Metabolic Syndrome in Arab Adults with Low Bone Mineral Density
Abstract
:1. Introduction
2. Materials and Methods
2.1. Study Design and Participants
2.2. Bone Mineral Density (BMD) Scan and T-Score
2.3. Anthropometry, Blood Collection and Sample Analysis
2.4. T-Score Tertiles and MetS Components
- Central obesity: waist circumference >102 cm (males), >88 cm (females).
- Hyperglycemia: fasting glucose >5.6 mmol/l or pharmacologic treatment for hyperglycemia (both sexes).
- Hypertriglyceridemia: serum triglycerides ≥1.7 mmol/l (both sexes).
- Low HDL-cholesterol: serum HDL-cholesterol <1.03 mmol/l (males), <1.30 mmol/l (females).
- Hypertension: systolic blood pressure >130 mmHg and/or diastolic blood pressure >85 mmHg or current use of antihypertensive medications.
2.5. Data Analysis
3. Results
3.1. General and Biochemical Characteristics of the Study Participants
3.2. Prevalence of Different MetS Components in T-Score Tertiles
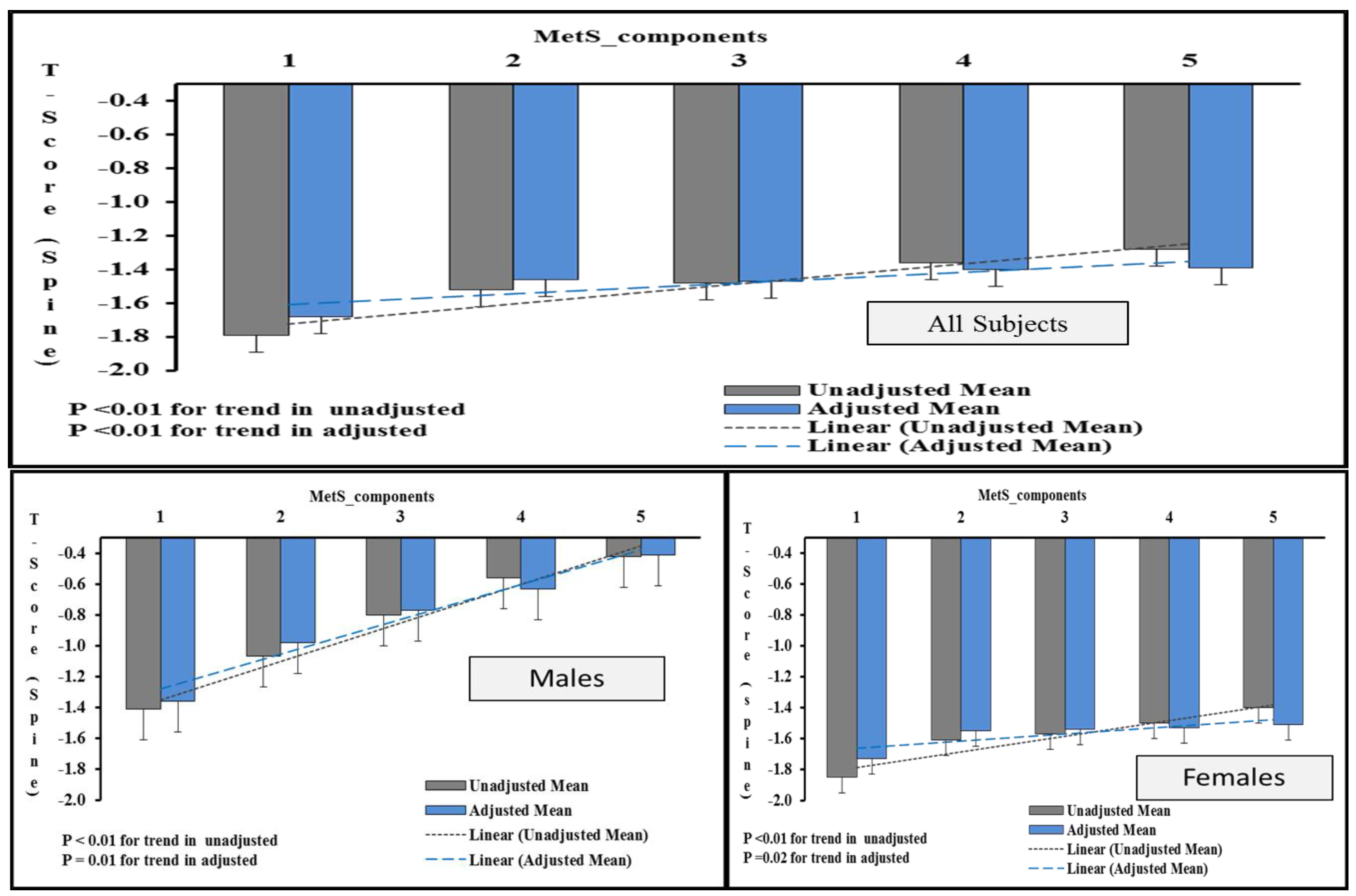
3.3. Association of T-score with Different Components of MetS and Full MetS.
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Maiorino, M.; Bellastella, G.; Giugliano, D.; Esposito, K. From inflammation to sexual dysfunctions: A journey through diabetes, obesity, and metabolic syndrome. J. Endocrinol. Investig. 2018, 41, 1249–12580. [Google Scholar] [CrossRef] [PubMed]
- Darroudi, S.; Fereydouni, N.; Tayefi, M.; Ahmadnezhad, M.; Zamani, P.; Tayefi, B.; Kharazmi, J.; Tavalaie, S.; Heidari-Bakavoli, A.; Azarpajouh, M.R. Oxidative stress and inflammation, two features associated with a high percentage body fat, and that may lead to diabetes mellitus and metabolic syndrome. BioFactors 2018, 45, 35–42. [Google Scholar] [CrossRef] [PubMed]
- Al-Nozha, M.; Al-Khadra, A.; Arafah, M.R.; Al-Maatouq, M.A.; Khalil, M.Z.; Khan, N.B.; Al-Mazrou, Y.Y.; Al-Marzouki, K.; Al-Harthi, S.S.; Abdullah, M.; et al. Metabolic syndrome in saudi arabia. Saudi Med. J. 2005, 26, 1918–1925. [Google Scholar] [PubMed]
- Al-Qahtani, D.A.; Imtiaz, M.L. Prevalence of metabolic syndrome in saudi adult soldiers. Saudi Med. J. 2005, 26, 1360–1366. [Google Scholar] [PubMed]
- Prasad, H.; Ryan, D.A.; Celzo, M.F.; Stapleton, D. Metabolic syndrome: Definition and therapeutic implications. Postgrad. Med. 2012, 124, 21–30. [Google Scholar] [CrossRef] [PubMed]
- Kaur, J. A comprehensive review on metabolic syndrome. Cardiol. Res. Pract. 2014, 2014, 943162. [Google Scholar] [CrossRef]
- Huang, P.L. A comprehensive definition for metabolic syndrome. Dis. Model. Mech. 2009, 2, 231–237. [Google Scholar] [CrossRef] [Green Version]
- Wong, S.; Chin, K.-Y.; Suhaimi, F.; Ahmad, F.; Ima-Nirwana, S. The relationship between metabolic syndrome and osteoporosis: A review. Nutrients 2016, 8, 347. [Google Scholar] [CrossRef]
- De Laet, C.; Kanis, J.; Odén, A.; Johanson, H.; Johnell, O.; Delmas, P.; Eisman, J.; Kroger, H.; Fujiwara, S.; Garnero, P. Body mass index as a predictor of fracture risk: A meta-analysis. Osteoporos. Int. 2005, 16, 1330–1338. [Google Scholar] [CrossRef]
- Janghorbani, M.; Van Dam, R.M.; Willett, W.C.; Hu, F.B. Systematic review of type 1 and type 2 diabetes mellitus and risk of fracture. Am. J. Epidemiol. 2007, 166, 495–505. [Google Scholar] [CrossRef]
- Schwartz, A.V.; Vittinghoff, E.; Bauer, D.C.; Hillier, T.A.; Strotmeyer, E.S.; Ensrud, K.E.; Donaldson, M.G.; Cauley, J.A.; Harris, T.B.; Koster, A. Association of bmd and frax score with risk of fracture in older adults with type 2 diabetes. JAMA 2011, 305, 2184–2192. [Google Scholar] [CrossRef] [PubMed]
- Oei, L.; Zillikens, M.C.; Dehghan, A.; Buitendijk, G.H.; Castaño-Betancourt, M.C.; Estrada, K.; Stolk, L.; Oei, E.H.; van Meurs, J.B.; Janssen, J.A. High bone mineral density and fracture risk in type 2 diabetes as skeletal complications of inadequate glucose control: The rotterdam study. Diabetes Care 2013, 36, 1619–1628. [Google Scholar] [CrossRef] [PubMed]
- Sun, K.; Liu, J.; Lu, N.; Sun, H.; Ning, G. Association between metabolic syndrome and bone fractures: A meta-analysis of observational studies. BMC Endocr. Disord. 2014, 14, 13. [Google Scholar] [CrossRef] [PubMed]
- Yamaguchi, T.; Kanazawa, I.; Yamamoto, M.; Kurioka, S.; Yamauchi, M.; Yano, S.; Sugimoto, T. Associations between components of the metabolic syndrome versus bone mineral density and vertebral fractures in patients with type 2 diabetes. Bone 2009, 45, 174–179. [Google Scholar] [CrossRef] [PubMed]
- Kim, H.; Oh, H.J.; Choi, H.; Choi, W.H.; Lim, S.-K.; Kim, J.G. The association between bone mineral density and metabolic syndrome: A Korean population-based study. J. Bone Miner. Metab. 2013, 31, 571–578. [Google Scholar] [CrossRef]
- Al-Daghri, N.M.; Al-Attas, O.S.; Wani, K.; Sabico, S.; Alokail, M.S. Serum uric acid to creatinine ratio and risk of metabolic syndrome in saudi type 2 diabetic patients. Sci. Rep. 2017, 7, 12104. [Google Scholar] [CrossRef] [PubMed]
- Von Muhlen, D.; Safii, S.; Jassal, S.; Svartberg, J.; Barrett-Connor, E. Associations between the metabolic syndrome and bone health in older men and women: The rancho bernardo study. Osteoporos. Int. 2007, 18, 1337–1344. [Google Scholar] [CrossRef]
- Hwang, D.-K.; Choi, H.-J. The relationship between low bone mass and metabolic syndrome in korean women. Osteoporos. Int. 2010, 21, 425–431. [Google Scholar] [CrossRef]
- Jeon, Y.K.; Lee, J.G.; Kim, S.S.; Kim, B.H.; Kim, S.-J.; Kim, Y.K.; Kim, I.J. Association between bone mineral density and metabolic syndrome in pre- and postmenopausal women. Endocr. J. 2011, 58, 87–93. [Google Scholar] [CrossRef] [Green Version]
- Hernández, J.L.; Olmos, J.M.; Pariente, E.; Martínez, J.; Valero, C.; García-Velasco, P.; Nan, D.; Llorca, J.; González-Macías, J. Metabolic syndrome and bone metabolism: The camargo cohort study. Menopause 2010, 17, 955–961. [Google Scholar] [CrossRef]
- El Maghraoui, A.; Rezqi, A.; El Mrahi, S.; Sadni, S.; Ghozlani, I.; Mounach, A. Osteoporosis, vertebral fractures and metabolic syndrome in postmenopausal women. BMC Endocr. Disord. 2014, 14, 93. [Google Scholar] [CrossRef] [PubMed]
- Muka, T.; Trajanoska, K.; Kiefte-de Jong, J.C.; Oei, L.; Uitterlinden, A.G.; Hofman, A.; Dehghan, A.; Zillikens, M.C.; Franco, O.H.; Rivadeneira, F. The association between metabolic syndrome, bone mineral density, hip bone geometry and fracture risk: The Rotterdam study. PLoS ONE 2015, 10, e0129116. [Google Scholar] [CrossRef] [PubMed]
- Xue, P.; Gao, P.; Li, Y. The association between metabolic syndrome and bone mineral density: A meta-analysis. Endocrine 2012, 42, 546–554. [Google Scholar] [CrossRef] [PubMed]
- Edelstein, S.L.; Barrett-Connor, E. Relation between body size and bone mineral density in elderly men and women. Am. J. Epidemiol. 1993, 138, 160–169. [Google Scholar] [CrossRef] [PubMed]
- Jankowska, E.; Rogucka, E.; Mędraś, M. Are general obesity and visceral adiposity in men linked to reduced bone mineral content resulting from normal ageing? A population-based study. Andrologia 2001, 33, 384–389. [Google Scholar] [CrossRef] [PubMed]
- Moon, S.-S.; Lee, Y.-S.; Kim, S.W. Association of nonalcoholic fatty liver disease with low bone mass in postmenopausal women. Endocrine 2012, 42, 423–429. [Google Scholar] [CrossRef] [PubMed]
- Nelson, L.R.; Bulun, S.E. Estrogen production and action. J. Am. Acad. Dermatol. 2001, 45, S116–S124. [Google Scholar] [CrossRef]
- Hofbauer, L.C.; Schoppet, M. Clinical implications of the osteoprotegerin/rankl/rank system for bone and vascular diseases. JAMA 2004, 292, 490–495. [Google Scholar] [CrossRef]
- Campos, R.M.; de Piano, A.; da Silva, P.L.; Carnier, J.; Sanches, P.L.; Corgosinho, F.C.; Masquio, D.C.; Lazaretti-Castro, M.; Oyama, L.M.; Nascimento, C.M. The role of pro/anti-inflammatory adipokines on bone metabolism in nafld obese adolescents: Effects of long-term interdisciplinary therapy. Endocrine 2012, 42, 146–156. [Google Scholar] [CrossRef]
- Cao, J.J. Effects of obesity on bone metabolism. J. Orthop. Surg. Res. 2011, 6, 30. [Google Scholar] [CrossRef]
- Kinjo, M.; Setoguchi, S.; Solomon, D.H. Bone mineral density in adults with the metabolic syndrome: Analysis in a population-based US sample. J. Clin. Endocrinol. Metab. 2007, 92, 4161–4164. [Google Scholar] [CrossRef] [PubMed]
- Holmberg, A.H.; Nilsson, P.; Nilsson, J.-A.; Akesson, K. The association between hyperglycemia and fracture risk in middle age. A prospective, population-based study of 22,444 men and 10,902 women. J. Clin. Endocrinol. Metab. 2008, 93, 815–822. [Google Scholar] [CrossRef] [PubMed]
- Thrailkill, K.M.; Lumpkin, C.K., Jr.; Bunn, R.C.; Kemp, S.F.; Fowlkes, J.L. Is insulin an anabolic agent in bone? Dissecting the diabetic bone for clues. Am. J. Physiol. -Endocrinol. Metab. 2005, 289, E735–E745. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Ivers, R.Q.; Cumming, R.G.; Mitchell, P.; Peduto, A.J. Diabetes and risk of fracture: The blue mountains eye study. Diabetes Care 2001, 24, 1198–1203. [Google Scholar] [CrossRef] [PubMed]
- Xu, S.; Jianqing, J.Y. Beneath the minerals, a layer of round lipid particles was identified to mediate collagen calcification in compact bone formation. Biophys. J. 2006, 91, 4221–4229. [Google Scholar] [CrossRef]
- Hanley, D.; Brown, J.; Tenenhouse, A.; Olszynski, W.; Ioannidis, G.; Berger, C.; Prior, J.; Pickard, L.; Murray, T.; Anastassiades, T. Associations among disease conditions, bone mineral density, and prevalent vertebral deformities in men and women 50 years of age and older: Cross-sectional results from the canadian multicentre osteoporosis study. J. Bone Miner. Res. 2003, 18, 784–790. [Google Scholar] [CrossRef] [PubMed]
- Mussolino, M.E.; Gillum, R. Bone mineral density and hypertension prevalence in postmenopausal women: Results from the third national health and nutrition examination survey. Ann. Epidemiol. 2006, 16, 395–399. [Google Scholar] [CrossRef]
- Krall, E.A.; Dawson-Hughes, B.; Hirst, K.; Gallagher, J.; Sherman, S.S.; Dalsky, G. Bone mineral density and biochemical markers of bone turnover in healthy elderly men and women. J. Gerontol. A Biol. Sci. Med. Sci. 1997, 52, M61–M67. [Google Scholar] [CrossRef]
- Abate, N.; Chandalia, M. The impact of ethnicity on type 2 diabetes. J. Diabetes Complicat. 2003, 17, 39–58. [Google Scholar] [CrossRef]
- Pocock, N.A.; Noakes, K.A.; Griffiths, M.; Bhalerao, N.; Sambrook, P.N.; Eisman, J.A.; Freund, J. A comparison of longitudinal measurements in the spine and proximal femur using lunar and hologic instruments. J. Bone Miner. Res. 1997, 12, 2113–2118. [Google Scholar] [CrossRef]
- Dragojevič, J.; Zupan, J.; Haring, G.; Herman, S.; Komadina, R.; Marc, J. Triglyceride metabolism in bone tissue is associated with osteoblast and osteoclast differentiation: a gene expression study. J. Bone Miner. Metab. 2013, 31, 512–519. [Google Scholar] [CrossRef] [PubMed]
- Sundararaghavan, V.; Mazur, M.M.; Evans, B.; Liu, J.; Ebraheim, N.A. Diabetes and bone health: Latest evidence and clinical implications. Ther. Adv. Musculoskelet. Dis. 2017, 9, 67–74. [Google Scholar] [CrossRef] [PubMed]
- Komorita, Y.; Iwase, M.; Idewaki, Y.; Fujii, H.; Ohkuma, T.; Ide, H.; Jodai, K.T.; Yoshinari, M.; Murao, K.A.; Oku, Y. Impact of hip fracture on all-cause mortality in Japanese patients with type 2 diabetes mellitus: The Fukuoka Diabetes Registry. J. Diabetes Investig. 2019. [Google Scholar] [CrossRef] [PubMed]
- Tencerova, M.; Frost, M.; Figeac, F.; Nielsen, T.K.; Ali, D.; Lauterlein, J.-J.L.; Andersen, T.L.; Haakonsson, A.K.; Rauch, A.; Madsen, J.S. Obesity-Associated Hypermetabolism and Accelerated Senescence of Bone Marrow Stromal Stem Cells Suggest a Potential Mechanism for Bone Fragility. Cell Rep. 2019, 27, 2050–2062. [Google Scholar] [CrossRef] [PubMed]
- Guh, D.P.; Zhang, W.; Bansback, N.; Amarsi, Z.; Birmingham, C.L.; Anis, A.H. The incidence of co-morbidities related to obesity and overweight: A systematic review and meta-analysis. BMC Public Health 2009, 9, 88. [Google Scholar] [CrossRef] [PubMed]
- Salamat, M.R.; Salamat, A.H.; Janghorbani, M. Association between obesity and bone mineral density by gender and menopausal status. Endocrinol. Metab. 2016, 31, 547–558. [Google Scholar] [CrossRef] [PubMed]
- Smith, B.; Lerner, M.; Bu, S.; Lucas, E.; Hanas, J.; Lightfoot, S.; Postier, R.; Bronze, M.; Brackett, D. Systemic bone loss and induction of coronary vessel disease in a rat model of chronic inflammation. Bone 2006, 38, 378–386. [Google Scholar] [CrossRef] [PubMed]

| Overall | Males | Females | |
|---|---|---|---|
| N | 1587 | 243 | 1344 |
| Anthropometrics | |||
| Age (years) | 56.7 ± 8.2 | 58.1 ± 9.4 | 56.4 ± 7.9 |
| BMI (kg/m2) | 32.4 ± 6.4 | 29.9 ± 5.2 | 32.93 ± 6.4 |
| Waist (cm) | 100.3 ± 14.1 | 103.7 ± 14.2 | 99.7 ± 14 |
| Hips (cm) | 107.9 ± 12.9 | 104.4 ± 12 | 108.6 ± 13 |
| Systolic BP (mmHg) | 126.2 ± 16.4 | 131.1 ± 13.1 | 125.4 ± 16.8 |
| Diastolic BP (mmHg) | 76.8 ± 9.9 | 79.5 ± 8.2 | 76.3 ± 10.1 |
| Risk Factors | |||
| Age (>50 years) $ | 77.4 | 79.8 | 77.0 |
| Family History | |||
| Diabetes Mellitus $ | 61.0 | 74.5 | 58.6 |
| Osteoporosis $ | 9.8 | 9.9 | 9.7 |
| Arthritis $ | 6.2 | 4.9 | 6.5 |
| Subject History | |||
| Diabetes Mellitus $ | 54.4 | 70.8 | 51.4 |
| Thyroid Disease $ | 8.1 | 2.5 | 9.2 |
| Barium Test (last 2 weeks) $ | 9.4 | 2.1 | 10.7 |
| Scoliosis of Spine $ | 7.8 | 1.6 | 8.9 |
| Kyphosis $ | 3.5 | 0.8 | 4.0 |
| Lost Height (2 years) $ | 8.8 | 1.6 | 10.0 |
| Fracture (last 5 years) $ | 10.7 | 5.3 | 11.7 |
| T-Score (L1–L4 Spine) | –1.49 ± 1.3 | –0.84 ± 1.3 | –1.60 ± 1.3 |
| Biochemical Characteristics | |||
| Glucose (mmol/l) # | 6.7 (5.5, 9.9) | 9.2 (6.5–14.1) | 6.5 (5.4–9.3) |
| Insulin (μU/ml) # | 10.4 (5.9, 18.4) | 21.6 (10.7, 33.6) | 9.4 (5.4, 15.6) |
| Total Cholesterol (mmol/l) | 5.0 ± 1.1 | 4.9 ± 1.3 | 5.08 ± 1.1 |
| Triglycerides (mmol/l) # | 1.6 (1.2, 2.2) | 1.9 (1.4, 2.8) | 1.55 (1.1, 2.2) |
| HDL-Cholesterol (mol/l) | 1.2 ± 0.4 | 1.1 ± 0.3 | 1.17 ± 0.4 |
| Calcium (mmol/l) | 2.3 ± 0.3 | 2.3 ± 0.2 | 2.3 ± 0.3 |
| Albumin (g/l) | 38.7 ± 6.7 | 40.2 ± 5.8 | 38.4 ± 6.8 |
| All (N = 1587) | Males (N = 243) | Females (N = 1344) | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| T-Score (L1–L4 Spine) | T1 | T2 | T3 | p | T1 | T2 | T3 | p | T1 | T2 | T3 | p |
| Central Obesity | 66.9 | 79.8 | 82.7 | <0.01 | 38.3 | 60.5 | 71.6 | <0.01 | 72.1 | 83.4 | 84.7 | <0.01 |
| Hyperglycemia | 69.9 | 73.8 | 74.0 | 0.25 | 86.4 | 80.2 | 91.4 | 0.12 | 66.9 | 72.7 | 70.8 | 0.16 |
| Low HDL-Cholesterol | 63.0 | 64.6 | 68.5 | 0.17 | 40.7 | 45.7 | 42.0 | 0.80 | 67.1 | 68.1 | 73.3 | 0.09 |
| Hypertriglyceridemia | 40.3 | 46.2 | 47.7 | 0.04 | 54.3 | 58.0 | 64.2 | 0.43 | 37.7 | 44.0 | 44.6 | 0.07 |
| Hypertension | 29.3 | 32.5 | 34.4 | 0.20 | 38.3 | 35.8 | 39.5 | 0.88 | 27.6 | 31.9 | 33.5 | 0.15 |
| Full MetS | 56.1 | 63.3 | 67.6 | <0.01 | 50.6 | 60.5 | 71.6 | 0.02 | 57.1 | 64.4 | 65.8 | 0.003 |
| MODEL | ALL | MALES | FEMALES | |||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| TERTILE | p | TERTILE | p | TERTILE | p | |||||||
| 1 | 2 | 3 | 1 | 2 | 3 | 1 | 2 | 3 | ||||
| CENTRAL OBESITY | ||||||||||||
| a | 1 | 1.96 (1.5–2.6) | 2.37 (1.8–3.2) | <0.01 | 1 | 2.47 (1.3–4.6) | 4.07 (2.1–7.9) | <0.01 | 1.0 | 1.94 (1.4–2.7) | 2.14 (1.5–2.9) | <0.01 |
| b | 1 | 1.95 (1.5–2.6) | 2.44 (1.8–2.3) | <0.01 | 1 | 2.58 (1.4–4.9) | 4.23 (2.2–8.3) | <0.01 | 1.0 | 1.95 (1.4–2.7) | 2.21 (1.6–3.1) | <0.01 |
| c | 1 | 1.98 (1.4–2.6) | 2.24 (1.6–3.1) | <0.01 | 1 | 1.94 (0.8–4.6) | 3.06 (1.3–7.4) | 0.04 | 1.0 | 2.01 (1.4–2.8) | 2.27 (1.6–3.3) | <0.01 |
| d | 1 | 1.88 (1.4–2.5) | 2.21 (1.6–3.0) | <0.01 | 1 | 1.97 (0.8–4.7) | 2.95 (1.2–7.1) | 0.04 | 1.0 | 1.82 (1.3–2.5) | 1.98 (1.4–2.8) | <0.01 |
| e | 1 | 1.90 (1.4–2.5) | 2.20 (1.6–3.0) | <0.01 | 1 | 2.00 (0.8–4.8) | 3.07 (1.2–7.5) | 0.04 | 1.0 | 1.83 (1.3–2.6) | 1.97 (1.4–2.8) | <0.01 |
| HYPERGLYCEMIA | ||||||||||||
| a | 1 | 1.21 (0.9–1.6) | 1.23 (0.9–1.6) | 0.25 | 1 | 0.64 (0.3–1.5) | 1.66 (0.6–4.5) | 0.12 | 1.0 | 1.32 (1.0–1.8) | 1.20 (0.9–1.6) | 0.16 |
| b | 1 | 1.32 (1.0–1.7) | 1.54 (1.2–2.1) | 0.01 | 1 | 0.82 (0.3–1.9) | 2.25 (0.8–6.4) | 0.10 | 1.0 | 1.40 (1.0–1.9) | 1.47 (1.1–2.0) | 0.02 |
| c | 1 | 1.28 (1.0–1.8) | 1.34 (1.2–2.2) | 0.04 | 1 | 0.71 (0.3–1.8) | 1.71 (0.6–5.1) | 0.21 | 1.0 | 1.32 (1.0–1.8) | 1.44 (1.1–2.0) | 0.05 |
| d | 1 | 1.18 (0.9–1.6) | 1.29 (0.9–1.7) | 0.23 | 1 | 0.66 (0.3–1.7) | 1.59 (0.5–4.8) | 0.24 | 1.0 | 1.25 (0.9–1.7) | 1.26 (0.9–1.7) | 0.29 |
| e | 1 | 1.17 (0.9–1.6) | 1.15 (0.8–1.6) | 0.57 | 1 | 0.62 (0.2–1.7) | 1.58 (0.5–5.1) | 0.26 | 1.0 | 1.25 (0.9–1.7) | 1.21 (0.8–1.6) | 0.41 |
| LOW HDL-CHOLESTEROL | ||||||||||||
| a | 1 | 1.07 (0.8–1.4) | 1.28 (1.0–1.6) | 0.16 | 1 | 1.22 (0.6–2.3) | 1.05 (0.6–1.9) | 0.80 | 1.0 | 1.05 (0.8–1.4) | 1.35 (1.0–1.8) | 0.09 |
| b | 1 | 1.08 (0.8–1.4) | 1.32 (1.0–1.7) | 0.11 | 1 | 1.43 (0.8–2.7) | 1.20 (0.6–2.3) | 0.55 | 1.0 | 1.05 (0.8–1.4) | 1.38 (1.0–1.9) | 0.08 |
| c | 1 | 1.05 (0.9–1.6) | 1.30 (1.0–1.9) | 0.32 | 1 | 1.19 (0.6–2.3) | 1.01 (0.5–1.9) | 0.84 | 1.0 | 1.02 (0.8–1.4) | 1.29 (0.9–1.8) | 0.21 |
| d | 1 | 0.96 (0.7–1.2) | 1.13 (0.9–1.5) | 0.46 | 1 | 1.20 (0.6–2.4) | 0.90 (0.4–1.8) | 0.69 | 1.0 | 0.94 (0.7–1.3) | 1.30 (0.9–1.7) | 0.21 |
| e | 1 | 0.96 (0.7–1.3) | 1.15 (0.9–1.5) | 0.39 | 1 | 1.17 (0.6–2.4) | 0.82 (0.4–1.7) | 0.59 | 1.0 | 0.94 (0.7–1.3) | 1.24 (0.9–1.7) | 0.18 |
| HYPERTRIGLYCERIDEMIA | ||||||||||||
| a | 1 | 1.27 (1.0–1.6) | 1.35 (1.1–1.7) | 0.04 | 1 | 1.16 (0.6–2.2) | 1.51 (0.8–2.8) | 0.43 | 1.0 | 1.30 (1.0–1.7) | 1.34 (1.0–1.7) | 0.06 |
| b | 1 | 1.29 (1.0–1.7) | 1.42 (1.1–1.8) | 0.02 | 1 | 1.25 (0.7–2.4) | 1.62 (0.8–3.1) | 0.34 | 1.0 | 1.30 (1.0–1.7) | 1.34 (1.0–1.8) | 0.07 |
| c | 1 | 1.25 (1.0–1.7) | 1.29 (1.2–1.9) | 0.04 | 1 | 1.18 (0.6–2.3) | 1.47 (0.8–2.9) | 0.51 | 1.0 | 1.20 (0.9–1.6) | 1.24 (0.9–1.7) | 0.29 |
| d | 1 | 1.18 (0.9–1.5) | 1.22 (0.9–1.6) | 0.30 | 1 | 1.24 (0.6–2.4) | 1.38 (0.7–2.7) | 0.64 | 1.0 | 1.16 (0.9–1.5) | 1.13 (0.8–1.5) | 0.56 |
| e | 1 | 1.17 (0.9–1.7) | 1.15 (0.9–1.5) | 0.46 | 1 | 1.16 (0.6–2.3) | 1.47 (0.7–2.9) | 0.56 | 1.0 | 1.16 (0.9–1.5) | 1.07 (0.8–1.5) | 0.61 |
| HYPERTENSION | ||||||||||||
| a | 1 | 1.16 (0.9–1.5) | 1.27 (1.0–1.6) | 0.20 | 1 | 0.90 (0.5–1.7) | 1.05 (0.6–1.9) | 0.88 | 1.0 | 1.23 (0.9–1.6) | 1.32 (1.0–1.8) | 0.15 |
| b | 1 | 1.12 (0.9–1.6) | 1.45 (0.9–1.9) | 0.06 | 1 | 1.07 (0.5–2.1) | 1.25 (0.6–2.4) | 0.80 | 1.0 | 1.27 (0.9–1.7) | 1.45 (1.1–1.9) | 0.05 |
| c | 1 | 1.20 (0.9–1.7) | 1.32 (1.0–1.9) | 0.21 | 1 | 0.95 (0.5–1.9) | 1.10 (0.6–2.2) | 0.91 | 1.0 | 1.24 (0.9–1.7) | 1.37 (1.0–1.9) | 0.13 |
| d | 1 | 1.10 (0.8–1.4) | 1.24 (0.9–1.6) | 0.33 | 1 | 0.93 (0.5–1.8) | 1.16 (0.6–2.3) | 0.79 | 1.0 | 1.11 (0.8–1.5) | 1.24 (0.9–1.7) | 0.40 |
| e | 1 | 1.10 (0.8–1.4) | 1.20 (0.9–1.6) | 0.50 | 1 | 0.90 (0.4–1.8) | 1.16 (0.6–2.4) | 0.77 | 1.0 | 1.11 (0.8–1.5) | 1.19 (0.9–1.6) | 0.56 |
| FULL METS | ||||||||||||
| a | 1 | 1.55 (1.2–2.0) | 1.57 (1.2–2.0) | <0.01 | 1 | 1.49 (0.8–2.8) | 2.46 (1.3–4.7) | 0.02 | 1.0 | 1.35 (1.0–1.7) | 1.45 (1.1–1.9) | <0.01 |
| b | 1 | 1.61 (1.2–2.1) | 1.74 (1.3–2.3) | <0.01 | 1 | 1.82 (0.9–3.5) | 3.05 (1.5–6.0) | <0.01 | 1.0 | 1.53 (1.2–2.0) | 1.59 (1.2–2.1) | <0.01 |
| c | 1 | 1.54 (1.1–2.0) | 1.62 (1.2–2.2) | <0.01 | 1 | 1.31 (0.6–2.7) | 2.10 (1.1–4.4) | 0.03 | 1.0 | 1.48 (1.1–2.0) | 1.48 (1.1–2.0) | <0.01 |
| e | 1 | 1.59 (1.2–2.1) | 1.63 (1.2–2.2) | <0.01 | 1 | 1.29 (0.6–2.5) | 2.12 (1.1–4.6) | 0.03 | 1.0 | 1.46 (1.1–2.0) | 1.47 (1.1–2.0) | <0.01 |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Wani, K.; Yakout, S.M.; Ansari, M.G.A.; Sabico, S.; Hussain, S.D.; Alokail, M.S.; Sheshah, E.; Aljohani, N.J.; Al-Saleh, Y.; Reginster, J.-Y.; et al. Metabolic Syndrome in Arab Adults with Low Bone Mineral Density. Nutrients 2019, 11, 1405. https://doi.org/10.3390/nu11061405
Wani K, Yakout SM, Ansari MGA, Sabico S, Hussain SD, Alokail MS, Sheshah E, Aljohani NJ, Al-Saleh Y, Reginster J-Y, et al. Metabolic Syndrome in Arab Adults with Low Bone Mineral Density. Nutrients. 2019; 11(6):1405. https://doi.org/10.3390/nu11061405
Chicago/Turabian StyleWani, Kaiser, Sobhy M. Yakout, Mohammed Ghouse Ahmed Ansari, Shaun Sabico, Syed Danish Hussain, Majed S. Alokail, Eman Sheshah, Naji J. Aljohani, Yousef Al-Saleh, Jean-Yves Reginster, and et al. 2019. "Metabolic Syndrome in Arab Adults with Low Bone Mineral Density" Nutrients 11, no. 6: 1405. https://doi.org/10.3390/nu11061405
APA StyleWani, K., Yakout, S. M., Ansari, M. G. A., Sabico, S., Hussain, S. D., Alokail, M. S., Sheshah, E., Aljohani, N. J., Al-Saleh, Y., Reginster, J.-Y., & Al-Daghri, N. M. (2019). Metabolic Syndrome in Arab Adults with Low Bone Mineral Density. Nutrients, 11(6), 1405. https://doi.org/10.3390/nu11061405







