Association between Dairy Product Intake and Risk of Fracture among Adults: A Cohort Study from China Health and Nutrition Survey
Abstract
1. Introduction
2. Materials and Methods
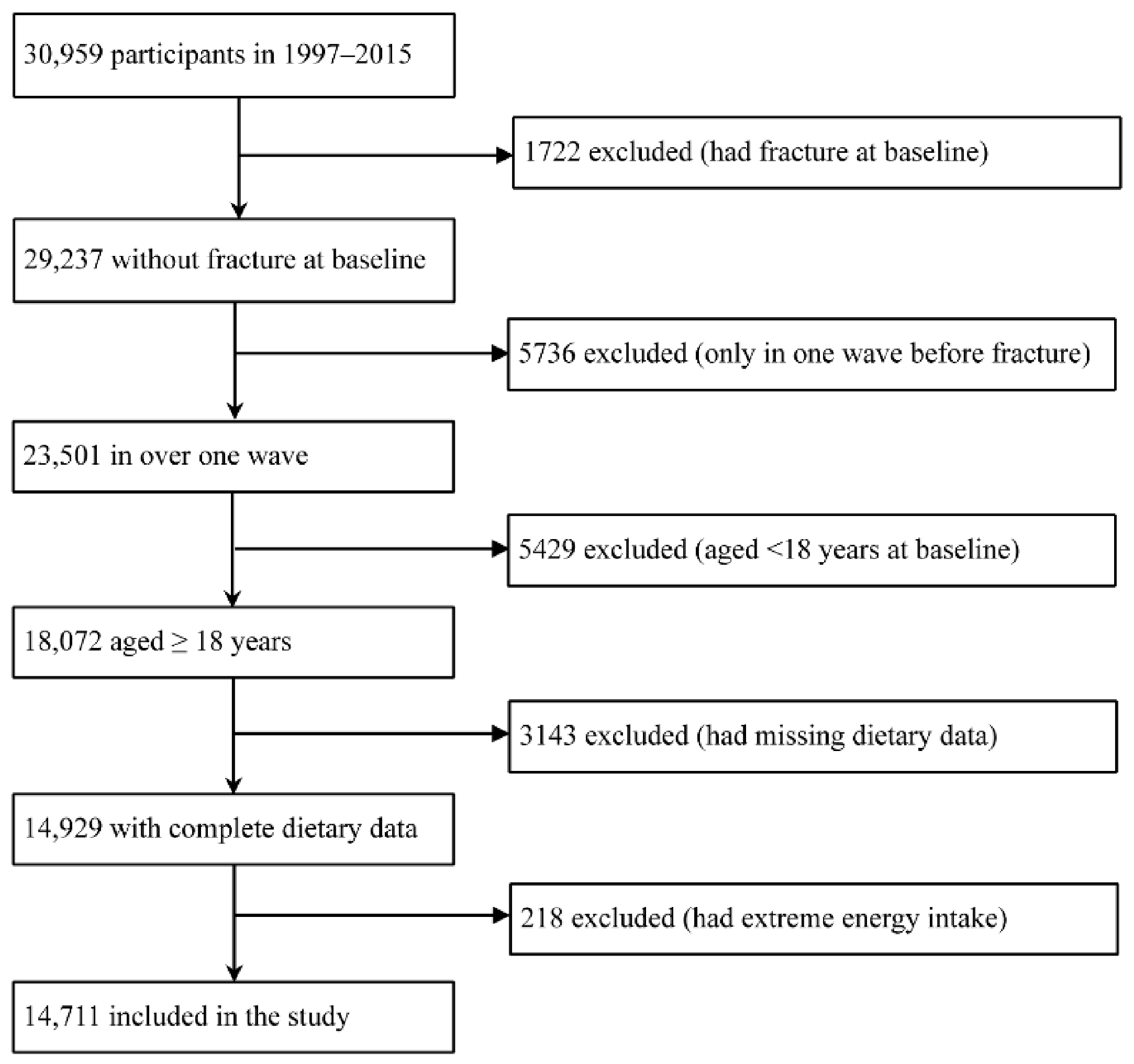
2.1. Study Population
2.2. Dietary Assessment
2.3. Definition of Fracture
2.4. Definition of Covariates
2.5. Statistical Analyses
3. Results
3.1. Basic Characteristics of Participants
3.2. Association between Dairy Product Intake and the Risk of Fracture
3.3. Associations of Calcium and Protein in Dairy Products with the Risk of Fracture
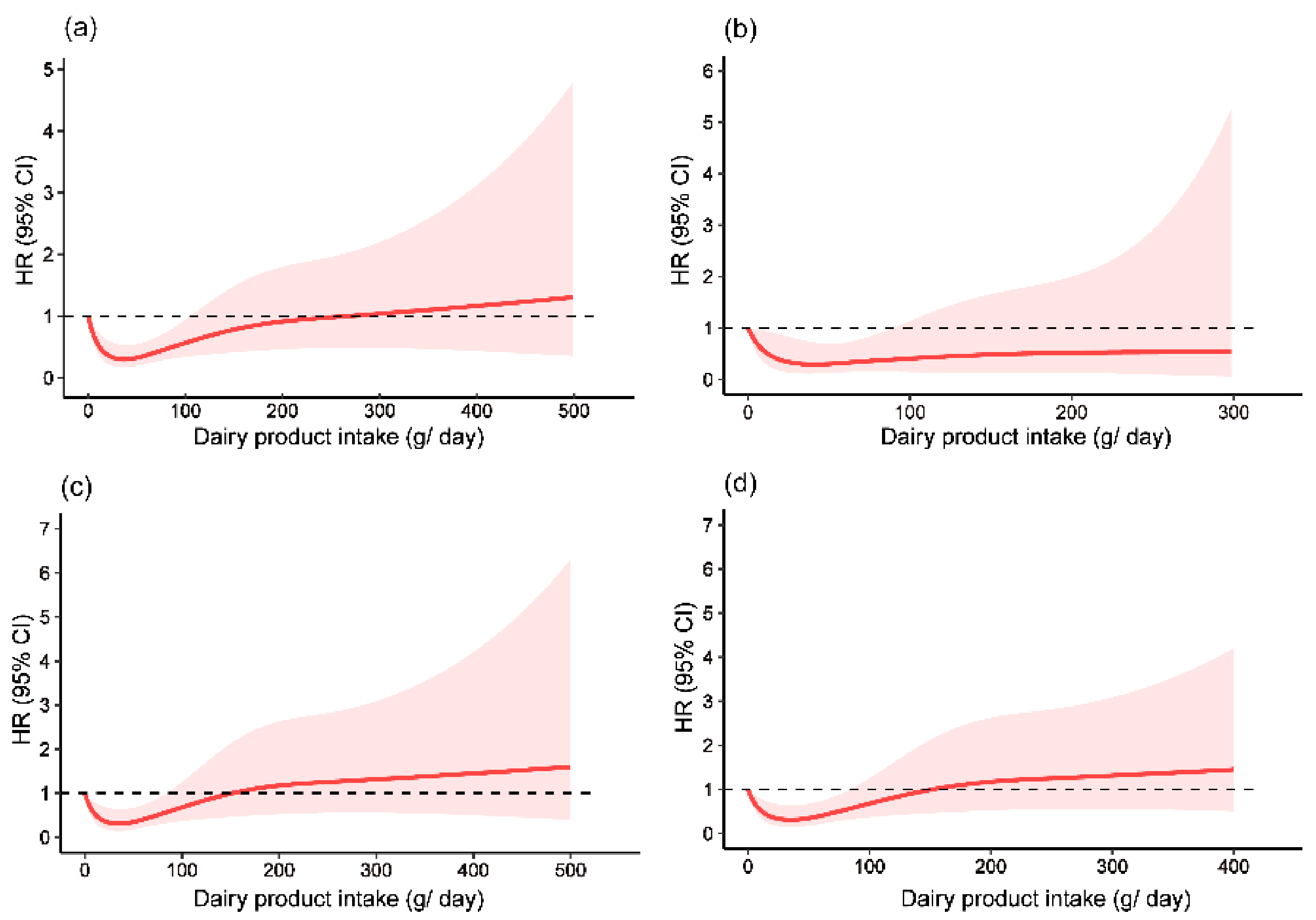
3.4. Nonlinear Associations between Dairy Product Intake and the Risk of Fracture
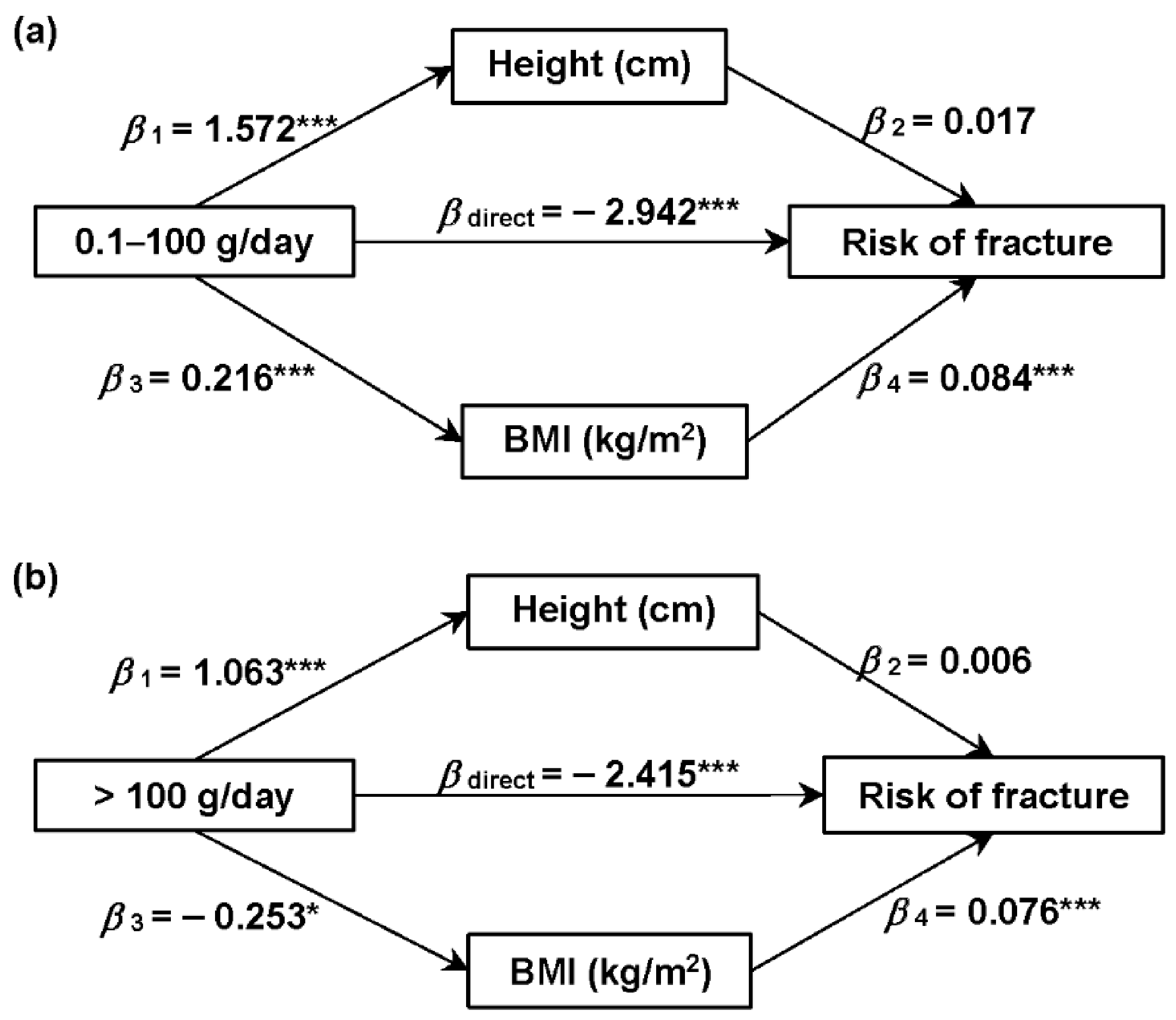
3.5. Mediation Effects of Height and BMI on the Associations between Dairy Product Intake and the Risk of Fracture
4. Discussion
4.1. Association between Dairy Product Intake and the Risk of Fracture
4.2. The Associations of Calcium and Protein in Dairy Products with the Risk of Fracture
4.3. The Appropriate Dairy Product Intake for Chinses Adults
4.4. The Mediation Effects of Height and BMI on the Associations between Dairy Products and the Risk of Fracture
4.5. Strengths and Limitations
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Wu, A.M.; Bisignano, C.; James, S.L.; Abady, G.G.; Abedi, A.; Abu-Gharbieh, E.; Alhassan, R.K.; Alipour, V.; Arabloo, J.; Asaad, M.; et al. Global, Regional, and National Burden of Bone Fractures in 204 Countries and Territories, 1990–2019: A Systematic Analysis from the Global Burden of Disease Study 2019. Lancet Healthy Longev. 2021, 2, e580–e592. [Google Scholar] [CrossRef]
- Si, L.; Winzenberg, T.M.; Jiang, Q.; Chen, M.; Palmer, A.J. Projection of Osteoporosis-Related Fractures and Costs in China: 2010–2050. Osteoporos. Int. 2015, 26, 1929–1937. [Google Scholar] [CrossRef] [PubMed]
- Si, L.; Winzenberg, T.M.; Chen, M.; Jiang, Q.; Palmer, A.J. Residual Lifetime and 10 Year Absolute Risks of Osteoporotic Fractures in Chinese Men and Women. Curr. Med. Res. Opin. 2015, 31, 1149–1156. [Google Scholar] [CrossRef] [PubMed]
- Drewnowski, A.; Fulgoni, V. Nutrient Profiling of Foods: Creating a Nutrient-Rich Food Index. Nutr. Rev. 2008, 66, 23–39. [Google Scholar] [CrossRef] [PubMed]
- Austialian Government. Australian Dietary Guidelines. Available online: https://www.eatforhealth.gov.au/guidelines/australian-dietary-guidelines-1-5 (accessed on 27 June 2013).
- Chinese Nutrition Society. Chinese Dietary Guideline (2016), 1st ed.; People’s Medical Publishing House: Beijing, China, 2016. [Google Scholar]
- U.S. Department of Agriculture; U.S. Department of Health and Human Services. Dietary Guidelines for Americans, 2020–2025. Available online: https://www.dietaryguidelines.gov/ (accessed on 27 June 2020).
- Thorning, T.K.; Raben, A.; Tholstrup, T.; Soedamah-Muthu, S.S.; Givens, I.; Astrup, A. Milk and Dairy Products: Good or Bad for Human Health? An Assessment of the Totality of Scientific Evidence. Food Nutr. Res. 2016, 60, 32527. [Google Scholar] [CrossRef] [PubMed]
- Na, X.; Lan, H.; Wang, Y.; Tan, Y.; Zhang, J.; Zhao, A. Association between Milk Intake and All-Cause Mortality among Chinese Adults: A Prospective Study. Nutrients 2022, 14, 292. [Google Scholar] [CrossRef] [PubMed]
- Michaëlsson, K.; Wolk, A.; Langenskiöld, S.; Basu, S.; Lemming, E.W.; Melhus, H.; Byberg, L. Milk Intake and Risk of Mortality and Fractures in Women and Men: Cohort Studies. BMJ 2014, 349, g6015. [Google Scholar] [CrossRef]
- Iuliano, S.; Hill, T.R. Dairy Foods and Bone Health Throughout the Lifespan: A Critical Appraisal of the Evidence. Br. J. Nutr. 2019, 121, 763–772. [Google Scholar] [CrossRef]
- Malmir, H.; Larijani, B.; Esmaillzadeh, A. Consumption of Milk and Dairy Products and Risk of Osteoporosis and Hip Fracture: A Systematic Review and Meta-Analysis. Crit. Rev. Food Sci. Nutr. 2020, 60, 1722–1737. [Google Scholar] [CrossRef]
- Wallace, T.C.; Jun, S.; Zou, P.; McCabe, G.P.; Craig, B.A.; Cauley, J.A.; Weaver, C.M.; Bailey, R.L. Dairy Intake Is Not Associated with Improvements in Bone Mineral Density or Risk of Fractures across the Menopause Transition: Data from the Study of Women’s Health across the Nation. Menopause 2020, 27, 879–886. [Google Scholar] [CrossRef]
- Włodarek, D.; Głąbska, D.; Kołota, A.; Adamczyk, P.; Czekajło, A.; Grzeszczak, W.; Drozdzowska, B.; Pluskiewicz, W. Calcium Intake and Osteoporosis: The Influence of Calcium Intake from Dairy Products on Hip Bone Mineral Density and Fracture Incidence—A Population-Based Study in Women over 55 Years of Age. Public Health Nutr. 2014, 17, 383–389. [Google Scholar] [CrossRef]
- Bian, S.; Hu, J.; Zhang, K.; Wang, Y.; Yu, M.; Ma, J. Dairy Product Consumption and Risk of Hip Fracture: A Systematic Review and Meta-Analysis. BMC Public Health 2018, 18, 165. [Google Scholar] [CrossRef]
- Fardellone, P. The Effect of Milk Consumption on Bone and Fracture Incidence, an Update. Aging Clin. Exp. Res. 2019, 31, 759–764. [Google Scholar] [CrossRef]
- Aslam, H.; Holloway-Kew, K.L.; Mohebbi, M.; Jacka, F.N.; Pasco, J.A. Association between Dairy Intake and Fracture in an Australian-Based Cohort of Women: A Prospective Study. BMJ Open 2019, 9, e031594. [Google Scholar] [CrossRef]
- Michaëlsson, K.; Wolk, A.; Lemming, E.W.; Melhus, H.; Byberg, L. Intake of Milk or Fermented Milk Combined with Fruit and Vegetable Consumption in Relation to Hip Fracture Rates: A Cohort Study of Swedish Women. J. Bone Miner. Res. 2018, 33, 449–457. [Google Scholar] [CrossRef]
- Benetou, V.; Orfanos, P.; Zylis, D.; Sieri, S.; Contiero, P.; Tumino, R.; Giurdanella, M.C.; Peeters, P.H.; Linseisen, J.; Nieters, A.; et al. Diet and Hip Fractures among Elderly Europeans in the Epic Cohort. Eur. J. Clin. Nutr. 2011, 65, 132–139. [Google Scholar] [CrossRef]
- Willett, W.C.; Ludwig, D.S. Milk and Health. N. Engl. J. Med. 2020, 382, 644–654. [Google Scholar] [CrossRef]
- Armstrong, M.E.; Kirichek, O.; Cairns, B.J.; Green, J.; Reeves, G.K. Relationship of Height to Site-Specific Fracture Risk in Postmenopausal Women. J. Bone Miner. Res. 2016, 31, 725–731. [Google Scholar] [CrossRef]
- Wang, L.; Yin, L.; Cheng, X.; Li, K.; Wang, Y.; Zhang, Y.; Duanmu, Y.Y.; Liu, X.; Deng, G.; Wang, Y.; et al. The Association of Calcium Intake with Osteoporotic Vertebral Fractures in a Large Chinese Cohort. Aging 2020, 12, 5500–5515. [Google Scholar] [CrossRef]
- Dehghan, M.; Mente, A.; Rangarajan, S.; Sheridan, P.; Mohan, V.; Iqbal, R.; Gupta, R.; Lear, S.; Wentzel-Viljoen, E.; Avezum, A.; et al. Association of Dairy Intake with Cardiovascular Disease and Mortality in 21 Countries from Five Continents (Pure): A Prospective Cohort Study. Lancet 2018, 392, 2288–2297. [Google Scholar] [CrossRef]
- University of North Carolina; Chinese Center for Disease Control and Prevention. China Health and Nutrition Survey. Available online: https://www.cpc.unc.edu/projects/china (accessed on 27 June 2015).
- Iuliano, S.; Poon, S.; Robbins, J.; Bui, M.; Wang, X.; de Groot, L.; van Loan, M.; Zadeh, A.G.; Nguyen, T.; Seeman, E. Effect of Dietary Sources of Calcium and Protein on Hip Fractures and Falls in Older Adults in Residential Care: Cluster Randomised Controlled Trial. BMJ 2021, 375, n2364. [Google Scholar] [CrossRef] [PubMed]
- Wang, G.Y. China Food Composition 1991; Peking University Medical Press: Beijing, China, 1991. [Google Scholar]
- Yang, Y.X.; Wang, G.Y.; Pan, X.C. China Food Composition 2002; Peking University Medical Press: Beijing, China, 2002. [Google Scholar]
- Xin, Y.Y. China Food Composition 2004; Peking University Medical Press: Beijing, China, 2005. [Google Scholar]
- Ainsworth, B.E.; Haskell, W.L.; Whitt, M.C.; Irwin, M.L.; Swartz, A.M.; Strath, S.J.; O’Brien, W.L.; Bassett, D.R., Jr.; Schmitz, K.H.; Emplaincourt, P.O.; et al. Compendium of Physical Activities: An Update of Activity Codes and Met Intensities. Med. Sci. Sports Exerc. 2000, 32, S498–S504. [Google Scholar] [CrossRef] [PubMed]
- Kemi, V.E.; Kärkkäinen, M.U.; Rita, H.J.; Laaksonen, M.M.; Outila, T.A.; Lamberg-Allardt, C.J. Low Calcium:Phosphorus Ratio in Habitual Diets Affects Serum Parathyroid Hormone Concentration and Calcium Metabolism in Healthy Women with Adequate Calcium Intake. Br. J. Nutr. 2010, 103, 561–568. [Google Scholar] [CrossRef] [PubMed]
- Lee, K.J.; Kim, K.S.; Kim, H.N.; Seo, J.A.; Song, S.W. Association between Dietary Calcium and Phosphorus Intakes, Dietary Calcium/Phosphorus Ratio and Bone Mass in the Korean Population. Nutr. J. 2014, 13, 114. [Google Scholar] [CrossRef]
- Feskanich, D.; Willett, W.C.; Colditz, G.A. Calcium, Vitamin D, Milk Consumption, and Hip Fractures: A Prospective Study among Postmenopausal Women. Am. J. Clin. Nutr. 2003, 77, 504–511. [Google Scholar] [CrossRef]
- Sahni, S.; Tucker, K.L.; Kiel, D.P.; Quach, L.; Casey, V.A.; Hannan, M.T. Milk and Yogurt Consumption Are Linked with Higher Bone Mineral Density but Not with Hip Fracture: The Framingham Offspring Study. Arch Osteoporos 2013, 8, 119. [Google Scholar] [CrossRef][Green Version]
- Hiligsmann, M.; Burlet, N.; Fardellone, P.; Al-Daghri, N.; Reginster, J.Y. Public Health Impact and Economic Evaluation of Vitamin D-Fortified Dairy Products for Fracture Prevention in France. Osteoporos. Int. 2017, 28, 833–840. [Google Scholar] [CrossRef]
- Holvik, K.; Meyer, H.E.; Laake, I.; Feskanich, D.; Omsland, T.K.; Søgaard, A.J. Milk Drinking and Risk of Hip Fracture: The Norwegian Epidemiologic Osteoporosis Studies (Norepos). Br. J. Nutr. 2019, 121, 709–718. [Google Scholar] [CrossRef]
- Sahni, S.; Mangano, K.M.; Tucker, K.L.; Kiel, D.P.; Casey, V.A.; Hannan, M.T. Protective Association of Milk Intake on the Risk of Hip Fracture: Results from the Framingham Original Cohort. J. Bone Miner. Res. 2014, 29, 1756–1762. [Google Scholar] [CrossRef]
- Feskanich, D.; Meyer, H.E.; Fung, T.T.; Bischoff-Ferrari, H.A.; Willett, W.C. Milk and Other Dairy Foods and Risk of Hip Fracture in Men and Women. Osteoporos. Int. 2018, 29, 385–396. [Google Scholar] [CrossRef]
- Cui, X.; Wang, L.; Zuo, P.; Han, Z.; Fang, Z.; Li, W.; Liu, J. D-Galactose-Caused Life Shortening in Drosophila Melanogaster and Musca Domestica Is Associated with Oxidative Stress. Biogerontology 2004, 5, 317–325. [Google Scholar] [CrossRef]
- Cui, X.; Zuo, P.; Zhang, Q.; Li, X.; Hu, Y.; Long, J.; Packer, L.; Liu, J. Chronic Systemic D-Galactose Exposure Induces Memory Loss, Neurodegeneration, and Oxidative Damage in Mice: Protective Effects of R-Alpha-Lipoic Acid. J. Neurosci. Res. 2006, 84, 647–654. [Google Scholar] [CrossRef]
- Hao, L.; Huang, H.; Gao, J.; Marshall, C.; Chen, Y.; Xiao, M. The Influence of Gender, Age and Treatment Time on Brain Oxidative Stress and Memory Impairment Induced by D-Galactose in Mice. Neurosci. Lett. 2014, 571, 45–49. [Google Scholar] [CrossRef]
- Wang, Y.; Jia, X.; Du, W.; Wang, Z.; Wang, H.; Zhang, B. Dairy Consumption Characteristics among Chinese Adult Residents from 1989 to 2011. Wei Sheng Yan Jiu 2017, 46, 409–433. [Google Scholar]
- Weaver, C.M. Milk Consumption and Bone Health. JAMA Pediatrics 2014, 168, 12–13. [Google Scholar] [CrossRef]
- FAO. The State of Food Insecurity in the World 2015. Meeting the 2015 International Hunger Targets: Taking Stock of Uneven Progress; FAO: Rome, Italy, 2015. [Google Scholar]
- Balk, E.M.; Adam, G.P.; Langberg, V.N.; Earley, A.; Clark, P.; Ebeling, P.R.; Mithal, A.; Rizzoli, R.; Zerbini, C.A.F.; Pierroz, D.D.; et al. Global Dietary Calcium Intake among Adults: A Systematic Review. Osteoporos. Int. 2017, 28, 3315–3324. [Google Scholar] [CrossRef]
- Timon, C.M.; O’Connor, A.; Bhargava, N.; Gibney, E.R.; Feeney, E.L. Dairy Consumption and Metabolic Health. Nutrients 2020, 12, 3040. [Google Scholar] [CrossRef]
- Hidayat, K.; Chen, J.S.; Wang, T.C.; Liu, Y.J.; Shi, Y.J.; Su, H.W.; Liu, B.; Qin, L.Q. The Effects of Milk Supplementation on Bone Health Indices in Adults: A Meta-Analysis of Randomized Controlled Trials. Adv. Nutr. 2021, 2021, nmab136. [Google Scholar] [CrossRef]
- Bonjour, J.P.; Ammann, P.; Chevalley, T.; Rizzoli, R. Protein Intake and Bone Growth. Can. J. Appl. Physiol. 2001, 26, S153–S166. [Google Scholar] [CrossRef]
- Kerstetter, J.E.; Kenny, A.M.; Insogna, K.L. Dietary Protein and Skeletal Health: A Review of Recent Human Research. Curr. Opin. Lipidol. 2011, 22, 16–20. [Google Scholar] [CrossRef]
- Matkovic, V.; Heaney, R.P. Calcium Balance During Human Growth: Evidence for Threshold Behavior. Am. J. Clin. Nutr. 1992, 55, 992–996. [Google Scholar] [CrossRef] [PubMed]
- Fang, A.; Li, K.; Shi, H.; He, J.; Li, H. Calcium Requirements for Chinese Adults by Cross-Sectional Statistical Analyses of Calcium Balance Studies: An Individual Participant Data and Aggregate Data Meta-Regression. Chin. Med. J. 2014, 127, 4250–4257. [Google Scholar]
- Talaei, M.; Pan, A.; Yuan, J.M.; Koh, W.P. Dairy Intake and Risk of Type 2 Diabetes. Clin. Nutr. 2018, 37, 712–718. [Google Scholar] [CrossRef] [PubMed]
- Wang, X.J.; Jiang, C.Q.; Zhang, W.S.; Zhu, F.; Jin, Y.L.; Woo, J.; Cheng, K.K.; Lam, T.H.; Xu, L. Milk Consumption and Risk of Mortality from All-Cause, Cardiovascular Disease and Cancer in Older People. Clin. Nutr. 2020, 39, 3442–3451. [Google Scholar] [CrossRef] [PubMed]
- Feskanich, D.; Bischoff-Ferrari, H.A.; Frazier, A.L.; Willett, W.C. Milk Consumption During Teenage Years and Risk of Hip Fractures in Older Adults. JAMA Pediatrics 2014, 168, 54–60. [Google Scholar] [CrossRef]
- De Laet, C.; Kanis, J.A.; Odén, A.; Johanson, H.; Johnell, O.; Delmas, P.; Eisman, J.A.; Kroger, H.; Fujiwara, S.; Garnero, P.; et al. Body Mass Index as a Predictor of Fracture Risk: A Meta-Analysis. Osteoporos. Int. 2005, 16, 1330–1338. [Google Scholar] [CrossRef]
- Wilkinson, K.R.; Tucker, L.A.; Davidson, L.E.; Bailey, B.W. Milk-Fat Intake and Differences in Abdominal Adiposity and Bmi: Evidence Based on 13,544 Randomly-Selected Adults. Nutrients 2021, 13, 1832. [Google Scholar] [CrossRef] [PubMed]
- Mendelian Randomization of Dairy Consumption Working Group. Dairy Consumption and Body Mass Index among Adults: Mendelian Randomization Analysis of 184802 Individuals from 25 Studies. Clin. Chem. 2018, 64, 183–191. [Google Scholar] [CrossRef]
- Guo, J.; Dougkas, A.; Elwood, P.C.; Givens, D.I. Dairy Foods and Body Mass Index over 10-Year: Evidence from the Caerphilly Prospective Cohort Study. Nutrients 2018, 10, 1515. [Google Scholar] [CrossRef]
- Compston, J.E.; Flahive, J.; Hosmer, D.W.; Watts, N.B.; Siris, E.S.; Silverman, S.; Saag, K.G.; Roux, C.; Rossini, M.; Pfeilschifter, J.; et al. Relationship of Weight, Height, and Body Mass Index with Fracture Risk at Different Sites in Postmenopausal Women: The Global Longitudinal Study of Osteoporosis in Women (Glow). J. Bone Miner. Res. 2014, 29, 487–493. [Google Scholar] [CrossRef]
- Chan, M.Y.; Frost, S.A.; Center, J.R.; Eisman, J.A.; Nguyen, T.V. Relationship between Body Mass Index and Fracture Risk Is Mediated by Bone Mineral Density. J. Bone Miner. Res. 2014, 29, 2327–2335. [Google Scholar] [CrossRef]
- Huang, H.L.; Pan, C.C.; Hsiao, Y.F.; Chen, M.C.; Kung, C.Y.; Kung, P.T.; Tsai, W.C. Associations of Body Mass Index and Diabetes with Hip Fracture Risk: A Nationwide Cohort Study. BMC Public Health 2018, 18, 1325. [Google Scholar] [CrossRef]
- Montazerifar, F.; Karajibani, M.; Alamian, S.; Sandoughi, M.; Zakeri, Z.; Dashipour, A.R. Age, Weight and Body Mass Index Effect on Bone Mineral Density in Postmenopausal Women. Health Scope 2014, 3, e14075. [Google Scholar] [CrossRef]
- Naghshi, S.; Sadeghi, O.; Larijani, B.; Esmaillzadeh, A. High Vs. Low-Fat Dairy and Milk Differently Affects the Risk of All-Cause, Cvd, and Cancer Death: A Systematic Review and Dose-Response Meta-Analysis of Prospective Cohort Studies. Crit. Rev. Food Sci. Nutr. 2021, 1–15. [Google Scholar] [CrossRef]
- van Aerde, M.A.; Soedamah-Muthu, S.S.; Geleijnse, J.M.; Snijder, M.B.; Nijpels, G.; Stehouwer, C.D.; Dekker, J.M. Dairy Intake in Relation to Cardiovascular Disease Mortality and All-Cause Mortality: The Hoorn Study. Eur. J. Nutr. 2013, 52, 609–616. [Google Scholar] [CrossRef]
- Um, C.Y.; Judd, S.E.; Flanders, W.D.; Fedirko, V.; Bostick, R.M. Associations of Calcium and Dairy Products with All-Cause and Cause-Specific Mortality in the Reasons for Geographic and Racial Differences in Stroke (Regards) Prospective Cohort Study. Nutr. Cancer 2017, 69, 1185–1195. [Google Scholar] [CrossRef]
| Overall Participants | |||||
|---|---|---|---|---|---|
| No Consumption | 0.1–100 g/Day | >100 g/Day | p | ||
| (n = 11,768) | (n = 2041) | (n = 902) | |||
| Age at baseline (years) | 41.0 (31.0, 53.0) | 43.0 (33.0, 55.0) | 51.0 (38.0, 61.0) | <0.001 | |
| Sex | 0.001 | ||||
| Men | 5595 (81.3) | 911 (13.2) | 378 (5.49) | ||
| Women | 6173 (78.9) | 1130 (14.4) | 524 (6.69) | ||
| Education level | <0.001 | ||||
| Junior high school or below | 2455 (61.6) | 976 (24.5) | 557 (14.0) | ||
| Senior high school or above | 9313 (86.9) | 1065 (9.93) | 345 (3.22) | ||
| Region of residence | <0.001 | ||||
| Eastern region | 3820 (68.0) | 1086 (19.3) | 710 (12.6) | ||
| Central region | 4693 (86.1) | 688 (12.6) | 69 (1.27) | ||
| Western region | 3255 (89.3) | 267 (7.33) | 123 (3.37) | ||
| Place of residence | <0.001 | ||||
| Urban area | 3398 (61.5) | 1386 (25.1) | 742 (13.4) | ||
| Rural area | 8370 (91.1) | 655 (7.13) | 160 (1.74) | ||
| Individual annual income (yuan) | 6347 (2721, 13,137) | 10,131 (5738, 18,000) | 21,000 (12,973, 31,858) | <0.001 | |
| Smoking history | <0.001 | ||||
| No | 7994 (78.8) | 1446 (14.2) | 708 (6.98) | ||
| Yes | 3773 (82.7) | 594 (13.0) | 193 (4.23) | ||
| Drinking history | <0.001 | ||||
| No | 7689 (80.5) | 1248 (13.1) | 611 (6.40) | ||
| Yes | 4079 (79.0) | 793 (15.4) | 291 (5.64) | ||
| BMI (kg/m2) | 22.8 (20.9, 25.1) | 23.4 (21.4, 25.7) | 23.5 (21.4, 25.8) | <0.001 | |
| Chronic disease history | <0.001 | ||||
| No | 8752 (81.6) | 1374 (12.8) | 603 (5.62) | ||
| Yes | 3016 (75.7) | 667 (16.8) | 299 (7.51) | ||
| Physical activity (MET-hour/week) | 132 (0.00, 614) | 180 (11.6, 605) | 501 (117, 1266) | <0.001 | |
| Intake of total energy (kcal/day) | 2094 (1766, 2437) | 2047 (1754, 2333) | 1885 (1554, 2217) | <0.001 | |
| Intake of total calcium (mg/day) | 342 (271, 432) | 411 (337, 503) | 584 (471, 732) | <0.001 | |
| Intake of calcium in dairy products (mg/day) | 0.00 (0.00, 0.00) | 39.3 (15.7, 69.3) | 173 (139, 236) | <0.001 | |
| Men | |||||
| No consumption | 0.1–100 g/Day | >100 g/Day | p | ||
| (n = 5595) | (n = 911) | (n = 378) | |||
| Age at baseline (years) | 42.0 (31.0, 53.0) | 44.0 (34.0, 55.0) | 54.0 (39.0, 64.0) | <0.001 | |
| Education level | <0.001 | ||||
| Junior high school or below | 1407 (65.9) | 471 (22.1) | 256 (12.0) | ||
| Senior high school or above | 4188 (88.2) | 440 (9.26) | 122 (2.57) | ||
| Region of residence | <0.001 | ||||
| Eastern region | 1832 (69.7) | 489 (18.6) | 307 (11.7) | ||
| Central region | 2221 (86.9) | 305 (11.9) | 29 (1.14) | ||
| Western region | 1542 (90.7) | 117 (6.88) | 42 (2.47) | ||
| Place of residence | <0.001 | ||||
| Urban area | 1630 (63.5) | 619 (24.1) | 316 (12.3) | ||
| Rural area | 3965 (91.8) | 292 (6.76) | 62 (1.44) | ||
| Individual annual income (yuan) | 11,866 (6770, 20,281) | 24,000 (14,118, 36,917) | <0.001 | ||
| Smoking history | <0.001 | ||||
| No | 2048 (78.3) | 365 (14.0) | 203 (7.76) | ||
| Yes | 3547 (83.1) | 545 (12.8) | 175 (4.10) | ||
| Drinking history | <0.001 | ||||
| No | 2086 (82.2) | 284 (11.2) | 168 (6.62) | ||
| Yes | 3509 (80.7) | 627 (14.4) | 210 (4.83) | ||
| BMI (kg/m2) | 23.9 (21.7, 25.8) | 23.9 (22.0, 26.0) | <0.001 | ||
| Chronic disease history | <0.001 | ||||
| No | 4152 (83.4) | 590 (11.9) | 235 (4.72) | ||
| Yes | 1443 (75.7) | 321 (16.8) | 143 (7.50) | ||
| Physical activity (MET-hour/week) | 7.70 (0.00, 282) | 40.8 (0.00, 347) | 274 (23.4, 1054) | <0.001 | |
| Intake of total energy (kcal/day) | 2299 (1968, 2628) | 2245 (1955, 2535) | 2069 (1746, 2405) | <0.001 | |
| Intake of total calcium (mg/day) | 363 (290, 458) | 439 (359, 531) | 606 (501, 751) | <0.001 | |
| Intake of calcium in dairy products (mg/day) | 0.00 (0.00, 0.00) | 38.7 (14.7, 69.3) | 173 (136, 235) | <0.001 | |
| Women | |||||
| No consumption | 0.1–100 g/Day | >100 g/Day | p | ||
| (n = 6173) | (n = 1130) | (n = 524) | |||
| Age at baseline (years) | 41.0 (30.0, 53.0) | 43.0 (32.0, 54.0) | 48.0 (37.0, 60.0) | <0.001 | |
| Education level | <0.001 | ||||
| Junior high school or below | 1048 (56.5) | 505 (27.2) | 301 (16.2) | ||
| Senior high school or above | 5125 (85.8) | 625 (10.5) | 223 (3.73) | ||
| Region of residence | <0.001 | ||||
| Eastern region | 1988 (66.5) | 597 (20.0) | 403 (13.5) | ||
| Central region | 2472 (85.4) | 383 (13.2) | 40 (1.38) | ||
| Western region | 1713 (88.1) | 150 (7.72) | 81 (4.17) | ||
| Place of residence | |||||
| Urban area | 1768 (59.7) | 767 (25.9) | 426 (14.4) | ||
| Rural area | 4405 (90.5) | 363 (7.46) | 98 (2.01) | ||
| Individual annual income (yuan) | 5455 (2327, 11,121) | 8955 (5000, 15,526) | 19,000 (11,549, 28,859) | <0.001 | |
| Smoking history | 0.51 | ||||
| No | 5946 (78.9) | 1081 (14.4) | 505 (6.70) | ||
| Yes | 226 (77.1) | 49 (16.7) | 18 (6.14) | ||
| Drinking history | <0.001 | ||||
| No | 5603 (79.9) | 964 (13.8) | 443 (6.32) | ||
| Yes | 570 (69.8) | 166 (20.3) | 81 (9.91) | ||
| BMI (kg/m2) | 22.8 (20.9, 25.2) | 23.2 (21.2, 25.6) | 23.0 (21.0, 25.5) | 0.007 | |
| Chronic disease history | <0.001 | ||||
| No | 4600 (80.0) | 784 (13.6) | 368 (6.40) | ||
| Yes | 1573 (75.8) | 346 (16.7) | 156 (7.52) | ||
| Physical activity (Met-hour/week) | 222 (101, 917) | 233 (126, 750) | 591 (204, 1398) | <0.001 | |
| Intake of total energy (kcal/day) | 1937 (1651, 2223) | 1885 (1652, 2146) | 1769 (1462, 2075) | <0.001 | |
| Intake of total calcium (mg/day) | 323 (258, 408) | 392 (320, 475) | 551 (459, 723) | <0.001 | |
| Intake of calcium in dairy products (mg/day) | 0.00 (0.00, 0.00) | 39.6 (17.3, 69.3) | 173 (139, 236) | <0.001 | |
| No Consumption | 0.1–100 g/Day | >100 g/Day | |
|---|---|---|---|
| (n = 11,768) | (n = 2041) | (n = 902) | |
| Overall Participants | |||
| Incidence (no. of fractures/ 1000 person-years) | 3.750 | 1.904 | 1.861 |
| Unadjusted Model | 1.00 (Reference) | 0.50 (0.36, 0.69) *** | 0.54 (0.29, 1.02) |
| Model 1 | 1.00 (Reference) | 0.38 (0.27, 0.53) *** | 0.32 (0.16, 0.64) ** |
| Model 2 | 1.00 (Reference) | 0.49 (0.34, 0.70) *** | 0.65 (0.33, 1.32) |
| Men | |||
| Incidence (no. of fractures/ 1000 person-years) | 3.743 | 1.045 | 0.866 |
| Unadjusted Model | 1.00 (Reference) | 0.27 (0.14, 0.52) *** | 0.24 (0.06, 0.97) * |
| Model 1 | 1.00 (Reference) | 0.23 (0.12, 0.45) *** | 0.17 (0.04, 0.72) * |
| Model 2 | 1.00 (Reference) | 0.32 (0.17, 0.62) ** | 0.36 (0.09, 1.50) |
| Women | |||
| Incidence (no. of fractures/ 1000 person-years) | 3.757 | 2.622 | 2.610 |
| Unadjusted Model | 1.00 (Reference) | 0.69 (0.47, 1.01) | 0.79 (0.39, 1.61) |
| Model 1 | 1.00 (Reference) | 0.50 (0.33, 0.76) ** | 0.44 (0.20, 0.96) * |
| Model 2 | 1.00 (Reference) | 0.62 (0.40, 0.96) * | 0.80 (0.35, 1.83) |
| No Consumption | 0.1–70 mg/Day | >70 mg/Day | |
|---|---|---|---|
| (n = 11,777) | (n = 1426) | (n = 1508) | |
| Overall Participants | |||
| Incidence (no. of fractures/ 1000 person-years) | 3.747 | 1.892 | 1.922 |
| Unadjusted Model | 1.00 (Reference) | 0.49 (0.34, 0.71) *** | 0.54 (0.34, 0.86) * |
| Model 1 | 1.00 (Reference) | 0.38 (0.26, 0.56) *** | 0.35 (0.21, 0.58) *** |
| Model 2 | 1.00 (Reference) | 0.39 (0.26, 0.58) *** | 0.35 (0.21, 0.59) *** |
| Model 3 | 1.00 (Reference) | 0.39 (0.27, 0.58) *** | 0.37 (0.22, 0.61) *** |
| Men | |||
| Incidence (no. of fractures/ 1000 person-years) | 3.740 | 1.078 | 0.909 |
| Unadjusted Model | 1.00 (Reference) | 0.28 (0.14, 0.57) *** | 0.25 (0.09, 0.67) ** |
| Model 1 | 1.00 (Reference) | 0.24 (0.12, 0.50) *** | 0.19 (0.07, 0.52) ** |
| Model 2 | 1.00 (Reference) | 0.25 (0.12, 0.51) *** | 0.19 (0.07, 0.53) ** |
| Model 3 | 1.00 (Reference) | 0.25 (0.12, 0.52) *** | 0.21 (0.07, 0.57) ** |
| Women | |||
| Incidence (no. of fractures/ 1000 person-years) | 3.753 | 2.567 | 2.734 |
| Unadjusted Model | 1.00 (Reference) | 0.67 (0.43, 1.02) | 0.81 (0.48, 1.37) |
| Model 1 | 1.00 (Reference) | 0.50 (0.32, 0.80) ** | 0.47 (0.26, 0.85) * |
| Model 2 | 1.00 (Reference) | 0.52 (0.32, 0.82) ** | 0.47 (0.26, 0.86) * |
| Model 3 | 1.00 (Reference) | 0.52 (0.32, 0.82) ** | 0.48 (0.27, 0.88) * |
| No Consumption | 0.1–2.8 g/Day | >2.8 g/Day | |
|---|---|---|---|
| (n = 11,777) | (n = 1956) | (n = 969) | |
| Overall Participants | |||
| Incidence (no. of fractures/ 1000 person-years) | 3.747 | 1.808 | 3.419 |
| Unadjusted Model | 1.00 (Reference) | 0.47 (0.34, 0.66) *** | 0.65 (0.37, 1.13) |
| Model 1 | 1.00 (Reference) | 0.37 (0.26, 0.53) *** | 0.37 (0.20, 0.68) ** |
| Model 2 | 1.00 (Reference) | 0.38 (0.27, 0.54) *** | 0.37 (0.20, 0.69) ** |
| Model 3 | 1.00 (Reference) | 0.38 (0.26, 0.54) *** | 0.37 (0.20, 0.69) ** |
| Men | |||
| Incidence (no. of fractures/ 1000 person-years) | 3.740 | 0.857 | 1.606 |
| Unadjusted Model | 1.00 (Reference) | 0.22 (0.11, 0.45) *** | 0.45 (0.17, 1.20) |
| Model 1 | 1.00 (Reference) | 0.19 (0.09, 0.40) *** | 0.33 (0.12, 0.92) * |
| Model 2 | 1.00 (Reference) | 0.20 (0.10, 0.41) *** | 0.33 (0.12, 0.92) * |
| Model 3 | 1.00 (Reference) | 0.20 (0.10, 0.41) *** | 0.34 (0.12, 0.96) * |
| Women | |||
| Incidence (no. of fractures/ 1000 person-years) | 3.753 | 2.606 | 2.712 |
| Unadjusted Model | 1.00 (Reference) | 0.69 (0.47, 1.01) | 0.82 (0.42, 1.61) |
| Model 1 | 1.00 (Reference) | 0.52 (0.35, 0.80) ** | 0.39 (0.18, 0.85) * |
| Model 2 | 1.00 (Reference) | 0.54 (0.35, 0.81) ** | 0.39 (0.18, 0.85) * |
| Model 3 | 1.00 (Reference) | 0.53 (0.35, 0.81) ** | 0.38 (0.17, 0.83) * |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Na, X.; Xi, Y.; Qian, S.; Zhang, J.; Yang, Y.; Zhao, A. Association between Dairy Product Intake and Risk of Fracture among Adults: A Cohort Study from China Health and Nutrition Survey. Nutrients 2022, 14, 1632. https://doi.org/10.3390/nu14081632
Na X, Xi Y, Qian S, Zhang J, Yang Y, Zhao A. Association between Dairy Product Intake and Risk of Fracture among Adults: A Cohort Study from China Health and Nutrition Survey. Nutrients. 2022; 14(8):1632. https://doi.org/10.3390/nu14081632
Chicago/Turabian StyleNa, Xiaona, Yuandi Xi, Sicheng Qian, Jian Zhang, Yucheng Yang, and Ai Zhao. 2022. "Association between Dairy Product Intake and Risk of Fracture among Adults: A Cohort Study from China Health and Nutrition Survey" Nutrients 14, no. 8: 1632. https://doi.org/10.3390/nu14081632
APA StyleNa, X., Xi, Y., Qian, S., Zhang, J., Yang, Y., & Zhao, A. (2022). Association between Dairy Product Intake and Risk of Fracture among Adults: A Cohort Study from China Health and Nutrition Survey. Nutrients, 14(8), 1632. https://doi.org/10.3390/nu14081632






