A Critical Analysis of the Use of Cilgavimab plus Tixagevimab Monoclonal Antibody Cocktail (Evusheld™) for COVID-19 Prophylaxis and Treatment
Abstract
:1. Introduction
2. Preclinical Development
3. Clinical Trials
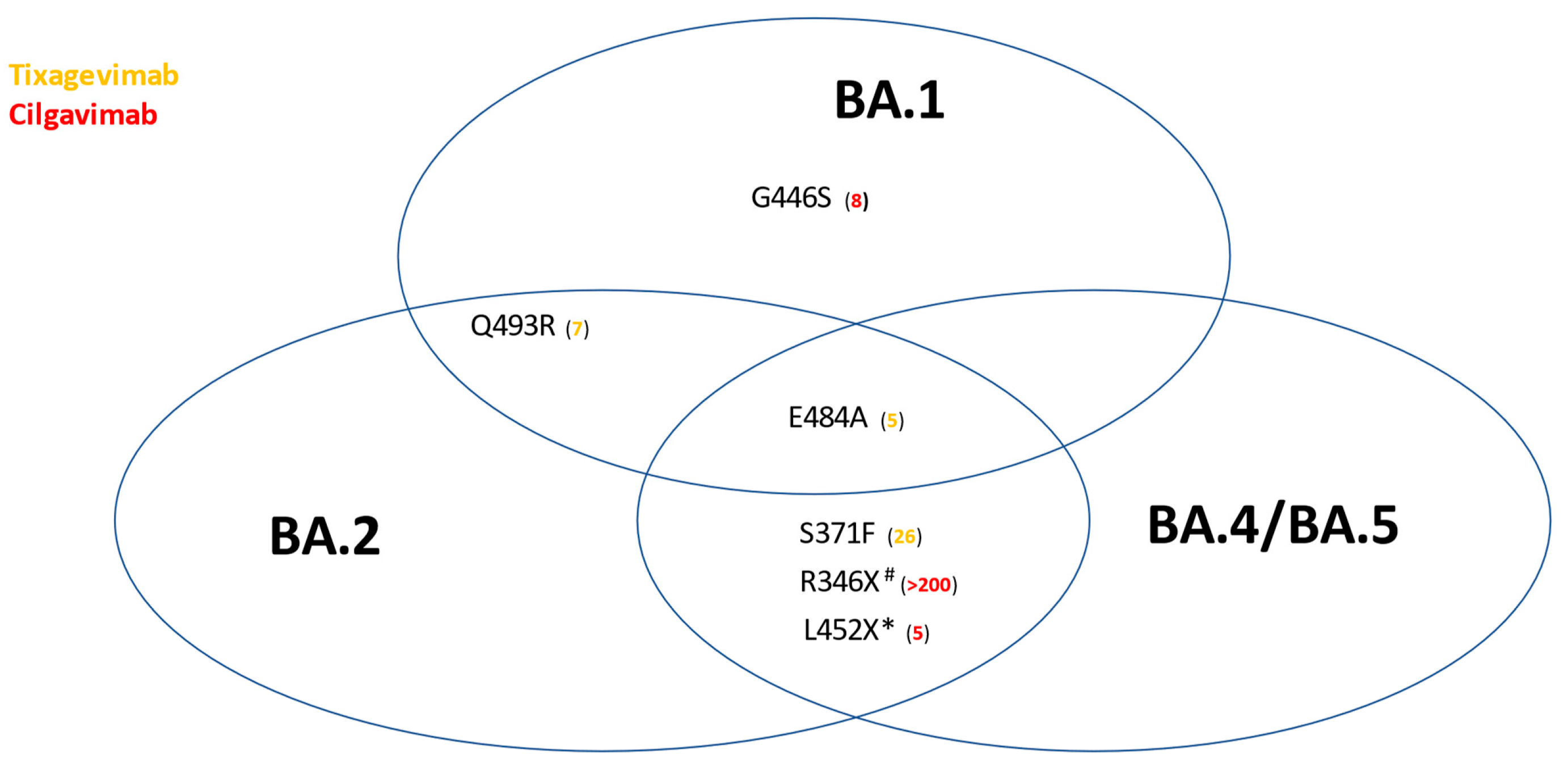
4. Baseline and Treatment-Emergent In Vitro Inefficacy against Omicron Sublineages
5. Post-Marketing Clinical Studies
6. Conclusions
| NCT (Ref) | Indication | Treatment Arm (n) | Control Arm (n) | Main Efficacy Outcome(s) |
|---|---|---|---|---|
| NCT04625725 (PROVENT) [11] | pre-exposure prophylaxis | 3433 | placebo (1717) | Symptomatic COVID-19 in 8 out of 3441 (0.2%) in the Evusheld™ group and in 17 out of 1731 (1.0%) in the placebo group (relative risk reduction, 76.7%); extended follow-up at a median of 6 months showed a relative risk reduction of 82.8%). 5 cases of severe or critical COVID-19 and 2 COVID-19-related deaths occurred, all in the placebo group. |
| NCT04625972 (STORM CHASER) [46] | post-exposure prophylaxis | 749 | placebo (372) | 33% (statistically not significant) relative risk reduction of symptomatic COVID-19 in the overall population 73% relative risk reduction for symptomatic COVID-19 in those PCR-negative at baseline (92% reduction for cases >7 days following dosing; 51% reduction for cases up to 7 days following dosing) |
| NCT04723394 (TACKLE) [14] | outpatient therapy | 452 | placebo (451) | Progression of COVID-19 or death at day 29 was 4% in the treatment group (3.5% if administered within day 5) vs. 9% in the placebo group (relative risk reduction of 50.5%) |
| NCT04501978 (ACTIV-3) | inpatient therapy | 710 | placebo (707) | Sustained recovery was 89% for Evusheld™ and 86% for placebo at day 90 regardless of serostatus. Mortality was 9% (61) with Evusheld™ versus 12% (86) with placebo |
| WHO VOC | Alpha | Beta | Gamma | Delta | Omicron | |||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| PANGOLIN name | B.1.1.7 | B.1.351 | P.1 | B.1.617.2 | BA.1 | BA.2 | BA.2.12.1 | BA.2.75 | BA.4/BA.5 | BA.4.6 | BA.4.7 | BA.5.9 |
| NextStrain name | 20I/S:501Y.V1 | 20H/S:501Y.V2 | 20J/S:501Y.V3 | 21A/S:478K and descendants 21I/21J | 21K (descendant of 21M) | 21L (descendant of 21M) | 22C | 22D | 22A/22B | - | - | - |
| UKHSA/PHE name | VOC-20DEC-01 | VOC-20DEC-02 | VOC-21JAN-02 | VUI-21APR02 | VUI-21NOV-01 | VUI-22JAN-01 | - | V-22JUL-1 | VOC-22APR-03/VOC-22APR-04 | - | - | - |
| GISAID name | GRY (formerly GR/501Y.V1) | GH/501Y.V2 | GR/501Y.V3 | G/452R.V3 | GRA (formerly GR/484A) | |||||||
| tixagevimab /AZD8895/COV2-2196 | ↓↓↓ [47] | ↓↓↓ [47] | = [48] | = [27,49,50,51,52,53,54] | ↓↓↓ [25,41,53,54,55,56,57,58,59,60] | ↓↓↓ [26,41,58,59,60,61,62,63,64] (including BA.2.11, BA.2 L452Q, BA.2 S704L, BA.2 HV69-70del, BA.2 F486V, BA.2 R493Q [60]) | ↓↓↓ [41,58,60,63,64] | ↓↓↓ [62,63,64,65,66] | ↓↓↓ [41,58,59,60,62,63,64] | ↓↓↓ [67,68] | ↓↓↓ [67,68] | ↓↓↓ [67,68] |
| cilgavimab /AZD1061/COV2-2130 | = [47] | = [47] | = [48] | ↓ [27,49,50,51,52,53,54] | ↓↓↓ [24,25,53,55,56,57,58,59,60] | ↓ [26,41,58,59,60,61,62,63,64] (including BA.2.11, BA.2 L452Q, BA.2 S704L, BA.2 HV69-70del, BA.2 F486V, BA.2 R493Q [60]) | ↓ [41,58,60,63,64] | ↓↓↓ [62,63,64,65,66] | ↓↓ [41,58,59,60,62,63,64,69] | ↓↓↓ [67,68] | ↓↓↓ [67,68] | ↓↓↓ [67,68] |
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Abbreviations
| EUA | emergence use authorization |
| RBD | receptor binding domain |
| VOC | variant of concern |
| RCT | randomized controlled trial |
References
- Finkelstein, M.T.; Mermelstein, A.G.; Parker Miller, E.; Seth, P.C.; Stancofski, E.D.; Fera, D. Structural Analysis of Neutralizing Epitopes of the SARS-CoV-2 Spike to Guide Therapy and Vaccine Design Strategies. Viruses 2021, 13, 134. [Google Scholar] [CrossRef] [PubMed]
- Focosi, D.; McConnell, S.; Casadevall, A.; Cappello, E.; Valdiserra, G.; Tuccori, M. Monoclonal antibody therapies against SARS-CoV-2. Lancet Infect. Dis. 2022, Jul 5. [Google Scholar] [CrossRef]
- Bruel, T.; Stefic, K.; Nguyen, Y.; Toniutti, D.; Staropoli, I.; Porrot, F.; Guivel-Benhassine, F.; Bolland, W.H.; Planas, D.; Hadjadj, J.; et al. Longitudinal analysis of serum neutralization of SARS-CoV-2 Omicron BA.2, BA.4 and BA.5 in patients receiving monoclonal antibodies. medRxiv 2022. [Google Scholar] [CrossRef]
- Robbie, G.J.; Criste, R.; Dall’acqua, W.F.; Jensen, K.; Patel, N.K.; Losonsky, G.A.; Griffin, M.P. A novel investigational Fc-modified humanized monoclonal antibody, motavizumab-YTE, has an extended half-life in healthy adults. Antimicrob. Agents Chemother. 2013, 57, 6147–6153. [Google Scholar] [CrossRef] [PubMed]
- Domachowske, J.B.; Khan, A.A.; Esser, M.T.; Jensen, K.; Takas, T.; Villafana, T.; Dubovsky, F.; Griffin, M.P. Safety, Tolerability and Pharmacokinetics of MEDI8897, an Extended Half-life Single-dose Respiratory Syncytial Virus Prefusion F-targeting Monoclonal Antibody Administered as a Single Dose to Healthy Preterm Infants. Pediatr. Infect. Dis. J. 2018, 37, 886–892. [Google Scholar] [CrossRef] [PubMed]
- Natarajan, H.; Crowley, A.R.; Butler, S.E.; Xu, S.; Weiner, J.A.; Bloch, E.M.; Littlefield, K.; Wieland-Alter, W.; Connor, R.I.; Wright, P.F.; et al. Markers of Polyfunctional SARS-CoV-2 Antibodies in Convalescent Plasma. mBio 2021, 12, e00765-21. [Google Scholar] [CrossRef] [PubMed]
- Goldblatt, D.; Alter, G.; Crotty, S.; Plotkin, S.A. Correlates of protection against SARS-CoV-2 infection and COVID-19 disease. Immunol. Rev. 2022; in press. [Google Scholar] [CrossRef]
- EMA Committee for Medicinal Products for Human Use (CHMP). Evushedl Assessment Report. Available online: https://www.ema.europa.eu/en/medicines/human/EPAR/evusheld (accessed on 17 August 2022).
- Loo, Y.M.; McTamney, P.M.; Arends, R.H.; Abram, M.E.; Aksyuk, A.A.; Diallo, S.; Flores, D.J.; Kelly, E.J.; Ren, K.; Roque, R.; et al. The SARS-CoV-2 monoclonal antibody combination, AZD7442, is protective in nonhuman primates and has an extended half-life in humans. Sci. Transl. Med. 2022, 14, eabl8124. [Google Scholar] [CrossRef]
- Focosi, D.; Franchini, M.; Pirofski, L.A.; Maggi, F.; Casadevall, A. Is SARS-CoV-2 viral clearance in nasopharyngal swabs an appropriate surrogate marker for clinical efficacy of neutralizing antibody-based therapeutics? Rev. Med. Virol. 2021, 32, e2314. [Google Scholar]
- Levin, M.J.; Ustianowski, A.; De Wit, S.; Launay, O.; Avila, M.; Templeton, A.; Yuan, Y.; Seegobin, S.; Ellery, A.; Levinson, D.J.; et al. Intramuscular AZD7442 (Tixagevimab-Cilgavimab) for Prevention of COVID-19. N. Engl. J. Med. 2022, 386, 2188–2200. [Google Scholar] [CrossRef]
- AZD7442 PROVENT Phase III Prophylaxis Trial Met Primary Endpoint in Preventing COVID-19. Available online: https://www.astrazeneca.com/media-centre/press-releases/2021/azd7442-prophylaxis-trial-met-primary-endpoint.html (accessed on 17 August 2022).
- AIFA. La CTS Amplia i Criteri di Prescrizione di Evusheld per la Profilassi Pre-Esposizione Nei Soggetti ad Alto Rischio di Malattia Severa COVID-19. Available online: https://www.aifa.gov.it/-/la-cts-amplia-i-criteri-di-prescrizione-di-evusheld-per-la-profilassi-pre-esposizione-nei-soggetti-ad-alto-rischio-di-malattia-severa-covid-19 (accessed on 17 August 2022).
- Montgomery, H.; Hobbs, F.D.R.; Padilla, F.; Arbetter, D.; Templeton, A.; Seegobin, S.; Kim, K.; Campos, J.A.S.; Arends, R.H.; Brodek, B.H.; et al. Efficacy and safety of intramuscular administration of tixagevimab–cilgavimab for early outpatient treatment of COVID-19 (TACKLE): A phase 3, randomised, double-blind, placebo-controlled trial. Lancet Respir. Med. 2022; in press. [Google Scholar] [CrossRef]
- AZD7442 Reduced Risk of Developing Severe COVID-19 or Death in TACKLE Phase III Outpatient Treatment Trial. Available online: https://www.astrazeneca.com/content/astraz/media-centre/press-releases/2021/azd7442-phiii-trial-positive-in-covid-outpatients.html (accessed on 22 February 2022).
- AIFA Authorises the Therapeutic Use of the Monoclonal Evusheld for the Early Treatment of COVID-19 in Subjects at Risk of Progression. Available online: https://www.aifa.gov.it/en/-/aifa-autorizza-l-utilizzo-terapeutico-del-monoclonale-evusheld-per-il-trattamento-precoce-del-covid-19-in-soggetti-a-rischio-di-progressione (accessed on 17 August 2022).
- Focosi, D.; Tuccori, M. Prescription of Anti-Spike Monoclonal Antibodies in COVID-19 Patients with Resistant SARS-CoV-2 Variants in Italy. Pathogens 2022, 11, 823. [Google Scholar] [CrossRef]
- ACTIV-3/Therapeutics for Inpatients with COVID-19 (TICO) Study Group; Nielsen, H.; Thisted, R.K.; Toft Petersen, K. Tixagevimab-cilgavimab for treatment of patients hospitalised with COVID-19: A randomised, double-blind, phase 3 trial. Lancet Respir. Med. 2022; ahead of print. [Google Scholar]
- Hypersensitivity reactions with tixagevimab/cilgavimab (Evusheld). Med. Lett. Drugs Ther. 2022, 64, 112.
- Kleiboeker, H.L.; Jorgenson, M.R.; Smith, J.A. Myalgia in liver transplant recipients after receiving tixagevimab/cilgavimab for pre-exposure prophylaxis of COVID-19: A case series. Transpl. Infect. Dis. 2022, e13932. [Google Scholar] [CrossRef]
- Addetia, A.; Park, Y.-J.; Starr, T.; Greaney, A.J.; Sprouse, K.; Bowen, J.E.; Tiles, S.W.; Van Voorhis, W.C.; Bloom, J.D.; Corti, D.; et al. Structural changes in the SARS-CoV-2 spike E406W mutant escaping a clinical monoclonal antibody cocktail. bioRxiv 2022. [Google Scholar] [CrossRef]
- Focosi, D.; Mazzetti, P.; Pistello, M.; Maggi, F. Viral infection neutralization tests: A focus on SARS-CoV-2 with implications for convalescent plasma therapy. Rev. Med. Virol. 2020, 31, e2170. [Google Scholar]
- Brady, T.; Zhang, T.; Tuffy, K.M.; Haskins, N.; Du, Q.; Lin, J.; Kaplan, G.; Novick, S.; Roe, T.L.; Ren, K.; et al. Qualification of a Biolayer Interferometry Assay to Support AZD7442 Resistance Monitoring. Microbiol. Spectr. 2022; ahead of print. [Google Scholar] [CrossRef]
- Dejnirattisai, W.; Huo, J.; Zhou, D.; Zahradník, J.; Supasa, P.; Liu, C.; Duyvesteyn, H.M.E.; Ginn, H.M.; Mentzer, A.J.; Tuekprakhon, A.; et al. SARS-CoV-2 Omicron-B.1.1.529 leads to widespread escape from neutralizing antibody responses. Cell 2022, 185, 467–484.e15. [Google Scholar] [CrossRef]
- VanBlargan, L.A.; Errico, J.M.; Halfmann, P.J.; Zost, S.J.; Crowe, J.E., Jr.; Purcell, L.A.; Kawaoka, Y.; Corti, D.; Fremont, D.H.; Diamond, M.S. An infectious SARS-CoV-2 B.1.1.529 Omicron virus escapes neutralization by therapeutic monoclonal antibodies. Nat. Med. 2022, 28, 490–495. [Google Scholar] [CrossRef]
- Bruel, T.; Hadjadj, J.; Maes, P.; Planas, D.; Seve, A.; Staropoli, I.; Guivel-Benhassine, F.; Porrot, F.; Bolland, W.-H.; Nguyen, Y.; et al. Serum neutralization of SARS-CoV-2 Omicron sublineages BA.1 and BA.2 in patients receiving monoclonal antibodies. Nat. Med. 2022, 28, 1297–1302. [Google Scholar] [CrossRef]
- Dong, J.; Zost, S.J.; Greaney, A.J.; Starr, T.N.; Dingens, A.S.; Chen, E.C.; Chen, R.E.; Case, J.B.; Sutton, R.E.; Gilchuk, P.; et al. Genetic and structural basis for SARS-CoV-2 variant neutralization by a two-antibody cocktail. Nat. Microbiol. 2021, 6, 1233–1244. [Google Scholar] [CrossRef]
- Starr, T.N.; Greaney, A.J.; Hilton, S.K.; Ellis, D.; Crawford, K.H.D.; Dingens, A.S.; Navarro, M.J.; Bowen, J.E.; Tortorici, M.A.; Walls, A.C.; et al. Deep Mutational Scanning of SARS-CoV-2 Receptor Binding Domain Reveals Constraints on Folding and ACE2 Binding. Cell 2020, 182, 1295–1310.e20. [Google Scholar] [CrossRef] [PubMed]
- Stadler, E.; Chai, K.L.; Schlub, T.E.; Cromer, D.; Polizzotto, M.N.; Kent, S.J.; Beecher, C.; White, H.; Turner, T.; Skoetz, N.; et al. Determinants of passive antibody efficacy in SARS-CoV-2 infection. medRxiv 2022. [Google Scholar] [CrossRef]
- Case, J.B.; Mackin, S.; Errico, J.M.; Chong, Z.; Madden, E.A.; Whitener, B.; Guarino, B.; Schmid, M.A.; Rosenthal, K.; Ren, K.; et al. Resilience of S309 and AZD7442 monoclonal antibody treatments against infection by SARS-CoV-2 Omicron lineage strains. Nat. Commun. 2022, 13, 3824. [Google Scholar] [CrossRef]
- FDA. Fact Sheet for Healthcare Providers: Emergency Use Authorization for Evusheld™ (Tixagevimab Co-Packaged with Cilgavimab). 2021. Available online: https://www.fda.gov/media/154701/download (accessed on 13 August 2022).
- Copin, R.; Baum, A.; Wloga, E.; Pascal, K.E.; Giordano, S.; Fulton, B.O.; Zhou, A.; Negron, N.; Lanza, K.; Chan, N.; et al. The monoclonal antibody combination REGEN-COV protects against SARS-CoV-2 mutational escape in preclinical and human studies. Cell 2021, 184, 3949–3961. [Google Scholar] [CrossRef]
- Benotmane, I.; Velay, A.; Thaunat, O.; Vargas, G.G.; Olagne, J.; Fafi-Kremer, S.; Caillard, S. Pre-exposure prophylaxis with Evusheld™ elicits limited neutralizing activity against the omicron variant in kidney transplant patients. medRxiv 2022. [Google Scholar] [CrossRef]
- Stuver, R.; Shah, G.L.; Korde, N.S.; Roeker, L.E.; Mato, A.R.; Batlevi, C.L.; Chung, D.J.; Doddi, S.; Falchi, L.; Gyurkocza, B.; et al. Activity of AZD7442 (tixagevimab-cilgavimab) against Omicron SARS-CoV-2 in patients with hematologic malignancies. Cancer Cell 2022, 40, 590–591. [Google Scholar] [CrossRef]
- Benotmane, I.; Velay, A.; Vargas, G.G.; Olagne, J.; Fafi-Kremer, S.; Thaunat, O.; Caillard, S. Breakthrough COVID-19 cases despite tixagevimab and cilgavimab (Evusheld™) prophylaxis in kidney transplant recipients. medRxiv 2022. [Google Scholar] [CrossRef]
- FDA Authorizes Revisions to Evusheld Dosing. Available online: https://www.fda.gov/drugs/drug-safety-and-availability/fda-authorizes-revisions-evusheld-dosing (accessed on 17 August 2022).
- AstraZeneca. Updated EVUSHELD Emergency Use Authorization (EUA) Dosage Recommendations for Patients Who Received an Initial Dose of 150 mg Tixagevimab and 150 mg Cilgavimab. Available online: https://www.fda.gov/media/156617/download (accessed on 17 August 2022).
- Karaba, A.H.; Kim, J.; Chiang, T.P.-Y.; Alejo, J.L.; Abedon, A.T.; Mitchell, J.; Chang, A.; Eby, Y.; Johnston, T.S.; Aytenfisu, T.Y.; et al. Omicron BA.1 and BA.2 Neutralizing Activity following Pre-Exposure Prophylaxis with Tixagevimab plus Cilgavimab in Vaccinated Solid Organ Transplant Recipients. medRxiv 2022. [Google Scholar] [CrossRef]
- Al Jurdi, A.; Morena, L.; Cote, M.; Bethea, E.; Azzi, J.; Riella, L.V. Tixagevimab/cilgavimab pre-exposure prophylaxis is associated with lower breakthrough infection risk in vaccinated solid organ transplant recipients during the Omicron wave. medRxiv 2022. [Google Scholar] [CrossRef] [PubMed]
- Young-Xu, Y.; Epstein, L.; Marconi, V.C.; Davey, V.; Zwain, G.; Smith, J.; Korves, C.; Cunningham, F.; Bonomo, R.; Ginde, A.A. Tixagevimab/Cilgavimab for Prevention of COVID-19 during the Omicron Surge: Retrospective Analysis of National VA Electronic Data. medRxiv 2022. [Google Scholar] [CrossRef]
- Kimura, I.; Yamasoba, D.; Tamura, T.; Nao, N.; Oda, Y.; Mitoma, S.; Ito, J.; Nasser, H.; Zahradnik, J.; Uriu, K.; et al. Virological characteristics of the novel SARS-CoV-2 Omicron variants including BA.2.12.1, BA.4 and BA.5. bioRxiv 2022. [Google Scholar] [CrossRef]
- Mahase, E. COVID-19: UK will not buy Evusheld owing to “insufficient data” on protection, government says. BMJ 2022, 378, o2021. [Google Scholar] [CrossRef]
- Anderson, T.S.; O’Donoghue, A.; Mechanic, O.; Dechen, T.; Stevens, J. Administration of Anti-SARS-CoV-2 Monoclonal Antibodies after US Food and Drug Administration Deauthorization. JAMA Netw. Open 2022, 5, e2228997. [Google Scholar] [CrossRef]
- Focosi, D.; Franchini, M.; Joyner, M.J.; Casadevall, A.; Sullivan, D.J. Analysis of anti-Omicron neutralizing antibody titers in different convalescent plasma sources. medRxiv 2021. [Google Scholar] [CrossRef]
- Senefeld, J.W.; Franchini, M.; Mengoli, C.; Cruciani, M.; Zani, M.; Gorman, E.K.; Focosi, D.; Casadevall, A.; Joyner, M.J. COVID-19 convalescent plasma for the treatment of immunocompromised patients: A systematic review. medRxiv 2022. [Google Scholar] [CrossRef]
- Update on AZD7442 STORM CHASER Trial in Post-Exposure Prevention of Symptomatic COVID-19. Available online: https://www.astrazeneca.com/media-centre/press-releases/2021/update-on-azd7442-storm-chaser-trial.html (accessed on 21 February 2022).
- Wang, P.; Nair, M.S.; Lihong, L.; Iketani, S.; Luo, Y.; Guo, Y.; Wang, M.; Yu, J.; Zhang, B.; Kwong, P.D.; et al. Antibody resistance of SARS-CoV-2 variants B.1.351 and B.1.1.7. Nature 2021, 593, 130–135. [Google Scholar] [CrossRef] [PubMed]
- Wang, P.; Wang, M.; Yu, J.; Cerutti, G.; Nair, M.S.; Huang, Y.; Kwong, P.D.; Shapiro, L.; Ho, D.D. Increased Resistance of SARS-CoV-2 Variant P.1 to Antibody Neutralization. Cell Host Microbe 2021, 29, 747–751. [Google Scholar] [CrossRef] [PubMed]
- Touret, F.; Baronti, C.; Pastorino, B.; Villarroel, P.M.S.; Ninove, L.; Nougairède, A.; de Lamballerie, X. In vitro activity of therapeutic antibodies against SARS-CoV-2 Omicron BA.1, BA.2 and BA.5. Sci. Rep. 2022, 12, 12609. [Google Scholar] [CrossRef]
- Misasi, J.; Wei, R.R.; Wang, L.; Pegu, A.; Wei, C.J.; Oloniniyi, O.K.; Zhou, T.; Zhao, B.; Choe, M.; Boruszczak, M.; et al. A multispecific antibody confers pan-reactive SARS-CoV-2 neutralization and prevents immune escape. bioRxiv 2022. [Google Scholar] [CrossRef]
- Takashita, E.; Kinoshita, N.; Yamayoshi, S.; Sakai-Tagawa, Y.; Fujisaki, S.; Ito, M.; Iwatsuki-Horimoto, K.; Chiba, S.; Halfmann, P.; Nagai, H.; et al. Efficacy of Antibodies and Antiviral Drugs against Covid-19 Omicron Variant. N. Engl. J. Med. 2022, 386, 995–998. [Google Scholar] [CrossRef]
- Boschi, C.; Colson, P.; Bancod, A.; Moal, V.; La Scola, B. Omicron Variant Escapes Therapeutic Monoclonal Antibodies (mAbs) Including Recently Released Evusheld®, Contrary to 8 Prior Main Variant of Concern (VOC). Clin. Infect. Dis. 2022, 75, e534–e535. [Google Scholar] [CrossRef]
- Cao, Y.R.; Wang, J.; Jian, F.; Xiao, T.; Song, W.; Yisimayi, A.; Huang, W.; Li, Q.; Wang, P.; An, R.; et al. Omicron escapes the majority of SARS-CoV-2 neutralizing antibodies of diverse epitopes. Nature 2021, 602, 657–663. [Google Scholar] [CrossRef]
- Liu, C.; Ginn, H.M.; Dejnirattisai, W.; Supasa, P.; Wang, B.; Tuekprakhon, A.; Nutalai, R.; Zhou, D.; Mentzer, A.J.; Zhao, Y.; et al. Considerable escape of SARS-CoV-2 variant Omicron to antibody neutralization. Nature 2021, 602, 671–675. [Google Scholar]
- Liu, L.; Iketani, S.; Guo, Y.; Chan, J.F.-W.; Wang, M.; Liu, L.; Luo, Y.; Chu, H.; Huang, Y.; Nair, M.S.; et al. Striking Antibody Evasion Manifested by the Omicron Variant of SARS-CoV-2. Nature 2021, 602, 676–681. [Google Scholar] [CrossRef] [PubMed]
- Aggarwal, A.; Ospina Stella, A.; Walker, G.; Akerman, A.; Milogiannakis, V.; Hoppe, A.C.; Mathivanan, V.; Fichter, C.; McAllery, S.; Amatayakul-Chantler, S.; et al. SARS-CoV-2 Omicron: Reduction of potent humoral responses and resistance to clinical immunotherapeutics relative to viral variants of concern. medRxiv 2021. [Google Scholar] [CrossRef]
- Touret, F.; Baronti, C.; Bouzidi, H.S.; de Lamballerie, X. In vitro evaluation of therapeutic antibodies against a SARS-CoV-2 Omicron B.1.1.529 isolate. Sci. Rep. 2022, 12, 4683. [Google Scholar] [CrossRef] [PubMed]
- Turelli, P.; Fenwick, C.; Raclot, C.; Genet, V.; Pantaleo, G.; Trono, D. P2G3 human monoclonal antibody neutralizes SARS-CoV-2 Omicron subvariants including BA.4 and BA.5 and Bebtelovimab escape mutants. bioRxiv 2022. [Google Scholar] [CrossRef]
- Andreano, E.; Paciello, I.; Pierleoni, G.; Maccari, G.; Antonelli, G.; Abbiento, V.; Pileri, P.; Benincasa, L.; Giglioli, G.; Piccini, G.; et al. mRNA vaccines and hybrid immunity use different B cell germlines to neutralize Omicron BA.4 and BA.5. bioRxiv 2022. [Google Scholar] [CrossRef]
- Yamasoba, D.; Kosugi, Y.; Kimura, I.; Fujita, S.; Uriu, K.; Ito, J.; Sato, K.; Genotype to Phenotype Japan (G2P-Japan) Consortium. Neutralisation sensitivity of SARS-CoV-2 omicron subvariants to therapeutic monoclonal antibodies. Lancet Infect. Dis. 2022, 22, 942–943. [Google Scholar] [CrossRef]
- Takashita, E.; Kinoshita, N.; Yamayoshi, S.; Sakai-Tagawa, Y.; Fujisaki, S.; Ito, M.; Iwatsuki-Horimoto, K.; Halfmann, P.; Watanabe, S.; Maeda, K.; et al. Efficacy of Antiviral Agents against the SARS-CoV-2 Omicron Subvariant BA.2. N. Engl. J. Med. 2022, 386, 1475–1477. [Google Scholar] [CrossRef]
- Sheward, D.J.; Kim, C.; Fischbach, J.; Muschiol, S.; Ehling, R.A.; Björkström, N.K.; Karlsson Hedestam, G.B.; Reddy, S.T.; Albert, J.; Peacock, T.P.; et al. Evasion of neutralizing antibodies by Omicron sublineage BA.2.75. bioRxiv 2022. [Google Scholar] [CrossRef]
- Wang, Q.; Iketani, S.; Li, Z.; Guo, Y.; Yeh, A.Y.; Liu, M.; Yu, J.; Sheng, Z.; Huang, Y.; Liu, L.; et al. Antigenic characterization of the SARS-CoV-2 Omicron subvariant BA.2.75. bioRxiv 2022. [Google Scholar] [CrossRef]
- Gruell, H.; Vanshylla, K.; Tober-Lau, P.; Hillus, D.; Sander, L.E.; Kurth, F.; Klein, F. Neutralization sensitivity of the SARS-CoV-2 Omicron BA.2.75 sublineage. bioRxiv 2022. [Google Scholar] [CrossRef]
- Yamasoba, D.; Kimura, I.; Kosugi, Y.; Uriu, K.; Fujita, S.; Ito, J.; Sato, K. Neutralization sensitivity of Omicron BA.2.75 to therapeutic monoclonal antibodies. bioRxiv 2022. [Google Scholar] [CrossRef]
- Cao, Y.; Yu, Y.; Song, W.; Jian, F.; Yisimayi, A.; Yue, C.; Feng, R.; Wang, P.; Yu, L.; Zhang, N.; et al. Neutralizing antibody evasion and receptor binding features of SARS-CoV-2 Omicron BA.2.75. bioRxiv 2022. [Google Scholar] [CrossRef]
- Jian, F.; Yu, Y.; Song, W.; Yisimayi, A.; Yu, L.; Gao, Y.; Zhang, N.; Wang, Y.; Shao, F.; Hao, X.; et al. Further humoral immunity evasion of emerging SARS-CoV-2 BA.4 and BA.5 subvariants. bioRxiv 2022. [Google Scholar] [CrossRef]
- Wang, Q.; Li, Z.; Ho, J.; Guo, Y.; Yeh, A.Y.; Liu, M.; Wang, M.; Yu, J.; Sheng, Z.; Huang, Y.; et al. Resistance of SARS-CoV-2 Omicron Subvariant BA.4.6 to Antibody Neutralization. bioRxiv 2022. [Google Scholar] [CrossRef]
- Cao, Y.R.; Yisimayi, A.; Jian, F.; Song, W.; Xiao, T.; Wang, L.; Du, S.; Wang, J.; Li, Q.; Chen, X.; et al. 2.12.1, BA.4 and BA.5 escape antibodies elicited by Omicron infection. Nature 2022, 608, 593–602. [Google Scholar] [CrossRef]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Focosi, D.; Casadevall, A. A Critical Analysis of the Use of Cilgavimab plus Tixagevimab Monoclonal Antibody Cocktail (Evusheld™) for COVID-19 Prophylaxis and Treatment. Viruses 2022, 14, 1999. https://doi.org/10.3390/v14091999
Focosi D, Casadevall A. A Critical Analysis of the Use of Cilgavimab plus Tixagevimab Monoclonal Antibody Cocktail (Evusheld™) for COVID-19 Prophylaxis and Treatment. Viruses. 2022; 14(9):1999. https://doi.org/10.3390/v14091999
Chicago/Turabian StyleFocosi, Daniele, and Arturo Casadevall. 2022. "A Critical Analysis of the Use of Cilgavimab plus Tixagevimab Monoclonal Antibody Cocktail (Evusheld™) for COVID-19 Prophylaxis and Treatment" Viruses 14, no. 9: 1999. https://doi.org/10.3390/v14091999
APA StyleFocosi, D., & Casadevall, A. (2022). A Critical Analysis of the Use of Cilgavimab plus Tixagevimab Monoclonal Antibody Cocktail (Evusheld™) for COVID-19 Prophylaxis and Treatment. Viruses, 14(9), 1999. https://doi.org/10.3390/v14091999







