68Ga-Radiolabeling and Pharmacological Characterization of a Kit-Based Formulation of the Gastrin-Releasing Peptide Receptor (GRP-R) Antagonist RM2 for Convenient Preparation of [68Ga]Ga-RM2
Abstract
:1. Introduction
2. Materials and Methods
2.1. Description of RM2 Kits
2.2. Stability of the RM2 Kits
2.3. Optimization of 68Ga Radiolabeling
3. Process Validation
3.1. Quality Control
3.2. Costs
4. In Vitro Characterization of [68Ga]Ga-RM2 Obtained from Kits
4.1. Lipophilicity
4.2. Cell Culture
4.3. Saturation Radioligand Binding Assay
4.4. Determination of Specific Cellular Internalization and Membrane-Bound Fraction of [68Ga]Ga-RM2
4.5. Determination of Cellular Efflux of [68Ga]Ga-RM2
4.6. Calcium Mobilization Assay
4.7. Statistical Analysis
5. Results
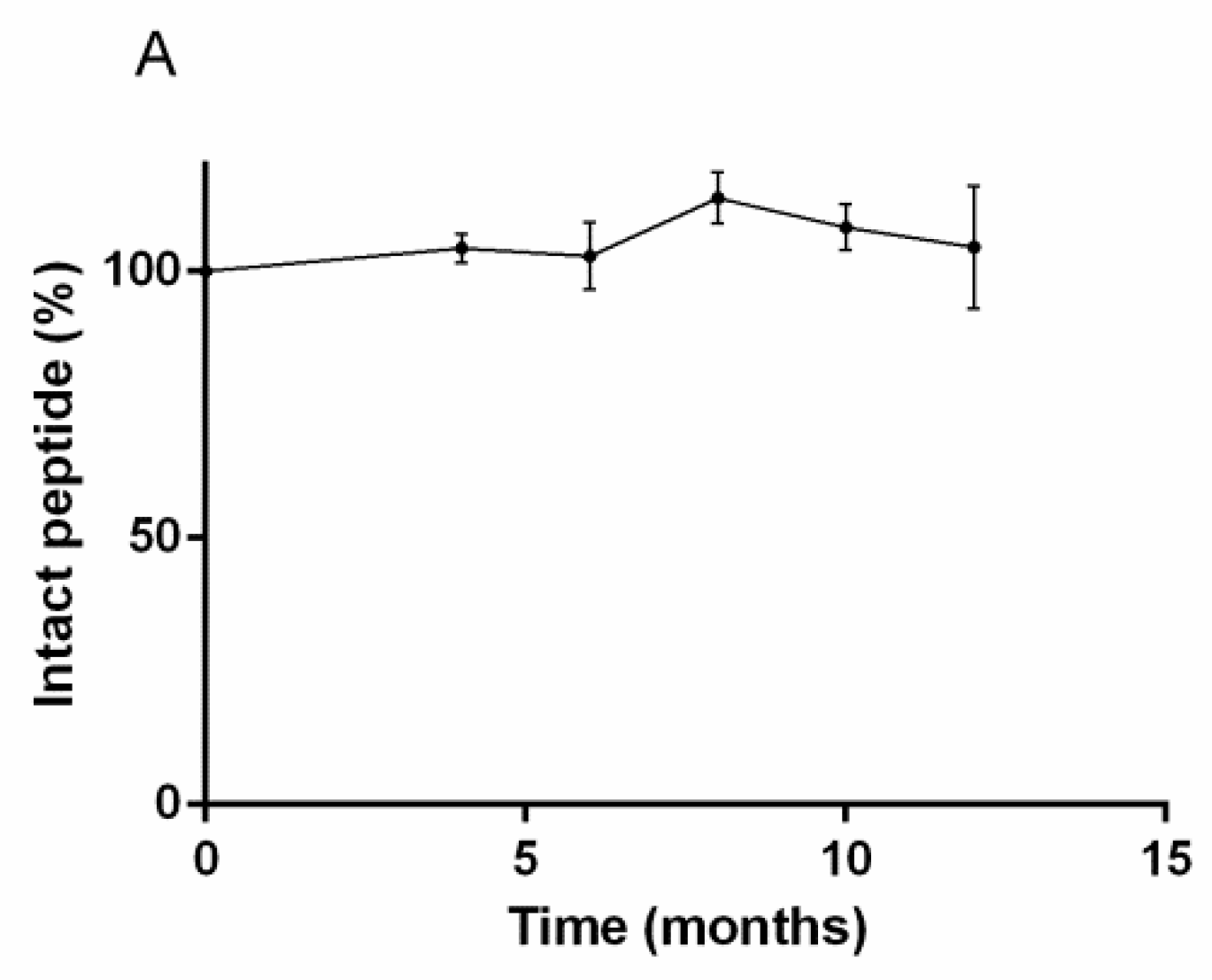
5.1. Stability of RM2 Kits
5.2. Optimization of RM2 Kits Radiolabeling with 68Ga
5.2.1. Influence of Reaction Volume
5.2.2. Influence of Heating Time
5.2.3. Influence of Temperature
5.2.4. Influence of Previous 4-h Generator Elution
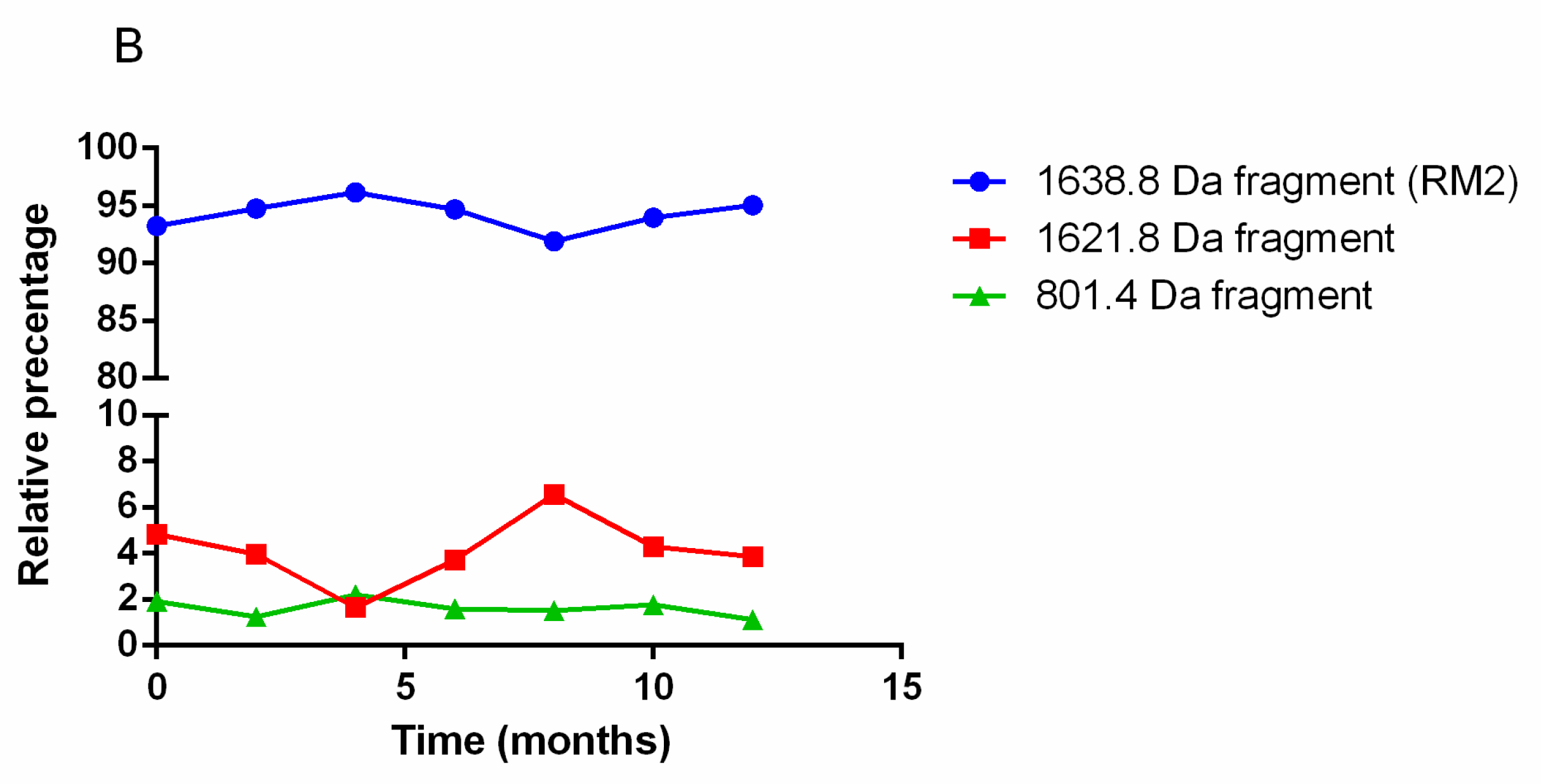
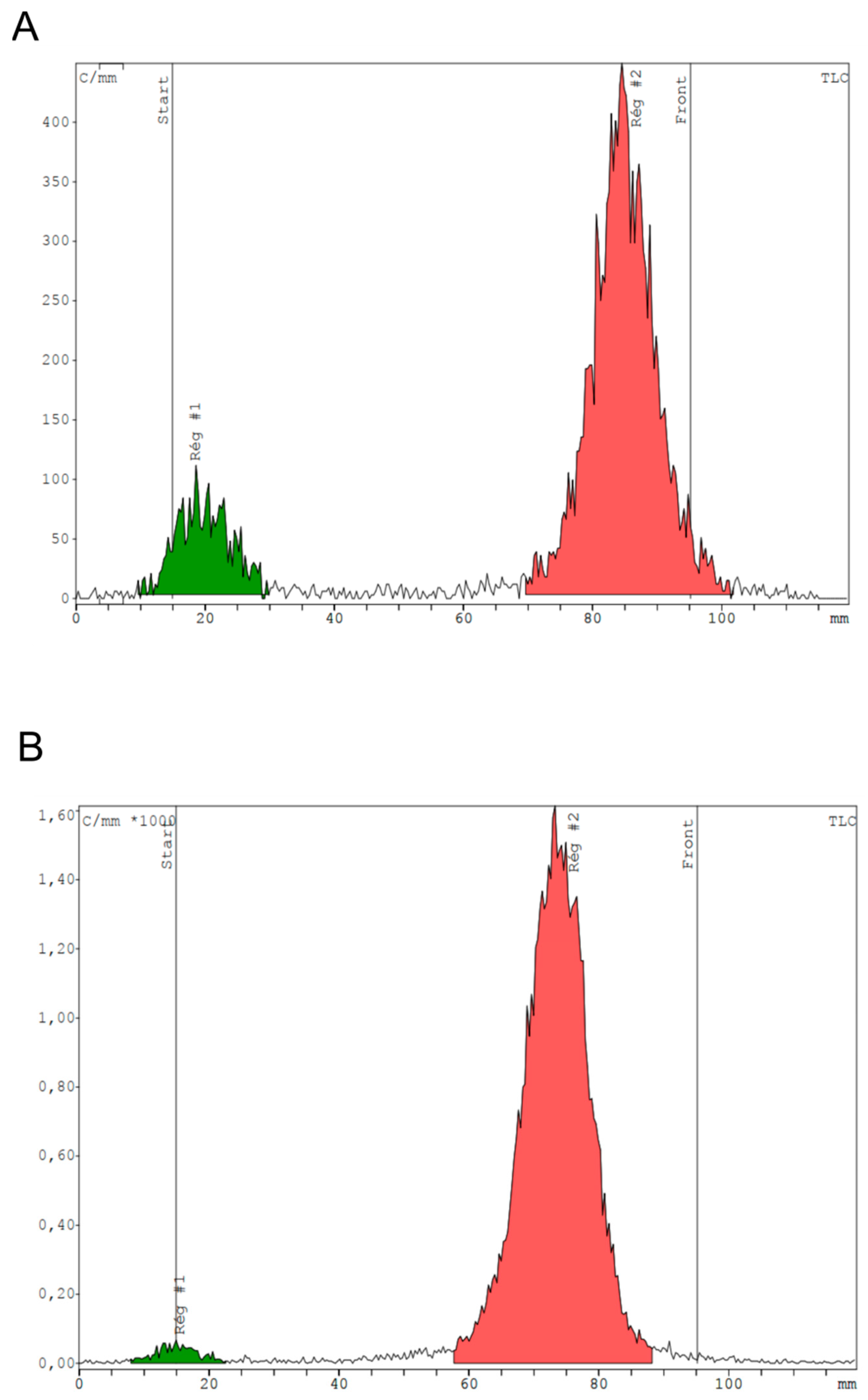
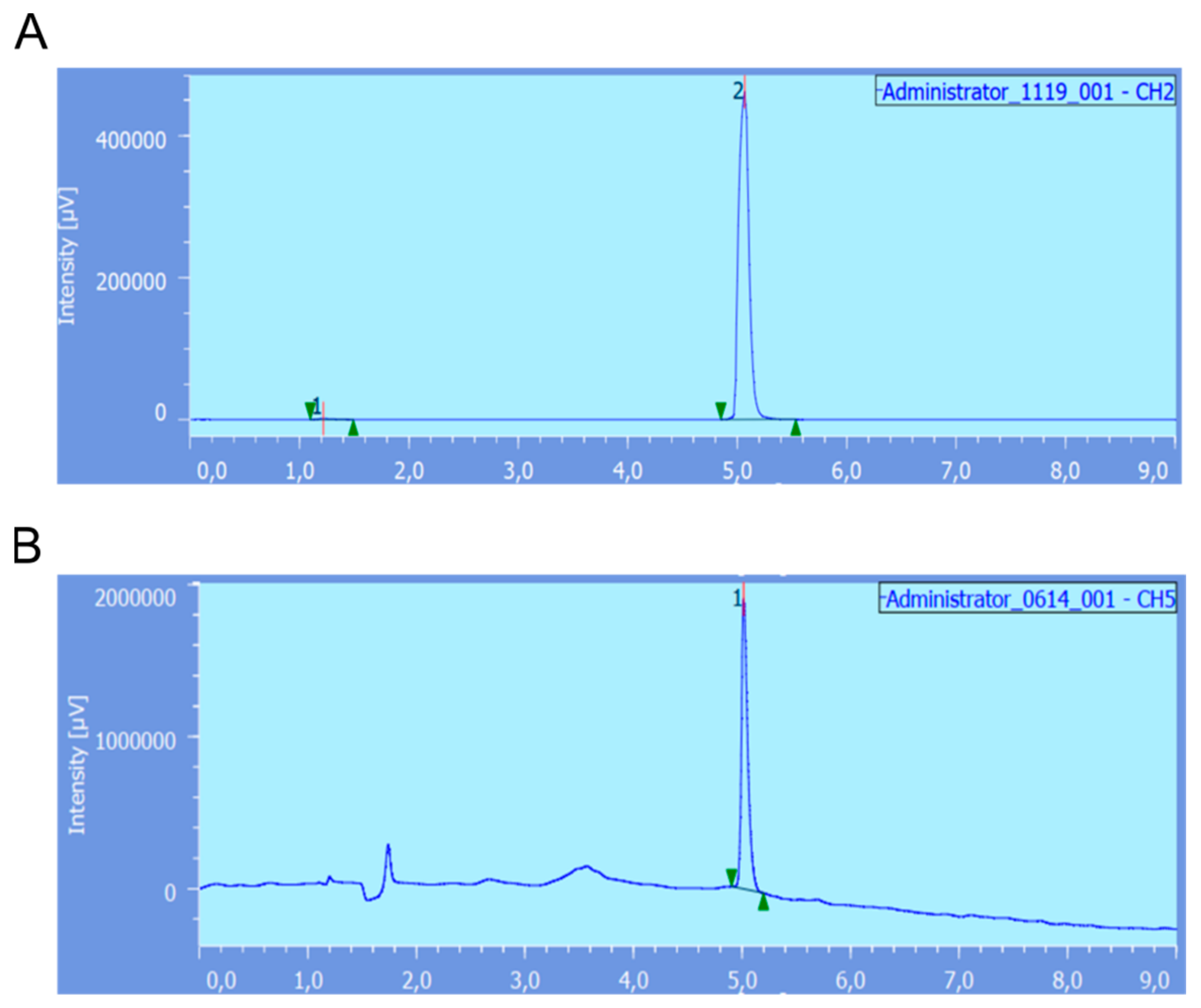
5.2.5. Quality Controls of [68Ga]Ga-RM2
6. Comparison of the Kit Formulation to the Module Production Route
7. Characterization of [68Ga]Ga-RM2 Produced by Kits
7.1. Determination of Lipophilicity
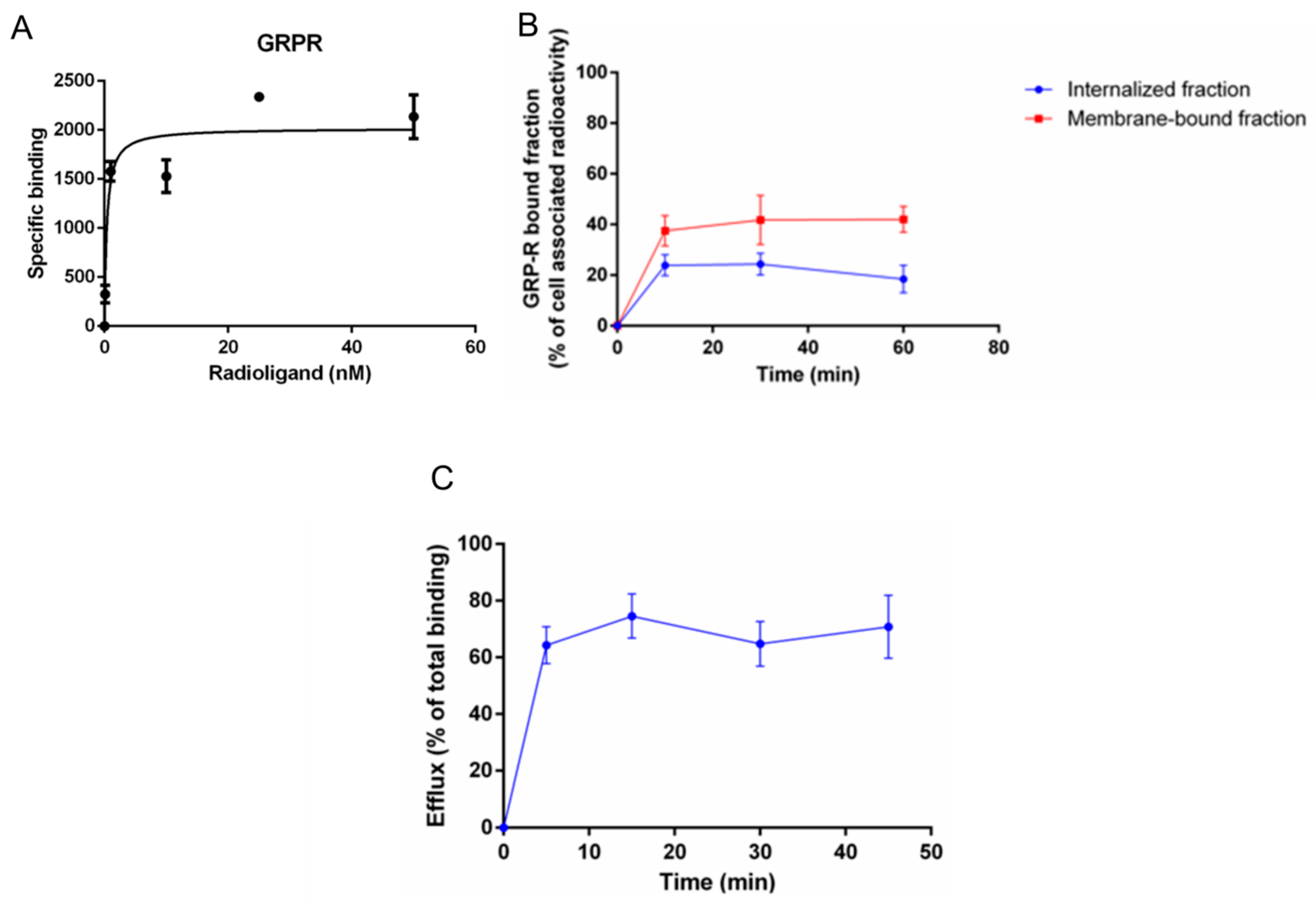
7.2. Saturation Radioligand Binding Assay
7.3. Determination of Cellular Internalization and Membrane-Bound Fraction of [68Ga]Ga-RM2
7.4. Determination of Cellular Efflux of [68Ga]Ga-RM2
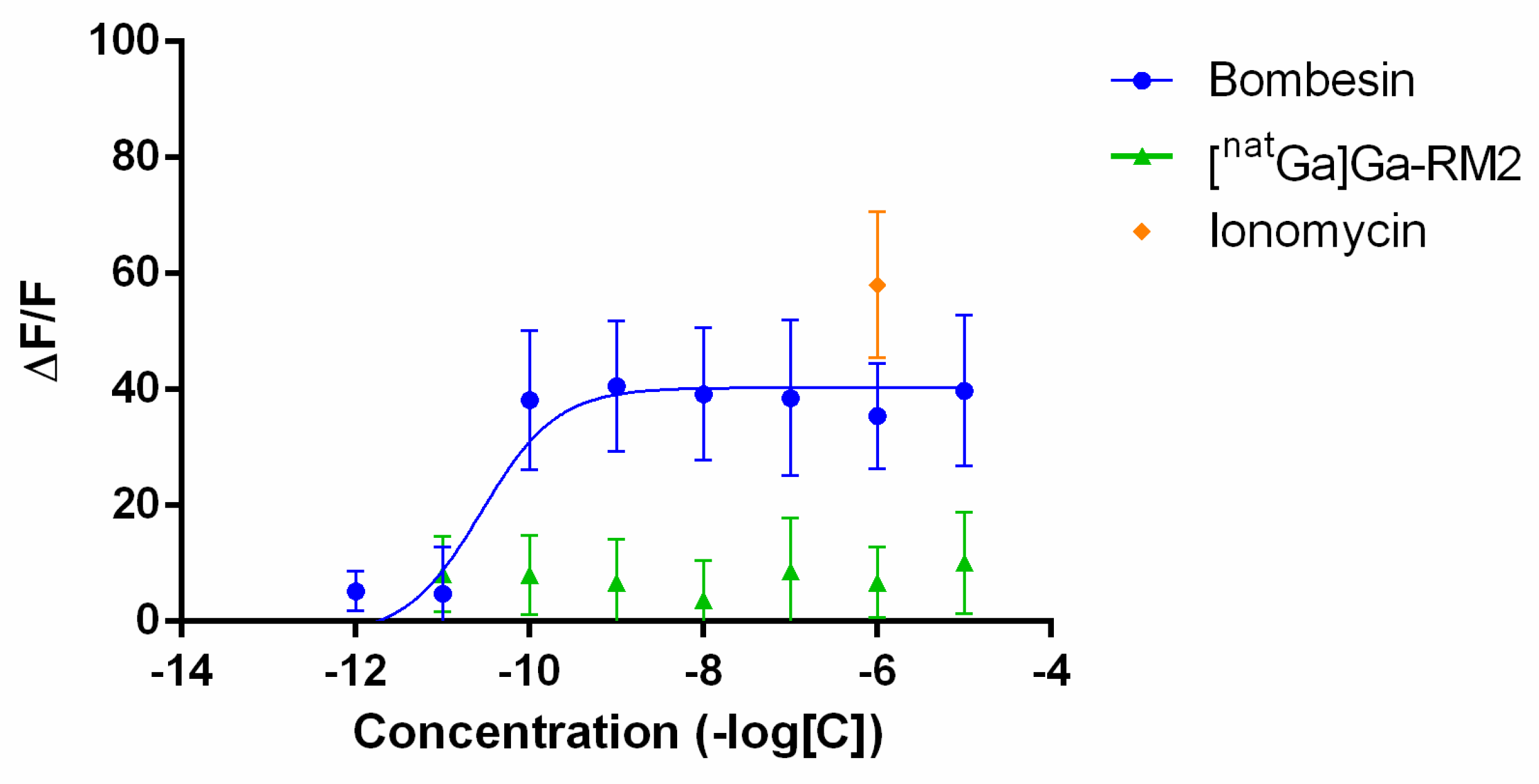
7.5. Intracellular Calcium Mobilization Assay
8. Discussion
9. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Morgat, C.; Mishra, A.K.; Varshney, R.; Allard, M.; Fernandez, P.; Hindié, E. Targeting Neuropeptide Receptors for Cancer Imaging and Therapy: Perspectives with Bombesin, Neurotensin, and Neuropeptide-Y Receptors. J. Nucl. Med. 2014, 55, 1650–1657. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Beer, M.; Montani, M.; Gerhardt, J.; Wild, P.J.; Hany, T.F.; Hermanns, T.; Müntener, M.; Kristiansen, G. Profiling gastrin-releasing peptide receptor in prostate tissues: Clinical implications and molecular correlates. Prostate 2012, 72, 318–325. [Google Scholar] [CrossRef]
- Körner, M.; Waser, B.; Rehmann, R.; Reubi, J.C. Early over-expression of GRP receptors in prostatic carcinogenesis. Prostate 2014, 74, 217–224. [Google Scholar] [CrossRef]
- Schollhammer, R.; Gallerande, H.D.; Yacoub, M.; Ranty, M.Q.; Barthe, N.; Vimont, D.; Hindié, E.; Fernandez, P.; Morgat, C. Comparison of the radiolabeled PSMA-inhibitor 111In-PSMA-617 and the radiolabeled GRP-R antagonist 111In-RM2 in primary prostate cancer samples. EJNMMI Res. 2019, 9, 52. [Google Scholar] [CrossRef]
- Touijer, K.A.; Michaud, L.; Alvarez, H.A.V.; Gopalan, A.; Kossatz, S.; Gonen, M.; Beattie, B.; Sandler, I.; Lyaschenko, S.; Eastham, J.A.; et al. Prospective Study of the Radiolabeled GRPR Antagonist BAY86-7548 for Positron Emission Tomography/Computed Tomography Imaging of Newly Diagnosed Prostate Cancer. Eur. Urol. Oncol. 2019, 2, 166–173. [Google Scholar] [CrossRef]
- Wieser, G.; Popp, I.; Rischke, H.C.; Drendel, V.; Grosu, A.; Bartholomä, M.; Weber, W.A.; Mansi, R.; Wetterauer, U.; Schultze-Seemann, W.; et al. Diagnosis of recurrent prostate cancer with PET/CT imaging using the gastrin-releasing peptide receptor antagonist 68Ga-RM2: Preliminary results in patients with negative or inconclusive [18F]Fluoroethylcholine-PET/CT. Eur. J. Nucl. Med. Mol. Imaging 2017, 44, 1463–1472. [Google Scholar] [CrossRef] [PubMed]
- Minamimoto, R.; Hancock, S.; Schneider, B.; Chin, F.T.; Jamali, M.; Loening, A.; Vasanawala, S.; Gambhir, S.S.; Iagaru, A. Pilot Comparison of 68Ga-RM2 PET and 68Ga-PSMA-11 PET in Patients with Biochemically Recurrent Prostate Cancer. J. Nucl. Med. 2016, 57, 557–562. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Kurth, J.; Krause, B.J.; Schwarzenböck, S.M.; Bergner, C.; Hakenberg, O.W.; Heuschkel, M. First-in-human dosimetry of gastrin-releasing peptide receptor antagonist [177Lu]Lu-RM2: A radiopharmaceutical for the treatment of metastatic castration-resistant prostate cancer. Eur. J. Nucl. Med. Mol. Imaging 2020, 47, 123–135. [Google Scholar] [CrossRef]
- Morgat, C.; MacGrogan, G.; Brouste, V.; Vélasco, V.; Sévenet, N.; Bonnefoi, H.; Fernandez, P.; Debled, M.; Hindié, E. Expression of Gastrin-Releasing Peptide Receptor in Breast Cancer and Its Association with Pathologic, Biologic, and Clinical Parameters: A Study of 1432 Primary Tumors. J. Nucl. Med. 2017, 58, 1401–1407. [Google Scholar] [CrossRef]
- Morgat, C.; Schollhammer, R.; Macgrogan, G.; Barthe, N.; Vélasco, V.; Vimont, D.; Cazeau, A.; Fernandez, P.; Hindié, E. Comparison of the binding of the gastrin-releasing peptide receptor (GRP-R) antagonist 68Ga-RM2 and 18F-FDG in breast cancer samples. PLoS ONE 2019, 14, e0210905. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Dalm, S.U.; Sieuwerts, A.M.; Look, M.P.; Melis, M.; van Deurzen, C.H.M.; Foekens, J.A.; de Jong, M.; Martens, J.W.M. Clinical Relevance of Targeting the Gastrin-Releasing Peptide Receptor, Somatostatin Receptor 2, or Chemokine C-X-C Motif Receptor 4 in Breast Cancer for Imaging and Therapy. J. Nucl. Med. 2015, 56, 1487–1493. [Google Scholar] [CrossRef] [Green Version]
- Stoykow, C.; Erbes, T.; Maecke, H.R.; Bulla, S.; Bartholomä, M.; Mayer, S.; Drendel, V.; Bronsert, P.; Werner, M.; Gitsch, G.; et al. Gastrin-releasing Peptide Receptor Imaging in Breast Cancer Using the Receptor Antagonist 68Ga-RM2 And PET. Theranostics 2016, 6, 1641–1650. [Google Scholar] [CrossRef] [PubMed]
- Baratto, L.; Duan, H.; Mäcke, H.; Iagaru, A. Imaging the Distribution of Gastrin-Releasing Peptide Receptors in Cancer. J. Nucl. Med. 2020, 61, 792–798. [Google Scholar] [CrossRef]
- Gruber, L.; Jiménez-Franco, L.D.; Decristoforo, C.; Uprimny, C.; Glatting, G.; Hohenberger, P.; Schoenberg, S.O.; Reindl, W.; Orlandi, F.; Mariani, M.; et al. MITIGATE-NeoBOMB1, a Phase I/IIa Study to Evaluate Safety, Pharmacokinetics, and Preliminary Imaging of 68Ga-NeoBOMB1, a Gastrin-Releasing Peptide Receptor Antagonist, in GIST Patients. J. Nucl. Med. 2020, 61, 1749–1755. [Google Scholar] [CrossRef] [PubMed]
- Schollhammer, R.; de Clermont, G.H.; Robert, G.; Yacoub, M.; Vimont, D.; Hindié, E.; Fernandez, P.; Morgat, C. 68Ga-PSMA-617 Compared With 68Ga-RM2 and 18F-FCholine PET/CT for the Initial Staging of High-Risk Prostate Cancer. Clin. Nucl. Med. 2019, 44, e535–e536. [Google Scholar] [CrossRef] [PubMed]
- Hennrich, U.; Benešová, M. [68Ga]Ga-DOTA-TOC: The First FDA-Approved 68Ga-Radiopharmaceutical for PET Imaging. Pharmaceuticals 2020, 13, 38. [Google Scholar] [CrossRef] [Green Version]
- Calderoni, L.; Farolfi, A.; Pianori, D.; Maietti, E.; Cabitza, V.; Lambertini, A.; Ricci, G.; Telo, S.; Lodi, F.; Castellucci, P.; et al. Evaluation of an Automated Module Synthesis and a Sterile Cold Kit–Based Preparation of 68Ga-PSMA-11 in Patients with Prostate Cancer. J. Nucl. Med. 2020, 61, 716–722. [Google Scholar] [CrossRef] [Green Version]
- Hofman, M.S.; Eu, P.; Jackson, P.; Hong, E.; Binns, D.; Iravani, A.; Murphy, D.; Mitchell, C.; Siva, S.; Hicks, R.J.; et al. Cold Kit for Prostate-Specific Membrane Antigen (PSMA) PET Imaging: Phase 1 Study of 68Ga-Tris(Hydroxypyridinone)-PSMA PET/CT in Patients with Prostate Cancer. J. Nucl. Med. 2018, 59, 625–631. [Google Scholar] [CrossRef] [Green Version]
- Jannsen, J.; Zerna, M.; Schieferstein, H.; Bickel, E.-M.; Oden, F.; Kiessling, N.; Berndt, M.; Muelle, A. Comparison of [68Ga] and [177Lu] labelled RM2 and NeoBOMB1–A Preclinical Study; Abstract 840, EMIM; European Society for Molecular Imaging: Glasgow, UK, 2019. [Google Scholar]
- Mansi, R.; Wang, X.; Forrer, F.; Waser, B.; Cescato, R.; Graham, K.; Borkowski, S.; Reubi, J.C.; Maecke, H.R. Development of a potent DOTA-conjugated bombesin antagonist for targeting GRPr-positive tumours. Eur. J. Nucl. Med. Mol. Imaging 2011, 38, 97–107. [Google Scholar] [CrossRef] [Green Version]
- Velikyan, I. Prospective of 68Ga-Radiopharmaceutical Development. Theranostics 2013, 4, 47–80. [Google Scholar] [CrossRef] [Green Version]
- Sudbrock, F.; Fischer, T.; Zimmermanns, B.; Guliyev, M.; Dietlein, M.; Drzezga, A.; Schomäcker, K. Characterization of SnO2-based 68Ge/68Ga generators and 68Ga-DOTATATE preparations: Radionuclide purity, radiochemical yield and long-term constancy. EJNMMI Res. 2014, 4, 36. [Google Scholar] [CrossRef] [Green Version]
- Morgat, C.; Hindié, E.; Mishra, A.K.; Allard, M.; Fernandez, P. Gallium-68: Chemistry and Radiolabeled Peptides Exploring Different Oncogenic Pathways. Cancer Biother. Radiopharm. 2013, 28, 85–97. [Google Scholar] [CrossRef] [PubMed]
- Vats, K.; Sharma, R.; Kameswaran, M.; Satpati, D.; Dash, A. Single vial cold kits optimized for preparation of gastrin releasing peptide receptor (GRPR)-radioantagonist 68Ga-RM2 using three different 68Ge/68Ga generators. J. Pharm. Biomed. Anal. 2019, 163, 39–44. [Google Scholar] [CrossRef]
- Fani, M.; Braun, F.; Waser, B.; Beetschen, K.; Cescato, R.; Erchegyi, J.; Rivier, J.E.; Weber, W.A.; Maecke, H.R.; Reubi, J.C. Unexpected Sensitivity of sst2 Antagonists to N-Terminal Radiometal Modifications. J. Nucl. Med. 2012, 53, 1481–1489. [Google Scholar] [CrossRef] [Green Version]
- Chastel, A.; Worm, D.J.; Alves, I.D.; Vimont, D.; Petrel, M.; Fernandez, S.; Garrigue, P.; Fernandez, P.; Hindié, E.; Beck-Sickinger, A.G.; et al. Design, synthesis, and biological evaluation of a multifunctional neuropeptide-Y conjugate for selective nuclear delivery of radiolanthanides. EJNMMI Res. 2020, 10, 16. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Popp, I.; Del Pozzo, L.; Waser, B.; Reubi, J.C.; Meyer, P.T.; Maecke, H.R.; Gourni, E. Approaches to improve metabolic stability of a statine-based GRP receptor antagonist. Nucl. Med. Biol. 2017, 45, 22–29. [Google Scholar] [CrossRef]
| Test | Specifications | Batch 1 | Batch 2 | Batch 3 |
|---|---|---|---|---|
| Volumetric activity (MBq/mL) | na | 22.65 | 28.00 | 20.23 |
| Molar activity (GBq/µmol) | na | 8.29 | 5.8 | 7.6 |
| Appearance | Clear and colourless | Complies | Complies | Complies |
| pH | 4–8 | 4.7 | 4.7 | 4.7 |
| Identification of 68Ga | 511/1022/1077 keV | Complies | Complies | Complies |
| 62–74 min | 67.17 | 67.90 | 67.61 | |
| Radiochemical purity (%) | ≥91 (HPLC) | 97.5 | 98.6 | 95.1 |
| ≥91 (TLC) | 95.3 | 98.3 | 94.4 | |
| Amount of [68Ga]Ga-RM2 (µg) | <50 | 38.1 | 45.3 | 31.8 |
| Bubble point test | ≥3.4 bars | 3.6 | 3.6 | 3.7 |
| Bacterial endotoxins (EU/mL) | <17.5 | <5 | <5 | <5 |
| Sterility | Sterile | Complies | Complies | Complies |
| Cost per Synthesis (€) MODULE | Cost per Synthesis (€) KIT | ||
|---|---|---|---|
| Chemicals | Water for chromatography | 5.8 | |
| Ethanol | 0.18 | ||
| Sodium acetate | 0.22 | 0.003 | |
| Hydrochloric acid | 0.83 | ||
| Sodium hydrogenophophate | 0.002 | 0.002 | |
| Sodium chloride | 0.14 | 0.0001 | |
| NaCl 0.9% | 0.72 | 0.72 | |
| Potassium dihydrogenophosphate | 0.0006 | 0.0006 | |
| Trifluoro acetic acid | 0.99 | 0.99 | |
| Consumables | Module cassette (including tubes, etc…) | 197.5 | |
| C18 sep-pack | 4.24 | ||
| Needles | 0.28 | 0.66 | |
| Syringes | 1.05 | 0.48 | |
| Pipette tips | 0.81 | ||
| Gloves | 0.39 | 0.39 | |
| Vials | 16.14 | 8.07 | |
| Filters | 1.94 | 1.94 | |
| Endotoxins cartridges | 51.6 | 51.6 | |
| Total | 282.1 | 65.7 | |
| [68Ga]Ga-RM2 | [111In]In-RM2 | [177Lu]Lu-RM2 | |
|---|---|---|---|
| LogD7.4 | −2.54 ± 0.04 | nd | nd |
| Affinity (Kd in nM) | 0.25 ± 0.19 | 2.9 ± 0.4 | nd |
| Membrane bound fraction (%) | 42.0 ± 5.1 (1 h) | 15.9 ± 0.9 (4 h) | 11.2 ± 0.8 (4 h) |
| Internalization (%) | 18.5 ± 5.4 (1 h) | 3.7 ± 0.4 (4 h) | 4.5 ± 0.6 (4 h) |
| Efflux (%) | 70.8 ± 11.1 (45 min) | nd | nd |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Chastel, A.; Vimont, D.; Claverol, S.; Zerna, M.; Bodin, S.; Berndt, M.; Chaignepain, S.; Hindié, E.; Morgat, C. 68Ga-Radiolabeling and Pharmacological Characterization of a Kit-Based Formulation of the Gastrin-Releasing Peptide Receptor (GRP-R) Antagonist RM2 for Convenient Preparation of [68Ga]Ga-RM2. Pharmaceutics 2021, 13, 1160. https://doi.org/10.3390/pharmaceutics13081160
Chastel A, Vimont D, Claverol S, Zerna M, Bodin S, Berndt M, Chaignepain S, Hindié E, Morgat C. 68Ga-Radiolabeling and Pharmacological Characterization of a Kit-Based Formulation of the Gastrin-Releasing Peptide Receptor (GRP-R) Antagonist RM2 for Convenient Preparation of [68Ga]Ga-RM2. Pharmaceutics. 2021; 13(8):1160. https://doi.org/10.3390/pharmaceutics13081160
Chicago/Turabian StyleChastel, Adrien, Delphine Vimont, Stephane Claverol, Marion Zerna, Sacha Bodin, Mathias Berndt, Stéphane Chaignepain, Elif Hindié, and Clément Morgat. 2021. "68Ga-Radiolabeling and Pharmacological Characterization of a Kit-Based Formulation of the Gastrin-Releasing Peptide Receptor (GRP-R) Antagonist RM2 for Convenient Preparation of [68Ga]Ga-RM2" Pharmaceutics 13, no. 8: 1160. https://doi.org/10.3390/pharmaceutics13081160
APA StyleChastel, A., Vimont, D., Claverol, S., Zerna, M., Bodin, S., Berndt, M., Chaignepain, S., Hindié, E., & Morgat, C. (2021). 68Ga-Radiolabeling and Pharmacological Characterization of a Kit-Based Formulation of the Gastrin-Releasing Peptide Receptor (GRP-R) Antagonist RM2 for Convenient Preparation of [68Ga]Ga-RM2. Pharmaceutics, 13(8), 1160. https://doi.org/10.3390/pharmaceutics13081160







