Emulsifiers Impact Colonic Length in Mice and Emulsifier Restriction is Feasible in People with Crohn’s Disease
Abstract
1. Introduction
2. Materials and Methods
2.1. Murine Study
2.2. Human Feasibility Study
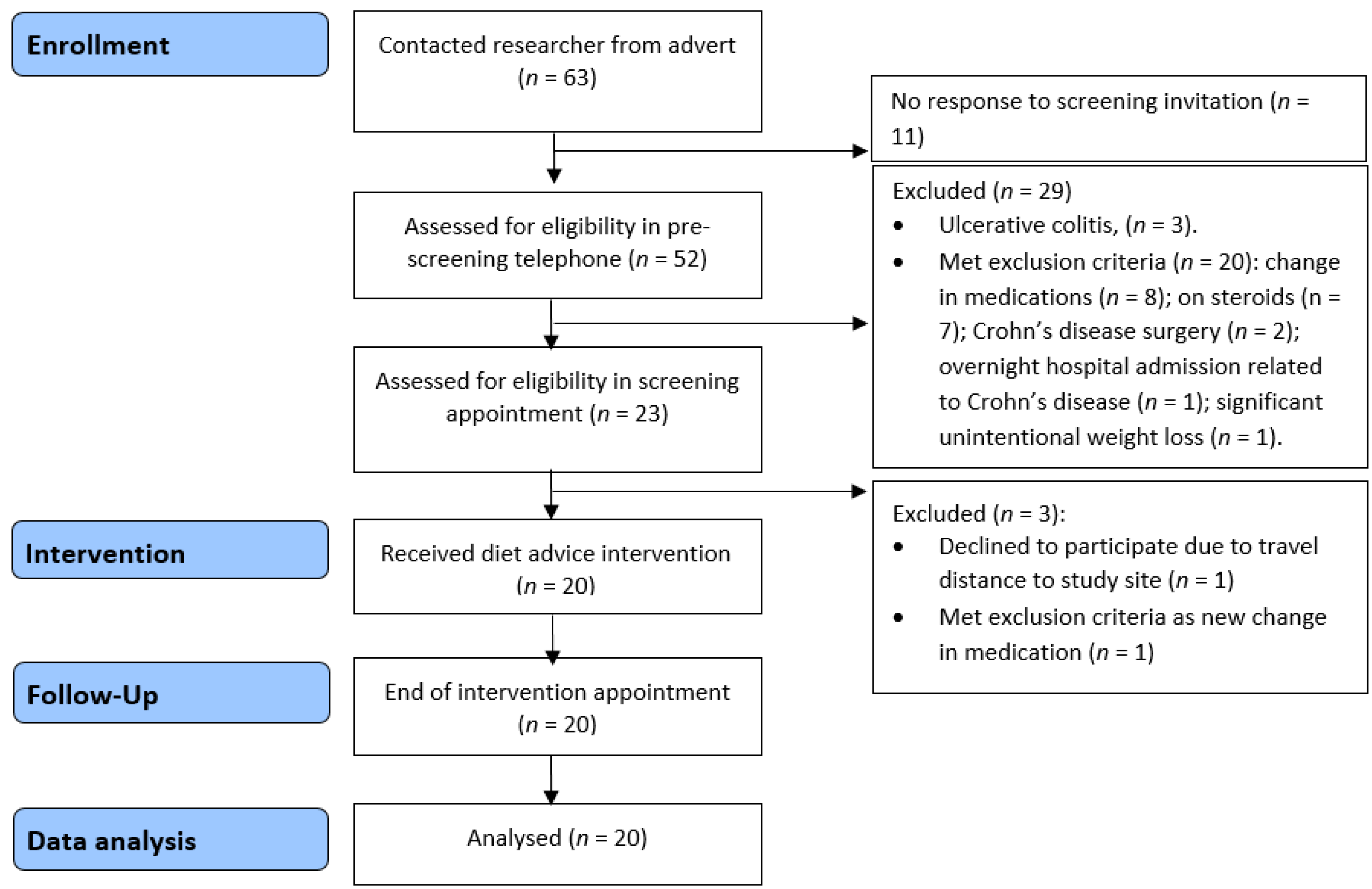
2.2.1. Study Design and Participants
2.2.2. Intervention
2.2.3. Outcome Measurement
2.3. Statistical Analysis
2.4. Ethical Considerations
3. Results
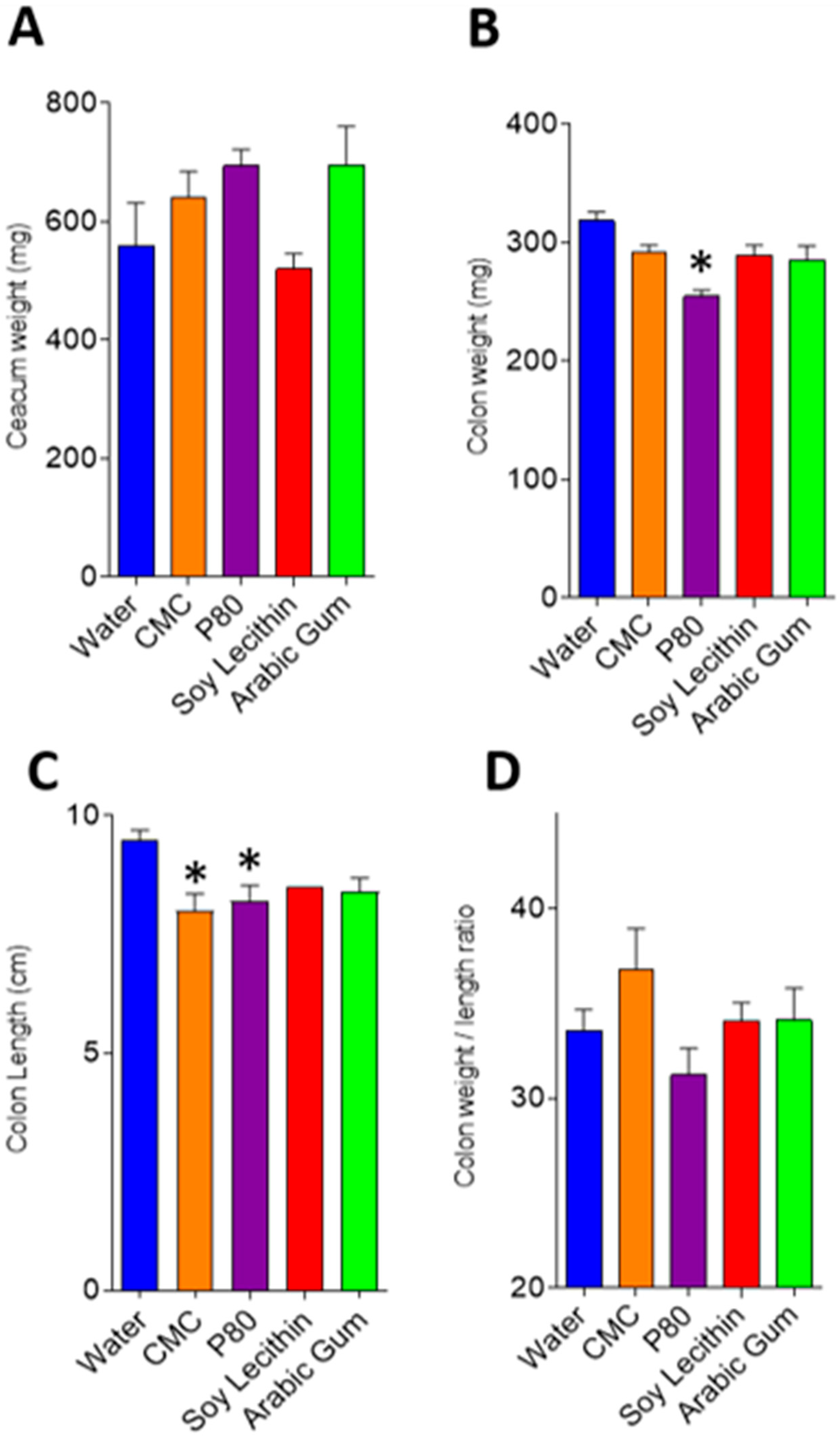
3.1. Murine Study
3.2. Feasibility Study
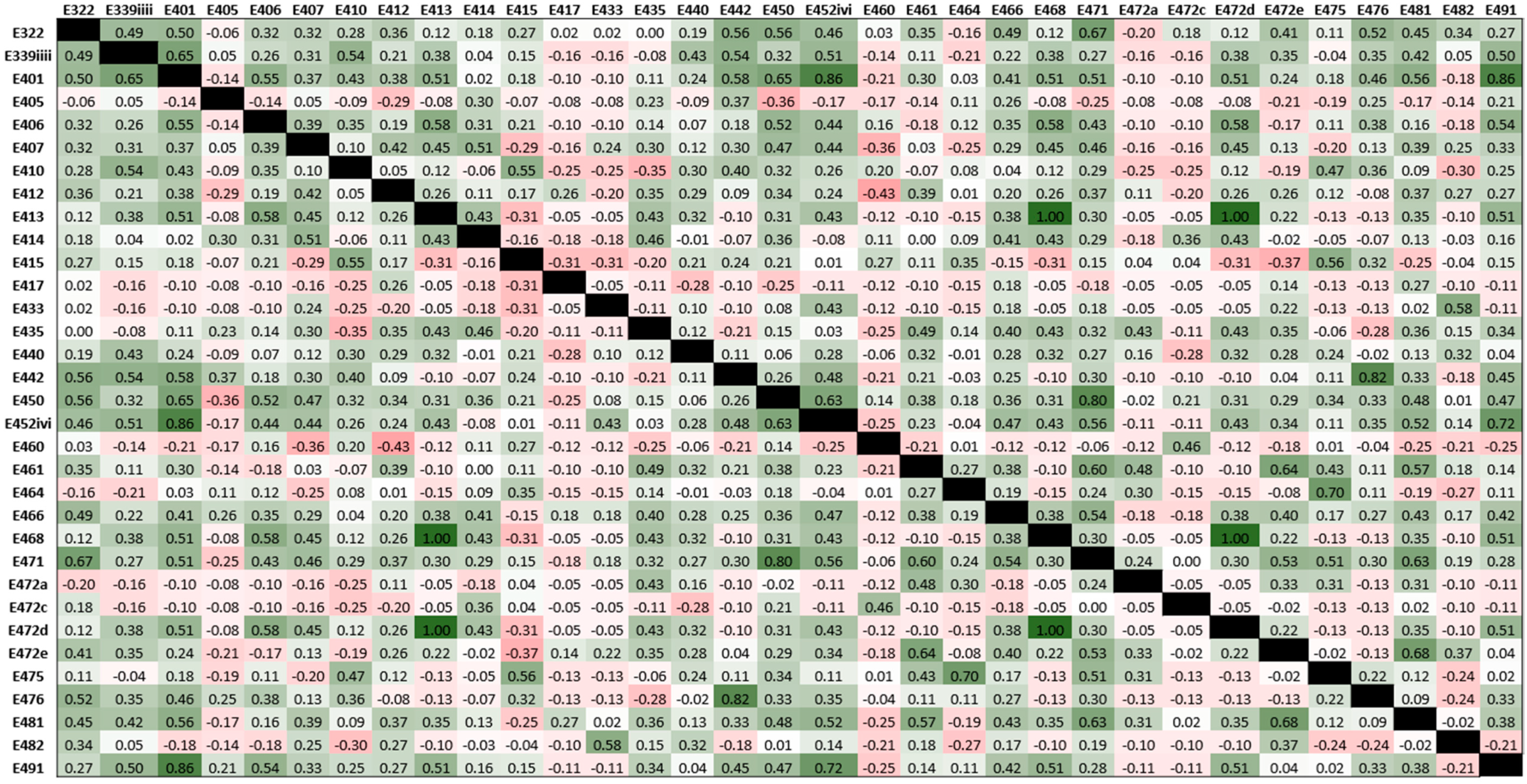
3.2.1. Emulsifier Exposure in Habitual Diet in Crohn’s Disease
3.2.2. Adherence to the Low Emulsifier Diet
3.2.3. Nutrient Intake, Anthropometry and Crohn’s Disease-Related Symptoms during Low Emulsifier Diet
3.2.4. Feasibility and Acceptability of the Low Emulsifier Diet
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Conflicts of Interest
References
- Ng, S.C.; Shi, H.Y.; Hamidi, N.; Underwood, F.E.; Tang, W.; Benchimol, E.I.; Panaccione, R.; Ghosh, S.; Wu, J.C.Y.; Chan, F.K.; et al. Worldwide incidence and prevalence of inflammatory bowel disease in the 21st century: A systematic review of population-based studies. Lancet 2018, 390, 2769–2778. [Google Scholar] [CrossRef]
- Molodecky, N.A.; Soon, I.S.; Rabi, D.M.; Ghali, W.A.; Ferris, M.; Chernoff, G.; Benchimol, E.I.; Panaccione, R.; Ghosh, S.; Barkema, H.W.; et al. Increasing incidence and prevalence of the inflammatory bowel diseases with time, based on systematic review. Gastroenterology 2012, 142, 46–54. [Google Scholar] [CrossRef]
- Piovani, D.; Danese, S.; Peyrin-Biroulet, L.; Nikolopoulos, G.K.; Lytras, T.; Bonovas, S. Environmental Risk Factors for Inflammatory Bowel Diseases: An Umbrella Review of Meta-analyses. Gastroenterology 2019, 157, 647–659.e4. [Google Scholar] [CrossRef] [PubMed]
- Roberts, C.L.; Rushworth, S.L.; Richman, E.; Rhodes, J.M. Hypothesis: Increased consumption of emulsifiers as an explanation for the rising incidence of Crohn’s disease. J. Crohn’s Colitis 2013, 7, 338–341. [Google Scholar] [CrossRef] [PubMed]
- Narula, N.; Dhillon, A.; Zhang, D.; Sherlock, M.E.; Tondeur, M.; Zachos, M. Enteral nutritional therapy for induction of remission in Crohn’s disease. Cochrane Database Syst. Rev. 2018, 4, CD000542. [Google Scholar] [CrossRef] [PubMed]
- Swaminath, A.; Feathers, A.; Ananthakrishnan, A.N.; Falzon, L.; Ferry, S.L. Systematic review with meta-analysis: Enteral nutrition therapy for the induction of remission in paediatric Crohn’s disease. Aliment. Pharmacol. Ther. 2017, 46, 645–656. [Google Scholar] [CrossRef]
- Levine, A.; Wine, E.; Assa, A.; Boneh, R.S.; Shaoul, R.; Kori, M.; Cohen, S.; Peleg, S.; Shamaly, H.; On, A.; et al. Crohn’s Disease Exclusion Diet Plus Partial Enteral Nutrition Induces Sustained Remission in a Randomized Controlled Trial. Gastroenterology 2019, 157, 440–450.e8. [Google Scholar] [CrossRef] [PubMed]
- Levine, A.; Boneh, R.S.; Wine, E. Evolving role of diet in the pathogenesis and treatment of inflammatory bowel diseases. Gut 2018, 67, 1726–1738. [Google Scholar] [CrossRef]
- Haskey, N.; Gibson, D.L. An Examination of Diet for the Maintenance of Remission in Inflammatory Bowel Disease. Nutrients 2017, 9, 259. [Google Scholar] [CrossRef] [PubMed]
- Riordan, A.M.; Ruxton, C.H.; Hunter, J.O. A review of associations between Crohn’s disease and consumption of sugars. Eur. J. Clin. Nutr. 1998, 52, 229–238. [Google Scholar] [CrossRef]
- Agus, A.; Denizot, J.; Thevenot, J.; Martinez-Medina, M.; Massier, S.; Sauvanet, P.; Bernalier-Donadille, A.; Denis, S.; Hofman, P.; Bonnet, R.; et al. Western diet induces a shift in microbiota composition enhancing susceptibility to Adherent-Invasive E. coli infection and intestinal inflammation. Sci. Rep. 2016, 6, 19032. [Google Scholar] [CrossRef] [PubMed]
- Martinez-Medina, M.; Denizot, J.; Dreux, N.; Robin, F.; Billard, E.; Bonnet, R.; Darfeuille-Michaud, A.; Barnich, N. Western diet induces dysbiosis with increased E coli in CEABAC10 mice, alters host barrier function favouring AIEC colonisation. Gut 2014, 63, 116–124. [Google Scholar] [CrossRef] [PubMed]
- Chassaing, B.; Koren, O.; Goodrich, J.K.; Poole, A.C.; Srinivasan, S.; Ley, R.E.; Gewirtz, A.T. Dietary emulsifiers impact the mouse gut microbiota promoting colitis and metabolic syndrome. Nature 2015, 519, 92–96. [Google Scholar] [CrossRef] [PubMed]
- McClements, D. Food Emulsions Principles, Practices and Techniques, 3rd ed.; Taylor & Francis Group: Boca Ranton, FL, USA, 2015. [Google Scholar]
- Garzon, R.; Hernando, I.; Llorca, E.; Rosell, C.M. Understanding the effect of emulsifiers on bread aeration during breadmaking. J. Sci. Food Agric. 2018, 98, 5494–5502. [Google Scholar] [CrossRef]
- Berton-Carabin, C.C.; Sagis, L.; Schroën, K. Formation, Structure, and Functionality of Interfacial Layers in Food Emulsions. Annu. Rev. Food Sci. Technol. 2018, 9, 551–587. [Google Scholar] [CrossRef]
- Dickinson, E. Hydrocolloids at interfaces and the influence on the properties of dispersed systems. Food Hydrocoll. 2003, 17, 25–39. [Google Scholar] [CrossRef]
- Roberts, C.L.; Keita, Å.V.; Duncan, S.H.; O’Kennedy, N.; Söderholm, J.D.; Rhodes, J.M.; Campbell, B.J. Translocation of Crohn’s disease Escherichia coli across M-cells: Contrasting effects of soluble plant fibres and emulsifiers. Gut 2010, 59, 1331–1339. [Google Scholar] [CrossRef]
- Fahoum, L.; Moscovici, A.M.; David, S.; Shaoul, R.; Rozen, G.; Meyron-Holtz, E.G.; Lesmes, U. Digestive fate of dietary carrageenan: Evidence of interference with digestive proteolysis and disruption of gut epithelial function. Mol. Nutr. Food Res. 2017, 61, 1600545. [Google Scholar] [CrossRef]
- Borthakur, A.; Bhattacharyya, S.; Dudeja, P.K.; Tobacman, J.K. Carrageenan induces interleukin-8 production through distinct Bcl10 pathway in normal human colonic epithelial cells. Am. J. Physiol. Gastrointest Liver Physiol. 2007, 292, G829–G838. [Google Scholar] [CrossRef]
- Bhattacharyya, S.; Gill, R.; Chen, M.L.; Zhang, F.; Linhardt, R.J.; Dudeja, P.K.; Tobacman, J.K. Toll-like receptor 4 mediates induction of the Bcl10-NFkappaB-interleukin-8 inflammatory pathway by carrageenan in human intestinal epithelial cells. J. Biol. Chem. 2008, 283, 10550–10558. [Google Scholar] [CrossRef]
- Choi, H.J.; Kim, J.; Park, S.H.; Do, K.H.; Yang, H.; Moon, Y. Pro-inflammatory NF-kappaB and early growth response gene 1 regulate epithelial barrier disruption by food additive carrageenan in human intestinal epithelial cells. Toxicol. Lett. 2012, 211, 289–295. [Google Scholar] [CrossRef] [PubMed]
- Borthakur, A.; Bhattacharyya, S.; Anbazhagan, A.N.; Kumar, A.; Dudeja, P.K.; Tobacman, J.K. Prolongation of carrageenan-induced inflammation in human colonic epithelial cells by activation of an NFkappaB-BCL10 loop. Biochim. Biophys. Acta 2012, 1822, 1300–1307. [Google Scholar] [CrossRef] [PubMed]
- Chassaing, B.; Van de Wiele, T.; De Bodt, J.; Marzorati, M.; Gewirtz, A.T. Dietary emulsifiers directly alter human microbiota composition and gene expression ex vivo potentiating intestinal inflammation. Gut 2017, 66, 1414–1427. [Google Scholar] [CrossRef] [PubMed]
- Sigall-Boneh, R.; Levine, A.; Lomer, M.; Wierdsma, N.; Allan, P.; Fiorino, G.; Gatti, S.; Jonkers, D.; Kierkuś, J.; Katsanos, K.H.; et al. Research Gaps in Diet and Nutrition in Inflammatory Bowel Disease. A Topical Review by D-ECCO Working Group [Dietitians of ECCO]. J. Crohn’s Colitis 2017, 11, 1407–1419. [Google Scholar] [CrossRef]
- Shah, R.; Kolanos, R.; DiNovi, M.J.; Mattia, A.; Kaneko, K.J. Dietary exposures for the safety assessment of seven emulsifiers commonly added to foods in the United States and implications for safety. Food Addit. Contam. Part A Chem. Anal. Control. Exp. Risk Assess 2017, 34, 905–917. [Google Scholar] [CrossRef]
- Bhattacharyya, S.; Shumard, T.; Xie, H.; Dodda, A.; Varady, K.A.; Feferman, L.; Halline, A.G.; Goldstein, J.L.; Hanauer, S.B.; Tobacman, J.K. A randomized trial of effects of the no-carrageenan diet on ulcerative colitis disease activity. Nutr. Healthy Aging 2017, 4, 181–192. [Google Scholar] [CrossRef]
- Sandall, A.M.; Wall, C.L.; Lomer, M.C.E. Nutrition Assessment in Crohn’s Disease using Anthropometric, Biochemical, and Dietary Indexes: A Narrative Review. J. Acad. Nutr. Diet. 2020, 120, 624–640. [Google Scholar] [CrossRef]
- Lancaster, G.A.; Dodd, S.; Williamson, P.R. Design and analysis of pilot studies: Recommendations for good practice. J. Eval. Clin. Pract. 2004, 10, 307–312. [Google Scholar] [CrossRef]
- Julious, S.A. Sample size of 12 per group rule of thumb for a pilot study. Pharm. Stat. 2005, 4, 287–291. [Google Scholar] [CrossRef]
- FAO & WHO. CODEX Alimentarius: International Food Standards; Class Names and the International Numbering System for Food Additives, Report No. CAC/GL 36-1989; FAO: Rome, Italy, 2017. [Google Scholar]
- Food Standards Agency. Approved Additives and E Numbers 2018 [Updated 1 March 2018]. Available online: https://www.food.gov.uk/business-guidance/approved-additives-and-e-numbers (accessed on 12 November 2018).
- Johnson, R.K. Dietary intake--how do we measure what people are really eating? Obes. Res. 2002, 10 (Suppl. S11), 63s. [Google Scholar] [CrossRef]
- The European Parliament and the Council of the European Union. Regulation (EC) No 1333/2008 of the European Parliament and of the Council of 16 December 2008 on Food Additives; The European Parliament and the Council of the European Union: Strasburg, France, 2008. [Google Scholar]
- Betts, J.A.; Chowdhury, E.A.; Gonzalez, J.T.; Richardson, J.D.; Tsintzas, K.; Thompson, D. Is breakfast the most important meal of the day? Proc. Nutr. Soc. 2016, 75, 464–474. [Google Scholar] [CrossRef] [PubMed]
- Leech, R.M.; Worsley, A.; Timperio, A.; McNaughton, S.A. Characterizing eating patterns: A comparison of eating occasion definitions. Am. J. Clin. Nutr. 2015, 102, 1229–1237. [Google Scholar] [CrossRef]
- McCance, R.A.; Widdowson, E.M. The Composition of Foods; Institute of Food Research (Great Britain) Public Health England, & Royal Society of Chemistry: London, UK, 2015. [Google Scholar]
- Public Health England (PHE). From Plate to Guide: What, Why and How for the Eatwell Model; PHE publication number: 2016451; Public Health England: London, UK, 2016. [Google Scholar]
- Public Health England (PHE). Nutrient Reference Intakes. Government Dietary Recommendations: Government Recommendations for Energy and Nutrients for Males and Females Aged 1–18 Years and 19+ Years; PHE Publication Number: 2016202; Public Health England: London, UK, 2016. [Google Scholar]
- Department of Health. UK Chief Medical Officers’ Low Risk Drinking Guidelines; Department of Health: London, UK, 2016.
- British Society of Gastroenterology. Guidelines for Osteoporosis in Inflammatory Bowel Disease and Coeliac Disease; British Society of Gastroenterology: London, UK, 2007. [Google Scholar]
- Scientific Advisory Committee on Nutrition. Salt and Health; The Food Standards Agency and the Department of Health: London, UK, 2003. [Google Scholar]
- Madden, A.M.; Smith, S. Body composition and morphological assessment of nutritional status in adults: A review of anthropometric variables. J. Hum. Nutr. Diet. 2016, 29, 7–25. [Google Scholar] [CrossRef] [PubMed]
- Bangor, A.; Kortum, P.T.; Miller, J.T. An empirical evaluation of the System Usability Scale. Int. J. Hum. Comput. Interact. 2008, 24, 574–594. [Google Scholar] [CrossRef]
- Hughes, L.; King, L.; Morgan, M.; Ayis, S.; Direkze, N.; Lomer, M.; Lindsay, J.O.; Whelan, K. Food-related Quality of Life in Inflammatory Bowel Disease: Development and Validation of a Questionnaire. J. Crohn’s Colitis 2016, 10, 194–201. [Google Scholar] [CrossRef]
- Czuber-Dochan, W.; Morgan, M.; Hughes, L.D.; Lomer, M.C.E.; Lindsay, J.O.; Whelan, K. Perceptions and psychosocial impact of food, nutrition, eating and drinking in people with inflammatory bowel disease: A qualitative investigation of food-related quality of life. J. Hum. Nutr. Diet. 2020, 33, 115–127. [Google Scholar] [CrossRef]
- Khanna, R.; Zou, G.; D’Haens, G.; Feagan, B.G.; Sandborn, W.J.; Vandervoort, M.K.; Rolleri, R.L.; Bortey, E.; Paterson, C.; Forbes, W.P.; et al. A retrospective analysis: The development of patient reported outcome measures for the assessment of Crohn’s disease activity. Aliment. Pharmacol. Ther. 2015, 41, 77–86. [Google Scholar] [CrossRef]
- Bodger, K.; Ormerod, C.; Shackcloth, D.; Harrison, M.; Collaborative, I.B.D.C. Development and validation of a rapid, generic measure of disease control from the patient’s perspective: The IBD-control questionnaire. Gut 2014, 63, 1092–1102. [Google Scholar] [CrossRef]
- Main and Subsidiary Food Groups. National Diet and Nutrition Survey. In Diet and Nutrition Survey of Infants and Young Children; Appendix M; MRC Human Nutrition Research, Department of Health: London, UK, 2011. [Google Scholar]
- Csáki, K.F.; Sebestyén, É. Who will carry out the tests that would be necessary for proper safety evaluation of food emulsifiers? Food Sci. Hum. Wellness 2019, 8, 126–135. [Google Scholar] [CrossRef]
- Boneh, R.S.; Chermesh, I.; Ben-Avraham, S.; Boaz, M.; Levine, A.; Shabat, C.S.; Yanai, H. Dietary Therapy With the Crohn’s Disease Exclusion Diet is a Successful Strategy for Induction of Remission in Children and Adults Failing Biological Therapy. J. Crohn’s Colitis 2017, 11, 1205–1212. [Google Scholar] [CrossRef]
- Svolos, V.; Hansen, R.; Nichols, B.; Quince, C.; Ijaz, U.Z.; Papadopoulou, R.T.; Edwards, C.A.; Watson, D.; Alghamdi, A.I.S.; Brejnrod, A.; et al. Treatment of Active Crohn’s Disease With an Ordinary Food-based Diet That Replicates Exclusive Enteral Nutrition. Gastroenterology 2019, 156, 1354–1367.e6. [Google Scholar] [CrossRef] [PubMed]
- Lomer, M.C.; Gourgey, R.; Whelan, K. Current practice in relation to nutritional assessment and dietary management of enteral nutrition in adults with Crohn’s disease. J. Hum. Nutr. Diet. 2014, 27, 28–35. [Google Scholar] [CrossRef]
- Melmed, G.Y.; Targan, S.R. Future biologic targets for IBD: Potentials and pitfalls. Nat. Rev. Gastroenterol. Hepatol. 2010, 7, 110–117. [Google Scholar] [CrossRef]
- Staudacher, H.M.; Irving, P.M.; Lomer, M.C.E.; Whelan, K. The challenges of control groups, placebos and blinding in clinical trials of dietary interventions. Proc. Nutr. Soc. 2017, 76, 203–212. [Google Scholar] [CrossRef] [PubMed]
- Nazarenkov, N.; Seeger, K.; Beeken, L.; Ananthakrishnan, A.N.; Khalili, H.; Lewis, J.D.; Konijeti, G.G. Implementing Dietary Modifications and Assessing Nutritional Adequacy of Diets for Inflammatory Bowel Disease. Gastroenterol. Hepatol. (N Y) 2019, 15, 133–144. [Google Scholar]
- Opstelten, J.L.; de Vries, J.H.M.; Wools, A.; Siersema, P.D.; Oldenburg, B.; Witteman, B.J.M. Dietary intake of patients with inflammatory bowel disease: A comparison with individuals from a general population and associations with relapse. Clin. Nutr. 2019, 38, 1892–1898. [Google Scholar] [CrossRef]
- Weaver, C.M.; Dwyer, J.; Fulgoni, V.L., III; King, J.C.; Leveille, G.A.; MacDonald, R.S.; Ordovas, J.; Schnakenberg, D. Processed foods: Contributions to nutrition. Am. J. Clin. Nutr. 2014, 99, 1525–1542. [Google Scholar] [CrossRef] [PubMed]
- Lewis, J.D.; Abreu, M.T. Diet as a Trigger or Therapy for Inflammatory Bowel Diseases. Gastroenterology 2017, 152, 398–414.e6. [Google Scholar] [CrossRef]
- McCormick, N.M.L.J. The Specific Carbohydrate Diet in the Treatment of Crohn’s Disease: A Systematic Review. J. Gastroenterol. Hepatol. Res. 2017, 6, 2392–2399. [Google Scholar] [CrossRef]
- Bryant, R.V.; Trott, M.J.; Bartholomeusz, F.D.; Andrews, J.M. Systematic review: Body composition in adults with inflammatory bowel disease. Aliment. Pharmacol. Ther. 2013, 38, 213–225. [Google Scholar] [CrossRef]
- Limdi, J.K.; Aggarwal, D.; McLaughlin, J.T. Dietary Practices and Beliefs in Patients with Inflammatory Bowel Disease. Inflamm. Bowel. Dis. 2015, 22, 164–170. [Google Scholar] [CrossRef] [PubMed]
- Chan, W.; Chen, A.; Tiao, D.; Selinger, C.; Leong, R. Medication adherence in inflammatory bowel disease. Intest. Res. 2017, 15, 434–445. [Google Scholar] [CrossRef] [PubMed]
- Torres, J.; Ellul, P.; Langhorst, J.; Mikocka-Walus, A.; Acosta, M.B.-D.; Basnayake, C.; Ding, N.J.S.; Gilardi, D.; Katsanos, K.; Moser, G.; et al. European Crohn’s and Colitis Organisation Topical Review on Complementary Medicine and Psychotherapy in Inflammatory Bowel Disease. J. Crohn’s Colitis 2019, 13, 673–685e. [Google Scholar] [CrossRef] [PubMed]
- European Food Safety Authority. EFSA’s Activities on Emerging Risks in 2015; EFSA 2016: EN-1100; The European Union: Parma, Italy, 2015. [Google Scholar]


| Characteristic | N = 20 |
|---|---|
| Sex, n (%) | |
| Male | 6 (30) |
| Female | 14 (70) |
| Age (year), mean (SD), min–max | 34.9 (10.1), 23–62 |
| Smoking status, n (%) | |
| Current smoker | 0 (0) |
| Previous smoker | 3 (15) |
| Non-smoker | 17 (85) |
| Disease duration (year), mean (SD), min–max | 13.1 (10.8), 2–40 |
| Current medications, n (%) | |
| 5-aminosalicyclic acid | 3 (15) |
| Thiopurines | 10 (50) |
| Biologics | 8 (40) |
| Food Group 1 | Contribution to Baseline Emulsifier Intake, N/N (%) | Sub-Food Group Contribution, % |
|---|---|---|
| Cereal and cereal products | 177/422 (42%) | Bread (21%) |
| Biscuits, buns, cakes, pastries and fruit pies (17%) | ||
| Pasta, rice, breakfast cereals and other cereals (4%) | ||
| Sugars, preserves and confectionery | 83/422 (20%) | Chocolate confectionary (13%) |
| Preserves and sweet spreads (6%) | ||
| Sugar confectionary (1%) | ||
| Miscellaneous | 53/422 (13%) | Savoury sauces (6%) |
| Nutrition powders, drinks and protein bar supplements (6%) | ||
| Meat alternatives (1%) | ||
| Milk and milk products | 42/422 (10%) | Cheese (3%) |
| Ice-cream (3%) | ||
| Other/alternative milks (2%) | ||
| Yoghurt (1%) | ||
| Fat spreads | 26/422 (6%) | Low fat spreads, margarines and oil (6%) |
| Non-alcoholic beverages | 21/422 (5%) | Non-alcoholic beverages (5%) |
| Savoury snacks | 9/422 (2%) | Crisps and savoury snacks (2%) |
| Meat and meat products | 4/422 (1%) | Processed meat (1%) |
| Fish and fish dishes | 4/422 (1%) | Fish and fish dishes (1%) |
| Vegetables and potatoes | 3/422 (1%) | Processed potato products (1%) |
| Nutrient | Absolute Intakes, Median (IQR) | Meeting National Guidelines, N (%) | ||||
|---|---|---|---|---|---|---|
| Baseline | Low Emulsifier Diet | p-Value | Baseline | Low Emulsifier Diet | p-Value | |
| Energy (kcal/day) | 2055 (587) | 1855 (620) | 0.025 | - | - | |
| Carbohydrate 1 (g/day) | 187.0 (66.9) | 182.5 (61.8) | 0.048 | 0 (0) | 1 (5) | 1.000 |
| Fibre 2 (g/day) | 21.2 (11.1) | 21.9 (12.1) | 0.627 | 4 (20) | 5 (25) | 1.000 |
| Total sugar (g/day) | 63.6 (48.9) | 65.7 (31.2) | 0.126 | - | - | - |
| Free sugars 1 (g/day) | 27.0 (15.0) | 24.8 (25.2) | 0.351 | 7 (35) | 8 (40) | 1.000 |
| Protein 3 (g/day) | 81.5 (35.1) | 75.3 (47.9) | 0.079 | 19 (95) | 18 (90) | 1.000 |
| Fat 1 (g/day) | 89.6 (21.1) | 79.6 (45.3) | 0.067 | 5 (25) | 3 (15) | 0.688 |
| Saturated fat 1 (g/day) | 31.2 (12.7) | 25.0 (14.8) | 0.048 | 5 (25) | 5 (25) | 1.000 |
| Alcohol 4 (g/day) | 7.8 (19.2) | 0.7 (10.7) | 0.016 | 14 (70) | 17 (85) | 0.375 |
| Calcium 2 (mg/day) | 813 (483) | 744 (178) | 0.015 | 13 (65) | 12 (60) | 1.000 |
| Iron 2 (mg/day) | 12.7 (5.7) | 13.5 (4.9) | 0.550 | 11 (55) | 9 (45) | 0.625 |
| Zinc 2 (mg/day) | 10.1 (4.3) | 9.3 (4.7) | 0.391 | 16 (80) | 15 (75) | 1.000 |
| Sodium 5 (mg/day) | 2465 (1276) | 1991 (1295) | 0.028 | 9 (45) | 12 (60) | 0.508 |
| Potassium 2 (mg/day) | 2813 (1392) | 3287 (1141) | 0.370 | 7 (35) | 8 (40) | 1.000 |
| Chloride (mg/day) | 3509 (1541) | 3288 (1711) | 0.052 | - | - | - |
| Phosphorus 2 (mg/day) | 1306 (465) | 1247 (547) | 0.313 | 20 (100) | 20 (100) | N/A |
| Magnesium 2 (mg/day) | 320 (128) | 356 (166) | 0.823 | 15 (75) | 14 (70) | 1.000 |
| Iodine 2 (µg/day) | 102 (70) | 81 (64) | 0.313 | 3 (15) | 2 (10) | 1.000 |
| Selenium 2 (µg/day) | 55.4 (37.7) | 55.0 (41.9) | 0.313 | 8 (40) | 6 (30) | 0.625 |
| Copper 2 (mg/day) | 1.29 (1.32) | 1.35 (1.05) | 0.502 | 12 (60) | 14 (70) | 0.688 |
| Manganese (mg/day) | 3.8 (1.9) | 3.9 (1.7) | 0.179 | - | - | - |
| Vitamin A 2 (µg/day) | 794 (611) | 948 (687) | 0.391 | 14 (70) | 16 (80) | 0.688 |
| Vitamin B1 2 (Thiamine) (mg/day) | 1.50 (0.78) | 1.46 (0.70) | 0.433 | 20 (100) | 19 (95) | 1.000 |
| Vitamin B2 2 (Riboflavin) (mg/day) | 1.49 (0.71) | 1.45 (0.82) | 0.627 | 17 (85) | 16 (80) | 1.000 |
| Vitamin B3 2 (Niacin) (mg/day) | 36.7 (14.8) | 33.0 (19.6) | 0.021 | 20 (100) | 20 (100) | N/A |
| Vitamin B5 (Pantothenic acid) (mg/day) | 5.51 (3.47) | 5.24 (3.16) | 0.794 | - | - | - |
| Vitamin B6 2 (Pyridoxine) (mg/day) | 1.55 (0.94) | 1.73 (0.60) | 0.911 | 18 (90) | 17 (85) | 1.000 |
| Vitamin B7 (Biotin) (µg/day) | 41.8 (23.7) | 34.6 (23.0) | 0.167 | - | - | - |
| Vitamin B9 2 (Folate) (µg/day) | 241.3 (123.3) | 247.3 (117.6) | 0.627 | 15 (75) | 14 (70) | 1.000 |
| Vitamin B12 2 (Cobalamin) (µg/day) | 4.98 (3.75) | 4.09 (2.86) | 0.021 | 20 (100) | 20 (100) | N/A |
| Vitamin C 2 (mg/day) | 74.6 (91.2) | 87.2 (80.9) | 0.433 | 15 (75) | 17 (85) | 0.625 |
| Vitamin D 2 (µg/day) | 3.3 (2.5) | 3.2 (4.1) | 0.737 | 2 (10) | 0 (0) | 0.500 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Sandall, A.M.; Cox, S.R.; Lindsay, J.O.; Gewirtz, A.T.; Chassaing, B.; Rossi, M.; Whelan, K. Emulsifiers Impact Colonic Length in Mice and Emulsifier Restriction is Feasible in People with Crohn’s Disease. Nutrients 2020, 12, 2827. https://doi.org/10.3390/nu12092827
Sandall AM, Cox SR, Lindsay JO, Gewirtz AT, Chassaing B, Rossi M, Whelan K. Emulsifiers Impact Colonic Length in Mice and Emulsifier Restriction is Feasible in People with Crohn’s Disease. Nutrients. 2020; 12(9):2827. https://doi.org/10.3390/nu12092827
Chicago/Turabian StyleSandall, Alicia M., Selina R. Cox, James O. Lindsay, Andrew T. Gewirtz, Benoit Chassaing, Megan Rossi, and Kevin Whelan. 2020. "Emulsifiers Impact Colonic Length in Mice and Emulsifier Restriction is Feasible in People with Crohn’s Disease" Nutrients 12, no. 9: 2827. https://doi.org/10.3390/nu12092827
APA StyleSandall, A. M., Cox, S. R., Lindsay, J. O., Gewirtz, A. T., Chassaing, B., Rossi, M., & Whelan, K. (2020). Emulsifiers Impact Colonic Length in Mice and Emulsifier Restriction is Feasible in People with Crohn’s Disease. Nutrients, 12(9), 2827. https://doi.org/10.3390/nu12092827






