In the last two years, there has been a surge in the number of publications on the trace element selenium (Se) and selenocysteine-containing selenoproteins in human health, largely due to the pandemic and the multiple roles that this micronutrient and Se-dependent selenoproteins play in various aspects of the disease. In early 2020, two publications increased the attention on Se status in the context of SARS-CoV-2, namely, a population-based analysis correlating cure rates with baseline Se status in different regions of China [1], and an analysis of individual patients who did or did not survive COVID-19 [2]. Both studies indicated that Se deficiency was a risk factor for severe disease progression, poor recovery, and eventually COVID-19-related death. Soon, these findings were supported by several observational studies, e.g., on regional Se supply and severity of COVID-19 disease [3], on patients with comorbidities [4], or on patients with a parallel deficiency in zinc, the second most important immune-relevant trace element [5,6,7]. Overall, a picture emerged in which Se is an important parameter for COVID-19 disease progression and survival, and severe Se deficiency measured in blood serving as a potential indicator of target cell Se deficiency associated with organ system dysfunction and death (Figure 1A).
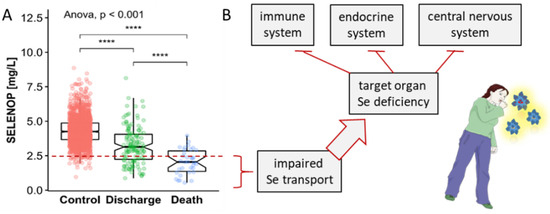
Figure 1.
Relationship between serum concentrations of the Se transporter selenoprotein P (SELENOP) and survival in COVID-19 and possible implications for Se supply to target organs and systemic defects. (A) Patients with COVID-19 display strongly reduced SELENOP concentrations compared to healthy adults (Controls). In particular, non-survivors (Death) showed very severe Se deficiency compared to survivors who left the hospital alive (Discharge). The red broken line indicates the 2.5th percentile of serum SELENOP as indicator of severe Se deficiency. (B) Severely reduced serum SELENOP concentrations indicate decreased Se transport to target organs, resulting in partial Se deficiency in the three major communication systems of the human organism, i.e., the immune, the endocrine and the central nervous system. The survival data have been published [2]. Spearman’s correlation test was applied (2-sided, 2-tailed), **** indicates p < 0.0001.
These results were not unexpected, as previous studies had pointed out the importance of Se status for the immune system and survival in critical illness [8]. The most solid data base for this essential link was provided by several studies in intensive care units, where Se deficiency was found to be an important predictor of severe disease course and sepsis-related mortality [9,10,11]. The underlying causes are not yet clear, but the negative acute-phase response of liver-derived selenoprotein P (SELENOP) and serum Se concentrations as biomarkers of poor systemic Se transport and target organ delivery appear to be related to the observed association between low circulating Se concentrations and unfavorable prognosis [12,13]. The strong decline in serum Se and SELENOP may directly lead to worsening disease, particularly in relation to the immune system [14], the endocrine system [15] and the central nervous system [16,17], where insufficiently low Se concentrations cause functional defects that can manifest in specific disease symptoms (Figure 1B).
It has been observed that severe Se deficiency due to pregnancy, inflammation or other conditions directly increases autoimmune disease risk [18,19,20]. The most conclusive data for this notion were obtained by comparing the incidence of autoimmune thyroid disease as a function of Se status [21], or thyroid disease prevalence in areas with low versus moderate baseline Se intake [22]. These observational findings have recently been supported by a focused molecular analysis of the role of the selenoprotein GPX4 in a specific severe autoimmune disease, i.e., systemic lupus erythematodes, in which downregulation of GPX4 gene transcription contributes to neutrophil ferroptosis as a key driver of neutropenia [23]. Similarly, humoral immunity has been shown to depend on follicular helper T-cells, which may undergo ferroptosis when GPX4 expression is low, leading to impaired immune responses to infection or vaccination in Se deficiency [24]. Importantly, these effects have been shown to be directly Se-dependent and seem preventable by Se supplementation, as demonstrated, e.g., in a well-conducted randomized controlled trial in pregnant women at risk of postpartum thyroiditis or by supplementation in COVID-19 patients, suggesting overall that severe Se deficiency is an addressable risk factor for long-term complications [25,26]. Whether this relationship also applies to COVID-19 and the long-COVID symptoms is not known, but currently seems plausible and requires experimental proof [20]. The observed Se deficiency in patients with COVID-19 may be secondary to increased inflammatory tone [27,28,29], hypoxia [30], and organ dysfunction [31,32,33], which develop in parallel and appear to worsen in those patients with poor prognosis [2].
Adequate Se status is not only a prerequisite for proper immune system functioning [34,35], but also of great importance for the central nervous system [16,36,37] and the endocrine control of energy and carbohydrate metabolism [38,39,40]. Pioneering work in some refined rodent model systems has shown that excess Se intake or transgenic overexpression of selenoproteins can impair glucose control, induce diabetes-like symptoms, and increase the risk of hyperglycemia [41,42]. Disruption of the regular peroxide-dependent signaling cascades by increased peroxidation appears to contribute to these defects [43,44]. Accordingly, a relationship between serum Se and insulin resistance has been reported from several observational studies. Thus, high Se status could impair normal insulin sensitivity, or conversely, circulating Se levels could be elevated in diabetes due to insulin resistance and elevation of hepatic SELENOP biosynthesis as a meaningful measure to protect from elevated circulating glucose levels. The latter explanation seems to be valid [45,46], as no increased type 2 diabetes mellitus risk was found in individuals taking Se supplements in the large supplementation studies [47]. Recent data from the NHANES III study, which analyzed the Se status of diabetic patients, suggest that serum Se concentrations correlate positively with life expectancy and protection from cardiovascular events [48]. Nevertheless, caution is mandatory as excessive supplemental Se intake can be toxic [49], and the use of very high therapeutic Se dosages may exceed the endogenous safety regulatory pathways that normally limit SELENOP biosynthesis to a certain maximum [50]. This may result in an oversupply of Se to target cells, which impairs regular peroxide-dependent signaling and leads to impaired control of insulin biosynthesis and insulin resistance.
The Se-dependent disruption of homeostatic control of carbohydrate metabolism can also be observed in the other direction, i.e., in Se deficiency. Marginal Se intake was linearly associated with hypoglycemia in a large observational study in China [51]. This surprising result provided a possible molecular and metabolic cause for poor survival in severe disease-related Se deficiency. Moreover, this notion accords with prior research on the association between Se deficiency as a risk factor for heart failure, cardiac events, and death from cardiovascular disease [52,53,54,55,56]. Therefore, new tools are needed to identify patients at risk for Se deficiency at an early stage, especially since Se intake cannot be reliably predicted or inferred from dietary habits [57,58]. Overall, the biological derangements resulting from severe Se deficiency are diverse and complex because multiple organ systems are involved, which interact, and the disorders develop dynamically (Figure 2).
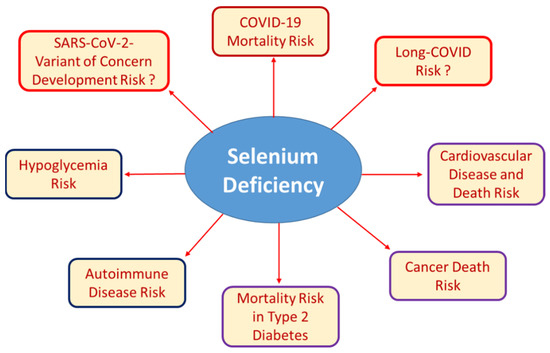
Figure 2.
Well-established and recently described associations of Se deficiency with certain health risks. Low Se status can result from insufficient nutritional supply, chronic disease, inflammation, infection, or as a result from pregnancy, surgery or other conditions of increased need. Severe Se deficiency is known to be associated with autoimmune disease and increased risk of mortality due to cancer, cardiovascular disease, or infection. Recent research has added hypoglycemia risk and poor survival of patients with COVID-19 or type 2 diabetes mellitus to the list of Se-dependent health issues. The importance of poor Se status for the development of SARS-CoV-2 variants of concern due to increased mutagenesis in Se-deficient hosts or for the development and resolution of long-COVID symptoms are other potential links, but respective studies and relevant data are not yet at hand.
Informative transgenic mouse models have highlighted the specific roles of individual selenoproteins causing some severe developmental, neurological, immunological, or metabolic phenotypes [59,60,61]. Similarly, rare human inherited diseases affecting regular selenoprotein biosynthesis have pinpointed some most relevant factors implicated in selenoprotein biosynthesis, and highlighted their association with developmental disorders, neuronal defects, infertility or the disruption of other regulatory pathways [62,63,64]. However, the problems we currently observe with COVID-19 rather result from acquired deficiencies due to the inflammatory disease and do not represent inherited or chronic defects. A similar severe decrease in circulating Se concentration has been observed before in severe sepsis [9] or at the end of pregnancy in areas of low Se supply [65]. Of note, all three conditions, i.e., COVID-19, sepsis and pregnancy, are associated with long-term sequelae and slow full recovery. It can take years to overcome sepsis [66], and similarly, pregnancy can directly cause permanent autoimmune disease [67,68] as well as chronic postpartum depression [69,70]. The supportive effects of supplemental administration of Se on mortality, progression, and recovery from sepsis are currently unclear [71], but positive studies have been reported [10]. Experience with Se in pregnancy is more consistent, and supplementation has been effective in preventing postpartum thyroiditis and postpartum depression [25,72,73]. The extent to which this experience can be extrapolated to COVID-19 and long-term impairment remains to be tested, but at least from experience, potential success in preventing severe Se deficiency during illness and convalescence seems likely, while adverse effects have not been reported when Se-deficient individuals were given adequate amounts of Se [46].
Knowledge of the role of Se in cancer, cardiovascular disease, and the other major non-communicable diseases is relatively solid and will expand further, in particular with respect to ageing [74,75,76], and by analytical studies applying several biomarkers of Se status in parallel [40,77,78]. Other important areas of future research include a better understanding of the Se status for fertility and early development, and the mechanisms of Se transport [31]. Recent reports indicate unexpectedly high variability of trace elements in the follicular fluid surrounding the maturing oocytes prior to ovulation [79], a direct relationship between Se concentration in amniotic fluid and development of small-for-gestational-age newborns [80], and an increased risk of a number of pregnancy complications in women with low Se levels in the first trimester [81]. The importance of iodine and thyroid hormones in these conditions and their homeostatic control is well established, and it seems imperative to give equal attention to the Se status.
Another urgent, remarkable, and well-characterized interaction between Se deficiency and COVID-19 involves the virus itself, i.e., its variability and mutation frequency. In some very elegant experiments, Melinda A. Beck’s group has demonstrated that Se-deficient host organisms provide a perfect environment for enhanced viral mutagenesis. Mice with low Se and vitamin E status or deficient of intracellular cytosolic glutathione peroxidase (GPX1) exhibited increased mutation rates of infectious viruses, allowing apathogenic viruses to evolve into highly pathogenic viral quasispecies, likely due to increased reactive oxygen species tone and consequent damages [82,83]. The extent to which Se deficiency in chronically ill, immunosuppressed or poorly supplied individuals contributes to the evolution of new variants of concern of the current SARS-CoV-2 virus remains to be investigated in the coming months [84]. Thus, again, efforts should be made to avoid severe Se deficiency on a population-wide scale and in individual at-risk patients to reduce the likelihood of increased mutagenesis and spread of new virus variants. However, it is unlikely that this can be achieved quickly and that the contribution of severe Se deficiency to pandemic spread and emergence of new viral strains can be directly attributed to low Se and causality demonstrated. From a personal point of view, actively avoiding Se deficiency through a wisely chosen diet or the use of dietary supplements seems to be a most sensible and efficient measure to reduce one’s health risks, to improve survival chances in disease and to avoid long-term sequelae after infection.
Funding
The research was supported by Deutsche Forschungsgemeinschaft (DFG), research unit FOR-2558 “TraceAge” (Scho 849/6-2), and CRC/TR 296 “Local control of TH action” (LocoTact, P17).
Acknowledgments
Intellectual support and essential motivation was provided by valuable and inspiring colleagues from the International Society for Selenium Research (ISSR).
Conflicts of Interest
L.S. holds shares of selenOmed GmbH, a company involved in Se status assessment and supplementation, and currently serves as president of the ISSR.
References
- Zhang, J.; Taylor, E.W.; Bennett, K.; Saad, R.; Rayman, M.P. Association between regional selenium status and reported outcome of COVID-19 cases in China. Am. J. Clin. Nutr. 2020, 111, 1297–1299. [Google Scholar] [CrossRef] [PubMed]
- Moghaddam, A.; Heller, R.A.; Sun, Q.; Seelig, J.; Cherkezov, A.; Seibert, L.; Hackler, J.; Seemann, P.; Diegmann, J.; Pilz, M.; et al. Selenium Deficiency Is Associated with Mortality Risk from COVID-19. Nutrients 2020, 12, 2098. [Google Scholar] [CrossRef]
- Zhang, H.Y.; Zhang, A.R.; Lu, Q.B.; Zhang, X.A.; Zhang, Z.J.; Guan, X.G.; Che, T.L.; Yang, Y.; Li, H.; Liu, W.; et al. Association between fatality rate of COVID-19 and selenium deficiency in China. BMC Infect. Dis. 2021, 21, 452. [Google Scholar] [CrossRef] [PubMed]
- Du Laing, G.; Petrovic, M.; Lachat, C.; De Boevre, M.; Klingenberg, G.J.; Sun, Q.; De Saeger, S.; De Clercq, J.; Ide, L.; Vandekerckhove, L.; et al. Course and Survival of COVID-19 Patients with Comorbidities in Relation to the Trace Element Status at Hospital Admission. Nutrients 2021, 13, 3304. [Google Scholar] [CrossRef]
- Heller, R.A.; Sun, Q.; Hackler, J.; Seelig, J.; Seibert, L.; Cherkezov, A.; Minich, W.B.; Seemann, P.; Diegmann, J.; Pilz, M.; et al. Prediction of survival odds in COVID-19 by zinc, age and selenoprotein P as composite biomarker. Redox Biol. 2021, 38, 101764. [Google Scholar] [CrossRef] [PubMed]
- Fromonot, J.; Gette, M.; Ben Lassoued, A.; Gueant, J.L.; Gueant-Rodriguez, R.M.; Guieu, R. Hypozincemia in the early stage of COVID-19 is associated with an increased risk of severe COVID-19. Clin. Nutr. 2021. [Google Scholar] [CrossRef] [PubMed]
- Skalny, A.V.; Timashev, P.S.; Aschner, M.; Aaseth, J.; Chernova, L.N.; Belyaev, V.E.; Grabeklis, A.R.; Notova, S.V.; Lobinski, R.; Tsatsakis, A.; et al. Serum Zinc, Copper, and Other Biometals Are Associated with COVID-19 Severity Markers. Metabolites 2021, 11, 244. [Google Scholar] [CrossRef]
- Hardy, G.; Hardy, I.; Manzanares, W. Selenium supplementation in the critically ill. Nutr. Clin. Pract. 2012, 27, 21–33. [Google Scholar] [CrossRef]
- Forceville, X.; Vitoux, D.; Gauzit, R.; Combes, A.; Lahilaire, P.; Chappuis, P. Selenium, systemic immune response syndrome, sepsis, and outcome in critically ill patients. Crit. Care Med. 1998, 26, 1536–1544. [Google Scholar] [CrossRef]
- Angstwurm, M.W.; Engelmann, L.; Zimmermann, T.; Lehmann, C.; Spes, C.H.; Abel, P.; Strauss, R.; Meier-Hellmann, A.; Insel, R.; Radke, J.; et al. Selenium in Intensive Care (SIC): Results of a prospective randomized, placebo-controlled, multiple-center study in patients with severe systemic inflammatory response syndrome, sepsis, and septic shock. Crit. Care Med. 2007, 35, 118–126. [Google Scholar] [CrossRef]
- Braunstein, M.; Kusmenkov, T.; Zuck, C.; Angstwurm, M.; Becker, N.P.; Bocker, W.; Schomburg, L.; Bogner-Flatz, V. Selenium and Selenoprotein P Deficiency Correlates With Complications and Adverse Outcome After Major Trauma. Shock 2020, 53, 63–70. [Google Scholar] [CrossRef] [PubMed]
- Nichol, C.; Herdman, J.; Sattar, N.; O’Dwyer, P.J.; St, J.O.R.D.; Littlejohn, D.; Fell, G. Changes in the concentrations of plasma selenium and selenoproteins after minor elective surgery: Further evidence for a negative acute phase response? Clin. Chem. 1998, 44, 1764–1766. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Renko, K.; Hofmann, P.J.; Stoedter, M.; Hollenbach, B.; Behrends, T.; Kohrle, J.; Schweizer, U.; Schomburg, L. Down-regulation of the hepatic selenoprotein biosynthesis machinery impairs selenium metabolism during the acute phase response in mice. FASEB J. 2009, 23, 1758–1765. [Google Scholar] [CrossRef] [PubMed]
- Avery, J.C.; Hoffmann, P.R. Selenium, Selenoproteins, and Immunity. Nutrients 2018, 10, 1203. [Google Scholar] [CrossRef] [Green Version]
- Kohrle, J.; Jakob, F.; Contempre, B.; Dumont, J.E. Selenium, the thyroid, and the endocrine system. Endocr. Rev. 2005, 26, 944–984. [Google Scholar] [CrossRef] [PubMed]
- Steinbrenner, H.; Sies, H. Selenium homeostasis and antioxidant selenoproteins in brain: Implications for disorders in the central nervous system. Arch. Biochem. Biophys. 2013, 536, 152–157. [Google Scholar] [CrossRef]
- Cardoso, B.R.; Roberts, B.R.; Bush, A.I.; Hare, D.J. Selenium, selenoproteins and neurodegenerative diseases. Metallomics 2015, 7, 1213–1228. [Google Scholar] [CrossRef] [Green Version]
- Hubalewska-Dydejczyk, A.; Duntas, L.; Gilis-Januszewska, A. Pregnancy, thyroid, and the potential use of selenium. Horm. Int. J. Endocrinol. Metab. 2020, 19, 47–53. [Google Scholar] [CrossRef] [Green Version]
- Filipowicz, D.; Majewska, K.; Kalantarova, A.; Szczepanek-Parulska, E.; Ruchala, M. The rationale for selenium supplementation in patients with autoimmune thyroiditis, according to the current state of knowledge. Endokrynol. Pol. 2021, 72, 153–162. [Google Scholar] [CrossRef]
- Schomburg, L. Selenium Deficiency Due to Diet, Pregnancy, Severe Illness, or COVID-19-A Preventable Trigger for Autoimmune Disease. Int. J. Mol. Sci. 2021, 22, 8532. [Google Scholar] [CrossRef]
- Derumeaux, H.; Valeix, P.; Castetbon, K.; Bensimon, M.; Boutron-Ruault, M.C.; Arnaud, J.; Hercberg, S. Association of selenium with thyroid volume and echostructure in 35-to 60-year-old French adults. Eur. J. Endocrinol. 2003, 148, 309–315. [Google Scholar] [CrossRef] [Green Version]
- Wu, Q.; Rayman, M.P.; Lv, H.J.; Schomburg, L.; Cui, B.; Gao, C.Q.; Chen, P.; Zhuang, G.H.; Zhang, Z.N.; Peng, X.G.; et al. Low Population Selenium Status Is Associated With Increased Prevalence of Thyroid Disease. J. Clin. Endocrinol. Metab. 2015, 100, 4037–4047. [Google Scholar] [CrossRef] [Green Version]
- Li, P.; Jiang, M.; Li, K.; Li, H.; Zhou, Y.; Xiao, X.; Xu, Y.; Krishfield, S.; Lipsky, P.E.; Tsokos, G.C.; et al. Glutathione peroxidase 4-regulated neutrophil ferroptosis induces systemic autoimmunity. Nat. Immunol. 2021, 22, 1107–1117. [Google Scholar] [CrossRef]
- Yao, Y.; Chen, Z.; Zhang, H.; Chen, C.; Zeng, M.; Yunis, J.; Wei, Y.; Wan, Y.; Wang, N.; Zhou, M.; et al. Selenium-GPX4 axis protects follicular helper T cells from ferroptosis. Nat. Immunol. 2021, 22, 1127–1139. [Google Scholar] [CrossRef]
- Negro, R.; Greco, G.; Mangieri, T.; Pezzarossa, A.; Dazzi, D.; Hassan, H. The influence of selenium supplementation on postpartum thyroid status in pregnant women with thyroid peroxidase autoantibodies. J. Clin. Endocrinol. Metab. 2007, 92, 1263–1268. [Google Scholar] [CrossRef]
- Notz, Q.; Herrmann, J.; Schlesinger, T.; Helmer, P.; Sudowe, S.; Sun, Q.; Hackler, J.; Roeder, D.; Lotz, C.; Meybohm, P.; et al. Clinical Significance of Micronutrient Supplementation in Critically Ill COVID-19 Patients with Severe ARDS. Nutrients 2021, 13, 2113. [Google Scholar] [CrossRef] [PubMed]
- Duntas, L.H. Selenium and Inflammation: Underlying Anti-inflammatory Mechanisms. Horm. Metab. Res. 2009, 41, 443–447. [Google Scholar] [CrossRef] [PubMed]
- Huang, Z.; Rose, A.H.; Hoffmann, P.R. The role of selenium in inflammation and immunity: From molecular mechanisms to therapeutic opportunities. Antioxid. Redox Signal. 2012, 16, 705–743. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Martitz, J.; Becker, N.P.; Renko, K.; Stoedter, M.; Hybsier, S.; Schomburg, L. Gene-specific regulation of hepatic selenoprotein expression by interleukin-6. Metallomics 2015, 7, 1515–1521. [Google Scholar] [CrossRef]
- Becker, N.P.; Martitz, J.; Renko, K.; Stoedter, M.; Hybsier, S.; Cramer, T.; Schomburg, L. Hypoxia reduces and redirects selenoprotein biosynthesis. Metallomics 2014, 6, 1079–1086. [Google Scholar] [CrossRef] [Green Version]
- Burk, R.F.; Hill, K.E. Regulation of Selenium Metabolism and Transport. Annu. Rev. Nutr. 2015, 35, 109–134. [Google Scholar] [CrossRef]
- Navarro-Alarcon, M.; Lopez-Ga de la Serrana, H.; Perez-Valero, V.; Lopez-Martinez, M.C. Selenium concentrations in serum of individuals with liver diseases (cirrhosis or hepatitis): Relationship with some nutritional and biochemical markers. Sci. Total Environ. 2002, 291, 135–141. [Google Scholar] [CrossRef]
- Girelli, D.; Olivieri, O.; Stanzial, A.M.; Azzini, M.; Lupo, A.; Bernich, P.; Menini, C.; Gammaro, L.; Corrocher, R. Low platelet glutathione peroxidase activity and serum selenium concentration in patients with chronic renal failure: Relations to dialysis treatments, diet and cardiovascular complications. Clin. Sci. 1993, 84, 611–617. [Google Scholar] [CrossRef]
- Ma, C.; Hoffmann, P.R. Selenoproteins as regulators of T cell proliferation, differentiation, and metabolism. Sem. Cell Dev. Biol. 2021, 115, 54–61. [Google Scholar] [CrossRef]
- Linterman, M.A.; Denton, A.E. Selenium saves ferroptotic TFH cells to fortify the germinal center. Nat. Immunol. 2021, 22, 1074–1076. [Google Scholar] [CrossRef]
- Pillai, R.; Uyehara-Lock, J.H.; Bellinger, F.P. Selenium and selenoprotein function in brain disorders. IUBMB Life 2014, 66, 229–239. [Google Scholar] [CrossRef] [PubMed]
- Schweizer, U.; Bohleber, S.; Zhao, W.; Fradejas-Villar, N. The Neurobiology of Selenium: Looking Back and to the Future. Front. Neurosci. 2021, 15, 652099. [Google Scholar] [CrossRef] [PubMed]
- Ishikura, K.; Misu, H.; Kumazaki, M.; Takayama, H.; Matsuzawa-Nagata, N.; Tajima, N.; Chikamoto, K.; Lan, F.; Ando, H.; Ota, T.; et al. Selenoprotein P as a diabetes-associated hepatokine that impairs angiogenesis by inducing VEGF resistance in vascular endothelial cells. Diabetologia 2014, 57, 1968–1976. [Google Scholar] [CrossRef] [PubMed]
- Moon, S.; Chung, H.S.; Yu, J.M.; Yoo, H.J.; Park, J.H.; Kim, D.S.; Park, Y.K.; Yoon, S.N. Association between serum selenium level and the prevalence of diabetes mellitus in U.S. population. J. Trace Elem. Med. Biol. 2019, 52, 83–88. [Google Scholar] [CrossRef] [PubMed]
- Cabral, M.; Kuxhaus, O.; Eichelmann, F.; Kopp, J.F.; Alker, W.; Hackler, J.; Kipp, A.P.; Schwerdtle, T.; Haase, H.; Schomburg, L.; et al. Trace element profile and incidence of type 2 diabetes, cardiovascular disease and colorectal cancer: Results from the EPIC-Potsdam cohort study. Eur. J. Nutr. 2021, 60, 3267–3278. [Google Scholar] [CrossRef] [PubMed]
- Huang, J.Q.; Zhou, J.C.; Wu, Y.Y.; Ren, F.Z.; Lei, X.G. Role of glutathione peroxidase 1 in glucose and lipid metabolism-related diseases. Free Radic. Biol. Med. 2018, 127, 108–115. [Google Scholar] [CrossRef]
- Saito, Y. Selenoprotein P as an in vivo redox regulator: Disorders related to its deficiency and excess. J. Clin. Biochem. Nutr. 2020, 66, 1–7. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Brigelius-Flohe, R.; Flohe, L. Selenium and redox signaling. Arch. Biochem. Biophys. 2017, 617, 48–59. [Google Scholar] [CrossRef]
- Mojadadi, A.; Au, A.; Salah, W.; Witting, P.; Ahmad, G. Role for Selenium in Metabolic Homeostasis and Human Reproduction. Nutrients 2021, 13, 3256. [Google Scholar] [CrossRef]
- Mao, J.Y.; Teng, W.P. The Relationship between Selenoprotein P and Glucose Metabolism in Experimental Studies. Nutrients 2013, 5, 1937–1948. [Google Scholar] [CrossRef] [Green Version]
- Schomburg, L. The other view: The trace element selenium as a micronutrient in thyroid disease, diabetes, and beyond. Hormones 2020, 19, 15–24. [Google Scholar] [CrossRef]
- Kohler, L.N.; Foote, J.; Kelley, C.P.; Florea, A.; Shelly, C.; Chow, H.S.; Hsu, P.; Batai, K.; Ellis, N.; Saboda, K.; et al. Selenium and Type 2 Diabetes: Systematic Review. Nutrients 2018, 10, 1924. [Google Scholar] [CrossRef] [Green Version]
- Qiu, Z.; Geng, T.; Wan, Z.; Lu, Q.; Guo, J.; Liu, L.; Pan, A.; Liu, G. Serum selenium concentrations and risk of all-cause and heart disease mortality among individuals with type 2 diabetes. Am. J. Clin. Nutr. 2021, 00, 1–8. [Google Scholar] [CrossRef]
- Morris, J.S.; Crane, S.B. Selenium toxicity from a misformulated dietary supplement, adverse health effects, and the temporal response in the nail biologic monitor. Nutrients 2013, 5, 1024–1057. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Brodin, O.; Hackler, J.; Misra, S.; Wendt, S.; Sun, Q.; Laaf, E.; Stoppe, C.; Bjornstedt, M.; Schomburg, L. Selenoprotein P as Biomarker of Selenium Status in Clinical Trials with Therapeutic Dosages of Selenite. Nutrients 2020, 12, 1067. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Wang, Y.; Rijntjes, E.; Wu, Q.; Lv, H.; Gao, C.; Shi, B.; Schomburg, L. Selenium deficiency is linearly associated with hypoglycemia in healthy adults. Redox Biol. 2020, 37, 101709. [Google Scholar] [CrossRef]
- Schomburg, L.; Orho-Melander, M.; Struck, J.; Bergmann, A.; Melander, O. Selenoprotein-P Deficiency Predicts Cardiovascular Disease and Death. Nutrients 2019, 11, 1852. [Google Scholar] [CrossRef] [Green Version]
- Al-Mubarak, A.A.; Beverborg, N.G.; Suthahar, N.; Gansevoort, R.T.; Bakker, S.J.L.; Touw, D.J.; de Boer, R.A.; van der Meer, P.; Bomer, N. High selenium levels associate with reduced risk of mortality and new onset heart failure: Data from PREVEND. Eur. J. Heart Fail. 2021. [Google Scholar] [CrossRef] [PubMed]
- Bomer, N.; Grote Beverborg, N.; Hoes, M.F.; Streng, K.W.; Vermeer, M.; Dokter, M.M.; IJmker, J.; Anker, S.D.; Cleland, J.G.F.; Hillege, H.L.; et al. Selenium and outcome in heart failure. Eur. J. Heart Fail. 2020, 22, 1415–1423. [Google Scholar] [CrossRef] [Green Version]
- Al-Mubarak, A.A.; van der Meer, P.; Bomer, N. Selenium, Selenoproteins, and Heart Failure: Current Knowledge and Future Perspective. Curr. Heart Fail. Rep. 2021, 18, 122–131. [Google Scholar] [CrossRef]
- Shimada, B.K.; Alfulaij, N.; Seale, L.A. The Impact of Selenium Deficiency on Cardiovascular Function. Int. J. Mol. Sci. 2021, 22, 713. [Google Scholar] [CrossRef] [PubMed]
- Al-Mubarak, A.A.; Grote Beverborg, N.; Anker, S.D.; Samani, N.J.; Dickstein, K.; Filippatos, G.; van Veldhuisen, D.J.; Voors, A.A.; Bomer, N.; van der Meer, P. A Clinical Tool to Predict Low Serum Selenium in Patients with Worsening Heart Failure. Nutrients 2020, 12, 2541. [Google Scholar] [CrossRef]
- Belhadj, M.; Kazi Tani, L.S.; Dennouni Medjati, N.; Harek, Y.; Dali Sahi, M.; Sun, Q.; Heller, R.; Behar, A.; Charlet, L.; Schomburg, L. Se Status Prediction by Food Intake as Compared to Circulating Biomarkers in a West Algerian Population. Nutrients 2020, 12, 3599. [Google Scholar] [CrossRef]
- Kasaikina, M.V.; Hatfield, D.L.; Gladyshev, V.N. Understanding selenoprotein function and regulation through the use of rodent models. Biochim. Biophys. Acta 2012, 1823, 1633–1642. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Conrad, M. Transgenic mouse models for the vital selenoenzymes cytosolic thioredoxin reductase, mitochondrial thioredoxin reductase and glutathione peroxidase 4. Biochim. Biophys. Acta 2009, 1790, 1575–1585. [Google Scholar] [CrossRef]
- Tsuji, P.A.; Santesmasses, D.; Lee, B.J.; Gladyshev, V.N.; Hatfield, D.L. Historical Roles of Selenium and Selenoproteins in Health and Development: The Good, the Bad and the Ugly. Int. J. Mol. Sci. 2022, 23, 5. [Google Scholar] [CrossRef]
- Schweizer, U.; Dehina, N.; Schomburg, L. Disorders of selenium metabolism and selenoprotein function. Curr. Opin. Pediatr. 2011, 23, 429–435. [Google Scholar] [CrossRef] [PubMed]
- Schoenmakers, E.; Chatterjee, K. Human Genetic Disorders Resulting in Systemic Selenoprotein Deficiency. Int. J. Mol. Sci. 2021, 22, 2927. [Google Scholar] [CrossRef] [PubMed]
- Santesmasses, D.; Gladyshev, V.N. Pathogenic Variants in Selenoproteins and Selenocysteine Biosynthesis Machinery. Int. J. Mol. Sci. 2021, 22, 11593. [Google Scholar] [CrossRef] [PubMed]
- Ambroziak, U.; Hybsier, S.; Shahnazaryan, U.; Krasnodebska-Kiljanska, M.; Rijntjes, E.; Bartoszewicz, Z.; Bednarczuk, T.; Schomburg, L. Severe selenium deficits in pregnant women irrespective of autoimmune thyroid disease in an area with marginal selenium intake. J. Trace Elem. Med. Biol. 2017, 44, 186–191. [Google Scholar] [CrossRef]
- Apitzsch, S.; Larsson, L.; Larsson, A.K.; Linder, A. The physical and mental impact of surviving sepsis—A qualitative study of experiences and perceptions among a Swedish sample. Arch. Public Health 2021, 79, 66. [Google Scholar] [CrossRef]
- Borba, V.V.; Zandman-Goddard, G.; Shoenfeld, Y. Exacerbations of autoimmune diseases during pregnancy and postpartum. Best Pract. Res. Clin. Endocrinol. Metab. 2019, 33, 101321. [Google Scholar] [CrossRef]
- Lazarus, J.H.; Parkes, A.B.; Premawardhana, L.D. Postpartum thyroiditis. Autoimmunity 2002, 35, 169–173. [Google Scholar] [CrossRef]
- Gedzyk-Nieman, S.A. Postpartum and Paternal Postnatal Depression: Identification, Risks, and Resources. Nurs. Clin. N. Am. 2021, 56, 325–343. [Google Scholar] [CrossRef]
- Swami, V.; Barron, D.; Smith, L.; Furnham, A. Mental health literacy of maternal and paternal postnatal (postpartum) depression in British adults. J. Ment. Health 2020, 29, 217–224. [Google Scholar] [CrossRef]
- Kong, L.; Wu, Q.; Liu, B. The impact of selenium administration on severe sepsis or septic shock: A meta-analysis of randomized controlled trials. Afr. Health Sci. 2021, 21, 277–285. [Google Scholar] [CrossRef]
- Leung, B.M.; Kaplan, B.J.; Field, C.J.; Tough, S.; Eliasziw, M.; Gomez, M.F.; McCargar, L.J.; Gagnon, L.; Team, A.P.S. Prenatal micronutrient supplementation and postpartum depressive symptoms in a pregnancy cohort. BMC Pregnancy Childbirth 2013, 13, 2. [Google Scholar] [CrossRef] [Green Version]
- Mantovani, G.; Isidori, A.M.; Moretti, C.; Di Dato, C.; Greco, E.; Ciolli, P.; Bonomi, M.; Petrone, L.; Fumarola, A.; Campagna, G.; et al. Selenium supplementation in the management of thyroid autoimmunity during pregnancy: Results of the “SERENA study”, a randomized, double-blind, placebo-controlled trial. Endocrine 2019, 66, 542–550. [Google Scholar] [CrossRef] [Green Version]
- Alehagen, U.; Opstad, T.B.; Alexander, J.; Larsson, A.; Aaseth, J. Impact of Selenium on Biomarkers and Clinical Aspects Related to Ageing. A Review. Biomolecules 2021, 11, 1478. [Google Scholar] [CrossRef]
- Zhang, Y.; Roh, Y.J.; Han, S.J.; Park, I.; Lee, H.M.; Ok, Y.S.; Lee, B.C.; Lee, S.R. Role of Selenoproteins in Redox Regulation of Signaling and the Antioxidant System: A Review. Antioxidants 2020, 9, 383. [Google Scholar] [CrossRef] [PubMed]
- Zhang, L.; Zeng, H.W.; Cheng, W.H. Beneficial and paradoxical roles of selenium at nutritional levels of intake in healthspan and longevity. Free Radic. Biol. Med. 2018, 127, 3–13. [Google Scholar] [CrossRef]
- Demircan, K.; Bengtsson, Y.; Sun, Q.; Brange, A.; Vallon-Christersson, J.; Rijntjes, E.; Malmberg, M.; Saal, L.H.; Ryden, L.; Borg, A.; et al. Serum selenium, selenoprotein P and glutathione peroxidase 3 as predictors of mortality and recurrence following breast cancer diagnosis: A multicentre cohort study. Redox Biol. 2021, 47, 102145. [Google Scholar] [CrossRef] [PubMed]
- Baker, J.R.; Umesh, S.; Jenab, M.; Schomburg, L.; Tjonneland, A.; Olsen, A.; Boutron-Ruault, M.C.; Rothwell, J.A.; Severi, G.; Katzke, V.; et al. Prediagnostic Blood Selenium Status and Mortality among Patients with Colorectal Cancer in Western European Populations. Biomedicines 2021, 9, 1521. [Google Scholar] [CrossRef] [PubMed]
- Schmalbrock, L.J.; Weiss, G.; Rijntjes, E.; Reinschissler, N.; Sun, Q.; Schenk, M.; Schomburg, L. Pronounced Trace Element Variation in Follicular Fluids of Subfertile Women Undergoing Assisted Reproduction. Nutrients 2021, 13, 4134. [Google Scholar] [CrossRef]
- Ogrizek Pelkic, K.; Sobocan, M.; Takac, I. Low Selenium Levels in Amniotic Fluid Correlate with Small-For-Gestational Age Newborns. Nutrients 2020, 12, 3046. [Google Scholar] [CrossRef] [PubMed]
- Lewandowska, M.; Wieckowska, B.; Sajdak, S.; Lubinski, J. First Trimester Microelements and Their Relationships with Pregnancy Outcomes and Complications. Nutrients 2020, 12, 1108. [Google Scholar] [CrossRef] [PubMed]
- Beck, M.A.; Nelson, H.K.; Shi, Q.; Van Dael, P.; Schiffrin, E.J.; Blum, S.; Barclay, D.; Levander, O.A. Selenium deficiency increases the pathology of an influenza virus infection. FASEB J. 2001, 15, 1481–1483. [Google Scholar] [CrossRef]
- Beck, M.A.; Shi, Q.; Morris, V.C.; Levander, O.A. Rapid genomic evolution of a non-virulent coxsackievirus B3 in selenium-deficient mice results in selection of identical virulent isolates. Nat. Med. 1995, 1, 433–436. [Google Scholar] [CrossRef]
- Wang, R.; Chen, J.; Wei, G.W. Mechanisms of SARS-CoV-2 Evolution Revealing Vaccine-Resistant Mutations in Europe and America. J. Phys. Chem. Lett. 2021, 12, 11850–11857. [Google Scholar] [CrossRef]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the author. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).