Cardiac Involvement in Autosomal Dominant Polycystic Kidney Disease
Abstract
1. Epidemiology, Genetics and Pathogenetsis
1.1. Kidney Polycystic Disease
1.2. Arterial Hypertension
1.3. Vascular Abnormalities
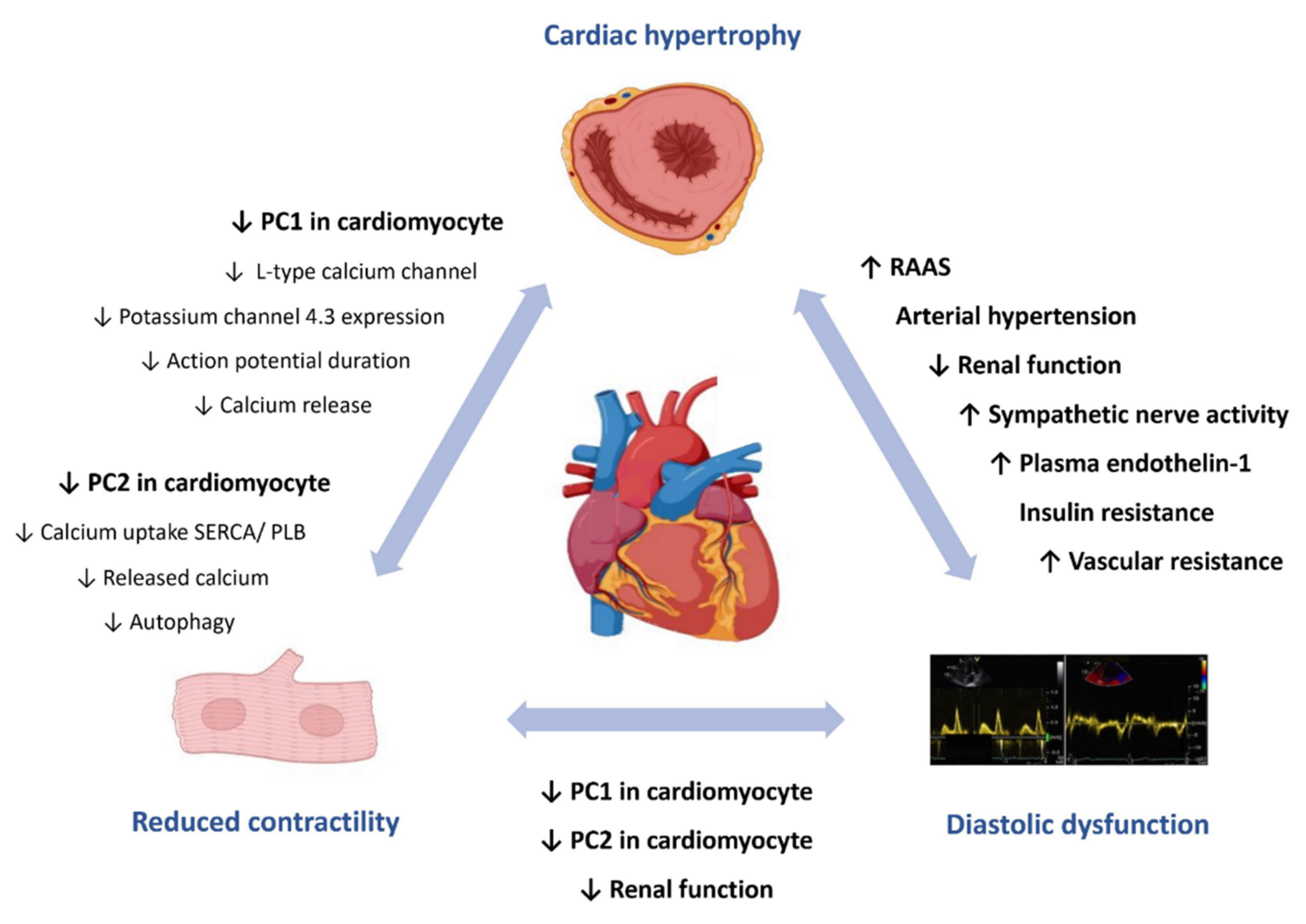
1.4. The Heart in ADPKD
2. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Torres, V.E.; Harris, P.C.; Pirson, Y. Autosomal dominant polycystic kidney disease. Lancet 2007, 369, 1287–1301. [Google Scholar] [CrossRef]
- Bergmann, C.; Guay-Woodford, L.M.; Harris, P.C.; Horie, S.; Peters, D.J.M.; Torres, V.E. Polycystic kidney disease. Nat. Rev. Dis. Primers 2018, 4, 50. [Google Scholar] [CrossRef]
- Schrier, R.W.; Mcfann, K.K.; Johnson, A.M. Epidemiological study of kidney survival in autosomal dominant polycystic kidney disease. Kidney Int. 2003, 63, 678–685. [Google Scholar] [CrossRef] [PubMed]
- Willey, C.J.; Blais, J.D.; Hall, A.K.; Krasa, H.B.; Makin, A.J.; Czerwiec, F.S. Prevalence of autosomal dominant polycystic kidney disease in the European Union. Nephrol. Dial. Transplant. 2017, 32, 1356–1363. [Google Scholar] [CrossRef] [PubMed]
- Willey, C.; Kamat, S.; Stellhorn, R.; Blais, J. Analysis of nationwide data to determine the incidence and diagnosed prevalence of autosomal dominant polycystic kidney disease in the USA: 2013–2015. Kidney Dis. 2019, 5, 107–117. [Google Scholar] [CrossRef] [PubMed]
- Kimberling, W.J.; Fain, P.R.; Kenyon, J.B.; Goldgar, D.; Sujansky, E.; Gabow, P.A. Linkage heterogeneity of autosomal dominant polycystic kidney disease. N. Engl. J. Med. 1988, 319, 913–918. [Google Scholar] [CrossRef]
- Ward, C.J.; Turley, H.; Ong, A.C.; Comley, M.; Biddolph, S.; Chetty, R.; Ratcliffe, P.J.; Gattner, K.; Harris, P.C. Polycystin, the polycystic kidney disease 1 protein, is expressed by epithelial cells in fetal, adult, and polycystic kidney. Proc. Natl. Acad. Sci. USA 1996, 93, 1524–1528. [Google Scholar] [CrossRef] [PubMed]
- Ibraghimov-Beskrovnaya, O.; Dackowski, W.R.; Foggensteiner, L.; Coleman, N.; Thiru, S.; Petry, L.R.; Burn, T.C.; Connors, T.D.; van Raay, T.; Bradley, J.; et al. Polycystin: In vitro synthesis, in vivo tissue expression, and subcellular localization identifies a large membrane-associated protein. Proc. Natl. Acad. Sci. USA 1997, 94, 6397–6402. [Google Scholar] [CrossRef]
- Peters, D.J.; Spruit, L.; Saris, J.J.; Ravine, D.; Sandkuijl, L.A.; Fossdal, R.; van Eijk, R.; Norby, S.; Constantinou-Deltas, C.D.; Pierides, A.; et al. Chromosome 4 localization of a second gene for autosomal dominant polycystic kidney disease. Nat. Genet. 1993, 5, 359–362. [Google Scholar] [CrossRef] [PubMed]
- Mochizuki, T.; Wu, G.; Hayashi, T.; Xenophontos, S.L.; Veldhuisen, B.; Saris, J.J.; Reynolds, D.M.; Cai, Y.; Gabow, P.A.; Pierides, A.; et al. PKD2, a gene for polycystic kidney disease that encodes an integral membrane protein. Science 1996, 272, 1339–1342. [Google Scholar] [CrossRef]
- Calvet, J.P.; Grantham, J.J. The genetics and physiology of polycystic kidney disease. Semin. Nephrol. 2001, 21, 107–123. [Google Scholar] [CrossRef]
- Grantham, J.J. Polycystic kidney disease: From the bedside to the gene and back. Curr. Opin. Nephrol. Hypertens. 2001, 10, 533–542. [Google Scholar] [CrossRef] [PubMed]
- Cornec-Le Gall, E.; Torres, V.E.; Harris, P.C. Genetic complexity of autosomal dominant polycystic kidney and liver diseases. J. Am. Soc. Nephrol. 2018, 29, 13–23. [Google Scholar] [CrossRef]
- Fedeles, S.V.; Tian, X.; Gallagher, A.R.; Mitobe, M.; Nishio, S.; Lee, S.H.; Cai, Y.; Geng, L.; Crews, C.M.; Somlo, S.A. Genetic interaction network of five genes for human polycystic kidney and liver diseases defines polycystin-1 as the central determinant of cyst formation. Nat. Genet. 2011, 43, 639–647. [Google Scholar] [CrossRef] [PubMed]
- Qian, F.; Germino, F.J.; Cai, Y.; Zhang, X.; Somlo, S.; Germino, G.G. PKD1 interacts with PKD2 through a probable coiled-coil domain. Nat. Genet. 1997, 16, 179–183. [Google Scholar] [CrossRef]
- Tsiokas, L.; Kim, E.; Arnould, T.; Sukhatme, V.P.; Walz, G. Homo- and heterodimeric interactions between the gene products of PKD1 and PKD2. Proc. Natl. Acad. Sci. USA 1997, 94, 6965–6970. [Google Scholar] [CrossRef] [PubMed]
- Hanaoka, K.; Qian, F.; Boletta, A.; Bhunia, A.K.; Piontek, K.; Tsiokas, L.; Sukhatme, V.P.; Guggino, W.B.; Germino, G.G. Co-assembly of polycystin-1 and -2 produces unique cation-permeable currents. Nature 2000, 408, 990–994. [Google Scholar] [CrossRef]
- Chauvet, V.; Tian, X.; Husson, H.; Grimm, D.H.; Wang, T.; Hiesberger, T.; Igarashi, P.; Bennett, A.M.; Ibraghimov-Beskrovnaya, O.; Somlo, S.; et al. Mechanical stimuli induce cleavage and nuclear translocation of the polycystin–1 C terminus. J. Clin. Investig. 2004, 114, 1433–1443. [Google Scholar] [CrossRef]
- Low, S.H.; Vasanth, S.; Larson, C.H.; Mukherjee, S.; Sharma, N.; Kinter, M.T.; Kane, M.E.; Obara, T.; Weimbs, T. Polycystin-1, STAT6, and P100 function in a pathway that transduces ciliary mechanosensation and is activated in polycystic kidney disease. Dev. Cell 2006, 10, 57–69. [Google Scholar] [CrossRef]
- Harris, P.C.; Torres, V.E. Genetic mechanisms and signaling pathways in autosomal dominant polycystic kidney disease (ADPKD). J. Clin. Investig. 2014, 124, 2315–2324. [Google Scholar] [CrossRef]
- Wallace, D.P. Cyclic AMP-mediated cyst expansion. Biochim. Biophys. Acta 2011, 1812, 1291–1300. [Google Scholar] [CrossRef] [PubMed]
- Mekahli, D.; Parys, J.B.; Bultynck, G.; Missiaen, L.; de Smedt, H. Polycystins and cellular Ca2+ signaling. Cell. Mol. Life Sci. 2013, 70, 2697–2712. [Google Scholar] [CrossRef] [PubMed]
- Rossetti, S.; Kubly, V.J.; Consugar, M.B.; Hopp, K.; Roy, S.; Horsley, S.W.; Chauveau, D.; Rees, L.; Barratt, T.M.; van’t Hoff, W.G.; et al. Incompletely penetrant PKD1 alleles suggest a role for gene dosage in cyst initiation in polycystic kidney disease. Kidney Int. 2009, 75, 848–855. [Google Scholar] [CrossRef]
- Chapin, H.C.; Caplan, M.J. The cell biology of polycystic kidney disease. J. Cell Biol. 2010, 191, 701–710. [Google Scholar] [CrossRef] [PubMed]
- Hateboer, N.; V Dijk, M.A.; Bogdanova, N.; Coto, E.; Saggar-Malik, A.K.; San Millan, J.L.; Torra, R.; Breuning, M.; Ravine, D. Comparison of phenotypes of polycystic kidney disease types 1 and 2. European PKD1–PKD2 study group. Lancet 1999, 353, 103–107. [Google Scholar] [CrossRef]
- Audrézet, M.P.; Cornec-Le Gall, E.; Chen, J.M.; Redon, S.; Quéré, I.; Creff, J.; Bénech, C.; Maestri, S.; Le Meur, Y.; Férec, C. Autosomal dominant polycystic kidney disease: Comprehensive mutation analysis of PKD1 and PKD2 in 700 unrelated patients. Hum. Mutat. 2012, 33, 1239–1250. [Google Scholar] [CrossRef]
- Heyer, C.M.; Sundsbak, J.L.; Abebe, K.Z.; Chapman, A.B.; Torres, V.E.; Grantham, J.J.; Bae, K.T.; Schrier, R.W.; Perrone, R.D.; Braun, W.E.; et al. Predicted mutation strength of nontruncating PKD1 mutations aids genotype-phenotype correlations in autosomal dominant polycystic kidney disease. J. Am. Soc. Nephrol. 2016, 27, 2872–2884. [Google Scholar] [CrossRef]
- MacDermot, K.D.; Saggar-Malik, A.K.; Economides, D.L. Prenatal diagnosis of autosomal dominant polycystic kidney disease (PKD1) presenting in utero and prognosis for very early onset disease. J. Med. Genet. 1998, 35, 13–16. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Igarashi, P.; Somlo, S. Genetics and pathogenesis of polycystic kidney disease. J. Am. Soc. Nephrol. 2002, 13, 2384–2398. [Google Scholar] [CrossRef]
- Wilson, P.D. Polycystic kidney disease. N. Engl. J. Med. 2004, 350, 151–164. [Google Scholar] [CrossRef] [PubMed]
- Grantham, J.J. Clinical practice. Autosomal dominant polycystic kidney disease. N. Engl. J. Med. 2008, 359, 1477–1485. [Google Scholar] [CrossRef] [PubMed]
- Zerres, K.; Rudnik-Schöneborn, S.; Deget, F. Childhood onset autosomal dominant polycystic kidney disease in sibs: Clinical picture and recurrence risk. German working group on paediatric nephrology (arbeitsgemeinschaft für pädiatrische nephrology). J. Med. Genet. 1993, 30, 583–588. [Google Scholar] [CrossRef] [PubMed]
- Shamshirsaz, A.A.; Reza Bekheirnia, M.; Kamgar, M.; Johnson, A.M.; McFann, K.; Cadnapaphornchai, M.; Nobakhthaghighi, N.; Schrier, R.W. Autosomal-dominant polycystic kidney disease in infancy and childhood: Progression and outcome. Kidney Int. 2005, 68, 2218–2224. [Google Scholar] [CrossRef] [PubMed]
- Gattone, V.H.; Wang, X.; Harris, P.C.; Torres, V.E. Inhibition of renal cystic disease development and progression by a vasopressin V2 receptor antagonist. Nat. Med. 2003, 9, 1323–1326. [Google Scholar] [CrossRef] [PubMed]
- Torres, V.E.; Wang, X.; Qian, Q.; Somlo, S.; Harris, P.C.; Gattone, V.H. Effective treatment of an orthologous model of autosomal dominant polycystic kidney disease. Nat. Med. 2004, 10, 363–364. [Google Scholar] [CrossRef]
- Nagao, S.; Nishii, K.; Katsuyama, M.; Kurahashi, H.; Marunouchi, T.; Takahashi, H.; Wallace, D.P. Increased water intake decreases progression of polycystic kidney disease in the PCK rat. J. Am. Soc. Nephrol. 2006, 17, 228–235. [Google Scholar] [CrossRef]
- Wong, H.; Vivian, L.; Weiler, G.; Filler, G. Patients with autosomal dominant polycystic kidney disease hyperfiltrate early in their disease. Am. J. Kidney Dis. 2004, 43, 624–628. [Google Scholar] [CrossRef]
- Chapman, A.B.; Johnson, A.; Gabow, P.A.; Schrier, R.W. The renin-angiotensin-aldosterone system and autosomal dominant polycystic kidney disease. N. Engl. J. Med. 1990, 323, 1091–1096. [Google Scholar] [CrossRef]
- Torres, V.E.; Wilson, D.M.; Burnett, J.C.J.; Johnson, C.M.; Offord, K.P. Effect of inhibition of converting enzyme on renal hemodynamics and sodium management in polycystic kidney disease. Mayo Clin. Proc. 1991, 66, 1010–1017. [Google Scholar] [CrossRef]
- Watson, M.; Macnicol, A.; Allan, P.; Wright, A. Effects of angiotensin-converting enzyme inhibition in adult polycystic kidney disease. Kidney Int. 1992, 41, 206–210. [Google Scholar] [CrossRef][Green Version]
- Harris, P.C.; Bae, K.T.; Rossetti, S.; Torres, V.E.; Grantham, J.J.; Chapman, A.B.; Guay-Woodford, L.M.; King, B.F.; Wetzel, L.H.; Baumgarten, D.A.; et al. Cyst number but not the rate of cystic growth is associated with the mutated gene in autosomal dominant polycystic kidney disease. J. Am. Soc. Nephrol. 2006, 17, 3013–3019. [Google Scholar] [CrossRef] [PubMed]
- Helal, I.; Reed, B.; Mettler, P.; Mc Fann, K.; Tkachenko, O.; Yan, X.D.; Schrier, R.W. Prevalence of cardiovascular events in patients with autosomal dominant polycystic kidney disease. Am. J. Nephrol. 2012, 36, 362–370. [Google Scholar] [CrossRef]
- Kelleher, C.L.; McFann, K.K.; Johnson, A.M.; Schrier, R.W. Characteristics of hypertension in young adults with autosomal dominant polycystic kidney disease compared with the general US population. Am. J. Hypertens. 2004, 17, 1029–1034. [Google Scholar] [CrossRef] [PubMed]
- Seeman, T.; Dusek, J.; Vondrák, K.; Bláhová, K.; Simková, E.; Kreisinger, J.; Dvorák, P.; Kyncl, M.; Hríbal, Z.; Janda, J. Renal concentrating capacity is linked to blood pressure in children with autosomal dominant polycystic kidney disease. Physiol. Res. 2004, 53, 629–634. [Google Scholar]
- Schrier, R.W. Hypertension and autosomal dominant polycystic kidney disease. Am. J. Kidney Dis. 2011, 57, 811–813. [Google Scholar] [CrossRef] [PubMed]
- Harrap, S.B.; Davies, D.L.; Macnicol, A.M.; Dominiczak, A.F.; Fraser, R.; Wright, A.F.; Watson, M.L.; Briggs, J.D. Renal, cardiovascular and hormonal characteristics of young adults with autosomal dominant polycystic kidney disease. Kidney Int. 1991, 40, 501–508. [Google Scholar] [CrossRef]
- Rahbari-Oskoui, F.; Williams, O.; Chapman, A. Mechanisms and management of hypertension in autosomal dominant polycystic kidney disease. Nephrol. Dial. Transplant. 2014, 29, 2194–2201. [Google Scholar] [CrossRef]
- Perrone, R.D.; Abebe, K.Z.; Schrier, R.W.; Chapman, A.B.; Torres, V.E.; Bost, J.; Kaya, D.; Miskulin, D.C.; Steinman, T.I.; Braun, W.; et al. Cardiac magnetic resonance assessment of left ventricular mass in autosomal dominant polycystic kidney disease. Clin. J. Am. Soc. Nephrol. 2011, 6, 2508–2515. [Google Scholar] [CrossRef] [PubMed]
- Schrier, R.W.; Abebe, K.Z.; Perrone, R.D.; Torres, V.E.; Braun, W.E.; Steinman, T.I.; Winklhofer, F.T.; Brosnahan, G.; Czarnecki, P.G.; Hogan, M.C.; et al. Blood pressure in early autosomal dominant polycystic kidney disease. N. Engl. J. Med. 2014, 371, 2255–2266. [Google Scholar] [CrossRef]
- Torres, V.E.; Abebe, K.Z.; Chapman, A.B.; Schrier, R.W.; Braun, W.E.; Steinman, T.I.; Winklhofer, F.T.; Brosnahan, G.; Czarnecki, P.G.; Hogan, M.C.; et al. Angiotensin blockade in late autosomal dominant polycystic kidney disease. N. Engl. J. Med. 2014, 371, 2267–2276. [Google Scholar] [CrossRef]
- Klein, I.H.; Ligtenberg, G.; Oey, P.L.; Koomans, H.A.; Blankestijn, P.J. Sympathetic activity is increased in polycystic kidney disease and associated with hypertension. J. Am. Soc. Nephrol. 2001, 12, 2427–2433. [Google Scholar] [PubMed]
- Merta, M.; Reiterová, J.; Rysavá, R.; Tesar, V.; Závada, J.; Jáchymová, M.; Zima, T. Role of endothelin and nitric oxide in the pathogenesis of arterial hypertension in autosomal dominant polycystic kidney disease. Physiol. Res. 2003, 52, 433–437. [Google Scholar]
- Vareesangthip, K.; Tong, P.; Wilkinson, R.; Thomas, T.H. Insulin resistance in adult polycystic kidney disease. Kidney Int. 1997, 52, 503–508. [Google Scholar] [CrossRef] [PubMed]
- Lumiaho, A.; Pihlajamäki, J.; Hartikainen, J.; Ikäheimo, R.; Miettinen, R.; Niemitukia, L.; Lampainen, E.; Laakso, M. Insulin resistance is related to left ventricular hypertrophy in patients with polycystic kidney disease type 1. Am. J. Kidney Dis. 2003, 41, 1219–1224. [Google Scholar] [CrossRef]
- Zeier, M.; Geberth, S.; Schmidt, K.G.; Mandelbaum, A.; Ritz, E. Elevated blood pressure profile and left ventricular mass in children and young adults with autosomal dominant polycystic kidney disease. J. Am. Soc. Nephrol. 1993, 3, 1451–1457. [Google Scholar]
- Martinez-Vea, A.; Bardaj, A.; Gutierrez, C.; Garca, C.; Peralta, C.; Marcas, L.; Oliver, J.A. Exercise blood pressure, cardiac structure, and diastolic dysfunction in young normotensive patients with polycystic kidney disease: A prehypertensive state. Am. J. Kidney Dis. 2004, 44, 216–223. [Google Scholar] [CrossRef]
- Geng, L.; Segal, Y.; Pavlova, A.; Barros, E.J.; Löhning, C.; Lu, W.; Nigam, S.K.; Frischauf, A.M.; Reeders, S.T.; Zhou, J. Distribution and developmentally regulated expression of murine polycystin. Am. J. Physiol. 1997, 272, F451–F459. [Google Scholar] [CrossRef]
- Markowitz, G.S.; Cai, Y.; Li, L.; Wu, G.; Ward, L.C.; Somlo, S.; D’Agati, V.D. Polycystin-2 expression is developmentally regulated. Am. J. Physiol. 1999, 277, F17–F25. [Google Scholar] [CrossRef]
- Griffin, M.D.; Torres, V.E.; Grande, J.P.; Kumar, R. Vascular expression of polycystin. J. Am. Soc. Nephrol. 1997, 8, 616–626. [Google Scholar] [PubMed]
- Torres, V.E.; Cai, Y.; Chen, X.; Wu, G.Q.; Geng, L.; Cleghorn, K.A.; Johnson, C.M.; Somlo, S. Vascular expression of polycystin 2. J. Am. Soc. Nephrol. 2001, 12, 1–9. [Google Scholar] [PubMed]
- Qian, Q.; Hunter, L.W.; Du, H.; Ren, Q.; Han, Y.; Sieck, G.C. PKD2+/− vascular smooth muscles develop exaggerated vasocontraction in response to phenylephrine stimulation. J. Am. Soc. Nephrol. 2007, 18, 485–493. [Google Scholar] [CrossRef] [PubMed]
- Kip, S.N.; Hunter, L.W.; Ren, Q.; Harris, P.C.; Somlo, S.; Torres, V.E.; Sieck, G.C.; Qian, Q. [Ca2+] i reduction increases cellular proliferation and apoptosis in vascular smooth muscle cells: Relevance to the ADPKD phenotype. Circ. Res. 2005, 96, 873–880. [Google Scholar] [CrossRef]
- Wang, D.; Iversen, J.; Wilcox, C.S.; Strandgaard, S. Endothelial dysfunction and reduced nitric oxide in resistance arteries in autosomal-dominant polycystic kidney disease. Kidney Int. 2003, 64, 1381–1388. [Google Scholar] [CrossRef] [PubMed]
- Bichet, D.; Peters, D.; Patel, A.J.; Delmas, P.; Honoré, E. Cardiovascular polycystins: Insights from autosomal dominant polycystic kidney disease and transgenic animal models. Trends Cardiovasc. Med. 2006, 16, 292–298. [Google Scholar] [CrossRef] [PubMed]
- Liu, D.; Wang, C.J.; Judge, D.P.; Halushka, M.K.; Ni, J.; Habashi, J.P.; Moslehi, J.; Bedja, D.; Gabrielson, K.L.; Xu, H.; et al. A Pkd1-Fbn1 genetic interaction implicates TGF-beta signaling in the pathogenesis of vascular complications in autosomal dominant polycystic kidney disease. J. Am. Soc. Nephrol. 2014, 25, 81–91. [Google Scholar] [CrossRef]
- Boulter, C.; Mulroy, S.; Webb, S.; Fleming, S.; Brindle, K.; Sandford, R. Cardiovascular, skeletal, and renal defects in mice with a targeted disruption of the Pkd1 gene. Proc. Natl. Acad. Sci. USA 2001, 98, 12174–12179. [Google Scholar] [CrossRef]
- Ecder, T.; Schrier, R.W. Cardiovascular abnormalities in autosomal-dominant polycystic kidney disease. Nat. Rev. Nephrol. 2009, 5, 221–228. [Google Scholar] [CrossRef] [PubMed]
- Patel, A.; Honoré, E. Polycystins and renovascular mechanosensory transduction. Nat. Rev. Nephrol. 2010, 6, 530–538. [Google Scholar] [CrossRef] [PubMed]
- Nowak, K.L.; Farmer, H.; Cadnapaphornchai, M.A.; Gitomer, B.; Chonchol, M. Vascular dysfunction in children and young adults with autosomal dominant polycystic kidney disease. Nephrol. Dial. Transplant. 2017, 32, 342–347. [Google Scholar] [CrossRef]
- Sharif-Naeini, R.; Folgering, J.H.; Bichet, D.; Duprat, F.; Lauritzen, I.; Arhatte, M.; Jodar, M.; Dedman, A.; Chatelain, F.C.; Schulte, U.; et al. Polycystin-1 and -2 dosage regulates pressure sensing. Cell 2009, 139, 587–596. [Google Scholar] [CrossRef] [PubMed]
- Clausen, P.; Feldt-Rasmussen, B.; Iversen, J.; Lange, M.; Eidemak, I.; Strandgaard, S. Flow-associated dilatory capacity of the brachial artery is intact in early autosomal dominant polycystic kidney disease. Am. J. Nephrol. 2006, 26, 335–339. [Google Scholar] [CrossRef]
- Kocaman, O.; Oflaz, H.; Yekeler, E.; Dursun, M.; Erdogan, D.; Demirel, S.; Alisir, S.; Turgut, F.; Mercanoglu, F.; Ecder, T. Endothelial dysfunction and increased carotid intima-media thickness in patients with autosomal dominant polycystic kidney disease. Am. J. Kidney Dis. 2004, 43, 854–860. [Google Scholar] [CrossRef] [PubMed]
- Peterson, K.M.; Franchi, F.; Loeffler, D.L.; Psaltis, P.J.; Harris, P.C.; Lerman, L.O.; Lerman, A.; Rodriguez-Porcel, M. Endothelial dysfunction occurs prior to clinical evidence of polycystic kidney disease. Am. J. Nephrol. 2013, 38, 233–240. [Google Scholar] [CrossRef]
- Klawitter, J.; Reed-Gitomer, B.Y.; McFann, K.; Pennington, A.; Klawitter, J.; Abebe, K.Z.; Klepacki, J.; Cadnapaphornchai, M.A.; Brosnahan, G.; Chonchol, M.; et al. Endothelial dysfunction and oxidative stress in polycystic kidney disease. Am. J. Physiol. Renal Physiol. 2014, 307, F1198–F1206. [Google Scholar] [CrossRef]
- Huang, J.L.; Woolf, A.S.; Kolatsi-Joannou, M.; Baluk, P.; Sandford, R.N.; Peters, D.J.; McDonald, D.M.; Price, K.L.; Winyard, P.J.; Long, D.A. Vascular endothelial growth factor C for polycystic kidney diseases. J. Am. Soc. Nephrol. 2016, 27, 69–77. [Google Scholar] [CrossRef]
- Outeda, P.; Huso, D.L.; Fisher, S.A.; Halushka, M.K.; Kim, H.; Qian, F.; Germino, G.G.; Watnick, T. Polycystin signaling is required for directed endothelial cell migration and lymphatic development. Cell Rep. 2014, 7, 634–644. [Google Scholar] [CrossRef] [PubMed]
- Lorthioir, A.; Joannidès, R.; Rémy-Jouet, I.; Fréguin-Bouilland, C.; Iacob, M.; Roche, C.; Monteil, C.; Lucas, D.; Renet, S.; Audrézet, M.P.; et al. Polycystin deficiency induces dopamine-reversible alterations in flow-mediated dilatation and vascular nitric oxide release in humans. Kidney Int. 2015, 87, 465–472. [Google Scholar] [CrossRef] [PubMed]
- Morel, N.; Vandenberg, G.; Ahrabi, A.K.; Caron, N.; Desjardins, F.; Balligand, J.L.; Horie, S.; Devuyst, O. PKD1 haploinsufficiency is associated with altered vascular reactivity and abnormal calcium signaling in the mouse aorta. Pflugers Archiv 2009, 457, 845–856. [Google Scholar] [CrossRef] [PubMed]
- Qian, Q.; Hunter, L.W.; Li, M.; Marin-Padilla, M.; Prakash, Y.S.; Somlo, S.; Harris, P.C.; Torres, V.E.; Sieck, G.C. Pkd2 haploinsufficiency alters intracellular calcium regulation in vascular smooth muscle cells. Hum. Mol. Genet. 2003, 12, 1875–1880. [Google Scholar] [CrossRef] [PubMed]
- Qian, Q.; Li, M.; Cai, Y.; Ward, C.J.; Somlo, S.; Harris, P.C.; Torres, V.E. Analysis of the polycystins in aortic vascular smooth muscle cells. J. Am. Soc. Nephrol. 2003, 14, 2280–2287. [Google Scholar] [CrossRef] [PubMed]
- Hassane, S.; Claij, N.; Lantinga-van Leeuwen, I.S.; van Munsteren, J.C.; van Lent, N.; Hanemaaijer, R.; Breuning, M.H.; Peters, D.J.; DeRuiter, M.C. Pathogenic sequence for dissecting aneurysm formation in a hypomorphic polycystic kidney disease 1 mouse model. Arterioscler. Thromb. Vasc. Biol. 2007, 27, 2177–2183. [Google Scholar] [CrossRef]
- Hadimeri, H.; Lamm, C.; Nyberg, G. Coronary aneurysms in patients with autosomal dominant polycystic kidney disease. J. Am. Soc. Nephrol. 1998, 9, 837–841. [Google Scholar]
- Belz, M.M.; Hughes, R.L.; Kaehny, W.D.; Johnson, A.M.; Fick-Brosnahan, G.M.; Earnest, M.P.; Gabow, P.A. Familial clustering of ruptured intracranial aneurysms in autosomal dominant polycystic kidney disease. Am. J. Kidney Dis. 2001, 38, 770–776. [Google Scholar] [CrossRef]
- Biagini, A.; Maffei, S.; Baroni, M.; Piacenti, M.; Terrazzi, M.; Paoli, F.; Trianni, G.; Picano, E.; Salvatore, L. Familiar clustering of aortic dissection in polycystic kidney disease. Am. J. Cardiol. 1993, 72, 741–742. [Google Scholar] [CrossRef]
- Neves, J.B.; Rodrigues, F.B.; Lopes, J.A. Autosomal dominant polycystic kidney disease and coronary artery dissection or aneurysm: A systematic review. Ren. Fail. 2016, 38, 493–502. [Google Scholar] [CrossRef]
- Jiang, L.C.; Cao, J.Y.; Chen, M. Coronary artery aneurysm combined with other multiple aneurysms at multiple locations: A case report and systematic review. Medicine 2017, 96, e9230. [Google Scholar] [CrossRef] [PubMed]
- Oomman, A.; Ramachandran, P.; Kumar, N.S. Combined presence of coronary artery ectasia and descending aortic dissection in polycystic kidney disease presenting as acute coronary syndrome. Indian Heart J. 2003, 55, 646–648. [Google Scholar] [PubMed]
- Lee, C.C.; Chang, W.T.; Fang, C.C.; Tsai, I.L.; Chen, W.J. Sudden death caused by dissecting thoracic aortic aneurysm in a patient with autosomal dominant polycystic kidney disease. Resuscitation 2004, 63, 93–96. [Google Scholar] [CrossRef]
- Nacasch, N.; Werner, M.; Golan, E.; Korzets, Z. Arterial dissections in autosomal dominant polycystic kidney disease—Chance association or part of the disease spectrum? Clin. Nephrol. 2010, 73, 478–481. [Google Scholar] [CrossRef]
- Silverio, A.; Prota, C.; Di Maio, M.; Polito, M.V.; Cogliani, F.M.; Citro, R.; Gigantino, A.; Iesu, S.; Piscione, F. Aortic dissection in patients with autosomal dominant polycystic kidney disease: A series of two cases and a review of the literature. Nephrology 2015, 20, 229–235. [Google Scholar] [CrossRef]
- Ivy, D.D.; Shaffer, E.M.; Johnson, A.M.; Kimberling, W.J.; Dobin, A.; Gabow, P.A. Cardiovascular abnormalities in children with autosomal dominant polycystic kidney disease. J. Am. Soc. Nephrol. 1995, 5, 2032–2036. [Google Scholar] [PubMed]
- Lumiaho, A.; Ikäheimo, R.; Miettinen, R.; Niemitukia, L.; Laitinen, T.; Rantala, A.; Lampainen, E.; Laakso, M.; Hartikainen, J. Mitral valve prolapse and mitral regurgitation are common in patients with polycystic kidney disease type 1. Am. J. Kidney Dis. 2001, 38, 1208–1216. [Google Scholar] [CrossRef]
- Chapman, A.B.; Johnson, A.M.; Rainguet, S.; Hossack, K.; Gabow, P.; Schrier, R.W. Left ventricular hypertrophy in autosomal dominant polycystic kidney disease. J. Am. Soc. Nephrol. 1997, 8, 1292–1297. [Google Scholar]
- Saggar-Malik, A.K.; Missouris, C.G.; Gill, J.S.; Singer, D.R.; Markandu, N.D.; MacGregor, G.A. Left ventricular mass in normotensive subjects with autosomal dominant polycystic kidney disease. BMJ 1994, 309, 1617–1618. [Google Scholar] [CrossRef] [PubMed]
- Martinez-Vea, A.; Valero, F.A.; Bardaji, A.; Gutierrez, C.; Broch, M.; Garcia, C.; Richart, C.; Oliver, J.A. Left ventricular hypertrophy in hypertensive patients with autosomal dominant polycystic kidney disease: Influence of blood pressure and humoral and neurohormonal factors. Am. J. Nephrol. 2000, 20, 193–200. [Google Scholar] [CrossRef]
- Bardají, A.; Vea, A.M.; Gutierrez, C.; Ridao, C.; Richart, C.; Oliver, J.A. Left ventricular mass and diastolic function in normotensive young adults with autosomal dominant polycystic kidney disease. Am. J. Kidney Dis. 1998, 32, 970–975. [Google Scholar] [CrossRef]
- Valero, F.A.; Martinez-Vea, A.; Bardají, A.; Gutierrez, C.; Garcia, C.; Richart, C.; Oliver, J.A. Ambulatory blood pressure and left ventricular mass in normotensive patients with autosomal dominant polycystic kidney disease. J. Am. Soc. Nephrol. 1999, 10, 1020–1026. [Google Scholar]
- Schrier, R.W. Renal volume; renin-angiotensin-aldosterone system; hypertension; and left ventricular hypertrophy in patients with autosomal dominant polycystic kidney disease. J. Am. Soc. Nephrol. 2009, 20, 1888–1893. [Google Scholar] [CrossRef]
- Chen, H.; Watnick, T.; Hong, S.N.; Daly, B.; Li, Y.; Seliger, S.L. Left ventricular hypertrophy in a contemporary cohort of autosomal dominant polycystic kidney disease patients. BMC Nephrol. 2019, 20, 386. [Google Scholar] [CrossRef]
- Mancuso, P.; Rahman, A.; Hershey, S.D.; Dandu, L.; Nibbelink, K.A.; Simpson, R.U. 1,25-Dihydroxyvitamin-D3 treatment reduces cardiac hypertrophy and left ventricular diameter in spontaneously hypertensive heart failure-prone (cp/+) rats independent of changes in serum leptin. J. Cardiovasc. Pharmacol. 2008, 51, 559–564. [Google Scholar] [CrossRef]
- Cadnapaphornchai, M.A.; McFann, K.; Strain, J.D.; Masoumi, A.; Schrier, R.W. Increased left ventricular mass in children with autosomal dominant polycystic kidney disease and borderline hypertension. Kidney Int. 2008, 74, 1192–1196. [Google Scholar] [CrossRef]
- Oflaz, H.; Alisir, S.; Buyukaydin, B.; Kocaman, O.; Turgut, F.; Namli, S.; Pamukcu, B.; Oncul, A.; Ecder, T. Biventricular diastolic dysfunction in patients with autosomal dominant polycystic kidney disease. Kidney Int. 2005, 68, 2244–2249. [Google Scholar] [CrossRef] [PubMed]
- Spinelli, L.; Pisani, A.; Giugliano, G.; Trimarco, B.; Riccio, E.; Visciano, B.; Remuzzi, G.; Ruggenenti, P. Data on the assessment of LV mechanics by speckle tracking echocardiography in ADPKD patients. Data Brief 2018, 21, 2075–2081. [Google Scholar] [CrossRef]
- Spinelli, L.; Pisani, A.; Giugliano, G.; Trimarco, B.; Riccio, E.; Visciano, B.; Remuzzi, G.; Ruggenenti, P.; ALADIN-Cardiovascular Study Group. Left ventricular dysfunction in ADPKD and effects of octreotide-LAR: A cross-sectional and longitudinal substudy of the ALADIN trial. Int. J. Cardiol. 2019, 275, 145–151. [Google Scholar] [CrossRef] [PubMed]
- Wu, G.; Somlo, S. Molecular genetics and mechanism of autosomal dominant polycystic kidney disease. Mol. Genet. Metab. 2000, 69, 1–15. [Google Scholar] [CrossRef] [PubMed]
- Wu, G.; Markowitz, G.S.; Li, L.; D’Agati, V.D.; Factor, S.M.; Geng, L.; Tibara, S.; Tuchman, J.; Cai, Y.; Park, J.H.; et al. Cardiac defects and renal failure in mice with targeted mutations in Pkd2. Nat. Genet. 2000, 24, 75–78. [Google Scholar] [CrossRef]
- Anyatonwu, G.I.; Estrada, M.; Tian, X.; Somlo, S.; Ehrlich, B.E. Regulation of ryanodine receptor dependent calcium signaling by polycystin-2. Proc. Natl. Acad. Sci. USA 2007, 104, 6454–6459. [Google Scholar] [CrossRef] [PubMed]
- Pedrozo, Z.; Criollo, A.; Battiprolu, P.K.; Morales, C.R.; Contreras-Ferrat, A.; Fernández, C.; Jiang, N.; Luo, X.; Caplan, M.J.; Somlo, S.; et al. Polycystin-1 is a cardiomyocyte mechanosensor that governs L-type Ca2+ channel protein stability. Circulation 2015, 131, 2131–2142. [Google Scholar] [CrossRef]
- Córdova-Casanova, A.; Olmedo, I.; Riquelme, J.A.; Barrientos, G.; Sánchez, G.; Gillette, T.G.; Lavandero, S.; Chiong, M.; Donoso, P.; Pedrozo, Z. Mechanical stretch increases L-type calcium channel stability in cardiomyocytes through a polycystin-1/AKT-dependent mechanism. Biochim. Biophys. Acta Mol. Cell Res. 2018, 1865, 289–296. [Google Scholar] [CrossRef]
- Balbo, B.E.; Amaral, A.G.; Fonseca, J.M.; de Castro, I.; Salemi, V.M.; Souza, L.E.; Dos Santos, F.; Irigoyen, M.C.; Qian, F.; Chammas, R.; et al. Cardiac dysfunction in Pkd1-deficient mice with phenotype rescue by galectin-3 knockout. Kidney Int. 2016, 90, 580–597. [Google Scholar] [CrossRef]
- Aránguiz, P.; Romero, P.; Vásquez, F.; Flores-Vergara, R.; Aravena, D.; Sánchez, G.; González, M.; Olmedo, I.; Pedrozo, Z. Polycystin-1 mitigates damage and regulates CTGF expression through AKT activation during cardiac ischemia/reperfusion. Biochim. Biophys. Acta Mol. Basis Dis. 2021, 1867, 165986. [Google Scholar] [CrossRef] [PubMed]
- Altamirano, F.; Schiattarella, G.G.; French, K.M.; Kim, S.Y.; Engelberger, F.; Kyrychenko, S.; Villalobos, E.; Tong, D.; Schneider, J.W.; Ramirez-Sarmiento, C.A.; et al. Polycystin-1 assembles with Kv channels to govern cardiomyocyte repolarization and contractility. Circulation 2019, 140, 921–936. [Google Scholar] [CrossRef] [PubMed]
- Paavola, J.; Schliffke, S.; Rossetti, S.; Kuo, I.Y.; Yuan, S.; Sun, Z.; Harris, P.C.; Torres, V.E.; Ehrlich, B.E. Polycystin-2 mutations lead to impaired calcium cycling in the heart and predispose to dilated cardiomyopathy. J. Mol. Cell Cardiol. 2013, 58, 199–208. [Google Scholar] [CrossRef] [PubMed]
- Volk, T.; Schwoerer, A.P.; Thiessen, S.; Schultz, J.H.; Ehmke, H. A polycystin-2-like large conductance cation channel in rat left ventricular myocytes. Cardiovasc. Res. 2003, 58, 76–88. [Google Scholar] [CrossRef]
- Kuo, I.Y.; Kwaczala, A.T.; Nguyen, L.; Russell, K.S.; Campbell, S.G.; Ehrlich, B.E. Decreased polycystin 2 expression alters calcium-contraction coupling and changes β-adrenergic signaling pathways. Proc. Natl. Acad. Sci. USA 2014, 111, 16604–16609. [Google Scholar] [CrossRef] [PubMed]
- Criollo, A.; Altamirano, F.; Pedrozo, Z.; Schiattarella, G.G.; Li, D.L.; Rivera-Mejías, P.; Sotomayor-Flores, C.; Parra, V.; Villalobos, E.; Battiprolu, P.K.; et al. Polycystin-2-dependent control of cardiomyocyte autophagy. J. Mol. Cell Cardiol. 2018, 118, 110–121. [Google Scholar] [CrossRef]
- Kuo, I.Y.; Chapman, A.B. Polycystins, ADPKD, and cardiovascular disease. Kidney Int. Rep. 2019, 5, 396–406. [Google Scholar] [CrossRef]
- Lee, J.J.; Cheng, S.J.; Huang, C.Y.; Chen, C.Y.; Feng, L.; Hwang, D.Y.; Kamp, T.J.; Chen, H.C.; Hsieh, P.C.H. Primary cardiac manifestation of autosomal dominant polycystic kidney disease revealed by patient induced pluripotent stem cell-derived cardiomyocytes. EBioMedicine 2019, 40, 675–684. [Google Scholar] [CrossRef]
- Chebib, F.T.; Hogan, M.C.; El-Zoghby, Z.M.; Irazabal, M.V.; Senum, S.R.; Heyer, C.M.; Madsen, C.D.; Cornec-Le Gall, E.; Behfar, A.; Harris, P.C.; et al. Autosomal dominant polycystic kidney patients may be predisposed to various cardiomyopathies. Kidney Int. Rep. 2017, 2, 913–923. [Google Scholar] [CrossRef] [PubMed]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Spinelli, L.; Giugliano, G.; Esposito, G. Cardiac Involvement in Autosomal Dominant Polycystic Kidney Disease. Cardiogenetics 2021, 11, 39-49. https://doi.org/10.3390/cardiogenetics11020006
Spinelli L, Giugliano G, Esposito G. Cardiac Involvement in Autosomal Dominant Polycystic Kidney Disease. Cardiogenetics. 2021; 11(2):39-49. https://doi.org/10.3390/cardiogenetics11020006
Chicago/Turabian StyleSpinelli, Letizia, Giuseppe Giugliano, and Giovanni Esposito. 2021. "Cardiac Involvement in Autosomal Dominant Polycystic Kidney Disease" Cardiogenetics 11, no. 2: 39-49. https://doi.org/10.3390/cardiogenetics11020006
APA StyleSpinelli, L., Giugliano, G., & Esposito, G. (2021). Cardiac Involvement in Autosomal Dominant Polycystic Kidney Disease. Cardiogenetics, 11(2), 39-49. https://doi.org/10.3390/cardiogenetics11020006





