COVID-19 Pandemic Response in Japan: What Is behind the Initial Flattening of the Curve?
Abstract
1. Introduction
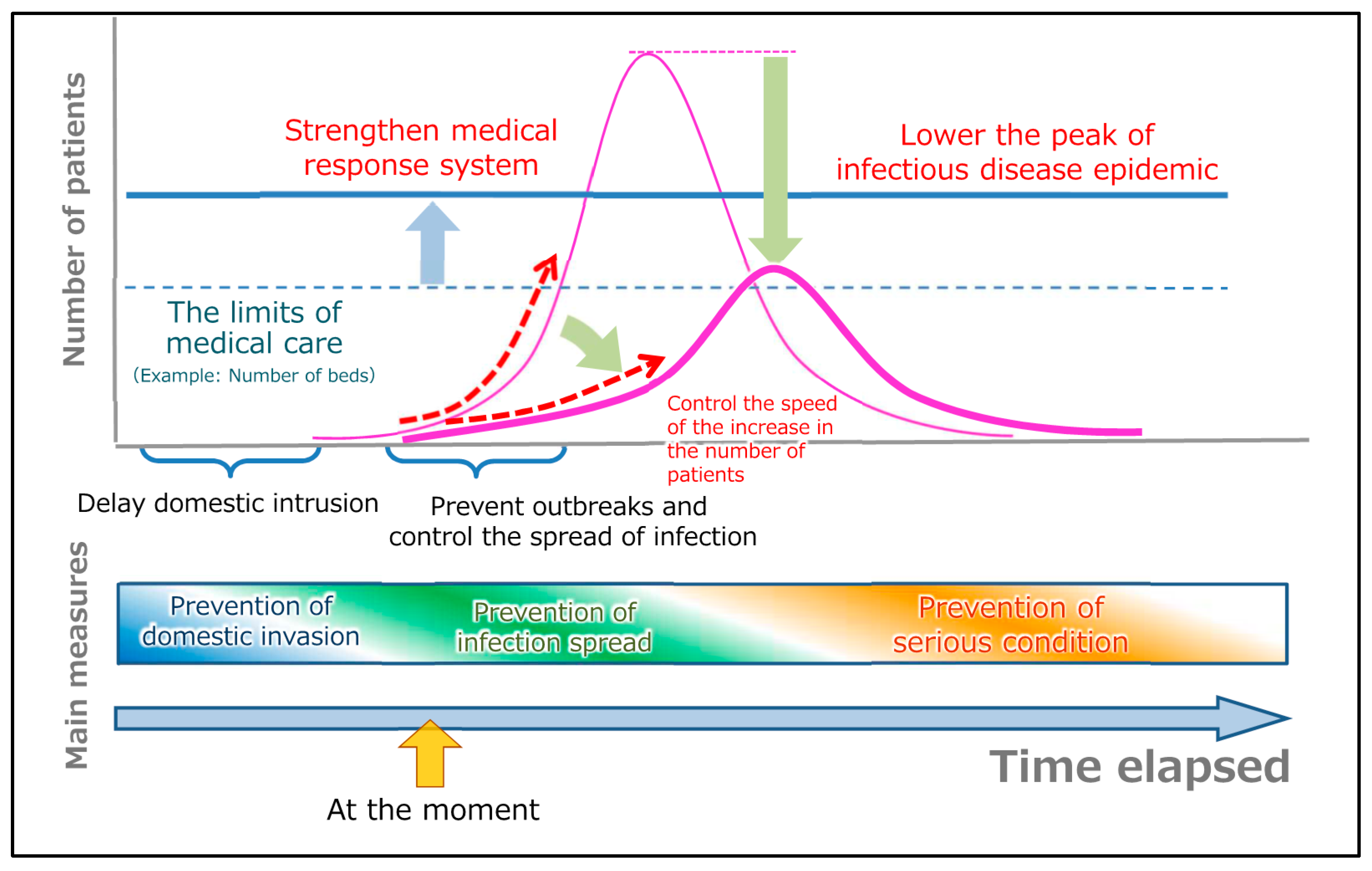
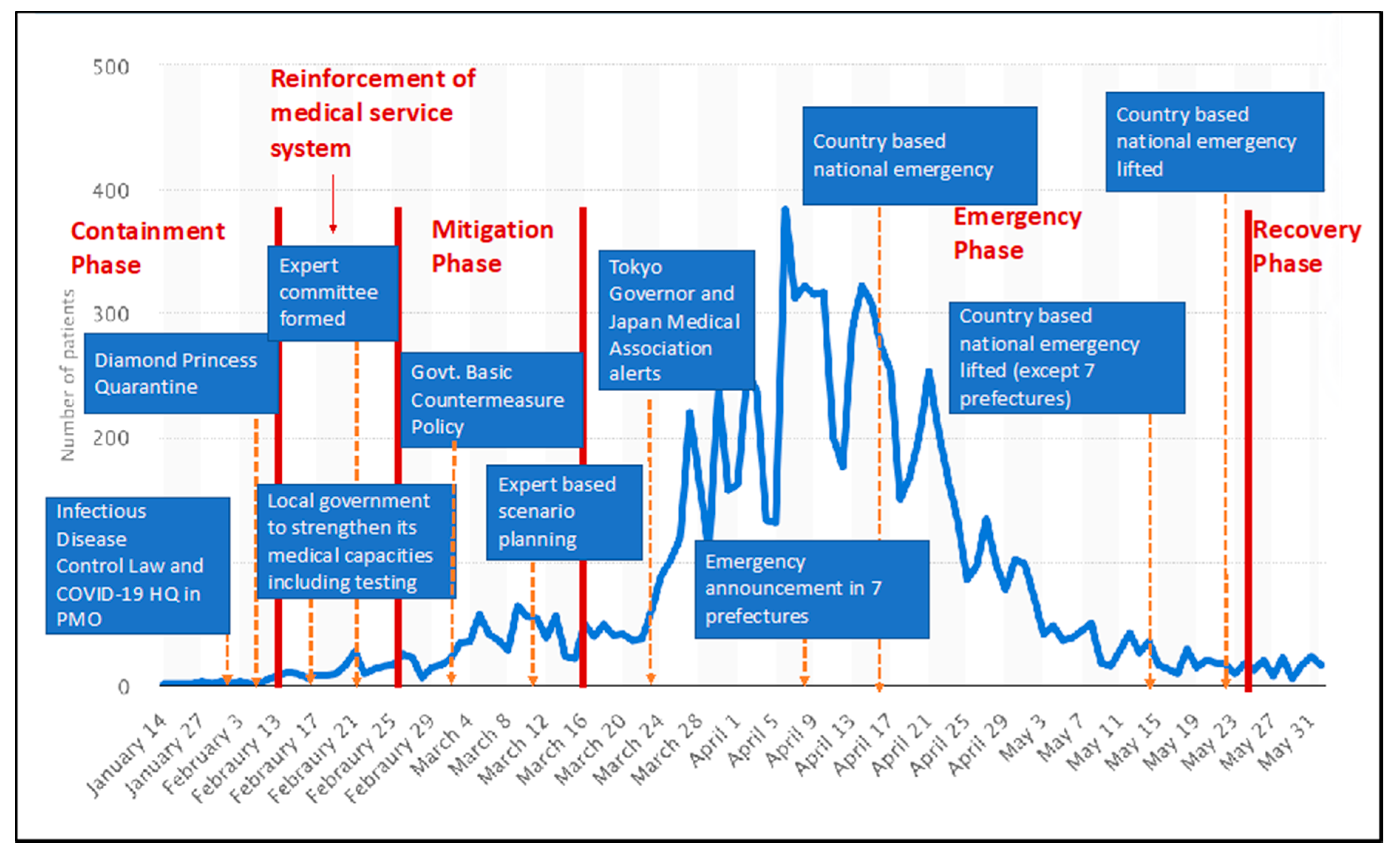
2. History of COVID-19 in Japan and Basic Policies and Measures Applied
3. Emergency Law in Japan and its Implications
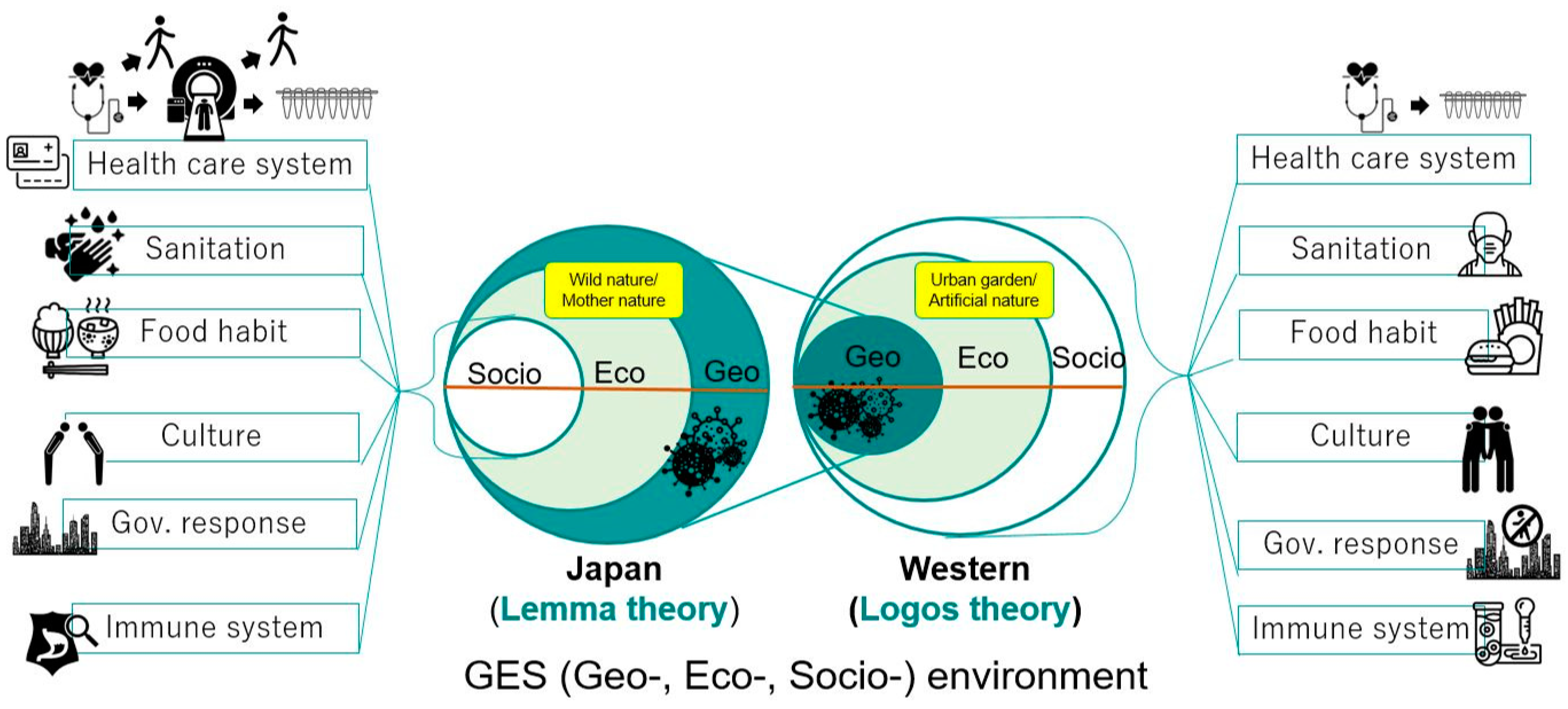
4. Characteristics of Japanese Lifestyles and Their Possible Implications
4.1. Culture
4.2. Healthcare System
- (1)
- Cold symptoms and/or a fever above 37.5 °C, which lasts for 4 days or more,
- (2)
- Elderly or those with preexisting health problems,
- (3)
- Heavy physical fatigue or trouble breathing.
4.3. Sanitation
4.4. Food Habits
4.5. Immune System
5. Discussion
6. Conclusion
- (1)
- Robust integrated health and emergency management policy, the basic healthcare system should be a core pillar of society. During the pandemic response, an integrated emergency response system is required, where decisions are made based on science and expert advice, and adaptive policy responses are ensured. Chan and Shaw (2020) provided several cases of incorporating public health in disaster risk reduction [46] and vice versa through the health emergency disaster risk management framework (WHO 2019) [47,48,49].
- (2)
- A healthy lifestyle is key to promote a healthy immune system. An ecosystem-based lifestyle change is essential, as exemplified above in the case of Japan. Mukherjee et al. (2020) argued for an ecosystem-based business continuity plan to recover from COVID-19.
- (3)
- Use of new and emerging technologies: online classes, meetings, telework, etc. Extensive use of 5G and other information-related developments is essential [3]
- (4)
Author Contributions
Funding
Conflicts of Interest
References
- WHO. COVID 10 Public Health Emergency of International Concern: Global Research and Innovation Forum; WHO: Geneva, Switzerland, 2020; p. 7. [Google Scholar]
- Hua, J.; Shaw, R. Corona Virus (COVID-19) "Infodemic" and Emerging Issues through a Data Lens: The Case of China. Int. J. Environ. Res. Public Health 2020, 17, 2309. [Google Scholar] [CrossRef] [PubMed]
- Shaw, R.; Kim, Y.K.; Hua, J. Governance, technology and citizen behavior in pandemic: Lessons from COVID-19 in East Asia. Prog. Disaster Sci. 2020. [Google Scholar] [CrossRef]
- Nippon.com. Coronavirus Cases by Country. 2020. Available online: https://www.nippon.com/en/japan-data/h00673/coronavirus-cases-by-country.html (accessed on 17 April 2020).
- MHLW. Current Situation and MHLW Response to COVID-19. Ministry of Health, Labor, and Welfare (in Japanese). 2020. Available online: https://www.mhlw.go.jp/stf/newpage_10904.html (accessed on 17 April 2020).
- MHLW. About coronavirus disease 2019. 2020. Available online: https://www.mhlw.go.jp/stf/seisakunitsuite/bunya/newpage_00032.html (accessed on 15 April 2020).
- PMO. Prime Minister Office of Government of Japan. 2020. Available online: http://japan.kantei.go.jp/ongoingtopics/_00013.html (accessed on 15 April 2020).
- Wiki. 2020 Coronavirus Pandemic in Japan. 2020. Available online: https://en.wikipedia.org/wiki/2020_coronavirus_pandemic_in_Japan (accessed on 15 April 2020).
- Rich, M.; Ueno, H. Japan’s Virus Success has Puzzled the World. Is its Luck Running Out? The New York Times. 2020. Available online: https://www.nytimes.com/2020/03/26/world/asia/japan-coronavirus.html (accessed on 7 April 2020).
- Mainichi Shimbun. State of Emergency for Tokyo and Six other Prefectures on April 7 To Ramp up Defenses against the Spread of the New Coronavirus. 2020. Available online: https://mainichi.jp/weekly/articles/20200417/wek/00m/040/002000c (accessed on 7 April 2020).
- Mine, Y. “Immigration Restrictions” and “Isolation” Comparison of Japanese Governments and Japanese Responses against New Coronavirus. Yahoo Japan News. 2020. Available online: https://headlines.yahoo.co.jp/hl?a=20200224-00010003-wordleaf-pol&p=1 (accessed on 7 April 2020).
- New Cases of Coronavirus Disease (COVID-19) Confirmed by day in Japan from January 14 to June 1 2020. Available online: https://www.statista.com/statistics/1105032/japan-new-confirmed-cases-of-coronavirus-by-day/ (accessed on 7 June 2020).
- Miyoshi, K.; Murayama, H. Mobility changes in Tokyo, The Global Data Science Project for COVID-19. 2020. Available online: https://www.covid19analytics.org/post/social-distancing (accessed on 10 May 2020).
- Takeda, T.; Kamagahara, Y.; Lu, X.; Kida, N.; Hara, T.; Ota, T. Study of the difference in the movement of experienced and inexperienced persons in Japanese bowing. In Advances in Intelligent Systems and Computing; Springer: Cham, Switzerland, 2017. [Google Scholar] [CrossRef]
- ThePrint. Social Distancing is the Norm in Japan. That’s why COVID-19 Spread is Slow there. The Print. 2020. Available online: https://theprint.in/health/social-distancing-is-the-norm-in-japan-thats-why-covid-19-spread-is-slow-there/384498/ (accessed on 7 April 2020).
- Imada, T. Cultural Narratives of Individualism and Collectivism: A Content Analysis of Textbook Stories in the United States and Japan. J. Cross-Cult. Psychol. 2012. [Google Scholar] [CrossRef]
- Furuya, S. Reinterpretation of Japanese Collectivism: Based on “Self-Interested Cooperation.” Global studies. Musashino Univ. Acad. Inst. Repositry. 2018. Available online: http://id.nii.ac.jp/1419/00000861/ (accessed on 7 April 2020).
- Ishii, M.; Hamamoto, M.; Tsuruoka, H. JMA perspectives on the universal health insurance system in Japan. Jpn. Med Assoc. J. 2010, 53, 139–143. [Google Scholar]
- Yano, H. Coronavirus: Why Japan tested so Few People. Retrieved 12 March 2020, from NIKKEI Asian Review. 2020. Available online: https://asia.nikkei.com/Spotlight/Coronavirus/Coronavirus-Why-Japan-tested-so-few-people (accessed on 7 April 2020).
- Information for Public. Q & A on Coronavirus Disease 2019 (COVID-19). Ministry of Health, Labor and Welfare. 2020. Available online: https://www.mhlw.go.jp/stf/seisakunitsuite/bunya/kenkou_iryou/dengue_fever_qa_00014.html (accessed on 7 April 2020).
- Ai, T.; Yang, Z.; Hou, H.; Zhan, C.; Chen, C.; Lv, W.; Xia, L. Correlation of Chest CT and RT-PCR Testing in Coronavirus Disease 2019 (COVID-19) in China: A Report of 1014 Cases. Radiology 2020. [Google Scholar] [CrossRef] [PubMed]
- UNICEF. Everything You need to Know about Washing your Hands to Protect against Coronavirus (COVID-19). Retrieved April 7, 2020, from UNICEF website. Available online: https://www.unicef.org/georgia/stories/everything-you-need-know-about-washing-your-hands-protect-against-coronavirus-covid-19 (accessed on 7 April 2020).
- Asia Development Bank. Sanitation and Sustainable Development in Asia. 2016. Available online: https://www.adb.org/sites/default/files/publication/209511/sanitation-sustainable-dev-japan.pdf (accessed on 3 April 2020).
- UNICEF. Handwashing with Soap, Critical in the Fight against Coronavirus, is ’out of reach’ for Billions—UNICEF. 2020. Available online: https://www.unicef.org/eap/press-releases/handwashing-soap-critical-fight-against-coronavirus-out-reach-billions-unicef (accessed on 7 April 2020).
- MHLW. The Results of the 1st “National Survey for New Corona Countermeasures” and Announcement of the 3rd “National Survey for New Corona Countermeasures.” Ministry of Health, Labor, and Welfare (in Japanese). 2020. Available online: https://www.mhlw.go.jp/stf/newpage_10798.html (accessed on 7 April 2020).
- Baseel, C. Gargling to Prevent Colds—Just a Japanese old Wives’ Tale? JAPANTODAY. 2014. Available online: https://japantoday.com/category/features/health/gargling-to-prevent-colds-just-an-japanese-old-wives-tale (accessed on 7 April 2020).
- Satomura, K.; Kitamura, T.; Kawamura, T.; Shimbo, T.; Watanabe, M.; Kamei, M.; Tamakoshi, A. Prevention of upper respiratory tract infections by gargling: A randomized trial. Am. J. Prev. Med. 2005. [Google Scholar] [CrossRef] [PubMed]
- Bell, V.; Ferrão, J.; Pimentel, L.; Pintado, M.; Fernandes, T. One Health, Fermented Foods, and Gut Microbiota. Foods 2018, 195. [Google Scholar] [CrossRef] [PubMed]
- Veld, E.V.T. 7 Japanese Superfoods to Boost your Immune System. 2020. Available online: https://japantoday.com/category/features/food/7-japanese-superfoods-to-boost-your-immune-system (accessed on 7 April 2020).
- Déléris, P.; Nazih, H.; Bard, J.M. Seaweeds in Human Health. In Seaweed in Health and Disease Prevention; Academic Press: Cambridge, MA, USA, 2016. [Google Scholar] [CrossRef]
- Wildish seaweed. Can Irish Seaweed help in the Fight against Viruses? 2020. Available online: https://www.wildirishseaweeds.com/can-irish-seaweed-help-in-the-fight-against-viruses/ (accessed on 7 April 2020).
- Nania, R. How Chronic Conditions Complicate Coronavirus Infections. AARP. 2020. Available online: https://www.aarp.org/health/conditions-treatments/info-2020/chronic-conditions-coronavirus.html (accessed on 7 April 2020).
- Knapton, S. Coronavirus has Mutated into more Aggressive Disease, say Scientists. The Telegragh. 2020. Available online: https://www.telegraph.co.uk/science/2020/03/04/coronavirus-has-mutated-aggressive-disease-say-scientists/ (accessed on 7 April 2020).
- Kamikubo, Y.; Takahashi, A. Epidemiological Tools that Predict Partial Herd Immunity to SARS Coronavirus 2. MedRxiv 2020. [Google Scholar] [CrossRef]
- Nishijima, S.; Suda, W.; Oshima, K.; Kim, S.W.; Hirose, Y.; Morita, H.; Hattori, M. The gut microbiome of healthy Japanese and its microbial and functional uniqueness. DNA Res. 2016. [Google Scholar] [CrossRef] [PubMed]
- Kida, S. Image Diagnosis in Japan 2 -Comparison of CT and MRI Numbers and imaging Frequency with OECD Countries-. Imacel Academy. 2018. Available online: https://lp-tech.net/articles/8fix9 (accessed on 7 April 2020).
- McCarthy, N. Where Europeans Wash Their Hands After Using The Toilet. Statista. 2020. Available online: https://www.statista.com/chart/4111/do-europeans-wash-their-hands-after-using-the-toilet/ (accessed on 7 April 2020).
- Palahí, M.; Pantsar, M.; Costanza, M.; Kubiszewski, M.; Potočnik, J.; Stuchtey, M.; Bas, L. Investing in Nature to Transform the Post COVID-19 Economy: A 10-point Action Plan to create a circular bio-economy devoted to sustainable wellbeing. 2020. Available online: https://www.thesolutionsjournal.com/article/investing-nature-transform-post-covid-19-economy-10-point-action-plan-create-circular-bioeconomy-devoted-sustainable-wellbeing/ (accessed on 9 June 2020).
- Hagihara, Y.; Hagihara, K. Chapter 2 Water Resources Conflict Management: Social Risk Management. In Coping with Regional Vulnerability, New Frontiers in Regional Science: Asian Perspectives 4; Hagihara, K., Asahi, C., Eds.; Springer: Tokyo, Japan, 2016; pp. 21–41. [Google Scholar]
- Hagihara, Y. Adaptive System Planning Methodology for Environmental Risk Management; Kyoto University Press: Kyoto, Japan, 2008. (In Japanese) [Google Scholar]
- AFP BB News. The Cause of the Corona Pandemic is "Disrespect of Animals" Said by Mr. Goodall, a primatologist.. 2020. Available online: https://www.afpbb.com/articles/-/3278221 (accessed on 12 April 2020).
- Jacobo, J. Venice Canals are Clear enough to see Fish as Coronavirus Halts Tourism in the City. abc NEWS. 2020. Available online: https://abcnews.go.com/International/venice-canals-clear-fish-coronavirus-halts-tourism-city/story?id=69662690 (accessed on 17 April 2020).
- Orjollet, S.; Christensen, S. VIDEO: Why Coronavirus could Help Save China’s Endangered Species. CAPITAL NEWSPAPERS. 2020. Available online: https://capitalnewspapers.co.za/afp/938372/video-why-coronavirus-could-help-save-chinas-endangered-species (accessed on 17 April 2020).
- Mavrodieva, A.; Shaw, R. Disaster and climate change issues in Japan’s Society 5.0—A discussion. Sustainability 2020, 12, 1893. [Google Scholar] [CrossRef]
- Shaw, R.; Chatterjee, R.; Dabral, A. Integrating Biological Hazards (including Pandemic) into Disaster Risk Reduction (DRR) Planning, Annex Document; UNDRR: Baltimore, MD, USA, 2020; p. 71. [Google Scholar]
- Chan, E.; Shaw, R. Overview of health-EDRM and health issues in DRR: Practices and challenges. In Public Health and Disasters; Chan, E.Y.Y., Shaw, R., Eds.; Springer: Singapore, 2020; pp. 1–6. [Google Scholar]
- WHO. Health Emergency and Disaster Risk Management Framework; WHO: Geneva, Switzerland, 2019. [Google Scholar]
- DeWitt, A.; Djlante, R.; Shaw, R. Building holistic resilience: Tokyo’s 2050 strategy. Asia Pac. J. 2020, 18, 1–5. [Google Scholar]
- Djlante, R.; Shaw, R.; DeWit, A. Building resilience against biological hazards and pandemics: COVID-19 and its implications for the Sendai Framework. Prog. Disaster Sci. 2020. [Google Scholar] [CrossRef]
- Mukherjee, M.; Chatterjee, R.; Khanna, B.K.; Dhillon, P.P.S.; Kumar, A.; Bajwa, S.; Shaw, R. Ecosystem-centric business continuity planning (Eco-centric BCP)- a post COVID19 new normal. Progress Disaster Sci. 2020. In press. [Google Scholar]
| Aspect / Factors | Japan | Overseas |
|---|---|---|
| 1. Government Response | ||
| Lockdown | No, but declared a state of emergency for seven prefectures that then evolved to a nationwide emergency state | Yes |
| Immigration restrictions | Yes | Yes |
| Remote work | Applied | Applied |
| Closing schools | Applied | Applied |
| 2. Culture | ||
| Greeting | Bow, sometimes shake hands | Shake hands, hug, Cheek kissing |
| Social distancing | Moderate | Low |
| Wearing a mask | No emotional resistance
| Emotional resistance |
| 3. Health Care System | ||
| National Health Insurance Program | Universal (for all people) | Regional disparities |
| Medical system (guideline for COVID-19, CT scan, etc.) | Available with detailed guidelines | Available |
| PCR No. of CT [36] | After CT scan 107/million | Following diagnosis OECD: 25/million |
| 4. Sanitation | ||
| Basic handwashing with soap | Educated since childhood Frequent | Regional disparities Washing hands after toilet [37]: Italy 57%, UK 75% |
| Gargling throat | Educated since childhood | Not common |
| Hot water bathing | Japanese custom Almost all houses have a bathtub | Shower instead of immersion bath |
| Ventilating a room | Open window | Air conditioner |
| Disinfection gel | At the entrance of a building or in a washroom | Regional disparities |
| Wet towel | Served when eating out | Served rarely |
| 5. Food Habits | ||
| Eat seaweeds | Yes (marine algae, marine plants) | Rarely |
| Eat fermented food | Yes (miso, soy source, tsukemono) something that includes lactic acid bacteria) | Few (e.g., yogurt, cheese, beer, wine) but a different type of Japanese foods |
| Cutlery | Chopsticks | Folk, knife, spoon, but sometimes use hands |
| 6. Immune System | ||
| Spread type of COVID-19 | S-type spread from China earlier than L-type, generating partial resistance | L-type spread |
| Intestinal environment | About 90% of Japanese have intestinal flora with genes for enzymes that disassemble dietary fiber in seaweed | Less than 15% have genes found in Japanese population |
| Response measure | Individuals take action to enhance their immune system | Depend on immunological mechanisms of vaccination |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Tashiro, A.; Shaw, R. COVID-19 Pandemic Response in Japan: What Is behind the Initial Flattening of the Curve? Sustainability 2020, 12, 5250. https://doi.org/10.3390/su12135250
Tashiro A, Shaw R. COVID-19 Pandemic Response in Japan: What Is behind the Initial Flattening of the Curve? Sustainability. 2020; 12(13):5250. https://doi.org/10.3390/su12135250
Chicago/Turabian StyleTashiro, Ai, and Rajib Shaw. 2020. "COVID-19 Pandemic Response in Japan: What Is behind the Initial Flattening of the Curve?" Sustainability 12, no. 13: 5250. https://doi.org/10.3390/su12135250
APA StyleTashiro, A., & Shaw, R. (2020). COVID-19 Pandemic Response in Japan: What Is behind the Initial Flattening of the Curve? Sustainability, 12(13), 5250. https://doi.org/10.3390/su12135250