A Perspective towards Multi-Hazard Resilient Systems: Natural Hazards and Pandemics
Abstract
:1. Introduction
“There may and likely will come a time in which we have both an airborne disease that is deadly, and in order for us to deal with that effectively, we have to put in place an infrastructure - not just here at home, but globally - that allows us to see it quickly, isolate it quickly, respond to it quickly, so that if and when a new strain of flu like the Spanish flu crops up five years from now or a decade from now, we’ve made the investment and we’re further along to be able to catch it”.
2. Worldwide Experience on Natural Hazards and Pandemic
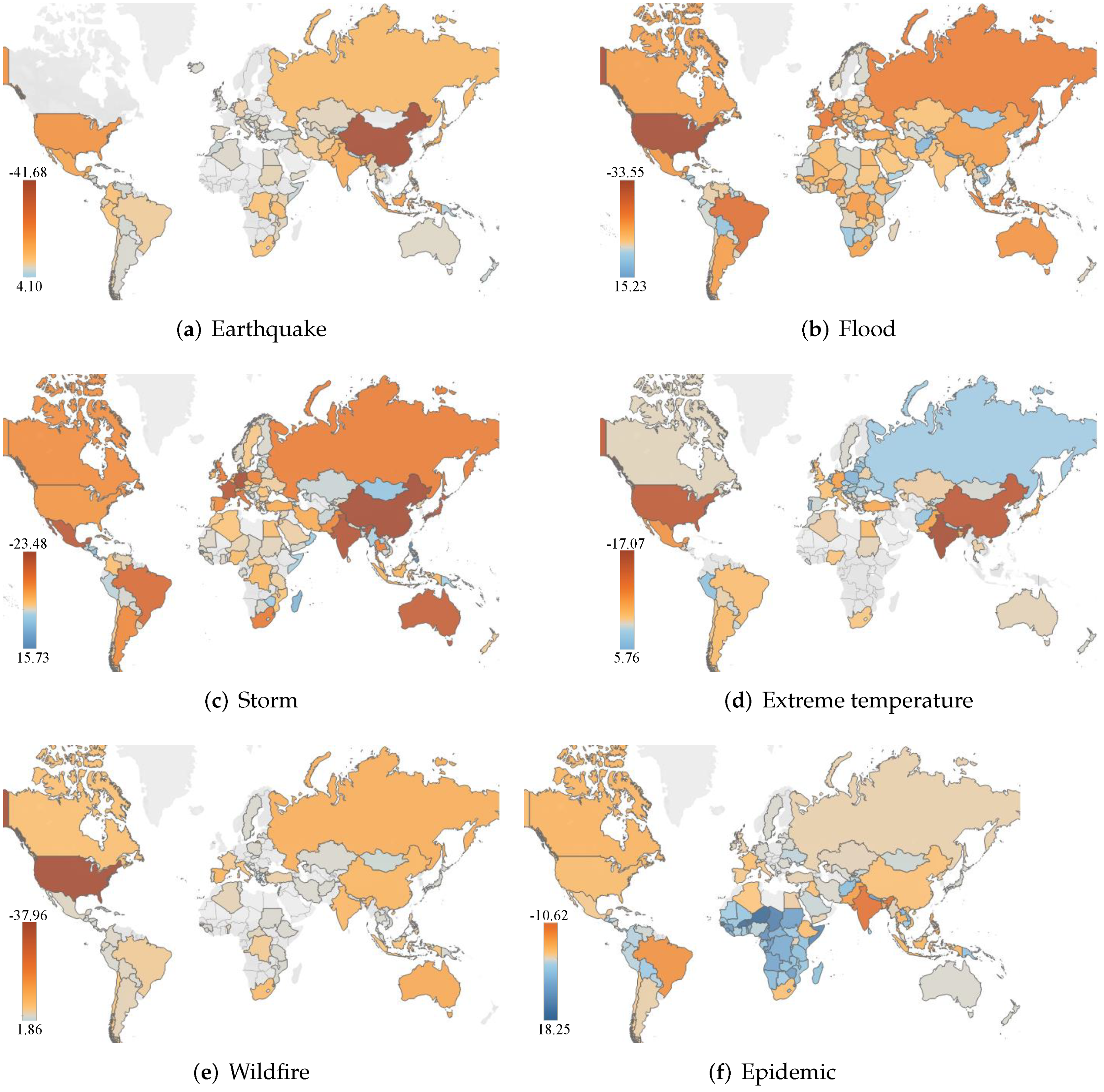
2.1. Comparison of Historical Natural Hazard and Pandemic Mortality Statistics
2.2. Recent Natural Hazards in the COVID-19 Era
- Cyclones/Hurricanes:
- –
- Between 1–6 April 2020, the Southwest Pacific Ocean islands (i.e., Solomon Islands, Vanuatu, Fiji, Tonga) were hit by tropical cyclone Harold [34]. In Sanma (Vanuatu), about 85% of the population lost their homes, and 20% of healthcare facilities were damaged. At the time Harold hit Vanuatu, it was Category 5. Harold impacted the Solomon Islands with devastating winds accompanied by heavy rains, river flooding, very rough seas, high ocean waves, and coastal flooding, including storm surge. About 59,000 people were affected, with 27 people reported missing at sea. Harold hit Fiji as a Category 4 on the night of 7 April. More than 1541 were sheltered across 52 evacuation centers as of 14 April. Social gathering restrictions and other COVID-19 protocols remained in force. In Tonga, significant damage to the water supply and food crops were reported.
- –
- Tropical Storm Amanda, the first of the Eastern Pacific Ocean hurricane season, formed on Sunday 31 May 2020 along the coast of Guatemala and quickly moved inland. According to USAToday, it killed at least 17 people in El Salvador and Guatemala, where heavy rains produced flooding and landslides. A World Food Program (WFP) rapid food security assessment in El Salvador estimated that over 336,000 people could be pushed into severe food insecurity. WFP also requested USD 19 million to support the government of El Salvador in its response to COVID-19.
- –
- On 2 June 2020, tropical storm Cristobal formed off the coast of Mexico, and moved towards Texas, Louisiana, and the Florida Panhandle. Cristobal moved over southeastern Louisiana on 7 June, and impacted southern Wisconsin by 10 June. The governor of Texas announced that the COVID-19 pandemic and tropical storm Cristobal combined for a unique challenge. He encouraged local officials to adopt evacuation strategies that take into account COVID-19; for example, (1) using more vehicles for evacuations to allow for more spacing between people, or (2) using hotels for the displaced population instead of convention center-type settings. Frausto-Martínez et al. [35] tracked the potential interaction of tropical storm Cristobal in the Western Yucatan Peninsula, Mexico with an increase in the number of COVID-19 positive cases. A numerical analysis was first conducted to identify the tropical storm’s extreme characteristics. Second, an analysis was performed using the reported flooding and rainfall information. Third, data on the confirmed positive cases of COVID-19 was post-processed. They reported no direct evidence for an increase in number of infectious cases in 10 out of 11 municipal areas. However, in one case, there was a sudden increase in the number of positive cases.
- –
- On 22 August 2020, tropical storm Laura brought heavy rainfall to Haiti and the Dominican Republic (with some locations recording about 300 mm of rain in one day). At least 11 fatalities have been reported. Several rivers broke their banks, and several floods were reported in Greater Santo Domingo. Civil Protection urged residents near the Artibonite River to evacuate their homes after flood gates of the Peligre Dam were opened [36]. The Haiti government placed an overnight curfew in an effort to stem the spread of COVID-19. The effects of Hurricane Laura in the United States were also destructive. It made landfall in Louisiana on August 27 as a Category 4 hurricane and caused around USD 17.5 billion damage and 33 fatalities. State emergencies were declared in Louisiana and Mississippi, and the Louisiana Department of Health tweeted “If evacuating: In addition to standard supplies like adequate meds and pet supplies, be sure to include items that help protect you and others from COVID-19 in your go kit, such as hand sanitizer with at least 60% alcohol, soap, disinfectant wipes and 2 masks for each person”. Laura caused disruption to testing centers, as well as disruption of water supplies. Non-congregate sheltering was recommended due to high rates of community spread. Shelters for evacuees were opened with cots set farther apart to maintain social distancing. Moreover, disrupted evacuations put many at shelter-in-place at risk from natural hazards. A number of agencies, including FEMA, pulled back their typical field response due to the pandemic, which may hamper relief efforts and delay distribution of post-disaster financial assistance.
- –
- On 16 September 2020, Hurricane Sally made its way inland, and killed at least one person in Alabama, U.S. According to the National Weather Service (NWS), the storm dumped ~760 mm and 630 mm of rain in Alabama and Florida, respectively. Nearly 500,000 homes and businesses lost power. Hurricane Sally put a pause on COVID-19 testing, because the sites were shut down for a week [36].
- –
- On 17 and 18 September 2020, cyclone Ianos (also known as Medicane Ianos) impacted Greece. It caused severe damage to the structures and infrastructures comprising health facilities including health centers and hospitals. Flooding was reported in several cities, resulting in four fatalities. Mavroulis et al. [37] tracked the number of affected people for one week before and three weeks after the event for 16 regional units of Greece. They reported 16%, 21% and 83% increase in the number of positive cases in three successive weeks after Medicane Ianos compared to a week before event.
- Droughts:
- –
- According to Mishra et al. [38], the co-occurrence of drought and the COVID-19 pandemic occurred across many countries to different degrees. The western U.S., southeastern Australia, southeast Asia, and south America, Africa, and Europe experienced both hazards. Populations at-risk were similar for drought and COVID-19 (e.g., older adults, those with lower socioeconomic status, those with pre-existing conditions, migrant workers, etc.). The COVID-19 outbreak limited access of millions of people to clean water. It increased the hardship of those in the farming sector to sell their produce. Moreover, COVID-19 disrupted food distribution and demand. Several reports have been published about the potential interaction of COVID-19 and drought, for example, in Zimbabwe (See FEWS NET), U.S., Italy (See The-Local), and others. In Madagascar, three years of drought combined with COVID-19 and brought the people to crisis point. According to WaterAid, nearly half of the 25 million people who live in Madagascar already had no access to clean water, and a staggering three-quarters lived in poverty.
- Earthquakes:
- –
- On 21 March 2020, a magnitude 5.6 earthquake hit west-central Epirus [39]. Mavroulis et al. [37] post-processed publicly-available data on the daily reported laboratory-confirmed COVID-19 number of cases in Greece and correlated them with the Epirus earthquake. They concluded that the impact of this earthquake on the pandemic evolution in northwestern Greece was negligible (only 2 out of 5 positive cases during the post-earthquake period could be attributed to this event).
- –
- On 22 March 2020, a magnitude 5.3 earthquake hit the city of Zagreb, Croatia [40]. This resulted in one fatality, 27 injured, ~6200 damaged buildings, and over 1900 buildings becoming uninhabitable. COVID-19 testing was disrupted for hours in hospitals. The earthquake caused widespread unrest, causing people to leave their homes and compromising social distancing measures [41]. Svetina et al. [42] proposed a resilience framework with a case study of earthquake in Zagreb during pandemic.
- –
- On 7 May 2020, an early morning magnitude 5.1 earthquake hit Tehran, Iran. At least two people died and about 38 were injured, but no other major damage was observed. According to Reuters, officials urged people to observe mandated social distancing measures to prevent the spread of COVID-19, even as some slept outdoors for fear of aftershocks.
- –
- On 30 October 2020, a magnitude 6.9 earthquake struck the eastern part of Greece and the western part of Turkey (the epicenter was located in the northern Samos Island) [43]. A total of 119 deaths and over 1030 injuries were reported in both Turkey and Samos Island, nearly all of them due to partial or total collapse of structures and the subsequent tsunami. By comparing the number of positive cases pre- and post-earthquake, [37] concluded that the impact of the Samos earthquake on COVID-19 in the eastern part of Greece was low (with only 12 reported positive cases compared to a previous 7 cases).
- Floods:
- –
- On 1 May 2020, after a long rainy week, part of an earth-fill dam broke along the Sardoba Reservoir in Uzbekistan, leading to flooding. Four people died, ~50 were injured, and 70,000 were evacuated from 22 villages. The reservoir was 29 m deep and completed in 2017 (capacity 922 Mm) [44]. While there is no solid information on the regional COVID-19 spread, the number of fatalities does not show any change (only one death is reported) for three weeks after the dam break in the whole of Uzbekistan (based on WHO data). At the time of the dam break, Uzbekistan was at the initial stage of virus spread (the main peak started mid-June) and therefore, there was no significant connection observed between flooding and pandemic. It is noteworthy that in the highly affected regions, the mass movement due to dam failure may increase the spread of virus.
- –
- On 19 May 2020, following heavy rains, the Edenville Dam was breached, and the Sanford Dam downstream overflowed, causing a major flood in Midland County, Michigan, United States. Sanford Dam is an 11 m concrete dam completed in 1925 (capacity of 18.5 Mm). Edenville Dam is a 16.5 m earthfill dam completed in 1924 (capacity of 81.6 Mm). Both dams are categorized as high hazards by the National Inventory of Dams [45]. These dam failures forced the evacuation of 11,000 people, including patients in the Midland Hospital. It was fortunate that both dams had emergency action plans (EAPs) in place. An EAP is a document that identifies (1) potential incidents around the dam, (2) the affected areas by the less of reservoir, and (3) pre-planned actions to be followed to minimize loss of life and property damage.
- –
- Several weeks of torrential monsoon rains during June and July 2020 caused flooding and landslides in Bangladesh, Bhutan, India, and Nepal, and killed over 700 people. According to UNICEF, over 4 million children were estimated to be impacted and in urgent need of life-saving support. The COVID-19 pandemic made the situation complicated as the number of positive cases accelerated in some of the affected areas.
- –
- On 9 August 2020, a large amount of rain (300 mm within 8 h) was recorded in Steni station and intense lightning activity was reported in Evia Island, Greece. Several rivers overflowed their banks, and the flooding caused eight fatalities and extensive damage to buildings and infrastructure [46], water supply, and electricity networks. There were water and electricity shut-offs in several villages. While the flooding occurred in the beginning of the second wave of the pandemic in Greece, tracking the number of COVID-19 positive cases one week before and three weeks after the event showed no relation between the pandemic and flooding [37].
- Tornado:
- –
- Between 12 and 13 April of 2020, dozens of tornadoes impacted a number of southeastern United States. Homes were obliterated and 36 fatalities were reported. Many had to move to shelters, which were attempting to implement social distancing and other COVID-19 precautions, and some were turned away due to a shortage of face masks [47].
- Wildfire:
- –
- Since 21 March 2020, more than 374 wildfires were reported through the forests in Iran’s Zagros Mountains. Wildfires raged across five provinces and burned more than 50,000 hectares of forests [48].
- –
- Lightning strikes in August 2020 sparked a number of fires in western U.S. states, notably California, Oregon, and Washington. Warm temperatures and dry conditions fueled additional fires. These wildfires expanded quickly, resulting in more than 40 deaths, destroying more than 7000 structures, scorching more than five million acres across the three states, and forcing tens of thousands of residents to evacuate [49]. The wildfires caused significant air quality degradation, contributing to hazardous conditions that may have adverse effects for those infected with, recovering from, or vulnerable to COVID-19.
- –
- Between 12 and 20 October of 2020, multiple fall wildfires occurred in Colorado, including near major population centers like Fort Collins, Boulder, and Estes Park (as reported by inciweb). This led to evacuation orders for thousands of residents, raising concerns about COVID-19 transmission, especially when an outbreak was reported at a Colorado Springs fire station in El Paso County.
- Extreme weather:
- –
- In February of 2021, a series of winter storms brought significant amounts of sleet and ice, as well as subfreezing temperatures, across the southern United States [50]. The storms resulted in vast power outages in Texas, largely attributed to a failure to winterize the Texas electric grid [51]. At the peak of the outages, nearly 4.5 million Texas homes and businesses were without power. Dozens of Texans filed lawsuits against the Electric Reliability Council of Texas (ERCOT) and local power companies. In addition to the devastating impacts on millions of residents and businesses, the power outages impacted recovering COVID-19 patients at home who were dependent on plug-in breathing machines and portable oxygen tanks [52]. The lack of reliable oxygen, in combination with extreme cold at home, forced many patients to return to already overwhelmed hospitals. Moreover, dangerous travel conditions, distribution delays, and the power outages resulted in vaccine delays [53]. As of 31 March 2021, the power outages resulted in 3123 vaccine doses being wasted [54].
3. Resilience to Natural Hazards
3.1. Resilience of Structures and Infrastructure Systems
- Three desired results:
- –
- More reliable: since it has a lower probability of reaching limit states.
- –
- Fast recovery: the rapidity of functionality restoration during a disaster is paramount to resilient systems.
- –
- Low socio-economic consequences: the reduced probability of significant service reductions and fast recovery decreases the impact of extreme events on a society.
- Four properties:
- –
- Robustness: the ability to withstand a given extreme event and still deliver a service.
- –
- Rapidity: the speed with which a structure recovers from such an event to reach a high functionality level.
- –
- Redundancy: the extent to which components of the system are substitutable.
- –
- Resourcefulness: the capacity to make the appropriate budget available, identify problems, establish priorities, and mobilize resources after an extreme event.
- Four dimensions:
- –
- Technical: includes all the technological aspects associated with construction.
- –
- Organizational: includes all the management activities and plans, maintenance, and response to emergencies.
- –
- Social: includes societal effects and impacts of mitigation actions.
- –
- Economic: includes all the direct and indirect costs due to the loss of functionality and the subsequent restoration.
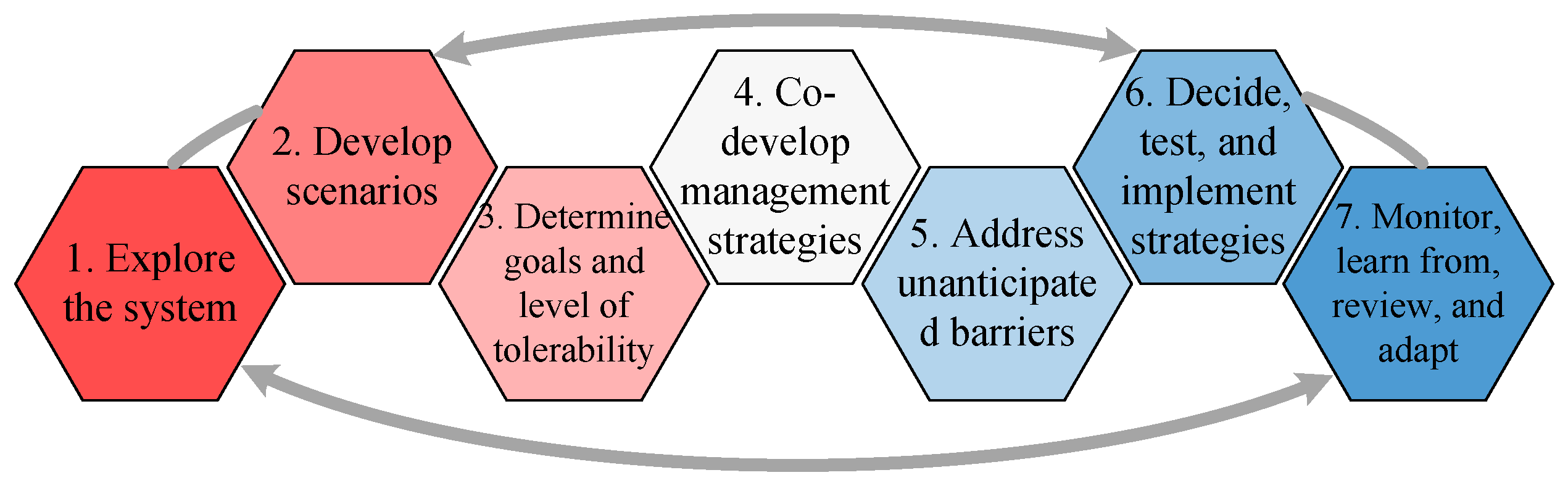
3.2. Resilience of Socio-Ecological Systems
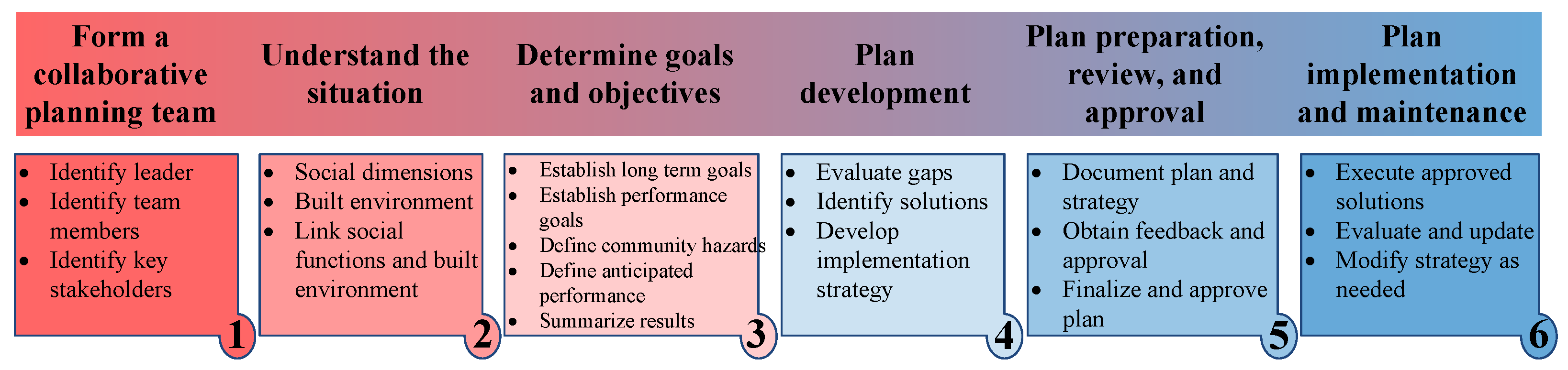
3.3. Planning for Resilient Communities
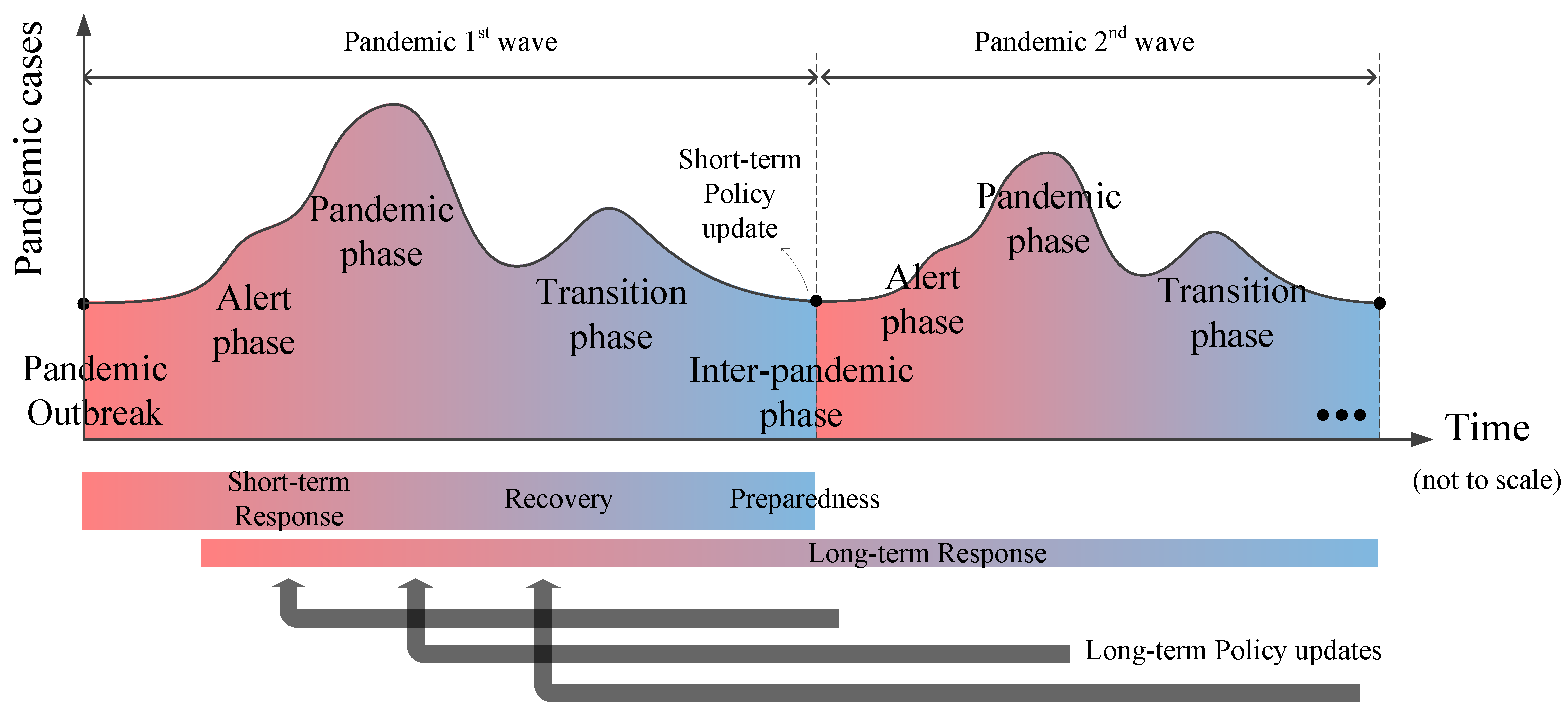
4. Pandemic-Centered Resilience
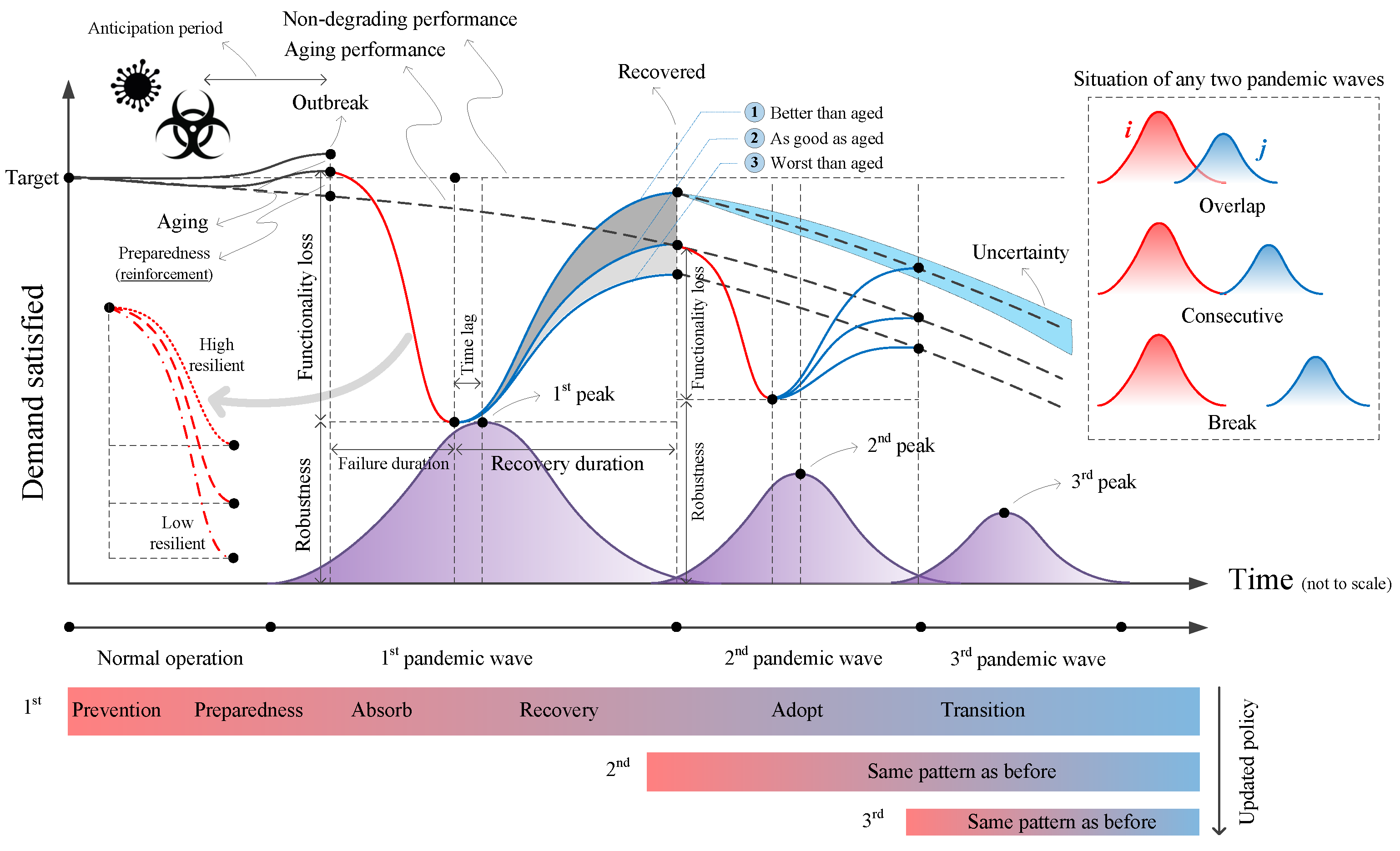
- They might highly overlap (e.g., Iran COVID-19 confirmed cases);
- They may just touch each other (e.g., Italy, Spain, and Japan COVID-19 confirmed cases);
- There might be a gap/break between waves (e.g., Spanish flu pandemic).
5. Perspectives into Resilience during Pandemic and Natural Hazard
- Natural hazard prior to pandemic: In this scenario, a natural hazard (e.g., flood, earthquake, or hurricane) occurs and affects the fundamentals of a healthcare system and consequently contributes to an outbreak. The 2004 South Asian tsunami, which hit sixteen countries and caused 250,000 fatalities, is an example of this dynamic [141]. The impacts of the tsunami contributed to factors leading to an acute respiratory infection outbreak in Indonesia [142]. In another case, a 2010 magnitude 7.0 earthquake in Haiti caused about 200,000 fatalities [143]. About nine months later, a cholera outbreak began to spread across the country, killing about 8000 people. Prior to the 2010 earthquake, no history of cholera in Haiti was reported. Other examples of pandemic after earthquake or flooding can be found in [144,145].
- Natural hazard during a pandemic: In this scenario, a design level natural hazard (e.g., flood, earthquake, and hurricane) occurs during an ongoing pandemic outbreak. This will have an adverse effect on capacity of the healthcare system. Examples of this scenario have been presented in Section 2.2 for the current COVID-19 outbreak. This case may even be worsen by sequential/cascading natural hazards during a pandemic. Two notable examples of compound hazards are post-earthquake fire [146] and flooding into nuclear power plants (e.g., in 2020, the Midland dam failure prompted an emergency notification at a nearby nuclear research reactor [147]).
- Most importantly, an ongoing pandemic overloads the healthcare system and reduces the system’s ability to provide appropriate and timely emergency medical services and thus may increase fatalities due to the occurrence of a natural hazard.
- Filling up the remaining capacity of the healthcare system with victims from the natural hazard decreases the capacity to test for infectious disease, and can therefore contribute to an increase in transmission.
- At the same time, both the pandemic and the natural hazard may lead to a decline in elective medical services, with negative public health consequences as well consequences for healthcare providers [155].
- An improper response to a natural hazard may increase the spread of an infectious disease and ultimately fatalities [156]. Response activities without precautions such as distancing measures may spread the virus, and extreme measures taken to lessen virus disease consequences could lead to inadequate responses to natural hazard management, causing other negative effects [154]. For example, extreme caution in evacuating high-rise buildings after an earthquake may put occupants at greater risk from building failure.
- Mass evacuation and sheltering in communal centers, without appropriate face covering and social distancing, increases the spread of an infectious disease.
- Evacuation capacity may be limited, because the occupancies of emergency shelter facilities are reduced during a pandemic when compared to preexisting emergency plans [157].
- Those infected (or even those without proper infectious disease protections) might be turned away from important services due to fear of viral spread. For example, during the April 2020 tornado in Crossville, Alabama, a family was not allowed to stay at a tornado shelter because the they did not have enough face masks for every family member [47].
- Locally specific context of the multi-hazard scenario is also very important. According to Dincer and Gillanders [158], in communities with high corruption, observing the social distancing during sheltering and also implementation of the mitigation strategies is difficult. They used two primary measures for corruption, one based on corruption convictions and the other based on news stories related to corruption. A measure of compliance based on cell phone activity constructed by SafeGraph is also used. In order to evaluate the robustness of the adopted metrics, they also tested a new metric, the corruption reflections index (CRI), which uses corruption stories covered in Associated Press (AP) news wires, which are electronically available online via LexisNexis.
- During a pandemic, travel restrictions between and within countries drastically reduce international and non-local agencies’ ability to deploy medical teams to the most affected regions of the world.
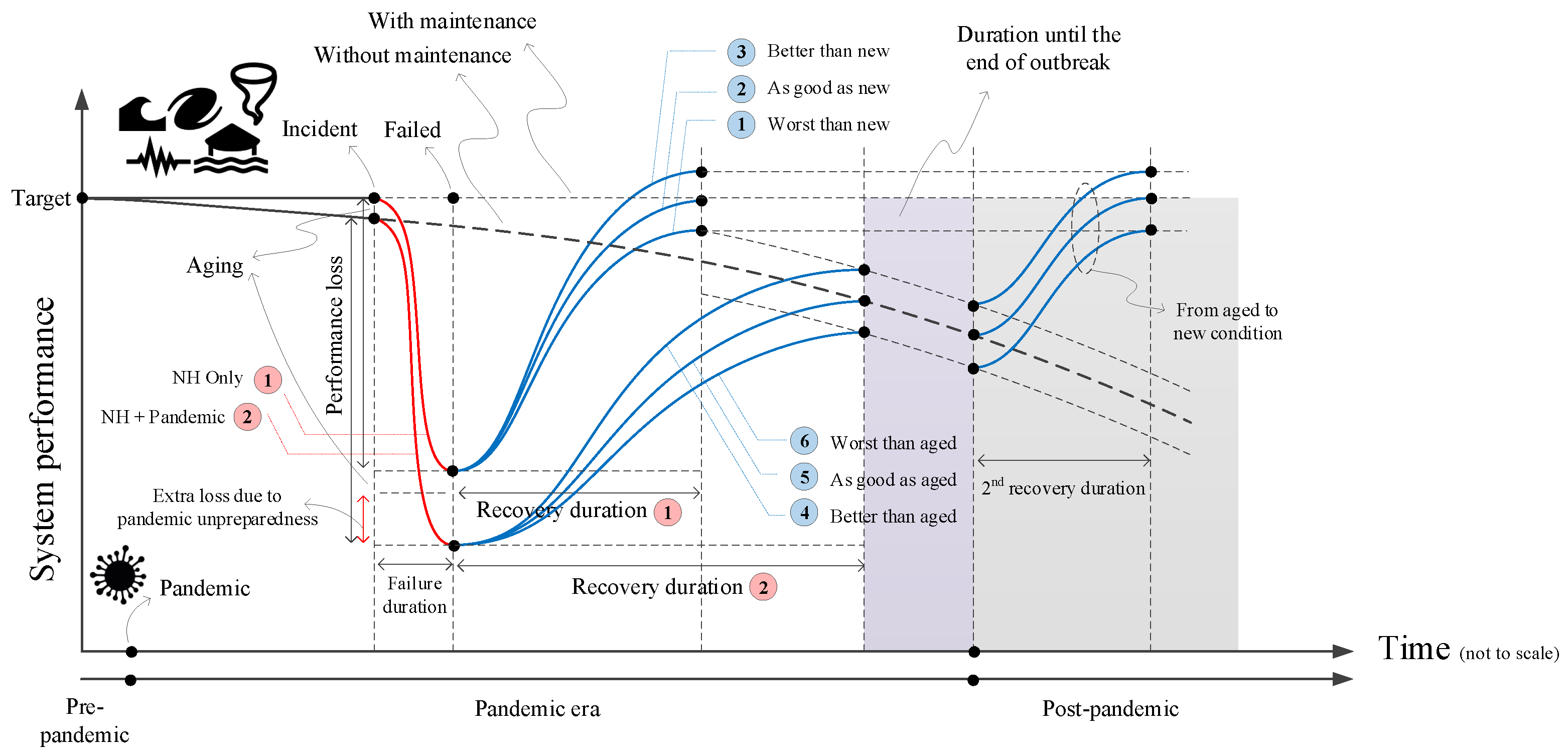
- In the first scenario, illustrated by Figure 9, the objective is to examine the resilience of the built environment under a natural hazard, and the way it is affected by presence of a pandemic.
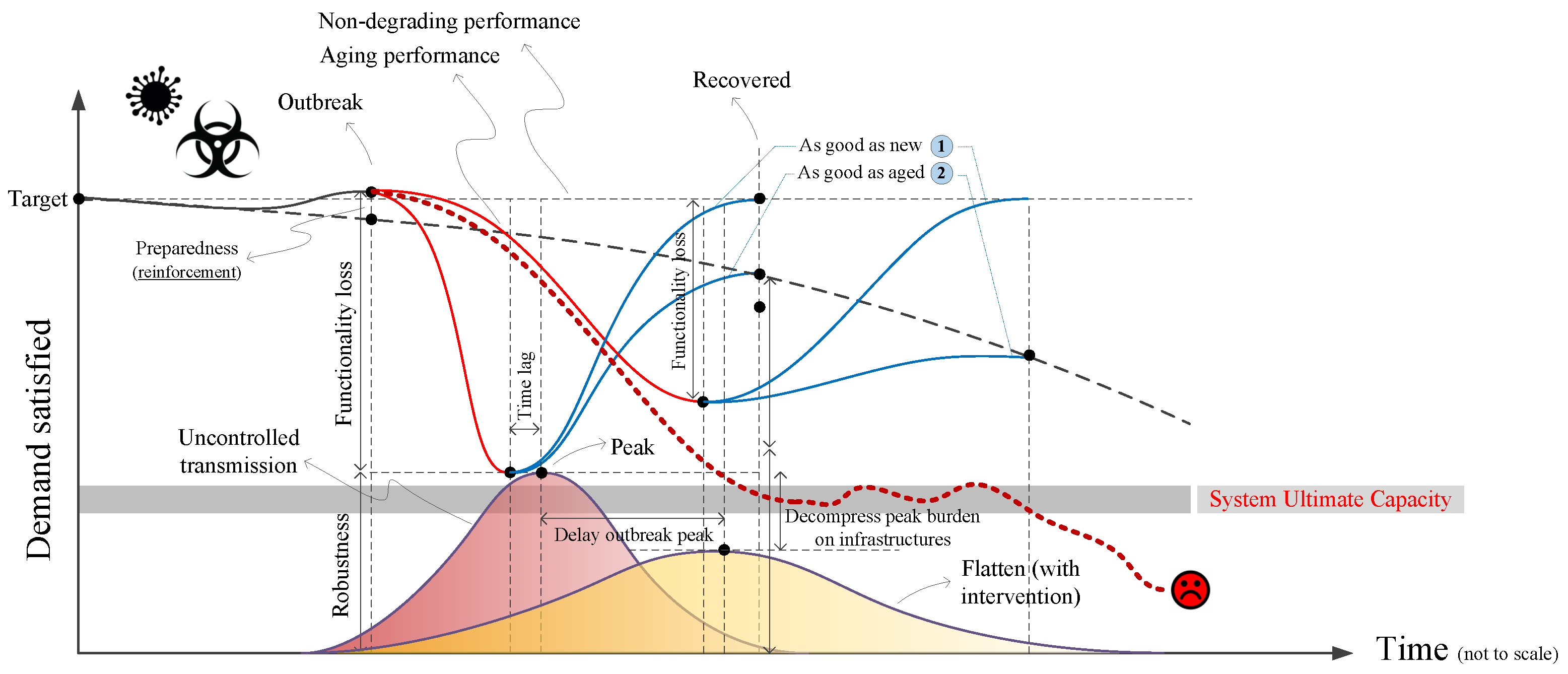
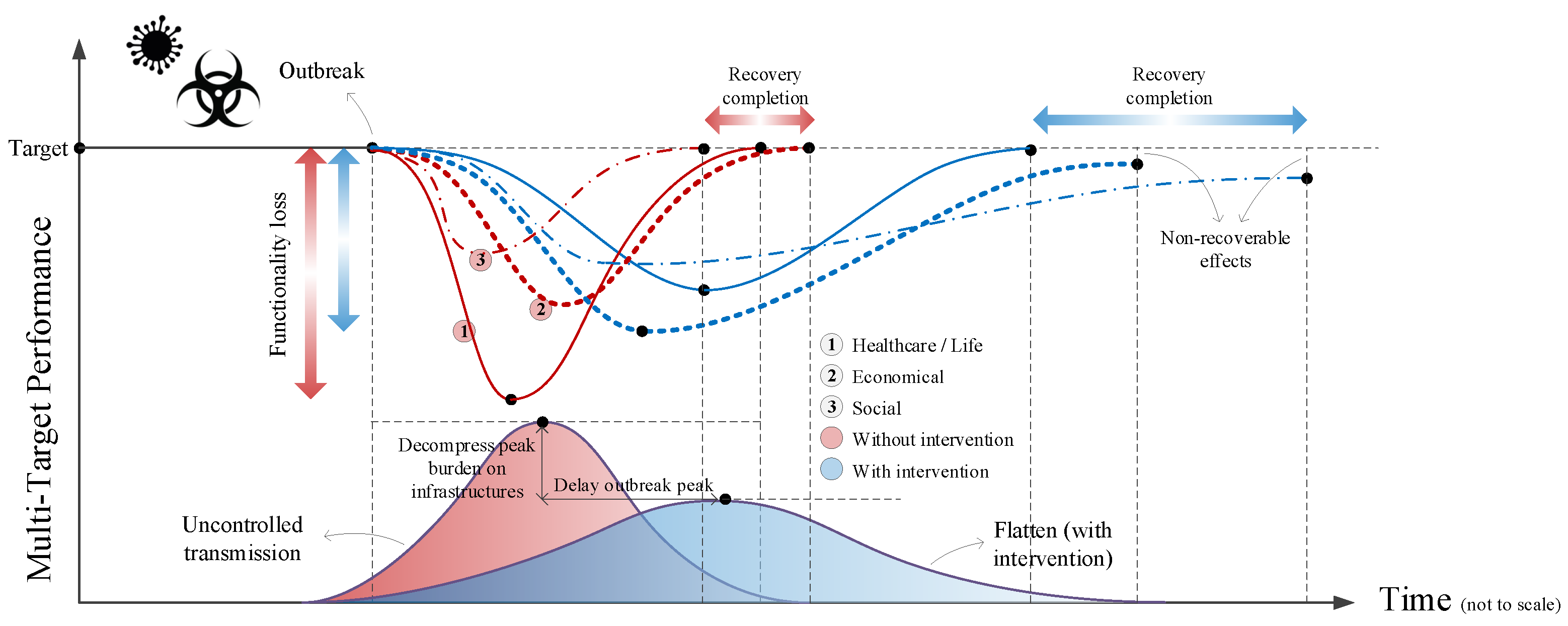
- In the second scenario, illustrated by Figure 10, the objective is to focus on the resilience of healthcare systems during pandemic, and the way it may be affected by a sudden shock (i.e., a natural hazard).
5.1. First Scenario: Resilience of Built-Environment Systems in a Natural Hazard and Pandemic
5.2. Second Scenario: Healthcare System Resilience in a Pandemic with Addition of Natural Hazard Shock
6. Conclusions and Future Direction
- The post-hazard performance and functionality of the built environment is dependent upon considerations of design, flow of materials, and operational requirements of restoration and maintenance; for example, whether materials, skilled personnel, and labor nearby are accessible to begin rapid repair.
- Economic impacts significantly affect the ability of local, state, and tribal governments to raise revenue that supports the operation, maintenance, and restoration of structures and infrastructure systems and other elements of the built environment. As the pandemic continues over time, potential accumulation of deferred maintenance activities could result in unexpected reductions in functionality under hazard conditions or some other unforeseen loading event.
- Economic impacts from both natural hazard events and pandemics can persist into the medium- and long-term, with the impacts of pandemics potentially persisting far longer than the impacts of natural hazards, for developed counties, depending on the magnitude of the event(s). For developing counties the impact from devastating natural hazards persists for decades.
- Combined social and economic impacts may shift expectation for demands on the built environment and expectations for restoration of functionality. The COVID-19 pandemic is a hazard event that has a long time horizon, requires dramatically different uses of some elements of the built environment, and may change how those elements function to serve the needs of occupants or users. Changes in regional or national cultural norms may also influence expectations for functionality and maintenance of systems.
- Disaster preparedness may help with response to a pandemic. For example, in a survey of small businesses, 23% of respondents that have implemented natural hazard planning in the past reported that such planning was helpful for coping with COVID-19 [167].
- Data availability and data analytics play an important role in increasing the resilience of society to natural hazards [168,169]. Therefore, exploring the capabilities and limitations of social networks is important as a potential tool to indirectly increase disaster preparedness. Multiple studies have been dedicated to investigating the role of the social network during the pandemic and its connection to a resilient society [170,171,172]. However, there is limited research that investigates the role of social media in the prevention and preparedness of events at the intersection of pandemic and natural hazards [173,174]. Eyre et al. [175] discussed the role of social media during the recovery stage from the pandemic (See Figure 4).
- How can we effectively collect and use data associated with co-occurrence of pandemic and natural hazard (e.g., social media data) at the regional and national levels with minimum potential bias (due to the objective nature of multi-hazards)?
- How to quantify the imposed risk to critical infrastructures (i.e., healthcare, energy [177] and power, information and cyber-technology, transportation, communications, water and wastewater, nuclear reactors, dams, etc.) due to combined pandemic and natural hazards?
- How to prioritize the risk reduction elements on the structures and critical infrastructures under a multi-objective (e.g., health, social, economical) and multi-constraint (e.g., political) condition?
- How to make sure all the resilience-centered tasks on operating, maintaining, and repairing critical infrastructure will continue in a reliable way, while the majority of the crew work remotely?
- How to quantify the importance of redundancy in both personnel (if they become sick) and infrastructures (if they are damaged) and their interaction during the pandemic plus natural hazards.
- How can we quantify the uncertainties in the observed vs. expected societal impacts, which affect the resilience of the healthcare system in response to the pandemic and natural hazards?
- How do we map Bruneau et al.’s [3] aspects of resilience to the co-occurrence of a natural hazard and a pandemic? For instance, in terms of desired results, do we prioritize restoring functionality of the healthcare system at the expense of recovery of the transportation network?
- What are the losses to society from natural hazard-induced disruptions to testing and treatment of infected populations during a pandemic? For example, can we quantify the excess cases or deaths associated with the inability to test, trace, and treat due to a disruption to the built infrastructure? While a few small studies found no correlation between a natural hazard event and COVID-19 cases or deaths, it is difficult to draw conclusions without a deeper investigations into the counterfactual (e.g., through an event study).
- On the other hand, can we quantify the impact of a pandemic on response and recovery to an acute natural hazard, such as an earthquake or flood? For instance, some of the cases cited in this paper suggest the policy response to the COVID-19 pandemic presented challenges for evacuations. Can we quantify excess losses from natural hazards that are due to the pandemic? Are they negligible? Moreover, several studies have shown the effectiveness of GIS-based data in evacuation planning during natural hazards [178]. Similar studies have been conducted on evacuation and transportation during pandemic [179,180]. Rajabifard et al. [181] discussed the connection between pandemic, geospatial information, and community resilience. Therefore, we need to quantify how GIS-based data can be combined with information about infected populations to reduce the spread of the virus during natural hazard-induced evacuations [182,183,184].
- While most of this paper has focused on the co-occurrence of an acute natural hazard event (e.g., earthquake, hurricane) during a pandemic, it is also important to consider the intersection of chronic and persistent hazard events (e.g., drought, extreme weather) during a pandemic. For instance, extreme cold in February of 2021 led to a failure of the electric grid in Texas. How much of the failure was driven by the excess demand for power by people at home? On the other hand, if vaccines had not been available, how costly would this disruption have been to testing and treating patients? What are the different challenges of a chronic vs. acute hazard occurring during a pandemic?
- Much of natural hazard resilience focus to-date has addressed system failure and restoration, functionality, and independencies of a range of designed and engineered systems. The COVID-19 pandemic raises questions about how we reflect the simultaneous impacts of natural and pandemic hazards on social and economic systems in traditional planning and design approaches?
- How can the level of function or service of social and economic systems, which are disrupted by pandemic, social, or economic disruptions, be quantitively linked to the performance of elements of the built and natural environment?
- While this paper presented a unified framework to combine the natural hazards and pandemic, it is also important to quantify the impact of different types of natural hazards when they are combined with pandemic scenario. For example, an earthquake typically occurs without any prior warning in a short period of time (e.g., few minutes) [42]. However, a flood is typically predictable (except sudden dam break [185]) and may last for few hours to days [186]. This requires slightly different strategies to address the compound natural hazard-pandemic resilience scenario. A detailed discussion for hurricane-pandemic hazards can be found in [187,188].
Author Contributions
Funding
Data Availability Statement
Conflicts of Interest
References
- Holling, C.S. Resilience and stability of ecological systems. Annu. Rev. Ecol. Syst. 1973, 4, 1–23. [Google Scholar] [CrossRef] [Green Version]
- Waller, M.A. Resilience in ecosystemic context: Evolution of the concept. Am. J. Orthopsychiatry 2001, 71, 290–297. [Google Scholar] [CrossRef] [PubMed]
- Bruneau, M.; Chang, S.E.; Eguchi, R.T.; Lee, G.C.; O’Rourke, T.D.; Reinhorn, A.M.; Shinozuka, M.; Tierney, K.; Wallace, W.A.; Von Winterfeldt, D. A framework to quantitatively assess and enhance the seismic resilience of communities. Earthq. Spectra 2003, 19, 733–752. [Google Scholar] [CrossRef] [Green Version]
- Presidential Policy Directive 21. Presidential Policy Directive—Critical Infrastructure Security and Resilience. 2013. Available online: https://obamawhitehouse.archives.gov/the-press-office/2013/02/12/presidential-policy-directive-critical-infrastructure-security-and-resil (accessed on 30 January 2018).
- Johnson, J.L.; Wiechelt, S.A. Introduction to the special issue on resilience. Subst. Use Misuse 2004, 39, 657–670. [Google Scholar] [CrossRef]
- Van der Leeuw, S.E.; Aschan-Leygonie, C. A long-term perspective on resilience in socio-natural systems. In Micro-Meso-Macro: Addressing Complex Systems Couplings; World Scientific: London, UK, 2005; pp. 227–264. [Google Scholar]
- Magis, K. Community resilience: An indicator of social sustainability. Soc. Nat. Resour. 2010, 23, 401–416. [Google Scholar] [CrossRef]
- Labaka, L.; Hernantes, J.; Sarriegi, J.M. A holistic framework for building critical infrastructure resilience. Technol. Forecast. Soc. Chang. 2016, 103, 21–33. [Google Scholar] [CrossRef]
- Vallejo, L.; Mullan, M. Climate-Resilient Infrastructure: Getting the Policies Right. Environment Working Papers No. 121. 2017. Available online: https://dx.doi.org/10.1787/02f74d61-en (accessed on 14 February 2022).
- Nikolaou, S.; Kourkoulis, R.; Diaz-Fanas, G. Earthquake-Resilient Infrastructure: The Missing Link. In Geotechnical Earthquake Engineering and Soil Dynamics V: Seismic Hazard Analysis, Earthquake Ground Motions, and Regional-Scale Assessment; American Society of Civil Engineers: Reston, VA, USA, 2018; pp. 79–90. [Google Scholar]
- Lhomme, S.; Serre, D.; Diab, Y.; Laganier, R. Analyzing resilience of urban networks: A preliminary step towards more flood resilient cities. Nat. Hazards Earth Syst. Sci. 2013, 13, 221. [Google Scholar] [CrossRef] [Green Version]
- Litman, T. Pandemic-Resilient Community Planning: Practical Ways to Help Communities Prepare for, Respond to, and Recover from Pandemics and Other Economic, Social and Environmental Shocks. 2020. Available online: https://www.vtpi.org/PRCP.pdf (accessed on 14 February 2022).
- Carvalhaes, T.; Markolf, S.; Helmich, A.; Kim, Y.; Li, R.; Natarajan, M.; Bondank, E.; Ahmad, N.; Chester, M. COVID-19 as a Harbinger of Transforming Infrastructure Resilience. Front. Built Environ. 2020, 6, 148. [Google Scholar] [CrossRef]
- United Nations ESCAP. Resilience in a Riskier World: Managing Systemic Risks from Biological and Other Natural Hazards. 2021. Available online: https://hdl.handle.net/20.500.12870/3811 (accessed on 14 February 2022).
- Lai, S.; Ruktanonchai, N.W.; Zhou, L.; Prosper, O.; Luo, W.; Floyd, J.R.; Wesolowski, A.; Santillana, M.; Zhang, C.; Du, X.; et al. Effect of non-pharmaceutical interventions to contain COVID-19 in China. Nature 2020, 585, 410–413. [Google Scholar] [CrossRef]
- Masrur, A.; Yu, M.; Luo, W.; Dewan, A. Space-time patterns, change, and propagation of COVID-19 risk relative to the intervention scenarios in Bangladesh. Int. J. Environ. Res. Public Health 2020, 17, 5911. [Google Scholar] [CrossRef]
- World Health Organization. Coronavirus Disease 2019 (COVID-19): Situation Report, 80. 2020. Available online: https://www.who.int/docs/default-source/coronaviruse/situation-reports/20200409-sitrep-80-covid-19.pdf (accessed on 30 April 2020).
- Mackenzie, J.S.; Smith, D.W. COVID-19: A novel zoonotic disease caused by a coronavirus from China: What we know and what we don’t. Microbiol. Aust. 2020, 41, 45–50. [Google Scholar] [CrossRef] [PubMed]
- Mazinani, M.; Rude, B. The novel zoonotic Coronavirus disease 2019 (COVID-19) pandemic: Health perspective on the outbreak. J. Healthc. Qual. Res. 2021, 36, 47–51. [Google Scholar] [CrossRef] [PubMed]
- Wu, Y.C.; Chen, C.S.; Chan, Y.J. The outbreak of COVID-19: An overview. J. Chin. Med. Assoc. 2020, 83, 217. [Google Scholar] [CrossRef] [PubMed]
- Hellewell, J.; Abbott, S.; Gimma, A.; Bosse, N.I.; Jarvis, C.I.; Russell, T.W.; Munday, J.D.; Kucharski, A.J.; Edmunds, W.J.; Sun, F.; et al. Feasibility of controlling COVID-19 outbreaks by isolation of cases and contacts. Lancet Glob. Health 2020, 8, e488–e496. [Google Scholar] [CrossRef] [Green Version]
- Yang, Y.; Peng, F.; Wang, R.; Guan, K.; Jiang, T.; Xu, G.; Sun, J.; Chang, C. The deadly coronaviruses: The 2003 SARS pandemic and the 2020 novel coronavirus epidemic in China. J. Autoimmun. 2020, 109, 102434. [Google Scholar] [CrossRef]
- Kleinman, A.; Watson, J.L. SARS in China: Prelude to Pandemic? Stanford University Press: Redwood City, CA, USA, 2006. [Google Scholar]
- Brysse, K.; Oreskes, N.; O’Reilly, J.; Oppenheimer, M. Climate change prediction: Erring on the side of least drama? Glob. Environ. Chang. 2013, 23, 327–337. [Google Scholar] [CrossRef]
- Kircher, C.A.; Seligson, H.A.; Bouabid, J.; Morrow, G.C. When the big one strikes again—Estimated losses due to a repeat of the 1906 San Francisco earthquake. Earthq. Spectra 2006, 22, 297–339. [Google Scholar] [CrossRef] [Green Version]
- UNISDR (United Nations International Strategy for Disaster Reduction) Sendai framework for disaster risk reduction 2015–2030. In Proceedings of the 3rd United Nations World Conference on DRR, Sendai, Japan, 14–18 March 2015; pp. 14–18.
- Maini, R.; Clarke, L.; Blanchard, K.; Murray, V. The Sendai Framework for Disaster Risk Reduction and its indicators-where does health fit in? Int. J. Disaster Risk Sci. 2017, 8, 150–155. [Google Scholar] [CrossRef] [Green Version]
- Semenza, J.C.; Menne, B. Climate change and infectious diseases in Europe. Lancet Infect. Dis. 2009, 9, 365–375. [Google Scholar] [CrossRef]
- Caminade, C.; McIntyre, K.M.; Jones, A.E. Impact of recent and future climate change on vector-borne diseases. Ann. N. Y. Acad. Sci. 2019, 1436, 157. [Google Scholar] [CrossRef] [Green Version]
- Hulme, M.; Lidskog, R.; White, J.M.; Standring, A. Social scientific knowledge in times of crisis: What climate change can learn from coronavirus (and vice versa). Wiley Interdiscip. Rev. Clim. Chang. 2020, 11, e656. [Google Scholar] [CrossRef] [PubMed]
- Hassan, E.M.; Mahmoud, H.N. Orchestrating performance of healthcare networks subjected to the compound events of natural disasters and pandemic. Nat. Commun. 2021, 12, 1–12. [Google Scholar] [CrossRef] [PubMed]
- Shi, W.; Hall, B.J. What can we do for people exposed to multiple traumatic events during the coronavirus pandemic? Asian J. Psychiatry 2020, 51, 102065. [Google Scholar] [CrossRef] [PubMed]
- Merad, M. Some Elements of Analysis of the Bibliography on Risk and Resilience on COVID-19. In COVID-19: Systemic Risk and Resilience; Springer: Cham, Switzerland, 2021; pp. 17–34. [Google Scholar]
- World Meteorological Organization. Tropical Cyclone Harold Challenges Disaster and Public Health Management. 2020. Available online: https://public.wmo.int/en/media/news/tropical-cyclone-harold-challenges-disaster-and-public-health-management (accessed on 30 April 2020).
- Frausto-Martínez, O.; Aguilar-Becerra, C.D.; Colín-Olivares, O.; Sánchez-Rivera, G.; Hafsi, A.; Contreras-Tax, A.F.; Uhu-Yam, W.D. COVID-19, Storms, and Floods: Impacts of Tropical Storm Cristobal in the Western Sector of the Yucatan Peninsula, Mexico. Sustainability 2020, 12, 9925. [Google Scholar] [CrossRef]
- Copernicus. Flood List. 2020. Available online: http://floodlist.com/america (accessed on 30 September 2020).
- Mavroulis, S.; Mavrouli, M.; Lekkas, E. Geological and hydrometeorological hazards and related disasters amid COVID-19 pandemic in Greece: Post-disaster trends and factors affecting the COVID-19 evolution in affected areas. Saf. Sci. 2021, 138, 105236. [Google Scholar] [CrossRef]
- Mishra, A.; Bruno, E.; Zilberman, D. Compound natural and human disasters: Managing drought and COVID-19 to sustain global agriculture and food sectors. Sci. Total Environ. 2020, 754, 142210. [Google Scholar] [CrossRef]
- Valkaniotis, S.; Briole, P.; Ganas, A.; Elias, P.; Kapetanidis, V.; Tsironi, V.; Fokaefs, A.; Partheniou, H.; Paschos, P. The Mw = 5.6 Kanallaki Earthquake of 21 March 2020 in West Epirus, Greece: Reverse Fault Model from InSAR Data and Seismotectonic Implications for Apulia-Eurasia Collision. Geosciences 2020, 10, 454. [Google Scholar] [CrossRef]
- Čivljak, R.; Markotić, A.; Capak, K. Earthquake in the time of COVID-19: The story from Croatia (CroVID-20). J. Glob. Health 2020, 10, e010349. [Google Scholar] [CrossRef]
- Peitl, V.; Golubić Zatezalo, V.; Karlović, D. Mental Health Issues and Psychological Crisis Interventions during the COVID-19 Pandemic and Earthquakes in Croatia. Arch. Psychiatry Res. Int. J. Psychiatry Relat. Sci. 2020, 56, 193–198. [Google Scholar]
- Svetina, L.; Kosec, A.; Curkovic, M.; Iskra, A.N. A case study of complex disasters within the resilience framework in Zagreb, Croatia: Two earthquakes in one pandemic. Environ. Res. 2022, 204, 112079. [Google Scholar] [CrossRef]
- Papadimitriou, P.; Kapetanidis, V.; Karakonstantis, A.; Spingos, I.; Kassaras, I.; Sakkas, V.; Kouskouna, V.; Karatzetzou, A.; Pavlou, K.; Kaviris, G.; et al. First Results on the Mw= 6.9 Samos Earthquake of 30 October 2020. Bull. Geol. Soc. Greece 2020, 56, 251–279. [Google Scholar] [CrossRef]
- Putz, C. 70,000 Evacuated After Breach in Uzbek Dam, Investigation Into Failure Launched. The Diplomat, 2020. [Google Scholar]
- NID. National Inventory of Dams. 2019. Available online: https://nid-test.sec.usace.army.mil/ords/f?p=105:22:13023978711032::NO::: (accessed on 30 May 2020).
- Lekkas, E.; Mavroulis, S.; Gogou, M.; Papadopoulos, G.; Triantafyllou, I.; Katsetsiadou, K.; Kranis, H.; Skourtsos, E.; Carydis, P.; Voulgaris, N.; et al. The October 30, 2020 M w 6.9 Samos (Greece) earthquake. Newsl. Environ. Disaster Cris. Manag. Strateg. Dep. Dyn. Tecton. Appl. Geol. Fac. Geol. Geoenviron. Natl. Kapodistr. Univ. Athens Athens Greece 2020, 21, 156. [Google Scholar]
- Andrews, R. What Happens If a ’Big One’ Strikes during the Pandemic? 2020. Available online: https://www.preventionweb.net/news/what-happens-if-big-one-strikes-during-pandemic (accessed on 30 May 2020).
- Kheshti, M. Protect Iran’s Zagros forests from wildfires. Science 2020, 369, 1066. [Google Scholar] [CrossRef] [PubMed]
- BBC News. US West Coast Fires in Maps, Graphics and Images. 2020. Available online: https://www.bbc.com/news/world-us-canada-54180049 (accessed on 30 September 2020).
- Doss-Gollin, J.; Farnham, D.J.; Lall, U.; Modi, V. How unprecedented was the February 2021 Texas cold snap? Environ. Res. Lett. 2021, 16, 064056. [Google Scholar] [CrossRef]
- Price, A.; Schler, B. Winter storm blackouts plagued Texas in 2011, too. Recommendations made afterward went unenforced. USA Today. 2021. Available online: https://www.usatoday.com/story/news/nation/2021/02/18/state-energy-winter-protections-lacking-reports-have-suggested/4490501001/ (accessed on 13 July 2021).
- Hixenbauh, M.; Trevizo, P. Texans recovering from COVID-19 relied on machines to help them breathe. Then the power went out. The Texas Tribune. 2021. Available online: https://www.texastribune.org/2021/03/09/texas-covid-power-outages/ (accessed on 12 July 2021).
- Harper, K.B. Hundreds of thousands of COVID-19 vaccine deliveries, injections delayed by winter storm. The Texas Tribune. 2021. Available online: https://www.texastribune.org/2021/02/16/texas-coronavirus-vaccine-winter-storm/ (accessed on 12 July 2021).
- Cobler, N. Spoiled vaccines from Texas winter storms top 3,000. Austin American-Statesman. Available online: https://www.statesman.com/story/news/coronavirus/2021/03/31/spoiled-covid-vaccines-texas-winter-storms-february-top-3-000/4807780001/ (accessed on 13 July 2021).
- Davidson, J.L.; Jacobson, C.; Lyth, A.; Dedekorkut-Howes, A.; Baldwin, C.L.; Ellison, J.C.; Holbrook, N.J.; Howes, M.J.; Serrao-Neumann, S.; Singh-Peterson, L.; et al. Interrogating resilience: Toward a typology to improve its operationalization. Ecol. Soc. 2016, 21. [Google Scholar] [CrossRef] [Green Version]
- Bruneau, M.; Reinhorn, A. Exploring the concept of seismic resilience for acute care facilities. Earthq. Spectra 2007, 23, 41–62. [Google Scholar] [CrossRef] [Green Version]
- Cimellaro, G.P.; Reinhorn, A.M.; Bruneau, M. Framework for analytical quantification of disaster resilience. Eng. Struct. 2010, 32, 3639–3649. [Google Scholar] [CrossRef]
- Bocchini, P.; Frangopol, D.; Ummenhofer, T.; Zinke, T. Resilience and sustainability of civil infrastructure: Toward a unified approach. J. Infrastruct. Syst. 2013, 20, 04014004. [Google Scholar] [CrossRef]
- Deodatis, G.; Ellingwood, B.; Frangopol, D. Safety, Reliability, Risk and Life-Cycle Performance of Structures and Infrastructures; CRC Press: Boca Raton, FL, USA, 2014. [Google Scholar]
- Sharma, N.; Tabandeh, A.; Gardoni, P. Resilience analysis: A mathematical formulation to model resilience of engineering systems. Sustain. Resilient Infrastruct. 2017, 3, 49–67. [Google Scholar] [CrossRef] [Green Version]
- Clavin, C.T.; Dabreau, A.M.; Walpole, E.H. Resilience, Adaptation, and Sustainability Plan Assessment Methodology: An Annotated Bibliography, Technical Note 2117; Technical Report; National Institute of Standards and Technology: Gaithersburg, MD, USA, 2020.
- Ayyub, B.M. Systems resilience for multihazard environments: Definition, metrics, and valuation for decision making. Risk Anal. 2014, 34, 340–355. [Google Scholar] [CrossRef] [PubMed]
- Ayyub, B.M. Resilience metrics for multi-hazard environments. In Vulnerability, Uncertainty, and Risk: Quantification, Mitigation, and Management; American Society of Civil Engineers: Reston, VA, USA, 2014; pp. 925–936. [Google Scholar]
- Haimes, Y.Y. On the definition of resilience in systems. Risk Anal. 2009, 29, 498–501. [Google Scholar] [CrossRef] [PubMed]
- Sattar, S.; McAllister, T.; Johnson, K.; Clavin, C.; Segura, C.; McCabe, S.; Fung, J.; Abrahams, L.; Sylak-Glassman, E.; Levitan, M.; et al. Research Needs to Support Immediate Occupancy Building Performance Objective Following Natural Hazard Events, NIST Special Publication 1224; Technical Report; National Institute of Standards and Technology: Gaithersburg, MD, USA, 2018.
- NIST-FEMA. Recommended Options for Improving the Built Environment for Post-Earthquake Reoccupancy and Functional Recovery Time, FEMA P-2090/NIST SP-1254; Technical Report; Federal Emergency Management Agency: Washington, DC, USA; National Institute of Standards and Technology: Gaithersburg, MD, USA, 2020.
- Folke, C. Resilience: The emergence of a perspective for social–ecological systems analyses. Glob. Environ. Chang. 2006, 16, 253–267. [Google Scholar] [CrossRef]
- Gunderson, L.H. Ecological resilience—In theory and application. Annu. Rev. Ecol. Syst. 2000, 31, 425–439. [Google Scholar] [CrossRef] [Green Version]
- Holling, C.S. Engineering resilience versus ecological resilience. Eng. Ecol. Constraints 1996, 31, 32. [Google Scholar]
- Scheffer, M. Critical Transitions in Nature and Society; Princeton University Press: Princeton, NJ, USA, 2009; Volume 16. [Google Scholar]
- Folke, C.; Carpenter, S.R.; Walker, B.; Scheffer, M.; Chapin, T.; Rockström, J. Resilience thinking: Integrating resilience, adaptability and transformability. Ecol. Soc. 2010, 15. [Google Scholar] [CrossRef]
- Walker, B.; Salt, D. Resilience Practice: Building Capacity to Absorb Disturbance and Maintain Function; Island Press: Washington, DC, USA, 2012. [Google Scholar]
- Leenhardt, P.; Teneva, L.; Kininmonth, S.; Darling, E.; Cooley, S.; Claudet, J. Challenges, insights and perspectives associated with using social-ecological science for marine conservation. Ocean Coast. Manag. 2015, 115, 49–60. [Google Scholar] [CrossRef]
- Cutter, S.L.; Ahearn, J.A.; Amadei, B.; Crawford, P.; Eide, E.A.; Galloway, G.E.; Goodchild, M.F.; Kunreuther, H.C.; Li-Vollmer, M.; Schoch-Spana, M.; et al. Disaster resilience: A national imperative. Environ. Sci. Policy Sustain. Dev. 2013, 55, 25–29. [Google Scholar] [CrossRef]
- Cutter, S.L. Linkages between vulnerability and resilience. In Vulnerability and Resilience to Natural Hazards; Cambridge University Press: Cambridge, UK, 2018; pp. 257–270. [Google Scholar]
- Koliou, M.; van de Lindt, J.W.; McAllister, T.P.; Ellingwood, B.; Dillard, M.; Cutler, H. State of the research in community resilience: Progress and challenges. Sustain. Resilient Infrastruct. 2020, 5, 131–151. [Google Scholar] [CrossRef]
- Farokhnia, K.; van de Lindt, J.W.; Koliou, M. Selection of Residential Building Design Requirements to Achieve Community Functionality Goals under Tornado Loading. Pract. Period. Struct. Des. Constr. 2020, 25, 04019035. [Google Scholar] [CrossRef]
- C.R.P. NIST. Community Resilience Planning Guide for Buildings and Infrastructure Systems, Volume I, Special Publication 1190; Technical Report; National Institute of Standards and Technology: Gaithersburg, MD, USA, 2016.
- C.R.P. NIST. Community Resilience Planning Guide for Buildings and Infrastructure Systems, Volume II, Special Publication 1190; Technical Report; National Institute of Standards and Technology: Gaithersburg, MD, USA, 2016.
- Legido-Quigley, H.; Asgari, N.; Teo, Y.Y.; Leung, G.M.; Oshitani, H.; Fukuda, K.; Cook, A.R.; Hsu, L.Y.; Shibuya, K.; Heymann, D. Are high-performing health systems resilient against the COVID-19 epidemic? Lancet 2020, 395, 848–850. [Google Scholar] [CrossRef] [Green Version]
- Wister, A.; Speechley, M. COVID-19: Pandemic risk, resilience and possibilities for aging research. Can. J. Aging/Rev. Can. Vieil. 2020, 39, 344–347. [Google Scholar] [CrossRef] [PubMed]
- Legido-Quigley, H.; Mateos-García, J.T.; Campos, V.R.; Gea-Sánchez, M.; Muntaner, C.; McKee, M. The resilience of the Spanish health system against the COVID-19 pandemic. Lancet Public Health 2020, 5, e251–e252. [Google Scholar] [CrossRef] [Green Version]
- Santarone, K.; McKenney, M.; Elkbuli, A. Preserving mental health and resilience in frontline healthcare workers during COVID-19. Am. J. Emerg. Med. 2020, 38, 1530–1531. [Google Scholar] [CrossRef]
- Plomecka, M.B.; Gobbi, S.; Neckels, R.; Radziński, P.; Skórko, B.; Lazerri, S.; Almazidou, K.; Dedić, A.; Bakalović, A.; Hrustić, L.; et al. Mental Health Impact of COVID-19: A global study of risk and resilience factors. medRxiv 2020. [Google Scholar] [CrossRef]
- Prime, H.; Wade, M.; Browne, D.T. Risk and resilience in family well-being during the COVID-19 pandemic. Am. Psychol. 2020, 75, 631. [Google Scholar] [CrossRef]
- Rahman, M.; Chowdhury, M.; Garcia-Ballestas, E.; Florez, W.; Agrawal, A.; Moscote-Salazar, L.R. COVID 19 and Resilience: Neurosurgical perspectives. World Neurosurg. 2020. [Google Scholar] [CrossRef]
- D’Orazio, M.; Bernardini, G.; Quagliarini, E. Sustainable and resilient strategies for touristic cities against COVID-19: An agent-based approach. arXiv 2020, arXiv:2005.12547. [Google Scholar] [CrossRef]
- Worstell, J. Ecological resilience of food systems in response to the COVID-19 crisis. J. Agric. Food Syst. Community Dev. 2020, 9, 1–8. [Google Scholar] [CrossRef] [Green Version]
- Hobbs, J.E. Food supply chains during the COVID-19 pandemic. Can. J. Agric. Econ. Can. D’agroecon. 2020, 68, 171–176. [Google Scholar] [CrossRef] [Green Version]
- Golan, M.S.; Jernegan, L.H.; Linkov, I. Trends and applications of resilience analytics in supply chain modeling: Systematic literature review in the context of the COVID-19 pandemic. Environ. Syst. Decis. 2020, 40, 222–243. [Google Scholar] [CrossRef] [PubMed]
- Ivanov, D. Viable supply chain model: Integrating agility, resilience and sustainability perspectives—Lessons from and thinking beyond the COVID-19 pandemic. Ann. Oper. Res. 2020, 1–21. [Google Scholar] [CrossRef] [PubMed]
- Palin, P.J. Supply Chain Resilience: Push and Pull in Catastrophes. J. Crit. Infrastruct. Policy 2020, 1, 17–35. [Google Scholar] [CrossRef]
- Hart, C.; Nash, F. Teacher Resilience during COVID: Burnout and Trauma. 2020. Available online: https://www.rti.org/insights/coaching-teacher-resilience-during-covid-19-burnout-and-trauma (accessed on 30 May 2020).
- Baker, S.R.; Bloom, N.; Davis, S.J.; Terry, S.J. COVID-Induced Economic Uncertainty; Technical Report; National Bureau of Economic Research: Cambridge, MA, USA, 2020. [Google Scholar]
- Baldwin, R.; Evenett, S. COVID-19 and Trade Policy: Why Turning Inward Won’t Work. 2020. Available online: https://voxeu.org/system/files/epublication/Covid-19_and_Trade_Policy.pdf (accessed on 30 December 2020).
- Amekudzi-Kennedy, A.; Labi, S.; Woodall, B.; Marsden, G.; Grubert, E. Role of Socially-Equitable Economic Development in Creating Resilient and Sustainable Systems: COVID-19-Related Reflections. Preprints 2020, 2020040336. [Google Scholar] [CrossRef]
- Hynes, W.; Trump, B.; Kirman, A.; Latini, C.; Linkov, I. Complexity, Interconnectedness and Resilience: Why a Paradigm Shift in Economics is Needed to Deal with Covid 19 and Future Shocks. In COVID-19: Systemic Risk and Resilience; Springer: Amsterdam, The Netherlands, 2021; pp. 61–73. [Google Scholar]
- Bostrom, A.; Bohm, G.; OConnor, R.E.; Hanss, D.; Bodi-Fernandez, O.; Halder, P. Comparative risk science for the coronavirus pandemic. J. Risk Res. 2020, 23, 902–911. [Google Scholar] [CrossRef]
- Bryce, C.; Ring, P.; Ashby, S.; Wardman, J. Resilience in the face of uncertainty: Early lessons from the COVID-19 pandemic. J. Risk Res. 2020, 23, 880–887. [Google Scholar] [CrossRef]
- Barton, M.A.; Christianson, M.; Myers, C.G.; Sutcliffe, K. Resilience in action: Leading for resilience in response to COVID-19. BMJ Leader 2020, 000260. [Google Scholar] [CrossRef]
- Sadati, A.K.; MH, B.L.; Bagheri Lankarani, K. Risk Society, Global Vulnerability and Fragile Resilience; Sociological View on the Coronavirus Outbreak. Shiraz E-Med. J. 2020, 21, e102263. [Google Scholar] [CrossRef] [Green Version]
- Collins, A.; Florin, M.V.; Renn, O. COVID-19 risk governance: Drivers, responses and lessons to be learned. J. Risk Res. 2020, 23, 1073–1082. [Google Scholar] [CrossRef]
- Aven, T.; Bouder, F. The COVID-19 pandemic: How can risk science help? J. Risk Res. 2020, 23, 849–854. [Google Scholar] [CrossRef] [Green Version]
- Dryhurst, S.; Schneider, C.R.; Kerr, J.; Freeman, A.L.; Recchia, G.; Van Der Bles, A.M.; Spiegelhalter, D.; van der Linden, S. Risk perceptions of COVID-19 around the world. J. Risk Res. 2020, 23, 994–1006. [Google Scholar] [CrossRef]
- Figari, F.; Fiorio, C.V. Welfare Resilience in the Immediate Aftermath of the COVID-19 Outbreak in Italy. Available online: https://cepr.org/content/covid-economics-vetted-and-real-time-papers-0#block-block-9 (accessed on 31 May 2020).
- CDC. The Continuum of Pandemic Phases. 2016. Available online: https://www.cdc.gov/flu/pandemic-resources/planning-preparedness/global-planning-508.html (accessed on 31 May 2020).
- Menoni, S.; Schwarze, R. Recovery during a crisis: Facing the challenges of risk assessment and resilience management of COVID-19. Environ. Syst. Decis. 2020, 40, 189–198. [Google Scholar] [CrossRef] [PubMed]
- Hynes, W.; Trump, B.; Love, P.; Linkov, I. Bouncing forward: A resilience approach to dealing with COVID-19 and future systemic shocks. Environ. Syst. Decis. 2020, 40, 174–184. [Google Scholar] [CrossRef] [PubMed]
- Keenan, J.M. COVID, resilience, and the built environment. Environ. Syst. Decis. 2020, 40, 216–221. [Google Scholar] [CrossRef]
- Anderson, R.M.; Heesterbeek, H.; Klinkenberg, D.; Hollingsworth, T.D. How will country-based mitigation measures influence the course of the COVID-19 epidemic? Lancet 2020, 395, 931–934. [Google Scholar] [CrossRef]
- San Lau, L.; Samari, G.; Moresky, R.T.; Casey, S.E.; Kachur, S.P.; Roberts, L.F.; Zard, M. COVID-19 in humanitarian settings and lessons learned from past epidemics. Nat. Med. 2020, 26, 647–648. [Google Scholar]
- Van Bavel, J.J.; Baicker, K.; Boggio, P.S.; Capraro, V.; Cichocka, A.; Cikara, M.; Crockett, M.J.; Crum, A.J.; Douglas, K.M.; Druckman, J.N.; et al. Using social and behavioural science to support COVID-19 pandemic response. Nat. Hum. Behav. 2020, 4, 460–471. [Google Scholar] [CrossRef]
- Aubin, J.P. Une approche viabiliste du couplage des systèmes climatique et économique. Nat. Sci. Sociétés 2010, 18, 277–286. [Google Scholar] [CrossRef] [Green Version]
- International Risk Governance Center. Guidelines for the Governance of Systemic Risks: In Systems and Organisations in the Context of Transitions; International Risk Governance Center: Lausanne, Switzerland, 2018. [Google Scholar]
- Massaro, E.; Ganin, A.; Perra, N.; Linkov, I.; Vespignani, A. Resilience management during large-scale epidemic outbreaks. Sci. Rep. 2018, 8, 1859. [Google Scholar] [CrossRef] [Green Version]
- Jovanović, A.; Klimek, P.; Renn, O.; Schneider, R.; Øien, K.; Brown, J.; DiGennaro, M.; Liu, Y.; Pfau, V.; Jelić, M.; et al. Assessing resilience of healthcare infrastructure exposed to COVID-19: Emerging risks, resilience indicators, interdependencies and international standards. Environ. Syst. Decis. 2020, 40, 252–286. [Google Scholar] [CrossRef]
- Sell, T.; Lien, O.; Toner, E. A Framework for Healthcare Resilience during Widespread Electrical Power Loss. J. Crit. Infrastruct. Policy 2020, 1, 13–26. [Google Scholar] [CrossRef]
- Mills, C.E.; Robins, J.M.; Lipsitch, M. Transmissibility of 1918 pandemic influenza. Nature 2004, 432, 904–906. [Google Scholar] [CrossRef] [PubMed]
- Sanche, S.; Lin, Y.T.; Xu, C.; Romero-Severson, E.; Hengartner, N.; Ke, R. High Contagiousness and Rapid Spread of Severe Acute Respiratory Syndrome Coronavirus 2. Emerg. Infect. Dis. 2020, 26, 1470–1477. [Google Scholar] [CrossRef] [PubMed]
- Dehning, J.; Zierenberg, J.; Spitzner, F.P.; Wibral, M.; Neto, J.P.; Wilczek, M.; Priesemann, V. Inferring change points in the spread of COVID-19 reveals the effectiveness of interventions. Science 2020, 369, eabb9789. [Google Scholar] [CrossRef]
- Khachfe, H.H.; Chahrour, M.; Sammouri, J.; Salhab, H.A.; Makki, B.E.; Fares, M.Y. An Epidemiological Study on COVID-19: A Rapidly Spreading Disease. Cureus 2020, 12, e7313. [Google Scholar] [CrossRef] [Green Version]
- Lurie, N. Engla, Journal-2010-New engla nd journal. N. Engl. J. Med. 2020, 41, 1969–1973. [Google Scholar] [CrossRef]
- Goldfarb, D.S.; Benstein, J.A.; Zhdanova, O.; Hammer, E.; Block, C.A.; Caplin, N.J.; Thompson, N.; Charytan, D.M. Impending shortages of kidney replacement therapy for covid-19 patients. Clin. J. Am. Soc. Nephrol. 2020, 15, 880–882. [Google Scholar] [CrossRef]
- Rasmussen, S.; Sperling, P.; Poulsen, M.S.; Emmersen, J.; Andersen, S. Medical students for health-care staff shortages during the COVID-19 pandemic. Lancet 2020, 395, e79–e80. [Google Scholar] [CrossRef]
- Badreldin, H.A.; Atallah, B. Global drug shortages due to COVID-19: Impact on patient care and mitigation strategies. Res. Soc. Adm. Pharm. 2020, 17, 1946–1949. [Google Scholar] [CrossRef]
- Inoue, H.; Todo, Y. The propagation of economic impacts through supply chains: The case of a mega-city lockdown to prevent the spread of COVID-19. PLoS ONE 2020, 15, e0239251. [Google Scholar] [CrossRef]
- Guan, D.; Wang, D.; Hallegatte, S.; Davis, S.J.; Huo, J.; Li, S.; Bai, Y.; Lei, T.; Xue, Q.; Coffman, D.; et al. Global supply-chain effects of COVID-19 control measures. Nat. Hum. Behav. 2020, 4, 577–587. [Google Scholar] [CrossRef] [PubMed]
- Djalante, R.; Shaw, R.; DeWit, A. Building resilience against biological hazards and pandemics: COVID-19 and its implications for the Sendai Framework. Prog. Disaster Sci. 2020, 6, 100080. [Google Scholar] [CrossRef] [PubMed]
- Panchal, N.; Kamal, R.; Orgera, K.; Cox, C.; Garfield, R.; Hamel, L.; Chidambaram, P. The implications of COVID-19 for mental health and substance use. Kais. Fam. Found. 2020, 21, 1–16. [Google Scholar]
- Marko, C.; Andro, K.; Petrana, B. Stay home while going out–possible impacts of earthquake co-occurring with COVID-19 pandemic on mental health and vice versa. Brain Behav. Immun. 2020, 87, 82. [Google Scholar] [CrossRef]
- Ma, L.; Shapira, G.; De Walque, D.; Do, Q.T.; Friedman, J.; Levchenko, A.A. The Intergenerational Mortality Tradeoff of COVID-19 Lockdown Policies; Technical Report; National Bureau of Economic Research: Cambridge, MA, USA, 2021. [Google Scholar]
- Ravindran, S.; Shah, M. Unintended Consequences of Lockdowns: COVID-19 and the Shadow Pandemic; Working Paper 27562; National Bureau of Economic Research: Cambridge, MA, USA, 2020. [Google Scholar]
- Brown, C.S.; Ravallion, M. Inequality and the Coronavirus: Socioeconomic Covariates of Behavioral Responses and Viral Outcomes Across US Counties; Working Paper 27549; National Bureau of Economic Research: Cambridge, MA, USA, 2020. [Google Scholar]
- Benitez, J.A.; Courtemanche, C.J.; Yelowitz, A. Racial and Ethnic Disparities in COVID-19: Evidence from Six Large Cities; Working Paper 27592; National Bureau of Economic Research: Cambridge, MA, USA, 2020. [Google Scholar]
- Helgeson, J.F.; Aminpour, P.; Fung, J.F.; Henriquez, A.R.; Zycherman, A.; Butry, D.; Nierenberg, C.; Zhang, Y. Natural hazards compound COVID-19 impacts on small businesses disproportionately for historically underrepresented group operators. Int. J. Disaster Risk Reduct. 2022, 72, 102845. [Google Scholar] [CrossRef]
- Boustan, L.P.; Kahn, M.E.; Rhode, P.W.; Yanguas, M.L. The Effect of Natural Disasters on Economic Activity in US Counties: A Century of Data; Working Paper 23410; National Bureau of Economic Research: Cambridge, MA, USA, 2017. [Google Scholar]
- Hsiang, S.M.; Jina, A.S. The Causal Effect of Environmental Catastrophe on Long-Run Economic Growth: Evidence From 6700 Cyclones; Working Paper 20352; National Bureau of Economic Research: Cambridge, MA, USA, 2014. [Google Scholar]
- Jordà, s.; Singh, S.R.; Taylor, A.M. Longer-Run Economic Consequences of Pandemics; Working Paper 26934; National Bureau of Economic Research: Cambridge, MA, USA, 2020. [Google Scholar]
- Noy, I.; Doan, N.; Ferrarini, B.; Park, D. Measuring the Economic Risk of COVID-19. Glob. Policy 2020, 11, 413–423. [Google Scholar] [CrossRef]
- Cavallo, E.; Galiani, S.; Noy, I.; Pantano, J. Catastrophic natural disasters and economic growth. Rev. Econ. Stat. 2013, 95, 1549–1561. [Google Scholar] [CrossRef] [Green Version]
- Ramalanjaona, G. Impact of 2004 tsunami in the islands of Indian ocean: Lessons learned. Emerg. Med. Int. 2011, 2011, 920813. [Google Scholar] [CrossRef] [PubMed]
- Guha-Sapir, D.; van Panhuis, W.G. Health impact of the 2004 Andaman Nicobar earthquake and tsunami in Indonesia. Prehospital Disaster Med. 2009, 24, 493–499. [Google Scholar] [CrossRef] [Green Version]
- Doocy, S.; Cherewick, M.; Kirsch, T. Mortality following the Haitian earthquake of 2010: A stratified cluster survey. Popul. Health Metr. 2013, 11, 5. [Google Scholar] [CrossRef] [Green Version]
- Miyagawa, S.; Satoh, M.; Furuya, S.; Yamada, Y.; Shaw, R. External Support and Community Cooperation during Long-Term Sheltering—From the Case of the Great East Japan Earthquake. In Public Health and Disasters; Springer: Berlin/Heidelberg, Germany, 2020; pp. 201–219. [Google Scholar]
- Kondo, H.; Seo, N.; Yasuda, T.; Hasizume, M.; Koido, Y.; Ninomiya, N.; Yamamoto, Y. Post-flood—Infectious diseases in Mozambique. Prehospital Disaster Med. 2002, 17, 126–133. [Google Scholar] [CrossRef] [PubMed]
- Mousavi, S.; Bagchi, A.; Kodur, V.K. Review of post-earthquake fire hazard to building structures. Can. J. Civ. Eng. 2008, 35, 689–698. [Google Scholar] [CrossRef]
- Gunter, P. U.S. Unprepared for Nuclear Accident during Pandemic. 2020. Available online: https://www.commondreams.org/newswire/2020/05/22/us-unprepared-nuclear-accident-during-pandemic (accessed on 31 May 2020).
- Watson, J.T.; Gayer, M.; Connolly, M.A. Epidemics after natural disasters. Emerg. Infect. Dis. 2007, 13, 1–5. [Google Scholar] [CrossRef]
- Lemonick, D.M. Epidemics after natural disasters. Am. J. Clin. Med. 2011, 8, 144–152. [Google Scholar]
- Kouadio, I.K.; Aljunid, S.; Kamigaki, T.; Hammad, K.; Oshitani, H. Infectious diseases following natural disasters: Prevention and control measures. Expert Rev. Anti-Infect. Ther. 2012, 10, 95–104. [Google Scholar] [CrossRef]
- Spiegel, P.B.; Le, P.; Ververs, M.T.; Salama, P. Occurrence and overlap of natural disasters, complex emergencies and epidemics during the past decade (1995–2004). Confl. Health 2007, 1, 2. [Google Scholar] [CrossRef] [Green Version]
- IASC Working Group XVI-th Meeting. Definition of Complex Emergencies; Technical Report; Inter-Agency Standing Committee: New York, NY, USA, 1994. [Google Scholar]
- Salama, P.; Spiegel, P.; Talley, L.; Waldman, R. Lessons learned from complex emergencies over past decade. Lancet 2004, 364, 1801–1813. [Google Scholar] [CrossRef]
- Hariri-Ardebili, M.A. Living in a multi-risk chaotic condition: Pandemic, natural hazards and complex emergencies. Int. J. Environ. Res. Public Health 2020, 17, 5635. [Google Scholar] [CrossRef]
- Deryugina, T.; Gruber, J.; Sabety, A. Natural Disasters and Elective Medical Services: How Big is the Bounce-Back? Working Paper 27505; National Bureau of Economic Research: Cambridge, MA, USA, 2020. [Google Scholar]
- Ishiwatari, M.; Koike, T.; Hiroki, K.; Toda, T.; Katsube, T. Managing disasters amid COVID-19 pandemic: Approaches of response to flood disasters. Prog. Disaster Sci. 2020, 6, 100096. [Google Scholar] [CrossRef]
- Ebrahim, S.H.; Memish, Z.A. COVID-19–the role of mass gatherings. Travel Med. Infect. Dis. 2020, 34, 101617. [Google Scholar] [CrossRef]
- Dincer, O.; Gillanders, R. Shelter in place? Depends on the place: Corruption and social distancing in American states. Soc. Sci. Med. 2021, 269, 113569. [Google Scholar] [CrossRef]
- Bambarén, C. Legal issues of humanitarian assistance after the 2007 earthquake in Pisco, Peru. Prehospital Disaster Med. 2010, 25, 203–206. [Google Scholar] [CrossRef] [PubMed]
- Li, X.H.; Zheng, J.C. Efficient post-disaster patient transportation and transfer: Experiences and lessons learned in emergency medical rescue in Aceh after the 2004 Asian tsunami. Mil. Med. 2014, 179, 913–919. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- World Health Organization. Minimum Technical Standards and Recommendations for Rehabilitation—Emergency Medical Teams; Technical Report; World Health Organization: Geneva, Switzerland, 2016. [Google Scholar]
- Fakhruddin, B.; Blanchard, K.; Ragupathy, D. Are we there yet? The transition from response to recovery for the COVID-19 pandemic. Prog. Disaster Sci. 2020, 7, 100102. [Google Scholar] [CrossRef] [PubMed]
- Kirsch, T.D.; Mitrani-Reiser, J.; Bissell, R.; Sauer, L.M.; Mahoney, M.; Holmes, W.T.; Santa Cruz, N.; De La Maza, F. Impact on hospital functions following the 2010 Chilean earthquake. Disaster Med. Public Health Prep. 2010, 4, 122–128. [Google Scholar] [CrossRef] [PubMed]
- Yavari, S.; Chang, S.E.; Elwood, K.J. Modeling post-earthquake functionality of regional health care facilities. Earthq. Spectra 2010, 26, 869–892. [Google Scholar] [CrossRef]
- Ceferino, L.; Kiremidjian, A.S.; Deierlein, G.G. Probabilistic Model for Regional Multiseverity Casualty Estimation due to Building Damage Following an Earthquake. Spec. Collect. ASCE-ASME J. Risk Uncertain. Eng. Syst. Part A Civ. Eng. 2018, 4, 04018023. [Google Scholar] [CrossRef]
- Ceferino, L.; Mitrani-Reiser, J.; Kiremidjian, A.; Deierlein, G.; Bambarén, C. Effective plans for hospital system response to earthquake emergencies. Nat. Commun. 2020, 11, 1–12. [Google Scholar] [CrossRef]
- Helgeson, J.F.; Fung, J.F.; Roa-Henriques, A.; Zhang, Y.; Zycherman, A.; Nierenberg, C.; Butry, D.T.; Ramkissoon, D. Complex Event Resilience of Small- and Medium-Sized Enterprises: Natural Disaster Planning during the COVID-19 Pandemic; Special Publication Forthcoming; National Institute of Standards and Technology: Gaithersburg, MD, USA, 2020.
- Wang, Z.; Ye, X. Social media analytics for natural disaster management. Int. J. Geogr. Inf. Sci. 2018, 32, 49–72. [Google Scholar] [CrossRef]
- Li, Z.; Wang, C.; Emrich, C.T.; Guo, D. A novel approach to leveraging social media for rapid flood mapping: A case study of the 2015 South Carolina floods. Cartogr. Geogr. Inf. Sci. 2018, 45, 97–110. [Google Scholar] [CrossRef]
- Fearnley, C.J.; Dixon, D. Early warning systems for pandemics: Lessons learned from natural hazards. Int. J. Disaster Risk Reduct. 2020, 49, 101674. [Google Scholar] [CrossRef] [PubMed]
- AI-Youbi, A.O.; Al-Hayani, A.; Bardesi, H.J.; Basheri, M.; Lytras, M.D.; Aljohani, N.R. The King Abdulaziz University (KAU) pandemic framework: A methodological approach to leverage social media for the sustainable management of higher education in crisis. Sustainability 2020, 12, 4367. [Google Scholar] [CrossRef]
- Zhou, S. Impact of pandemic proximity and media use on risk perception during COVID-19 in China. Geomat. Nat. Hazards Risk 2022, 13, 591–609. [Google Scholar] [CrossRef]
- Mirbabaie, M.; Bunker, D.; Stieglitz, S.; Marx, J.; Ehnis, C. Social media in times of crisis: Learning from Hurricane Harvey for the coronavirus disease 2019 pandemic response. J. Inf. Technol. 2020, 35, 195–213. [Google Scholar] [CrossRef]
- Mukherjee, S.; Kumar, R.; Bala, P.K. Managing a natural disaster: Actionable insights from microblog data. J. Decis. Syst. 2022, 31, 134–149. [Google Scholar] [CrossRef]
- Eyre, R.; De Luca, F.; Simini, F. Social media usage reveals recovery of small businesses after natural hazard events. Nat. Commun. 2020, 11, 1–10. [Google Scholar] [CrossRef] [PubMed]
- Bostick, T.P. Ten Strategies for Leadership during COVID-19: A Plan of Action for Decision Makers in Times of Critical Change. In COVID-19: Systemic Risk and Resilience; Springer: Cham, Switzerland, 2021; pp. 11–16. [Google Scholar]
- Gilbert, A.Q.; Bazilian, M.D. The COVID-19 Pandemic: Energy Market Disruptions and Resilience. J. Crit. Infrastruct. Policy 2020, 1, 73–83. [Google Scholar] [CrossRef]
- Kawamura, Y.; Dewan, A.M.; Veenendaal, B.; Hayashi, M.; Shibuya, T.; Kitahara, I.; Nobuhara, H.; Ishii, K. Using GIS to develop a mobile communications network for disaster-damaged areas. Int. J. Digit. Earth 2014, 7, 279–293. [Google Scholar] [CrossRef]
- Shah, P.; Patel, C.R. Prevention is better than cure: An application of big data and geospatial technology in mitigating pandemic. Trans. Indian Natl. Acad. Eng. 2020, 5, 187–192. [Google Scholar] [CrossRef]
- Hill, S.; Hutton, N.S.; Whytlaw, J.L.; Yusuf, J.E.; Behr, J.G.; Landaeta, E.; Diaz, R. Changing Logistics of Evacuation Transportation in Hazardous Settings during COVID-19. Nat. Hazards Rev. 2021, 22, 04021029. [Google Scholar] [CrossRef]
- Rajabifard, A.; Paez, D.; Foliente, G. COVID-19 Pandemic, Geospatial Information, and Community Resilience: Global Applications and Lessons; Taylor & Francis: Abingdon, UK, 2021. [Google Scholar]
- Nakai, H.; Itatani, T.; Horiike, R. Construction of an evacuee placement model for tsunami shelters considering physical distancing to prevent COVID-19 infection. Prog. Disaster Sci. 2021, 11, 100183. [Google Scholar] [CrossRef]
- Ghorbanzadeh, M. Accessibility-Based Assessment and Modeling of Evacuations and Sheltering for Hurricanes and Pandemics. Ph.D. Thesis, The Florida State University, Tallahassee, FL, USA, 2021. [Google Scholar]
- Page-Tan, C.; Fraser, T. CoViD-19 to go? The role of disasters and evacuation in the CoViD-19 pandemic. Glob. Environ. Chang. 2022, 73, 102471. [Google Scholar] [CrossRef] [PubMed]
- Hariri-Ardebili, M.A.; Lall, U. Superposed natural hazards and pandemics: Breaking dams, floods, and COVID-19. Sustainability 2021, 13, 8713. [Google Scholar] [CrossRef]
- Tripathy, S.S.; Bhatia, U.; Mohanty, M.; Karmakar, S.; Ghosh, S. Flood evacuation during pandemic: A multi-objective framework to handle compound hazard. Environ. Res. Lett. 2021, 16, 034034. [Google Scholar] [CrossRef]
- Hutton, N.S.; Mumford, S.W.; Saitgalina, M.; Yusuf, J.E.; Behr, J.G.; Diaz, R.; Kiefer, J.J. Nonprofit capacity to manage hurricane-pandemic threat: Local and national perspectives on resilience during COVID-19. Int. J. Public Adm. 2021, 44, 984–993. [Google Scholar] [CrossRef]
- Dargin, J.S.; Li, Q.; Jawer, G.; Xiao, X.; Mostafavi, A. Compound hazards: An examination of how hurricane protective actions could increase transmission risk of COVID-19. Int. J. Disaster Risk Reduct. 2021, 65, 102560. [Google Scholar] [CrossRef] [PubMed]


Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Hariri-Ardebili, M.A.; Sattar, S.; Johnson, K.; Clavin, C.; Fung, J.; Ceferino, L. A Perspective towards Multi-Hazard Resilient Systems: Natural Hazards and Pandemics. Sustainability 2022, 14, 4508. https://doi.org/10.3390/su14084508
Hariri-Ardebili MA, Sattar S, Johnson K, Clavin C, Fung J, Ceferino L. A Perspective towards Multi-Hazard Resilient Systems: Natural Hazards and Pandemics. Sustainability. 2022; 14(8):4508. https://doi.org/10.3390/su14084508
Chicago/Turabian StyleHariri-Ardebili, Mohammad Amin, Siamak Sattar, Katherine Johnson, Christopher Clavin, Juan Fung, and Luis Ceferino. 2022. "A Perspective towards Multi-Hazard Resilient Systems: Natural Hazards and Pandemics" Sustainability 14, no. 8: 4508. https://doi.org/10.3390/su14084508
APA StyleHariri-Ardebili, M. A., Sattar, S., Johnson, K., Clavin, C., Fung, J., & Ceferino, L. (2022). A Perspective towards Multi-Hazard Resilient Systems: Natural Hazards and Pandemics. Sustainability, 14(8), 4508. https://doi.org/10.3390/su14084508









