Esophagitis Dissecans Superficialis (EDS) Secondary to Hair Dye Ingestion: Case Report and Literature Review
Abstract
1. Introduction
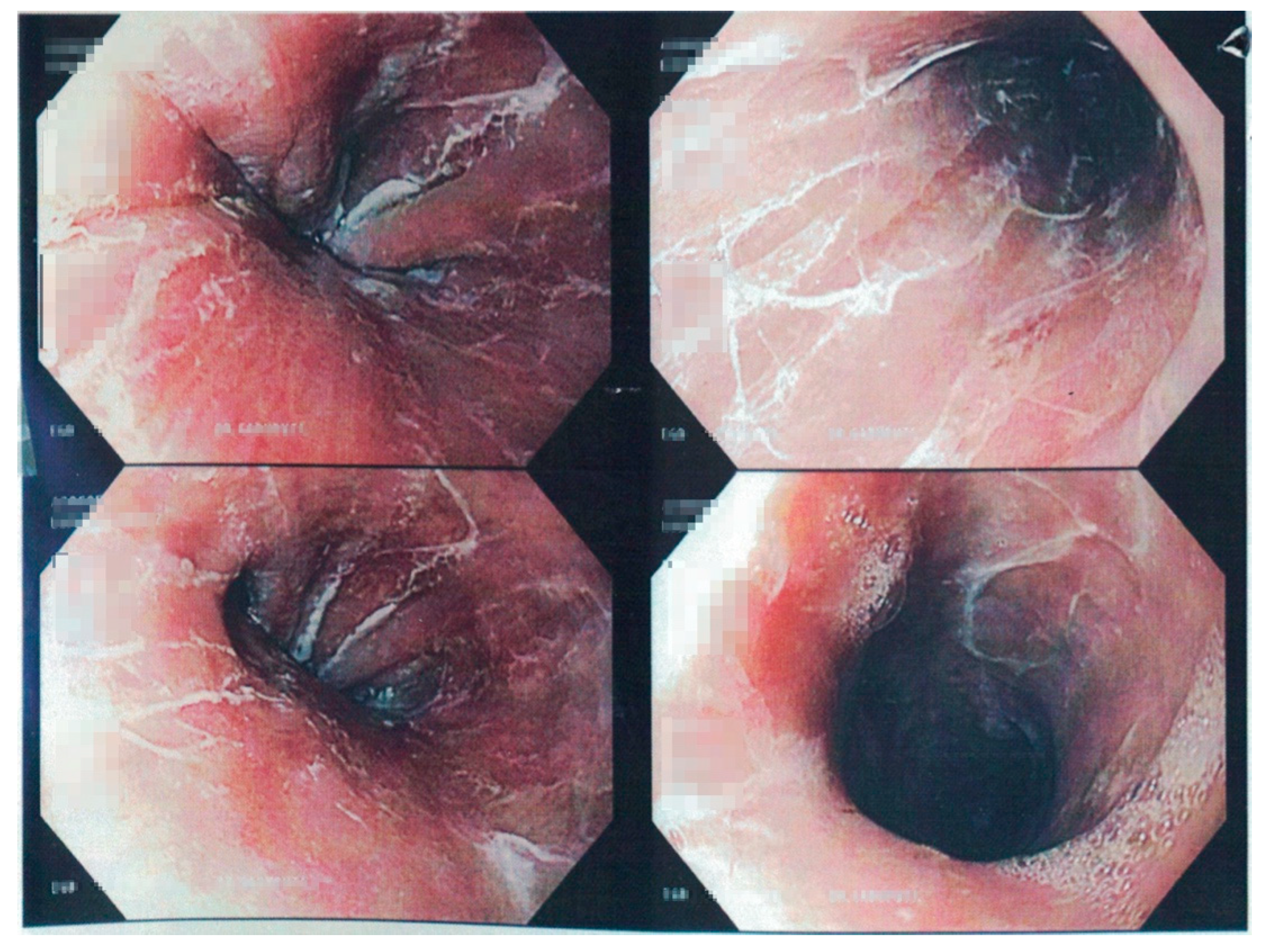
2. Case Report
3. Discussion
4. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Carmack, S.W.; Vemulapalli, R.; Spechler, S.J.; Genta, R.M. Esophagitis dissecans superficialis (“sloughing esophagitis”): A clinicopathologic study of 12 cases. Am. J. Surg. Pathol. 2009, 33, 1789–1794. [Google Scholar] [CrossRef] [PubMed]
- Hart, P.A.; Romano, R.C.; Moreira, R.K.; Ravi, K.; Sweetser, S. Esophagitis Dissecans Superficialis: Clinical, Endoscopic, and Histologic Features. Dig. Dis. Sci. 2015, 60, 2049–2057. [Google Scholar] [CrossRef] [PubMed]
- Fiani, E.; Guisset, F.; Fontanges, Q.; Devière, J.; Lemmers, A. Esophagitis dissecans superficialis: A case series of 7 patients and review of the literature. Acta Gastroenterol. Belg. 2017, 80, 371–375. [Google Scholar] [PubMed]
- Purdy, J.K.; Appelman, H.D.; McKenna, B.J. Sloughing esophagitis is associated with chronic debilitation and medications that injure the esophageal mucosa. Mod. Pathol. 2012, 25, 767–775. [Google Scholar] [CrossRef] [PubMed]
- Hage-Nassar, G.; Rotterdam, H.; Frank, D.; Green, P.H. Esophagitis dissecans superficialis associated with celiac disease. Gastrointest. Endosc. 2003, 57, 140–141. [Google Scholar] [CrossRef] [PubMed]
- Hokama, A.; Yamamoto, Y.; Taira, K.; Nakamura, M.; Kobashigawa, C.; Nakamoto, M.; Hirata, T.; Kinjo, N.; Kinjo, F.; Takahashi, K.; et al. Esophagitis dissecans superficialis and autoimmune bullous dermatoses: A review. World J. Gastrointest. Endosc. 2010, 16, 252–256. [Google Scholar] [CrossRef] [PubMed]
- Yogarajah, M.; Sivasambu, B.; Jaffe, E.A. Bullous systemic lupus erythematosus associated with esophagitis dissecans superficialis. Case Rep. Rheumatol. 2015, 2015, 930683. [Google Scholar] [CrossRef] [PubMed]
- Lamine, H.; Bochra, B.; Mouna, M.; Heykel, E.; Monia, T.; Mohamed Masaddak, A. Esophagitis dissecans superficialis due to severe nonsteroidal anti-inflammatory drugs toxicity. Presse Med. 2018, 47 Pt 1, 695–697. [Google Scholar] [CrossRef]
- Hokama, A.; Ihama, Y.; Nakamoto, M.; Kinjo, N.; Kinjo, F.; Fujita, J. Esophagitis dissecans superficialis associated with bisphosphonates. Endoscopy 2007, 39 (Suppl. S1), E91. [Google Scholar] [CrossRef] [PubMed]
- Nasir, U.M.; Rodgers, B.; Panchal, D.; Choi, C.; Ahmed, S.; Ahlawat, S. Ferrous Sulfate-Induced Esophageal Injury Leading to Esophagitis Dissecans Superficialis. Case Rep. Gastroenterol. 2020, 14, 172–177. [Google Scholar] [CrossRef] [PubMed]
- Abbass, K.; Haveman, L.; Gertner, E. Esophagitis dissecans superficialis due to severe methotrexate toxicity. Endoscopy 2014, 46 (Suppl. S1), E99–E100. [Google Scholar] [CrossRef] [PubMed]
- Da Silva, J.R.; Pinho, R.; Ponte, A.; Silva, M.; Furtado, A.; Carvalho, J. Esophagitis dissecans superficialis associated with severe clindamycin toxicity. J. Gastrointest. Liver Dis. 2014, 23, 363. [Google Scholar] [CrossRef]
- Mukkanna, K.S.; Stone, N.M.; Ingram, J.R. Para-phenylenediamine allergy: Current perspectives on diagnosis and management. J. Asthma Allergy 2017, 10, 9–15. [Google Scholar] [CrossRef] [PubMed]
- Beck, R.N. Oesophagitis dissecans superficialis. Br. Med. J. 1954, 1, 501–502. [Google Scholar] [CrossRef]
- Mehta, V.; Nayak, S.; Balachandran, C. Pigmented contact cheilitis to paraphenylenediamine. Indian J. Dermatol. 2010, 55, 119–120. [Google Scholar] [CrossRef] [PubMed]
- Van Belle, A.B.; Cochez, P.M.; de Heusch, M.; Pointner, L.; Opsomer, R.; Raynaud, P.; Achouri, Y.; Hendrickx, E.; Cheou, P.; Warnier, G.; et al. IL-24 contributes to skin inflammation in Para-Phenylenediamine-induced contact hypersensitivity. Sci. Rep. 2019, 9, 1852. [Google Scholar] [CrossRef] [PubMed]
- Umair, S.F.; Amin, I.; Urrehman, A. Hair Dye poisoning: “An early intervention”. Pak. J. Med. Sci. 2018, 34, 230–232. [Google Scholar] [CrossRef] [PubMed]
- Verma, R.; Tewari, N.; Jaiswal, S.; Rastogi, V.; Singh, D.; Tiwari, A. Fatal poisoning caused by oral ingestion of a hair dye. Internet J. Emerg. Intensive Care Med. 2007, 11, 1. [Google Scholar]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Then, E.O.; Grantham, T.; Lopez, M.; Reddy, M.; Gaduputi, V. Esophagitis Dissecans Superficialis (EDS) Secondary to Hair Dye Ingestion: Case Report and Literature Review. Clin. Pract. 2021, 11, 185-189. https://doi.org/10.3390/clinpract11020026
Then EO, Grantham T, Lopez M, Reddy M, Gaduputi V. Esophagitis Dissecans Superficialis (EDS) Secondary to Hair Dye Ingestion: Case Report and Literature Review. Clinics and Practice. 2021; 11(2):185-189. https://doi.org/10.3390/clinpract11020026
Chicago/Turabian StyleThen, Eric Omar, Tyler Grantham, Michell Lopez, Madhavi Reddy, and Vinaya Gaduputi. 2021. "Esophagitis Dissecans Superficialis (EDS) Secondary to Hair Dye Ingestion: Case Report and Literature Review" Clinics and Practice 11, no. 2: 185-189. https://doi.org/10.3390/clinpract11020026
APA StyleThen, E. O., Grantham, T., Lopez, M., Reddy, M., & Gaduputi, V. (2021). Esophagitis Dissecans Superficialis (EDS) Secondary to Hair Dye Ingestion: Case Report and Literature Review. Clinics and Practice, 11(2), 185-189. https://doi.org/10.3390/clinpract11020026




