Trends in Magnesium Intake among Hispanic Adults, the National Health and Nutrition Examination Survey (NHANES) 1999–2014
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Population
2.2. Assessments of Magnesium Intake
2.3. Statistical Analysis
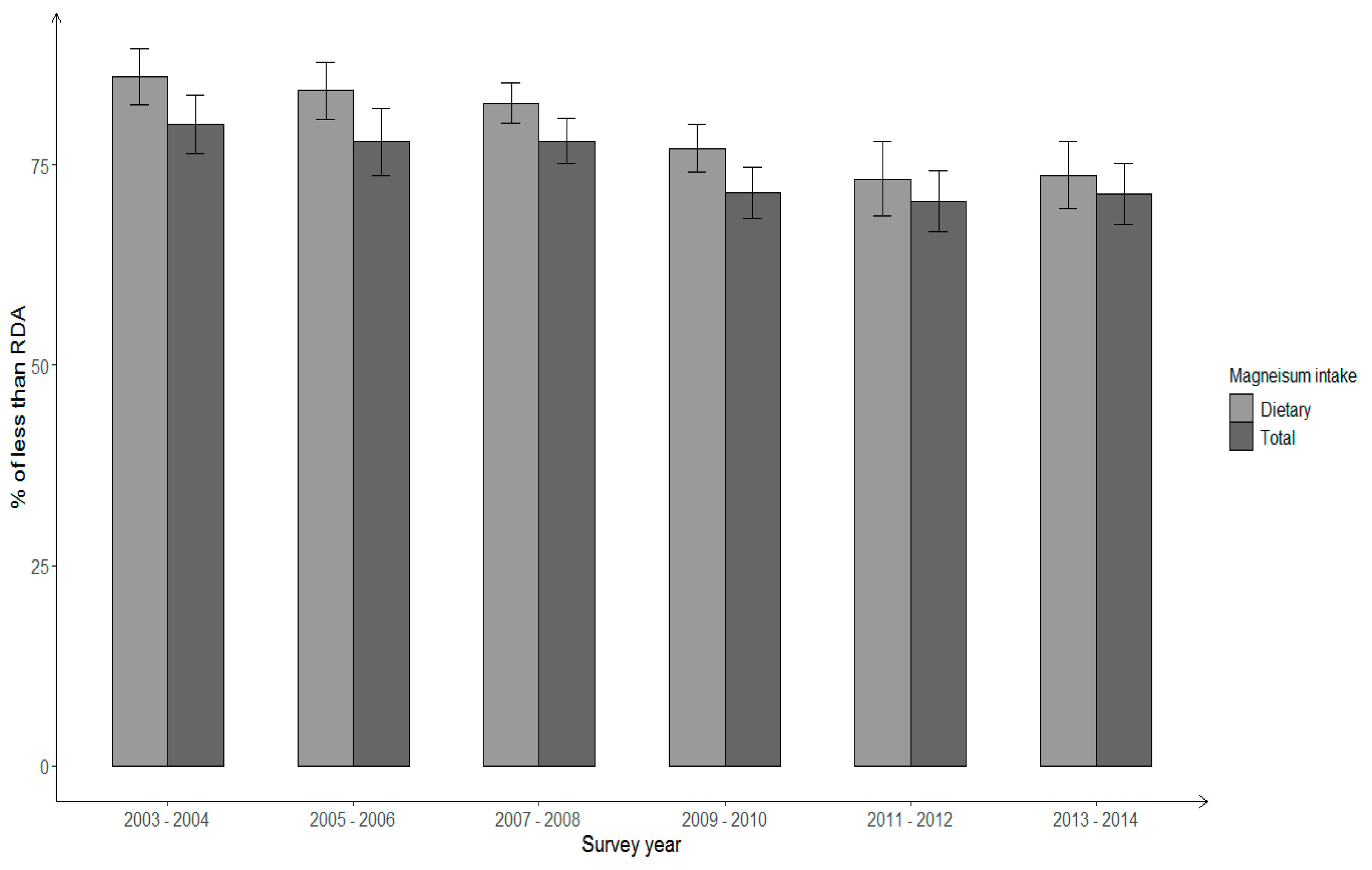
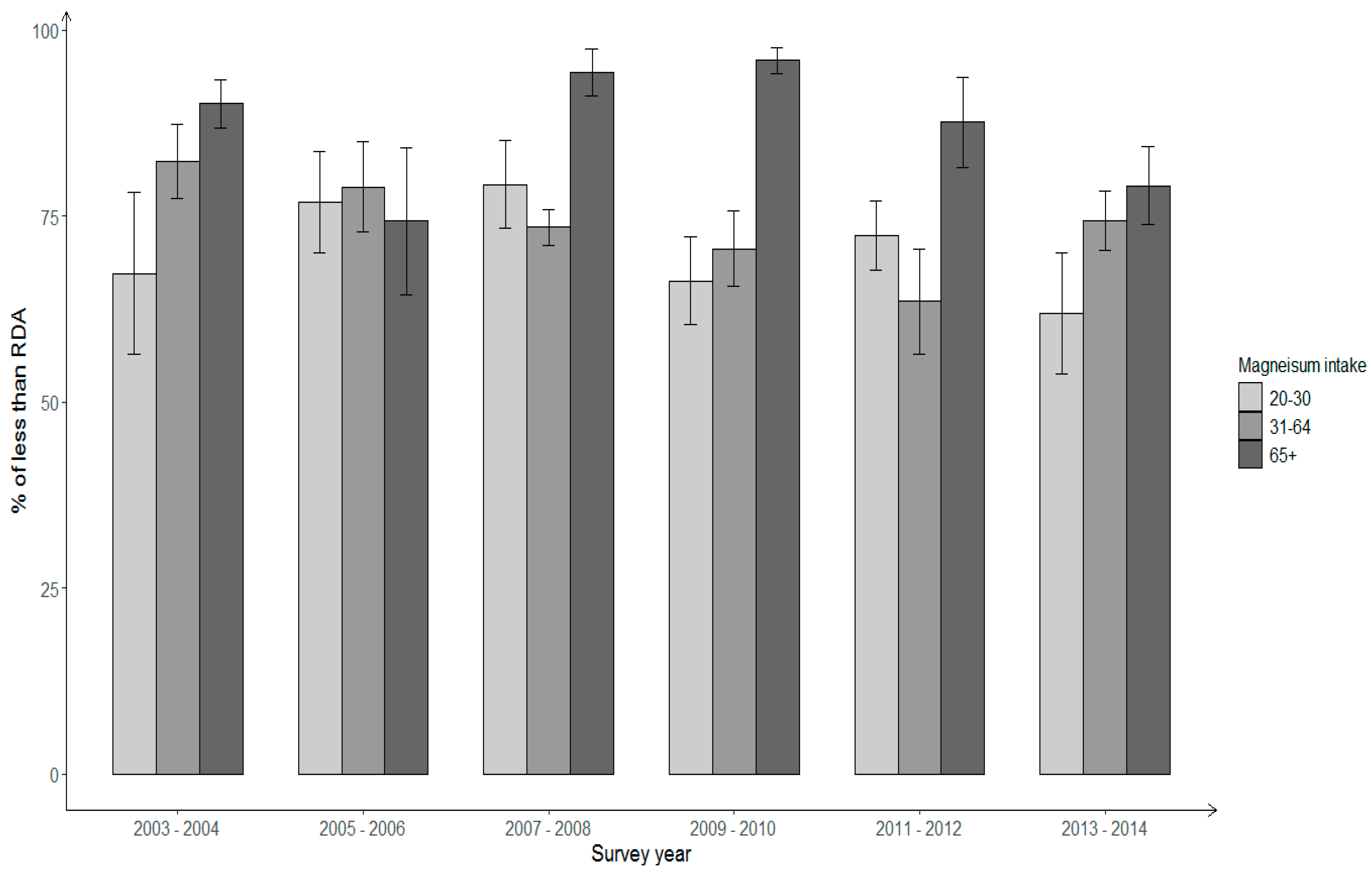
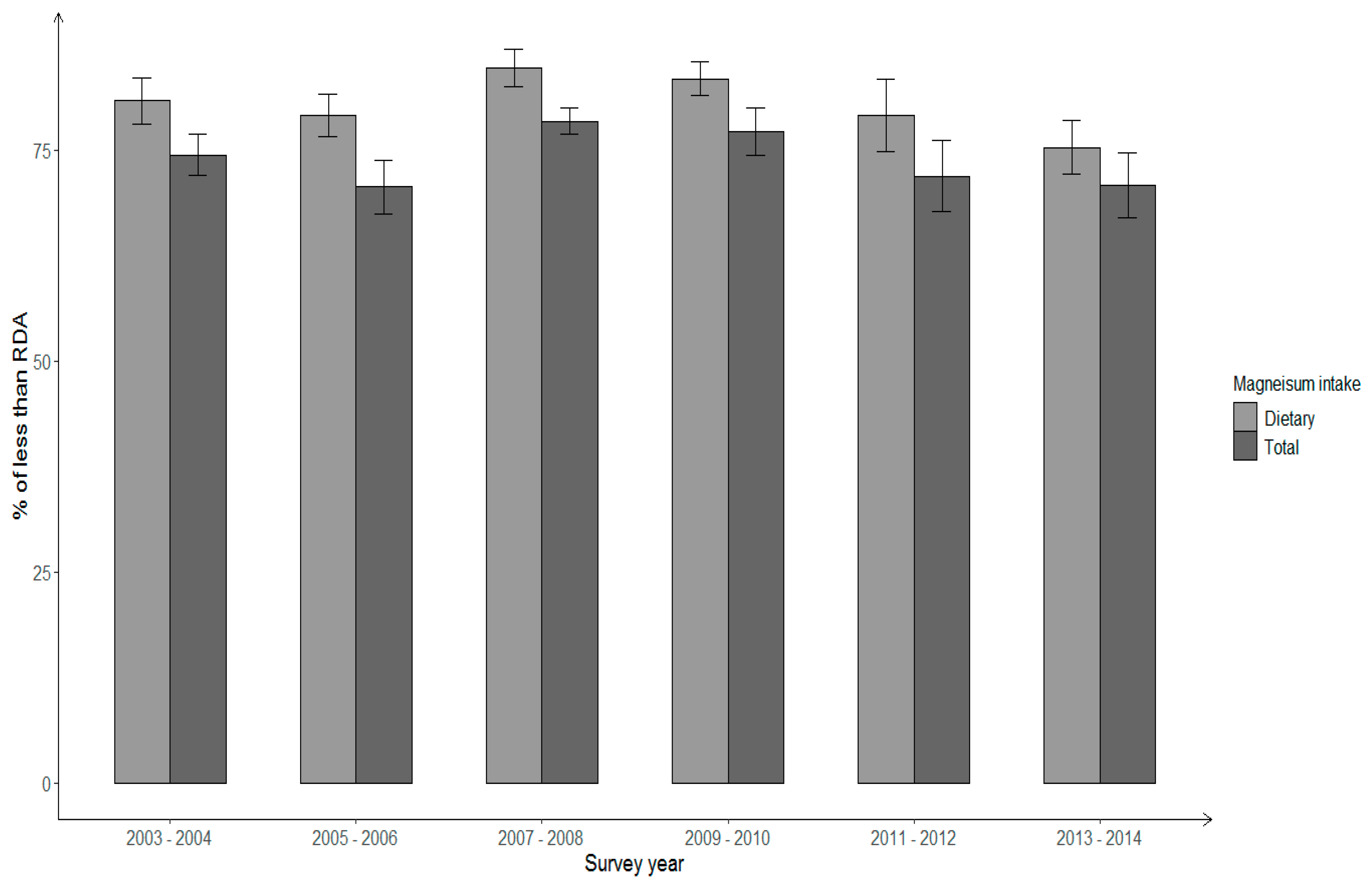
3. Results
4. Discussion
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Rosanoff, A.; Dai, Q.; Shapses, S.A. Essential nutrient interactions: Does low or suboptimal magnesium status interact with vitamin d and/or calcium status? Adv. Nutr. 2016, 7, 25–43. [Google Scholar] [CrossRef] [PubMed]
- Volpe, S.L. Magnesium in disease prevention and overall health. Adv. Nutr. 2013, 4, 378S–383S. [Google Scholar] [CrossRef] [PubMed]
- Zhang, Y.; Xun, P.; Wang, R.; Mao, L.; He, K. Can magnesium enhance exercise performance? Nutrients 2017, 9, 946. [Google Scholar] [CrossRef]
- Hayhoe, R.P.; Lentjes, M.A.; Luben, R.N.; Khaw, K.T.; Welch, A.A. Dietary magnesium and potassium intakes and circulating magnesium are associated with heel bone ultrasound attenuation and osteoporotic fracture risk in the epic-norfolk cohort study. Am. J. Clin. Nutr. 2015, 102, 376–384. [Google Scholar] [CrossRef] [PubMed]
- de Baaij, J.H.; Hoenderop, J.G.; Bindels, R.J. Magnesium in man: Implications for health and disease. Physiol. Rev. 2015, 95, 1–46. [Google Scholar] [CrossRef] [PubMed]
- Institute of Medicine (US) Standing Committee on the Scientific Evaluation of Dietary Reference Intakes. Dietary Reference Intakes for Calcium, Phosphorus, Magnesium, Vitamin D, and Fluoride; National Academies Press: Washington, DC, USA, 1997. [Google Scholar]
- Ross, A.C.; Caballero, B.; Cousins, R.J.; Tucker, K.L.; Ziegler, T.R. Modern Nutrition in Health and Disease, 11th ed.; Jones & Bartlett Learning: Philadelphia, PA, USA, 2012. [Google Scholar]
- Solati, M.; Ouspid, E.; Hosseini, S.; Soltani, N.; Keshavarz, M.; Dehghani, M. Oral magnesium supplementation in type ii diabetic patients. Med. J. Islamic Repub. Iran 2014, 28, 67. [Google Scholar]
- He, K.; Liu, K.; Daviglus, M.L.; Morris, S.J.; Loria, C.M.; Van Horn, L.; Jacobs, D.R., Jr.; Savage, P.J. Magnesium intake and incidence of metabolic syndrome among young adults. Circulation 2006, 113, 1675–1682. [Google Scholar] [CrossRef]
- Huang, J.-H.; Lu, Y.-F.; Cheng, F.-C.; Lee, J.N.-Y.; Tsai, L.-C. Correlation of magnesium intake with metabolic parameters, depression and physical activity in elderly type 2 diabetes patients: A cross-sectional study. Nutr. J. 2012, 11, 41. [Google Scholar] [CrossRef] [PubMed]
- Hopping, B.N.; Erber, E.; Grandinetti, A.; Verheus, M.; Kolonel, L.N.; Maskarinec, G. Dietary fiber, magnesium, and glycemic load alter risk of type 2 diabetes in a multiethnic cohort in hawaii. J. Nutr. 2009, 140, 68–74. [Google Scholar] [CrossRef] [PubMed]
- Hruby, A.; McKeown, N.; Song, Y.; Djoussé, L. Dietary magnesium and genetic interactions in diabetes and related risk factors: A brief overview of current knowledge. Nutrients 2013, 5, 4990–5011. [Google Scholar] [CrossRef]
- Del Gobbo, L.C.; Imamura, F.; Wu, J.H.; de Oliveira Otto, M.C.; Chiuve, S.E.; Mozaffarian, D. Circulating and dietary magnesium and risk of cardiovascular disease: A systematic review and meta-analysis of prospective studies. Am. J. Clin. Nutr. 2013, 98, 160–173. [Google Scholar] [CrossRef] [PubMed]
- Qu, X.; Jin, F.; Hao, Y.; Li, H.; Tang, T.; Wang, H.; Yan, W.; Dai, K. Magnesium and the risk of cardiovascular events: A meta-analysis of prospective cohort studies. PLoS ONE 2013, 8, e57720. [Google Scholar] [CrossRef] [PubMed]
- Jahnen-Dechent, W.; Ketteler, M. Magnesium basics. Clin. Kidney J. 2012, 5, i3–i14. [Google Scholar] [CrossRef] [PubMed]
- Chen, G.; Pang, Z.; Liu, Q. Magnesium intake and risk of colorectal cancer: A meta-analysis of prospective studies. Eur. J. Clin. Nutr. 2012, 66, 1182. [Google Scholar] [CrossRef] [PubMed]
- Ko, H.J.; Youn, C.H.; Kim, H.M.; Cho, Y.J.; Lee, G.H.; Lee, W.K. Dietary magnesium intake and risk of cancer: A meta-analysis of epidemiologic studies. Nutr. Cancer 2014, 66, 915–923. [Google Scholar] [CrossRef] [PubMed]
- Agarwal, S.; Reider, C.; Brooks, J.R.; Fulgoni, V.L., III. Comparison of prevalence of inadequate nutrient intake based on body weight status of adults in the united states: An analysis of nhanes 2001–2008. J. Am. Coll. Nutr. 2015, 34, 126–134. [Google Scholar] [CrossRef]
- U.S. Department of Health Human Services; U.S. Department of Agriculture. 2015–2020 Dietary Guidelines for American, 8th ed.; 2015. Available online: https://health.gov/dietaryguidelines/2015/guidelines/ (accessed on 3 June 2019).
- Fryar, C.D.; Wright, J.D.; Eberhardt, M.S.; Dye, B.A. Trends in Nutrient Intakes and Chronic Health Conditions Among Mexican-American Adults, a 25-Year Profile: United States, 1982–2006. Natl Health Stat Report 2012, 28, 1–20. [Google Scholar]
- Cason, K.; Nieto-Montenegro, S.; Chavez-Martinez, A. Food choices, food sufficiency practices, and nutrition education needs of hispanic migrant workers in pennsylvania. Top. Clin. Nutr. 2006, 21, 145–158. [Google Scholar] [CrossRef][Green Version]
- Haile, R.W.; John, E.M.; Levine, A.J.; Cortessis, V.K.; Unger, J.B.; Gonzales, M.; Ziv, E.; Thompson, P.; Spruijt-Metz, D.; Tucker, K.L. A review of cancer in us hispanic populations. Cancer Prev. Res. 2012, 5, 150–163. [Google Scholar] [CrossRef]
- Ford, E.S.; Giles Wh Fau-Dietz, W.H.; Dietz, W.H. Prevalence of the metabolic syndrome among us adults: Findings from the third national health and nutrition examination survey. JAMA 2002, 287, 356–359. [Google Scholar] [CrossRef]
- Menke, A.; Casagrande, S.; Geiss, L.; Cowie, C.C. Prevalence of and trends in diabetes among adults in the united states, 1988–2012 prevalence of and trends in diabetes among us adultsprevalence of and trends in diabetes among us adults. JAMA 2015, 314, 1021–1029. [Google Scholar] [CrossRef] [PubMed]
- Johnson, C.L.; Dohrmann, S.M.; Burt, V.; Mohadjer, L.K. National health and nutrition examination survey: Sample design, 2011–2014. Vital Health Stat. 2 2014, 162, 1–33. [Google Scholar]
- Centers for Disease Control and Prevention. National Health and Nutrition Examination Survey Mec in-Person Dietary Interviewers Procedures Manual; Department of Health and Human Services (US): Hyattsville, MD, USA, 2002.
- Blanton, C.A.; Moshfegh, A.J.; Baer, D.J.; Kretsch, M.J. The usda automated multiple-pass method accurately estimates group total energy and nutrient intake. J. Nutr. 2006, 136, 2594–2599. [Google Scholar] [CrossRef] [PubMed]
- Moshfegh, A.J.; Rhodes, D.G.; Baer, D.J.; Murayi, T.; Clemens, J.C.; Rumpler, W.V.; Paul, D.R.; Sebastian, R.S.; Kuczynski, K.J.; Ingwersen, L.A. The us department of agriculture automated multiple-pass method reduces bias in the collection of energy intakes. Am. J. Clin. Nutr. 2008, 88, 324–332. [Google Scholar] [CrossRef] [PubMed]
- Ahluwalia, N.; Dwyer, J.; Terry, A.; Moshfegh, A.; Johnson, C. Update on nhanes dietary data: Focus on collection, release, analytical considerations, and uses to inform public policy. Adv. Nutr. 2016, 7, 121–134. [Google Scholar] [CrossRef] [PubMed]
- Tooze, J.A.; Midthune, D.; Dodd, K.W.; Freedman, L.S.; Krebs-Smith, S.M.; Subar, A.F.; Guenther, P.M.; Carroll, R.J.; Kipnis, V. A new statistical method for estimating the usual intake of episodically consumed foods with application to their distribution. J. Am. Diet. Assoc. 2006, 106, 1575–1587. [Google Scholar] [CrossRef] [PubMed]
- Halton, T.L.; Willett, W.C.; Liu, S.; Manson, J.E.; Stampfer, M.J.; Hu, F.B. Potato and french fry consumption and risk of type 2 diabetes in women. Am. J. Clin. Nutr. 2006, 83, 284–290. [Google Scholar] [CrossRef]
- Bowen, D.J.; Jabson, J.M.; Barrington, W.E.; Littman, A.J.; Patrick, D.L.; Moudon, A.V.; Albano, D.; Beresford, S.A.A. Environmental and individual predictors of healthy dietary behaviors in a sample of middle aged hispanic and caucasian women. Int. J. Environ. Res. Public Health 2018, 15, 2277. [Google Scholar] [CrossRef]
- Welch, A.A.; Skinner, J.; Hickson, M. Dietary magnesium may be protective for aging of bone and skeletal muscle in middle and younger older age men and women: Cross-sectional findings from the uk biobank cohort. Nutrients 2017, 9, 1189. [Google Scholar] [CrossRef]
- Andrews, K.W.; Gusev, P.A.; Dang, P.; Savarala, S.; Oh, L.; Atkinson, R.; McNeal, M. Adult Multivitamin/Mineral (Amvm-2017) Dietary Supplement Study Research Summary; 2017. Available online: https://dietarysupplementdatabase.usda.nih.gov/dsid_database/Res%20Summ%20DSID%204%20Adult%20MVM-8-2-17%20final.pdf (accessed on 21 May 2019).
- Bailey, R.L.; Fulgoni III, V.L.; Keast, D.R.; Dwyer, J.T. Dietary supplement use is associated with higher intakes of minerals from food sources. Am. J. Clin. Nutr. 2011, 94, 1376–1381. [Google Scholar] [CrossRef]
- Roark, R.A.; Niederhauser, V.P. Fruit and vegetable intake: Issues with definition and measurement. Public Health Nutr. 2013, 16, 2–7. [Google Scholar] [CrossRef] [PubMed]
| Demographics a | 1999–2000 | 2001–2002 | 2003–2004 | 2005–2006 | 2007–2008 | 2009–2010 | 2011–2012 | 2013–2014 |
|---|---|---|---|---|---|---|---|---|
| (n = 1288) | (n = 1087) | (n = 928) | (n = 911) | (n = 1475) | (n = 1603) | (n = 914) | (n = 1098) | |
| Age, years | ||||||||
| 20–34 | 314 (39.0) | 343 (41.1) | 231 (39.4) | 324 (42.1) | 396 (38.5) | 426 (37.7) | 252 (39.2) | 277 (37.2) |
| 35–49 | 345 (31.9) | 335 (34.8) | 244 (37.0) | 271 (34.7) | 390 (33.9) | 477 (36.4) | 240 (32.6) | 334 (35.9) |
| 50–64 | 318 (18.9) | 209 (14.8) | 183 (14.6) | 183 (15.6) | 431 (18.8) | 440 (16.9) | 273 (19.7) | 300 (18.3) |
| ≥65 | 311 (10.2) | 200 (9.3) | 270 (8.9) | 133 (7.6) | 258 (8.8) | 260 (9.1) | 149 (8.4) | 187 (8.6) |
| Gender | ||||||||
| Male | 633 (49.2) | 574 (53.0) | 488 (53.8) | 491 (54.1) | 711 (53.8) | 779 (53.4) | 471 (52.3) | 528 (51.4) |
| Female | 655 (50.8) | 513 (47.0) | 440 (46.2) | 420 (45.9) | 764 (46.2) | 824 (46.6) | 443 (47.7) | 570 (48.6) |
| Race/Ethnicity | ||||||||
| Mexican American | 1037 (46.3) | 902 (52.8) | 808 (68.1) | 784 (68.8) | 894 (63.1) | 1029 (62.8) | 456 (55.1) | 652 (61.1) |
| Other Hispanic | 251 (53.7) | 185 (47.2) | 120 (31.9) | 127 (31.2) | 581 (36.9) | 574 (37.2) | 458 (44.9) | 446 (38.9) |
| PIR b | ||||||||
| <1.0 | 307 (25.4) | 256 (28.2) | 267 (27.4) | 266 (27.5) | 364 (28.5) | 436 (33.3) | 264 (32.1) | 297 (30.1) |
| 1.0–1.84 | 374 (32.7) | 301 (28.1) | 252 (25.4) | 239 (29.4) | 376 (29.4) | 387 (28.0) | 222 (25.3) | 256 (26.8) |
| ≥1.85 | 398 (41.9) | 450 (43.7) | 359 (47.2) | 347 (43.2) | 553 (42.1) | 537 (38.7) | 344 (42.6) | 413 (43.2) |
| Supplement use | ||||||||
| Yes | 291 (25.5) | 255 (22.1) | 244 (23.9) | 206 (23.8) | 335 (20.6) | 367 (21.9) | 187 (19.7) | 226 (18.7) |
| Factors | 1999–2000 | 2001–2002 | 2003–2004 | 2005–2006 | 2007–2008 | 2009–2010 | 2011–2012 | 2013–2014 | p-Value for Trend a |
|---|---|---|---|---|---|---|---|---|---|
| (n = 1288) | (n = 1087) | (n = 928) | (n = 911) | (n = 1475) | (n = 1603) | (n = 914) | (n = 1098) | ||
| Overall | 275.06 ± 7.20 | 275.72 ± 7.49 | 290.87 ± 6.15 | 302.80 ± 7.21 | 296.40 ± 7.45 | 307.19 ± 5.35 | 315.06 ± 8.69 | 319.21 ± 7.54 | <0.0001 |
| Gender | |||||||||
| Male | 317.08 ± 10.31 | 317.92 ± 6.91 | 328.15 ± 10.28 | 333.57 ± 9.31 | 336.31 ± 7.88 | 354.59 ± 8.33 | 359.79 ± 11.90 | 364.68 ± 9.79 | <0.0001 |
| Female | 236.62 ± 11.98 | 227.57 ± 9.69 | 250.07 ± 7.44 | 265.70 ± 7.18 | 250.86 ± 8.38 | 255.87 ± 6.39 | 266.02 ± 7.63 | 272.82 ± 6.86 | <0.0001 |
| Race/Ethnicity | |||||||||
| Mexican American | 282.49 ± 8.39 | 292.79 ± 5.98 | 299.91 ± 7.61 | 311.02 ± 9.29 | 299.20 ± 9.31 | 320.87 ± 7.02 | 327.79 ± 11.96 | 327.83 ± 10.79 | <0.0001 |
| Other Hispanic | 269.09 ± 9.93 | 254.14 ± 8.50 | 267.99 ± 13.01 | 279.56 ± 14.18 | 291.65 ± 9.43 | 284.98 ± 6.86 | 299.05 ± 10.40 | 305.20 ± 10.29 | <0.0001 |
| Age, years | |||||||||
| 20–34 | 284.31 ± 11.01 | 278.37 ± 8.40 | 319.75 ± 12.95 | 301.16 ± 8.93 | 293.57 ± 12.46 | 316.10 ± 9.78 | 320.33 ± 11.77 | 324.83 ± 13.60 | <0.0001 |
| 35–49 | 283.87 ± 10.34 | 278.09 ± 8.34 | 278.93 ± 12.54 | 317.90 ± 9.35 | 318.85 ± 10.85 | 318.74 ± 10.03 | 329.81 ± 11.60 | 319.28 ± 4.37 | <0.0001 |
| 50–64 | 264.81 ± 18.80 | 290.35 ± 16.76 | 264.00 ± 13.11 | 299.99 ± 20.03 | 290.48 ± 7.83 | 290.20 ± 5.95 | 304.61 ± 12.25 | 326.90 ± 12.14 | <0.0001 |
| ≥65 | 231.40 ± 18.15 | 231.57 ± 12.79 | 255.64 ± 13.90 | 259.46 ± 18.71 | 241.18 ± 6.21 | 258.69 ± 7.797 | 264.52 ± 10.47 | 280.61 ± 10.67 | <0.0001 |
| PIR | |||||||||
| <1.0 | 240.83 ± 11.90 | 240.97 ± 15.78 | 261.40 ± 12.47 | 290.48 ± 17.98 | 277.88 ± 16.53 | 300.17 ± 8.08 | 302.61 ± 14.66 | 298.43 ± 9.15 | <0.0001 |
| 1.0–1.84 | 263.40 ± 13.96 | 273.43 ± 11.46 | 305.30 ± 12.46 | 298.77 ± 12.12 | 283.43 ± 12.84 | 309.75 ± 7.59 | 320.73 ± 17.25 | 346.06 ± 13.36 | <0.0001 |
| ≥1.85 | 303.08 ± 13.07 | 297.16 ± 8.55 | 299.52 ± 10.25 | 308.57 ± 11.91 | 316.34 ± 6.28 | 310.82 ± 10.69 | 320.48 ± 9.47 | 318.31 ± 9.44 | <0.0001 |
| Factors | 1999–2000 | 2001–2002 | 2003–2004 | 2005–2006 | 2007–2008 | 2009–2010 | 2011–2012 | 2013–2014 | p-Value for Trend a |
|---|---|---|---|---|---|---|---|---|---|
| (n = 1288) | (n = 1087) | (n = 928) | (n = 911) | (n = 1475) | (n = 1603) | (n = 914) | (n = 1098) | ||
| Overall | 303.89 ± 7.35 | 296.74 ± 6.73 | 312.43 ± 5.95 | 323.68 ± 8.36 | 313.97 ± 8.27 | 323.28 ± 5.78 | 329.90 ± 9.18 | 331.78 ± 8.11 | <0.0001 |
| Gender | |||||||||
| Male | 343.22 ± 8.06 | 340.40 ± 6.67 | 347.55 ± 11.47 | 353.72 ± 10.69 | 356.22 ± 10.95 | 370.19 ± 8.65 | 372.67 ± 12.35 | 373.03 ± 10.47 | <0.0001 |
| Female | 267.92 ± 14.48 | 246.92 ± 9.48 | 273.99 ± 6.32 | 287.47 ± 7.92 | 265.77 ± 7.56 | 272.49 ± 8.23 | 283.00 ± 7.77 | 289.70 ± 8.37 | <0.0001 |
| Race/Ethnicity | |||||||||
| Mexican American | 307.88 ± 8.78 | 316.66 ± 6.72 | 320.00 ± 8.29 | 331.09 ± 10.62 | 312.56 ± 10.21 | 338.18 ± 7.18 | 343.74 ± 12.75 | 338.67 ± 11.30 | <0.0001 |
| Other Hispanic | 300.69 ± 9.82 | 271.56 ± 7.78 | 293.26 ± 12.98 | 302.75 ± 15.14 | 316.34 ± 13.46 | 299.08 ± 7.86 | 312.48 ± 11.03 | 320.59 ± 10.51 | <0.0001 |
| Age, years | |||||||||
| 20–34 | 302.85 ± 10.52 | 292.77 ± 6.24 | 329.04 ± 12.58 | 315.91 ± 11.11 | 311.09 ± 14.78 | 328.27 ± 9.71 | 325.15 ± 11.89 | 330.46 ± 13.58 | <0.0001 |
| 35 – 49 | 318.30 ± 12.99 | 299.24 ± 9.86 | 297.57 ± 11.63 | 340.48 ± 12.40 | 333.25 ± 10.27 | 332.38 ± 11.35 | 353.80 ± 14.62 | 330.91 ± 5.85 | <0.0001 |
| 50 – 64 | 305.08 ± 25.58 | 322.17 ± 15.66 | 306.78 ± 20.91 | 320.92 ± 15.85 | 312.61 ± 8.53 | 316.09 ± 7.75 | 324.81 ± 14.65 | 341.32 ± 13.67 | 0.0010 |
| ≥ 65 | 260.98 ± 12.22 | 264.64 ± 15.28 | 305.24 ± 22.85 | 301.27 ± 22.14 | 260.67 ± 7.91 | 281.71 ± 7.17 | 278.84 ± 12.93 | 320.26 ± 21.53 | 0.0046 |
| PIR | |||||||||
| <1.0 | 263.48 ± 11.03 | 265.28 ± 15.79 | 271.48 ± 13.14 | 297.22 ± 18.19 | 286.04 ± 16.83 | 311.95 ± 8.36 | 310.76 ± 14.86 | 308.53 ± 9.74 | <0.0001 |
| 1.0–1.84 | 283.82 ± 13.83 | 287.52 ± 9.48 | 330.10 ± 11.56 | 320.32 ± 9.39 | 299.26 ± 13.56 | 323.62 ± 8.21 | 328.20 ± 17.03 | 361.14 ± 12.52 | <0.0001 |
| ≥1.85 | 341.34 ± 13.44 | 323.35 ± 9.67 | 326.78 ± 10.91 | 338.44 ± 13.24 | 343.16 ± 9.64 | 333.50 ± 12.57 | 346.33 ± 10.35 | 331.97 ± 10.37 | <0.0001 |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Liu, J.; Huang, Y.; Dai, Q.; Fulda, K.G.; Chen, S.; Tao, M.-H. Trends in Magnesium Intake among Hispanic Adults, the National Health and Nutrition Examination Survey (NHANES) 1999–2014. Nutrients 2019, 11, 2867. https://doi.org/10.3390/nu11122867
Liu J, Huang Y, Dai Q, Fulda KG, Chen S, Tao M-H. Trends in Magnesium Intake among Hispanic Adults, the National Health and Nutrition Examination Survey (NHANES) 1999–2014. Nutrients. 2019; 11(12):2867. https://doi.org/10.3390/nu11122867
Chicago/Turabian StyleLiu, Jialiang, Yuhan Huang, Qi Dai, Kimberly G. Fulda, Shande Chen, and Meng-Hua Tao. 2019. "Trends in Magnesium Intake among Hispanic Adults, the National Health and Nutrition Examination Survey (NHANES) 1999–2014" Nutrients 11, no. 12: 2867. https://doi.org/10.3390/nu11122867
APA StyleLiu, J., Huang, Y., Dai, Q., Fulda, K. G., Chen, S., & Tao, M.-H. (2019). Trends in Magnesium Intake among Hispanic Adults, the National Health and Nutrition Examination Survey (NHANES) 1999–2014. Nutrients, 11(12), 2867. https://doi.org/10.3390/nu11122867





