Dietary Fiber, Gut Microbiota, and Metabolic Regulation—Current Status in Human Randomized Trials
Abstract
1. Introduction
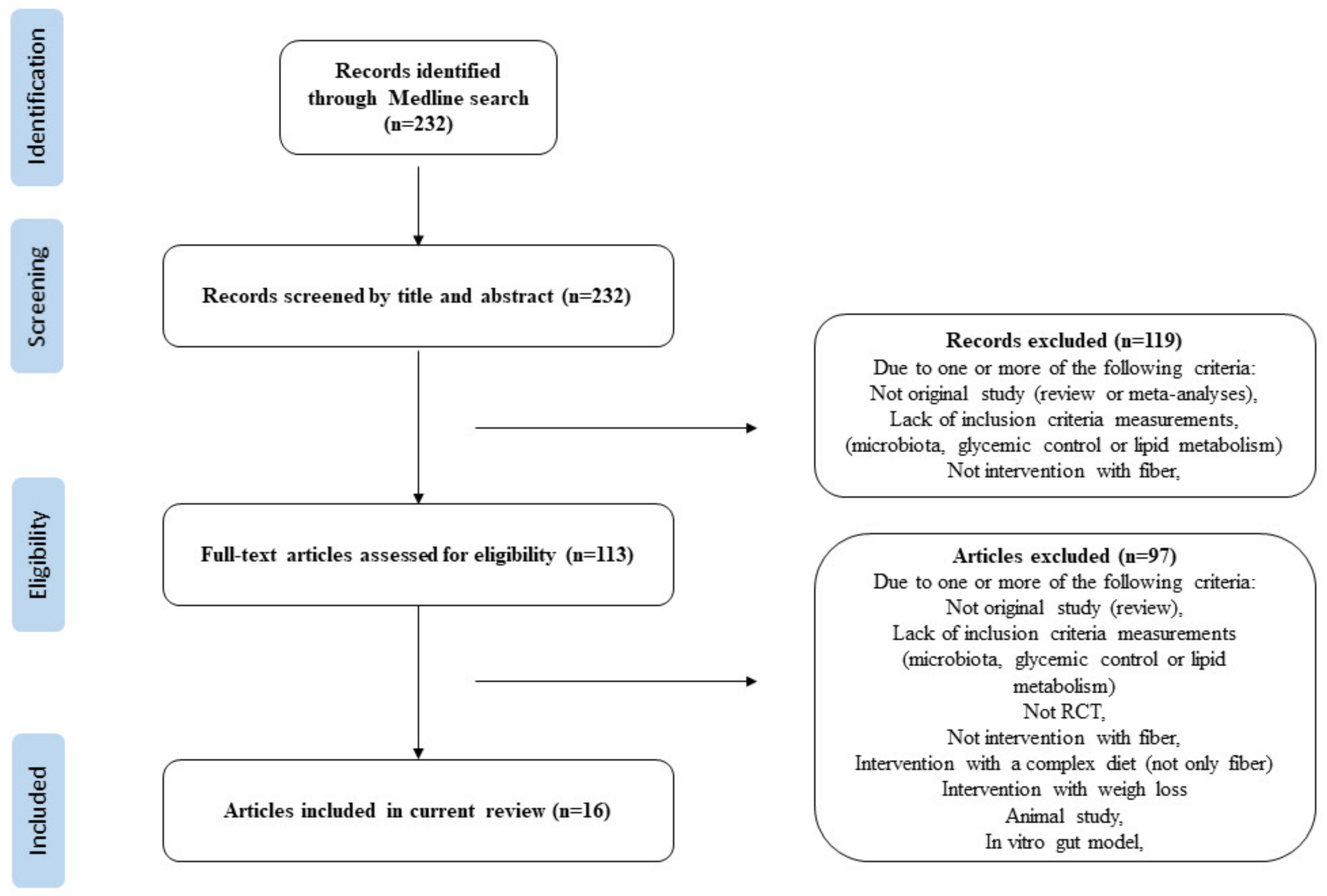
2. Materials and Methods
3. Results
3.1. Healthy Normal-Weight Individuals
3.2. Overweight and Obese Individuals
3.3. Individuals with Metabolic Related Disorders
4. Discussion
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- World Helth Organization. The Top 10 Causes of Death; WHO: Geneva, Switzerland, 2018. [Google Scholar]
- Collaborators GBDD. Health effects of dietary risks in 195 countries, 1990-2017: A systematic analysis for the Global Burden of Disease Study 2017. Lancet 2019, 393, 1958–1972. [Google Scholar] [CrossRef]
- Forouzanfar, M.H.; Afshin, A.; Alexander, L.T.; Anderson, H.R.; Bhutta, Z.A.; Biryukov, S.; Brauer, M.; Burnett, R.; Cercy, K.; Charlson, F.; et al. Global, regional, and national comparative risk assessment of 79 behavioural, environmental and occupational, and metabolic risks or clusters of risks, 1990–2015: A systematic analysis for the Global Burden of Disease Study 2015. Lancet 2016, 388, 1659–1724. [Google Scholar] [CrossRef]
- De Munter, J.S.L.; Hu, F.B.; Spiegelman, N.; Franz, M.; Van Dam, R.M. Whole Grain, Bran, and Germ Intake and Risk of Type 2 Diabetes: A Prospective Cohort Study and Systematic Review. PLoS Med. 2007, 4, e261. [Google Scholar] [CrossRef] [PubMed]
- Schulz, M.; Heidemann, C.; Schulze, M.B.; Schienkiewitz, A.; Hoffmann, K.; Boeing, H. Fiber and Magnesium Intake and Incidence of Type 2 Diabetes. Arch. Intern. Med. 2007, 167, 956–965. [Google Scholar] [CrossRef] [PubMed]
- Anderson, J.W.; Baird, P.; Davis, R.H., Jr.; Ferreri, S.; Knudtson, M.; Koraym, A.; Waters, V.; Williams, C.L. Health benefits of dietary fiber. Nutr. Rev. 2009, 67, 188–205. [Google Scholar] [CrossRef]
- Makki, K.; Deehan, E.C.; Walter, J.; Bäckhed, F. The Impact of Dietary Fiber on Gut Microbiota in Host Health and Disease. Cell Host Microbe 2018, 23, 705–715. [Google Scholar] [CrossRef]
- Cornejo-Pareja, I.; Muñoz-Garach, A.; Clemente-Postigo, M.; Tinahones, F.J. Importance of gut microbiota in obesity. Eur. J. Clin. Nutr. 2018, 72, 26–37. [Google Scholar] [CrossRef]
- Blander, J.M.; Longman, R.S.; Iliev, I.D.; Sonnenberg, G.F.; Artis, D. Regulation of inflammation by microbiota interactions with the host. Nat. Immunol. 2017, 18, 851–860. [Google Scholar] [CrossRef]
- Jie, Z.; Xia, H.; Zhong, S.-L.; Feng, Q.; Li, S.; Liang, S.; Zhong, H.; Liu, Z.; Gao, Y.; Zhao, H.; et al. The gut microbiome in atherosclerotic cardiovascular disease. Nat. Commun. 2017, 8, 845. [Google Scholar] [CrossRef]
- Tilg, H.; Moschen, A. Microbiota and diabetes: An evolving relationship. Gut 2014, 63, 1513–1521. [Google Scholar] [CrossRef]
- Barko, P.; McMichael, M.; Swanson, K.; Williams, D. The Gastrointestinal Microbiome: A Review. J. Vet. Intern. Med. 2017, 32, 9–25. [Google Scholar] [CrossRef] [PubMed]
- Sekirov, I.; Russell, S.L.; Antunes, L.C.M.; Finlay, B.B. Gut Microbiota in Health and Disease. Physiol. Rev. 2010, 90, 859–904. [Google Scholar] [CrossRef] [PubMed]
- Guarner, F.; Malagelada, J.-R. Gut flora in health and disease. Lancet 2003, 361, 512–519. [Google Scholar] [CrossRef]
- Rinninella, E.; Raoul, P.; Cintoni, M.; Franceschi, F.; Miggiano, G.A.D.; Gasbarrini, A.; Mele, M.C. What is the Healthy Gut Microbiota Composition? A Changing Ecosystem across Age, Environment, Diet, and Diseases. Microorganisms 2019, 7, 14. [Google Scholar] [CrossRef]
- Underwood, M.A. Intestinal dysbiosis: Novel mechanisms by which gut microbes trigger and prevent disease. Prev. Med. 2014, 65, 133–137. [Google Scholar] [CrossRef]
- Lin, L.; Zhang, J. Role of intestinal microbiota and metabolites on gut homeostasis and human diseases. BMC Immunol. 2017, 18, 2. [Google Scholar] [CrossRef]
- Ley, R.E.; Turnbaugh, P.J.; Klein, S.; Gordon, J.I. Human gut microbes associated with obesity. Nature 2006, 444, 1022–1023. [Google Scholar] [CrossRef]
- Koh, A.; De Vadder, F.; Kovatcheva-Datchary, P.; Bäckhed, F. From Dietary Fiber to Host Physiology: Short-Chain Fatty Acids as Key Bacterial Metabolites. Cell 2016, 165, 1332–1345. [Google Scholar] [CrossRef]
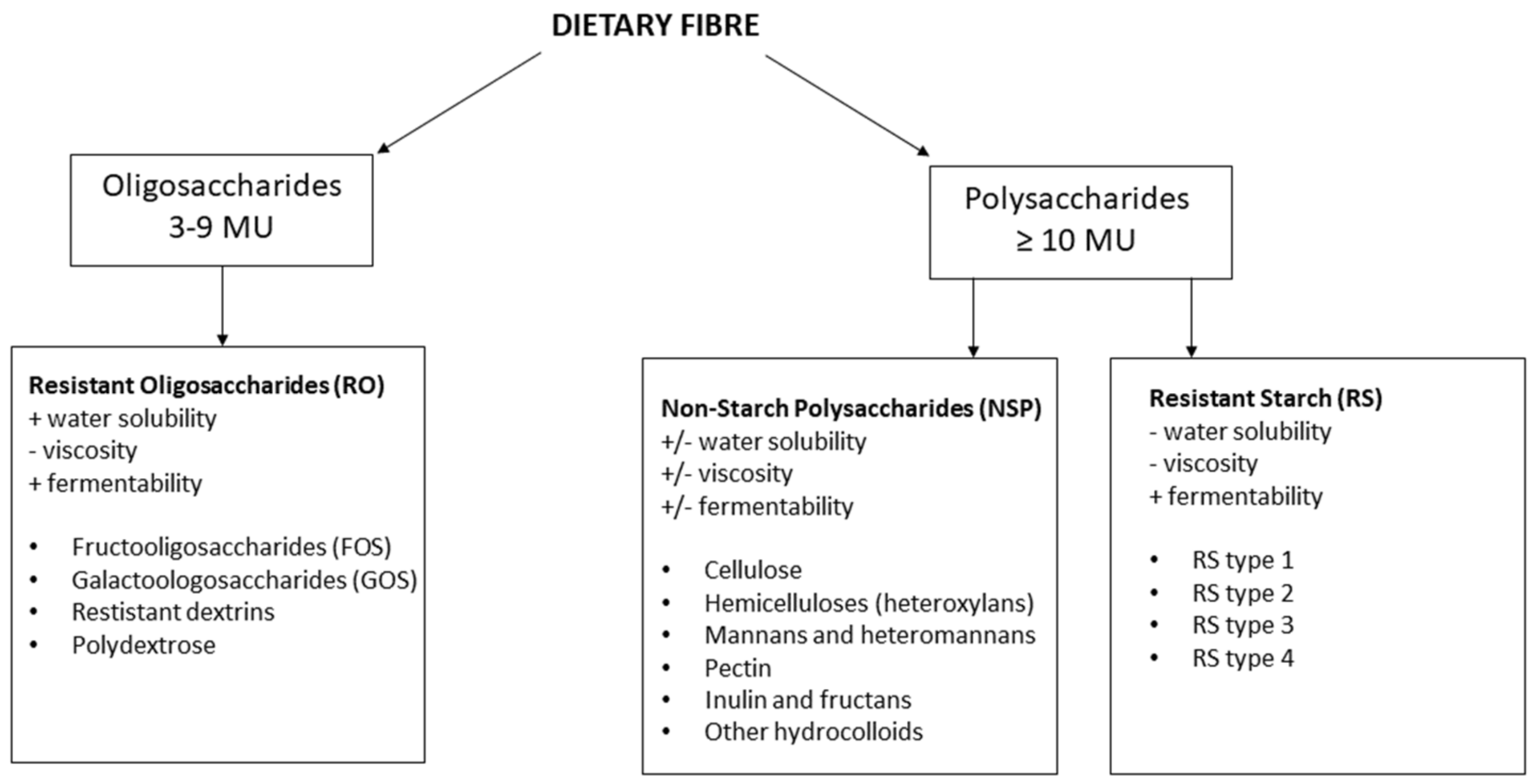
- Dhingra, D.; Michael, M.; Rajput, H.; Patil, R.T. Dietary fibre in foods: A review. J. Food Sci. Technol. 2011, 49, 255–266. [Google Scholar] [CrossRef]
- Stephen, A.M.; Champ, M.M.-J.; Cloran, S.J.; Fleith, M.; Van Lieshout, L.; Mejborn, H.; Burley, V. Dietary fibre in Europe: Current state of knowledge on definitions, sources, recommendations, intakes and relationships to health. Nutr. Res. Rev. 2017, 30, 149–190. [Google Scholar] [CrossRef]
- Jones, J.M. CODEX-aligned dietary fiber definitions help to bridge the ‘fiber gap’. Nutr. J. 2014, 13, 34. [Google Scholar] [CrossRef] [PubMed]
- Le Poul, E.; Loison, C.; Lannoy, V.; Brézillon, S.; Dupriez, V.; Vassart, G.; Parmentier, M.; Detheux, M.; Struyf, S.; Springael, J.-Y.; et al. Functional Characterization of Human Receptors for Short Chain Fatty Acids and Their Role in Polymorphonuclear Cell Activation. J. Boil. Chem. 2003, 278, 25481–25489. [Google Scholar] [CrossRef] [PubMed]
- Canfora, E.E.; Jocken, J.W.; Blaak, E.E. Short-chain fatty acids in control of body weight and insulin sensitivity. Nat. Rev. Endocrinol. 2015, 11, 577–591. [Google Scholar] [CrossRef] [PubMed]
- Morrison, D.J.; Preston, T. Formation of short chain fatty acids by the gut microbiota and their impact on human metabolism. Gut Microbes 2016, 7, 189–200. [Google Scholar] [CrossRef]
- Hong, Y.-H.; Nishimura, Y.; Hishikawa, D.; Tsuzuki, H.; Miyahara, H.; Gotoh, C.; Choi, K.-C.; Feng, D.D.; Chen, C.; Lee, H.-G.; et al. Acetate and Propionate Short Chain Fatty Acids Stimulate Adipogenesis via GPCR43. Endocrinology 2005, 146, 5092–5099. [Google Scholar] [CrossRef]
- Liu, H.; Wang, J.; He, T.; Becker, S.; Zhang, G.; Li, D.; Ma, X. Butyrate: A Double-Edged Sword for Health? Adv. Nutr. 2018, 9, 21–29. [Google Scholar] [CrossRef]
- Knudsen, K.E.; Lærke, H.N.; Hedemann, M.S.; Nielsen, T.S.; Ingerslev, A.K.; Nielsen, D.S.G.; Theil, P.K.; Purup, S.; Hald, S.; Schioldan, A.G.; et al. Impact of Diet-Modulated Butyrate Production on Intestinal Barrier Function and Inflammation. Nutrients 2018, 10, 1499. [Google Scholar] [CrossRef]
- Tuomainen, M.; Lindstrom, J.; Lehtonen, M.; Auriola, S.; Pihlajamäki, J.; Peltonen, M.; Tuomilehto, J.; Uusitupa, M.; De Mello, V.D.; Hanhineva, K. Associations of serum indolepropionic acid, a gut microbiota metabolite, with type 2 diabetes and low-grade inflammation in high-risk individuals. Nutr. Diabetes 2018, 8, 35. [Google Scholar] [CrossRef]
- Sun, Q.; Wedick, N.M.; Pan, A.; Townsend, M.K.; Cassidy, A.; Franke, A.A.; Rimm, E.B.; Hu, F.B.; van Dam, R.M. Gut Microbiota Metabolites of Dietary Lignans and Risk of Type 2 Diabetes: A Prospective Investigation in Two Cohorts of U.S. Women. Diabetes Care 2014, 37, 1287–1295. [Google Scholar] [CrossRef]
- Sandberg, J.C.; Kovatcheva-Datchary, P.; Björck, I.; Bäckhed, F.; Nilsson, A.C. Abundance of gut Prevotella at baseline and metabolic response to barley prebiotics. Eur. J. Nutr. 2018, 58, 2365–2376. [Google Scholar] [CrossRef]
- Kovatcheva-Datchary, P.; Nilsson, A.C.; Akrami, R.; Lee, Y.S.; De Vadder, F.; Arora, T.; Hallén, A.; Martens, E.; Björck, I.; Bäckhed, F. Dietary Fiber-Induced Improvement in Glucose Metabolism Is Associated with Increased Abundance of Prevotella. Cell Metab. 2015, 22, 971–982. [Google Scholar] [CrossRef] [PubMed]
- Vanegas, S.M.; Meydani, M.; Barnett, J.B.; Goldin, B.; Kane, A.; Rasmussen, H.; Brown, C.; Vangay, P.; Knights, D.; Jonnalagadda, S.; et al. Substituting whole grains for refined grains in a 6-wk randomized trial has a modest effect on gut microbiota and immune and inflammatory markers of healthy adults. Am. J. Clin. Nutr. 2017, 105, 635–650. [Google Scholar] [CrossRef] [PubMed]
- Costabile, A.; Klinder, A.; Fava, F.; Napolitano, A.; Fogliano, V.; Leonard, C.; Gibson, G.R.; Tuohy, K. Whole-grain wheat breakfast cereal has a prebiotic effect on the human gut microbiota: A double-blind, placebo-controlled, crossover study. Br. J. Nutr. 2007, 99, 110–120. [Google Scholar] [CrossRef] [PubMed]
- Costabile, A.; Bergillos-Meca, T.; Rasinkangas, P.; Korpela, K.; de Vos, W.M.; Gibson, G.R. Effects of Soluble Corn Fiber Alone or in Synbiotic Combination with Lactobacillus rhamnosus GG and the Pilus-Deficient Derivative GG-PB12 on Fecal Microbiota, Metabolism, and Markers of Immune Function: A Randomized, Double-Blind, Placebo-Controlled, Crossover Study in Healthy Elderly (Saimes Study). Front. Immunol. 2017, 8, 1443. [Google Scholar] [PubMed]
- Kjølbæk, L.; Benítez-Páez, A.; del Pulgar, E.M.G.; Brahe, L.K.; Liebisch, G.; Matysik, S.; Rampelli, S.; Vermeiren, J.; Brigidi, P.; Larsen, L.H.; et al. Arabinoxylan oligosaccharides and polyunsaturated fatty acid effects on gut microbiota and metabolic markers in overweight individuals with signs of metabolic syndrome: A randomized cross-over trial. Clin. Nutr. 2019, 39, 67–79. [Google Scholar] [CrossRef] [PubMed]
- Canfora, E.E.; Van Der Beek, C.M.; Hermes, G.D.; Goossens, G.H.; Jocken, J.W.; Holst, J.J.; Van Eijk, H.M.; Venema, K.; Smidt, H.; Zoetendal, E.G.; et al. Supplementation of Diet With Galacto-oligosaccharides Increases Bifidobacteria, but Not Insulin Sensitivity, in Obese Prediabetic Individuals. Gastroenterology 2017, 153, 87–97. [Google Scholar] [CrossRef]
- Chambers, E.; Byrne, C.S.; Morrison, D.J.; Murphy, K.G.; Preston, T.; Tedford, M.; Garcia-Perez, I.; Fountana, S.; Serrano-Contreras, J.I.; Holmes, E.; et al. Dietary supplementation with inulin-propionate ester or inulin improves insulin sensitivity in adults with overweight and obesity with distinct effects on the gut microbiota, plasma metabolome and systemic inflammatory responses: A randomised cross-over trial. Gut 2019, 68, 1430–1438. [Google Scholar]
- Schutte, S.; Esser, D.; Hoevenaars, F.P.M.; Hooiveld, G.J.; Priebe, M.G.; Vonk, R.J.; Wopereis, S.; Afman, L.A. A 12-wk whole-grain wheat intervention protects against hepatic fat: The Graandioos study, a randomized trial in overweight subjects. Am. J. Clin. Nutr. 2018, 108, 1264–1274. [Google Scholar] [CrossRef]
- Weickert, M.O.; Arafat, A.; Blaut, M.; Alpert, C.; Becker, N.; Leupelt, V.; Rudovich, N.N.; Möhlig, M.; Pfeiffer, A.F.H. Changes in dominant groups of the gut microbiota do not explain cereal-fiber induced improvement of whole-body insulin sensitivity. Nutr. Metab. 2011, 8, 90. [Google Scholar] [CrossRef]
- Lambert, J.E.; Parnell, J.A.; Tunnicliffe, J.M.; Han, J.; Sturzenegger, T.; Reimer, R.A. Consuming yellow pea fiber reduces voluntary energy intake and body fat in overweight/obese adults in a 12-week randomized controlled trial. Clin. Nutr. 2017, 36, 126–133. [Google Scholar] [CrossRef]
- Ghetti, F.; De Oliveira, D.G.; De Oliveira, J.M.; Ferreira, L.E.V.V.D.C.; Cesar, D.E.; Moreira, A.P. Effects of Dietary Intervention on Gut Microbiota and Metabolic-Nutritional Profile of Outpatients with Non-Alcoholic Steatohepatitis: A Randomized Clinical Trial. J. Gastrointest. Liver Dis. 2019, 28, 279–287. [Google Scholar] [CrossRef] [PubMed]
- Velikonja, A.; Lipoglavšek, L.; Zorec, M.; Orel, R.; Avguštin, G. Alterations in gut microbiota composition and metabolic parameters after dietary intervention with barley beta glucans in patients with high risk for metabolic syndrome development. Anaerobe 2019, 55, 67–77. [Google Scholar] [CrossRef] [PubMed]
- Zhao, L.; Zhang, F.; Ding, X.; Wu, G.; Lam, Y.Y.; Wang, X.; Fu, H.; Xue, X.; Lu, C.; Ma, J.; et al. Gut bacteria selectively promoted by dietary fibers alleviate type 2 diabetes. Science 2018, 359, 1151–1156. [Google Scholar] [CrossRef] [PubMed]
- Connolly, M.L.; Tzounis, X.; Tuohy, K.; Lovegrove, J. Hypocholesterolemic and Prebiotic Effects of a Whole-Grain Oat-Based Granola Breakfast Cereal in a Cardio-Metabolic “At Risk” Population. Front. Microbiol. 2016, 7, 1755. [Google Scholar] [CrossRef]
- Pedersen, C.; Gallagher, E.; Horton, F.; Ellis, R.J.; Ijaz, U.Z.; Wu, H.; Jaiyeola, E.; Diribe, O.; Duparc, T.; Cani, P.D.; et al. Host–microbiome interactions in human type 2 diabetes following prebiotic fibre (galacto-oligosaccharide) intake. Br. J. Nutr. 2016, 116, 1869–1877. [Google Scholar] [CrossRef]
- Wang, Y.; Ames, N.; Tun, H.; Tosh, S.M.; Jones, P.J.; Khafipour, E. High Molecular Weight Barley β-Glucan Alters Gut Microbiota Toward Reduced Cardiovascular Disease Risk. Front. Microbiol. 2016, 7, 129. [Google Scholar] [CrossRef]
- Reimer, R.A.; Willis, H.J.; Park, H.; Soto-Vaca, A.; Tunnicliffe, J.M.; Madsen, K.L. Inulin-type fructans and whey protein both modulate appetite but only fructans alter gut microbiota in adults with overweight/obesity: A randomized controlled trial. Mol. Nutr. Food Res. 2017, 61, 1700484. [Google Scholar] [CrossRef]
- Carlson, J.L.; Erickson, J.M.; Hess, J.M.; Gould, T.J.; Slavin, J. Prebiotic Dietary Fiber and Gut Health: Comparing the in Vitro Fermentations of Beta-Glucan, Inulin and Xylooligosaccharide. Nutr. 2017, 9, 1361. [Google Scholar] [CrossRef]
- So, D.; Whelan, K.; Rossi, M.; Morrison, M.; Holtmann, G.J.; Kelly, J.T.; Shanahan, E.R.; Staudacher, H.; Campbell, K.L. Dietary fiber intervention on gut microbiota composition in healthy adults: A systematic review and meta-analysis. Am. J. Clin. Nutr. 2018, 107, 965–983. [Google Scholar] [CrossRef]
- Baxter, N.T.; Schmidt, A.W.; Venkataraman, A.; Kim, K.S.; Waldron, C.; Schmidt, T.M.; Britton, R.; Walter, J. Dynamics of Human Gut Microbiota and Short-Chain Fatty Acids in Response to Dietary Interventions with Three Fermentable Fibers. mBio 2019, 10, e02566-18. [Google Scholar] [CrossRef]
- Lozupone, C.A.; Stombaugh, J.I.; Gordon, J.I.; Jansson, J.; Knight, R. Diversity, stability and resilience of the human gut microbiota. Nature 2012, 489, 220–230. [Google Scholar] [CrossRef] [PubMed]
- Christensen, L.; Roager, H.M.; Astrup, A.; Hjorth, M.F. Microbial enterotypes in personalized nutrition and obesity management. Am. J. Clin. Nutr. 2018, 108, 645–651. [Google Scholar] [CrossRef] [PubMed]
- Hjorth, M.F.; Roager, H.M.; Larsen, T.M.; Poulsen, S.K.; Licht, T.R.; Bahl, M.I.; Zohar, Y.; Astrup, A. Pre-treatment microbial Prevotella-to-Bacteroides ratio, determines body fat loss success during a 6-month randomized controlled diet intervention. Int. J. Obes. 2017, 42, 580–583. [Google Scholar] [CrossRef] [PubMed]
- Simpson, H.L.; Campbell, B.J. Review article: Dietary fibre-microbiota interactions. Aliment. Pharmacol. Ther. 2015, 42, 158–179. [Google Scholar] [CrossRef] [PubMed]
- Sinha, R.; Chen, J.; Amir, A.; Vogtmann, E.; Shi, J.; Inman, K.S.; Flores, R.; Sampson, J.; Knight, R.; Chia, N. Collecting Fecal Samples for Microbiome Analyses in Epidemiology Studies. Cancer Epidemiol. Biomark. Prev. 2015, 25, 407–416. [Google Scholar] [CrossRef] [PubMed]
- Sinha, R.; Abu-Ali, G.; Vogtmann, E.; Fodor, A.A.; Ren, B.; Amir, A.; Schwager, E.; Crabtree, J.; Ma, B.; The Microbiome Quality Control Project Consortium; et al. Assessment of variation in microbial community amplicon sequencing by the Microbiome Quality Control (MBQC) project consortium. Nat. Biotechnol. 2017, 35, 1077–1086. [Google Scholar] [CrossRef]
- Brooks, J.P.; Edwards, D.J.; Harwich, M.D.; Rivera, M.C.; Fettweis, J.M.; Serrano, M.G.; Reris, R.A.; Sheth, N.U.; Huang, B.; Girerd, P. The truth about metagenomics: Quantifying and counteracting bias in 16S rRNA studies. BMC Microbiol. 2015, 15, 66. [Google Scholar] [CrossRef]
- Laudadio, I.; Fulci, V.; Palone, F.; Stronati, L.; Cucchiara, S.; Carissimi, C. Quantitative Assessment of Shotgun Metagenomics and 16S rDNA Amplicon Sequencing in the Study of Human Gut Microbiome. OMICS J. Integr. Boil. 2018, 22, 248–254. [Google Scholar] [CrossRef]
- Hartley, L.; May, M.D.; Loveman, E.; Colquitt, J.L.; Rees, K. Dietary fibre for the primary prevention of cardiovascular disease. Cochrane Database Syst. Rev. 2016. [Google Scholar] [CrossRef]
- Tosh, S.M. Review of human studies investigating the post-prandial blood-glucose lowering ability of oat and barley food products. Eur. J. Clin. Nutr. 2013, 67, 310–317. [Google Scholar] [CrossRef]
- Wang, Z.; Zhao, Y. Gut microbiota derived metabolites in cardiovascular health and disease. Protein Cell 2018, 9, 416–431. [Google Scholar] [CrossRef] [PubMed]
- Zhang, J.; Wei, Z.; Chen, J. A distance-based approach for testing the mediation effect of the human microbiome. Bioinformatics 2018, 34, 1875–1883. [Google Scholar] [CrossRef] [PubMed]
| Methods | Principals | +/− | |
|---|---|---|---|
| Non-targeted DNA-based approach | Non-targeted shotgun metagenomics |
| + Not limited by primer bias, choice of variable regions or PCR competition − Less tolerant of low biomass − Less tolerant of contaminating DNA |
| Targeted DNA-based approaches | 16S rRNA/ITS amplicon massive parallel sequencing |
| + Can be performed on low biomass samples + Tolerates contaminating DNA − Limited by primer bias, choice of the variable region, PCR competition |
| Targeted quantitative PCR (qPCR) |
| + Not limited by PCR bias or competition + Can be performed on low biomass samples + Tolerates contaminating DNA − Only selected taxa are quantified | |
| Microarray—HITChip (Human intestinal tract chip) |
| + Can be performed on low biomass samples + Tolerates contaminating DNA − Limited by primer bias, choice of variable region, PCR competition − Only pre-defined taxa are identified | |
| Fluorescent in situ hybridization (FISH) |
| + Can be performed on low biomass samples + Tolerates contaminating DNA − Limited by subjective measures, labor-intensive − Only selected taxa are quantified | |
| Study | Subject Characteristics | Study Design | Intervention | Changes Related to Gut Microbiota | Changes Related to Metabolic Regulation |
|---|---|---|---|---|---|
| Sandberg et al., Eur J Nutr, 2019 [31] | n = 99, BMI 24, 64 year, M/F, stratified in 3 groups based on Prevotella/Bacteroides ratio + total group | 2 × 3 days Crossover | (1) White wheat bread (fiber 10.7 g/day) (2) Barley kernel bread (fiber 36.4 g/day) | Stratified on Prevotella/Bacteroides ratio Prevotella/Bacteroides ratio was not predictive of the metabolic response. | ↓ iAUC Glu (after barley kernel bread all groups) ↓ iAUC Ins (after barley kernel bread all groups) ↔ NEFA |
| Costabile et al., Front Immunol, 2017 [35] | n = 36, BMI 26–28, 60–80 year, M/F | 4 × 21 days Crossover | (1) Maltodextrin (2) Soluble corn fiber (SCF) (8 g/day) (3) Lactobacillus rhamnosus GG + SCF (8 g/day) (4) Pilus-deficient L. rhamnosus GG-PB12 + SCF (8 g/day) | (3), (4) ↑ Parabacteroides (2), (3) ↑ Ruminococcaceae incertae sedis (3) ↓ Oscillospira (3), (4) ↓ Desulfovibrio | ↔ Glu ↔ TC, LDL-C, HDL-C, TG, NEFA Within group: (3) ↓ TC, LDL-C (participants with TC > 5 mmol/L)) |
| Vanegas et al., Am J Clin Nutr, 2017 [33] | n = 81, BMI 26, 55 year, M/F | 6 weeks Parallel | (1) Refined-grain diet (fiber 8 g/1000 kcal) (2) Whole-grain diet (fiber 16 g/1000 kcal) | ↔ Phylum level ↓ Enterobacteriaceae ↑ Lachnospira, Roseburia Correlations: ↑ Lachnospira and Roseburia and acetate and butyrate ↑ SCFA (stool), acetate (stool) | ↔ LDL-C, HDL-C, VLDL-C, TG Within group: (2) ↓ TC |
| Kovatcheva-Datchary et al., Cell Metab, 2015 [32] | n = 39, BMI 18–28, 50–70 year, M/F Responders, n = 10 Non-responders, n = 10 | 2 × 3 days Crossover | (1) White wheat bread (fiber 9.1 g/day) (2) Barley kernel bread (fiber 37.6 g/day) | Responders vs. non-responders: ↑ Bacteroidetes ↑ Prevotella/Bacteroides ratio | ↓ Glu, Ins (postprandial) Responders vs. non-responders: ↓ iAUC Glu ↓ iAUC Ins |
| Costabile et al., Br J Nutr, 2008 [34] | n = 31, BMI 20–30, 25 year, M/F | 2 × 3 weeks Crossover | (1) Wheat bran cereal, 48 g, breakfast (fiber 27 g/100 g) (2) 100% whole-grain cereal, 48 g, breakfast (fiber 11.8 g/100 g) | ↑ Bifidobacteria, Lactobacilli, ↔ Total bacteria, Bacteroides spp., Clostridia, Atopobium spp., Bifidobacterium spp., Eubacterium rectale group ↔ Acetate, Butyrate, Caprionate, Propionate Within groups: (1), (2) ↑ Lactobacilli/Enterococci ratio (2) ↑ Bifidobacterium spp. | ↔ Glu, Ins ↔ TC, TG, HDL-C |
| Study | Subject Characteristics | Study Design | Intervention | Changes Related to Gut Microbiota | Changes Related to Metabolic Regulation |
|---|---|---|---|---|---|
| Chambers et al., Gut, 2019 [38] | n = 12, BMI 30, 60 yaer, M/F | 3 × 42 days crossover | (1) High cellulose (20 g/day) (2) High inulin (20 g/day) (3) Inulin-propionate ester (IPE) (20 g/day) | IPE and inulin compared to cellulose: ↓ Diversity of bacterial species Inulin compared to cellulose: ↓ Enrichment (changes in evenness), ↔ Phyla level, ↑ Actinobacteria, Anaerostipes hadrus, Bifidobacterium faecale, Bacteroides caccae ↓ Clostridia, Clostridiales, Blautia obeum, Blautia luti, Oscillibacter spp., Blautia faecis, Ruminococcus faecis IPE compared to cellulose: ↔ Phyla level,↑ Bacteroides uniformis, Bacteroides xylanisolvens, ↓ Blautia obeum, Eubacterium ruminantium ↑ Propionate (% in serum), ↔ propionate (uM in feces and serum, % in feces), acetate (% and uM in feces and serum), butyrate (% and uM in feces and serum) IPE compared to inulin: ↔ Phyla level, ↑ Fusicatenibacter saccharivorans, ↓ Anaerostipes hadrus, Blautia faecale, Prevotelle copri | IPE and Inulin compared with cellulose: ↓ Ins, HOMA-IR, AT-IR, ↑ Matsuda ISI |
| Kjølbæk et al., Clin Nutr, 2019 [36] | n = 27, BMI 25–40, 18–60 yaer, M/F | 2 × 4 weeks Crossover | (1) n3 PUFA (3.6 g/day) (2) Arabinoxylan oligosaccharides (10.4 g/day) | Within groups: (2) in responders: ↑ Actinobacteria, Eubacterium rectale, Faecalibacterium prusnitzii, Bifidobacterium faecale, Bifidobacterium stercoris, Bifidobacterium dolescentis, Blautia wexlerae, Bifidobacterium angulatum, Bifidobacterium merycicum, Bifidobacterium pseudocatenulatum, Bifidobacterium catenulatum, Fusicatenibacter saccharivorans, Bifidobacterium longum, Ruminococcus obeum, Dorea longgicaterna, Eubacterium hallii, Blautia luti ↓ Clostridium methylpentosum, Anaerotruncus colihominis, Erysipelothrix rhusiopathiae | ↔ Glu, Ins, HOMA-IR, HOMA-β ↔ TC, HDL-C, LDL-C, VLDL-C, ApoB |
| Schutte et al., Am J Clin Nutr, 2018 [39] | n = 50, BMI 25–35, 61 year, M/F | 12 weeks Parallel | (1) Refined wheat (98 g/day) (2) Whole-grain wheat (98 g/day) | ↑ α-diversity, ↔ Lachnospiraceae and Ruminovoccaceae (and genera within these families) | ↔ Glu, Ins, HOMA-IR ↔ TC, HDL-C, TG, NEFA ↓ IHTG |
| Canfora et al., Gastroenterology, 2017 [37] | n = 44, BMI 28–40, pre-diabetic, 45–70 year, M/F | 12 weeks Parallel | (1) Maltodextrin (15 g/day) (2) Galacto oligosaccharides (15 g/day) | ↑ Bifidobacterium spp., Prevotella oralis, Prevotella melaninogenica ↓ Bacteroides stercoris, Sutterella wadsworthia ↔ Fecal microbial richness or diversity ↔ SCFA (fecal and plasma) | ↔ Glu, Ins, HOMA-IR, GLP-1 ↔ TG, NEFA |
| Lambert et al., Clin Nutr, 2017 [41] | n = 50, BMI 33, 44 year, M/F | 12 weeks Parallel | (1) Wafers without pea fiber (2) Wafers with pea fiber (15 g/day) | ↔ Total bacteria, Bacteroides/Prevotella spp., Bifidobacterium spp., Enterobacteriaceae, Methanobrevibacter spp., Firmicutes, Lactobacillus spp., Clostridium leptum (C-IV), Clostridium coccoides (C-XIVa), Clostridium cluster I, Clostridium cluster XI, Roseburia spp. | ↔ Glu, Ins, HbA1c ↔ TC, LDL-C, HDL-C, TG, TC/HDL-C ratio |
| Weickert et al., Nutr Metab, 2011 [40] | n = 69, BMI >30, 55.3 year, M/F | 18 weeks, Parallel | (1) Control diet (fiber 14 g/day) (2) High cereal-fiber diet, HCF (fiber 43 g/day) (3) High protein diet, HP (28 E% protein, 14 g/day fiber) (4) Combined HCF and HP diet (23 E% protein, 26 g/day fiber) | ↔ Dominant groups of gut bacteria ↔ Fecal acetate, propionate, butyrate, valerate Within groups: (3) ↑ Valerate | Within groups (2) ↑ Ins sensitivity (Euglycaemic hyperinsulinaemic clamps) |
| Study | Subject Characteristics | Study Design | Intervention | Changes Related to Gut Microbiota | Changes Related to Metabolic Regulation |
|---|---|---|---|---|---|
| De Faria Ghetti et al., J Gastrointestin Liver Dis, 2019 [42] | n = 40, NASH, BMI 31, 50.6 y (Control), 48.3 year (DIET), M/F | 3 months Parallel | (1) Control group (nutritional orientation) (2) The DIET group (fiber 30 g/day + nutritional orientation) | Within groups: (2) ↑ Density of total microorganisms (1) ↓ Bacteroidetes, Verrucomicrobiales | ↓ Ins, HOMA-IR, ↓ TC Within groups: (2) ↓ Glu, HOMA-IR, TC, TG ↓ TC, LDL-C, TG |
| Velikonja et al., Ana in Microbiome, 2019 [43] | n = 43, MetS, BMI not reported, 50.9 year, M/F | 4 weeks Parallel | (1) Control (Bread without b-glucan) (2) Bread with b-glucan (6 g/day) | Within groups: (2) ↓ Microbial diversity and richness, Higher basal abundance of Bifidobacterium spp and Akkermansia municiphila within the intervention group (2) ↑ Fecal propionate (1) ↓ Fecal acetate | Within group: (1) (2) ↔ Glu and Ins after OGTT (2) ↓ TC (1) (2) ↔ LDL-C, HDL-C, TG |
| Zhao et al., Science, 2018 [44] | n = 43, T2D, BMI not reported, 35–70 year, M/F | 84 days Parallel | (1) Usual diet according to the Chinese Diabetes Society + acarbose (fiber 16.1 g/day) (2) Wholegrains, traditional Chinese medicinal foods and prebiotics + acarbose (fiber 37.1 g/day) | ↑ SCFA-producing strains Within groups: (1) (2) ↓ Gene richness, tended to be higher in the (2) than in (1) this trend was associated with better clinical outcomes in group (2) | ↓ HbA1c, Glu, GLP-1 AUC |
| Connolly et al., Front Microbiol, 2016 [45] | n = 30, mildly hypercholesterolemia or glucose-intolerant, BMI 26, 42 year, M/F | 2 × 6 weeks crossover | (1) Non-whole-grain breakfast cereals 45g/day (fiber 3.0 g/day, no β-glucan) (2) Whole-grain oat granola 45 g/day (fiber 6.3 g/day and 2.9 g/day β-glucan) | ↑ Bifidobacterium spp., Lactobacillus spp., total bacterial count ↔ Acetate, Propionate, Butyrate Within groups: (1) ↓ Bifidobacterium spp., total bacterial count (2) ↑ Bifidobacterium spp., Lactobacillus spp., total bacterial count | ↔ Glu, Ins, HOMA-IR, QUICKI ↓ TC, LDL-C ↔ HDL-C. TG Within groups: (1) ↑ TC (2) ↓ TC |
| Pedersen et al., Br J Nutr, 2016 [46] | n = 29, T2D, BMI 30, 42–65 year, M | 12 weeks Parallel | (1) Maltodextrin (5.5 g/day) (2) Galacto oligosaccharides (5.5 g/day) | ↔ Bacterial abundance or diversity Within groups: (2) ↑ Diversity Shannon indices Correlations: ↓ Veillonellaceae and Glu response | ↔ Glu, Ins, C-peptide (fasting or response IVGTT) ↔ TC, LDL-C |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Myhrstad, M.C.W.; Tunsjø, H.; Charnock, C.; Telle-Hansen, V.H. Dietary Fiber, Gut Microbiota, and Metabolic Regulation—Current Status in Human Randomized Trials. Nutrients 2020, 12, 859. https://doi.org/10.3390/nu12030859
Myhrstad MCW, Tunsjø H, Charnock C, Telle-Hansen VH. Dietary Fiber, Gut Microbiota, and Metabolic Regulation—Current Status in Human Randomized Trials. Nutrients. 2020; 12(3):859. https://doi.org/10.3390/nu12030859
Chicago/Turabian StyleMyhrstad, Mari C. W., Hege Tunsjø, Colin Charnock, and Vibeke H. Telle-Hansen. 2020. "Dietary Fiber, Gut Microbiota, and Metabolic Regulation—Current Status in Human Randomized Trials" Nutrients 12, no. 3: 859. https://doi.org/10.3390/nu12030859
APA StyleMyhrstad, M. C. W., Tunsjø, H., Charnock, C., & Telle-Hansen, V. H. (2020). Dietary Fiber, Gut Microbiota, and Metabolic Regulation—Current Status in Human Randomized Trials. Nutrients, 12(3), 859. https://doi.org/10.3390/nu12030859





