In Vitro Evaluation of Eudragit Matrices for Oral Delivery of BCG Vaccine to Animals
Abstract
1. Introduction
2. Materials and Methods
2.1. Materials
2.2. Preparation of BCG-Loaded Eudragit® Matrices
2.3. BCG Viability during Matrix Formulation
2.4. BCG Viability Following Matrix Incubation in SGF and SIF
2.5. Statistical Analysis
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- World Health Organization. Global Tuberculosis Report 2018; World Health Organization: Geneva, Switzerland, 2018. [Google Scholar]
- Waters, W.R.; Palmer, M.V.; Buddle, B.M.; Vordermeier, H.M. Bovine tuberculosis vaccine research: Historical perspectives and recent advances. Vaccine 2012, 30, 2611–2622. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. Roadmap for Zoonotic Tuberculosis; World Health Organization: Geneva, Switzerland, 2017. [Google Scholar]
- Buddle, B.M.; Vordermeier, H.M.; Chambers, M.A.; de Klerk-Lorist, L.M. Efficacy and Safety of BCG Vaccine for Control of Tuberculosis in Domestic Livestock and Wildlife. Front. Vet. Sci. 2018, 5, 259. [Google Scholar] [CrossRef] [PubMed]
- Gowtage, S.; Williams, G.A.; Henderson, R.; Aylett, P.; MacMorran, D.; Palmer, S.; Robertson, A.; Lesellier, S.; Carter, S.P.; Chambers, M.A. Testing of a palatable bait and compatible vaccine carrier for the oral vaccination of European badgers (Meles meles) against tuberculosis. Vaccine 2017, 35, 987–992. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Coutant, T.; Vergneau-Grosset, C.; Langlois, I. Overview of Drug Delivery Methods in Exotics, Including Their Anatomic and Physiologic Considerations. Vet. Clin. N. Am. Exot. Anim. Pract. 2018, 21, 215–259. [Google Scholar] [CrossRef] [PubMed]
- Boyd, B.J. Past and future evolution in colloidal drug delivery systems. Expert Opin. Drug Deliv. 2008, 5, 69–85. [Google Scholar] [CrossRef]
- Li, P.; Nielsen, H.M.; Mullertz, A. Oral delivery of peptides and proteins using lipid-based drug delivery systems. Expert Opin. Drug Deliv. 2012, 9, 1289–1304. [Google Scholar] [CrossRef]
- Aburahma, M.H. Bile salts-containing vesicles: Promising pharmaceutical carriers for oral delivery of poorly water-soluble drugs and peptide/protein-based therapeutics or vaccines. Drug Deliv. 2016, 23, 1847–1867. [Google Scholar] [CrossRef]
- Kremer, L.; Dupre, L.; Riveau, G.; Capron, A.; Locht, C. Systemic and mucosal immune responses after intranasal administration of recombinant Mycobacterium bovis bacillus Calmette-Guerin expressing glutathione S-transferase from Schistosoma haematobium. Infect. Immun. 1998, 66, 5669–5676. [Google Scholar]
- Monteiro-Maia, R.; Ortigao-de-Sampaio, M.B.; Pinho, R.T.; Castello-Branco, L.R. Modulation of humoral immune response to oral BCG vaccination by Mycobacterium bovis BCG Moreau Rio de Janeiro (RDJ) in healthy adults. J. Immune Based Ther. Vaccines 2006, 4, 4. [Google Scholar] [CrossRef]
- Cosgrove, C.A.; Castello-Branco, L.R.; Hussell, T.; Sexton, A.; Giemza, R.; Phillips, R.; Williams, A.; Griffin, G.E.; Dougan, G.; Lewis, D.J. Boosting of cellular immunity against Mycobacterium tuberculosis and modulation of skin cytokine responses in healthy human volunteers by Mycobacterium bovis BCG substrain Moreau Rio de Janeiro oral vaccine. Infect. Immun. 2006, 74, 2449–2452. [Google Scholar] [CrossRef]
- Skinner, M.A.; Keen, D.L.; Parlane, N.A.; Hamel, K.L.; Yates, G.F.; Buddle, B.M. Improving protective efficacy of BCG vaccination for wildlife against bovine tuberculosis. Res. Vet. Sci. 2005, 78, 231–236. [Google Scholar] [CrossRef]
- Buddle, B.M.; Aldwell, F.E.; Keen, D.L.; Parlane, N.A.; Yates, G.; de Lisle, G.W. Intraduodenal vaccination of brushtail possums with bacille Calmette-Guerin enhances immune responses and protection against Mycobacterium bovis infection. Int. J. Tuberc. Lung Dis. 1997, 1, 377–383. [Google Scholar]
- Dobakhti, F.; Rahimi, F.; Dehpour, A.R.; Taghikhani, M.; Ajdary, S.; Rafiei, S.; Rafiee-Tehrani, M. Stabilizing effects of calcium alginate microspheres on Mycobacterium bovis BCG intended for oral vaccination. J. Microencapsul. 2006, 23, 844–854. [Google Scholar] [CrossRef]
- Gormley, E.; Ni Bhuachalla, D.; O’Keeffe, J.; Murphy, D.; Aldwell, F.E.; Fitzsimons, T.; Stanley, P.; Tratalos, J.A.; McGrath, G.; Fogarty, N.; et al. Oral Vaccination of Free-Living Badgers (Meles meles) with Bacille Calmette Guerin (BCG) Vaccine Confers Protection against Tuberculosis. PLoS ONE 2017, 12, e0168851. [Google Scholar] [CrossRef]
- Nol, P.; Lyashchenko, K.P.; Greenwald, R.; Esfandiari, J.; Waters, W.R.; Palmer, M.V.; Nonnecke, B.J.; Keefe, T.J.; Thacker, T.C.; Rhyan, J.C.; et al. Humoral immune responses of white-tailed deer (Odocoileus virginianus) to Mycobacterium bovis BCG vaccination and experimental challenge with M. bovis. Clin. Vaccine Immunol. 2009, 16, 323–329. [Google Scholar] [CrossRef]
- Nugent, G.; Yockney, I.J.; Whitford, E.J.; Cross, M.L.; Aldwell, F.E.; Buddle, B.M. Field Trial of an Aerially-Distributed Tuberculosis Vaccine in a Low-Density Wildlife Population of Brushtail Possums (Trichosurus vulpecula). PLoS ONE 2016, 11, e0167144. [Google Scholar] [CrossRef]
- Gou, J.; Liang, Y.; Miao, L.; Chao, Y.; Zhang, Y.; Yin, T.; He, H.; Tang, X. The promoting effect of enteric materials on the oral absorption of larotaxel-loaded polymer-lipid hybrid nanoparticles. Eur. J. Pharm. Sci. 2018, 124, 288–294. [Google Scholar] [CrossRef]
- Oshi, M.A.; Naeem, M.; Bae, J.; Kim, J.; Lee, J.; Hasan, N.; Kim, W.; Im, E.; Jung, Y.; Yoo, J.W. Colon-targeted dexamethasone microcrystals with pH-sensitive chitosan/alginate/Eudragit S multilayers for the treatment of inflammatory bowel disease. Carbohydr. Polym. 2018, 198, 434–442. [Google Scholar] [CrossRef]
- Longet, S.; Aversa, V.; O’Donnell, D.; Tobias, J.; Rosa, M.; Holmgren, J.; Coulter, I.S.; Lavelle, E.C. Thermostability of the coating, antigen and immunostimulator in an adjuvanted oral capsule vaccine formulation. Int. J. Pharm. 2017, 534, 60–70. [Google Scholar] [CrossRef]
- Srivastava, A.; Gowda, D.V.; Madhunapantula, S.V.; Siddaramaiah. Development and Efficacy Assessment of an Enteric Coated Porous Tablet Loaded With F4 Fimbriae for Oral Vaccination of Piglets against F4+ Escherichia coli Infections. Curr. Drug Deliv. 2016, 13, 121–130. [Google Scholar] [CrossRef]
- Stadler, M.; Viernstein, H. Optimization of a formulation containing viable lactic acid bacteria. Int. J. Pharm. 2003, 256, 117–122. [Google Scholar] [CrossRef]
- Huyghebaert, N.; Vermeire, A.; Neirynck, S.; Steidler, L.; Remaut, E.; Remon, J.P. Development of an enteric-coated formulation containing freeze-dried, viable recombinant Lactococcus lactis for the ileal mucosal delivery of human interleukin-10. Eur. J. Pharm. Biopharm. 2005, 60, 349–359. [Google Scholar] [CrossRef]
- Levine, M.M.; Ferreccio, C.; Abrego, P.; Martin, O.S.; Ortiz, E.; Cryz, S. Duration of efficacy of Ty21a, attenuated Salmonella typhi live oral vaccine. Vaccine 1999, 17 (Suppl. 2), S22–S27. [Google Scholar] [CrossRef]
- de Barros, J.M.S.; Scherer, T.; Charalampopoulos, D.; Khutoryanskiy, V.V.; Edwards, A.D. A laminated polymer film formulation for enteric delivery of live vaccine and probiotic bacteria. J. Pharm. Sci. 2014, 103, 2022–2032. [Google Scholar] [CrossRef]
- Ratliff, T.L.; Ritchey, J.K.; Brandhorst, J.; Hanna, M.G., Jr. Time-dependent aggregation of reconstituted BCG vaccine. J. Urol. 1994, 152, 2147–2150. [Google Scholar] [CrossRef]
- Gheorghiu, M.; Lagranderie, M.; Balazuc, A.M. Stabilisation of BCG vaccines. Dev. Biol. Stand. 1996, 87, 251–261. [Google Scholar]
- Gheorghiu, M.; Lagrange, P.H.; Fillastre, C. The stability and immunogenicity of a dispersed-grown freeze-dried Pasteur BCG vaccine. J. Biol. Stand. 1988, 16, 15–26. [Google Scholar] [CrossRef]
- Groves, M.J. BCG: The Past, Present and Future of a Tuberculosis Vaccine. J. Pharm. Pharmacol. 1997, 49 (Suppl. 1), 7–15. [Google Scholar] [CrossRef]
- Rezwan, M.; Laneelle, M.A.; Sander, P.; Daffe, M. Breaking down the wall: Fractionation of mycobacteria. J. Microbiol. Methods 2007, 68, 32–39. [Google Scholar] [CrossRef]
- Jin, T.H.; Nguyen, L.; Qu, T.; Tsao, E. Improved formulation and lyophilization cycle for rBCG vaccine. Vaccine 2011, 29, 4848–4852. [Google Scholar] [CrossRef]
- Ohtake, S.; Wang, Y.J. Trehalose: Current use and future applications. J. Pharm. Sci. 2011, 100, 2020–2053. [Google Scholar] [CrossRef]


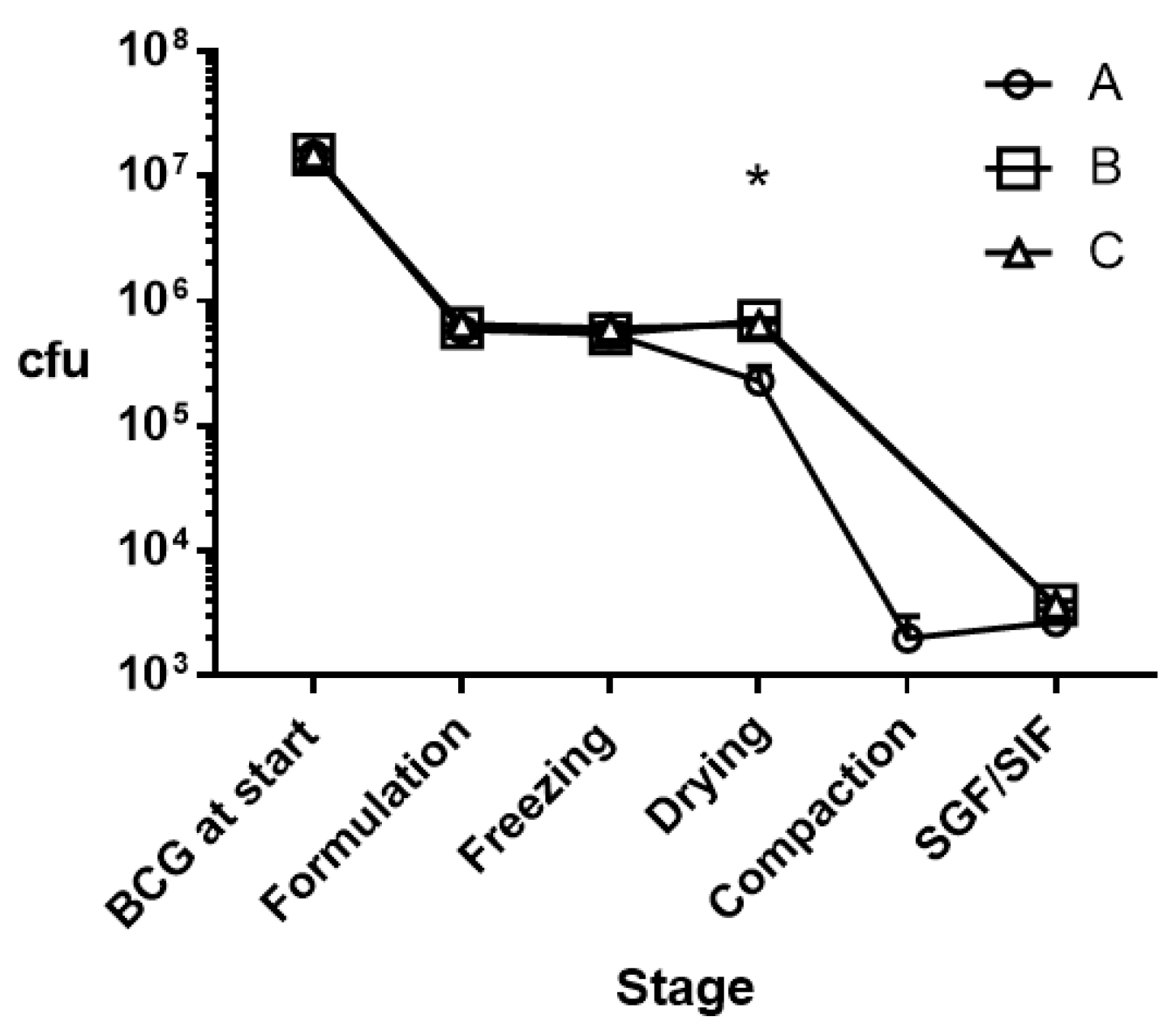
| Matrix 1 | Suspension (pH 7) | Freezing (−20 °C/6 h) | Freeze Drying (24 h) | Dry Powder Compaction | Matrix Exposure to SGF and SIF |
|---|---|---|---|---|---|
| A | 5.9 ± 0.4 × 105 | 5.5 ± 0.4 × 105 | 2.3 ± 0.7 × 105 | 2.0 ± 1.0 × 103 | 2.7 ± 0.1 × 103 |
| B | 6.1 ± 0.4 × 105 | 5.5 ± 1.1 × 105 | 7.0 ± 0.2 × 105 * | ND | 3.7 ± 0.3 × 103 |
| C | 6.5 ± 0.5 × 105 | 6.1 ± 0.5 × 105 | 6.5 ± 0.3 × 105 * | ND | 3.7 ± 0.2 × 103 |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Saleem, I.; Coombes, A.G.A.; Chambers, M.A. In Vitro Evaluation of Eudragit Matrices for Oral Delivery of BCG Vaccine to Animals. Pharmaceutics 2019, 11, 270. https://doi.org/10.3390/pharmaceutics11060270
Saleem I, Coombes AGA, Chambers MA. In Vitro Evaluation of Eudragit Matrices for Oral Delivery of BCG Vaccine to Animals. Pharmaceutics. 2019; 11(6):270. https://doi.org/10.3390/pharmaceutics11060270
Chicago/Turabian StyleSaleem, Imran, Allan G. A. Coombes, and Mark A. Chambers. 2019. "In Vitro Evaluation of Eudragit Matrices for Oral Delivery of BCG Vaccine to Animals" Pharmaceutics 11, no. 6: 270. https://doi.org/10.3390/pharmaceutics11060270
APA StyleSaleem, I., Coombes, A. G. A., & Chambers, M. A. (2019). In Vitro Evaluation of Eudragit Matrices for Oral Delivery of BCG Vaccine to Animals. Pharmaceutics, 11(6), 270. https://doi.org/10.3390/pharmaceutics11060270







