison, B.; Curran, L.; Oliver, C.; Stough, C. Effects of a combined extract of ginkgo biloba and bacopa monniera on cognitive function in healthy humans. Hum. Psychopharmacol. 2004, 19, 91–96. [Google Scholar] [CrossRef] [PubMed]
- Stough, C.; Downey, L.A.; Lloyd, J. Examining the nootropic effects of a special extract of bacopa monniera on human cognitive functioning: 90 day double-blind placebo-contrlled randomized trial. Phytother. Res. 2008, 22, 1629–1634. [Google Scholar] [CrossRef] [PubMed]
- Pase, M.P.; Kean, J.; Sarris, J.; Neale, C.; Scholey, A.B.; Stough, C. The cognitive-enhancing effects of bacopa monnieri: A systematic review of randomized, controlled human clinical trials. J. Altern. Complement. Med. 2012, 18, 647–652. [Google Scholar] [CrossRef] [PubMed]
- Morgan, A.; Stevens, J. Does bacopa monnieri improve memory performance in older persons? Results of a randomized, placebo-controlled, double-blind trial. J. Altern. Complement. Med. 2010, 16, 753–759. [Google Scholar] [CrossRef] [PubMed]
- Sharma, R.; Chaturvedi, C.; Tewari, P.V. Efficacy of bacopa monnieri in revitalizing intellectual functions in children. J. Res. Educ. Indian Med. 1987, 1, 1–12. [Google Scholar]
- Kalra, V.; Zamir, H.; Pandey, R.M.; Kulkarni, K.S. A randomized double blind placebo-controlled drug trial with mentat in children with attention deficit hyperactivity disorder. Neurosci. Today 2002, 6, 223–227. [Google Scholar]
- Dave, U.; Chauvan, V.; Dalvi, J. Evaluation of BR-16 A (mentat) in cognitive and behavioural dysfunction of mentally retarded children—A placebo-controlled study (study ii). Indian J. Pediatr. 1993, 60, 423–428. [Google Scholar] [CrossRef] [PubMed]
- Jauhari, N.; Singh, Y.D.; Kushwaha, K.P.; Rastogi, C.K.; Asthana, O.P.; Srivastava, J.S.; Rathi, A.K. Clinical evaluation of bacopa monniera extract on behavioural and cognitive functions in children suffering from attention deficit hyperactivity disorder. Central Drug Research Institute (CDRI): Varanasi, India, 2001; in press. [Google Scholar]
- Negi, K.; Singh, Y.; Kushwaha, K.; Rastogi, C.; Rathi, A.; Srivastava, J.; Asthana, O.; Gupta, R. Clinical evaluation of memory enhancing properties of memory plus in children with attention deficit hyperactivity disorder. Indian J. Psychiatry 2000, 42, 2. [Google Scholar]
- United Nations Office for South-South Cooperation. U. Memory enhancer: Bacopa monniera standardized fraction. In Volume 10: Examples of the Development of Pharmaceutical Products from Medicinal Plants; United Nations Office for South-South Cooperation: Lucknow, India, 2003; pp. 29–44. [Google Scholar]
- Maurya, R.; Gupta, C.M. Traditional herbs for modern medicine. Tech. Monitor 2006, 43, 23–36. [Google Scholar]
- Downey, L.A.; Kean, J.; Nemeh, F.; Lau, A.; Poll, A.; Gregory, R.; Murray, M.; Rourke, J.; Patak, B.; Pase, M.; et al. An acute, double-blind, placebo-controlled crossover study of 320 mg and 640 mg doses of a special extract of bacopa monnieri (CDRI 08) on sustained cognitive performance. Phytother. Res. 2013, 27, 1407–1413. [Google Scholar] [CrossRef] [PubMed]
- Conners, C.K.; Sitarenios, G.; Parker, J.D.A.; Epstein, J.N. The revised conners’ parent rating scale (CPRS-R): Factor structure, reliability, and criterion validity. J. Abnorm. Child Psychol. 1998, 26, 257–268. [Google Scholar] [CrossRef] [PubMed]
- Conners, C.K. A teacher rating scale for use in drug studies with children. Am. J. Psychiatry 1969, 126, 884–888. [Google Scholar] [CrossRef] [PubMed]
- Conners, C.K. Symptom patterns in hyperkinetic, neurotic, and normal children. Child Dev. 1970, 41, 667–682. [Google Scholar] [CrossRef]
- Gualtieri, C.T.; Johnson, L.G. Reliability and validity of a computerized neurocognitive test battery, CNS vital signs. Arch. Clin. Neuropsychol. 2006, 21, 623–643. [Google Scholar] [CrossRef] [PubMed]
- Wada, N.; Yamashita, Y.; Matsuishi, T.; Ohtani, Y.; Kato, H. The test of variables of attention (TOVA) is useful in the diagnosis of Japanese male children with attention deficit hyperactivity disorder. Brain Dev. 2000, 22, 378–382. [Google Scholar] [CrossRef]
- Llorente, A.M.; Voigt, R.; Jensen, C.L.; Fraley, J.K.; Heird, W.C.; Rennie, K.M. The test of variables of attention (TOVA): Internal consistency (q 1 vs. Q2 and q3 vs. Q4) in children with attention deficit/hyperactivity disorder (ADHD). Child Neuropsychol. 2008, 14, 314–322. [Google Scholar] [CrossRef] [PubMed]
- Jensen, A.R. Individual differences in the hick paradigm. In Speed of Information-Processing and Intelligence; Ablex Publishing Corporation: Norwood, NJ, USA, 1987; p. 74. [Google Scholar]
- Helsel, W.J.; Matson, J.L. The assessment of depression in children: The internal structure of the child depression inventory (cdi). Behav. Res. Ther. 1984, 22, 289–298. [Google Scholar] [CrossRef]
- Kovacs, M. The children’s depression, inventory (CDI). Psychopharmacol. Bull. 1985, 21, 995–998. [Google Scholar] [PubMed]
- Smucker, M.; Craighead, W.E.; Craighead, L.; Green, B. Normative and reliability data for the children’s depression inventory. J. Abnorm. Child Psychol. 1986, 14, 25–39. [Google Scholar] [CrossRef] [PubMed]
- Biggs, S.N.; Kennedy, J.D.; Martin, A.J.; van den Heuvel, C.J.; Lushington, K. Psychometric properties of an omnibus sleep problems questionnaire for school-aged children. Sleep Med. 2012, 13, 390–395. [Google Scholar] [CrossRef] [PubMed]
- Busner, J.; Targum, S.D. The clinical global impressions scale: Applying a research tool in clinical practice. Psychiatry (Edgmont) 2007, 4, 28–37. [Google Scholar] [PubMed]
- Barry, R.J.; Clarke, A.R.; Johnstone, S.J.; McCarthy, R.; Selikowitz, M. Electroencephalogram î¸/î² ratio and arousal in attention-deficit/hyperactivity disorder: Evidence of independent processes. Biol. Psychiatry 2009, 66, 398–401. [Google Scholar] [CrossRef] [PubMed]
- Loo, S.K.; Barkley, R.A. Clinical utility of eeg in attention deficit hyperactivity disorder. Appl. Neuropsychol. 2005, 12, 64–76. [Google Scholar] [CrossRef] [PubMed]
- Barry, R.J.; Clarke, A.R.; Johnstone, S.J.; Oades, R.D. Electrophysiology in attention-deficit/hyperactivity disorder. Int. J. Psychophysiol. 2005, 58, 1–3. [Google Scholar] [CrossRef] [PubMed]
- Clarke, A.R.; Barry, R.J.; Dupuy, F.E.; Heckel, L.D.; McCarthy, R.; Selikowitz, M.; Johnstone, S.J. Behavioural differences between eeg-defined subgroups of children with attention-deficit/hyperactivity disorder. Clin. Neurophysiol. 2011, 122, 1333–1341. [Google Scholar] [CrossRef] [PubMed]
- Clarke, A.R.; Barry, R.J.; Dupuy, F.E.; McCarthy, R.; Selikowitz, M.; Heaven, P.C.L. Childhood eeg as a predictor of adult attention-deficit/hyperactivity disorder. Clin. Neurophysiol. 2011, 122, 73–80. [Google Scholar] [CrossRef] [PubMed]
- Clarke, A.R.; Barry, R.J.; McCarthy, R.; Selikowitz, M. Age and sex effects in the eeg: Differences in two subtypes of attention-deficit/hyperactivity disorder. Clin. Neurophysiol. 2001, 112, 815–826. [Google Scholar] [CrossRef]
- Rogers, N.L.; Cole, S.A.; Lan, H.-C.; Crossa, A.; Demerath, E.W. New saliva DNA collection method compared to buccal cell collection techniques for epidemiological studies. Am. J. Hum. Biol. 2007, 19, 319–326. [Google Scholar] [CrossRef] [PubMed]
- Iwasiow, R.M.; Desbois, A.; Birnboim, H.C. Long-Term Stability of DNA from Saliva Samples Stored in the Oragene® Self-Collection Kit; DNA Genotek: Ottawa, ON, Canada, 2011. [Google Scholar]
- Slopien, A.; Dmitrzak-Weglarz, M.; Rybakowski, F.; Rajewski, A.; Hauser, J. Genetic background of ADHD: Population studies, genes of the catecholamine system. Psychiatr. Polska 2006, 40, 19–31. [Google Scholar]
- Das, A.; Shanker, G.; Nath, C.; Pal, R.; Singh, S.; Singh, H. A comparative study in rodents of standardized extracts of bacopa monniera and ginkgo biloba: Anticholinesterase and cognitive enhancing activities. Pharmacol. Biochem. Behav. 2002, 73, 893–900. [Google Scholar] [CrossRef]
- Wechsler, D. Wechsler Intelligence Scale for Children, Manual; The Psychological Corp.: Oxford, UK, 1949; p. 113. [Google Scholar]
- Dave, U.P.; Wasim, P.; Joshua, J.; Geetharani, P.; Murali, B.; Mayachari, A.; Venkateshwarlu, K.; Saxena, V.; Deepak, M.; Amit, A. Bacomind®: A cognitive enhancer in children requiring individual education programme. J. Pharmacol. Toxicol. 2008, 3, 302–310. [Google Scholar]
- Setlik, J.; Bond, G.R.; Ho, M. Adolescent prescription adhd medication abuse is rising along with prescriptions for these medications. Pediatrics 2009, 124, 875–880. [Google Scholar] [CrossRef] [PubMed]
© 2015 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons by Attribution (CC-BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Kean, J.D.; Kaufman, J.; Lomas, J.; Goh, A.; White, D.; Simpson, D.; Scholey, A.; Singh, H.; Sarris, J.; Zangara, A.; et al. A Randomized Controlled Trial Investigating the Effects of a Special Extract of Bacopa monnieri (CDRI 08) on Hyperactivity and Inattention in Male Children and Adolescents: BACHI Study Protocol (ANZCTRN12612000827831). Nutrients 2015, 7, 9931-9945. https://doi.org/10.3390/nu7125507
Kean JD, Kaufman J, Lomas J, Goh A, White D, Simpson D, Scholey A, Singh H, Sarris J, Zangara A, et al. A Randomized Controlled Trial Investigating the Effects of a Special Extract of Bacopa monnieri (CDRI 08) on Hyperactivity and Inattention in Male Children and Adolescents: BACHI Study Protocol (ANZCTRN12612000827831). Nutrients. 2015; 7(12):9931-9945. https://doi.org/10.3390/nu7125507
Chicago/Turabian StyleKean, James D., Jordy Kaufman, Justine Lomas, Antionette Goh, David White, David Simpson, Andrew Scholey, Hemant Singh, Jerome Sarris, Andrea Zangara, and et al. 2015. "A Randomized Controlled Trial Investigating the Effects of a Special Extract of Bacopa monnieri (CDRI 08) on Hyperactivity and Inattention in Male Children and Adolescents: BACHI Study Protocol (ANZCTRN12612000827831)" Nutrients 7, no. 12: 9931-9945. https://doi.org/10.3390/nu7125507
APA StyleKean, J. D., Kaufman, J., Lomas, J., Goh, A., White, D., Simpson, D., Scholey, A., Singh, H., Sarris, J., Zangara, A., & Stough, C. (2015). A Randomized Controlled Trial Investigating the Effects of a Special Extract of Bacopa monnieri (CDRI 08) on Hyperactivity and Inattention in Male Children and Adolescents: BACHI Study Protocol (ANZCTRN12612000827831). Nutrients, 7(12), 9931-9945. https://doi.org/10.3390/nu7125507