Alternative Leadership in Flexible Surge Capacity—The Perceived Impact of Tabletop Simulation Exercises on Thai Emergency Physicians Capability to Manage a Major Incident
Abstract
:1. Introduction
2. Aim
3. Method
3.1. Population
3.2. Course Design
3.3. Pre- and Post-Course Test
3.4. Observational Evaluation
3.5. Observational Evaluation
4. Results
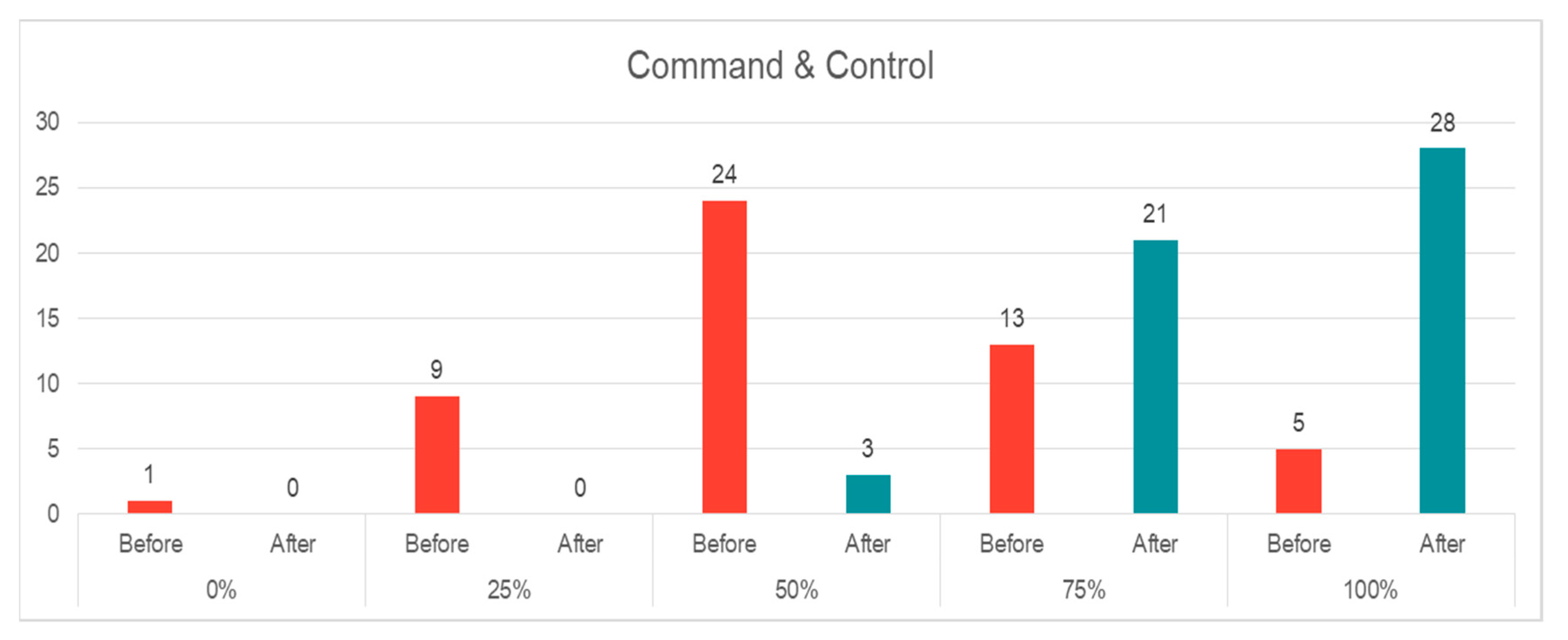
- Command and control (C2): There was an increasing knowledge of C2 after the course. Around 20% of the EPs (n = 10) had little or very little knowledge about C2, and 46% (n = 24) had medium knowledge. At the end of the course, there was a shift to the positive end, where the majority of our participants had a good to a very good understanding of C2 function (n = 49, 94%) (Figure 1). The change was statistically significant (p = 0.00, z = −5.436).
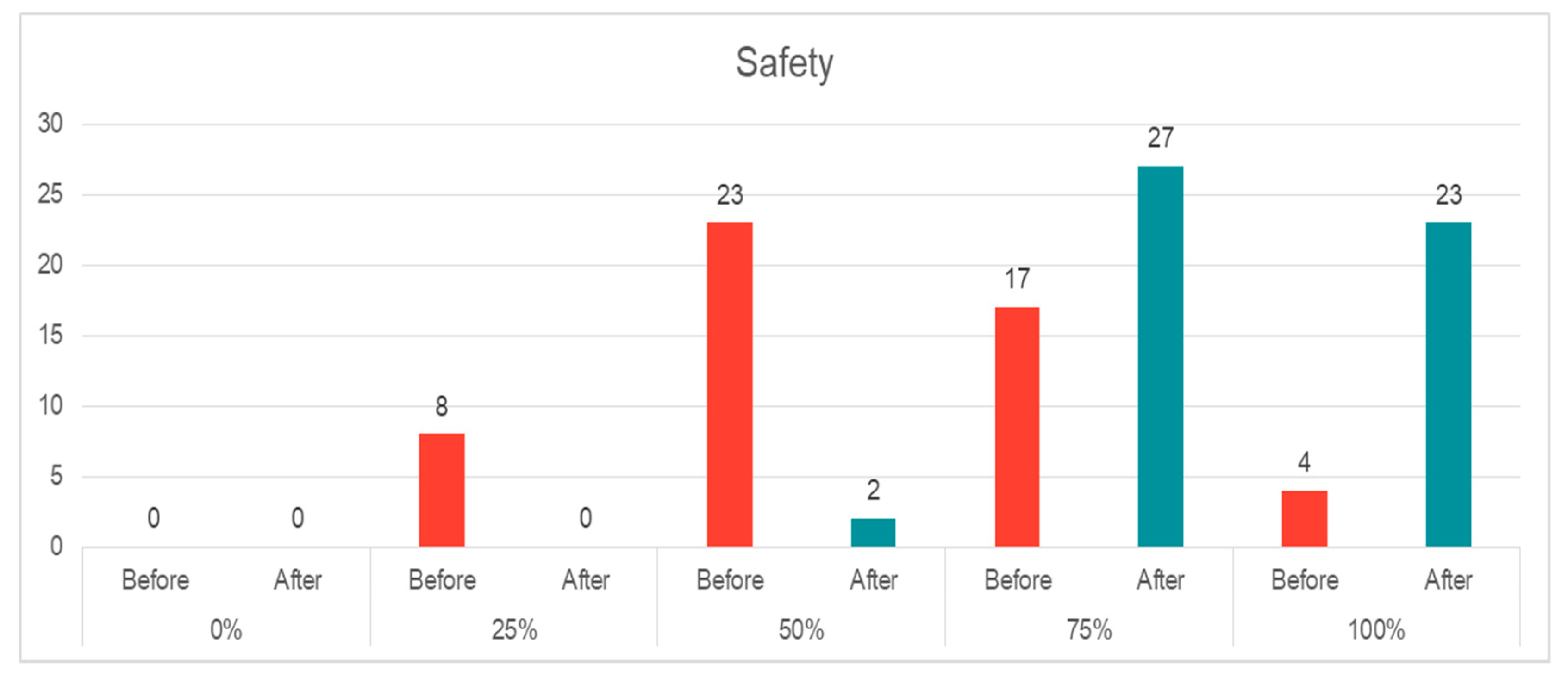
- Safety: There was an increasing knowledge of safety issues after the course. Around 15% of the EPs (n = 8) had no or very little knowledge about safety issues, and 44% (n = 23) had medium knowledge. At the end of the course, there was a shift to the positive end, where the majority of our participants had a good to a very good understanding of safety issues (n = 50, 96%) (Figure 2). The change was statistically significant (p = 0.00, z = −6.056).
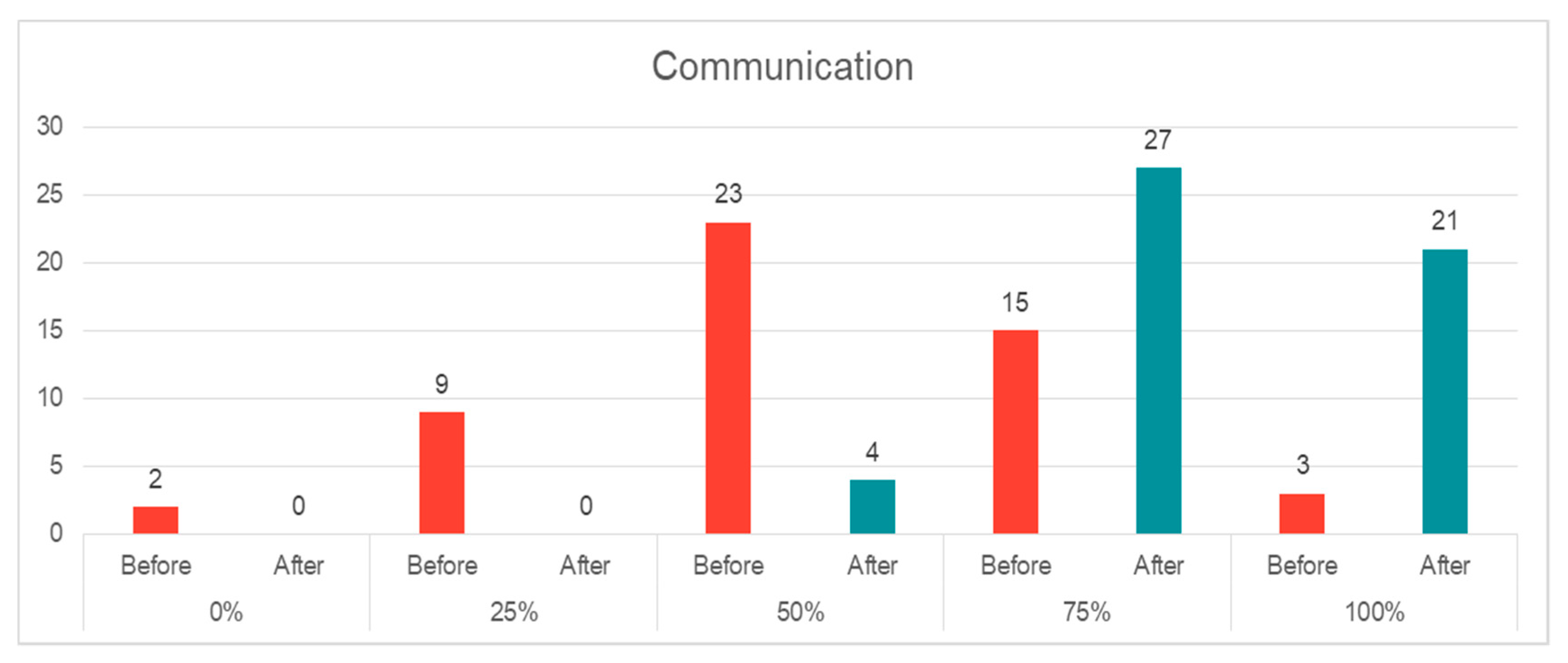
- Communication: There was an increasing knowledge of communication ways and difficulties after the course. Around 21% (n = 11) of the EPs had none or very little knowledge about communications issues, and 44% (n = 23) had medium knowledge. At the end of the course, there was a shift to the positive end, where the majority of our participants had a good to a very good understanding of safety issues (n = 48, 92%) (Figure 3). The change was statistically significant (p = 0.00, z = −5.872).
- Assessment: There was an increasing knowledge about the importance of the assessment during a major incident after the course. Around 17% (n = 9) of the EPs had no or very little knowledge about assessment and its association with the incident management, and 48% (n = 25) had medium knowledge. At the end of the course, there was a shift to the positive end, where the majority of our participants had a good to a very good understanding of assessment issues (n = 48, 92%) (Figure 4). The change was statistically significant (p = 0.00, z = −5.464).
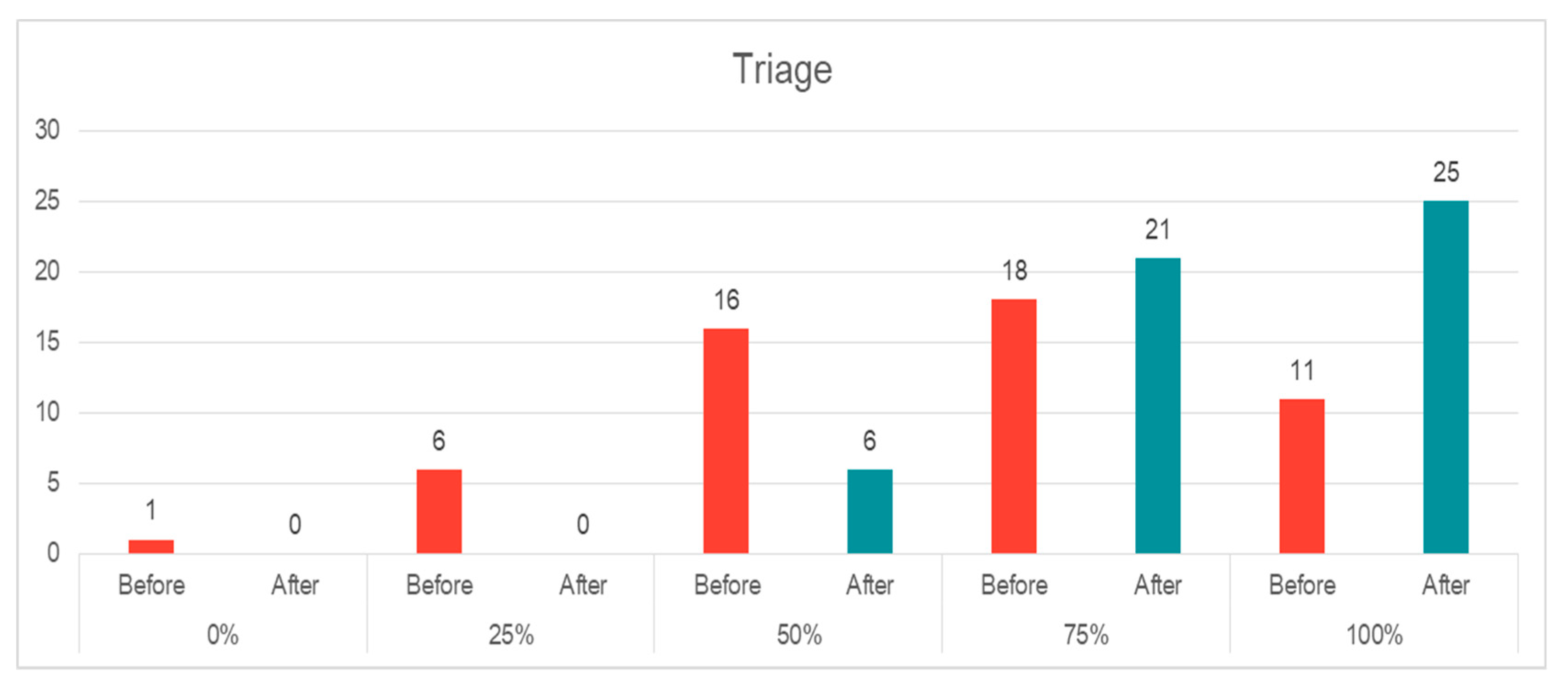
- Triage: There was an increasing knowledge about the importance of triage and associated dilemmas during a major incident after the course. Around 17% (n = 9) of the EPs had no or very little knowledge about triage and its role during incident management, and 30% (n = 16) had medium knowledge. Although 29 EPs reported a good or very good knowledge, there was still a shift to the positive end at the end of the course, where the majority of our participants had a good to a very good understanding of triage issues (n = 46, 88%) (Figure 5). The change was statistically significant (p = 0.00, z = −4.585).
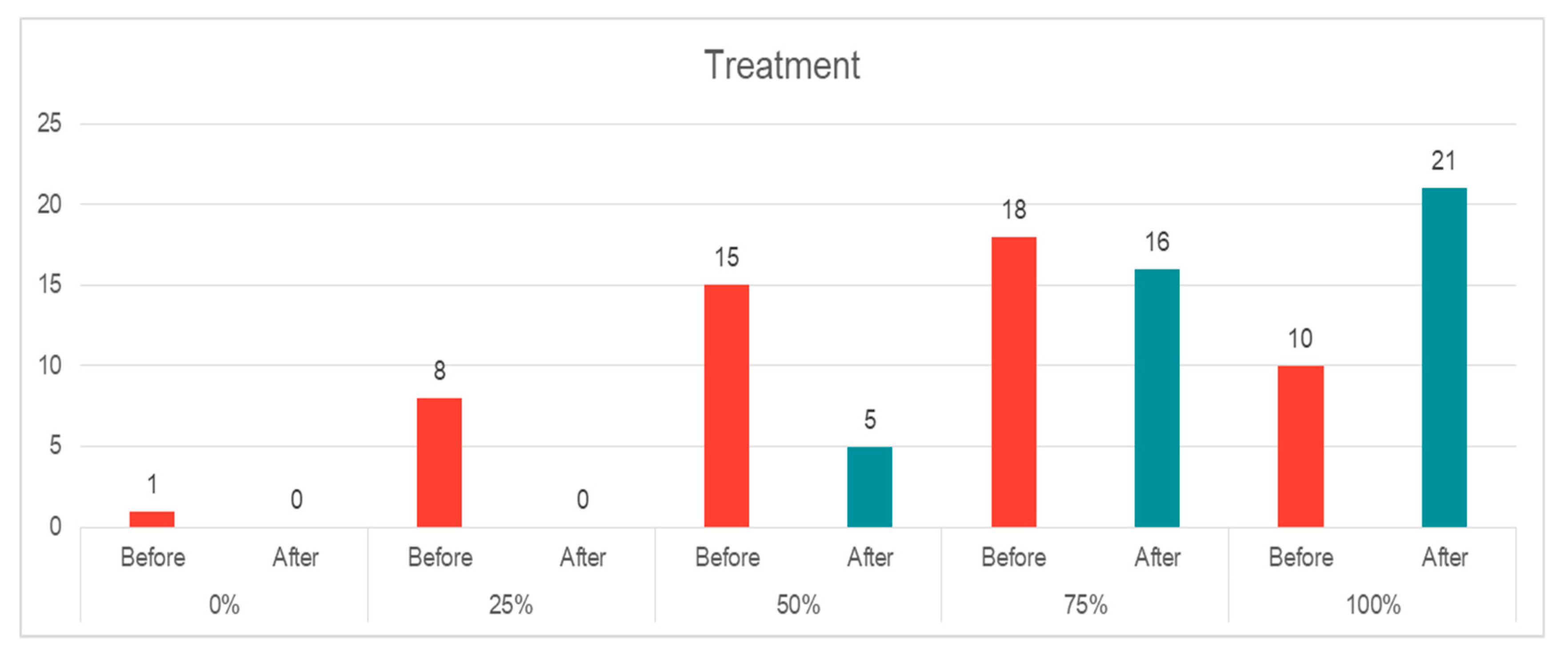
- Treatment: There was an increasing knowledge about the treatment alternatives and options at the right time and right place during a major incident after the course. Around 17% (n = 9) of the EPs had none or very little knowledge about the treatment given during incident management, and 28% (n = 15) had medium knowledge. Although 28 EPs reported good or very good knowledge, there was still a shift to the positive end at the end of the course, where the majority of the participants had good to a very good understanding of triage issues (n = 37, 71%) (Figure 6). The change was statistically significant (p = 0.00, z = −5.287).
- Transport: There was an increasing knowledge about the importance of triage and associated dilemmas during a major incident after the course. Around 21% (n = 11) of the EPs had none or very little knowledge about triage and its role during incident management, and 32% (n = 17) had medium knowledge. At the end of the course, there was a shift to the positive end, where the majority of our participants had a good to a very good understanding of assessment issues (n = 38, 73%) (Figure 7). The change was statistically significant (p = 0.00, z = −5.634).
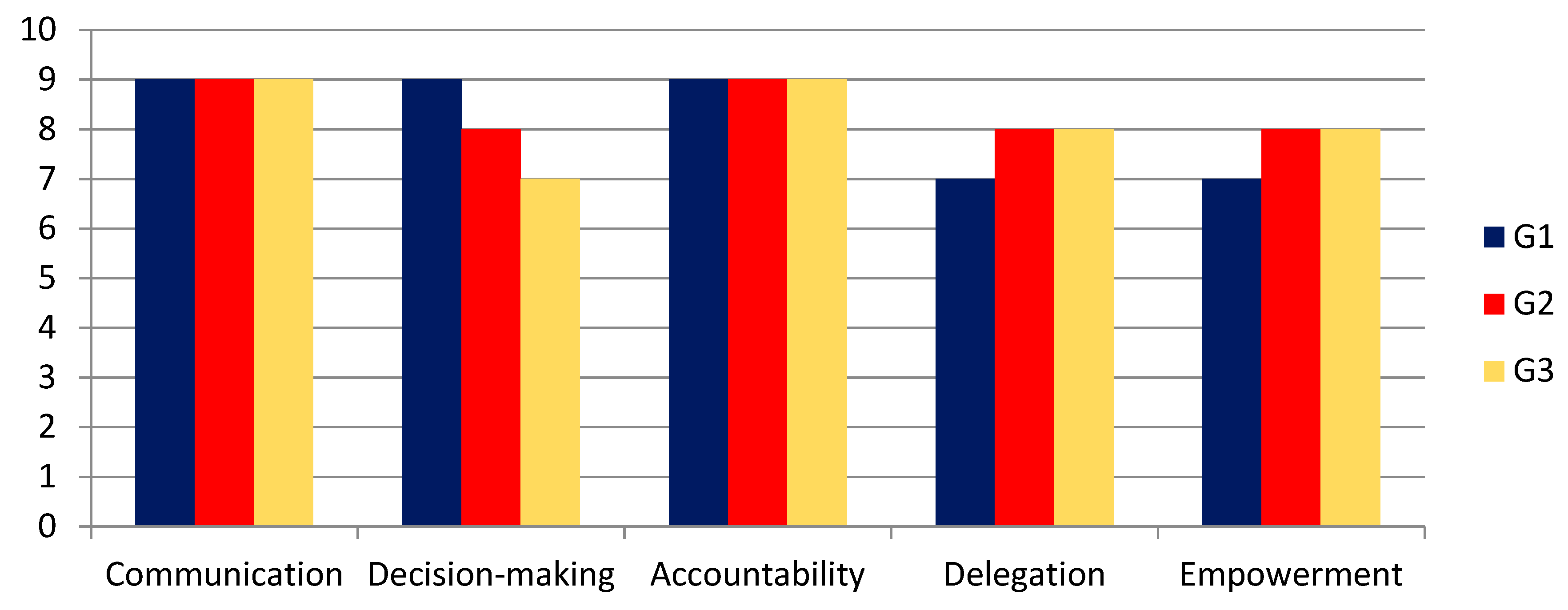
- Observations: Two critical observations were reported (Figure 8). Both observers collected their documented results in which they had specifically commented on the ability of decision-making, communication, accountability, empowerment of other group member and delegation of tasks. Consensus was made and the groups were exposed to the observers’ understanding to unearth individual motivations or behaviors that were not immediately obvious in a group setting [24,25].
- During the exercises, each team selected its leader with three leadership styles, without any previous knowledge and spontaneously;
- Consensus leadership (G3): The leader tried to reach consensus with other members before any decision. Slower decision-making process.
- Passive leadership (G2): The leader laid back and observed other members and only interrupted if needed. Decisions were made, but sometimes not of the leader.
- Active Leadership (G1): The leader had the last word in every decision and continuously directed the group. Less delegation and empowerment.
- Each group developed its communication method consisting of a mobile telephone, paper-based messages, and signs.
5. Discussion
6. Limitations
7. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
Appendix A
Appendix A.1. Scenarios, 3LC Exercises, Bangkok, Thailand
Scenario 1: A bomb
Scenario 2: A Fire in a Tall Building
Scenario 3: Riot and Active Shooter
References
- WHO. Hospital Emergency Response Checklist. An All-Hazards Tool for Hospital Administrators and Emergency Managers. 2011. Available online: http://www.euro.who.int/__data/assets/pdf_file/0008/268766/Hospital-emergency-response-checklist-Eng.pdf (accessed on 25 June 2020).
- Vitalii, S.; Khorram-Manesh, A.; Nyberg, L. Disaster cycle and management. In Handbook of Disaster and Emergency Management; Khorram-Manesh, A., Ed.; Kompendiet: Göteborg, Sweden, 2017; Chapter 2; pp. 23–29. [Google Scholar]
- United Nations International Strategy for Disaster Reduction (UNISDR). Terminology on Disaster Risk Reduction; United Nations: Geneva, Switzerland, 2009; Available online: https://www.unisdr.org/files/7817_UNISDRTerminologyEnglish.pdf (accessed on 25 June 2020).
- Hick, J.; Christian, M.; Sprung, C. Surge Capacity and Infrastructure considerations for mass critical care. Intensive Care Med. 2010, 36, 11–20. [Google Scholar] [CrossRef]
- Barbich, D.; Koenig, K. Understanding Surge Capacity: Essential Elements. Acad. Emerg. Med. 2006, 6, 1098–1102. [Google Scholar] [CrossRef] [PubMed]
- Kaji, A.; Koenig, K.L.; Bey, T. Surge capacity for healthcare systems: A conceptual framework. Acad. Emerg. Med. 2006, 13, 1157–1159. [Google Scholar] [CrossRef] [PubMed]
- Bonnet, C.; Peery, B.; Cantrill, S.; Pons, P.; Haukoos, J.; McVaney, K.; Colwell, C. Surge capacity: A proposed conceptual framework. Am. J. Emerg. Med. 2007, 25, 297–306. [Google Scholar] [CrossRef] [PubMed]
- Runkle, J.D.; Brock-Martin, A.; Karmus, W.; Svendsen, E.R. Secondary Surge Capacity: A framework for understanding long-term access to primary care for medically vulnerable populations in disaster recovery. Am. J. Public Health 2012, 102, 24–32. [Google Scholar] [CrossRef] [PubMed]
- Adams, L.M. Exploring the concept of surge capacity. Issues Nurs. 2009, 14, 2. [Google Scholar] [CrossRef]
- Khorram-Manesh, A. Flexible Surge Capacity—Public Health, Public Education, and Disaster Management. Health Promot. Perspect 2020, 10, 175–179. [Google Scholar] [CrossRef]
- The Lancet Editorial. Disaster prevention should be equal. Lancet Glob. Health 2017, 5, 1047. [Google Scholar] [CrossRef]
- Krolik, M. Exploring a rights-based approach to disaster management. Aust. J. Emerg. Manag. 2013, 28, 44–48. Available online: https://knowledge.aidr.org.au/resources/ajem-oct-2013-exploring-a-rights-based-approach-to-disaster-management/ (accessed on 14 July 2020).
- Rice, K.; Felizzi, M.V.; Hagelgans, D. Human Rights-Based Approach to Disaster Management: Valparaiso, Chile. J. Hum. Rights Soc. Work 2017, 2, 117–127. [Google Scholar] [CrossRef] [Green Version]
- Prytz, E.G.; Rybing, J.; Carlström, E.; Khorram-Manesh, A.; Jonson, C.O. Exploring prehospital C2-work during a mass gathering event. Int. J. Emerg. Serv. 2015, 4, 227–241. [Google Scholar] [CrossRef] [Green Version]
- Khorram-Manesh, A.; Lönroth, H.; Rotter, P.; Wilhelmsson, M.; Aremyr, J.; Berner, A.; Nero Andersson, A.; Carlström, E. Non-medical aspects of civilian-military collaboration in management of major incidents. Eur. J. Trauma Emerg. Surg. 2017, 43, 595–603. [Google Scholar] [CrossRef] [Green Version]
- Khorram-Manesh, A.; Hedelin, A.; Örtenwall, P. Regional coordination in medical emergencies and major incidents; plan, execute and teach. Scand. J. Trauma Resusc. Emerg. Med. 2009, 17, 32. [Google Scholar] [CrossRef] [Green Version]
- Kahn, C.A.; Koenig, K.L.; Schultz, C.H. Emergency physician disaster deployment: Issues to consider and model policy. Prehosp. Disaster Med. 2017, 32, 462–464. [Google Scholar] [CrossRef]
- Sammut, J.; Cato, D.; Homer, T. Major Incident Medical Management and Support (MIMMS): A practical multiple casualty, disaster-site training course for all Australian healthcare personnel. Emerg. Med. 2001, 13, 174–180. [Google Scholar] [CrossRef]
- Sittichanbuncha, Y.; Prachanukool, T.; Sarathep, P.; Sawanyawisuth, K. An emergency medical service in Thailand—Providers perspectives. J. Med. Assoc. Thai 2014, 97, 1016–1021. [Google Scholar]
- Khorram-Manesh, A.; Angthong, C.; Pangma, A.; Sulannakarn, S.; Burivong, R.; Jarayabhand, R.; Örtenwall, P. Hospital Evacuation; Learning from the Past? Flooding of Bangkok 2011. BJMMR 2014, 4, 395–415. [Google Scholar] [CrossRef]
- Khorram-Manesh, A.; Berlin, J.; Carlström, E. Two validated ways of the ability of decision-making in emergencies, Results from a literature review. Bull. Emerg. Trauma 2016, 4, 186–196. [Google Scholar]
- Sorensen, J.; Magnussen, L.I.; Torgersen, G.E.; Christiansen, A.M.; Carlstrom, E. Percieved Usefulness of Maritime Cross-Border Collaboration Exercises. Arts Soc. Sci. J. 2018, 9, 1–5. [Google Scholar] [CrossRef]
- Magnussen, L.I.; Carlström, E.; Sörensen, J.L.; Torgersen, G.E.; Hagenes, E.F.; Kristiansen, E. Learning and Usefulness stemming from collaboration in a maritime crisis management exercise in Northern Norway. Disaster Prev. Manag. 2018, 27, 129–140. [Google Scholar] [CrossRef]
- Berlin, J.; Carlström, E. The three level collaboration exercise—Impact of learning and usefulness. J. Conting. Crisis Manag. (JCCM) 2015, 23, 257–265. [Google Scholar] [CrossRef]
- Aykal, G.; Kespali, M.; Aydin, Ö.; Esen, H.; Yegin, A.; Gungör, F.; Yilmaz, N. Pre-Test and Post-Test Applications to Shape the Education of Phlebotomists in a Quality Management Program: An Experience in a Training Hospital. J. Med. Biochem. 2016, 35, 347–353. [Google Scholar] [PubMed]
- Takala, E.P.; Pehkonen, I.; Forsman, M.; Hansson, G.Å.; Mathiassen, S.E.; Neumann, W.P.; Sjögaard, G.; Veiersted, K.B.; Westgaard, R.H.; Winkel, J. Systematic evaluation of observational methods assessing biomechanical exposures at work. Scand. J. Work Environ. Health 2010, 36, 3–24. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Luna-Reyes, L.F.; Lines Andersen, D. Collecting and analyzing qualitative data for system dynamics: Methods and models. Syst. Dyn. Rev. 2004. [Google Scholar] [CrossRef]
- Lofland, J.; Lofland, L.H. Analyzing Social Setting: A Guide to Qualitative Observation and Analysis, 2nd ed.; Wadsworth: Belmont, CA, USA, 1984. [Google Scholar]
- Moynihan, D.P. Learning under uncertainty: Networks in crisis management. Public Admin. Rev. 2008, 68, 350–365. [Google Scholar] [CrossRef] [Green Version]
- Glantz, V.; Phattharapornjaroen, P.; Carlström, E.; Khorram-Manesh, A. Regional Flexible Surge Capacity—A flexible response system. Sustainability 2020, 12, 5984. [Google Scholar] [CrossRef]
- World Health Organization (WHO). Sustainable Development Goals (SDGs). Available online: https://www.who.int/sdg/en/ (accessed on 25 June 2020).
- Khorram-Manesh, A.; Plegas, P.; Peyravi, M.; Carlström, E. Immediate Response to Major Incidents: Defining an immediate responder! Eur. J. Trauma Emerg. Surg. 2019. [Google Scholar] [CrossRef] [Green Version]
- Khorram-Manesh, A.; Berlin, J.; Ljung Roseke, L.; Aremyr, J.; Sörensson, J.; Carlström, E. Emergency Management and Preparedness Training for Youth (EMPTY): The Results of the First Swedish pilot Study. Disaster Med. Public Health Prep. 2018, 12, 685–688. [Google Scholar] [CrossRef]
- Khorram-Manesh, A. Learning to Respect Diversity, Gender Equality, and Collaboration: A childhood Agenda or the Content of a Leadership Development Program; Magnussen, L.I., Ed.; Disaster, Diversity, and Emergency Preparation; IOS Press: Amsterdam, The Netherlands, 2019; pp. 11–18. [Google Scholar] [CrossRef]
- Jahangirian, M.; Naseer, A.; Stergioulas, L.; Young, T.; Eldabi, T.; Brailsford, S.; Patel, B.; Harper, P. Simulation in health-care: Lessons from other sectors. Oper. Res. Int. J. 2012, 12, 45–55. [Google Scholar] [CrossRef]


© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Phattharapornjaroen, P.; Glantz, V.; Carlström, E.; Dahlén Holmqvist, L.; Khorram-Manesh, A. Alternative Leadership in Flexible Surge Capacity—The Perceived Impact of Tabletop Simulation Exercises on Thai Emergency Physicians Capability to Manage a Major Incident. Sustainability 2020, 12, 6216. https://doi.org/10.3390/su12156216
Phattharapornjaroen P, Glantz V, Carlström E, Dahlén Holmqvist L, Khorram-Manesh A. Alternative Leadership in Flexible Surge Capacity—The Perceived Impact of Tabletop Simulation Exercises on Thai Emergency Physicians Capability to Manage a Major Incident. Sustainability. 2020; 12(15):6216. https://doi.org/10.3390/su12156216
Chicago/Turabian StylePhattharapornjaroen, Phatthranit, Viktor Glantz, Eric Carlström, Lina Dahlén Holmqvist, and Amir Khorram-Manesh. 2020. "Alternative Leadership in Flexible Surge Capacity—The Perceived Impact of Tabletop Simulation Exercises on Thai Emergency Physicians Capability to Manage a Major Incident" Sustainability 12, no. 15: 6216. https://doi.org/10.3390/su12156216
APA StylePhattharapornjaroen, P., Glantz, V., Carlström, E., Dahlén Holmqvist, L., & Khorram-Manesh, A. (2020). Alternative Leadership in Flexible Surge Capacity—The Perceived Impact of Tabletop Simulation Exercises on Thai Emergency Physicians Capability to Manage a Major Incident. Sustainability, 12(15), 6216. https://doi.org/10.3390/su12156216






