Photostability Testing of a Third-Generation Retinoid—Tazarotene in the Presence of UV Absorbers
Abstract
1. Introduction
2. Materials and Methods
2.1. Reagents
2.2. Reagent Solutions Preparation
2.3. Photostability Assessments
2.4. In Vitro Cytotoxicity Assays
2.4.1. Investigated Solutions
2.4.2. Cell Lines and Cell Growth Inhibitory Assay
2.5. In Silico Toxicity Prediction
2.6. Ultra-Performance Liquid Chromatography–Tandem Mass Spectrometry Analysis
2.7. Statistical Analysis
3. Results and Discussion
3.1. Method Validation
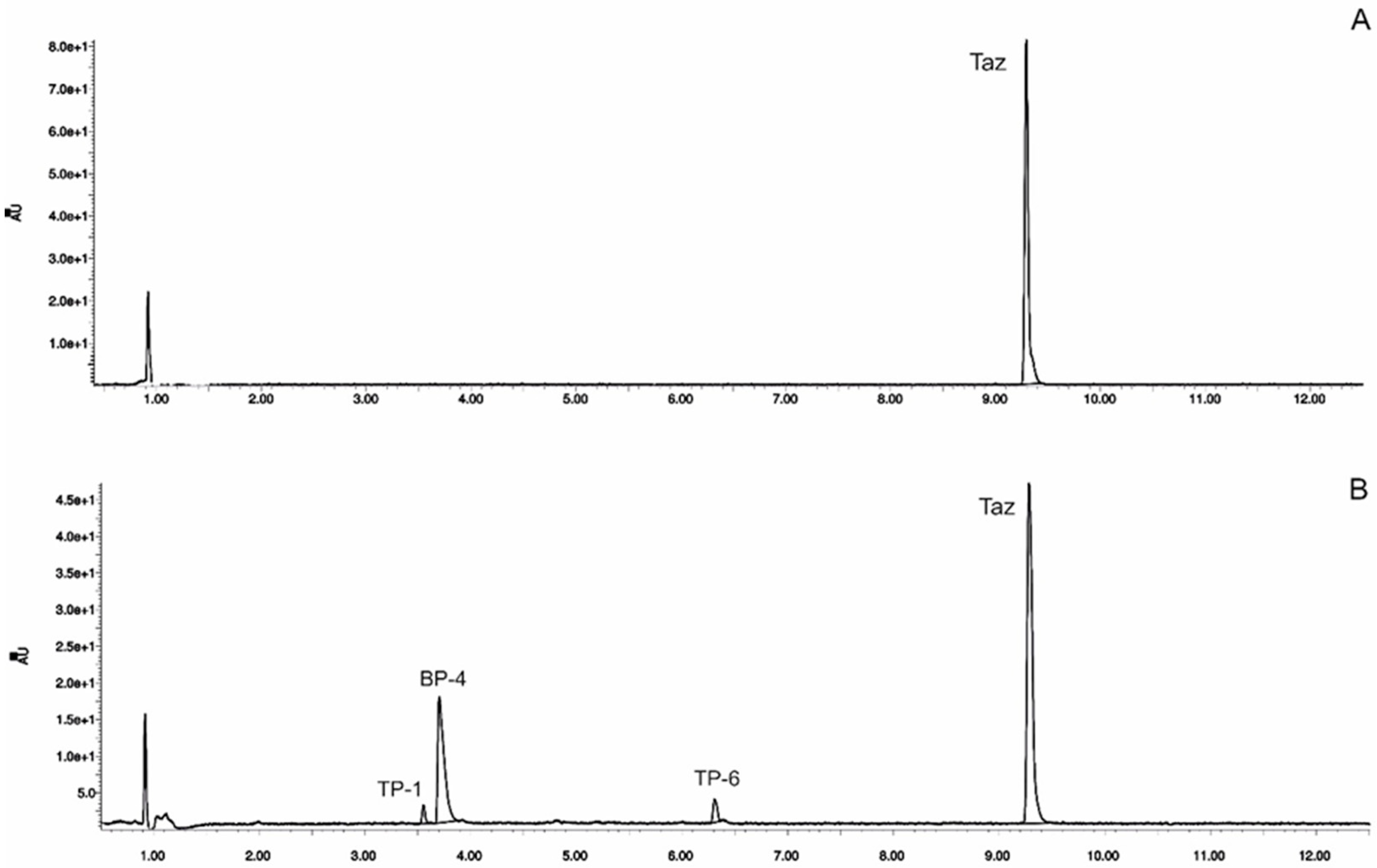
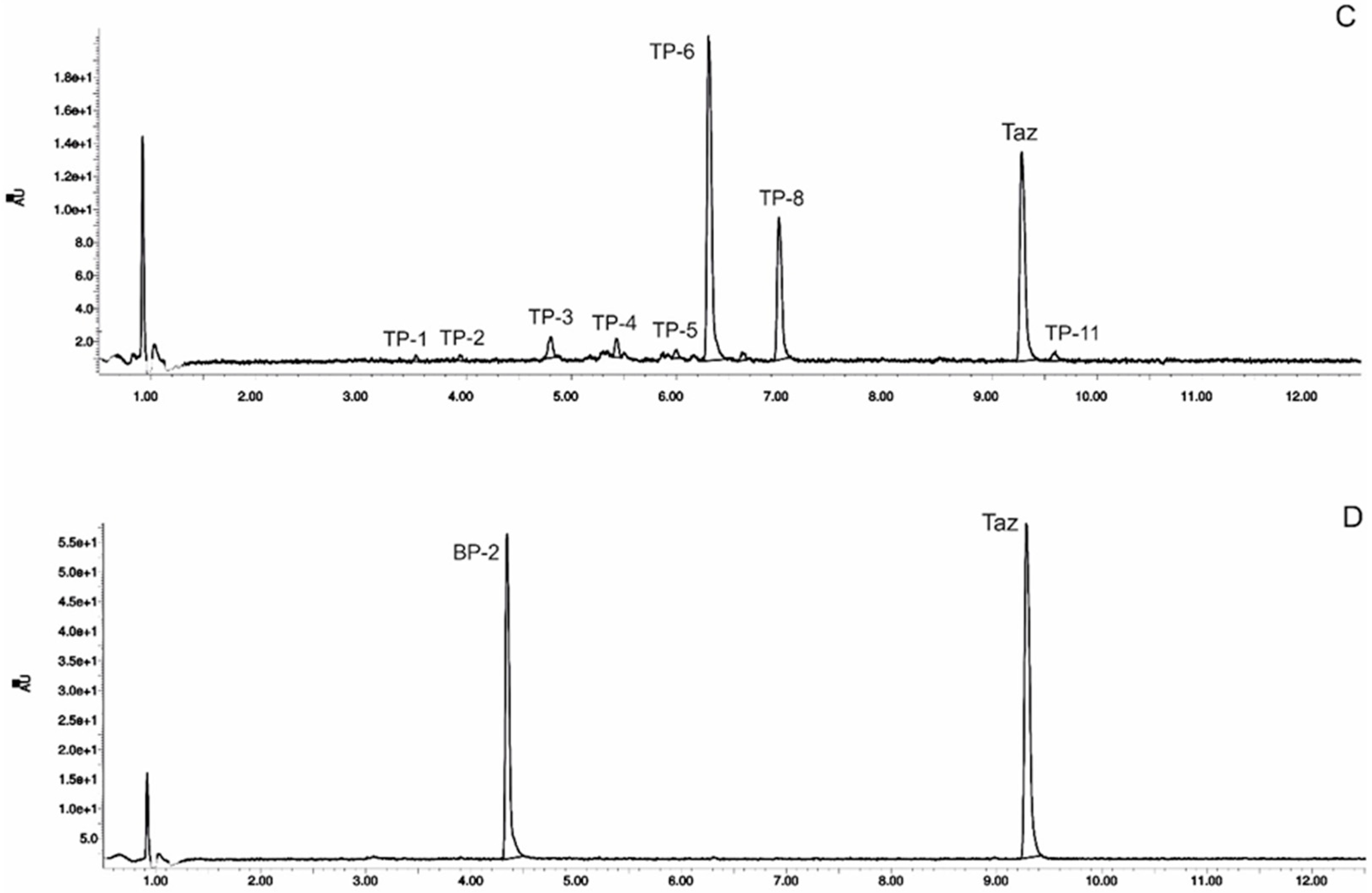
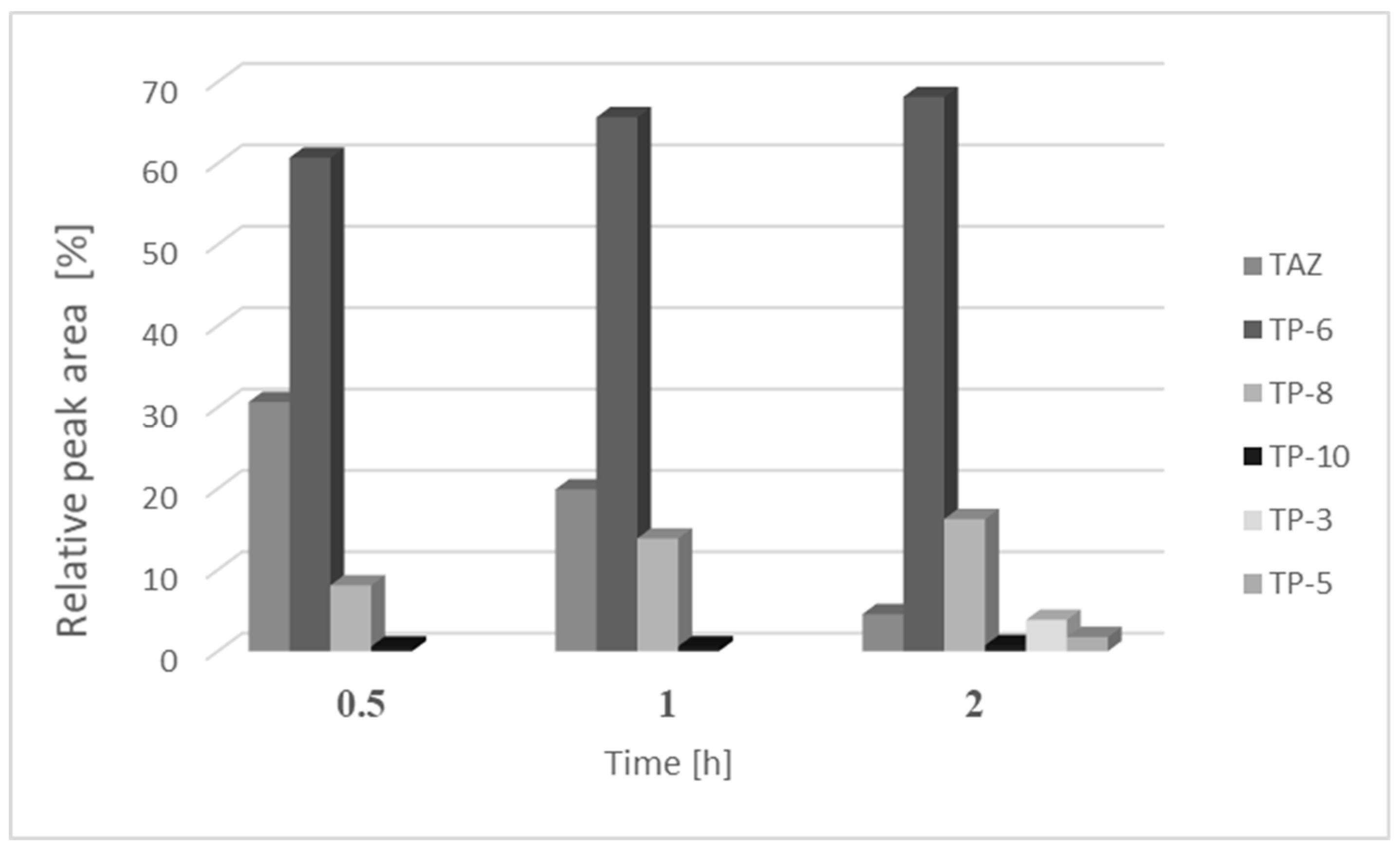
3.2. Identification of Photocatalytic Degradation Products of Tazarotene
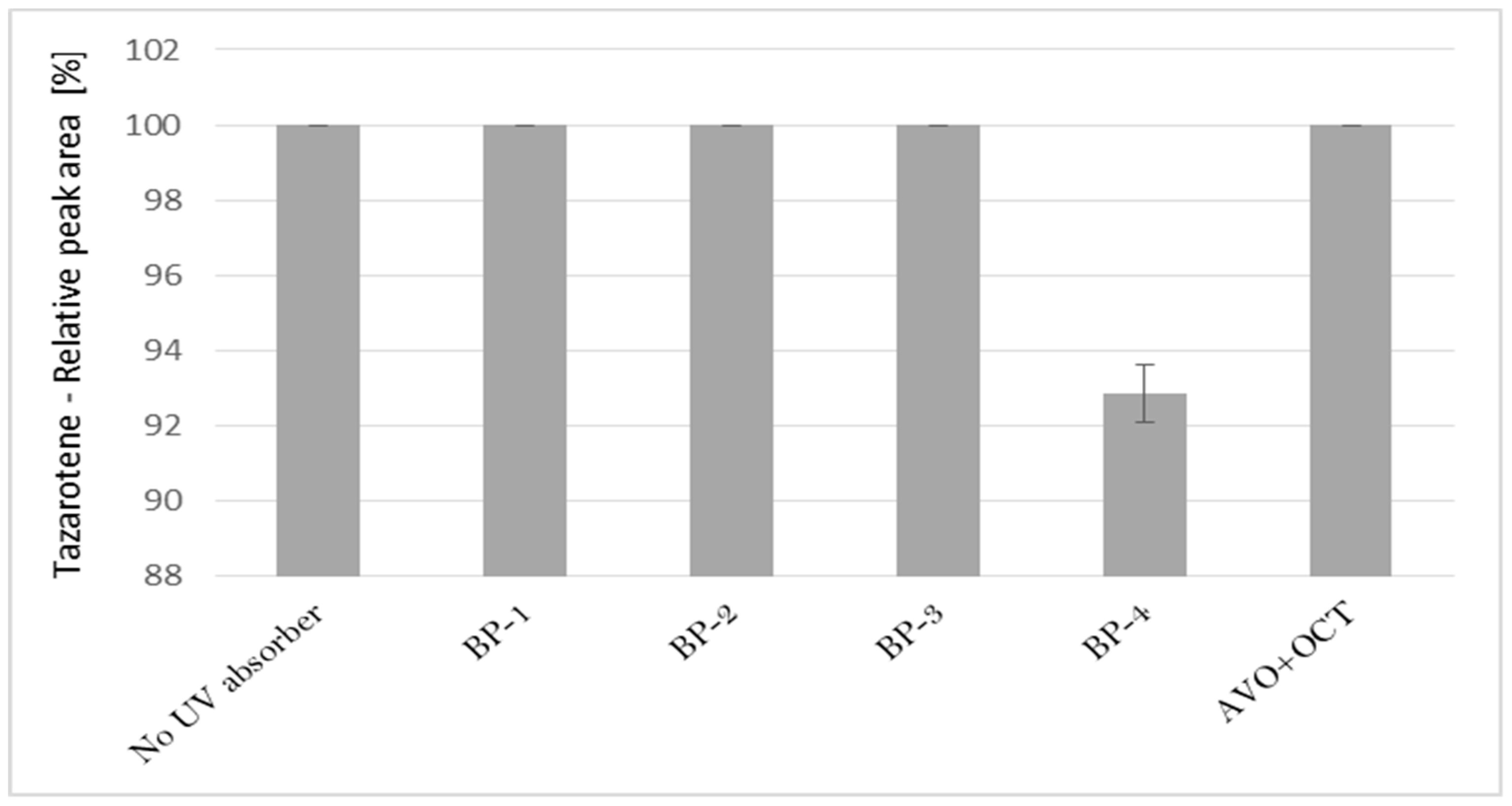
3.3. UV Irradiation of Tazarotene in the Presence of Organic UV Absorbers
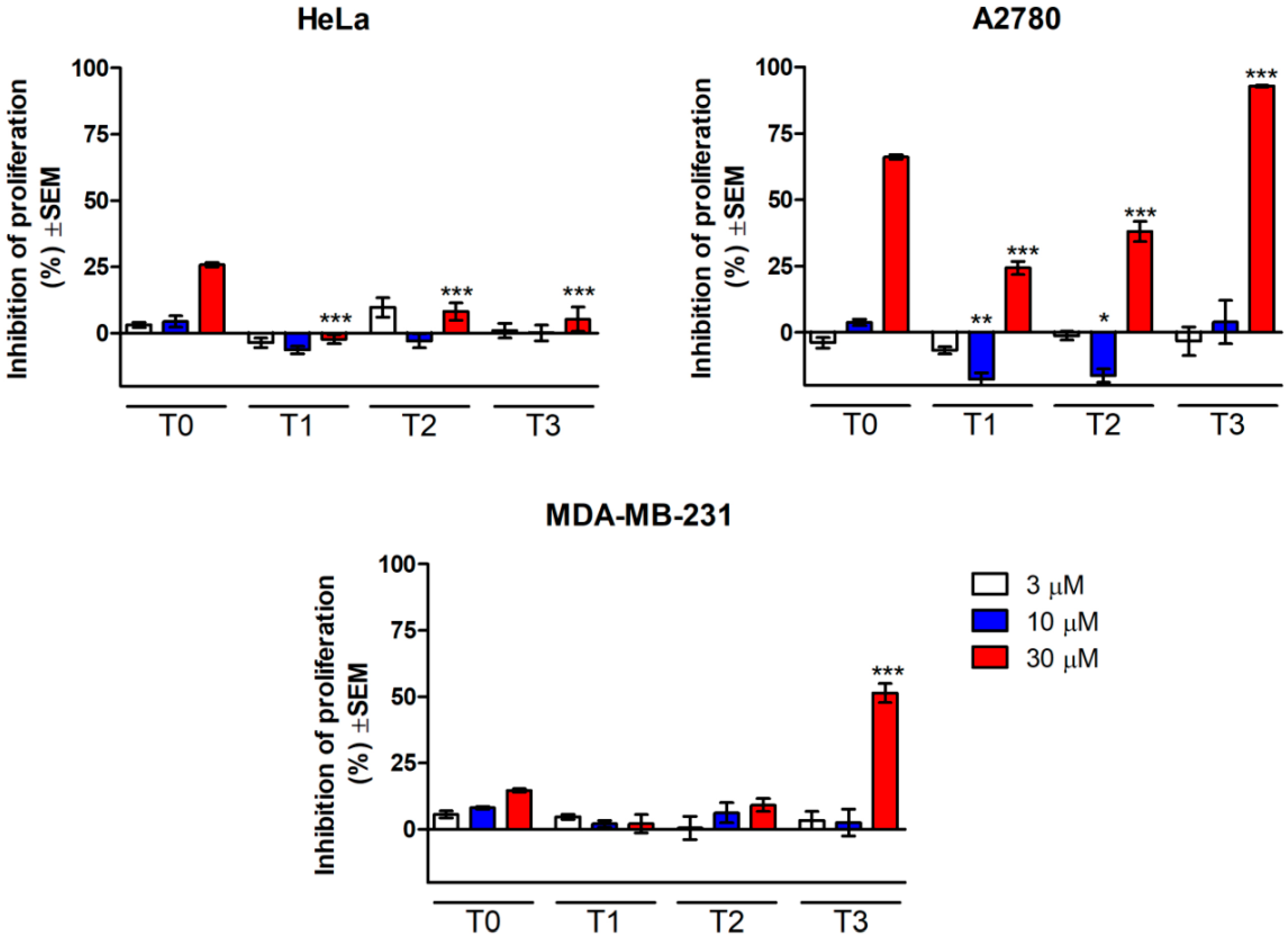
3.4. Cytotoxic Risk Assay
3.5. In Silico Toxicity Predictions
4. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Gregoriou, S.; Kritsotaki, E.; Katoulis, A.; Rigopoulos, D. Use of tazarotene foam for the treatment of acne vulgaris. Clin. Cosmet. Investig. Dermatol. 2014, 7, 165–170. [Google Scholar]
- Talpur, R.; Cox, K.; Duvic, M. Efficacy and safety of topical tazarotene: A review. Expert Opin. Drug Metab. Toxicol. 2009, 5, 195–210. [Google Scholar] [CrossRef]
- Chandraratna, R.A. Tazarotene-first of a new generation of receptor-selective retinoids. Br. J. Dermatol. 1996, 135, 18–25. [Google Scholar] [CrossRef]
- Nagulakonda, N.N.M.; Ananthula, R.S.; Krishnamurthy, T.; Rao, M.R.P.; Rao, G.N. Quantification and In Silico Toxicity Assessment of Tazarotene and its Impurities for a Quality and Safe Drug Product Development. J. Chromatogr. Sci. 2019, 57, 625–635. [Google Scholar] [CrossRef]
- FDA. Tazorac. Available online: https://www.accessdata.fda.gov/drugsatfda_docs/label/2011/020600s008lbl.pdf (accessed on 11 May 2020).
- Yeung, H.; Takeshita, J.; Mehta, N.N.; Kimmel, S.E.; Ogdie, A.; Margolis, D.J.; Shin, D.B.; Attor, R.; Troxel, A.B.; Gelfand, J.M. Psoriasis severity and the prevalence of major medical comorbidity: A population-based study. JAMA Dermatol. 2014, 149, 1173–1179. [Google Scholar] [CrossRef]
- Clinical Pharmacology Andbiopharmaceutics Review(S). 2011. Available online: https://www.accessdata.fda.gov/drugsatfda_docs/nda/2012/202428Orig1s000ClinPharmR.pdf (accessed on 11 May 2020).
- Tang-Liu, D.D.; Matsumoto, R.M.; Usansky, J.I. Clinical pharmacokinetics and drug metabolism of tazarotene: A novel topical treatment for acne and psoriasis. Clin. Pharmacokinet. 1999, 37, 273–287. [Google Scholar] [CrossRef] [PubMed]
- Dayal, S.; Kaura, R.; Sahu, P.; Jain, V.K. Tazarotene gel with narrow-band UVB phototherapy: A synergistic combination in psoriasis. An. Bras. Dermatol. 2018, 93, 385–390. [Google Scholar] [CrossRef]
- Behrens, S.; Grundmann-Kollmann, M.; Schiener, R.; Peter, R.U.; Kerscher, M. Combination phototherapy of psoriasis with narrow-band UVB irradiation and topical tazarotene gel. J. Am. Acad. Dermatol. 2000, 42, 493–495. [Google Scholar] [CrossRef]
- Medical Review(S). 2011. Available online: https://www.accessdata.fda.gov/drugsatfda_docs/nda/2012/202428Orig1s000MedR.pdf (accessed on 11 May 2020).
- Ogden, S.; Samuel, M.; Griffiths, C.E. A review of tazarotene in the treatment of photodamaged skin. Clin. Interv. Aging 2008, 3, 71–76. [Google Scholar] [CrossRef] [PubMed]
- Agbai, O.N.; Buster, K.; Sanchez, M.; Hernandez, C.; Kundu, R.V.; Chiu, M.; Roberts, W.E.; Draelos, Z.D.; Bhushan, R.; Taylor, S.C.; et al. Skin cancer and photoprotection in people of color: A review and recommendations for physicians and the public. J. Am. Acad. Dermatol. 2014, 70, 748–762. [Google Scholar] [CrossRef] [PubMed]
- Baertschi, S.W.; Clapham, D.; Foti, C.; Kleinman, M.H.; Kristensen, S.; Reed, R.A.; Templeton, A.C.; Tønnesen, H.H. Implications of In-Use Photostability: Proposed Guidance for Photostability Testing and Labeling to Support the Administration of Photosensitive Pharmaceutical Products, Part 2: Topical Drug Product. J. Pharm. Sci. 2015, 104, 2688–2701. [Google Scholar] [CrossRef] [PubMed]
- Gaspar, L.R.; Maia Campos, P.M. Evaluation of the photostability of different UV filter combinations in a sunscreen. Int. J. Pharm. 2006, 307, 123–128. [Google Scholar] [CrossRef] [PubMed]
- Kryczyk, A.; Żmudzki, P.; Koczurkiewicz, P.; Piotrowska, J.; Pękala, E.; Hubicka, U. The impact of ZnO and TiO2 on the stability of clotrimazole under UVA irradiation: Identification of photocatalytic degradation products and in vitro cytotoxicity assessment. J. Pharm. Biomed. Anal. 2017, 145, 283–292. [Google Scholar] [CrossRef] [PubMed]
- Tønnesen, H.H. Formulation and stability testing of photolabile drugs. Int. J. Pharm. 2001, 225, 1–14. [Google Scholar] [CrossRef]
- Hecker, D.; Worsley, J.; Yueh, G.; Kuroda, K.; Lebwohl, M. Interactions between tazarotene and ultraviolet light. J. Am. Acad. Dermatol. 1999, 41, 927–930. [Google Scholar] [CrossRef]
- Kryczyk-Poprawa, A.; Żmudzki, P.; Koczurkiewicz, P.; Pękala, E.; Hubicka, U. Photostability of Terbinafine Under UVA Irradiation: The Effect of UV Absorbers. Photochem. Photobiol. 2019, 95, 911–923. [Google Scholar] [CrossRef]
- Q1B Photostability Testing of New Drug Substances and Products. Available online: https://www.ich.org/page/quality-guidelines (accessed on 11 May 2020).
- Kryczyk-Poprawa, A.; Kwiecień, A.; Opoka, W. Photostability of Topical Agents Applied to the Skin: A Review. Pharmaceutics 2019, 12, 10. [Google Scholar] [CrossRef]
- Heurung, A.R.; Raju, S.I.; Warshaw, E.M. Benzophenones. Dermatitis 2014, 25, 3–10. [Google Scholar] [CrossRef]
- Krause, M.; Frederiksen, H.; Sundberg, K.; Jørgensen, F.S.; Jensen, L.N.; Nørgaard, P.; Jørgensen, C.; Ertberg, P.; Juul, A.; Drzewiecki, K.T.; et al. Presence of benzophenones commonly used as UV filters and absorbers in paired maternal and fetal samples. Environ. Int. 2018, 110, 51–60. [Google Scholar] [CrossRef]
- Briasco, B.; Capra, P.; Mannucci, B.; Perugini, P. Stability Study of Sunscreens with Free and Encapsulated UV Filters Contained in Plastic Packaging. Pharmaceutics 2017, 9, 19. [Google Scholar] [CrossRef]
- FDA. Sunscreen Drug Products for over-the-Counter Human Use. Available online: https://www.accessdata.fda.gov/scripts/cdrh/cfdocs/cfcfr/CFRSearch.cfm?CFRPart=352&showFR=1 (accessed on 11 May 2020).
- Muhd Julkapli, N.; Bagheri, S.; Bee Abd Hamid, S. Recent advances in heterogeneous photocatalytic decolorization of synthetic dyes. Sci. World J. 2014, 692307. [Google Scholar] [CrossRef] [PubMed]
- Kryczyk, A.; Żmudzki, P.; Hubicka, U. Determination of itraconazole and its photodegradation products with kinetic evaluation by ultra-performance liquid chromatography/tandem mass spectrometry. Biomed. Chromatogr. 2016, 30, 1733–1743. [Google Scholar] [CrossRef] [PubMed]
- Mosmann, T. Rapid colorimetric assay for cellular growth and survival: Application to proliferation and citotoxicity assays. J. Immunol. Methods 1983, 65, 55–63. [Google Scholar] [CrossRef]
- Osiris Property Explorer. Available online: https://www.organic-chemistry.org/prog/peo/ (accessed on 11 May 2020).
- Roy, C.; Chakrabarty, J. Development and Validation of a Stability-Indicating RP-HPLC Method for the Simultaneous Determination of Phenoxyethanol, Methylparaben, Propylparaben, Mometasone Furoate, and Tazarotene in Topical Pharmaceutical Dosage Formulation. Sci. Pharm. 2013, 81, 951–967. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Singh, D.K.; Sahu, A.; Balhara, A.; Giri, S.; Singh, S. Insights into the degradation chemistry of tazarotene, a third generation acetylenic retinoid: LC-HRMS (Orbitrap), LC-MSn and NMR characterization of its degradation products, and prediction of their physicochemical and ADMET properties. J. Pharm. Biomed. 2020, 185, 113316. [Google Scholar] [CrossRef]
- Roy, C.; Patel, H.B.; Chakrabarty, J. Stability indicating RP-HPLC method development and validation for determination of process related impurities and degradation products of tazarotene in tazarotene topical formulation. Indo Am. J. Pharm. 2013, 3, 1400–1413. [Google Scholar]
- Menter, A. Pharmacokinetics and safety of tazarotene. J. Am. Acad. Dermatol. 2000, 43 Pt 3, S31–S35. [Google Scholar] [CrossRef]
- Yu, Z.; Sefton, J.; Lew-Kaya, D.; Walker, P.; Yu, D.; Tang-Liu, D.D. Pharmacokinetics of tazarotene cream 0.1% after a single dose and after repeat topical applications at clinical or exaggerated application rates in patients with acne vulgaris or photodamaged skin. Clin. Pharmacokinet. 2003, 42, 921–929. [Google Scholar] [CrossRef]
- Madhu, C.; Duff, S.; Baumgarten, V.; Rix, P.; Small, D.; Tang-Liu, D. Metabolic deesterification of tazarotene in human blood and rat and human liver microsomes. J. Pharm. Sci. 1997, 86, 972–974. [Google Scholar] [CrossRef]
| Compound | RT (min) | [M+H+] | Fragmentation Ions | Structure |
|---|---|---|---|---|
| TP-1 | 3.52 | 412.1 | 192.1, 204.1, 310.1, 366.1, 384.1 | 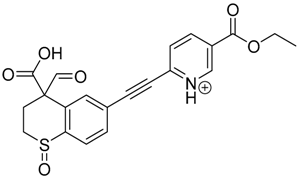 |
| TP-2 | 3.94 | 428.1 | 382.1, 400.1 | 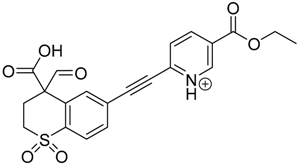 |
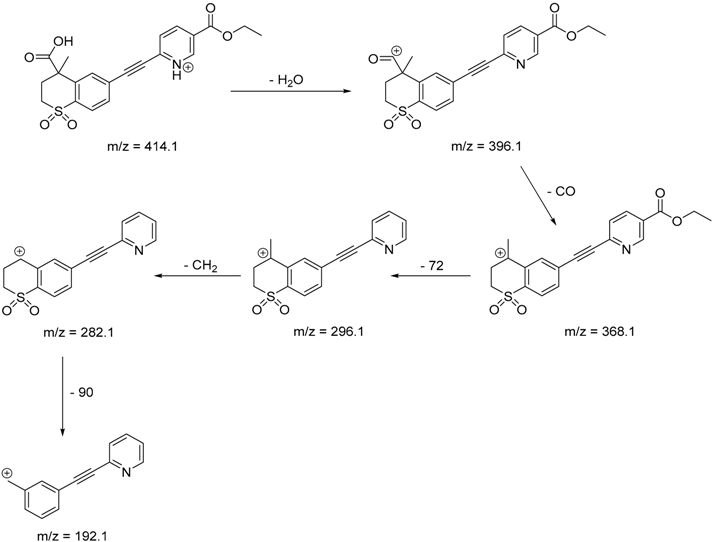
| TP-3 | 4.80 | 414.1 | 192.1, 282.1, 296.1, 368.1, 396.1 | 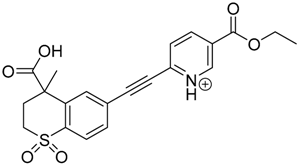 |
| TP-4 | 5.43 | 430.1 | 178.1, 204.1, 294.1, 312.1, 356.1, 384.1 | 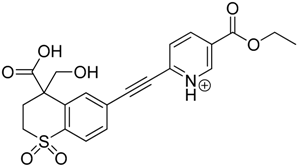 |
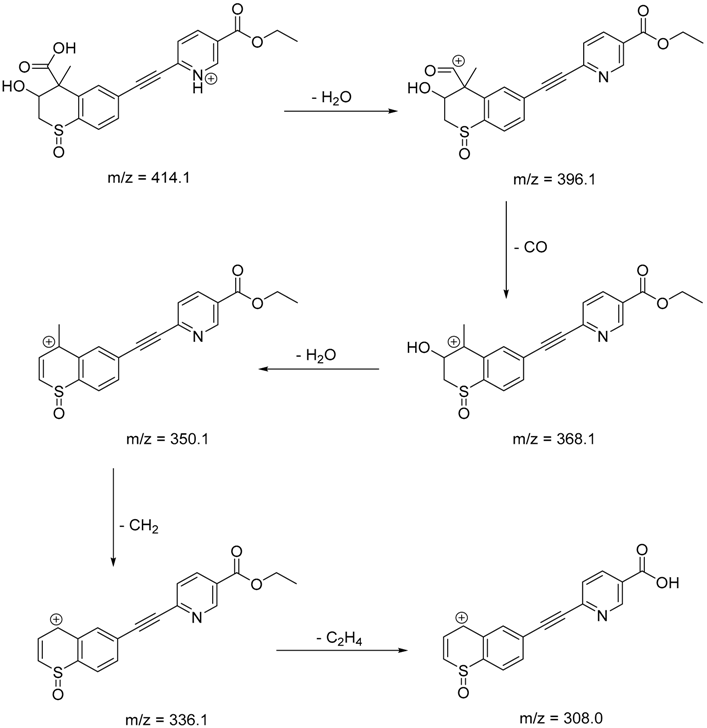
| TP-5 | 6.00 | 414.1 | 308.0, 336.1, 350.1, 368.1, 396.1 |  |
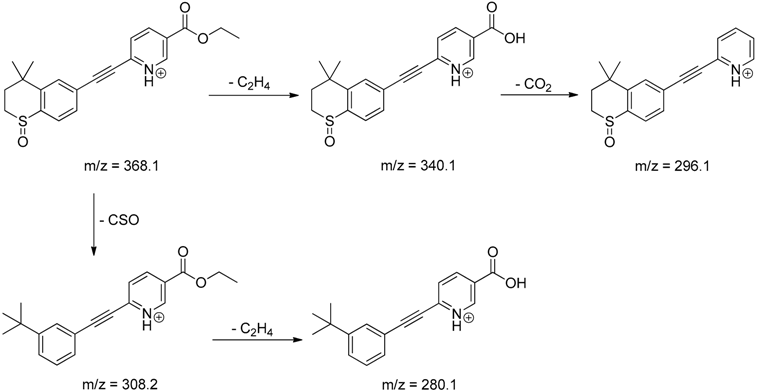
| TP-6 | 6.30 | 368.1 | 280.1, 296.1, 308.2, 340.1 |  |
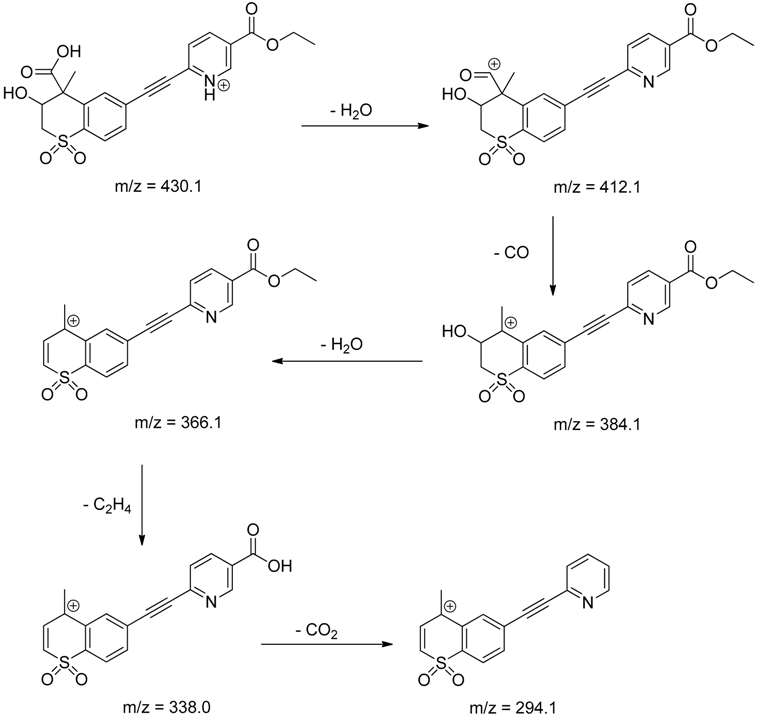
| TP-7 | 6.62 | 430.1 | 294.1, 338.0, 366.1, 384.1, 412.1 | 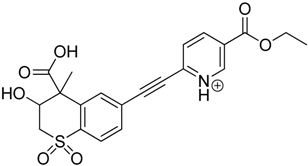 |
| TP-8 | 6.97 | 384.1 | 356.1 | 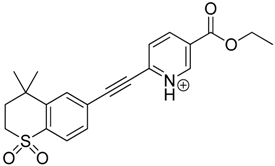 |
| TP-9 | 7.47 | 368.1 | 262.1, 280.1, 269.1, 340.1 |  |
| TP-10 | 8.49 | 366.1 | 252.1, 280.1, 294.1, 338.1 | 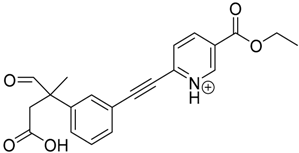 |
| Tazarotene | 9.28 | 352.1 | 222.1, 266.1, 294.1, 308.2, 324.1 | 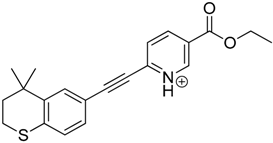 |
| TP-11 | 9.60 | 280.1 | 136.1, 156.1, 236.1 | 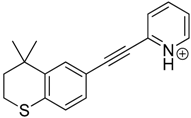 |
| Tazarotene |
|---|
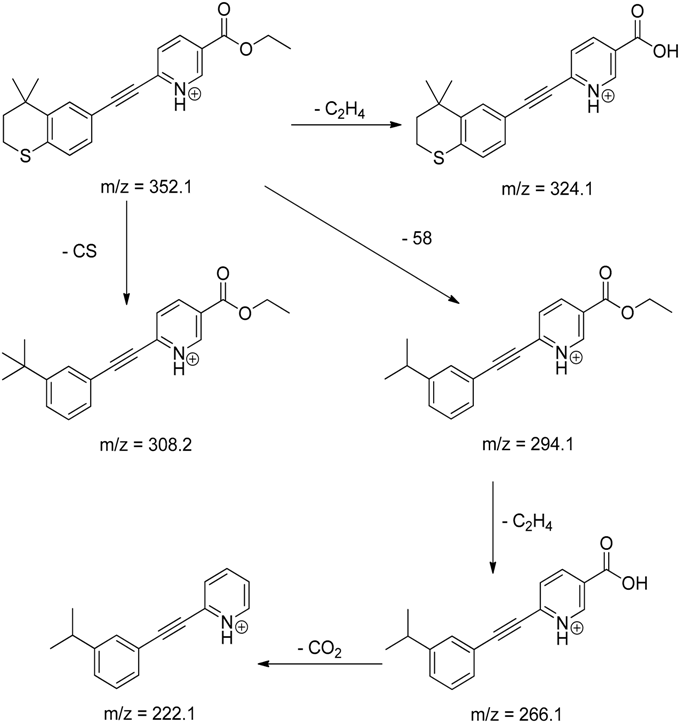 |
| TP-1 |
 |
| TP-2 |
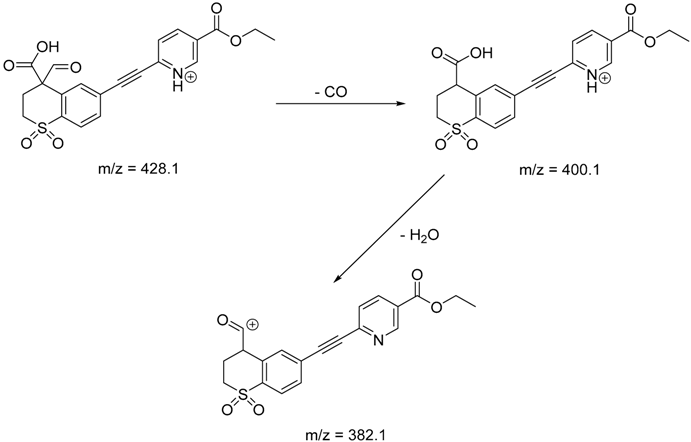 |
| TP-3 |
 |
| TP-4 |
 |
| TP-5 |
 |
| TP-6 |
 |
| TP-7 |
 |
| TP-8 |
 |
| TP-9 |
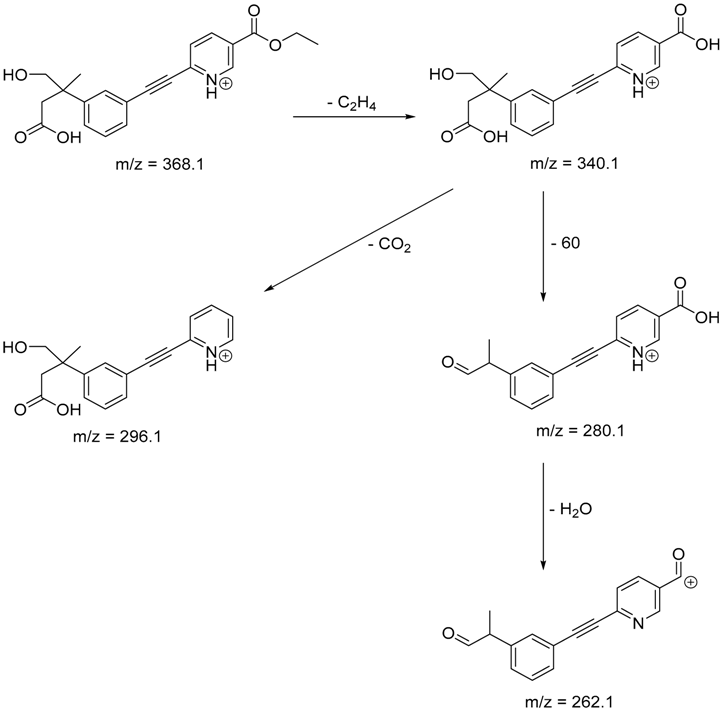 |
| TP-10 |
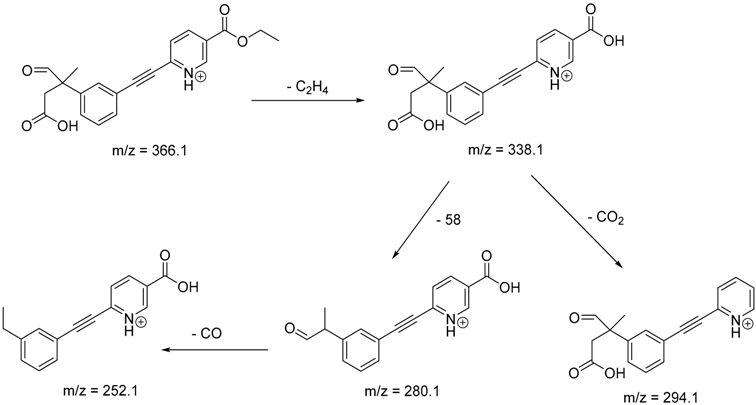 |
| TP-11 |
 |
| Compound | Mutagenic | Tumorigenic | Irritant | Reproductive Effective |
|---|---|---|---|---|
| Tazarotene | - | - | - | - |
| TP-1 | - | - | - | - |
| TP-2 | - | - | - | +/− |
| TP-3 | - | - | - | +/− |
| TP-4 | - | - | - | +/− |
| TP-5 | - | - | - | - |
| TP-6 | - | - | - | - |
| TP-7 | - | - | - | +/− |
| TP-8 | - | - | - | +/− |
| TP-9 | - | - | - | - |
| TP-10 | - | - | +/− | - |
| TP-11 | - | - | - | - |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Kryczyk-Poprawa, A.; Zupkó, I.; Bérdi, P.; Żmudzki, P.; Popiół, J.; Muszyńska, B.; Opoka, W. Photostability Testing of a Third-Generation Retinoid—Tazarotene in the Presence of UV Absorbers. Pharmaceutics 2020, 12, 899. https://doi.org/10.3390/pharmaceutics12090899
Kryczyk-Poprawa A, Zupkó I, Bérdi P, Żmudzki P, Popiół J, Muszyńska B, Opoka W. Photostability Testing of a Third-Generation Retinoid—Tazarotene in the Presence of UV Absorbers. Pharmaceutics. 2020; 12(9):899. https://doi.org/10.3390/pharmaceutics12090899
Chicago/Turabian StyleKryczyk-Poprawa, Agata, István Zupkó, Péter Bérdi, Paweł Żmudzki, Justyna Popiół, Bożena Muszyńska, and Włodzimierz Opoka. 2020. "Photostability Testing of a Third-Generation Retinoid—Tazarotene in the Presence of UV Absorbers" Pharmaceutics 12, no. 9: 899. https://doi.org/10.3390/pharmaceutics12090899
APA StyleKryczyk-Poprawa, A., Zupkó, I., Bérdi, P., Żmudzki, P., Popiół, J., Muszyńska, B., & Opoka, W. (2020). Photostability Testing of a Third-Generation Retinoid—Tazarotene in the Presence of UV Absorbers. Pharmaceutics, 12(9), 899. https://doi.org/10.3390/pharmaceutics12090899






