COVID-19 Could Leverage a Sustainable Built Environment
Abstract
1. Introduction
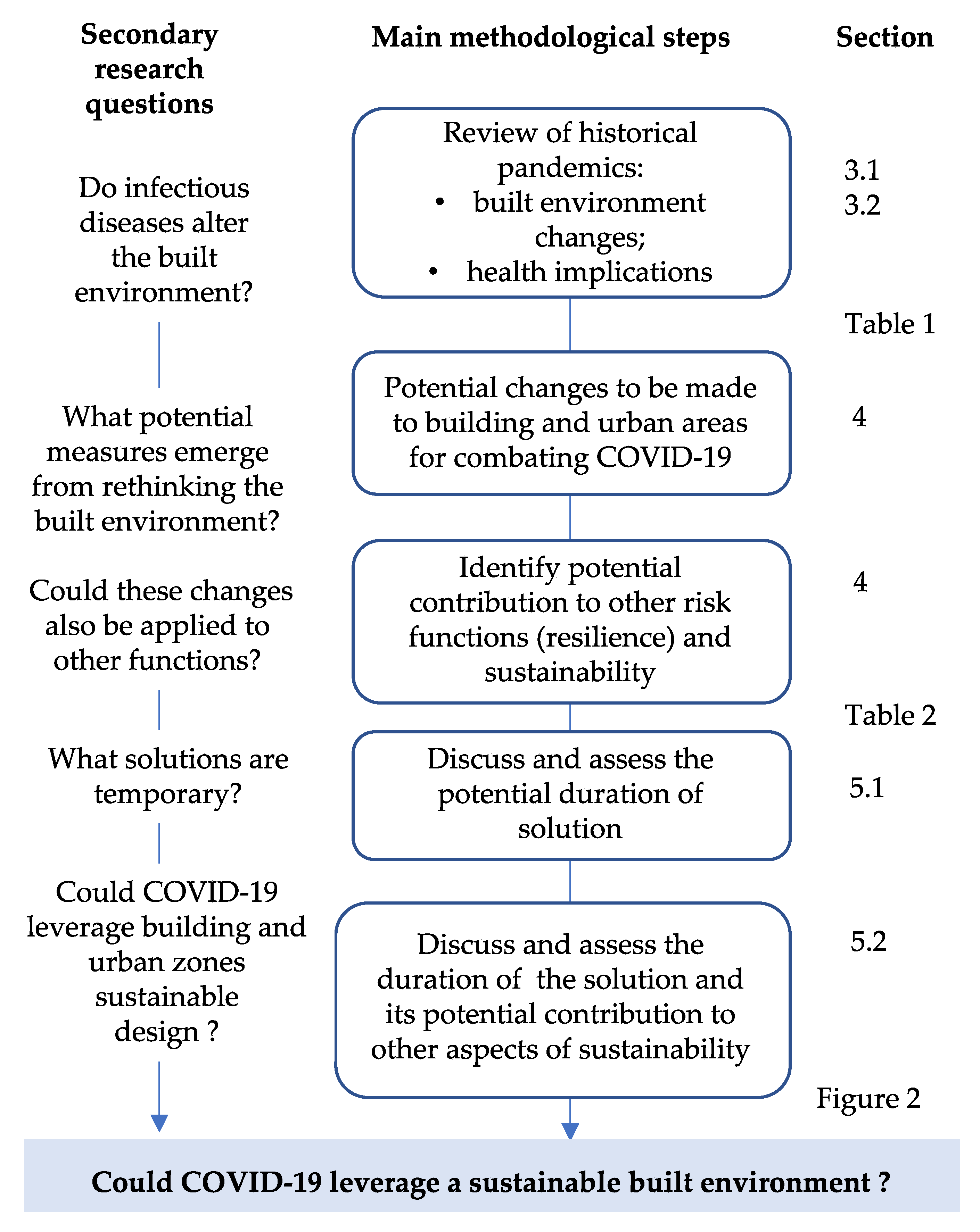
2. Research Methodology
- The duration (or the need for renewal) of the solution to ensure that it continues to function as a form of risk reduction, with the following time limits being stipulated: 1 day or less, 1 month or less, 1 year or less, 5 years or less, 10 years or less or 25 years.
- The level of benefit of potential solutions for COVID-19 risk reduction is defined on a scale from 0 to 5, where 0 means solutions that make no contribution; 1 corresponds to solutions that conform to public health conditions; 2 means solutions that reduce the risk of transmission; 3 means solutions that prevent transmission between people; 4 means solutions that prevent inter-community transmission; and 5 means solutions that provide ways of treating the virus.
- A scale from 0 to 10 was also defined to assess the contribution of the solution for COVID-19 to other aspects of sustainability, where 1 means that the solution brings only benefits in the fight against COVID-19 and 10 means that (in addition to having benefits for fighting COVID-19) the solution is also a potential solution with very positive impacts in terms of sustainability.
3. Can Infectious Disease Bring Alterations to the Built Environment?
3.1. Diseases and Alterations to the Built Environment
3.2. Urban Areas and Buildings Affect the Spread of Infectious Diseases
4. Rethinking Buildings and Urban Areas for Integrating Potential Measures to Control the COVID-19 Pandemic
4.1. Urban Areas
4.2. Buildings
5. Discussion
5.1. Which Solutions will not be Merely Temporary?
5.2. Could COVID-19 Risk Control Measures Leverage a Sustainable Built Environment?
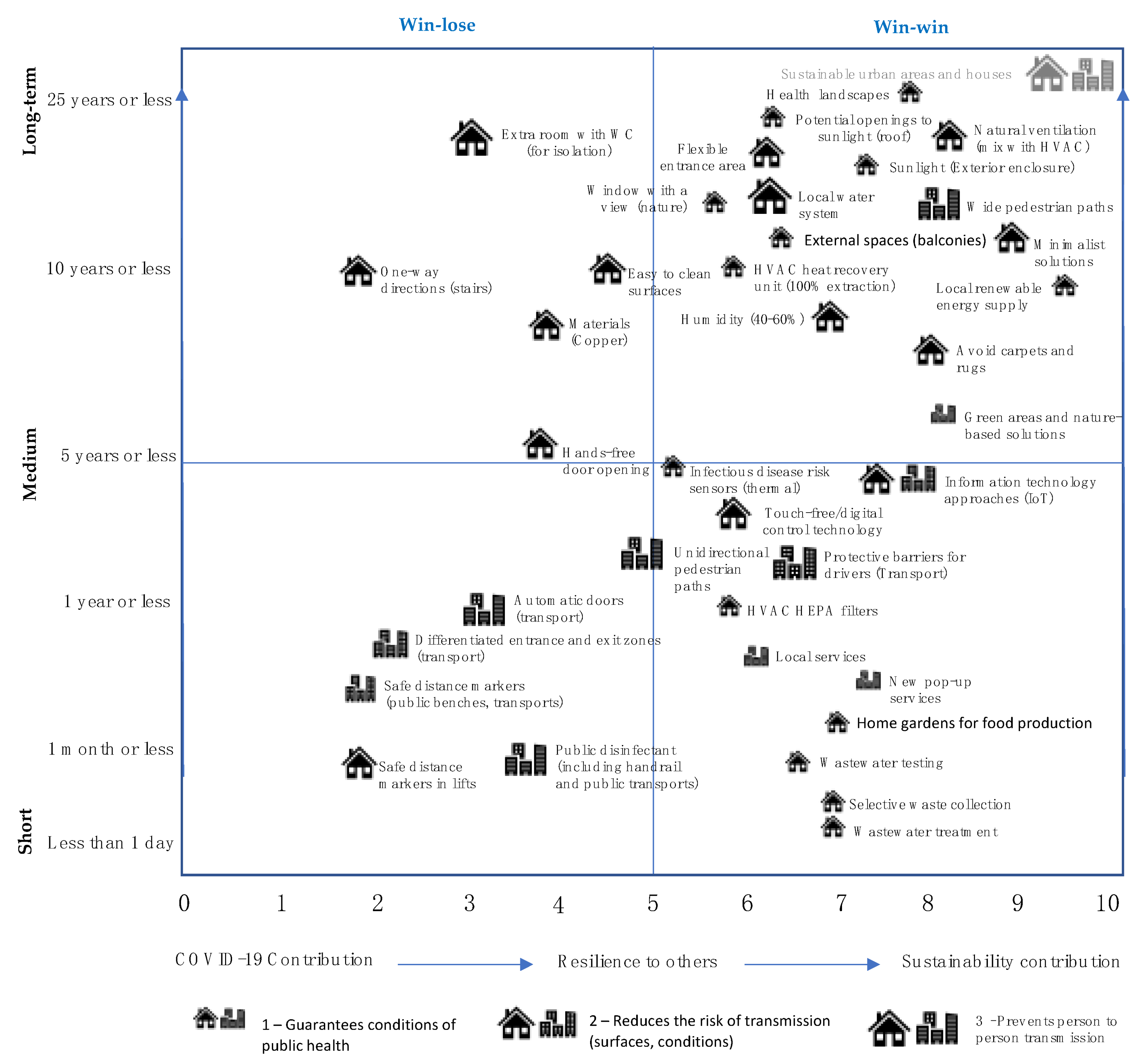
- Mainly COVID-19 risk reduction measures: safe distance markers (lifts, public transport), disinfectant, hands-free door opening or possible replacements of materials with others (such as copper) that reduce virus residence time, unidirectional stairs. When the outbreak finishes, the potential of these measures will also end, although they may return in the event of other outbreaks, so they may be considered temporary or intermittent;
- Incremental measures: measures that will also bring benefits in terms of increasing resilience and whose potential could be adopted in the future, such as thermal sensors, new HVAC filters, touch-free digital and other IT solutions, unidirectional pedestrian paths; supplementary wastewater monitoring and treatment, more selective solid waste collection and treatment;
- Factorial measures: measures that not only contribute to risk reduction (also increasing resilience, together with an improved public health contribution), but also increase the search for sustainability in a broader perspective: minimalist design in buildings, avoiding carpets and rugs, flexible entrance areas, balconies, landscapes and the views from windows, increasing open access to sunlight, natural ventilation, new HVAC systems in non-residential buildings (linear flow extractions, increased humidity control, recovery) with potential mixed modes and a search for near-zero energy buildings. On an urban scale: increased green areas and nature-based solutions, local food production, renewable energy supply, local closed water cycle and the search for sustainable urban areas and buildings;
- Disruptive changes: besides the factorial measures, a disruptive option expands the level and the typologies of measures (not included in Figure 2). This will imply a change in lifestyle and the built environment in order to integrate a holistic approach with a structural reduction in resource consumptions and emissions (e.g., carbon neutral buildings), based on environmental sustainability, social inclusivity and a circular economy, of which sustainable urban areas and buildings are just one component.
6. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Jones, D.S. History in a Crisis—Lessons for Covid-19. N. Engl. J. Med. 2020, 382, 1681–1683. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization (WHO). Q&As on COVID-19 and Related Health Topics. Available online: https://www.who.int/emergencies/diseases/novel-coronavirus-2019/question-and-answers-hub (accessed on 26 May 2020).
- Wilder-Smith, A.; Chiew, C.J.; Lee, V.J. Can we contain the COVID-19 outbreak with the same measures as for SARS? Lancet Infect. Dis. 2020, 20, e102–e107. [Google Scholar] [CrossRef]
- World Health Organization (WHO). WHO Coronavirus Disease (COVID-19) Dashboard. Available online: https://covid19.who.int/ (accessed on 20 July 2020).
- Ozili, P.K.; Arun, T. Spillover of COVID-19: Impact on the Global Economy. 2020. Available online: https://mpra.ub.uni-muenchen.de/99850/1/MPRA_paper_99850.pdf (accessed on 13 July 2020).
- Nicola, M.; Alsafi, Z.; Sohrabi, C.; Kerwan, A.; Al-Jabir, A.; Iosifidis, C.; Agha, M.; Agha, R. The socio-economic implications of the coronavirus pandemic (COVID-19): A review. Int. J. Surg. 2020, 78, 185–193. [Google Scholar] [CrossRef] [PubMed]
- Brooks, S.K.; Webster, R.K.; Smith, L.E.; Woodland, L.; Wessely, S.; Greenberg, N.; Rubin, G.J. The psychological impact of quarantine and how to reduce it: Rapid review of the evidence. Lancet 2020, 395, 912–920. [Google Scholar] [CrossRef]
- Paital, B. Nurture to nature via COVID-19, a self-regenerating environmental strategy of environment in global context. Sci. Total Environ. 2020, 729, 139088. [Google Scholar] [CrossRef]
- Klemeš, J.J.; Fan, Y.; Van Fan, Y.; Tan, R.R.; Jiang, P. Minimising the present and future plastic waste, energy and environmental footprints related to COVID-19. Renew. Sustain. Energy Rev. 2020, 127, 109883. [Google Scholar] [CrossRef]
- Helm, D. The Environmental Impacts of the Coronavirus. Environ. Resour. Econ. 2020, 76, 21–38. [Google Scholar] [CrossRef]
- Lin, W. Evental Infrastructure: Momentous Geographies of Technoscience Production. 2020. Available online: https://www.tandfonline.com/doi/full/10.1080/24694452.2020.1724766 (accessed on 13 July 2020).
- Jacobsen, K.H. Will COVID-19 generate global preparedness? Lancet 2020, 395, 1013–1014. [Google Scholar] [CrossRef]
- United Nations, Department of Economic and Social Affairs, Population Division (2019). World Urbanization Prospects. The 2018 Revision (ST/ESA/SER.A/420).; United Nations, Department of Economic and Social Affairs, Population Division (2019): New York, NY, USA, 2019. [Google Scholar]
- Reyes, R.; Ahn, R.; Thurber, K.; Burke, T.F. Urbanization and Infectious Diseases: General Principles, Historical Perspectives, and Contemporary Challenges. In Challenges in Infectious Diseases. Emerging Infectious Diseases of the 21st Century; Fong, I., Ed.; Springer: Berlin/Heidelberg, Germany, 2013; pp. 123–146. ISBN 978-1-4614-4496-1. [Google Scholar]
- Honigsbaum, M. The Pandemic Century: One Hundred Years of Panic, Hysteria and Hubris; W. W. Norton & Company: New York, NY, USA, 2020. [Google Scholar]
- Web of Science (WoS). Available online: https://login.webofknowledge.com/ (accessed on 5 June 2020).
- ScienceDirect (SD). Available online: https://www.sciencedirect.com/ (accessed on 5 June 2020).
- Dietz, L.; Horve, P.F.; Coil, D.A.; Fretz, M.; Eisen, J.A.; Van Den Wymelenberg, K. 2019 Novel Coronavirus (COVID-19) Pandemic: Built Environment Considerations To Reduce Transmission. MSystems 2020, 5, e00245-20. [Google Scholar] [CrossRef]
- Eykelbosh, A. COVID-19 Precautions for Multi—Unit Residential Buildings. 2020. Available online: https://ncceh.ca/sites/default/files/COVID-19%20Precautions%20for%20Multiunit%20Residential%20Buildings%20-%20March%2031%202020.pdf (accessed on 13 July 2020).
- Cirrincione, L.; Plescia, F.; Ledda, C.; Rapisarda, V.; Martorana, D.; Moldovan, R.; Theodoridou, K.; Cannizzaro, E. COVID-19 Pandemic: Prevention and Protection Measures to be Adopted at the Workplace. Sustainability 2020, 12, 3603. [Google Scholar] [CrossRef]
- Leal Filho, W.; Brandli, L.L.; Lange Salvia, A.; Rayman-Bacchus, L.; Platje, J. COVID-19 and the UN Sustainable Development Goals: Threat to Solidarity or an Opportunity? Sustainability 2020, 12, 5343. [Google Scholar] [CrossRef]
- Frank, L.D.; Iroz-Elardo, N.; MacLeod, K.E.; Hong, A. Pathways from built environment to health: A conceptual framework linking behavior and exposure-based impacts. J. Transp. Health 2019, 12, 319–335. [Google Scholar] [CrossRef]
- Jordan, D.P. Transforming Paris: The Life and Labors of Baron Haussman. University of Chicago Press: Chicago, IL, USA, 1995. [Google Scholar]
- Kirkland, S. Paris Reborn: Napoléon III, Baron Haussmann, and the Quest to Build a Modern City. St. Martin’s Press: New York, NY, USA, 2014. [Google Scholar]
- Cazzolla Gatti, R. Coronavirus outbreak is a symptom of Gaia’s sickness. Ecol. Modell. 2020, 426, 109075. [Google Scholar] [CrossRef] [PubMed]
- Sofo, A.; Sofo, A. Converting Home Spaces Into Food Gardens At the Time of Covid-19 Quarantine: All the Benefits of Plants in This Difficult and Unprecedented Period. 2020. Available online: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7171439/ (accessed on 13 July 2020).
- Cohen, M.J. Does the COVID-19 outbreak mark the onset of a sustainable consumption transition? Sustain. Sci. Pract. Policy 2020, 16, 1–3. [Google Scholar] [CrossRef]
- Acuto, M. COVID-19: Lessons for an Urban(izing) World. One Earth 2020, 2, 317–319. [Google Scholar] [CrossRef]
- Belfiglio, V.J. Control of epidemics in the Roman army: 27 B.C.–A.D. 476. Int. J. Community Med. Public Health 2017, 4, 1387. [Google Scholar] [CrossRef][Green Version]
- Bruun, C. The Water Supply of Ancient Rome: A Study of Roman Imperial Administration. Societas scientiarum Fennica: Helsinki, Finland, 1991. [Google Scholar]
- Follet, K. World Without End: A Novel (Kingsbridge); Penguin Books: London, UK, 2010. [Google Scholar]
- Cohn, S.K. Epidemiology of the Black Death and Successive Waves of Plague. Med. Hist. 2008, 52, 74–100. [Google Scholar] [CrossRef]
- Bramanti, B.; Stenseth, N.C.; Walløe, L.; Xu, L. Plague: A Disease Which Changed the Path of Human Civilization. 2016. Available online: https://www.researchgate.net/publication/308959724_Plague_A_Disease_Which_Changed_the_Path_of_Human_Civilization (accessed on 13 July 2020).
- Sloan, A.W. Medical and social aspects of the great plague of London in 1665. S. Afr. Med. J. 1973, 47, 270–276. [Google Scholar]
- Lilley, K.D. Urban planning after the Black Death: Townscape transformation in later medieval England (1350–1530). Urban History 2015, 42, 22–42. [Google Scholar] [CrossRef]
- Vereycken, K. Leonardo da Vinci Imagines The First Modern City. Exec. Intell. Rev. 2010, 37, 53–55. [Google Scholar]
- Glass, R.I.; Black, R.E. The epidemiology of cholera. In Cholera; Braua, D., Greenough, W.B., Eds.; Springer: Boston, MA, USA; ISBN 9781475796889.
- Lippi, D.; Gotuzzo, E.; Caini, S. Cholera. Microbiol. Spectr. 2016, 4. [Google Scholar] [CrossRef]
- Tulodziecki, D. A case study in explanatory power: John Snow’s conclusions about the pathology and transmission of cholera. Stud. Hist. Philos. Sci. Part C Stud. Hist. Philos. Biol. Biomed. Sci. 2011, 42, 306–316. [Google Scholar] [CrossRef] [PubMed]
- Szczygiel, B.; Hewitt, R. Nineteenth-Century Medical Landscapes: John H. Rauch, Frederick Law Olmsted, and the Search for Salubrity. Bull. Hist. Med. 2000, 74, 708–734. [Google Scholar] [CrossRef] [PubMed]
- Ball, L. Cholera and the Pump on Broad Street: The Life and Legacy of John Snow. Hist. Teacher 2009, 43, 105–119. [Google Scholar]
- Gandy, M. The Paris Sewers and the Rationalization of Urban Space. Trans. Inst. Br. Geogr. 1999, 24, 23–44. [Google Scholar] [CrossRef]
- Campbell, M. What tuberculosis did for modernism: The influence of a curative environment on modernist design and architecture. Med. Hist. 2005, 49, 463–488. [Google Scholar] [CrossRef]
- Abdullah Ali, F. The Influence of Le Corbusier On the emergence of the Aesthetic Values in the Modern Architecture of Cyprus. J. Contemp. Urban Aff. 2018, 2, 1–12. [Google Scholar] [CrossRef]
- Martini, M.; Gazzaniga, V.; Behzadifar, M.; Bragazzi, N.L.; Barberis, I. The history of tuberculosis: The social role of sanatoria for the treatment of tuberculosis in Italy between the end of the 19 th century and the middle of the 20 th. J. Prev. Med. Hyg. 2018, 59, E323–E327. [Google Scholar] [CrossRef]
- Adams, A.; Schwartzman, K.; Theodore, D. Collapse and expand: Architecture and tuberculosis therapy in Montreal, 1909, 1933, 1954. Technol. Cult. 2008, 49, 908–942. [Google Scholar] [CrossRef]
- Mann, T. Der Zauberberg; Fischer, S.: Berlin, Germany, 1924. [Google Scholar]
- Kamradt-Scott, A. Changing perceptions of pandemic influenza and public health responses. Am. J. Public Health 2012, 102, 90–98. [Google Scholar] [CrossRef]
- Rosner, D. Lessons Learned from the 1918–1919 Influenza Pandemic in Minneapolis and St. Paul, Minnesota. Public Health Rep. 2007, 122, 803–810. [Google Scholar] [CrossRef]
- Baldwin, A.N. Sars and the built environment in Hong Kong. Proc. Inst. Civ. Eng. Munic. Eng. 2006, 159, 37–42. [Google Scholar] [CrossRef]
- Oxley, D. ‘The seat of death and terror’: Urbanization, stunting, and smallpox. Econ. Hist. Rev. 2003, 56, 623–656. [Google Scholar] [CrossRef]
- Connolly, C.; Keil, R.; Ali, S.H. Extended urbanisation and the spatialities of infectious disease: Demographic change, infrastructure and governance. 2020. Available online: https://journals.sagepub.com/doi/full/10.1177/0042098020910873 (accessed on 13 July 2020).
- Barberis, I.; Bragazzi, N.L.; Galluzzo, L.; Martini, M. The history of tuberculosis: From the first historical records to the isolation of Koch’s bacillus. J. Prev. Med. Hyg. 2017, 58, E9–E12. [Google Scholar] [CrossRef]
- The New York Times Style Magazine. In Search of Lost Time in Europe’s Sanatoriums. Available online: https://www.nytimes.com/2018/02/18/t-magazine/sanatorium-europe-history.html (accessed on 14 July 2020).
- Dezeen Du Besset-Lyon. Transforms Former Sanatorium into Clermont-Ferrand School of Architecture. Available online: https://www.dezeen.com/2015/11/11/clermont-ferrand-school-of-architecture-du-besset-lyon-architectes-urbanistes-former-sanatorium-france/ (accessed on 14 July 2020).
- Neiderud, C.J. How urbanization affects the epidemiology of emerging infectious diseases. Infect. Ecol. Epidemiol. 2015, 5, 27060. [Google Scholar] [CrossRef]
- Brizuela, N.G.; Garcia-Chan, N.; Pulido, H.G.; Chowell, G. Understanding the role of urban design in disease spreading. 2020. Available online: https://www.biorxiv.org/content/10.1101/766667v2.full (accessed on 13 July 2020).
- European Comission (EC). COVID-19: Guidelines on the Progressive Restoration of Transport Services and Connectivity. European Commission: Brussels, Belgium, 2020. [Google Scholar]
- World Health Organization (WHO). Strengthening Preparedness for COVID-19 in Cities and Urban Settings: Interim Guidance forLocal Authorities; World Health Organization: Geneva, Switzerland, 2020; Licence: CC BY-NC-SA 3.0 IGO. [Google Scholar]
- Weston Williamson + Partners Weston Williamson + Partners Envisions Social-Distancing Office. Available online: https://www.dezeen.com/2020/05/14/weston-williamson-social-distancing-office/ (accessed on 29 May 2020).
- Semple, S.; Cherrie, J.W. Covid-19: Protecting Worker Health. Ann. Work Expo. Health 2020, 64, 461–464. [Google Scholar] [CrossRef]
- Larsson, N. Pandemics and the Built Environment. 2020. Available online: https://www.researchgate.net/publication/342376251_Pandemics_and_the_Built_Environment_22June20 (accessed on 13 July 2020).
- van den Bosch, M.; Ode Sang, Å. Urban natural environments as nature-based solutions for improved public health—A systematic review of reviews. Environ. Res. 2017, 158, 373–384. [Google Scholar] [CrossRef]
- Kurnitski, J.; Boerstra, A.; Franchimon, F.; Mazzarella, L.; Hogeling, J.; Hovorka, F.; Seppänen, O. REHVA COVID-19 guidance document. 2020. Available online: https://www.rehva.eu/fileadmin/user_upload/REHVA_COVID-19_guidance_document_ver2_20200403_1.pdf (accessed on 13 July 2020).
- Marr, L.C.; Tang, J.W.; Van Mullekom, J.; Lakdawala, S.S. Mechanistic insights into the effect of humidity on airborne influenza virus survival, transmission and incidence. J. R. Soc. Interface 2019, 16, 20180298. [Google Scholar] [CrossRef]
- Moriyama, M.; Hugentobler, W.J.; Iwasaki, A. Seasonality of Respiratory Viral Infections. Annu. Rev. Virol. 2020, 7, 1–19. [Google Scholar] [CrossRef]
- van Doremalen, N.; Bushmaker, T.; Morris, D.H.; Holbrook, M.G.; Gamble, A.; Williamson, B.N.; Tamin, A.; Harcourt, J.L.; Thornburg, N.J.; Gerber, S.I.; et al. Aerosol and Surface Stability of SARS-CoV-2 as Compared with SARS-CoV-1. N. Engl. J. Med. 2020. [Google Scholar] [CrossRef]
- Kampf, G.; Todt, D.; Pfaender, S.; Steinmann, E. Persistence of coronaviruses on inanimate surfaces and their inactivation with biocidal agents. J. Hosp. Infect. 2020, 104, 246–251. [Google Scholar] [CrossRef] [PubMed]
- Schuit, M.; Gardner, S.; Wood, S.; Bower, K.; Williams, G.; Freeburger, D.; Dabisch, P. The Influence of Simulated Sunlight on the Inactivation of Influenza Virus in Aerosols. J. Infect. Dis. 2019, 221, 372–378. [Google Scholar] [CrossRef] [PubMed]
- Nghiem, L.D.; Morgan, B.; Donner, E.; Short, M.D. The COVID-19 pandemic: Considerations for the waste and wastewater services sector. Case Stud. Chem. Environ. Eng. 2020, 1, 100006. [Google Scholar] [CrossRef]
- World Health Organization (WHO). Q&A on Coronaviruses (COVID-19). Available online: https://www.who.int/emergencies/diseases/novel-coronavirus-2019/question-and-answers-hub/q-a-detail/q-a-coronaviruses (accessed on 11 May 2020).
- Ko, W.H.; Schiavon, S.; Zhang, H.; Graham, L.T.; Brager, G.; Mauss, I.; Lin, Y.-W. The impact of a view from a window on thermal comfort, emotion, and cognitive performance. Build. Environ. 2020, 175, 106779. [Google Scholar] [CrossRef]
- Preiss, S.; Kramer, A. Foot-operated door opener to eliminate the door handle as a source of contamination. GMS Krankenhhyg. Interdiszip. 2011, 6, 10. [Google Scholar] [CrossRef]
- Chen, C.; Zhang, X.-J.; Wang, Y.; Zhu, L.-X.; Liu, J. Waste water disinfection during SARS epidemic for microbiological and toxicological control. Biomed. Environ. Sci. 2006, 19, 173–178. [Google Scholar]
- Tronville, P.; Rivers, R.D. International standards: Filters for buildings and gas turbines. Filtr. Sep. 2005, 42, 39–43. [Google Scholar] [CrossRef]
- Becher, R.; Øvrevik, J.; Schwarze, P.E.; Nilsen, S.; Hongslo, J.K.; Bakke, J.V. Do carpets impair indoor air quality and cause adverse health outcomes: A review. Int. J. Environ. Res. Public Health 2018, 15, 184. [Google Scholar] [CrossRef]
- Canadian Psychological Association. Traumatic Stress Section Executive Managing COVID-19 Anxiety—Resources. Available online: https://cpa.ca/resources-for-managing-covid-19-anxiety-cpa-traumatic-stress-section/ (accessed on 13 July 2020).
- Martineau, A.R.; Jolliffe, D.A.; Hooper, R.L.; Greenberg, L.; Aloia, J.F.; Bergman, P.; Dubnov-Raz, G.; Esposito, S.; Ganmaa, D.; Ginde, A.A.; et al. Vitamin D supplementation to prevent acute respiratory tract infections: Systematic review and meta-analysis of individual participant data. 2017. Available online: https://www.bmj.com/content/356/bmj.i6583 (accessed on 13 July 2020).
- Abraham, A.; Sommerhalder, K.; Abel, T. Landscape and well-being: A scoping study on the health-promoting impact of outdoor environments. Int. J. Public Health 2009, 55, 59–69. [Google Scholar] [CrossRef]
- Pinter-Wollman, N.; Jelic, A.; Wells, N.M. The impact of the built environment on health behaviours and disease transmission in social systems. Philos. Trans. R. Soc. B Biol. Sci. 2018, 373, 20170245. [Google Scholar] [CrossRef]
- Saez, M.; Tobias, A.; Varga, D.; Barceló, M.A. Effectiveness of the measures to flatten the epidemic curve of COVID-19. The case of Spain. Sci. Total Environ. 2020, 727, 138761. [Google Scholar] [CrossRef] [PubMed]
- Yeom, S.; Kim, H.; Hong, T.; Park, H.S.; Lee, D.-E. An integrated psychological score for occupants based on their perception and emotional response according to the windows’ outdoor view size. Build. Environ. 2020, 180, 107019. [Google Scholar] [CrossRef]
- Writing Urban Places COST Socially Distanced—Windows Looking (and Listening) to Nature Where I Resided. Available online: https://writingurbanplaces.eu/wup-news/socially-distanced-windows-looking-and-listening-to-nature-where-i-resided/ (accessed on 14 July 2020).
- Alaloul, W.S.; Liew, M.S.; Zawawi, N.A.W.A.; Kennedy, I.B. Industrial Revolution 4.0 in the construction industry: Challenges and opportunities for stakeholders. Ain Shams Eng. J. 2020, 11, 225–230. [Google Scholar] [CrossRef]
- Brattig, N.W.; Tanner, M.; Bergquist, R.; Utzinger, J. Impact of environmental changes on infectious diseases: Key findings from an international conference in Trieste, Italy in May 2017. 2017. Available online: https://www.sciencedirect.com/science/article/abs/pii/S0001706X19312252 (accessed on 13 July 2020).
- Mears, M.; Brindley, P.; Jorgensen, A.; Ersoy, E.; Maheswaran, R. Greenspace spatial characteristics and human health in an urban environment: An epidemiological study using landscape metrics in Sheffield, UK. Ecol. Indic. 2019, 106, 105464. [Google Scholar] [CrossRef]
- Allen, J.G.; Macomber, J.D. Healthy Buildings: How Indoor Spaces Drive Performance and Productivity; Harvard University Press: Cambridge, MA, USA, 2020; ISBN 9780674237971. [Google Scholar]
- Keenan, J.M. COVID, resilience, and the built environment. Environ. Syst. Decis. 2020, 40, 216–221. [Google Scholar] [CrossRef] [PubMed]
- Alirol, E.; Getaz, L.; Stoll, B.; Chappuis, F.; Loutan, L. Urbanisation and infectious diseases in a globalised world. Lancet. Infect. Dis. 2011, 11, 131–141. [Google Scholar] [CrossRef]
- Braithwaite, R.; Warren, R. The African American Petri Dish. 2020. Available online: https://preprint.press.jhu.edu/jhcpu/sites/default/files/02_warren.pdf1762847 (accessed on 13 July 2020).
- Schulz, A.J.; Mehdipanah, R.; Chatters, L.M.; Reyes, A.G.; Neblett, E.W.; Israel, B.A. Moving Health Education and Behavior Upstream: Lessons From COVID-19 for Addressing Structural Drivers of Health Inequities. Health Educ. Behav. 2020, 47, 519–524. [Google Scholar] [CrossRef]
- Sherr, L.; Cluver, L.; Desmond, C.; Toska, E.; Aber, L.; Dhaliwal, M.; Webb, D.; Dugbazah, J. A new vehicle to accelerate the UN Sustainable Development Goals. Lancet Glob. Health 2020, 8, e637–e638. [Google Scholar] [CrossRef]
- Wijburg, G. The de-financialization of housing: Towards a research agenda. 2019. Available online: https://www.tandfonline.com/doi/full/10.1080/02673037.2020.1762847 (accessed on 13 July 2020).
- Djalante, R.; Shaw, R.; DeWit, A. Building resilience against biological hazards and pandemics: COVID-19 and its implications for the Sendai Framework. Prog. Disaster Sci. 2020, 6, 100080. [Google Scholar] [CrossRef]
- Kanda, W.; Kivimaa, P. What opportunities could the COVID-19 outbreak offer for sustainability transitions research on electricity and mobility? Energy Res. Soc. Sci. 2020, 68, 101666. [Google Scholar] [CrossRef]
- Gills, B. Deep Restoration: From The Great Implosion to The Great Awakening. Globalizations 2020, 17, 577–579. [Google Scholar] [CrossRef]
- Forester, J. Kindness, Planners’ Response to Vulnerability, and an Ethics of Care in the Time of Covid-19. Plan. Theory Pract. 2020, 21, 185–188. [Google Scholar] [CrossRef]
- Hepburn, C.; O’Callaghan, B.; Stern, N.; Stiglitz, J.; Zenghelis, D. Will COVID-19 fiscal recovery packages accelerate or retard progress on climate change? Oxford Rev. Econ. Policy 2020, 36, 1–48. [Google Scholar] [CrossRef]
- Keim, M.E. Building Human Resilience: The Role of Public Health Preparedness and Response As an Adaptation to Climate Change. Am. J. Prev. Med. 2008, 35, 508–516. [Google Scholar] [CrossRef]
- Queiroz, M.M.; Ivanov, D.; Dolgui, A.; Fosso Wamba, S. Impacts of epidemic outbreaks on supply chains: Mapping a research agenda amid the COVID-19 pandemic through a structured literature review. 2020. Available online: https://link.springer.com/article/10.1007/s10479-020-03685-7 (accessed on 13 July 2020).
- Lucchese, M.; Pianta, M. The Coming Coronavirus Crisis: What Can We Learn? Intereconomics 2020, 55, 98–104. [Google Scholar] [CrossRef]
| Epidemiological Disease | Dimension (% of World or Regions) and Time of Duration | Behaviour | Built Environment (Infrastructure, Buildings, Urban Areas, Green Spaces) | Ref. |
|---|---|---|---|---|
| Infectious diseases in the Roman Empire (second century) | - | Isolation tents near hospitals. | - | [29] |
| - | Infrastructure: Aqueducts, public baths, division of water and sanitation systems. | [30] | ||
| Black Death (fourteenth century) | Three pandemics responsible for the death of 50–75 million people worldwide [14]. | Quarantine and restrictions on movements. Closure of public baths and advice to avoid contact with animals. | - | [33] |
| Closure of ports. | [32] | |||
| - | Urban planning begins to create more space between buildings—Elimination of dirty and cramped neighbourhoods. Larger public spaces with more organised layouts. | [35] | ||
| Cholera (nineteenth century) | Six outbreaks between nineteenth and twentieth centuries, responsible for millions of deaths (50% fatality rate) [37]. | Quarantine for individuals and cargo arriving at ports. | - | [37] |
| - | Green areas: Parks in the middle of cities. | [40] | ||
| - | Urban design: Long avenues and open spaces (e.g., Paris). | [23,24] | ||
| - | Sanitation: Creation of infrastructure with improved sewage systems. | |||
| Tuberculosis (nineteenth century) | The disease survived for over 70,000 years, infecting nearly 2 billion people worldwide [53]. | Sanatoriums. | [45] | |
| Building design: Terraces, balconies and flat roofs. Modern urban design. | [43,46] | |||
| Social isolation. | Building design: revolving summer houses. Furniture: reclining chairs. | [43] | ||
| Spanish Flu (twentieth century, 1918–1919) | Was responsible for the deaths of 50 million people between 1918–1919 [14]. | Social distancing —closure of public spaces (churches, theatres, schools). | - | [14] |
| Use of gauze masks. | - | [49] | ||
| SARS-CoV-1 (twenty-first century, 2003–2004) | 8000 cases and more than 800 deaths reported in 26 different countries after 8 months [3]. | Quarantine and social distancing. | - | [3] |
| - | Local building design: Improved ventilation and drainage systems in specific areas of Asia (e.g., Hong Kong). | [50] |
| Built Environment System | Measure | COVID-19 Benefits | Resilience (to Other Vulnerabilities) | Sustainability |
|---|---|---|---|---|
| Street paths | Unidirectional pedestrian paths [59]. | Avoids people crossing with one another. | Useful for preventing the transmission of other infectious diseases between people. | The contribution is highly dependent on the adopted solution. |
| Wider pedestrian paths: reducing the width of roads (temporarily or not) and increasing pedestrian areas and cycle tracks [59]. | Allows for safe distances between people. | Increases mobility and reduces carbon emissions. | ||
| Public equipment | Safety (distance) markers on benches. | Allows for safe distances between people. | Useful for preventing the transmission of other infectious diseases. | Less space available for services. |
| Distribution of public disinfectant containers or washing infrastructures in strategic locations [59]. | Public hygiene. | Useful for preventing the transmission of other infectious diseases. | Greater use of cleaning (disinfection) products. | |
| More local services (energy, food). | Decentralisation of services and greater local supply. | Ensures basic services available for any extreme situation. | Reduces the need for people to travel (benefits in terms of reduced energy consumption and associated emissions). | |
| New pop-up service points: bicycle repairs and free water for cyclists and walkers [60]. | Motivates and supports active mobility. | Increases mobility and reduces carbon emissions. | ||
| Roller handrail disinfection system [60]. | Disinfection of a common contact surface | Ecological and economic balance. | ||
| Public transport facilities | Protective barriers for public transport drivers (buses, trams) [58,61]. | Physical protection to avoid social contact. | Useful for other vulnerabilities, such as robberies. | Potentially less space available. |
| Automatic doors [58]. | Avoids contact with common surfaces. | Useful for other public health vulnerabilities. | Must ensure appropriate use for all. | |
| Differentiation between entrance and exit doors [58]. | Avoids people crossing with one another. | Useful for other public health vulnerabilities. | Potentially less space available. | |
| Safety distance markers between seats. | Social distancing. | Useful for other public health vulnerabilities. | Potentially less space available. Reduces energy consumption and cost efficiency. | |
| Safety distance markers at stops and in waiting areas [62]. | Social distancing. | Useful for other public health vulnerabilities. | Potentially less space available. | |
| Public disinfectant containers [58]. | Public hygiene. | Useful for other public health vulnerabilities. | Ecological and economic balance. | |
| Green areas and nature-based solutions | Natural environments in urban areas [63]. | Could improve public health and may also mitigate the effects of climate change [63]. | Biodiversity and climate change. | |
| Information technology (smart cities) | Integrates risk of new infections in IoT (Internet of things) approaches. | Risk identification (apps) and potential reduction in transmission through greater information. | Increases resilience, especially if the information allows governance with users. | Reduces the need for resources. |
| Main Group | Group Elements | Measure | COVID-19 Benefits | Resilience (to COVID-19 and Other Vulnerabilities) | Sustainability | |
|---|---|---|---|---|---|---|
| Structure | Foundations | - | - | Reduces risk: seismic, wind and landslides. Flexibility. | ||
| Basement construction | - | - | Reduces risk: seismic, wind and landslides. Flexibility. | |||
| Shell | Super structure | - | - | Reduces risk: seismic, wind and landslides. Flexibility. | ||
| Exterior Enclosure | Sunlight (achieved through orientation, glazed openings and open blinds). | Although there is no evidence of the effect of sunlight on SARS-CoV-2 [71], some viruses, such as influenza, are sensitive to sunlight [69]. | Good bioclimatic and energy performance. | |||
| Providing a window with a view. | Windows are the main point of contact with the exterior of the building. Pleasant views (e.g., the surrounding nature) can influence psychological well-being (increased concentration, reduced stress, comfort, emotions) [72]. | |||||
| Roofing | Potential openings for light or roof access. | Promotes natural lighting—potential outside uses. | Guarantees physical and thermal protection. | |||
| Interiors | Interior construction | Hands-free door opening (e.g., using elbow or foot) [73]. | Avoids using your hands to open the doors, reducing the possibility of spreading SARS-CoV-1 and other viruses. | Access to all. | ||
| Interior finishes | Easy to clean (homogeneous without pores). | Easy to eliminate SARS-CoV-2 and other pathogens, avoiding other contaminations. | Fewer cleaning products and lower toxicity. | |||
| Selection of materials that reduce virus’s residence time* (e.g., copper and others) [67]. | Positive for reducing residence time (or avoiding accommodation) of SARS-CoV-2 and other pathogens, avoiding other contaminations. | Important that LCA (Life cycle Assessment) and LCC (Life Cycle Cost) have a good balance for each functional unit, for example, recycled materials. | ||||
| Services | Conveying | Lifts: safe distance markers (2 m), depending on the lift capacity [19]. | It allows social distancing, preventing the spread of SARS-CoV-2 and other viruses. | More energy spent per person (reducing lift capacity). | ||
| Stairs allow passage to different floors (one way). Distance and direction markers on stairs. | Unidirectional circulation could reduce the risk of contact. Stairs ensure social distancing and direction. | Reduces risk of infection, but could create problems in emergencies, such as fires. Lowers the capacity of service use. | ||||
| Water system | Water system. | Ensures appropriate hygiene conditions. | Balance between water supply requirements and the reduction of potable water consumption. | |||
| Routine wastewater testing. | This can be used to detect the presence of SARS-CoV-2, but also other viruses, indicating the risk of contagion [70]. | Reduces risks. | ||||
| Wastewater disinfection: residual free chlorine (>0.5 mg/L), residual chlorine dioxide (>2.19 mg/L) or UV radiation [74]. | Chen et al. (2006) concluded that disinfection by UV radiation and chlorine dioxide were the most efficient means of fighting SARS-CoV-1 [74]. It may be effective against other viruses. | Reduces risks. | ||||
| HVAC | Mixed modes, with natural ventilation. | Constant air renewal to reduce the possibility of the virus remaining in the form of aerosolised particles inside the building [64]. Other psychological benefits. | Besides reducing the risk of the virus and other microorganisms, allows for the elimination of certain polluting particles. Potential energy saving measures. | |||
| HEPA (high-efficiency particulate air) filters [75]. | Capable of removing at least 99.97% of particles with sizes starting from 0.3 μm [75]. | |||||
| Heat recovery unit [64]. | Ensures 100% separation between incoming and outgoing air [64]. | Ensures good air quality. | ||||
| 40–60% relative humidity [66]. | Reduces virus residence time in aerosolised particles [65]. | |||||
| Risk protection systems | Enlarges the risk protection system to include infectious diseases (thermal sensors). | Detects the presence of the virus. | Enlarges the risk detection system and actions to other dimensions. | Strong contribution to risk identification. | ||
| Energy systems | Reliable power supply ensures that not only core systems for the management of health programmes can function effectively, but also the specific building’s needs. | Ensures appropriate function conditions (air conditioning if necessary). | All activities are highly dependent on access to a reliable energy supply. The creation of a local renewable supply could help to increase the resilience of systems. | Potential opportunities for low carbon consumption (renewable energy) and/or local energy supply system. | ||
| Information systems | Information technology makes it possible to manage situations and users. | Reduces presence, optimises ventilation and other options. | Some devices can simultaneously reduce unnecessary energy and water consumption. Fewer disinfection products needed. | Prevents polluting aerosolised particles from remaining in the air longer, due to dry environments. | ||
| Touch-free technologies (switches and bathroom equipment). | Technologies, such as smartphone controls, motion sensors and voice controls, reduce the need for contact with various common surfaces and reduce the spread of pathogens. | Makes it possible to control other risks. Reduces manual control. | An optimisation solution could enable the user to control the programme by voice, in order to reduce the consumption of resources. | |||
| Waste | Specific (separate) collection for quarantined houses or areas with outbreaks of contagion: Incineration and strict disinfection of collection vehicles [70]. | The virus can remain on plastic and other surfaces for several days. Rubbish bags can be a potential vector of transmission. Special care in areas with high risk of contagion can prevent other infections [70]. | Lower activity reduces the amount of waste in landfills but also reduces recycling. Incineration emits polluting gases. | Depends on the solution and whether it is integrated into a lower consumption of resources and improves recyclability. | ||
| Equipment and furniture | Equipment | Ensures easy cleaning solutions. | Reduces the risk of cross contamination | Fewer disinfection products. | ||
| Select materials that reduce the virus’s residence time (e.g., copper) [67]. | Positive for reducing residence time (or avoiding accommodation) of SARS-CoV-1 and other pathogens, preventing other contaminations. | Important that LCA and LCC have a good balance for each functional unit, for example, recycled materials. | ||||
| Minimalist solutions, fewer places that can offer a pathway to the virus. | Reducing places of contamination could reduce the potential for contamination. | Fewer objects lead to more flexible solutions and prevent objects from falling. | Reduction of materials. If less toxic LCA is reduced and LCC is good, this could be a sustainable positive direction. | |||
| Furniture | Avoid using carpets and rugs [76]. | Helps to reduces the concentration of pathogenic agents inside the building. | Positive, if fewer, impacts in life cycle. | |||
| Building divisions | Entrance | Flexible entrance (to be adapted to a decontamination zone), with washbasins at the entrance (or in bathroom) [62]. | Prevents pathogens from entering the main building divisions (either through potentially contaminated clothing or objects, or by hand). | - | ||
| Room | Extra room for occupants who need to isolate [62] (preferably with private bathroom). | Isolation of potentially contaminated residents. Reduces risk of contagion from SARS-CoV-1 and other infections. | Increases the space per building and the energy consumption (as costs). | |||
| External spaces | Balconies, terraces, flat roofs | Provides at least one outdoor area, with considerable space. | Allows people to take physical exercise, get fresh air and sunlight, while avoiding social contact. Fresh air [77] and vitamin D are beneficial for human health, including respiratory problems [78], even more so in confinement situations. | Thermal bridge care. Can be used for food production and other activities [26]. | ||
| Home gardens for food production | Uses external spaces for home gardens. | Food production with economic, recreational and health benefits [26]. | ||||
| Landscape | Immediate surroundings | Health-promoting landscapes (natural green landscapes, offering conditions of security and connectivity, as well as several amenities, including physical exercise equipment) [79]. | Landscapes influence health and well-being. They have the potential to promote mental health, reduce stress, raise happiness levels and promote social cohesion, as well as offering physiological benefits. | Maintenance of ecosystem services, preparation for adaptation to climate change, guarantee of other functionalities. | ||
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Pinheiro, M.D.; Luís, N.C. COVID-19 Could Leverage a Sustainable Built Environment. Sustainability 2020, 12, 5863. https://doi.org/10.3390/su12145863
Pinheiro MD, Luís NC. COVID-19 Could Leverage a Sustainable Built Environment. Sustainability. 2020; 12(14):5863. https://doi.org/10.3390/su12145863
Chicago/Turabian StylePinheiro, Manuel Duarte, and Nuno Cardoso Luís. 2020. "COVID-19 Could Leverage a Sustainable Built Environment" Sustainability 12, no. 14: 5863. https://doi.org/10.3390/su12145863
APA StylePinheiro, M. D., & Luís, N. C. (2020). COVID-19 Could Leverage a Sustainable Built Environment. Sustainability, 12(14), 5863. https://doi.org/10.3390/su12145863






