The Role of Vitamin D in Early Knee Osteoarthritis and Its Relationship with Their Physical and Psychological Status
Abstract
:1. Introduction
2. Materials and Methods
2.1. Study Design
2.2. Participants
2.3. Outcome Measures
2.3.1. Vitamin D and Parathyroid Hormone Levels
2.3.2. Pain and Disability Variables
Pain Intensity
Western Ontario and McMaster Universities Osteoarthritis Index (WOMAC)
2.3.3. Functional Variables
Five-Time Sit to Stand
Walking Speed
2.3.4. Psychological Variables
Anxiety and Depression Symptoms
Social Participation
2.4. Procedures
2.5. Statistical Analysis
3. Results
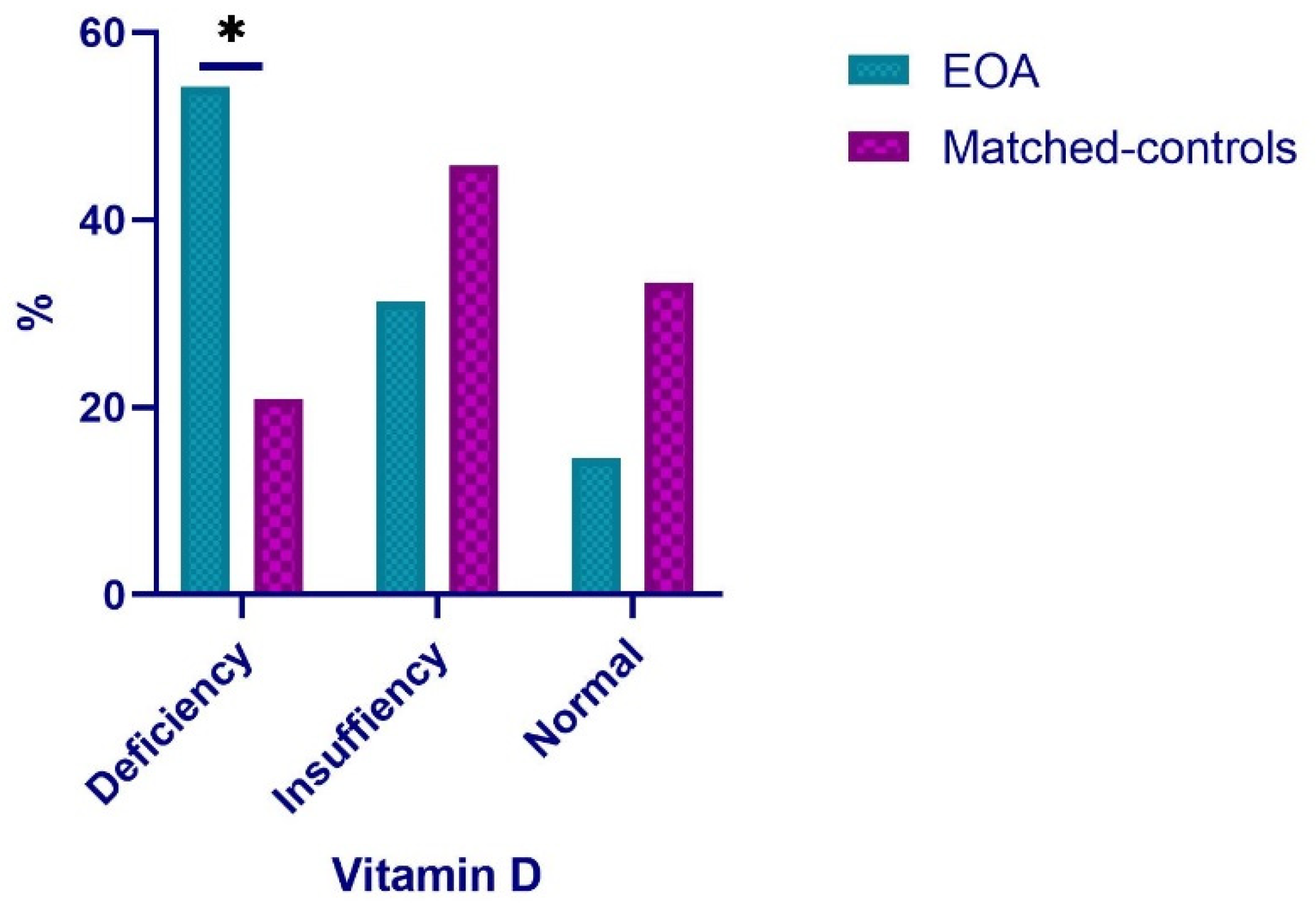
3.1. Vitamin D and PTH Levels
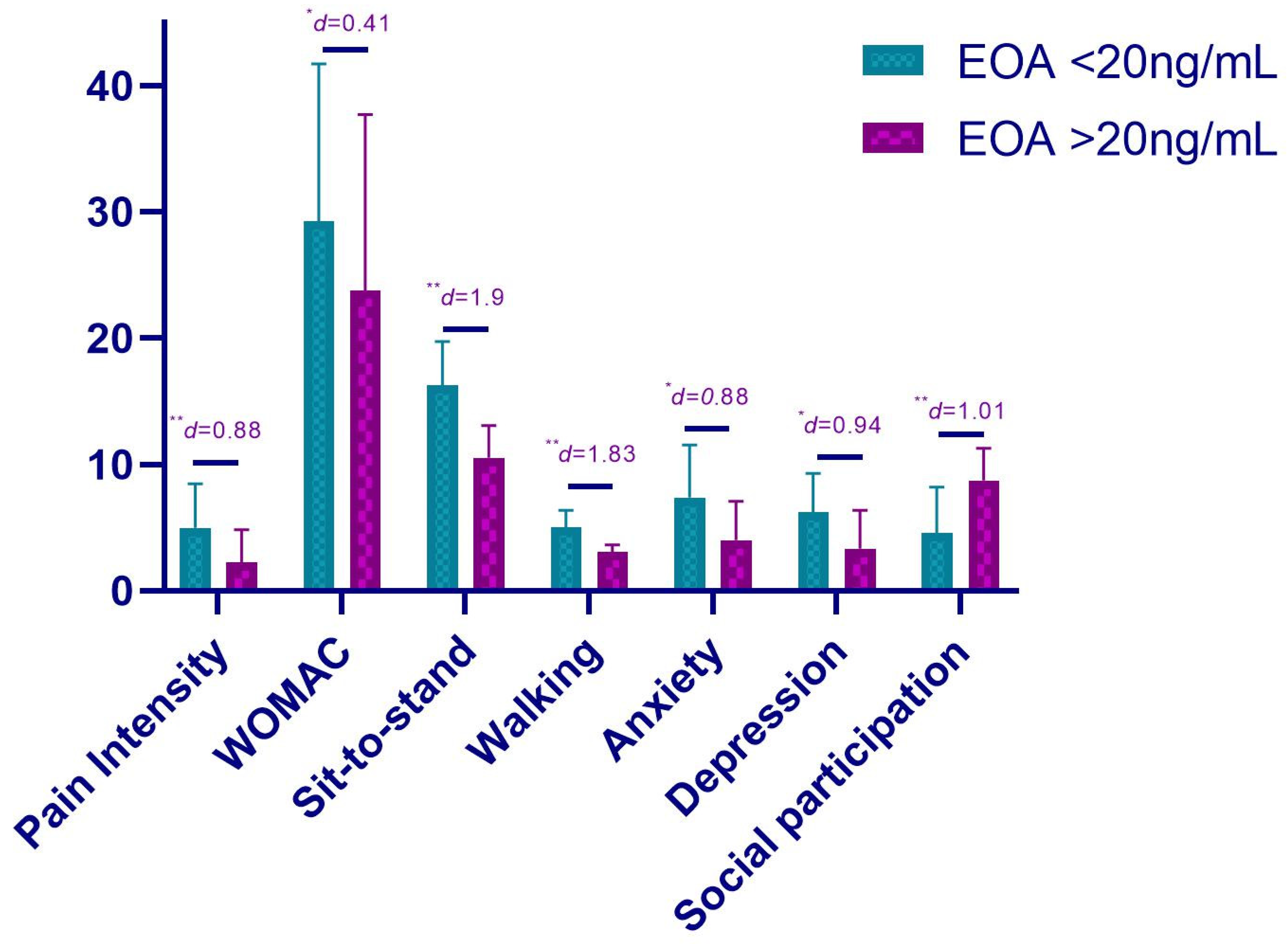
3.2. Physical and Psychological Status
3.3. Correlation Analysis
4. Discussion
Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Conflicts of Interest
References
- Vos, T.; Flaxman, A.D.; Naghavi, M.; Lozano, R.; Michaud, C.; Ezzati, M.; Shibuya, K.; Salomon, J.A.; Abdalla, S.; Aboyans, V.; et al. Years Lived with Disability (YLDs) for 1160 Sequelae of 289 Diseases and Injuries 1990-2010: A Systematic Analysis for the Global Burden of Disease Study 2010. Lancet 2012, 380, 2163–2196. [Google Scholar] [CrossRef]
- Mora, J.C.; Przkora, R.; Cruz-Almeida, Y. Knee Osteoarthritis: Pathophysiology and Current Treatment Modalities. J. Pain Res. 2018, 11, 2189. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Salaffi, F.; Carotti, M.; Stancati, A.; Grassi, W. Health-Related Quality of Life in Older Adults with Symptomatic Hip and Knee Osteoarthritis: A Comparison with Matched Healthy Controls. Aging Clin. Exp. Res. 2005, 17, 255–263. [Google Scholar] [CrossRef]
- Chiba, D.; Nakamura, T.; Fu, F.H. Early Osteoarthritis—Definition, Pathogenesis, Diagnosis, Management and Prevention: Management. Ann. Jt. 2019, 4, 5. [Google Scholar] [CrossRef]
- Neogi, T.; Zhang, Y. Osteoarthritis Prevention. Curr. Opin. Rheumatol. 2011, 23, 185–191. [Google Scholar] [CrossRef] [Green Version]
- Favero, M.; Ramonda, R.; Goldring, M.B.; Goldring, S.R.; Punzi, L. Early Knee Osteoarthritis. RMD Open 2015, 1, e000062. [Google Scholar] [CrossRef] [PubMed]
- Holick, M.F.; Chen, T. Vitamin D Deficiency: A Worldwide Problem with Health Consequences. Am. J. Clin. Nutr. 2008, 87, 1080S–1086S. [Google Scholar] [CrossRef] [Green Version]
- Cashman, K.D.; Dowling, K.G.; Škrabáková, Z.; Gonzalez-Gross, M.; Valtueña, J.; De Henauw, S.; Moreno, L.; Damsgaard, C.T.; Michaelsen, K.F.; Mølgaard, C.; et al. Vitamin D Deficiency in Europe: Pandemic? Am. J. Clin. Nutr. 2016, 103, 1033–1044. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- McAlindon, T.; LaValley, M.; Schneider, E.; Nuite, M.; Lee, J.Y.; Price, L.L.; Lo, G.; Dawson-Hughes, B. Effect of Vitamin D Supplementation on Progression of Knee Pain and Cartilage Volume Loss in Patients With Symptomatic Osteoarthritis: A Randomized Controlled Trial. JAMA 2013, 309, 155–162. [Google Scholar] [CrossRef] [Green Version]
- Souberbielle, J.-C.; Brazier, F.; Piketty, M.-L.; Cormier, C.; Minisola, S.; Cavalier, E. How the Reference Values for Serum Parathyroid Hormone Concentration Are (or Should Be) Established? J. Endocrinol. Investig. 2016, 40, 241–256. [Google Scholar] [CrossRef]
- Anderson, P.H.; Turner, A.G.; Morris, H.A. Vitamin D Actions to Regulate Calcium and Skeletal Homeostasis. Clin. Biochem. 2012, 45, 880–886. [Google Scholar] [CrossRef] [PubMed]
- Mabey, T.; Honsawek, S. Role of Vitamin D in Osteoarthritis: Molecular, Cellular, and Clinical Perspectives. Int. J. Endocrinol. 2015, 2015, 383918. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Park, C.Y. Vitamin D in the Prevention and Treatment of Osteoarthritis: From Clinical Interventions to Cellular Evidence. Nutrients 2019, 11, 243. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Holick, M.F. High Prevalence of Vitamin D Inadequacy and Implications for Health. Mayo Clin. Proc. 2006, 81, 353–373. [Google Scholar] [CrossRef] [Green Version]
- Antony, B.; Ding, C. Vitamin D and Osteoarthritis: Disparity between Observational Studies and Clinical Trials. Int. J. Rheum. Dis. 2017, 20, 671–674. [Google Scholar] [CrossRef]
- Yu, Y.; Liu, D.; Feng, D.; Zhao, J. Association between Vitamin D and Knee Osteoarthritis: A PRISMA-Compliant Meta-Analysis. Z. Fur Orthop. Und Unf. 2021, 159, 281–287. [Google Scholar] [CrossRef]
- Hussain, S.; Singh, A.; Akhtar, M.; Najmi, A.K. Vitamin D Supplementation for the Management of Knee Osteoarthritis: A Systematic Review of Randomized Controlled Trials. Rheumatol. Int. 2017, 37, 1489–1498. [Google Scholar] [CrossRef]
- Felson, D.T.; Hodgson, R. Identifying and Treating Preclinical and Early Osteoarthritis. Rheum. Dis. Clin. N. Am. 2014, 40, 699–710. [Google Scholar] [CrossRef] [Green Version]
- Neogi, T.; Bowes, M.A.; Niu, J.; De Souza, K.M.; Vincent, G.R.; Goggins, J.; Zhang, Y.; Felson, D.T. Magnetic Resonance Imaging-Based Three-Dimensional Bone Shape of the Knee Predicts Onset of Knee Osteoarthritis: Data from the Osteoarthritis Initiative. Arthritis Rheum. 2013, 65, 2048–2058. [Google Scholar] [CrossRef] [Green Version]
- Madry, H.; Kon, E.; Condello, V.; Peretti, G.M.; Steinwachs, M.; Seil, R.; Berruto, M.; Engebretsen, L.; Filardo, G.; Angele, P. Early Osteoarthritis of the Knee. Knee Surg. Sports Traumatol. Arthrosc. 2016, 24, 1753–1762. [Google Scholar] [CrossRef]
- Wu, Z.; Malihi, Z.; Stewart, A.W.; Lawes, C.M.M.; Scragg, R. The Association between Vitamin D Concentration and Pain: A Systematic Review and Meta-Analysis. Public Health Nutr. 2018, 21, 2022–2037. [Google Scholar] [CrossRef] [PubMed]
- Cakar, M.; Ayanoglu, S.; Cabuk, H.; Seyran, M.; Dedeoglu, S.S.; Gurbuz, H. Association between Vitamin D Concentrations and Knee Pain in Patients with Osteoarthritis. PeerJ 2018, 6, e4670. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Javadian, Y.; Adabi, M.; Heidari, B.; Babaei, M.; Firouzjahi, A.; Ghahhari, B.Y.; Hajian-Tilaki, K. Quadriceps Muscle Strength Correlates With Serum Vitamin D and Knee Pain in Knee Osteoarthritis. Clin. J. Pain 2017, 33, 67–70. [Google Scholar] [CrossRef] [PubMed]
- Muraki, S.; Dennison, E.; Jameson, K.; Boucher, B.J.; Akune, T.; Yoshimura, N.; Judge, A.; Arden, N.K.; Javaid, K.; Cooper, C. Association of Vitamin D Status with Knee Pain and Radiographic Knee Osteoarthritis. Osteoarthr. Cartil. 2011, 19, 1301–1306. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Tague, S.E.; Clarke, G.L.; Winter, M.K.; McCarson, K.E.; Wright, D.E.; Smith, P.G. Vitamin D Deficiency Promotes Skeletal Muscle Hypersensitivity and Sensory Hyperinnervation. J. Neurosci. Off. J. Soc. Neurosci. 2011, 31, 13728–13738. [Google Scholar] [CrossRef]
- von Känel, R.; Müller-Hartmannsgruber, V.; Kokinogenis, G.; Egloff, N. Vitamin D and Central Hypersensitivity in Patients with Chronic Pain. Pain Med. 2014, 15, 1609–1618. [Google Scholar] [CrossRef] [Green Version]
- Roesel, T.R. Does the Central Nervous System Play a Role in Vitamin D Deficiency-Related Chronic Pain? Pain 2009, 143, 159–160. [Google Scholar] [CrossRef]
- Cantorna, M.T.; Humpal-Winter, J.; DeLuca, H.F. In Vivo Upregulation of Interleukin-4 Is One Mechanism Underlying the Immunoregulatory Effects of 1,25-Dihydroxyvitamin D(3). Arch. Biochem. Biophys. 2000, 377, 135–138. [Google Scholar] [CrossRef]
- Amer, M.; Qayyum, R. Relation between Serum 25-Hydroxyvitamin D and C-Reactive Protein in Asymptomatic Adults (from the Continuous National Health and Nutrition Examination Survey 2001 to 2006). Am. J. Cardiol. 2012, 109, 226–230. [Google Scholar] [CrossRef]
- Sun, Q.; Zhen, G.; Li, T.P.; Guo, Q.; Li, Y.; Su, W.; Xue, P.; Wang, X.; Wan, M.; Guan, Y.; et al. Parathyroid Hormone Attenuates Osteoarthritis Pain by Remodeling Subchondral Bone in Mice. eLife 2021, 10, e66532. [Google Scholar] [CrossRef]
- Raja, S.N.; Carr, D.B.; Cohen, M.; Finnerup, N.B.; Flor, H.; Gibson, S.; Keefe, F.J.; Mogil, J.S.; Ringkamp, M.; Sluka, K.A.; et al. The Revised International Association for the Study of Pain Definition of Pain: Concepts, Challenges, and Compromises. Pain 2020, 161, 1976–1982. [Google Scholar] [CrossRef] [PubMed]
- Simpson, R.U.; Thomas, G.A.; Arnold, A.J. Identification of 1,25-Dihydroxyvitamin D3 Receptors and Activities in Muscle. J. Biol. Chem. 1985, 260, 8882–8891. [Google Scholar] [CrossRef]
- Wassner, S.J.; Li, J.B.; Sperduto, A.; Norman, M.E. Vitamin D Deficiency, Hypocalcemia, and Increased Skeletal Muscle Degradation in Rats. J. Clin. Investig. 1983, 72, 102–112. [Google Scholar] [CrossRef] [PubMed]
- Scragg, R.; Camargo, C.A.J. Frequency of Leisure-Time Physical Activity and Serum 25-Hydroxyvitamin D Levels in the US Population: Results from the Third National Health and Nutrition Examination Survey. Am. J. Epidemiol. 2008, 168, 577–591. [Google Scholar] [CrossRef] [Green Version]
- Bouassida, A.; Latiri, I.; Bouassida, S.; Zalleg, D.; Zaouali, M.; Feki, Y.; Gharbi, N.; Zbidi, A.; Tabka, Z. Parathyroid Hormone and Physical Exercise: A Brief Review. J. Sports Sci. Med. 2006, 5, 367–374. [Google Scholar]
- Brahm, H.; Piehl-Aulin, K.; Ljunghall, S. Bone Metabolism during Exercise and Recovery: The Influence of Plasma Volume and Physical Fitness. Calcif. Tissue Int. 1997, 61, 192–198. [Google Scholar] [CrossRef]
- Thorsen, K.; Kristoffersson, A.; Hultdin, J.; Lorentzon, R. Effects of Moderate Endurance Exercise on Calcium, Parathyroid Hormone, and Markers of Bone Metabolism in Young Women. Calcif. Tissue Int. 1997, 60, 16–20. [Google Scholar] [CrossRef]
- Maïmoun, L.; Manetta, J.; Couret, I.; Dupuy, A.M.; Mariano-Goulart, D.; Micallef, J.P.; Peruchon, E.; Rossi, M. The Intensity Level of Physical Exercise and the Bone Metabolism Response. Int. J. Sports Med. 2006, 27, 105–111. [Google Scholar] [CrossRef]
- Holick, M.F.; Binkley, N.C.; Bischoff-Ferrari, H.A.; Gordon, C.M.; Hanley, D.A.; Heaney, R.P.; Murad, M.H.; Weaver, C.M. Evaluation, Treatment, and Prevention of Vitamin D Deficiency: An Endocrine Society Clinical Practice Guideline. J. Clin. Endocrinol. Metab. 2011, 96, 1911–1930. [Google Scholar] [CrossRef] [Green Version]
- Knippenberg, S.; Damoiseaux, J.; Bol, Y.; Hupperts, R.; Taylor, B.V.; Ponsonby, A.-L.; Dwyer, T.; Simpson, S.; van der Mei, I.A.F. Higher Levels of Reported Sun Exposure, and Not Vitamin D Status, Are Associated with Less Depressive Symptoms and Fatigue in Multiple Sclerosis. Acta Neurol. Scand. 2014, 129, 123–131. [Google Scholar] [CrossRef]
- Lindström, M.; Hanson, B.S.; Östergren, P.-O. Socioeconomic Differences in Leisure-Time Physical Activity: The Role of Social Participation and Social Capital in Shaping Health Related Behaviour. Soc. Sci. Med. 2001, 52, 441–451. [Google Scholar] [CrossRef]
- Farr, J.N.; Going, S.B.; Lohman, T.G.; Rankin, L.; Kasle, S.; Cornett, M.; Cussler, E. Physical Activity Levels in Patients with Early Knee Osteoarthritis Measured by Accelerometry. Arthritis Care Res. 2008, 59, 1229–1236. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Wanner, M.; Richard, A.; Martin, B.; Linseisen, J.; Rohrmann, S. Associations between Objective and Self-Reported Physical Activity and Vitamin D Serum Levels in the US Population. Cancer Causes Control 2015, 26, 881–891. [Google Scholar] [CrossRef] [PubMed] [Green Version]
| Measures | EOA (n = 48) | Controls (n = 48) | p Value |
|---|---|---|---|
| Age (years) | 52.36 ± 5.02 | 50.72 ± 6.87 | 0.46 |
| BMI (kg/m2) | 26.98 ± 4.36 | 27.50 ± 3.89 | 0.43 |
| Gender | 0.17 | ||
| Women | 39 (81.3) | 43 (89.6) | |
| Men | 9 (18.7) | 5 (10.4) | |
| Economic status | 0.86 | ||
| Easy | 8 (16.7) | 3 (6.3) | |
| Fairly easy | 35 (72.9) | 38 (79.2) | |
| With some difficulties | 3 (6.2) | 7 (14.5) | |
| With great difficulties | 2 (4.2) | 0 (0) | |
| Alcohol | 0.65 | ||
| Never | 10 (22.2) | 8 (16.7) | |
| Seldom | 20 (41.7) | 18 (37.5) | |
| 1–2 times/month | 4 (8.3) | 8 (16.7) | |
| 1–2 times/week | 7 (14.3) | 12 (25) | |
| 1 time day | 5 (10.3) | 2 (4.1) | |
| More than 1 a day | 2 (4.1) | 0 (0) | |
| Smoking | 0.27 | ||
| Yes | 3 (6.25) | 6 (12.5) | |
| No | 10 (22.2) | 20 (41.7) | |
| Ex | 35 (72.9) | 22 (45.8) |
| Measures | EOA | Controls | Mean Difference (95% CI) | Effect Size (d) |
|---|---|---|---|---|
| Vitamin D (Serum 25(OH)D concentration) | 22.30 ± 7.3 | 29.31 ± 2.59 | −7.01 ** (−10.39 to −1.23) | 0.88 |
| PTH concentration | 40.78 ± 15.53 | 39.36 ± 14.76 | −1.42 (3.15 to −7.69) | - |
| Measures | EOA Deficiency (<20 ng/mL) | EOA Sufficiency (>20 ng/mL) | Mean Difference (95% CI) | Effect Size (d) |
|---|---|---|---|---|
| Pain intensity | 4.95 ± 3.52 | 2.22 ± 2.59 | 2.73 ** (−3.39 to −0.76) | 0.88 |
| WOMAC Total | 29.27 ± 12.45 | 23.76 ± 13.93 | 5.51 * (−14.65 to −6.64) | 0.41 |
| Sit-to-stand (s) | 16.29 ± 3.44 | 10.53 ± 2.54 | 5.76 ** (−6.34 to −0.81) | 1.90 |
| Walking speed (km/h) | 4.99 ± 1.38 | 3.07 ± 0.54 | 1.92 ** (−1.34 to −0.11) | 1.83 |
| Anxiety | 7.36 ± 4.17 | 4.01 ± 3.05 | 4.35 * (−3.86 to −2.15) | 0.88 |
| Depression | 6.21 ± 3.06 | 3.31 ± 3.06 | 2.9 * (−2.96 to −0.15) | 0.94 |
| Social participation | 4.57 ± 3.61 | 8.73 ± 2.55 | −4.16 ** (−2.82 to −1.14) | 1.01 |
| Vitamin D (Serum 25(OH)D Concentration) | PTH | |
|---|---|---|
| Pain intensity | −0.651 ** | −0.686 ** |
| WOMAC Total | −0.443 * | −0.234 |
| Anxiety | −0.623 ** | −0.153 |
| Depression | −0.351 * | −0.041 |
| Social participation | 0.355 * | 0.331 * |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Alabajos-Cea, A.; Herrero-Manley, L.; Suso-Martí, L.; Viosca-Herrero, E.; Cuenca-Martínez, F.; Varangot-Reille, C.; Blanco-Díaz, M.; Calatayud, J.; Casaña, J. The Role of Vitamin D in Early Knee Osteoarthritis and Its Relationship with Their Physical and Psychological Status. Nutrients 2021, 13, 4035. https://doi.org/10.3390/nu13114035
Alabajos-Cea A, Herrero-Manley L, Suso-Martí L, Viosca-Herrero E, Cuenca-Martínez F, Varangot-Reille C, Blanco-Díaz M, Calatayud J, Casaña J. The Role of Vitamin D in Early Knee Osteoarthritis and Its Relationship with Their Physical and Psychological Status. Nutrients. 2021; 13(11):4035. https://doi.org/10.3390/nu13114035
Chicago/Turabian StyleAlabajos-Cea, Ana, Luz Herrero-Manley, Luis Suso-Martí, Enrique Viosca-Herrero, Ferran Cuenca-Martínez, Clovis Varangot-Reille, María Blanco-Díaz, Joaquín Calatayud, and José Casaña. 2021. "The Role of Vitamin D in Early Knee Osteoarthritis and Its Relationship with Their Physical and Psychological Status" Nutrients 13, no. 11: 4035. https://doi.org/10.3390/nu13114035
APA StyleAlabajos-Cea, A., Herrero-Manley, L., Suso-Martí, L., Viosca-Herrero, E., Cuenca-Martínez, F., Varangot-Reille, C., Blanco-Díaz, M., Calatayud, J., & Casaña, J. (2021). The Role of Vitamin D in Early Knee Osteoarthritis and Its Relationship with Their Physical and Psychological Status. Nutrients, 13(11), 4035. https://doi.org/10.3390/nu13114035










