Proactive and Strategic Healthcare Public-Private Partnerships (PPPs) in the Coronavirus (Covid-19) Epoch
Abstract
1. Public-Private Partnerships (PPPs) as an Optional Solution?
It is impossible to overstate the importance of healthcare—after all, worldwide economic growth and development depend on it—but governments’ ability to provide affordable, quality healthcare dwindles every year. The challenge is now to engage private partners to deliver public benefits. Innovative, forward-looking public-private partnerships in healthcare do this, giving businesses an unparalleled opportunity to do well while doing good [1] (p. 1).
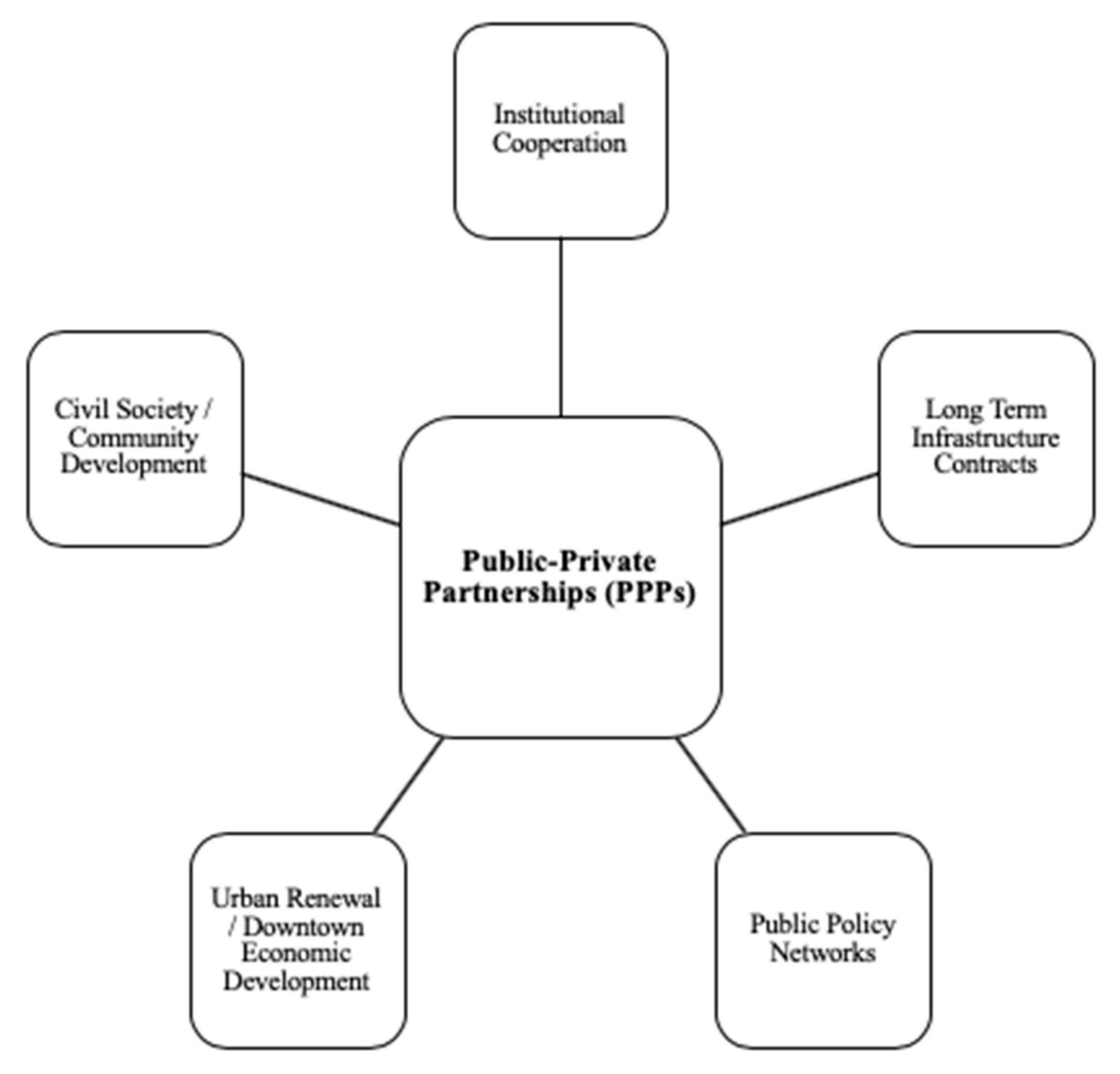
2. What Do We Mean by Public-Private Partnerships (PPPs)?
- Are we referring to voluntary short-term philanthropic partnerships and alliances between the governments (public sector) and industry (private sector)? or
- Are we referring to (un)conventional PPPs which involve contractual arrangements between the public and private sectors to provide public works, goods, and services over a defined period of time, in a partnership that improves delivery efficiencies though innovation, risk sharing, and mobilization of joint resources [8,9,10,11]?
- infrastructure-based models—i.e., building and/or refurbishing public healthcare infrastructure;
- discrete Clinical Services models—i.e., adding or expanding clinical service delivery capacity; and
- integrated PPP models—i.e., bundled packages of both infrastructure and clinical services.
3. A Multifaceted Approach to Healthcare PPPs
4. Components of a Healthcare PPP Strategy
5. Short-Term, Reactive PPP Projects and Partnerships (0 to 12 Months)
- encouraging informal philanthropic partnerships between the public and private sectors to bridge pressing needs;
- improving supply chains through incentives from the public sector (i.e., National Health Authorities) that avoid unnecessary cost escalations for needed products;
- promoting collaborative actions where national and subnational government agencies identify and mobilize resources (e.g., pharmaceuticals, medical instruments, PPE, etc.) according to shifting locational needs;
- bolstering access to digital infrastructure that allows healthcare stakeholders to be fleetfooted in their decision making and responsiveness;
- creating healthcare data systems that collect information on how the pandemic spreads as well as “lessons learned” for future events;
- incentivizing private sector-led solutions that are non-proprietary/open source; and
- relaxing unnecessary bureaucratic red tape that hinders meaningful sector partnerships.
break the public-sector monopoly, inject … flexibility into provision of [healthcare services], extend the public sector’s access to technical, financial, and physical resources, and improve service quality, all while operating in increasingly uncertain policy environments [6] (p. 162).
6. Medium-Term, Proactive PPP Projects and Partnerships (1 to 5 Years)
7. Long-Term, Future-Proofed PPP Projects and Partnerships (5+ Years)
- all (if possible) national government health ministries;
- the World Health Organization (WHO);
- NATO and its equivalents;
- the International Red Cross/Crescent;
- aid organizations (e.g., USAID, JICA, etc.);
- multilateral development banks; and
- regional associations like the European Union (EU).
8. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- International Finance Corporation (IFC). Health PPPs. Handshake IFC’s Q. J. Public Priv. Partnersh. 2011, 3, 1–75. [Google Scholar]
- John Hopkins University (JHU). COVID-19 Dashboard; Center for Systems Science and Engineering (CSSE), JHU: Baltimore, MD, USA, 2020. [Google Scholar]
- Hodge, G.; Carsten, G. Public-private partnerships: Governance scheme or language game? Aust. J. Public Adm. 2010, 69, S8–S22. [Google Scholar] [CrossRef]
- Harty, C.; Roine, L. The futures of construction management research. Constr. Manag. Econ. 2017, 35, 392–403. [Google Scholar] [CrossRef]
- Marsilio, M.; Giulia, C.; Corrado, C. The intellectual structure of research into PPPS: A bibliometric analysis. Public Manag. Rev. 2011, 13, 763–782. [Google Scholar] [CrossRef]
- Casady, C.B.; Kent, E.; Raymond, E.L.; Richard Scott, W. (Re)Defining Public-Private Partnerships (PPPs) in the New Public Governance (NPG) Paradigm: An Institutional Maturity Perspective. Public Manag. Rev. 2020, 22, 161–183. [Google Scholar] [CrossRef]
- Hodge, G.A.; Carsten, G. Public-Private Partnerships: An International Performance Review. Public Adm. Rev. 2007, 67, 545–558. [Google Scholar] [CrossRef]
- Organization for Economic Cooperation & Development (OECD). Recommendation of the Council on Principles for Public Governance of Public-Private Partnerships; OECD: Paris, France, 2012. [Google Scholar]
- Schomaker, R.M. Public-private governance regimes in the global sphere. Public Organ. Rev. 2017, 17, 121–138. [Google Scholar] [CrossRef]
- Casady, C.B.; Kent, E.; Raymond, E.L.; Richard Scott, W. Examining the State of Public-Private Partnership (PPP) Institutionalization in the United States. Eng. Proj. Organ. J. 2018, 8, 177–198. [Google Scholar]
- Casady, C.B. Examining the Institutional Drivers of Public-Private Partnership (PPP) Market Performance: A Fuzzy Set Qualitative Comparative Analysis (fsQCA). Public Manag. Rev. 2020. [Google Scholar] [CrossRef]
- Cruz, C.O.; Rui, C.M. Integrating infrastructure and clinical management in PPPs for health care. J. Manag. Eng. 2013, 29, 471–481. [Google Scholar] [CrossRef]
- Abdel Aziz, A.; Shu, W. PPPs for Healthcare Facilities in British Columbia: A Preliminary Analysis. In Proceedings of the ASCE Construction Research Congress, Tempe, AZ, USA, 8–10 March 2020. [Google Scholar]
- Abuzaineh, N.; Brashers, E.; Foong, S.; Feachem, R.; da Rita, P. PPPs in Healthcare: Models, Lessons and Trends for the Future. Healthcare Public Private Partnership Series, No. 4; The Global Health Group, Institute for Global Health Sciences, University of California, San Francisco and PwC: San Francisco, CA, USA, 2018. [Google Scholar]
- Buse, K.; Andrew, M.H. Seven habits of highly effective global public–private health partnerships: Practice and potential. Soc. Sci. Med. 2007, 64, 259–271. [Google Scholar] [CrossRef] [PubMed]
- Baxter, D. How Will Coronavirus Affect Public-Private Partnerships? World Bank Blogs: Washington, DC, USA, 2020. [Google Scholar]
- Baxter, D. The Need for Sustainable PPP Recovery Strategies in a Post-COVID-19 World; LinkedIn: Sunnyvale, CA, USA, 2020. [Google Scholar]
- Ranney, M.L.; Valerie, G.; Ashish, K.J. Critical supply shortages—The need for ventilators and personal protective equipment during the Covid-19 pandemic. N. Engl. J. Med. 2020, 382, e41. [Google Scholar] [CrossRef] [PubMed]
- Opara, M.; Fathi, E.; Oliver, O.; Hussein, W. Effects of the Institutional Environment on Public-Private Partnership (P3) Projects: Evidence from Canada. Account. Forum 2017, 41, 77–95. [Google Scholar] [CrossRef]
- United Nations Economic Commission for Europe (UNECE). What Are People-First PPPs? UNECE International Center of Excellence: Geneva, Switzerland, 2019. [Google Scholar]
- Khorram-Manesh, A. Flexible surge capacity–public health, public education, and disaster management. Health Promot. Perspect. 2020, 10, 1–5. [Google Scholar]
- Salamon, L. The New Governance and the Tools of Public Action: An Introduction. In The Tools of Government: A Guide to the New Governance; Salamon, L., Elliot, O.V., Eds.; Oxford University Press: New York, NY, USA, 2002; pp. 1–48. [Google Scholar]
- Nishtar, S. Public–private ’partnerships’ in health—A global call to action. Health Res. Policy Syst. 2004, 2, 5. [Google Scholar] [CrossRef] [PubMed]
- Albalate, D.; Germà, B.; Richard Geddes, R. Do Public-Private-Partnership-Enabling Laws Increase Private Investment in Transportation Infrastructure? J. Law Econ. 2020, 63, 43–70. [Google Scholar] [CrossRef]
- Baxter, D. Future-Proofing Resilient PPPs; World Bank Blogs: Washington, DC, USA, 2017. [Google Scholar]
- Hanlon, B.O.; Mark, H.; Cynthia, E.; David, C. An Action Plan to Engage the Private Sector in the Response to COVID-19; Interim Guidance; World Health Organization (WHO): Geneva, Switzerland, 2020. [Google Scholar]
- Hodge, G.; Carsten, G.; Mhamed, B. Do PPP’s work? What and how have we been learning so far? Public Manag. Rev. 2018, 20, 1105–1121. [Google Scholar] [CrossRef]
- Kettl, D.F. Sharing Power: Public Governance and Private Markets; Brookings Institution Press: Washington, DC, USA, 2011. [Google Scholar]
- Teisman, G.R.; Erik-Hans, K. Partnership arrangements: Governmental rhetoric or governance scheme? Public Adm. Rev. 2002, 62, 197–205. [Google Scholar] [CrossRef]
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Baxter, D.; Casady, C.B. Proactive and Strategic Healthcare Public-Private Partnerships (PPPs) in the Coronavirus (Covid-19) Epoch. Sustainability 2020, 12, 5097. https://doi.org/10.3390/su12125097
Baxter D, Casady CB. Proactive and Strategic Healthcare Public-Private Partnerships (PPPs) in the Coronavirus (Covid-19) Epoch. Sustainability. 2020; 12(12):5097. https://doi.org/10.3390/su12125097
Chicago/Turabian StyleBaxter, David, and Carter B. Casady. 2020. "Proactive and Strategic Healthcare Public-Private Partnerships (PPPs) in the Coronavirus (Covid-19) Epoch" Sustainability 12, no. 12: 5097. https://doi.org/10.3390/su12125097
APA StyleBaxter, D., & Casady, C. B. (2020). Proactive and Strategic Healthcare Public-Private Partnerships (PPPs) in the Coronavirus (Covid-19) Epoch. Sustainability, 12(12), 5097. https://doi.org/10.3390/su12125097