The Diabetes Eating Problem Survey-Revised (DEPS-R) in a Greek Adult Population with Type 1 Diabetes Mellitus: Model Comparison Supporting a Single Factor Structure
Abstract
:1. Introduction
1.1. Diabetes Mellitus and Diabulimia
1.2. Factors Associated with Development of EDs in People with T1DM
1.3. The Diabetes Eating Problem Survey-Revised Version (DEPS-R)
1.4. Objective of the Present Study
2. Materials and Methods
2.1. Participants
2.2. Screening Tool
2.3. Sample and Data Collection Procedure
2.4. Analytical Approach-Statistical Analysis
3. Results
3.1. Participants
3.2. DEPS-R Scale
3.3. Association between Patient Characteristics and Scores on DEPS-R
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Wade, T.D. Recent Research on Bulimia Nervosa. Psychiatr. Clin. 2019, 42, 21–32. [Google Scholar] [CrossRef] [PubMed]
- Toni, G.; Berioli, M.G.; Cerquiglini, L.; Ceccarini, G.; Grohmann, U.; Principi, N.; Esposito, S. Eating disorders and disordered eating symptoms in adolescents with type 1 diabetes. Nutrients 2017, 9, 906. [Google Scholar] [CrossRef] [Green Version]
- Falcão, M.A.; Francisco, R. Diabetes, eating disorders and body image in young adults: An exploratory study about “diabulimia”. Eat Weight Disord. 2017, 22, 675–682. [Google Scholar] [CrossRef] [PubMed]
- Keane, S.; Clarke, M.; Murphy, M.; McGrath, D.; Smith, D.; Farrelly, N.; MacHale, S. Disordered eating behaviour in young adults with type 1 diabetes mellitus. J. Eat. Disord. 2018, 6, 1–6. [Google Scholar] [CrossRef]
- Weinger, K.; Beverly, E.A. Barriers to achieving glycemic targets: Who omits insulin and why? Diabetes Care Am. Diabetes Assoc. 2010, 33, 450–452. [Google Scholar] [CrossRef] [Green Version]
- Broadley, M.M.; White, M.J.; Andrew, B. Executive function is associated with diabetes-specific disordered eating in young adults with type 1 diabetes. J. Psychosom. Res. 2018, 111, 1–12. [Google Scholar] [CrossRef] [Green Version]
- Neumark-Sztainer, D.; Patterson, J.; Mellin, A.; Ackard, D.M.; Utter, J.; Story, M.; Sockalosky, J. Weight control practices and disordered eating behaviors among adolescent females and males with type 1 diabetes: Associations with sociodemographics, weight concerns, familial factors, and metabolic outcomes. Diabetes Care 2002, 25, 1289–1296. [Google Scholar] [CrossRef] [Green Version]
- Markowitz, J.T.; Butler, D.A.; Volkening, L.K.; Antisdel, J.E.; Anderson, B.J.; Laffel, L.M.B. Brief screening tool for disordered eating in diabetes: Internal consistency and external validity in a contemporary sample of pediatric patients with type 1 diabetes. Diabetes Care 2010, 33, 495–500. [Google Scholar] [CrossRef] [Green Version]
- Pinna, F.; Diana, E.; Sanna, L.; Deiana, V.; Manchia, M.; Nicotra, E.; Fiorillo, A.; Albert, U.; Nivoli, A.; Volpe, U.; et al. Assessment of eating disorders with the diabetes eating problems survey—Revised (DEPS-R) in a representative sample of insulin-treated diabetic patients: A validation study in Italy. BMC Psychiatry 2017, 17, 262. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Wisting, L.; Wonderlich, J.; Skrivarhaug, T.; Dahl-Jørgensen, K.; Rø, Ø. Psychometric properties and factor structure of the diabetes eating problem survey—Revised (DEPS-R) among adult males and females with type 1 diabetes. J. Eat. Disord. 2019, 7, 1–7. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Pursey, K.M.; Hart, M.; Jenkins, L.; McEvoy, M.; Smart, C.E. Screening and identification of disordered eating in people with type 1 diabetes: A systematic review. J. Diabetes Complicat. 2020, 34, 107522. [Google Scholar] [CrossRef] [PubMed]
- Saßmann, H.; Albrecht, C.; Busse-Widmann, P.; Hevelke, L.K.; Kranz, J.; Markowitz, J.T.; Marshall, L.F.; Meurs, S.; De Soye, I.H.; Lange, K. Psychometric properties of the German version of the Diabetes Eating Problem Survey-Revised: Additional benefit of disease-specific screening in adolescents with Type 1 diabetes. Diabet. Med. 2015, 32, 1641–1647. [Google Scholar] [CrossRef]
- Gagnon, C.; Aime, A.; Belanger, C. Psychometric properties of the French Diabetes Eating Problem Survey–Revised (DEPS-R). BAOJ Diabet. 2017, 3, 1–8. [Google Scholar]
- Sancanuto, C.; Jiménez-Rodríguez, D.; Tébar, F.J.; Hernández-Morante, J.J. Translation and validation of the Diabetes Eating Problem Survey to screen eating disorders in patients with type-1 diabetes mellitus. Med. Clín. 2017, 148, 548–554. [Google Scholar] [CrossRef]
- Atik Altınok, Y.; Özgür, S.; Meseri, R.; Özen, S.; Darcan, Ş.; Gökşen, D. Reliability and validity of the diabetes eating problem survey in Turkish children and adolescents with type 1 diabetes mellitus. JCRPE J. Clin. Res. Pediatr. Endocrinol. 2017, 9, 323–328. [Google Scholar] [CrossRef] [PubMed]
- Wisting, L.; Frøisland, D.H.; Skrivarhaug, T.; Dahl-Jørgensen, K.; Rø, Ø. Psychometric properties, norms, and factor structure of the diabetes eating problem survey-revised in a large sample of children and adolescents with type 1 diabetes. Diabetes Care 2013, 36, 2198–2202. [Google Scholar] [CrossRef] [Green Version]
- Lv, W.; Zhong, Q.; Guo, J.; Luo, J.; Dixon, J.; Whittemore, R. Instrument context relevance evaluation, translation, and psychometric testing of the diabetes eating problem survey-revised (DEPS-R) among people with type 1 diabetes in China. Int. J. Environ. Res. Public Health 2021, 18, 3450. [Google Scholar] [CrossRef] [PubMed]
- Apergi, Κ.; Romanidou, Μ.; Abdelkhalek, H.; Tripsianis, G.; Gonidakis, F. Reliability and validity of the Diabetes Eating Problem Survey in Greek adults with type 1 diabetes mellitus. Psychiatrike 2020, 31, 310–320. [Google Scholar] [CrossRef]
- Bentler, P.M. Comparative fit indexes in structural models. Psychol. Bull. 1990, 107, 238–246. [Google Scholar] [CrossRef]
- Hu, L.T.; Bentler, P.M. Cutoff criteria for fit indexes in covariance structure analysis: Conventional criteria versus new alternatives. Struct. Equ. Model. 1999, 6, 1–55. [Google Scholar] [CrossRef]
- Smith, T.M.; Krishnan, S.; Hong, I.; Reistetter, T.A. Measurement validity of the low vision independence measure (LVIM). Am. J. Occup. Ther. 2019, 73, 7303205070p1–7303205070p11. [Google Scholar] [CrossRef] [PubMed]
- Marsh, H.W.; Balla, J. Goodness of fit in confirmatory factor analysis: The effects of sample size and model parsimony. Qual. Quant. 1994, 28, 185–217. [Google Scholar] [CrossRef]
- Mulaik, S.A.; James, L.R.; Van Alstine, J.; Bennett, N.; Lind, S.; Stilwell, C.D. Evaluation of goodness-of-fit indices for structural equation models. Psychol. Bull. 1989, 105, 430–445. [Google Scholar] [CrossRef]
- Wisting, L.; Skrivarhaug, T.; Dahl-Jørgensen, K.; Rø, Ø. Prevalence of disturbed eating behavior and associated symptoms of anxiety and depression among adult males and females with type 1 diabetes. J. Eat. Disord. 2018, 6, 1–10. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Ryman, B.; MacIsaac, J.; Robinson, T.; Miller, M.R.; Herold Gallego, P. Assessing the clinical utility of the diabetes eating problem survey-revised (DEPS-R) in adolescents with type 1 diabetes. Endocrinol. Diabetes Metab. 2019, 2, 67. [Google Scholar] [CrossRef] [PubMed] [Green Version]
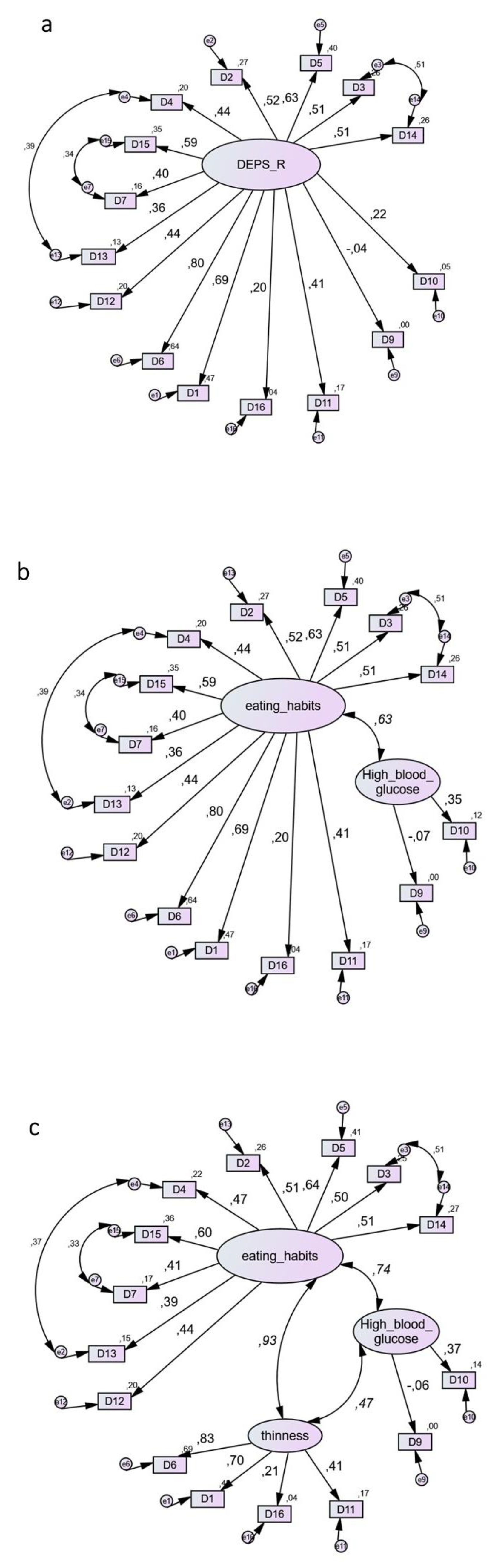
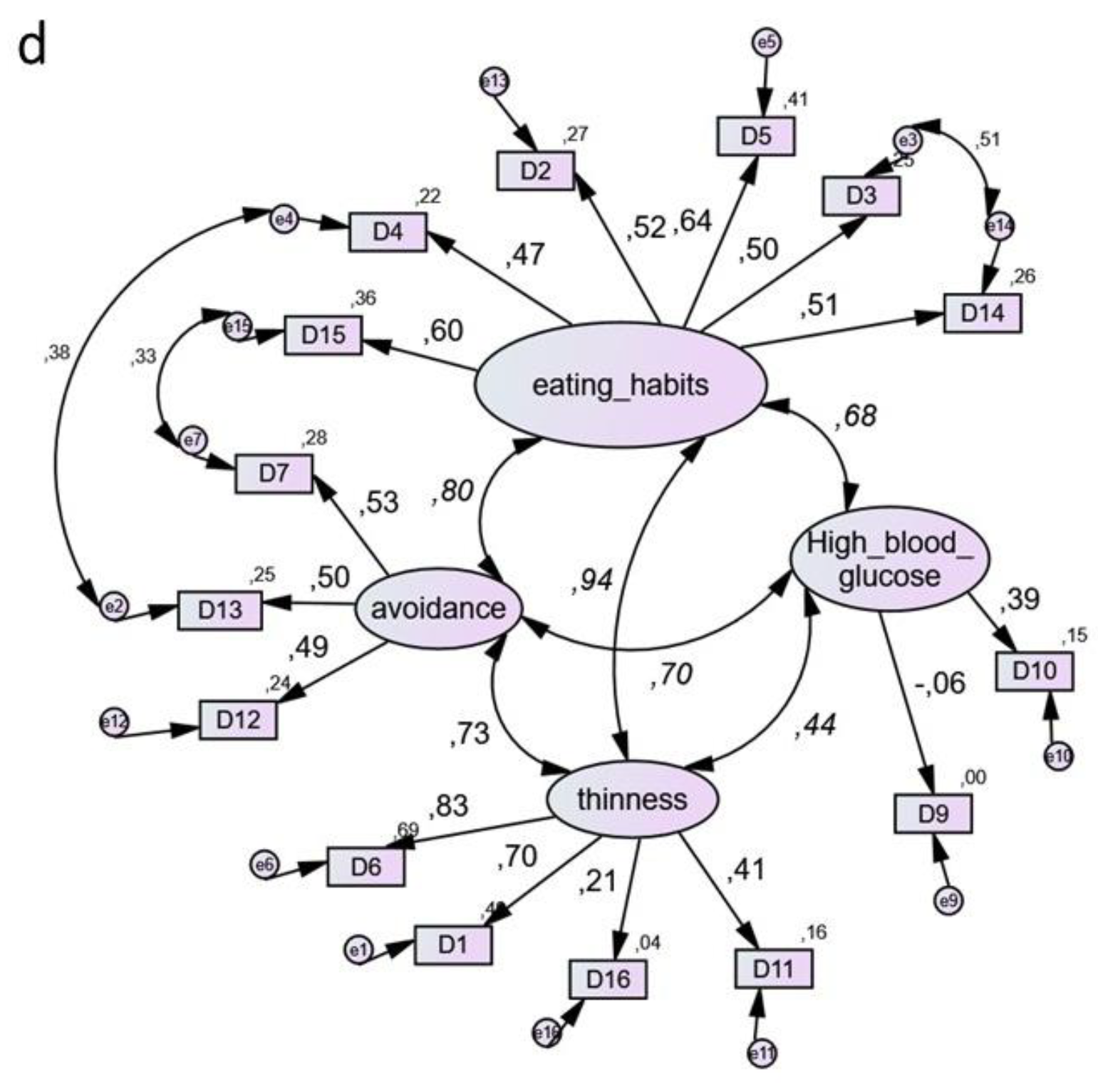
| Characteristics | All (N = 103) | Male (N = 25) | Female (N = 78) | p-Value |
|---|---|---|---|---|
| Sociodemographic | ||||
| Age (Median, IQR; years) | 37 (22) | 40 (20.5) | 35 (21.5) | 0.035 |
| Anthropometric | ||||
| Weight (Median, IQR; kg) | 68.5 (22) | 80 (13) | 63 (15) | ≤0.001 |
| Height (Median, IQR; cm) | 167 (14) | 178 (13) | 165 (9) | ≤0.001 |
| BMI (Median, IQR; kg/m2) | 23.96 (5.79) | 25.51 (3.94) | 23.27 (5.83) | 0.012 |
| Clinical | ||||
| Diabetes Duration (Mean, SD; years) | 18.32 ± 12.4 | 20.64 ± 12.38 | 17.58 ± 12.4 | 0.285 1 |
| Type of treatment (N; %) | ||||
| MDI | 72 (69.9%) | 15 (60%) | 57 (73.1%) | 0.322 2 |
| CSII | 31 (30.1%) | 10 (40%) | 21 (26.9%) | |
| Use of CGM (N, %; Yes) | 75 (73.5%) | 20 (80%) | 55 (71.4%) | 0.560 2 |
| Total daily dose (Median, IQR; iu) | 37 (18) | 40 (23.5) | 36.5 (20) | 0.047 |
| Glycemic control | ||||
| FBG (Mean, SD; mg/dL) | 113.2 ± 31.42 | 115.32 ± 43.04) | 112.53 ± 28.53 | 0.285 1 |
| HbA1c (Median, IQR; %) | 6.8 (1) | 6.8 (1) | 6.8 (1) | 0.754 |
| BG measurements/day (Median, IQR) | 7.0 (10) | 5.5 (4.8) | 7.0 (11) | 0.010 |
| Hypoglycemic events (Median, IQR) | 5.0 (6) | 5.0 (10) | 5.0 (6) | 0.844 |
| TIR (Median, IQR; %) | 71.5 (22.5) | 79.5 (15.8) | 68.5 (24.5) | 0.058 |
| TAR (Median, IQR; %) | 19 (24) | 14 (13) | 20.5 (25) | 0.144 |
| TBR (Median, IQR; %) | 6 (9) | 8 (8) | 5 (9) | 0.440 |
| Characteristics | DEPS-R Negative | DEPS-R Positive | p-Value |
|---|---|---|---|
| (N = 72) | (N = 31) | ||
| Sociodemographic | |||
| Gender (N; %) | |||
| Male | 18 (25%) | 7 (22.6%) | 0.990 1 |
| Female | 54 (75%) | 24 (77.4%) | |
| Age (Median, IQR; years) | 37 (23.8) | 37 (21) | 0.986 |
| Anthropometric data | |||
| Weight (Median, IQR; kg) | 63 (19) | 80 (20) | ≤0.001 |
| Height (Median, IQR; cm) | 167 (13) | 167 (13) | 0.727 |
| BMI (Median, IQR; kg/m2) | 22.99 (5.05) | 26.08 (8.46) | ≤0.001 |
| Clinical | |||
| Diabetes Duration (Mean, SD; years) | 17.92 (13) | 19.26 (11.04) | 0.617 2 |
| Type of treatment (N; %) | |||
| MDI | 50 (69.4%) | 22 (71%) | 1.000 1 |
| CSII | 22 (30.6%) | 9 (29%) | |
| Use of CGM (N, %) | |||
| No | 17 (23.6%) | 10 (33.3%) | 0.443 1 |
| Yes | 55 (76.4%) | 20 (66.7%) | |
| Total daily dose (Median, IQR; iu) | 35 (15) | 46 (31) | ≤0.001 |
| Glycemic control | |||
| FBG (Mean, SD; mg/dL) | 108.71 ± 26.86 | 121.85 ± 37.78 | 0.078 2 |
| HbA1c (Median, IQR; %) | 6.5 (1) | 7 (2) | 0.004 |
| BG measurements/day (Median, IQR) | 7.0 (7.5) | 7.0 (20) | 0.295 |
| Hypoglycemic events (Median, IQR) | 5.5 (6.5) | 5 (7.5) | 0.16 |
| TIR (Median, IQR; %) | 75 (21.5) | 62.5 (25) | 0.027 |
| TAR (Median, IQR; %) | 16.5 (23) | 20 (22) | 0.202 |
| TBR (Median, IQR; %) | 6 (8) | 5 (11) | 0.94 |
| OR (95% CI) | p-Value | |
|---|---|---|
| BMI (kg/m2) | 1.33 (1.10–1.60) | 0.003 |
| TIR (%) | 0.96 (0.92–0.99) | 0.022 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Karastogiannidou, C.; Giannoulaki, P.; Samaras, I.; Kotzakioulafi, E.; Didangelos, T.; Bocsan, I.C.; Vassilopoulou, E. The Diabetes Eating Problem Survey-Revised (DEPS-R) in a Greek Adult Population with Type 1 Diabetes Mellitus: Model Comparison Supporting a Single Factor Structure. Nutrients 2021, 13, 2375. https://doi.org/10.3390/nu13072375
Karastogiannidou C, Giannoulaki P, Samaras I, Kotzakioulafi E, Didangelos T, Bocsan IC, Vassilopoulou E. The Diabetes Eating Problem Survey-Revised (DEPS-R) in a Greek Adult Population with Type 1 Diabetes Mellitus: Model Comparison Supporting a Single Factor Structure. Nutrients. 2021; 13(7):2375. https://doi.org/10.3390/nu13072375
Chicago/Turabian StyleKarastogiannidou, Calliope, Parthena Giannoulaki, Ioannis Samaras, Evangelia Kotzakioulafi, Triantafyllos Didangelos, Ioana Corina Bocsan, and Emilia Vassilopoulou. 2021. "The Diabetes Eating Problem Survey-Revised (DEPS-R) in a Greek Adult Population with Type 1 Diabetes Mellitus: Model Comparison Supporting a Single Factor Structure" Nutrients 13, no. 7: 2375. https://doi.org/10.3390/nu13072375
APA StyleKarastogiannidou, C., Giannoulaki, P., Samaras, I., Kotzakioulafi, E., Didangelos, T., Bocsan, I. C., & Vassilopoulou, E. (2021). The Diabetes Eating Problem Survey-Revised (DEPS-R) in a Greek Adult Population with Type 1 Diabetes Mellitus: Model Comparison Supporting a Single Factor Structure. Nutrients, 13(7), 2375. https://doi.org/10.3390/nu13072375









