Methodological Principles of Nasal Food Challenge
Abstract
1. Introduction
2. Materials and Methods
2.1. Ethical Statements
2.2. Study Participants
2.3. Data Collection
2.4. Study Design and Setting
2.5. Statistical Analyses
3. Results
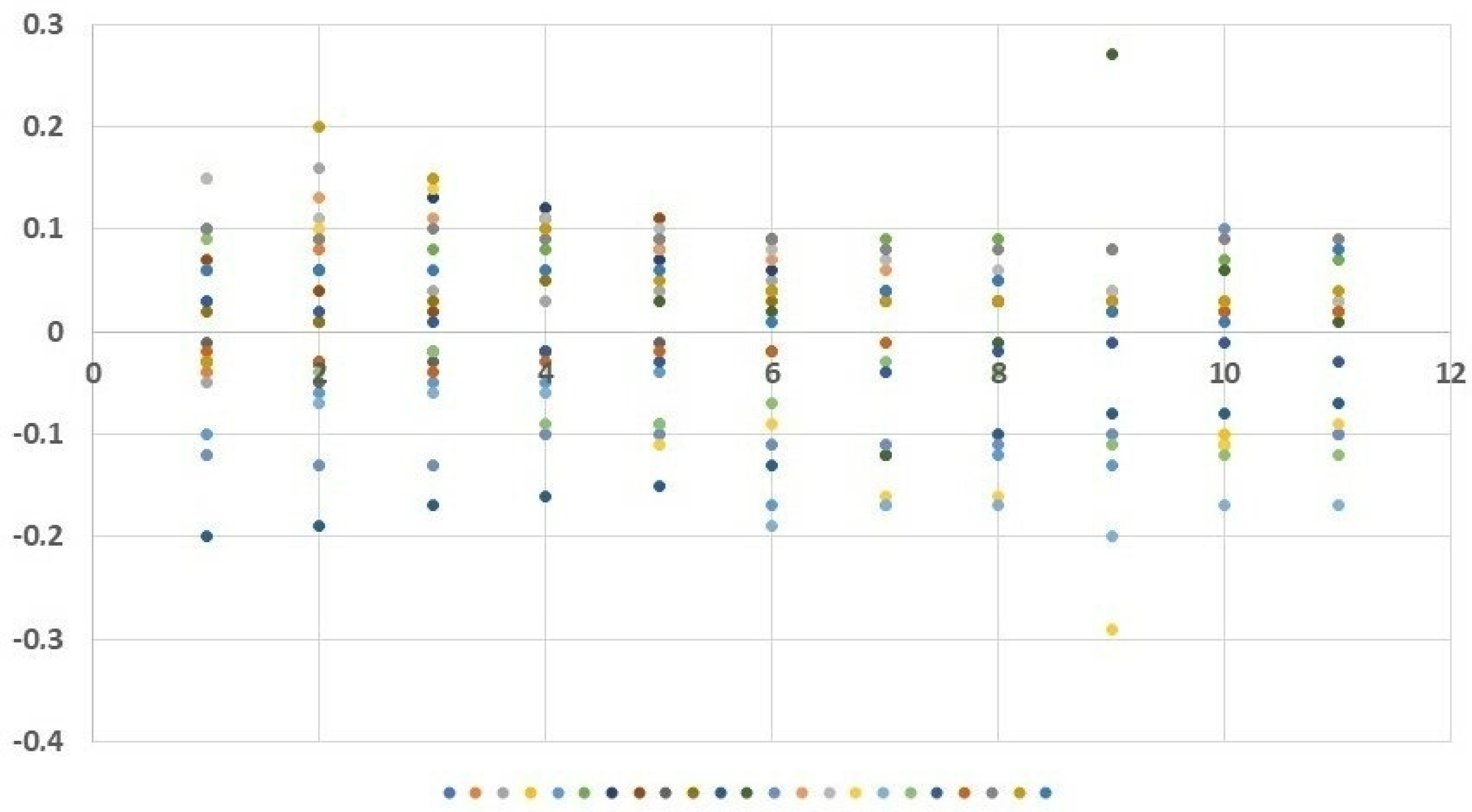
3.1. Variability of Nasal Flow at Individual Time Points in Relation to an Increasing Dose of Allergen Administered
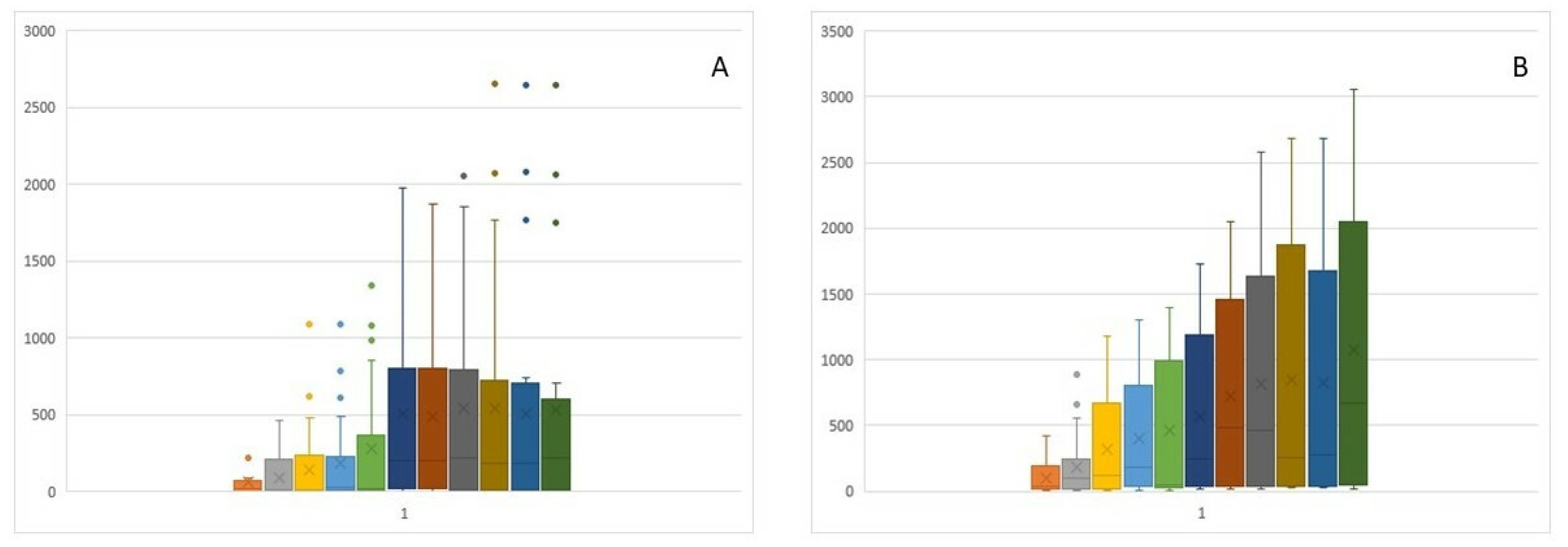
3.2. Mean Optical Density, Onset, and Greatest Change in Flow Measured by Optical Rhinometry
4. Discussion
4.1. Benefits of Nasal Provocation Test in Diagnosing Food Allergies
4.2. Limitation of Study
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Sicherer, S.H.; Sampson, H.A. Food allergy: A review and update on epidemiology, pathogenesis, diagnosis, prevention, and management. J. Allergy Clin. Immunol. 2018, 141, 41–58. [Google Scholar] [CrossRef]
- Passanisi, S.; Lombardo, F.; Crisafulli, G.; Salzano, G.; Aversa, T.; Pajno, G.B. Novel diagnostic techniques and therapeutic strategies for IgE-mediated food allergy. Allergy Asthma Proc. 2021, 42, 124–130. [Google Scholar] [CrossRef] [PubMed]
- Eiwegger, T.; Hung, L.; San Diego, K.E.; O’Mahony, L.; Upton, J. Recent developments and highlights in food allergy. Allergy 2019, 74, 2355–2367. [Google Scholar] [CrossRef]
- Bartuzi, Z.; Kaczmarski, M.; Czerwionka-Szaflarska, M.; Małaczynska, T.; Krogulska, A. The diagnosis and management of food allergies. Position paper of the Food Allergy Section the Polish Society of Allergology. Adv. Dermatol. Allergol. 2017, 34, 391–404. [Google Scholar] [CrossRef] [PubMed]
- Augé, J.; Vent, J.; Agache, I.; Airaksinen, L.; Mozo, P.C.; Chaker, A.; Cingi, C.; Durham, S.; Fokkens, W.; Gevaert, P.; et al. EAACI Position paper on the standardization of nasal allergen challenges. Allergy 2018, 73, 1597–1608. [Google Scholar] [CrossRef]
- Samoliński, B.; Rapiejko, P.; Krzych-Fałta, E.; Gotlib, T.; Emeryk, A.; Buczyłko, K.; Chełmińska, M.; Chełmiński, K.; Niedoszytko, M.; Świerczyńska-Krępa, M.; et al. Standardy wykonywania donosowych prób prowokacyjnych. Adv. Dermatol. Allergol. 2010, XXVII, 141–160. [Google Scholar]
- Samoliński, B.; Krzych-Fałta, E. Definicja donosowej próby prowokacyjnej i donosowej próby prowokacyjnej z alergenem, klasyfikacja. Adv. Dermatol. Allergol. 2010, XXVII, 166–169. [Google Scholar]
- Samoliński, B.; Rapiejko, P. The early reaction after nasal airway challenge with allergen. Adv. Dermatol. Allergol. 2010, XXVII, 170–172. [Google Scholar]
- Pepper, A.N.; Ledford, D.K. Nasal and ocular challenges. J. Allergy Clin. Immunol. 2018, 141, 1570–1577. [Google Scholar] [CrossRef]
- Bousquet, J.; Heinzerling, L.; Bachert, C.; Papadopoulos, N.G.; Bousquet, P.J.; Burney, P.G.; Canonica, G.W.; Cox, L.; Haahtela, T.; Carlsen, K.C.L.; et al. Practical guide to skin prick tests in allergy to aeroallergens. Allergy 2012, 67, 18–24. [Google Scholar] [CrossRef]
- Muraro, A.; Werfel, T.; Hoffmann-Sommergruber, K.; Roberts, G.; Beyer, K.; Bindslev-Jensen, C.; Cardona, V.; Dubois, A.; Dutoit, G.; Eigenmann, P.; et al. EAACI food allergy and anaphylaxis guidelines: Diagnosis and management of food allergy. Allergy 2014, 69, 1008–1025. [Google Scholar] [CrossRef]
- Wüstenberg, E.G.; Zahnert, T.; Huttenbrink, K.B.; Hummel, T. Comparison of Optical Rhinometry and Active Anterior Rhinomanometry Using Nasal Provocation Testing. Arch. Otolaryngol. Head Neck Surg. 2007, 133, 344–349. [Google Scholar] [CrossRef]
- Mittenzwey, H.; Wustenberg, E.G.; Leupold, W. Optical rhinometry: Application on children and adolescents for nasal provocation tests. Pediatr. Allergy Immunol. 2007, 18, 372–377. [Google Scholar] [CrossRef]
- Wüthrich, B. History of food allergy. Chem. Immunol. Allergy 2014, 100, 109–119. [Google Scholar] [CrossRef]
- Cafarotti, A.; Giovannini, M.; Begìn, P.; Brough, H.A.; Arasi, S. Management of IgE-mediated food allergy in the 21st century. Clin. Exp. Allergy 2023, 53, 25–38. [Google Scholar] [CrossRef]
- Turner, P.J.; Tang, M.L.K.; Wood, R.A. Food Allergy and Eosinophilic Gastrointestinal Diseases—The Next 10 Years. J. Allergy Clin. Immunol. Pract. 2023, 11, 72–78. [Google Scholar] [CrossRef]
- Kowalski, M.L.; Ansotegui, I.; Aberer, W.; Al-Ahmad, M.; Akdis, M.; Ballmer-Weber, B.K.; Beyer, K.; Blanca, M.; Brown, S.; Bunnag, C.; et al. Risk and safety requirements for diagnostic and therapeutic procedures in allergology: World Allergy Organization Statement. World Allergy Organ. J. 2016, 9, 33. [Google Scholar] [CrossRef]
- Kvenshagen, B.K.; Jacobsen, M. The value of mucosal allergen challenge for the diagnosis of food allergy. Curr. Opin. Allergy Clin. Immunol. 2013, 13, 268–272. [Google Scholar] [CrossRef]
- Amlot, P.L.; Urbanek, R.; Youlten, L.J.F. Type I allergy to egg and milk proteins: Comparison of skin prick tests with nasal, buccal and gastric provocation tests. Int. Archs. Allergy Appl. Immun. 1985, 77, 171–173. [Google Scholar] [CrossRef]
- Clark, A.; Mangat, J.; Tay, S.; King, Y.; Monk, C.J.; White, P.A.; Ewan, P.W. Facial thermography is a sensitive and specific method for assessing food challenge outcome. Allergy 2007, 62, 744–749. [Google Scholar] [CrossRef]
- Clark, A.; Mangat, J.; King, Y.; Islam, S.; Anagnostou, K.; Foley, L.; Deighton, J.; Ewan, P. Thermographic imaging during nasal peanut challenge may be useful in the diagnosis of peanut allergy. Allergy 2012, 67, 574–576. [Google Scholar] [CrossRef] [PubMed]
- Seppey, M.; Hessler, C.; Bruchez, M.; Savary, M.; Pécoud, A. Facial thermography during nasal provocation tests with histamine and allergen. Allergy 1993, 48, 314–318. [Google Scholar] [CrossRef]
- Gelis, S.; Rueda, M.; Pascal, M.; Fernández-Caldas, E.; Fernández, E.; Araujo-Sánchez, G.; Bartra, J.; Valero, A. Usefulness of the Allergen Specific Nasal Provocation Test in the Diagnosis of Shellfish. J. Investig. Allergol. Clin. Immunol. 2022, 32, 460–470. [Google Scholar] [CrossRef] [PubMed]
- Dona, D.W.; Suphioglu, C. Egg Allergy: Diagnosis and Immunotherapy. Int. J. Mol. Sci. 2020, 21, 5010. [Google Scholar] [CrossRef]
- Keil, T.; McBride, D.; Grimshaw, K.; Niggemann, B.; Xepapadaki, P.; Zannikos, K.; Sigurdardottir, S.T.; Clausen, M.; Reche, M.; Pascual, C.; et al. The multinational birth cohort of EuroPrevall: Background, aims and methods. Allergy 2010, 65, 482–490. [Google Scholar] [CrossRef]
- Leech, S.C.; Ewan, P.W.; Skypala, I.J.; Brathwaite, N.; Lajeunesse, M.E.; Heath, S.; Ball, H.; James, P.; Murphy, K.; Clark, A.T. BSACI 2021 guideline for the management of egg allergy. Clin. Exp. Allergy 2021, 51, 1262–1278. [Google Scholar] [CrossRef]
- Trogen, B.; Jacobs, S.; Nowak-Wegrzyn, A. Early Introduction of Allergenic Foods and the Prevention of Food Allergy. Nutrients 2022, 14, 2565. [Google Scholar] [CrossRef]
- Krzych-Fałta, E.; Wojas, O.; Namysłowski, A.; Samoliński, B.; Białek, S.; Furmańczyk, K. Reactivity of nasal cavity mucosa in the nasal cow’s milk allergen provocation test. Adv. Dermatol. Allergol. 2023, XL, 87–92. [Google Scholar] [CrossRef]

| Female | Male | Urban | Rural | General | |
|---|---|---|---|---|---|
| Age Mean (years), | 33.5 | 34.4 | 35.2 *** | 26.3 *** | 33.8 |
| Age SD | 8.5 | 5.9 | 7.5 | 4 | 7.7 |
| Height Mean (cm), | 168.7 * | 181.1 * | 172.2 | 171.8 | 172.2 |
| Height SD | 3.9 | 4.1 | 7.0 | 7.4 | 6.9 |
| Weight Mean (kg), | 63.1 ** | 75.1 ** | 66.8 | 64.5 | 66.4 |
| Weight SD | 4.6 | 6.4 | 7.6 | 7.3 | 7.5 |
| BMI Mean, | 22.2 | 22.9 | 22.5 | 21.8 | 22.4 |
| BMI SD | 1.5 | 1.1 | 1.4 | 1.2 | 1.4 |
| Assessment of nasal patency | |||||
| Acoustic rhinometry | Female | Male | Urban | Rural | General |
| MCA-1R Mean | 0.351 | 0.347 | 0.355 | 0.323 | 0.350 |
| MCA-1R SD | 0.058 | 0.081 | 0.065 | 0.053 | 0.064 |
| MCA-1L Mean | 0.343 | 0.299 | 0.337 | 0.295 | 0.330 |
| MCA-1L SD | 0.063 | 0.062 | 0.068 | 0.030 | 0.065 |
| MCA-2R Mean | 1.711 | 1.621 | 1.703 | 1.595 | 1.686 |
| MCA-2R SD | 0.423 | 0.423 | 0.422 | 0.357 | 0.407 |
| MCA-2L Mean | 1.676 | 1.630 | 1.704 **** | 1.448 **** | 1.663 |
| MCA-2L SD | 0.401 | 0.361 | 0.403 | 0.137 | 0.383 |
| FENO Mean (ppb), | 393.722 | 524.714 | 435.191 | 405.250 | 430.4 |
| FENO SD | 140.938 | 167.927 | 170.825 | 47.352 | 157.237 |
| Spirometry | 93.600 | ||||
| FEV1/FVC Mean (%), | 93.389 | 94.143 | 93.476 | 94.250 | 5.346 |
| FEV1/FVC SD | 5.414 | 5.551 | 5.662 | 3.775 | |
| 92.240 | |||||
| FEV1 Mean (L), | 92.111 | 92.571 | 91.905 | 94.000 | 7.293 |
| FEV1 SD | 7.529 | 7.208 | 7.334 | 7.874 | |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Krzych-Fałta, E.; Czerwińska, M.E.; Białek, S.; Furmańczyk, K.; Samoliński, B.; Grodner, B.; Sybilski, A.; Nowicka, G.; Wojas, O. Methodological Principles of Nasal Food Challenge. Nutrients 2023, 15, 3816. https://doi.org/10.3390/nu15173816
Krzych-Fałta E, Czerwińska ME, Białek S, Furmańczyk K, Samoliński B, Grodner B, Sybilski A, Nowicka G, Wojas O. Methodological Principles of Nasal Food Challenge. Nutrients. 2023; 15(17):3816. https://doi.org/10.3390/nu15173816
Chicago/Turabian StyleKrzych-Fałta, Edyta, Monika E. Czerwińska, Sławomir Białek, Konrad Furmańczyk, Bolesław Samoliński, Błażej Grodner, Adam Sybilski, Grażyna Nowicka, and Oksana Wojas. 2023. "Methodological Principles of Nasal Food Challenge" Nutrients 15, no. 17: 3816. https://doi.org/10.3390/nu15173816
APA StyleKrzych-Fałta, E., Czerwińska, M. E., Białek, S., Furmańczyk, K., Samoliński, B., Grodner, B., Sybilski, A., Nowicka, G., & Wojas, O. (2023). Methodological Principles of Nasal Food Challenge. Nutrients, 15(17), 3816. https://doi.org/10.3390/nu15173816







