Abstract
The vagina has been considered a potential drug administration route for centuries. Most of the currently marketed and investigated vaginal formulations are composed with the use of natural or synthetic polymers having different functions in the product. The vaginal route is usually investigated as an administration site for topically acting active ingredients; however, the anatomical and physiological features of the vagina make it suitable also for drug systemic absorption. In this review, the most important natural and synthetic polymers used in vaginal products are summarized and described, with special attention paid to the properties important in terms of vaginal application. Moreover, the current knowledge on the commonly applied and innovative dosage forms designed for vaginal administration was presented. The aim of this work was to highlight the most recent research directions and indicate challenges related to vaginal drug administrations. As revealed in the literature overview, intravaginal products still gain enormous scientific attention, and novel polymers and formulations are still explored. However, there are research areas that require more extensive studies in order to provide the safety of novel vaginal products.
Keywords:
vagina; polymers; mucoadhesion; drug delivery systems; nanoparticles; gels; films; patches 1. Introduction
The first known data concerning the vaginal application of therapeutics appeared in medical books from Ancient Egypt. The Kahun Medical Papyrus (dating from 2250 years B.C.) is considered to be the oldest known gynecological handbook. Among others, it contained specific information on treating vaginal inflammations and described various methods of contraception [1]. Interestingly, some of the treatment methods proposed back then may now be considered controversial and even risky. One of the most interesting formulations described in the ancient documents were contraceptive suppositories, composed of crocodile manure mixed with honey and sodium carbonate. Another ancient source of vaginal prescriptions is the Papyrus Ebers (about 1550 B.C.), which describes contraceptive tampons made of lint and soaked in honey and acacia tips. Acacia shrub was used as a popular source of gum arabic. After the insertion of a tampon, the gum released lactic acid which acidified the vagina [2,3,4]. Nowadays, lactic acid is a well-known and very common spermicidal agent used in modern contraceptive gels and creams [5,6]. It is also noteworthy that in the 15th century, people already had the knowledge that some substances are able to penetrate to the systemic circulation after vaginal administration. A quite common, however inglorious practice, was the vaginal application of arsenic or other poisonous substances in order to induce abortion or commit suicide [7].
At present, vaginal formulations are mostly used to deliver topically acting drugs such as antimicrobials [8,9,10,11,12], spermicides [13,14], antimycotics [15] or to introduce drugs to the systemic circulation [16,17,18], mostly for hormonal therapy or contraception [19,20]. Much interest is also focused on the vaginal delivery of microbicides in order to inhibit sexual transmission of HIV [21,22], HPV [23,24,25] or HSV [26,27,28].
The abundance of blood vessels in the vagina is a definite advantage, especially in relation to systemic formulations [29,30,31,32]. The primary benefit is the fact that active substances do not undergo the first-pass hepatic metabolism. Furthermore, the vaginal epithelium has a very suitable permeability, even in the case of drugs with a high molecular weight such as peptides or proteins [33,34,35].
When compared to the oral route, there are several benefits of vaginal administration. These include, for example, reduction in the dose, less frequent dosing, reduced sideeffects, no hepatic first-pass effect. However, some challenges have to be overcome, including dilution by vaginal fluid or peristaltic activity of the vaginal wall [36].
Among the known vaginal malfunctions, the most common include bacterial vaginosis, aerobic vaginitis, candidiasis, sexually transmitted infections, atrophic vaginitis, desquamative inflammatory vaginitis, cervicitis, and mucoid ectopy. The symptoms related to them are usually non-specific such as itching, burning, pain, abnormal bleeding, or discharge. However, most of the mentioned can also be associated with vaginal dermatoses, allergic and irritant reactions [37].
According to data given by the Centers for Disease Control and Prevention, bacterial vaginosis (BV) is the most common vaginal infection among women betweenthe age of 15 and 44. It is estimated that in the United States, the prevalence of women who suffered from BV reached about 21.2 million in 2004 [38,39,40]. Among vaginal infections, candidiasis is the second most common. Other vaginal diseases include vaginal or vulvar cancers. In general, they are regarded as rare, with 0.7 per 100,000 diagnosed with vaginal and 2.6 per 100,000 with vulvar in the year 2017.
To properly design a vaginal formulation, it has to be taken into account that the conditions in the vaginal cavity are very unstable. The acidity, temperature, production of vaginal fluid, and thickness of the epithelium strongly depend on the phase of the menstrual cycle, sexual activity, age of the patient, and concomitant diseases [41,42,43,44].
Most vaginal drug delivery systems contain various types of natural or synthetic polymers. Their main role is to assure the contact of the drug with the site of action as long as it is possible and provide a controlled drug release, repeatedly and in a predictive manner. A large variety of vaginal drug delivery systems are already in use or under investigation. These include gels, creams, foams, tablets, capsules, suppositories, pellets, microparticles, nanoparticles, patches, films, or rings. The aim of the presented paper was to prepare acomprehensive review of the latest developments in the field of polymer-based vaginal drug delivery systems, indicate the most extensively investigated research directions, and discuss future trends and possible obstacles in the studies focusing on vaginal drug delivery.
2. Anatomy and Physiology of the Vagina
The human vagina is a fibromuscular tubular organ that connects the vulva, cervix, and uterus, and the organs of the upper reproductive tract [45]. It is divided into two parts, the upper and lower, which originate from the mesoderm and epiderm, respectively [46]. The vaginal wall is composed of three layers: i. epithelium, which is the inner mucosal layer (tunica mucosa) and consists mainly of non-keratinized squamous cells, ii. muscle layer (tunica muscularis) built of smooth muscle cells and iii. external (outer) membrane filled with collagen [46,47]. The inner surface of the vagina is built of transverse folds called wrinkles (lat. Rugae vaginales). They are responsible for maintaining the correct tension and stiffness of the whole organ. The thickness of the epithelium changes during the menstrual cycle in the range of 200–300 microns. Its properties depend mainly on the level of sex hormones. Estrogens produced during the proliferative phase induce the growth and cornification of the epithelial layer [48,49,50]. During pregnancy, an epithelial cell layer is thin. In the menstrual cycle, the concentration of enzymes from the group of aminopeptidases and endopeptidases in the vaginal fluid changes [51,52]. This may create a problem with the selection of thecorrect dose of the active substance. Drug release, distribution, and absorption after vaginal administration strongly depend on the amount and the properties of the vaginal fluid. The fluid usually contains components from vaginal wall transudate, cervical and vestibular glands secretions, exfoliated epithelium cells or residual urine, and fluids from the upper reproductive tract [53]. According to the extensive data presented by Owen and Katz [54], the organic compounds identified in the vaginal fluid include proteins, carbohydrates, and other small molecules such as urea, glucose or lactic and acetic acid, and others. The fluid also contains inorganic ions such as potassium, sodium, calcium, or chloride. However, it must be taken into account that the vaginal secretions vary according to the actual conditions, menstrual cycle phase, and existing diseases [55,56]. In physiological conditions, the fluid is usually thick, clear, or slightly opaque but can turn to creamy, clumpy, green, or yellow with a specific odor as a result of a bacterial, fungal, or other infection [57,58]. The physiological amount of the fluid is relatively small (usually between 0.5 and 1.0 mL). Nevertheless, it may dissolve or liquefy the formulation and have a negative influence on the formulation’s residence time or accelerate the disintegration resulting in weakening of the therapeutic activity. In the case of semisolid preparations, the fluid can weaken interactions within the polymer matrix and lead to a change of the rheological properties. Other factors that are crucial in drug release and distribution are pH and osmolarity of the vaginal environment [54], especially in the case of polymers with pH-sensitive moieties.
Physiological vaginal bacterial flora is a complex system. Its composition changes dynamically depending on many factors. The probiotic microbe that predominates in the vaginal environment is the anaerobic, rod-shaped lactic acid bacteria Lactobacillus acidophilus. It produces lactic acid, which maintains vaginal pH in the range of 3.5–4.5 [53,59,60,61]. Besides low pH, several other mechanisms have been developed to prevent the colonization of the vagina by exogenous pathogens. These include the production of antimicrobial bacteriocins, peroxidases, and other organic acids. Moreover, the vaginal wall epithelial cells constantly exfoliate, which results in the efficient removal of the microbes [53].
One of the most important factors that havea significant influence on the efficiency of the vaginal formulations is the adhesion to the mucous membrane. The mucoadhesive properties provide a longer residence time and a more intimate contact with the site of action. In the case of systemic delivery, the properly designed mucoadhesive systems are able to decrease the distribution of active pharmaceutical ingredients (API) throughout the vaginal cavity and promote its penetration into the systemic circulation [62].
The vaginal mucous membrane consists mainly of water, inorganic salts, carbohydrates, lipids, salts, DNA, enzymes, and mucins. Its features resemble the properties of hydrogels [32,63,64]. Mucin belongs to glycoproteins and is responsible for the formation of a hydrogel layer on the external mucosa [62]. Mucoadhesion can be defined as the phenomenon of adhesion and bonding of the polymers with the vaginal mucosa through physical and chemical interactions [65]. Connection and formation of mucoadhesive interactions can be divided into three stages: i. wetting and swelling of the polymer, ii. connection of the polymer chains with the chains of mucin, iii. formation of weak chemical bonds. Generally, it can be regarded that the greater the mucoadhesion ability of the polymer is, the longer the residence time of the drug formulation in the application site gets. Mucoadhesion of vaginal formulations depends mainly on the physicochemical properties of the polymer, including its molecular weight, degree of ionization, and functional group types [66]. Mucoadhesive polymers are divided into three groups: 1. polymers that reveal adhesive properties after being placed in a water environment; 2. polymers that connect with mucous membranes by non-specific binding such as non-covalent or electrostatic; 3. polymers with the ability to bind to specific receptors on the cells or surface of the mucosa [67].
Once the formulation reaches the vaginal mucosa, it can release the drug into the vaginal cavity or on the surface of the vaginal mucosa. Depending on the type of formulation and properties of the active compound, systemic activity can also be achieved as a result of permeation to the vaginal vascular system [68,69]. According to the studies presented by van der Bijl &van Eyk [70], the vaginal mucosa reveals a very similar permeability to water as buccal mucosa, but in comparison to the intestinal and colonic mucosa, its permeability is higher. In addition, it is more permeable for various drugs than intestinal and colonic mucosae, even in the case of compounds with amolecular weight higher than 300 kDa [70,71,72]. A scheme depicting the vaginal route is presented in Figure 1.
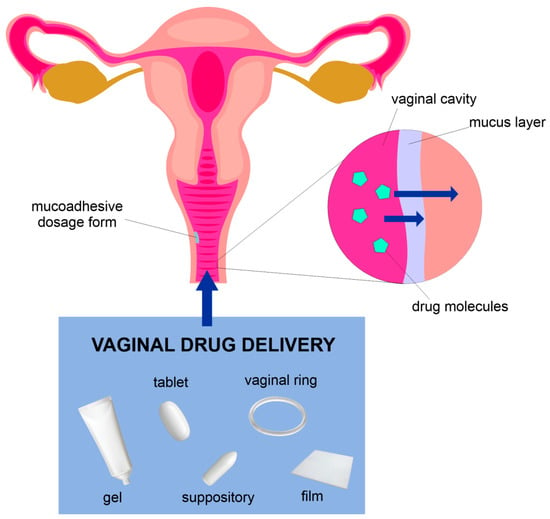
Figure 1.
Vaginal drug delivery route.
3. Polymers Used in Vaginal Drug Delivery Systems
3.1. Polymers of Natural Origin
3.1.1. Polymers from Plant Sources
Cellulose and Its Derivatives
Cellulose is regarded as the most abundant organic compound throughout the world [73]. It is an unbranched polysaccharide, built of 3000–14,000 glucose molecules linked by linear β-1,4-glycosidic bonds. It is the scaffold component of cell walls and tissues in most plants [74]. Pure and unmodified cellulose is insoluble in water and most organic solvents [75]. In order to obtain solubility and achieve swelling properties, the hydroxyl groups of the main backbone are subjected to esterification or etherification. The semisynthetic cellulose derivatives constitute a large and diverse group of compounds differing in terms of polarity, water solubility, swelling properties, and thus possible pharmaceutical and biomedical applications [76]. The most commonly used cellulose derivatives are microcrystalline cellulose (MCC), methylcellulose (MC), ethylcellulose (EC), hydroxyethyl cellulose (HEC), hydroxypropyl cellulose (HPC), hydroxypropyl methyl cellulose (HPMC), and sodium carboxymethyl cellulose (Na-CMC) [77,78].
Depending on the unique and varied properties, semisynthetic celluloses are widely used both in oral and topical drug delivery. In the case of tablet technology, their most popular applications include their use as binders, compressibility enhancers, fillers, diluents. Depending on the way of interacting with water, celluloses may be used for the modification of drug release by acting as disintegrants, matrix-forming components, or coating agents. Due to their swelling ability, they can also be used as thickeners and stabilizing agents in liquid and semisolid dosage forms. Because of the mucoadhesive properties, semisynthetic celluloses are often investigated as components of vaginal drug delivery systems, mostly in gels or viscous liquids but also tablets and micro- or nanoparticulate formulations [79,80,81].
- Pectin
Pectin is usually defined as a diverse and most complex group of oligosaccharides and polysaccharides abundantly occurring in plant cell walls. Its main component is the esterified D-galacturonic chain [82]. In the case of natural pectin, the acid groups are esterified with methoxy residues. The free hydroxyl groups can also occur in the acetylated form, and additionally, the galacturonic acid main chain can be substituted with rhamnose groups [83]. The presence of the latter disrupts the chain helix formation [84]. Depending on the source, pectin can also contain other xylose, galactose, or arabinose residues, located in side chains. Pectins are differentiated mainly due to methoxy group content and classified as high methoxy- (>50% esterified) and low methoxypectins (<50% esterified) [85]. It is noteworthy that this model may vary significantly in terms of particular domains, e.g., chain length, sugar composition, and the degree of methylation or acetylation [86]. Among the most important features of pectin, its resistance to the acidic environment is most beneficial in oral drug delivery with a modified release in the lower gastrointestinal tract. The gelation mechanism strongly depends on the methylation degree of the main linear structural element of the polymer. In the case of high methoxyl group content, a gel is formed at pH < 3.5, usually in thepresence of an additional substance (e.g., sucrose), decreasing water molecules activity [86]. In vaginal drug delivery studies, pectins are mainly investigated as mucoadhesive components of various formulations. Their pH-dependent behavior can also strongly influence the drug release mechanism [87].
Alginates
Alginates are biocompatible and biodegradable anionic polysaccharides occurring naturally in brown seaweeds (Phaeophyceae) [88]. Among the whole group, sodium alginate is the one most commonly used for pharmaceutical and biomedical purposes [89]. Alginic acid is a copolymer containing D-mannuronic and L-guluronic acids organized in blocks separated with sequences of the same units organized randomly [90]. The exact composition of the compound depends on its source of origin. Alginates reveal a high water binding capacity due to their hydrophilic nature [91]. In the presence of divalent and multivalent cations, alginate solution undergoes an ionotropic gelation process [92,93]. The properties of the obtained gel depend mostly on the composition of the polymer. Gel strength is higher in the case of compounds with a higher guluronic acid content [92]. Alginates can be applied as thickeners and stabilizers in liquid and semisolid pharmaceutical formulations [94]. They are also investigated as binders and hydrophilic matrix-forming agents in prolonged-release solid dosage forms [95]. Moreover, the ability to undergo ionotropic gelation may be advantageous in terms of in situ gelling system formulations [96,97].
- Starch
Starch is one of the most abundant plant polysaccharides and the main carbohydrate in the human diet [98]. In fact, it consists of two compounds: linear amylose (25%) and branched amylopectin (75%), both composed of multiple α-D-glucose units. In the first one, structural elements are linked with α-1,4 bonds, while in the other one, α-1,4, α-1,3, andα-1,6 bonds are observed [99,100]. Starch is insoluble in cold water, while at higher temperatures reveals a tendency to swell and form gels [101,102]. For vaginal drug delivery purposes, starch, as well as its derivatives, are investigated mainly as the component of tablets, micro- or nanoparticles, gels, etc. [103,104,105,106].
- Carrageenans
Carrageenans belong to a family of linear polysaccharides obtained from red seaweeds by alkaline extraction. The polymer chain is formed by repeating disaccharide units of alternating 3-linked β-D-galactopyranose, 4-linked α-D-galactopyranose or 4-linked α-D-galactopyranose or 4-linked 3,6-anhydro-α-D-galactopyranose [107]. Thereare three types of carrageenan mostly known for their application in vaginal formulations technology, which includes iota-carrageenan (ι-carrageenan), kappa-carrageenan (κ-carrageenan), and lambda-carrageenan (λ-carrageenan) [108]. Each type differs both in structure and the content of ester sulfate [109].According to specific and unique properties, carrageenans can be used both as excipients or active components of vaginal formulations. In the first case, they are mostly used as mucoadhesive additives or structure-forming agents in solid and semisolid formulations [110,111]. Moreover, carrageenans have the potency to inhibit microbial and viral infections, which is considered as their prevalence over other natural polymers in terms of transmission of vaginal infections [112,113].
3.1.2. Polymers Derived from Animal Sources
Chitosan
Chitosan is obtained as a product of deacetylation of chitin, a natural component of numerous invertebrate exoskeletons [114]. The reaction is usually performed in the presence of concentrated NaOH; however, the process may also be conducted with the use of a chitin deacetylase [115]. The most extensively exploited source of chitin used as a substrate to obtain chitosan isedible crustaceans such as shrimps and crabs [116,117]. Chitosan is a group of linear copolymers consisting of glucosamine and N-acetylglucosamine connected with β-1,4 bonds [118]. It is important to notice that chitosan differs significantly from its substrate in terms of solubility. Chitosan is soluble in acidic solutions thatarea result of the presence of free amine groups in the molecule. In the case of chitin, amine groups are mostly acetylated, which makes the polymer practically insoluble in an acidic and slightly alkaline environment [119].
Because of its interesting properties, chitosan is extensively investigated both as an active ingredient and as an excipient [120]. It is non-toxic, biodegradable, and biocompatible [121]; therefore, it can be safely applied as a component of pharmaceutical formulations [122,123]. Moreover, some antibacterial properties [124] and a hemostatic activity of chitosan were revealed [125]. Orally administered chitosan can effectively decrease the serum cholesterol level, which can be useful in hypercholesterolemia therapy and arteriosclerosis prevention [126]. It is also noteworthy that the polymer presents excellent mucoadhesive properties [127] and a gelling ability that is favorable in terms of topical formulation design [128,129]. Another interesting feature of chitosan related to the mucoadhesive characteristics is its ability to accelerate the wound-healing process. This property is related to the gradual depolymerization of chitosan. The products released in this reaction improve the organization of novel collagen fibers and enhance the production of hyaluronic acid [130,131].
Hyaluronic Acid
Hyaluronic acid is a glycosaminoglycan occurring naturally in the human body [132]. As a component of the extracellular and pericellular matrix, it is present in nearly all tissues of human and other vertebrates’ bodies [133]. It is most commonly known as an important component of synovial fluid [134]. Hyaluronic acid molecules consist of repeating units composed of D-glucuronic acid and N-acetyl-D-glucosamine connected by alternating β-1,4 and β-1,3 bonds. It is noteworthy that hyaluronic acid molecules are large, unbranched, with molar masses reaching even 107 Da [135]. They form double helices connected to each other as a result of interactions between hydrophobic areas formed by axial hydrogen atoms of CH groups connected into β-sheets. Adjacent planar structures are linked with hydrogen bonds into a three-dimensional network [136]. The physicochemical properties of hyaluronic acid strongly depend on its molecular weight and the concentration of the solution. Low molecular weight hyaluronic acid solutions reveal Newtonian properties while systems composed of large molecules are non-Newtonian, showing clearly the viscoelastic properties. The same tendency is observed when diluted and concentrated solutions are compared. Moreover, the rheological characteristics of hyaluronic acid solutions depend also on the pH, which is related to the presence of carboxylic groups in its molecule [136,137]. Hyaluronic acid has many important functions in the human body. Because of its high polarity, it can bind high amounts of water, which is important in terms of proper skin functioning [138]. Moreover, hyaluronic acid also serves as a scaffold for proteins and cells, affecting their proliferation and tissue regeneration [139]. During tissue damage and infections, hyaluronic acid is rapidly degraded into simple sugars. It was also found that the physiological activity of the polymer depended on its molecular weight. Large molecules usually act as matrix components and reveal immunosuppressive and anti-angiogenic properties. Medium-sized molecules are considered angiogenic and immunostimulatory agents, while small hyaluronic acid molecules play important roles in signal transduction through different pathways [135]. Currently, hyaluronic acid is widely applied in the medicine, pharmacy, and cosmetic industry. The most important medicinal areas employing hyaluronic acid are ophthalmic and plastic surgery, ophthalmology and wound healing. In surgical procedures, it is used as a filler to create operating space. Moreover, it can be applied as intra-articular injections in rheumatoid arthritis. According to Greenberg et al., hyaluronic acid improves viscoelastic properties of synovial fluid impaired in a degenerative process, inhibits further cartilage degradation, acts as an inflammatory agent and also exerts some analgesic effect [140]. Exceptionally high concentrations of hyaluronic acid are observed during inflammations of the vagina caused by the fungi (recurrent vulvovaginal candidiasis; RVVC) [141].
The first applications of hyaluronic acid were related to accelerated wound healing and skin recovery. Today, it is widely used in the cosmetic and pharmaceutical industries. It is a component of eye drops, intra-articular injectable solutions, lotions for bladder irrigation, aerosols used to treat asthma, solutions for mouthwash, and anti-acidic formulations. The potential use of hyaluronic acid in the prevention of viral infections is also investigated [142]. In the process of developing a formulation containing hyaluronic acid, it should be taken into account that it is degraded by hyaluronidase and hydroxyl radicals [143].
Gelatin
Gelatin is a natural biopolymer obtained from animal cartilage and bones as a result of collagen hydrolysis. The properties of the obtained product depend on the technological process employed to pretreat the animal material before collagen extraction. In alkaline conditions, amide groups of asparagine and glutamine are transformed into free carboxylic groups, while in the acidic process, these groups remain intact. As a result, products revealing different electrical properties are obtained. Gelatin produced at alkaline conditions contains more acidic groups that may undergo an ionization process in solution. Negative charge localized along the polymer chain results in the lowering of the isoelectric point when compared to the product obtained in acidic conditions. It is noteworthy that gelatin produced with the use of the method involving acidic hydrolysis is similar to the untreated collagen [144]. Gelatin reveals many advantageous properties important in pharmaceutical technology, e.g., excellent biocompatibility and biodegradability. Therefore, it is widely applied as a component of soft and hard capsule shells marketed all over the world [145]. Moreover, it has also been used in commercial formulations as a plasma expander (Gelofusin®, B. Braun Medical Ltd., Sheffield, UK), as a hemostatic agent for wound closure (Gelita®, B. Braun Medical Ltd., UK), and for impregnation of polyester, implants applied in reconstructive surgical procedures in the aorta and peripheral arteries (Uni-Graft®K DV, B. Braun Medical Ltd., UK) [146]. It is also widely used as a stabilizer in live attenuated viral vaccines; however, allergic reactions related to gelatin presence have been reported [147].
3.1.3. Microbial Polymers
Gellan Gum
Gellan is an anionic polysaccharide secreted by Sphingomonas (formerly Pseudomonas) elodea bacteria as a product of the fermentation process. Gellan molecules are linear and consist of repeating tetrasaccharide units containing l-rhamnose, d-glucose, and d-glucuronic acid moieties in the molar ratio 1:2:1. In the native form gellan main backbone is substituted with acetyl and L-glyceryl moieties, which can be removed in a hydrolysis process leading to obtaining the low-acetyl gellan gum. Both forms are commercially available [148]. The most important feature of gellan gum is its ability to form gels in the presence of mono-, di-, and trivalent cations, which can form coordinate bonds with carboxylic groups of the polymer and stabilize the three-dimensional structure. The properties of the obtained physical gels depend on the acetylation degree of the polymer. In the case of the low-acetylated form, the rigid and brittle product is obtained, while in the case of high-acetylated gellan soft semisolid gels are observed. The described feature is favorable in terms of in situ gelling systems forming upon contact with physiological fluids containing mentioned cations.
Xanthan Gum
Xanthan gum is a microbial polysaccharide obtained in a fermentation process of cabbage plant bacterium Xanthomonas campestris. The biopolymer has been produced industrially since 1964, and in the late 1960s, it was granted the approval of the FDA as a food additive. Currently, it is employed in several areas, e.g., the food industry, personal care products and pharmaceutics. It may act as a stabilizer in disperse systems such as emulsions and suspensions, and because of excellent swelling properties and a shear-thinning behavior, it may be used as a thickening agent in topical drug dosage forms and cosmetics, as well as a structure enhancing additive in food products [149,150].
The most important structural element of the xanthan molecule is a backbone consisting of glucose moieties connected with β-1,4-glycosidic bonds also observed in cellulose molecules. The cellulose backbone is connected to side chains consisting of two mannose and one glucuronic acid moieties. The side chains are attached to the main structural element through β-1,3-glycosidic bonds, and some of them are terminated with a pyruvic acid residue. Moreover, the hydroxyl group in position 6 of one or both mannose moieties may be esterified with acetic acid [151]. The conformation of xanthan molecules depends on the temperature.
At physiological conditions, they occur in the form of a helix, while at higher temperatures, the transition into a disordered state is observed. The same process can also be induced by dilution [152].
One of the most important properties of xanthan is its ability to swell and form physical gels revealing shear-thinning properties. The obtained solutions are stable in a wide range of environmental conditions, such as pH, temperature, and ionic strength [151]. Therefore, this polymer is widely investigated as a thickening agent in topical dosage forms, including dermal and ocular formulations. Moreover, swelling properties are advantageous in terms of prolonged release in oral drug delivery, and xanthan is studied as a hydrophilic carrier in matrix tablets.
3.2. Synthetic Polymers
3.2.1. Poloxamers
Poloxamers are synthetic block copolymers composed of hydrophobic poly(propylene oxide) (PPO) units with two hydrophilic blocks of poly(ethylene oxide) (PEO). The building blocks of poloxamer reveal different polarities, and the presence of both elements in the molecule makes it amphiphilic. The hydrophilic-lipophilic balance (HLB) value characterizing amphiphilic properties of poloxamer depends on the molar ratio of propylene oxide and ethylene oxide blocks [153]. The most important representative of this chemical class is poloxamer 407, registered as Kolliphor® P 407, previously known also as Pluronic® F 127 (BASF, Florham Park, NJ, USA) and Synperonic™ PE/F 127 (Croda Health Care, Plainsboro, NJ, USA). It is usually applied as a thickening agent in liquid and semisolid formulations and a solubilizing agent [154,155]. Another polymer frequently applied in pharmaceutical formulations is poloxamer 188. Both compounds differ from each other in terms of molecular weight, which is 4000 and 1800 for poloxamer 407 and 188, respectively. Another difference is EO blocks content, which is 70% in poloxamer 407 and 80% in poloxamer 188. These two parameters are crucial for the physicochemical properties of poloxamers. Their solubility in water increases with the contentof more hydrophilic ethylene oxide units and decreases at higher molecular weights [156]. One of the most important properties of poloxamer is its thermosensitivity. It was demonstrated that the increase in temperature resulted in the increase in the viscosity and the transformation from a liquid system into a semisolid one [157]. As the temperature increases polarity of more hydrophobic PPO blocks decreases that results in their further dehydration. In these conditions, poloxamer molecules form spherical micelles with a hydrophobic core composed of PPO units and a hydrophilic shell built of PEO chains. With a further increase in the temperature, micelles organize into a three-dimensional network, which is related to gelation. This process is fully reversible and takes place at a certain temperature, depending on the polymer concentration, molecular weight, and structure [158]. There are numerous studies describing pharmaceutical formulations with poloxamer composed in a way enabling gelation at physiological temperature [159,160,161,162,163,164,165]. These systems remain liquid at room temperature, which provides an easy application, for example, as an injection, rectal formulation, or ophthalmic drops. At the application site, they transform into gels that may provide a prolonged drug release or increase the residence time in the case of formulations applied rectally or vaginally. However, the lack of mucoadhesive properties is a major drawback of these polymers but can be improved by the addition of another mucoadhesive material [166].
3.2.2. Polyacrylates
Polyacrylates are a group of cationic and anionic synthetic esters of acrylic and methacrylic acids, with different structures and physicochemical properties. They are available in different forms (powders, granules, organic solutions, aqueous dispersions) and commercial products such as Eudragit® (Evonik Industries AG, Darmstadt, Germany), Kollicoat® (BASF, Florham Park, NJ, USA), Eudispert® (Röhm Pharma, Darmstadt, Germany). Specific polyacrylates differ in terms of their abilities of dissolution and swelling. Depending on the structure, they may form coating films with different solubilities at different pH values [167,168]. Mostly they are used as film-forming and coating components in the preparation of tablets, enteric-coated capsules, and oral dosage forms with a modified release. Polyacrylates can also be used to form the basis for semisolid, transdermal, vaginal, and rectal drug delivery systems. A copolymer of methacrylic acid with methyl ester of this acid (Eudispert®) is especially useful in these kinds of formulations because of its bioadhesive properties [168,169,170,171,172].
A special group of polyacrylates isCarbopols®. They are synthetic polymers of acrylic acid. They differ in molecular weight, number and type of crosslinks, and properties, especially viscosity and bioadhesion. The main backbone of these polymers is formed by acrylic acid residues, and its adjacent chains may be cross-linked by an allyl ether radical of sucrose or by pentaerythritol. The carboxyl groups comprise 52 to 68% of weight [173,174].
Carbopols are used as excipients in pharmacy. They play an important role as emulsifiers and emulsion stabilizers (e.g., PemulenTM) [175]. They are also used as release-modifying agents, hydrophilizing substances, binders, and viscosity modifiers. Due to the wide range of useful properties, Carbopols have been employed in numerous drug delivery systems. Aconcentration of 5–15% is used in the formation of capsules and tablets. They are excipients in liquid and semisolid formulations, for example, creams, gels, enemas, lotions, ointments for topical use, rectal and vaginal drugs. Carbopols are also tested for their application in multiple oral drug delivery systems and in the oral mucoadhesive systems with controlled release [174,176,177,178,179,180].
3.2.3. Polyvinylpyrrolidone
Povidone is a synthetic polymer formed by the linearly arranged 1-vinyl-2-pyrrolidone. The degree of polymerization determines the molecular weight of the compound, which influences the properties of polyvinylpyrrolidone [181]. Higher molecular weight causes an increase in viscosity and a decrease in solubility of this substance. Povidone is a white, hygroscopic powder with no specific odor, and it is easily soluble in water and many organic solvents. After oral application, it is not absorbed from the gastrointestinal tract and, when applied to the skin, does not cause irritation or sensitization. The polymer has been used as a stabilizer and thickener of the suspensions and solutions used orally and topically. It is also used as a solubilizer in oral and parenteral formulations, as a binding agent in the wet granulation process, and as a disintegrant in tablet technology [182,183].
3.2.4. Polyethylene Glycol
Polyethylene glycols are also known as macrogols. Depending on the degree of polymerization, they differ in molecular weight and consistency. With molecular weight increase, the increase in the viscosity may be observed, and the physical form can range from liquid to a hard wax. All kinds of polyethylene glycols are soluble in water and miscible with each other. They are stable, hydrophilic substances exhibiting no skin irritation. Furthermore, their removal from the skin is very easy, so they are often used as an ointment base and to prepare suppositories. Macrogols have also been applied in ocular and oral formulations, as well as injections [184,185,186].
4. The Examples of Polymer-Based Vaginal Formulations
Due to the fact that the drug delivered through the vaginal route has to overcome physiological and anatomical barriers to achieve a localized action or reach the systemic circulation, it is important for the drug form to have specific properties. Those are, for example, a long residence time at the site of action, proper parameters of drug release, and adhesion to the mucosa. Mucoadhesive formulations based on the appropriate polymers are particularly interesting and seem to be the most promising in the case of vaginal drug delivery. This group comprises conventional drug forms, e.g., ointments, creams, tablets, and suppositories, as well as newly discovered rings, nanoparticles, or films [187]. All listed drug forms are meant to optimize the action of the drugs administered into the vagina and will be described in detail in this chapter. The dosage form classification applied in this review is presented in Figure 2.
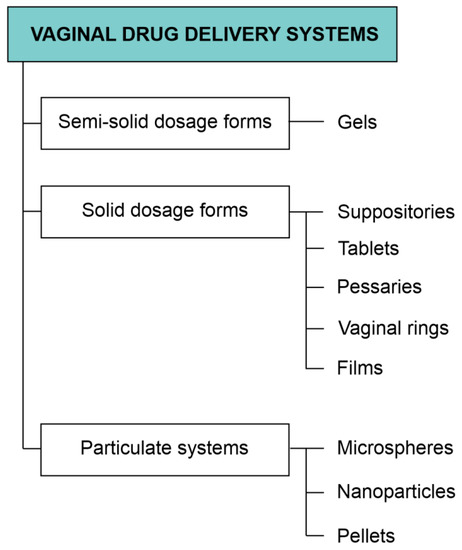
Figure 2.
Classification of the most extensively investigated vaginal dosage forms.
4.1. Semisolid Formulations
Among the most popular semisolid formulations intended for vaginal use, gels, creams, and less frequent ointments are mentioned [32,69,188,189]. The advantages of these systems comprise ease of application, high acceptability, and low production cost. However, semisolid systems are also considered problematic in terms of possible leaks, discomfort after application, messiness, and short residence time at the administration time, which might also contribute to the limited efficacy. In order to improve the therapeutic effect observed as a result of vaginal semisolid products, the therapy sometimes requires frequent administration, which might be considered an inconvenience [188,190]. Another approach involves the application of mucoadhesive polymers responsible for enhancing interactions with mucous membrane and increasing the residence time in the vagina. Some studies indicate the possibility of employing environmentally sensitive polymers increasing the viscosity of the formulation after the administration. In this way, the product is transforming from liquid to semisolid form upon contact with vaginal conditions. An important issue related to the application and effectiveness of vaginal products is acceptability by patients. It is noteworthy that semisolid dosage forms are considered by the patients as convenient in terms of application and are more likely to be preferred over vaginal rings, vaginal suppositories, and vaginal tablets [189,191]. However, it is noteworthy that patients’ acceptance is a complex issue and may depend on many cultural, socioeconomic and other factors [188,192]. Recently, one of the most frequently investigated areas in vaginal drug delivery is related to the formulation of antiviral agents-loaded products as potential preventive products in HIV and sexuallytransmitted infections (STIs). It was shown that in these products, the most important factor affecting patients’ preferences and choices is dosing frequency [193]. In this aspect as the biggest drawback of semisolids their poor retention time is mentioned [194].
4.1.1. Gels
Even though gels frequently occur in numerous scientific and non-scientific areas, the definition of the gel is difficult, and there are several different approaches to the description of these systems. According to Almdal et al. [195], gels are defined as soft, solid-like, or solid material consisting of two or more components. One of the components is liquid and occurs in a significantly higher amount than the other one. The proposed definition also emphasizes the specific rheological properties of gels, which is storage modulus (G’) significantly higher than loss modulus (G”) and exhibiting prolonged plateau. It is also noteworthy that heterogenous materials are excluded from this definition. According to Rogovina et al. [196], the gel is an elastic solid containing two or more components. One of the components is liquid, and the other one forms a three-dimensional network. The type of bonds occurring in the network determines gel type. Chemical gels are bonded with strong covalent bonds, while in physical ones, mostly hydrogen bonds are present. The network-forming component is usually a polymer; however, there is also a possibility to obtain gel with the use of low molecular weight gelators [197]. Considering the type of liquid component, gels can be classified as hydrogels when they are water-based or organogels when the liquid component is non-aqueous. The general classification of gels according to different criteria is depicted in Figure 3. It is noteworthy that gels applied in vaginal drug delivery are mostly weak physical hydrogels obtained with polymer gelling agents.
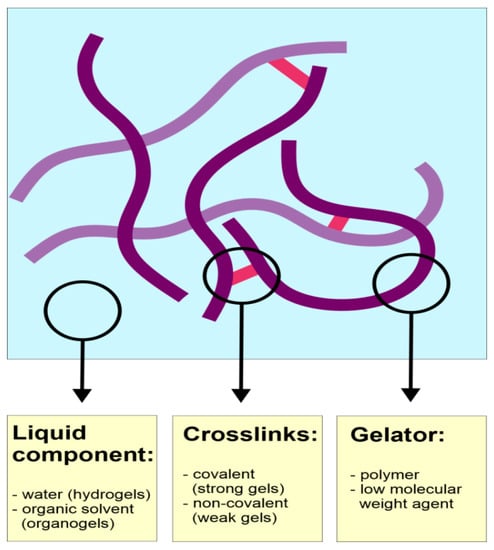
Figure 3.
Classification of gels according to different criteria.
Most of the investigated gel-based dosage forms aim at the delivery of antimicrobial agents in various vaginal infections, including fungal [11,36,198,199] and bacterial ones [12,199,200,201]. However, numerous studies focus on the effective delivery of contraceptive agents and the prevention of HIV transmission [202]. It is important to note that the safety and efficacy of several gel formulations containing mainly dapivirine and tenofovir were subjected to clinical trials [203]. Taking into consideration the most extensively investigated areas in terms of pharmaceutical technology and optimization of drug carriers, mucoadhesive and thermosensitive systems should be mentioned.
4.1.2. Mucoadhesive Drug Delivery Systems
Mucoadhesion occurs as a result of interaction between formulation components and vaginal mucous membrane or mucus layer lining its surface. The most important elements of mucus are mucins, water-soluble glycoproteins revealing a high degree of glycosylation. The subunits of mucin are connected with disulfide bridges and form large three-dimensional gel structures [31,204]. Components of mucoadhesive formulations interact with mucin through hydrogen bonds, van der Waals, or electrostatic interactions. Therefore, the most important feature of potentially mucoadhesive polymers is the presence of a large number of functional moieties, such as hydroxyl or carboxyl, sulfate, and amine groups. Other features positive or negative charges in the molecule, chain flexibility enabling interpenetration of polymer and mucin lattices, and favorable surface properties, allowing for spreading the formulation on the mucous membrane [205].
One of the most commonly used bioadhesive polymers is chitosan, a cationic linear polysaccharide obtained as a product of chitin deacetylation, also known for antimicrobial [206] and wound-healing properties [130]. Bonferoni et al. [207] investigated two types of chitosan differing in molecular weight as carriers for mucoadhesive gels designed for the controlled release of lactic acid. Taking into consideration the differences in the active ingredient release in different media, it was assumed that the release of lactic acid occurred as a result of diffusion and ionic displacement. It was also shown that the lower molecular weight of the polymer was associated with stronger bioadhesive interactions. The same research group [208] analyzed gels obtained with chitosan citrate, which was supposed to chelate calcium cations participating in the regulation of gap and tight junctions. As active ingredients, acyclovir and ciprofloxacin hydrochloride were used. The applied chitosan derivative was also tested for its activity toward proteolytic enzymes, carboxypeptidase A and leucine aminopeptidase. Inhibition of these enzymes is considered advantageous in terms of delivery of hydrophilic and macromolecular compounds through the mucous membrane. Even though the obtained permeation results were satisfactory when compared to controls, the comparison with chitosan hydrochloride did not show any statistically significant differences. Senyiğit et al. [209] analyzed chitosan-based gels with miconazole and econazole nitrates. In the study, the effects of polymer molecular weight on the active ingredients release, as well as vaginal retention and mucoadhesive properties, were investigated. Moreover, the antimicrobial properties of all formulations presented in the study were evaluated. It was shown that the formulation prepared with medium molecular weight polymer revealed the best properties in terms of vaginal drug delivery. Tuğcu-Demiröz et al. [210] presented comparative studies focused on different polymer gels designed for the systemic delivery of oxybutynin, an antimuscarinic agent applied in overactive bladder. As thickening agents, chitosan, hydroxypropyl methylcellulose (HPMC K100M), and poloxamer 407 were applied. The best cohesiveness and mucoadhesion were observed in the case of HPMC K100M. Moreover, the performance of all semisolid formulations in vivo was compared to the marketed product administered in tablets. It was shown that HPMC-based gel could be a suitable alternative to the oral formulation. Cevher et al. [211] investigated hydrogels containing chitosan and polycarbophil covalently modified with thioglycolic acid and cysteine, respectively. The obtained products were applied as carriers for clomiphene citrate for potential therapeutic application in human papilloma virus (HPV) infections. It was shown that polycarbophil and its thiol derivative could extend drug release up to 72 h, while in the case of chitosan and its derivative 12 h release was observed which is less favorable for the purpose described in the study. Moreover, it was found that mechanical properties of the designed systems depended strongly on the type of polymer and also on the content of conjugating agent.
Another frequently applied mucoadhesive polymer is hydroxypropyl methylcellulose (HPMC). Bilensoy et al. [212] formulated hydrogels containing both thermosensitive poloxamer 407 and Carbopol 934 or HPMC as bioadhesive agents. As an active agent, clotrimazole, a poorly water-soluble antifungal agent, was applied. In order to improve the solubility of clotrimazole, an inclusion complex with β-cyclodextrin was used. It was shown that clotrimazole complexation extended its release from hydrogels. Moreover, in the case of Carbopol-based gels, incompatibility resulting fromprecipitation was observed. HPMC-based gels allowed were stable and released the active ingredient in a continuously prolonged manner, which is a promising result in terms of vaginal drug delivery. Aka-Any-Grah et al. [213] presented a study focusing on thermosensitive and mucoadhesive vaginal hydrogels resistant to dilution with vaginal fluids. The investigated formulations contained Pluronic®F127 or a mixture of Pluronics®F127 and F68 as components providing thermosensitivity. As a mucoadhesive agent, HPMC was used. The results obtained with the use ofan ex vivo animal model indicate that in the case of hydrogels obtained with the combination of Pluronics, mucoadhesive properties were not affected by the dilution. On the other hand, both gels retained their gelling temperature close to 30°C even after dilution.
4.1.3. Thermosensitive Dosage Forms
Thermosensitive gels can be classified in more general terms as stimuli-responsive systems, which are defined as systems undergoing thickening upon physiological conditions. In vaginal drug delivery, the most frequently investigated stimuli-responsive systems remain liquid at room temperature and transform into gels at body temperature. Among the advantages of these systems, easy vaginal administration and suitable contact with folds and crevices of the vaginal mucous membrane should be mentioned. As a result of thermogelation, a more viscous medium is formed, which allows for prolonged release of the active ingredient and also improves the retention time at the administration site. The most commonly applied thermosensitive polymers are poloxamers, with the most frequently used poloxamer 407. It is generally regarded as non-toxic and useful as an excipient in dosage forms designed for the application via different administration routes. It also reveals advantageous thermosensitive properties that enable the formulation of liquid systems transforming into gels at physiological temperature range [155]. As a result, the applied formulation is more resistant to removal mechanisms occurring in the vagina [31]. It is noteworthy that gelation temperature and the properties of gel depend on the composition of the system. An important drawback of poloxamer-based systems in vaginal drug delivery is their poor mucoadhesive characteristics. In order to obtain the required residence time at the administration site, additional bioadhesive excipients are applied. Liu et al. [214] investigated the effect of carrageenan addition to poloxamer 407-based in situ forming a vaginal gel. The aim of the study was to obtain the sustained-release formulation for the delivery of acyclovir, a popular antiviral agent useful in the therapy of genital herpes. Carrageenan was considered a suitable excipient for the vaginal drug delivery system because of its efficacy in the prevention of HIV infections. Rheological studies revealed that the additional macromolecular component did not change the gelation temperature significantly. In vitroacyclovir release experiments showed that the process was slower in the presence of carrageenan, which was related to the retardation of poloxamer 407 dissolution and gel erosion. The observed effect depended on the concentration of carrageenan. The residence time was investigated in vivowith the use of a mouse model. In the performed studies, the carrageenan-enhanced system revealed significantly higher residence time compared to plain poloxamer-based gel.
Rossi et al. [201] performed a study focused on the systems composed of poloxamer 407 and chitosan lactate, as well as chitosan lactate and glycerophosphate mixtures. The investigated systems were loaded with amoxicillin trihydrate. The aim of the project was to obtain thermosensitive vehicles forming gel at physiological temperature for potential application in vaginal mucositis. It was found that the additional macromolecular compounds increased the gelation temperature of poloxamer to the physiological values. Gelation time of poloxamer/chitosan lactate mixture was extended after the dilution with simulated vaginal fluid. In the case of the chitosan derivatives mixture, no such effect was observed. However, the latter one displayed worse elastic properties and better bioadhesion than the poloxamer-based system. Zhou et al. [215] investigated thermosensitive in situ forming hydrogel with baicalein for vaginal administration. The active ingredient was applied as an inclusion complex with hydroxypropyl-γ-cyclodextrin. The hydrogel vehicle was obtained with the use of poloxamer 407, poloxamer 188, sodium alginate, hydroxypropyl methylcellulose (HPMC), and benzalkonium chloride. It was found that the obtained formulation had gelation temperature suitable for in situ vaginal gel and the drug release followed the Peppas equation, which indicates an erosion-based mechanism. The analyzed systems also showedsuitable efficacy in thein vivostudy performed with the use of an animal model. Another study describing poloxamer-based in situ forming a thermosensitive gel with incorporated cyclodextrin complex was presented by DeshkarandPalve [216]. The active ingredient employed in the study was voriconazole, an antifungal agent revealing low solubility in water. In the first step, the inclusion complex of the drug and hydroxypropyl-beta-cyclodextrin was obtained by spray drying. Next, in situ gelling formulation was prepared with the use of poloxamers 407 and 188 and various additional polymers as mucoadhesive agents. In the case of vaginal formulations, the suitable gelation temperature should lie within the 30–35 °C range. It was found that the addition of poloxamer 188 increased gelation temperature, while the addition of mucoadhesive agents had the opposite effect. The most promising properties important in terms of vaginal drug delivery were observed for the formulation containing 0.4% of hypromellose as mucoadhesive polymer. The optimized product revealed a gelation temperature of 31.7 ± 0.1 °C and hadsuitable bioadhesive properties. It was also shown that the application of inclusion complex-based gel instead of a plain one improved voriconazole uptake by tissues, which was shown in in vivo studies. A similar study was performed by Rençber et al. [217] for forming gel loaded with clotrimazole, a popular antifungal agent frequently applied in vaginal candidiasis. The optimized formulation composed of poloxamer 407, poloxamer 188 and hypromellose transformed from liquid to gel at about 34 °C. It was also found that the investigated system revealed suitable mucoadhesive properties and remained at the administration site for 24 h.
4.2. Suppositories, Tablets, and Pessaries
Conventional solid vaginal dosage forms, e.g., globules or suppositories, have been in very broad use for many years. Unfortunately, they present a set of drawbacks such as the tendency to irritation and problematic application. Poor retention of the active pharmaceutical ingredients due to the vagina’s self-cleansing or due to leakages may force patients to apply multiple doses daily. All mentioned disadvantages lead to a high inconvenience for the patients and may result in a low adherence and a lack of therapeutic effect. Hence, it has become a challenge for technologists to improve the already existing formulations. The phenomenon of mucoadhesion has become the basis for the development of modern vaginal tablets. Years of research have resulted in the creation of tablets, mini-tablets, pessaries, and other formulations characterized by prolonged vaginal residency, sustained API release, suitable efficacy, and convenience for the patients due to the usage of natural and synthetic polymers with high mucoadhesive properties.
These formulations are mostly used in the topical treatment of bacterial, viral, and fungal infections [129,218,219,220,221,222,223,224], as well as in PrEP (pre-exposure prophylaxis of sexual transmission of HIV) [225,226,227], inflammations [228], atrophic vaginitis [229] and dry vagina [230]. Vaginal tablets have also found application as a carrier of drugs in therapy of cancer [231,232] and probiotics [233]. It is noteworthy that it is crucial for listed therapies to maintain a long vaginal retention time in order to obtain a high effectivity. Hydroxypropyl methylcellulose (HPMC) turned out to be the most commonly used and most promising out of all examined polymers. McConville et al. have proven that the production of tablets containing only one excipient, the sustained-release polymer (HPMC), and releasing efficient doses of tenofovir, an HIV microbiocide, for up to 24 h is plausible [224]. HPMC tablets prepared by Perioli et al. presented prolonged mucoadhesion, very suitable hydration properties with the formation of a homogenous, gelled phase, and, most importantly, prolonged release of benzydamine. Even though Carbopol has brilliant mucoadhesive action, its addition to the formulation eventually resulted in the creation of a spongy, stiff object that could not ensure the linear release of the drug. Other authors supply the data explaining the gains of using HPMC in a combination of polymers [228]. After examining mixtures of HPMC, chitosan, guar gum, and Eudragit RS, Notario-Perez et al. consider joint features of HPMC and chitosan as the most useful. Obtained tablets remained adhered to the vaginal mucosa for 96 h releasing tenofovir for 72 h, which could be used to improve prophylaxis of HIV infection in women from developing countries [225]. A very innovatory solution was proposed by Cevher et al. Combination of mucoadhesive polymers, HPMC or xanthan gum with Carbopol®934P prolonged the formulation’s residence time while the usage of cyclodextrin inclusive complexes enhanced itraconazole’s solubility and antifungal activity and also decreased its toxicity, which led to a prolonged drug residency and effectivity [218]. HPMC could also be used in tablets as a mucoadhesive carrier for Pediococcuspentosaceus SB83, lyophilized bacteria with antilisterial and pH-reducing activity [233], and spray-dried microspheres packed with clotrimazole used in the antimycotic treatment of the genitourinary tract [219]. In this formulation, the combination of polymers (HPMC with sodium carboxymethylcellulose and Carbopol) helped to avoid burst effects when getting in contact with body fluids and provide controlled release of clotrimazole. Literature finds chitosan very suitable for the formulation of mucoadhesive vaginal tablets. Szymańska et al. investigated the features of clotrimazole tablets prepared with different concentrations of chitosan in three different conditions, using a porcine vaginal mucosa, gelatin disks, and mucin gel. The obtained results confirmed the presence of the bioadhesive properties of chitosan. Preparations containing 25% and 40% of chitosan were regarded as the best candidates for further experiments due to their lengthened residence on the vaginal tissue and stable, prolonged release of clotrimazole [220]. Chitosan may also undergo some behavior-changing modifications. The application of thiolated polymers was proposed by Baloglu et al.who designed preparations with econazole and miconazole nitrates and thiolated poly(acrylic acid)-cysteine [221]. Tablets with synthesized polymer possessed favorable water-uptake ratio and mucoadhesive features. It is worth noticing that thiol groups might be instable toward oxidation. Because of this issue, S-protected chitosan synthesized by thiolating the polymer and protecting the thiol groups from oxidation by an aromatic ligand, was obtained. In this case NAC-6-MNA was attached to chitosan by carbodiimide mediated amide bond. S-protected chitosan presented stronger mucoadhesive properties, prolonged the release of metronidazole, an antiprotozoal and antibacterial agent, from vaginal tablets, and enhanced its antimicrobial activity [129]. Pectins could also be used in modern vaginal drug delivery systems. Baloglu et al. claim that formulation consisting of Carbopol 934 and pectin (2:1) would find a possible application as a carrier for topical acting drugs and as a moisturizer in the dry vagina [230]. This mixture was proven to have the highest mucoadhesive strength and swelling volume. Moreover, it presented the lowest pH reduction. Since the vaginal pH is an issue worth considering, the acid-buffering bioadhesive tablets for vaginal infections must be mentioned. pH rise might be either a symptom or the cause of mixed vaginal infections. Tablets containing sodium monocitrate as a buffering agent ensure a pH 4.4, which is a feature of a healthy vagina. Moreover, their other ingredients, drugs such as metronidazole and clotrimazole and Lactobacillus acidophilus spores are efficient in the treatment of genitourinary infections. L. acidophilus normally inhabits healthy vagina and it is responsible for its acidic pH. Polycarbophil and sodium carboxymethyl cellulose presented the most suitable behavior for this composition of active agents [222]. The appearance of hyaluronic acid (HA) in the human organism and its biological functions make this polymer a great candidate for vaginal drug delivery. Its structure may be modified to obtain even better properties. Nowak et al. thiolated and preactivated it with 6-mercaptonicotinamide, which effectedhigher stability and enhanced the mucoadhesive values [234]. This solution helps to use the mucoadhesion ensured by disulfide bond formation from thiol groups yet still keeps the substance stable. Moreover, it was proven that HA itself may act as the therapeutic agent, not only the drug carrier. Vaginal tablets containing 5mg of hyaluronic acid were compared with 25 µg estradiol tablets. Both groups turned out to be successful in the therapy of atrophic vaginitis. Even though estradiol is still preferable, HA might find application in patients in which hormonal treatment is contraindicated or undesirable [229].
Mini-tablets have also gained some great attention lately. This dosage form is considered to be an improved formulation of conventional tablets. Numerous polymers were investigated for the production of mini-tablets targeting the vaginal route of administration by Hiorth et al. [231]. The goal of the researchers was to find a perfect formulation to deliver hexyl aminolevulinate hydrochloridum (HAL), a potential topical drug used in the photodynamic therapy of cancer, e.g., cervical cancer, to the vagina. Hydroxypropyl cellulose (HPC) and hydroxypropyl methylcellulose (HPMC) presented adequate mechanical properties, bioadhesive strength, and the release of the drug independent of the vaginal pH, which is crucial because vaginal delivery systems should consider that pH, viscosity, and many other features may vary and are influenced by woman’s age, hormone levels or sexual activity. Methylcellulose, microcrystalline cellulose, and hydroxyethyl cellulose showed no mucoadhesive properties and released whole drug doses within a few minutes. Multiparticulate drug delivery systems such as mini-tablets sized 1–3 mm provide a better spread of the drug inside the vagina, ensure a faster disintegration, longer retention, and even a loss of a few mini-tablets has less impact than in the conventional forms. Mini-tablets might be packed into capsules or applicators, which makes them easy to administer, causes no irritation, and even distribution. These advantages may help to raise the patient’s compliance and maintain a high therapeutic effect.
McConville et al. proposed a simple yet innovative and effective approach to the topic of multipurpose prevention technologies by forming multi-layered tablets helping to avoid pregnancy and sexually transmitted diseases [226]. Thanks to the use of Kollidon® SR and Kollidon® VA, desired drug release profiles and possible in vivo action were obtained. The drugs used in the experiment were antiretroviral dapivirine, contraceptive hormone levonorgestrel, and anti-herpes simplex agent acyclovir. Authors formed tablets consisting of 3–4 layers presenting the immediate or sustained release of API. Results were very promising and indicated a possible introduction of multifunctional multi-layered tablets to the pharmaceutical industry. Prepared tablets, for example, ensured an immediate boost of active substances with a prolonged liberation of dapivirine, which would provide contraceptive action as well as antiviral action. Using these formulations could possibly decrease the number of administered forms and lead to higher patients’ comfort, which would result in higher compliance and satisfying therapeutic effects. Described multifunctional dosage forms could be extremely useful in developing countries to stop the HIV epidemics and immense birth rate.
Osmotic pump tablets (OPTs) are known as an oral drug delivery system, but according to Rastogi et al., the vaginal route of administration is also an option for them [227]. The research team used a potential antiretroviral drug IQP-0528 to form vaginal tablets coated with a bioadhesive polymer (cellulose acetate or cellulose acetate phthalate) with a standard mechanism connected to water intake and release of the drug-loaded gel through an orifice. The results of the study proved that it is possible to prepare tablets delivering active agents in the vagina for 2–5 days. Furthermore, osmotic pump tablets may present the pH-dependent burst release of the drug. This phenomenon can be used to design an HIV-preventing formulation activated by the appearance of semen, which causes a pH change in the vaginal canal. Hence, the OPTs could improve patients’ adherence and effectiveness to PrEP. Even though the pessaries are not so popular, they might be as useful as other vaginal dosage forms. Ceschel et al. developed pessaries of semisynthetic solid triglycerides containing bioadhesive polymers such as polycarbophil, HPMC, and hyaluronic acid sodium salt, which keep the formulations in the vaginal tract for several days without any unwanted reactions. Described pessaries make a suitable carrier for imidazole antimycotic derivatives used to treat frequent mycotic infections, e.g., clotrimazole [223].
4.3. Vaginal Rings
There are several rings for contraception available in the pharmaceutical market: NuvaRing® (Merck and Co., Kenilworth, NJ, USA), Progering® (Laboratorios Andrómaco SA, Peñalolén, Chile), Annovera® (TherapeuticsMDInc, Boca Raton, FL, USA), Ornibel®/Ginoring® (Exeltis, Madrid, Spain) andEluRyngTM(Amneal Pharmaceuticals, Bridgewater, NJ, USA) NuvaRing® is made of ethylene vinyl acetate(EVA) copolymers. Its thickness is about 4 mm, and its diameter is 54 mm. It releases etonogestrel 0.012 mg and ethinyl estradiol 0.015 mgper day. It is used for 3 weeks, and a week interval between the subsequent applications is required. In contrast, Progering® was made of silicone elastomer. It provides 10mg of progesterone per day for 3 months. The subject of some clinical research studies isformulations combining antiviral and contraceptive action. Their aim is to increase the effectiveness of contraception and to prevent sexual transmission of HIV. The purpose of the research conducted by Thurman et al.was to compare the characteristics of vaginal rings and oral contraception [235]. It was found that topical delivery of the drug through the vaginal ring allowed for the reduction in drug doses and was associated with avoidance of a first-pass effect in the liver.
Another advantage of the vaginal rings is less pain and shorter menstruation. They are also comfortable in their stand-alone application and in control. These rings should not be felt during daily activities and do not interfere with sexual behavior. However, they can cause bleeding and vaginal inflammation.
4.4. Microspheres
More than 20 years ago, polymeric microspheres were evaluated as a carrier for drugs for vaginal application. Microspheres from hyaluronic acid esters as the carrier for salmon calcitonin were prepared by Rochina and co-workers [236]. They used the solvent extraction method for formulation. Spherical microspheres with smooth surface and diameter of about 10 µm were obtained. The efficiency of incorporation was high; approximately 80% to 90% of the peptide was recovered by extraction from the microspheres. Quantification of the extracted peptide in vivo confirmed that the biological activity of calcitonin was unaffected by the microsphere preparation process. Hyaluronic acid is the polymer that was also used for the study concerned with the possibility to restore the vaginal ecosystem with the microparticles containing probiotics and prebiotics. In 2011 Pliszczak et al. [237] published the results of the study of the design of a new vaginal bioadhesive delivery system based on pectinate-hyaluronic acid microparticles for probiotics and prebiotics encapsulation. Microparticles were produced by the emulsification/gelation method using calcium ions as the cross-linking agent. Inthe beginning, the influence of the main formulation and process parameters on the size distribution of unloaded microparticles wasconducted. Rheological measurements were also performed to investigate the bioadhesive properties of the gels used to obtain the final microparticles. Afterward, an experimental design was performed to determine the operating conditions suitable to obtain bioadhesive microparticles containing probiotics and prebiotics. The encapsulation system could enhance the effects of Lactobacillus sp. and protect them during the drying process and storage. The final microparticles had a mean diameter of 137 µm and allowed a complete release of probiotic strains after 16 h in a simulated vaginal fluid at 37 °C. Chitosan-alginate microspheres were developed by Maestrelli et al. [238] for cefixime vaginal administration to overcome problems associated with its oral administration. They prepared microparticles through ionotropic gelation using calcium chloride as the cross-linking agent. Entrapment efficiency increased with drug loading concentration in the starting solution, reaching a plateau at 30 mg/mL indicative of the achievement of an optimal drug-to-polymer ratio. The swelling properties of microspheres increased with the entrapped drug amount, and, interestingly, wateruptake reached its maximum value at the same drug loading concentration of 30 mg/mL. The relationship found between microspheres wateruptake and drug release rate confirmed the microspheres prepared with 30 mg/mL cefixime as the best formulation. Mucoadhesion studies indicated that all formulations assuredin situpermanence longer than 2 h. Microbiological studies showed the relation between cefixime release rate from microspheres and Escherichia coli viability reduction. They concluded that evaluated microspheres formulation could be used for effective local treatment of urogenital infections. The other technique for the microsphere preparation is the spray drying process, which was used by different groups and for different polymers [219,239]. Zhang et al. [239] used polymethacrylate salt for the delivery of tenofovir (a model HIV microbicide) and investigated spray-dried mucoadhesive and pH-sensitive microspheres. It has been shown that the sodium or potassium salts of the methacrylic copolymers Eudragit®L-100 and S-100 have the potential as a novel low-swellable mucoadhesive material. The optimized formulation has an average size of 4.73 µm with adrug loading of 2% (w/w). It has been shown that these microspheres can quickly respond to the pH change, releasing over 90% of the drug within 60 min. The mucoadhesion property of these microspheres is significantly improved compared to the 1% HEC gel formulation. Moreover, the findings in this study reveal that these microspheres arenoncytotoxic and non-immunogenic to vaginal/endocervical epithelial cells. There is also no observable cytotoxic effect on normal vaginal flora. In addition, Gupta et al. [219] used the methacrylic acid copolymers for the microsphere preparation. The aim of the research carried out by their team was the preparation and evaluation of vaginal tablets containing clotrimazole in the form of microspheres. To achieve a long-term therapeutic effect at the site of infection, mucoadhesive polymers: hydroxypropyl cellulose (HPMC), sodium carboxymethyl cellulose, and Carbopol® 934 were used as excipients for the tablets formulation. These microspheres with clotrimazole were prepared by using the spray drying technique with Eudragit RS-100 and Eudragit RL-100. The results indicate that the developed vaginal formulations exhibit controlled drug release. Next to spray-drying, spray-congealing is an interesting method of preparing mucoadhesive microparticles. It was evaluated by Albertini et al. [240], who investigated adhesive microparticles for the vaginal delivery of econazole nitrate. They prepared microparticles based on a lipid-hydrophilic matrix containing both a drug and a mucoadhesive substance with spray-congealing. This method, consisting ofthe atomization of dispersion of the drug in a molten carrier, is a solvent-free technique, which may be advantageous for the preparation of mucoadhesive microparticles. Several mucoadhesive polymers (chitosan, sodium carboxymethyl cellulose, and poloxamers) within the hydrophilic-hydrophobic meltable matrix (Gelucire 53/10, Gattefossé, France) were evaluated. The results showed that the solubility of econazole increased 15 times when it was microencapsulated in the Gelucire 53/10. Albertini et al. concluded that this fact could be correlated to the carrier’s amphiphilic structure (HLB = 10). Once the carrier dissolves in the fluid, it assembles into micelles arranging the hydrophobic part, which includes the drug inside and the hydrophilic portion, which acts as an interface between the simulated vaginal fluid and the drug outside. The addition of poloxamers to the lipophilic carrier provided the same effect, while the addition of chitosan and sodium carboxymethylcellulose to the carrier decreased the API solubility compared to Gelucire 53/10 used alone. This could probably be caused by the fact that the solubilization of the polymers interferes with the effect of the drug wettability and solubility enhancement due to the carrier [240]. In addition, the mucoadhesive properties of the microparticles were investigated. The residence time of the antifungal agent at the infection sites of the vaginal mucosa tissue are very important and mucoadhesive properties can increase it. The particles with the poloxamers showed the best results of the mucoadhesion test. Researchers concluded that spray-congealing technology may be considered as a novel and a solvent-free approach for the production of mucoadhesive microparticles for the vaginal delivery of econazole nitrate.
4.5. Pellets
Pellets are a kind of granules. Their sizes range from 300 to 1000 microns. Due to the small size, it can be expected that after vaginal application, they will stay at the surface of vaginal mucosa and will be less susceptible to the force of gravity than vaginal tablets. It is suggested thatpellets can be used as carriers for active substances or as matrices for probiotic bacteria [94,222]. Santos et al. [241] studied whether the addition of the carrier material itself affects the natural protective microflora in the vagina. They used starch-based pellets and lyophilized lactose-based pellets with probiotic bacteria. Gelatin capsules were filled with pellets and prepared for vaginal application. A non-treated control group was included to follow the natural evolution of pH and microflora during the menstrual cycle. No adverse effects on the vaginal and ectocervical mucosa were observed throughout the study period. Researchers concluded that fast-disintegrating starch pellets and lyophilized lactose/skimmed milk are acceptable carrier materials for the vaginal delivery of probiotic strains or other drugs. The research conducted by Poelvoorde et al. [106] focused on the properties of the vaginal non-disintegrating microcrystalline cellulose or disintegrating starch-based pellets. Pellets were administered to patients after being placed in hard gelatin capsules or capsules made from hydroxypropyl methylcellulose (HPMC). Researchers evaluated in vivo behavior (vaginal distribution and retention) and patient acceptability (irritation, discomfort) of pellets. Immediately after application, capsules made of HPMC exhibited better mucoadhesive properties, while the gelatin capsules presented a faster degradation. After the release from the capsules, pellets made from starch decomposed much faster than pellets based on microcrystalline cellulose. Although in vitro disintegration was faster for hard gelatin capsules compared to HPMC capsules, their in vivo behavior was similar as two out of five were still intact 6 h after administration. The authors concluded that slow capsule disintegration would limit the drug release rate. However, the disadvantage could be eliminated if pellets were administered using an applicator with a different design that does not require that pellets be packed in the capsule. Due to the disintegration of starch-based pellets, this formulation probably spread more easily over the vaginal mucosa and was better retained, although high-amylose starch (the main ingredient of the pellets) did not have mucoadhesive properties. A continuation of this work was a comparative analysis of starch pellets and a cream of cetomacrogols conducted by Mehta et al. [104]. They wanted to demonstrate the differences in the deposition of tracer substances after vaginal application. The authors used a technique of gamma scintigraphy and a magnetic resonance imaging method. The studies have been conducted on animals (sheep) and a group of human volunteers. It has been shown that pellets as a result of fast disintegration, covered vaginal epithelium to a degree similar to cream. Further research performed by Metha et al.was based on the preparation of fast-disintegrating tablets with pellets. They hypothesized that tablets would have a shorter disintegration time compared to the capsules, so pellets would distribute faster throughout the vaginal cavity with persistent longer retention [105,242]. The research team evaluated pellets compressed into fast-disintegrating tablets for their distribution and retention in sheep and women using gamma scintigraphy and MRI techniques. In sheep, the tablet disintegration was initiated within 30 min after administration, and within 2–4 h, the entire vagina was covered with the disintegrated pellets with a persistent spread up to 48 h. In women, disintegration was complete within 4 h, and persistent retention was up to 24 h [105]. The suitable intravaginal distribution and long retention time of the disintegrating tablets comprising starch-based pellets provide an interesting vaginal drug delivery platform. These tablets can be further explored as carriers for intravaginal delivery via the incorporation of drugs from different therapeutic groups in the starch-based pellets. On the basis of the research described above, some studies with bioadhesive pellets were prepared by Hiorth et al. [243]. The aim of the study proposed by this group was to develop bioadhesive pellets containing hexyl ester 5-aminolevulinic acid, a precursor of the photoactive substance, with a fast release for vaginal drug delivery. In contrast to the reported disintegrating pellet-based system, the aim of the current study was to develop bioadhesive pellets with a fast release of the active substance. Pellets were produced by extrusion/spheronization, and Carbopol® 934 was used to obtain bioadhesive properties that prolong the residence time in the vaginal tract. Researchers wanted to demonstrate the usefulness of polymers in the treatment of cervical cancer with the photodynamic method. It has been shown that the content of 8% of Carbopol had a positive impact on the mucoadhesive properties of pellets. They showed bioadhesive properties toward vaginal tissue. Investigated pellets were mechanically stable and released the drug load within 20 min in phosphate buffer at pH = 4.0 and 6.8 in the in vitrodissolution test. In addition, the investigated dosage forms exhibited a stability time of 6 to 7 weeks. Proposed delivery systems were suitable for the administration of hexyl ester 5-aminolevulinic acid to the vaginal cavity.
4.6. Nanoparticles
In recent years polymeric nanoparticles (NPs) have been widely described as the carriers of drugs for vaginal administration, for locally and systematically acting medicines. NPs are highly stable particles characterized by sizes under 1000 nm [244]. They can encapsulate a wide range of APIs and provide a controlled, prolonged and targeted delivery. The main purposes of the use of NPs in vaginal drug delivery comprise efficient delivery of microbicides, targeted delivery of siRNA, HIVprevention, tumors treatment, delivery of hydrophobic substances, prevention or treatment of sexually transmitted diseases, or delivery of antibiotics [245,246,247,248]. Either natural (e.g., chitosan, hyaluronic acid) or synthetic polymers can be used to prepare such dosage forms. Most researchers focus on synthetic compounds, including poly(lactic-co-glycolic) acid (PLGA),polyethylene glycol (PEG),(meth)acrylate polymers, polyesters (polycaprolactone), and many others. NPs for vaginal administration include a few types of dosage forms: polymeric nanoparticles (NPs), liposomes (LIPs) or cyclodextrins (CD), nanocapsules (NC) nanospheres (NS) [249,250,251,252]. NPs can solve some problems with drug formulation, e.g., poor water/oil solubility, degradation of API, toxicity, or unpleasant organoleptic properties.
4.6.1. Poly(lactic-co-glycolic) Acid
The most described polymer regarding NPs has recently been PLGA. Das Neves et al. tried to formulate the NPs based on PLGA loaded with dapivirine to provide effective delivery of this antiretroviral drug. They used an emulsion-solvent evaporation method and obtained particles with a mean diameter of 170 nm. The formulation was characterized by an initial burst effect up to 4 h followed by a sustained release for 24 h and a lower or at least similar toxicity compared to the free drug. Furthermore, drug retention in cell monolayers was significantly higher for the NPs compared to the free drug [245]. The evolution of vaginally-administered HIVprevention brought the combination of two or more antiretroviral drugs in one medical product. A study conducted by Cuhna-Reis et al. aimed to formulate a novel dosage form containing PLGA-based NPs loaded with tenofovir and efavirenz incorporated into a polymeric film, NPs-in-film. In vivo tests ran on mice revealed enhanced vaginal NPs retention and drug concentrations as well as prolonged drug release, compared to the administration of the same drugs in aqueous solutions. Moreover, the systemic exposure to both drugs was low, and the NPs-in-film was found to be safe for vaginal administration, as it caused no significant genital nor histological changes after application [249]. NPs-in-film has recently gained more interest in the case of antiretroviral delivery for HIV prevention. Work published by Machado et al. describing tenofovir-loaded poly(lactic-co-glycolic acid) (PLGA)/stearylamine(SA) composite NPs with a mean diameter of 127 nm, incorporated into hydroxypropyl methylcellulose/poly(vinyl alcohol)-based film, presented a formulation that could release NPs in just 9 min upon contact with the simulated vaginal fluid (SVF). The release was characterized by an initial burst (around 30% of the drug in 15 min), followed by a sustained release up to 24 h. Described dosage form was found tolerable for vaginal delivery and did not induce any histological changes or pro-inflammatory response, as administered upon 14 days to mice [253]. Many different compounds could be effective for vaginally-administered anti-HIV prevention, not only antiviral APIs. One of those ingredients is siRNA (small interfering RNA). Forthat purpose, Gu et al. tested the poly(ethylene glycol) (PEG)-functionalized poly(D, L-lactic-co-glycolic acid) (PLGA)/polyethylenimine (PEI)/siRNA NPs (siRNA-NP) prepared with a modified emulsion-solvent evaporation method. These PLGA-based NPs were functionalized with HLA-DR antibodies for targeted delivery to dendritic cells and loaded into a biodegradable film. NPs were rapidly released from the film after administration and were able to penetrate the epithelial layer and act locally with targeted cells [246]. PLGA-based NPs are also a suitable carrier for drugs in tumor treatment. Local delivery of chemotherapeutics may reduce systemic adverse reactions. Yang et al. presented a paper describing paclitaxel-loaded PLGA-based NPs (Figure 4). They have made some very interesting and important observation by comparing the mucoadhesion of conventional particles (CP) and mucus penetrating particles (MPP) coated with Pluronic F127. The first ones, as mucoadhesive structures were aggregated in cervical mucus (CVM) and did not achieve a proper distribution close to the tumor cells, while MPPs rapidly penetrated CVM and reached the targeted area. As a result, MPP suppressed the tumor growth more effectively and provided a sustained release, with a minimal effect of the initial burst [247].

Figure 4.
Characterization of PTX/PLGA nanoparticles in vitro. SEM images of (a) PTX/MPP and (b) PTX/CP; scale bar represents 1μm. (c) Cumulative in vitro release of PTX from PTX/PLGA nanoparticles over time [247].
Further coating functionalization of the NPs was proposed by Sims et al. They created PLGA-based NPs and coated them with MPG-a cell-penetrating peptide, PEG, MPG/PEG, and vimentin, respectively, and assessed the penetration in 3D human carcinoma cervical cell culture. As a result, they observed an even 66-fold increase in cell internalization in the case of MPG-NPs. The uptake of carcinoma cells was significantly enhanced, and PEG-NPs’ penetration was two-fold higher than MPG-NPs [254].
4.6.2. Polyethylene Glycol
The key polymer for mucus penetration is PEG-neutral, hydrophilic, and minimalizing mucoadhesion, allowing NPs’ compounds to penetrate through the MCV. Such properties of PEG were confirmed by Maisel et al. in their research. They had proven its anti-mucoadhesive feature ex vivo on human CVM and then administered PEG-coated NPs to the cervicovaginal tract of a mouse. As a result, they observed uniform distribution into the vaginal epithelium [255].
Jøraholmen et al. developed PEGylated liposomes with a diameter of 181 nm, able to penetrate MCV, containing interferon alpha-2b for the local therapy of human papillomavirus (HPV). In vitro, they observed no release, but ex vivo tests revealed an elevated TNF α-2b penetration compared to the control group. No mucin interactions were observed, so PEGylated liposomes could reach the deeper epithelium [250]. Another way to treat HPV-induced cervical lesions was proposed by Lechantour et al. They investigated the siRNA-loaded PEGylated lipoplexes for vaginal administration. In vivo studies in mice revealed a complete and sustained coverage of the mucosal epithelium, following a unique vaginal administration of fluorescent PEGylated lipoplexes. Coating lipoplexes with PEG allowed the release of active siRNA into the cytoplasm of HPV-positive cells and consequently induced biological responses and prevented the mucin proteins from aggregation on lipoplexes [256]. PEG is also a suitable polymer for the delivery of photosensitizers. Wang et al. presented boron-dipyrromethene (BDP)-loaded PEG-based NPs, obtained via the solvothermal method. Studies showed that NPs led to an improvement in both cellular uptake and mucus penetration in vitro and in vivo compared to BDP-loaded polymeric micelles. Authors concluded that the excellent photothermal activity of prepared formulation, inducing: tumor apoptosis upon irradiation, its high efficacy, and safety, make the NPs a promising tool in the treatment of severe cervical intraepithelial neoplasia [257].
4.6.3. (Meth)acrylate Polymers
Other compounds suitable for nanocarriers are numerous (meth)acrylate polymers. NPs prepared by Frank et al. were based on Eudragit® RS100 and Eudragit® S100, loaded with the Nile red, as a model of lipophilic substance and incorporated into chitosan gel as an intravaginal medium. NPs sized approximately 200 nm showed a higher penetration of nile red, especially in the case of nanocapsules (Eudragit® RS100), compared to free drugs [172]. The polymer itself is a base in the formulation prepared by Santos et al. The aim of this study was to create a coconut oil-core with the Eudragit®RS100 shell NPs, loaded with clotrimazole for candidiasis treatment. NPs were prepared with interfacial deposition of the polymer and presented an average diameter lower than 200 nm and high encapsulation efficiency, close to 100%. In vitro studies revealed higher stability against UV radiation for encapsulated clotrimazole and a prolonged release with no burst effect, whicheffected higher activity against Candida albicans and Candida glabrata [251]. In the study conducted by Melo et al., a continuation of nano-based antifungal dosage form was presented. The formulation based on Eudragit® RL100 was loaded with amphotericin B (AMB) and coated by hyaluronic acid (HA). NPs obtained by nanoprecipitation and coated by adsorption techniques exhibited approximately 148 nm of diameter and were characterized by a controlled API release during 96 h, followed by the zero-order kinetic profile. This manner provided constant therapeutic doses of AMB that inhibited the in vitro growth of C. albicans. In vitro studies ran on rats showed a rapid suppression of the 100% vaginal fungal burden in 24 h. Furthermore, it was suggested that HA coating interacted with the CD44 receptor on epithelial cells, and as a result, NPs might be internalized to efficiently exert their antifungal action [248].
4.6.4. Polyesters (Polycaprolactone)
Polycaprolactone (PCL) is a base polymer of NPs prepared in the work of Frank et al. Authors aimed to increase the adhesion and penetration through the vaginal mucosa in order to treat HPV infections bycombining nanocarriers and mucoadhesive semisolids. For this purpose, two formulations were obtained: (a) chitosan-coated poly(e-caprolactone)-nanocapsules incorporated into hydroxyethylcellulose gel, and (b) poly(e-caprolactone)-nanocapsules incorporated into chitosan hydrogel. As a result of their studies, chitosan-coated NCs combined with mucoadhesive gel wasdescribed as the most promising dosage form considering the permeability, mucoadhesion, and drug retention [258]. Different methods were used to obtain a similar goal by Varan et al. in their paper. Both anticancer (paclitaxel) and antiviral (cidofovir) drug combination was manufactured by inkjet printing onto an adhesive film to locally treat cervical cancers induced by HPV infections. Poorly soluble paclitaxel was encapsulated into a cyclodextrin complex, and cidofovir was encapsulated in polycaprolactone NPs sized below 200 nm (Figure 5). In vitrostudies showed effectiveness on human cervical adenocarcinoma cells with the synergistic effect of two drugs. Other advantages of such dosage form are personal dose fixing and prolonged-release possibilities [252].

Figure 5.
SEM photomicrographs of (a) free PCX (b) PCX:HP-β-CD, (c) PCX:6-O-CaproβCD, and (d) PCX:PCβCDC6 inclusion complexes [252].
PCL is also suitable to deliver the antifungal itraconazole. The authors obtained NCs and NSs by the nanoprecipitation method. Formulations were characterized by a high encapsulation efficiency, 99% and 97%, respectively, and the size below 190 nm and 120 nm, respectively. Then, NPs were incorporated into a vaginal viscous formulation and administered to female mice infected by C. albicans. Results showed high efficiency in fungal reduction only for NCs, compared to NSs and the drug solution. Furthermore, histological analysis showed significant differences between tissues correlated with inflammatory cytokines levels. NC-treated animals showed reduced cytokine levels, while NS- and solution-treated mice showed increased levels of cytokines and tissue inflammation. This shows a high potential of PCL-NCs in itraconazole treatment improvement and cytotoxicity reduction [259].
4.6.5. Polymers of a Natural Origin
Polymers of a natural origin are also investigated as a base of nanocarriers. One of the most described natural polymers is chitosan. Jøraholmen et al. prepared chitosan-coated LIPs loaded with clotrimazole for the local vaginal infection treatment in pregnant women in order to avoid systemic absorption. Sonicated liposomes were coated with chitosan in three different concentrations: 0.1%, 0.3%, and 0.6%. Their sizes ranged from 100 to 200 nm. In vitro release study showed a prolonged release of clotrimazole while the ex vivo experiments performed on the pregnant sheep vaginal tissue revealed that coating with chitosan assured an increased API tissue retention and a reduced penetration compared to the control. Lower chitosan concentration provided a higher mucoadhesive potential [250]. Chitosan NPs also have the potential to deliver peptides. In the work of Marciello et al., such NPs obtained by the ionotropic gelation method with pentasodium tripolyphosphate were incorporated into freeze-dried cylinders. In vitro release studies of insulin as a model peptide showed a rapid release with the burst effect, where more than 50% of the peptide was released during the first 15 min of the experiment. Nearly 100% of the peptide was released within 30 min. The nanoparticles’ ability to promote the peptide penetration into the vaginal mucosa was also proven during the studies (Figure 6) [260].
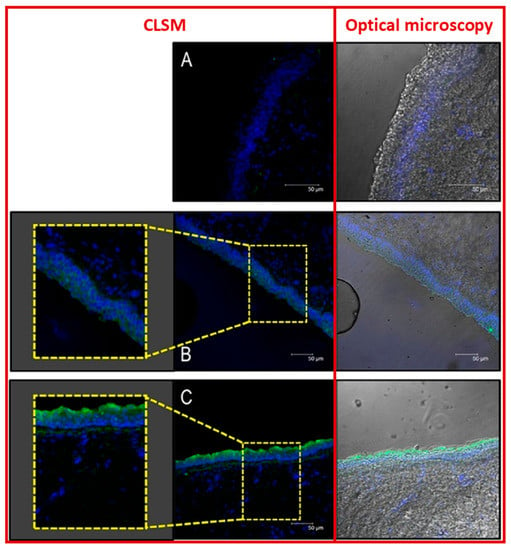
Figure 6.
CLSM (confocal laser scanning microscopy) images of porcine vaginal mucosa alone (A), placed in contact with a solution of insulin-FITC (B) and with a suspension of insulin-FITC loaded CS NPs (C). Zoom of a CLSM picture detail and an overlap with a micrograph of the same mucosa zone obtained by optical microscope.
The same method to obtain chitosan NPs was used by Rossi et al. They aimed to develop a formulation containing amoxicillin trihydrate-loaded NPs and to incorporate it into a fast-dissolving matrix for the treatment of atrophic vaginitis. NPs showed an in vitro mucoadhesion, wound healing (due to the presence of ascorbic acid), and improved antimicrobial properties, as referred to as a solution. Furthermore, NPs released in SVF from the matrix presented an unchanged size [261].
4.7. Vaginal Films
Vaginal filmsare another form of drug delivery systems formulated using a variety of polymers for achieving mucoadhesion as well as desirable release profiles of the actives. As a result, they are capable of combating some of the challenges presented in vaginal drug delivery: pH, cervical secretions, permeability, etc.
The films are solid dosage forms mostly prepared using aqueous polymers and plasticizers and may containan active ingredient [12]. They are usually preferred over traditional semisolid formulations because of patient-friendly application, better residence time, higher stability over a variety of conditions, and even aesthetic advantages [194,262,263]. They are usually soft, flexible, preferably colorless and odorless, and disperse or dissolve upon coming in contact with vaginal fluids to adhere and retain in the vaginal mucosa for prolonged durations [264]. Several polymers have been investigated over the years for formulating vaginal films, the most commonly used ones being polyvinyl alcohol [265,266,267,268,269,270,271] and cellulose derivatives [272,273,274] or a combination of both [194,249,253,275,276,277,278]. Other polymers have also been explored with or without the previously mentioned common options [223,263,279,280]. Cellulose acetate phthalate was initially considered an inactive pharmaceutical ingredient with film-forming properties but was later found to have antiviral activity of its own against genital herpes virus [281] and HIV [282] and has been formulated into a composite microbicidal vaginal film with hydroxypropyl cellulose while maintaining activity [272]. The most commonly used plasticizers to achieve desirable film characteristics are polyethylene glycol (PEG) and glycerine, but others have been used as well.
The most widely employed method for the fabrication of vaginal films is the solvent casting method [264], where solutions of polymers, plasticizers, actives, and other excipients are poured in a mold that is cast into films upon drying either at room temperature or under mild heating. The films are then cut into individual films if not poured directly into single film-sized molds [264].
More recently, Regev et al. developed microbicidal vaginal films containing dapivirine using the hot-melt extrusion (HME) technique while using a quality-by-design (QbD) approach [283]. When compared with solvent cast (SC) films of similar compositions, it was found that the HME films were thicker, heavier, had lower water content, and disintegrated faster than SC films while still being within acceptable attribute ranges for vaginal films. Even if not significantly advantageous over solvent casting, HME could be helpful to achieve continuous manufacturing and easier scalability.
The traditional vaginal film formulations are often modified to achieve additional advantageous properties. Cautela et al. formulated three types of composite films for delivery of two anti-HIV drugs: a single-layer film, a double-layer film with two halves of the film cast separately and bound together using a hydraulic press and nanoparticles (NPs) in film that contained a layer of drug-loaded NPs evenly dispersed and sandwiched between two non-drug films by means of a hydraulic press. The fastest drug release followed by an initial burst release was seen with the single-layer films, followed by the double-layer film, and finally, the slowest release was observed with the NPs-in-film, suggesting different ways to achieve a variety of drug release profiles as per therapeutic need [268]. Another recent innovationhas been demonstrated by Machado et al.in the form of a vaginal sheet, which consisted of a gelatin-based gel freeze-dried to form a sheet [284]. Formulated with lactose as a model powdered ingredient, the vaginal sheet was able to hold desired organoleptic characteristics, including texture, and showed buffering capacity with vaginal fluid stimulant (VFS). Garg et al.described films as three basic types: fast-disintegrating (flash release or flash dispersal films), non-disintegrating films (can be used to control residence time when combined with fast-disintegrating films), and medium disintegrating films [285]. Notario-Pérez et al. classified films based on film solubility: hydrophilic films (containing hydrophilic polymers and polar plasticizers) and non-water-soluble films (containing hydrophobic or amphiphilic polymers (to prolong drug release and residence time); based on film structure, monolayer single-polymer films, monolayer blend films, bilayer films, and multilayer films; and based on release mechanisms, stimuli-responsive or smart films [286].
Garg et al. suggested that a film formulation should be used as the delivery system when an intermediate onset of action is required in a product with moderate stability (in specialized packaging) when stored in ambient conditions [287]. Due to maximum efficacy, some crucial factors must be considered during the development of vaginal films, e.g., mucoadhesion, disintegration, drug release, stability, physicochemical characterization, mechanical properties.
Vaginal films have been investigated for a number of applications, with the most common ones being microbicidal owing to the most frequent diseases that affect the vagina. A strategy for employing microbicidal vaginal films is as a prophylactic tool for sexually transmitted diseases (STDs) [264,286]. Films have gained acceptability and preference over the traditional vaginal formulations for their patient-friendly use [288]. A variety of active ingredients have been loaded in vaginal films to find antiviral [281,289], antibacterial [12,290], and antifungal [291,292] applications. Vaginal films have also found their use as contraceptive devices due to their discrete nature and their ability to not only form physical barriers but also that of carrying spermicides. Frankmanet et al. showed the clinical relevance of C-film, a nonylphenoxypolyethoxyethanol vaginal film that was a reliable alternative to traditional contraceptive devices at the time [293]. Garg et al. developed and characterized sodium polystyrene sulfonate (PSS) noncytotoxic contraceptive films [194]. Multipurpose prevention technologies (MPT) that work as contraceptives while providing protection against STDs have gained a lot of interest fromresearchers as well as consumers [294,295]. Nonoxyl-9 (N-9) was one of the earliest marketed agents that showed multipurpose applications but did not prove to be very safe in later studies but has led to the development of other products with better safety and efficacy [296]. A combination of drugs hasbeen used in film formulations for MPT benefits or to have higher efficacy compared to single drug delivery systems [249,266,277,285]. Monoclonal antibodies (mABs), whichhave been shown to be effective in the prevention of infections after vaginal application, have found their way into a vaginal multipurpose prevention filmMB66 [270]. The film developed by Politch et al. is a combination of two human mABs, VRC01, and HSV8, together providing protection against HIV-1 and HSV-1 and 2, and hasshown safety and efficacy in a Phase I clinical trial [270]. Another explored the application of vaginal films is for the treatment of female sexual arousal disorder (FSAD) as shown by Yoo et al.for mucosal delivery of nitric oxide (NO) [279]. Their s-nitroglutathione (GSNO) films displayed significantly enhanced duration of action of GSNO, which is an NO donor, and also showed enhanced vaginal blood perfusion in a rat model without any cytotoxicity. Patents have been filed on vaginal films for a variety of applications, such as drug delivery of analgesics, anesthetics, anti-inflammatory, antimicrobials, vitamins, hormones, proteins, etc. [297]; deodorizing [298]; contraception, infections, itch relief, cleansing, and lubrication [299]; Lactobacillus for prevention of infections or restoration of flora [300]; pH regulation, drug and hormone delivery [301] and more. A notable mention is the application of the mixed solvency concept by Gahlot&Maheshwari for the preparation of metronidazole vaginal films for bacterial vaginosis (BV) [274]. They were able to solubilize the poorly water-soluble drug using a combination of aqueous solubilizers, niacinamide: sodium benzoate: urea: caffeine (15:10:10:5), which according to mixed solvency concept exhibit a synergistic solvent action in combination while also minimizing the amount of each individual excipient in the formulation [274]. In recent advancement of vaginal film formulations, Notario-Pérez et al. developed “smart microbicide” films that are pH-sensitive and could change the release behavior of the drug to a rapid release in vaginal pH conditions after ejaculation (pH 7–8) from a sustained-release profile under typical vaginal conditions (pH 4–5) [302].
5. Conclusions and Future Directions
An impressive evolution of novel manufacturing techniques thatprovide entirely new possibilities to develop very sophisticated formulations and platforms fordrug delivery via the vaginal route, followed by local action or systemic effects, can be recently observed (Table 1).
Advantageous features of the vagina as a potential drug administration site have been recognized and used for many years [29], even though the full potential of the vaginal route seems to be underestimated, as it was noted in other comprehensive reviews related to this subject [262]. The most important research area in vaginal drug delivery focuses on local action, which is a natural consequence of numerous diseases and conditions, including bacterial, viral, and fungal infections or vaginal atrophy and dryness, potentially occurring in vagina. However, vaginal drug delivery systems are also applied to exert systemic actions. The most extensively investigated directions are hormone delivery in menopause management and contraception. Moreover, vaginal formulations are also investigated as potentially useful preventive agents in sexually transmitted diseases including HIV infections prevention. However, some of the vaginal physiological features are challenging in terms of drug delivery, especially the high variability of vaginal conditions, such as amount, composition and pH of vaginal fluids. On the other hand, these conditions also vary intraindividually, which may also contribute to different therapeutic responses in the same subject.
As far as the polymers applied in vaginal drug delivery are concerned, the most important research directions are related to the increase in the residence time in the vaginal cavity. For this purpose, mucoadhesive and smart polymers, increasing viscosity upon contact with the physiological environment, are frequently investigated. It is important to note that the polymer properties can be tailored with the use of chemical modifications to obtain the desired product characteristics [303]. However, it must be emphasized that in the case of any newly synthesized excipient, detailed studies regarding potential toxicity and irritancy toward vaginal mucosa are necessary. Most of the available literature reports focus on formulation studies and investigate the properties of the analyzed systems with the use of in vitro tests and ex vivo animal models, which is not sufficient for the proper safety evaluation. Therefore, in future product evaluations, more attention should be paid to the toxicity of the potential vaginal drug delivery systems. Moreover, there are also other safety concerns regarding vaginal products. In the case of hormone-loaded systems, the risk of active ingredient transfer to a sexual partner during coitus has been indicated [304]. Another important issue is unwanted systemic exposure to the active ingredient as a result of the drug absorption from topical intravaginal products to the systemic circulation. However, even though this phenomenon was indicated elsewhere as a potential therapeutic problem, according to the available literature reports, only a small amount of the active ingredient can be absorbed and exert the systemic effects and the risk of serious side effects is negligible [305].
It must also be emphasized that the research studies cited in this paper do not present uniform testing protocols for the drug release and permeation across the vaginal mucosa. Some of the investigated formulations are tested for drug release only, and in some cases, excised animal mucosa is applied in ex vivo permeation tests. However, the exact correlations between the ex vivo and in vivo animal studies and pharmacokinetic parameters in humans are scarce, and this research area requires more scientific attention in future studies. As it was already mentioned, animal models usually display some differences with respect to human anatomy and physiology, which indicates the need to develop novel biosimilar models for drug permeation testing.
A large number of concepts and ongoing projects, as reflected in the numerous scientific papers, is consequently pushing the technology of polymer-based vaginal formulations to the new level of coping with such inconveniences as poor bioadhesion, short residence time, thinning with vaginal fluids, insufficient dispersion in the vaginal cavity or rapid drug release. However, the proper safety testing protocols included at the initial stage of the project related to vaginal drug delivery would be useful in further pharmaceutical product development.

Table 1.
Polymer-based vaginal formulations.
Table 1.
Polymer-based vaginal formulations.
| API(s) | Formulation | Polymer(s) | References |
|---|---|---|---|
| --- | bioadhesive tablets | Carbopol®934, pectin, PVP, ethyl anhydrated maleic resins | Baloğlu et al. (2003) [230] |
| --- | dendrimers | SPL7013 BHA.lys15lys16(NHCOCH2O)1-(3,6-naphth(SO3Na)32 (BHA: benzhydrylamine) | Gong et al. (2005) [306] |
| --- | gel | Pluronics® F127 and F68, HPMC chitosan-thioglycolic acid conjugates; polycarbophil, Pluronic F 127 | Aka-Any-Grah et al. (2010) [213] Friedl et al. (2013) [307] Podaralla et al. (2014) [308] |
| --- | gel-microemulsions | carageenan, xanthan gum | D’Cruz et al. (2001) [309] |
| --- | microparticles | CMC | Kejdušová et al. (2015) [310] |
| --- | mucoadhesive sponges | HEC 250M | Furst et al. (2015) [77] |
| --- | nanoparticles | chitosan, poly(isobutylcyanoacrylate); | Pradines et al. (2015) [311] |
| --- | peptide-derivatized dendrimers | --- | Luganini (2011) [312] |
| --- | tablets | hyaluronic acid | Ekin et al. (2011) [229] |
| 4′-ethynyl-2-fluoro-2′-deoxyadenosine (EFdA) | film | PVA; HPMC E5 | Zhang et al. (2013) [275] |
| abacavir | bioadhesive film | Alg-Na, HPMC | Ghosal et al. (2014) [289] |
| film | Alg-Na; HPMC E5; HPMC-PVP blend | Ghosal et al. (2014) [289] | |
| acyclovir | in situ gel | poloxamer, carageenan, Carbopol 934p-NF | Liu et al. (2009) [214] |
| insitu forming hydrogel | hyaluronic acid, poloxamer F127 F68 | Mayol et al. (2008) [166] | |
| acyclovir, ciprofloxacin | gel | chitosan citrate | Bonferoni et al. (2008) [208] |
| amoxicilin | hydrogel | PEG-dendrimercrosslinks | Navath et al. (2011) [313] |
| fast-dissolving matrix | PVP | Rossi et al. (2017) [261] | |
| amphotericin B | insitu gel | poloxamer 407, HPCD | Kim et al. (2010) [314] |
| amphotericin, fluconazole | liquid crystal precursor mucoadhesive system | chitosan, poloxamer | Salmazi et al. (2015) [315] |
| arctigenin | liposome-based gel | pH-sensitive liposomes | Chen et al. (2012) [316] |
| baicalein | insitu gel | poloxamer, HPCD | Zhou et al. (2013) [215] |
| benzydamine HCl | tablets | HPMC, Carbopol 940 | Perioli et al. (2011) [228] |
| camptothecin | nanoparticles | PLGA | Blum et al. (2011) [317] |
| chlorhexidine | inserts | chitosan, CMC | Bigucci et al. (2015) [318] |
| chlorhexidine digluconate | freeze-dried polimer complexes | Alg-Na, chitosan | Abruzzo et al. (2013) [319] |
| cisplatin | nanofibersgels, films | PLA, PEO, HPMC, Carbopol | Zong et al. (2015) [320] |
| clindamycin phosphate | bioadhesive system | HPC, xanthan gum | Dobaria and Mashru (2010) [321] |
| clomiphenecitrate | gel | polycarbophil-cysteinę and chitosan-thioglycolic acid conjugates | Cevher et al. (2008) [211] |
| clotrimazole | gel | Pluronic®F127, polycarbophil, Carbopol. HPC, PVP poloxamers 407 and 188 | Bilensoy et al. (2006) [212] Chang et al. (2002) [322] |
| film | HPC, Alg-Na | Mishra et al. (2016) [323] | |
| nanocapsules | Eudragit RS100 | Santos et al. (2014) [251] | |
| tablets | chitosan, (silicified MCC, potato starch, | Szymańska et al. (2014) [220] | |
| tablets with microspheres | Eudragit RS-100 and RL-100 | Gupta et al. (2013) [219] | |
| clotrimazole, metronidazole | acid-buferring tablet | polycarbophil, HMPC | Alam et al. (2007) [222] |
| coumarin-6 | nanoparticles | PLGA | Cu et al. (2011) [324] |
| CSIC | film | PVA-HPMC K4M blend; PEG 4000 | Gong et al. (2017) [276] |
| dapivirine | film | PVA, HPMC 4000, PEG 8000 PEO, HPC | Akil et al. (2011) [278] Regev et al. (2019) [283] |
| nanoparticles | poly(ε-caprolactone) PLGA | Neves et al. (2014) [325] Neves and Sarmento (2015) [245] | |
| dapivirine and tenofovir | film | PVA | Akil et al. (2014) [266] |
| disulfiram | tablets | MCC, maize starch | Baffoe et al. (2014) [232] |
| doxorubicin | nanoparticles | carboxyl modified polystyrene | Ensign et al. (2013) [326] |
| econazole | film | gelatin, PVP, Soluplus®, and Gelucire® evaluated for solid dispersions | Dolci et al. (2020) [292] |
| microparticle-loaded gel | chitosan lactate, poloxamer 407, Eudragit RS | Parodi et al. (2013) [327] | |
| econazole and miconazole nitrate | gel | chitosan | Şenyigit et al. (2014) [209] |
| econazole nitrate, miconazole nitrate | tablets | thiolated poly(acrylic acid)-cysteine (PAA-Cys) conjugate | Baloglu et al. (2011) [221] |
| econazole nitrate | microparticles | chitosan, Na-CMC, poloxamers | Albertini et al. (2009) [240] |
| Efda and 5-chloro-3-phenylsulfonylindole-2-carboxamide (CSIC) | film | PVA, HPMC E5, PEG 4000 | Zhang et al. (2015) [277] |
| fluconazole | film | HPMC chitosan:pectin (75:25) | Kumar et al. (2013) [273] Mishra et al. (2017) [291] |
| fluorescent labeled NPs | film | PVA, carrageenan, PEG | Traore et al. (2018) [267] |
| FSAD S-nitrosoglutathione (GSNO) | film | Carbopol 934P, HPMC, PEG | Yoo et al. (2009) [279] |
| griffithsin/carrageenan | fast-dissolving insert | carrageenan, HEC, xanthan gum | Lal et al. (2018) [113] |
| griffithsin/carrageenan | fast-dissolving insert | carrageenan | Derby et al. (2018) [328] |
| hexylaminolevulinate hydrochloridum | pellets | MCC, Carbopol | Hiorth et al. (2012) [243] |
| bioadhesive mini-tablets | MC, HEC, HPC, MCC | Hiorth et al. (2014) [231] | |
| HIV; IQP-0528 | film | PLGA:Eudragit S 100 nanoparticle encapsulated drug in polymeric films | Srinivasan et al. (2016) [329] |
| HIV and VC; Ebselen | rapidly soluble film | β-cyclodextrin, PVA, Soluplus® | Vartak et al. (2020) [269] |
| HIV-1 reverse transcriptase inhibitors UC781, tenofovir | gel | HEC, Carbopol®974P | Mahalingam et al. (2010) [330] |
| IQP-0528 (non-nucleoside reverse transcriptase inhibitor) | osmotic pump tablets | HPC, CAP, Carbopol 974P | Rastogi et al. (2013) [227] |
| itraconazole | bioadhesive tablets | cyclodextrins | Cevher et al. (2014) [218] |
| film | HPC, PEG 400 | Dobaria et al. (2009) [331] | |
| insitu gel | HPMC E50, poloxamers 188 and 407 | Karavana et al. (2012) [332] | |
| itraconazole, tea tree oil | thermosensitive gel | Lutrol®F127 | Mirza et al. (2013) [333] |
| lactic acid | gel | chitosan poloxamer 408, chitosan | Bonferoni et al. (2006) [207] Rossi et al. (2014) [201] |
| tablets | MC, chitosan | Małolepsza-Jarmołowska (2007) [334] | |
| M48U1 anti-HIV microbicide | gel | Pluronic®F127, F68, HPMC | Bouchemal et al. (2013) [335] |
| maraviroc and emtricitabine | non-aqueous gels | silicone elastomer | Forbes et al. (2014) [336] |
| metronidazole | film | HPMC E5 S-protected gellan gum | Gahlot and Maheshwari (2018) [274] Jalil et al. (2019) [337] |
| gel | chitosan, HEC, 5-methylpyrrolidinone-chitosan (MPCS); PF-127 | Perioli et al. (2008) [338] Ibrahim et al. (2012) [339] | |
| tablets | chitosan, Alg-Na, MCC, CMC; chitosan (FG90C), polyvinylpyrrolidone (PVPK90) and polycarbophil (PCPAA1) | El-Kamel et al. (2002) [340] Perioli et al. (2009) [341] | |
| tablets with preliposomes | MCC, starch, pectin, chitosan | Vanić et al. (2014) [342] | |
| microbicidal-STD pathogens (HIV, HSC); bacteria associated with BV Cellulose acetate phthalate (CAP) | film | HPC | Neurath et al. (2003) [272] |
| microbicidal for HIV and HSV; mAB VRC01-N; mAB HSV8-N | film | PVA, maltitol, polysorbate 20 | Politch et al. (2021) [270] |
| icrobicides PHI-113, PHI-346, PHI-443 | self-emulsyfying gel | PEG 400, MCC, xanthan gum | D’Cruz et al. (2005) [343] |
| MIV-150/zinc acetate/carrageenan | gel | carrageenan | Friedland et al. (2016) [344] |
| MIV-150/zinc acetate/carrageenan | gel | carrageenan | Kenney et al. (2012) [345] |
| maraviroc | electrospun fibers | PVP, PEO | Ball andWoodrow (2014) [346] |
| Na fluorescein, nile red | nanoparticles | Eudragit S-100, PVP | Yoo et al. (2011) [167] |
| natamycin | tablets | HPMC, xanthan gum, Carbopol 934 P, cyclodextrins | Cevher et al. (2008) [347] |
| nile red | polymeric nanocapsules in hydrogel | chitosan, Eudragit | Frank et al. (2014) [172] |
| nystatin | gel | poly(acrylic acid)-cysteine conjugate and the new poly(acrylic acid)-cysteamineconjugate | Hombach et al. (2009) [348] |
| microparticles | Alg-Na, poloxamer 407, chitosan | Martín-Villena et al. (2013) [349] | |
| ovoalbumin | microparticles | PLGA | Kuo-Haller et al. (2010) [350] |
| gel | chitosan, HPMC K100M, Pluronic F 127 | Tuğcu-Demiroz et al. (2013) [210] | |
| polyherbal microbicides | cream | Alg-Na, xanthan gum | Talwar et al. (2008|) [351] |
| polystyrene sulfonate (PSS) | film | HPMC, HEC, PVA | Garg et al. (2005) [194] |
| probiotic microorganisms | microparticles | pectinate, hyaluronic acid | Pliszczak et al. (2011) [237] |
| progesterone | hydrogel | glycolchitin | Almomen et al. (2015) [352] |
| mucoadhesive emulsion | cyclomethicone pentamer | Campaña-Seoane (2014) [353] | |
| propranolol HCl | gel | guar gum, Alg-Na, xanthan gum, HPMC 4000, Na-CMC, carbomer 934, 940 | Tasdighi et al. (2012) [354] |
| proteins, insulin | flux controlled pump, pellets | HEC, HPC, CG, | Teller et al. (2014) [355] |
| pyrimidinedione IQP-0528 | film | PVA | Ham et al. (2012) [271] |
| raltegravir + efavirenz | nanoparticles loaded gel | Pluronic®F127 and F68 | Date et al. (2012) [356] |
| saquinavir | nanoparticles loaded gel | HEC, PLGA, PVA | Yang et al. (2013) [357] |
| sertaconazole | microemulsion-based gel | Carbopol 940 | PatelandPatel (2012) [358] |
| sertaconazole | tablets | Cbp 934P, CH, CMC-Na, Alg-Na, MC, HPMC, HPC | Patel et al. (2011) [359] |
| siRNA-loaded nanoparticles with anti-HLA-DR antibody (siRNA-NP-Ab) | film | PLGA-PEG/PEI/siRNA-NP PVA-λ-carageenan film | Gu et al. (2015) [246] |
| SPL7013 sulphonated dendrimer | gel | Carbopol® | Mumper et al. (2009) [360] |
| STDs sodium dodecyl sulfate (SDS) | film | Carbopol 934P, HPMC, PEG | Yoo et al. (2006) [263] |
| Streptococcus vaccine | microparticles | Resomer, RG 503 PLG | Hunter et al. (2001) [361] |
| tebuconazole | nanoparticles | tetraethylorthosilicate | Mas et al. (2014) [362] |
| tenofovir | film | drug-loaded PLGA/SA composite NPs incorporated into a PVA-HPMC film; EC: xanthan gum (2:1) | Machado et al. (2016) [253] Cazorla-Luna et al. (2020) [363] |
| microparticles | Eudragit S-100 sodium salt | Zhang et al. (2013) [239] | |
| nanoparticles | chitosan; hyaluronic acid | Meng et al. (2011); Meng et al. (2014) [364,365] Agrahari et al. (2014) [366] | |
| tablets | HPMC, Kollidon SR | McConville et al. (2013) [224] | |
| SLN | PAA | Alukda et al. (2011) [367] | |
| films | HPMC-Zein (1:5) blend, PEG Eudragit RL, RS, L and S | Notario-Perez et al. (2019) [280] Notario-Perez et al. (2021) [301] | |
| tenofovir + efavirenz | film | drug-loaded PLGA NPs in HPMC-PVA films | Cunha-Reis et al. (2016) [249] |
| tenofovir disoproxil fumarate and emricitabine | film | Eudragit®L100 NPs in PVA films | Cautela et a. (2019) [268] |
| tenofovir, emtricitabine | tablets | microcrystalline cellulose, crospovidone, hydroxyethyl cellulose | Clark et al. (2014) [368] |
| tenofovir, maraviroc | dendrimers | carbosilane | Sepúlveda-Crespo et al. (2014) [369] |
| tenofovir, maraviroc, dapivirine | film | sodium CMC, HPMC, HEC; PVA, PVP-K90, PVP-K30 | Akil et al. (2015) [370] |
| tenofovir, tenofovirdisoproxil fumarate | nanoparticles | PLGA, Eudragit | Zhang et al. (2011) [371] |
| tioconazole | film | chitosan-HPMC, PEG 400 | Calvo et al. (2019) [372] |
| UAMC01398 | solid dispersion film | HPMC, PEG 400 | Grammen et al. (2014) [373] |
Author Contributions
Conceptualization: T.O., A.F. (Anna Froelich); literature research: all authors; writing: Introduction, The Anatomy and Physiology of the Vagina—T.O., Polymers Used in Vaginal Druf Delivery Systems—T.O., A.T., Semisolid Formulations—A.F. (Anna Froelich), Suppositories, Tablets, and Pessaries—A.T., M.E., K.G., Vaginal Rings—J.W.-B., Microspheres, Pellets—B.J., J.W.-B., Nanoparticles—P.G., A.F., Vaginal Films—V.P., Conclusions and Fututre Perspectives—A.F., T.O., master table—A.T., T.O. original draft preparation, A.F., T.O.; writing-review and editing, T.O., A.F., B.M.-K.; supervision, T.O., B.M.-K. All authors have read and agreed to the published version of the manuscript.
Funding
Part of the research was funded by the European Union’s Horizon 2020 research and innovation program under the Marie Skłodowska-Curie grant agreement no. 778051 and the Ministry of Science and Higher Education of Poland fund for supporting internationally co-financed projects in 2018–2022 (agreement no. 3899/H2020/2018/2).
Conflicts of Interest
The authors declare no conflict of interest.
Abbreviations
| AMB | Amphotericin B; |
| BV | Bacterial vaginosis; |
| CD | Cyclodextrins; |
| CLSM | Confocal scanning laser microscopy |
| CMC | Carboxymethyl cellulose; |
| CP | Conventional particles; |
| EC | Ethyl cellulose; |
| EC | Ethylcellulose; |
| EVA | Ethylenacetate of vinyl; |
| FSAD | Female sexual arousal disorder; |
| HA | Hyaluronic acid; |
| HEC | Hydroxyethyl cellulose; |
| HIV | Human immunodeficiency virus; |
| HLB | Hydrophilic-lipophilic balance; |
| HME | Hot-melt extrusion; |
| HPC | Hydroxypropyl cellulose; |
| HPMC | Hydroxypropyl methylcellulose; |
| HSV | Herpes simplex virus; |
| LIPs | Liposomes; |
| mAB | Monoclonal antibody; |
| MC | Methylcellulose; |
| MCC | Microcrystalline cellulose; |
| MPP | Mucus penetrating particles; |
| Na-CMC | Sodium carboxymethyl cellulose; |
| NC | Nanocapsules; |
| NP | Nanoparticles; |
| NPs | Polymeric nanoparticles; |
| NS | Nanospheres; |
| OPTs | Osmotic pump tablets; |
| PCL | Polycaprolactone; |
| PEG | Poly(ethylene glycol); |
| PEI | Polyethylenimine; |
| PEO | Poly(ethylene oxide); |
| PEO | Polyethylene oxide; |
| PLGA | Poly(lactic-co-glycolic acid); |
| PLGA | Poly(lactic-co-glycolic) acid; |
| PPO | Poly(propylene oxide); |
| PrEP | Pre-exposure prophylaxis of sexual transmission; |
| PVA | Polyvinyl alcohol; |
| PVP | Polyvinylpyrrolidone; |
| QbD | Quality-by-design; |
| RVVC | Recurrent vulvovaginal candidiasis; |
| SC | Solvent casted; |
| siRNA | Small interfering RNA; |
| STD | Sexually transmitted disease; |
| STIs | Sexuallytransmitted infections; |
| VC | Vaginal candidiasis; |
| VFS | Vaginal fluid stimulant |
References
- Stevens, J.M. Gynaecology from Ancient Egypt: The papyrus Kahun: A translation of the oldest treatise on gynaecology that has survived from the ancient world. Med. J. Aust. 1975, 2, 949–952. [Google Scholar] [CrossRef]
- Contraception—An Ancient Interest—Contraceptive, Women, Methods, and Practice. Available online: https://science.jrank.org/pages/1761/Contraception-An-ancient-interest.html (accessed on 12 February 2020).
- Smith, L. The Kahun Gynaecological Papyrus: Ancient Egyptian medicine. J. Fam. Plan. Reprod. Health Care 2011, 37, 54–55. [Google Scholar] [CrossRef] [PubMed]
- Hasan, I.; Zulkifle, M.; Ansari, A.H.; Sherwani, A.M.K.; Shakir, M. History of Ancient Egyptian Obstetrics & Gynecology: A Review. J. Microb. Biotechnol.Res. 2011, 1, 35–39. [Google Scholar]
- Britton, L.E.; Alspaugh, A.; Greene, M.Z.; McLemore, M.R. CE: An evidence-based update on contraception. Am. J. Nurs. 2020, 120, 22–33. [Google Scholar] [CrossRef] [PubMed]
- New Non-Hormonal Contraceptive Gel Found to Be Effective. Available online: https://www.pharmacytimes.com/view/new-non-hormonal-contraceptive-found-to-be-effective (accessed on 24 May 2021).
- Whorton, J.C. The Arsenic Century: How Victorian Britain was Poisoned at Home, Work, and Play; Oxford University Press: Oxford, UK, 2011; p. 412. [Google Scholar]
- Donders, G. Diagnosis and management of bacterial vaginosis and other types of abnormal vaginal bacterial flora: A review. Obstet. Gynecol. Surv. 2010, 65, 462–473. Available online: http://www.ncbi.nlm.nih.gov/pubmed/20723268 (accessed on 12 February 2020). [CrossRef]
- Macklaim, J.M.; Clemente, J.C.; Knight, R.; Gloor, G.B.; Reid, G. Changes in vaginal microbiota following antimicrobial and probiotic therapy. Microb. Ecol. Health Dis. 2015, 26, 27799. Available online: http://www.microbecolhealthdis.net/index.php/mehd/article/view/27799 (accessed on 12 February 2020). [CrossRef] [PubMed]
- Tanphaichitr, N.; Srakaew, N.; Alonzi, R.; Kiattiburut, W.; Kongmanas, K.; Zhi, R.; Li, W.; Baker, M.; Wang, G.; Hickling, D. Potential use of antimicrobial peptides as vaginal spermicides/microbicides. Pharmaceuticals 2016, 9, 13. Available online: http://www.ncbi.nlm.nih.gov/pubmed/26978373 (accessed on 12 February 2020). [CrossRef] [PubMed]
- Johal, H.S.; Garg, T.; Rath, G.; Goyal, A.K. Advanced topical drug delivery system for the management of vaginal candidiasis. Drug Deliv. 2016, 23, 550–563. [Google Scholar] [CrossRef]
- Palmeira-de-Oliveira, R.; Palmeira-de-Oliveira, A.; Martinez-de-Oliveira, J. New strategies for local treatment of vaginal infections. Adv. Drug Deliv. Rev. 2015, 92, 105–122. [Google Scholar] [CrossRef]
- Baptista, M.; Tavares, R.; Ramalho-Santos, J. Spermicidal and microbicidal compounds: In search of an efficient multipurpose strategy. Curr. Med. Chem. 2014, 21, 3693–3700. Available online: http://www.ncbi.nlm.nih.gov/pubmed/25174922 (accessed on 12 February 2020). [CrossRef]
- Subramanian, B.; Agarwal, T.; Ghorai, S.K.; Mandal, P.; Chattopadhyay, S.; Basak, P.; Maiti, T.K.; Guha, S.K. Biocompatible polyvinyl alcohol and RISUG® blend polymeric films with spermicidal potential. Biomed. Mater. 2019, 14, 035017. [Google Scholar] [CrossRef]
- Daniel, S.; Rotem, R.; Koren, G.; Lunenfeld, E.; Levy, A. Vaginal antimycotics and the risk for spontaneous abortions. Am. J. Obstet. Gynecol. 2018, 218, 601.e1–601.e7. Available online: http://www.ncbi.nlm.nih.gov/pubmed/29510088 (accessed on 13 February 2020). [CrossRef] [PubMed]
- El-Hammadi, M.; Arias, J. Nano-sized platforms for vaginal drug delivery. Curr. Pharm. Des. 2015, 21, 1633–1644. [Google Scholar] [CrossRef]
- Gupta, S.; Gabrani, R.; Ali, J.; Dang, S. Exploring novel approaches to vaginal drug delivery. Recent Pat. Drug Deliv. Formul. 2011, 5, 82–94. [Google Scholar] [CrossRef]
- Bassi, P.; Kaur, G. Innovations in bioadhesive vaginal drug delivery system. Expert Opin. Ther. Pat. 2012, 22, 1019–1032. Available online: http://www.ncbi.nlm.nih.gov/pubmed/22860765 (accessed on 13 February 2020). [CrossRef]
- Naumova, I.; Castelo-Branco, C. Current treatment options for postmenopausal vaginal atrophy. Int.J. Womens Health 2018, 10, 387–395. Available online: http://www.ncbi.nlm.nih.gov/pubmed/30104904 (accessed on 13 February 2020). [CrossRef]
- Veres, S.; Miller, L.; Burington, B. A comparison between the vaginal ring and oral contraceptives. Obstet. Gynecol. 2004, 104, 555–563. Available online: http://www.ncbi.nlm.nih.gov/pubmed/15339769 (accessed on 13 February 2020). [CrossRef] [PubMed]
- Gao, Y.; Yuan, A.; Chuchuen, O.; Ham, A.; Yang, K.H.; Katz, D.F. Vaginal deployment and tenofovir delivery by microbicide gels. Drug Deliv. Transl. Res. 2015, 5, 279–294. Available online: http://www.ncbi.nlm.nih.gov/pubmed/25874971 (accessed on 13 February 2020). [CrossRef]
- Ferguson, L.M.; Rohan, L.C. The importance of the vaginal delivery route for antiretrovirals in HIV prevention. Ther. Deliv. 2011, 2, 1535–1550. Available online: http://www.ncbi.nlm.nih.gov/pubmed/22468220 (accessed on 13 February 2020). [CrossRef]
- Madanchi, H.; Shoushtari, M.; Kashani, H.; Sardari, S. Antimicrobial peptides of the vaginal innate immunity and their role in the fight against sexually transmitted diseases. N. Microbes N. Infect. 2020, 34, 100627. [Google Scholar] [CrossRef] [PubMed]
- Novetsky, A.P.; Keller, M.J.; Gradissimo, A.; Chen, Z.; Morgan, S.L.; Xue, X.; Strickler, H.D.; Fernández-Romero, J.A.; Burk, R.; Einstein, M.H. In vitro inhibition of human papillomavirus following use of a carrageenan-containing vaginal gel. Gynecol. Oncol. 2016, 143, 313–318. [Google Scholar] [CrossRef] [PubMed]
- Rodríguez, A.; Kleinbeck, K.; Mizenina, O.; Kizima, L.; Levendosky, K.; Jean-Pierre, N.; Villegas, G.; Ford, B.E.; Cooney, M.L.; Teleshova, N.; et al. In vitro and in vivo evaluation of two carrageenan-based formulations to prevent HPV acquisition. Antivir. Res. 2014, 108, 88–93. [Google Scholar] [CrossRef] [PubMed]
- Baptista, M.; Ramalho-Santos, J. Spermicides, microbicides and antiviral agents: Recent advances in the development of novel multi-functional compounds. Mini Rev. Med. Chem. 2009, 9, 1556–1567. Available online: http://www.eurekaselect.com/openurl/content.php?genre=article&issn=1389-5575&volume=9&issue=13&spage=1556 (accessed on 13 February 2020). [CrossRef] [PubMed]
- First Multipurpose Gel Designed to Prevent HIV, HSV, and HPV Simultaneously in Women and Men Advances in Clinical Trials. Population Council. Available online: https://www.popcouncil.org/news/first-multipurpose-gel-designed-to-prevent-hiv-hsv-and-hpv-simultaneously-i (accessed on 24 May 2021).
- Price, C.F.; Tyssen, D.; Sonza, S.; Davie, A.; Evans, S.; Lewis, G.R.; Xia, S.; Spelman, T.; Hodsman, P.; Moench, T.R.; et al. SPL7013 gel (vivagel®) retains potent HIV-1 and HSV-2 inhibitory activity following vaginal administration in humans. PLoS ONE 2011, 6, 24095. [Google Scholar] [CrossRef] [PubMed]
- Hussain, A.; Ahsan, F. The vagina as a route for systemic drug delivery. J. Control Release 2005, 103, 301–313. [Google Scholar] [CrossRef]
- Barton, D.L.; Shuster, L.T.; Dockter, T.; Atherton, P.J.; Thielen, J.; Birrell, S.N.; Sood, R.; Griffin, P.; Terstriep, S.A.; Mattar, B.; et al. Systemic and local effects of vaginal dehydroepiandrosterone (DHEA): NCCTG N10C1 (Alliance). Support. Care Cancer 2017, 26, 1335–1343. Available online: http://www.ncbi.nlm.nih.gov/pubmed/29164377 (accessed on 13 February 2020). [CrossRef] [PubMed]
- Caramella, C.M.; Rossi, S.; Ferrari, F.; Bonferoni, M.C.; Sandri, G. Mucoadhesive and thermogelling systems for vaginal drug delivery. Adv. Drug Deliv. Rev. 2015, 92, 39–52. [Google Scholar] [CrossRef] [PubMed]
- Vermani, K.; Garg, S. The scope and potential of vaginal drug delivery. Pharm. Sci. Technol. Today 2000, 3, 359–364. [Google Scholar] [CrossRef]
- Machado, R.M.; Palmeira-De-Oliveira, A.; Gaspar, C.; de Oliveira, J.M.; Palmeira-De-Oliveira, R. Studies and methodologies on vaginal drug permeation. Adv. Drug Deliv. Rev. 2015, 92, 14–26. [Google Scholar] [CrossRef]
- Machado, A.; das Neves, J. Tissue-based in vitro and ex vivo models for vaginal permeability studies. In Concepts and Models for Drug Permeability Studies: Cell and Tissue based In Vitro Culture Models; Elsevier: Amsterdam, The Netherlands, 2016; pp. 273–308. [Google Scholar]
- Morrow, R.J.; Woolfson, A.D.; Donnelly, L.; Curran, R.; Andrews, G.; Katinger, D.; Malcolm, R.K. Sustained release of proteins from a modified vaginal ring device. Eur. J. Pharm. Biopharm. 2011, 77, 3–10. Available online: http://www.ncbi.nlm.nih.gov/pubmed/21055465 (accessed on 13 February 2020). [CrossRef]
- Srikrishna, S.; Cardozo, L. The vagina as a route for drug delivery: A review. Int. Urogynecology J. 2012, 24, 537–543. Available online: https://link.springer.com/article/10.1007/s00192-012-2009-3 (accessed on 20 May 2020). [CrossRef]
- Sherrard, J.; Wilson, J.; Donders, G.; Mendling, W.; Jensen, J.S. 2018 European (IUSTI/WHO) International Union against sexually transmitted infections (IUSTI) World Health Organisation (WHO) guideline on the management of vaginal discharge. Int. J. STD AIDS 2018, 29, 1258–1272. Available online: https://pubmed.ncbi.nlm.nih.gov/30049258/ (accessed on 20 May 2020). [CrossRef] [PubMed]
- CDC—Bacterial Vaginosis Statistics. Available online: https://www.cdc.gov/std/bv/stats.htm (accessed on 20 May 2021).
- Vaginal and Vulvar Cancers Statistics. Available online: https://www.cdc.gov/cancer/vagvulv/statistics/index.htm (accessed on 20 May 2021).
- Koumans, E.H.; Sternberg, M.; Bruce, C.; McQuillan, G.; Kendrick, J.; Sutton, M.; Markowitz, L.E. The prevalence of bacterial vaginosis in the United States, 2001-2004; associations with symptoms, sexual behaviors, and reproductive health. Sex. Transm. Dis. 2007, 34, 864–869. Available online: https://pubmed.ncbi.nlm.nih.gov/17621244/ (accessed on 13 February 2020). [CrossRef] [PubMed]
- Katz, D.F.; Yuan, A.; Gao, Y. Vaginal drug distribution modeling. Adv. Drug Deliv. Rev. 2015, 92, 2–13. Available online: http://www.ncbi.nlm.nih.gov/pubmed/25933938 (accessed on 13 February 2020). [CrossRef] [PubMed]
- Melis, G.B.; Ibba, M.T.; Steri, B.; Kotsonis, P.; Matta, V.; Paoletti, A.M. Role of pH as a regulator of vaginal physiological environment. Minerva Ginecol. 2000, 52, 111–121. Available online: http://www.ncbi.nlm.nih.gov/pubmed/10900941 (accessed on 13 February 2020). [PubMed]
- Mercer, B.M.; Miodovnik, M.; Thurnau, G.R.; Goldenberg, R.L.; Das, A.F.; Ramsey, R.D.; A Rabello, Y.; Meis, P.J.; Moawad, A.H.; Iams, J.D.; et al. The preterm prediction study: Significance of vaginal infections. National Institute of Child Health and Human Development Maternal-Fetal Medicine Units Network. Am.J. Obs. Gynecol. 1995, 173, 1231–1235. Available online: http://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&dopt=Citation&list_uids=7485327 (accessed on 13 February 2020).
- Stojanović, N.; Plećaš, D.; Plešinac, S. Normal vaginal flora, disorders and application of probiotics in pregnancy. Arch. Gynecol. Obstet. 2012, 286, 325–332. [Google Scholar] [CrossRef] [PubMed]
- Barnhart, K.T.; Izquierdo, A.; Pretorius, E.S.; Shera, D.M.; Shabbout, M.; Shaunik, A. Baseline dimensions of the human vagina. Hum. Reprod. 2006, 21, 1618–1622. Available online: http://www.ncbi.nlm.nih.gov/pubmed/16478763 (accessed on 13 February 2020). [CrossRef]
- Graziottin, A.; Gambini, D. Anatomy and physiology of genital organs—women. In Handbook of Clinical Neurology; Elsevier: Amsterdam, The Netherlands, 2015; pp. 39–60. [Google Scholar]
- Hickey, M.; Pillai, G.; Higham, J.; Sullivan, M.; Horncastle, D.; Doherty, D.; Stamp, G. Changes in endometrial blood vessels in the endometrium of women with hormone replacement therapy-related irregular bleeding. Hum. Reprod. 2003, 18, 1100–1106. Available online: http://www.ncbi.nlm.nih.gov/pubmed/12721191 (accessed on 13 February 2020). [CrossRef][Green Version]
- Cunha, G.R. The dual origin of vaginal epithelium. Am. J. Anat. 1975, 143, 387–392. [Google Scholar] [CrossRef]
- Nilsson, K.; Risberg, B.; Heimer, G. The vaginal epithelium in the postmenopause—cytology, histology and pH as methods of assessment. Maturitas 1995, 21, 51–56. Available online: http://www.ncbi.nlm.nih.gov/pubmed/7731384 (accessed on 13 February 2020). [CrossRef]
- Boutin, E.L.; Cunha, G.R. Estrogen-induced epithelial proliferation and cornification are uncoupled in sinus vaginal epithelium associated with uterine stroma. Differentiation 1998, 62, 171–178. [Google Scholar] [CrossRef] [PubMed]
- Farage, M.; Maibach, H. Lifetime changes in the vulva and vagina. Arch. Gynecol. Obstet. 2006, 273, 195–202. [Google Scholar] [CrossRef] [PubMed]
- Mårdh, P.A. The vaginal ecosystem. Am. J. Obstet. Gynecol. 1991, 165, 1163–1168. [Google Scholar] [CrossRef]
- Valore, E.V.; Park, C.H.; Igreti, S.L.; Ganz, T. Antimicrobial components of vaginal fluid. Am. J. Obstet. Gynecol. 2002, 187, 561–568. Available online: http://www.ncbi.nlm.nih.gov/pubmed/12237628 (accessed on 13 February 2020). [CrossRef] [PubMed]
- Owen, D.H.; Katz, D.F. A vaginal fluid simulant. Contraception 1999, 59, 91–95. [Google Scholar] [CrossRef]
- Chen, K.C.; Forsyth, P.S.; Buchanan, T.M.; Holmes, K.K. Amine content of vaginal fluid from untreated and treated patients with nonspecific vaginitis. J. Clin. Investig. 1979, 63, 828–835. Available online: http://www.ncbi.nlm.nih.gov/pubmed/447831 (accessed on 13 February 2020). [CrossRef] [PubMed]
- Rajan, N.; Cao, Q.; Anderson, B.E.; Pruden, D.L.; Sensibar, J.; Duncan, J.L.; Schaeffer, A.J. Roles of glycoproteins and oligosaccharides found in human vaginal fluid in bacterial adherence. Infect. Immun. 1999, 67, 5027–5032. Available online: http://www.ncbi.nlm.nih.gov/pubmed/10496874 (accessed on 20 February 2020). [CrossRef]
- Sobel, J.D.; Faro, S.; Force, R.W.; Foxman, B.; Ledger, W.; Nyirjesy, P.R.; Reed, B.D.; Summers, P.R. Vulvovaginal candidiasis: Epidemiologic, diagnostic, and therapeutic considerations. Am. J. Obstet. Gynecol. 1998, 178, 203–211. [Google Scholar] [CrossRef]
- Heine, P.; McGregor, J.A. Trichomonas vaginalis: A reemerging pathogen. Clin. Obstet. Gynecol. 1993, 36, 137–144. Available online: http://www.ncbi.nlm.nih.gov/pubmed/8435938 (accessed on 20 February 2020). [CrossRef]
- Pascual, L.M.; Daniele, M.B.; Pájaro, C.; Barberis, L. Lactobacillus species isolated from the vagina: Identification, hydrogen peroxide production and nonoxynol-9 resistance. Contraception 2006, 73, 78–81. [Google Scholar] [CrossRef]
- Linhares, I.M.; Summers, P.R.; Larsen, B.; Giraldo, P.C.; Witkin, S.S. Contemporary perspectives on vaginal pH and lactobacilli. Am. J. Obstet. Gynecol. 2011, 204, 120.e1–120.e5. Available online: http://www.ncbi.nlm.nih.gov/pubmed/20832044 (accessed on 13 February 2020). [CrossRef] [PubMed]
- Caillouette, J.C.; Sharp, J.; Zimmerman, G.J.; Roy, S. Vaginal pH as a marker for bacterial pathogens and menopausal status. Am. J. Obstet. Gynecol. 1997, 176, 1270–1277. [Google Scholar] [CrossRef]
- Andrews, G.P.; Laverty, T.P.; Jones, D.S. Mucoadhesive polymeric platforms for controlled drug delivery. Eur. J. Pharm. Biopharm. 2009, 71, 505–518. Available online: http://www.ncbi.nlm.nih.gov/pubmed/18984051 (accessed on 13 February 2020). [CrossRef] [PubMed]
- Kale, V. Vaginal mucosa—A promising site for drug therapy. Br. J. Pharm. Res. 2013, 3, 983–1000. [Google Scholar] [CrossRef]
- Sigurdsson, H.H.; Kirch, J.; Lehr, C.-M. Mucus as a barrier to lipophilic drugs. Int. J. Pharm. 2013, 453, 56–64. Available online: https://linkinghub.elsevier.com/retrieve/pii/S0378517313004572 (accessed on 13 February 2020). [CrossRef] [PubMed]
- Smart, J.D.; Kellaway, I.W.; Worthington, H.E.C. An in-vitro investigation of mucosa-adhesive materials for use in controlled drug delivery. Pharm. Pharmacol. 2011, 36, 295–299. [Google Scholar] [CrossRef] [PubMed]
- Roy, S.; Pal, K.; Anis, A.; Pramanik, K.; Prabhakar, B. Polymers in mucoadhesive drug-delivery systems: A brief note. Monomers Polym. 2009, 12, 483–495. [Google Scholar] [CrossRef]
- Sriamornsak, P.; Wattanakorn, N.; Takeuchi, H. Study on the mucoadhesion mechanism of pectin by atomic force microscopy and mucin-particle method. Carbohydr. Polym. 2010, 79, 54–59. [Google Scholar] [CrossRef]
- Hartman, C.G. The permeability of the vaginal mucosa. Ann. N. Y. Acad. Sci. 1959, 83, 318–327. Available online: http://www.ncbi.nlm.nih.gov/pubmed/14400131 (accessed on 13 February 2020). [CrossRef]
- Das Neves, J.; Bahia, M.F. Gels as vaginal drug delivery systems. Int. J. Pharm. 2006, 318, 1–14. [Google Scholar] [CrossRef] [PubMed]
- Van der Bijl, P.; van Eyk, A.D. Comparative in vitro permeability of human vaginal, small intestinal and colonic mucosa. Int. J. Pharm. 2003, 261, 147–152. Available online: http://www.ncbi.nlm.nih.gov/pubmed/12878403 (accessed on 13 February 2020). [CrossRef]
- Der Bijl, P.; van Eyk, A.D.; Thompson, I.O.C.; Stander, I.A. Diffusion rates of vasopressin through human vaginal and buccal mucosa. Eur. J. Oral. Sci. 1998, 106, 958–962. Available online: http://www.ncbi.nlm.nih.gov/pubmed/9786326 (accessed on 13 February 2020). [CrossRef] [PubMed]
- Van Eyk, A.D.; Van der Bijl, P. Comparative permeability of various chemical markers through human vaginal and buccal mucosa as well as porcine buccal and mouth floor mucosa. Arch. Oral Biol. 2004, 49, 387–392. Available online: http://www.ncbi.nlm.nih.gov/pubmed/15041486 (accessed on 13 February 2020). [CrossRef]
- Shokri, J.; Adibki, K. Application of cellulose and cellulose derivatives in pharmaceutical industries. In Cellulose—Medical, Pharmaceutical and Electronic Applications; InTech: London, UK, 2013. [Google Scholar]
- Sahin, H.T.; Arslan, M.B. A study on physical and chemical properties of cellulose paper immersed in various solvent mixtures. Int. J. Mol. Sci. 2008, 9, 78–88. [Google Scholar] [CrossRef] [PubMed]
- Burchard, W. Solubility and solution structure of cellulose derivatives. Cellulose 2003, 10, 213–225. [Google Scholar] [CrossRef]
- Kristl, J.; Peppas, N.A.; Baumgartner, S. Network structure of cellulose ethers used in pharmaceutical applications during swelling and at equilibrium. Pharm Res. 2002, 19, 1084–1090. Available online: http://www.ncbi.nlm.nih.gov/pubmed/12240932 (accessed on 13 February 2020).
- Furst, T.; Piette, M.; Lechanteur, A.; Evrard, B.; Piel, G. Mucoadhesive cellulosic derivative sponges as drug delivery system for vaginal application. Eur. J. Pharm. Biopharm. 2015, 95, 128–135. Available online: http://www.ncbi.nlm.nih.gov/pubmed/25660908 (accessed on 13 February 2020). [CrossRef]
- Shaghaleh, H.; Xu, X.; Wang, S. Current progress in production of biopolymeric materials based on cellulose, cellulose nanofibers, and cellulose derivatives. RSC Adv. 2018, 8, 825–842. [Google Scholar] [CrossRef]
- Yadav, V.K.; Gupta, A.B.; Kumar, R.; Yadav, J.S.; Kumar, B. Mucoadhesive polymers: Means of improving the mucoadhesive properties of drug delivery system. J. Chem. Pharm. Res. 2010, 2, 418–432. [Google Scholar]
- Kamel, S.; Ali, N.; Jahangir, K.; Shah, S.M.; El-Gendy, A.A. Pharmaceutical significance of cellulose: A review. Express Polym. Lett. 2008, 2, 758–778. [Google Scholar] [CrossRef]
- Jain, S.; Sandhu, P.S.; Malvi, R.; Gupta, B. Cellulose derivatives as thermoresponsive polymer: An overview. J. Appl. Pharm. Sci. 2013, 3, 139–144. [Google Scholar]
- Mohnen, D. Pectin structure and biosynthesis. Curr. Opin. Plant Biol. 2008, 11, 266–277. [Google Scholar] [CrossRef]
- Round, A.N.; Rigby, N.M.; MacDougall, A.; Morris, V.J. A new view of pectin structure revealed by acid hydrolysis and atomic force microscopy. Carbohydr. Res. 2010, 345, 487–497. [Google Scholar] [CrossRef] [PubMed]
- Morris, V.J.; Gromer, A.; Kirby, A.R.; Bongaerts, R.J.; Gunning, A.P. Using AFM and force spectroscopy to determine pectin structure and (bio) functionality. Food Hydrocoll. 2011, 25, 230–237. [Google Scholar] [CrossRef]
- Ralet-Renard, M.-C.; Lerouge, P.; Quéméner, B. Mass spectrometry for pectin structure analysis. Carbohydr. Res. 2009, 344, 1798–1807. [Google Scholar] [CrossRef] [PubMed]
- Willats, W.G.; Knox, J.P.; Mikkelsen, J.D. Pectin: New insights into an old polymer are starting to gel. Trends Food Sci. Technol. 2006, 17, 97–104. [Google Scholar] [CrossRef]
- Klemetsrud, T.; Jonassen, H.; Hiorth, M.; Kjøniksen, A.-L.; Smistad, G. Studies on pectin-coated liposomes and their interaction with mucin. Colloids Surf. B Biointerfaces 2013, 103, 158–165. Available online: http://www.ncbi.nlm.nih.gov/pubmed/23201733 (accessed on 13 February 2020). [CrossRef]
- Gacesa, P. Alginates. Carbohydr. Polym. 1988, 8, 161–182. [Google Scholar] [CrossRef]
- Hecht, H.; Srebnik, S. Structural characterization of sodium alginate and calcium alginate. Biomacromolecules 2016, 17, 2160–2167. [Google Scholar] [CrossRef]
- Johnson, F.A.; Craig, D.Q.M.; Mercer, A.D. Characterization of the block structure and molecular weight of sodium alginates. J. Pharm. Pharmacol. 2011, 49, 639–643. Available online: http://www.ncbi.nlm.nih.gov/pubmed/9255704 (accessed on 13 February 2020). [CrossRef]
- Sutherland, I.W. Alginates. In Biomaterials; Palgrave Macmillan: London, UK, 1991; pp. 307–331. [Google Scholar] [CrossRef]
- Poncelet, D.; Babak, V.; Dulieu, C.; Picot, A. A physico-chemical approach to production of alginate beads by emulsification-internal ionotropic gelation. Colloids Surf. A Physicochem. Eng. Asp. 1999, 155, 171–176. [Google Scholar] [CrossRef]
- Leong, J.-Y.; Lam, W.-H.; Ho, K.-W.; Voo, W.-P.; Lee, M.F.-X.; Lim, H.P.; Lim, S.-L.; Tey, B.-T.; Poncelet, D.; Chan, E.-S. Advances in fabricating spherical alginate hydrogels with controlled particle designs by ionotropic gelation as encapsulation systems. Particuology 2016, 24, 44–60. [Google Scholar] [CrossRef]
- Tønnesen, H.H.; Karlsen, J. Alginate in drug delivery systems. Drug Dev. Ind. Pharm. 2002, 28, 621–630. Available online: http://www.ncbi.nlm.nih.gov/pubmed/12149954 (accessed on 13 February 2020). [CrossRef] [PubMed]
- Ching, S.H.; Bansal, N.; Bhandari, B. Alginate gel particles—A review of production techniques and physical properties. Crit. Rev. Food Sci. Nutr. 2017, 57, 1133–1152. Available online: http://www.ncbi.nlm.nih.gov/pubmed/25976619 (accessed on 13 February 2020). [CrossRef] [PubMed]
- Boyd, J.; Turvey, J.R. Structural studies of alginic acid, using a bacterial poly-α-L-guluronate lyase. Carbohydr. Res. 1978, 66, 187–194. [Google Scholar] [CrossRef]
- Ingar Draget, K.; Østgaard, K.; Smidsrød, O. Homogeneous alginate gels: A technical approach. Carbohydr. Polym. 1990, 14, 159–178. [Google Scholar] [CrossRef]
- Zhu, F. Composition, structure, physicochemical properties, and modifications of cassava starch. Carbohydr. Polym. 2015, 122, 456–480. [Google Scholar] [CrossRef]
- Tester, R.F.; Karkalas, J.; Qi, X. Starch—Composition, fine structure and architecture. J. Cereal Sci. 2004, 39, 151–165. [Google Scholar] [CrossRef]
- Wu, A.C.; Li, E.; Gilbert, R.G. Exploring extraction/dissolution procedures for analysis of starch chain-length distributions. Carbohydr. Polym. 2014, 114, 36–42. [Google Scholar] [CrossRef]
- Cai, J.; Man, J.; Huang, J.; Liu, Q.; Wei, W.; Wei, C. Relationship between structure and functional properties of normal rice starches with different amylose contents. Carbohydr. Polym. 2015, 125, 35–44. [Google Scholar] [CrossRef] [PubMed]
- Bemiller, J.N. Pasting, paste, and gel properties of starch-hydrocolloid combinations. Carbohydr. Polym. 2011, 86, 386–423. [Google Scholar] [CrossRef]
- Güler, M.A.; Gök, M.K.; Figen, A.K.; Özgümüş, S. Swelling, mechanical and mucoadhesion properties of Mt/starch-g-PMAA nanocomposite hydrogels. Appl. Clay. Sci. 2015, 112–113, 44–52. [Google Scholar] [CrossRef]
- Mehta, S.; Verstraelen, H.; Peremans, K.; Villeirs, G.; Vermeire, S.; De Vos, F.; Mehuys, E.; Remon, J.P.; Vervaet, C. Vaginal distribution and retention of a multiparticulate drug delivery system, assessed by gamma scintigraphy and magnetic resonance imaging. Int. J. Pharm. 2012, 426, 44–53. Available online: http://www.ncbi.nlm.nih.gov/pubmed/22265911 (accessed on 14 February 2020). [CrossRef]
- Mehta, S.; Verstraelen, H.; Vandaele, L.; Mehuys, E.; Remon, J.P.; Vervaet, C. Vaginal distribution and retention of tablets comprising starch-based multiparticulates: Evaluation by colposcopy. Drug Dev. Ind. Pharm. 2012, 39, 1944–1950. [Google Scholar] [CrossRef]
- Poelvoorde, N.; Verstraelen, H.; Verhelst, R.; Saerens, B.; De Backer, E.; Santiago, G.L.D.S.; Vervaet, C.; Vaneechoutte, M.; De Boeck, F.; Van Bortel, L.; et al. In vivo evaluation of the vaginal distribution and retention of a multi-particulate pellet formulation. Eur. J. Pharm. Biopharm. 2009, 73, 280–284. Available online: http://www.ncbi.nlm.nih.gov/pubmed/19524668 (accessed on 14 February 2020). [CrossRef]
- Carrageenan—An Overview. ScienceDirect Topics. Available online: https://www.sciencedirect.com/topics/neuroscience/carrageenan (accessed on 26 May 2021).
- Shen, Y.-R.; Kuo, M.-I. Effects of different carrageenan types on the rheological and water-holding properties of tofu. LWT 2017, 78, 122–128. [Google Scholar] [CrossRef]
- Therkelsen, G.H. Carrageenan. In Industrial Gums: Polysaccharides and Their Derivatives, 3rd ed; Elsevier: Amsterdam, The Netherlands, 2012; pp. 145–180. [Google Scholar]
- Pacheco-Quito, E.-M.; Ruiz-Caro, R.; Rubio, J.; Tamayo, A.; Veiga, M.-D. Carrageenan-based acyclovir mucoadhesive vaginal tablets for prevention of genital herpes. Mar. Drugs 2020, 18, 249. Available online: www.mdpi.com/journal/marinedrugs (accessed on 26 May 2021). [CrossRef]
- Elias, C.J.; Coggins, C.; Alvarez, F.; Brache, V.; Fraser, I.S.; Lacarra, M.; Lähteenmäkl, P.; Massai, R.; Mishell, D.R.; Phillips, D.M.; et al. Colposcopic evaluation of a vaginal gel formulation of iota-carrageenan. Contraception 1997, 56, 387–389. [Google Scholar] [CrossRef]
- Sánchez-Sánchez, M.-P.; Martín-Illana, A.; Ruiz-Caro, R.; Bermejo, P.; Abad, M.-J.; Carro, R.; Bedoya, L.-M.; Tamayo, A.; Rubio, J.; Fernández-Ferreiro, A.; et al. Chitosan and kappa-carrageenan vaginal acyclovir formulations for prevention of genital herpes. In vitro and ex vivo evaluation. Mar. Drugs 2015, 13, 5976–5992. Available online: www.mdpi.com/journal/marinedrugsArticle (accessed on 26 May 2021). [CrossRef]
- Lal, M.; Lai, M.; Ugaonkar, S.; Wesenberg, A.; Kizima, L.; Rodriguez, A.; Levendosky, K.; Mizenina, O.; Fernández-Romero, J.; Zydowsky, T. Development of a vaginal fast-dissolving insert combining griffithsin and carrageenan for potential use against sexually transmitted infections. J. Pharm. Sci. 2018, 107, 2601–2610. [Google Scholar] [CrossRef] [PubMed]
- Al Sagheer, F.; Al-Sughayer, M.; Muslim, S.; Elsabee, M. Extraction and characterization of chitin and chitosan from marine sources in Arabian Gulf. Carbohydr. Polym. 2009, 77, 410–419. [Google Scholar] [CrossRef]
- Islam, S.; Bhuiyan, M.A.R.; Islam, M.N. Chitin and chitosan: Structure, properties and applications in biomedical engineering. J. Polym. Environ. 2017, 25, 854–866. [Google Scholar] [CrossRef]
- De Andrade, S.M.B.; Ladchumananandasivam, R.; da Rocha, B.G.; Belarmino, D.D.; Galvão, A.O. The use of exoskeletons of shrimp (Litopenaeus vanammei) and crab (Ucides cordatus) for the extraction of chitosan and production of nanomembrane. Mater. Sci. Appl. 2012, 3, 495–508. [Google Scholar]
- Puvvada, Y.S.; Vankayalapati, S.; Sukhavasi, S. Extraction of chitin from chitosan from exoskeleton of shrimp for application in the pharmaceutical industry. Int. Curr. Pharm. J. 2012, 1, 258–263. [Google Scholar] [CrossRef]
- Pillai, C.; Paul, W.; Sharma, C.P. Chitin and chitosan polymers: Chemistry, solubility and fiber formation. Prog. Polym. Sci. 2009, 34, 641–678. [Google Scholar] [CrossRef]
- Ravindra, R.; Krovvidi, K.R.; Khan, A. Solubility parameter of chitin and chitosan. Carbohydr. Polym. 1998, 36, 121–127. [Google Scholar] [CrossRef]
- Riva, R.; Ragelle, H.; Rieux, A.D.; Duhem, N.; Jérôme, C.; Préat, V. Chitosan and chitosan derivatives in drug delivery and tissue engineering. Adv. Polym. Sci. 2011, 244, 19–44. [Google Scholar]
- Baldrick, P. The safety of chitosan as a pharmaceutical excipient. Regul. Toxicol. Pharmacol. 2010, 56, 290–299. [Google Scholar] [CrossRef] [PubMed]
- Applications of Chitosan and Chitosan Derivatives in Drug Delivery. Available online: https://www.researchgate.net/publication/228468813_Applications_of_Chitosan_and_Chitosan_Derivatives_in_Drug_Delivery (accessed on 21 February 2020).
- Illum, L. Chitosan and its use as a pharmaceutical excipient. Pharm. Res. 1998, 15, 1326–1331. Available online: http://www.ncbi.nlm.nih.gov/pubmed/9755881 (accessed on 21 February 2020). [CrossRef]
- Tang, H.; Zhang, P.; Kieft, T.L.; Ryan, S.J.; Baker, S.M.; Wiesmann, W.P.; Rogelj, S. Antibacterial action of a novel functionalized chitosan-arginine against Gram-negative bacteria. Acta Biomater. 2010, 6, 2562–2571. [Google Scholar] [CrossRef]
- Jegatheeswaran, S.; Bhanot, U.; Siriwardena, A. In vivo evaluation of the chitosan-based haemostatic agent omni-stat® in porcine liver resection and in liver injury. Eur. Surg. Res. 2012, 49, 73–79. Available online: http://www.ncbi.nlm.nih.gov/pubmed/22906964 (accessed on 21 February 2020). [CrossRef] [PubMed]
- Zhang, H.-L.; Tao, Y.; Guo, J.; Hu, Y.-M.; Su, Z.-Q. Hypolipidemic effects of chitosan nanoparticles in hyperlipidemia rats induced by high fat diet. Int. Immunopharmacol. 2011, 11, 457–461. Available online: http://www.ncbi.nlm.nih.gov/pubmed/21215349 (accessed on 21 February 2020). [CrossRef] [PubMed]
- Sogias, I.A.; Williams, A.C.; Khutoryanskiy, V.V. Why is chitosan mucoadhesive? Biomacromolecules 2008, 9, 1837–1842. Available online: http://www.ncbi.nlm.nih.gov/pubmed/18540644 (accessed on 21 February 2020). [CrossRef] [PubMed]
- Alsarra, I.A. Chitosan topical gel formulation in the management of burn wounds. Int. J. Biol. Macromol. 2009, 45, 16–21. Available online: http://www.ncbi.nlm.nih.gov/pubmed/19447254 (accessed on 21 February 2020). [CrossRef] [PubMed]
- Lupo, N.; Fodor, B.; Muhammad, I.; Yaqoob, M.; Matuszczak, B.; Bernkop-Schnürch, A. Entirely S-protected chitosan: A promising mucoadhesive excipient for metronidazole vaginal tablets. Acta Biomater. 2017, 64, 106–115. Available online: http://www.ncbi.nlm.nih.gov/pubmed/29030305 (accessed on 21 February 2020). [CrossRef] [PubMed]
- Dai, T.; Tanaka, M.; Huang, Y.-Y.; Hamblin, M.R. Chitosan preparations for wounds and burns: Antimicrobial and wound-healing effects. Expert Rev. Anti Infect. Ther. 2011, 9, 857–879. [Google Scholar] [CrossRef]
- Jayakumar, R.; Prabaharan, M.; Nair, S.; Tamura, H. Novel chitin and chitosan nanofibers in biomedical applications. Biotechnol. Adv. 2010, 28, 142–150. [Google Scholar] [CrossRef] [PubMed]
- Ekici, S.; Ilgin, P.; Butun, S.; Sahiner, N. Hyaluronic acid hydrogel particles with tunable charges as potential drug delivery devices. Carbohydr. Polym. 2011, 84, 1306–1313. [Google Scholar] [CrossRef]
- Papakonstantinou, E.; Roth, M.; Karakiulakis, G. Hyaluronic acid: A key molecule in skin aging. Derm. Endocrinol. 2012, 4, 253–258. [Google Scholar] [CrossRef]
- Tamer, T.M. Hyaluronan and synovial joint: Function, distribution and healing. Interdiscip. Toxicol. 2013, 6, 111–125. [Google Scholar] [CrossRef]
- Kogan, G.; Šoltés, L.; Stern, R.; Gemeiner, P. Hyaluronic acid: A natural biopolymer with a broad range of biomedical and industrial applications. Biotechnol. Lett. 2006, 29, 17–25. [Google Scholar] [CrossRef]
- Brown, M.; Jones, S.A. Hyaluronic acid: A unique topical vehicle for the localized delivery of drugs to the skin. J. Eur. Acad. Dermatol. Venereol. 2005, 19, 308–318. Available online: http://www.ncbi.nlm.nih.gov/pubmed/15857456 (accessed on 21 February 2020). [CrossRef] [PubMed]
- Falcone, S.J.; Palmeri, D.M.; Berg, R.A. Rheological and cohesive properties of hyaluronic acid. J. Biomed. Mater. Res. Part A 2006, 76, 721–728. Available online: http://www.ncbi.nlm.nih.gov/pubmed/16315193 (accessed on 21 February 2020). [CrossRef] [PubMed]
- Fallacara, A.; Baldini, E.; Manfredini, S.; Vertuani, S. Hyaluronic acid in the third millennium. Polymers 2018, 10, 701. Available online: http://www.ncbi.nlm.nih.gov/pubmed/30960626 (accessed on 21 February 2020). [CrossRef] [PubMed]
- Hyaluronic Acid in Inflammation and Tissue Regeneration. Wounds Research. Available online: https://www.woundsresearch.com/article/hyaluronic-acid-inflammation-and-tissue-regeneration (accessed on 21 February 2020).
- Greenberg, D.; Stoker, A.; Kane, S.; Cockrell, M.; Cook, J. Biochemical effects of two different hyaluronic acid products in a co-culture model of osteoarthritis. Osteoarthr. Cartil. 2006, 14, 814–822. [Google Scholar] [CrossRef] [PubMed]
- Lev-Sagie, A.; Nyirjesy, P.; Tarangelo, N.; Bongiovanni, A.M.; Bayer, C.; Linhares, I.M.; Giraldo, P.C.; Ledger, W.J.; Witkin, S.S. Hyaluronan in vaginal secretions: Association with recurrent vulvovaginal candidiasis. Am. J. Obstet. Gynecol. 2009, 201, 206.e1–206.e5. Available online: http://www.ncbi.nlm.nih.gov/pubmed/19646572 (accessed on 24 February 2020). [CrossRef]
- Cermelli, C.; Cuoghi, A.; Scuri, M.; Bettua, C.; Neglia, R.G.; Ardizzoni, A.; Blasi, E.; Iannitti, T.; Palmieri, B. In vitro evaluation of antiviral and virucidal activity of a high molecular weight hyaluronic acid. Virol. J. 2011, 8, 141. Available online: http://www.ncbi.nlm.nih.gov/pubmed/21439070 (accessed on 24 February 2020). [CrossRef]
- Nomura, K.; Murakami, K.; Shozu, M.; Nakama, T.; Yui, N.; Inoue, M. Local application of danazol-loaded hyaluronic acid hydrogel to endometriosis in a rat model. Fertil. Steril. 2006, 85, 1157–1167. [Google Scholar] [CrossRef] [PubMed]
- Young, S.; Wong, M.; Tabata, Y.; Mikos, A.G. Gelatin as a delivery vehicle for the controlled release of bioactive molecules. J. Control. Release 2005, 109, 256–274. [Google Scholar] [CrossRef]
- Karim, A.; Bhat, R. Fish gelatin: Properties, challenges, and prospects as an alternative to mammalian gelatins. Food Hydrocoll. 2009, 23, 563–576. [Google Scholar] [CrossRef]
- B. Braun Sharing Expertise. Available online: https://www.bbraun.co.uk/en.html (accessed on 6 November 2020).
- Yavuz, S.T.; Sahiner, U.M.; Sekerel, B.E.; Tuncer, A.; Kalayci, O.; Sackesen, C. Anaphylactic reactions to measles-mumps-rubella vaccine in three children with allergies to hen’s egg and cow’s milk. Acta Paediatr. 2011, 100, e94–e96. [Google Scholar] [CrossRef]
- Bacelar, A.H.D.; Correia, J.S.; Oliveira, J.M.; Reis, R.L. Recent progress in gellan gum hydrogels provided by functionalization strategies. J. Mater. Chem. B 2016, 4, 6164–6174. [Google Scholar] [CrossRef] [PubMed]
- García-Ochoa, F.; Santos, V.E.; Casas, J.; Gomez, E. Xanthan gum: Production, recovery, and properties. Biotechnol. Adv. 2000, 18, 549–579. [Google Scholar] [CrossRef]
- Rodríguez Couto, S.; Sanromán, M.Á. Application of solid-state fermentation to food industry—A review. J. Food Eng. 2006, 76, 291–302. [Google Scholar] [CrossRef]
- Rosalam, S.; England, R. Review of xanthan gum production from unmodified starches by Xanthomonas campestris SP. Enzym. Microb. Technol. 2006, 39, 197–207. [Google Scholar] [CrossRef]
- Bejenariu, A.; Popa, M.; Le Cerf, D.; Picton, L. Stiffness xanthan hydrogels: Synthesis, swelling characteristics and controlled release properties. Polym. Bull. 2008, 61, 631–641. [Google Scholar] [CrossRef]
- Bodratti, A.; Alexandridis, P. Formulation of poloxamers for drug delivery. J. Funct. Biomater. 2018, 9, 11. [Google Scholar] [CrossRef] [PubMed]
- Djekic, L.; Čalija, B.; Medarević, Đ. Gelation behavior, drug solubilization capacity and release kinetics of poloxamer 407 aqueous solutions: The combined effect of copolymer, cosolvent and hydrophobic drug. J. Mol. Liq. 2020, 303, 112639. [Google Scholar] [CrossRef]
- Russo, E.; Villa, C. Poloxamer hydrogels for biomedical applications. Pharmaceutics 2019, 11, 671. [Google Scholar] [CrossRef]
- Schmolka, I.R. A review of block polymer surfactants. J. Am. Oil Chem. Soc. 1977, 54, 110–116. [Google Scholar] [CrossRef]
- Fakhari, A.; Corcoran, M.; Schwarz, A. Thermogelling properties of purified poloxamer 407. Heliyon 2017, 3, e00390. [Google Scholar] [CrossRef]
- Dumortier, G.; Grossiord, J.L.; Agnely, F.; Chaumeil, J.C. A review of poloxamer 407 pharmaceutical and pharmacological characteristics. Pharm. Res. 2006, 23, 2709–2728. [Google Scholar] [CrossRef] [PubMed]
- Lu, C.; Liu, M.; Fu, H.; Zhang, W.; Peng, G.; Zhang, Y.; Cao, H.; Luo, L. Novel thermosensitive in situ gel based on poloxamer for uterus delivery. Eur. J. Pharm. Sci. 2015, 77, 24–28. [Google Scholar] [CrossRef]
- Yuan, Y.; Cui, Y.; Zhang, L.; Zhu, H.-P.; Guo, Y.-S.; Zhong, B.; Hu, X.; Zhang, L.; Wang, X.-H.; Chen, L. Thermosensitive and mucoadhesive in situ gel based on poloxamer as new carrier for rectal administration of nimesulide. Int. J. Pharm. 2012, 430, 114–119. [Google Scholar] [CrossRef] [PubMed]
- Zaki, N.M.; A Awad, G.; Mortada, N.D.; El Hady, S.S.A. Enhanced bioavailability of metoclopramide HCl by intranasal administration of a mucoadhesive in situ gel with modulated rheological and mucociliary transport properties. Eur. J. Pharm. Sci. 2007, 32, 296–307. [Google Scholar] [CrossRef]
- Xuan, J.-J.; Balakrishnan, P.; Oh, D.H.; Yeo, W.H.; Park, S.M.; Yong, C.S.; Choi, H.-G. Rheological characterization and in vivo evaluation of thermosensitive poloxamer-based hydrogel for intramuscular injection of piroxicam. Int. J. Pharm. 2010, 395, 317–323. [Google Scholar] [CrossRef]
- Kojarunchitt, T.; Hook, S.; Rizwan, S.; Rades, T.; Baldursdottir, S. Development and characterisation of modified poloxamer 407 thermoresponsive depot systems containing cubosomes. Int. J. Pharm. 2011, 408, 20–26. [Google Scholar] [CrossRef]
- Asasutjarit, R.; Thanasanchokpibull, S.; Fuongfuchat, A.; Veeranondha, S. Optimization and evaluation of thermoresponsive diclofenac sodium ophthalmic in situ gels. Int. J. Pharm. 2011, 411, 128–135. [Google Scholar] [CrossRef]
- Soliman, K.A.; Ullah, K.; Shah, A.; Jones, D.S.; Singh, T.R. Poloxamer-based in situ gelling thermoresponsive systems for ocular drug delivery applications. Drug Discov. Today 2019, 24, 1575–1586. [Google Scholar] [CrossRef]
- Mayol, L.; Quaglia, F.; Borzacchiello, A.; Ambrosio, L.; I La Rotonda, M. A novel poloxamers/hyaluronic acid in situ forming hydrogel for drug delivery: Rheological, mucoadhesive and in vitro release properties. Eur. J. Pharm. Biopharm. 2008, 70, 199–206. [Google Scholar] [CrossRef]
- Yoo, J.W.; Giri, N.; Lee, C.H. PH-sensitive Eudragit nanoparticles for mucosal drug delivery. Int. J. Pharm. 2011, 403, 262–267. [Google Scholar] [CrossRef]
- Thakral, S.; Thakral, N.K.; Majumdar, D.K. Eudragit®: A technology evaluation. Expert Opin. Drug Deliv. 2012, 10, 131–149. [Google Scholar] [CrossRef]
- Ivanova, N.A.; Trapani, A.; Di Franco, C.; Mandracchia, D.; Trapani, G.; Franchini, C.; Corbo, F.; Tripodo, G.; Kolev, I.N.; Stoyanov, G.S.; et al. In vitro and ex vivo studies on diltiazem hydrochloride-loaded microsponges in rectal gels for chronic anal fissures treatment. Int. J. Pharm. 2019, 557, 53–65. [Google Scholar] [CrossRef] [PubMed]
- Ramineni, S.K.; Dziubla, T.D.; Cunningham, L.L.; Puleo, D.A. Local delivery of imiquimod in hamsters using mucoadhesive films and their residence time in human patients. Oral Surg. Oral Med. Oral Pathol. Oral Radiol. 2014, 118, 665–673. [Google Scholar] [CrossRef]
- Chantasart, D.; Tocanitchart, P.; Wongrakpanich, A.; Teeranachaideekul, V.; Junyaprasert, V.B. Fabrication and evaluation of Eudragit® polymeric films for transdermal delivery of piroxicam. Pharm. Dev. Technol. 2017, 23, 771–779. [Google Scholar] [CrossRef] [PubMed]
- Guterres, S.; Frank, L.A.; Sandri, G.; D’Autilia, F.; Contri, R.V.; Bonferoni, M.C.; Caramella, C.; Frank, A.G.; Pohlmann, A.R. Chitosan gel containing polymeric nanocapsules: A new formulation for vaginal drug delivery. Int. J. Nanomed. 2014, 9, 3151–3161. [Google Scholar] [CrossRef] [PubMed]
- Cao, F.; Zhang, X.; Ping, Q. New method for ophthalmic delivery of azithromycin by poloxamer/carbopol-based in situ gelling system. Drug Deliv. 2010, 17, 500–507. [Google Scholar] [CrossRef] [PubMed]
- Islam, M.T.; Rodríguez-Hornedo, N.; Ciotti, S.; Ackermann, C. Rheological characterization of topical carbomer gels neutralized to different pH. Pharm. Res. 2004, 21, 1192–1199. [Google Scholar] [CrossRef]
- Shahin, M.; Hady, S.A.; Hammad, M.; Mortada, N. Optimized formulation for topical administration of clotrimazole using Pemulen polymeric emulsifier. Drug Dev. Ind. Pharm. 2010, 37, 559–568. [Google Scholar] [CrossRef]
- Zhang, X.; Gu, X.; Wang, X.; Wang, H.; Mao, S. Tunable and sustained-release characteristics of venlafaxine hydrochloride from chitosan–carbomer matrix tablets based on in situ formed polyelectrolyte complex film coating. Asian J. Pharm. Sci. 2018, 13, 566–574. [Google Scholar] [CrossRef]
- Rashad, A.A.; El-Helaly, S.N.; El Rehim, R.T.A.; El Gazayerly, O. Core-in-cup/liquisol dual tackling effect on azelnidipine buccoadhesive tablet micromeritics, in vitro release, and mucoadhesive strength. Acta Pharm. 2019, 69, 381–398. [Google Scholar] [CrossRef] [PubMed]
- Green, J.T.; Thomas, G.A.O.; Rhodes, J.; Evans, B.K.; Russell, M.A.H.; Feyerabend, C.; Fuller, G.S.; Newcombe, R.G.; Sandborn, W.J. Pharmacokinetics of nicotinic carbomer enemas: A new treatment modality for ulcerative colitis. Clin. Pharmacol. Ther. 1997, 61, 340–3488. [Google Scholar] [CrossRef]
- Wang, L.; Tang, X. A novel ketoconazole bioadhesive effervescent tablet for vaginal delivery: Design, in vitro and “in vivo” evaluation. Int. J. Pharm. 2008, 350, 181–187. [Google Scholar] [CrossRef] [PubMed]
- Singla, A.K.; Chawla, M.; Singh, A. Potential applications of carbomer in oral mucoadhesive controlled drug delivery system: A review. Drug Dev. Ind. Pharm. 2000, 26, 913–924. [Google Scholar] [CrossRef]
- Michálek, J.; Vacík, J.; Kúdelková, J.; Ježová, N. Hydrogels for biomedical use based on 1-vinyl-2-pyrrolidone crosslinked with macromonomers. Angew. Makromol. Chem. 1996, 239, 151–160. [Google Scholar] [CrossRef]
- Goodwin, M.J.; Musa, O.M.; Berry, D.J.; Steed, J.W. Small-molecule povidone analogues in coamorphous pharmaceutical phases. Cryst. Growth Des. 2018, 18, 701–709. [Google Scholar] [CrossRef]
- Bühler, V. Polyvinylpyrrolidone Excipients for Pharmaceuticals: Povidone, Crospovidone and Copovidone. Springer: Berlin/Heidelberg, Germany, 2005; pp. 5–120. [Google Scholar]
- D’Souza, A.A.; Shegokar, R. Polyethylene glycol (PEG): A versatile polymer for pharmaceutical applications. Expert Opin. Drug Deliv. 2016, 13, 1257–1275. [Google Scholar] [CrossRef]
- Noda, Y.; Watanabe, K.; Sanagawa, A.; Sobajima, Y.; Fujii, S. Physicochemical properties of macrogol ointment and emulsion ointment blend developed for regulation of water absorption. Int. J. Pharm. 2011, 419, 131–136. [Google Scholar] [CrossRef]
- Harris, J.M. Poly (Ethylene Glycol) Chemistry: Biotechnical and Biomedical Applicationse; Springer: Berlin/Heidelberg, Germany, 2013; pp. 1–385. [Google Scholar]
- Acarturk, F. Mucoadhesive Vaginal Drug Delivery Systems. Recent Pat. Drug Deliv. Formul. 2009, 3, 193–205. [Google Scholar] [CrossRef]
- Machado, R.M.; Palmeira-De-Oliveira, A.; Martinez-De-Oliveira, J.; Palmeira-De-Oliveira, R. Vaginal semisolid products: Technological performance considering physiologic parameters. Eur. J. Pharm. Sci. 2017, 109, 556–568. [Google Scholar] [CrossRef] [PubMed]
- Palmeira-De-Oliveira, R.; Duarte, P.; Palmeira-De-Oliveira, A.; Das Neves, J.; Amaral, M.H.; Breitenfeld, L.; Martinez-De-Oliveira, J. Women’s experiences, preferences and perceptions regarding vaginal products: Results from a cross-sectional web-based survey in Portugal. Eur. J. Contracept. Reprod. Health Care 2015, 20, 259–271. [Google Scholar] [CrossRef] [PubMed]
- Baloglu, E.; Bernkop-Schnürch, A.; Karavana, S.Y.; Senyigit, Z.A. Strategies to prolong the intravaginal residence time of drug delivery systems. J. Pharm. Pharm. Sci. 2009, 12, 312–336. [Google Scholar] [CrossRef] [PubMed]
- Palmeira-de-Oliveira, R.; Duarte, P.; Palmeira-de-Oliveira, A.; das Neves, J.; Amaral, M.; Breitenfeld, L.; Martinez-de-Oliveira, J. What do Portuguese women prefer regarding vaginal products? Results from a cross-sectional web-based survey. Pharmaceutics 2014, 6, 543–556. [Google Scholar] [CrossRef]
- Nappi, R.E.; Liekens, G.; Brandenburg, U. Attitudes, perceptions and knowledge about the vagina: The International Vagina Dialogue Survey. Contraception 2006, 73, 493–500. [Google Scholar] [CrossRef]
- Van Den Berg, J.J.; Rosen, R.K.; Bregman, D.E.; Thompson, L.A.; Jensen, K.M.; Kiser, P.F.; Katz, D.F.; Buckheit, K.; Buckheit, R.W., Jr.; Morrow, K.M. “set it and forget it”: Women’s perceptions and opinions of long-acting topical vaginal gels. AIDS Behav. 2014, 18, 862–870. [Google Scholar] [CrossRef]
- Garg, S.; Vermani, K.; Garg, A.; Anderson, R.A.; Rencher, W.B.; Zaneveld, L.J.D. Development and characterization of bioadhesive vaginal films of sodium polystyrene sulfonate (PSS), a novel contraceptive antimicrobial agent. Pharm. Res. 2005, 22, 584–595. [Google Scholar] [CrossRef]
- Almdal, K.; Dyre, J.; Hvidt, S.; Kramer, O. Towards a phenomenological definition of the term “gel”. Polym. Gels Netw. 1993, 1, 5–17. [Google Scholar] [CrossRef]
- Rogovina, L.Z.; Vasil’Ev, V.G.; Braudo, E.E. Definition of the concept of polymer gel. Sci. Ser. C 2008, 50, 85–92. [Google Scholar] [CrossRef]
- Yang, X.; Zhang, G.; Zhang, D. Stimuli responsive gels based on low molecular weight gelators. J. Mater. Chem. 2012, 22, 38–50. [Google Scholar] [CrossRef]
- Salah, S.; Awad, G.E.; Makhlouf, A.I. Improved vaginal retention and enhanced antifungal activity of miconazole microsponges gel: Formulation development and in vivo therapeutic efficacy in rats. Eur. J. Pharm. Sci. 2018, 114, 255–266. [Google Scholar] [CrossRef] [PubMed]
- Menard, J.P. Antibacterial treatment of bacterial vaginosis: Current and emerging therapies. Int. J. Women’s Health 2011, 3, 295–305. [Google Scholar] [CrossRef]
- Friend, D.R. Advances in vaginal drug delivery. Drug Deliv. Transl. Res. 2011, 1, 183–184. [Google Scholar] [CrossRef] [PubMed]
- Rossi, S.; Ferrari, F.; Bonferoni, M.C.; Sandri, G.; Faccendini, A.; Puccio, A.; Caramella, C. Comparison of poloxamer-and chitosan-based thermally sensitive gels for the treatment of vaginal mucositis. Drug Dev. Ind. Pharm. 2013, 40, 352–360. [Google Scholar] [CrossRef] [PubMed]
- Yu, M.; Vajdy, M. Mucosal HIV transmission and vaccination strategies through oral compared with vaginal and rectal routes. Expert Opin. Biol. Ther. 2010, 10, 1181–1195. [Google Scholar] [CrossRef] [PubMed]
- Home—ClinicalTrials.gov. Available online: https://clinicaltrials.gov/ (accessed on 28 January 2021).
- De Araújo Pereira, R.R.; Bruschi, M.L. Vaginal mucoadhesive drug delivery systems. Drug Dev. Ind. Pharm. 2012, 38, 643–652. [Google Scholar] [CrossRef]
- Khutoryanskiy, V.V. Advances in mucoadhesion and mucoadhesive polymers. Macromol. Biosci. 2011, 11, 748–764. [Google Scholar] [CrossRef]
- Kong, M.; Chen, X.G.; Xing, K.; Park, H.J. Antimicrobial properties of chitosan and mode of action: A state of the art review. Int. J. Food Microbiol. 2010, 144, 51–63. [Google Scholar] [CrossRef]
- Bonferoni, M.C.; Giunchedi, P.; Scalia, S.; Rossi, S.; Sandri, G.; Caramella, C. Chitosan gels for the vaginal delivery of lactic acid: Relevance of formulation parameters to mucoadhesion and release mechanisms. AAPS PharmSciTech 2006, 7, E141–E147. [Google Scholar] [CrossRef]
- Bonferoni, M.C.; Sandri, G.; Rossi, S.; Ferrari, F.; Gibin, S.; Caramella, C. Chitosan citrate as multifunctional polymer for vaginal delivery. Evaluation of penetration enhancement and peptidase inhibition properties. Eur. J. Pharm. Sci. 2008, 33, 166–176. [Google Scholar] [CrossRef]
- Şenyiğit, Z.A.; Karavana, S.Y.; Eraç, B.; Gürsel, Ö.; Limoncu, M.H.; Baloğlu, E. Evaluation of chitosan based vaginal bioadhesive gel formulations for antifungal drugs. Acta Pharm. 2014, 64, 139–156. [Google Scholar] [CrossRef] [PubMed]
- Demiröz, F.N.T.; Acartürk, F.; Erdoğan, D. Development of long-acting bioadhesive vaginal gels of oxybutynin: Formulation, in vitro and in vivo evaluations. Int. J. Pharm. 2013, 457, 25–39. [Google Scholar] [CrossRef]
- Cevher, E.; Sensoy, D.; Taha, M.A.M.; Araman, A. Effect of thiolated polymers to textural and mucoadhesive properties of vaginal gel Formulations prepared with polycarbophil and chitosan. AAPS PharmSciTech 2008, 9, 953–965. [Google Scholar] [CrossRef] [PubMed]
- Bilensoy, E.; Rouf, M.A.; Vural, I.; Šen, M.; Hincal, A.A. Mucoadhesive, thermosensitive, prolonged-release vaginal gel for clotrimazole: β-cyclodextrin complex. AAPS PharmSciTech 2006, 7, E54–E60. [Google Scholar] [CrossRef] [PubMed]
- Aka-Any-Grah, A.; Bouchemal, K.; Koffi, A.; Agnely, F.; Zhang, M.; Djabourov, M.; Ponchel, G. Formulation of mucoadhesive vaginal hydrogels insensitive to dilution with vaginal fluids. Eur. J. Pharm. Biopharm. 2010, 76, 296–303. [Google Scholar] [CrossRef]
- Liu, Y.; Zhu, Y.; Wei, G.; Lu, W. Effect of carrageenan on poloxamer-based in situ gel for vaginal use: Improved in vitro and in vivo sustained-release properties. Eur. J. Pharm. Sci. 2009, 37, 306–312. [Google Scholar] [CrossRef] [PubMed]
- Zhou, Q.; Zhong, L.; Wei, X.; Dou, W.; Chou, G.; Wang, Z. Baicalein and hydroxypropyl-γ-cyclodextrin complex in poloxamer thermal sensitive hydrogel for vaginal administration. Int. J. Pharm. 2013, 454, 125–134. [Google Scholar] [CrossRef]
- Deshkar, S.S.; Palve, V.K. Formulation and development of thermosensitive cyclodextrin-based in situ gel of voriconazole for vaginal delivery. J. Drug Deliv. Sci. Technol. 2019, 49, 277–285. [Google Scholar] [CrossRef]
- Rençber, S.; Karavana, S.Y.; Şenyiğit, Z.A.; Eraç, B.; Limoncu, M.H.; Baloğlu, E. Mucoadhesive in situ gel formulation for vaginal delivery of clotrimazole: Formulation, preparation, and in vitro/in vivo evaluation. Pharm. Dev. Technol. 2016, 22, 551–561. [Google Scholar] [CrossRef]
- Cevher, E.; Açma, A.; Sinani, G.; Aksu, B.; Zloh, M.; Mülazımoğlu, L. Bioadhesive tablets containing cyclodextrin complex of itraconazole for the treatment of vaginal candidiasis. Int. J. Biol. Macromol. 2014, 69, 124–136. [Google Scholar] [CrossRef]
- Gupta, N.V.; Natasha, S.; Getyala, A.; Bhat, R.S. Bioadhesive vaginal tablets containing spray dried microspheres loaded with clotrimazole for treatment of vaginal Candidiasis. Acta Pharm. 2013, 63, 359–372. [Google Scholar] [CrossRef] [PubMed]
- Szymańska, E.; Winnicka, K.; Amelian, A.; Cwalina, U. Vaginal chitosan tablets with clotrimazole-design and evaluation of mucoadhesive properties using porcine vaginal mucosa, mucin and gelatine. Chem. Pharm. Bull. 2014, 62, 160–167. [Google Scholar] [CrossRef] [PubMed]
- Baloglu, E.; Senyıgıt, Z.A.; Karavana, S.Y.; Vetter, A.; Metın, D.Y.; Polat, S.H.; Guneri, T.; Bernkop-Schnurch, A. In vitro evaluation of mucoadhesive vaginal tablets of antifungal drugs prepared with thiolated polymer and development of a new dissolution technique for vaginal formulations. Chem. Pharm. Bull. 2011, 59, 952–958. [Google Scholar] [CrossRef]
- Alam, M.A.; Ahmad, F.J.; Khan, Z.I.; Khar, R.K.; Ali, M. Development and evaluation of acid-buffering bioadhesive vaginal tablet for mixed vaginal infections. AAPS PharmSciTech 2007, 8, 229–236. [Google Scholar] [CrossRef]
- Ceschel, G.C.; Maffei, P.; Borgia, S.L.; Ronchi, C.; Rossi, S. Development of a mucoadhesive dosage form for vaginal administration. Drug Dev. Ind. Pharm. 2001, 27, 541–547. [Google Scholar] [CrossRef]
- McConville, C.; Friend, D.R.; Clark, M.R.; Malcolm, K. Preformulation and development of a once-daily sustained-release tenofovir vaginal tablet tablet containing a single excipient. J. Pharm. Sci. 2013, 102, 1859–1868. [Google Scholar] [CrossRef]
- Notario-Pérez, F.; Cazorla-Luna, R.; Martín-Illana, A.; Ruiz-Caro, R.; Tamayo, A.; Rubio, J.; Veiga, M.-D. Optimization of tenofovir release from mucoadhesive vaginal tablets by polymer combination to prevent sexual transmission of HIV. Carbohydr. Polym. 2018, 179, 305–316. [Google Scholar] [CrossRef] [PubMed]
- McConville, C.; Major, I.; Devlin, B.; Brimer, A. Development of a multi-layered vaginal tablet containing dapivirine, levonorgestrel and acyclovir for use as a multipurpose prevention technology. Eur. J. Pharm. Biopharm. 2016, 104, 171–179. [Google Scholar] [CrossRef]
- Rastogi, R.; Teller, R.S.; Mesquita, P.M.M.; Herold, B.C.; Kiser, P.F. Osmotic pump tablets for delivery of antiretrovirals to the vaginal mucosa. Antivir. Res. 2013, 100, 255–258. [Google Scholar] [CrossRef]
- Perioli, L.; Ambrogi, V.; Pagano, C.; Massetti, E.; Rossi, C. New solid mucoadhesive systems for benzydamine vaginal administration. Colloids Surf. B Biointerfaces 2011, 84, 413–420. [Google Scholar] [CrossRef]
- Ekin, M.; Yaşar, L.; Savan, K.; Temur, M.; Uhri, M.; Gencer, I.; Kıvanç, E. The comparison of hyaluronic acid vaginal tablets with estradiol vaginal tablets in the treatment of atrophic vaginitis: A randomized controlled trial. Arch. Gynecol. Obstet. 2010, 283, 539–543. [Google Scholar] [CrossRef]
- Baloǧlu, E.; Özyazici, M.; Hizarcioǧlu, S.Y.; Karavana, H.A. An in vitro investigation for vaginal bioadhesive formulations: Bioadhesive properties and swelling states of polymer mixtures. II Farmaco 2003, 58, 391–396. [Google Scholar] [CrossRef]
- Hiorth, M.; Nilsen, S.; Tho, I. Bioadhesive mini-tablets for vaginal drug delivery. Pharmaceutics 2014, 6, 494–511. Available online: https://pubmed.ncbi.nlm.nih.gov/25166286/ (accessed on 21 March 2021). [CrossRef] [PubMed]
- Baffoe, C.S.; Nguyen, N.; Boyd, P.; Wang, W.; Morris, M.; McConville, C. Disulfiram-loaded immediate and extended release vaginal tablets for the localised treatment of cervical cancer. J. Pharm. Pharmacol. 2015, 67, 189–198. [Google Scholar] [CrossRef] [PubMed]
- Borges, S.; Costa, P.; Silva, J.; Teixeira, P. Effects of processing and storage on pediococcus pentosaceus SB83 in vaginal formulations: Lyophilized powder and tablets. Biomed. Res. Int. 2013, 2013. [Google Scholar] [CrossRef]
- Nowak, J.; Laffleur, F.; Bernkop-Schnürch, A. Preactivated hyaluronic acid: A potential mucoadhesive polymer for vaginal delivery. Int. J. Pharm. 2015, 478, 383–389. [Google Scholar] [CrossRef]
- Thurman, A.; Clark, M.; Hurlburt, J.; Doncel, G. Intravaginal rings as delivery systems for microbicides and multipurpose prevention technologies. Int. J. Women’s Health 2013, 5, 695–708. Available online: /pmc/articles/PMC3808127/ (accessed on 24 April 2021). [CrossRef]
- Rochira, M.; Miglietta, M.R.; Richardson, J.L.; Ferrari, L.; Beccaro, M.; Benedetti, L. Novel vaginal delivery systems for calcitonin. II. Preparation and characterization of HYAFF® microspheres containing calcitonin. Int. J. Pharm. 1996, 144, 19–26. [Google Scholar] [CrossRef]
- Pliszczak, D.; Bourgeois, S.; Bordes, C.; Valour, J.-P.; Mazoyer, M.-A.; Orecchioni, A.; Nakache, E.; Lanteri, P. Improvement of an encapsulation process for the preparation of pro- and prebiotics-loaded bioadhesive microparticles by using experimental design. Eur. J. Pharm. Sci. 2011, 44, 83–92. [Google Scholar] [CrossRef]
- Maestrelli, F.; Jug, M.; Cirri, M.; Kosalec, I.; Mura, P. Characterization and microbiological evaluation of chitosan-alginate microspheres for cefixime vaginal administration. Carbohydr. Polym. 2018, 192, 176–183. [Google Scholar] [CrossRef] [PubMed]
- Zhang, T.; Zhang, C.; Agrahari, V.; Murowchick, J.B.; Oyler, N.A.; Youan, B.B.C. Spray drying tenofovir loaded mucoadhesive and pH-sensitive microspheres intended for HIV prevention. Antivir. Res. 2013, 97, 334–346. [Google Scholar] [CrossRef]
- Albertini, B.; Passerini, N.; Di Sabatino, M.; Vitali, B.; Brigidi, P.; Rodriguez, L. Polymer-lipid based mucoadhesive microspheres prepared by spray-congealing for the vaginal delivery of econazole nitrate. Eur. J. Pharm. Sci. 2009, 36, 591–601. [Google Scholar] [CrossRef]
- Santiago, G.L.; Verstraelen, H.; Poelvoorde, N.; De Corte, S.; Claeys, G.; Trog, M.; De Backer, E.; Saerens, B.; Vervaet, C.; De Boeck, F.; et al. A pilot study evaluating the safety of vaginal administration of a multi-particulate pellet formulation. Eur. J. Pharm. Biopharm. 2009, 73, 399–403. [Google Scholar] [CrossRef]
- Mehta, S.; De Beer, T.; Remon, J.P.; Vervaet, C. Effect of disintegrants on the properties of multiparticulate tablets comprising starch pellets and excipient granules. Int. J. Pharm. 2012, 422, 310–317. [Google Scholar] [CrossRef]
- Hiorth, M.; Liereng, L.; Reinertsen, R.; Tho, I. Formulation of bioadhesive hexylaminolevulinate pellets intended for photodynamic therapy in the treatment of cervical cancer. Int. J. Pharm. 2013, 441, 544–554. [Google Scholar] [CrossRef] [PubMed]
- Pinto Reis, C.; Neufeld, R.J.; Ribeiro, A.J.; Veiga, F.; Nanoencapsulation, I. Methods for preparation of drug-loaded polymeric nanoparticles. Nanomed. Nanotechnol. Biol. Med. 2006, 2, 8–21. [Google Scholar] [CrossRef]
- Das Neves, J.; Sarmento, B. Precise engineering of dapivirine-loaded nanoparticles for the development of anti-HIV vaginal microbicides. Acta Biomater. 2015, 18, 77–87. [Google Scholar] [CrossRef]
- Gu, J.; Yang, S.; Ho, E.A. Biodegradable film for the targeted delivery of siRNA-loaded nanoparticles to vaginal immune cells. Mol. Pharm. 2015, 12, 2889–2903. [Google Scholar] [CrossRef]
- Yang, M.; Yu, T.; Wang, Y.Y.; Lai, S.K.; Zeng, Q.; Miao, B.; Hanes, J. Vaginal delivery of paclitaxel via nanoparticles with non-mucoadhesive surfaces suppresses cervical tumor growth. Adv. Healthc. Mater. 2014, 3, 1044–1052. [Google Scholar] [CrossRef] [PubMed]
- Melo, C.M.; Cardoso, J.F.; Perassoli, F.B.; Neto, A.S.D.O.; Pinto, L.M.; Marques, M.B.D.F.; Mussel, W.D.N.; Magalhães, J.; Moura, S.A.D.L.; Araújo, M.G.D.F.; et al. Amphotericin B-loaded eudragit RL100 nanoparticles coated with hyaluronic acid for the treatment of vulvovaginal candidiasis. Carbohydr. Polym. 2020, 230, 115608. [Google Scholar] [CrossRef] [PubMed]
- Cunha-Reis, C.; Machado, A.; Barreiros, L.; Araújo, F.; Nunes, R.; Seabra, V.; Ferreira, D.; Segundo, M.; Sarmento, B.; das Neves, J. Nanoparticles-in-film for the combined vaginal delivery of anti-HIV microbicide drugs. J. Control. Release 2016, 243, 43–53. [Google Scholar] [CrossRef] [PubMed]
- Jøraholmen, M.W.; Basnet, P.; Acharya, G.; Škalko-Basnet, N. PEGylated liposomes for topical vaginal therapy improve delivery of interferon alpha. Eur. J. Pharm. Biopharm. 2017, 113, 132–139. [Google Scholar] [CrossRef]
- Santos, S.S.; Lorenzoni, A.; Pegoraro, N.S.; Denardi, L.B.; Alves, S.H.; Schaffazick, S.R.; Cruz, L. Formulation and in vitro evaluation of coconut oil-core cationic nanocapsules intended for vaginal delivery of clotrimazole. Colloids Surf. B Biointerfaces 2014, 116, 270–276. [Google Scholar] [CrossRef]
- Varan, C.; Wickström, H.; Sandler, N.; Aktaş, Y.; Bilensoy, E. Inkjet printing of antiviral PCL nanoparticles and anticancer cyclodextrin inclusion complexes on bioadhesive film for cervical administration. Int. J. Pharm. 2017, 531, 701–713. [Google Scholar] [CrossRef]
- Machado, A.; Cunha-Reis, C.; Araújo, F.; Nunes, R.; Seabra, V.; Ferreira, D.; das Neves, J.; Sarmento, B. Development and in vivo safety assessment of tenofovir-loaded nanoparticles-in-film as a novel vaginal microbicide delivery system. Acta Biomater. 2016, 44, 332–340. [Google Scholar] [CrossRef]
- Sims, L.B.; Curtis, L.T.; Frieboes, H.B.; Steinbach-Rankins, J.M. Enhanced uptake and transport of PLGA-modified nanoparticles in cervical cancer. J. Nanobiotechnology 2016, 14, 1–12. [Google Scholar] [CrossRef]
- Maisel, K.; Reddy, M.; Xu, Q.; Chattopadhyay, S.; Cone, R.; Ensign, L.M.; Hanes, J. Nanoparticles coated with high molecular weight PEG penetrate mucus and provide uniform vaginal and colorectal distribution in vivo. Nanomedicine 2016, 11, 1337–1343. [Google Scholar] [CrossRef] [PubMed]
- Lechanteur, A.; Furst, T.; Evrard, B.; Delvenne, P.; Piel, G.; Hubert, P. Promoting vaginal distribution of E7 and MCL-1 siRNA-silencing nanoparticles for cervical cancer treatment. Mol. Pharm. 2017, 14, 1706–1717. [Google Scholar] [CrossRef]
- Wang, X.; Fu, L.; Lin, W.; Zhang, W.; Pei, Q.; Zheng, X.; Liu, S.; Zhang, T.; Xie, Z. Vaginal delivery of mucus-penetrating organic nanoparticles for photothermal therapy against cervical intraepithelial neoplasia in mice. J. Mater. Chem. B 2019, 7, 4528–4537. [Google Scholar] [CrossRef]
- Frank, L.A.; Chaves, P.S.; D’Amore, C.M.; Contri, R.V.; Frank, A.G.; Beck, R.; Pohlmann, A.R.; Buffon, A.; Guterres, S.S. The use of chitosan as cationic coating or gel vehicle for polymeric nanocapsules: Increasing penetration and adhesion of imiquimod in vaginal tissue. Eur. J. Pharm. Biopharm. 2017, 114, 202–212. [Google Scholar] [CrossRef]
- Lucena, P.A.; Nascimento, T.L.; Gaeti, M.P.N.; De Ávila, R.I.; Mendes, L.P.; Vieira, M.S.; Fabrini, D.; Amaral, A.C.; Lima, E.M. In vivo vaginal fungal load reduction after treatment with itraconazole-loaded polycaprolactone-nanoparticles. J. Biomed. Nanotechnol. 2018, 14, 1347–1358. [Google Scholar] [CrossRef] [PubMed]
- Marciello, M.; Rossi, S.; Caramella, C.; Remuñán-López, C. Freeze-dried cylinders carrying chitosan nanoparticles for vaginal peptide delivery. Carbohydr. Polym. 2017, 170, 43–51. [Google Scholar] [CrossRef] [PubMed]
- Rossi, S.; Vigani, B.; Puccio, A.; Bonferoni, M.C.; Sandri, G.; Ferrari, F. Chitosan ascorbate nanoparticles for the vaginal delivery of antibiotic drugs in atrophic vaginitis. Mar. Drugs 2017, 15, 319. [Google Scholar] [CrossRef]
- Lalan, M.S.; Patel, V.N.; Misra, A. Polymers in vaginal drug delivery: Recent advancements. In Applications of Polymers in Drug Delivery; Elsevier: Amsterdam, The Netherlands, 2021; pp. 281–303. [Google Scholar]
- Yoo, J.-W.; Dharmala, K.; Lee, C.H. The physicodynamic properties of mucoadhesive polymeric films developed as female controlled drug delivery system. Int. J. Pharm. 2006, 309, 139–145. [Google Scholar] [CrossRef]
- Machado, R.M.; Palmeira-De-Oliveira, A.; de Oliveira, J.M.; Palmeira-De-Oliveira, R. Vaginal films for drug delivery. J. Pharm. Sci. 2013, 102, 2069–2081. [Google Scholar] [CrossRef]
- Rohan, L.C.; Sassi, A.B. Vaginal drug delivery systems for HIV prevention. AAPS J. 2009, 11, 78–87. [Google Scholar] [CrossRef]
- Akil, A.; Devlin, B.; Cost, M.; Rohan, L.C. Increased dapivirine tissue accumulation through vaginal film codelivery of dapivirine and tenofovir. Mol. Pharm. 2014, 11, 1533–1541. [Google Scholar] [CrossRef]
- Traore, Y.L.; Fumakia, M.; Gu, J.; A Ho, E. Dynamic mechanical behaviour of nanoparticle loaded biodegradable PVA films for vaginal drug delivery. J. Biomater. Appl. 2018, 32, 1119–1126. [Google Scholar] [CrossRef]
- Cautela, M.P.; Moshe, H.; Sosnik, A.; Sarmento, B.; Das Neves, J. Composite films for vaginal delivery of tenofovir disoproxil fumarate and emtricitabine. J. Pharm. Biopharm. 2019, 138, 3–10. [Google Scholar] [CrossRef]
- Vartak, R.; Patki, M.; Menon, S.; Jablonski, J.; Mediouni, S.; Fu, Y.; Valente, S.T.; Billack, B.; Patel, K. β-cyclodextrin polymer/Soluplus® encapsulated Ebselen ternary complex (EβpolySol) as a potential therapy for vaginal candidiasis and pre-exposure prophylactic for HIV. Int. J. Pharm. 2020, 589, 119863. [Google Scholar] [CrossRef]
- Politch, J.A.; Cu-Uvin, S.; Moench, T.R.; Tashima, K.T.; Marathe, J.G.; Guthrie, K.M.; Cabral, H.; Nyhuis, T.; Brennan, M.; Zeitlin, L.; et al. Safety, acceptability, and pharmacokinetics of a monoclonal antibody-based vaginal multipurpose prevention film (MB66): A Phase I randomized trial. PLoS Med. 2021, 18, e1003495. [Google Scholar] [CrossRef]
- Ham, A.S.; Rohan, L.C.; Boczar, A.; Yang, L.; Buckheit, K.W.; Buckheit, R.W. Vaginal film drug delivery of the pyrimidinedione IQP-0528 for the prevention of HIV infection. Pharm. Res. 2012, 29, 1897–1907. [Google Scholar] [CrossRef]
- Neurath, A.R.; Strick, N.; Li, Y.-Y. Water dispersible microbicidal cellulose acetate phthalate film. BMC Infect. Dis. 2003, 3, 27. [Google Scholar] [CrossRef]
- Kumar, L.; Reddy, M.S.; Shirodkar, R.K.; Pai, G.K.; Krishna, V.T.; Verma, R. Preparation and characterisation of fluconazole vaginal films for the treatment of vaginal Candidiasis. Indian J. Pharm. Sci. 2013, 75, 585–590. [Google Scholar]
- Gahlot, N.; Maheshwari, R.K. Formulation and development of vaginal films of poorly water soluble drug, metronidazole, using mixed solvency concept and their evaluations. J. Drug Deliv. Ther. 2018, 8, 41–48. [Google Scholar] [CrossRef]
- Zhang, W.; Parniak, M.A.; Sarafianos, S.G.; Cost, M.R.; Rohan, L.C. Development of a vaginal delivery film containing EFdA, a novel anti-HIV nucleoside reverse transcriptase inhibitor. Int. J. Pharm. 2014, 461, 203–213. [Google Scholar] [CrossRef]
- Gong, T.; Zhang, W.; Parniak, M.A.; Graebing, P.W.; Moncla, B.; Gupta, P.; Empey, K.M.; Rohan, L.C. Preformulation and Vaginal Film Formulation Development of Microbicide Drug Candidate CSIC for HIV Prevention. J. Pharm. Innov. 2017, 12, 142–154. [Google Scholar] [CrossRef] [PubMed]
- Zhang, W.; Hu, M.; Shi, Y.; Gong, T.; Dezzutti, C.S.; Moncla, B.; Sarafianos, S.G.; Parniak, M.A.; Rohan, L.C. Vaginal microbicide film combinations of two reverse transcriptase inhibitors, EFdA and CSIC, for the prevention of HIV-1 sexual transmission. Pharm. Res. 2015, 32, 2960–2972. [Google Scholar] [CrossRef]
- Akil, A.; Parniak, M.A.; Dezzuitti, C.S.; Moncla, B.J.; Cost, M.R.; Li, M.; Rohan, L.C. Development and characterization of a vaginal film containing dapivirine, a non-nucleoside reverse transcriptase inhibitor (NNRTI), for prevention of HIV-1 sexual transmission. Drug Deliv. Transl. Res. 2011, 1, 209–222. [Google Scholar] [CrossRef]
- Yoo, J.-W.; Acharya, G.; Lee, C.H. In vivo evaluation of vaginal films for mucosal delivery of nitric oxide. Biomaterials 2009, 30, 3978–3985. [Google Scholar] [CrossRef]
- Notario-Pérez, F.; Martín-Illana, A.; Cazorla-Luna, R.; Ruiz-Caro, R.; Bedoya, L.-M.; Peña, J.; Veiga, M.-D. Development of mucoadhesive vaginal films based on HPMC and zein as novel formulations to prevent sexual transmission of HIV. Int. J. Pharm. 2019, 570, 118643. [Google Scholar] [CrossRef]
- Gyotoku, T.; Aurelian, L.; Neurath, A.R. Cellulose acetate phthalate (CAP): An “inactive” pharmaceutical excipient with antiviral activity in the mouse model of genital herpesvirus infection. Antivir. Chem. Chemother. 1999, 10, 327–332. [Google Scholar] [CrossRef][Green Version]
- Lu, H.; Zhao, Q.; Wallace, G.; Liu, S.; He, Y.; Shattock, R.; Neurath, A.R.; Jiang, B.S. Cellulose acetate 1,2-benzenedicarboxylate inhibits infection by cell-free and cell-associated primary HIV-1 isolates. AIDS Res. Hum. Retrovir. 2006, 22, 411–418. [Google Scholar] [CrossRef]
- Regev, G.; Patel, S.K.; Moncla, B.J.; Twist, J.; Devlin, B.; Rohan, L.C. Novel Application of Hot Melt Extrusion for the Manufacturing of Vaginal Films Containing Microbicide Candidate Dapivirine. AAPS PharmSciTech 2019, 20, 239. [Google Scholar] [CrossRef]
- Machado, R.S.M.; Tomás, M.; Palmeira-De-Oliveira, A.; de Oliveira, J.M.; Palmeira-De-Oliveira, R. The vaginal sheet: An innovative form of vaginal film for the treatment of vaginal infections. Drug Dev. Ind. Pharm. 2020, 46, 135–145. [Google Scholar] [CrossRef]
- Garg, S.; Goldman, D.; Krumme, M.; Rohan, L.C.; Smoot, S.; Friend, D.R. Advances in development, scale-up and manufacturing of microbicide gels, films, and tablets. Antivir. Res. 2010, 88, S19–S29. [Google Scholar] [CrossRef]
- Notario-Pérez, F.; Cazorla-Luna, R.; Martín-Illana, A.; Galante, J.; Ruiz-Caro, R.; das Neves, J.; Veiga, M.-D. Design, fabrication and characterisation of drug-loaded vaginal films: State-of-the-art. J. Control. Release 2020, 327, 477–499. [Google Scholar] [CrossRef] [PubMed]
- Garg, S.; Tambwekar, K.R.; Vermani, K.; Kandarapu, R.; Garg, A.; Waller, D.P.; Zaneveld, L.J. Development pharmaceutics of microbicide formulations. Part II: Formulation, evaluation, and challenges. AIDS Patient Care STDs 2003, 17, 377–399. [Google Scholar] [CrossRef] [PubMed]
- Drumond, N.; van Riet-Nales, D.A.; Karapinar-Çarkit, F.; Stegemann, S. Patients’ appropriateness, acceptability, usability and preferences for pharmaceutical preparations: Results from a literature review on clinical evidence. Int. J. Pharm. 2017, 521, 294–305. [Google Scholar] [CrossRef]
- Ghosal, K.; Ranjan, A.; Bhowmik, B.B. A novel vaginal drug delivery system: Anti-HIV bioadhesive film containing abacavir. J. Mater. Sci. Mater. Med. 2014, 25, 1679–1689. [Google Scholar] [CrossRef]
- Bassi, P.; Kaur, G. Bioadhesive vaginal drug delivery of nystatin using a derivatized polymer: Development and characterization. Eur. J. Pharm. Biopharm. 2015, 96, 173–184. [Google Scholar] [CrossRef]
- Mishra, R.; Soni, K.; Mehta, T. Mucoadhesive vaginal film of fluconazole using cross-linked chitosan and pectin: In vitro and in vivo study. J. Therm. Anal. Calorim. 2017, 130, 1683–1695. [Google Scholar] [CrossRef]
- Dolci, L.S.; Albertini, B.; Di Filippo, M.F.; Bonvicini, F.; Passerini, N.; Panzavolta, S. Development and in vitro evaluation of mucoadhesive gelatin films for the vaginal delivery of econazole. Int. J. Pharm. 2020, 591, 119979. [Google Scholar] [CrossRef]
- Frankman, O.; Raabe, N.; A Ingemansson, C. Clinical Evaluation of C-Film, a Vaginal Contraceptive. J. Int. Med Res. 1975, 3, 292–296. [Google Scholar] [CrossRef]
- Hynes, J.S.; Sales, J.M.; Sheth, A.N.; Lathrop, E.; Haddad, L.B. Interest in multipurpose prevention technologies to prevent HIV/STIs and unintended pregnancy among young women in the United States. Contraception 2018, 97, 277–284. [Google Scholar] [CrossRef] [PubMed]
- Schreier, J.; Sales, J.; Sheth, A.; Lathrop, E.; Haddad, L. Interest in multipurpose prevention technologies for protection against unintended pregnancy, human immunodeficiency virus and other sexually transmitted infections among women in the united states. Am. J. Obstet. Gynecol. 2017, 217, 731. [Google Scholar] [CrossRef]
- Fernandes, T.; Baxi, K.; Sawarkar, S.; Sarmento, B.; das Neves, J. Vaginal multipurpose prevention technologies: Promising approaches for enhancing women’s sexual and reproductive health. Expert Opin. Drug Deliv. 2020, 17, 379–393. [Google Scholar] [CrossRef] [PubMed]
- Repka, M.; Repka, S.; Mcginity, J. Bioadhesive Hot-Melt Extruded Film for Topical and Mucosal Adhesion Applications and Drug Delivery and Process for Preparation Thereof. U.S. Patent US6375963B1, 23 April 2002. [Google Scholar]
- Leon, T.; Gabel, P. Dissolvable Vaginal Deodorizing Films and Methods of Vaginal Deodorizing Utilizing Pliable Dissolvable Film. WO2004103232A1, 2 December 2004. [Google Scholar]
- Maniar, M.; Parandoosh, S. Ph-Responsive Film for Intravaginal Delivery of a Beneficial Agent. US20060018951A1, 4 April 2005. [Google Scholar]
- Yang, J.T.; Gao, H.M. Lactobacillus Drug Film. CN101199555A, 15 December 2006. [Google Scholar]
- Staab, R.J. Methods for Delivery of Medication Using a Dissolvable Device. US20130136784A1, 16 October 2009. [Google Scholar]
- Notario-Pérez, F.; Galante, J.; Martín-Illana, A.; Cazorla-Luna, R.; Sarmento, B.; Ruiz-Caro, R.; das Neves, J.; Veiga, M.D. Development of pH-sensitive vaginal films based on methacrylate copolymers for topical HIV-1 pre-exposure prophylaxis. Acta Biomater. 2021, 121, 316–327. [Google Scholar] [CrossRef]
- Griesser, J.; Hetényi, G.; Bernkop-Schnürch, A. Thiolated hyaluronic acid as versatile mucoadhesive polymer: From the chemistry behind to product developments-What are the capabilities? Polymers 2018, 10, 243. Available online: www.mdpi.com/journal/polymers (accessed on 20 May 2021). [CrossRef]
- Cook, M.T.; Brown, M. Polymeric gels for intravaginal drug delivery. J. Control. Release 2018, 270, 145–157. [Google Scholar] [CrossRef]
- Borin, M.T. Systemic absorption of clindamycin following intra vaginal application of clindamycin phosphate 1% cream. J. Clin. Pharmacol. 1990, 30, 33–38. Available online: https://accp1.onlinelibrary.wiley.com/doi/full/10.1002/j.1552-4604.1990.tb03435.x (accessed on 20 May 2021). [CrossRef]
- Gong, E.; Matthews, B.; McCarthy, T.; Chu, J.; Holan, G.; Raff, J.; Sacks, S. Evaluation of dendrimer SPL7013, a lead microbicide candidate against herpes simplex viruses. Antivir. Res. 2005, 68, 139–146. [Google Scholar] [CrossRef]
- Friedl, H.E.; Dünnhaupt, S.; Waldner, C.; Bernkop-Schnürch, A. Preactivated thiomers for vaginal drug delivery vehicles. Biomaterials 2013, 34, 7811–7818. [Google Scholar] [CrossRef]
- Podaralla, S.; Alt, C.; Shankar, G.N. Formulation development and evaluation of innovative two-polymer (SR-2P) bioadhesive vaginal gel. AAPS PharmSciTech 2014, 15, 928–938. [Google Scholar] [CrossRef]
- D’Cruz, O.J.; Uckun, F.M. Gel-microemulsions as vaginal spermicides and intravaginal drug delivery vehicles. Contraception 2001, 64, 113–123. [Google Scholar] [CrossRef]
- Kejdušová, M.; Vysloužil, J.; Kubová, K.; Celer, V.; Krásna, M.; Pechová, A.; Vyskočilová, V.; Košťál, V. Antimicrobial properties of microparticles based on carmellose cross-linked by Cu2+ ions. BioMed Res. Int. 2015, 2015, 1–9. [Google Scholar] [CrossRef]
- Pradines, B.; Bories, C.; Vauthier, C.; Ponchel, G.; Loiseau, P.M.; Bouchemal, K. Drug-free chitosan coated poly(isobutylcyanoacrylate) nanoparticles are active against Trichomonas vaginalis and non-toxic towards pig vaginal mucosa. Pharm. Res. 2014, 32, 1229–1236. [Google Scholar] [CrossRef] [PubMed]
- Luganini, A.; Nicoletto, S.F.; Pizzuto, L.; Pirri, G.; Giuliani, A.; Landolfo, S.; Gribaudo, G. Inhibition of herpes simplex virus type 1 and type 2 infections by peptide-derivatized dendrimers. Agents Chemother. 2011, 55, 3231–3239. [Google Scholar] [CrossRef] [PubMed]
- Navath, R.S.; Menjoge, A.R.; Dai, H.; Romero, R.; Kannan, S.; Kannan, R.M. Injectable PAMAM dendrimer-PEG hydrogels for the treatment of genital infections: Formulation and in vitro and in vivo evaluation. Mol. Pharm. 2011, 8, 1209–1223. [Google Scholar] [CrossRef] [PubMed]
- Kim, Y.T.; Shin, B.K.; Garripelli, V.K.; Kim, J.K.; Davaa, E.; Jo, S.; Park, J.S. A thermosensitive vaginal gel formulation with HPγCD for the pH-dependent release and solubilization of amphotericin B. Eur. J. Pharm. Sci. 2010, 41, 399–406. [Google Scholar] [CrossRef]
- Calixto, G.M.F.; Salmazi, R.; Bernegossi, J.; Ramos, M.A.D.S.; Bauab, T.; Chorilli, M. A Curcumin-loaded liquid crystal precursor mucoadhesive system for the treatment of vaginal candidiasis. Int. J. Nanomed. 2015, 10, 4815–4824. [Google Scholar] [CrossRef]
- Chen, D.; Sun, K.; Mu, H.; Tang, M.; Liang, R.; Wang, A.; Liu, W. pH and temperature dual-sensitive liposome gel based on novel cleavable mPEG-Hz-CHEMS polymeric vaginal delivery system. Int. J. Nanomed. 2012, 7, 2621–2630. [Google Scholar] [CrossRef]
- Blum, J.S.; Weller, C.E.; Booth, C.J.; Babar, I.A.; Liang, X.; Slack, F.; Saltzman, W.M. Prevention of K-Ras- and Pten-mediated intravaginal tumors by treatment with camptothecin-loaded PLGA nanoparticles. Drug Deliv. Transl. Res. 2011, 1, 383–394. [Google Scholar] [CrossRef] [PubMed]
- Bigucci, F.; Abruzzo, A.; Vitali, B.; Saladini, B.; Cerchiara, T.; Gallucci, M.C.; Luppi, B. Vaginal inserts based on chitosan and carboxymethylcellulose complexes for local delivery of chlorhexidine: Preparation, characterization and antimicrobial activity. Int. J. Pharm. 2015, 478, 456–463. [Google Scholar] [CrossRef] [PubMed]
- Abruzzo, A.; Bigucci, F.; Cerchiara, T.; Saladini, B.; Gallucci, M.; Cruciani, F.; Vitali, B.; Luppi, B. Chitosan/alginate complexes for vaginal delivery of chlorhexidine digluconate. Carbohydr. Polym. 2013, 91, 651–658. [Google Scholar] [CrossRef]
- Zong, S.; Wang, X.; Yang, Y.; Wu, W.; Li, H.; Ma, Y.; Lin, W.; Sun, T.; Huang, Y.; Xie, Z.; et al. The use of cisplatin-loaded mucoadhesive nanofibers for local chemotherapy of cervical cancers in mice. Eur. J. Pharm. Biopharm. 2015, 93, 127–135. [Google Scholar] [CrossRef] [PubMed]
- Dobaria, N.; Mashru, R. Design and in vitro evaluation of a novel bioadhesive vaginal drug delivery system for clindamycin phosphate. Pharm. Dev. Technol. 2009, 15, 405–414. [Google Scholar] [CrossRef]
- Chang, J.Y.; Oh, Y.-K.; Choi, H.-G.; Kim, Y.B.; Kim, C.-K. Rheological evaluation of thermosensitive and mucoadhesive vaginal gels in physiological conditions. Int. J. Pharm. 2002, 241, 155–163. [Google Scholar] [CrossRef]
- Mishra, R.; Joshi, P.; Mehta, T. Formulation, development and characterization of mucoadhesive film for treatment of vaginal candidiasis. Int. J. Pharm. Investig. 2016, 6, 47–55. [Google Scholar] [CrossRef]
- Cu, Y.; Booth, C.J.; Saltzman, W.M. In vivo distribution of surface-modified PLGA nanoparticles following intravaginal delivery. J. Control. Release 2011, 156, 258–264. [Google Scholar] [CrossRef]
- Das Neves, J.; Araújo, F.; Andrade, F.; Amiji, M.; Bahia, M.F.; Sarmento, B. Biodistribution and pharmacokinetics of Dapivirine-loaded nanoparticles after vaginal delivery in mice. Pharm. Res. 2014, 31, 1834–1845. [Google Scholar] [CrossRef]
- Ensign, L.M.; Hoen, T.E.; Maisel, K.; Cone, R.A.; Hanes, J.S. Enhanced vaginal drug delivery through the use of hypotonic formulations that induce fluid uptake. Biomaterials 2013, 34, 6922–6929. [Google Scholar] [CrossRef] [PubMed]
- Parodi, B.; Russo, E.; Caviglioli, G.; Baldassari, S.; Gaglianone, N.; Schito, A.M.; Cafaggi, S. A chitosan lactate/poloxamer 407-based matrix containing Eudragit RS microparticles for vaginal delivery of econazole: Design and in vitro evaluation. Drug Dev. Ind. Pharm. 2013, 39, 1911–1920. [Google Scholar] [CrossRef]
- Derby, N.; Lal, M.; Aravantinou, M.; Kizima, L.; Barnable, P.; Rodriguez, A.; Lai, M.; Wesenberg, A.; Ugaonkar, S.; Levendosky, K.; et al. Griffithsin carrageenan fast dissolving inserts prevent SHIV HSV-2 and HPV infections in vivo. Nat. Commun. 2018, 9, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Srinivasan, P.; Zhang, J.; Martin, A.; Kelley, K.; McNicholl, J.M.; Buckheit, R.W., Jr.; Smith, J.M.; Ham, A.S. Safety and pharmacokinetics of quick-dissolving polymeric vaginal films delivering the antiretroviral IQP-0528 for preexposure prophylaxis. Antimicrob. Agents Chemother. 2016, 60, 4140–4150. [Google Scholar] [CrossRef] [PubMed]
- Mahalingam, A.; Smith, E.; Fabian, J.; Damian, F.R.; Peters, J.J.; Clark, M.R.; Friend, D.R.; Katz, D.F.; Kiser, P.F. Design of a semisolid vaginal microbicide gel by relating composition to properties and performance. Pharm. Res. 2010, 27, 2478–2491. [Google Scholar] [CrossRef]
- Dobaria, N.B.; Badhan, A.C.; Mashru, R.C. A novel itraconazole bioadhesive film for vaginal delivery: Design, optimization, and physicodynamic characterization. AAPS PharmSciTech 2009, 10, 951–959. [Google Scholar] [CrossRef]
- Karavana, S.Y.; Rençbe, S.; Şenyiğit, Z.A.; Baloğlu, E. A New In-Situ Gel Formulation of Itraconazole for Vaginal Administration. Pharmacol. Pharm. 2012, 3, 417–426. [Google Scholar] [CrossRef]
- Mirza, M.A.; Ahmad, S.; Mallick, N.; Manzoor, N.; Talegaonkar, S.; Iqbal, Z. Development of a novel synergistic thermosensitive gel for vaginal candidiasis: An in vitro, in vivo evaluation. Colloids Surf. B Biointerfaces 2013, 103, 275–282. [Google Scholar] [CrossRef]
- Małolepsza-Jarmołowska, K. Studies on gynecological hydrophilic lactic acid preparations part 8: Use of chitosan as lactic acid carrier in intravaginal tablets. Acta Pol. Pharm. Drug Res. 2007, 64, 69–72. [Google Scholar]
- Bouchemal, K.; Frelichowska, J.; Martin, L.; Moal, V.L.-L.; Le Grand, R.; Dereuddre-Bosquet, N.; Djabourov, M.; Aka-Any-Grah, A.; Koffi, A.; Ponchel, G. Note on the formulation of thermosensitive and mucoadhesive vaginal hydrogels containing the miniCD4 M48U1 as anti-HIV-1 microbicide. Int. J. Pharm. 2013, 454, 649–652. [Google Scholar] [CrossRef]
- Forbes, C.J.; McCoy, C.F.; Murphy, D.J.; Woolfson, A.D.; Moore, J.P.; Evans, A.; Shattock, R.J.; Malcolm, R.K. Modified silicone elastomer vaginal gels for sustained release of antiretroviral HIV microbicides. J. Pharm. Sci. 2014, 103, 1422–1432. [Google Scholar] [CrossRef]
- Jalil, A.; Asim, M.H.; Le, N.-M.N.; Laffleur, F.; Matuszczak, B.; Tribus, M.; Bernkop–Schnürch, A. S-protected gellan gum: Decisive approach towards mucoadhesive antimicrobial vaginal films. Int. J. Biol. Macromol. 2019, 130, 148–157. [Google Scholar] [CrossRef] [PubMed]
- Perioli, L.; Ambrogi, V.; Venezia, L.; Pagano, C.; Ricci, M.; Rossi, C. Chitosan and a modified chitosan as agents to improve performances of mucoadhesive vaginal gels. Colloids Surf. B Biointerfaces 2008, 66, 141–145. [Google Scholar] [CrossRef] [PubMed]
- Ibrahim, E.-S.A.; Ismail, S.; Fetih, G.; Shaaban, O.; Hassanein, K.; Ellah, N.A. Development and characterization of thermosensitive pluronic-based metronidazole in situ gelling formulations for vaginal application. Acta Pharm. 2012, 62, 59–70. [Google Scholar] [CrossRef]
- El-Kamel, A.; Sokar, M.; Naggar, V.; Al Gamal, S. Chitosan and sodium alginate-based bioadhesive vaginal tablets. Vol. 4, AAPS PharmSci. AAPS PharmSci 2002, 4, 224–230. [Google Scholar] [CrossRef]
- Perioli, L.; Ambrogi, V.; Pagano, C.; Scuota, S.; Rossi, C. FG90 chitosan as a new polymer for metronidazole mucoadhesive tablets for vaginal administration. Int. J. Pharm. 2009, 377, 120–127. [Google Scholar] [CrossRef] [PubMed]
- Vanić, Ž.; Planinšek, O.; Škalko-Basnet, N.; Tho, I. Tablets of pre-liposomes govern in situ formation of liposomes: Concept and potential of the novel drug delivery system. Eur. J. Pharm. Biopharm. 2014, 88, 443–454. [Google Scholar] [CrossRef]
- D’Cruz, O.J.; Samuel, P.; Uckun, F.M. Conceival, a novel noncontraceptive vaginal vehicle for lipophilic microbicides. AAPS PharmSciTech 2005, 6, E56–E64. [Google Scholar] [CrossRef][Green Version]
- Friedland, B.A.; Hoesley, C.J.; Plagianos, M.; Hoskin, E.; Zhang, S.; Teleshova, N.; Alami, M.; Novak, L.; Kleinbeck, K.R.; Katzen, L.L.; et al. First-in-human trial of MIV-150 and zinc acetate coformulated in a carrageenan gel: Safety, pharmacokinetics, acceptability, adherence, and pharmacodynamics. J. Acquir. Immune Defic. Syndr. 2016, 73, 489–496. [Google Scholar] [CrossRef]
- Kenney, J.; Singer, R.; Derby, N.; Aravantinou, M.; Abraham, C.J.; Menon, R.; Seidor, S.; Zhang, S.; Gettie, A.; Blanchard, J.F.; et al. A single dose of a MIV-150/zinc acetate gel provides 24h of protection against vaginal simian human immunodeficiency virus reverse transcriptase infection, with more limited protection rectally 8-24h after gel use. AIDS Res. Hum. Retrovir. 2012, 28, 1476–1484. [Google Scholar] [CrossRef] [PubMed]
- Ball, C.; Woodrow, K.A. Electrospun solid dispersions of maraviroc for rapid intravaginal preexposure prophylaxis of HIV. Antimicrob. Agents Chemother. 2014, 58, 4855–4865. [Google Scholar] [CrossRef] [PubMed]
- Cevher, E.; Şensoy, D.; Zloh, M.; Mülazımoğlu, L. Preparation and characterisation of natamycin: γ-cyclodextrin inclusion complex and its evaluation in vaginal mucoadhesive formulations. J. Pharm. Sci. 2008, 97, 4319–4335. [Google Scholar] [CrossRef] [PubMed]
- Hombach, J.; Palmberger, T.F.; Bernkop-Schnürch, A. Development and in vitro evaluation of a mucoadhesive vaginal delivery system for nystatin. J. Pharm. Sci. 2009, 98, 555–564. [Google Scholar] [CrossRef] [PubMed]
- Martín-Villena, M.; Fernández-Campos, F.; Calpena-Campmany, A.; DE Februaryrer, N.B.; Ruiz-Martínez, M.; Clares-Naveros, B. Novel microparticulate systems for the vaginal delivery of nystatin: Development and characterization. Carbohydr. Polym. 2013, 94, 1–11. [Google Scholar] [CrossRef]
- Kuo-Haller, P.; Cu, Y.; Blum, J.; Appleton, J.A.; Saltzman, W.M. Vaccine delivery by polymeric vehicles in the mouse reproductive tract induces sustained local and systemic immunity. Mol. Pharm. 2010, 7, 1585–1595. [Google Scholar] [CrossRef] [PubMed]
- Talwar, G.; Dar, S.A.; Rai, M.K.; Reddy, K.; Mitra, D.; Kulkarni, S.V.; Doncel, G.F.; Buck, C.; Schiller, J.T.; Muralidhar, S.; et al. A novel polyherbal microbicide with inhibitory effect on bacterial, fungal and viral genital pathogens. Int. J. Antimicrob. Agents 2008, 32, 180–185. [Google Scholar] [CrossRef] [PubMed]
- Almomen, A.; Cho, S.; Yang, C.-H.; Aliyah, A.; Jarboe, E.A.; Peterson, C.M.; Huh, K.M.; Janát-Amsbury, M.M. Thermosensitive progesterone hydrogel: A safe and effective new formulation for vaginal application. Pharm. Res. 2015, 32, 2266–2279. [Google Scholar] [CrossRef]
- Campaña-Seoane, M.; Peleteiro, A.; Laguna, R.; Otero-Espinar, F.J. Bioadhesive emulsions for control release of progesterone resistant to vaginal fluids clearance. Int. J. Pharm. 2014, 477, 495–505. [Google Scholar] [CrossRef]
- Tasdighi, E.; Azar, Z.J.; Mortazavi, S.A. Development and In-vitro evaluation of a contraceptive vagino-adhesive propranolol hydrochloride gel. Iran. J. Pharm. Res. 2012, 11, 13–26. [Google Scholar]
- Teller, R.S.; Rastogi, R.; Johnson, T.J.; Blair, M.J.; Hitchcock, R.W.; Kiser, P.F. Intravaginal flux controlled pump for sustained release of macromolecules. Pharm. Res. 2014, 31, 2344–2353. [Google Scholar] [CrossRef] [PubMed]
- Date, A.A.; Shibata, A.; Goede, M.; Sanford, B.; La Bruzzo, K.; Belshan, M.; Destache, C.J. Development and evaluation of a thermosensitive vaginal gel containing raltegravir+efavirenz loaded nanoparticles for HIV prophylaxis. Antivir. Res. 2012, 96, 430–436. [Google Scholar] [CrossRef] [PubMed]
- Ho, E.; Chen, Y.; Dash, A.; Sayre, C.; Davies, N.; Gu, K.; Yang, S. Novel intravaginal nanomedicine for the targeted delivery of saquinavir to CD+ immune cells. Int. J. Nanomed. 2013, 8, 2847–2858. [Google Scholar] [CrossRef][Green Version]
- Patel, A.; Patel, J. Mucoadhesive microemulsion based prolonged release vaginal gel for anti-fungal drug. J. Pharm. Tech. Res. 2012, 2. [Google Scholar]
- Patel, A. Development and evaluation of mucoadhesive vaginal tablet of sertaconazole for vaginal candidiasis. Int. J. PharmTech Res. 2011, 3, 2175–2182. [Google Scholar]
- Mumper, R.J.; Bell, M.A.; Worthen, D.R.; Cone, R.A.; Lewis, G.R.; Paull, J.; Moench, T.R. Formulating a sulfonated antiviral dendrimer in a vaginal microbicidal gel having dual mechanisms of action. Drug Dev. Ind. Pharm. 2009, 35, 515–524. [Google Scholar] [CrossRef]
- Hunter, S.K.; Andracki, M.E.; Krieg, A.M. Biodegradable microspheres containing group B streptococcus vaccine: Immune response in mice. Am. J. Obstet. Gynecol. 2001, 185, 1174–1179. [Google Scholar] [CrossRef]
- Mas, N.; Galiana, I.; Hurtado, S.; Mondragón, L.; Bernardos, A.; Sancenón, F.; Murguía, J.R. Enhanced antifungal efficacy of tebuconazole using gated pH-driven mesoporous nanoparticles. Int. J. Nanomed. 2014, 9, 2597–2606. [Google Scholar]
- Cazorla-Luna, R.; Notario-Pérez, F.; Martín-Illana, A.; Bedoya, L.-M.; Tamayo, A.; Rubio, J.; Ruiz-Caro, R.; Veiga, M.-D. Development and in vitro/ ex vivo characterization of vaginal mucoadhesive bilayer films based on ethylcellulose and biopolymers for vaginal sustained release of tenofovir. Biomacromolecules 2020, 21, 2309–2319. [Google Scholar] [CrossRef]
- Meng, J.; Sturgis, T.F.; Youan, B.-B.C. Engineering tenofovir loaded chitosan nanoparticles to maximize microbicide mucoadhesion. Eur. J. Pharm. Sci. 2011, 44, 57–67. [Google Scholar] [CrossRef]
- Meng, J.; Zhang, T.; Agrahari, V.; Ezoulin, M.J.; Youan, B.-B.C. Comparative biophysical properties of tenofovir-loaded, thiolated and nonthiolated chitosan nanoparticles intended for HIV prevention. Nanomedicine 2014, 9, 1595–1612. [Google Scholar] [CrossRef]
- Agrahari, V.; Zhang, C.; Zhang, T.; Li, W.; Gounev, T.K.; Oyler, N.A.; Youan, B.-B.C. Hyaluronidase-sensitive nanoparticle templates for triggered release of HIV/AIDS microbicide in vitro. AAPS J. 2013, 16, 181–193. [Google Scholar] [CrossRef] [PubMed]
- Alukda, D.; Sturgis, T.; Youan, B.C. Formulation of tenofovir-loaded functionalized solid lipid nanoparticles intended for HIV prevention. J. Pharm. Sci. 2011, 100, 3345–3356. [Google Scholar] [CrossRef] [PubMed]
- Clark, M.R.; Peet, M.M.; Davis, S.; Doncel, G.F.; Friend, D.R. Evaluation of rapidly disintegrating vaginal tablets of tenofovir, emtricitabine and their combination for HIV-1 prevention. Pharmaceutics 2014, 6, 616–631. [Google Scholar] [CrossRef] [PubMed]
- Sepúlveda-Crespo, D.; Serramía, M.J.; Sánchez-Rodríguez, J.; Lorente, R.; Gómez, R.; De La Mata, F.J.; Jimenez, J.L.; Muñoz-Fernández, M.Á. Broad-spectrum Anti-HIV-1 activity of anionic carbosilane dendrimers and synergy in combination with maraviroc and tenofovir as topical microbicide. AIDS Res. Hum. Retrovir. 2014, 30, A144. [Google Scholar] [CrossRef]
- Akil, A.; Agashe, H.; Dezzutti, C.S.; Moncla, B.J.; Hillier, S.L.; Devlin, B.; Shi, Y.; Uranker, K.; Rohan, L.C. Formulation and characterization of polymeric films containing combinations of antiretrovirals (ARVs) for HIV prevention. Pharm. Res. 2014, 32, 458–468. [Google Scholar] [CrossRef]
- Zhang, T.; Sturgis, T.F.; Youan, B.B.C. PH-responsive nanoparticles releasing tenofovir intended for the prevention of HIV transmission. Eur. J. Pharm. Biopharm. 2011, 79, 526–536. [Google Scholar] [CrossRef]
- Calvo, N.L.; Svetaz, L.A.; Alvarez, V.A.; Quiroga, A.D.; Lamas, M.C.; Leonardi, D. Chitosan-hydroxypropyl methylcellulose tioconazole films: A promising alternative dosage form for the treatment of vaginal candidiasis. Int. J. Pharm. 2019, 556, 181–191. [Google Scholar] [CrossRef]
- Grammen, C.; Mooter, G.V.D.; Appeltans, B.; Michiels, J.; Crucitti, T.; Ariën, K.K.; Augustyns, K.; Augustijns, P.; Brouwers, J. Development and characterization of a solid dispersion film for the vaginal application of the anti-HIV microbicide UAMC01398. Int. J. Pharm. 2014, 475, 238–244. [Google Scholar] [CrossRef]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).