Effects of High vs. Low Glycemic Index of Post-Exercise Meals on Sleep and Exercise Performance: A Randomized, Double-Blind, Counterbalanced Polysomnographic Study
Abstract
1. Introduction
2. Materials and Methods
2.1. Participants
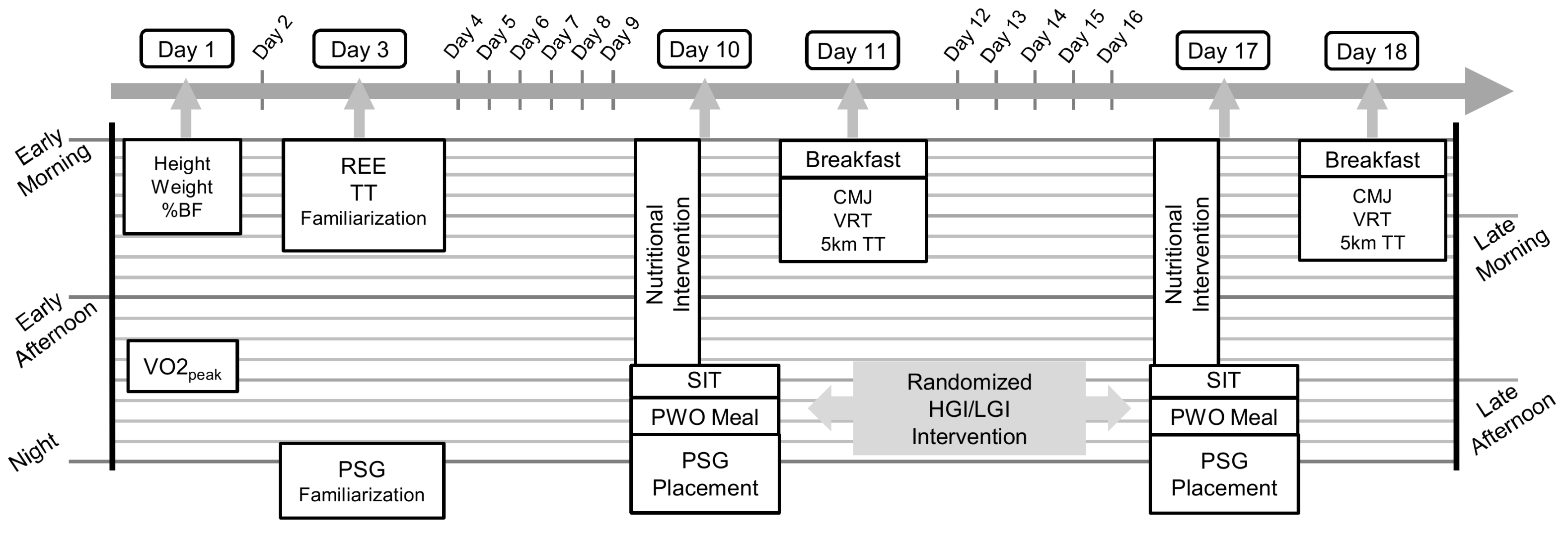
2.2. Study Design
2.3. Preliminary Testing
2.4. Nutritional Intervention and Assessment of Dietary Intake
2.5. Sprint Interval Training Regime
2.6. Polysomnography
2.7. Exercise Performance Testing
2.8. Statistical Analysis
3. Results
3.1. Preliminary Data
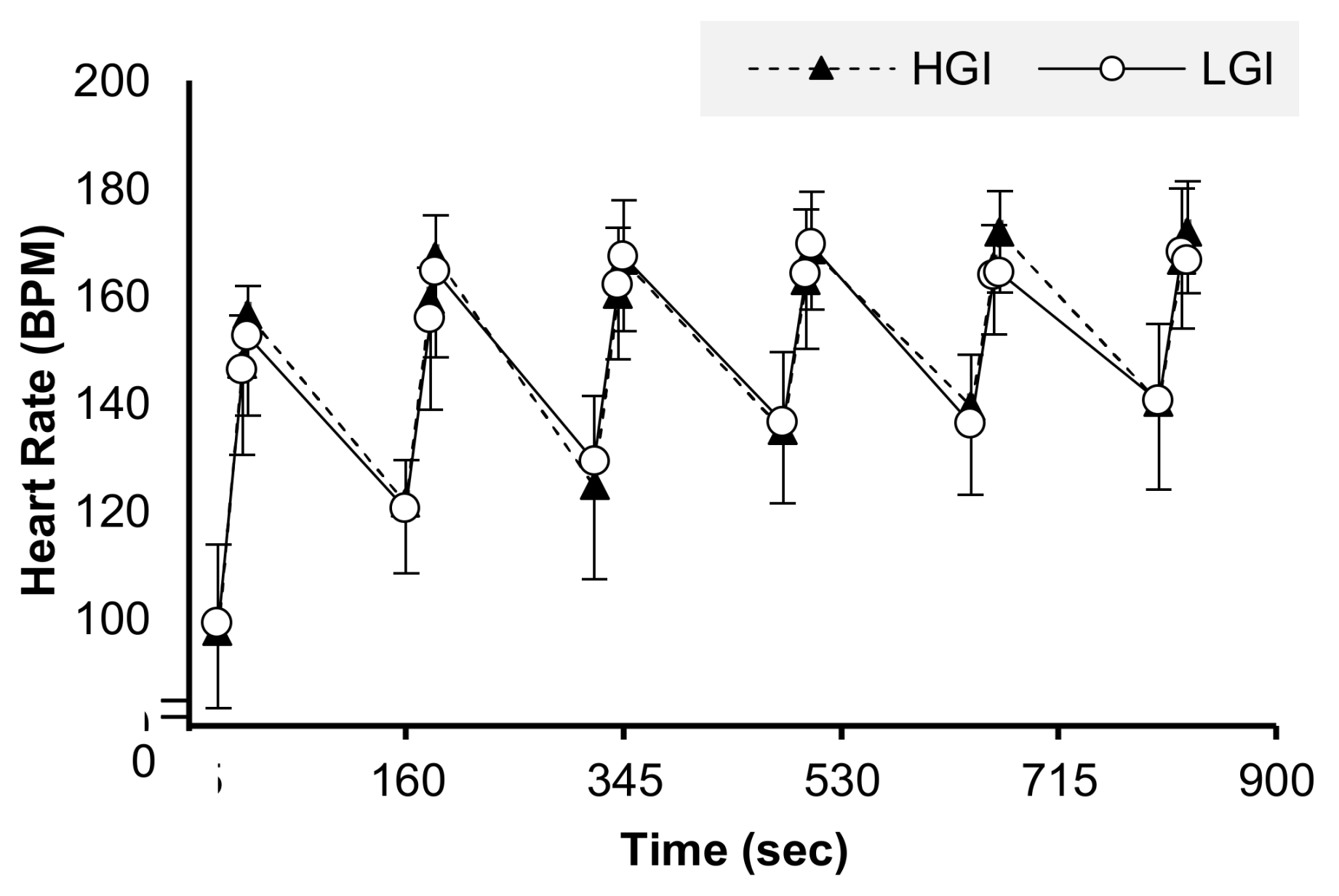
3.2. SIT-related Data
3.3. Polysomnography-Related Data
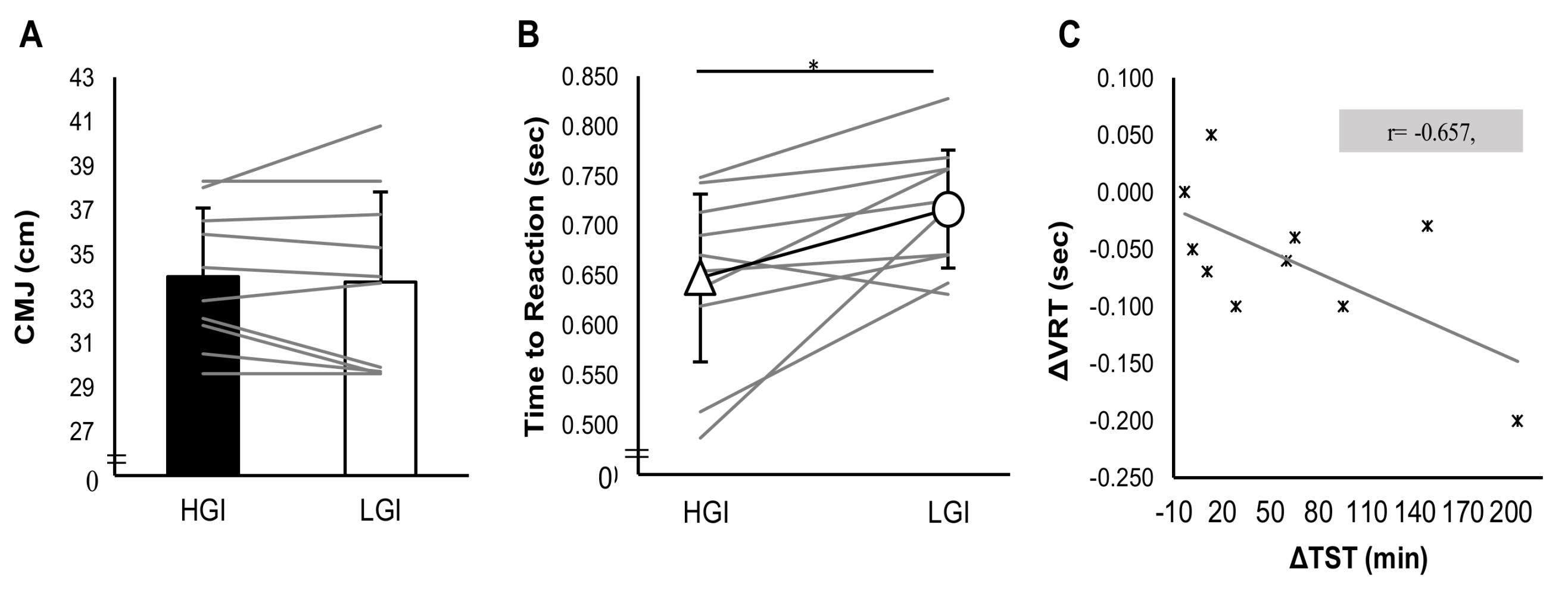
3.4. Exercise Performance Data
3.5. Correlations Between Sleep-Related Parameters and Exercise Performance-Related Parameters
3.6. Statistical Power
4. Discussion
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Leeder, J.; Glaister, M.; Pizzoferro, K.; Dawson, J.; Pedlar, C. Sleep duration and quality in elite athletes measured using wristwatch actigraphy. J. Sports Sci. 2012, 30, 541–545. [Google Scholar] [CrossRef] [PubMed]
- Swinbourne, R.; Gill, N.; Vaile, J.; Smart, D. Prevalence of poor sleep quality, sleepiness and obstructive sleep apnoea risk factors in athletes. Eur. J. Sport Sci. 2016, 16, 850–858. [Google Scholar] [CrossRef] [PubMed]
- Drew, M.; Vlahovich, N.; Hughes, D.; Appaneal, R.; Burke, L.M.; Lundy, B.; Rogers, M.; Toomey, M.; Watts, D.; Lovell, G.; et al. Prevalence of illness, poor mental health and sleep quality and low energy availability prior to the 2016 Summer Olympic Games. Br. J. Sports Med. 2018, 52, 47–53. [Google Scholar] [CrossRef] [PubMed]
- Vitale, J.A.; Bonato, M.; Galasso, L.; La Torre, A.; Merati, G.; Montaruli, A.; Roveda, E.; Carandente, F. Sleep quality and high intensity interval training at two different times of day: A crossover study on the influence of the chronotype in male collegiate soccer players. Chronobiol. Int. 2017, 34, 260–268. [Google Scholar] [CrossRef] [PubMed]
- MacInnis, M.J.; Gibala, M.J. Physiological adaptations to interval training and the role of exercise intensity. J. Physiol. 2017, 595, 2915–2930. [Google Scholar] [CrossRef] [PubMed]
- Halson, S.L. Sleep in elite athletes and nutritional interventions to enhance sleep. Sports Med. 2014, 44 (Suppl. 1), S13–S23. [Google Scholar] [CrossRef]
- Rae, D.E.; Chin, T.; Dikgomo, K.; Hill, L.; McKune, A.J.; Kohn, T.A.; Roden, L.C. One night of partial sleep deprivation impairs recovery from a single exercise training session. Eur. J. Appl. Physiol. 2017, 117, 699–712. [Google Scholar] [CrossRef] [PubMed]
- Youngstedt, S.D. Effects of exercise on sleep. Clin. Sports Med. 2005, 24, 355–365. [Google Scholar] [CrossRef] [PubMed]
- Pallesen, S.; Gundersen, H.S.; Kristoffersen, M.; Bjorvatn, B.; Thun, E.; Harris, A. The Effects of Sleep Deprivation on Soccer Skills. Percept. Mot. Skills 2017, 124, 812–829. [Google Scholar] [CrossRef] [PubMed]
- Skein, M.; Wingfield, G.; Gale, R.; Washington, T.L.; Minett, G.M. Sleep quantity and quality during consecutive day heat training with the inclusion of cold-water immersion recovery. J. Therm. Biol. 2018, 74, 63–70. [Google Scholar] [CrossRef] [PubMed]
- Wada, K.; Yata, S.; Akimitsu, O.; Krejci, M.; Noji, T.; Nakade, M.; Takeuchi, H.; Harada, T. A tryptophan-rich breakfast and exposure to light with low color temperature at night improve sleep and salivary melatonin level in Japanese students. J. Circadian Rhythms 2013, 11, 4. [Google Scholar] [CrossRef] [PubMed]
- Pigeon, W.R.; Carr, M.; Gorman, C.; Perlis, M.L. Effects of a tart cherry juice beverage on the sleep of older adults with insomnia: A pilot study. J. Med. Food 2010, 13, 579–583. [Google Scholar] [CrossRef] [PubMed]
- Silber, B.Y.; Schmitt, J.A. Effects of tryptophan loading on human cognition, mood, and sleep. Neurosci. Biobehav. Rev. 2010, 34, 387–407. [Google Scholar] [CrossRef] [PubMed]
- Porter, J.M.; Horne, J.A. Bed-time food supplements and sleep: Effects of different carbohydrate levels. Electroencephalogr. Clin. Neurophysiol. 1981, 51, 426–433. [Google Scholar] [CrossRef]
- Afaghi, A.; O’Connor, H.; Chow, C.M. High-glycemic-index carbohydrate meals shorten sleep onset. Am.J. Clin. Nutr. 2007, 85, 426–430. [Google Scholar] [CrossRef] [PubMed]
- Thomas, D.T.; Erdman, K.A.; Burke, L.M. American College of Sports Medicine Joint Position Statement. Nutrition and Athletic Performance. Med. Sci. Sports Exerc. 2016, 48, 543–568. [Google Scholar] [CrossRef] [PubMed]
- Phillips, S.M.; Sproule, J.; Turner, A.P. Carbohydrate ingestion during team games exercise: Current knowledge and areas for future investigation. Sports Med. 2011, 41, 559–585. [Google Scholar] [CrossRef] [PubMed]
- Fernstrom, J.D.; Wurtman, R.J. Brain serotonin content: Physiological regulation by plasma neutral amino acids. Science 1972, 178, 414–416. [Google Scholar] [CrossRef] [PubMed]
- Jackson, A.S.; Pollock, M.L. Generalized equations for predicting body density of men. Br. J. Nutr. 1978, 40, 497–504. [Google Scholar] [CrossRef] [PubMed]
- Compher, C.; Frankenfield, D.; Keim, N.; Roth-Yousey, L.; Evidence Analysis Working, G. Best practice methods to apply to measurement of resting metabolic rate in adults: A systematic review. J. Am. Diet. Assoc. 2006, 106, 881–903. [Google Scholar] [CrossRef] [PubMed]
- Atkinson, F.S.; Foster-Powell, K.; Brand-Miller, J.C. International tables of glycemic index and glycemic load values: 2008. Diabetes Care 2008, 31, 2281–2283. [Google Scholar] [CrossRef] [PubMed]
- Petit, E.; Mougin, F.; Bourdin, H.; Tio, G.; Haffen, E. A 20-min nap in athletes changes subsequent sleep architecture but does not alter physical performances after normal sleep or 5-h phase-advance conditions. Eur. J. Appl. Physiol. 2014, 114, 305–315. [Google Scholar] [CrossRef] [PubMed]
- Berry, R.B.; Gamaldo, C.E.; Harding, S.M.; Brooks, R.; Lloyd, R.M.; Vaughn, B.V.; Marcus, C.L. AASM Scoring Manual Version 2.2 Updates: New Chapters for Scoring Infant Sleep Staging and Home Sleep Apnea Testing. J. Clin. Sleep Med. 2015, 11, 1253–1254. [Google Scholar] [CrossRef] [PubMed]
- Afaghi, A.; O’Connor, H.; Chow, C.M. Acute effects of the very low carbohydrate diet on sleep indices. Nutr. Neurosci. 2008, 11, 146–154. [Google Scholar] [CrossRef] [PubMed]
- Ferracioli-Oda, E.; Qawasmi, A.; Bloch, M.H. Meta-analysis: Melatonin for the treatment of primary sleep disorders. PLoS ONE 2013, 8, e63773. [Google Scholar] [CrossRef] [PubMed]
- Cheikh, M.; Hammouda, O.; Gaamouri, N.; Driss, T.; Chamari, K.; Cheikh, R.B.; Dogui, M.; Souissi, N. Melatonin ingestion after exhaustive late-evening exercise improves sleep quality and quantity, and short-term performances in teenage athletes. Chronobiol. Int. 2018, 1–13. [Google Scholar] [CrossRef] [PubMed]
- Herrera, C.P. Total sleep time in Muslim football players is reduced during Ramadan: A pilot study on the standardized assessment of subjective sleep-wake patterns in athletes. J. Sports Sci. 2012, 30 (Suppl. 1), S85–S91. [Google Scholar] [CrossRef]
- Wurtman, R.J.; Hefti, F.; Melamed, E. Precursor control of neurotransmitter synthesis. Pharmacol. Rev. 1980, 32, 315–335. [Google Scholar] [PubMed]
- Fidalgo, S.; Ivanov, D.K.; Wood, S.H. Serotonin: From top to bottom. Biogerontology 2013, 14, 21–45. [Google Scholar] [CrossRef] [PubMed]
- Brzezinski, A. Melatonin in humans. N. Engl. J. Med. 1997, 336, 186–195. [Google Scholar] [CrossRef] [PubMed]
- Ortega, J.F.; Fernandez-Elias, V.E.; Hamouti, N.; Pallares, J.G.; Mora-Rodriguez, R. Higher insulin-sensitizing response after sprint interval compared to continuous exercise. Int. J. Sports Med. 2015, 36, 209–214. [Google Scholar] [CrossRef] [PubMed]
- Kamdar, B.B.; Kaplan, K.A.; Kezirian, E.J.; Dement, W.C. The impact of extended sleep on daytime alertness, vigilance, and mood. Sleep Med. 2004, 5, 441–448. [Google Scholar] [CrossRef] [PubMed]
- Taheri, M.; Arabameri, E. The effect of sleep deprivation on choice reaction time and anaerobic power of college student athletes. Asian J. Sports Med. 2012, 3, 15–20. [Google Scholar] [CrossRef] [PubMed]
- Mah, C.D.; Mah, K.E.; Kezirian, E.J.; Dement, W.C. The effects of sleep extension on the athletic performance of collegiate basketball players. Sleep 2011, 34, 943–950. [Google Scholar] [CrossRef] [PubMed]
- Swinbourne, R.; Miller, J.; Smart, D.; Dulson, D.K.; Gill, N. The Effects of Sleep Extension on Sleep, Performance, Immunity and Physical Stress in Rugby Players. Sports 2018, 6, 42. [Google Scholar] [CrossRef] [PubMed]
- Fullagar, H.; Skorski, S.; Duffield, R.; Meyer, T. The effect of an acute sleep hygiene strategy following a late-night soccer match on recovery of players. Chronobiol. Int. 2016, 33, 490–505. [Google Scholar] [CrossRef] [PubMed]
- Skein, M.; Duffield, R.; Minett, G.M.; Snape, A.; Murphy, A. The effect of overnight sleep deprivation after competitive rugby league matches on postmatch physiological and perceptual recovery. Int. J. Sports Physiol. Perform. 2013, 8, 556–564. [Google Scholar] [CrossRef] [PubMed]
- Lucas, S.J.; Anson, J.G.; Palmer, C.D.; Hellemans, I.J.; Cotter, J.D. The impact of 100 hours of exercise and sleep deprivation on cognitive function and physical capacities. J. Sports Sci. 2009, 27, 719–728. [Google Scholar] [CrossRef] [PubMed]
- Heung-Sang Wong, S.; Sun, F.H.; Chen, Y.J.; Li, C.; Zhang, Y.J.; Ya-Jun Huang, W. Effect of pre-exercise carbohydrate diets with high vs low glycemic index on exercise performance: A meta-analysis. Nutr. Rev. 2017, 75, 327–338. [Google Scholar] [CrossRef] [PubMed]
- Ormsbee, M.J.; Gorman, K.A.; Miller, E.A.; Baur, D.A.; Eckel, L.A.; Contreras, R.J.; Panton, L.B.; Spicer, M.T. Nighttime feeding likely alters morning metabolism but not exercise performance in female athletes. Appl. Physiol. Nutr. Metab. 2016, 41, 719–727. [Google Scholar] [CrossRef] [PubMed]
- Oliver, S.J.; Costa, R.J.; Laing, S.J.; Bilzon, J.L.; Walsh, N.P. One night of sleep deprivation decreases treadmill endurance performance. Eur. J. Appl. Physiol. 2009, 107, 155–161. [Google Scholar] [CrossRef] [PubMed]
- Chase, J.D.; Roberson, P.A.; Saunders, M.J.; Hargens, T.A.; Womack, C.J.; Luden, N.D. One night of sleep restriction following heavy exercise impairs 3-km cycling time-trial performance in the morning. Appl. Physiol. Nutr. Metab. 2017, 42, 909–915. [Google Scholar] [CrossRef] [PubMed]
- O’Donnell, S.; Bird, S.; Jacobson, G.; Driller, M. Sleep and stress hormone responses to training and competition in elite female athletes. Eur. J. Sport Sci. 2018, 18, 611–618. [Google Scholar] [CrossRef] [PubMed]
- Killer, S.C.; Svendsen, I.S.; Jeukendrup, A.E.; Gleeson, M. Evidence of disturbed sleep and mood state in well-trained athletes during short-term intensified training with and without a high carbohydrate nutritional intervention. J. Sports Sci. 2017, 35, 1402–1410. [Google Scholar] [CrossRef] [PubMed]
| HGI Trial | LGI Trial | p value | |
|---|---|---|---|
| TST (min) | 426.0 ± 71.7 | 363.6 ± 49.0 | 0.019 * |
| N1 (%) | 14.2 ± 8.8 | 15.2 ± 10.4 | 0.059 |
| N2 (%) | 34.5 ± 13.1 | 33.4 ± 9.8 | 0.741 |
| N3 (%) | 20.8 ± 10.8 | 22.7 ± 13.3 | 0.495 |
| REM (%) | 28.6 ± 10.9 | 28.8 ± 12.2 | 0.959 |
| SE (%) | 89.0 ± 4.3 | 80.9 ± 10.6 | 0.049 * |
| SOL (min) | 5.7 ± 1.9 | 24.6 ± 8.1 | 0.026 * |
| REM onset latency (min) | 55.9 ± 39.4 | 84.8 ± 51.8 | 0.286 |
| Deep sleep onset latency (min) | 57.2 ± 66.8 | 62.6 ± 44.6 | 0.132 |
| Total wake time (min) | 47.4 ± 21.7 | 80.3 ± 43.6 | 0.034 * |
| Arousal index (number/h) | |||
| REM | 22.6 ± 8.6 | 22.1 ± 12.1 | 0.871 |
| NREM | 16.4 ± 7 | 18.4 ± 10.1 | 0.371 |
| Total | 18.5 ± 6.8 | 19.9 ± 10 | 0.239 |
| HGI Trial | LGI Trial | p value | |
|---|---|---|---|
| 5-km TT (sec) | 461.6 ± 45.3 | 475.4 ± 53.3 | 0.441 |
| Wavg | 143.9 ± 35.7 | 145.0 ± 35.7 | 0.877 |
| Wmax | 212.5 ± 84.3 | 221.5 ± 61.3 | 0.621 |
| RPMave | 98.6 ± 10.3 | 95.6 ± 11.5 | 0.444 |
| RPMmax | 129.3 ± 20.5 | 129.0 ± 24.2 | 0.963 |
| HRstart | 99.7 ± 20.7 | 91.7 ± 17.2 | 0.019 * |
| HRave | 152.2 ± 14.6 | 148.4 ± 12.8 | 0.189 |
| HRmax | 173.9 ± 10.4 | 169.4 ± 10.1 | 0.077 |
| HRend | 173.3 ± 10.4 | 166.0 ± 10.0 | 0.010 * |
| Exercise Performance-Related Parameters | CMJ (cm) | VRTmin (sec) | VRTmax (sec) | VRTaverage (sec) | 5 km TT (min) |
|---|---|---|---|---|---|
| Sleep-Related Parameters | |||||
| TST (min) | −0.277 | −0.051 | −0.093 | −0.171 | −0.055 |
| N1 (%) | 0.276 | −0.002 | −0.155 | −0.086 | −0.033 |
| N2 (%) | −0.137 | −0.2 | −0.29 | −0.278 | −0.114 |
| N3 (%) | 0.091 | −0.03 | 0.101 | 0.085 | 0.149 |
| REM (%) | −0.08 | 0.197 | 0.303 | 0.247 | 0.073 |
| SE (%) | 0.103 | −0.222 | −0.089 | −0.108 | 0.023 |
| SOL (min) | −0.118 | 0.417 | 0.367 | 0.329 | 0.186 |
| REM onset latency(min) | −0.182 | 0.208 | 0.24 | 0.289 | −0.002 |
| Deep sleep onset latency (min) | −0.237 | 0.489 * | 0.321 | 0.361 | 0.012 |
| Total wake time (min) | −0.068 | 0.247 | 0.159 | 0.206 | −0.121 |
| Arousal index (no/h) | |||||
| REM | 0.325 | −0.005 | −0.148 | −0.128 | −0.004 |
| NREM | 0.148 | 0.123 | 0.063 | 0.07 | 0.105 |
| Total | 0.229 | 0.125 | 0.004 | 0.02 | 0.067 |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Vlahoyiannis, A.; Aphamis, G.; Andreou, E.; Samoutis, G.; Sakkas, G.K.; Giannaki, C.D. Effects of High vs. Low Glycemic Index of Post-Exercise Meals on Sleep and Exercise Performance: A Randomized, Double-Blind, Counterbalanced Polysomnographic Study. Nutrients 2018, 10, 1795. https://doi.org/10.3390/nu10111795
Vlahoyiannis A, Aphamis G, Andreou E, Samoutis G, Sakkas GK, Giannaki CD. Effects of High vs. Low Glycemic Index of Post-Exercise Meals on Sleep and Exercise Performance: A Randomized, Double-Blind, Counterbalanced Polysomnographic Study. Nutrients. 2018; 10(11):1795. https://doi.org/10.3390/nu10111795
Chicago/Turabian StyleVlahoyiannis, Angelos, George Aphamis, Eleni Andreou, George Samoutis, Giorgos K. Sakkas, and Christoforos D. Giannaki. 2018. "Effects of High vs. Low Glycemic Index of Post-Exercise Meals on Sleep and Exercise Performance: A Randomized, Double-Blind, Counterbalanced Polysomnographic Study" Nutrients 10, no. 11: 1795. https://doi.org/10.3390/nu10111795
APA StyleVlahoyiannis, A., Aphamis, G., Andreou, E., Samoutis, G., Sakkas, G. K., & Giannaki, C. D. (2018). Effects of High vs. Low Glycemic Index of Post-Exercise Meals on Sleep and Exercise Performance: A Randomized, Double-Blind, Counterbalanced Polysomnographic Study. Nutrients, 10(11), 1795. https://doi.org/10.3390/nu10111795








