Breastfeeding and Inborn Errors of Amino Acid and Protein Metabolism: A Spreadsheet to Calculate Optimal Intake of Human Milk and Disease-Specific Formulas
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Design and Population
2.2. Methodology
3. Results
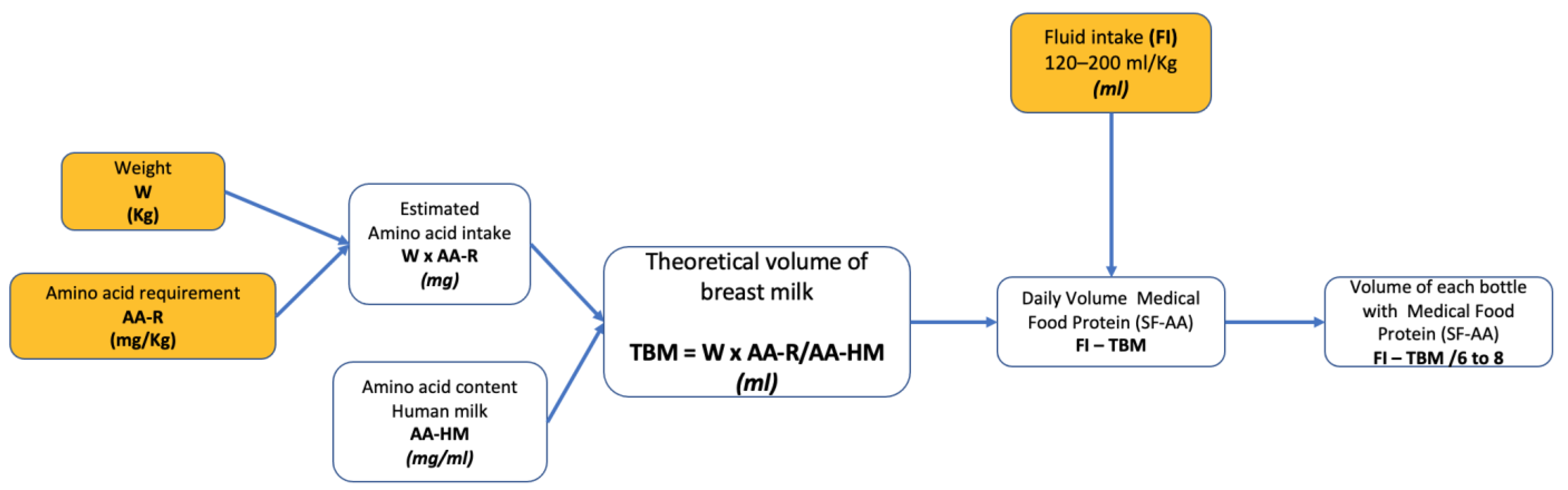
3.1. Scenario 1: Special Formula Lacking the Limiting Amino Acid Is Available
3.2. Scenario 2: Total Amount of Protein Intake Must Be Calculated
4. Discussion
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Hicks, S.D.; Confair, A.; Warren, K.; Chandran, D. Levels of Breast Milk MicroRNAs and Other Non-Coding RNAs Are Impacted by Milk Maturity and Maternal Diet. Front. Immunol. 2022, 12, 785217. [Google Scholar] [CrossRef] [PubMed]
- ESPGAN Committee on Nutrition. Guidelines on Infant Nutrition. III. Recommendations for Infant Feeding. Acta Paediatr. Scand. 1982, 302, 1–27. [Google Scholar]
- Morrow, A.L.; Ruiz-Palacios, G.M.; Jiang, X.; Newburg, D.S. Human-milk glycans that inhibit pathogen binding protect breast-feeding infants against infectious diarrhea. J. Nutr. 2005, 135, 1304–1307. [Google Scholar] [CrossRef] [PubMed]
- Wu, S.; Ren, L.; Li, J.; Shen, X.; Zhou, Q.; Miao, Z.; Jia, W.; He, F.; Cheng, R. Breastfeeding might partially contribute to gut microbiota construction and stabilization of propionate metabolism in cesarean-section infants. Eur. J. Nutr. 2023, 62, 615–631. [Google Scholar] [CrossRef]
- Binns, C.; Lee, M.; Yun Low, W. The long-term public health benefits of breastfeeding. Asia Pac. J. Public Health 2016, 28, 7–14. [Google Scholar] [CrossRef]
- MacDonald, A.; van Wegberg, A.M.J.; Ahring, K.; Beblo, S.; Bélanger-Quintana, A.; Burlina, A.; Campistol, J.; Coşkun, T.; Feillet, F.; Giżewska, M.; et al. PKU dietary handbook to accompany PKU guidelines. Orphanet J. Rare Dis. 2020, 15, 171, Erratum in: Orphanet J. Rare Dis. 2020, 15, 230. [Google Scholar] [CrossRef]
- Bernstein, L.; Rohr, F.; Van Calcar, S. (Eds.) Nutrition Management of Inherited Metabolic Diseases, 2nd ed.; Springer: Cham, Switzerland, 2022. [Google Scholar]
- Banta-Wright, S.A.; Shelton, K.C.; Lowe, N.D.; Knafl, K.A.; Houck, G.M. Breast-feeding success among infants with phenylketonuria. J. Pediatr. Nurs. 2012, 27, 319–327. [Google Scholar] [CrossRef]
- McCabe, L.; Ernest, A.E.; Neifert, M.R.; Yannicelli, S.; Nord, A.M.; Garry, P.J.; McCabe, E.R. The management of breast feeding among infants with phenylketonuria. J. Inherit. Metab. Dis. 1989, 12, 467–474. [Google Scholar] [CrossRef]
- Kose, E.; Aksoy, B.; Kuyum, P.; Tuncer, N.; Arslan, N.; Ozturk, Y. The Effects of Breastfeeding in Infants With Phenylketonuria. J. Pediatr. Nurs. 2018, 38, 27–32. [Google Scholar] [CrossRef]
- Banta-Wright, S.A.; Press, N.; Knafl, K.A.; Steiner, R.D.; Houck, G.M. Breastfeeding infants with phenylketonuria in the United States and Canada. Breastfeed. Med. 2014, 9, 142–148. [Google Scholar] [CrossRef]
- Huner, G.; Baykal, T.; Demir, F.; Demirkol, M. Breastfeeding experience in inborn errors of metabolism other than phenylketonuria. J. Inherit. Metab. Dis. 2005, 28, 457–465. [Google Scholar] [CrossRef]
- Giordano, M.; Castellino, P.; De Fronzo, R.A. Differential responsiveness of protein synthesis and degradation to amino acid availability in humans. Diabetes 1996, 45, 393–399. [Google Scholar] [CrossRef] [PubMed]
- MacDonald, A.; Singh, R.; Rocha, J.; Van Spronsen, F. Optimising amino acid absorption: Essential to improve nitrogen balance and metabolic control in phenylketonuria. Nutr. Res. Rev. 2019, 32, 70–78. [Google Scholar] [CrossRef]
- Gidrewicz, D.A.; Fenton, T.R. A systematic review and meta-analysis of the nutrient content of preterm and term breast milk. BMC Pediatr. 2014, 14, 216. [Google Scholar] [CrossRef] [PubMed]
- Oppe, T. The Composition of Mature Human Milk-Report of a Party of the Committee on Medical Aspects of Food Policy; Department of Health and Social Security: London, UK, 1977. [Google Scholar]
- Van Calcar, S. Nutrition management of phenylketonuria. In Nutrition Management of Inherited Metabolic Diseases, 2nd ed.; Bernstein, L., Rohr, F., Van Calcar, S., Eds.; Springer: Cham, Switzerland, 2022; pp. 127–152. [Google Scholar]
- Larson, A. Hereditary tyrosinemia. In Nutrition Management of Inherited Metabolic Diseases, 2nd ed.; Bernstein, L., Rohr, F., van Calcar, S., Eds.; Springer: Cham, Switzerland, 2022; pp. 189–196. [Google Scholar]
- Boy, N.; Mühlhausen, C.; Maier, E.M.; Ballhausen, D.; Baumgartner, M.R.; Beblo, S.; Burgard, P.; Chapman, K.A.; Dobbelaere, D.; Heringer-Seifert, J.; et al. Recommendations for diagnosing and managing individuals with glutaric aciduria type 1: Third revision. J. Inherit. Metab. Dis. 2023, 46, 482–519. [Google Scholar] [CrossRef] [PubMed]
- Couce, M.L.; Balcells, S.; Sánchez-Pintos, P.; Aldámiz-Echevarría, L.; del Toro, M.; Grinberg, D. Protocolo de homocistinuria. In Protocolos de Diagnóstico y Tratamiento de los Errores Congénitos del Metabolismo, 2nd ed.; Gil, D., Ed.; Ergon: Madrid, Spain, 2017; pp. 167–180. [Google Scholar]
- Morris, A.A.; Kožich, V.; Santra, S.; Andria, G.; Ben-Omran, T.I.; Chakrapani, A.B.; Crushell, E.; Henderson, M.J.; Hochuli, M.; Huemer, M.; et al. Guidelines for the diagnosis and management of cystathionine beta-synthase deficiency. J. Inherit. Metab. Dis. 2017, 40, 49–74. [Google Scholar] [CrossRef]
- Frazier, D.M.; Allgeier, C.; Homer, C.; Marriage, B.J.; Ogata, B.; Rohr, F.; Splett, P.L.; Stembridge, A.; Singh, R.H. Nutrition management guideline for maple syrup urine disease: An evidence- and consensus-based approach. Mol. Genet. Metab. 2014, 112, 210–217. [Google Scholar] [CrossRef] [PubMed]
- Knerr, I.; Vockley, J.; Gibson, K.M. Disorders of Leucine, Isoleucine, and Valine Metabolism. In Physician’s Guide to the Diagnosis, Treatment and Follow-Up of Inherited Metabolic Diseases; Blau, N., Duran, M., Gibson, K.M., Dionisi-Vici, C., Eds.; Springer: Berlin/Heidelberg, Germany, 2014; pp. 103–142. [Google Scholar]
- Southeast Regional Genetics Network (SERN) and Genetic Metabolic Dietitians International (GMDI). Propionic Acidemia Nutrition Management Guidelines. Available online: https://southeastgenetics.org/ngp/guidelines.php (accessed on 28 May 2023).
- Forny, P.; Hörster, F.; Ballhausen, D.; Chakrapani, A.; Chapman, K.A.; Dionisi-Vici, C.; Dixon, M.; Grünert, S.C.; Grunewald, S.; Haliloglu, G.; et al. Guidelines for the diagnosis and management of methylmalonic acidaemia and propionic acidaemia: First revision. J. Inherit. Metab. Dis. 2021, 44, 566–592. [Google Scholar] [CrossRef]
- McLeod, E. Nutrition Management of Urea Cycle Disorders. In Nutrition Management of Inherited Metabolic Diseases, 2nd ed.; Bernstein, L., Rohr, F., van Calcar, S., Eds.; Springer: Cham, Switzerland, 2022; pp. 225–240. [Google Scholar]
- Häberle, J.; Burlina, A.; Chakrapani, A.; Dixon, M.; Karall, D.; Lindner, M.; Mandel, H.; Martinelli, D.; Pintos-Morell, G.; Santer, R.; et al. Suggested guidelines for the diagnosis and management of urea cycle disorders: First revision. J. Inherit. Metab. Dis. 2019, 42, 1192–1230. [Google Scholar] [CrossRef]
- British Inherited Metabolic Diseases Group. BIMDG Website. Newborn Screening Guidelines. Available online: https://www.bimdg.org.uk/site/guidelines-enbs.asp?t=5 (accessed on 18 July 2023).
- Singh, R.H.; Cunningham, A.C.; Mofidi, S.; Douglas, T.D.; Frazier, D.M.; Hook, D.G.; Jeffers, L.; McCune, H.; Moseley, K.D.; Ogata, B.; et al. Updated, web-based nutrition management guideline for PKU: An evidence and consensus based approach. Mol. Genet. Metab. 2016, 118, 72–83. [Google Scholar] [CrossRef]
- McCabe, E.R.; McCabe, L. Issues in the dietary management of phenylketonuria: Breast-feeding and trace-metal nutriture. Ann. N. Y. Acad. Sci. 1986, 477, 215–222. [Google Scholar] [CrossRef] [PubMed]
- Pinto, A.; Adams, S.; Ahring, K.; Allen, H.; Almeida, M.F.; Garcia-Arenas, D.; Arslan, N.; Assoun, M.; Atik Altınok, Y.; Barrio-Carreras, D.; et al. Early feeding practices in infants with phenylketonuria across Europe. Mol. Genet. Metab. Rep. 2018, 16, 82–89. [Google Scholar] [CrossRef] [PubMed]
- Motzfeldt, K.; Lilje, R.; Nylander, G. Breastfeeding in phenylketonuria. Acta Paediatr. 1999, 88 (Suppl. 432), 25–27. [Google Scholar] [CrossRef] [PubMed]
- Dermirkol, M.; Gokcay, G.; Kuru, N.; Donmez, S.; Baykal, T.; Seckin, Y. Feasibility of breastfeeding in inborn errors of metabolism: Experience in phenylketonuria. Ann. Nutr. Metab. 2001, 45, 497–498. [Google Scholar]
- Van Rijn, M.; Bekhof, J.; Dijkstra, T.; Smit, P.G.; Moddermam, P.; van Spronsen, F.J. A different approach to breast-feeding of the infant with phenylketonuria. Eur. J. Pediatr. 2003, 162, 323–326. [Google Scholar] [CrossRef]
- Zuvadelli, J.; Paci, S.; Salvatici, E.; Giorgetti, F.; Cefalo, G.; Re Dionigi, A.; Rovelli, V.; Banderali, G. Breastfeeding in Phenylketonuria: Changing Modalities, Changing Perspectives. Nutrients 2022, 14, 4138. [Google Scholar] [CrossRef]
- Yilmaz, O.; Cochrane, B.; Wildgoose, J.; Pinto, A.; Evans, S.; Daly, A.; Ashmore, C.; MacDonald, A. Phenylalanine free infant formula in the dietary management of phenylketonuria. Orphanet J. Rare Dis. 2023, 18, 16. [Google Scholar] [CrossRef]
- De Laet, C.; Dionisi-Vici, C.; Leonard, J.V.; McKiernan, P.; Mitchell, G.; Monti, L.; de Baulny, H.O.; Pintos-Morell, G.; Spiekerkötter, U. Recommendations for the management of tyrosinaemia type 1. Orphanet J. Rare Dis. 2013, 8, 8. [Google Scholar] [CrossRef]
- Chinsky, J.M.; Singh, R.; Ficicioglu, C.; van Karnebeek, C.D.M.; Grompe, M.; Mitchell, G.; Waisbren, S.E.; Gucsavas-Calikoglu, M.; Wasserstein, M.P.; Coakley, K.; et al. Diagnosis and treatment of tyrosinemia type I: A US and Canadian consensus group review and recommendations. Genet. Med. 2017, 19, 1380–1395. [Google Scholar] [CrossRef]
- Daly, A.; McDonald, A.; Preece, M.A.; Hendriksz, C.; Chakrapani, A.; McKiernan, P. Successfull breast feeding in tyrosinaemia I. J. Inherit. Metab. Dis. 2005, 28 (Suppl. 1), 45. [Google Scholar]
- Kölker, S.; Boy, S.P.; Heringer, J.; Müller, E.; Maier, E.M.; Ensenauer, R.; Mühlhausen, C.; Schlune, A.; Greenberg, C.R.; Koeller, D.M.; et al. Complementary dietary treatment using lysine-free, arginine-fortified amino acid supplements in glutaric aciduria type I—A decade of experience. Mol. Genet. Metab. 2012, 107, 72–80. [Google Scholar] [CrossRef] [PubMed]
- Pichler, K.; Michel, M.; Zlamy, M.; Scholl-Buergi, S.; Ralser, E.; Jörg-Streller, M.; Karall, D. Breast milk feeding in infants with inherited metabolic disorders other than phenylketonuria—A 10-year single-center experience. J. Perinat. Med. 2017, 45, 375–382. [Google Scholar] [CrossRef] [PubMed]
- Gokcay, G.; Baykal, T.; Gokdemir, Y.; Demirkol, M. Breast feeding in organic acidaemias. J. Inherit. Metab. Dis. 2006, 29, 304–310. [Google Scholar] [CrossRef] [PubMed]
- British Inherited Metabolic Diseases Group. Glutaric Aciduria Type 1 (GA1) Dietetic Management Pathway. Available online: https://www.bimdg.org.uk/store/enbs//GA1_Dietetic_management_pathway_April_2015_117794_12052015.pdf (accessed on 28 May 2023).
- British Inherited Metabolic Diseases Group. Homocystinuria (HCU) Dietetic Management Pathway. Available online: https://www.bimdg.org.uk/store/enbs//HCU_Dietetic_Management_Pathway_V1_April_2015_215380_12052015.pdf (accessed on 28 May 2023).
- Dixon, M.; MacDonald, A.; White, F.; Stafford, J. Disorders of amino acid metabolism, organic acidaemias and urea cycle disorders. In Clinical Paediatric Dietetics, 4th ed.; Shaw, V., Ed.; Wiley: Chichester, UK, 2015; pp. 381–525. [Google Scholar]
- MacDonald, A.; Depondt, E.; Evans, S.; Daly, A.; Hendriksz, C.; Chakrapani, A.; Saudubray, J.M. Breast feeding in IMD. J. Inherit. Metab. Dis. 2006, 29, 299–303. [Google Scholar] [CrossRef] [PubMed]
- Zeybek, A.C.; Bicer, N.; Kiykim, E.; Zubarioglu, T.; Cansever, M.S.; Aydin, A. Importance of early diagnosis of homocystinuria and free breastfeeding initiation. J. Inherit. Metab. Dis. 2015, 38 (Suppl. 1), S35–S378. [Google Scholar]
- Dixon, M.A.; MacDonald, A.; Chakrapani, A.B.; Sharp, J.; Millman, G.; Rogozinski, H.; Walter, J.; Jameson, E.; Abulhoul, L. Breast feeding in pyridoxine non-responsive homocystinuria (HCU). J. Inherit. Metab. Dis. 2014, 37 (Suppl. 1), S27–S185. [Google Scholar]
- Touati, G.; Nassogne, M.C.; Depondt, E.; Assoun, M.; Dubois, S.; Rabier, D.; Saudubray, J.M. Breastfeeding in maple syrup urine disease (MSUD). J. Inherit. Metab. Dis. 2001, 24 (Suppl. 1), 37. [Google Scholar]
- Jurecki, E.; Ueda, K.; Frazier, D.; Rohr, F.; Thompson, A.; Hussa, C.; Obernolte, L.; Reineking, B.; Roberts, A.M.; Yannicelli, S.; et al. Nutrition management guideline for propionic acidemia: An evidence- and consensus-based approach. Mol. Genet. Metab. 2019, 126, 341–354. [Google Scholar] [CrossRef] [PubMed]
- Kamper, A.; Brandauer, M.; Hattinger, E.; Mayr, J.; Sperl, W. Breast feeding in a patient with neonatal onset of citrullinemia. J. Inherit. Metab. Dis. 2001, 24 (Suppl. 1), 42. [Google Scholar]
| Nutritional Component | Per 100 mL |
|---|---|
| Kilocalories | 70 Kcal |
| Protein | 1.07 g |
| Phenylalanine | 46 mg |
| Tyrosine | 36 mg |
| Lysine | 90 mg |
| Methionine | 18 mg |
| Leucine | 116 mg |
| Isoleucine | 64 mg |
| Valine | 83 mg |
| IEM | Limited Essential AA/Protein | RDI (0–6 m) | Kcal/kg/d | Protein g/kg/d |
|---|---|---|---|---|
| PKU [6,17] | Phe | 45–55 mg/kg/d | 80–100 | 0.8–1.3 (SF-AA) |
| TYR-1 [18] | Tyr | 95–275 mg/d (Tyr) 185–550 mg/d (Phe) | 120 | 2.5–3.5 (TP) |
| GA- I [19] | Lys | 100 mg/kg/d | 80–100 | 0.8–1.3 (SF-AA) |
| HCU [20,21] | Met | 90–120 mg/d | 95–145 | 2.5–3.5 (TP) |
| MSUD [22] | Leu, Ile, Val | 40–100 mg/d (Leu) 30–90 mg/d (Ile) 40–95 mg/d (Val) | 95–145 | 2.5–3.5 (TP) |
| IVA [23] | Leu | 50–140 mg/kg/d | 90–120 | 2.5–3.0 (TP) |
| MMA/PA [24,25] | Protein | 0.9–1.5 g/kg/d (IP) | 72–109 | 1.5–1.8 g/kg/d (TP) |
| UCD [26,27] | Protein | 0.8–1.1 g/kg/d (IP) | 80–100 | 1.2–2.2 g/kg/d (TP) |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Vitoria-Miñana, I.; Couce, M.-L.; González-Lamuño, D.; García-Peris, M.; Correcher-Medina, P. Breastfeeding and Inborn Errors of Amino Acid and Protein Metabolism: A Spreadsheet to Calculate Optimal Intake of Human Milk and Disease-Specific Formulas. Nutrients 2023, 15, 3566. https://doi.org/10.3390/nu15163566
Vitoria-Miñana I, Couce M-L, González-Lamuño D, García-Peris M, Correcher-Medina P. Breastfeeding and Inborn Errors of Amino Acid and Protein Metabolism: A Spreadsheet to Calculate Optimal Intake of Human Milk and Disease-Specific Formulas. Nutrients. 2023; 15(16):3566. https://doi.org/10.3390/nu15163566
Chicago/Turabian StyleVitoria-Miñana, Isidro, María-Luz Couce, Domingo González-Lamuño, Mónica García-Peris, and Patricia Correcher-Medina. 2023. "Breastfeeding and Inborn Errors of Amino Acid and Protein Metabolism: A Spreadsheet to Calculate Optimal Intake of Human Milk and Disease-Specific Formulas" Nutrients 15, no. 16: 3566. https://doi.org/10.3390/nu15163566
APA StyleVitoria-Miñana, I., Couce, M.-L., González-Lamuño, D., García-Peris, M., & Correcher-Medina, P. (2023). Breastfeeding and Inborn Errors of Amino Acid and Protein Metabolism: A Spreadsheet to Calculate Optimal Intake of Human Milk and Disease-Specific Formulas. Nutrients, 15(16), 3566. https://doi.org/10.3390/nu15163566









