The Nutrition Transition in Africa: Can It Be Steered into a More Positive Direction?
Abstract
:1. Introduction: The Problem and Objectives of This Narrative Review
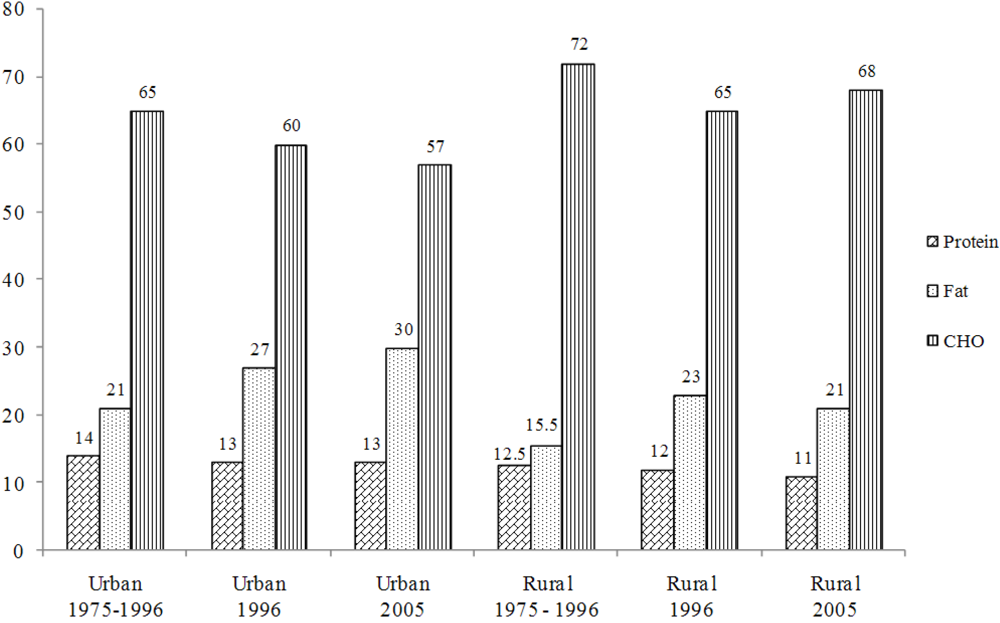
2. The Nutrition Transition in Africa
| Nutrient (unit) Recommended intake (INL98) * | Rural women; Living in deep rural areas | Rural women; From farms | Women living in informal settlements | Urban middle class women | Urban upper class women |
|---|---|---|---|---|---|
| N = 290 | N = 148 | N = 172 | N = 292 | N = 105 | |
| Calcium (mg) | 384 (14) | 418 (20) | 387 (18) | 408 (14) | 512 (23) |
| INL98 = 800 | |||||
| Zinc (mg) | 7.8 (0.2) | 7.1 (0.3) | 7.6 (0.3) | 8.2 (0.2) | 10.6 (0.3) |
| INL98 = 12 | |||||
| Iron (mg) | 8.4 (0.2) | 7.5 (0.3) | 8.3 (0.2) | 10.4 (0.4) | 10.4 (0.4) |
| INL98 = 18 | |||||
| Vit ** A (RE) | 573 (40) | 533 (56) | 773 (82) | 892 (40) | 1248 (86) |
| INL98 = 800 | |||||
| Vit C (mg) | 30 (2) | 25 (3) | 32 (3) | 43 (2) | 83 (4) |
| INL98 = 60 |
3. The Consequences of the Nutrition Transition in Africa

4. The Determinants of the Nutrition Transition in Africa

5. “New” Directions for Policy and Interventions
- Plan for holistic, integrated nutrition interventions which will be aligned to all other health promotion campaigns in a country, such as improvement of mother-and child health, anti-smoking, responsible alcohol use, living with a specific condition such as HIV/AIDS or diabetes, school nutrition programs, increased activity initiatives, and others.
- All interventions should be evidence-based, addressing proven public health problems in the country, with methods known to be potentially successful. A starting point would be to use quality baseline data, scientific theory for planning, and implementation methods to change societal behavior.
- Under- and over-nutrition should be addressed simultaneously. Interventions should aim for optimal, balanced, adequate, but prudent diets for all. This means that food security for all should be a high priority, and that both the under-nourished and “over-nourished” (overfed) people in a population should be reached with positive messages of how to choose a healthy diet.
- Involve communities in the planning of the nutrition intervention, using a “bottom-up” rather than a “top-down” approach. Many programs have shown that community ‘buy-in” is necessary for compliance to advice and recommendations.
- Get all stakeholders on board from the planning stage to ensure that they will help in the implementation of the policy and/or intervention(s). These stakeholders should include local governance bodies, the agricultural and food industries (all involved in production, distribution and marketing of food and beverages), non-governmental organizations, united nations organizations, medical schemes, advertising industry, all institutions providing meals to consumers such as the army, homes for the elderly, schools, etc. All these stakeholders are collectively responsible for creating the food environment from which consumers make their choices. They should all work together to ensure an environment in which safe, healthy, cultural and traditional choices are available and affordable. Countries could consider legislation to help to create this environment, such as a ban on advertisements of undesirable foods and beverages on children’s television programs, or a-ban on selling energy-rich, nutrient-poor foods in school canteens. The food industry realizes that there is a market for “healthier foods” but their agenda and motives in developing and marketing these foods are still questionable.
- Focus on diversification of diets (a food-based approach) rather than a reliance on fortified foods and supplements, where possible. There may be circumstances where fortification and supplementation will be necessary to address specific micronutrient deficiencies, provided that there is good evidence that these deficiencies pose a public health problem. Also, there must be convincing evidence that fortification and supplementation would be safe and effective.
- It is a human right to be food and nutrition secure. Therefore, in addition of “creating” a suitable food environment, individuals should be enabled to make the right choices. This means appropriate consumer education and social marketing to target groups with strategies that will help to change behavior. Consumer-friendly and understandable food-based dietary guidelines [39] are useful to promote healthy eating and educate consumers on healthy dietary choices.
- Nutrition “capacity” within the health and other sectors in all African countries should be developed and increased. Even rich, developed, industrialized countries, have insufficient nutritionists and dietitians to “serve” the population. Therefore, nutrition capacity to promote healthier diets can be increased by training other professionals (physicians, nurses, pharmacists, agriculturists, and others) in nutrition.
- Only implement interventions at scale after thorough field-testing in appropriate target groups. All interventions should be evaluated regularly after implementation to adapt and change if they are not working. These evaluations should include input, process, output, outcome and impact assessments.
- Use all available resources to implement interventions aimed at healthier eating. Innovative, creative and original use of available infrastructure and existing programs, based on knowledge of local beliefs, attitudes and practices, could ensure positive results.
6. Research Challenges for Africa
7. Conclusions
References
- Waage, J.; Banerji, R.; Campbell, O.; Chirwa, E.; Collender, G.; Dieltiens, V.; Dorward, V.; Godfrey-Faussett, P.; Hanvoravongchai, P.; Kingdon, G. The Millenium Development Goals: A cross-sectorial analysis and principles for goal setting after 2015. 2010. Available online: http://www.thelancet.com (accessed on 4 October 2010).
- Omran, A.R. The epidemiologic transition: A theory of the epidemiology of population change. Milbank Mem. Fund Q. 1971, 49, 509–538. [Google Scholar]
- World Health Organization, The World Health Report 2002: Reducing Risks, Promoting Healthy Life; WHO: Geneva, Switzerland, 2002.
- Popkin, B.M. An overview on the nutrition transition and its health implications: The Bellagio meeting. Public Health Nutr. 2002, 5, 93–103. [Google Scholar]
- Vorster, H.H. The emergence of cardiovascular disease during urbanization of Africans. Public Health Nutr. 2002, 5, 239–243. [Google Scholar]
- Popkin, B.M.; Gordon-Larsen, P. The nutrition transition: worldwide obesity dynamics and their determinants. Int. J. Obes. 2004, 28, S2–S9. [Google Scholar]
- The Global Burden of Disease: A Comprehensive Assessment of Mortality and Disability from Diseases, Injury, and Risk Factors in 1990 and Projected to 2020; Murray, C.J.L.; Lopez, A.D. (Eds.) Global Burden of Disease and Injuries Series, Harvard School of Public Health: Cambridge, MA, USA, 1996; Volume 1.
- Joint World Health Organisation (WHO)/Food and Agriculture Organisation (FAO) Expert Consultation, Diet, Nutrition and the Prevention of Chronic Diseases; WHO: Geneva, Switzerland, 2003.
- Drewnowski, A.; Popkin, B.M. The nutrition transition: New trends in the global diet. Nutr. Rev. 1997, 55, 31–43. [Google Scholar]
- MacIntyre, U.E. Dietary intakes of Africans in transition in the North-West Province. Potchefstroom University for Christian Higher Education, Potchefstroom, South Africa, 1998. [Google Scholar]
- Vorster, H.H.; Wissing, M.P.; Venter, C.S.; Kruger, H.S.; Kruger, A.; Malan, N.T.; De Ridder, J.H.; Veldman, F.J.; Steyn, H.S.; Margetts, B.M.; MacIntyre, U. The impact of urbanization on physical, physiological and mental health of Africans in the North West Province of South Africa: The THUSA study. S. Afr. J. Sci. 2000, 96, 505–514. [Google Scholar]
- MacIntyre, U.E.; Kruger, H.S.; Venter, C.S.; Vorster, H.H. Dietary intakes of an African population in different stages of transition in the North West Province, South Africa: The THUSA study. Nutr. Res. 2002, 22, 230–256. [Google Scholar]
- Kruger, H.S.; Venter, C.S.; Vorster, H.H. Obesity in African women in the North West Province, South Africa, is associated with an increased risk of non-communicable diseases: The THUSA stud. Br. J. Nutr. 2001, 86, 733–740. [Google Scholar]
- Academy of Science of South Africa (ASSAf), HIV/AIDS, TB and Nutrition. Scientific Inquiry into the Nutritional Influences on Human Immunity with Special Reference to HIV Infection and Active TB in South Africa; ASSAf: Pretoria, South Africa, 2007.
- Vorster, H.H.; Oosthuizen, W.; Jerling, J.C.; Veldman, F.J.; Burger, H.M. The Nutritional Status of South Africans: A Review of the Literature from 1975–1996 (Volume 1: Narrative; Volume 2: Reference Tables); Health Systems Trust: Durban, South Africa, 1997. [Google Scholar]
- Kruger, A. South Africa baseline study.; North-West University: Potchefstroom, South Africa., 2005; unpublished work. [Google Scholar]
- Venter, C.S.; MacIntyre, U.E.; Vorster, H.H. The development and testing of a food portion photograph book for use in an African population. J. Hum. Nutr. Diet. 2000, 13, 205–218. [Google Scholar]
- Goedecke, J.H.; Jennings, C.L.; Lambert, E.V. Obesity in South Africa. In Chronic Diseases ofLifestyle in South Africa: 1995-2005; Steyn, K., Fourie, J., Temple, N.Z., Eds.; Medical Research Council: Cape Town, South Africa, 2006; pp. 65–79. [Google Scholar]
- Hawkes, C. Uneven dietary development: Linking the policies and processes of globalization with the nutrition transition, obesity and diet-related chronic diseases. Glob. Health 2006, 2, 4–22. [Google Scholar]
- Puoane, T.; Steyn, K.; Bradshaw, D.; Laubscher, R.; Fourie, J.; Lambert, V.; Mbananga, N. Obesity in South Africa: The South African demographic and health survey. Obes. Res. 2002, 10, 1038–1048. [Google Scholar]
- Labadarios, D.; Swart, R.; Dannhauser, A.; Kuzwayo, P.; Maunder, E.M.W.; Gericke, G.; Scloss, I.; Ntse, P.R.; Kruger, H.S.; Steyn, N.P. Executive summary of the National Food Consumption Survey Fortification Baseline (NFCS-FB-I) South Africa, 2005. S. Afr. J. Clin. Nutr. 2008, 21, 247–300. [Google Scholar]
- Bradshaw, D.; Schneider, M.; Norman, R.; Bourne, D. Mortality patterns of chronic diseases of lifestyle in South Africa. In Chronic Diseases ofLifestyle in South Africa: 1995-2005; Steyn, K., Fourie, J., Temple, N.Z., Eds.; Medical Research Council: Cape Town, South Africa, 2006; pp. 9–22. [Google Scholar]
- Wyndham, C.H. Trends with time of cardiovascular mortality rates in the populations of the RSA for the period 1968-1977. S. Afr. Med. J. 1982, 61, 987–993. [Google Scholar]
- Vorster, H.H.; Bourne, L.T.; Venter, C.S.; Oosthuizen, W. Contribution of nutrition to the health transition in developing countries: A framework for research and intervention. Nutr. Rev. 1999, 57, 341–349. [Google Scholar]
- Barker, D.J.P. Fetal origins of coronary heart disease. Br. Med. J. 1995, 311, 171–174. [Google Scholar]
- Kruger, H.S.; Margetts, B.M.; Vorster, H.H. Evidence for relatively greater subcutaneous fat deposition in stunted girls in the North West Province, South Africa, as compared with non-stunted girl. Nutrition 2004, 20, 564–569. [Google Scholar]
- Opie, L.H.; Mayosi, B.M. Cardiovascular disease in sub-Saharan Africa. Circulation 2005, 112, 3536–3540. [Google Scholar]
- United Nations Children’s Fund. The State of the World’s Children 2008: Child Survival; UNICEF: New York, NY, USA, 2008.
- Coca-Cola, Company Annual Review; Coca-Cola: Atlanta, GA, USA, 2008.
- Du Plessis, A.; Malan, L.; Malan, N.T. Coping and metabolic syndrome indicators in urban black South African men: The SABPA study. Cardiovasc. J. Afr. 2010, 21, 268–273. [Google Scholar]
- Malan, L.; Schutte, A.E.; Malan, N.T.; Wissing, M.P.; Vorster, H.H.; Steyn, H.S.; van Rooyen, J.M.; Huisman, H.W. Coping mechanisms, perception of health and cardiovascular dysfunction in Africans. Int. J. Psychophysiol. 2006, 61, 158–166. [Google Scholar] [CrossRef] [PubMed]
- Schwarz, P.E.H.; Towers, G.W.; van der Merwe, A.; Perez-Perez, L.; Rheeder, P.; Schulze, J.; Bornstein, S.R.; Licinio, J.; Wong, M.-L.; Schutte, A.E.; Olckers, A. Global meta-analysis of the C-11377G alteration in the ADIPOQ gene indicates the presence of population-specific effects: Challenge for global health initiatives. Pharmacogenomics J. 2009, 9, 42–48. [Google Scholar]
- Olckers, A.; Towers, G.W.; van der Merwe, A.; Schwarz, P.E.H.; Rheeder, P.; Schutte, A.E. Protective effect against type 2 diabetes mellitus identified within the ACDC gene in a black South African diabetic cohort. Metabolism 2007, 56, 587–592. [Google Scholar]
- Puska, P.; Pietinen, P.; Ulla, U. Influencing public nutrition for non-communicable disease prevention: From community intervention to national program: Experiences from Finland. Public Health Nutr. 2002, 5, 245–251. [Google Scholar]
- Vorster, H.H.; Kruger, A.; Venter, C.S.; Margetts, B.M.; MacIntyre, U.E. Cardiovascular disease risk factors and socioeconomic position of Africans in transition: The THUSA study. Cardiovasc. J. Afr. 2007, 18, 282–289. [Google Scholar]
- Reddy, K.K.R.; Rao, A.P.; Reddy, T.P.K. Socioeconomic status and the prevalence of coronary heart disease risk factors. Asia Pac. J. Clin. Nutr. 2002, 11, 98–103. [Google Scholar]
- Irribarren, C.; Luepker, R.V.; McGovern, P.G.; Arnett, D.K.; Blackburn, H. Twelve-year trends in cardiovascular disease risk factors in the Minnesota heart survey. Arch. Intern. Med. 1997, 157, 873–880. [Google Scholar]
- Nishi, N.; Makino, K.; Fukuda, H.; Tatara, K. Effects of socioeconomic indicators on coronary risk factors, self-rated health and psychological well-being among urban Japanese civil servants. Soc. Sci. Med. 2004, 58, 1159–1170. [Google Scholar]
- World Health Organization, Procedural Manual for the Development of Regional and Country-Specific Food-Based Dietary Guidelines (FBDGs); WHO: Geneva, Switzerland, 2010; in press.
© 2011 by the authors; licensee MDPI, Basel, Switzerland. This article is an open-access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Vorster, H.H.; Kruger, A.; Margetts, B.M. The Nutrition Transition in Africa: Can It Be Steered into a More Positive Direction? Nutrients 2011, 3, 429-441. https://doi.org/10.3390/nu3040429
Vorster HH, Kruger A, Margetts BM. The Nutrition Transition in Africa: Can It Be Steered into a More Positive Direction? Nutrients. 2011; 3(4):429-441. https://doi.org/10.3390/nu3040429
Chicago/Turabian StyleVorster, Hester H., Annamarie Kruger, and Barrie M. Margetts. 2011. "The Nutrition Transition in Africa: Can It Be Steered into a More Positive Direction?" Nutrients 3, no. 4: 429-441. https://doi.org/10.3390/nu3040429
APA StyleVorster, H. H., Kruger, A., & Margetts, B. M. (2011). The Nutrition Transition in Africa: Can It Be Steered into a More Positive Direction? Nutrients, 3(4), 429-441. https://doi.org/10.3390/nu3040429




