Interventions to Promote Healthy Meals in Full-Service Restaurants and Canteens: A Systematic Review and Meta-Analysis
Abstract
1. Introduction
2. Materials and Methods
2.1. Search Strategy
2.2. Screening
2.3. Inclusion and Exclusion Criteria
2.4. Data Extraction and Management
2.5. Data Synthesis
2.6. Outcomes
2.7. Data Analysis
2.8. Risk of Bias and Quality Criteria
3. Results
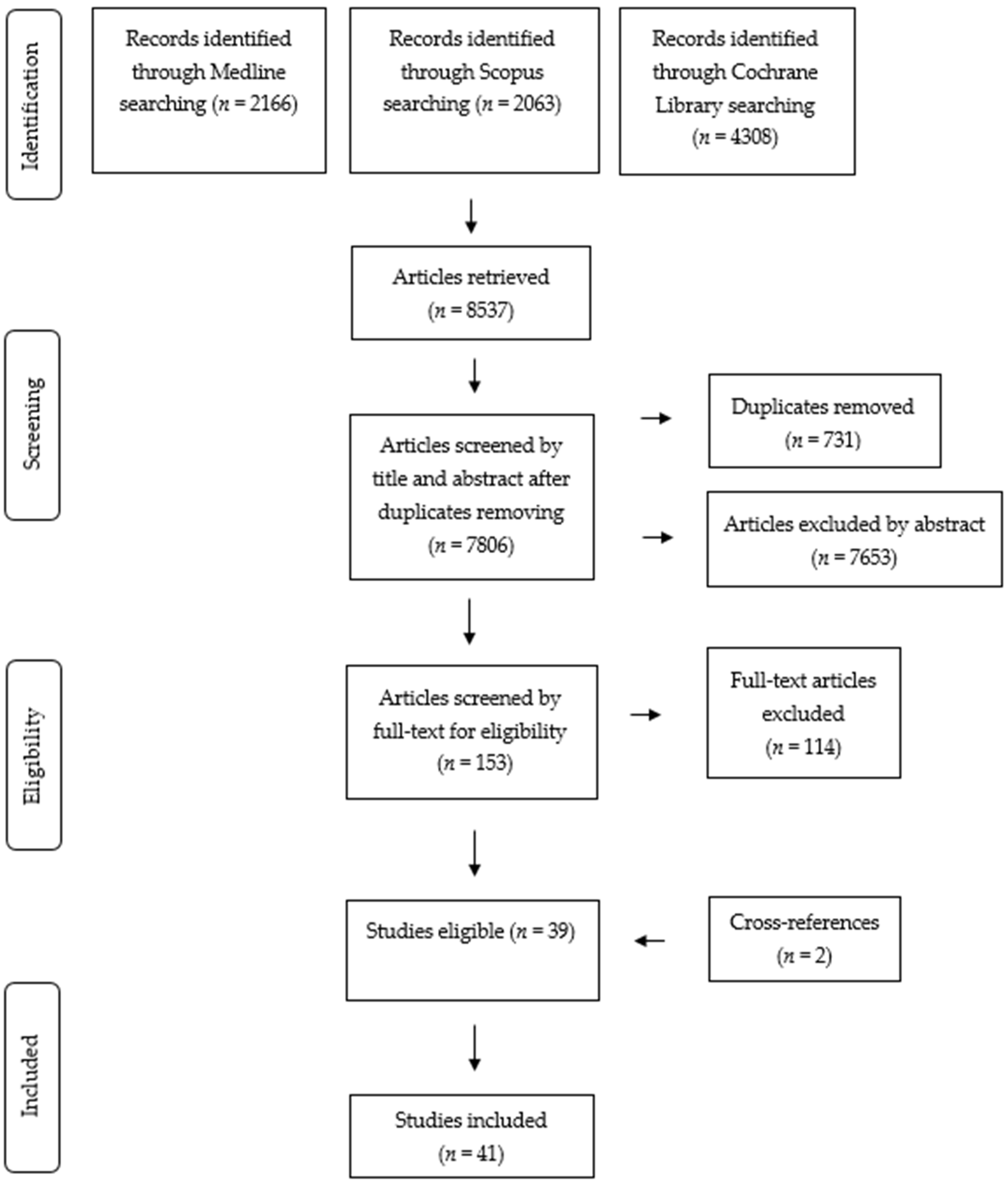
3.1. Results of the Search
3.2. General Characteristics of the Included Intervention Studies
3.3. Settings of the Included Studies
3.4. Samples of the Included Studies
3.5. Intervention Duration
3.6. Intervention Type
3.7. Outcomes
3.8. Dietary Intake Outcome Category
3.9. Food Availability Outcome Category
3.10. Food Purchase Outcome Category
3.11. Results of the Meta-Analysis
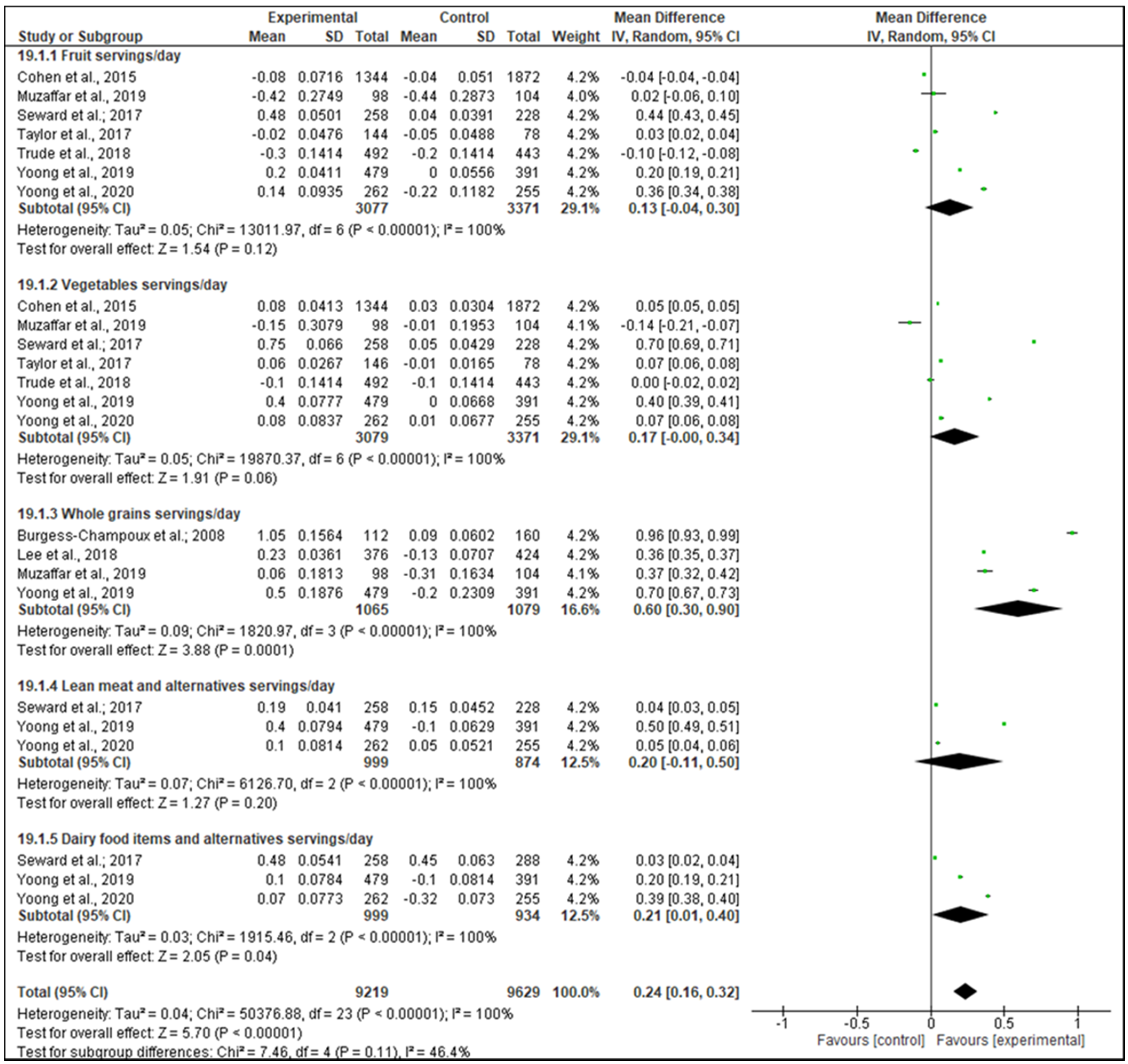
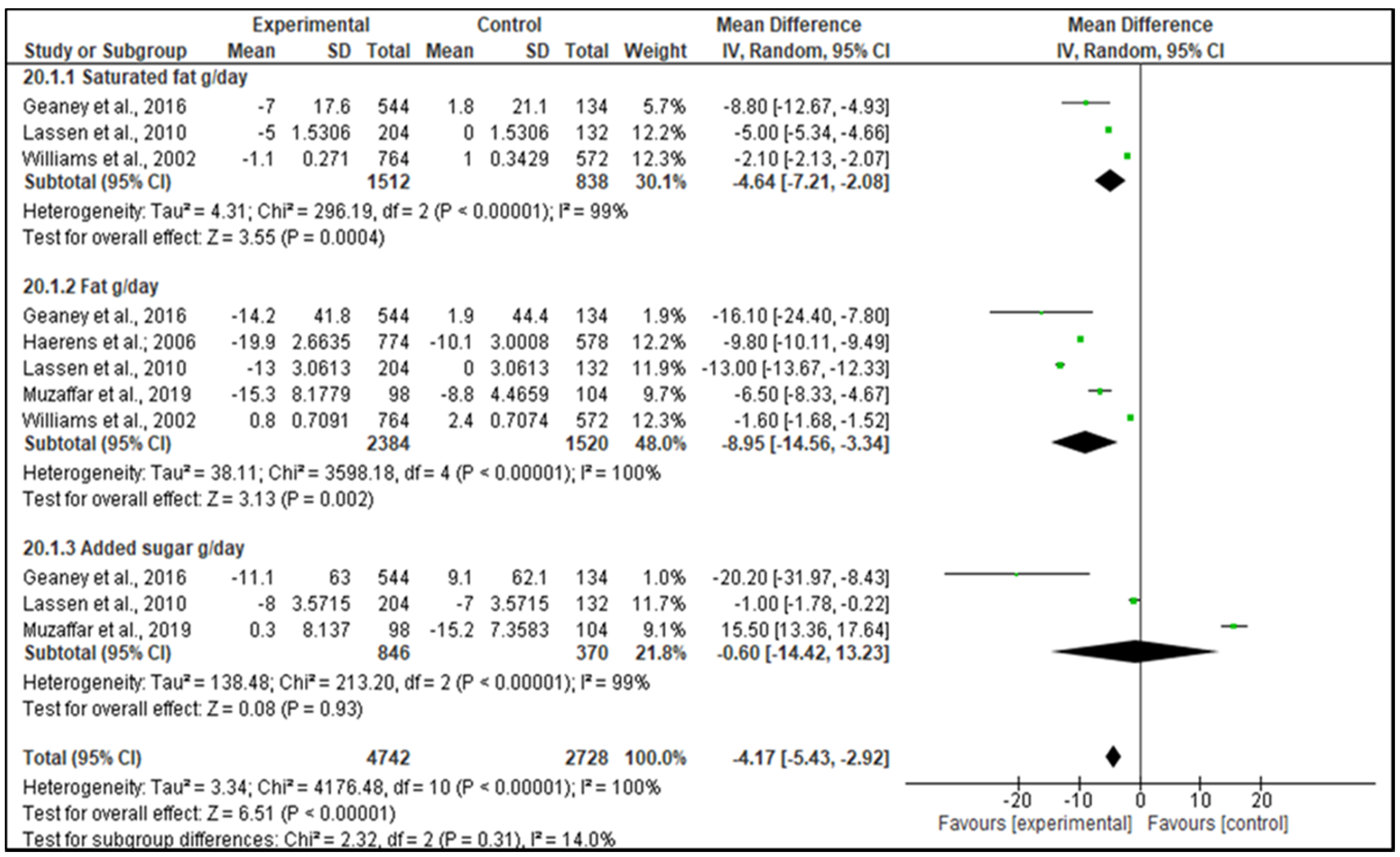
3.11.1. Dietary Intake Meta-Analysis
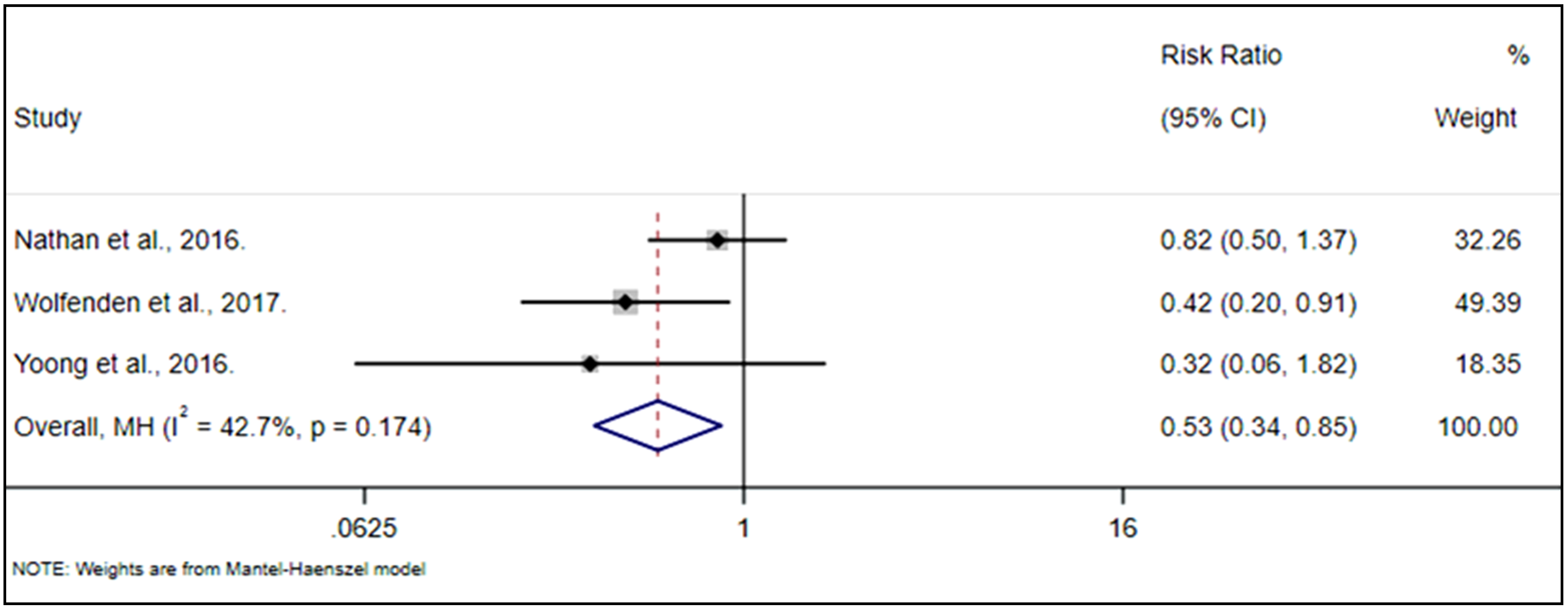
3.11.2. Food Availability Meta-Analysis
3.12. Quality Assessment Results
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
Abbreviations
References
- Jia, X.; Liu, J.; Chen, B.; Jin, D.; Fu, Z.; Liu, H.; Du, S.; Popkin, B.M.; Mendez, M.A. Differences in nutrient and energy contents of commonly consumed dishes prepared in restaurants v. at home in Hunan Province, China. Public Health Nutr. 2018, 21, 1307–1318. [Google Scholar] [CrossRef]
- Jabs, J.; Devine, C.M. Time scarcity and food choices: An overview. Appetite 2006, 47, 196–204. [Google Scholar] [CrossRef]
- Myhre, J.B.; Loken, E.B.; Wandel, M.; Andersen, L.F. Eating location is associated with the nutritional quality of the diet in Norwegian adults. Public Health Nutr. 2014, 17, 915–923. [Google Scholar] [CrossRef] [PubMed]
- Lake, A.A.; Burgoine, T.; Stamp, E.; Grieve, R. The foodscape: Classification and field validation of secondary data sources across urban/rural and socio-economic classifications in England. Int. J. Behav. Nutr. Phys. Act. 2012, 9, 37. [Google Scholar] [CrossRef] [PubMed]
- Suggs, L.S.; Della Bella, S.; Rangelov, N.; Marques-Vidal, P. Is it better at home with my family? The effects of people and place on children’s eating behavior. Appetite 2018, 121, 111–118. [Google Scholar] [CrossRef]
- Fulkerson, J.A.; Larson, N.; Horning, M.; Neumark-Sztainer, D. A review of associations between family or shared meal frequency and dietary and weight status outcomes across the lifespan. J. Nutr. Educ. Behav. 2014, 46, 2–19. [Google Scholar] [CrossRef] [PubMed]
- Lin, B.; Guthrie, J. Nutritional Quality of Food Prepared at Home and Away from Home, 1977–2008, EIB-105; U.S. Department of Agriculture, Economic Research Service: Washington, DC, USA, 2012.
- Swinburn, B.; Caterson, I.; Seidell, J.; James, W. Diet, nutrition and the prevention of excess weight gain and obesity. Public Health Nutr. 2004, 7, 123–146. [Google Scholar] [CrossRef]
- WHO and FAO Diet, Nutrition, and the Prevention of Chronic Diseases (Report of a joint WHO and FAO Expert Consulation). WHO Tech. Rep. Ser. 2003, 916, 1–160.
- Zang, J.; Luo, B.; Wang, Y.; Zhu, Z.; Wang, Z.; He, X.; Wang, W.; Guo, Y.; Chen, X.; Wang, C.; et al. Eating Out-of-Home in Adult Residents in Shanghai and the Nutritional Differences among Dining Places. Nutrients 2018, 10, 951. [Google Scholar] [CrossRef] [PubMed]
- Penney, T.; Burgoine, T.; Monsivais, P. Relative Density of Away from Home Food Establishments and Food Spend for 24,047 Households in England: A Cross-Sectional Study. Int. J. Environ. Res. Public Health 2018, 15, 2821. [Google Scholar] [CrossRef] [PubMed]
- Patel, A.A.; Lopez, N.V.; Lawless, H.T.; Njike, V.; Beleche, M.; Katz, D.L. Reducing calories, fat, saturated fat, and sodium in restaurant menu items: Effects on consumer acceptance. Obesity 2016, 24, 2497–2508. [Google Scholar] [CrossRef] [PubMed]
- Freedman, M.R.; Brochado, C. Reducing Portion Size Reduces Food Intake and Plate Waste. Obesity 2010, 18, 1864–1866. [Google Scholar] [CrossRef]
- Kerins, C.; McSharry, J.; Hayes, C.; Perry, I.J.; Geaney, F.; Kelly, C. Barriers and facilitators to implementation of menu labelling interventions to support healthy food choices: A mixed methods systematic review protocol. Syst. Rev. 2018, 7, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Unilever Food Solutions World Report Menu: Seductive Nutrition; Unilever Food Solutions: London, UK, 2012; pp. 1–16.
- Hillier-Brown, F.C.; Summerbell, C.D.; Moore, H.J.; Routen, A.; Lake, A.A.; Adams, J.; White, M.; Araujo-Soares, V.; Abraham, C.; Adamson, A.J.; et al. The impact of interventions to promote healthier ready-to-eat meals (to eat in, to take away or to be delivered) sold by specific food outlets open to the general public: A systematic review. Obes. Rev. 2017, 18, 227–246. [Google Scholar] [CrossRef]
- Wright, B.; Bragge, P. Interventions to promote healthy eating choices when dining out: A systematic review of reviews. Br. J. Health Psychol. 2018, 23, 278–295. [Google Scholar] [CrossRef]
- Valdivia Espino, J.N.; Guerrero, N.; Rhoads, N.; Simon, N.-J.; Escaron, A.L.; Meinen, A.; Nieto, F.J.; Martinez-Donate, A.P. Community-Based Restaurant Interventions to Promote Healthy Eating: A Systematic Review. Prev. Chronic Dis. 2015, 12. [Google Scholar] [CrossRef] [PubMed]
- Public Health England. Strategies for Encouraging Healthier ‘O ut of Home’ Food Provision A Toolkit for Local Councils Working with Small Food Businesses; Public Health England: London, UK, 2017.
- Pérez-Rodrigo, C.; Klepp, K.-I.; Yngve, A.; Sjöström, M.; Stockley, L.; Aranceta, J. The school setting: An opportunity for the implementation of dietary guidelines. Public Health Nutr. 2001, 4, 717–724. [Google Scholar] [CrossRef] [PubMed]
- Smith, S.A.; Lake, A.A.; Summerbell, C.; Araujo-Soares, V.; Hillier-Brown, F. The effectiveness of workplace dietary interventions: Protocol for a systematic review and meta-analysis. Syst. Rev. 2016, 5, 1–6. [Google Scholar] [CrossRef] [PubMed]
- Moher, D.; Liberati, A.; Tetzlaff, J.; Altman, D.G.; Altman, D.; Antes, G.; Atkins, D.; Barbour, V.; Barrowman, N.; Berlin, J.A.; et al. Preferred reporting items for systematic reviews and meta-analyses: The PRISMA statement (Chinese edition). J. Chin. Integr. Med. 2009, 7, 889–896. [Google Scholar] [CrossRef]
- Ouzzani, M.; Hammady, H.; Fedorowicz, Z.; Elmagarmid, A. Rayyan QCRI. Available online: Rayyan.ai (accessed on 3 November 2020).
- Methley, A.M.; Campbell, S.; Chew-Graham, C.; McNally, R.; Cheraghi-Sohi, S. PICO, PICOS and SPIDER: A comparison study of specificity and sensitivity in three search tools for qualitative systematic reviews. BMC Health Serv. Res. 2014, 14. [Google Scholar] [CrossRef]
- Delaney, T.; Wyse, R.; Yoong, S.L.; Sutherland, R.; Wiggers, J.; Ball, K.; Campbell, K.; Rissel, C.; Lecathelinais, C.; Wolfenden, L. Cluster randomized controlled trial of a consumer behavior intervention to improve healthy food purchases from online canteens. Am. J. Clin. Nutr. 2017, 106, 1311–1320. [Google Scholar] [CrossRef] [PubMed]
- Ayala, G.X.; Castro, I.A.; Pickrel, J.L.; Lin, S.-F.; Williams, C.B.; Madanat, H.; Jun, H.-J.; Zive, M. A Cluster Randomized Trial to Promote Healthy Menu Items for Children: The Kids’ Choice Restaurant Program. Int. J. Environ. Res. Public Health 2017, 14, 1494. [Google Scholar] [CrossRef] [PubMed]
- Cohen, J.F.W.; Richardson, S.A.; Cluggish, S.A.; Parker, E.; Catalano, P.J.; Rimm, E.B. Effects of Choice Architecture and Chef-Enhanced Meals on the Selection and Consumption of Healthier School Foods. JAMA Pediatr. 2015, 169, 431. [Google Scholar] [CrossRef]
- Thorndike, A.N.; Riis, J.; Levy, D.E. Social norms and financial incentives to promote employees’ healthy food choices: A randomized controlled trial. Prev. Med. 2016, 86, 12–18. [Google Scholar] [CrossRef]
- Habib-Mourad, C.; Ghandour, L.A.; Moore, H.J.; Nabhani-Zeidan, M.; Adetayo, K.; Hwalla, N.; Summerbell, C. Promoting healthy eating and physical activity among school children: Findings from Health-E-PALS, the first pilot intervention from Lebanon. BMC Public Health 2014, 14, 1–11. [Google Scholar] [CrossRef] [PubMed]
- Lugtenberg, M.; Burgers, J.S.; Westert, G.P. Effects of evidence-based clinical practice guidelines on quality of care: A systematic review. Qual. Saf. Health Care 2009, 18, 385–392. [Google Scholar] [CrossRef]
- Yamada, J.; Shorkey, A.; Barwick, M.; Widger, K.; Stevens, B.J. The effectiveness of toolkits as knowledge translation strategies for integrating evidence into clinical care: A systematic review. BMJ Open 2015, 5. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. Healthy Diet; World Health Organization: Geneva, Switzerland, 2015.
- Dobbs, R.; Sawers, C.; Thompson, F.; Manyika, J.; Woetzel, J.; Child, P.; McKenna, S.; Spatharou, A. Overcoming obesity: An initial economic analysis Discussion paper. McKinsey Glob. Inst. 2014, 1–71. [Google Scholar]
- Chernev, A. Product assortment and consumer choice: An interdisciplinary review. Found. Trends Mark. 2011, 6, 1–61. [Google Scholar] [CrossRef]
- Grant, J.; Hunter, A. Measuring inconsistency in knowledgebases. J. Intell. Inf. Syst. 2006, 27, 159–184. [Google Scholar] [CrossRef]
- Effective Public Health Practice Project. Quality Assessment Tool for Quantitative Studies Component Ratings; Effective Public Health Practice Project: Hamilton, ON, Canada, 1998; pp. 2–5. [Google Scholar]
- Beets, M.W.; Weaver, R.G.; Turner-McGrievy, G.; Huberty, J.; Ward, D.S.; Freedman, D.; Hutto, B.; Moore, J.B.; Beighle, A. Making Healthy Eating Policy Practice: A Group Randomized Controlled Trial on Changes in Snack Quality, Costs, and Consumption in After-School Programs. Am. J. Health Promot. 2016, 30, 521–531. [Google Scholar] [CrossRef] [PubMed]
- Cohen, J.F.W.; Rimm, E.B.; Bryn Austin, S.; Hyatt, R.R.; Kraak, V.I.; Economos, C.D. A food service intervention improves whole grain access at lunch in rural elementary schools. J. Sch. Health 2014, 84, 212–219. [Google Scholar] [CrossRef] [PubMed]
- Grady, A.; Wolfenden, L.; Wiggers, J.; Rissel, C.; Finch, M.; Flood, V.; Salajan, D.; O’Rourke, R.; Stacey, F.; Wyse, R.; et al. Effectiveness of a web-based menu-planning intervention to improve childcare service compliance with dietary guidelines: Randomized controlled trial. J. Med. Internet Res. 2020, 22, 1–16. [Google Scholar] [CrossRef]
- Martínez-Donate, A.P.; Riggall, A.J.; Meinen, A.M.; Malecki, K.; Escaron, A.L.; Hall, B.; Menzies, A.; Garske, G.; Nieto, F.J.; Nitzke, S. Evaluation of a pilot healthy eating intervention in restaurants and food stores of a rural community: A randomized community trial. BMC Public Health 2015, 15. [Google Scholar] [CrossRef] [PubMed]
- Nathan, N.; Yoong, S.L.; Sutherland, R.; Reilly, K.; Delaney, T.; Janssen, L.; Robertson, K.; Reynolds, R.; Chai, L.K.; Lecathelinais, C.; et al. Effectiveness of a multicomponent intervention to enhance implementation of a healthy canteen policy in Australian primary schools: A randomised controlled trial. Int. J. Behav. Nutr. Phys. Act. 2016, 13, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Nik Rosmawati, N.H.; Wan Manan, W.M.; Noor Izani, N.J.; Nik Nurain, N.H.; Razlina, A.R. Impact of food nutrition intervention on food handlers’ knowledge and competitive food serving: A randomized controlled trial. Int. Food Res. J. 2017, 24, 1046–1056. [Google Scholar]
- Seward, K.; Wolfenden, L.; Finch, M.; Wiggers, J.; Wyse, R.; Jones, J.; Yoong, S.L. Improving the implementation of nutrition guidelines in childcare centres improves child dietary intake: Findings of a randomised trial of an implementation intervention. Public Health Nutr. 2018, 21, 607–617. [Google Scholar] [CrossRef]
- De Souza, R.A.G.; Mediano, M.F.F.; de Moura Souza, A.; Sichieri, R. Reducing the use of sugar in public schools: A randomized cluster trial. Rev. Saude Publica 2013, 47. [Google Scholar] [CrossRef]
- Wolfenden, L.; Kingsland, M.; Rowland, B.C.; Dodds, P.; Gillham, K.; Yoong, S.L.; Sidey, M.; Wiggers, J. Improving availability, promotion and purchase of fruit and vegetable and non sugar-sweetened drink products at community sporting clubs: A randomised trial. Int. J. Behav. Nutr. Phys. Act. 2015, 12, 35. [Google Scholar] [CrossRef] [PubMed]
- Wolfenden, L.; Nathan, N.; Janssen, L.M.; Wiggers, J.; Reilly, K.; Delaney, T.; Williams, C.M.; Bell, C.; Wyse, R.; Sutherland, R.; et al. Multi-strategic intervention to enhance implementation of healthy canteen policy: A randomised controlled trial. Implement. Sci. 2017, 12, 6. [Google Scholar] [CrossRef]
- Yoong, S.L.; Nathan, N.; Wolfenden, L.; Reilly, K.; Janssen, L.; Preece, S.; Butler, P.; Wiggers, J.; Sutherland, R.; Delaney, T.; et al. CAFÉ: A multicomponent audit and feedback intervention to improve implementation of healthy food policy in primary school canteens: A randomised controlled trial. Int. J. Behav. Nutr. Phys. Act. 2016, 13, 1–11. [Google Scholar] [CrossRef] [PubMed]
- Story, M.; Snyder, M.P.; Anliker, J.; Weber, J.L.; Cunningham-Sabo, L.; Stone, E.J.; Chamberlain, A.; Ethelbah, B.; Suchindran, C.; Ring, K. Changes in the nutrient content of school lunches: Results from the Pathways study. Prev. Med. 2003, 37, S35–S45. [Google Scholar] [CrossRef]
- Haerens, L.; Deforche, B.; Maes, L.; Cardon, G.; Stevens, V.; De Bourdeaudhuij, I. Evaluation of a 2-year physical activity and healthy eating intervention in middle school children. Health Educ. Res. 2006, 21, 911–921. [Google Scholar] [CrossRef] [PubMed]
- Lassen, A.D.; Thorsen, A.V.; Sommer, H.M.; Fagt, S.; Trolle, E.; Biltoft-Jensen, A.; Tetens, I. Improving the diet of employees at blue-collar worksites: Results from the Food at Work intervention study. Public Health Nutr. 2010, 14, 965–974. [Google Scholar] [CrossRef]
- Muzaffar, H.; Nikolaus, C.J.; Ogolsky, B.G.; Lane, A.; Liguori, C.; Nickols-Richardson, S.M. Promoting Cooking, Nutrition, and Physical Activity in Afterschool Settings. Am. J. Health Behav. 2019, 43, 1050–1063. [Google Scholar] [CrossRef]
- Lee, R.M.; Giles, C.M.; Cradock, A.L.; Emmons, K.M.; Okechukwu, C.; Kenney, E.L.; Thayer, J.; Gortmaker, S.L. Impact of the Out-of-School Nutrition and Physical Activity (OSNAP) Group Randomized Controlled Trial on Children’s Food, Beverage, and Calorie Consumption among Snacks Served. J. Acad. Nutr. Diet. 2018, 118, 1425–1437. [Google Scholar] [CrossRef] [PubMed]
- Anderson, A.S.; Porteous, L.E.G.; Foster, E.; Higgins, C.; Stead, M.; Hetherington, M.; Ha, M.-A.; Adamson, A.J. The impact of a school-based nutrition education intervention on dietary intake and cognitive and attitudinal variables relating to fruits and vegetables. Public Health Nutr. 2005, 8, 650–656. [Google Scholar] [CrossRef]
- Ochoa-Avilés, A.; Verstraeten, R.; Huybregts, L.; Andrade, S.; Van Camp, J.; Donoso, S.; Ramírez, P.L.; Lachat, C.; Maes, L.; Kolsteren, P. A school-based intervention improved dietary intake outcomes and reduced waist circumference in adolescents: A cluster randomized controlled trial. Nutr. J. 2017, 16, 1–12. [Google Scholar] [CrossRef]
- Siega-Riz, A.M.; El Ghormli, L.; Mobley, C.; Gillis, B.; Stadler, D.; Hartstein, J.; Volpe, S.L.; Virus, A.; Bridgman, J. The effects of the HEALTHY study intervention on middle school student dietary intakes. Int. J. Behav. Nutr. Phys. Act. 2011, 8. [Google Scholar] [CrossRef] [PubMed]
- Trude, A.C.B.; Surkan, P.J.; Cheskin, L.J.; Gittelsohn, J. A multilevel, multicomponent childhood obesity prevention group-randomized controlled trial improves healthier food purchasing and reduces sweet-snack consumption among low-income African-American youth. Nutr. J. 2018, 17, 96. [Google Scholar] [CrossRef]
- Warren, J.M.; Henry, C.J.K.; Lightowler, H.J.; Bradshaw, S.M.; Perwaiz, S. Evaluation of a pilot school programme aimed at the prevention of obesity in children. Health Promot. Int. 2003, 18, 287–296. [Google Scholar] [CrossRef] [PubMed]
- Yoong, S.L.; Grady, A.; Seward, K.; Finch, M.; Wiggers, J.; Lecathelinais, C.; Wedesweiler, T.; Wolfenden, L. The Impact of a Childcare Food Service Intervention on Child Dietary Intake in Care: An Exploratory Cluster Randomized Controlled Trial. Am. J. Health Promot. 2019, 33, 991–1001. [Google Scholar] [CrossRef] [PubMed]
- Yoong, S.L.; Grady, A.; Wiggers, J.H.; Stacey, F.G.; Rissel, C.; Flood, V.; Finch, M.; Wyse, R.; Sutherland, R.; Salajan, D.; et al. Child-level evaluation of a web-based intervention to improve dietary guideline implementation in childcare centers: A cluster-randomized controlled trial. Am. J. Clin. Nutr. 2020, 111, 854–863. [Google Scholar] [CrossRef]
- Bogart, L.M.; Cowgill, B.O.; Elliott, M.N.; Klein, D.J.; Hawes-Dawson, J.; Uyeda, K.; Elijah, J.; Binkle, D.G.; Schuster, M.A. A randomized controlled trial of Students for Nutrition and exercise: A community-based participatory research study. J. Adolesc. Health 2014, 55, 415–422. [Google Scholar] [CrossRef]
- Webb, K.L.; Solomon, L.S.; Sanders, J.; Akiyama, C.; Crawford, P.B. Menu labeling responsive to consumer concerns and shows promise for changing patron purchases. J. Hunger Environ. Nutr. 2011, 6, 166–178. [Google Scholar] [CrossRef]
- Bell, A.C.; Davies, L.; Francis, J.L.; Finch, M.; Wiggers, J.; Sutherland, R.; Wolfenden, L. An implementation intervention to encourage healthy eating in centre-based child-care services: Impact of the Good for Kids Good for Life programme. Public Health Nutr. 2014, 18, 1610–1619. [Google Scholar] [CrossRef] [PubMed]
- Burgess-Champoux, T.L.; Chan, H.W.; Rosen, R.; Marquart, L.; Reicks, M. Healthy whole-grain choices for children and parents: A multi-component school-based pilot intervention. Public Health Nutr. 2008, 11, 849–859. [Google Scholar] [CrossRef] [PubMed]
- Geaney, F.; Kelly, C.; Di Marrazzo, J.S.; Harrington, J.M.; Fitzgerald, A.P.; Greiner, B.A.; Perry, I.J. The effect of complex workplace dietary interventions on employees’ dietary intakes, nutrition knowledge and health status: A cluster controlled trial. Prev. Med. 2016, 89, 76–83. [Google Scholar] [CrossRef] [PubMed]
- Quinn, E.L.; Johnson, D.B.; Podrabsky, M.; Saelens, B.E.; Bignell, W.; Krieger, J. Effects of a behavioral economics intervention on food choice and food consumption in middle-school and high- school cafeterias. Prev. Chronic Dis. 2018, 15. [Google Scholar] [CrossRef]
- Bogart, L.M.; Elliott, M.N.; Uyeda, K.; Hawes-Dawson, J.; Klein, D.J.; Schuster, M.A. Preliminary healthy eating outcomes of SNaX, a pilot community-based intervention for adolescents. J. Adolesc. Health 2011, 48, 196–202. [Google Scholar] [CrossRef] [PubMed]
- Williams, C.L.; Bollella, M.C.; Strobino, B.A.; Spark, A.; Nicklas, T.A.; Tolosi, L.B.; Pittman, B.P. “Healthy-start”: Outcome of an intervention to promote a heart healthy diet in preschool children. J. Am. Coll. Nutr. 2002, 21, 62–71. [Google Scholar] [CrossRef] [PubMed]
- Kenney, E.L.; Gortmaker, S.L.; Carter, J.E.; Howe, M.C.W.; Reiner, J.F.; Cradock, A.L. Grab a cup, fill it up! An intervention to promote the 1 of drinking water and increase student water consumption during school lunch. Am. J. Public Health 2015, 105, 1777–1783. [Google Scholar] [CrossRef]
- Taylor, J.C.; Zidenberg-Cherr, S.; Linnell, J.D.; Feenstra, G.; Scherr, R.E. Impact of a multicomponent, school-based nutrition intervention on students’ lunchtime fruit and vegetable availability and intake: A pilot study evaluating the Shaping Healthy Choices Program. J. Hunger Environ. Nutr. 2018, 13, 415–428. [Google Scholar] [CrossRef]
- Giles, C.M.; Kenney, E.L.; Gortmaker, S.L.; Lee, R.M.; Thayer, J.C.; Mont-Ferguson, H.; Cradock, A.L. Increasing water availability during afterschool snack: Evidence, strategies, and partnerships from a group randomized trial. Am. J. Prev. Med. 2012, 43, S136–S142. [Google Scholar] [CrossRef] [PubMed]
- Wyse, R.; Gabrielyan, G.; Wolfenden, L.; Yoong, S.; Swigert, J.; Delaney, T.; Lecathelinais, C.; Ooi, J.Y.; Pinfold, J.; Just, D. Can changing the position of online menu items increase selection of fruit and vegetable snacks? A cluster randomized trial within an online canteen ordering system in Australian primary schools. Am. J. Clin. Nutr. 2019, 109, 1422–1430. [Google Scholar] [CrossRef] [PubMed]
- Morshed, A.B.; Davis, S.M.; Keane, P.C.; Myers, O.B.; Mishra, S.I. The Impact of the CHILE Intervention on the Food Served in Head Start Centers in Rural New Mexico. J. Sch. Health 2016, 86, 414–423. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Stroebele, N.; De Castro, J.M. Effect of ambience on food intake and food choice. Nutrition 2004, 20, 821–838. [Google Scholar] [CrossRef] [PubMed]
- McMorrow, L.; Ludbrook, A.; Macdiarmid, J.I.; Olajide, D. Perceived barriers towards healthy eating and their association with fruit and vegetable consumption. J. Public Health 2017, 39, 330–338. [Google Scholar] [CrossRef]
- Amore, L.; Buchthal, O.V.; Banna, J.C. Identifying perceived barriers and enablers of healthy eating in college students in Hawai’i: A qualitative study using focus groups. BMC Nutr. 2019, 5, 1–11. [Google Scholar] [CrossRef] [PubMed]
- Amine, E.K.; Baba, N.H.; Belhadj, M.; Deurenberg-Yap, M.; Djazayery, A.; Forrestre, T.; Galuska, D.A.; Herman, S.; James, W.P.T.; M’Buyamba Kabangu, J.R.; et al. Diet, nutrition and the prevention of chronic diseases. World Health Organ. Tech. Rep. Ser. 2003. [Google Scholar] [CrossRef]
- Ni Mhurchu, C.; Aston, L.; Jebb, S. Effects of worksite health promotion interventions on employee diets: A systematic review. BMC Public Health 2010, 10, 62. [Google Scholar] [CrossRef] [PubMed]
- Black, A.P.; D’Onise, K.; McDermott, R.; Vally, H.; O’Dea, K. How effective are family-based and institutional nutrition interventions in improving children’s diet and health? A systematic review. BMC Public Health 2017, 17, 1–19. [Google Scholar] [CrossRef]
- Baker, P.; Friel, S. Food systems transformations, ultra-processed food markets and the nutrition transition in Asia. Global. Health 2016, 12. [Google Scholar] [CrossRef]
- Clinton-McHarg, T.; Janssen, L.; Delaney, T.; Reilly, K.; Regan, T.; Nathan, N.; Wiggers, J.; Yoong, S.L.; Wyse, R.; Grady, A.; et al. Availability of food and beverage items on school canteen menus and association with items purchased by children of primary-school age. Public Health Nutr. 2018, 21, 2907–2914. [Google Scholar] [CrossRef]
- Young, K.; Kennedy, V.; Kingsland, M.; Sawyer, A.; Rowland, B.; Wiggers, J.; Wolfenden, L. Healthy food and beverages in senior community football club canteens in New South Wales, Australia. Health Promot. J. Aust. 2012, 23, 149–152. [Google Scholar] [CrossRef] [PubMed]
- Economos, C.D.; Folta, S.C.; Goldberg, J.; Hudson, D.; Collins, J.; Baker, Z.; Lawson, E.; Nelson, M. A community-based restaurant initiative to increase availability of healthy menu options in somerville, Massachusetts: Shape up somerville. Prev. Chronic Dis. 2009, 6, 1–8. [Google Scholar]
- Kim, M.; Budd, N.; Batorsky, B.; Krubiner, C.; Manchikanti, S.; Waldrop, G.; Trude, A.; Gittelsohn, J. Barriers to and Facilitators of Stocking Healthy Food Options: Viewpoints of Baltimore City Small Storeowners. Ecol. Food Nutr. 2017, 56, 17–30. [Google Scholar] [CrossRef] [PubMed]
- Boelsen-Robinson, T.; Blake, M.R.; Backholer, K.; Hettiarachchi, J.; Palermo, C.; Peeters, A. Implementing healthy food policies in health services: A qualitative study. Nutr. Diet. 2019, 76, 336–343. [Google Scholar] [CrossRef] [PubMed]
- Taylor, J.P.; Evers, S.; McKenna, M. Determinants of Healthy Eating in Children and Youth. Can. J. Public Health 2005, 96 (Suppl. 3), S22–S29. [Google Scholar] [CrossRef]
- Mendes, L.L.; Pessoa, M.C.; Duarte, C.K. Comments on the Article: “Food Environment Research in Low- and Middle-Income Countries: A Systematic Scoping Review”. Adv. Nutr. 2020, 11, 1044–1045. [Google Scholar] [CrossRef]
| Criteria | Description |
|---|---|
| Population | Restaurant and canteen consumers (children and adults) and their staff. |
| Intervention | Restaurant- and canteen-based interventions concerning the promotion of healthy meals. |
| Comparison group | Comparison Group as a CG receiving any intervention. |
| Outcomes | Improvement in the promotion of healthy foods offered in restaurants and canteens; increase in the offer and the demand for healthy meals. |
| Setting | Restaurants and canteens. |
| Study | Study Design and Type of Intervention | Setting | Country | Study Samples | Age | Duration 1 | Effectiveness | Between Groups Significance | Between Groups No Significant Changes |
|---|---|---|---|---|---|---|---|---|---|
| Ayala et al.; 2017. | Cluster RCT; 3-arm restaurant-based intervention. | Community (restaurants) | USA | 8 restaurants (Menu-plus IG n = 4; Menu-only CG n = 4) and weekend dinner customers (n = N/A). | ≥12 y | 2 m | Food purchase x | − | Weekly sales of new child menus ($/week). |
| Anderson et al.; 2005. | RCT; school-based nutrition education intervention. | School | Scotland | 4 schools (IG n = 2; CG n = 2) and 129 students (IG n = 64; CG n = 65). | 6–7 y and 10–11 y | 9 m | Dietary intake ✓x | ↑ Fruit (g). | Vegetables (g), total F&V (g), energy (kJ), % energy as fat/carbohydrate/protein, starch (g), sucrose (g). |
| Beets et al.; 2016. | RCT; multistep adaptive intervention. | Community (after-school program) | USA | 9 schools (IG n = 3; CG n = 6), 4 churches (IG n = 3; CG n = 1), 7 communities (IG n = 4; CG n = 3) and 1765 students (IG n = 895; CG n = 870). | 6–12 y | 12 m | Food availability x | ↑ F&V (days), ↑ dips (days); ↓ desserts (days), ↓ salty unflavored snacks (days), ↓total sweetened beverages (days), ↓ 100% fruit juice (days). | Dairy unsweetened snacks (days), dairy sweetened snacks (days), salty flavored snacks (days), unsweetened cereals (days), sugar-sweetened cereals (days), water, unflavored milk (days). |
| Bogart et al.; 2014. | RCT; multicomponent intervention. | School | USA | 10 schools (IG n = 5; CG n = 5) and 3039 students (IG n = 1515; CG n = 1524). | ±12–13 y | 5 w | Food purchase ✓x | ↑ All lunches (servings), ↑ free/reduced lunch (servings), ↑ full-price lunches (servings); ↑fruit servings during intervention; ↓ snack sales. | Fruit and vegetable servings postintervention. |
| Cohen et al.; 2014. | RCT; single-component intervention. | School | USA | 8 schools (IG n = 4; CG n = 4) and 2746 students (IG n = 1550; CG n = 1196). | 6–12 y | 1 w | Food availability ✓x | ↑ % of days offering WG (lunch). | WG and RG (options/breakfast and lunch), % of days offering WG (breakfast), % of days offering RG (breakfast and lunch). |
| Cohen et al.; 2015 | RCT; 4-arm chef and choice architecture school-based intervention. | School | USA | 14 schools (Chef IG-A n = 2; Smart Café IG-B n = 4; Chef plus Smart Café IG-C n = 2; CG n = 6) and 2638 students (Chef IG-A n = 379; Smart Café IG-B n = 651; Chef plus Smart Café IG-C n = 672; CG n = 936). | 8–16 y | 7 m (long-term intervention) | Dietary intake ✓x(IG-A, IG-C);x (IG-B). | ↑ cups of fruits (IG-A), ↑ cups of vegetables (IG-A, IG-C), ↑ % of vegetables (IG-A, IG-C). | % Entrée, % cups of fruit (IG-B, IG-C), Cups of vegetable (IG-B), % of fruit (IG-A, IG-B, IG-C), % of vegetables (IG-B). |
| Food purchase ✓x (IG-A, IG-B, IG-C) | ↑ % of students selecting fruit and vegetables (IG-A, IG-B, IG-C). | % of students selecting entrée (p = N/A). | |||||||
| Delaney et al.; 2017. | Cluster RCT; consumer behavior intervention. | School | Australia | 10 schools (IG n = 5; CG n = 5) and 2714 students (IG n = 1144; CG n = 1570). | 5–12 y | 2 m (+2 m follow-up) | Food purchase ✓x | ↑ Green menu items (%); ↓ energy (kJ), ↓ sodium (mg), ↓ saturated fat (g), ↓ red menu items (%). | Sugar (g). |
| Giles et al.; 2012. | RCT; environmental and policy change intervention. | Community (after-school programs) | USA | 20 after-school programs (IG n = 10; CG n = 10) and 145 students (IG n = 62; CG n = 83). | ±8 y | 6 m | Food purchase ✓x | ↑ water (ounces), ↑ frequency of water served/day; ↓ kcal from beverages served/day. | 100% juice (ounces and frequency of service), milk (ounces and frequency of service). |
| Grady et al.; 2020. | RCT; web-based menu-planning intervention. | School (childcare centers) | Australia | 54 childcare centers (IG n = 27; CG n = 27) and 54 menu planners (IG n = 27; CG n = 27). | 3–6 y | 12 m | Food availability ✓x | ↑ Fruit (servings), ↑ meat and alternatives (servings); ↓ discretionary foods (unhealthy) (times/day). | Servings of: vegetables, cereals and breads, dairy and alternatives. |
| Habib-Mourad et al.; 2014. | Pilot cluster RCT; multicomponent intervention. | School | Lebanon | 8 schools (IG n = 4; CG n = 4) and 374 students (IG n = 193; CG n = 181). | 9–11 y | 3 m | Food purchase ✓x | ↓ Chips (%, n), ↓ chocolate (%, n), ↓ soft drinks (%, n). | Sweetened beverages (p = N/A), croissant (%, n), manoushe (%, n). |
| Dietary intake ✓x | ↓ Chips (%, n), ↓ soft drinks (%, n). | Chocolate (%, n), sweetened drinks (%, n), fruit (%, n), sandwich (%, n). | |||||||
| Haerens et al.; 2006. | RCT; 3-arm environmental and computer-tailored intervention. | School | Belgium | 15 schools (parental involvement IG-A n = 5; intervention alone IG-B n = 5; CG n = 5) and 2840 students (IG-A n = 1226; IG-B/CG n = N/A). | ±13 y | 2 y | Dietary intake ✓x (girls); x (boys). | ↓ Fat (g) (girls), ↓ %E from fat (girls). | Fat (g) (boys), %E from fat (boys), pieces of fruit (boys and girls), soft drinks (glass) (boys and girls), water (glass) (boys and girls). |
| Kenney et al.; 2015. | Cluster RCT; school cafeteria-based intervention. | School | USA | 10 schools (IG n = 5; CG n = 5) and 1599 students (IG n = 725; CG n = 874). | 6–18 y | 3 w | Dietary intake ✓x | ↑ Water (ounces), ↑ % students consuming free water; ↓ % students consuming 100%juice, ↓ % students consuming sugar-sweetened beverages. | % students consuming milk, % students consuming other beverages. |
| Lassen et al.; 2010. | Cluster RCT; participatory and empowerment-based intervention. | Workplace | Denmark | 8 workplaces (IG n = 5; CG n= 3) and 168 employees (IG n = 102; CG n = 66). | ±42 y | 6 m | Dietary intake ✓x | ↑ Fiber (g/10 MJ), %E in carbohydrate; ↓ fat (g/day), ↓ saturated fat (g/day), ↓ fat (%E/day), ↓ cake and sweets (g/day and g/10 MJ). | Energy (kJ), protein (%E/day), added sugar (g/day and g/10 MJ), fiber (g/day), F&V (g/day and g/10 MJ), potatoes (g/day and g/10 MJ). |
| Lee et al.; 2018. | Cluster RCT; multilevel intervention. | Community (after-school programs) | USA | 20 after-school programs (IG n = 10; CG n = 10) and 400 students (IG n = 188; CG n = 212). | ≥5 y | 9 m | Dietary intake ✓ (for on-site food services) | ↑ whole grains (servings), ↑ F&V (servings); ↓ ounces 100% juice, ↓ foods with trans fats (servings), ↓ food and beverage calories (servings). | ‒ |
| Martínez-Donate et al.; 2015. | Pilot RCT; food environment restaurant and food store-based intervention. | Community (food stores and restaurants) | USA | 14 restaurants (IG n = 7; CG n = 7), 4 food stores (IG n = 2; CG n = 2), 721 restaurant customers (IG n = 319; CG n = 402) and 601 food store customers (IG n = 299; CG n = 302). | N/A | 10 m | Food purchase x | ‒ | % of restaurant orders, % of food store. purchases. |
| Food availability x | ‒ | Restaurant and food store nutrition environment (NEMS-R NEMS-S). | |||||||
| Morshed et al.; 2016. | Cluster RCT; multilevel obesity-prevention intervention. | School (childcare centers) | Mexico | 16 childcare centers (IG n = 8; CG n = 8) and children (n = N/A). | 3 y | 2 y | Food availability ✓x | ↓ Daily grams of fat from milk. | Fruit (servings), vegetables (servings), whole grains (servings), discretionary fat (grams), added sugar (teaspoons). |
| Muzaffar et al.; 2019. | Cluster RCT; peer education intervention. | Community (after-school programs) | USA | 7 school groups (peer-led IG n = 4; adult-led CG n = 3) and 101 children (IG n = 49; CG n = 52). | 11–14 y | 3 m | Dietary intake ✓x | ↑ Whole grains (servings). | Total kcal/day, fruits (servings), vegetables (servings), total fat/sugar/fiber/salt (g). |
| Nathan et al.; 2016. | RCT; multicomponent intervention. | School | Australia | 53 schools (IG n = 28; CG n = 25) and 499 students (IG mean n = 232; CG mean n = 267). | 5–12 y | 9 m | Food availability ✓ | ↑ Menu with no red/banned items, ↑ menu with >50% of green items. | ‒ |
| Ochoa-Avilés et al.; 2017. | Cluster RCT; curriculum and environment-based intervention. | School | Ecuador | 20 schools (IG n = 10; CG n = 10) and 1430 students (IG n = 702; CG n = 728). | 12–14 y | 28 m | Dietary intake ✓x | ↑ F&V (g); ↓ added sugar (g), ↓ unhealthy snacking (g). | Unhealthy snacking at school (proportion difference), breakfast intake (proportion difference), fat (%E/day). |
| Rosmawati et al.; 2017. | Cluster RCT; school-canteen intervention. | School | Malaysia | 16 schools (IG n = 8; CG n = 8) and 110 food handlers (IG n = 52; CG n = 58). | 18–55 y | 6 w (+12 w follow-up) | Food availability ✓x | ↑ Milk and milk products (% served food). | % served food: carbohydrate, protein, fat, added sugar, vegetable, fruits, forbidden and not recommended foods, fast foods. |
| Seward et al.; 2017. | RCT; multistrategy intervention. | School (childcare centers) | Australia | 45 childcare centers (IG n = 25; CG n = 20), canteen cooks (IG n = 25; CG n = 20), and 243 students (IG n = 129; CG n = 114). | N/A | 6 m | Food availability ✓ | Servings of: ↑ vegetables, ↑ fruit, ↑ breads and cereals, ↑ meat and alternatives, ↑ dairy; ↓ discretionary foods (unhealthy). | ‒ |
| Dietary intake ✓x | ↑ Vegetables (servings), ↑ fruit (servings). | Servings of: breads and cereals, meat, dairy, discretionary. | |||||||
| Siega-Riz et al.; 2011. | Cluster RCT; school-based intervention. | School | USA | 42 schools (IG n = 21; CG n = 21) and 3908 students (IG n = 1964; CG n = 1944). | 10–14 y | 30 m (five school semesters) | Dietary intake ✓x | ↑ Fruit (g), ↑ water (g). | Energy (kcal), carbohydrates (g), protein (g), fat (g), fiber (g), grains (g), vegetables (g), legumes (g), sweets (g), sweetened beverages (g), fruit juice (g), fat and whole milk (g), 1% fat milk (g). |
| Souza et al.; 2013. | Cluster RCT; nutrition educational intervention. | School | Brazil | 20 schools (IG n = 10; CG n = 10), 95 school lunch chefs (IG n = 47; CG n = 48) aged ±46 years, and students (n = N/A). | N/A | 7 m | Food availability x | − | kg/child of: sugar, donuts, milky coffee, banana cereals, chocolate cereals, chocolate milk, powdered milk, cake mix. |
| Dietary intake x | − | Energy (kcal), carbohydrates (%), lipid (%), protein (%), % energy derived from sugar/sweets/sugary drinks, portions/day of added sugar/sugary drinks/sweets. | |||||||
| Story et al.; 2003. | RCT; multicomponent multicenter intervention. | School | USA | 41 schools (IG n = 21; CG n = 20) and 1700 students (IG/CG n = N/A). | 7–9 y | 3 y | Food availability ✓x | ↑ % energy from carbohydrates; ↓ % energy from total fat and saturated fat. | Total calories (kcal), total fat (g), saturated fat (g), protein (g), % energy from protein, carbohydrates (g), total sugars (g), sucrose (g), dietary fiber (g), sodium (mg). |
| Taylor et al.; 2017. | Pilot RCT; multicomponent intervention. | School | USA | 2 schools (IG n = 1; CG n = 1) and 294 students (IG n = 161; CG n = 133). | 9–10 y | 9 m | Dietary intake ✓x | ↑ Vegetable (cups). | Fruit (cups). |
| Food purchase x | ‒ | Vegetable (cups), fruit (cups). | |||||||
| Thorndike et al.; 2016. | RCT; 3-arm social norm intervention. | Workplace (hospital cafeteria) | USA | 1 hospital and 2672 employees (feedback-only IG-A n = 877; feedback-incentive IG-B n = 925; CG n = 870). | ≥18 y | 3 m | Food purchase ✓(IG-B); x (IG-A) | ↑ Green menu items (%) (IG-B). | Green menu items (IG-A) (%). |
| Trude et al.; 2018. | Cluster RCT; multilevel and multicomponent intervention. | Community (recreation centers including wholesalers, corner stores and carryout restaurants) | USA | 30 recreation center zones (IG n = 14; CG n = 16) and 401 child–caregiver dyads (IG n = 209; CG n = 192). | 9–15 y | 14 m | Dietary intake ✓x | ↓ % kcal from sweets (13-15y). | Total daily caloric intake, sugary beverages (kcal), fruit punch (ounces), dietary total sugar (g), dietary sodium (mg), fruit (total cups), vegetable (total cups), fat (servings) (9–15y); % kcal from sweets (9–12y). |
| Food purchase ✓x | ↑ healthier foods and beverages items per week (9–12y); ↑ unhealthy foods and beverages items per week (9–12y). | Healthy and unhealthy foods and beverages items per week (13–15y). | |||||||
| Warren et al.; 2003. | Pilot RCT; 4-arm school and family-based intervention. | School | UK | 3 schools and 218 students (Eat Smart IG-A n = 56; Play Smart IG-B n = 54; Eat/Play Smart IG-C n = 54; Be Smart CG n = 54). | 5–7 y | 5 m | Dietary intake x (IG-A, IG-B, IG-C) | − | Weekly portion frequency of: vegetables, salads, fresh fruit, other fruit, confectionery, crisps (IG-A, IG-B, IG-C). |
| Webb et al.; 2011. | Pilot RCT; menu labeling intervention. | Workplace (hospital cafeteria) | USA | 6 cafeterias (menu board plus poster labeling IG n = 2; CG n = 2) and 554 customers (IG n = 334; CG n = 220). | >18 y | 2 m | Food purchase ✓x | ↑ % target side dishes (healthy), ↑ % target snacks (healthy). | % target entrées (healthy) (data N/A). |
| Wolfenden et al.; 2015. | Cluster RCT; multicomponent intervention. | Community (sporting clubs) | Australia | 85 sporting clubs (IG n = 42; CG n = 43) and 1394 club members (IG n = 689; CG n = 705). | ±34 y | 2.5 y | Food availability ✓x | ↑ F&V availability and promotion (%, n). | Non sugar-sweetened beverages (%, n). |
| Food purchase ✓ | ↑ F&V (%, n items purchased), ↑ no sugar-sweetened beverages (%, n items purchased). | ‒ | |||||||
| Wolfenden et al.; 2017. | RCT; multistrategic intervention. | School | Australia | 70 schools (IG n = 35; CG n = 35) and 509 students (IG mean n = 256; CG mean n = 253). | 5–12 y | 12/14 m | Food availability ✓ | ↑ Menu with no red/banned items, ↑ menu with >50% of green items. | ‒ |
| Food purchase ✓x | ↓ Total fat (g). | Energy (kJ), sodium (mg). | |||||||
| Wyse et al.; 2019. | Cluster RCT; online menu choice architecture intervention. | School | Australia | 6 schools (IG n = 3; CG n = 3) and 1938 students (IG n = 1203; CG n = 735). | 4–12 y | 4 w | Food purchase x | ‒ | % lunch orders containing target items (Fruit & Vegetable), % lunch order items that are target items (Fruit & Vegetable). |
| Yoong et al.; 2016. | RCT; multicomponent intervention. | School | Australia | 72 schools (IG n = 36; CG n = 36) and 426 students (IG mean n = 216; CG mean n = 210). | 5–12 y | 12 m | Food availability ✓x | ↓ % of red items in the menu. | Menus with no red or banned foods and beverages, menus with >50% of green items, % of amber, and green items. |
| Yoong et al.; 2019. | Cluster RCT; food service multistrategy intervention. | School (childcare centers) | Australia | 28 childcare centers (IG n = 15; CG n = 13), 395 students (IG n = 220; CG n = 175) and 28 cooks (IG n = 15; CG n = 13). | 2–5 y | 6 m | Dietary intake ✓x | ↑ Vegetables (servings), ↑ whole grain cereals (servings), ↑ meat/meat alternatives (servings). | Fruit (servings), dairy/dairy alternatives (servings). |
| Yoong et al., 2020. | Cluster RCT; web-based menu-planning intervention. | School (childcare centers) | Australia | 35 childcare centers (IG/CG n = N/A) and 220 children for baseline dietary data observation (IG n = 112; CG n = 108). | 2–6 y | 12 m | Dietary intake ✓x | ↑ Fruit (servings), ↑ dairy and alternatives (servings); ↓ cereals and bread (servings), ↓ discretionary foods (unhealthy) (times consumed). | Vegetables (servings), meat and alternatives (servings). |
| Bell et al.; 2014. | Non-RCT; implementation intervention. | School (childcare centers) | Australia | 431 childcare centers (IG n = 240; CG n = 191) and 153 children (IG n = 79; CG n = 74). | 3–6 y | 20 m (+ 5-m follow-up) | Food availability x | ↑ Vegetable (servings); ↓ high-fat/salt/sugar food (items), ↓sweetened beverages (items); ↓ fruit (servings). | ‒ |
| Bogart et al.; 2011. | Pilot non-RCT; obesity-prevention and peer leader advocacy intervention. | School | USA | 2 middle schools (IG n = 1; CG n = 1) and 399 students (IG/CG n = N/A). | ±13 y | 5 w | Food purchase ✓ | ↑ Fruits (% students served); ↑ healthy entrées (% students served). | ‒ |
| Dietary intake x | ‒ | Soda (%students drink), sports/fruit drinks (% students drink). | |||||||
| Burgess-Champoux et al.; 2008. | Pilot non-RCT; multicomponent school-based intervention. | School | USA | 2 schools (IG n = 1; CG n = 1) and 150 parent/child pairs (IG n = 67; CG n = 83). | ±10 y | 3 m | Dietary intake ✓x | ↑ WG (servings), ↑ fiber (g); ↓ RG (servings). | Energy (kcal). |
| Geaney et al.; 2016. | Cluster non-RCT; 4-arm workplace-based intervention. | Workplace | Ireland | 4 workplaces (Education IG-A n = 1; Environment IG-B n = 1; Combined IG-C n = 1; CG n = 1) and 517 employees (Education IG-A n = 107; Environment IG-B n = 71; Combined IG-C n = 272; CG n = 67). | 18–64 y | ±7 9 months (intervention+ follow-up) | Dietary intake ✓x | ↓ Salt (g) (IG-C), ↓ saturated fat (g/day for IG-A, IG-C, and %E for IG-B, IG-C), ↓ total sugars (g) (IG-B). | Salt intake (g) (IG-A, IG-B), total energy (kcal), total fat (g/day and %E), saturated fat (g) (IG-B), %E saturated fat (IG-A), total sugars (g) (IG-A, IG-C), fiber (g) (IG-A, IG-B, IG-C). |
| Quinn et al.; 2018. | Non-RCT; behavioral economics-based choice architecture intervention. | School | USA | 11 schools (IG n = 6; CG n = 5) and 2245 students (IG n = 1026; CG n = 1219). | 11–18 y | 7 m | Dietary intake x (among students who selected) | ↑ proportion students consuming fruit (including juice), ↑ fruit items consumed (excluding juice), ↑ vegetables items consumed (including potatoes) in favor of the CG. | Proportion students consuming: fruit (including/excluding juice), vegetables (including/excluding potatoes), low-fat milk; mean number of: fruit (including/excluding juice), vegetables (including/excluding potatoes), low-fat milk. |
| Food purchase ✓x | ↑ proportion students selecting fruit (including/excluding juice); ↑ fruit items (including/excluding juice). | Proportion students selecting: vegetables (including/excluding potatoes), low-fat milk; mean number of: vegetables (including/excluding potatoes), low-fat milk. | |||||||
| Williams et al.; 2002. | Cluster non-RCT; 3-arm nutrition education and food service intervention. | School (childcare centers) | USA | 9 childcare centers (nutrition education IG-A n = 3; safety education IG-B n = 3; CG n = 3) and 1296 students (IG/CG n = N/A). | 2–5 y | 20 m | Dietary intake ✓x (results of IG-A and IG-B are presented together) | ↓ Saturated fat (g), ↓ fat and saturated fat (% kcal), ↑ iron (mg), ↑ magnesium (mg). | Fat (g), kcal, cholesterol (mg), protein (g), fiber (g), calcium (mg), zinc (mg), Vitamin A and Folic Acid and Vitamin B12 (microgram), Vitamin E and C (mg), riboflavin (mg). |
| Setting | Studies | Outcome Categories | |||||
|---|---|---|---|---|---|---|---|
| Food Availability | Dietary Intake | Food Purchase | |||||
| Consumer-Based Strategies | Establishment-Based Strategies | Consumer-Based Strategies | Establishment-Based Strategies | Consumer-Based Strategies | Establishment-Based Strategies | ||
| School | Anderson et al.; 2005. | ✓x a, b, c | ✓x d | ||||
| Bogart et al.; 2014. | ✓x a, b, c | ✓x d, h, i, k | |||||
| Cohen et al.; 2014. | ✓x e, f, g | ||||||
| Cohen et al., 2015. | ✓x (IG-A, C) x (IG-B) IG-A: d, f, g; IG-B and IG-C: d, f, g, i | ✓x (IG-A, B, C) d, f, g, i | |||||
| Delaney et al.; 2017. | ✓x d, i, h, k | ||||||
| Grady et al., 2020 | ✓x e | ||||||
| Habib-Mourad et al.; 2014. | ✓x a, b, c | ✓x d | ✓x a, b, c | ✓x d | |||
| Haerens et al.; 2006 | ✓x (girls), x (boys) IG-A, B: a, b IG-A: c | ✓x (girls), x (boys) IG-A, B: d, e, f, g, h | |||||
| Kenney et al.; 2015. | ✓x a | ✓x d | |||||
| Morshed et al.; 2016. | ✓x a, b, c | ✓x d, e, f, g, k | |||||
| Nathan et al.; 2016. | ✓ c | ✓ d, e, f, g, h, j | |||||
| Ochoa-Avilés et al.; 2017. | ✓x a, b, c | ✓x e, f | |||||
| Rosmawati et al.; 2017. | ✓x e, f, g | ||||||
| Seward et al.; 2017. | ✓ d, f, g, h | ✓x d, f, g, h | |||||
| Siega-Riz et al.; 2011. | ✓x a, b, c | ✓x d | |||||
| Souza et al.; 2013. | x e, f | x e, f | |||||
| Story et al.; 2003. | ✓x e, f, g, j | ||||||
| Taylor et al.; 2017. | ✓x a, b, c | ✓x d, e, j | x a, b, c | x d, e, j | |||
| Warren et al.; 2003. | x IG-A and C: a, b, c; IG-B: b, c | x IG-A, B, C: j | |||||
| Wolfenden et al.; 2017. | ✓ c | ✓ d, e, f, g, h, j | ✓x c | ✓x d, e, f, g, h, j | |||
| Wyse et al.; 2019. | x g, i | ||||||
| Yoong et al.; 2016. | ✓x d, e, g, h | ||||||
| Yoong et al.; 2019. | ✓x e, f, g, h | ||||||
| Yoong et al., 2020. | ✓x e, f, g, h | ||||||
| Bell et al.; 2014. | x a, c | x e, f, g, h, j | |||||
| Bogart et al.; 2011. | x a, b | x d, f, i, j | ✓ a, b | ✓ d, f, i, j | |||
| Burgess-Champoux et al.; 2008. | ✓x a, b, c | ✓x d, f, g, h | |||||
| Quinn et al.; 2018. | x d, e, f, g, i, j | ✓x d, e, f, g, i, j | |||||
| Williams et al.; 2002. | ✓x IG-A, B: d, f | ||||||
| Community | Ayala et al.; 2017. | x a | x d, f, g, h, i | ||||
| Beets et al.; 2016. | x d, f, g | ||||||
| Giles et al.; 2012 | ✓x c | ✓x d, e, f, g, h, j | |||||
| Lee et al.; 2018. | ✓ a, b, c | ✓ d, e, f, g, h, j | |||||
| Martínez-Donate et al.; 2015. | x a, b | x d, g, i | x a, b | x d, g, i | |||
| Muzaffar et al.; 2019. | ✓x a, b | ✓x e, j | |||||
| Trude et al.; 2018. | ✓x a, b, c | ✓x f, i, j | ✓x a, b, c | ✓x f, i, j | |||
| Wolfenden et al.; 2015. | ✓x a | ✓x d, e, f, g, h, i, j, l | ✓ a | ✓ d, e, f, g, h, i, j, l | |||
| Workplace | Lassen et al.; 2010. | ✓x a, b | ✓x d, e, f | ||||
| Thorndike et al.; 2016. | x(IG-A), ✓(IG-B) IG-A and B: a | ✓(IG-B) IG-B: l | |||||
| Webb et al.; 2011. | ✓x a | ✓x i, k | |||||
| Geaney et al.; 2016. | ✓x (IG-A, B, C) IG-A and C: a, b | ✓x (IG-A, B, C) IG-A: g, k; IG-B: d, g, i, l; IG-C: d, g, i, k, l | |||||
| Setting | Outcome Categories | ||
|---|---|---|---|
| Food Availability | Dietary Intake | Food Purchase | |
| School | The involvement of the students’ families, as a consumer-based strategy, together with the application of multiple establishment-based strategies, seemed to be effective in improving food availability in the school setting. | The application of consumer-based strategies together with the implementation of a menu with healthier options and limitation of the unhealthier ones, applied alone or in combination with other establishment-based strategies, seemed to be effective in improving dietary intake in the school setting. On the other hand, the provision of monetary incentives/rewards/recognition for the participating school canteen was not effective. | The application of consumer-based strategies together with the implementation of a menu with healthier options and limitation of the unhealthier ones, applied alone or in combination with other establishment-based strategies, seemed to be effective in improving food purchases in the school setting. |
| Community | No recommendation can be provided about both consumer- and establishment-based strategies. | The application of consumer-based strategies, together with establishment-based strategies such as the provision of monetary incentives/rewards/recognition for the participating restaurant or canteen, seemed to be effective in improving dietary intake in the community setting. | The application of multiple establishment-based strategies, including monetary incentives/rewards/recognition for the participating restaurant or canteen, seemed to be effective in improving food purchases in the community setting. |
| Workplace | Outcome not evaluated. | The application of consumer-based strategies together with the implementation of a menu with healthier options and limitation of the unhealthier ones, as an establishment-based strategy, seemed to be effective in improving dietary intake in the workplace setting; however more evidence is needed. | No recommendation can be provided about both consumer- and establishment-based strategies. |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Mandracchia, F.; Tarro, L.; Llauradó, E.; Valls, R.M.; Solà, R. Interventions to Promote Healthy Meals in Full-Service Restaurants and Canteens: A Systematic Review and Meta-Analysis. Nutrients 2021, 13, 1350. https://doi.org/10.3390/nu13041350
Mandracchia F, Tarro L, Llauradó E, Valls RM, Solà R. Interventions to Promote Healthy Meals in Full-Service Restaurants and Canteens: A Systematic Review and Meta-Analysis. Nutrients. 2021; 13(4):1350. https://doi.org/10.3390/nu13041350
Chicago/Turabian StyleMandracchia, Floriana, Lucia Tarro, Elisabet Llauradó, Rosa Maria Valls, and Rosa Solà. 2021. "Interventions to Promote Healthy Meals in Full-Service Restaurants and Canteens: A Systematic Review and Meta-Analysis" Nutrients 13, no. 4: 1350. https://doi.org/10.3390/nu13041350
APA StyleMandracchia, F., Tarro, L., Llauradó, E., Valls, R. M., & Solà, R. (2021). Interventions to Promote Healthy Meals in Full-Service Restaurants and Canteens: A Systematic Review and Meta-Analysis. Nutrients, 13(4), 1350. https://doi.org/10.3390/nu13041350






