Angioedema and COVID-19: A New Dermatological Manifestation?
Abstract
1. Introduction
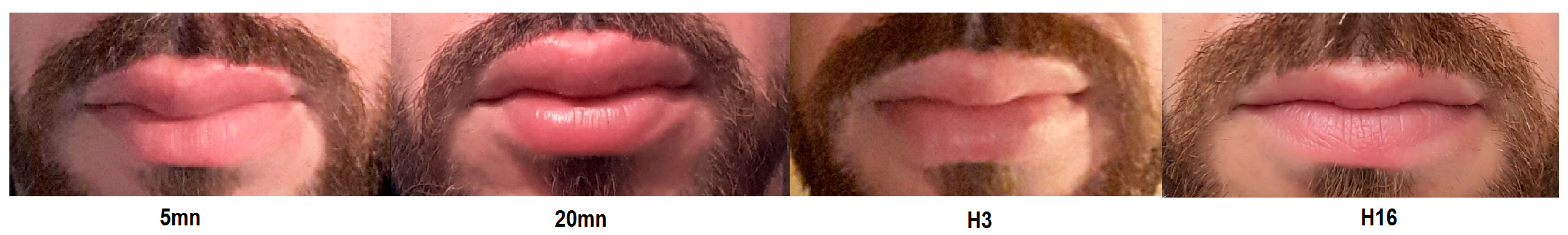
2. Case Report
3. Discussion
4. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Li, X.-Y.; Dai, W.-J.; Wu, S.-N.; Yang, X.-Z.; Wang, H.-G. The occurrence of diarrhea in COVID-19 patients. Clin. Res. Hepatol. Gastroenterol. 2020, 44, 284–285. [Google Scholar] [CrossRef] [PubMed]
- Lechien, J.R.; Chiesa-Estomba, C.M.; De Siati, D.R.; Horoi, M.; Le Bon, S.D.; Rodriguez, A.; Dequanter, D.; Blecic, S.; El Afia, F.; Distinguin, L.; et al. Olfactory and gustatory dysfunctions as a clinical presentation of mild-to-moderate forms of the coronavirus disease (COVID-19): A multicenter European study. Eur. Arch. Oto-Rhino-Laryngol. 2020, 277, 2251–2261. [Google Scholar] [CrossRef] [PubMed]
- Corrales, A.E.; Pérez-Santiago, L.; Silva, E.; Guillen-Climent, S.; García-Vázquez, A.; Ramón, M.D. Cutaneous manifestations in COVID-19: A new contribution. J. Eur. Acad. Dermatol. Venereol. 2020, 34. [Google Scholar] [CrossRef]
- Casas, C.G.; Català, A.; Hernández, G.C.; Rodríguez-Jiménez, P.; Fernández-Nieto, D.; Lario, A.R.; Fernández, I.N.; Ruiz-Villaverde, R.; Falkenhain-López, D.; Velasco, M.L.; et al. Classification of the cutaneous manifestations of COVID-19: A rapid prospective nationwide consensus study in Spain with 375 cases. Br. J. Dermatol. 2020, 183, 71–77. [Google Scholar] [CrossRef] [PubMed]
- Barbarot, S.; Doutre, M.S.; Kluger, N.; Martin, L.; Meunier, L.; Penso-Assathiany, D.; Petit, A.; Prigent, F.; Revuz, J.; Senet, P. Annales de Dermatologie et de Vénéréologie; Elsevier Masson: Issy-les-Moulineaux, France, 2005; Volume 132, pp. 71–76. [Google Scholar]
- Imbalzano, E.; Casciaro, M.; Quartuccio, S.; Minciullo, P.L.; Cascio, A.; Calapai, G.; Gangemi, S. Association between urticaria and virus infections: A systematic review. Allergy Asthma Proc. 2016, 37, 18–22. [Google Scholar] [CrossRef] [PubMed]
- Recalcati, S. Cutaneous manifestations in COVID-19: A first perspective. J. Eur. Acad. Dermatol. Venereol. 2020, 34. [Google Scholar] [CrossRef] [PubMed]
- Henry, D.; Ackerman, M.; Sancelme, E.; Finon, A.; Esteve, E. Urticarial eruption in COVID-19 infection. J. Eur. Acad. Dermatol. Venereol. 2020, 34. [Google Scholar] [CrossRef] [PubMed]
- Zhang, Y.; Cao, W.; Xiao, M.; Li, Y.J.; Yang, Y.; Zhao, J.; Zhou, X.; Jiang, W.; Zhao, Y.Q.; Zhang, S.Y.; et al. Clinical and coagulation characteristics of 7 patients with critical COVID-2019 pneumonia and acro-ischemia. Zhonghua Xue Ye Xue Za Zhi=Zhonghua Xueyexue Zazhi 2020, 41, E006. [Google Scholar] [PubMed]
- Zhang, C.; Wu, Z.; Li, J.-W.; Zhao, H.; Wang, G.-Q. Cytokine release syndrome in severe COVID-19: Interleukin-6 receptor antagonist tocilizumab may be the key to reduce mortality. Int. J. Antimicrob. Agents 2020, 55, 105954. [Google Scholar] [CrossRef] [PubMed]
- Sarzi-Puttini, P.; Giorgi, V.; Sirotti, S.; Marotto, D.; Ardizzone, S.; Rizzardini, G.; Antinori, S.; Galli, M. COVID-19, cytokines and immunosuppression: What can we learn from severe acute respiratory syndrome? Clin. Exp. Rheumatol. 2020, 38, 337–342. [Google Scholar] [PubMed]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Royer, P.-Y.; Zayet, S.; Jacquin-Porretaz, C.; Kadiane-Oussou, N.J.; Toko, L.; Gendrin, V.; Klopfenstein, T. Angioedema and COVID-19: A New Dermatological Manifestation? Infect. Dis. Rep. 2021, 13, 23-25. https://doi.org/10.3390/idr13010004
Royer P-Y, Zayet S, Jacquin-Porretaz C, Kadiane-Oussou NJ, Toko L, Gendrin V, Klopfenstein T. Angioedema and COVID-19: A New Dermatological Manifestation? Infectious Disease Reports. 2021; 13(1):23-25. https://doi.org/10.3390/idr13010004
Chicago/Turabian StyleRoyer, Pierre-Yves, Souheil Zayet, Claire Jacquin-Porretaz, N’dri Juliette Kadiane-Oussou, Lynda Toko, Vincent Gendrin, and Timothée Klopfenstein. 2021. "Angioedema and COVID-19: A New Dermatological Manifestation?" Infectious Disease Reports 13, no. 1: 23-25. https://doi.org/10.3390/idr13010004
APA StyleRoyer, P.-Y., Zayet, S., Jacquin-Porretaz, C., Kadiane-Oussou, N. J., Toko, L., Gendrin, V., & Klopfenstein, T. (2021). Angioedema and COVID-19: A New Dermatological Manifestation? Infectious Disease Reports, 13(1), 23-25. https://doi.org/10.3390/idr13010004





