Public Health Implications of Wasting and Stunting Relationship in Children under Five Years Highly Vulnerable to Undernutrition in Guatemala: The REDAC Study
Abstract
1. Introduction
2. Materials and Methods
2.1. Anthropometry and Nutritional Status Indicators
2.2. Data Quality Assurance
2.3. Statistical Analysis
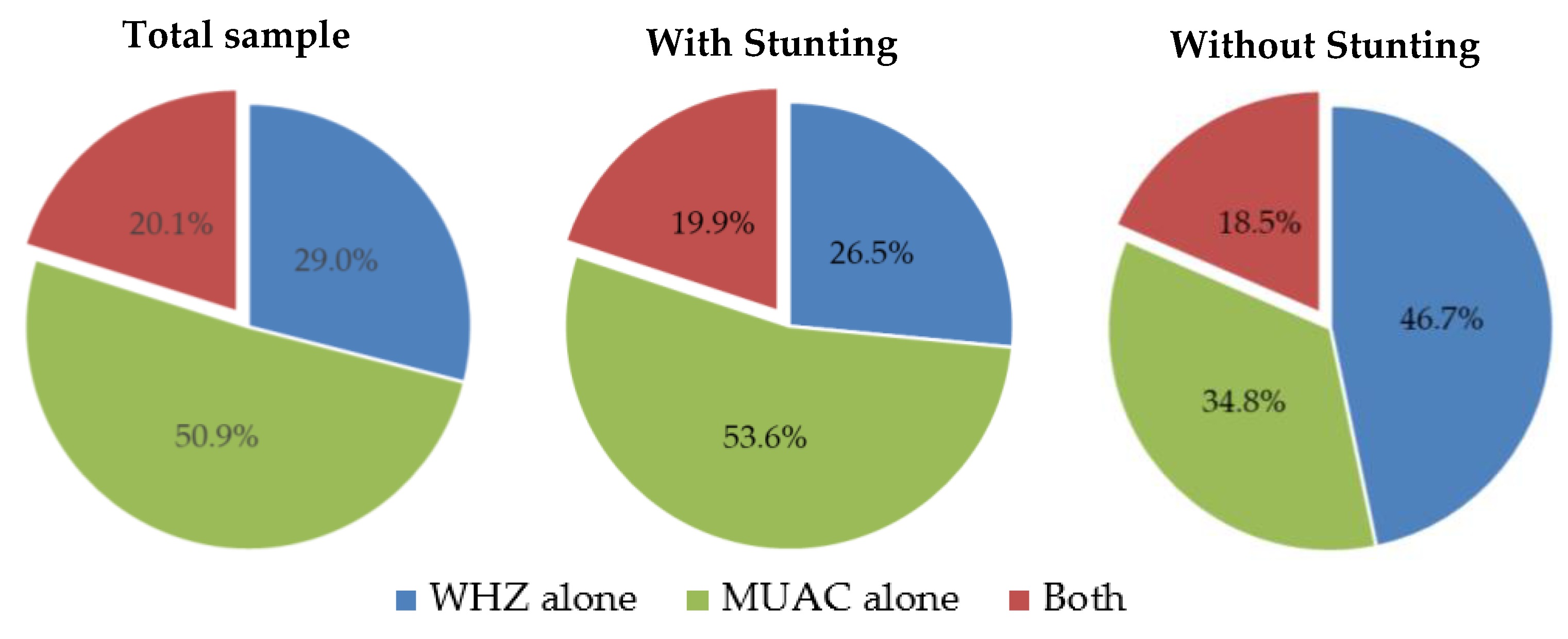
3. Results
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Beveridge, L.; Whitfield, S.; Fraval, S.; Van Wijk, M.; Van Etten, J.; Mercado, L.; Hammond, J.; Davila, L.; Suchini, J.G.; Challinor, A. Experiences and drivers of food insecurity in Guatemala’s Dry Corridor: Insights from the Integration of Ethnographic and Household Survey Data. Front Sustain. Food Syst. 2019, 3, 65. [Google Scholar] [CrossRef]
- Programa Mundial de Alimentos. Eventos Climáticos Adversos en el Corredor Seco Centroamericano Dejan a 1.4 Millones de Personas en Necesidad de Asistencia Alimentaria Urgente. 2019. Available online: https://es.wfp.org/1.4-millones-necesitan-asistencia-alimentaria-urgente-en-Corredor-Seco-centroamericano (accessed on 12 July 2022).
- Rosales, S.; Lemus, I.; García, E. Índice de Pobreza Multidimensional en Guatemala (IPM Gt). Ministerio de Desarrollo Social. 2019. Available online: https://mppn.org/es/paises_participantes/guatemala/ (accessed on 12 July 2022).
- World Bank Group. Guatemala’s Water Supply, Sanitation, and Hygiene Poverty Diagnostic Challenges and Opportunities. 2018. Available online: https://openknowledge.worldbank.org/handle/10986/29454 (accessed on 12 July 2022).
- Ministerio de Salud Pública y Asistencia Social (MSPAS), Instituto Nacional de Estadística (INE) y Secretaría de Planificación y Programación de la Presidencia (Segeplán). VI Encuesta Nacional de Salud Materno Infantil 2014–2015. 2017. Available online: http://www.siinsan.gob.gt/siinsan/documentos/vi-encuesta-nacional-de-salud-materno-infantil-ensmi-2014-2015/ (accessed on 13 July 2022).
- Gobierno de Guatemala, USAID, Fhi360. La Malnutrición en Guatemala. Frenando el Desarrollo de Nuestro País. 2017. Available online: https://www.fantaproject.org/sites/default/files/resources/Guatemala-PROFILES-CSO-SPANISH-Jul2017_0.pdf (accessed on 12 July 2022).
- UNICEF. La Desnutrición Infantil. Causas, Consecuencias y Estrategias para su Prevención y Tratamiento. 2011. Available online: https://www.unicef.es/sites/unicef.es/files/Dossierdesnutricion.pdf (accessed on 12 July 2022).
- World Health Organization. Guideline: Updates on the Management of Severe Acute Malnutrition in Infants and Children. 2013. Available online: https://www.who.int/publications/i/item/9789241506328 (accessed on 12 July 2022).
- Ministerio de Salud Pública y Asistencia Social (MSPAS), Departamento de Epidemiología. Protocolo de Vigilancia Epidemiológica Desnutrición Aguda. 2018. Available online: http://epidemiologia.mspas.gob.gt/files/Publicaciones%202018/Protocolos/Vigilancia%20Epidemiol%C3%B3gica%20Desnutrici%C3%B3n%20Aguda.pdf (accessed on 14 July 2022).
- Ministerio de Salud Pública y Asistencia Social (MSPAS). Protocolo Para el Tratamiento en Centros de Recuperación Nutricional de la Desnutrición Aguda Severa y Modera Sin Complicaciones en el Paciente Pediátrico. 2009. Available online: https://www.paho.org/gut/index.php?option=com_docman&view=download&alias=168-protocolo-para-centros-recuperacion-nutricional-mspas2009&category_slug=desnutricion-aguda&Itemid=518 (accessed on 14 July 2022).
- Ministerio de Salud Pública y Asistencia Social (MSPAS). Protocolo Para el Tratamiento Ambulatorio de Niños con Desnutrición Aguda Severa Sin Complicaciones en la Comunidad. 2009. Available online: http://www.sesan.gob.gt/wordpress/wp-content/uploads/2019/07/Protocolo-para-el-Tratamiento-Ambulatorio-de-Ninos-con-Desnutricion-Aguda.pdf (accessed on 14 July 2022).
- Ministerio de Salud Pública y Asistencia Social (MSPAS). Protocolo Para el Tratamiento Ambulatorio de Niños y Niñas con Desnutrición Aguda Moderada sin Complicaciones. 2010. Available online: http://www.siinsan.gob.gt/siinsan/wp-content/uploads/cedesan2/libros/Protocolo-Tratamiento-ambulatorio-DA-MODERADA.pdf (accessed on 14 July 2022).
- Roberfroid, D.; Huybregts, L.; Lachat, C.; Vrijens, F.; Kolsteren, P.; Guesdon, B. Inconsistent diagnosis of acute malnutrition by weight-for-height and mid-upper arm circumference: Contributors in 16 cross-sectional surveys from South Sudan, the Philippines, Chad, and Bangladesh. Nutr. J. 2015, 14, 86. [Google Scholar] [CrossRef] [PubMed]
- SMART Methodology—Standardized Monitoring and Assessment of Relief and Transitions. 2019. Available online: https://smartmethodology.org/survey-planning-tools/herramientas-para-smart/ (accessed on 20 July 2022).
- World Health Organization. The WHO Child Growth Standards. 2007. Available online: https://www.who.int/childgrowth/standards/en/ (accessed on 20 July 2022).
- World Health Organization. OMS Anthro v. 3.2.2. Available online: https://www.who.int/childgrowth/software/es/ (accessed on 20 July 2022).
- Svedberg, P. Poverty and Undernutrition: Theory, Measurement and Policy; Oxford University Press: Oxford, UK, 2000. [Google Scholar]
- World Health Organization & UNICEF. Recommendations for Data Collection, Analysis, and Reporting on Anthropometric Indicators in Children under 5 Years Old. 2019. Available online: https://www.who.int/nutrition/publications/anthropometry-data-quality-report/en/ (accessed on 20 July 2022).
- Landis, J.R.; Koch, G.G. The measurement of observer agreement for categorical data. Biometrics 1977, 33, 159–174. [Google Scholar] [CrossRef] [PubMed]
- Díez-Navarro, A.; Marrodán, M.D. La desnutrición infantil en el mundo: Herramientas para su diagnóstico. In Avances en Alimentación, Nutrición y Dietética; Martínez-Álvarez, J.R., Villarino, A., Eds.; Punto Didot: Madrid, Spain, 2018; pp. 77–96. [Google Scholar]
- Vollmer, S.; Harttgen, K.; Kupka, R.; Subramanian, S.V. Levels and trends of childhood undernutrition by wealth and education according to a Composite Index of Anthropometric Failure: Evidence from 146 Demographic and Health Surveys from 39 countries. BMJ Glob. Health 2017, 2, e000206. [Google Scholar] [CrossRef] [PubMed]
- Thurstans, S.; Opondo, C.; Seal, A.; Wells, J.; Khara, T.; Briend, A.; Myatt, M.; Garenne, M.; Sear, R.; Kerac, M. Boys are more likely to be undernourished than girls: A systematic review and meta-analysis of sex differences in undernutrition. BMJ Glob. Health 2020, 5, e004030. [Google Scholar] [CrossRef] [PubMed]
- Díez-Navarro, A.; Marrodán, M.; Gómez, A.; Rivero, E.; Vargas, A.; Pacheco, J.L.; Sánchez-Álvarez, M.; López-Ejeda, N.; Moreno-Romero, S.; Prado, C.; et al. Female eco-stability and severe malnutrition in children: Evidence from humanitarian aid interventions of Action against hunger in African, Asian and Latin American countries. Nutr. Clin. Diet. Hosp. 2017, 34, 127–134. [Google Scholar]
- Myatt, M.; Khara, T.; Schoenbuchner, S.; Pietzsch, S.; Dolan, C.; Lelijveld, N.; Briend, A. Children who are both wasted and stunted are also underweight and have a high risk of death: A descriptive epidemiology of multiple anthropometric deficits using data from 51 countries. Arch. Public Health 2018, 76, 28. [Google Scholar] [CrossRef] [PubMed]
- Wasting-Stunting Technical Interest Group (WaSt TIG). Child Wasting and Stunting: Time to Overcome the Separation. A Briefing Note for Policy Makers and Programme Implementers. 2018. Available online: https://www.ennonline.net/attachments/2912/WaSt-policy-brief.pdf (accessed on 16 August 2022).
- Díez-Navarro, A. Análisis Comparativo de Indicadores Antropométricos para el Diagnóstico de la Desnutrición Infantil. Ph.D. Thesis, Universidad Complutense de Madrid, Madrid, Spain, 2018. Available online: https://eprints.ucm.es/49811/1/T40502.pdf (accessed on 16 August 2022).
- Grellety, E.; Golden, M.H. Severely malnourished children with a low weight-for-height have a higher mortality than those with a low mid-upper-arm circumference: I. Empirical data demonstrates Simpson’s paradox. Nutr. J. 2018, 17, 79. [Google Scholar] [CrossRef] [PubMed]
- Grellety, E.; Golden, M.H. Weight-for-height and mid-upper-arm circumference should be used independently to diagnose acute malnutrition: Policy implications. BMC Nutr. 2016, 2, 10. [Google Scholar] [CrossRef]
- De Onis, M.; Borghi, E.; Arimond, M.; Webb, P.; Croft, T.; Saha, K.; De-Regil, L.M.; Thuita, F.; Heidkamp, R.; Krasevec, J.; et al. Prevalence thresholds for wasting, overweight and stunting in children under 5 years. Publ. Health Nutr. 2019, 22, 175–179. [Google Scholar] [CrossRef] [PubMed]
- Leidman, E.; Couture, A.; Hulland, E.; Biluka, O. Concordance between estimates of acute malnutrition measured by weight-forheight and by mid-upper arm circumference after age adjustment: Population-representative surveys from humanitarian settings. BMC Nutr. 2019, 5, 39. [Google Scholar] [CrossRef] [PubMed]
- Rasmussen, J.; Andersen, A.; Fisker, A.B.; Ravn, H.; Sodemann, M.; Rodrigues, A.; Benn, C.S.; Aaby, P. Mid-upper-arm-circumference and mid-upper-arm circumference z-score: The best predictor of mortality? Eur. J. Clin. Nutr. 2012, 66, 998–1003. [Google Scholar] [CrossRef] [PubMed]
- Briend, A.; Álvarez, J.L.; Avril, N.; Bahwere, P.; Bailey, J.; Berkley, J.A.; Binns, P.; Blackwell, N.; Dale, N.; Deconinck, H.; et al. Low mid-upper arm circumference identifies children with a High Risk of death who should be the priority target for treatment. BMC Nutr. 2016, 2, 63. [Google Scholar] [CrossRef]
- Schwhinger, C.; Golden, M.H.; Grellety, E.; Robertfroid, D.; Guesdon, B. Severe acute malnutrition and mortality in children in the community: Comparison of indicators in a multi-country pooled analysis. PLoS ONE 2019, 14, e0219745. [Google Scholar] [CrossRef] [PubMed]
- Miller, M.A.; Mallory, K.; Escobedo, M.; Tarot, A.C.; Abdel-Rahman, S. Assessing the effectiveness of a novel mid-upper arm circumference Z-score tape in a community setting in Guatemala. Arch. Public Health 2019, 77, 44. [Google Scholar] [CrossRef] [PubMed]
| Anthropometric Indicators | Total Median [IQR] | Boys Median [IQR] | Girls Median [IQR] | p-Value |
|---|---|---|---|---|
| Weight (kg) | 10.0 [8.1, 12.3] | 10.2 [8.2, 12.4] | 9.9 [7.9, 12.1] | <0.001 |
| Height (cm) | 79.4 [70.3, 87.7] | 79.9 [70.5, 87.7] | 79.0 [10.2, 87.7] | 0.028 |
| MUAC (mm) | 144 [135, 153] | 145 [137, 153] | 143 [135, 152] | <0.001 |
| HAZ (z-score) | −2.7 [−3.4, −1.9] | −2.8 [−3.5, −2.0] | −2.7 [−3.4, −1.9] | <0.001 |
| WAZ (z-score) | −1.6 [−2.4, −0.91] | −1.7 [−2.4, −0.9] | −1.6 [−2.4, −0.9] | 0.147 NS |
| WHZ (z-score) | −0.07 [−0.7, 0.6] | −0.09 [−0.8, 0.6] | −0.05 [−0.7, 0.6] | 0.020 |
| MUACAZ (z-score) | −0.8 [−1.4, −0.2] | −0.8 [−1.5, −0.13] | −0.8 [−1.4, −0.2] | 0.482 NS |
| Malnutrition Categories | Total % (N) | Boys % (N) | Girls % (N) | p-value |
| STUNTING (HAZ) | 73.0% (9119) | 74.9% (25.1) | 71.0% (4387) | <0.001 |
| Moderate | 33.7% (4211) | 33.6% (2125) | 33.8% (2086) | 0.877 NS |
| Severe | 39.3% (4908) | 41.3% (2607) | 37.2% (2301) | <0.001 |
| WASTING (WHZ) * | 2.8% (355) | 3.4% (222) | 2.1% (133) | <0.001 |
| Moderate | 2.2% (278) | 2.7% (175) | 1.6% (103) | <0.001 |
| Severe | 0.6% (77) | 0.7% (47) | 0.5% (30) | 0.064 NS |
| WASTING (MUAC) * | 4.4% (519) | 3.7% (223) | 5.0% (296) | 0.001 |
| Moderate | 3.8% (452) | 3.3% (196) | 4.3% (256) | 0.003 |
| Severe | 0.6% (67) | 0.5% (27) | 0.7% (40) | 0.102 NS |
| WASTING (MUACAZ) * | 10.6% (1253) | 11.1% (662) | 10.0% (591) | 0.051 NS |
| Moderate | 9.2% (1091) | 9.7% (716) | 8.8% (517) | 0.098 NS |
| Severe | 1.4% (162) | 1.5% (889) | 1.3% (74) | 0.294 NS |
| UNDERWEIGHT (WAZ) | 36.3% (4678) | 37.1 (2413) | 35.5% (2265) | 0.053 NS |
| Moderate | 24.9% (3206) | 26.1% (1697) | 23.6% (1509) | 0.001 |
| Severe | 11.4% (1472) | 11.0% (716) | 11.8% (756) | 0.139 NS |
| Total % (N) | Boys % (N) | Girls % (N) | p-Value | |
|---|---|---|---|---|
| Without failure | 25.8% (3220) | 23.8% (1503) | 27.8% (1717) | <0.001 |
| * Wasting only | 0.3% (39) | 0.2% (14) | 0.4% (25) | 0.067 NS |
| * Wasting + Underweight | 0.1% (18) | 0.2% (13) | 0.1% (5) | 0.066 NS |
| Stunting + * Wasting + Underweight | 1.0 (120) | 1.1% (67) | 0.9% (53) | 0.244 NS |
| Stunting + Underweight | 32.8% (4092) | 33.4% (2108) | 32.2% (1984) | 0.127 NS |
| Stunting only | 39.2% (4886) | 40.4% (2545) | 38.0% (2341) | 0.005 |
| Underweight only | 0.8% (95) | 0.8% (52) | 0.7% (43) | 0.411 NS |
| CIAF | 74.2% (9250) | 76.1% (4799) | 72.3% (4451) | <0.001 |
| Wasting Indicator | Total Sample | With Stunting | Without Stunting | Difference | ꭓ2 p-Value | Odds Ratio | 95% C.I. | |
|---|---|---|---|---|---|---|---|---|
| Total | WHZ | 2.8% (355) | 2.9% (268) | 1.8% (62) | +1.1% | 0.001 | 1.621 | 1.226–2.143 |
| MUAC | 4.4% (519) | 4.8% (420) | 1.9% (52) | +2.9% | <0.001 | 2.614 | 1.953–3.499 | |
| MUACAZ | 10.6% (1253) | 11.9% (1032) | 3.2% (82) | +8.7% | <0.001 | 4.337 | 3.448–5.454 | |
| Boys | WHZ | 3.4% (222) | 3.5% (166) | 2.3% (36) | +1.2% | 0.015 | 1.566 | 1.089–2.255 |
| MUAC | 3.7% (223) | 3.9% (173) | 1.7% (21) | +2.2% | <0.001 | 2.380 | 1.507–3.760 | |
| MUACAZ | 11.1% (662) | 12.3% (550) | 3.9% (49) | +8.4% | <0.001 | 3.462 | 2.566–4.669 | |
| Girls | WHZ | 2.1% (133) | 2.3% (102) | 1.5% (26) | +0.8% | 0.028 | 1.619 | 1.049–2.499 |
| MUAC | 5.0% (296) | 5.9% (247) | 2.1% (31) | +3.8% | <0.001 | 2.879 | 1.972–4.203 | |
| MUACAZ | 10.0% (591) | 11.5% (482) | 2.3% (33) | +9.2% | <0.001 | 5.589 | 3.907–7.994 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
López-Ejeda, N.; Medialdea, L.; Vargas, A.; Coronado, J.; García-Arias, M.Á.; Marrodán, M.D. Public Health Implications of Wasting and Stunting Relationship in Children under Five Years Highly Vulnerable to Undernutrition in Guatemala: The REDAC Study. Nutrients 2022, 14, 3945. https://doi.org/10.3390/nu14193945
López-Ejeda N, Medialdea L, Vargas A, Coronado J, García-Arias MÁ, Marrodán MD. Public Health Implications of Wasting and Stunting Relationship in Children under Five Years Highly Vulnerable to Undernutrition in Guatemala: The REDAC Study. Nutrients. 2022; 14(19):3945. https://doi.org/10.3390/nu14193945
Chicago/Turabian StyleLópez-Ejeda, Noemí, Laura Medialdea, Antonio Vargas, Jessica Coronado, Miguel Ángel García-Arias, and María Dolores Marrodán. 2022. "Public Health Implications of Wasting and Stunting Relationship in Children under Five Years Highly Vulnerable to Undernutrition in Guatemala: The REDAC Study" Nutrients 14, no. 19: 3945. https://doi.org/10.3390/nu14193945
APA StyleLópez-Ejeda, N., Medialdea, L., Vargas, A., Coronado, J., García-Arias, M. Á., & Marrodán, M. D. (2022). Public Health Implications of Wasting and Stunting Relationship in Children under Five Years Highly Vulnerable to Undernutrition in Guatemala: The REDAC Study. Nutrients, 14(19), 3945. https://doi.org/10.3390/nu14193945






