Pharmacodynamics and Pharmacokinetics of a New Type of Compound Lansoprazole Capsule in Gastric Ulcer Rats and Beagle Dogs: Importance of Adjusting Oxidative Stress and Inflammation
Abstract
:1. Introduction
2. Materials and Methods
2.1. Chemicals and Materials
2.2. Pharmacodynamic Study in Rats
2.2.1. Animals
2.2.2. Glacial Acetic-Acid-Induced Gastric Ulcer Model
2.2.3. Macroscopic Gastric Ulcer Assay
2.2.4. Histopathological Observation
2.2.5. Immunohistochemistry Evaluation for VEGF and COX-2
2.2.6. Western Blotting Determination for VEGF and COX-2
2.2.7. Measurement of SOD, MDA and H+-K+-ATP Enzymes Activity Levels
2.3. Pharmacokinetic Study in Dogs
2.3.1. Animals
2.3.2. Instruments
2.3.3. Solution Preparation
2.3.4. Sample Preparation
2.3.5. Method Validation
2.3.6. Method Application
2.4. Data Analysis and Statistics
3. Results
3.1. Pharmacodynamic Studies in Rats
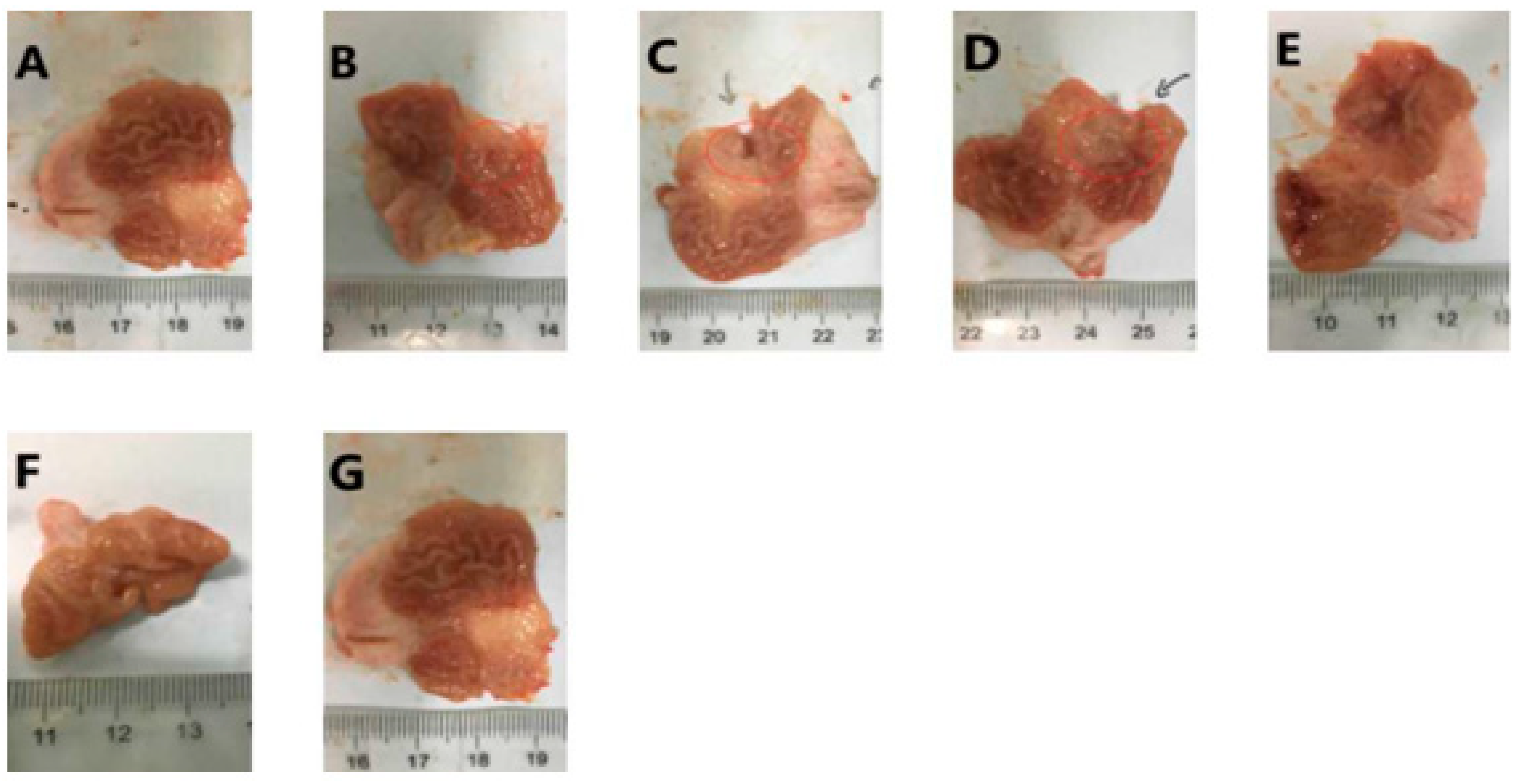
3.1.1. Macroscopic Evaluation of Compound LSZ Capsule against Glacial Acetic-Acid-Induced Gastric Ulcer
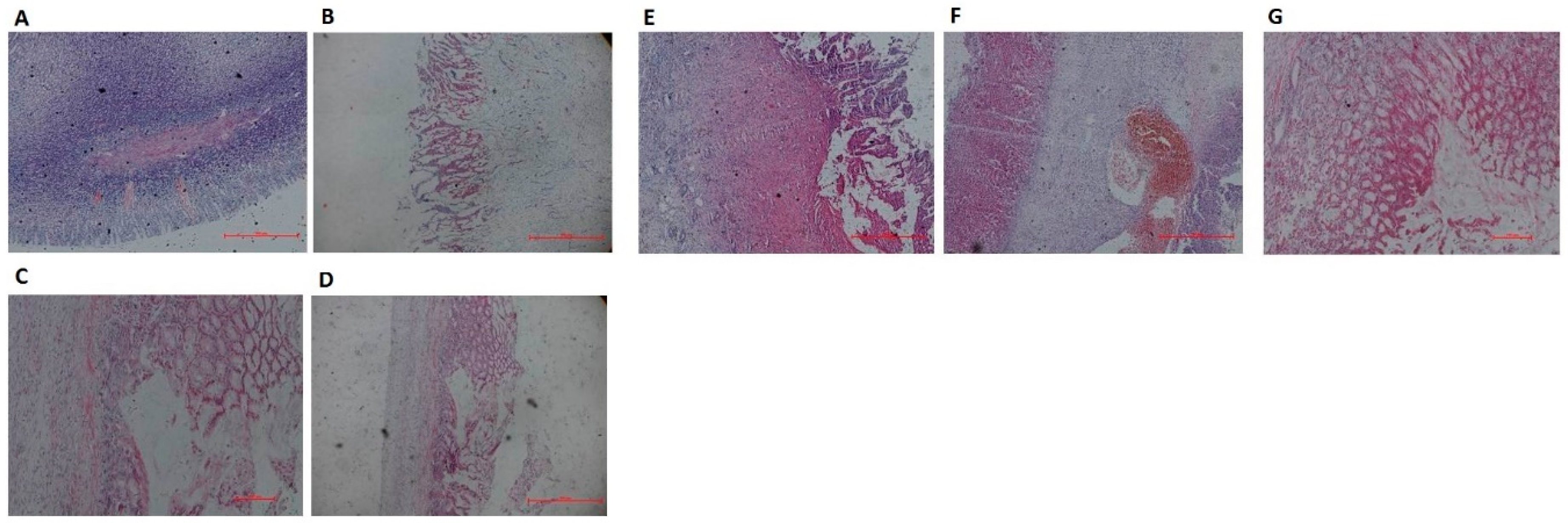
3.1.2. Histological Evaluation of Compound LSZ Capsule against Glacial Acetic-Acid-Induced Gastric Ulcer
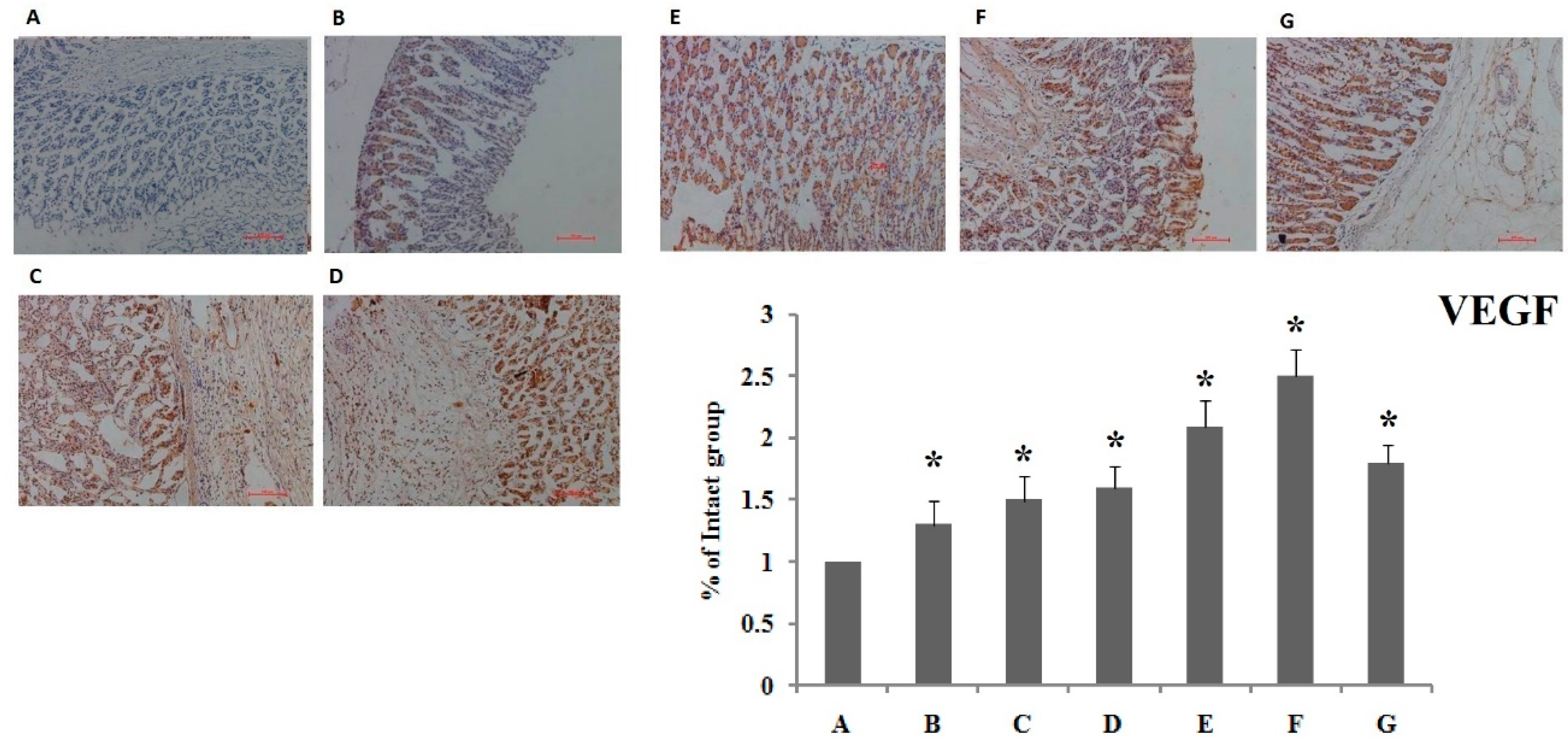
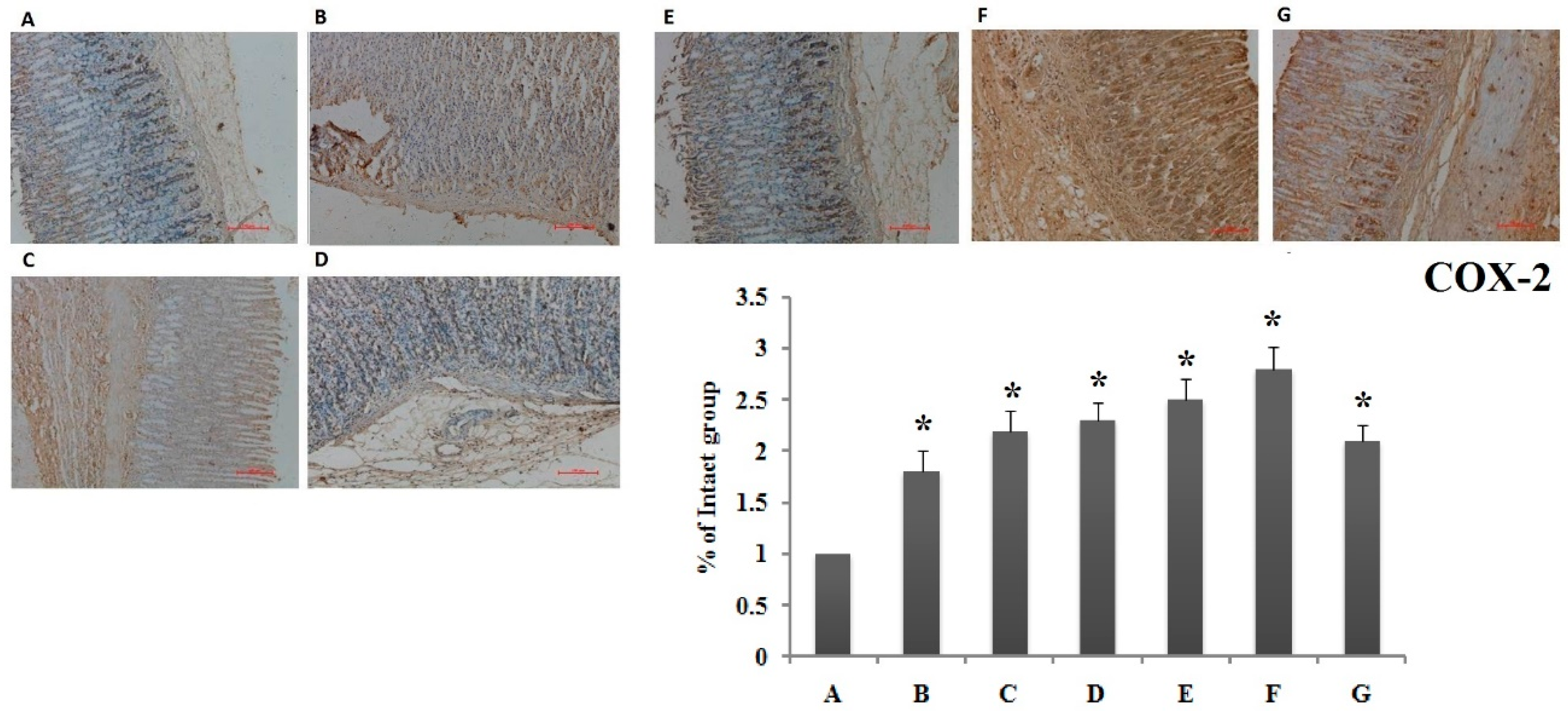
3.1.3. Immunohistochemistry Evaluation for VEGF and COX-2
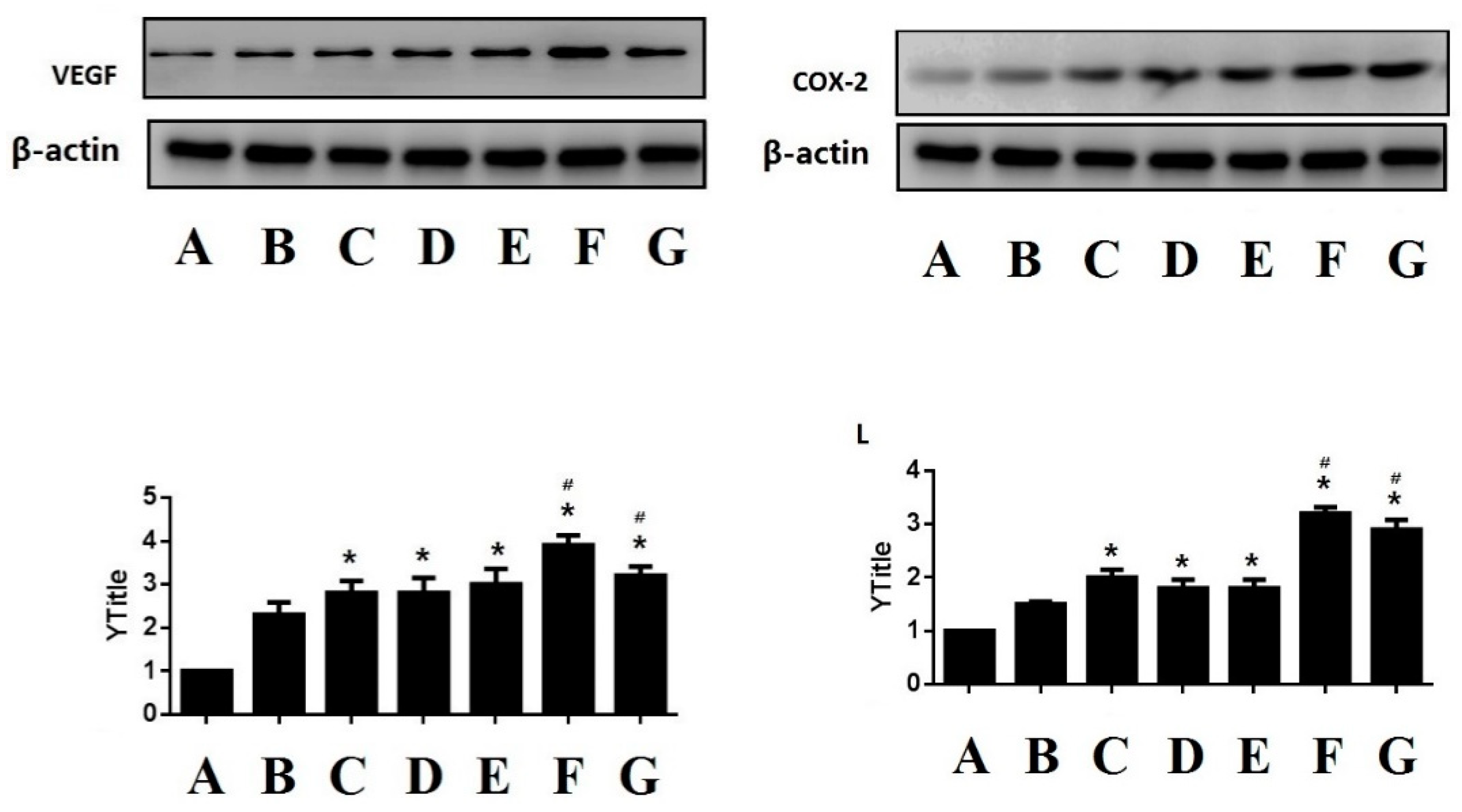
3.1.4. Western Blotting Determination for VEGF and COX-2
3.1.5. Measurement of SOD, MDA and H+-K+-ATP Enzymes Activity Levels
3.2. Pharmacokinetic Study in Dogs
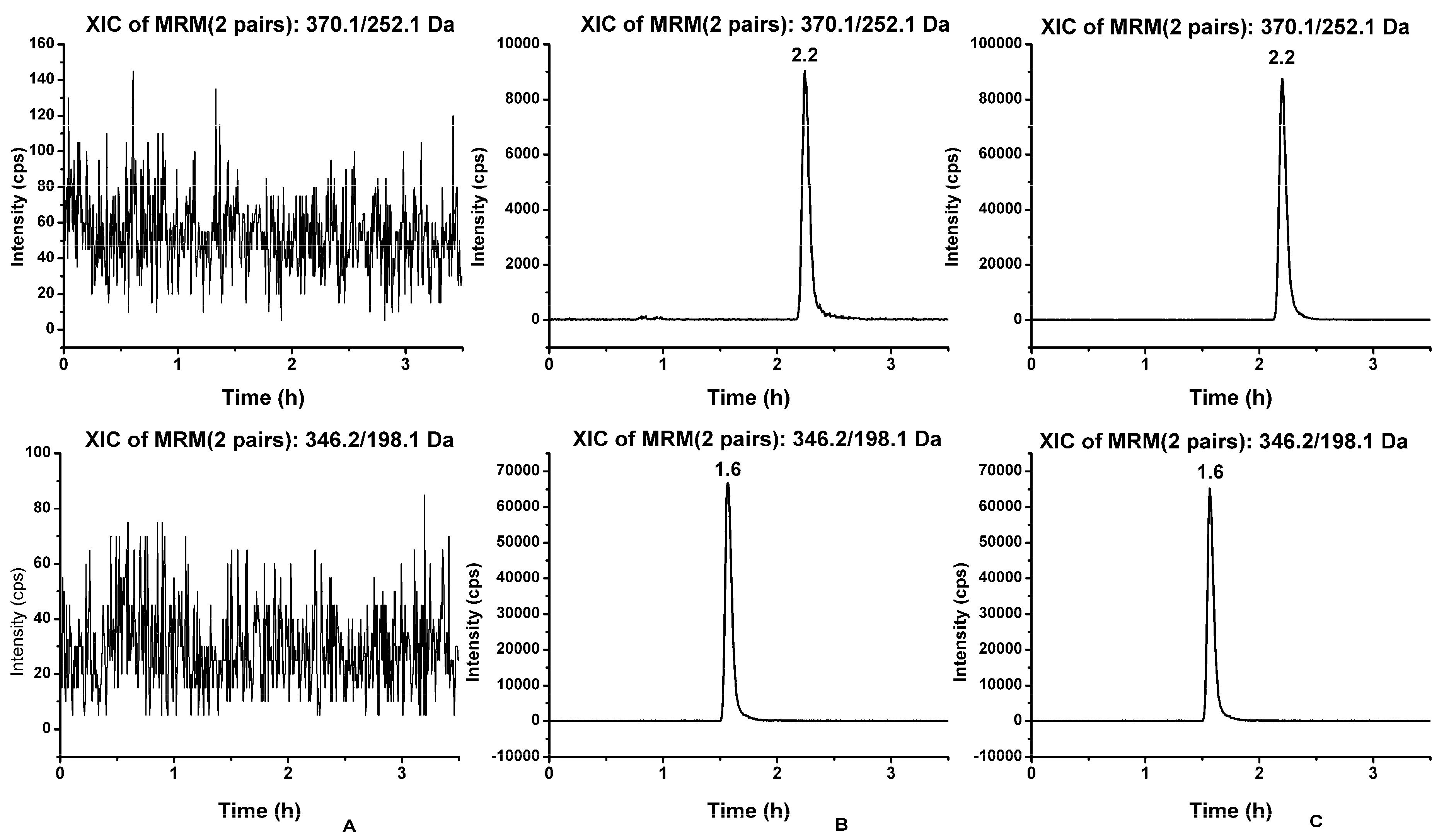
3.2.1. Method Validation
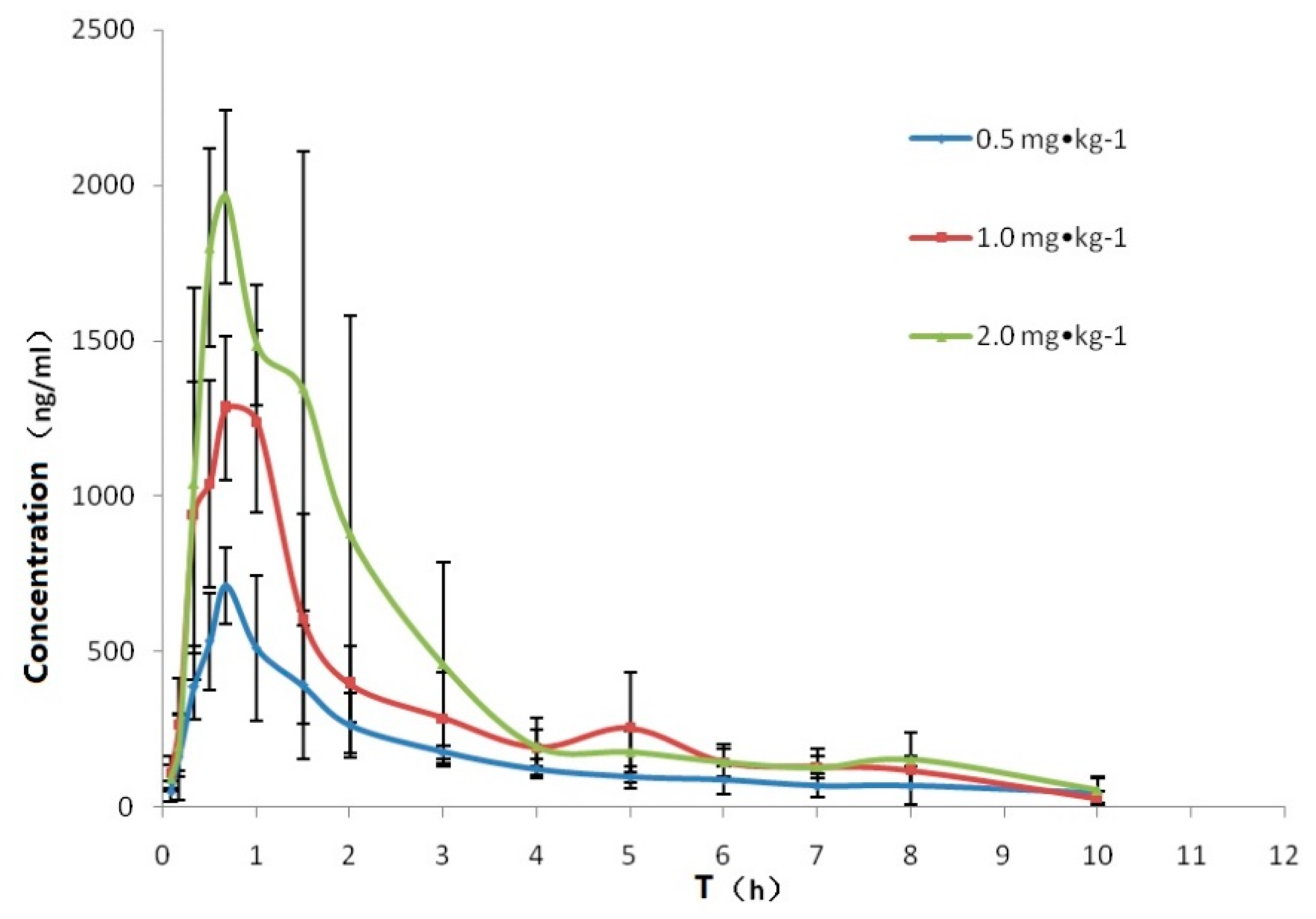
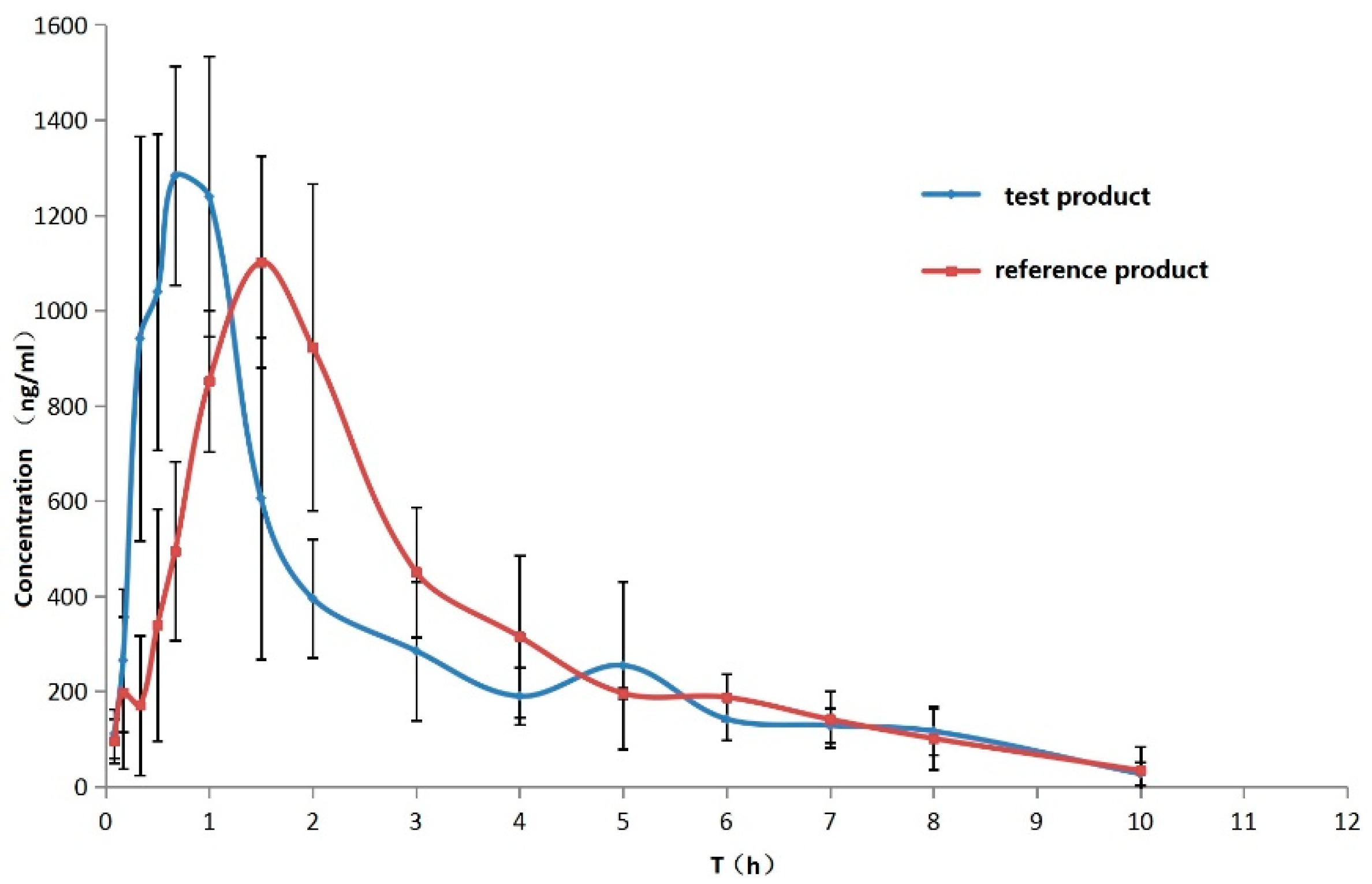
3.2.2. Method Application
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
Abbreviations
| LSZ | Lansoprazole |
| PPI | proton pump inhibitor |
| SOD | superoxide dismutase |
| MDA | malondialdehyde |
| VEGF | Vascular endothelial growth factor |
| COX-2 | Cyclic oxygenase 2 |
| UPLC | ultra-high performance liquid chromatography |
| AUC | area under the curve |
| Cmax | maximum concentration |
References
- Barradell, L.B.; Faulds, D.; McTavish, D. Lansoprazole. A review of its pharmacodynamic and pharmacokinetic properties and its therapeutic efficacy in acid-related disorders. Drugs 1992, 44, 225–250. [Google Scholar] [CrossRef] [PubMed]
- Dugger, H.A.; Carlson, J.D.; Henderson, W. Bioequivalence evaluation of lansoprazole 30-mg capsules (Lanfast and Lanzor) in healthy volunteers. Eur. J. Pharm. Biopharm. 2001, 51, 153–157. [Google Scholar] [CrossRef]
- Inatomi, N.; Nitta, K.; Sakurai, Y. Pharmacological and clinical profile of lansoprazole (Takepron IV injection 30mg). Nihon YakurigakuZasshi 2008, 131, 149–156. [Google Scholar] [CrossRef]
- Gremse, D.A. Lansoprazole: Pharmacokinetics, pharmacodynamics and clinical uses. Expert Opin. Pharmacother. 2001, 2, 1663–1670. [Google Scholar] [CrossRef] [PubMed]
- Hussein, Z.; Granneman, G.R.; Mukherjee, D. Age-related differences in the pharmacokinetics and pharmacodynamics of lansoprazole. Br. J. Clin. Pharmacol. 1993, 36, 391–398. [Google Scholar] [CrossRef]
- Miner, P.; Katz, P.O.; Chen, Y. Gastric acid control with esomeprazole, lansoprazole, omeprazole, pantoprazole, and rabeprazole: A five-way crossover study. Am. J. Gastroenterol. 2003, 98, 2616–2620. [Google Scholar] [CrossRef] [PubMed]
- Zeng, Y.; Ye, Y.; Liang, D. Meta-analysis of the efficacy of lansoprazole and omeprazole for the treatment of H. pylori-associated duodenal ulcer. Int. J. Physiol. Pathophysiol. Pharmacol. 2015, 7, 158–164. [Google Scholar] [PubMed]
- Oliveira, C.H.; Barrientos-Astigarraga, R.E.; Abib, E. Lansoprazole quantification in human plasma by liquid chromatography-electrospray tandem mass spectrometry. J. Chromatogr. B Anal. Technol. Biomed. Life Sci. 2003, 783, 453–459. [Google Scholar] [CrossRef]
- Sakurai, Y.; Hirayama, M.; Hashimoto, M. Population pharmacokinetics and proton pump inhibitory effects of intravenous lansoprazole in healthy Japanese males. Biol. Pharm. Bull. 2007, 30, 2238–2243. [Google Scholar] [CrossRef] [PubMed]
- Uno, T.; Yasui-Furukori, N.; Takahata, T. Determination of lansoprazole and two of its metabolites by liquid-liquid extraction and automated column-switching high-performance liquid chromatography: Application to measuring CYP2C19 activity. J. Chromatogr. B Anal. Technol. Biomed. Life Sci. 2005, 816, 309–314. [Google Scholar] [CrossRef]
- Wu, G.L.; Zhou, H.L.; Shentu, J.Z. Determination of lansoprazole in human plasma by rapid resolution liquid chromatography-electrospray tandem mass spectrometry: Application to a bioequivalence study on Chinese volunteers. J. Pharm. Biomed. Anal. 2008, 48, 1485–1489. [Google Scholar] [CrossRef] [PubMed]
- Zhang, D.; Yang, M.; Liu, M. Pharmacokinetics of lansoprazole and its main metabolites after single intravenous doses in healthy Chinese subjects. Xenobiotica Fate Foreign Compd. Biol. Syst. 2012, 42, 1156–1162. [Google Scholar] [CrossRef] [PubMed]
- Alai, M.; Lin, W.J. Application of nanoparticles for oral delivery of acid-labile lansoprazole in the treatment of gastric ulcer: In vitro and in vivo evaluations. Int. J. Nanomed. 2015, 10, 4029–4041. [Google Scholar]
- Barakatm, N.S.; Almurshedi, A.S. Design and development of gliclazide-loaded chitosan for oral sustained drug delivery: In vitro/in vivo evaluation. J. Microencapsul. 2011, 28, 122–133. [Google Scholar] [CrossRef] [PubMed]
- Frazzoni, M.; De Micheli, E.; Grisendi, A. Lansoprazole vs. omeprazole for gastro-oesophageal reflux disease: A pH-metric comparison. Aliment. Pharmacol. Ther. 2002, 16, 35–39. [Google Scholar] [CrossRef] [PubMed]
- Jyothi, N.V.N.; Prasanna, P.M.; Sakarkar, S.N. Microencapsulation techniques, factors influencing encapsulation efficiency. J. Microencapsul. 2010, 27, 187–197. [Google Scholar] [CrossRef] [PubMed]
- Davit, B.; Braddy, A.C.; Conner, D.P. International guidelines for bioequivalence of systemically available orally administered generic drug products: A survey of similarities and differences. AAPS J. 2013, 15, 974–990. [Google Scholar] [CrossRef] [PubMed]
- Rediguieri, C.F.; Cristofoletti, R.; Soares, K.C. Similarities and differences of international guidelines for bioequivalence: An update of the Brazilian requirements. AAPS J. 2014, 16, 350–351. [Google Scholar] [CrossRef] [PubMed]
- Yang, L.Y.; Li, X.M.; Cui, K. The study of the antiulcer of fructus schisandrae. J. Harbin Commun. 2015, 31, 271–273. [Google Scholar]
- Zhuo, B.F.; Liu, X.W.; Xiao, W.P. Experimental study on the therapeutic effect of weiwei fang on gastric ulcer rats. New TCM 2009, 41, 93–95. [Google Scholar]
- Laine, L.; Weinstein, W.M. Histology of alcoholic hemorrhagic “gastritis”: A prospective evaluation. Gastroenterology 1988, 94, 1254–1262. [Google Scholar] [CrossRef]
- Drug Class Review: Cyclo-Oxygenase (COX)-2 Inhibitors and Non-Steroidal Anti-Inflammatory Drugs (NSAIDs): Final Report Update 3; Oregon Health & Science University: Portland, OR, USA, 2006.
- Zhao, L.S.; Zhao, Y.; Li, Q. A fast, sensitive, and high throughput method for the determination of cefuroxime lysine in dog plasma by UPLC–MS/MS. Talanta 2012, 89, 84–90. [Google Scholar] [CrossRef] [PubMed]
- Food and Drug Administration. Guidance for Industry: Bioanalytical Method Validation; FDA: Rockville, MD, USA, 2008.
- ICH. ICH Harmonization Tripartite Guideline. Guidelines for Good Clinical Practice. International Conference of Harmonization of Technical Requirements for Registration of Pharmaceuticals for Human Uses; ICH: Geneva, Switzerland, 1996. [Google Scholar]
- Wei, B.B.; Liu, M.Y.; Chen, Z.X. UPLC-MS/MS method for determination of schisandrin in rat plasma and brain microdialysates: Application to a comparative pharmacokinetic and brain distribution study in normal and Alzheimer’s disease rats. Anal. Methods 2017, 9, 4740–4746. [Google Scholar] [CrossRef]
- Bi, J.H.; Yang, T.R. The effects of the Liujunzi decoction and its removal on the level of pepsin, SOD and MDA in spleen deficiency gastric ulcer model rats. J. N. J. Univ. Chin. Med. 2010, 26, 280–282. [Google Scholar]
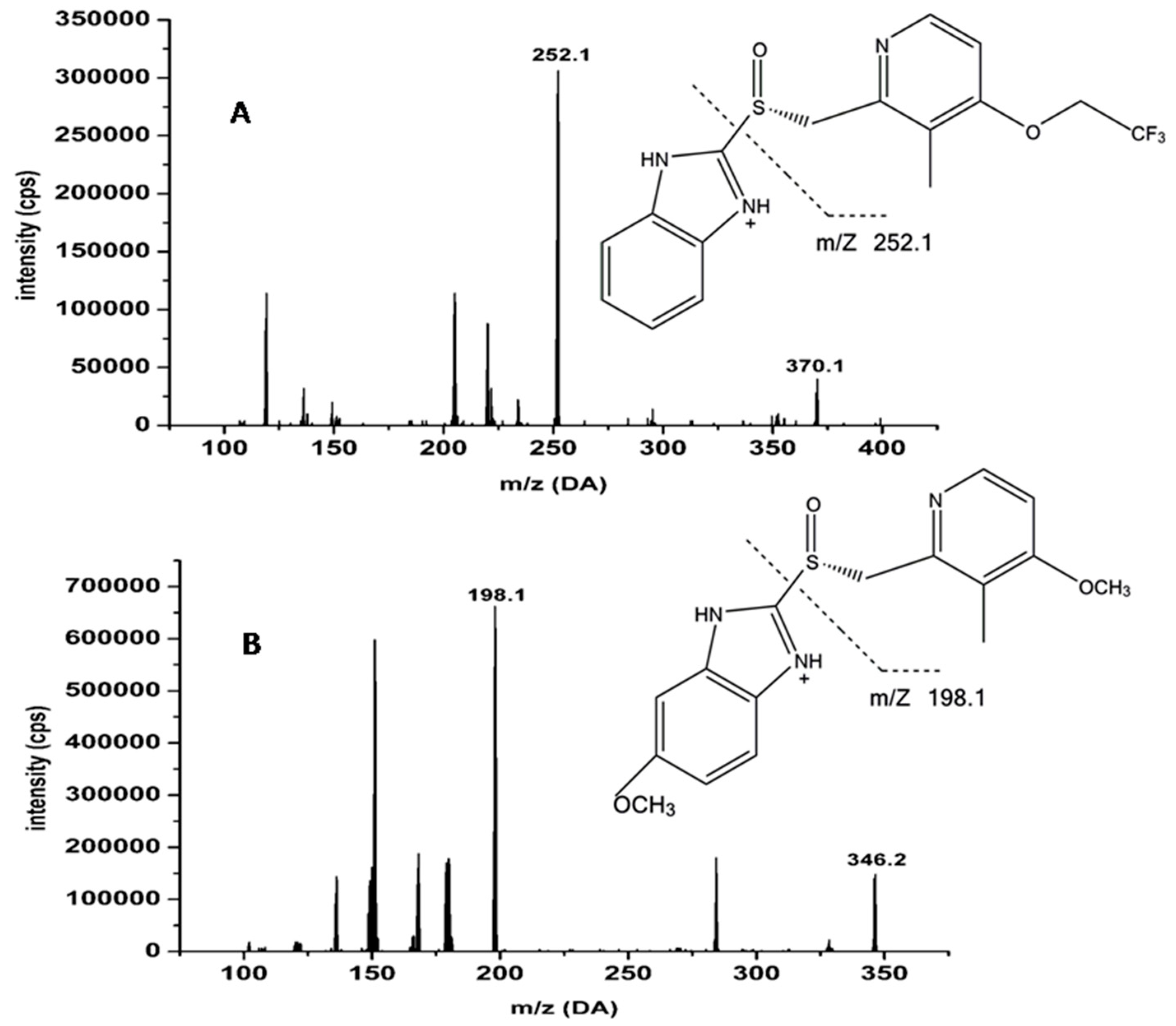
| Analytes | Q1 (amu) | Q3 (amu) | DP (V) | CE (eV) | tR (min) |
|---|---|---|---|---|---|
| lansoprazole | 370.1 | 252.1 | 70 | 23 | 2.2 |
| omeprazole (IS) | 346.2 | 198.1 | 70 | 30 | 1.6 |
| Groups | UI | Gastroprotection (%) |
|---|---|---|
| Intact | 0 | 0 |
| Model | 39.40 ± 7.73 | 0 |
| reference product | 20.60 ± 5.29 * | 48.5 |
| LSZ (2.7 mg/kg) | 28.30 ± 7.29 * | 29.8 |
| compound LSZ-L | 25.20 ± 4.75 * | 37.0 |
| compound LSZ-M | 0.70 ± 0.29 ** | 98.2 |
| compound LSZ-H | 8.50 ± 5.32 * | 79.3 |
| Groups | SOD (μmol*g−1 Pro) | MDA (μmol*g−1 Pro) | H+-K+-ATP enzyme activity (mmol/g h) |
|---|---|---|---|
| Intact | 201.23 ± 16.50 | 73.08 ± 8.76 | 7.13 ± 0.48 |
| Model | 156.12 ± 12.00 | 97.57 ± 7.77 | 8.65 ± 0.54 |
| reference product | 166.96 ± 12.53 * | 72.65 ± 8.98 * | 7.82 ± 0.54 * |
| LSZ (2.7 mg/kg) | 170.12 ± 13.19 * | 75.32 ± 10.77 * | 7.91 ± 0.76 * |
| compound LSZ-L | 170.00 ± 10.08 * | 87.00 ± 9.67 * | 7.83 ± 0.84 * |
| compound LSZ-M | 187.21 ± 8.20 * | 40.05 ± 6.93 ** | 7.20 ± 0.93 * |
| compound LSZ-H | 172.01 ± 9.40 * | 54.58 ± 7.73 * | 7.52 ± 0.39 * |
| Analytes | Concentration | Intra-Day | Inter-Day | Accuracy | Recovery | Matrix Effect |
|---|---|---|---|---|---|---|
| (ng·mL−1) | R.S.D. (%) | R.S.D. (%) | (RE%) | (%, mean ± SD) | (%, mean ± SD) | |
| lansoprazole | 10 | 9.4 | 12.4 | −1.8 | 83.69 ± 3.80 | 82.68 ± 4.81 |
| 125 | 7.1 | 2.0 | 1.1 | 78.35 ± 5.24 | 90.53 ± 1.20 | |
| 2000 | 5.1 | 13.3 | −1.2 | 94.70 ± 3.39 | 82.13 ± 0.34 |
| Analytes | Concentration (ng·mL−1) | 24 h, Room Temperature | 45 Days, −20 °C | 3 Freeze-Thaw Cycles | 10 h, 4 °C | ||||
|---|---|---|---|---|---|---|---|---|---|
| lansoprazole | 10 | 10.00 | 12.08 | 9.11 | 4.06 | 9.64 | 10.03 | 9.35 | 7.2 |
| 125 | 132.80 | 5.28 | 123.82 | 11.27 | 119.79 | 8.83 | 124.51 | 4.3 | |
| 2000 | 2024.38 | 8.40 | 1853.17 | 2.92 | 2128.46 | 4.07 | 2088.22 | 2.9 | |
| Parameters | 0.5 mg·kg−1 | 1.0 mg·kg−1 | 2.0 mg·kg−1 | 1.0 mg·kg−1 (RP) |
|---|---|---|---|---|
| AUC0–t (μgh/L) | 1652 ± 589.7 | 3010 ± 536.8 | 4330 ± 1024 | 3314 ± 307.4 |
| AUC0–∞ (μgh/L) | 2533 ± 1695 | 3151 ± 569.4 | 4630 ± 938.0 | 3487 ± 242.7 |
| T1/2 (h) | 1.66 ± 1.16 | 1.87 ± 1.12 | 2.76 ± 2.03 | 1.7 ± 1.22 |
| Tmax (h) | 0.67 ± 0 | 0.81 ± 0.22 | 0.56 ± 0.14 | 1.67 ± 0.23 * |
| Cmax (ng/L) | 710.6 ± 123.7 | 1391 ± 198.3 | 2067 ± 266.4 | 1197 ± 185.7 |
| MRT (h) | 2.83 ± 0.37 | 2.72 ± 0.50 | 2.5 ± 0.41 | 3.01 ± 0.23 |
| CL (L/h/kg) | 2.72 ± 1.39 | 3.27 ± 0.63 | 4.46 ± 0.85 | 2.88 ± 0.22 |
| Vd (L/kg) | 23.14 ± 18.10 | 8.58 ± 4.62 | 17.54 ± 12.94 | 7.04 ± 4.94 |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Wei, B.; Wang, Y.; Wu, H.; Liu, M.; Yao, W.; Wei, M. Pharmacodynamics and Pharmacokinetics of a New Type of Compound Lansoprazole Capsule in Gastric Ulcer Rats and Beagle Dogs: Importance of Adjusting Oxidative Stress and Inflammation. Pharmaceutics 2019, 11, 49. https://doi.org/10.3390/pharmaceutics11020049
Wei B, Wang Y, Wu H, Liu M, Yao W, Wei M. Pharmacodynamics and Pharmacokinetics of a New Type of Compound Lansoprazole Capsule in Gastric Ulcer Rats and Beagle Dogs: Importance of Adjusting Oxidative Stress and Inflammation. Pharmaceutics. 2019; 11(2):49. https://doi.org/10.3390/pharmaceutics11020049
Chicago/Turabian StyleWei, Binbin, Yan Wang, Huizhe Wu, Mingyan Liu, Weifan Yao, and Minjie Wei. 2019. "Pharmacodynamics and Pharmacokinetics of a New Type of Compound Lansoprazole Capsule in Gastric Ulcer Rats and Beagle Dogs: Importance of Adjusting Oxidative Stress and Inflammation" Pharmaceutics 11, no. 2: 49. https://doi.org/10.3390/pharmaceutics11020049
APA StyleWei, B., Wang, Y., Wu, H., Liu, M., Yao, W., & Wei, M. (2019). Pharmacodynamics and Pharmacokinetics of a New Type of Compound Lansoprazole Capsule in Gastric Ulcer Rats and Beagle Dogs: Importance of Adjusting Oxidative Stress and Inflammation. Pharmaceutics, 11(2), 49. https://doi.org/10.3390/pharmaceutics11020049





