The Use of a Non-Conventional Long-Lived Gallium Radioisotope 66Ga Improves Imaging Contrast of EGFR Expression in Malignant Tumours Using DFO-ZEGFR:2377 Affibody Molecule
Abstract
1. Introduction
2. Materials and Methods
2.1. Production of 66Ga
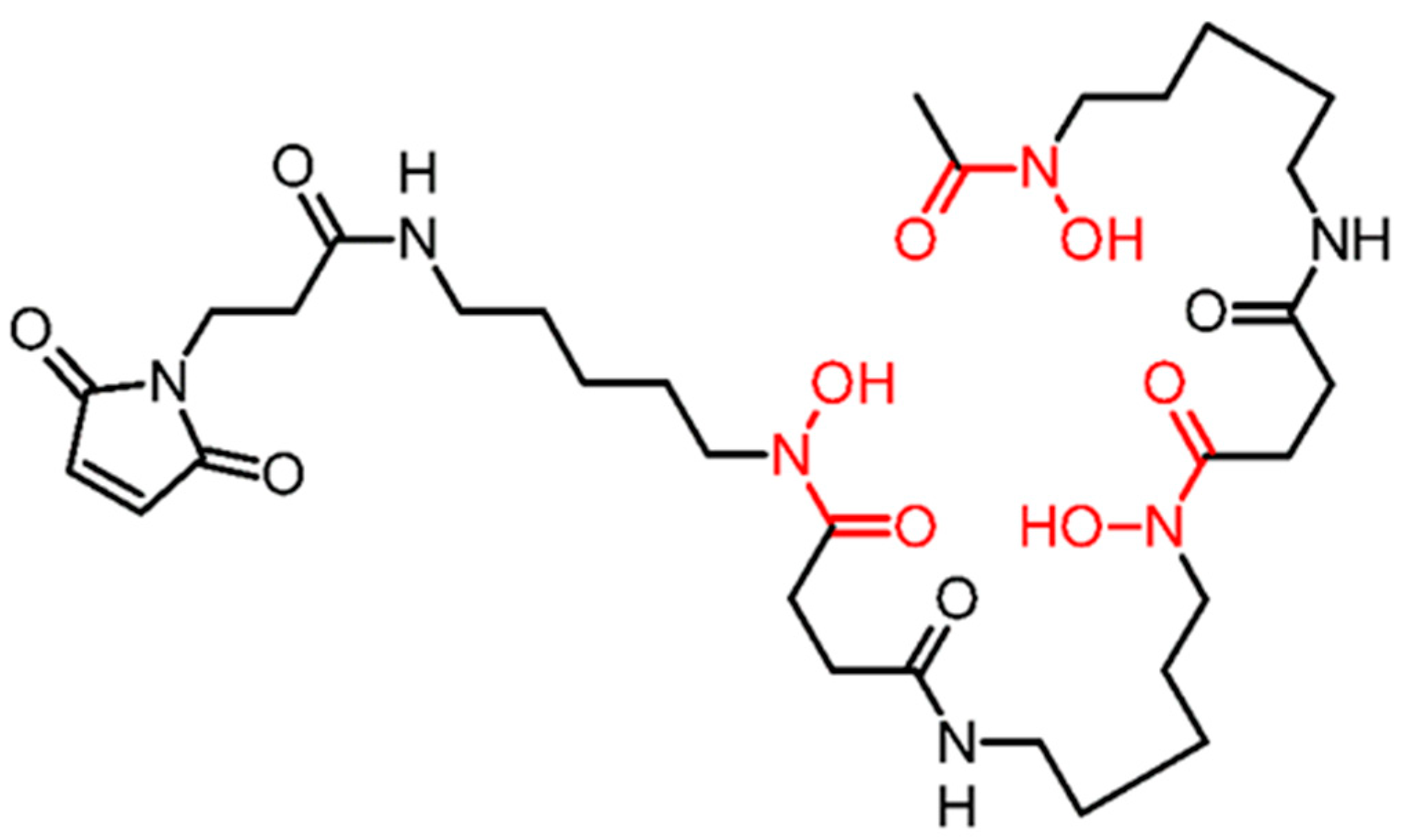
2.2. Radiolabelling and In Vitro Stability
2.3. In Vitro Studies
2.4. In Vivo Studies
3. Results
3.1. Nuclide Production and Radiolabelling
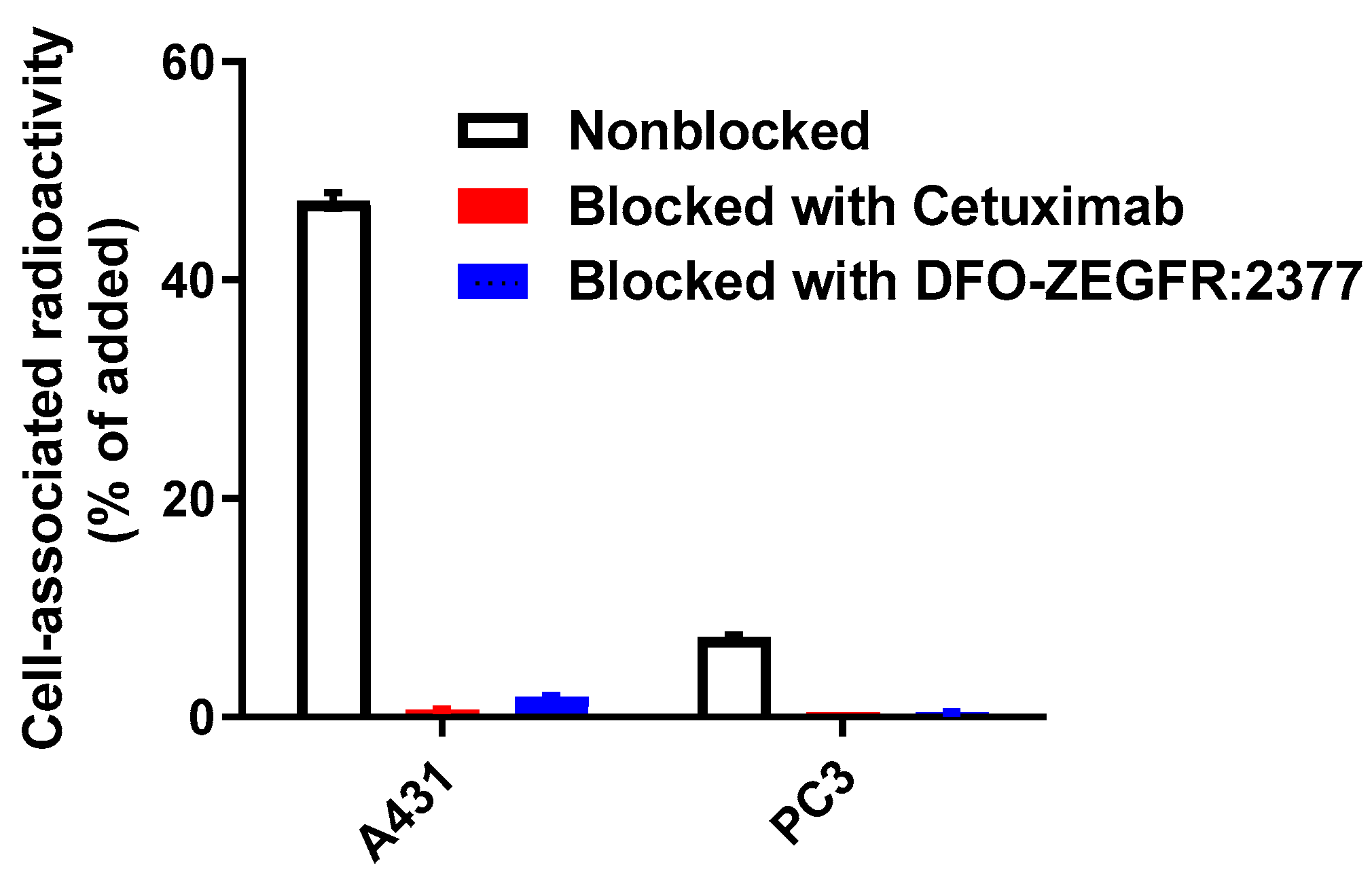
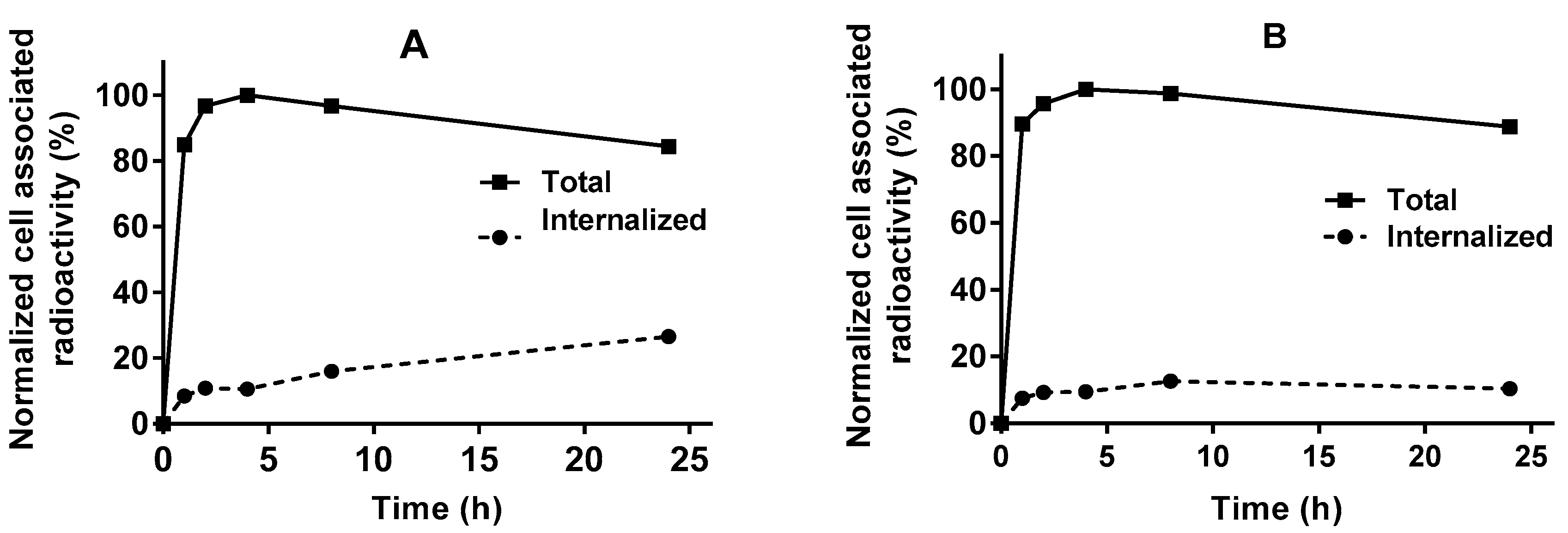
3.2. In Vitro Studies
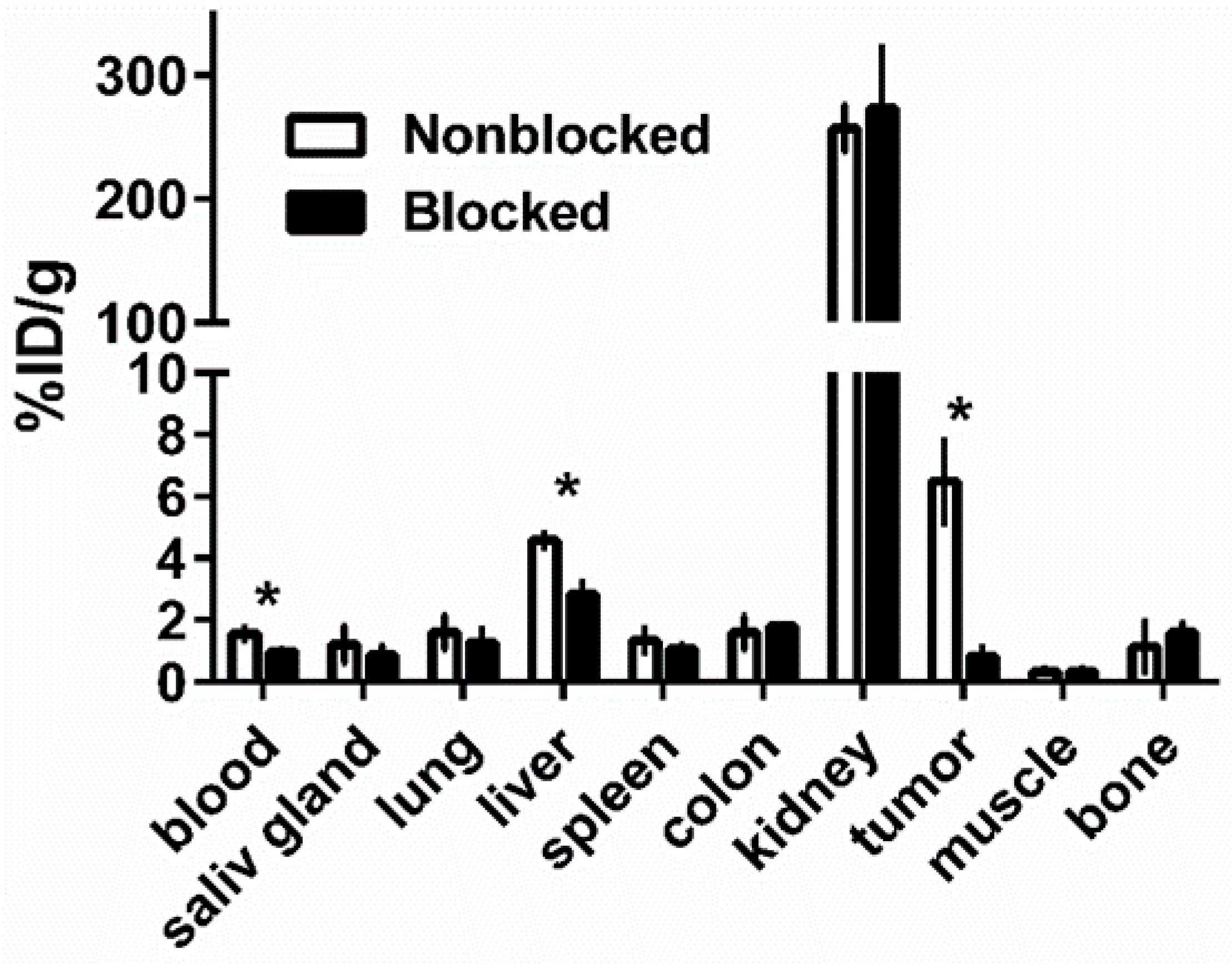
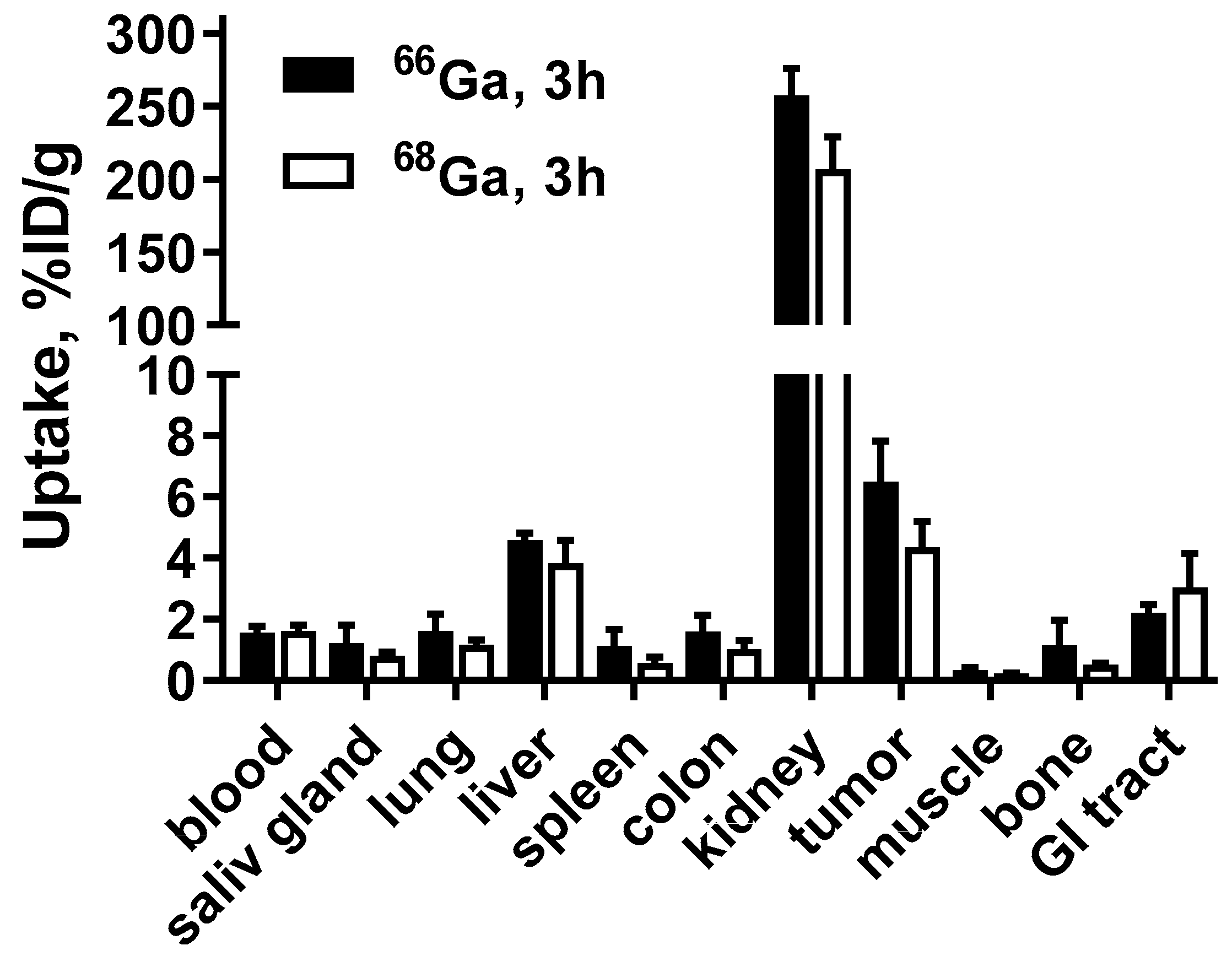
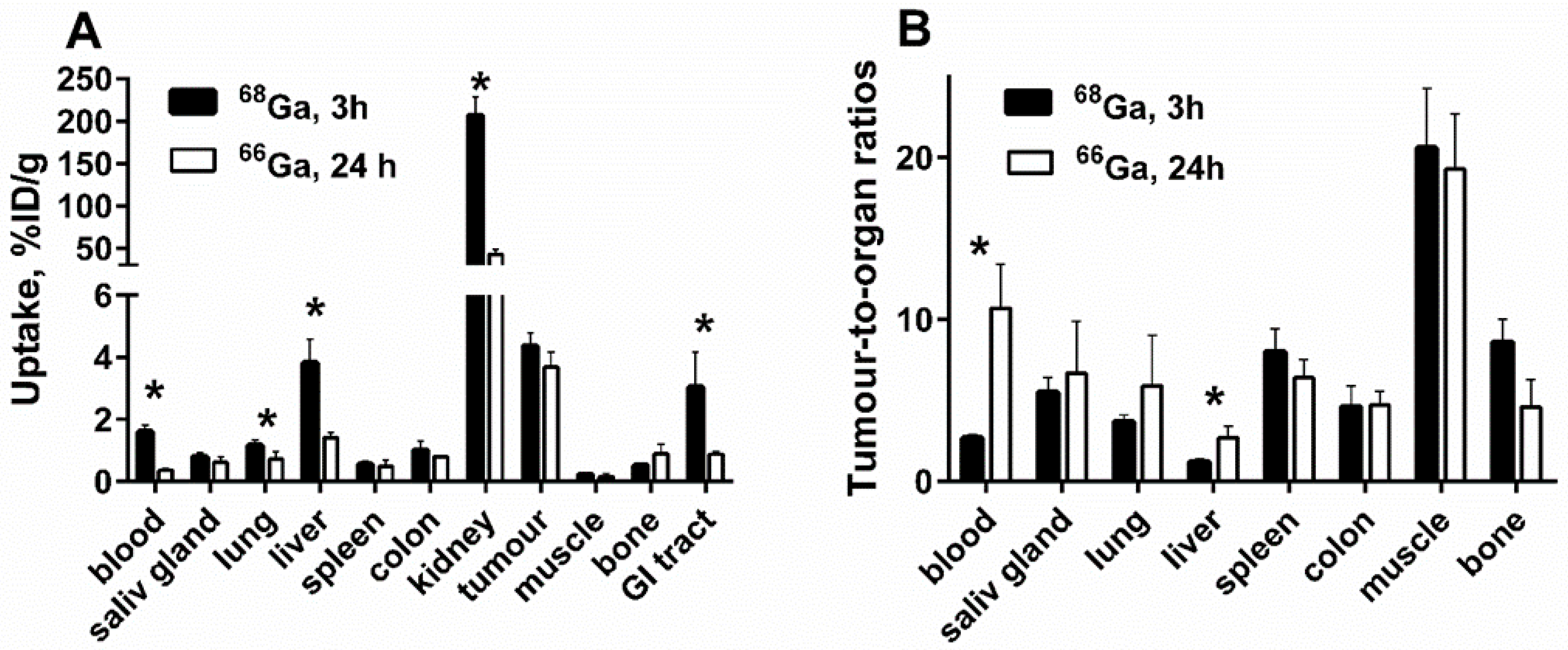
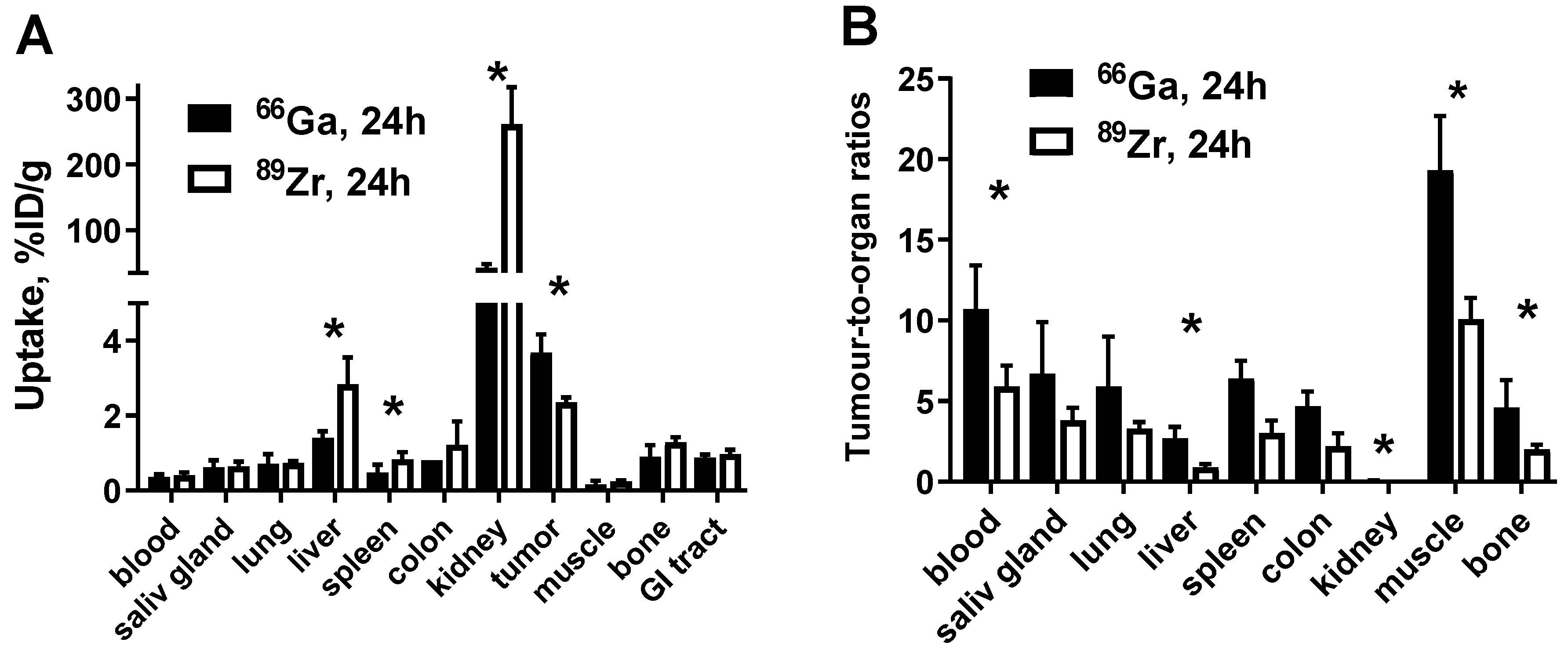
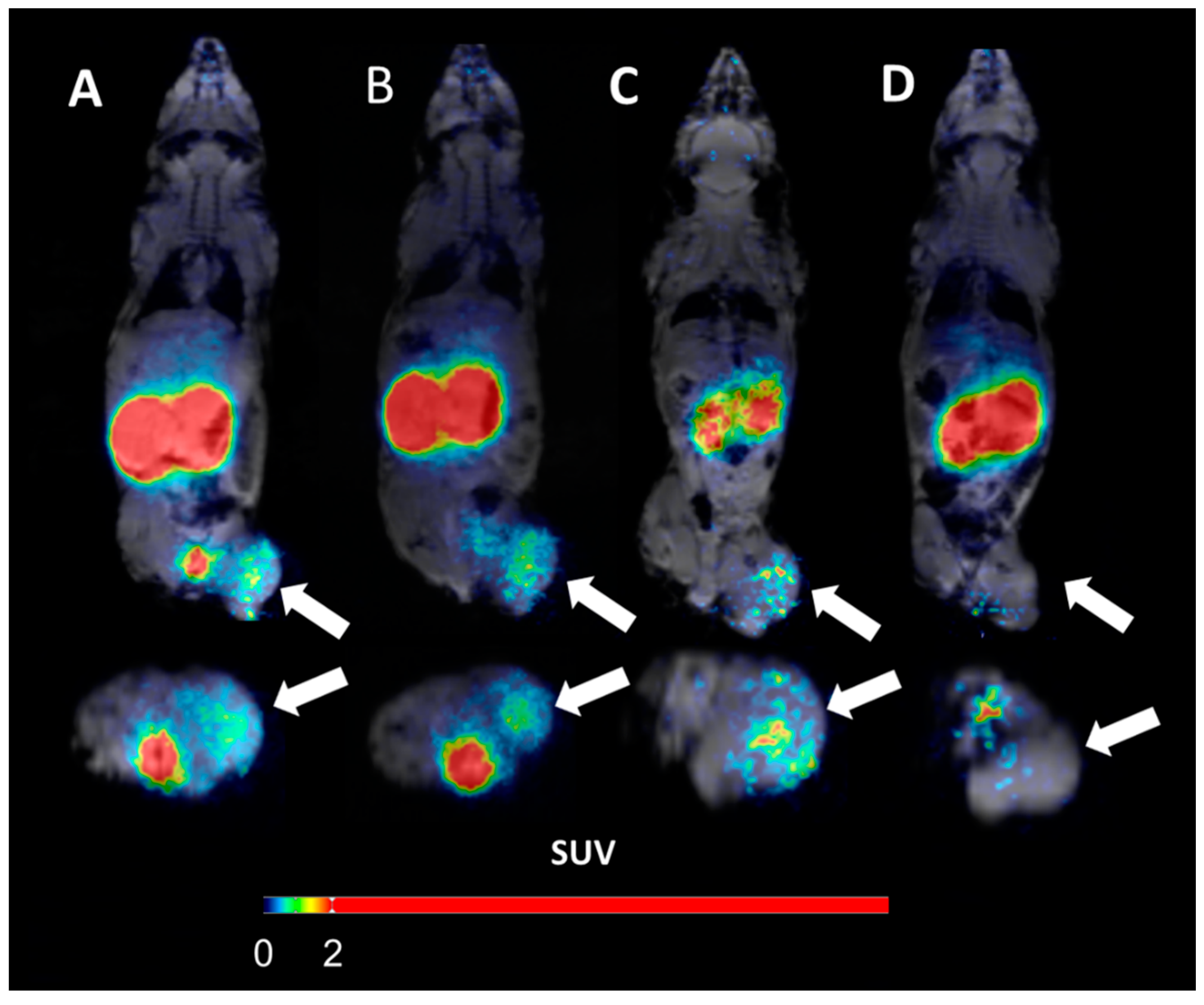
3.3. In Vivo Studies
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Roskoski, R., Jr. The ErbB/HER family of protein-tyrosine kinases and cancer. Pharmacol. Res. 2014, 79, 34–74. [Google Scholar] [CrossRef] [PubMed]
- Yarden, Y.; Sliwkowski, M.X. Untangling the ErbB signalling network. Nat. Rev. Mol. Cell. Biol. 2001, 2, 127–137. [Google Scholar] [CrossRef] [PubMed]
- Yewale, C.; Baradia, D.; Vhora, I.; Patil, S.; Misra, A. Epidermal growth factor receptor targeting in cancer: A review of trends and strategies. Biomaterials 2013, 34, 8690–8707. [Google Scholar] [CrossRef]
- Scartozzi, M.; Bearzi, I.; Berardi, R.; Mandolesi, A.; Fabris, G.; Cascinu, S. Epidermal growth factor receptor (EGFR) status in primary colorectal tumors does not correlate with EGFR expression in related metastatic sites: Implications for treatment with EGFR-targeted monoclonal antibodies. J. Clin. Oncol. 2004, 22, 4772–4778. [Google Scholar] [CrossRef]
- Kersting, C.; Packeisen, J.; Leidinger, B.; Brandt, B.; Von Wasielewski, R.; Winkelmann, W.; Van Diest, P.J.; Gosheger, G.; Buerger, H. Pitfalls in immunohistochemical assessment of EGFR expression in soft tissue arcomas. J. Clin. Pathol. 2006, 59, 585–590. [Google Scholar] [CrossRef]
- Choong, L.Y.; Lim, S.; Loh, M.C.; Man, X.; Chen, Y.; Toy, W.; Pan, M.; Chen, C.S.; Poonepalli, A.; Hande, M.P.; et al. Progressive loss of epidermal growth factor receptor in a subpopulation of breast cancers: Implications in target-directed therapeutics. Mol. Cancer Ther. 2007, 6, 2828–2842. [Google Scholar] [CrossRef] [PubMed]
- Divgi, C.R.; Welt, S.; Kris, M.; Real, F.X.; Yeh, S.D.; Gralla, R.; Merchant, B.; Schweighart, S.; Unger, M.; Larson, S.M.; et al. Phase I and imaging trial of indium 111-labeled anti-epidermal growth factor receptor monoclonal antibody 225 in patients with squamous cell lung carcinoma. J. Natl. Cancer Inst. 1991, 83, 97–104. [Google Scholar] [CrossRef]
- Aerts, H.J.; Dubois, L.; Perk, L.; Vermaelen, P.; Van Dongen, G.A.; Wouters, B.G.; Lambin, P. Disparity between in vivo EGFR expression and 89Zr-labeled cetuximab uptake assessed with PET. J. Nucl. Med. 2009, 50, 123–131. [Google Scholar] [CrossRef]
- Cai, W.; Chen, K.; He, L.; Cao, Q.; Koong, A.; Chen, X. Quantitative PET of EGFR expression in xenograft-bearing mice using 64Cu labeled cetuximab, a chimeric anti-EGFR monoclonal antibody. Eur. J. Nucl. Med. Mol. Imaging 2007, 34, 850–858. [Google Scholar] [CrossRef]
- Kim, E.; Kim, B.S.; Choi, D.B.; Chi, S.G.; Choi, T.H. Enhanced tumor retention of radioiodinated anti-epidermal growth factor receptor antibody using novel bifunctional iodination linker for radioimmunotherapy. Oncol. Rep. 2016, 35, 3159. [Google Scholar] [CrossRef]
- Shih, B.B.; Chang, Y.F.; Cheng, C.C.; Yang, H.J.; Chang, K.W.; Ho, A.S.; Lin, H.C.; Yeh, C.; Chang, C.C. SPECT imaging evaluation of (111)indium-chelated cetuximab for diagnosing EGFR positive tumor in an HCT-15-induced colorectal xenograft. J. Chin. Med. Assoc. 2017, 80, 766–773. [Google Scholar] [CrossRef]
- Chang, A.J.; De Silva, R.A.; Lapi, S.E. Development and characterization of 89Zr-labeled panitumumab for immuno-positron emission tomographic imaging of the epidermal growth factor receptor. Mol. Imaging 2013, 12, 17–27. [Google Scholar] [PubMed]
- Nayak, T.K.; Garmestani, K.; Baidoo, K.E.; Milenic, D.E.; Brechbiel, M.W. Preparation, biological evaluation, and pharmacokinetics of the human anti-HER1 monoclonal antibody panitumumab labeled with 86Y for quantitative PET of carcinoma. J. Nucl. Med. 2010, 51, 942–950. [Google Scholar] [CrossRef] [PubMed]
- Cheson, B.D. Radioimmunotherapy of non-Hodgkin lymphomas. Blood 2003, 10, 391–398. [Google Scholar] [CrossRef]
- Even, A.J.G.; Hamming-Vrieze, O.; Van Elmpt, W.; Winnepenninckx, V.J.; Heukelom, J.; Tesselaar, M.E.; Vogel, W.V.; Hoeben, A.; Zegers, C.M.; Vugts, D.J.; et al. Quantitative assessment of Zirconium-89 labeled cetuximab using PET/CT imaging in patients with advanced head and neck cancer: A theragnostic approach. Oncotarget 2017, 8, 3870–3880. [Google Scholar] [CrossRef] [PubMed]
- Lub-de Hooge, M.N.; Kosterink, J.G.; Perik, P.J.; Nijnuis, H.; Tran, L.; Bart, J.; Suurmeijer, A.J.; de Jong, S.; Jager, P.L.; de Vries, E.G.E. Preclinical characterisation of 111In-DTPA-trastuzumab. Br. J. Pharmacol. 2004, 143, 99–106. [Google Scholar] [CrossRef] [PubMed]
- Terwisscha van Scheltinga, A.G.; Ogasawara, A.; Pacheco, G.; Vanderbilt, A.N.; Tinianow, J.N.; Gupta, N.; Li, D.; Firestein, R.; Marik, J.; Scales, S.J.; et al. Preclinical Efficacy of an Antibody-Drug Conjugate Targeting Mesothelin Correlates with Quantitative 89Zr-ImmunoPET. Mol. Cancer Ther. 2017, 16, 134–142. [Google Scholar] [CrossRef] [PubMed]
- Ulaner, G.A.; Hyman, D.M.; Ross, D.S.; Corben, A.; Chandarlapaty, S.; Goldfarb, S.; McArthur, H.; Erinjeri, J.P.; Solomon, S.B.; Kolb, H.; et al. Detection of HER2-Positive Metastases in Patients with HER2-Negative Primary Breast Cancer Using 89Zr-Trastuzumab PET/CT. J. Nucl. Med. 2016, 57, 1523–1528. [Google Scholar] [CrossRef] [PubMed]
- Tsai, W.K.; Wu, A.M. Aligning physics and physiology: Engineering antibodies for radionuclide delivery. J. Labelled Comp. Radiopharm. 2018, 61, 693–714. [Google Scholar] [CrossRef]
- Ståhl, S.; Gräslund, T.; Karlström, A.E.; Frejd, F.Y.; Nygren, P.Å.; Löfblom, J. Afbody molecules in biotechnological and medical applications. Trends Biotechnol. 2017, 35, 691–712. [Google Scholar] [CrossRef] [PubMed]
- Krasniqi, A.; D’Huyvetter, M.; Devoogdt, N.; Frejd, F.Y.; Sörensen, J.; Orlova, A.; Keyaerts, M.; Tolmachev, V. Same-Day Imaging Using Small Proteins: Clinical Experience and Translational Prospects in Oncology. J. Nucl. Med. 2018, 59, 885–891. [Google Scholar] [CrossRef] [PubMed]
- Tolmachev, V.; Orlova, A. Affibody Molecules as Targeting Vectors for PET Imaging. Cancers 2020, 12, 651. [Google Scholar] [CrossRef] [PubMed]
- Tolmachev, V.; Rosik, D.; Wållberg, H.; Sjöberg, A.; Sandström, M.; Hansson, M.; Wennborg, A.; Orlova, A. Imaging of EGFR Expression in Murine Xenografts Using Site-Specifically Labelled Anti-EGFR 111In-DOTA-ZEGFR:2377 Affibody Molecule: Aspect of the Injected Tracer Amount. Eur. J. Nucl. Med. Mol. Imaging 2010, 37, 613–622. [Google Scholar] [CrossRef] [PubMed]
- Andersson, K.G.; Oroujeni, M.; Garousi, J.; Mitran, B.; Ståhl, S.; Orlova, A.; Löfblom, J.; Tolmachev, V. Feasibility of imaging of epidermal growth factor receptor expression with ZEGFR:2377 affibody molecule labeled with 99mTc using a peptide-based cysteine-containing chelator. Int. J. Oncol. 2016, 49, 2285–2293. [Google Scholar] [CrossRef]
- Miao, Z.; Ren, G.; Liu, H.; Qi, S.; Wu, S.; Cheng, Z. PET of EGFR expression with an 18F-labeled affibody molecule. J. Nucl. Med. 2012, 53, 1110–1118. [Google Scholar] [CrossRef] [PubMed]
- Su, X.; Cheng, K.; Jeon, J.; Shen, B.; Venturin, G.T.; Hu, X.; Rao, J.; Chin, F.T.; Wu, H.; Cheng, Z. Comparison of Two Site-Specifically 18F-Labeled Affibodies for PET Imaging of EGFR Positive Tumors. Mol. Pharm. 2014, 11, 3947–3956. [Google Scholar] [CrossRef] [PubMed]
- Garousi, J.; Andersson, K.G.; Dam, J.H.; Olsen, B.B.; Mitran, B.; Orlova, A.; Buijs, J.; Ståhl, S.; Löfblom, J.; Thisgaard, H.; et al. The use of radiocobalt as a label improves imaging of EGFR using DOTA-conjugated Affibody molecule. Sci. Rep. 2017, 7, 5961–5971. [Google Scholar] [CrossRef]
- Oroujeni, M.; Garousi, J.; Andersson, K.G.; Löfblom, J.; Mitran, B.; Orlova, A.; Tolmachev, V. Preclinical Evaluation of [68Ga]Ga-DFO-ZEGFR:2377:A Promising Affibody-Based Probe for Noninvasive PET Imaging of EGFR Expression in Tumors. Cells 2018, 7, 141. [Google Scholar] [CrossRef]
- Miao, Z.; Ren, G.; Liu, H.; Jiang, L.; Cheng, Z. Small-animal PET imaging of human epidermal growth factor receptor positive tumor with a 64Cu labeled affibody protein. Bioconjug. Chem. 2010, 5, 947–954. [Google Scholar] [CrossRef] [PubMed]
- Zhao, P.; Yang, X.; Qi, S.; Liu, H.; Jiang, H.; Hoppmann, S.; Cao, Q.; Chua, M.S.; So, S.K.; Cheng, Z. Molecular imaging of hepatocellular carcinoma xenografts with epidermal growth factor receptor targeted affibody probes. Biomed. Res. Int. 2013, 2013, 759057–759068. [Google Scholar] [CrossRef] [PubMed]
- Garousi, J.; Andersson, K.G.; Mitran, B.; Pichl, M.L.; Ståhl, S.; Orlova, A.; Löfblom, J.; Tolmachev, V. PET imaging of epidermal growth factor receptor expression in tumors using 89Zr-labeled ZEGFR:2377 affbody molecules. Int. J. Oncol. 2016, 48, 1325–1332. [Google Scholar] [CrossRef]
- Summer, D.; Garousi, J.; Oroujeni, M.; Mitran, B.; Andersson, K.G.; Vorobyeva, A.; Löfblom, J.; Orlova, A.; Tolmachev, V.; Decristoforo, C. Cyclic versus Noncyclic Chelating Scaffold for 89Zr-Labeled ZEGFR:2377Affibody Bioconjugates Targeting Epidermal Growth Factor Receptor Overexpression. Mol. Pharm. 2018, 15, 175–185. [Google Scholar] [CrossRef] [PubMed]
- Yokoyama, A.; Ohmomo, Y.; Horiuchi, K.; Saji, H.; Tanaka, H.; Yamamoto, K.; Ishii, Y.; Torizuka, K. Deferoxamine, a Promising Bifunctional Chelating Agent for Labeling Proteins with Gallium: Ga-67 DF-HSA:Concise Communication. J. Nucl. Med. 1982, 23, 909–914. [Google Scholar] [PubMed]
- Vosjan, M.J.W.D.; Perk, L.R.; Roovers, R.C.; Visser, G.W.M.; Marijke Stigter-van Walsum, M.P.; van Bergen En Henegouwen, M.P.; Van Dongen, G.A.M.S. Facile labelling of an anti-epidermal growth factor receptor Nanobody with 68Ga via a novel bifunctional desferal chelate for immuno-PET. Eur. J. Nucl. Med. Mol. Imaging 2011, 38, 753–763. [Google Scholar] [CrossRef]
- Tsionou, M.I.; Knapp, C.E.; Foley, C.A.; Munteanu, C.R.; Cakebread, A.; Imberti, C.; Eykyn, T.R.; Young, J.D.; Paterson, B.M.; Blower, P.J.; et al. Comparison of macrocyclic and acyclic chelators for gallium-68 radiolabelling. RSC Adv. 2017, 7, 49586–49599. [Google Scholar] [CrossRef] [PubMed]
- Hider, R.C.; Kong, X. Chemistry and biology of siderophores. Nat. Prod. Rep. 2010, 27, 637–657. [Google Scholar] [CrossRef] [PubMed]
- Lewis, M.R.; Reichert, D.E.; Laforest, R.; Margenaua, W.H.; Shefer, R.E.; Klinkowstein, R.E.; Hughey, B.J.; Welch, M.J. Production and purification of gallium-66 for preparation of tumor-targeting radiopharmaceuticals. Nucl. Med. Biol. 2002, 6, 701−706. [Google Scholar] [CrossRef]
- Goethals, P.; Coene, M.; Slegers, G.; Agon, P.; Deman, J.; Schelstraete, K. Cyclotron production of carrier-free 66Ga as a positron emitting label of albumin colloids for clinical use. Eur. J. Nucl. Med. 1988, 14, 152−154. [Google Scholar] [CrossRef] [PubMed]
- Engle, J.W.; Hong, H.; Zhang, Y.; Valdovinos, H.F.; Myklejord, D.V.; Barnhart, T.E.; Theuer, C.P.; Nickles, R.J.; Cai, W. Positron emission tomography imaging of tumor angiogenesis with a 66Ga-labeled monoclonal antibody. Mol. Pharm. 2012, 9, 1441–1448. [Google Scholar] [CrossRef]
- Ugur, Ö.; Kothari, P.J.; Finn, R.D.; Zanzonico, P.; Ruan, S.; Guenther, I.; Maecke, H.R.; Larson, S.M. Ga-66 labeled somatostatin analogue DOTA-DPhe1-Tyr3-octreotide as a potential agent for positron emission tomography imaging and receptor mediated internal radiotherapy of somatostatin receptor positive tumors. J. Nucl. Med. Biol. 2002, 29, 147−157. [Google Scholar] [CrossRef]
- Rinne, S.S.; Gagnon, K.; Abouzayed, A.; Tolnachev, V.; Orlova, A. 66Ga-PET-Imaging of GRPR-expression in prostate cancer: Production and characterization of [66Ga]Ga-NOTA-PEG2-RM26. Sci. Rep. 2021, 11, 3631. [Google Scholar] [CrossRef] [PubMed]
- Yang, X.D.; Jia, X.C.; Corvalan, J.R.; Wang, P.; Davis, C.G. Development of ABX-EGF, a fully human anti-EGF receptor monoclonal antibody, for cancer therapy. Crit. Rev. Oncol. Hematol. 2001, 38, 17–23. [Google Scholar] [CrossRef]
- Malmberg, J.; Tolmachev, V.; Orlova, A. Imaging agents for in vivo molecular profiling of disseminated prostate cancer–targeting EGFR receptors in prostate cancer: Comparison of cellular processing of [111In]-labeled affibody molecule Z (EGFR:2377) and cetuximab. Int. J. Oncol. 2011, 38, 1137–1143. [Google Scholar]
- Wållberg, H.; Orlova, A. Slow internalization of anti-HER2 synthetic affibody monomer 111In-DOTA-ZHER2:342-pep2: Implications for development of labeled tracers. Cancer Biother. Radiopharm. 2008, 23, 435–442. [Google Scholar] [CrossRef]
- Garousi, J.; Orlova, A.; Frejd, F.Y.; Tolmachev, V. Imaging using radiolabelled targeted proteins: Radioimmunodetection and beyond. EJNMMI Radiopharm. Chem. 2020, 5, 16. [Google Scholar] [CrossRef]
- Tolmachev, V.; Stone-Elander, S. Radiolabelled proteins for positron emission tomography: Pros and cons of labelling methods. Biochim. Biophys. Acta 2010, 1800, 487–510. [Google Scholar] [CrossRef]
- Tolmachev, V.; Orlova, A. Influence of labelling methods on biodistribution and imaging properties of radiolabelled pep-tides for visualisation of molecular therapeutic targets. Curr. Med. Chem. 2010, 17, 2636–2655. [Google Scholar] [CrossRef]
- Björkelund, H.; Gedda, L.; Barta, P.; Malmqvist, M.; Andersson, K. Gefitinib induces epidermal growth factor receptor dimers which alters the interaction characteristics with 125I-EGF. PLoS ONE 2011, 6, e24739. [Google Scholar] [CrossRef]
- Sörensen, J.; Velikyan, I.; Sandberg, D.; Wennborg, A.; Feldwisch, J.; Tolmachev, V.; Orlova, A.; Sandström, M.; Lubberink, M.; Olofsson, H.; et al. Measuring HER2-Receptor Expression In Metastatic Breast Cancer Using [68Ga]ABY-025 Affibody PET/CT. Theranostics 2016, 6, 262–271. [Google Scholar] [CrossRef] [PubMed]
- Carver, R.S.; Stevenson, M.C.; Scheving, L.A.; Russell, W.E. Diverse expression of ErbB receptor proteins during rat liver development and regeneration. Gastroenterology 2002, 123, 2017–2027. [Google Scholar] [CrossRef]
- Heskamp, S.; Raavé, R.; Boerman, O.; Rijpkema, M.; Goncalves, V.; Denat, F. 89Zr-Immuno-Positron Emission Tomography in Oncology: State-of-the-Art 89Zr Radiochemistry. Bioconjug. Chem. 2017, 28, 2211–2223. [Google Scholar] [CrossRef] [PubMed]
| ka1 (1/M×s) × 104 | ka1 (1/s) × 10−6 | KD1 (pM) | Weight1, % | ka2 (1/M×s) × 104 | kd2 (1/s) × 10−3 | KD2 (nM) | Weight2, % |
|---|---|---|---|---|---|---|---|
| 2.2 ± 0.1 | 4.0 ± 0.5 | 342 ± 15 | 74.1 ± 0.1 | 3.5 ± 0.1 | 1.03 ± 0.05 | 29.2 ± 0.2 | 8.0 ± 0.8 |
| Uptake, %ID/g | Tumor-to-Organ Ratio | |||||
|---|---|---|---|---|---|---|
| 3 h | 6 h | 24 h | 3 h | 6 h | 24 h | |
| Blood | 1.6 ± 0.2 a,b | 1.2 ± 0.1 a,c | 0.4 ± 0.1 b,c | 4.2 ± 0.6 b | 4.2 ± 0.6 c | 10.7 ± 2.7 b,c |
| Salivary gland | 1.2 ± 0.6 | 0.7 ± 0.3 | 0.6 ± 0.2 | 5.9 ± 2.1 | 7.4 ± 2.7 | 6.7 ± 3.2 |
| Lung | 1.6 ± 0.6 b | 0.9 ± 0.3 c | 0.7 ± 0.3 b,c | 4.2 ± 1.0 | 5.1 ± 0.4 | 5.9 ± 3.1 |
| Liver | 4.6 ± 0.2 a,b | 3.5 ± 0.3 a,c | 1.4 ± 0.2 b,c | 1.4 ± 0.3 b | 1.5 ± 0.3 c | 2.7 ± 0.7 b,c |
| Spleen | 1.3 ± 0.4 a,b | 0.7 ± 0.2 a | 0.5 ± 0.2 b | 5.0 ± 0.3 | 8.2 ± 3.1 | 9.4 ± 5.4 |
| Colon | 1.6 ± 0.5 | 1.0 ± 0.3 | 0.811 ± 0.001 | 4.4 ± 1.4 | 5.5 ± 1.4 | 4.7 ± 0.9 |
| Kidneys | 257 ± 19 a,b | 166 ± 17 a,c | 42 ± 6 b,c | 0.025 ± 0.005 b | 0.031 ± 0.002 c | 0.088 ± 0.014 b,c |
| Tumor | 6.5 ± 1.3 b | 5.1 ± 0.5 c | 3.7 ± 0.5 b,c | - | - | - |
| Muscle | 0.3 ± 0.1 | 0.2 ± 0.1 | 0.2 ± 0.1 | 18 ± 1 | 24 ± 7 | 19 ± 3 |
| Bone | 1.4 ± 0.8 | 0.9 ± 0.3 | 0.9 ± 0.3 | 10 ± 5 | 6.2 ± 1.7 | 4.6 ± 1.7 |
| GI * | 2.2 ± 0.3 | 1.5 ± 0.1 | 0.9 ± 0.1 | - | - | - |
| Carcass * | 8.2 ± 0.9 | 6.2 ± 0.5 | 3.8 ± 0.3 | - | - | - |
| Uptake, %ID/g | Tumor-to-Organ Ratio | |
|---|---|---|
| 3 h | 3 h | |
| Blood | 1.6 ± 0.2 | 2.7 ± 0.2 |
| Salivary gland | 0.8 ± 0.1 | 5.5 ± 0.9 |
| Lung | 1.2 ± 0.2 | 3.7 ± 0.4 |
| Liver | 3.8 ± 0.8 | 1.2 ± 0.2 |
| Spleen | 0.6 ± 0.1 | 8.0 ± 1.4 |
| Colon | 1.0 ± 0.3 | 4.6 ± 1.3 |
| Kidneys | 207 ± 22 | 0.021 ± 0.001 |
| Tumor | 4.4 ± 0.7 | - |
| Muscle | 0.22 ± 0.03 | 20.6 ± 3.7 |
| Bone | 0.5 ± 0.1 | 8.6 ± 1.4 |
| GI * | 3.0 ± 1.1 | - |
| Carcass * | 6.7 ± 1.0 | - |
| Uptake, %ID/g | Tumor-to-Organ Ratio | |
|---|---|---|
| 24 h | 24 h | |
| Blood | 0.4 ± 0.1 | 5.9 ± 1.3 |
| Salivary gland | 0.6 ± 0.1 | 3.8 ± 0.8 |
| Lung | 0.7 ± 0.1 | 3.3 ± 0.4 |
| Liver | 2.8 ± 0.7 | 0.9 ± 0.2 |
| Spleen | 0.8 ± 0.2 | 3.0 ± 0.8 |
| Colon | 0.9 ± 0.1 | 2.2 ± 0.8 |
| Kidneys | 261 ± 56 | 0.009 ± 0.002 |
| Tumor | 2.4 ± 0.1 | - |
| Muscle | 0.24 ± 0.03 | 10.1 ± 1.3 |
| Bone | 1.3 ± 0.1 | 2.0 ± 0.3 |
| GI * | 1.0 ± 0.1 | - |
| Carcass * | 5.1 ± 1.3 | - |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Oroujeni, M.; Xu, T.; Gagnon, K.; Rinne, S.S.; Weis, J.; Garousi, J.; Andersson, K.G.; Löfblom, J.; Orlova, A.; Tolmachev, V. The Use of a Non-Conventional Long-Lived Gallium Radioisotope 66Ga Improves Imaging Contrast of EGFR Expression in Malignant Tumours Using DFO-ZEGFR:2377 Affibody Molecule. Pharmaceutics 2021, 13, 292. https://doi.org/10.3390/pharmaceutics13020292
Oroujeni M, Xu T, Gagnon K, Rinne SS, Weis J, Garousi J, Andersson KG, Löfblom J, Orlova A, Tolmachev V. The Use of a Non-Conventional Long-Lived Gallium Radioisotope 66Ga Improves Imaging Contrast of EGFR Expression in Malignant Tumours Using DFO-ZEGFR:2377 Affibody Molecule. Pharmaceutics. 2021; 13(2):292. https://doi.org/10.3390/pharmaceutics13020292
Chicago/Turabian StyleOroujeni, Maryam, Tianqi Xu, Katherine Gagnon, Sara S. Rinne, Jan Weis, Javad Garousi, Ken G. Andersson, John Löfblom, Anna Orlova, and Vladimir Tolmachev. 2021. "The Use of a Non-Conventional Long-Lived Gallium Radioisotope 66Ga Improves Imaging Contrast of EGFR Expression in Malignant Tumours Using DFO-ZEGFR:2377 Affibody Molecule" Pharmaceutics 13, no. 2: 292. https://doi.org/10.3390/pharmaceutics13020292
APA StyleOroujeni, M., Xu, T., Gagnon, K., Rinne, S. S., Weis, J., Garousi, J., Andersson, K. G., Löfblom, J., Orlova, A., & Tolmachev, V. (2021). The Use of a Non-Conventional Long-Lived Gallium Radioisotope 66Ga Improves Imaging Contrast of EGFR Expression in Malignant Tumours Using DFO-ZEGFR:2377 Affibody Molecule. Pharmaceutics, 13(2), 292. https://doi.org/10.3390/pharmaceutics13020292









