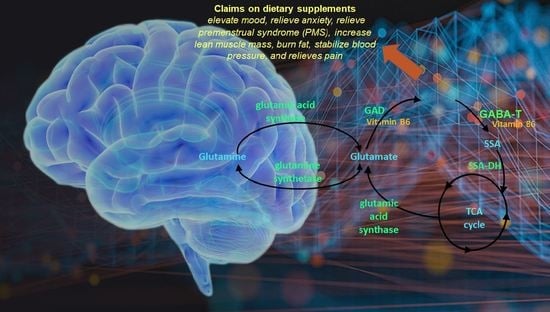
United States Pharmacopeia (USP) Safety Review of Gamma-Aminobutyric Acid (GABA)
Abstract
1. Introduction
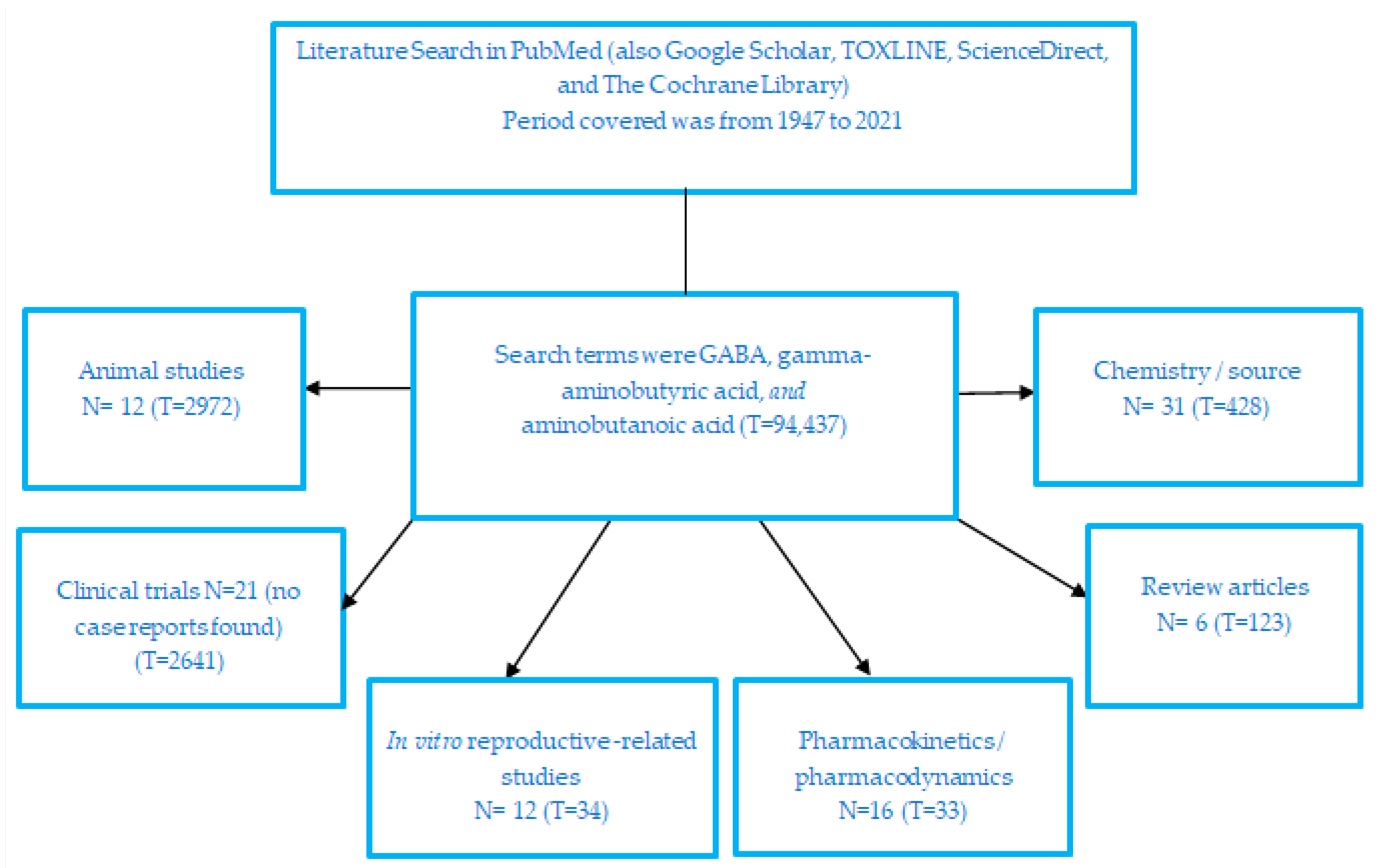
2. Literature Search Method
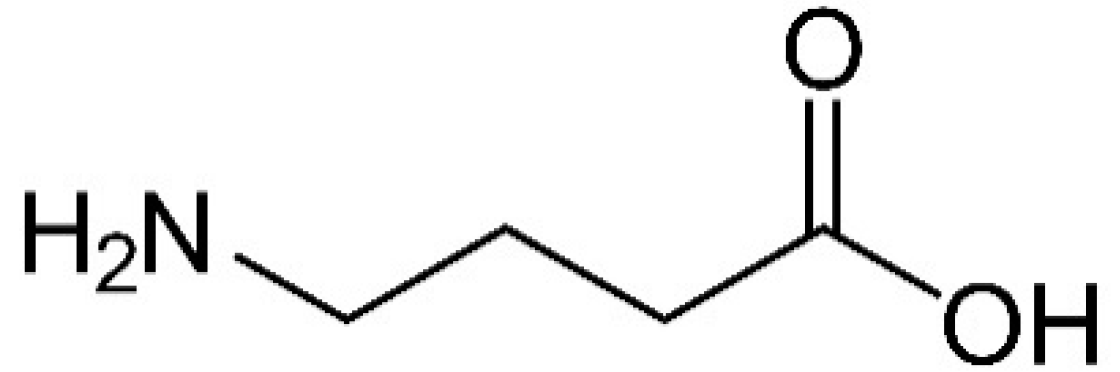
3. GABA Chemistry, Natural Sources, and Metabolism
3.1. Natural Sources of GABA
3.2. Commercial Sources of GABA
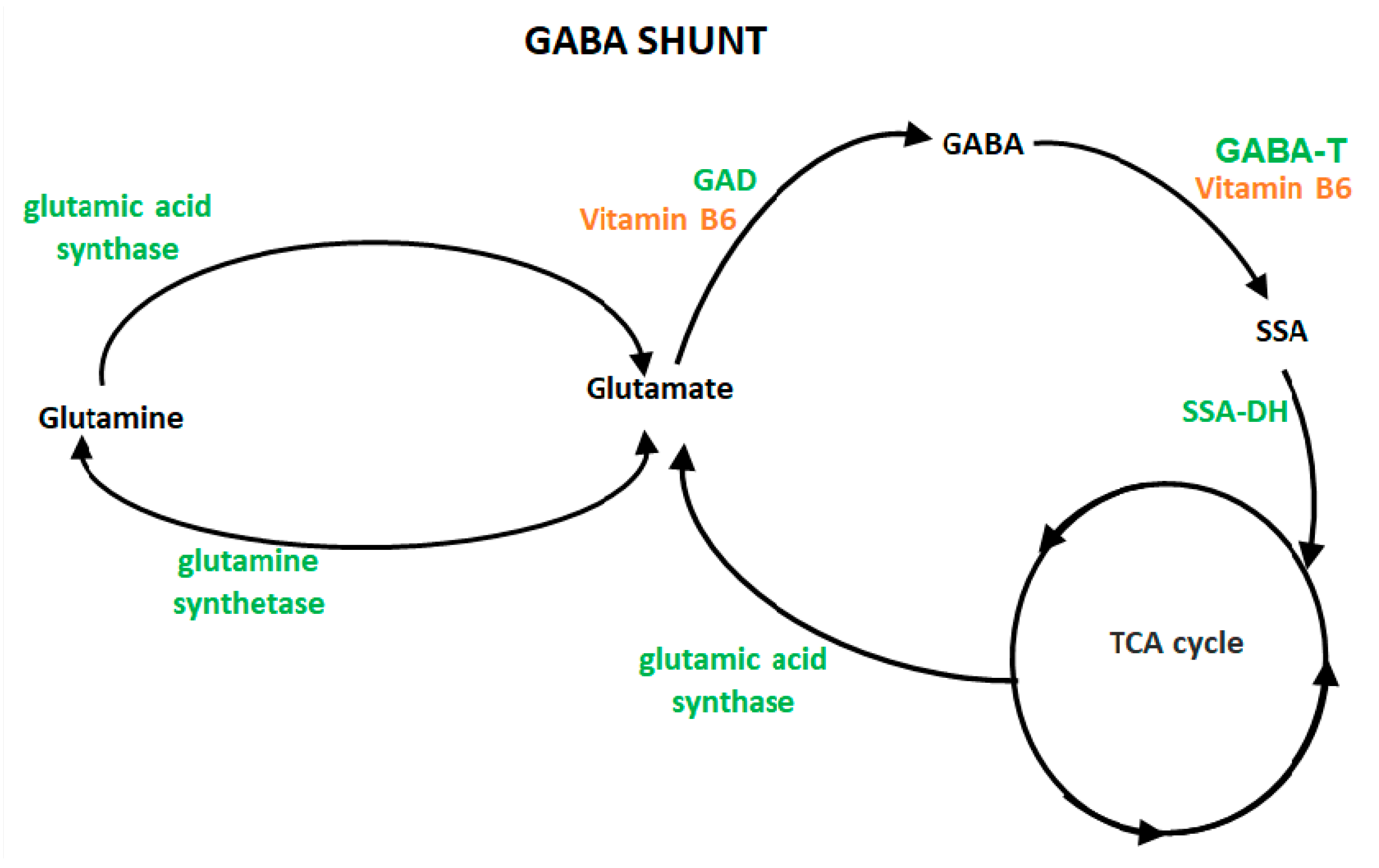
3.3. Metabolism of GABA
4. Pharmacopeial Quality Standards for GABA
5. Regulatory Status of GABA and Intake Levels
Some individuals may experience a minor tingling of the skin and/or slight shortness of breath shortly after taking GABA. This is characteristic of this amino acid and quickly subsides.[40]
6. Clinical Evidence of GABA Safety
6.1. Clinical Studies
6.2. Effects of GABA on Blood Pressure
6.3. Effects of GABA on Growth Hormone Levels
6.4. Effect of GABA on Sleep and Stress
6.5. Other Studies
6.6. Adverse Events Associated with GABA Intake
7. Animal Toxicology and In Vitro Studies
7.1. Acute Toxicity Studies
7.2. Sub-Chronic Toxicity Studies
7.3. Genotoxicity
7.4. Reproductive Effects of GABA
8. Pharmacokinetics of GABA
9. Potential Interactions of GABA with Drugs
10. Safety of GABA as Dietary Ingredient
11. Concluding Remarks
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| AABA | Alpha-aminobutyric acid |
| AE | Adverse event |
| AER | Adverse event report |
| ARTG | Australian Register of Therapeutic Goods |
| BABA | Beta-aminobutyric acid |
| BBB | Blood–brain barrier |
| BMI | Body mass index |
| BP | Blood pressure |
| CAERS | Center for Food Safety and Applied Nutrition (CFSAN) Adverse Event Reporting System |
| CAS | Chemical Abstract Services |
| CP | C-peptide |
| CSR | Cochrane systematic review |
| DAEN | Database of Adverse Event Notifications |
| DBP | Diastolic blood pressure |
| DS | Dietary supplements |
| DSHEA | Dietary Supplement Health and Education Act |
| DSLD | Dietary Supplement Label Database |
| EFSA | European Food Safety Authority |
| EMA | European Medicines Agency |
| EPA | U.S. Environmental Protection Agency |
| FDA | U.S. Food and Drug Administration |
| FMG | Fermented milk containing GABA |
| GABA GABAA | Gamma-aminobutyric acid GABA A receptor |
| GH | Growth hormone |
| GAD | Glutamate decarboxylase |
| USPNF GC | USPNF General Chapter |
| GRN | GRAS notice |
| HDL | High-density lipoprotein |
| HPLC | High-performance liquid chromatography |
| IGR | Immunoreactive glucagon |
| IR | Infrared |
| IRI | Immunoreactive insulin |
| JECFA | Joint FAO/WHO Expert Committee on Food Additives |
| JFRL | Japan Food Research Laboratories |
| LDH | Lactate dehydrogenase |
| LNHPD | Licensed Natural Health Products Database |
| MHRA | Medicines and Healthcare Products Regulatory Agency |
| NNHPD | Natural and Non-prescription Health Products Directorate (Canada) |
| NDIN | New Dietary Ingredient Notification |
| NHPID | Natural Health Products Ingredients Database |
| NIH | National Institutes of Health |
| NLT | Not less than |
| NMT | Not more than |
| NNHPD | Natural and Non-Prescription Health Products Directorate |
| PSP | Pyridoxal phosphate |
| SBP | Systolic blood pressure |
| TGA | Therapeutic Goods Administration |
| UNII | Unique Ingredient Identifier |
| UNPA | United Natural Products Alliance |
| USP | U.S. Pharmacopeial Convention |
References
- Cooper, J.R.; Roth, R.H. The Biochemical Basis of Neuropharmacology; Oxford University Press: Oxford, UK, 2003. [Google Scholar]
- Enna, S.J. GABA; Academic Press; Elsevier: San Diego, CA, USA, 2006. [Google Scholar]
- Miller, M.W. GABA as a Neurotransmitter in Gastropod Molluscs. Biol. Bull. 2019, 236, 144–156. [Google Scholar] [CrossRef] [PubMed]
- Effros, R.M. Alpha aminobutyric acid, an alternative measure of hepatic injury in sepsis? Transl. Res. 2011, 158, 326–327. [Google Scholar] [CrossRef] [PubMed]
- Medici, V.; Peerson, J.M.; Stabler, S.P.; French, S.W.; Gregory III, J.F.; Virata, M.C.; Halsted, C.H. Impaired homocysteine transsulfuration is an indicator of alcoholic liver disease. J. Hepatol. 2010, 53, 551–557. [Google Scholar] [CrossRef] [PubMed]
- Yudkoff, M.; Blazer-Yost, B.; Cohn, R.; Segal, S. On the clinical significance of the plasma alpha-amino-n-butyric acid:leucine ratio. Am. J. Clin. Nutr. 1979, 32, 282–285. [Google Scholar] [CrossRef]
- Baccelli, I.; Glauser, G.; Mauch-Mani, B. The accumulation of β-aminobutyric acid is controlled by the plant’s immune system. Planta 2017, 246, 791–796. [Google Scholar] [CrossRef] [PubMed]
- Steward, F.; Thompson, J.; Dent, C. γ-Aminobutyric acid: A constituent of the potato tuber. Science 1949, 110, 439–440. [Google Scholar]
- Roberts, M.R. Does GABA Act as a Signal in Plants? Hints from Molecular Studies: Hints from Molecular Studies. Plant Signal. Behav. 2007, 2, 408–409. [Google Scholar] [CrossRef]
- Bloom, F.E.; Iversen, L.L. Localizing 3H-GABA in nerve terminals of rat cerebral cortex by electron microscopic autoradiography. Nature 1971, 229, 628–630. [Google Scholar] [CrossRef]
- Wan, Y.; Wang, Q.; Prud’homme, G.J. GABAergic system in the endocrine pancreas: A new target for diabetes treatment. Diabetes Metab. Syndr. Obes. 2015, 8, 79–87. [Google Scholar]
- Gladkevich, A.; Korf, J.; Hakobyan, V.; Melkonyan, K. The peripheral GABAergic system as a target in endocrine disorders. Auton. Neurosci. 2006, 124, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Hepsomali, P.; Groeger, J.A.; Nishihira, J.; Scholey, A. Effects of Oral Gamma-Aminobutyric Acid (GABA) Administration on Stress and Sleep in Humans: A Systematic Review. Front. Neurosci. 2020, 14, 923. [Google Scholar] [CrossRef] [PubMed]
- Ngo, D.H.; Vo, T.S. An Updated Review on Pharmaceutical Properties of Gamma-Aminobutyric Acid. Molecules 2019, 24, 2678. [Google Scholar] [CrossRef]
- NMCD. Natural Medicine (Formerly Natural Standards and Natural Medicines Comprehensive Database. Available online: https://naturalmedicines.therapeuticresearch.com/databases/food,-herbs-supplements/professional.aspx?productid=464 (accessed on 8 June 2015).
- Thorne, R.I. Gamma-aminobutyric acid (GABA), Monograph. Altern. Med. Rev. 2007, 12, 274–279. [Google Scholar]
- MarketWatch. GABA Market Size, 2021 Regions Will Have the Highest Revenue, Which Will Emerge in Importance in the Market 2026. 2021. Available online: https://www.marketwatch.com/press-release/gaba-market-size-2021-regions-will-have-the-highest-revenue-which-will-emerge-in-importance-in-the-market-2026-2021-04-25 (accessed on 10 May 2021).
- USP. Guideline for the Admission of Dietary Supplement Ingredients to the USP–NF Monograph Development Process. Available online: https://www.usp.org/sites/default/files/usp/document/get-involved/submission-guidelines/guideline-for-the-admission-of-dietary-supplement-ingredients.pdf (accessed on 30 July 2021).
- US Food and Drug Administration; US National Library of Medicine. Substance Registration System-Unique Ingredient Indentifier (UNII). 2021. Available online: https://fdasis.nlm.nih.gov/srs/ (accessed on 24 March 2021).
- Gamma-Aminobuytyric-Acid. United States National Institutes of Health. 2021. Available online: https://pubchem.ncbi.nlm.nih.gov/compound/gamma-Aminobutyric-acid (accessed on 5 May 2021).
- Gan, R.-Y.; Lui, W.-Y.; Wu, K.; Chan, C.L.; Dai, S.H.; Sui, Z.Q.; Corke, H. Bioactive compounds and bioactivities of germinated edible seeds and sprouts: An updated review. Trends Food Sci. Technol. 2017, 59, 1–14. [Google Scholar] [CrossRef]
- Akihiro, T.; Koike, S.; Tani, R.; Tominaga, T.; Watanabe, S.; Iijima, Y.; Ezura, H. Biochemical mechanism on GABA accumulation during fruit development in tomato. Plant Cell Physiol. 2008, 49, 1378–1389. [Google Scholar] [CrossRef]
- Oh, S.-H.; Moon, Y.-J.; Oh, C.-H. γ-Aminobutyric acid (GABA) content of selected uncooked foods. Prev. Nutr. Food Sci. 2003, 8, 75–78. [Google Scholar] [CrossRef]
- Nikmaram, N.; Dar, B.N.; Roohinejad, S.; Koubaa, M.; Barba, F.J.; Greiner, R.; Johnson, S.K. Recent advances in gamma-aminobutyric acid (GABA) properties in pulses: An overview. J. Sci. Food Agric. 2017, 97, 2681–2689. [Google Scholar] [CrossRef]
- Li, L.; Liu, B.; Zheng, X. Bioactive ingredients in adzuki bean sprouts. J. Med. Plants Res. 2011, 5, 5894–5898. [Google Scholar]
- Martínez-Villaluenga, C.; Kuo, Y.-H.; Lambein, F.; Frías, J.; Vidal-Valverde, C. Kinetics of free protein amino acids, free non-protein amino acids and trigonelline in soybean (Glycine max L.) and lupin (Lupinus angustifolius L.) sprouts. Eur. Food Res. Technol. 2006, 224, 177–186. [Google Scholar] [CrossRef]
- Xu, J.-G.; Hu, Q.-P. Changes in γ-aminobutyric acid content and related enzyme activities in Jindou 25 soybean (Glycine max L.) seeds during germination. LWT Food Sci. Technol. 2014, 55, 341–346. [Google Scholar] [CrossRef]
- Briguglio, M.; Dell’Osso, B.; Panzica, G.; Malgaroli, A.; Banfi, G.; Zanaboni Dina, C.; Porta, M. Dietary Neurotransmitters: A Narrative Review on Current Knowledge. Nutrients 2018, 10, 591. [Google Scholar] [CrossRef]
- Seok, J.-H.; Park, K.-B.; Kim, Y.-H.; Bae, M.-O.; Lee, M.-K.; Oh, S.-H. Production and characterization of kimchi with enhanced levels of γ-aminobutyric acid. Food Sci. Biotechnol. 2008, 17, 940–946. [Google Scholar]
- Tsushida, T.; Murai, T. Conversion of glutamic acid to. Gamma.-aminobutyric acid in tea leaves under anaerobic conditions. Agric. Biol. Chem. 1987, 51, 2865–2871. [Google Scholar] [CrossRef]
- Diana, M.; Quílez, J.; Rafecas, M. Gamma-aminobutyric acid as a bioactive compound in foods: A review. J. Funct. Foods 2014, 10, 407–420. [Google Scholar] [CrossRef]
- Nantong Licheng Biological Engineeering Co. Ltd.: Asignee Biological method for preparing gamma-aminobutyric acid CN102796779B. 2013. 2012.
- Chung-Ang University Industry-University Cooperation Foundation, Rice Tech, South Korea: Assignee. Novel Strain of Lactic Acid Bacteria Capable of Producing Gamma-Amino Butyric Acid and Preparing Method for Gamma-Amino Butyric Acid Using the Same KR20120007917A. 2012.
- Hanshan Normal University: Assignee. Method for biologically synthesizing gamma-aminobutyric acid by pediococcus pentosaceus CN101654689A. 2011.
- Coda, R.; Melama, L.; Rizzello, C.G.; Curiel, J.A.; Sibakov, J.; Holopainen, U.; Sozer, N. Effect of air classification and fermentation by Lactobacillus plantarum VTT E-133328 on faba bean (Vicia faba L.) flour nutritional properties. Int. J. Food Microbiol. 2015, 193, 34–42. [Google Scholar] [CrossRef]
- Dhakal, R.; Bajpai, V.K.; Baek, K.-H. Production of GABA (γ-aminobutyric acid) by microorganisms: A review. Braz. J. Microbiol. 2012, 43, 1230–1241. [Google Scholar] [CrossRef] [PubMed]
- Xu, N.; Wei, L.; Liu, J. Biotechnological advances and perspectives of gamma-aminobutyric acid production. World J. Microbiol. Biotechnol. 2017, 33, 64. [Google Scholar] [CrossRef] [PubMed]
- Zhu, N.; Wang, T.; Ge, L.; Li, Y.; Zhang, X.; Bao, H. Gamma-Amino Butyric Acid (GABA) Synthesis Enabled by Copper-Catalyzed Carboamination of Alkenes. Org. Lett. 2017, 19, 4718–4721. [Google Scholar] [CrossRef] [PubMed]
- Martin, D.L.; Rimvall, K. Regulation of γ-aminobutyric acid synthesis in the brain. J. Neurochem. 1993, 60, 395–407. [Google Scholar] [CrossRef]
- The Dietary Supplements Labels Database (DSLD). 2021. Available online: http://www.dsld.nlm.nih.gov/dsld/index.jsp (accessed on 30 July 2021).
- U.S. Food and Drug Administration. GRAS Notices. 2021. Available online: https://www.cfsanappsexternal.fda.gov/scripts/fdcc/?set=GRASNotices&sort=GRN_No&order=DESC&startrow=1&type=basic&search=Pharma%20Foods%20International%20Co.%2C%20LTD (accessed on 30 March 2021).
- Pharma Foods International Co., Ltd. Gamma-Amino Butyric Acid (GABA) GRAS Determination. GRAS Notice No. GRN 000257; Pharma Foods International Co., Ltd.: Kyoto, Japan, 2008. [Google Scholar]
- Substances Added to Food (Formerly EAFUS) 2018. Available online: https://www.cfsanappsexternal.fda.gov/scripts/fdcc/index.cfm?set=FoodSubstances&id=AMINOBUTYRICACID (accessed on 2 June 2021).
- Environmental Protection Agency, USA. L-Glutamic Acid and Gamma Aminobutyric Acid: Order Denying Objections to Issuance of Tolerance. 40 CFR Part 180; EPA: Washington, DC, USA, 2004; Volume 69. Available online: http://www.epa.gov/edocket (accessed on 30 July 2021).
- NHPD. Listing of Drugs Currently Regulated as New Drugs (The New Drugs List). 2012. Available online: http://www.hc-sc.gc.ca/dhp-mps/prodpharma/applic-demande/guide-ld/newdrug-drognouv/ndrugs_ndrogue-eng.php#fnb4 (accessed on 25 June 2021).
- EFSA. EFSA Panel on Dietetic Products, Nutrition and Allergies (NDA); Scientific Opinion on the Substantiation of Health Claims Related to Gamma-Aminobutyric Acid and Cognitive Function (ID 1768) Pursuant to Article 13 of Regulation (EC) No 1924/2006 on Request from the European Commission. EFSA J. 2009, 7, 1274. Available online: http://www.efsa.europa.eu/en/efsajournal/doc/1274.pdf (accessed on 2 June 2021).
- New Zealand. Misuse of Drugs Act. 1975. Available online: https://www.legislation.govt.nz/act/public/1975/0116/latest/DLM436101.html (accessed on 30 July 2021).
- Natural and Non-Prescription Health Products Directorate (NNHPD). Natural Health Products Ingredients Database. 4-aminobutanoic acid. Group 7: Ingredients with Relaxation Action. 2021. Available online: http://webprod.hc-sc.gc.ca/nhpid-bdipsn/atReq.do?atid=fonc.cognitive.func&lang=eng (accessed on 30 July 2021).
- JECFA. Joint FAO/WHO Expert Committee on Food Additives World Health Organization, Evaluation of Certain Food Additives and Contaminants: Sixty-First Report of the Joint FAO/WHO Expert Committee on Food Additives; World Health Organization: Geneva, Switzerland, 2004; Volume 61. [Google Scholar]
- Cavagnini, F.; Pinto, M.; Dubini, A.; Invitti, C.; Cappelletti, G.; Polli, E.E. Effects of gamma aminobutyric acid (GABA) and muscimol on endocrine pancreatic function in man. Metabolism 1982, 31, 73–77. [Google Scholar] [CrossRef]
- Kimura, M. Effects of fermented milk containing γ-aminobutyric acid on normal adult subjects. Jpn. J. Food Chem. 2002, 9, 1–6. [Google Scholar]
- Yamatsu, A. The Beneficial Effects of Coffee on Stress and Fatigue can be Enhanced by the Addition of GABA―A Randomized, Double‒blind, Placebo Controlled, Crossover‒designed Study. Jpn. Pharmacol. Ther. 2015, 43, 515–519. [Google Scholar]
- Yamatsu, A.; Yamashita, Y.; Maru, I.; Yang, J.; Tatsuzaki, J.; Kim, M. The Improvement of Sleep by Oral Intake of GABA and Apocynum venetum Leaf Extract. J. Nutr. Sci. Vitaminol. 2015, 61, 182–187. [Google Scholar] [CrossRef]
- Yamatsu, A. Beneficial action of GABA on sleep and frequent night urination in the elderly. Jpn. Pharmacol. Ther. 2013, 41, 985–988. [Google Scholar]
- Yoshida, S.; Haramoto, M.; Fukuda, T.; Mizuno, H.; Tanaka, A.; Nishimura, M.; Nishihira, J. Optimization of a gamma-aminobutyric acid (GABA) enrichment process for Hokkaido white rice and the effects of GABA-enriched white rice on stress relief in humans. Nippon Shokuhin Kagaku Kogaku Kaishi. 2015, 62, 95–103. [Google Scholar] [CrossRef]
- Okada, T.; Sugishita, T.; Murakami, T.; Murai, H.; Saikusa, T.; Horino, T.; Takahashi, T. Effect of the defatted rice germ enriched with GABA for sleeplessness, depression, autonomic disorder by oral administration. Nippon. Shokuhin Kagaku Kogaku Kaishi J. Jpn. Soc. Food Sci. Technol. 2000, 47, 596–603. [Google Scholar] [CrossRef]
- Tanaka, H.; Watanabe, K.; Ma, M.; Hirayama, M.; Kobayashi, T.; Oyama, H.; Aizawa, Y. The Effects of gamma-Aminobutyric Acid, Vinegar, and Dried Bonito on Blood Pressure in Normotensive and Mildly or Moderately Hypertensive Volunteers. J. Clin. Biochem. Nutr. 2009, 45, 93–100. [Google Scholar] [CrossRef] [PubMed]
- Powers, M.E.; Yarrow, J.F.; Mccoy, S.C.; Borst, S.E. Growth hormone isoform responses to GABA ingestion at rest and after exercise. Med. Sci. Sports Exerc. 2008, 40, 104. [Google Scholar] [CrossRef] [PubMed]
- Byun, J.-I.; Shin, Y.Y.; Chung, S.-E.; Shin, W.C. Safety and efficacy of gamma-aminobutyric acid from fermented rice germ in patients with insomnia symptoms: A randomized, double-blind trial. J. Clin. Neurol. 2018, 14, 291. [Google Scholar] [CrossRef] [PubMed]
- Watanabe, T.; Yamada, T.; Tanaka, H.; Jiang, S.; Mazumder, T.K.; Nagai, S.H.I.R.O.; Tsuji, K.E.I.S.U.K.E. Antihypertensive effect of gamma-aminobutyric acid-enriched Agaricus blazei on spontaneously hypertensive rats. J. Jpn. Soc. Food Sci. Technol. 2002, 49, 166–173. [Google Scholar] [CrossRef]
- Matsubara, F.; Ueno, H.; Tadano, K.; Suyama, T.; Imaizumi, K.; Suzuki, T.; Saruta, T. Effects of GABA supplementation on blood pressure and safety in adults with mild hypertension. Jpn. Pharmacol. Ther. 2002, 30, 963–972. [Google Scholar]
- Inoue, K.; Shirai, T.; Ochiai, H.; Kasao, M.; Hayakawa, K.; Kimura, M.; Sansawa, H. Blood-pressure-lowering effect of a novel fermented milk containing gamma-aminobutyric acid (GABA) in mild hypertensives. Eur. J. Clin. Nutr. 2003, 57, 490–495. [Google Scholar] [CrossRef]
- Kajimoto, O.; Hirata, H.; Nishimura, A. Hypotensive action of novel fermented milk containing γ-aminobutyric acid (GABA) in subjects with mild or moderate hypertension. J. Nutr. Food 2003, 6, 51–64. [Google Scholar]
- Kajimoto, O.; Hirata, H.; Nakagawa, S.; Kajimoto, Y.; Hayakawa, K.; Kimura, M. Hypotensive effect of fermented milk containing gamma-aminobutyric acid (GABA) in subjects with high normal blood pressure. J. Jpn. Soc. Food Sci. Technol. 2004, 51, 79–86. [Google Scholar] [CrossRef]
- Kanehira, T.; Nakamura, Y.; Nakamura, K.; Horie, K.; Horie, N.; Furugori, K.; Yokogoshi, H. Relieving occupational fatigue by consumption of a beverage containing γ-amino butyric acid. J. Nutr. Sci. Vitaminol. 2011, 57, 9–15. [Google Scholar] [CrossRef] [PubMed]
- Cavagnini, F.; Benetti, G.; Invitti, C.; Ramella, G.; Pinto, M.; Lazza, M.; Müller, E. Effect of γ-Aminobutyric Acid on Growth Hormone and Prolactin Secretion in Man: Influence of Pimozide and Domperidone*. J. Clin. Endocrinol. Metab. 1980, 51, 789–792. [Google Scholar] [CrossRef] [PubMed]
- Cavagnini, F.; Invitti, C.; Pinto, M.; Maraschini, C.; Di Landro, A.; Dubini, A.; Marelli, A. Effect of acute and repeated administration of gamma aminobutyric acid (GABA) on growth hormone and prolactin secretion in man. Acta Endocrinol. 1980, 93, 149–154. [Google Scholar] [CrossRef]
- Hinton, T.; Jelinek, H.F.; Viengkhou, V.; Johnston, G.A.; Matthews, S. Effect of GABA-Fortified Oolong Tea on Reducing Stress in a University Student Cohort. Front. Nutr. 2019, 6, 27. [Google Scholar] [CrossRef]
- Fujibayashi, M. Activation autonomic nervous system activity by the oral ingestion of GABA. J. Jpn. Soc. Nutr. Food Sci. 2008, 61, 129–133. [Google Scholar] [CrossRef]
- Nakamura, H.; Takishima, T.; Kometani, T.; Yokogoshi, H. Psychological stress-reducing effect of chocolate enriched with γ-aminobutyric acid (GABA) in humans: Assessment of stress using heart rate variability and salivary chromogranin A. Int. J. Food Sci. Nutr. 2009, 60, 106–113. [Google Scholar] [CrossRef] [PubMed]
- Okita, Y.; Nakamura, H.; Kouda, K.; Takahashi, I.; Takaoka, T.; Kimura, M.; Sugiura, T. Effects of vegetable containing gamma-aminobutyric acid on the cardiac autonomic nervous system in healthy young people. J. Physiol. Anthropol. 2009, 28, 101–107. [Google Scholar] [CrossRef] [PubMed]
- Yoto, A.; Murao, S.; Motoki, M.; Yokoyama, Y.; Horie, N.; Takeshima, K.; Yokogoshi, H. Oral intake of gamma-aminobutyric acid affects mood and activities of central nervous system during stressed condition induced by mental tasks. Amino Acids 2012, 43, 1331–1337. [Google Scholar] [CrossRef] [PubMed]
- Abdou, A.M.; Higashiguchi, S.; Horie, K.; Kim, M.; Hatta, H.; Yokogoshi, H. Relaxation and immunity enhancement effects of gamma-aminobutyric acid (GABA) administration in humans. Biofactors 2006, 26, 201–208. [Google Scholar] [CrossRef]
- Yamakoshi, J.; Shiojo, R.; Nakagawa, S.; Izui, N. Hypotensive effects and safety of less-salt soy sauce containing y-aminobutyric acid (GABA) on high-normal blood pressure and mild hypertensive subjects. Yakuri Chiryo. 2006, 34, 691–709. [Google Scholar]
- Shin, Y.Y.; Byun, J.-I.; Chung, S.-E.; Seong, M.J.; Cho, H.A.; Cha, H.K.; Shin, W.C. Effect of low and high-dose GABA from unpolished rice-germ on timing and quality of sleep: A randomized double-blind placebo-controlled trial. J. Sleep Med. 2016, 13, 60–66. [Google Scholar] [CrossRef]
- Reid, S.N.; Ryu, J.-k.; Kim, Y.; Jeon, B.H. The effects of fermented Laminaria japonica on short-term working memory and physical fitness in the elderly. Evid. Based Complementary Altern. Med. 2018, 2018. [Google Scholar] [CrossRef]
- NIH. Evaluation of Safety and Diabetes Status upon Oral Treatment with GABA in Patients with Longstanding Type-1 Diabetes. ClinicalTrials.gov Identifier: NCT03635437. Updated September 16, 2020. 2021. Available online: https://clinicaltrials.gov/ct2/show/study/NCT03635437 (accessed on 13 April 2021).
- The Cochrane Collaboration. Available online: http://www.cochrane.org/cochrane-reviews (accessed on 14 November 2020).
- Health Canada. Canada Vigilance Adverse Reaction. Available online: http://webprod3.hc-sc.gc.ca/arquery-rechercheei/index-eng.jsp (accessed on 28 February 2021).
- The Australian Therapeutic Goods Administration. Available online: http://tga.gov.au/ (accessed on 25 July 2021).
- Pharma Foods International Co., Ltd. Acute Toxicity Test; Japan Food Research Laboratories for Pharma Foods International Co., Ltd. (PFI); (cited in GRN 000595); Nishikyo-Ku Kyoto, Japan, 2002. Available online: https://www.fda.gov/media/97030/download (accessed on 25 July 2021).
- Oshima, Y.; Kasahara, A.; Shibata, M.; Mogi, M. [Studies on DL-alpha-lipoic acid derivatives. II. On the Pharmacological activities of 4-(DL-alpha-lipamido) butyric acid (LABA)]. (cited in GRN 000257). Yakugaku Zasshi 1965, 85, 463–468. [Google Scholar] [CrossRef][Green Version]
- Hayami, Y.; Kotamtani, K.; Hashimoto, K.; Hanazumk, C.; Komemochi, C. Short-Term Toxicity Tests Using PG2K20. Japan Science Diet Association for Pharma Foods International Co., Ltd. (PFI): Nishikyo-Ku Kyoto, Japan, 2005. [Google Scholar]
- Takeshima, K.; Yamatsu, A.; Yamashita, Y.; Watabe, K.; Horie, N.; Masuda, K.; Kim, M. Subchronic toxicity evaluation of gamma-aminobutyric acid (GABA) in rats. Food Chem. Toxicol. 2014, 68, 128–134. [Google Scholar] [CrossRef]
- Yang, H.; Xing, R.; Liu, S.; Yu, H.; Li, P. Analysis of the protective effects of gamma-aminobutyric acid during fluoride-induced hypothyroidism in male Kunming mice. Pharm. Biol. 2019, 57, 29–37. [Google Scholar] [CrossRef]
- Osawa, T.; Goto, T.; Oyama, W.; Yasutake, N.; Onoue, M. Mutagenicicty test of gamma-aminobutyric acid-containing fermented milk “GABA-10” and GABA-25” using DNA repair system (cited in GRN 000 595). Yakuruto Kenkyujo Kenkyu Hokokushu 2005, 23, 67–72. [Google Scholar]
- Calogero, A.E.; Hall, J.; Fishel, S.; Green, S.; Hunter, A.; D’Agata, R. Effects of gamma-aminobutyric acid on human sperm motility and hyperactivation. Mol. Hum. Reprod. 1996, 2, 733–738. [Google Scholar] [CrossRef] [PubMed]
- de las Heras, M.A.; Valcarcel, A.; Perez, L.J. In vitro capacitating effect of gamma-aminobutyric acid in ram spermatozoa. Biol. Reprod. 1997, 56, 964–968. [Google Scholar] [CrossRef] [PubMed]
- Shi, Q.X.; Yuan, Y.Y.; Roldan, E.R. gamma-Aminobutyric acid (GABA) induces the acrosome reaction in human spermatozoa. Mol. Hum. Reprod 1997, 3, 677–683. [Google Scholar] [CrossRef]
- Kurata, S.; Hiradate, Y.; Umezu, K.; Hara, K.; Tanemura, K. Capacitation of mouse sperm is modulated by GABA (gamma-aminobutyric acid) concentration. J. Reprod. Dev. 2019, 65, 327–334. [Google Scholar] [CrossRef]
- Yanagimachi, R. Mechanisms of fertilization in mammals. In Fertilization and Embryonic Development In Vitro; Springer: Berlin/Heidelberg, Germany, 1981; pp. 81–182. [Google Scholar]
- Licht, P.; Harbarth, P.; Merz, W.E. Evidence for a modulation of human chorionic gonadotropin (hCG) subunit messenger ribonucleic acid levels and hCG secretion by gamma-aminobutyric acid in human first trimester placenta in vitro. Endocrinology 1992, 130, 490–496. [Google Scholar] [CrossRef] [PubMed]
- Ritta, M.N.; Campos, M.B.; Calandra, R.S. Effect of GABA and benzodiazepines on testicular androgen production. Life Sci. 1987, 40, 791–798. [Google Scholar] [CrossRef]
- Awapara, J.; Landua, A.J.; Fuerst, R.; Seale, B. Free gamma-aminobutyric acid in brain. J. Biol. Chem. 1950, 187, 35–39. [Google Scholar] [CrossRef]
- Awapara, J. Occurrence of free gamma-aminobutyric acid in brain and its formation from L-glutamic acid. Tex. Rep. Biol. Med. 1950, 8, 443–447. [Google Scholar]
- Elliott, K.A.; Hobbiger, F. gamma Aminobutyric acid; circulatory and respiratory effects in different species; re-investigation of the anti-strychnine action in mice. J. Physiol. 1959, 146, 70–84. [Google Scholar] [CrossRef]
- Van Gelder, N.M.; Elliott, K.A. Disposition of gamma-aminobutyric acid administered to mammals. J. Neurochem. 1958, 3, 139–143. [Google Scholar] [CrossRef]
- Hespe, W.; Roberts, E.; Prins, H. Autoradiographic investigation of the distribution of [14C]GABA in tissues of normal and aminooxyacetic acid-treated mice. Brain Res. 1969, 14, 663–671. [Google Scholar] [CrossRef]
- Thwaites, D.T.; Basterfield, L.; McCleave, P.M.; Carter, S.M.; Simmons, N.L. Gamma-Aminobutyric acid (GABA) transport across human intestinal epithelial (Caco-2) cell monolayers. Br. J. Pharmacol. 2000, 129, 457–464. [Google Scholar] [CrossRef] [PubMed]
- Nacher, A.; Polache, A.; Moll-Navarro, M.J.; Pla-Delfina, J.M.; Merino, M. Intestinal absorption pathway of gamma-aminobutyric acid in rat small intestine. Biopharm. Drug Dispos. 1994, 15, 359–371. [Google Scholar] [CrossRef] [PubMed]
- Li, J.; Zhang, Z.; Liu, X.; Wang, Y.; Mao, F.; Mao, J.; Wang, Q. Study of GABA in Healthy Volunteers: Pharmacokinetics and Pharmacodynamics. Front. Pharmacol. 2015, 6, 260. [Google Scholar] [CrossRef] [PubMed]
- Kuriyama, K.; Sze, P. Blood-brain barrier to H 3-γ-aminobutyric acid in normal and amino oxyacetic acid-treated animals. Neuropharmacology 1971, 10, 103–108. [Google Scholar] [CrossRef]
- Oldendorf, W.H. Brain uptake of radiolabeled amino acids, amines, and hexoses after arterial injection. Am. J. Physiol. 1971, 221, 1629–1639. [Google Scholar] [CrossRef] [PubMed]
- Frey, H.H.; Loscher, W. Cetyl GABA: Effect on convulsant thresholds in mice and acute toxicity. Neuropharmacology 1980, 19, 217–220. [Google Scholar] [CrossRef]
- Krantis, A. The involvement of GABA-transaminase in the blood-brain barrier to radiolabelled GABA. Acta Neuropathol. 1984, 64, 61–67. [Google Scholar] [CrossRef]
- Al-Awadi, M.; Pavlik, A.; Al-Sarraf, H. Increased brain uptake and brain to blood efflux transport of 14 C-GABA in spontaneously hypertensive rats. Life Sci. 2006, 79, 847–853. [Google Scholar] [CrossRef]
- Al-Sarraf, H. Transport of 14 C-γ-aminobutyric acid into brain, cerebrospinal fluid and choroid plexus in neonatal and adult rats. Dev. Brain Res. 2002, 139, 121–129. [Google Scholar] [CrossRef]
- Knych, H.K.; Steinmetz, S.J.; McKemie, D.S. Endogenous concentrations, pharmacokinetics, and selected pharmacodynamic effects of a single dose of exogenous GABA in horses. J. Vet. Pharmacol. Ther. 2015, 38, 113–122. [Google Scholar] [CrossRef]
- Kakee, A.; Takanaga, H.; Terasaki, T.; Naito, M.; Tsuruo, T.; Sugiyama, Y. Efflux of a suppressive neurotransmitter, GABA, across the blood-brain barrier. J. Neurochem. 2001, 79, 110–118. [Google Scholar] [CrossRef] [PubMed]
- Takahashi, H.; Sumi, M.; Koshino, F. Effect of gamma-aminobutyric acid (GABA) on normotensive or hypertensive rats and men. Jpn. J. Physiol. 1961, 11, 89–95. [Google Scholar] [CrossRef] [PubMed]
- Shimada, M.; Hasegawa, T.; Nishimura, C.; Kan, H.; Kanno, T.; Nakamura, T.; Matsubayashi, T. Anti-Hypertensive Effect of γ-Aminobutyric Acid (GABA)-Rich Chlorella on High-Normal Blood Pressure and Borderline Hypertension in Placebo-Controlled Double-Blind Study. Clin. Exp. Hypertens. 2009, 31, 342–354. [Google Scholar] [CrossRef]
- Abe, Y.; Umemura, S.; Sugimoto, K.; Hirawa, N.; Kato, Y.; Yokoyama, N.; Ishii, M. Effect of green tea rich in γ-aminobutyric acid on blood pressure of Dahl salt-sensitive rats. Am. J. Hypertens. 1995, 8, 74–79. [Google Scholar] [CrossRef]
- Hayakawa, K.; Kimura, M.; Kasaha, K.; Matsumoto, K.; Sansawa, H.; Yamori, Y. Effect of a γ-aminobutyric acid-enriched dairy product on the blood pressure of spontaneously hypertensive and normotensive Wistar–Kyoto rats. Br. J. Nutr. 2004, 92, 411–417. [Google Scholar] [CrossRef] [PubMed]
- Yoshimura, M.; Toyoshi, T.; Sano, A.; Izumi, T.; Fujii, T.; Konishi, C.; Obata, A. Antihypertensive effect of a gamma-aminobutyric acid rich tomato cultivar ‘DG03-9’ in spontaneously hypertensive rats. J. Agric. Food Chem. 2010, 58, 615–619. [Google Scholar] [CrossRef]
- Loeb, C.; Benassi, E.; Bo, G.-P.; Cocito, L.; Maffini, M.; Scotto, P. Preliminary evaluation of the effect of GABA and phosphatidylserine in epileptic patients. Epilepsy Res. 1987, 1, 209–212. [Google Scholar] [CrossRef]
- Boonstra, E.; de Kleijn, R.; Colzato, L.S.; Alkemade, A.; Forstmann, B.U.; Nieuwenhuis, S. Neurotransmitters as food supplements: The effects of GABA on brain and behavior. Front. Psychol. 2015, 6, 1520. [Google Scholar] [CrossRef]
- Bessman, S.P.; Rossen, J.; Layne, E.C. Gamma-Aminobutyric acid-glutamic acid transamination in brain. J. Biol. Chem. 1953, 201, 385–391. [Google Scholar] [CrossRef]
- Kim, S.; Jo, K.; Hong, K.B.; Han, S.H.; Suh, H.J. GABA and l-theanine mixture decreases sleep latency and improves NREM sleep. Pharm. Biol. 2019, 57, 65–73. [Google Scholar] [CrossRef] [PubMed]
- Kajimoto, H.H.; Nakagawa, S.; Kajimoto, Y.; Hayakawa, K.; Kimura, M. Hypotensive effect of fermented milk containing y-aminobutyric acid (GABA) in subjects with high normal blood pressure. Nihon Shokuhin Kagaku Kogakkaishi 2003, 51, 79–86. [Google Scholar]
- Kato, I.; Shimizu, S.; Kobayashi, T. Single-dose 1 month repeated dose, and 3-month repeated dose oral toxicity studies of fermented milk containing.Gamma.-aminobutyric acid (GABA) in rodents. Yakuruto Kenkyujo Kenkyu Hokokushu 2005, 24, 43–66. [Google Scholar]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Oketch-Rabah, H.A.; Madden, E.F.; Roe, A.L.; Betz, J.M. United States Pharmacopeia (USP) Safety Review of Gamma-Aminobutyric Acid (GABA). Nutrients 2021, 13, 2742. https://doi.org/10.3390/nu13082742
Oketch-Rabah HA, Madden EF, Roe AL, Betz JM. United States Pharmacopeia (USP) Safety Review of Gamma-Aminobutyric Acid (GABA). Nutrients. 2021; 13(8):2742. https://doi.org/10.3390/nu13082742
Chicago/Turabian StyleOketch-Rabah, Hellen A., Emily F. Madden, Amy L. Roe, and Joseph M. Betz. 2021. "United States Pharmacopeia (USP) Safety Review of Gamma-Aminobutyric Acid (GABA)" Nutrients 13, no. 8: 2742. https://doi.org/10.3390/nu13082742
APA StyleOketch-Rabah, H. A., Madden, E. F., Roe, A. L., & Betz, J. M. (2021). United States Pharmacopeia (USP) Safety Review of Gamma-Aminobutyric Acid (GABA). Nutrients, 13(8), 2742. https://doi.org/10.3390/nu13082742