The Transdermal Delivery of Therapeutic Cannabinoids
Abstract
:1. Introduction
Cannabinoid’s Receptors
2. Delivery Routes and Bioavailability of Cannabinoids
3. Transdermal Delivery of Cannabinoids
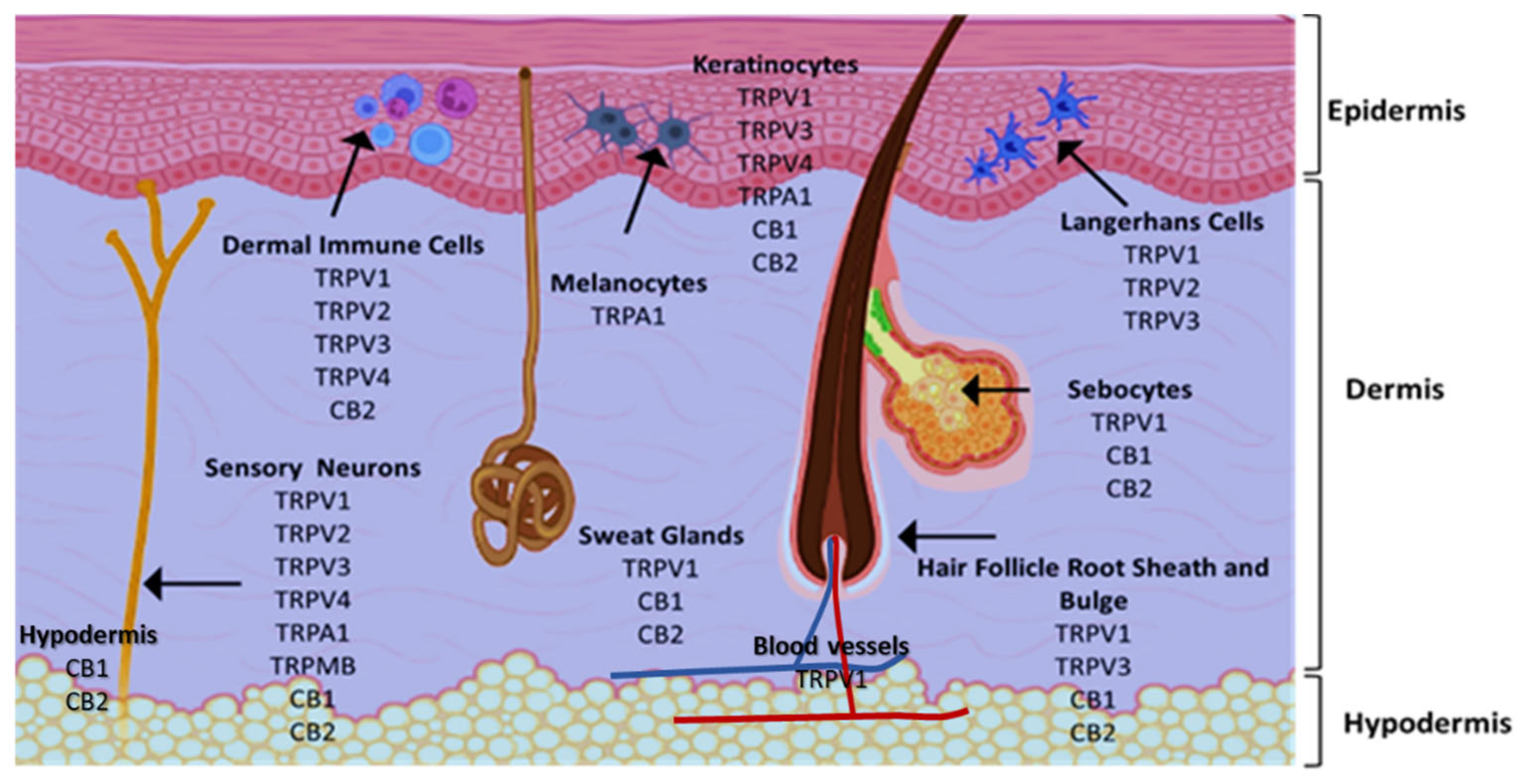
3.1. Skin as a Potential Route
3.2. Importance of Transdermal Drug Delivery Studies
3.3. Transdermal Delivery of Cannabinoids and Challenges
| Citations | Formulation | Active Substance | Concentrate | Applications | Result |
|---|---|---|---|---|---|
| [19] | Ointment | Cannabidiol (CBD) | - | Inflammatory skin diseases and cutaneous scars (psoriasis, atopic dermatitis, and scars) | Improved skin parameters such as hydration, transepidermal water loss, and elasticity in humans |
| [20] | Hydroalcoholic proprietary gel | Cannabidiol (CBD) | 2.5 g CBD/100 g gel permeation enhancer (Transcutol® HP) | The prevention of relapse to drug use (alcohol or cocaine) | CBD has potential in relapse prevention in the rat model |
| [40] | Gel | Cannabidiol (CBD) | 6.2 and 62 mg/day | Inflammation and pain | Reduction of proinflammatory markers, joint swelling, and immune infiltration in rat model of arthritis |
| [63] | Patches | Δ8-THC | 16 mg/mL D8 -THC in 1:1:1 (v/v/v) of propylene glycol:water:ethanol | Making a transcutaneous drug system (TTS) for Δ8-THC | Gradually enhanced Δ8-THC plasma concentration and preserved steady-state plasma levels 24 h after removing the patch |
| [52] | Patches | Cannabidiol (CBD) | 3% w/w CBD and 40% w/w EtOH | Chronic inflammatory diseases | Significant cumulation of CBD in the skin of murine models |
| [102] | Gel | Cannabidiol (CBD) | The 1%, 2.5%, and 5% (w/w) CBD gels | Alcohol-induced neurodegeneration | Neuroprotection and reduction of alcohol-induced neurodegeneration in rodent models |
| [105] | Microemulsion | Acidic cannabinoids (THCA and CBDA) | 1.0% (w/w) of cannabinoids, 5% (w/w) of Capryol® 90, 44% (w/w) Surfactant mixture (2:1, Procetyl® AWS and Ethanol) and 50.0% (w/w) distilled water | Permeation enhancement | A significant improvement of the permeation of THCA and CBDA in vitro. |
| [106] | Stimuli-responsive chitosan/ZnO NPs | CBD | - | Treatment-resistant epilepsy patient | Carrier showed superior drug loading capacity with the prolonged release of CBD for six days and great biosafety tforL929 mouse fibroblasts (the connective tissue cells) |
| [109] | Polysaccharide cryogels containing β-cyclodextrin | CBD | - | Skin malignancies | The designed platform showed a high drug loading efficiency with biocompatibility and bi-phasic drug release with an initial burst and a later slow release. Showed dose-dependent cytotoxicity on two cancer cell lines (MJ and HUT-78) |
| [110] | Nanocomposite HEC/PM cryogel | CBD | - | Cutaneous lesions due to CTCL (cutaneous T-cell lymphoma) | Sustained topical CBD delivery |
| [112] | Emulsions stabilized with chitosan/collagen peptides nanoparticles | CBD | 0.6 g CBD in olive oil and liquid paraffin mixture to make 6 mg/mL | Cosmetic purposes | Effective penetration of nanoparticles through deeper skin layers |
| [113] | Microemulgel | CBD | 1% w/w CBD Solutol HS 15 (20%, surfactant), Transcutol P (9%, cosolvent), isopropyl myristate (5%, oil phase), water (66%) | Skin diseases | Highly stable formulation, controlled drug release, retention in the skin layers |
| [114] | Prodrug (D9-tetrahydrocannabinol amino acid dicarboxylate prodrug) | THC analogue | - | Glaucoma treatment | Reduced intraocular pressure |
| [115] | Topical CBD (oil, cream, and spray) | Cannabidiol (CBD) | Epidermolysis bullosa | Decrease in pain and blistering; fast wound healing; no effects reported | |
| [116] | Topical MC oil | CBD and THC | THC 5 mg/mL CBD 6 mg/mL | Patients with pyoderma gangrenosum | Improve pain management and improve baseline pain levels |
| [117] | Cream | Cannabidiol (CBD) | CBD-infused oil (75 mg/mL or 150 mg/mL) | Pharmacokinetics | Probable incomplete transdermal absorption in healthy dogs |
4. Conclusions
Author Contributions
Funding
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| 2-AGE | 2-arachidonylglyceryl ether (Noladin ether) |
| 2-AG | 2-arachidonoylglycerol |
| AEA | Anandamide (N-arachidonoylethanolamine) |
| AjA | Ajulemic acid |
| CBC | Cannabichromene |
| CBD | Cannabidiol |
| CBDV | Cannabigerovarin |
| CBG | Cannabigerol |
| CBN | Cannabinol |
| MET | (R)-methanandamid |
| MRSA | Methicillin-resistant Staphylococcus aureus |
| O-AEA | O-arachidonoyl ethanolamine |
| PEA | Palmidrol |
| THC | Delta-9-tetrahydrocannabinol |
| THCA-A | Tetrahydrocannabinolic acid |
| THCVA | Delta 9—tetrahydrocannabivarin carboxylic acid |
| THCV | Delta 9—tetrahydrocannabivarin |
| TRPA | Transient receptor potential Ankyrin |
| TRPC | Transient receptor potential canonical |
| TRPM | Transient receptor potential melastatin |
| TRPML | Transient receptor potential mucolipin |
| TRPP | Transient receptor potential polycystin |
| TRPV | Transient receptor potential vanilloid |
| Δ-8-THC | Delta-8-tetrahydrocannabinol |
References
- Thomas, B.; El Sohly, M.A. The botany of Cannabis sativa L. In The Analytical Chemistry of Cannabis; Elsevier: Waltham, MA, USA, 2016; pp. 1–26. [Google Scholar]
- Chandra, S.; Lata, H.; El Sohly, M.A. Cannabis Sativa L.-Botany and Biotechnology; Springer: Berlin/Heidelberg, Germany, 2017. [Google Scholar]
- Josefina, F.-S.I.; Robert, V. Secondary metabolism in cannabis. Phytochem. Rev. 2008, 3, 615. [Google Scholar]
- Wróbel, T.; Dreger, M.; Wielgus, K.; Słomski, R. The application of plant in vitro cultures in cannabinoid production. Biotechnol. Lett. 2018, 40, 445–454. [Google Scholar] [CrossRef] [PubMed]
- Pacula, R.L.; Smart, R. Medical marijuana and marijuana legalization. Annu. Rev. Clin. Psychol. 2017, 13, 397–419. [Google Scholar] [CrossRef] [PubMed]
- Roberto, D. The Use of Endogenous and Synthetic Cannabinoids in Prostate Cancer Therapy; University of Toronto: Toronto, QC, Canada, 2018. [Google Scholar]
- Kovalchuk, O.; Kovalchuk, I. Cannabinoids as anticancer therapeutic agents. Cell Cycle 2020, 19, 961–989. [Google Scholar] [CrossRef]
- Marks, D.H.; Friedman, A. The therapeutic potential of cannabinoids in dermatology. Skin Ther. Lett. 2018, 23, 1–5. [Google Scholar]
- Sarfaraz, S.; Adhami, V.M.; Syed, D.N.; Afaq, F.; Mukhtar, H. Cannabinoids for cancer treatment: Progress and promise. Cancer Res. 2008, 68, 339–342. [Google Scholar] [CrossRef] [Green Version]
- Von Bayern, A.M.P.; Heathcote, R.J.P.; Rutz, C.; Kacelnik, A. The role of experience in problem solving and innovative tool use in crows. Curr. Biol. 2009, 19, 1965–1968. [Google Scholar] [CrossRef] [Green Version]
- Russo, E.B. Taming THC: Potential cannabis synergy and phytocannabinoid-terpenoid entourage effects. Br. J. Pharmacol. 2011, 163, 1344–1364. [Google Scholar] [CrossRef]
- Russo, E.B.; Marcu, J. Cannabis pharmacology: The usual suspects and a few promising leads, in Advances in pharmacology. Adv. Pharmacol. 2017, 80, 67–134. [Google Scholar]
- Carlini, E.A. The good and the bad effects of (-) trans-delta-9-tetrahydrocannabinol (Delta 9-THC) on humans. Toxicon 2004, 44, 461–467. [Google Scholar] [CrossRef]
- Explore Chemistry. Quickly Find Chemical Information from Authoritative Sources. Available online: https://pubchem.ncbi.nlm.nih.gov (accessed on 1 December 2021).
- Bruni, N.; Della Pepa, C.; Oliaro-Bosso, S.; Pessione, E.; Gastaldi, D.; Dosio, F. Cannabinoid Delivery Systems for Pain and Inflammation Treatment. Molecules 2018, 23, 2478. [Google Scholar] [CrossRef] [Green Version]
- Adelli, G.R.; Bhagav, P.; Taskar, P.; Hingorani, T.; Pettaway, S.; Gul, W.; El Sohly, M.A.; Repka, M.A.; Majumdar, S. Development of a Delta9-Tetrahydrocannabinol Amino Acid-Dicarboxylate Prodrug with Improved Ocular Bioavailability. Investig. Ophthalmol. Vis. Sci. 2017, 58, 2167–2179. [Google Scholar] [CrossRef] [Green Version]
- Wassmann, C.S.; Højrup, P.; Klitgaard, J.K. Cannabidiol is an effective helper compound in combination with bacitracin to kill Gram-positive bacteria. Sci. Rep. 2020, 10, 4112. [Google Scholar] [CrossRef]
- Velasco, G.; Sánchez, C.; Guzmán, M. Towards the use of cannabinoids as antitumour agents. Nat. Rev. Cancer 2012, 12, 436–444. [Google Scholar] [CrossRef]
- Palmieri, B.; Laurino, C.; Vadalà, M. A therapeutic effect of cbd-enriched ointment in inflammatory skin diseases and cutaneous scars. Clin. Ter. 2019, 170, e93–e99. [Google Scholar]
- Gonzalez-Cuevas, G.; Martin-Fardon, R.; Kerr, T.M.; Stouffer, D.G.; Parsons, L.H.; Hammell, D.C.; Banks, S.L.; Stinchcomb, A.L.; Weiss, F. Unique treatment potential of cannabidiol for the prevention of relapse to drug use: Preclinical proof of principle. Neuropsychopharmacology 2018, 43, 2036–2045. [Google Scholar] [CrossRef] [Green Version]
- Koch, N.; Nassar, N.; Bachari, A.; Schanknecht, E.; Telukutla, S.; Zomer, R.; Piva, T.J.; Mantri, N. Cannabidiol aqueous solubility enhancement: Comparison of three amorphous formulations strategies using different type of polymers. Int. J. Pharm. 2020, 589, 119812. [Google Scholar] [CrossRef]
- Singh, K.; Nassar, N.; Bachari, A.; Schanknecht, E.; Telukutla, S.; Zomer, R.; Piva, T.J.; Mantri, N. The Pathophysiology and the Therapeutic Potential of Cannabinoids in Prostate Cancer. Cancers 2021, 13, 4107. [Google Scholar] [CrossRef]
- Bachari, A.; Piva, T.J.; Salami, S.A.; Jamshidi, N.; Mantri, N. Roles of Cannabinoids in Melanoma: Evidence from In Vivo Studies. Int. J. Mol. Sci. 2020, 21, 6040. [Google Scholar] [CrossRef]
- Grotenhermen, F. Cannabinoids for therapeutic use. Am. J. Drug Deliv. 2004, 2, 229–240. [Google Scholar] [CrossRef]
- Grotenhermen, F.; Müller-Vahl, K. The therapeutic potential of cannabis and cannabinoids. Dtsch. Arztebl. Int. 2012, 109, 495–501. [Google Scholar] [CrossRef]
- Iqbal, J.; Abbasi, B.A.; Ahmad, R.; Batool, R.; Mahmood, T.; Ali, B.; Khalil, A.T.; Kanwal, S.; Afzal Shah, S.; Alam, M.M.; et al. Potential phytochemicals in the fight against skin cancer: Current landscape and future perspectives. Biomed. Pharmacother. 2019, 109, 1381–1393. [Google Scholar] [CrossRef]
- Simmerman, E.; Qin, X.; Jack, C.Y.; Baban, B. Cannabinoids as a potential new and novel treatment for melanoma: A pilot study in a murine model. J. Surg. Res. 2019, 235, 210–215. [Google Scholar] [CrossRef]
- Malhotra, P.; Casari, I.; Falasca, M. Therapeutic potential of cannabinoids in combination cancer therapy. Adv. Biol. Regul. 2021, 79, 100774. [Google Scholar] [CrossRef]
- Bíró, T.; Tóth, B.I.; Haskó, G.; Paus, R.; Pacher, P. The endocannabinoid system of the skin in health and disease: Novel perspectives and therapeutic opportunities. Trends Pharmacol. Sci. 2009, 30, 411–420. [Google Scholar] [CrossRef] [Green Version]
- Lu, Y.; Anderson, H.D. Cannabinoid signaling in health and disease. Can. J. Physiol. Pharmacol. 2017, 95, 311–327. [Google Scholar] [CrossRef]
- Katz, J.; Costarides, A.P. Facts vs. Fiction: The Role of Cannabinoids in the Treatment of Glaucoma. Curr. Ophthalmol. Rep. 2019, 7, 177–181. [Google Scholar] [CrossRef]
- McKallip, R.J.; Lombard, C.; Fisher, M.; Martin, B.R.; Ryu, S.; Grant, S.; Nagarkatti, P.S.; Nagarkatti, M.J.B. Targeting CB2 cannabinoid receptors as a novel therapy to treat malignant lymphoblastic disease. Blood 2002, 100, 627–634. [Google Scholar] [CrossRef] [Green Version]
- Ramer, R.; Heinemann, K.; Merkord, J.; Rohde, H.; Salamon, A.; Linnebacher, M.; Hinz, B. COX-2 and PPAR-γ confer cannabidiol-induced apoptosis of human lung cancer cells. Mol. Cancer Ther. 2013, 12, 69–82. [Google Scholar] [CrossRef] [Green Version]
- Pertwee, R.G.; Howlett, A.; Abood, M.E.; Alexander, S.; Di Marzo, V.; Elphick, M.; Greasley, P.; Hansen, H.S.; Kunos, G.; Mackie, K.J.P.r. International union of basic and clinical pharmacology. Lxxix. Cannabinoid receptors and their ligands: Beyond cb1 and cb2. Pharmacol. Rev. 2010, 62, 588–631. [Google Scholar] [CrossRef] [Green Version]
- Wall, M.E.; Sadler, B.M.; Brine, D.; Taylor, H.; Perez-Reyes, M. Metabolism, disposition, and kinetics of delta-9-tetrahydrocannabinol in men and women. Clin. Pharmacol. Ther. 1983, 34, 352–363. [Google Scholar] [CrossRef]
- Sawzdargo, M.; Nguyen, T.; Lee, D.K.; Lynch, K.R.; Cheng, R.; Heng, H.H.; George, S.R.; O’Dowd, B.F. Identification and cloning of three novel human G protein-coupled receptor genes GPR52, ΨGPR53 and GPR55: GPR55 is extensively expressed in human brain. Brain Res. Mol. Brain Res. 1999, 64, 193–198. [Google Scholar] [CrossRef]
- Venkatachalam, K.; Montell, C. TRP channels. Annu. Rev. Biochem. 2007, 76, 387–417. [Google Scholar] [CrossRef] [Green Version]
- Caterina, M.J. TRP Channel Cannabinoid Receptors in Skin Sensation, Homeostasis, and Inflammation. ACS Chem. Neurosci. 2014, 5, 1107–1116. [Google Scholar] [CrossRef]
- An, D.; Peigneur, S.; Hendrickx, L.A.; Tytgat, J. Targeting Cannabinoid Receptors: Current Status and Prospects of Natural Products. Int. J. Mol. Sci. 2020, 21, 5064. [Google Scholar] [CrossRef]
- Hammell, D.; Zhang, L.; Ma, F.; Abshire, S.; McIlwrath, S.; Stinchcomb, A.; Westlund, K. Transdermal cannabidiol reduces inflammation and pain-related behaviours in a rat model of arthritis. Eur. J. Pain 2016, 20, 936–948. [Google Scholar] [CrossRef]
- Eubanks, L.M.; Rogers, C.J.; Beuscher; Koob, G.F.; Olson, A.J.; Dickerson, T.J.; Janda, K.D. A Molecular Link between the Active Component of Marijuana and Alzheimer’s Disease Pathology. Mol. Pharm. 2006, 3, 773–777. [Google Scholar] [CrossRef] [Green Version]
- Velasco, G.; Sánchez, C.; Guzmán, M. Endocannabinoids and cancer. Endocannabinoids 2015, 231, 449–472. [Google Scholar]
- Velasco, G.; Sánchez, C.; Guzmán, M. Anticancer mechanisms of cannabinoids. Curr. Oncol. 2016, 23, S23. [Google Scholar] [CrossRef] [Green Version]
- Eagleston, L.R.; Kalani, N.K.; Patel, R.R.; Flaten, H.K.; Dunnick, C.A.; Dellavalle, R.P. Cannabinoids in dermatology: A scoping review. Dermatol. Online J. 2018, 24, 1. [Google Scholar] [CrossRef]
- Tijani, A.O.; Thakur, D.; Mishra, D.; Frempong, D.; Chukwunyere, U.I.; Puri, A. Delivering therapeutic cannabinoids via skin: Current state and future perspectives. J. Control. Release 2021, 334, 427–451. [Google Scholar] [CrossRef] [PubMed]
- Pacher, P.; Bátkai, S.; Kunos, G. The endocannabinoid system as an emerging target of pharmacotherapy. Pharmacol. Rev. 2006, 58, 389–462. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Pucci, M.; Pirazzi, V.; Pasquariello, N.; Maccarrone, M. Endocannabinoid signaling and epidermal differentiation. Eur. J. Dermatol. 2011, 21 (Suppl. S2), 29–34. [Google Scholar] [CrossRef] [PubMed]
- Sheriff, T.; Lin, M.J.; Dubin, D.; Khorasani, H. The potential role of cannabinoids in dermatology. J. Dermatol. Treat. 2019, 31, 1–7. [Google Scholar] [CrossRef]
- Demuth, D.G.; Molleman, A. Cannabinoid signalling. Life Sci. 2006, 78, 549–563. [Google Scholar] [CrossRef]
- Glodde, N.; Jakobs, M.; Bald, T.; Tüting, T.; Gaffal, E. Differential role of cannabinoids in the pathogenesis of skin cancer. Life Sci. 2015, 138, 35–40. [Google Scholar] [CrossRef]
- Alkilani, A.Z.; McCrudden, M.T.; Donnelly, R.F. Transdermal drug delivery: Innovative pharmaceutical developments based on disruption of the barrier properties of the stratum corneum. Pharmaceutics 2015, 7, 438–470. [Google Scholar] [CrossRef] [Green Version]
- Lodzki, M.; Godin, B.; Rakou, L.; Mechoulam, R.; Gallily, R.; Touitou, E. Cannabidiol-transdermal delivery and anti-inflammatory effect in a murine model. J. Control. Release 2003, 93, 377–387. [Google Scholar] [CrossRef]
- Lucas, C.J.; Galettis, P.; Schneider, J. The pharmacokinetics and the pharmacodynamics of cannabinoids. Br. J. Clin. Pharm. 2018, 84, 2477–2482. [Google Scholar] [CrossRef] [Green Version]
- Hellriegel, E.T.; Bjornsson, T.D.; Hauck, W.W. Interpatient variability in bioavailability is related to the extent of absorption: Implications for bioavailability and bioequivalence studies. Clin. Pharmacol. Ther. 1996, 60, 601–607. [Google Scholar] [CrossRef]
- Millar, S.A.; Stone, N.L.; Yates, A.S.; O’Sullivan, S.E. A Systematic Review on the Pharmacokinetics of Cannabidiol in Humans. Front. Pharmacol. 2018, 9, 1365. [Google Scholar] [CrossRef]
- Grotenhermen, F. Pharmacokinetics and Pharmacodynamics of Cannabinoids. Clin. Pharmacokinet. 2003, 42, 327–360. [Google Scholar] [CrossRef] [PubMed]
- Pacifici, R.; Marchei, E.; Salvatore, F.; Guandalini, L.; Busardò, F.P.; Pichini, S. Evaluation of long-term stability of cannabinoids in standardized preparations of cannabis flowering tops and cannabis oil by ultra-high-performance liquid chromatography tandem mass spectrometry. Clin. Chem. Lab. Med. (CCLM) 2018, 56, 94–96. [Google Scholar] [CrossRef] [PubMed]
- Mazzetti, C.; Ferri, E.; Pozzi, M.; Labra, M. Quantification of the content of cannabinol in commercially available e-liquids and studies on their thermal and photo-stability. Sci. Rep. 2020, 10, 3697. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Ohlsson, A.; Lindgren, J.E.; Andersson, S.; Agurell, S.; Gillespie, H.; Hollister, L.E. Single-dose kinetics of deuterium-labelled cannabidiol in man after smoking and intravenous administration. Biomed. Environ. Mass Spectrom. 1986, 13, 77–83. [Google Scholar] [CrossRef] [PubMed]
- Samara, E.; Bialer, M.; Mechoulam, R. Pharmacokinetics of cannabidiol in dogs. Drug Metab. 1988, 16, 469–472. [Google Scholar]
- Mechoulam, R.; Parker, L.A.; Gallily, R. Cannabidiol: An overview of some pharmacological aspects. J. Clin. Pharmacol. 2002, 42, 11S–19S. [Google Scholar] [CrossRef]
- Merrick, J.; Lane, B.; Sebree, T.; Yaksh, T.; O’Neill, C.; Banks, S.L. Identification of Psychoactive Degradants of Cannabidiol in Simulated Gastric and Physiological Fluid. Cannabis Cannabinoid Res. 2016, 1, 102–112. [Google Scholar] [CrossRef] [Green Version]
- Valiveti, S.; Hammell, D.C.; Earles, D.C.; Stinchcomb, A. Transdermal delivery of the synthetic cannabinoid WIN 55,212-2: In vitro/in vivo correlation. Pharm. Res 2004, 21, 1137–1145. [Google Scholar] [CrossRef]
- Ohlsson, A.; Lindgren, J.E.; Wahlén, A.; Agurell, S.; Hollister, L.E.; Gillespie, H.K. Single dose kinetics of deuterium labelled Δ1-tetrahydrocannabinol in heavy and light cannabis users. Biol. Mass Spectrom. 1982, 9, 6–10. [Google Scholar] [CrossRef]
- Agurell, S.; Leander, K. Stability, transfer and absorption of cannabinoid constituents of cannabis (hashish) during smoking. Acta Pharm. Suec. 1971, 8, 391. [Google Scholar] [PubMed]
- Vandevenne, M.; Vandenbussche, H.; Verstraete, A. Detection time of drugs of abuse in urine. Acta Clin. Belg. 2000, 55, 323–333. [Google Scholar] [CrossRef]
- Widman, M.; Agurell, S.; Ehrnebo, M.; Jones, G. Binding of (+)- and (minus)-delta-1-tetrahydrocannabinols and (minus)-7-hydroxy-delta-1-tetrahydrocannabinol to blood cells and plasma proteins in man. J. Pharm. Pharmacol. 1974, 26, 914–916. [Google Scholar] [CrossRef] [PubMed]
- Ngwa, W.; Kumar, R.; Moreau, M.; Dabney, R.; Herman, A. Nanoparticle Drones to Target Lung Cancer with Radiosensitizers and Cannabinoids. Front. Oncol. 2017, 7, 208. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Hollister, L.; Gillespie, H.; Ohlsson, A.; Lindgren, J.E.; Wahlen, A.; Agurell, S. Do plasma concentrations of δ9-tetrahydrocannabinol reflect the degree of intoxication? J. Clin. Pharmacol. 1981, 21, 171S–177S. [Google Scholar] [CrossRef] [PubMed]
- Stella, B.; Baratta, F.; Della Pepa, C.; Arpicco, S.; Gastaldi, D.; Dosio, F.J.D. Cannabinoid formulations and delivery sys-tems: Current and future options to treat pain. Drugs 2021, 81, 1513–1557. [Google Scholar] [CrossRef]
- Huestis, M.A. Human cannabinoid pharmacokinetics. Chem. Biodivers. 2007, 4, 1770–1804. [Google Scholar] [CrossRef] [Green Version]
- Paudel, K.S.; Hammell, D.C.; Agu, R.U.; Valiveti, S.; Stinchcomb, A.L. Cannabidiol bioavailability after nasal and transdermal application: Effect of permeation enhancers. Drug Dev. Ind. Pharm. 2010, 36, 1088–1097. [Google Scholar] [CrossRef]
- Bryson, N.; Sharma, A. Nasal Cannabidiol Compositions. WO Patent WO2017208072A2, 7 December 2017. [Google Scholar]
- Thomas, B.J.; Finnin, B.C. The transdermal revolution. Drug Discov. Today 2004, 9, 697–703. [Google Scholar] [CrossRef]
- Stinchcomb, A.L.; Valiveti, S.; Hammell, D.C.; Ramsey, D.R. Human skin permeation of delta8-tetrahydrocannabinol, cannabidiol and cannabinol. J. Pharm. Pharmacol. 2004, 56, 291–297. [Google Scholar] [CrossRef]
- Yeroushalmi, S.; Nelson, K.; Sparks, A.; Friedman, A. Perceptions and recommendation behaviors of dermatologists for medical cannabis: A pilot survey. Complement. Ther. Med. 2020, 55, 102552. [Google Scholar] [CrossRef] [PubMed]
- Hess, C.; Krämer, M.; Madea, B. Topical application of THC containing products is not able to cause positive cannabinoid finding in blood or urine. Forensic Sci. Int. 2017, 272, 68–71. [Google Scholar] [CrossRef] [PubMed]
- Bolzinger, M.-A.; Briançon, S.; Pelletier, J.; Chevalier, Y. Penetration of drugs through skin, a complex rate-controlling membrane. Curr. Opin. Colloid Interface Sci. 2012, 17, 156–165. [Google Scholar] [CrossRef]
- Kong, M.; Chen, X.G.; Kweon, D.K.; Park, H.J. Investigations on skin permeation of hyaluronic acid based nanoemulsion as transdermal carrier. Carbohydr. Polym. 2011, 86, 837–843. [Google Scholar] [CrossRef]
- Filon, F.L.; Mauro, M.; Adami, G.; Bovenzi, M.; Crosera, M. Nanoparticles skin absorption: New aspects for a safety profile evaluation. Regul. Toxicol. Pharmacol. 2015, 72, 310–322. [Google Scholar] [CrossRef]
- Larraneta, E.; Lutton, R.E.; Woolfson, A.D.; Donnelly, R.F. Microneedle arrays as transdermal and intradermal drug delivery systems: Materials science, manufacture and commercial development. Mater. Sci. Eng. 2016, 104, 1–32. [Google Scholar] [CrossRef] [Green Version]
- Moser, K.; Kriwet, K.; Naik, A.; Kalia, Y.N.; Guy, R.H. Passive skin penetration enhancement and its quantification in vitro. Eur. J. Pharm. Biopharm. 2001, 52, 103–112. [Google Scholar] [CrossRef]
- Godin, B.; Touitou, E. Transdermal skin delivery: Predictions for humans from in vivo, ex vivo and animal models. Adv. Drug Deliv. Rev. 2007, 59, 1152–1161. [Google Scholar] [CrossRef]
- Goyal, R.; Macri, L.K.; Kaplan, H.M.; Kohn, J. Nanoparticles and nanofibers for topical drug delivery. J. Control. Release 2016, 240, 77–92. [Google Scholar] [CrossRef] [Green Version]
- Prausnitz, M.R.; Langer, R. Transdermal drug delivery. Nat. Biotechnol. 2008, 26, 1261–1268. [Google Scholar] [CrossRef]
- Di Meglio, P.; Perera, G.K.; Nestle, F.O. The multitasking organ: Recent insights into skin immune function. Immunity 2011, 35, 857–869. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Ye, Y.; Wang, C.; Zhang, X.; Hu, Q.; Zhang, Y.; Liu, Q.; Wen, D.; Milligan, J.; Bellotti, A.; Huang, L. A melanin-mediated cancer immunotherapy patch. Sci. Immunol. 2017, 2, eaan5692. [Google Scholar] [CrossRef] [Green Version]
- Gu, Z.; Chen, X. Towards Enhancing Skin Drug Delivery. Adv. Drug Deliv. Rev. 2018, 127, 1–2. [Google Scholar] [CrossRef]
- Al-Kassas, R.; Wen, J.; Cheng, A.E.-M.; Kim, A.M.-J.; Liu, S.S.M.; Yu, J. Transdermal delivery of propranolol hydrochloride through chitosan nanoparticles dispersed in mucoadhesive gel. Carbohydr. Polym. 2016, 153, 176–186. [Google Scholar] [CrossRef] [PubMed]
- Tanner, T.; Marks, R.J.S.R. Technology, Delivering drugs by the transdermal route: Review and comment. Skin Res. Technol. 2008, 14, 249–260. [Google Scholar] [CrossRef] [PubMed]
- Ngo, H.V.; Tran, P.H.; Lee, B.-J.; Tran, T.T.J.N. Development of film-forming gel containing nanoparticles for transdermal drug delivery. Nanotechnology 2019, 30, 415102. [Google Scholar] [CrossRef]
- Mahato, R. Pharmaceutical Dosage Forms and Drug Delivery; CRS press: Boca Raton, FL, USA, 2002; Volume 6000, pp. 196–197. [Google Scholar]
- Thomas, B.; El Sohly, M.J. Chapter 3-medical cannabis formulations. In The Analytical Chemistry of Cannabis: Quality Assessment, Assurance, and Regulation of Medicinal Marijuana and Cannabinoid Preparations; Elsevier: Amsterdam, The Netherlands, 2016; Volume 1, pp. 43–61. [Google Scholar]
- Cichewicz, D.L.; Welch, S.P.; Smith, F.L. Enhancement of transdermal fentanyl and buprenorphine antinociception by transdermal Δ9-tetrahydrocannabinol. Eur. J. Pharmacol. 2005, 525, 74–82. [Google Scholar] [CrossRef]
- Wiedersberg, S.; Guy, R.H. Transdermal drug delivery: 30+ years of war and still fighting! J. Control. Release 2014, 190, 150–156. [Google Scholar] [CrossRef] [Green Version]
- Dosio, F.; Arpicco, S.; Stella, B.; Fattal, E. Hyaluronic acid for anticancer drug and nucleic acid delivery. Adv. Drug Deliv. Rev. 2016, 97, 204–236. [Google Scholar] [CrossRef]
- Fairbairn, J.; Liebmann, J.; Rowan, M.G. The stability of cannabis and its preparations on storage. J. Pharm. Pharmacol. Biochem. Behav. 1976, 28, 1–7. [Google Scholar] [CrossRef]
- Adusumilli, N.C.; Hazuka, E.L.; Friedman, A.J. Nanotechnology to deliver cannabinoids in dermatology. Precis. Nanomed. 2021, 4, 787–794. [Google Scholar] [CrossRef]
- Abrahamov, A.; Abrahamov, A.; Mechoulam, R. An efficient new cannabinoid antiemetic in pediatric oncology. Life Sci. 1995, 56, 2097–2102. [Google Scholar] [CrossRef]
- Razdan, R.K. Structure-activity relationships in cannabinoids. Pharmacol. Rev. 1986, 38, 75–149. [Google Scholar] [PubMed]
- Valiveti, S.; Hammell, D.C.; Earles, D.C.; Stinchcomb, A.L. In vitro/in vivo correlation studies for transdermal Δ8-THC development. J. Pharm. Sci. 2004, 93, 1154–1164. [Google Scholar] [CrossRef] [PubMed]
- Liput, D.J.; Hammell, D.C.; Stinchcomb, A.L.; Nixon, K. Transdermal delivery of cannabidiol attenuates binge alcohol-induced neurodegeneration in a rodent model of an alcohol use disorder. Pharmacol. Biochem. Behav. 2013, 111, 120–127. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Touitou, E.; Fabin, B.; Dany, S.; Almog, S. Transdermal delivery of tetrahydrocannabinol. Int. J. Pharm. 1988, 43, 9–15. [Google Scholar] [CrossRef]
- Casiraghi, A.; Musazzi, U.M.; Centin, G.; Franzè, S.; Minghetti, P. Topical Administration of Cannabidiol: Influence of Vehicle-Related Aspects on Skin Permeation Process. Pharmaceuticals 2020, 13, 337. [Google Scholar] [CrossRef]
- Park, C.; Zuo, J.; Somayaji, V.; Lee, B.-J.; Löbenberg, R. Development of a novel cannabinoid-loaded microemulsion towards an improved stability and transdermal delivery. Int. J. Pharm. 2021, 604, 120766. [Google Scholar] [CrossRef]
- Radwan-Pragłowska, J.; Janus, Ł.; Piątkowski, M.; Sierakowska, A.; Szajna, E.; Matýsek, D.; Bogdał, D. Development of Stimuli-Responsive Chitosan/ZnO NPs Transdermal Systems for Controlled Cannabidiol Delivery. Polymers 2021, 13, 211. [Google Scholar] [CrossRef]
- Marczewska, J.; Karwicka, E.; Drozd, J.; Anuszewskal, E.; Sliwinska, A.; Nosov, A.; Olszowska, O. Assessment of cyto-toxic and genotoxic activity of alcohol extract of polyscias filicifolia shoot, leaf, cell biomass of suspension culture and saponin fraction. Acta Pol. Pharm. 2011, 68, 703–710. [Google Scholar]
- Scheffer, I.E.; Hulihan, J.; Messenheimer, J.; Ali, S.; Keenan, N.; Griesser, J.; Gutterman, D.L.; Sebree, T.; Sadleir, L.G. Safety and Tolerability of Transdermal Cannabidiol Gel in Children with Developmental and Epileptic Encephalopathies: A Nonrandomized Controlled Trial. JAMA Netw. Open 2021, 4, e2123930. [Google Scholar] [CrossRef] [PubMed]
- Momekova, D.; Danov, Y.; Momekov, G.; Ivanov, E.; Petrov, P. Polysaccharide Cryogels Containing β-Cyclodextrin for the Delivery of Cannabidiol. Pharmaceutics 2021, 13, 1774. [Google Scholar] [CrossRef] [PubMed]
- Momekova, D.; Ivanov, E.; Konstantinov, S.; Ublekov, F.; Petrov, P.D. Nanocomposite Cryogel Carriers from 2-Hydroxyethyl Cellulose Network and Cannabidiol-Loaded Polymeric Micelles for Sustained Topical Delivery. Polymers 2020, 12, 1172. [Google Scholar] [CrossRef]
- Pavithra, P.S.; Mehta, A.; Verma, R.S. Synergistic interaction of β-caryophyllene with aromadendrene oxide 2 and phytol induces apoptosis on skin epidermoid cancer cells. Phytomedicine 2018, 47, 121–134. [Google Scholar] [CrossRef]
- Sharkawy, A.; Silva, A.M.; Rodrigues, F.; Barreiro, F.; Rodrigues, A. Pickering emulsions stabilized with chitosan/collagen peptides nanoparticles as green topical delivery vehicles for cannabidiol (CBD). Colloids Surf. A Physicochem. Eng. Asp. 2021, 631, 127677. [Google Scholar] [CrossRef]
- Vanti, G.; Grifoni, L.; Bergonzi, M.C.; Antiga, E.; Montefusco, F.; Caproni, M.; Bilia, A.R. Development and optimisation of biopharmaceutical properties of a new microemulgel of cannabidiol for locally-acting dermatological delivery. Int. J. Pharm. 2021, 607, 121036. [Google Scholar] [CrossRef]
- Cairns, E.A.; Baldridge, W.H.; Kelly, M.E.M. The endocannabinoid system as a therapeutic target in glaucoma. Neural Plast. 2016, 2016, 1–10. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Chelliah, M.P.; Zinn, Z.; Khuu, P.; Teng, J.M. Self-initiated use of topical cannabidiol oil for epidermolysis bullosa. Pediatr. Dermatol. 2018, 35, e224–e227. [Google Scholar] [CrossRef]
- Maida, V.; Corban, J. Topical medical cannabis: A new treatment for wound pain—Three cases of Pyoderma Gangrenosum. J. Pain Symptom Manag. 2017, 54, 732–736. [Google Scholar] [CrossRef] [Green Version]
- Bartner, L.R.; McGrath, S.; Rao, S.; Hyatt, L.K.; Wittenburg, L.A. Pharmacokinetics of cannabidiol administered by 3 delivery methods at 2 different dosages to healthy dogs. Can. J. Vet. Res. 2018, 82, 178–183. [Google Scholar]
- Scheuplein, R.J.; Blank, I.H. Mechanism of percutaneous absorption. IV. Penetration of nonelectrolytes (alcohols) from aqueous solutions and from pure liquids. J. Investig. Dermatol. 1973, 60, 286–296. [Google Scholar] [CrossRef] [Green Version]
- Challapalli, P.V.; Stinchcomb, A.L. In vitro experiment optimization for measuring tetrahydrocannabinol skin permeation. Int. J. Pharm. 2002, 241, 329–339. [Google Scholar] [CrossRef]
- Rabiei, M.; Kashanian, S.; Samavati, S.S.; Jamasb, S.; McInnes, S.J.P. Nanomaterial and advanced technologies in transdermal drug delivery. J. Drug Target. 2020, 28, 356–367. [Google Scholar] [CrossRef] [PubMed]
- Cristino, L.; Bisogno, T.; di Marzo, V. Cannabinoids and the expanded endocannabinoid system in neurological disorders. Nat. Rev. Neurol. 2019, 16, 1–21. [Google Scholar] [CrossRef] [PubMed]
- Mokoena, D.R.; George, B.P.; Abrahamse, H. Enhancing breast cancer treatment using a combination of cannabidiol and gold nanoparticles for photodynamic therapy. Int. J. Mol. Sci. 2019, 20, 4771. [Google Scholar] [CrossRef] [Green Version]
- Gujjar, M.; Arbiser, J.; Coulon, R.; Banga, A.K. Localized delivery of a lipophilic proteasome inhibitor into human skin for treatment of psoriasis. J. Drug Target. 2016, 24, 503–507. [Google Scholar] [CrossRef] [PubMed]
- Premjeet, S.; Bilandi, A.; Sahil, K.; Akanksha, M.; Bihani, S.G.L. Transdermal drug delivery system (patches), applications in present scenario. Int. J. Res. Pharm. Chem. 2011, 1, 1139–1151. [Google Scholar]
| Cannabinoids | Compounds |
|---|---|
| Plant-derived cannabinoids (phytocannabinoids) | THC, CBC, CBD, CBG, CBDV, THCV, THCAV, Δ-8-THC |
| Endocannabinoids | AEA, 2-AG, PEA, O-AEA, 2-AGE, 9-Octadecenamide |
| Synthetic cannabinoids | JWH-015, Dronabinol, Nabilone, WIN-55, 212-2, Rimonabant, CP55940, ACEA, Hu-308, AjA, (R)-methanandamide (MET) |
| Phytocannabinoids | Therapeutic Effects | Citations |
|---|---|---|
THC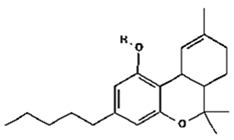 | Modulation of pain, spasticity, sedation, and mood; Bronchodilator; Neuroprotective and antioxidant; Antipruritic in cholestatic jaundice; Anti-inflammatory (power: 20× aspirin and 2× hydrocortisone); Analgesic; Anti-nausea/emesis (which is induced by chemotherapy); Appetite promoter Antitumorogenic | [10,11,12,13,14,15,16,17,18] |
CBD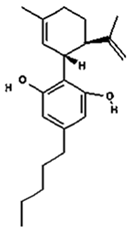 | Anticonvulsive; Anti-inflammatory and immunosuppressive (psoriasis, atopic dermatitis, and abrasions); Neuroprotective and antioxidative; Antipsychotic; Counteracts the intoxicating effects of cannabis; Anxiolytic; Addiction treatment; Antimicrobial (Gram-positives bacterial cutaneous infections); Antitumour | [11,12,14,17,18,19,20,21] |
CBG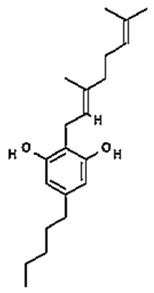 | Muscle relaxant; Analgesic; Antifungal (modest); Antineoplastic; Antidepressant; Inhibition of keratinocyte proliferation in psoriasis; Antibiotic activity against methicillin-resistant Staphylococcus aureus (MRSA); | [11,12,14,17,18,21] |
CBC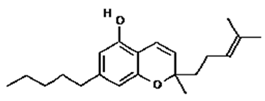 | Analgesic; Anti-inflammatory | [8,9,13] |
CBN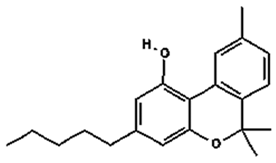 | Sedative; Anticonvulsive; Anti-inflammatory; Antibiotic (with anti-MRSA activity); Inhibition of keratinocyte proliferation; Osteogensis promoting | [11,12,14] |
THCV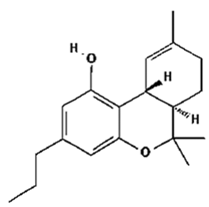 | Promotion of weight loss; Anticonvulsive; Suppression of hyperalgesia and inflammation; Appetite suppression; Counteracts the intoxicating effects of THC | [11,12,14] |
THCA-A | Immunomodulatory; Anti-inflammatory; Neuroprotective; Antineoplastic | [11,12,14] |
CBDV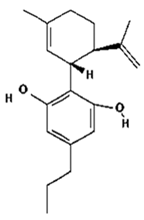 | Anticonvulsant | [11,12,14] |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Mahmoudinoodezh, H.; Telukutla, S.R.; Bhangu, S.K.; Bachari, A.; Cavalieri, F.; Mantri, N. The Transdermal Delivery of Therapeutic Cannabinoids. Pharmaceutics 2022, 14, 438. https://doi.org/10.3390/pharmaceutics14020438
Mahmoudinoodezh H, Telukutla SR, Bhangu SK, Bachari A, Cavalieri F, Mantri N. The Transdermal Delivery of Therapeutic Cannabinoids. Pharmaceutics. 2022; 14(2):438. https://doi.org/10.3390/pharmaceutics14020438
Chicago/Turabian StyleMahmoudinoodezh, Haleh, Srinivasa Reddy Telukutla, Sukhvir Kaur Bhangu, Ava Bachari, Francesca Cavalieri, and Nitin Mantri. 2022. "The Transdermal Delivery of Therapeutic Cannabinoids" Pharmaceutics 14, no. 2: 438. https://doi.org/10.3390/pharmaceutics14020438
APA StyleMahmoudinoodezh, H., Telukutla, S. R., Bhangu, S. K., Bachari, A., Cavalieri, F., & Mantri, N. (2022). The Transdermal Delivery of Therapeutic Cannabinoids. Pharmaceutics, 14(2), 438. https://doi.org/10.3390/pharmaceutics14020438








