1. Introduction
Recurrent pregnancy loss (RPL) is described as the occurrence of two or three repeated abortions, prior to the 20th week of pregnancy [
1]. The frequency of RPL is approximately 1–2%, affecting 5% of couples [
1]. There are numerous risk factors, mainly metabolic and anatomic, accompanied by systematic abnormalities and infections [
2,
3]. To this date, even though there are a plethora of studies regarding the etiologic factors of RPL, the full comprehension of the immune dysregulation that causes miscarriages seems to be elusive [
4].
Leukocytes are a significant component of the human endometrium of the female reproductive system. Their numbers increase to 10% of stromal cells, in the proliferative phase. Prior to the phase of implantation is the secretory phase, in which 20% of endometrial cells are leukocytes. In early pregnancy, the proportion of leukocytes increases to 30% of the decidual cells [
5]. This indicates their implication in RPL [
6,
7,
8,
9].
CD4 (cluster of differentiation 4) cells are glycoproteins, which are located on the surface of immune cells, more specifically on the surface of Th (T-helper) cells, monocytes, macrophages, and dendritic cells [
6]. CD8 (cluster of differentiation 8) cells are transmembrane glycoproteins, which function as coreceptors of the TCR (T-cell receptor) [
6]. Class I proteins of the MHC have the capacity to bind CD8 cells and TCRs [
6]. Darmochwal-Kolarz et al. [
7] studied the variations in the lymphocyte phenotype of women with unexplained pregnancy losses in comparison with healthy ones. They found that the number of CD4
+ T-lymphocytes and CD8
+ T-cells was significantly higher in patients with recurrent pregnancy loss.
The CD3 antigen is expressed mostly in T-lymphocytes and less in other cells, e.g., Purkinje cells, macrophages, and Hodgkin and Reed–Sternberg cells. It is expressed not only in the early maturation of T-lymphocytes but also in the pre-thymocyte cortical stage and is located within the perinuclear space of the cells [
8]. Mengyang Du et al. gathered blood samples from RPL cases and observed that, in the peripheral blood of these women, CD3
+ T-cells were significantly increased in comparison with a control group consisting of women with a normal pregnancy. The risk of miscarriage was increased proportionally to the augmentation of women with the level of CD3
+ cells. However, the miscarriage risk did not appear to further increase when the level of CD3
+ T cells exceeded 67.84% [
9].
CD20 is an antigen expressed in B-lymphocytes, particularly in mature B cells. It is not expressed in active plasmocytes [
10]. CD20 is a non-glycosylated phosphoprotein, consisting of three hydrophobic regions that are embedded in the cellular membrane [
10,
11]. It is structured by two long ends—one amino and one carboxyl—which are located intracellularly, with only a portion of the antigen exposed extracellularly [
10,
11]. This protein has a variety of functions, such as the modulation of B-lymphocytes, proliferation, and differentiation. The CD20 molecule is expressed primarily during the development of pre-B-lymphocytes [
11]. In an investigation undertaken with RPL patients, levels of CD45
+, CD56
+, CD16
+, CD3
+, CD8
+, and CRTH2
+ cells were similar to those in control groups. No significant difference in lymphocyte subset numbers or percentages was noted between patients whose later pregnancy was successful and those whose later pregnancy was unsuccessful [
9].
In recent years, studies have attempted to figure out the relationship between regulatory T-cells and RPL cases. It is widely believed that these cells play a vital role in establishing and maintaining the maternal–fetal immune tolerance [
12,
13].
Taking into account that nearly 50% of RPL cases are still classified as unexplained [
14], we performed this immunohistochemical study in order to contribute to the scientific community with more knowledge on the matter. Our hypothesis was based on the immunological profile of RPL. Thus, we studied the markers CD3, CD4, CD8, and CD20 and their implication in RPL. We expected a significant expression of immune cells in the endometrial tissues of women with recurrent miscarriages in the first trimester of gestation, compared to those with a normal early pregnancy until termination. Regardless of the comparative outcome, we consider whether or not specific cells contribute to the pathophysiology of unexplained recurrent miscarriages.
2. Materials and Methods
The miscarriage experimental group comprised 20 Caucasian Greek women, aged between 35 and 42 years, who miscarried during the first trimester of gestation. The control group consisted of 20 healthy Caucasian Greek women, aged between 27 and 39 years, who electively terminated their pregnancies during the first trimester of gestation. Informed consent was collected from all patients, and Ethical Committee approval was received. All 20 females from the experimental group (EG) underwent a very specific background check. They reported at least three miscarriages of unexplained etiology. Women with fewer than three miscarriages (even without an etiology, were excluded from the study). Additionally, several abnormalities and known causes of miscarriages were evaluated, in order for their exclusion (
Table 1). Thus, the inclusion criteria constituted RPL cases with no known anatomical or systematic abnormality. The inclusion and exclusion parameters were further assessed through an explorative pathological examination. The study was conducted according to the guidelines of the Declaration of Helsinki and approved by the Institutional Review Board (or Bioethics Committee) of Aristotle University of Thessaloniki (School of Medicine) (Number of approval: 4-198/17-7-2019).
2.1. Pathology Examination
Tissue specimens were collected and prepared for the microscope. They were collected immediately after miscarriage or elective abortion and washed with distilled water for removal of mucus and blood. These specimens were placental endometrial tissue that was set to be discarded. Pathology examination of the tissues and immunohistochemical analysis was performed. Then, tissues were studied under a stereomicroscope, so that specimens from decidua, villus chorion and parts of the embryo could be distinguished and examined for formation abnormalities or placental lesions. Specimens with formation abnormalities or placental lesions were excluded from the study. In order to evaluate any morphological abnormality with the optical microscope, specimens were stained with eosin-haematoxylin. Specimens were collected from the distinguished decidua and the villus chorion. They were stabilized in aqueous solution of neutral formalin 10% v/v for 12–24 h. Subsequent to this, specimens were placed in an automatic machine for further processing, including fixation, dehydration, xylene clarification and paraffin embedding. Then, paraffin-embedded blocks of specimens were cut in 3 mm sections and transferred to positive-charged and properly prepared glass plates, which were kept in an oven at 37–40 °C for 30–45 min. Afterwards, specimens were stained with haematoxylin-eosin solution (Harris). Many specimens were excluded due to errors on the process of collecting the tissues and anatomical deficiencies. The stained specimens were examined with a microscope and the most suitable of them were selected for immunohistochemical study.
Furthermore, in order to perform immunohistochemistry, four antibodies were selected: CD3, CD4, CD8, and CD20. These antibodies were obtained from DAKO Products. The dilution for each antibody’s solution is 1:100 for CD3, 1:50 for CD4 and CD8, and 1:200 for CD20.
Immunohistochemistry
In all specimens, the sites of decidua basalis and trophoblast (chorionic villi) were identified using the cytokeratin antibody (CK7), which is positive in chorionic villi. Moreover, in order to distinguish the chorionic villi (trophoblast) from the decidual cells at the feto-maternal interface, duplicate sections were stained with a monoclonal antibody against prolactin, for the visualization of decidual cells. The unstained specimens were further processed using an automatic machine (Bond Max) that carried out the following standard procedures of our laboratory. First, deparaffinization was performed in xylene. Afterwards, specimens were immersed in absolute alcohol, in degressive densities 100%, 96% and 70% v/v, consecutively, and were rinsed with distilled water. Antigen retrieval was performed by incubation at various temperatures, depending on the antibody that was examined each time. Following this procedure, specimens were first rinsed with PBS buffer, then incubated in H2O2 for 5 min, to quench endogenous peroxidase activity and finally rinsed again with PBS buffer. Afterwards, specimens were covered with a solution of the primary tonic monoclonal antibody. These antibodies, as mentioned previously, are CD3, CD4, CD8, CD20 and were obtained from DAKO Products. The dilution for each antibody’s solution is 1:100 for CD3, 1:50 for CD4 and CD8, and 1:200 for CD20. Tonsil was used as an appropriate control. Eventually, specimens were washed using WAS solution. For the detection of immunohistochemical staining, specimens were firstly immersed in Post Primary solution. After being washed, specimens were immersed in polymer solution and then in chromogen diaminobenzidine (DAB) solution. Finally, specimens were stained with Haematoxylin–Eosin. Following the previous stages that were performed by the automatic processor, specimens were rinsed in tap water and dehydrated with escalating densities of ethanol solution (70, 96, and 100% v/v, consecutively) and xylene. Then, they were covered with tape, placed in glass plates and immersed in Canada balsam. After the immunohistochemical staining procedure, specimens were thoroughly examined.
2.2. Microscopic Evaluation
An optical ZeissTM microscope was used and photographs were taken using a ContaxTM camera, attached to the microscope. In total, endometrial specimens—from decidua basalis, trophoblast and decidua parietalis—were examined by 2 independent researchers, specialized in pathology evaluation. The intensity of staining was evaluated on a 4-scale measure. The evaluation of the intensities was performed on the main sites of our tissue, of which there were three: decidua basalis, trophoblast, and decidua parietalis. The examination was managed by two independent researchers, specialists in the field of pathology evaluation. The intensity of staining was qualitatively evaluated as negative (–), weak (+), moderate (++) and strong (+++) based on each researcher’s observations on the microscope. A distinct granular brown stain was scored as positive. According to several studies, to be considered as positive, specimens should present at least 5% of granular stains. Above that score, the evaluation is weak (5–20%), then moderate (20–60%), and finally, strong (consecutively, up to a score of >60%). This is a widely approved consensus among the pathologists for the staining in immunohistochemistry methods.
2.3. Statistical Analysis
The results were statistically analyzed and confirmed for their significance using the Mann–Whitney U test. The data were checked for normal distribution prior to the selection of the Mann–Whitney U test. Our two independent researchers evaluated the intensity of all specimens twice on a blinded process, randomly presented from a third party. The final findings of each observer were collated and differences were noted. Our findings on the staining were quite conspicuous, since the intensities of each researcher were rather similar. There were a few discrepancies, mostly among weak and moderate intensities, but they were exceeded.
Our distinguished data were divided into two independent groups, and Mann–Whitney’s null hypothesis was checked. The level of significance was at 0.05—two-tailed hypothesis—and the p-value was estimated for each study undertaken among the two groups. The null hypothesis asserts that the two samples are identical and do not differ significantly (p-value > 0.05), while the alternative hypothesis means that results differ significantly (p-value < 0.05). In order to evaluate each case study and perform the statistics, we used the SPSS Statistics software. Our results were double-checked using the Mann–Whitney Test Online Calculator (accessed on 5 May 2021). The photographic material that follows is merely an indicating proportion of the study that was performed.
4. Discussion
The immunological environment of early pregnancy is rather complicated, especially between the RPL and abortion cases, which consisted of the experimental and control group of the present experiment. This study aimed to comparatively evaluate placental tissues received from the two distinguished groups. However, one should be cautious regarding the control group, as elective termination may not be able to provide a realistic depiction of the normal maternal-fetus environment. Regarding the immunohistochemical investigation, the present experiment made an attempt to correlate the imbalance of CD3, CD4, CD8, and CD20 levels, and the dysregulation of the immune system in the endometrial tissue, with the RPL pathogenesis (up to 80% of RPL cases) [
15,
16]. This study provides a comprehensive comparison of the CD3
+, CD4
+, CD8
+, and CD20
+ levels, in the decidua (both basalis and parietalis) and the chorionic villi, among women with RPL and women who electively terminated their pregnancy. Significant differences on the expression of the studied markers were found in the decidua parietalis (
Table 2,
Table 3 and
Table 4) (
Figure 9,
Figure 10 and
Figure 11).
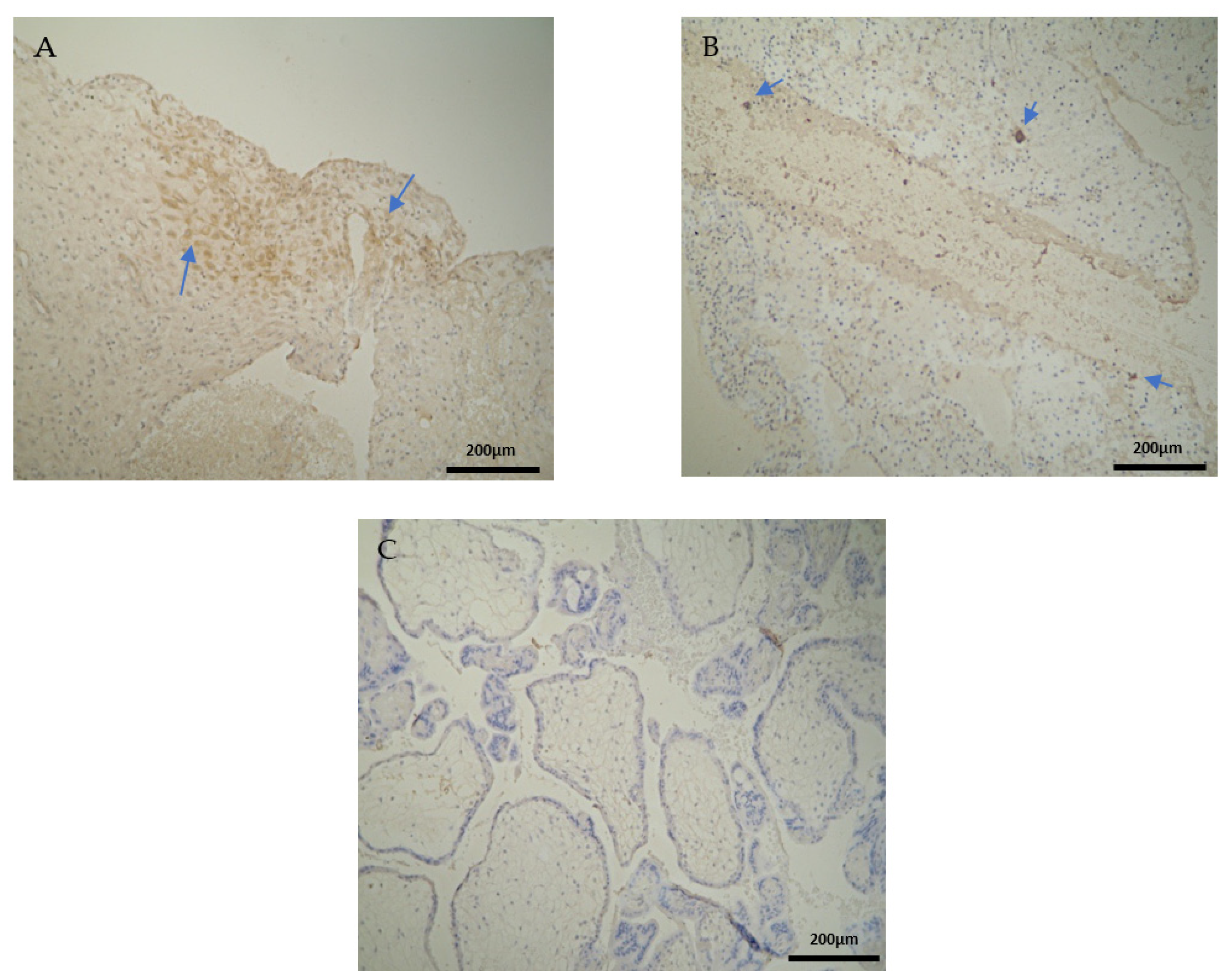
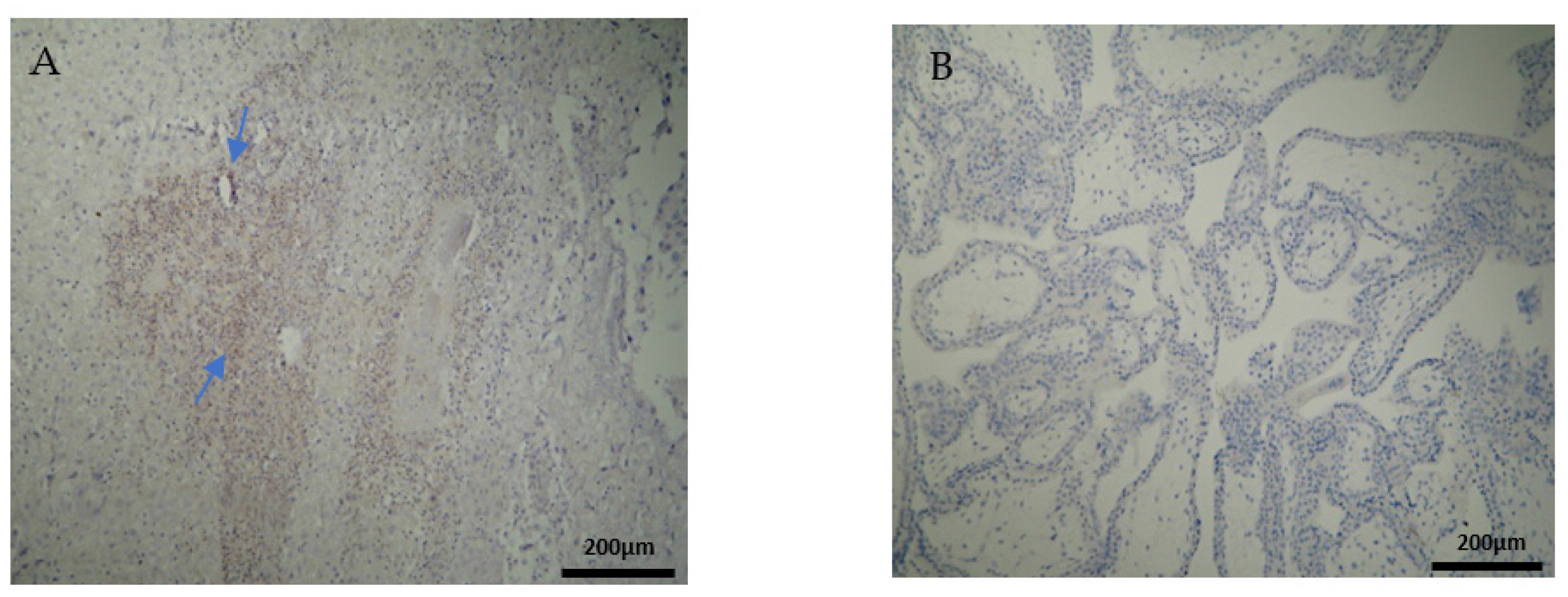
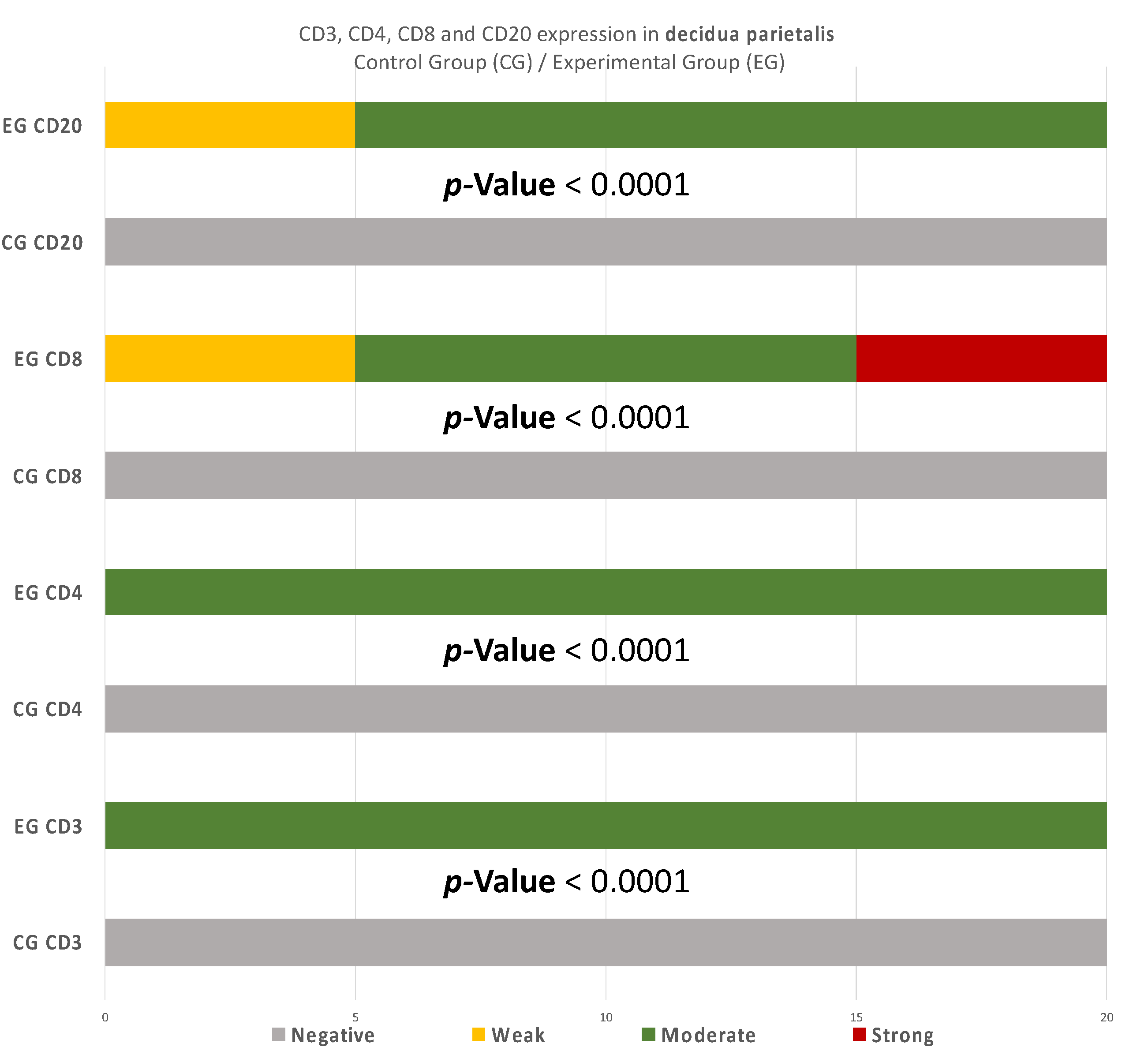
To begin with, the miscarriage group samples presented a significantly higher expression in all the CD3 cells that were studied, in comparison to the control group samples (
p-value < 0.00001) (
Table 5). The moderate CD3 expression found in the EG is in agreement with Du et al. [
9]. These results differ from Kolanska K et al. [
17], who did not observe significant disparities on the CD3
+ levels, among the experimental and control group. However, the fact that the present miscarriage group appeared to have a positive expression of CD3 in the decidua parietalis (
Table 2) supports the hypothesis [
9] that the risk of miscarriage phenomena increases proportionally to the augmentation of the CD3
+ levels in the mothers’ peripheral blood. Given the current data—that maternal adaptive immune cells display a more activated phenotype in the decidua parietalis than the decidua basalis [
18]—there is a strong indicator that increased CD3
+ cells in the DP may contribute significantly to the occurrence of RPL phenomena. In addition, Quinn K et al. [
19] has shown that the DP has a significantly higher ratio of T-regulator cells expression in comparison to the DB.
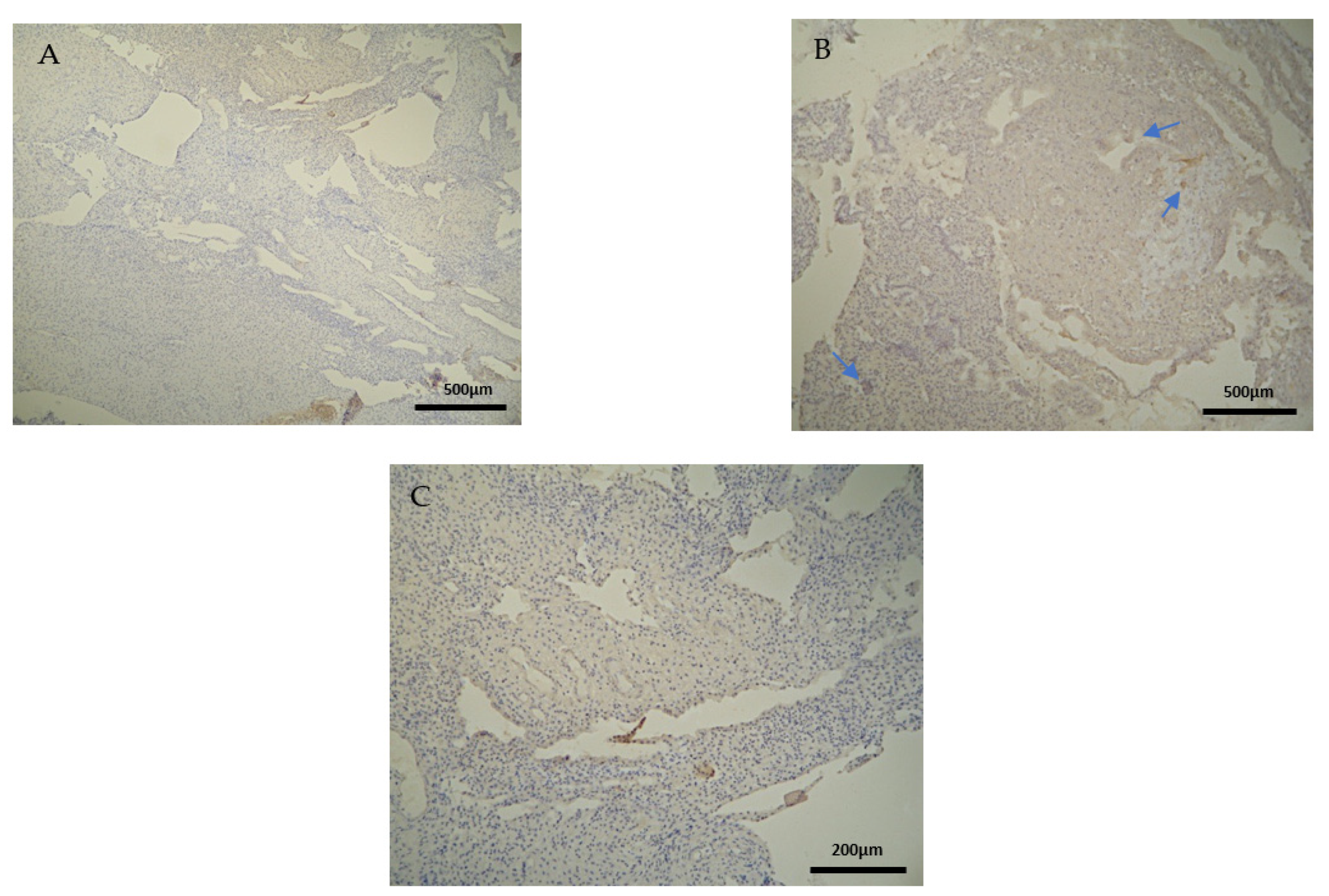
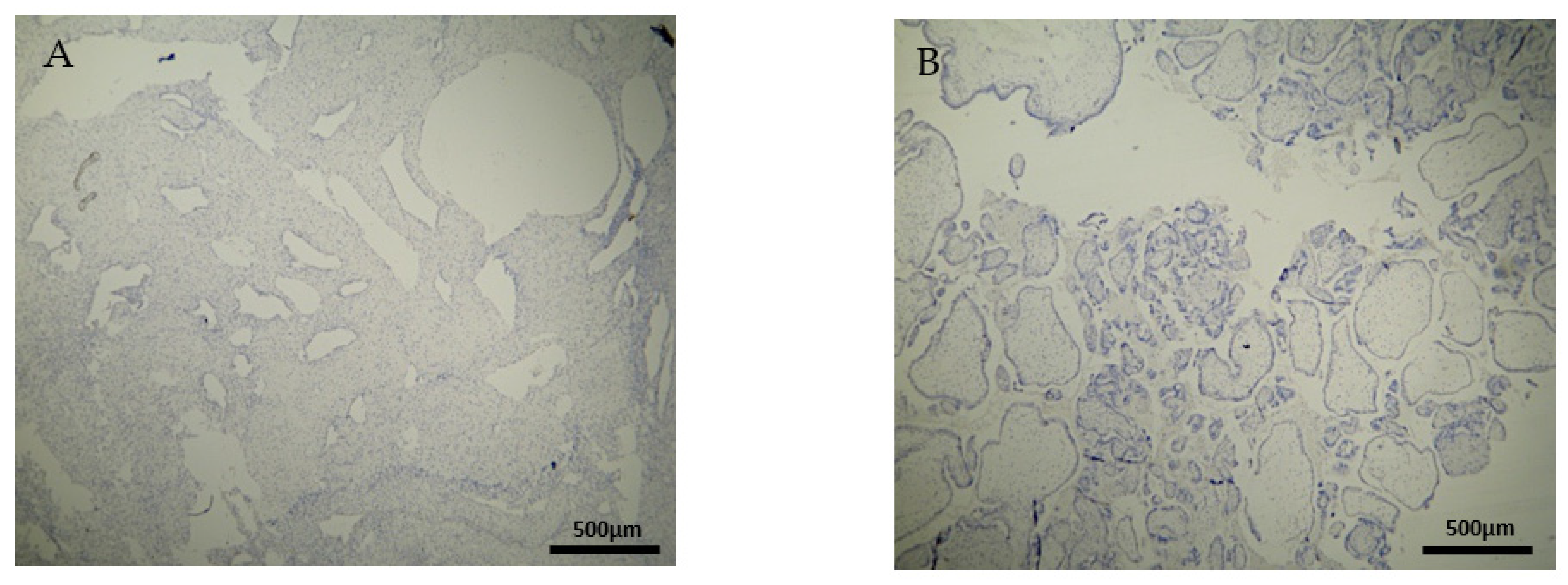
Likewise, there was a significant expression of CD4
+ cells in the decidua parietalis of all RPL cases. The CG samples were negative (
p-value < 0.00001) (
Table 6). This particular finding arouses suspicion regarding the implication of CD3
+ and CD4
+ presence in the decidua parietalis tissues and their participation to RPL phenomena. There is suspicion that the strong CD4
+ expression in the decidua parietalis is in accordance with the CD4
+ positive serum levels in mothers’ peripheral blood, since they were observed to be particularly high in several RPL cases [
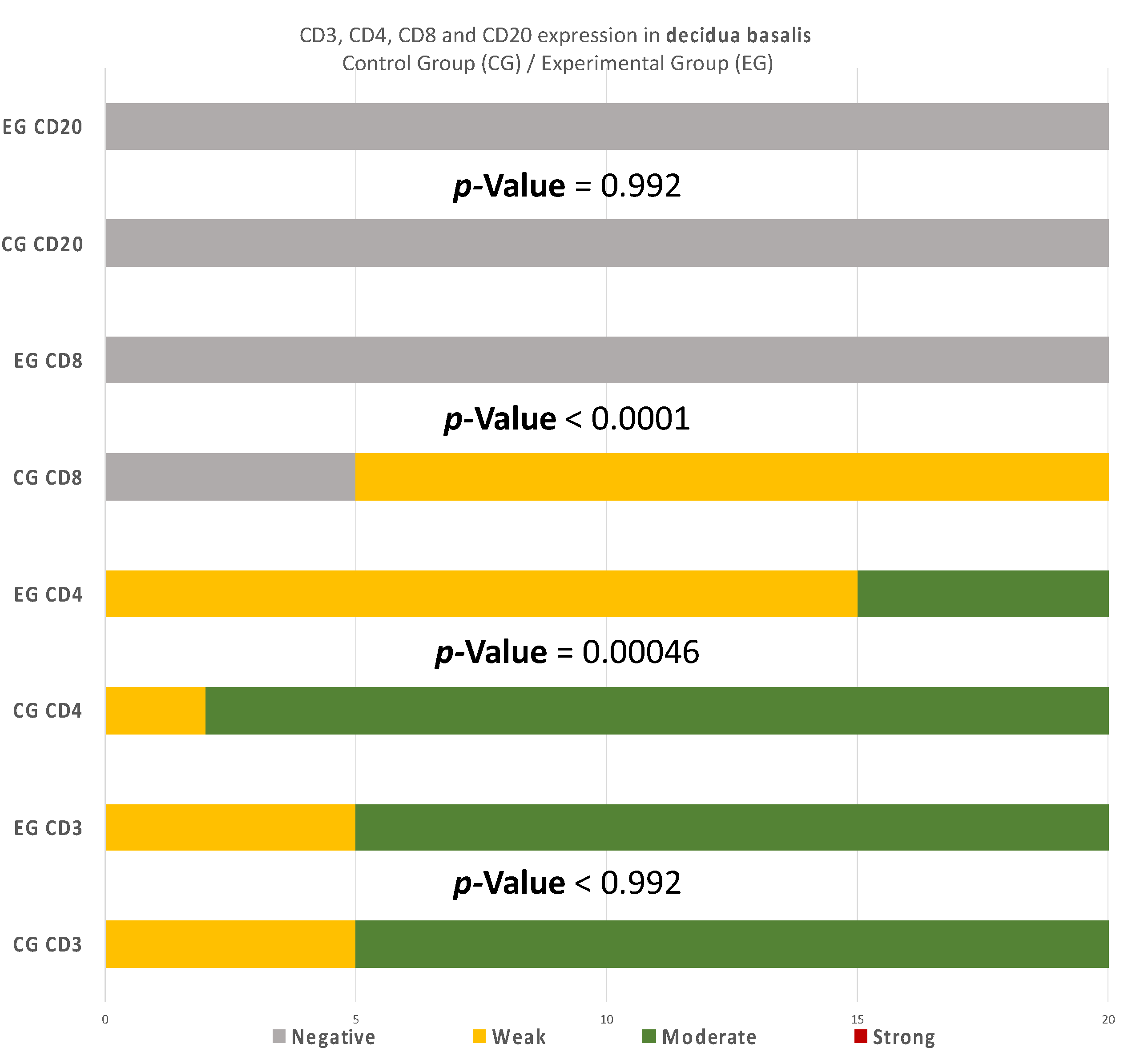
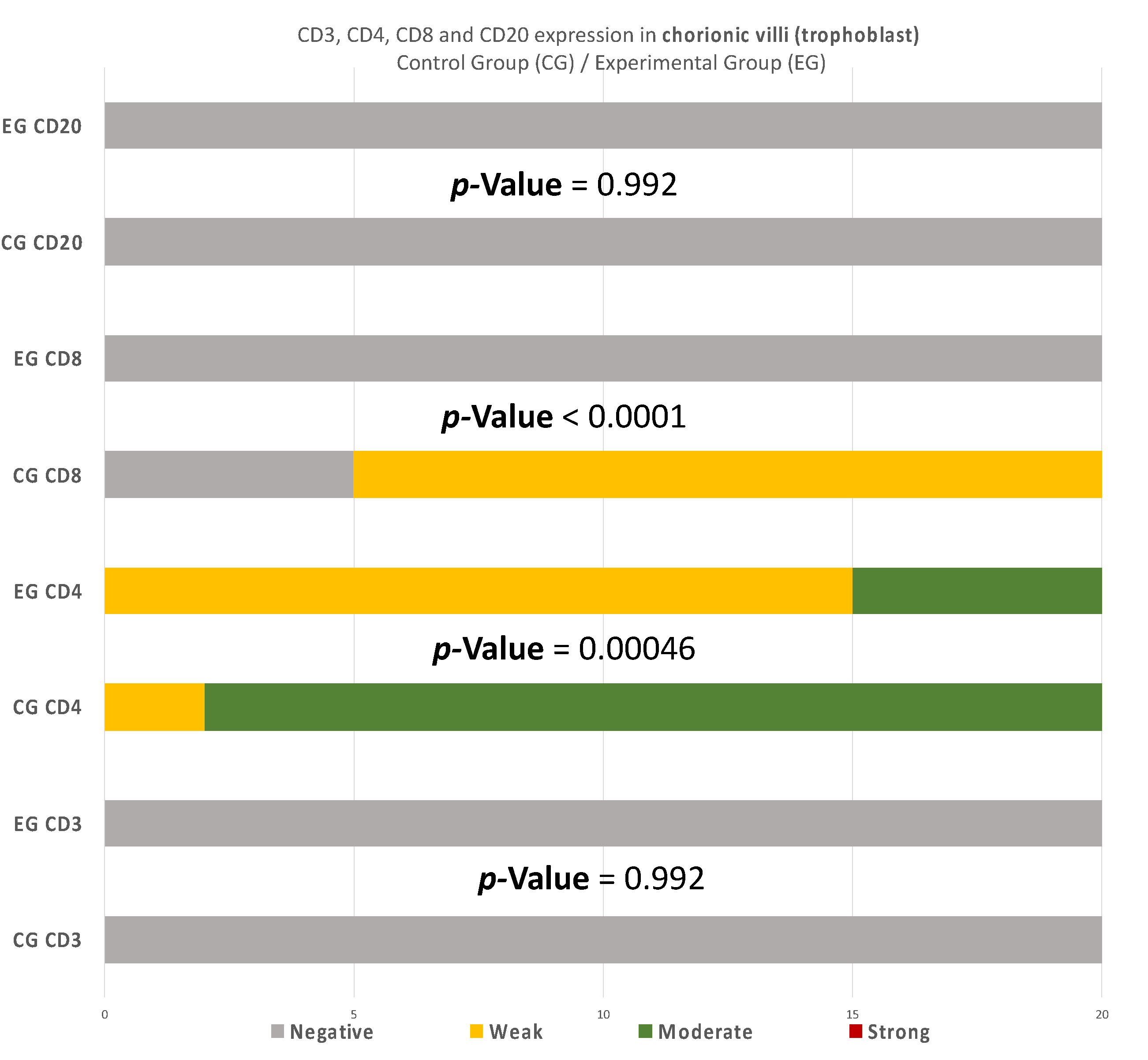
7]. Contrary to the decidua parietalis, the expression of CD4
+ in the decidua basalis and chorionic villi displayed an interesting variety of distribution. In most specimens, the control group demonstrated a moderate staining, while the experimental group appeared with low intensity (
p-value = 0.00046) (
Table 7). According to Li et al. [
20] and Inada et al. [
21], the percentage of CD4
+ positive cells was lower in the decidua samples of early recurrent miscarriage patients, comparing to women with a normal early pregnancy. These interesting studies were in full accordance with the CD4
+ levels found in the DB of our experimental and control group samples. This particular discovery leads us to the conclusion that T-cells in the decidua basalis and chorionic villi, are essential for a normal early pregnancy. In addition to that—according to Logiodice et al. [
22]—CD4
+ T-cells that were presented in the decidua of women who experienced a successful pregnancy were producing IL-4 (Interleukin), whereas in women with RPL, there was no IL-4 production. In the present study, we did not investigate the expression of CD25 for Treg-cells; thus, the aforementioned findings raise the question for further immunohistochemical analyses.
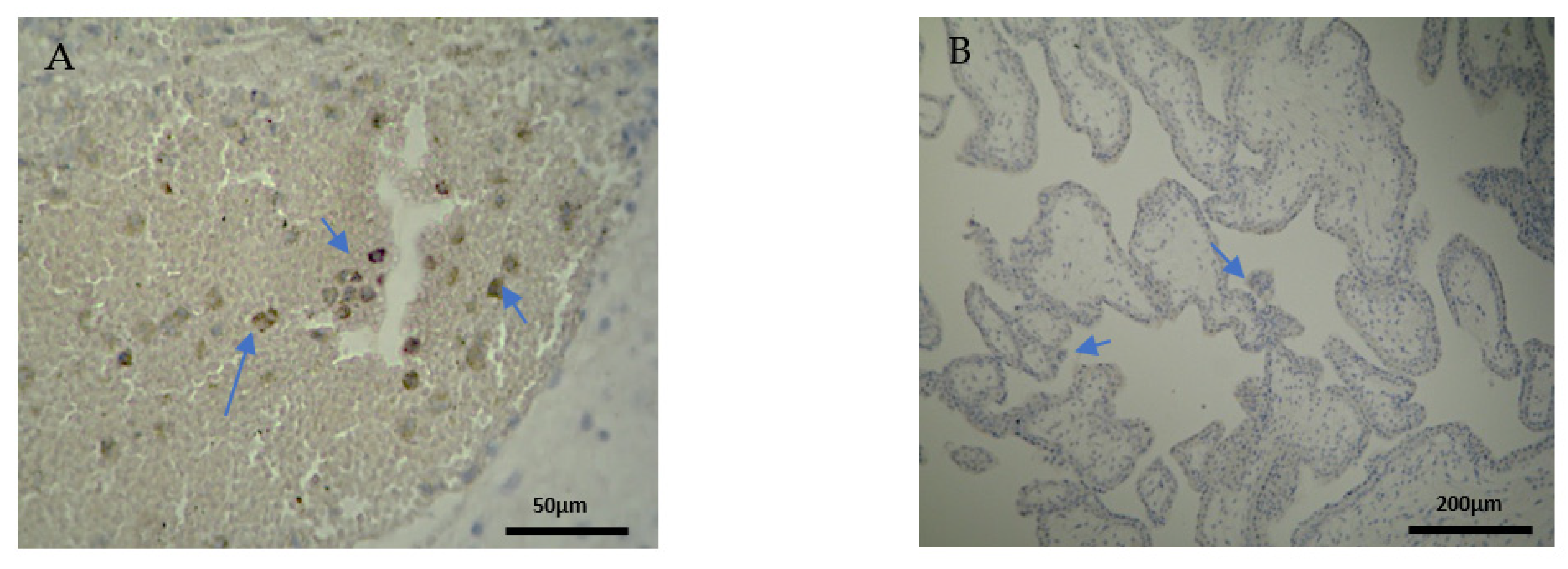
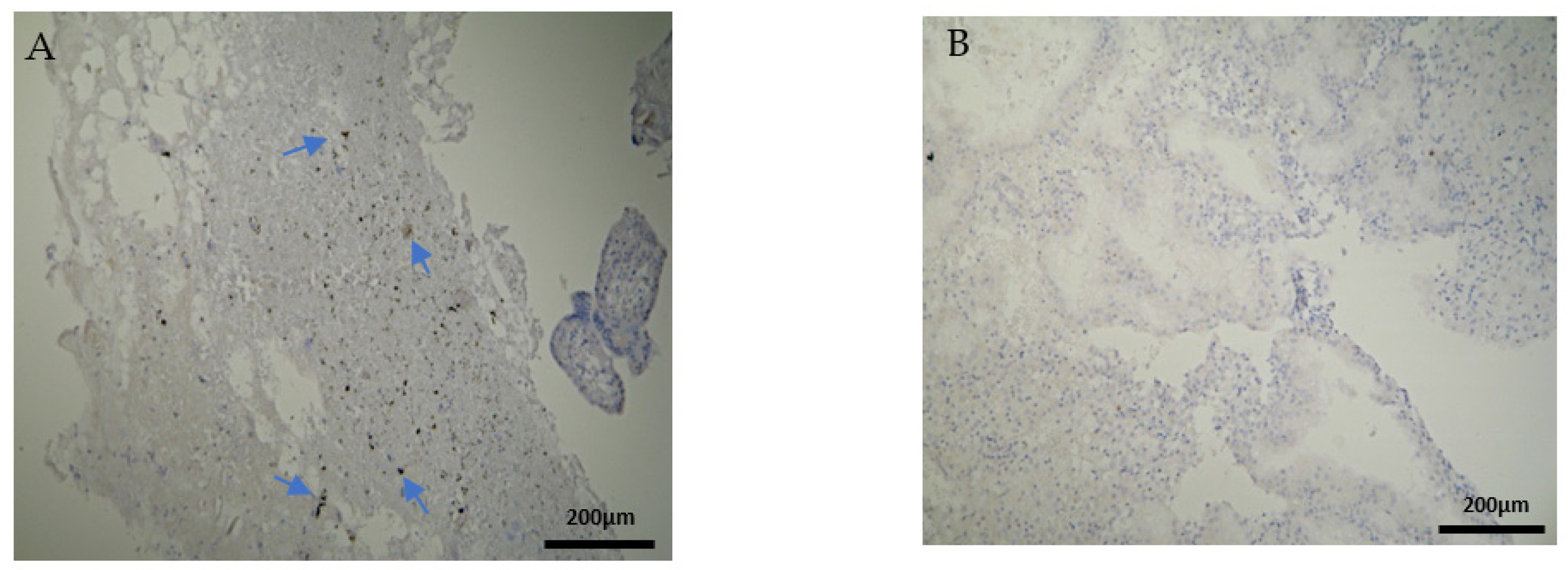
Furthermore, there were conspicuous disparities of CD8
+ levels in the decidua parietalis among the two groups (
p-value < 0.00001) (
Table 7). One should definitely wonder whether the strong CD8
+ antigen expression—similar to the DP of our EG samples—stands as an accomplice to the immune dysregulation, which leads to a potential pregnancy loss. The zero presence of CD8
+ positive expression in the CG specimens strengthens the above hypothesis. According to further experiments, Darassejeze et al. [
23] found that the prolonged activation of CD8
+ cells was directly linked to the augmentation of miscarriage rates on rats. The aggregated positive expression near decidual vessels in our EG samples comes into full accordance with the conclusions of Russel et al. [
24]. Despite these results, Lachapelle et al. [
25] observed that the percentage of endometrial CD8
+ T-Lymphocytes was significantly decreased in RPL cases. Our findings were quite similar to the aforementioned observation, since there was zero positive CD8 T-cells in both decidua basalis and chorionic villi of our EG samples. The control group’s results strengthen these findings, as a significant percentage of CD8
+ T-cells was found, which is expected for a normal pregnancy to occur (
p-value < 0.00001) (
Table 7). Moreover, Johnsen G et al. [
26] suggested that the absence of CD8
+ in the decidua basalis, could be involved in further complications, such as the development of acute atherosis—a common spiral arterial lesion in preeclampsia. The analysis of the presence of CD8
+ T-cells seems to be a rather controversial issue, as one could be led to contradictory results, depending on the site of study.
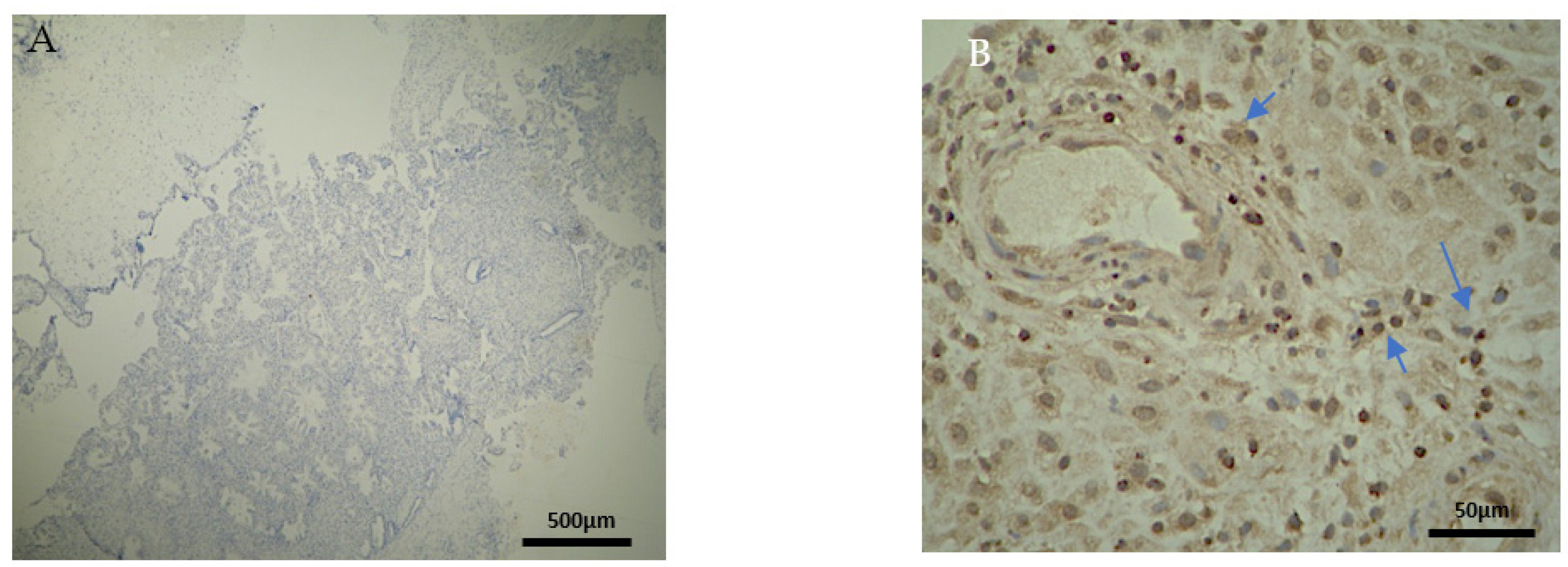
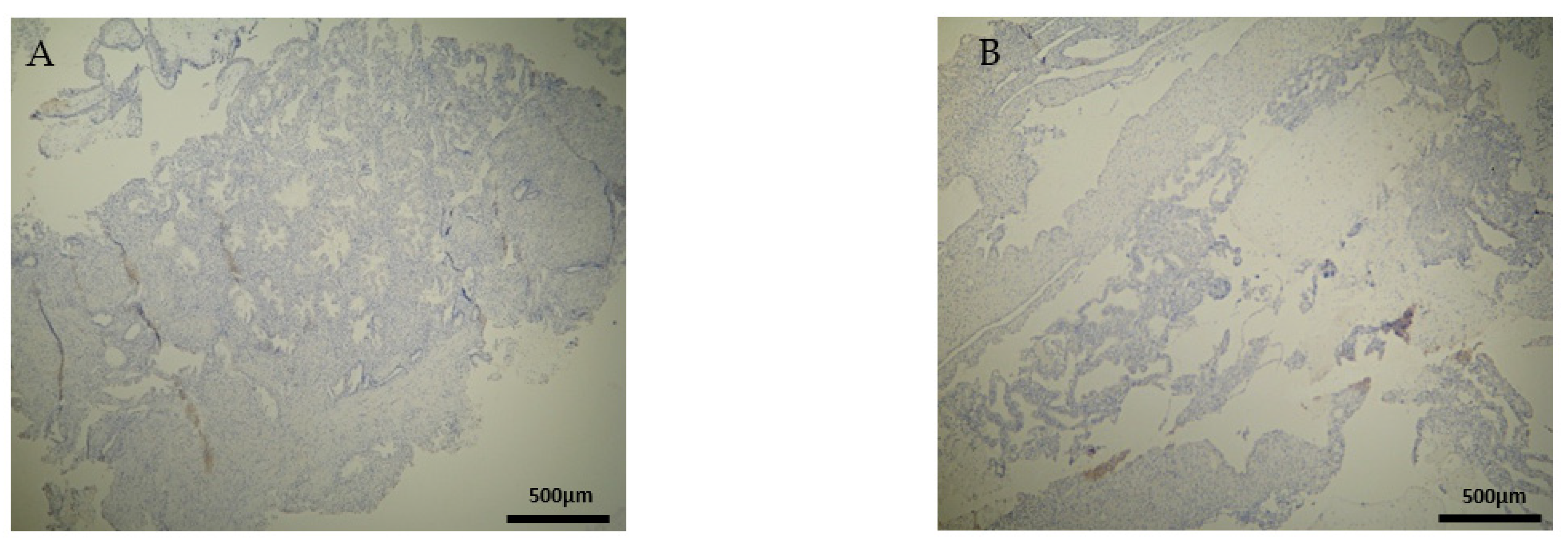
Recurrent miscarriages are associated by some studies with increased numbers of CD20
+ lymphocytes [
9,
27]. In our experiment, an intense staining in the DP of the EG samples was found, contrary to the CG samples, where there was no expression. This antithesis establishes fundamental evidence of the strong relationship between RPL and the presence of CD3
+, CD4
+, CD8
+, and CD20
+ cells in the decidua parietalis (
p-value < 0.00001) (
Table 8).
4.1. Inconsistencies and Cohesions
Based on prominent studies, there should not be any T- or B-cell expression observed in placenta tissues [
28]. The present immunohistochemical study did not observe any expression regarding the studied markers in the decidua parietalis of the electively terminations (control group). However, the control group exhibited notable differences in the decidua basalis and trophoblast, which was not expected based on the aforementioned study [
28]. There is an implication that some CD4 subsets minimize the embryotoxic state of other CD4 subsets; thus, it should be furthered studied [
29]. Some other CD4 subsets initiate inflammatory processes through many cytokines. However, even in this case, there is a fragile balance that is crucial for placentation and early pregnancy [
30]. For instance, even though TNF-a (induced by a CD4 subset) is the main culprit for several immunopathologic complications, it has been reported to have a protective role regarding the fetoplacental regulation [
31]. Unfortunately, our study is limited to the subset analysis. It seems that CD4(+)CD25(+) Treg-cells are essential in the induction and maintenance of the essential immune-tolerance of normal pregnancy [
32]. The CD4 levels in our study are intriguing and rather thought-provoking, especially regarding the control group. Additionally, several studies have shown that positive functional regulatory T-cells are decreased in the decidua basalis and chorionic villi of the RPL cases [
12,
33,
34]. Our conclusive data were in full accordance to them and provided even more evidence regarding the CD
+ levels in the DB and how they may affect the immunological regulation, which could lead to a miscarriage. The lower intensity of CD4
+ and CD8
+ in trophoblast and decidua basalis seems to negatively affect the course of a normal pregnancy, perhaps due to a significant reduction of the maternal immune tolerance. Regarding the CD20 cells, apart from the soaring levels in decidua parietalis, there was no significant difference in the decidua basalis and chorionic villi among the two groups. Positive T-cells were found in the decidua parietalis, displaying a more activated phenotype, with a higher intensity of staining, in comparison to those isolated from the DB and the trophoblast. This is a rather interesting outcome, as the decidua parietalis is not located in the maternal–fetal connective interface, and one would definitely not expect to find more activated T-cells there (at least not compared to the DB). This enacts as a proof of correlation among RPL cases and the increased levels of T-cells in the DP.
Finally, despite the contradiction, it should also be mentioned that there are several cases, e.g., Bohlmann et al. [
35] and Michimata et al. [
36], which did not observe a significant relationship between altered endometrial immunity and the RPL cases. Although the main culprits regarding immune dysregulation are known, the specific details that lead to RPL are still elusive. It is interesting that a study conducted among women with unexplained miscarriages and healthy fertile women with successful pregnancies revealed elevated CD4 lymphocytes in patients with recurrent pregnancy loss [
7]. This study was not performed using electively terminations as controls; thus, despite the fact that we agree on the expression on RPL cases, it is not feasible to apply a proper comparison. Regardless of the methodological differences, each research is significant as it contributes on the elucidation of the immunological imbalance of early pregnancy. After all, despite so many remarkable studies, RPL remains an “unexplained” phenomenon to almost half of the cases [
37].
4.2. Clinical Implications
The clinical approach of the RPL depends on the pathogenesis of each condition. Chromosomal causes, anatomical abnormalities, clotting disorders, and hormonal and immunological causes must be investigated as a priority, as there are specific treatments for each condition. In order to understand the mechanisms of the unexplained RPL, researchers should collect as many data as possible regarding the immunological response when such phenomena occur. Thus, more experimental studies should be conducted. Immunization and maternal antibodies’ “behavior” might hold the key not only for setting a diagnosis but also for preventing pregnancy loss. There are several widely used and available algorithms assisting clinicians on the evaluation of each condition and offering possible explanation to parents suffering from miscarriages [
38]. However, these algorithms come with painstakingly evaluation that put pressure not only on the couple but on the healthcare system as well. Diagnosis and possible treatment should be based on the causal factors of the RPL [
38]. Therefore, clarifying the “picture” of the immunological reaction in the developmental tissue environment (e.g., decidua, trophoblast, etc.) might assist in the development of improved and rigorous algorithms for diagnosis and even new therapeutic interventions.
4.3. Limitations and Strengths
This study has some limitation. As already mentioned, the percentage of the specific immune cells may be subjected to a margin of error due to the immunohistochemical evaluation of staining with a single antibody and not with a double-staining method. Another limitation is the lack of comparative laboratory methods (e.g., flow cytometry), in order to determine the specific cell levels on mothers’ peripheral blood, alongside the immunohistochemical placental evaluation. Generally, it seems that the immunological balance between mother and fetus is rather sensitive and volatile. Despite our exclusion criteria and the hypothesis (RPL vs. electively termination cases), there are many unknown factors that may affect the results. However, the study adds extra knowledge regarding the importance of distinguishing the sites of immunohistochemical evaluation, as the decidua parietalis presented conspicuous dissimilarities in comparison to the DB and trophoblast. Hopefully, with more studies, we will be able to narrow down the factors and utterly comprehend the process of immune dysregulation that leads to RPL.