A Pilot Clinical Study of Liquid Ubiquinol Supplementation on Cardiac Function in Pediatric Dilated Cardiomyopathy
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Design and Subjects
2.2. Intervention
2.3. Anthropometric and Hematologic Measurements
2.4. Assessments of Cardiac Function and Symptoms of Heart Failure
2.5. Statistical Analysis
3. Results
3.1. Characteristics of the Subjects
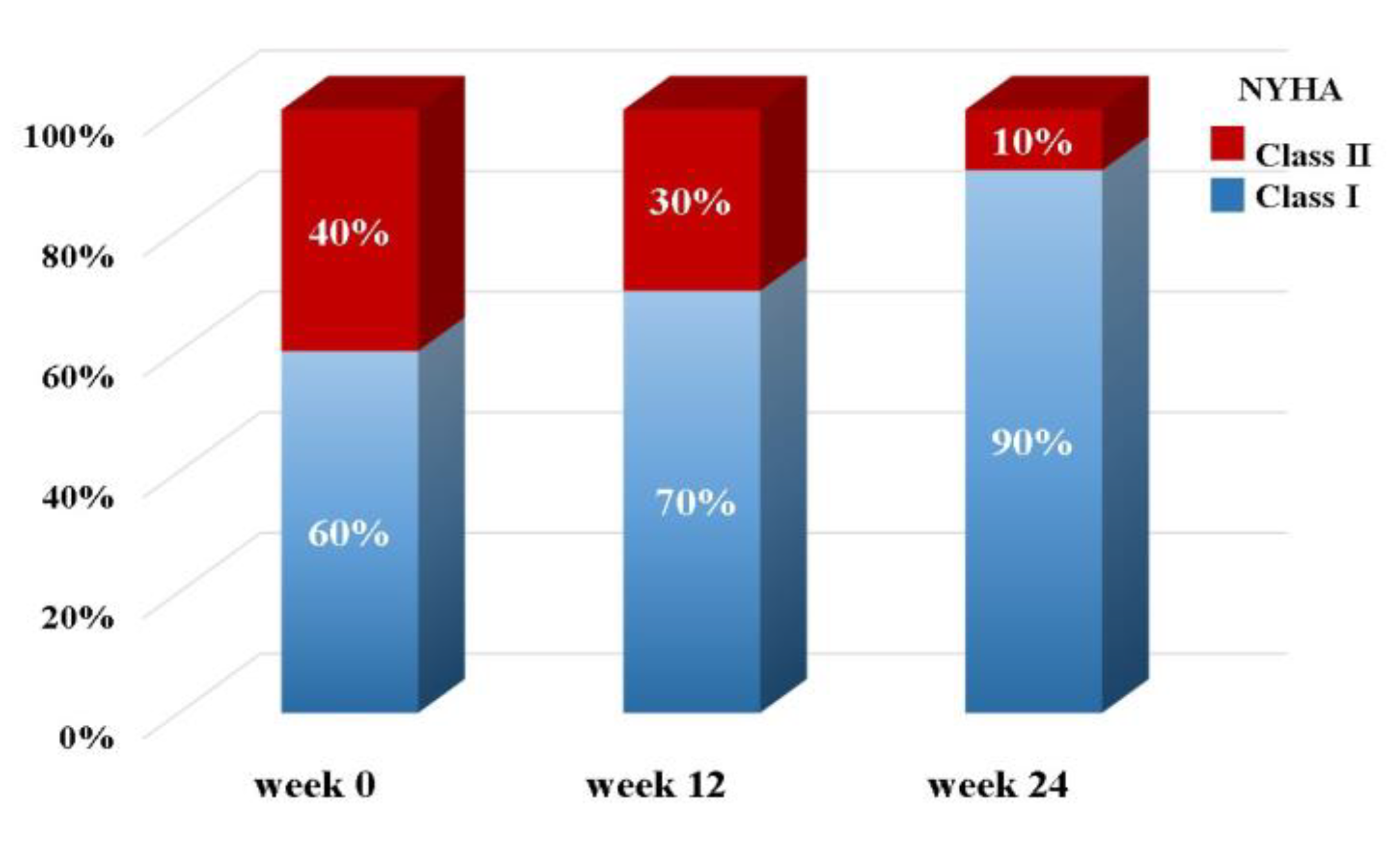
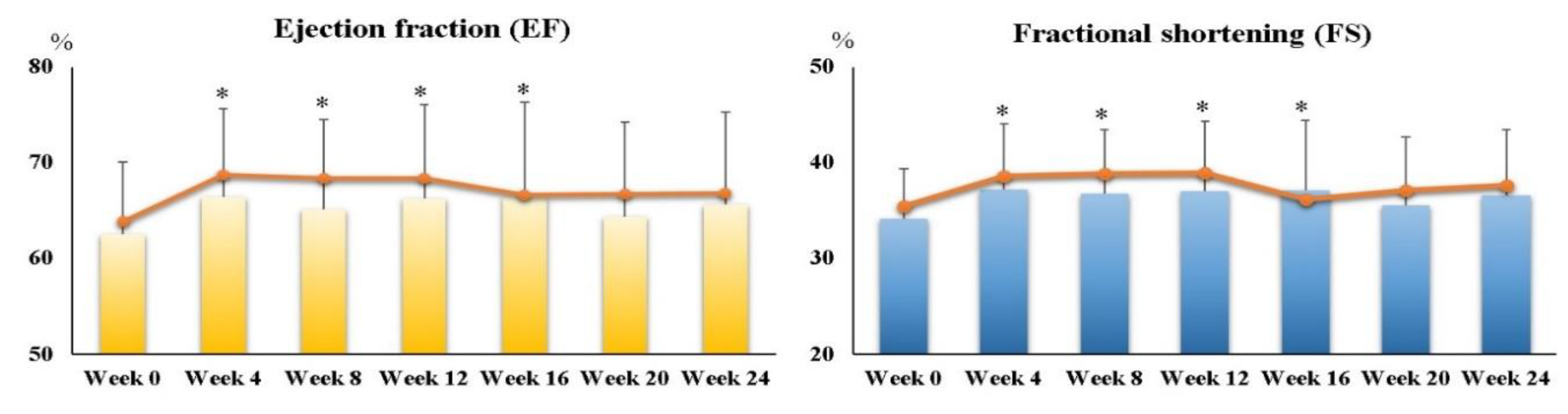
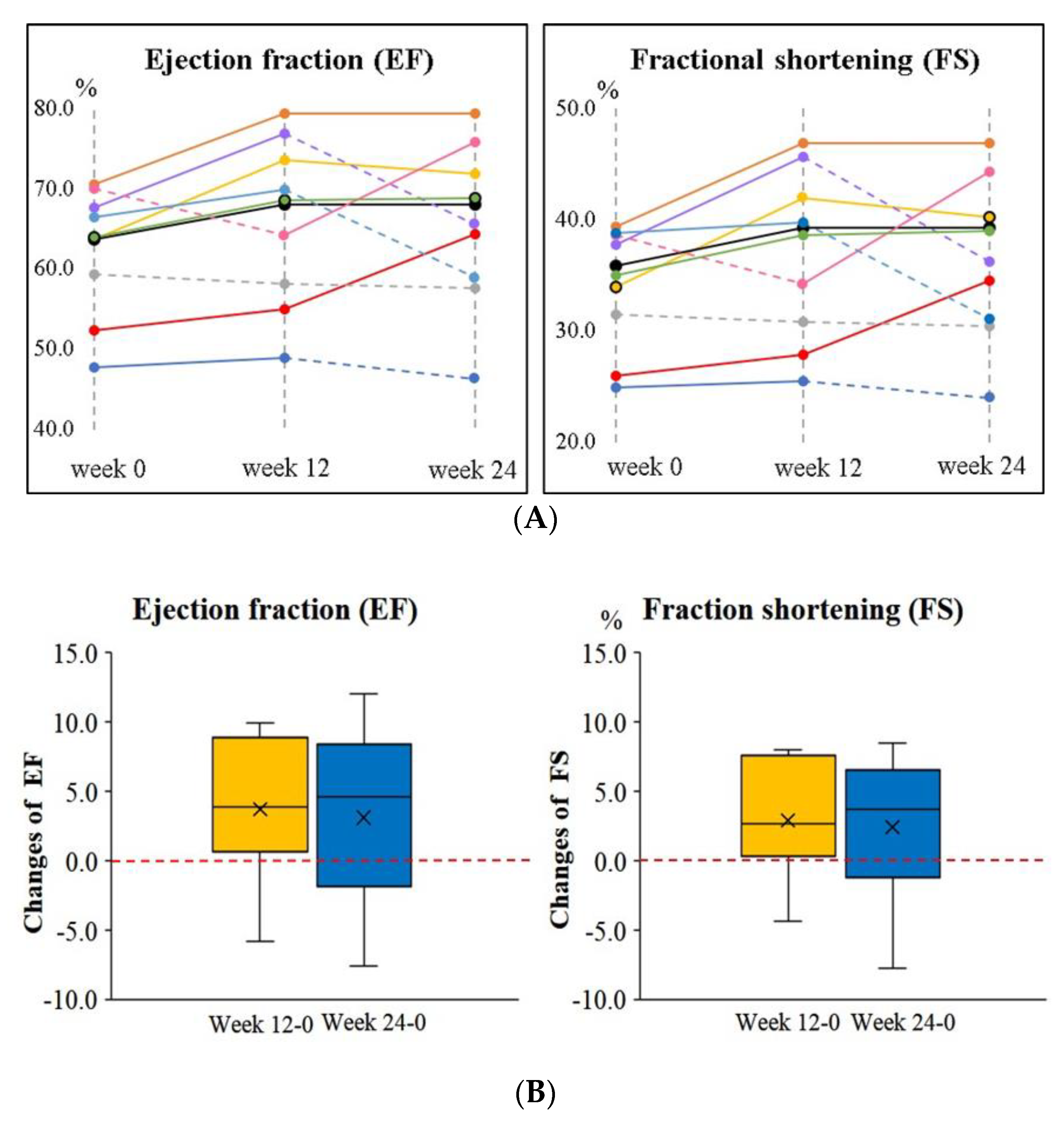
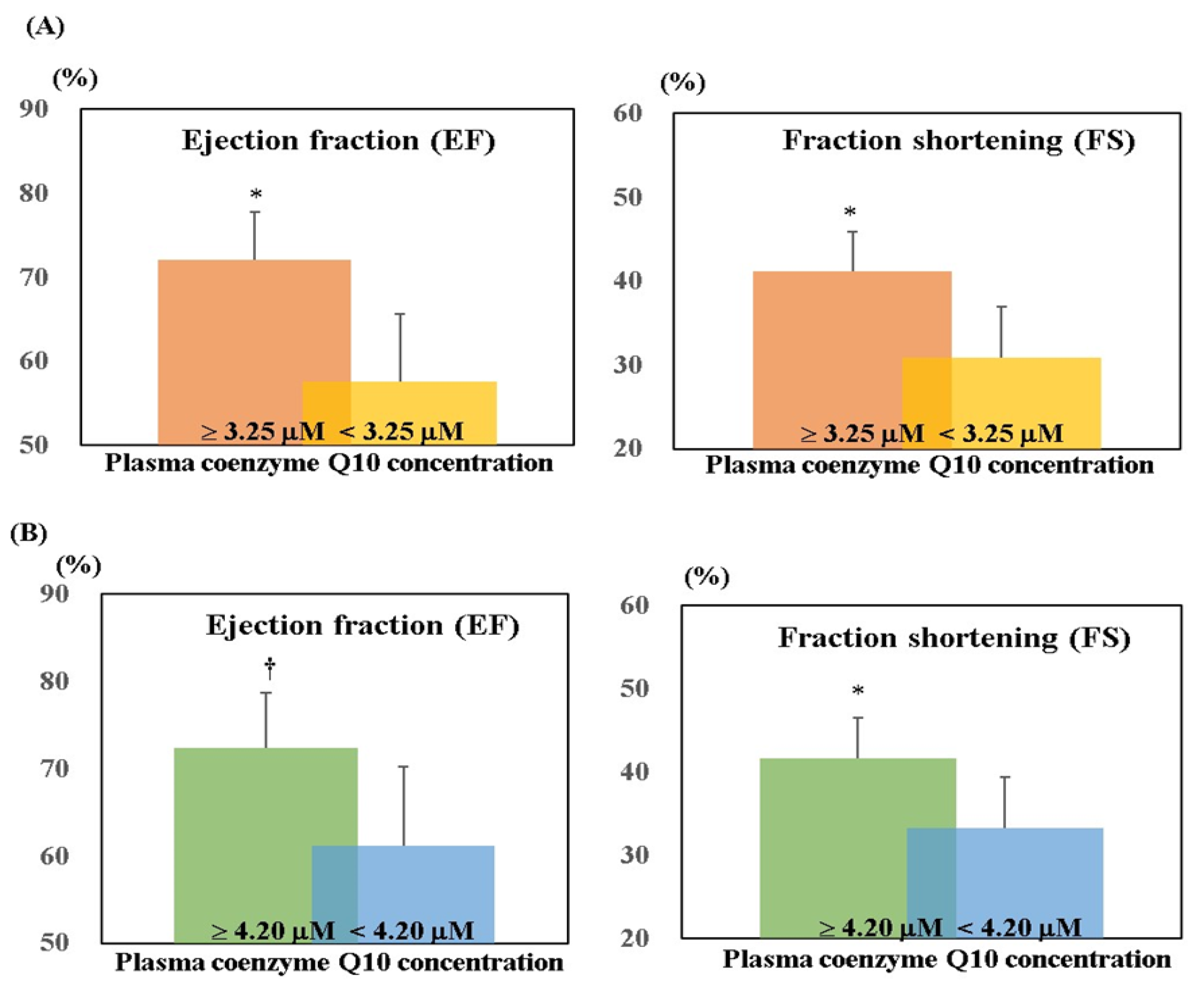
3.2. Cardiac Function and Symptoms of Heart Failure after Supplementation
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
Abbreviations
| ATP | adenosine triphosphate |
| BNP | B-type natriuretic peptide |
| CI | cardiac index |
| CK | creatine kinase |
| CK-MB | creatine kinase-muscle/brain |
| CO | cardiac output |
| EDV | end-diastolic volume |
| EF | ejection fractions |
| ESV | end-systolic volume |
| ET | ejection time |
| FS | fractional shortening |
| HR | heart rate |
| ICT | isovolumetric contraction time |
| IRT | isovolumetric relaxation time |
| LVIDd | left ventricular internal diameter end-diastole |
| LVIDs | left ventricular internal diameter end-systole |
| LVOTd | left ventricular outflow tract diameter |
| MPI | myocardial performance index |
| NT-pro BNP | N-terminal pro BNP |
| NYHA | New York Heart Association |
| PDCM | pediatric dilated cardiomyopathy |
| SV | stroke volume |
References
- Nugent, A.W.; Daubeney, P.E.; Chondros, P.; Carlin, J.B.; Cheung, M.; Wilkinson, L.C.; Davis, A.M.; Kahler, S.G.; Chow, C.W.; Wilkinson, J.L.; et al. The epidemiology of childhood cardiomyopathy in Australia. N. Engl. J. Med. 2003, 348, 1639–1646. [Google Scholar] [CrossRef]
- Oh, J.H.; Hong, Y.M.; Choi, J.Y.; Kim, S.J.; Jung, J.W.; Sohn, S.; Hyun, M.C.; Noh, C.I.; Lee, J.W.; Park, I.S. Idiopathic cardiomyopathies in Korean children. 9-Year Korean Multicenter Study. Circ. J. 2011, 75, 2228–2234. [Google Scholar] [CrossRef]
- Lipshultz, S.E.; Cochran, T.R.; Briston, D.A.; Brown, S.R.; Sambatakos, P.J.; Miller, T.L.; Carrillo, A.A.; Corcia, L.; Sanchez, J.E.; Diamond, M.B.; et al. Pediatric cardiomyopathies: Causes, epidemiology, clinical course, preventive strategies and therapies. Future Cardiol. 2013, 9, 817–848. [Google Scholar] [CrossRef]
- Towbin, J.A.; Lowe, A.M.; Colan, S.D.; Sleeper, L.A.; Orav, E.J.; Clunie, S.; Messere, J.; Cox, G.F.; Lurie, P.R.; Hsu, D.; et al. Incidence, causes, and outcomes of dilated cardiomyopathy in children. JAMA 2006, 296, 1867–1876. [Google Scholar] [CrossRef]
- Franklin, O.; Burch, M. Dilated cardiomyopathy in childhood. Images Paediatr. Cardiol. 2000, 2, 3–10. [Google Scholar]
- Morrow, W.R. Cardiomyopathy and heart transplantation in children. Curr. Opin. Cardiol. 2000, 15, 216–223. [Google Scholar] [CrossRef]
- Birnbaum, B.F.; Simpson, K.E.; Canter, C.E. Heart transplantation in pediatric cardiomyopathies. Expert Rev. Cardiovasc. Ther. 2013, 11, 1677–1690. [Google Scholar] [CrossRef]
- Weng, K.P.; Lin, C.C.; Huang, S.H.; Hsieh, K.S. Idiopathic dilated cardiomyopathy in children: A single medical center’s experience. J. Chin. Med. Assoc. 2005, 68, 368–372. [Google Scholar] [CrossRef]
- Ernster, L.; Dallner, G. Biochemical, physiological and medical aspects of ubiquinone function. Biochim. Biophys. Acta 1995, 1271, 195–204. [Google Scholar] [CrossRef]
- Siemieniuk, E.; Skrzydlewska, E. Coenzyme Q10: Its biosynthesis and biological significance in animal organisms and in humans. Postepy Hig. Med. Dosw. 2005, 59, 150–159. [Google Scholar]
- Bentinger, M.; Tekle, M.; Dallner, G. Coenzyme Q–biosynthesis and functions. Biochem. Biophys. Res. Commun. 2010, 396, 74–79. [Google Scholar] [CrossRef]
- Mae, T.; Sakamoto, Y.; Morikawa, S.; Hidaka, T. Pharmacetical Compostition Comprising Coenzyme Q10. U.S. Patent 6,184,255B1, 6 February 2001. [Google Scholar]
- Bhagavan, H.N.; Chopra, R.K. Plasma coenzyme Q10 response to oral ingestion of coenzyme Q10 formulations. Mitochondrion 2007, 7, S78–S88. [Google Scholar] [CrossRef]
- Elshershari, H.; Ozer, S.; Ozkutlu, S.; Ozme, S. Potential usefulness of coenzyme Q10 in the treatment of idiopathic dilated cardiomyopathy in children. Int. J. Cardiol. 2003, 88, 101–102. [Google Scholar] [CrossRef]
- Soongswang, J.; Sangtawesin, C.; Durongpisitkul, K.; Laohaprasitiporn, D.; Nana, A.; Punlee, K.; Kangkagate, C. The effect of coenzyme Q10 on idiopathic chronic dilated cardiomyopathy in children. Pediatr. Cardiol. 2005, 26, 361–366. [Google Scholar] [CrossRef] [PubMed]
- Kocharian, A.; Shabanian, R.; Rafiei-Khorgami, M.; Kiani, A.; Heidari-Bateni, G. Coenzyme Q10 improves diastolic function in children with idiopathic dilated cardiomyopathy. Cardiol. Young 2009, 19, 501–506. [Google Scholar] [CrossRef] [PubMed]
- Zmitek, J.; Smidovnik, A.; Fir, M.; Prosek, M.; Zmitek, K.; Walczak, J.; Pravst, I. Relative bioavailability of two forms of a novel water-soluble coenzyme Q10. Ann. Nutr. MeTab. 2008, 52, 281–287. [Google Scholar] [CrossRef] [PubMed]
- Bergamini, C.; Moruzzi, N.; Sblendido, A.; Lenaz, G.; Fato, R. A water soluble CoQ10 formulation improves intracellular distribution and promotes mitochondrial respiration in cultured cells. PLoS ONE 2012, 7, e33712. [Google Scholar] [CrossRef]
- Littarru, G.P.; Mosca, F.; Fattorini, D.; Bompadre, S. Method to Assay Coenzyme Q10 in Blood Plasma or Blood Serum. U.S. Patent 7,303,921, 4 December 2007. [Google Scholar]
- Soja, A.M.; Mortensen, S.A. Treatment of congestive heart failure with coenzyme Q10 illuminated by meta-analyses of clinical trials. Mol. Asp. Med. 1997, 18, S159–S168. [Google Scholar] [CrossRef]
- Langsjoen, P.H.; Langsjoen, A.M. Coenzyme Q10 in cardiovascular disease with emphasis on heart failure and myocardial ischaemia. Asia Pac. Heart J. 1998, 7, 160–168. [Google Scholar] [CrossRef]
- Sander, S.; Coleman, C.I.; Patel, A.A.; Kluger, J.; White, C.M. The impact of coenzyme Q10 on systolic function in patients with chronic heart failure. J. Card. Fail. 2006, 12, 464–472. [Google Scholar] [CrossRef]
- Fotino, A.D.; Thompson-Paul, A.M.; Bazzano, L.A. Effect of coenzyme Q₁₀ supplementation on heart failure: A meta-analysis. Am. J. Clin. Nutr. 2013, 97, 268–275. [Google Scholar] [CrossRef]
- Saini, R. Coenzyme Q10: The essential nutrient. J. Pharm. Bioallied Sci. 2011, 3, 466–467. [Google Scholar] [CrossRef]
- Adarsh, K.; Kaur, H.; Mohan, V. Coenzyme Q10 (CoQ10) in isolated diastolic heart failure in hypertrophic cardiomyopathy (HCM). Biofactors 2008, 32, 145–149. [Google Scholar] [CrossRef]
- Potgieter, M.; Pretorius, E.; Pepper, M.S. Primary and secondary coenzyme Q10 deficiency: The role of therapeutic supplementation. Nutr. Rev. 2013, 71, 180–188. [Google Scholar] [CrossRef]
- Onur, S.; Niklowitz, P.; Jacobs, G.; Lieb, W.; Menke, T.; Döring, F. Association between serum level of ubiquinol and NT-proBNP, a marker for chronic heart failure, in healthy elderly subjects. Biofactors 2015, 41, 35–43. [Google Scholar] [CrossRef]
- Bates, A.; Shen, Q.; Hiebert, J.B.; Thimmesch, A.; Pierce, J.D. Myocardial energetics and ubiquinol in diastolic heart failure. Nurs. Health Sci. 2014, 16, 428–433. [Google Scholar] [CrossRef]
- Sharma, A.; Fonarow, G.C.; Butler, J.; Ezekowitz, J.A.; Felker, G.M. Coenzyme Q10 and heart failure: A state-of-the-art review. Circ. Heart Fail. 2016, 9, e002639. [Google Scholar] [CrossRef]
- Huang, M.; Zhang, X.; Chen, S.; Sun, Y.; Xiao, Y.; Sun, J.; Huang, M.; Chen, S.; Liu, F. The effect of carvedilol treatment on chronic heart failure in pediatric patients with dilated cardiomyopathy: A prospective, randomized-controlled study. Pediatr. Cardiol. 2013, 34, 680–685. [Google Scholar] [CrossRef]
- Saxena, A.; Anil, O.M.; Juneja, R. Clinical and echocardiographic outcome in patients receiving carvedilol for treatment of dilated cardiomyopathy. Indian J. Pediatr. 2013, 80, 549–554. [Google Scholar] [CrossRef]
- Miles, M.V.; Horn, P.S.; Tang, P.H.; Morrison, J.A.; Miles, L.; DeGrauw, T.; Pesce, A.J. Age-related changes in plasma coenzyme Q10 concentrations and redox state in apparently healthy children and adults. Clin. Chim. Acta 2004, 347, 139–144. [Google Scholar] [CrossRef]
- Hossein-Nia, M.; Baig, K.; Goldman, J.H.; Keeling, P.J.; Caforio, A.L.; Holt, D.W.; McKenna, W.J. Creatine kinase isoforms as circulating markers of deterioration in idiopathic dilated cardiomyopathy. Clin. Cardiol. 1997, 20, 55–60. [Google Scholar] [CrossRef] [PubMed]
- Yilmaz, A.; Yalta, K.; Turgut, O.O.; Yilmaz, M.B.; Ozyol, A.; Kendirlioglu, O.; Karadas, F.; Tandogan, I. Clinical importance of elevated CK-MB and troponin I levels in congestive heart failure. Adv. Ther. 2006, 23, 1060–1067. [Google Scholar] [CrossRef] [PubMed]
- Hamilton, J.S.; Sharpe, P.C. Two cases of inflammatory muscle disease presenting with raised serum concentrations of troponin T. J. Clin. Pathol. 2005, 58, 1323–1324. [Google Scholar] [CrossRef] [PubMed]
- Schmelzer, C.; Lindner, I.; Rimbach, G.; Niklowitz, P.; Menke, T.; Döring, F. Functions of coenzyme Q10 in inflammation and gene expression. Biofactors 2008, 32, 179–183. [Google Scholar] [CrossRef] [PubMed]
- Schmelzer, C.; Lorenz, G.; Rinbach, G.; Doring, F. In vitro effects of the reduced form of coenzyme Q(10) on secretion levels of TNF-alpha and chemokines in response to LPS in the human monocytic cell line THP-1. J. Clin. Biochem. Nutr. 2009, 44, 62–66. [Google Scholar] [CrossRef] [PubMed]
- Hirano, M.; Garone, C.; Quinzii, C.M. CoQ(10) deficiencies and MNGIE: Two treatable mitochondrial disorders. Biochim. Biophys. Acta 2012, 1820, 625–631. [Google Scholar] [CrossRef] [PubMed]
- Quinzii, C.M.; Hirano, M. Coenzyme Q and mitochondrial disease. Dev. Disabil. Res. Rev. 2010, 16, 183–188. [Google Scholar] [CrossRef] [PubMed]
- El-Hattab, A.W.; Scaglia, F. Mitochondrial Cardiomyopathies. Front. Cardiovasc. Med. 2016, 3, 25. [Google Scholar] [CrossRef] [PubMed]
| PDCM (n = 10) | |
|---|---|
| Gender (n, boys/girls) | 5/5 |
| Age (y) | 9.9 ± 5.8 (9.0) 1 |
| Height (cm) | 134.3 ± 28.8 (131.0) |
| Body weight (kg) | 35.0 ± 20.0 (26.3) |
| Body mass index (kg/m2) | 17.7 ± 3.3 (16.0) |
| Head circumference (cm) | 51.7 ± 2.8 (51.0) |
| Mid-upper arm circumferences (cm) | 19.0 ± 4.8 (17.0) |
| Dose of liquid ubiquinol (mg/d) | 349.5 ± 200.4 (262.5) |
| Medications (n, %) | |
| Angiotensin II receptor antagonist | 4 (40%) |
| Angiotensin-converting enzyme inhibitors | 4 (40%) |
| Beta-blockers | 1 (10%) |
| Digoxin | 3 (30%) |
| Loop diuretics | 4 (40%) |
| Potassium-sparing diuretics | 4 (40%) |
| Week 0 | Week 12 | Week 24 | p Values | |
|---|---|---|---|---|
| Echocardiography | ||||
| EF (%) | 62.56 ± 7.47 (63.85) 1 | 66.28 ± 9.78 (68.35) | 65.67 ± 9.63 (66.85) | 0.15 |
| FS (%) | 34.20 ± 5.22 (35.45) | 37.07 ± 7.28 (38.98) | 36.59 ± 6.86 (37.60) | 0.19 |
| CO (L/min) | 10.77 ± 14.47 (5.83) | 16.36 ± 26.16 (5.72) | 14.62 ± 26.18 (5.62) | 0.73 |
| SV (mL) | 159.96 ± 274.25 (72.73) | 176.32 ± 217.88 (84.10) | 144.40 ± 217.56 (55.96) | 0.44 |
| HR (beat/min) | 82.15 ± 27.82 (85.00) | 82.6 ± 33.18 (83.75) | 86.50 ± 27.07 (92.00) | 0.93 |
| LVOTd (cm) | 1.75 ± 0.78 (1.60) | 1.87 ± 0.61 (1.80) | 1.68 ± 0.63 (1.65) | 0.25 |
| EDV (mL) | 133.92 ± 104.69 (107.50) | 132.75 ± 99.49 (109.00) | 135.16 ± 98.41 (99.20) | 0.93 |
| ESV (mL) | 53.12 ± 50.17 (38.05) | 48.14 ± 46.70 (33.00) | 51.05 ± 48.42 (41.45) | 0.15 |
| LVIDd (cm) | 5.00 ± 1.61 (4.80) | 4.99 ± 1.57 (4.83) | 5.05 ± 1.53 (4.64) | 0.89 |
| LVIDs (cm) | 3.32 ± 1.20 (3.10) | 3.17 ± 1.18 (2.92) | 3.25 ± 1.21 (3.22) | 0.22 |
| CI (L/(min*m2)) | 8.36 ± 8.61 (5.82) | 12.15 ± 15.74 (5.60) | 10.39 ± 15.71 (5.05) | 0.73 |
| MPI | 0.84 ± 0.47 (0.66) | 0.76 ± 0.34 (0.89) | 0.75 ± 0.47 (0.70) | 0.48 |
| Hematology | ||||
| BNP (pg/mL) | 115.6 ± 152.2 (56.9) | 157.4 ± 212.1 (48.8) | 148.0 ± 217.2 (50.8) | 0.63 |
| NT-Pro BNP (pg/mL) | 357.1 ± 451.6 (236.0) | 527.2 ± 703.8 (365.5) | 458.3 ± 694.3 (191.5) | 0.23 |
| CK (U/L) | 238.0 ± 344.0 (135.5) | 436.2 ± 772.7 (141.5) | 181.9 ± 105.5 (141.5) | 0.70 |
| CK-MB (U/L) | 14.2 ± 6.65 (16.0) | 10.8 ± 6.5 (12.0) | 12.6 ± 8.4 (11.0) | 0.52 |
| Plasma Coenzyme Q10 Concentration (μM) | ||
|---|---|---|
| Week 12 | Week 24 | |
| EF (%) | 0.48 (0.15) 1 | 0.37 (0.28) |
| FS (%) | 0.37 (0.28) | 0.26 (0.45) |
| CK (U/L) | −0.33 (0.33) | −0.75 (<0.05) |
| CK-MB (U/L) | −0.48 (0.17) | −0.31 (0.37) |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Chen, F.-L.; Chang, P.-S.; Lin, Y.-C.; Lin, P.-T. A Pilot Clinical Study of Liquid Ubiquinol Supplementation on Cardiac Function in Pediatric Dilated Cardiomyopathy. Nutrients 2018, 10, 1697. https://doi.org/10.3390/nu10111697
Chen F-L, Chang P-S, Lin Y-C, Lin P-T. A Pilot Clinical Study of Liquid Ubiquinol Supplementation on Cardiac Function in Pediatric Dilated Cardiomyopathy. Nutrients. 2018; 10(11):1697. https://doi.org/10.3390/nu10111697
Chicago/Turabian StyleChen, Fong-Lin, Po-Sheng Chang, Yi-Chin Lin, and Ping-Ting Lin. 2018. "A Pilot Clinical Study of Liquid Ubiquinol Supplementation on Cardiac Function in Pediatric Dilated Cardiomyopathy" Nutrients 10, no. 11: 1697. https://doi.org/10.3390/nu10111697
APA StyleChen, F.-L., Chang, P.-S., Lin, Y.-C., & Lin, P.-T. (2018). A Pilot Clinical Study of Liquid Ubiquinol Supplementation on Cardiac Function in Pediatric Dilated Cardiomyopathy. Nutrients, 10(11), 1697. https://doi.org/10.3390/nu10111697





