Reference Results for Blood Parameter Changes and Recovery after Pelvic Radiation without Chemotherapy
Abstract
1. Introduction
2. Materials and Methods
3. Results
4. Discussion
4.1. Erythrocytes (Red Blood Cells)/Hemoglobin
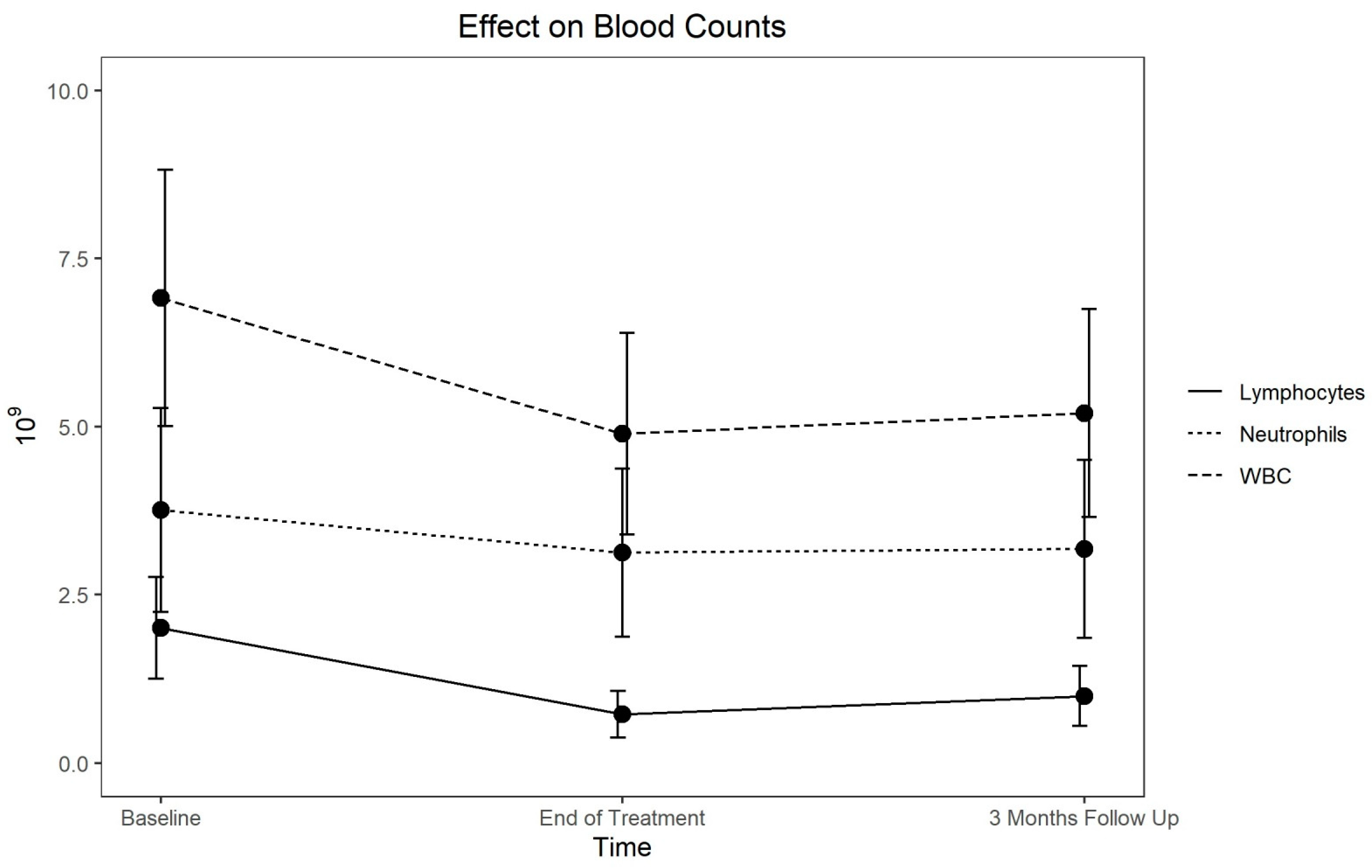
4.2. White Blood Cells
4.3. Granulocytes, Neutrophils, Eosinophils and Basophils
4.4. Lymphocytes
4.5. Monocytes
4.6. Platelets
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Swanson, G.; Hammonds, K.; Jhavar, S. Short-term haematogical effects of deprivation and radiotherapy in prostate cancer patients. Open J. Urol. 2021, 11, 103–111. [Google Scholar] [CrossRef]
- Heylmann, D.; Ponath, V.; Kindler, T.; Kaina, B. Comparison of DNA repair and radiosensitivity of different blood cell populations. Sci. Rep. 2021, 11, 2478. [Google Scholar] [CrossRef] [PubMed]
- Fliedner, T.M. The role of blood stem cells in hematopoietic cell renewal. Stem Cells. 1998, 16 (Suppl. S1), 13–29. [Google Scholar] [CrossRef] [PubMed]
- Hendry, J.H.; West, C.M. Apoptosis and mitotic cell death: Their relative contributions to normal-tissue and tumour radiation response. Int. J. Radiat. Biol. 1997, 71, 709–719. [Google Scholar] [CrossRef] [PubMed]
- Clift, R.A.; Buckner, C.D.; Appelbaum, F.R.; Sullivan, K.M.; Storb, R.; Thomas, E.D. Long-term follow-up of a randomized trial of two irradiation regimens for patients receiving allogeneic marrow transplants during first remission of acute myeloid leukemia. Blood 1998, 92, 1455–1456. [Google Scholar] [CrossRef]
- Brindle, J.M.; Trindade, A.A.; Shah, A.P.; Jokisch, D.; Patton, P.W.; Pichardo, J.C.; Bolch, W.E. Linear regression model for predicting patient-specific total skeletal spongiosa volume for use in molecular radiotherapy dosimetry. J. Nucl. Med. 2006, 47, 1875–1883. [Google Scholar]
- Davis, R.W.; Dole, N.; Izzo, M.J.; Young, L.E. Hemolytic effect of radiation; observations on renal bile fistula dogs subjected to total body radiation and on human blood irradiated in vitro. J. Lab. Clin. Med. 1950, 35, 528–537. [Google Scholar]
- Schiffer, L.M.; Atkins, H.L.; Chanana, A.D.; Cronkite, E.P.; Greenberg, M.L.; Johnson, H.A.; Robertson, J.S.; Stryckmans, P.A. Extracorporeal irradiation of the blood in humans: Effects upon erythrocyte survival. Blood 1966, 27, 831–843. [Google Scholar] [CrossRef]
- Button, L.N.; DeWolf, W.C.; Newburger, P.E.; Jacobson, M.; Kevy, S. The effects of irradiation on blood components. Transfusion 1981, 21, 419–426. [Google Scholar] [CrossRef]
- Moore, G.L.; Ledford, M.E. Effects of 4000 rad irradiation on the in vitro storage properties of packed red cells. Transfusion 1985, 25, 583–585. [Google Scholar] [CrossRef]
- Suda, B.A.; Leitman, S.F.; Davey, R.J. Characteristics of red cells irradiated and subsequently frozen for long-term storage. Transfusion 1993, 33, 389–392. [Google Scholar] [CrossRef] [PubMed]
- Davey, R.J.; McCoy, N.C.; Yu, M.; Sullivan, J.; Spiegel, D.; Leitman, S. The effect of prestorage irradiation on posttransfusion red cell survival. Transfusion 1992, 32, 525–528. [Google Scholar] [CrossRef] [PubMed]
- Bashir, F.A.; Parry, J.M.; Windsor, P.M. Use of a modified hemi-body irradiation technique for metastatic carcinoma of the prostate: Report of a 10-year experience. Clin. Oncol. (R. Coll. Radiol.) 2008, 20, 591–598. [Google Scholar] [CrossRef] [PubMed]
- Miszczyk, M.; Majewski, W. Hematologic toxicity of conformal radiotherapy and intensity modulated radiotherapy in prostate and bladder cancer patients. Asian Pac. J. Cancer Prev. 2018, 19, 2803–2806. [Google Scholar] [CrossRef]
- Valerius, N.H.; Johansen, K.S.; Nielsen, O.S.; Platz, P.; Rosenkvist, J.; Sørensen, H. Effect of in vitro X-irradiation on lymphocyte and granulocyte function. Scand. J. Haematol. 1981, 27, 9–18. [Google Scholar] [CrossRef] [PubMed]
- Lundgren, M.S.F.S.; Cavalcanti, M.S.M.; Sampaio, D.A. Weekly monitoring of the effects of conventional external beam radiation therapy on patients with head and neck, chest, and pelvis cancer by means of blood cells count. Radiol. Bras. 2008, 41, 29–33. [Google Scholar] [CrossRef]
- Zachariah, B.; Jacob, S.S.; Gwede, C.; Cantor, A.; Patil, J.; Casey, L. Effect of fractionated regional external beam radiotherapy on peripheral blood cell count. Int. J. Radiat. Oncol. Biol. Phys. 2001, 50, 465–472. [Google Scholar] [CrossRef]
- Girinsky, T.; Socie, G.; Cosset, J.M.; Malaise, E.P. Blood lymphocyte subsets after the first fraction in patients given hyperfractionated total body irradiation for bone marrow transplantation. Br. J. Cancer. 1991, 63, 646–647. [Google Scholar] [CrossRef][Green Version]
- Tang, C.; Liao, Z.; Gomez, D.; Levy, L.; Zhuang, Y.; Gebremichael, R.A.; Hong, D.S.; Komaki, R.; Welsh, J.W. Lymphopenia association with gross tumor volume and lung V5 and its effects on non-small cell lung cancer patient outcomes. Int. J. Radiat. Oncol. Biol. Phys. 2014, 89, 1084–1091. [Google Scholar] [CrossRef]
- Wild, A.T.; Herman, J.M.; Dholakia, A.S.; Moningi, S.; Lu, Y.; Rosati, L.M.; Hacker-Prietz, A.; Assadi, R.K.; Saeed, A.M.; Pawlik, T.M.; et al. Lymphocyte-sparing effect of stereotactic body radiation therapy in patients with unresectable pancreatic cancer. Int. J. Radiat. Oncol. Biol. Phys. 2016, 94, 571–579. [Google Scholar] [CrossRef]
- Belka, C.; Ottinger, H.; Kreuzfelder, E.; Weinmann, M.; Lindemann, M.; Lepple-Wienhues, A.; Budach, W.; Grosse-Wilde, H.; Bamberg, M. Impact of localized radiotherapy on blood immune cells counts and function in humans. Radiother. Oncol. 1999, 50, 199–204. [Google Scholar] [CrossRef]
- Buescher, E.S.; Gallin, J.I. Radiation effects on cultured human monocytes and on monocyte-derived macrophages. Blood 1984, 63, 1402–1407. [Google Scholar] [CrossRef] [PubMed]
- Greenberg, M.L.; Chanana, A.D.; Cronkite, E.P.; Schiffer, L.M.; Stryckmans, P.A. Extracorporeal irradiation of blood in man: Radiation resistance of circulating platelets. Radiat. Res. 1968, 35, 147–154. [Google Scholar] [CrossRef] [PubMed]
- Duguid, J.K.; Carr, R.; Jenkins, J.A.; Hutton, J.L.; Lucas, G.F.; Davies, J.M. Clinical evaluation of the effects of storage time and irradiation on transfused platelets. Vox Sang. 1991, 60, 151–154. [Google Scholar] [CrossRef] [PubMed]
- Rock, G.; Adams, G.A.; Labow, R.S. The effects of irradiation on platelet function. Transfusion 1988, 28, 451–455. [Google Scholar] [CrossRef] [PubMed]
- Moroff, G.; George, V.M.; Siegl, A.M.; Luban, N.L. The influence of irradiation on stored platelets. Transfusion 1986, 26, 453–456. [Google Scholar] [CrossRef]
- Bahtiyar, N.; Onaran, İ.; Aydemir, B.; Baykara, O.; Toplan, S.; Agaoglu, F.Y.; Akyolcu, M.C. Monitoring of platelet function parameters and microRNA expression levels in patients with prostate cancer treated with volumetric modulated arc radiotherapy. Oncol Lett. 2018, 16, 4745–4753. [Google Scholar] [CrossRef]
| Baseline Mean (SD) | EOT Mean (SD) | Percent Change from Baseline (SD) | 3-Month Mean (SD) | Percentage Change from Baseline (SD) | p Value | Final Mean (SD) | Change from Baseline (SD) | p Value | |
|---|---|---|---|---|---|---|---|---|---|
| Hgb | 13.95 (1.32) | 12.96 (1.33) | −7.1% (6.32) | 13.24 (1.34) | −4.9% (7.17) | <0.0001 | 13.36 (1.51) | −4.0% (9.55) | <0.0001 |
| RBC | 4.65 (0.46) | 4.26 (0.50) | −8.6% (6.56) | 4.35 (0.47) | −6.6% (7.07) | <0.0001 | 4.44 (0.51) | −4.6% (8.94) | <0.0001 |
| WBC | 6.91 (1.91) | 4.89 (1.50) | −27.6% (18.82) | 5.20 (1.55) | −22.7% (18.32) | <0.0001 | 5.86 (1.70) | −12.4% (24.33) | <0.0001 |
| Granulocytes | 4.03 (1.52) | 3.37 (1.24) | −12.2% (30.93) | 3.43 (1.32) | −10.2% (29.74) | <0.0001 | 3.83 (1.47) | +1.4% (42.60) | 0.1236 |
| Eosinophils | 0.23 (0.19) | 0.21 (0.18) | +12.7% (98.66) | 0.21 (0.14) | +15.2% (118.22) | 0.2289 | 0.21 (0.20) | +15.7% (143.54) | 0.1169 |
| Basophils | 0.04 (0.03) | 0.03 (0.03) | −21.4% (61.74) | 0.03 (0.03) | −7.4% (79.12) | 0.0004 | 0.04 (0.03) | +28.4% (144.33) | 0.0263 |
| Neutrophils | 3.76 (1.51) | 3.13 (1.25) | −11.2% (41.24) | 3.18 (1.32) | −9.7% (33.89) | <0.0001 | 3.58 (1.47) | +3.85% (53.74) | 0.2711 |
| Lymphocytes | 2.01 (0.76) | 0.72 (0.35) | −62.5% (15.95) | 1.00 (0.44) | −48.8% (17.05) | <0.0001 | 1.18 (0.48) | −38.2% (24.27) | <0.0001 |
| Monocytes | 0.62 (0.21) | 0.57 (0.20) | −2.2% (33.97) | 0.54 (0.18) | −9.6% (29.23) | <0.0001 | 0.59 (0.20) | +1.4% (37.16) | 0.1453 |
| Platelets | 218.20 (51.30) | 188.95 (48.18) | −12.7% (16.99) | 202.50 (46.18) | −6.2% (14.91) | <0.0001 | 214.29 (57.09) | −0.1% (22.39) | 0.1336 |
| Parameter | Normal Range | % in Normal Range | % in Normal * Range End of Treatment | % Normal * Range 3 Months | % Normal * Range Final |
|---|---|---|---|---|---|
| Hemoglobin | 14–18 g/dL | 49% | 41% | 57% | 59% |
| Red blood cell count | 4.7–6.1 × 1012/L | 45% | 38% | 41% | 52% |
| WBC | 4–8–10.8 × 109/L | 85% | 53% | 67% | 79% |
| Granulocyte | 1.92–8.64 × 109/L | 95% | 92% | 93% | 95% |
| Lymphocyte | 0.72–4.32 × 109/L | 98% | 40% | 72% | 86% |
| Monocyte | 0–1.08 × 109/L | 96% | 99% | 99% | 98% |
| Eosinophils | 0–0.76 × 109/L | 98% | 99% | 99% | 99% |
| Basophils | 0–0.22 × 109/L | 100% | 100% | 100% | 100% |
| Platelets | 150–450 × 109/L | 94% | 85% | 93% | 92% |
| Pelvis/Lymphatic (Pelvic Bone) | Small Prostate/Fossa | |||||
|---|---|---|---|---|---|---|
| Gy | cc (SD) | Mean (%) (SD) | Median (%) (IQR) | cc | Mean (%) (SD) | Median (%) (IQR) |
| V10 | 1170 (333) | 70 (18) | 77 (69, 81) | 887 (274) | 53 (15) | 58 (52, 62) |
| V20 | 919 (320) | 55 (18) | 61 (56, 66) | 531 (206) | 32 (11) | 34 (30, 39) |
| V30 | 625 (253) | 37 (14) | 42 (37, 46) | 280 (123) | 17 (7) | 18 (14, 21) |
| V40 | 359 (167) | 22 (10) | 24 (19, 27) | 164 (73) | 10 (4) | 11 (8, 12) |
| V50 | 178 (86) | 11 (5) | 12 (8, 14) | 103 (46) | 6 (3) | 7 (5, 8) |
| V60 | 25 (19) | 2 (1) | 1 (1, 2) | 25 (12) | 2 (1) | 1 (1, 2) |
| V70 | 6 (9) | 0 (1) | 0 (0, 1) | 48 (8) | 3 (1) | 1 (0, 1) |
| Large Field | Baseline Mean (SD) | EOT Mean (SD) | Change from Baseline (SD) | p-Value | 3 Month Mean (SD) | Change from Baseline (SD) | p-Value | Final Mean (SD) | Change from Baseline (SD) | p-Value |
|---|---|---|---|---|---|---|---|---|---|---|
| Hgb | 13.96 (1.29) | 12.87 (1.31) | −7.8% (7.3) | <0.0001 | 13.18 (1.38) | −5.3% (7.2) | <0.0001 | 13.31 (1.58) | −4.5% (9.7) | <0.0001 |
| RBC | 4.65 (0.46) | 4.22 (0.50) | −9.5% (6.4) | <0.0001 | 4.31 (0.48) | −7.4% (7.0) | <0.0001 | 4.42 (0.53) | −5.1% (9.0) | <0.0001 |
| WBC | 6.86 (1.92) | 4.71 (1.44) | −29.7% (18.3) | <0.0001 | 5.08 (1.57) | −23.9% (18.5) | <0.0001 | 5.74 (1.69) | −13.3% (24.6) | <0.0001 |
| Granulocytes | 4.01 (1.55) | 3.28 (1.25) | −14.1% (31.1) | <0.0001 | 3.39 (1.37) | −10.5% (30.9) | <0.0001 | 3.77 (1.48) | +1.2% (44.2) | 0.1092 |
| Eosinophils | 0.22 (0.16) | 0.21 (0.18) | −12.8% (203.3) | 0.3297 | 0.20 (0.13) | +17.8% (127.8) | 0.1843 | 0.20 (0.21) | +18.3% (155.0) | 0.1261 |
| Basophils | 0.04 (0.03) | 0.02 (0.03) | −23.2% (61.4) | <0.0001 | 0.03 (0.03) | −7.0% (83.9) | 0.0013 | 0.04 (0.03) | +28.6% (151.8) | 0.0529 |
| Neutrophils | 3.75 (1.53) | 3.05 (1.26) | −13.4% (42.5) | <0.0001 | 3.15 (1.38) | −10.0% (35.4) | <0.0001 | 3.52 (1.48) | +3.6% (55.9) | 0.2111 |
| Lymphocytes | 1.99 (0.76) | 0.64 (0.26) | −65.8% (13.3) | <0.0001 | 0.92 (0.39) | −51.7% (14.8) | <0.0001 | 1.12 (0.44) | −40.1% (24.1) | <0.0001 |
| Monocytes | 0.61 (0.21) | 0.56 (0.20) | −2.7% (35.7) | 0.0023 | 0.53 (0.18) | −9.3% (30.6) | <0.0001 | 0.59 (0.21) | +2.8% (38.9) | 0.3535 |
| Platelets | 218.13 (51.25) | 185.42 (46.51) | −14.2% (17.3) | <0.0001 | 201.47 (44.32) | −6.6% (15.9) | <0.0001 | 214.44 (57.30) | +0.1% (24.0) | 0.1590 |
| Small field | ||||||||||
| Hgb | 13.90 (1.44) | 13.40 (1.35) | −3.8% (5.4) | <0.0001 | 13.56 (1.10) | −2.5% (6.6) | <0.0001 | 13.65 (1.13) | −1.4% (8.4) | 0.0413 |
| RBC | 4.63 (0.47) | 4.45 (.49) | −4.0% (5.3) | <0.0001 | 4.51 (0.41) | −3.0% (6.1) | <0.0001 | 4.53 (0.40) | -2.0% (8.4) | 0.0092 |
| WBC | 7.16 (1.82) | 5.79 (1.45) | −17.0% (18.1) | <0.0001 | 5.79 (1.31) | −16.7% (16.6) | <0.0001 | 6.44 (1.65) | −7.9% (22.4) | 0.0163 |
| Granulocytes | 4.13 (1.42) | 3.78 (1.13) | −2.6% (28.2) | 0.3877 | 3.60 (1.00) | −8.9% (22.8) | 0.0085 | 4.13 (1.41) | +2.3% (33.5) | 0.9786 |
| Eosinophils | 0.28 (0.30) | 0.24 (0.15) | +12.6% (71.1) | 0.7849 | 0.23 (0.15) | +1.2% (38.6) | 0.8001 | 0.22 (0.16) | +2.6% (55.9) | 0.8364 |
| Basophils | 0.04 (0.02) | 0.03 (0.02) | −11.9% (63.6) | 0.1225 | 0.03 (0.02) | −9.3% (46.7) | 0.1670 | 0.04 (0.02) | +27.7% (98.3) | 0.2338 |
| Neutrophils | 3.81 (1.44) | 3.52 (1.10) | −0.2% (32.0) | 0.6851 | 3.34 (0.99) | −7.9% (24.9) | 0.0329 | 3.86 (1.40) | +5.4% (41.2) | 0.9059 |
| Lymphocytes | 2.14 (0.73) | 1.13 (0.44) | −45.3% (17.6) | <0.0001 | 1.39 (0.51) | −33.3% (19.9) | <0.0001 | 1.47 (0.57) | −28.4% (22.8) | <0.0001 |
| Monocytes | 0.65 (0.20) | 0.62 (0.17) | +0.3% (24.5) | 0.8454 | 0.57 (0.18) | −10.9% (20.6) | 0.0004 | 0.60 (0.19) | −5.6% (25.8) | 0.1323 |
| Platelets | 218.56 (52.11) | 206.46 (52.86) | −5.0% (13.0) | 0.0003 | 207.44 (54.53) | −4.2% (8.32) | 0.0024 | 213.57 (56.6) | -1.0% (11.9) | 0.7657 |
| Patients Starting in Normal Range | Small Field | Large Field | Small vs. Large Field p-Values | |||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Small Field | Large Field | Below Normal End of Treatment | Below Normal at 3 Months | Below Normal at Follow Up | Below Normal End of Treatment | Below Normal at 3 Months | Below Normal at Follow Up | At Baseline | Below Normal End of Treatment | Below Normal at 3 Months | Below Normal at Follow Up | |
| 52% | 49% | Hgb | 33% | 25% | 36% | 64% | 46% | 42% | 0.6755 | 0.0055 | 0.0551 | 0.5566 |
| 42% | 45% | RBC | 37% | 32% | 30% | 67% | 64% | 51% | 0.5918 | 0.0125 | 0.0078 | 0.0850 |
| 88% | 85% | WBC | 27% | 18% | 14% | 51% | 36% | 22% | 0.1020 | 0.0185 | 0.0294 | 0.3275 |
| 98% | 94% | Granulocytes | 0% | 5% | 4% | 10% | 7% | 5% | 0.6727 | 0.0476 | 0.5336 | 1.0000 |
| 98% | 98% | Eosinophils | 0% | 0% | 0% | 1% | 1% | 17% | 0.8135 | 0.4432 | 0.5378 | 0.6326 |
| 100% | 100% | Basophils | 0% | 0% | 0% | 0% | 0% | 3% | na | 0.6584 | 0.6642 | 0.6596 |
| 98% | 98% | Lymphocytes | 11% | 2% | 2% | 69% | 33% | 1% | 0.4521 | <0.0001 | <0.0001 | 0.0116 |
| 96% | 96% | Monocytes | 2% | 0% | 0% | 0% | 1% | 3% | 0.8520 | 0.1996 | 0.5360 | 0.2776 |
| 96% | 94% | Platelets | 7% | 5% | 11% | 16% | 8% | 7% | 0.6001 | 0.1033 | 0.4556 | 0.2864 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Swanson, G.P.; Hammonds, K.; Jhavar, S. Reference Results for Blood Parameter Changes and Recovery after Pelvic Radiation without Chemotherapy. Hematol. Rep. 2022, 14, 155-164. https://doi.org/10.3390/hematolrep14020023
Swanson GP, Hammonds K, Jhavar S. Reference Results for Blood Parameter Changes and Recovery after Pelvic Radiation without Chemotherapy. Hematology Reports. 2022; 14(2):155-164. https://doi.org/10.3390/hematolrep14020023
Chicago/Turabian StyleSwanson, Gregory P., Kendall Hammonds, and Sameer Jhavar. 2022. "Reference Results for Blood Parameter Changes and Recovery after Pelvic Radiation without Chemotherapy" Hematology Reports 14, no. 2: 155-164. https://doi.org/10.3390/hematolrep14020023
APA StyleSwanson, G. P., Hammonds, K., & Jhavar, S. (2022). Reference Results for Blood Parameter Changes and Recovery after Pelvic Radiation without Chemotherapy. Hematology Reports, 14(2), 155-164. https://doi.org/10.3390/hematolrep14020023






