Insulin Resistance Is Inversely Associated with the Status of Vitamin D in Both Diabetic and Non-Diabetic Populations
Abstract
1. Introduction
2. Materials and Methods
Statistical Analysis and Outcome Measures
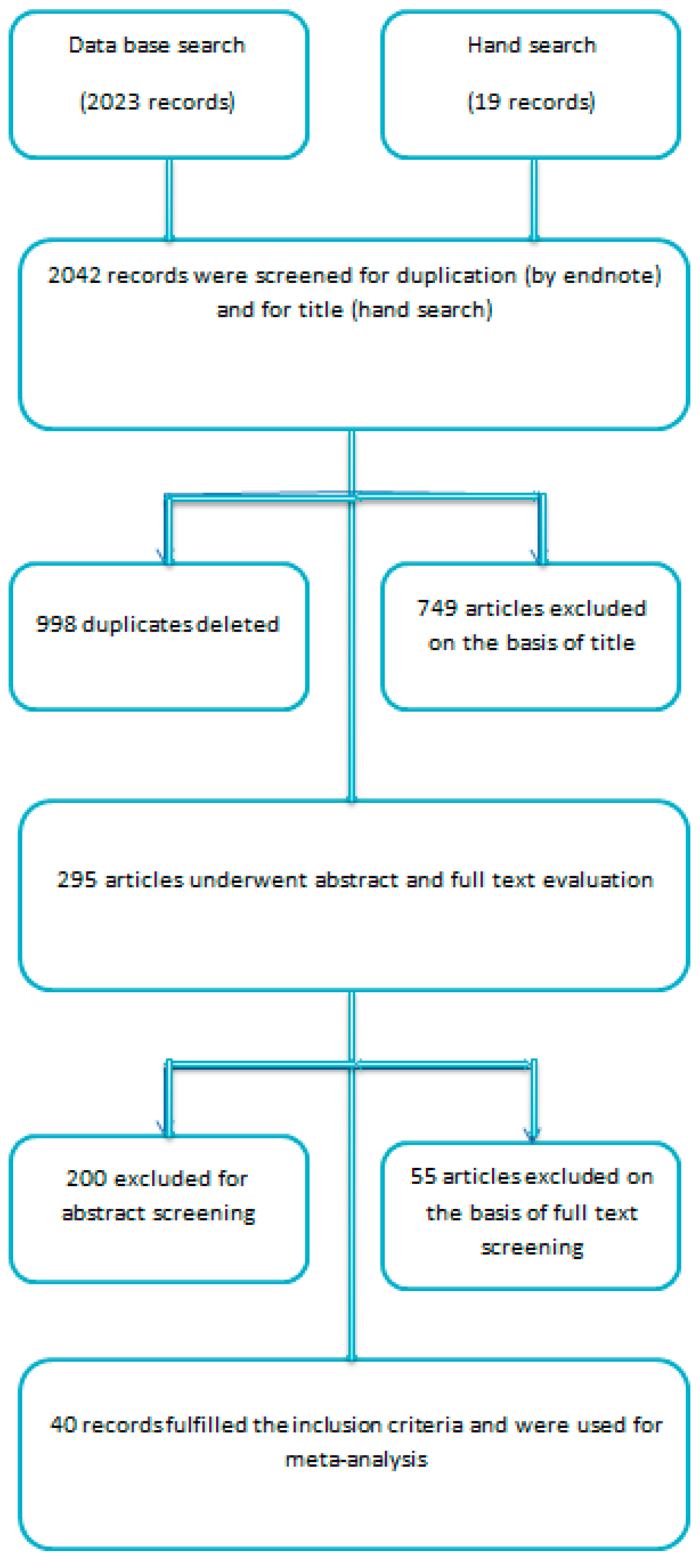
3. Results
3.1. Excluded Studies on the Basis of Full Text Evaluation
3.2. Included Studies
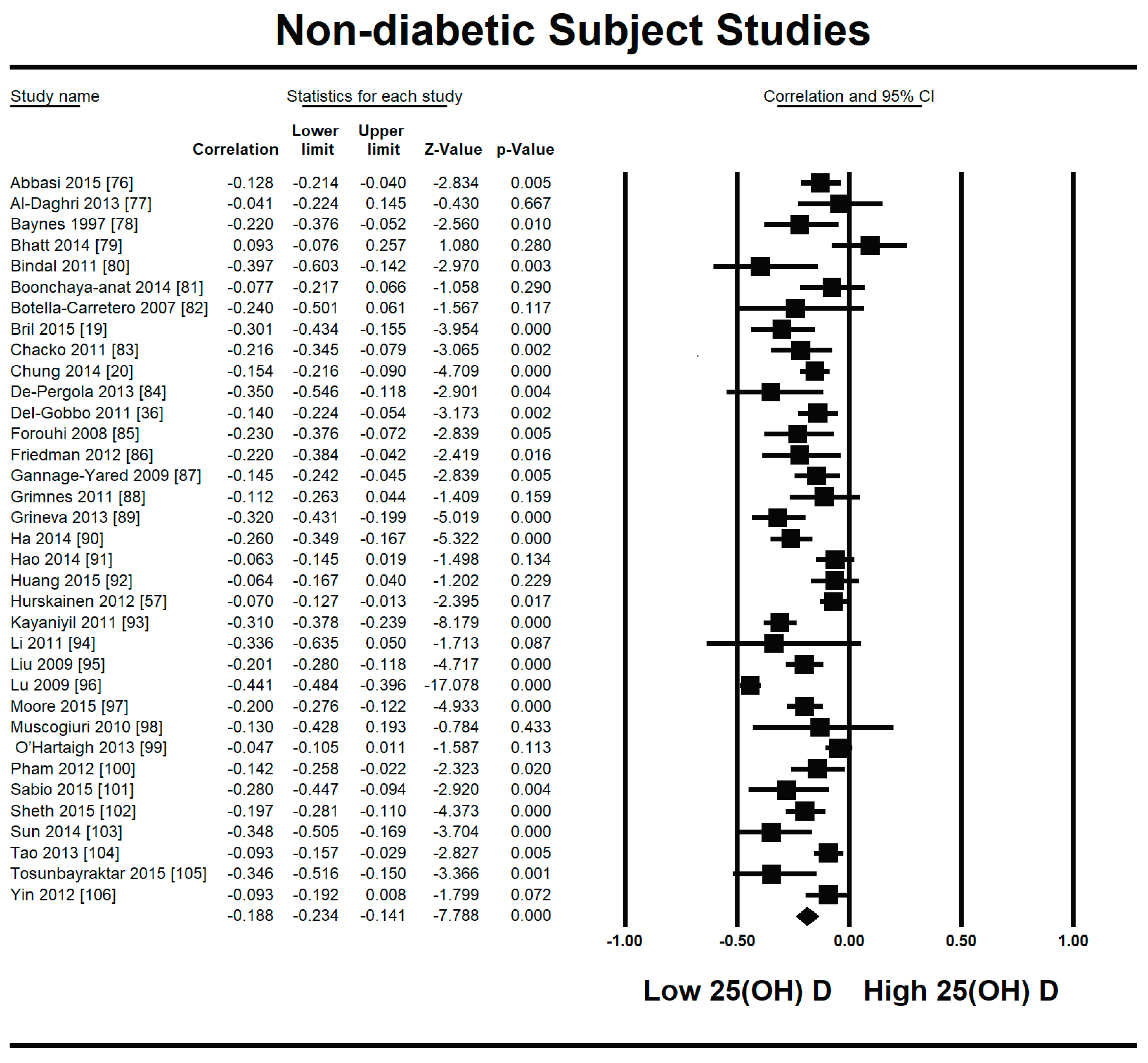
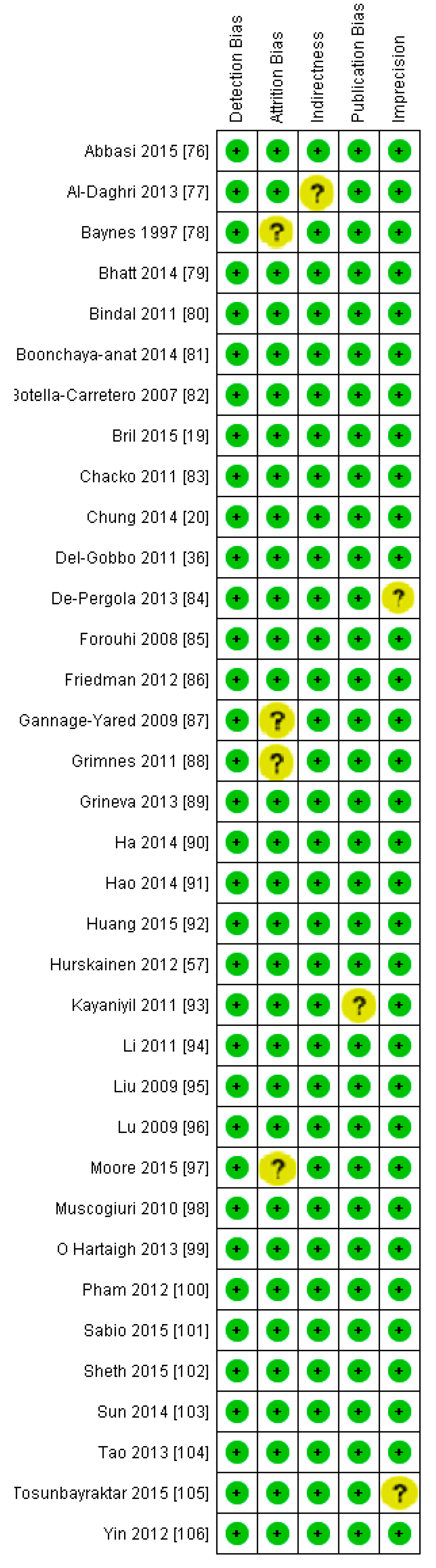
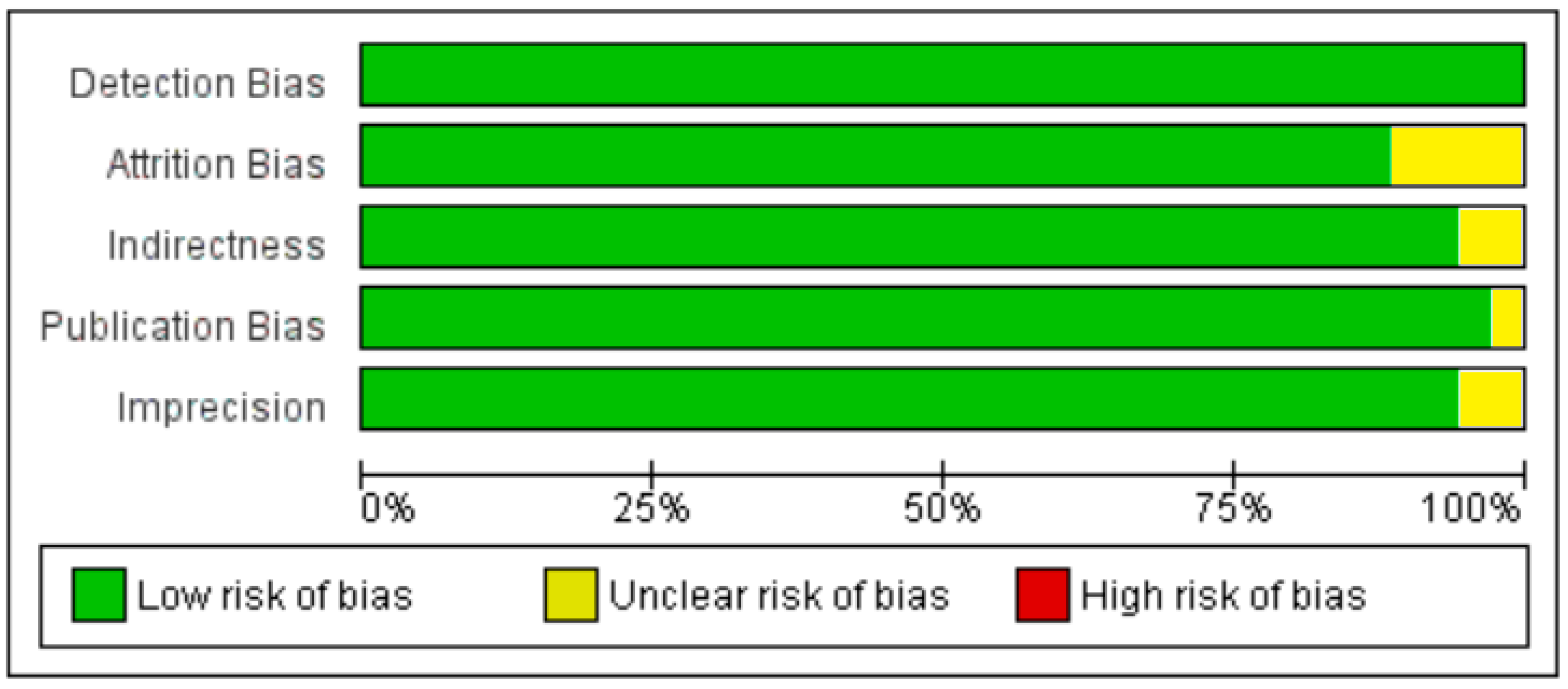
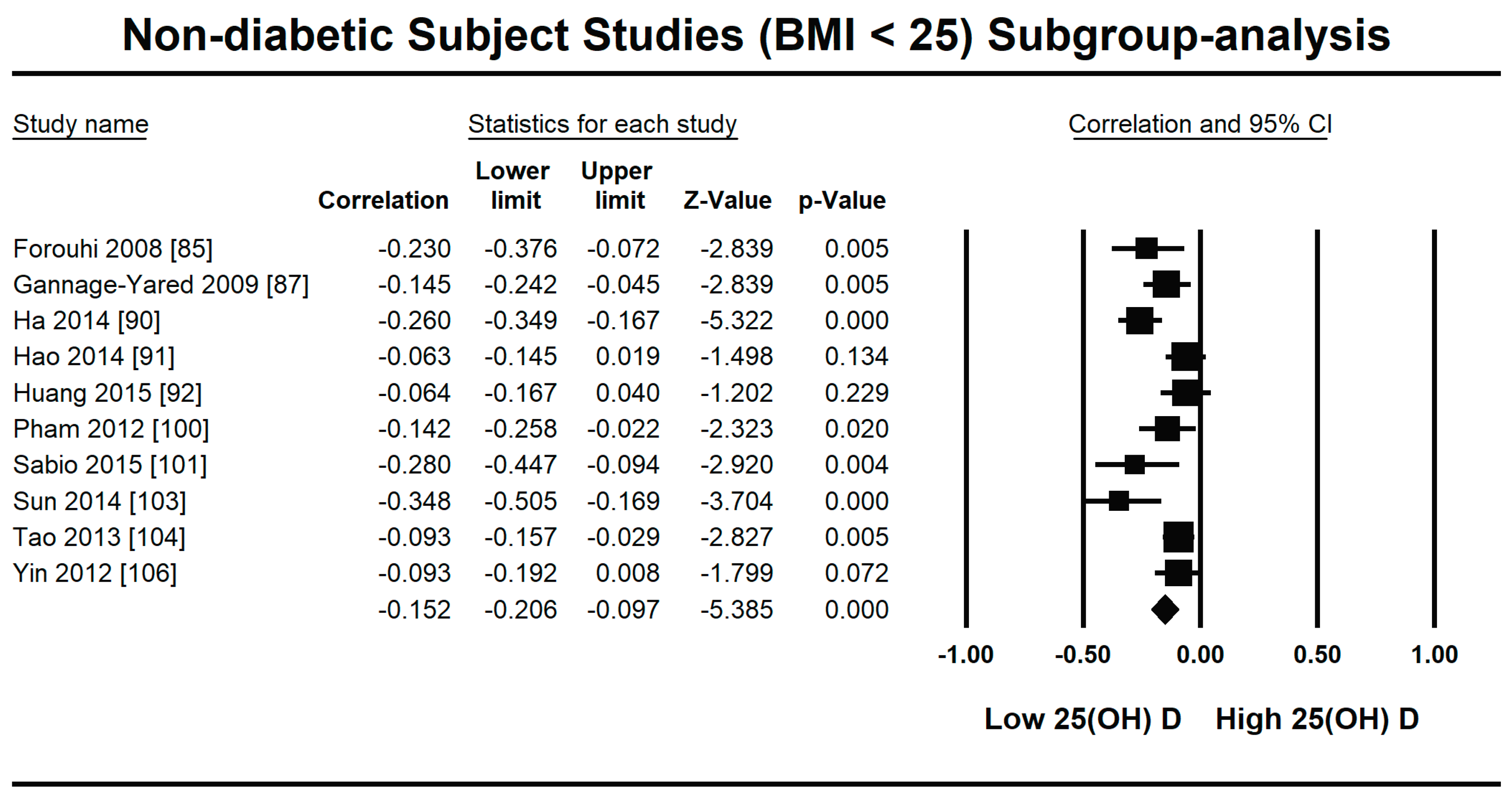
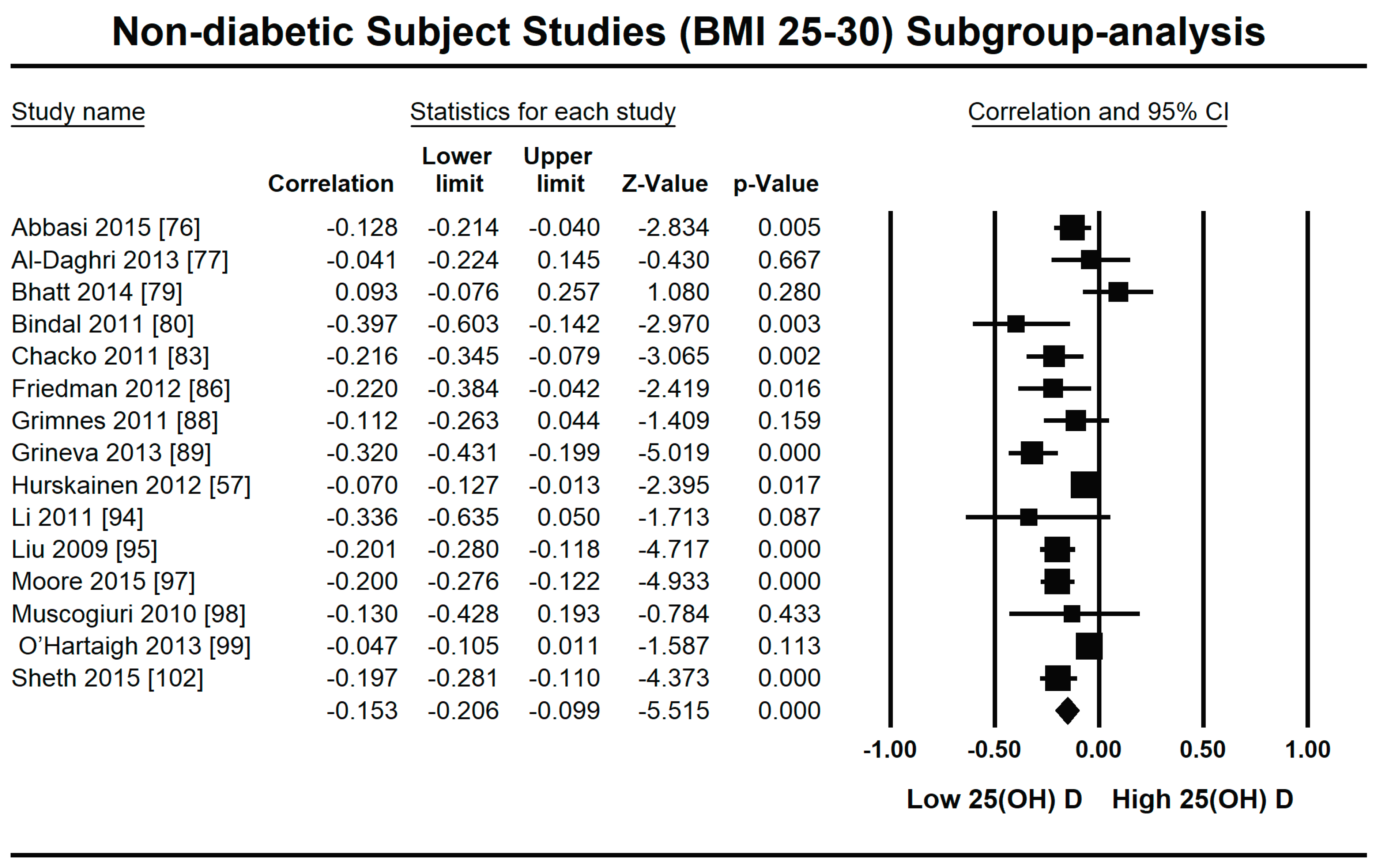
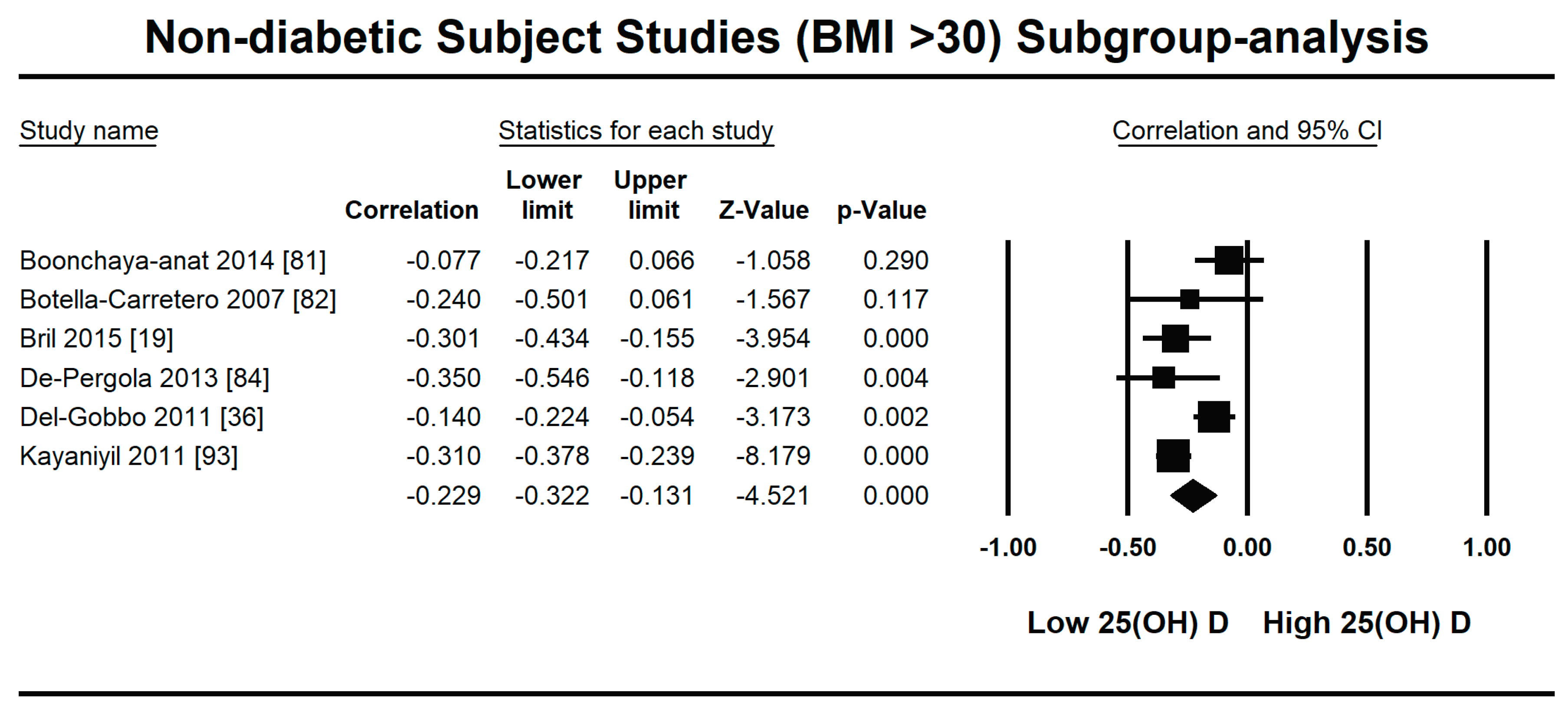
3.2.1. Meta-Analysis and Meta-Regression for Non-Diabetes Patient Studies
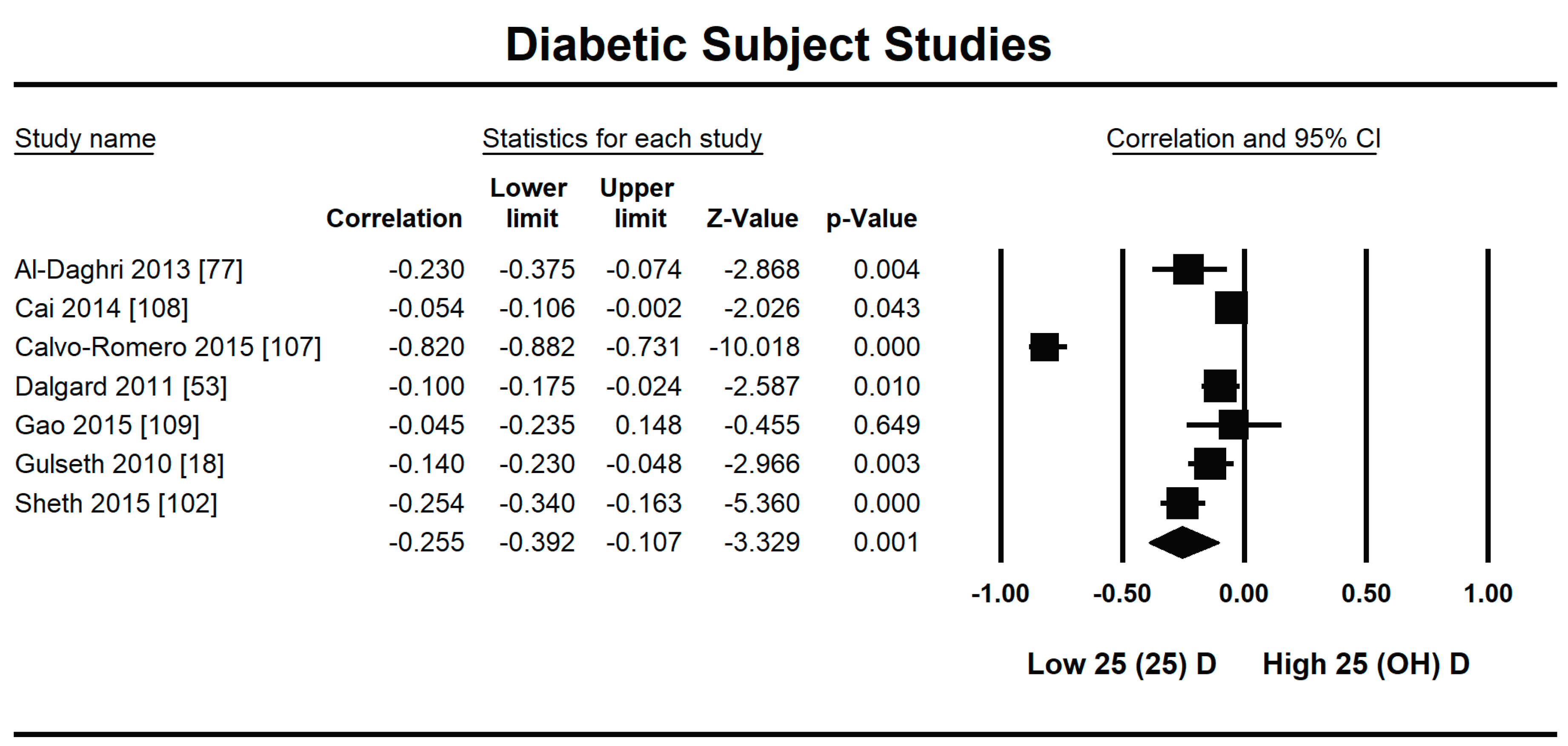
3.2.2. Meta-Analysis and Meta-Regression for Diabetes Patient Studies
4. Discussion
Strengths and Weaknesses
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Kahn, S.E.; Hull, R.L.; Utzschneider, K.M. Mechanisms Linking Obesity to Insulin Resistance and Type 2 Diabetes. Nature 2006, 444, 840–846. [Google Scholar] [CrossRef] [PubMed]
- Ravier, M.A.; Rutter, G.A. Glucose or Insulin, but not Zinc Ions, Inhibit Glucagon Secretion from Mouse Pancreatic Alpha-cells. Diabetes 2006, 54, 1789–1797. [Google Scholar] [CrossRef] [PubMed]
- Williamson, J.R.; Browning, E.T.; Olson, M. Interrelations between Fatty Acid Oxidation and the Control of Gluconeogenesis in Perfused Rat Liver. Adv. Enzym. Regul. 1968, 6, 67–100. [Google Scholar] [CrossRef]
- Dunaif, A. Insulin Resistance and the Polycystic Ovary Syndrome: Mechanism and Implications for Pathogenesis. Endocr. Rev. 1997, 18, 774–800. [Google Scholar]
- Marchesini, G.; Brizi, M.; Morselli-Labate, A.M.; Bianchi, G.; Bugianesi, E.; McCullough, A.J.; Forlani, G.; Melchionda, N. Association of Nonalcoholic Fatty Liver Disease with Insulin Resistance. Am. J. Med. 1999, 107, 450–455. [Google Scholar] [CrossRef]
- Petersen, K.F.; Oral, E.A.; Dufour, S.; Befroy, D.; Ariyan, C.; Yu, C.; Cline, G.W.; DePaoli, A.M.; Taylor, S.I.; Gorden, P.; et al. Leptin Reverses Insulin Resistance and Hepatic Steatosis in Patients with Severe Lipodystrophy. J. Clin. Investig. 2002, 109, 1345–1350. [Google Scholar] [CrossRef] [PubMed]
- Kahn, S.E. The relative contributions of insulin resistance and beta-cell dysfunction to the pathophysiology of Type 2 diabetes. Diabetologia 2003, 46, 3–19. [Google Scholar] [CrossRef] [PubMed]
- Kasuga, M. Insulin Resistance and Pancreatic Beta Cell Failure. J. Clin. Investig. 2006, 116, 1756–1760. [Google Scholar] [CrossRef] [PubMed]
- Schwartz, S.S.; Epstein, S.; Corkey, B.E.; Grant, S.F.A.; Gavin, I.J.R.; Aguilar, R.B.; Herman, M.E. A Unified Pathophysiological Construct of Diabetes and its Complications. Trends Endocrinol. Metab. 2017, 28, 645–655. [Google Scholar] [CrossRef]
- Al Mheid, I.; Patel, R.S.; Tangpricha, V.; Quyyumi, A.A. Vitamin D and Cardiovascular Disease: Is the Evidence Solid? Eur. Heart J. 2013, 34, 3691–3698. [Google Scholar] [CrossRef]
- Tomson, J.; Emberson, J.; Hill, M.; Gordon, A.; Armitage, J.; Shipley, M. Vitamin D and Risk of Death from Vascular and Non-vascular Causes in the Whitehall Study and Meta-analyses of 12,000 Deaths. Eur. Heart J. 2013, 34, 1365–1374. [Google Scholar] [CrossRef]
- Seo, J.A.; Eun, C.R.; Cho, H.; Lee, S.K.; Yoo, H.J.; Kim, S.G. Low Vitamin D Status is Associated with Non-alcoholic Fatty Liver Disease Independent of Visceral Obesity in Korean Adults. PLoS ONE 2013, 8, e75197. [Google Scholar] [CrossRef]
- Dattola, A.; Silvestri, M.; Bennardo, L.; Passante, M.; Scali, E.; Patruno, C.; Nistico, S.P. Role of Vitamins in Skin Health: A Systematic Review. Curr. Nutr. Rep. 2020, 9, 226–235. [Google Scholar] [CrossRef]
- Chiu, K.C.; Chu, A.; Go, V.L.W.; Saad, M.F. Hypovitaminosis D is Associated with Insulin Resistance and Cell Dysfunction. Am. J. Clin. Nutr. 2004, 79, 820–825. [Google Scholar] [CrossRef]
- Pittas, A.G.; Lau, J.; Hu, F.B. Dawson-Hughes, B. The Role of Vitamin D and Calcium in Type 2 Diabetes. A Systematic Review and Meta-Analysis. J. Clin. Endocrinol. Metab. 2007, 92, 2017–2029. [Google Scholar] [CrossRef]
- Kositsawat, J.; Freeman, V.; Gebber, B.; Geraci, S. Association of A1c Levels with Vitamin D Status in U.S. Adults. Diabetes Care 2010, 33, 1236–1238. [Google Scholar] [CrossRef]
- Hypponen, E.; Power, C. Vitamin D Status and Glucose Homeostasis in the 1958 British Bird Cohort: The role of obesity. Diabetes Care 2006, 29, 2244–2246. [Google Scholar] [CrossRef]
- Gulseth, H.L.; Gjelstad, I.M.F.; Tierney, A.C.; Lovengrove, J.A.; Defoort, C.; Blaak, E.E.; Lopez-Miranda, J.; Kiec-Wilk, B.; Ris, U.; Roshe, H.; et al. Serum Vitamin D Concentration Does Not Predict Insulin Action or Secretion in European Subjects with the Metabolic Syndrome. Diabetes Care 2010, 33, 923–925. [Google Scholar] [CrossRef]
- Bril, F.; Maximos, M.; Portillo-Sanchez, P.; Biernacki, D.; Lomonaco, R.; Subbarayan, S.; Correa, M.; Lo, M.; Suman, A.; Cusi, K. Relationship of Vitamin D with Insulin Resistance and Disease Severity in Non-alcoholic Steatohepatitis. J. Hepatol. 2015, 62, 405–411. [Google Scholar] [CrossRef]
- Chung, S.J.; Lee, Y.A.; Hong, H.; Kang, M.J.; Kwon, H.J.; Shin, C.H.; Yang, S.W. Inverse Relationship between Vitamin D Status and Insulin Resistance and the Risk of Impaired Fasting Glucose in Korean Children and Adolescents: The Korean National Health and Nutrition Examination Survey (KNHANES) 2009–2010. Public Health Nutr. 2014, 17, 795–802. [Google Scholar] [CrossRef]
- Alvarez, J.A.; Ashraf, A. Role of Vitamin D in Insulin Secretion and Insulin Sensitivity for Glucose Homeostasis. Int. J. Endocrinol. 2010. [Google Scholar] [CrossRef]
- Dutta, D.; Maisnam, I.; Shrivastava, A.; Sinha, A.; Ghosh, S.; Mukhopadhyay, P.; Mukhopadhyay, S.; Chowdhury, S. Serum Vitamin-D Predicts Insulin Resistance in Individuals with Prediabetes. Indian J. Med. Res. 2013, 138, 853–860. [Google Scholar]
- Kabadi, S.M.; Lee, B.K.; Liu, L. Joint Effects of Obesity and Vitamin D Insufficiency on Insulin Resistance and Type 2 Diabetes: Results from the NHANES 2001–2006. Diabetes Care 2012, 35, 2048–2054. [Google Scholar] [CrossRef]
- Kim, S.; Lim, J.; Kye, S.; Joung, H. Association between Vitamin D Status and Metabolic Syndrome Risk among Korean Population: Based on the Korean National Health and Nutrition Examination Survey IV-2, 2008. Diabetes Res. Clin. Pract. 2012, 96, 230–236. [Google Scholar] [CrossRef]
- Kobzaa, V.M.; Feet, J.C.; Zhoua, J.; Conley, T.B.; Peacock, M.; Reger, H.B.I.; Palmad, G.D.; Campbell, W.W. Vitamin D Status and Resistance Exercise Trainingindependently Affect Glucose Tolerance in Older Adults. Nutr. Res. 2013, 33, 349–357. [Google Scholar] [CrossRef]
- Liu, J.; Tan, J.; Jeynes, B. Serum 25(OH) Vitamin D Level, Femur Length, and Risk of Type 2 Diabetes among Adults. Appl. Physiol. Nutr. Metab. 2013, 6, 264–270. [Google Scholar] [CrossRef]
- Nguyen, V.T.; Li, X.; Elli, E.F.; Ayloo, S.M.; Castellanos, K.J.; Fantuzzi, G.; Freels, S.; Braunschweig, C.L. Vitamin D, Inflammation, and Relations to Insulin Resistance in Premenopausal Women with Morbid Obesity. Obesity 2015, 23, 1591–1597. [Google Scholar] [CrossRef]
- Pannu, P.K.; Piers, L.S.; Soares, M.J.; Zhao, Y.; Ansari, Z. Vitamin D Status is Inversely Associated with Markers of Risk for Type 2 Diabetes: A Population Based Study in Victoria, Australia. PLoS ONE 2017, 12, e0178825. [Google Scholar] [CrossRef] [PubMed]
- Scragg, R.; Sowers, M.R.; Bell, C. Serum 25-Hydroxyvitamin D, Diabetes, and Ethnicity in the Third National Health and Nutrition Examination Survey. Diabetes Care 2004, 27, 2813–2818. [Google Scholar] [CrossRef]
- Weiler, H.A.; Lowea, J.; Krahnb, J.; William, D. LesliecOsteocalcin and Vitamin D Status are Inversely Associated with Homeostatic Model Assessment of Insulin Resistance in Canadian Aboriginal and White Women: The First Nations Bone Health Study. J. Nutr. Biochem. 2013, 24, 412–418. [Google Scholar] [CrossRef] [PubMed]
- Alkharfy, K.M.; Al-Daghri, N.M.; Sabico, S.B.; Al-Othman, A.; Moharram, O.; Alokail, M.S.; Al-Saleh, Y.; Kumar, S.; Chrousos, G.P. Vitamin D Supplementation in Patients with Diabetes Mellitus Type 2 on Different Therapeutic Regimens: A One-year Prospective Study. Cardiovasc. Diabetol. 2013, 12, 113. [Google Scholar] [CrossRef]
- Al-Shoumer, K.A.; Al-Asoosi, A.A.; Ali, A.H.; Nair, V.S. Does Insulin Resistance in Type 2 Diabetes Alter Vitamin D Status? Prim. Care Diabetes 2013, 7, 283–287. [Google Scholar] [CrossRef] [PubMed]
- Gedik, O.; Akalin, S. Effects of Vitamin D Deficiency and Repletion on Insulin and Glucagon Secretion in Man. Diabetologia 1986, 29, 142–145. [Google Scholar] [CrossRef] [PubMed]
- Bardini, G.; Giannini, S.; Romano, D.; Rotella, C.M.; Mannucci, E. Lipid Accumulation Product and 25-OH-Vitamin D Deficiency in Type 2 Diabetes. Rev. Diabet. Stud. 2013, 10, 243–251. [Google Scholar] [CrossRef]
- Nimitphong, H.; Chailurkit, L.; Chanprasertyothin, S.; Sritara, P.; Ongphiphadhanakul, B. The Association of Vitamin D Status and Fasting Glucose According to Body Fat Mass in Young Healthy Thais. Endocr. Disord. 2013, 13, 60. [Google Scholar] [CrossRef]
- Del-Gobbo, L.C.; Song, Y.; Dannenbaum, D.A.; Dewailly, E.; Egeland, G.M. Serum 25-Hydroxyvitamin D Is not Associated with Insulin Resistance or Beta Cell Function in Canadian Cree. J. Nutr. 2011, 141, 290–295. [Google Scholar] [CrossRef]
- Diaz, G.M.; Gonza, L.; Ramos-Trautmann, G.; Marie, C.; Palacios, C. Vitamin D Status Is Associated with Metabolic Syndrome in a Clinic-Based Sample of Hispanic Adults. Metab. Syndr. Relat. Disord. 2016, 14, 259–264. [Google Scholar] [CrossRef]
- Hidayat, R.; Setiati, S.; Soewondo, P. The Association Between Vitamin D Deficiency and Type 2 Diabetes Mellitus in Elderly Patients. Age 2010, 42, 123–129. [Google Scholar]
- Hirani, V.; Cumming, R.G.; Le Couteur, D.G.; Naganathan, V.; Blyth, F.; Handelsman, D.J.; Waite, L.M.; Seibel, M.J. Low Levels of 25-Hydroxy Vitamin D and Active 1,25-Dihydroxyvitamin D Independently Associated with Type 2 Diabetes Mellitus in Older Australian Men: The Concord Health and Ageing in Men Project. J. Am. Geriatr. Soc. 2014, 62, 1741–1747. [Google Scholar] [CrossRef]
- Husemoen, L.L.; Thuesen, B.H.; Fenger, M.; Jorgensen, T.; Glumer, C.; Svensson, J.; Ovesen, L.; Witte, D.R.; Linneberg, A. Serum 25(OH)D and Type 2 Diabetes Association in a General Population: A Prospective Study. Diabetes Care 2012, 35, 1695–1700. [Google Scholar] [CrossRef]
- Justice, J.N.; Pierpoint, L.A.; Mani, D.; Schwartz, R.S.; Enoka, R.M. Motor Function is Associated with 1,25(OH)2D and Indices of Insulin–glucose Dynamics in Non-diabetic Older Adults. Aging Clin. Exp. Res. 2014, 26, 249–254. [Google Scholar] [CrossRef] [PubMed]
- Kabadi, S.M.; Liu, L.; Auchincloss, A.H.; Zakeri, I.F. Multivariate Path Analysis of Serum 25-hydroxyvitamin D Concentration, Inflammation, and Risk of Type 2 Diabetes Mellitus. Dis. Mark. 2013, 35, 187–193. [Google Scholar] [CrossRef] [PubMed]
- Khor, G.L.; Chee, W.S.S.; Shariff, Z.M.; Poh, B.K.; Arumugam, M.; Rahman, J.A.; Theobaldb, H.E. High Prevalence of Vitamin D Insufficiency and Its Association with BMI-for-age among Primary School Children in Kuala Lumpur, Malaysia. BMC Public Health 2011, 1, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Lee, B.; Park, S.; Kim, Y. Age- and Gender-specific Associations between Low Serum 25-hydroxyvitamin D Level and Type 2 Diabetes in the Korean General Population: Analysis of 2008–2009 Korean National Health and Nutrition Examination Survey data. Asia Pac. J. Clin. Nutr. 2012, 21, 536–546. [Google Scholar]
- Li, L.; Yin, X.; Yao, C.; Zhu, X.; Wu, X. Serum 25-hydroxyvitamin D, Parathyroid Hormone, and Their Association with Metabolic Syndrome in Chinese. Endocrine 2013, 44, 465–472. [Google Scholar] [CrossRef]
- Lu, L.; Wu, Y.; Qi, Q.; Liu, C.; Gan, W. Associations of Type 2 Diabetes with Common Variants in PPARD and the Modifying Effect of Vitamin D among Middle-Aged and Elderly Chinese. PLoS ONE 2012, 7, e34895. [Google Scholar] [CrossRef]
- Marques-Vidal, P.; Vollenweider, P.; Guessous, I.; Henry, H.; Boulat, O.; Waeber, G.; Jornayvaz, F.R. Serum Vitamin D Concentrations Are Not Associated with Insulin Resistance in Swiss Adults. J. Nutr. 2015, 145, 2117–2122. [Google Scholar] [CrossRef]
- Tsur, A.; Feldman, B.S.; Feldhammer, I.; Hoshen, M.B.; Leibowitz, G.; Balicer, R.D. Decreased Serum Concentrations of 25-hydroxycholecalciferol are Associated with Increased Risk of Progression to Impaired Fasting Glucose and Diabetes. Diabetes Care 2013, 36, 1361–1367. [Google Scholar] [CrossRef]
- Wright, O.R.L.; Hickman, I.J.; Petchey, W.G.; Sullivan, C.M.; Ong, C.; Rose, F.J.; Ng, C.; Prins, J.B.; Whitehead, J.P.; Moore-Sullivan, T.M. The Effect of 25-hydroxyvitamin D on Insulin Sensitivity in Obesity: Is It Mediated via Adiponectin? Can. J. Physiol. Pharmacol. 2013, 91, 496–501. [Google Scholar] [CrossRef]
- Wright, C.S.; Weinheimer-Haus, E.M.; Fleet, J.C.; Peacock, M.; Campbell, W.W. The Apparent Relation between Plasma 25-Hydroxyvitamin D and Insulin Resistance Is Largely Attributable to Central Adiposity in Overweight and Obese Adults. J. Nutr. 2015, 145, 2683–2689. [Google Scholar] [CrossRef]
- Zoppini, G.; Galletti, A.; Targher, G.; Brangani, C.; Pichiri, I.; Negri, C.; Stoico, V.; Cacciatori, V.; Bonora, E. Glycated Haemoglobin Is Inversely Related to Serum Vitamin D Levels in Type 2 Diabetic Patients. PLoS ONE 2013, 8, e82733. [Google Scholar] [CrossRef]
- Bellan, M.; Guzzaloni, G.; Rinaldi, M.; Merlotti, E.; Ferrari, C.; Tagliaferri, A.; Pirisi, M.; Aimaretti, G.; Scacchi, M.; Marzullo, P. Altered Glucose Metabolism Rather Than Naïve Type 2 Diabetes Mellitus (T2DM) is Related to Vitamin D Status in Severe Obesity. Cardiovasc. Diabetol. 2014, 13, 57. [Google Scholar] [CrossRef]
- Dalgard, C.; Skaalum, M.; Weihe, P.P.; Grandjean, P. Vitamin D Status in Relation to Glucose Metabolism and Type 2 Diabetes in Septuagenarians. Diabetes Care 2011, 34, 1284–1288. [Google Scholar] [CrossRef]
- Heras, J.D.L.; Rajkumar, K.; Lee, S.; Bacha, F.; Holick, M.F.; Arslanian, S.A. 25-Hydroxyvitamin D in Obese Youth Across theSpectrumofGlucose Tolerance from Normal to Prediabetes to Type 2 Diabetes. Diabetes Care 2013, 36, 2048–2053. [Google Scholar] [CrossRef]
- Esteghamatia, A.; Aryanab, B.; Esteghamatia, A.; Nakhjavania, M. Differences in Vitamin D Concentration between Metabolically Healthy Andunhealthy Obese Adults: Associations with Inflammatory and Cardiometabolicmarkers in 4391 Subjects. Diabetes Metab. 2014, 40, 347–355. [Google Scholar] [CrossRef]
- Huang, Y.; Li, X.; Wang, M.; Ning, H.; Lima, A.; Li, Y.; Sun, C. Lipoprotein lipase links vitamin D, insulin resistance, and type 2 diabetes: A cross-sectional epidemiological study. Cardiovasc. Diabetol. 2013, 12, 17. [Google Scholar] [CrossRef]
- Hurskainen, A.R.; Virtanen, J.K.; Tuomainen, T.P.; Nurmi, T.; Voutilainen, S. Association of Serum 25-hydroxyvitamin D with Type 2 Diabetes and Markers of Insulin Resistance in a General Older Population in Finland. Diabetes Metab. Res. Rev. 2012, 28, 418–423. [Google Scholar] [CrossRef]
- Jiang, H.; Peng, S. The Relationship between Serum Vitamin D and HOMA-IR in Overweight Elderly Patients. Int. J. Cardiol. 2014, 177, 1100–1102. [Google Scholar] [CrossRef]
- Park, H.Y.; Lim, Y.; Kim, J.H.; Bae, S.; Oh, S.; Hong, Y. Association of Serum 25-Hydroxyvitamin D Levels with Markers for Metabolic Syndrome in the Elderly: A Repeated Measure Analysis. J. Korean Med. Sci. 2012, 27, 653–660. [Google Scholar] [CrossRef]
- Kavadar, G.; Demircioglu, D.T.; Ozgonenel, L.; Emre, T.Y. The Relationship between Vitamin D Status, Physical Activity and Insulin Resistance in Overweight and Obese Subjects. Bosn. J. Basic Med. Sci. 2015, 15, 62–66. [Google Scholar] [CrossRef]
- Kim, J. Association between Serum Vitamin D, Parathyroid Hormone and Metabolic Syndrome in Middle-aged and Older Korean Adults. Eur. J. Clin. Nutr. 2015, 69, 425–430. [Google Scholar] [CrossRef] [PubMed]
- Kim, M.K.; Kang, M.I.; Oh, K.W.; Kwon, H.S.; Lee, J.H.; Lee, W.C.; Yoon, K.; Ho, Y. The Association of Serum Vitamin D Level with Presence of Metabolic Syndrome and Hypertension in Middle-aged Korean Subjects. Clin. Endocrinol. 2010, 73, 330–338. [Google Scholar] [CrossRef] [PubMed]
- Lim, S.; Kim, M.J.; Choi, S.H.; Shin, C.S.; Park, K.S.; Jang, H.C.; Billings, L.K.; Meigs, J.B. Association of Vitamin D Deficiency with Incidence of Type 2 Diabetes in High-risk Asian Subjects. Am. J. Clin. Nutr. 2013, 97, 524–530. [Google Scholar] [CrossRef] [PubMed]
- Morisset, A.; Tardio, V.; Weisnagel, J.; Lemieux, S.; Bergeron, J.; Gagnon, C. Associations Between Serum 25-Hydroxyvitamin D, Insulin Sensitivity, Insulin Secretion, and B-Cell Function According to Glucose Tolerance Status. Metab. Syndr. Relat. Disord. 2015, 13, 208–214. [Google Scholar] [CrossRef]
- Nielsen, N.O.; Bjerregaard, P.; Rønn, P.F.; Friis, H.; Andersen, S.; Melbye, M. Associations between Vitamin D Status and Type 2 Diabetes Measures among Inuit in Greenland May Be Affected by Other Factors. PLoS ONE 2016, 11. [Google Scholar] [CrossRef]
- Pinelli, N.R.; Jaber, L.A.; Brown, M.B.; Herman, W.H. 3Serum 25-Hydroxy Vitamin D and Insulin Resistance, Metabolic Syndrome, and Glucose Intolerance Among Arab Americans. Diabetes Care 2010, 33, 373–1375. [Google Scholar] [CrossRef]
- Rhee, S.Y.; Hwang, Y.C.; Chung, H.Y.; Woo, J.T. Vitamin D and Diabetes in Koreans: Analyses Based on the Fourth Korea National Health and Nutrition Examination Survey (KNHANES), 2008–2009. Diabetic Med. 2012, 1003–1010. [Google Scholar] [CrossRef]
- Esteghamati, A.; Aryan, Z.; Esteghamati, A.R.; Nakhjavani, M. Vitamin D Deficiency is Associated with Insulin Resistance in Nondiabetics and Reduced Insulin Production in Type 2 Diabetics. Horm. Metab. Res. 2015, 47, 273–279. [Google Scholar] [CrossRef]
- Al-Daghri, N.M.; Al-Attas, O.S.; Al-Okail, M.S.; Alkharfy, K.M.; Al-Yousef, M.A.; Nadhrah, H.M.; Sabico, S.B.; Chrousos, G.P. Severe Hypovitaminosis D is Widespread and more Common in Non-diabetics Than Diabetics in Saudi Adults. Saudi Med. J. 2010, 31, 775–780. [Google Scholar]
- Eraslan, S.; Kizilgul, M.; Uzunlulu, M.; Colak, Y.; Ozturk, O.; Tuncer, I. Frequency of Metabolic Syndrome and 25-hydroxyvitamin D3 Levels in Patients with Non-alcoholic Fatty Liver Disease. Minerva Med. 2013, 104, 447–453. [Google Scholar]
- Hutchinson, M.S.; Figenschau, Y.; Almås, B.; Njølstad, I.; Jorde, R. Serum 25-hydroxyvitamin D Levels in Subjects with Reduced Glucose Tolerance and Type 2 Diabetes–The Tromsø OGTT-study. Int. J Vitam. Nutr. Res. 2011, 81, 317–327. [Google Scholar] [CrossRef]
- Imura, H.; Seino, Y.; Ishida, H. Osteopenia and Circulating Levels of Vitamin D Metabolites in Diabetes Mellitus. J. Nutr. Sci. Vitaminol. 1985, 31, 27–32. [Google Scholar] [CrossRef]
- Nomata, S.; Kadowaki, S.; Yamatani, T.; Fukase, M.; Fujita, T. Effect of 1 Alpha (OH)-vitamin D3 on Insulin Secretion in Diabetes Mellitus. Bone Miner. 1986, 1, 187–192. [Google Scholar]
- Mhatre, M.; Hall, M. Student Forum: Does Calcium and Vitamin D Intake Affect Incidence of Type 2 Diabetes Mellitus and Insulin Resistance Syndrome? Consult. Pharm. 2010, 25, 379–381. [Google Scholar] [CrossRef]
- Mirzaei, K.; Hossein-Nezhad, A.; Keshavarz, S.A.; Eshaghi, S.M.; Koohdani, F.; Saboor-Yaraghi, A.A.; Hosseini, S.; Tootee, A.; Djalali, M. Insulin Resistance via Modification of PGC1α Function Identifying a Possible Preventive Role of Vitamin D Analogues in Chronic Inflammatory State of Obesity. A Double Blind Clinical Trial Study. Minerva Med. 2014, 105, 63–78. [Google Scholar]
- Abbasi, F.; Blasey, C.; Feldman, D.; Caulfield, M.P.; Hantash, F.M.; Reaven, G.M. Low Circulating 25-Hydroxyvitamin D Concentrations Are Associated with Defects in Insulin Action and Insulin Secretion in Persons with Prediabetes. J. Nutr. 2015, 145, 714–719. [Google Scholar] [CrossRef]
- Al-Daghri, N.M.; Al-Attas, O.S.; Alokail, M.S.; Alkharfy, K.M.; Al-Othman, A.; Draz, H.M.; Yakout, S.M.; Al-Saleh, Y.; Al-Yousef, M.; Sabico, S. Hypovitaminosis D Associations with Adverse Metabolic Parameters are Accentuated in Patients with Type 2 Diabetes Mellitus: A Body Mass Index-independent Role of Adiponectin? J. Endocrinol. Investig. 2013, 36, 1–6. [Google Scholar]
- Baynes, K.C.R.; Boucher, B.J.; Feskens, E.J.M.; Kromhout, D. Vitamin D Glucose Tolerance and Insulinaemia in Elderly Men. Diabetologia 1997, 40, 344–347. [Google Scholar] [CrossRef]
- Bhatt, S.P.; Misra, A.; Sharma, M.; Guleria, R.; Pandey, R.M.; Luthra, K.; Vikram, N.K. Vitamin D Insufficiency is Associated with Abdominal Obesity in Urban Asian Indians without Diabetes in North India. Diabetes Technol. Ther. 2014, 16, 392–396. [Google Scholar] [CrossRef]
- Bindal, M.E.; Taskapan, H. Hypovitaminosis D and Insulin Resistance in Peritoneal Dialysis Patients. Int. Urol. Nephrol. 2011, 43, 527–534. [Google Scholar] [CrossRef]
- Boonchaya-anant, P.; Holick, F.M.; Caroline, M. ApovianSerum 25-Hydroxyvitamin D Levels and Metabolic Health Status in Extremely Obese Individuals. Obesity 2014, 22, 2539–2543. [Google Scholar] [PubMed]
- Botella-Carretero, J.I.; Alvarez-Blasco, F.; Villafruela, J.J.; Balsa, J.A.; Vazquez, C.; Escobar-Morreale, H.F. Vitamin D Deficiency is Associated with the Metabolic Syndrome in Morbid Obesity. Clin. Nutr. 2007, 26, 573–580. [Google Scholar] [CrossRef]
- Chacko, S.A.; Song, Y.; Manson, J.E.; Horn, L.V.; Eaton, C.; Martin, L.W.; McTiernan, A.; Curb, J.D.; Wylie-Rosett, J.; Phillips, L.S. Serum 25-hydroxyvitamin D Concentrations in Relation to Cardiometabolic Risk Factors and Metabolic Syndrome in Postmenopausal Women. Am. J. Clin. Nutr. 2011, 94, 209–217. [Google Scholar] [CrossRef] [PubMed]
- De-Pergola, G.; Nitti, A.; Bartolomeo, N.; Gesuita, A.; Giagulli, V.A.; Triggiani, V.; Guastamacchia, E.; Silvestris, F. Possible Role of Hyperinsulinemia and Insulin Resistance in Lower Vitamin D Levels in Overweight and Obese Patients. BioMed Res. Int. 2013. [Google Scholar] [CrossRef] [PubMed]
- Forouhi, N.G.; Luan, J.; Cooper, A.; Boucher, B.J.; Wareham, N.J. Baseline Serum 25-hydroxy Vitamin D is Predictive of Future Glycemic Status and Insulin Resistance. Diabetes 2008, 57, 2619–2625. [Google Scholar] [CrossRef] [PubMed]
- Friedman, D.J.; Bhatt, N.; Hayman, N.S.; Nichols, B.J.; Herman, M.; Nikolaev, N.; Danziger, J. Impact of Activated Vitamin D on Insulin Resistance in Nondiabetic Chronic Kidney Disease Patients. Clin. Endocrinol. 2012, 77, 56–61. [Google Scholar] [CrossRef] [PubMed]
- Gannage-Yared, M.L.; Chedid, R.; Khalife, S.; Azzi, E.; Zoghbi, F.; Halaby, G. Vitamin D in Relation to Etabolic Risk Factors, Insulin Sensitivity and Adiponectin in a Young Middle-Eastern Population. Eur. J. Endocrinol. 2009, 160, 965–971. [Google Scholar] [CrossRef] [PubMed]
- Grimnes, G.; Figenschau, Y.; Almås, B.; Jorde, R. Vitamin D, Insulin Secretion, Sensitivity, and Lipids Results from a Case-Control Study and a Randomized Controlled Trial Using Hyperglycemic Clamp Technique. Diabetes 2011, 60, 2748–2757. [Google Scholar] [CrossRef]
- Grineva, E.N.; Karonova, T.; Micheeva, E.; Belyaeva, O.; Nikitina, I.L. Vitamin D Deficiency is a Risk Factor for Obesity and Diabetes Type 2 in Women at Late Reproductive Age. Aging 2013, 5, 575–581. [Google Scholar]
- Ha, C.; Han, T.; Lee, S.; Cho, J.; Kang, H. Association between Serum Vitamin D Status and Metabolic Syndrome in Korean Young Men. Epidemiology 2014, 46, 513–519. [Google Scholar] [CrossRef]
- Hao, Y.; Ma, X.; Shen, Y.; Ni, J.; Luo, Y.; Xiao, Y.; Bao, Y.; Jia, W. Associations of Serum 25-Hydroxyvitamin D3 Levels with Visceral Adipose Tissue in Chinese Men with Normal Glucose Tolerance. PLoS ONE 2014, 9, e86773. [Google Scholar] [CrossRef]
- Huang, C.; Chang, H.; Lu, C.; Tseng, F.; Lee, L.; Huang, K. Vitamin D Status and Risk of Metabolic Syndrome among Non-diabetic Young Adults. Clin. Nutr. 2015, 34, 484–489. [Google Scholar] [CrossRef]
- Kayaniyil, S.; Vieth, R.; Harris, S.B.; Retnakaran, R.; Knight, J.A.; Gerstein, H.C.; Perkins, B.A.; Zinman, B.; Hanley, A.J. Association of 25(OH)D and PTH with Metabolic Syndrome and Its Traditional and Nontraditional Components. J. Clin. Endocrinol. Metab. 2011, 96, 168–175. [Google Scholar] [CrossRef]
- Li, H.W.R.; Brereton, R.E.; Anderson, R.A.; Wallace, A.M.; Ho, C.K.M. Vitamin D Deficiency is Common and Associated with Metabolic Risk Factors in Patients with Polycystic Ovary Syndrome. Metab. Clin. Exp. 2011, 60, 1475–1481. [Google Scholar] [CrossRef]
- Liu, E.; Meigs, J.B.; Pittas, A.G.; McKeown, N.M.; Economos, C.D.; Booth, S.L.; Jacques, P.F. Plasma 25-Hydroxyvitamin D Is Associated with Markers of the Insulin Resistant Phenotype in Nondiabetic Adults. J. Nutr. 2009, 139, 329–334. [Google Scholar] [CrossRef]
- Lu, L.; Yu, Z.; Pan, A.; Hu, F.B.; Franco, O.H.; Li, H.; Li, X.; Yang, X.; Chen, Y.; Lin, X. Plasma 25-hydroxyvitamin D Concentration and Metabolic Syndrome among Middle-aged and Elderly Chinese Individuals. Diabetes Care 2009, 32, 1278–1283. [Google Scholar] [CrossRef]
- Moore, A.; Hochner, H.; Sitlani, C.M.; Williams, M.A.; Hoofnagle, A.N.; de Boer, I.H.; Kestenbaum, B.; Siscovic, D.S.; Friedlander, Y.; Enquobahrie, D.A. Plasma Vitamin D is Associated with Fasting Insulin and Homeostatic Model Assessment of Insulin Resistance in Young Adult Males, but Not Females, of the Jerusalem Perinatal Study. Public Health Nutr. 2015, 18, 1324–1331. [Google Scholar] [CrossRef]
- Muscogiuri, G.; Sorice, G.P.; Prioletta, A.; Policola, C.; Casa, S.D.; Pontecorvi, A.; Giaccari, A. 25-Hydroxyvitamin D Concentration Correlates with Insulin-Sensitivity and BMI in Obesity. Obesity 2010, 18, 1906–1910. [Google Scholar] [CrossRef]
- O’Hartaigh, B.; Thomas, G.N.; Silbernagel, G.N.; Bosch, J.A.; Pilz, S.; Loerbroks, A.; Kleber, M.E.; Grammer, T.B.; Bohm, B.O.; Marz, W. Association of 25-hydroxyvitamin D with Type 2 Diabetes among Patients Undergoing Coronary Angiography: Cross-sectional Findings from the LUdwigshafen Risk and Cardiovascular Health (LURIC) Study. Clin. Endocrinol. 2013, 79, 192–198. [Google Scholar] [CrossRef]
- Pham, N.M.; Akter, S.; Kurotani, K.; Nanri, A.; Sato, M.; Hayabuchi, H.; Yasuda, K.; Mizoue, T. Serum 25-hydroxyvitamin D and Markers of Insulin Resistance in a Japanese Working Population. Eur. J. Clin. Nutr. 2012, 66, 1323–1328. [Google Scholar] [CrossRef]
- Sabio, J.M.; Vargas-Hitos, J.A.; Martinez-Bordonado, J.; Navarrete-Navarrete, N.; Diaz-Chamorro, A.; Olvera-Porcel, C.; Zamora, M.; Jiménez-Alonso, J. Association between Low 25-hydroxyvitamin D, Insulin Resistance and Arterial Stiffness in Nondiabetic Women with Systemic Lupus Erythematosus. Lupus 2015, 24, 155–163. [Google Scholar] [CrossRef]
- Sheth, J.J.; Shah, A.; Sheth, F.J.; Trivedi, S.; Lele, M.; Shah, N.; Thakor, P.; Vaidya, R. Does Vitamin D Play a Significant Role in Type 2 Diabetes? BMC Endocr. Disord. 2015, 15, 5. [Google Scholar] [CrossRef]
- Sun, X.; Cao, Z.; Tanisawa, K.; Ito, T.; Oshima, S.; Higuchi, M. The Relationship between Serum 25-Hydroxyvitamin D Concentration, Cardiorespiratory Fitness, and Insulin Resistance in Japanese Men. Nutrients 2014, 7, 91–102. [Google Scholar] [CrossRef]
- Tao, M.; Zhang, Z.; Yao-hua, K.E.; Jin-wei, H.E.; Wen-zhen, F.U.; Chang-qing, Z.; Zhen-lin, Z. Association of Serum 25-hydroxyvitamin D with Insulin Resistance and β-cell Function in a Healthy Chinese Female Population. Acta Pharmacol. Sin. 2013, 34, 1070–1074. [Google Scholar] [CrossRef]
- Tosunbayraktar, G.; Bas, M.; Kut, A.; Buyukkaragoz, A.H. Low Serum 25(OH)D Levels are Assocıated to Higher BMI and Metabolic Syndrome Parameters in Adults Subjects in Turkey. Afr. Health Sci. 2015, 15, 1161–1169. [Google Scholar] [CrossRef]
- Yin, X.; Sun, Q.; Zhang, X.; Lu, Y.; Sun, C.; Cui, Y.; Wang, S. Serum 25(OH)D is Inversely Associated with Metabolic Syndrome Risk Profile among Urban Middle-aged Chinese Population. Nutr. J. 2012, 11, 68. [Google Scholar] [CrossRef]
- Calvo-Romero, J.M.; Ramiro-Lozano, J.M. Vitamin D Levels in Patients with Type 2 Diabetes Mellitus. J. Investig. Med. 2015, 63, 921–923. [Google Scholar] [CrossRef]
- Cai, X.; Hu, Z.; Chen, L.; Han, X.; Ji, L. Analysis of the Associations between Vitamin D and Albuminuria or Beta-Cell Function in Chinese Type 2 Diabetes. BioMed Res. 2014. [Google Scholar] [CrossRef]
- Gao, Y.; Wu, X.; Fu, Q.; Li, Y.; Yang, T.; Tang, W. The Relationship between Serum 25-hydroxyvitamin D and Insulin Sensitivity and Beta Cell Function in Newly Diagnosed Type 2 Diabetes. J. Diabetes Res. 2015. [Google Scholar] [CrossRef]
- Rosen, C.J.; Adams, J.S.; Bikle, D.D.; Black, D.M.; Demay, M.B.; Manson, J.E.; Murad, M.H.; Kovacs, C.S. The Nonskeletal Effects of Vitamin D: An Endocrine Society Scientific Statement. Endocr. Rev. 2012, 33, 456–492. [Google Scholar] [CrossRef]
- Palomer, X.; González-Clemente, J.M.; Blanco-Vaca, F.; Mauricio, D. Role of Vitamin D in the Pathogenesis of Type 2 Diabetes Mellitus. Diabetes Obes. Metab. 2008, 10, 185–197. [Google Scholar] [CrossRef] [PubMed]
- Stein, E.M.; Strain, G.; Sinha, N.; Ortiz, D.; Pomp, A.; Dakin, G.; McMahon, D.J.; Bockman, R.; Silverberg, S.J. Vitamin D Insufficiency Prior to Bariatric Surgery: Risk Factors and a Pilot Treatment Study. Clin. Endocrinol. 2009, 71, 176–183. [Google Scholar] [CrossRef] [PubMed]
- Wamberg, L.; Cullberg, K.B.; Rejnmark, L.; Richelsen, B.; Pedersen, S.B. Investigations of the Anti-inflammatory Effects of Vitamin D in Adipose Tissue: Results from an in vitro Study and a Randomized Controlled Trial. Horm. Metab. Res. 2013, 45, 456–462. [Google Scholar] [CrossRef] [PubMed]
- Xu, H.; Barnes, G.T.; Yang, Q. Chronic Inflammation in Fat Plays a Crucial Role in the Development of Obesity-related Insulin Resistance. J. Clin. Investig. 2003, 112, 1821–1830. [Google Scholar] [CrossRef]
- Sasso, F.C.; Pafundi, P.C.; Marfella, R.; Calabrò, P.; Piscione, F.; Furbatto, F.; Esposito, G.; Galiero, R.; Gragnano, F.; Rinaldi, L.; et al. Adiponectin and Insulin Resistance are Related to Restenosis and Overall New PCI in Subjects with Normal Glucose Tolerance: The Prospective AIRE Study. Cardiovasc. Diabetol. 2019, 18, 24. [Google Scholar] [CrossRef]
- Mathieu, C.; Van Etten, E.; Gysemans, C. In vitro and in vivo Analysis of the Immune System of Vitamin D Receptor Knockout Mice. J. Bone Miner. Res. 2001, 16, 2057–2065. [Google Scholar] [CrossRef]
- Healy, K.D.; Frahm, M.A.; DeLuca, H.F. 1,25-Dihydroxyvitamin D3 Up-regulates the Renal Vitamin D Receptor through Indirect Gene Activation and Receptor Stabilization. Arch. Biochem. Biophys. 2005, 433, 466–473. [Google Scholar] [CrossRef]
- Cade, C.; Norman, A.W. Rapid Normalization/Stimulation by 1,25-dihydroxyvitamin D3 of Insulin Secretion and Glucose Tolerance in the Vitamin D-deficient Rat. Endocrinology 1987, 120, 1490–1497. [Google Scholar] [CrossRef]
- Rafiq, S.; Jeppesen, P.B. Is Hypovitaminosis D Related to Incidence of Type 2 Diabetes and High Fasting Glucose Level in Healthy Subjects: A Systematic Review and Meta-analysis of Observational Studies. Nutrients 2018, 10, 59. [Google Scholar] [CrossRef]
- Alkharfy, K.M.; Al-Daghri, N.M.; Yakout, S.M. Calcitriol Attenuates Weight-related Systemic Inflammation and Ultrastructural Changes of the Liver in a Rodent Model. Basic Clin. Pharmacol. Toxicol. 2012, 112, 42–49. [Google Scholar] [CrossRef]
- Barnard, W.F.; Saxena, V.K.; Wenny, B.N.; DeLuisi, J.J. Daily Surface UV Exposure and Its Relationship to Surface Pollutant Measurements. J. Air Waste Manag. Assoc. 2003, 53, 237–245. [Google Scholar] [CrossRef]
- Elminir, H.K. Sensitivity of Ultraviolet Solar Radiation to Anthropogenic Air Pollutants and Weather Conditions. Atmos. Res. 2007, 84, 250–264. [Google Scholar] [CrossRef]
- Alam, U.; Arul-Devah, V.; Javed, S. Vitamin D and Diabetic Complications: True or False Prophet? Diabetes Ther. 2016, 7, 11–26. [Google Scholar] [CrossRef]
- Kaul, K.; Hodgkinson, A.; Tarr, J.M.; Kohner, E.M.; Chibber, R. Is Inflammation a Common Retinal-renal-nerve Pathogenic Link in Diabetes? Curr. Diabetes Rev. 2010, 6, 294–303. [Google Scholar] [CrossRef]
- Burton, J.M.; Kimball, S.; Vieth, R. A Phase I/II Dose-escalation Trial of Vitamin D3 and Calcium in Multiple Sclerosis. Neurology 2010, 74, 1852–1859. [Google Scholar] [CrossRef]
- Holmøy, T.; Moen, S.M. Assessing Vitamin D in the Central Nervous System. Acta Neurol. Scand. Suppl. 2010, 122, 88–92. [Google Scholar] [CrossRef]
- Simon, K.C.; Munger, K.L.; Ascherio, A. Vitamin D and Multiple Sclerosis: Epidemiology, Immunology, and Genetics. Curr. Opin. Neurol. 2012, 25, 246–251. [Google Scholar] [CrossRef]
- Fex, S.A.; Dahlin, L.B. Repair of the Peripheral Nerve—Remyelination That Works. Brain Sci. 2013, 3, 1182–1197. [Google Scholar]
- Neveu, I.; Naveilhan, P.; Jehan, F. 1,25-Dihydroxyvitamin D3 Regulates the Synthesis of Nerve Growth Factor in Primary Cultures of Glial Cells. Brain Res. Mol. Brain Res. 1994, 24, 70–76. [Google Scholar] [CrossRef]
- Ito, S.; Ohtsuki, S.; Nezu, Y.; Koitabashi, Y.; Murata, S.; Terasaki, T. 1,25-Dihydroxyvitamin D3 Enhances Cerebral Clearance of Human Amyloid-b Peptide (1-40) from Mouse Brain Across the Blood-brain Barrier. Fluids Barriers CNS 2011, 8, 1–10. [Google Scholar] [CrossRef]
- Generini, S.; Tuveri, M.A.; Matucci Cerinic, M.; Mastinu, F.; Manni, L.; Aloe, L. Topical Application of Nerve Growth Factor in Human Diabetic Foot Ulcers. A Study of Three Cases. Exp. Clin. Endocrinol. Diabetes 2004, 112, 542–544. [Google Scholar] [CrossRef] [PubMed]


Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Rafiq, S.; Jeppesen, P.B. Insulin Resistance Is Inversely Associated with the Status of Vitamin D in Both Diabetic and Non-Diabetic Populations. Nutrients 2021, 13, 1742. https://doi.org/10.3390/nu13061742
Rafiq S, Jeppesen PB. Insulin Resistance Is Inversely Associated with the Status of Vitamin D in Both Diabetic and Non-Diabetic Populations. Nutrients. 2021; 13(6):1742. https://doi.org/10.3390/nu13061742
Chicago/Turabian StyleRafiq, Shamaila, and Per Bendix Jeppesen. 2021. "Insulin Resistance Is Inversely Associated with the Status of Vitamin D in Both Diabetic and Non-Diabetic Populations" Nutrients 13, no. 6: 1742. https://doi.org/10.3390/nu13061742
APA StyleRafiq, S., & Jeppesen, P. B. (2021). Insulin Resistance Is Inversely Associated with the Status of Vitamin D in Both Diabetic and Non-Diabetic Populations. Nutrients, 13(6), 1742. https://doi.org/10.3390/nu13061742





