Transcriptome Sequencing of the Spleen Reveals Antiviral Response Genes in Chickens Infected with CAstV
Abstract
1. Introduction
2. Materials and Methods
2.1. Virus and Animals
2.2. Animal Experiments
2.3. RNA Quantification and Quality Control
2.4. Library Preparation for Transcriptome Sequencing
2.5. Data Analysis
2.6. Accession Number
2.7. qRT-PCR for Confirmation
2.8. Statistical Analysis of qRT-PCR
3. Results
3.1. Clinical Features of the CAstV-infected Chickens
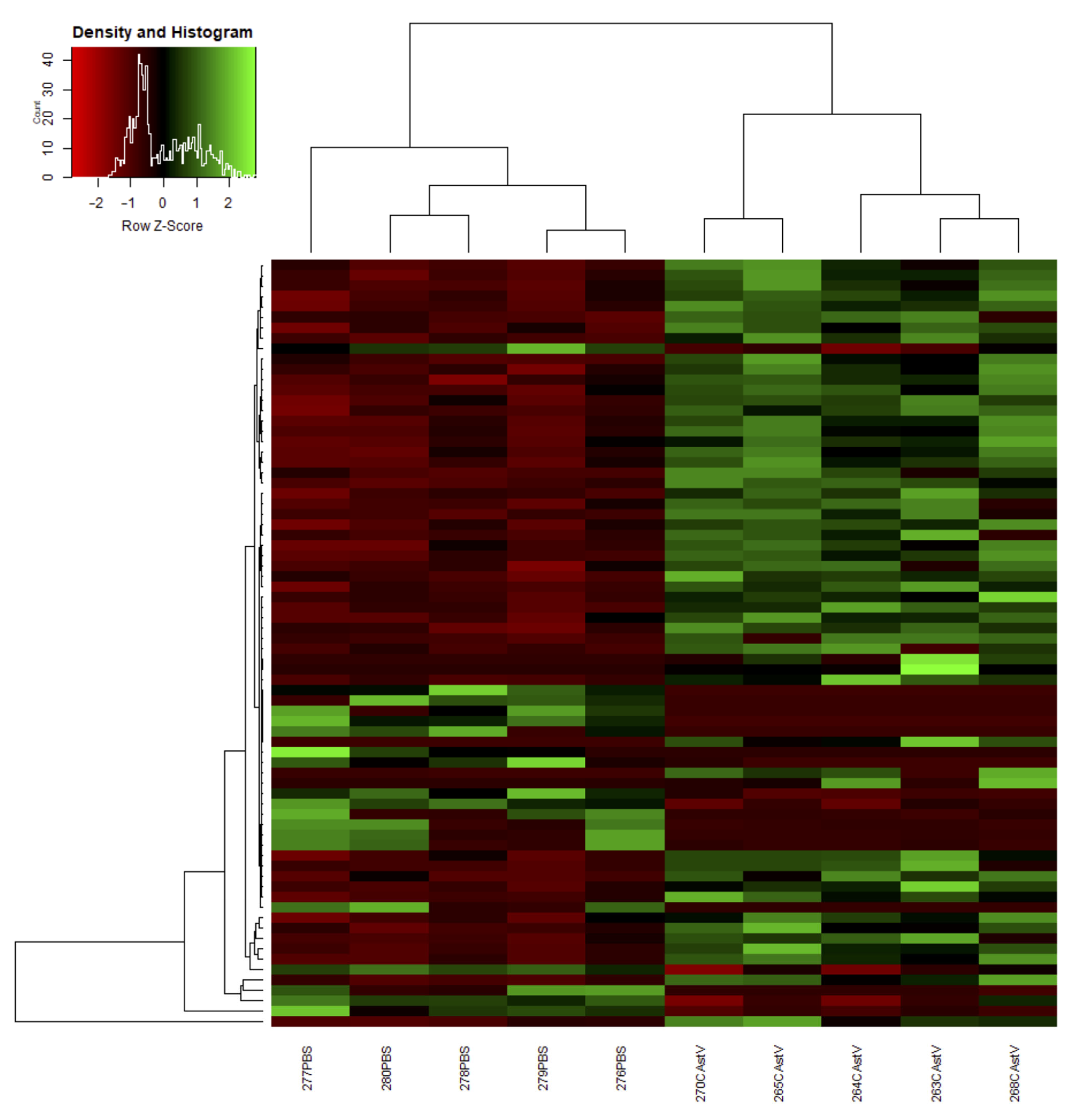
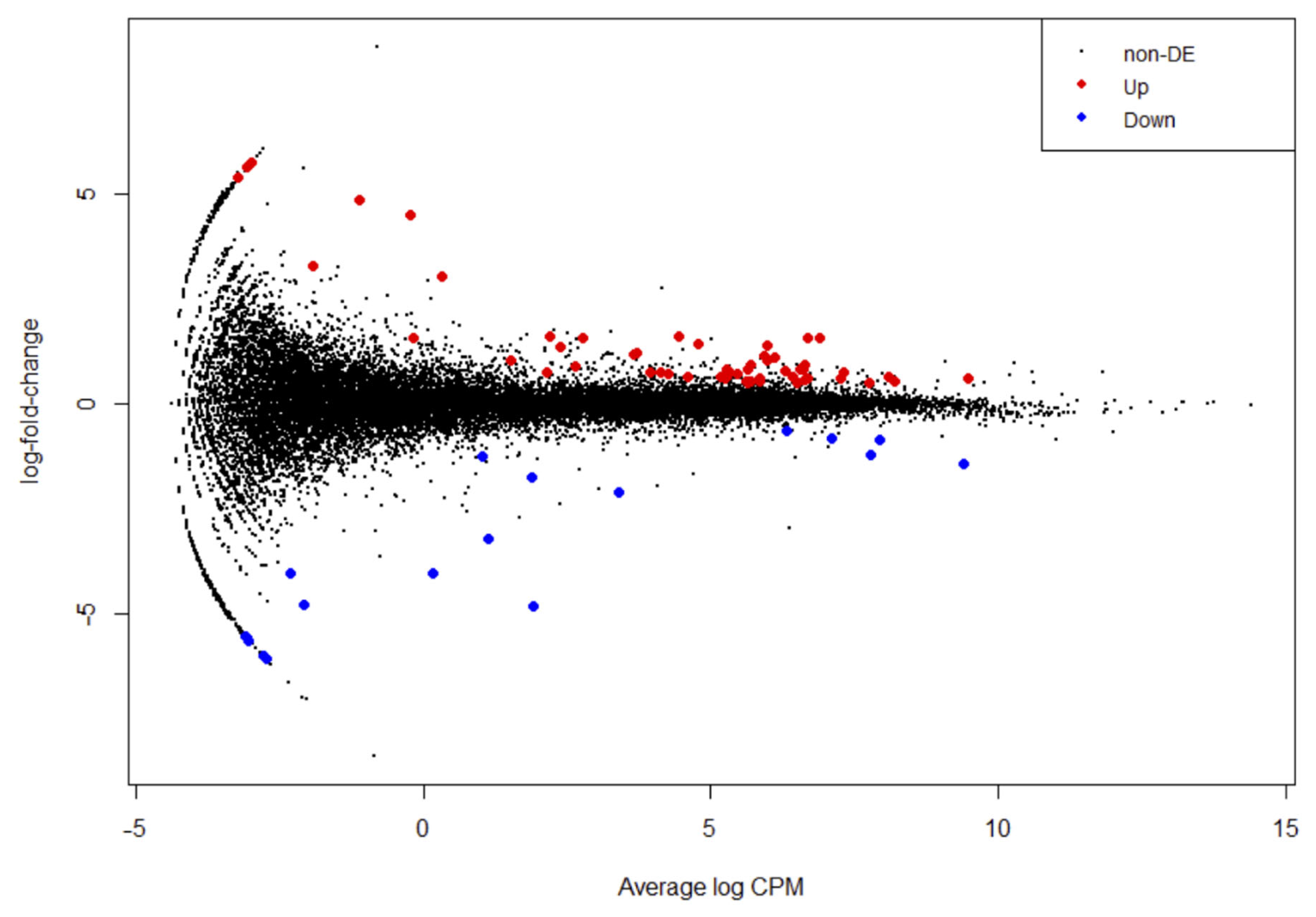
3.2. Differential Expression Analysis
3.3. GO Analysis of DEGs after CAstV Infection
3.4. Pathway Enrichment after CAstV Infection in the Chicken Spleen
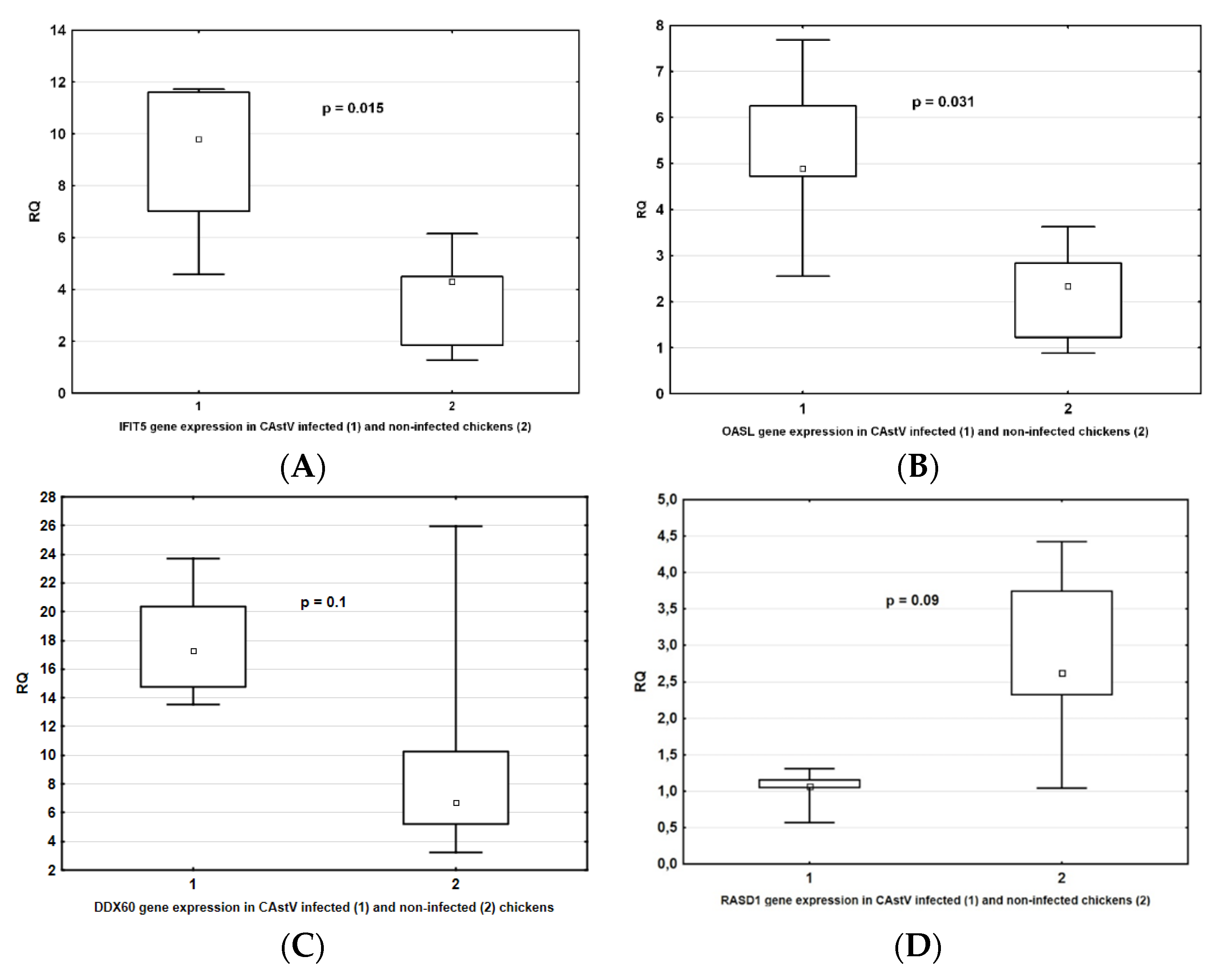
3.5. Verification of DEGs by qRT-PCR
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Ulloa, J.C.; Gutiérrez, M.F. Genomic analysis of two ORF2 segments of new porcine astrovirus isolates and their close relationship with human astroviruses. Can. J. Microbiol. 2010, 56, 569–577. [Google Scholar] [CrossRef]
- Domańska-Blicharz, K.; Lisowska, A.; Jacukowicz, A.; Pikuła, A.; Minta, Z. Cross-sectional survey of selected enteric viruses in Polish turkey flocks between 2008 and 2011. BMC Veter-Res. 2017, 13, 1–10. [Google Scholar] [CrossRef] [PubMed]
- Smyth, V.J. A Review of the Strain Diversity and Pathogenesis of Chicken Astrovirus. Viruses 2017, 9, 29. [Google Scholar] [CrossRef]
- Meliopoulos, V.A.; Kayali, G.; Burnham, A.; Oshansky, C.M.; Thomas, P.G.; Gray, G.; Beck, M.A.; Schultz-Cherry, S. Detection of Antibodies against Turkey Astrovirus in Humans. PLoS ONE 2014, 9, e96934. [Google Scholar] [CrossRef]
- International Committee on Taxonomy of Viruses. ICTV Virus Taxononomy: 2019 Release. Available online: http://ictvonline.org/proposals/2010.017acV.A.v3.Avastrovirus.pdf (accessed on 3 March 2021).
- Shirai, J.; Nakamura, K.; Nozaki, H.; Kawamura, H. Differences in the Induction of Urate Deposition of Specific-Pathogen-Free Chicks Inoculated with Avian Nephritis Virus Passaged by Five Different Methods. Avian Dis. 1991, 35, 269. [Google Scholar] [CrossRef]
- Bulbule, N.R.; Mandakhalikar, K.D.; Kapgate, S.S.; Deshmukh, V.V.; Schat, K.A.; Chawak, M.M. Role of chicken astrovirus as a causative agent of gout in commercial broilers in India. Avian Pathol. 2013, 42, 464–473. [Google Scholar] [CrossRef]
- McNulty, M.; Allan, G.; Connor, T.; McFerran, J.; McCracken, R. An entero?like virus associated with the runting syndrome in broiler chickens. Avian Pathol. 1984, 13, 429–439. [Google Scholar] [CrossRef]
- Spackman, D.; Gough, R.E.; Collins, M.S.; Lanning, D. Isolation of an enterovirus-like agent from the meconium of dead-in-shell chicken embryos. Veter-Rec. 1984, 114, 216–218. [Google Scholar] [CrossRef] [PubMed]
- Decaesstecker, M.; Charlier, G.; Meulemans, G. Significance of parvoviruses, enterolike viruses and reoviruses in the aetiology of the chicken malabsorption syndrome. Avian Pathol. 1986, 15, 769–782. [Google Scholar] [CrossRef] [PubMed]
- Smyth, J.A.; Connor, T.J.; McNeilly, F.; Moffet, D.A.; Calvert, V.M.; McNulty, M.S. Studies on the pathogenicity of enterovirus-like viruses in chickens. Avian Pathol. 2007, 36, 119–126. [Google Scholar] [CrossRef]
- Oluwayelu, D.O.; Todd, D.; Ball, N.W.; Scott, A.N.J.; Oladele, O.A.; Emikpe, B.; Fagbohun, O.A.; Owoade, A.A.; Olaleye, O.D. Isolation and Preliminary Characterization of Chicken Anemia Virus from Chickens in Nigeria. Avian Dis. 2005, 49, 446–450. [Google Scholar] [CrossRef] [PubMed]
- French, D.; Stayer, P.; Riley, E.; Vanhooser, S.; Ferro, P. Impact of astrovirus challenge on a commercial broiler breeder flock and subsequent progeny. In Proceedings of the 153rd Annual Meeting of the American Veterinary Medical Association, San Antonio, TX, USA, 6–9 September 2016; p. 7. [Google Scholar]
- Long, K.E.; Hastie, G.M.; Ojkić, D.; Brash, M.L. Economic Impacts of White Chick Syndrome in Ontario, Canada. Avian Dis. 2017, 61, 402–408. [Google Scholar] [CrossRef]
- Nuñez, L.F.N.; Parra, S.H.S.; Mettifogo, E.; Catroxo, M.H.B.; Astolfi-Ferreira, C.; Ferreira, A.J.P. Isolation of chicken astrovirus from specific pathogen-free chicken embryonated eggs. Poult. Sci. 2015, 94, 947–954. [Google Scholar] [CrossRef] [PubMed]
- Sajewicz-Krukowska, J.; Pać, K.; Lisowska, A.; Pikuła, A.; Minta, Z.; Króliczewska, B.; Domańska-Blicharz, K. Astrovirus-induced ‘‘white chicks’’ condition—Field observation, virus detection, and preliminary characterization. Avian Pathol. 2016, 45, 2–12. [Google Scholar] [CrossRef]
- Smyth, V.J.; Jewhurst, H.L.; Adair, B.M.; Todd, D. Detection of chicken astrovirus by reverse transcriptase-polymerase chain reaction. Avian Pathol. 2009, 38, 293–299. [Google Scholar] [CrossRef] [PubMed]
- Long, K.E.; Ouckama, R.M.; Weisz, A.; Brash, M.L.; Ojkic, D. White Chick Syndrome Associated with Chicken Astrovirus in Ontario, Canada. Avian Dis. 2018, 62, 247–258. [Google Scholar] [CrossRef]
- Sajewicz-Krukowska, J.; Domanska-Blicharz, K. Nearly full-length genome sequence of a novel astrovirus isolated from chickens with ‘white chicks’ condition. Arch. Virol. 2016, 161, 2581–2587. [Google Scholar] [CrossRef]
- Kato, H.; Takeuchi, O.; Sato, S.; Yoneyama, M.; Yamamoto, M.; Matsui, K.; Uematsu, S.; Jung, A.; Kawai, T.; Ishii, K.; et al. Differential roles of MDA5 and RIG-I helicases in the recognition of RNA viruses. Nature 2006, 441, 101–105. [Google Scholar] [CrossRef]
- Wang, J.; Kurt-Jones, E.A.; Finberg, R.W. Innate immunity to respiratory viruses. Cell. Microbiol. 2007, 9, 1641–1646. [Google Scholar] [CrossRef]
- Loo, Y.-M.; Fornek, J.; Crochet, N.; Bajwa, G.; Perwitasari, O.; Martinez-Sobrido, L.; Akira, S.; Gill, M.A.; Garcia-Sastre, A.; Katze, M.G.; et al. Distinct RIG-I and MDA5 Signaling by RNA Viruses in Innate Immunity. J. Virol. 2008, 82, 335–345. [Google Scholar] [CrossRef]
- Ehrhardt, C.; Seyer, R.; Hrincius, E.R.; Eierhoff, T.; Wolff, T.; Ludwig, S. Interplay between influenza A virus and the innate immune signaling. Microbes Infect. 2010, 12, 81–87. [Google Scholar] [CrossRef]
- Yilmaz, A.; Shen, S.; Adelson, D.; Xavier, S.; Zhu, J.J. Identification and sequence analysis of chicken Toll-like receptors. Immunogenetics 2004, 56, 743–753. [Google Scholar] [CrossRef]
- Yu, S.; Mao, H.; Jin, M.; Lin, X. Transcriptomic Analysis of the Chicken MDA5 Response Genes. Genes 2020, 11, 308. [Google Scholar] [CrossRef] [PubMed]
- Yoneyama, M.; Kikuchi, M.; Matsumoto, K.; Imaizumi, T.; Miyagishi, M.; Taira, K.; Foy, E.; Loo, Y.M.; Gale, M., Jr.; Akira, S.; et al. Shared and unique functions of the DExD/H-box helicases RIG-I, MDA5, and LGP2 in antiviral innate immunity. J. Immunol. 2005, 175, 2851–2858. [Google Scholar] [CrossRef] [PubMed]
- Komuro, A.; Horvath, C.M. RNA- and Virus-Independent Inhibition of Antiviral Signaling by RNA Helicase LGP2. J. Virol. 2006, 80, 12332–12342. [Google Scholar] [CrossRef]
- Takeuchi, O.; Akira, S. Recognition of viruses by innate immunity. Immunol. Rev. 2007, 220, 214–224. [Google Scholar] [CrossRef] [PubMed]
- Takeuchi, O.; Akira, S. Pattern Recognition Receptors and Inflammation. Cell 2010, 140, 805–820. [Google Scholar] [CrossRef]
- Kato, H.; Takeuchi, O.; Mikamo-Satoh, E.; Hirai, R.; Kawai, T.; Matsushita, K.; Hiiragi, A.; Dermody, T.S.; Fujita, T.; Akira, S. Length-dependent recognition of double-stranded ribonucleic acids by retinoic acid–inducible gene-I and melanoma differentiation–associated gene 5. J. Exp. Med. 2008, 205, 1601–1610. [Google Scholar] [CrossRef]
- Gitlin, L.; Benoit, L.; Song, C.; Cella, M.; Gilfillan, S.; Holtzman, M.J.; Colonna, M. Melanoma Differentiation-Associated Gene 5 (MDA5) Is Involved in the Innate Immune Response to Paramyxoviridae Infection In Vivo. PLOS Pathog. 2010, 6, e1000734. [Google Scholar] [CrossRef]
- Yu, L.; Zhang, X.; Wu, T.; Su, J.; Wang, Y.; Wang, Y.; Baoyang, R.; Xiaosai, N.; Yantao, W. Avian infectious bronchitis virus disrupts the melanoma differentiation associated gene 5 (MDA5) signaling pathway by cleavage of the adaptor protein MAVS. BMC Vet. Res. 2017, 13, 332. [Google Scholar] [CrossRef]
- Smyth, V.J.; Jewhurst, H.L.; Wilkinson, D.S.; Adair, B.M.; Gordon, A.W.; Todd, D. Development and evaluation of real-time TaqMan(R) RT-PCR assays for the detection of avian nephritis virus and chicken astrovirus in chickens. Avian Pathol. 2010, 39, 467–474. [Google Scholar] [CrossRef] [PubMed]
- Andrews, S. FastQC: A Quality Control TOOL for High Throughput Sequence Data. 2010. Available online: http://www.bioinformatics.babraham.ac.uk/projects/fastqc (accessed on 2 February 2021).
- Bolger, A.M.; Lohse, M.; Usadel, B. Trimmomatic: A flexible trimmer for Illumina sequence data. Bioinformatics 2014, 30, 2114–2120. [Google Scholar] [CrossRef] [PubMed]
- Dobin, A.; Davis, C.A.; Schlesinger, F.; Drenkow, J.; Zaleski, C.; Jha, S.; Batut, P.; Chaisson, M.; Gingeras, T.R. STAR: Ultrafast universal RNA-seq aligner. Bioinformatics 2013, 29, 15–21. [Google Scholar] [CrossRef]
- Pertea, M.; Pertea, G.M.; Antonescu, C.M.; Chang, T.-C.; Mendell, J.T.; Salzberg, S.L. StringTie enables improved reconstruction of a transcriptome from RNA-seq reads. Nat. Biotechnol. 2015, 33, 290–295. [Google Scholar] [CrossRef]
- Fu, J.; Frazee, A.C.; Collado-Torres, L.; Jaffe, A.E.; Leek, J.T. Ballgown: Flexible, Isoform-Level Differential EXPRESSION Analysis. R Package Version 2.16.0; Biorxiv 003665; 2014. Available online: https://rdrr.io/bioc/ballgown/ (accessed on 2 February 2021).
- Love, M.I.; Huber, W.; Anders, S. Moderated estimation of fold change and dispersion for RNA-seq data with DESeq2. Genome Biol. 2014, 15, 550. [Google Scholar] [CrossRef] [PubMed]
- Bioconductor. Open Source Software for Bioinformatics. Available online: https://bioconductor.org (accessed on 3 February 2021).
- g:Profiler. Available online: https://biit.cs.ut.ee/gprofiler/index.cgi (accessed on 5 February 2021).
- The Gene Ontology Home Page. Available online: http://geneontology.org/ (accessed on 1 August 2012).
- KEGG. Available online: http://www.genome.jp/kegg/ (accessed on 10 January 2009).
- Cong, F.; Liu, X.; Han, Z.; Shao, Y.; Kong, X.; Liu, S. Transcriptome analysis of chicken kidney tissues following coronavirus avian infectious bronchitis virus infection. BMC Genom. 2013, 14, 743. [Google Scholar] [CrossRef]
- Vora, P.; Youdim, A.; Thomas, L.S.; Fukata, M.; Tesfay, S.Y.; Lukasek, K.; Michelsen, K.S.; Wada, A.; Hirayama, T.; Arditi, M.; et al. Beta-defensin-2 expression is regulated by TLR signaling in intestinal epithelial cells. J. Immunol. 2004, 173, 5398–5405. [Google Scholar] [CrossRef]
- Nuñez, L.F.N.; Santander-Parra, S.H.; Kyriakidis, N.C.; Astolfi-Ferreira, C.S.; Buim, M.R.; De La Torre, D.; Ferreira, A.J.P. Molecular Characterization and Determination of Relative Cytokine Expression in Naturally Infected Day-Old Chicks with Chicken Astrovirus Associated to White Chick Syndrome. Animals 2020, 10, 1195. [Google Scholar] [CrossRef] [PubMed]
- Smyth, V.J.; Trudgett, J.; Wylie, M. Chicken astrovirus detected in hatchability problems associated with “white chicks”. Vet. Rec. 2013, 173, 403–404. [Google Scholar] [CrossRef]
- Wang, X.; Zhang, J.; Meng, R.; Jiang, Y.; Liang, S.; Zhang, Y.; Xie, M.; Zhou, Z.; Hou, S. Host Differences Affecting Resistance and Susceptibility of the Second Generation of a Pekin Duck Flock to Duck Hepatitis A Virus Genotype 3. Front. Microbiol. 2017, 8, 1128. [Google Scholar] [CrossRef]
- Wang, Q.; Liu, M.; Xu, L.; Wu, Y.; Huang, Y. Transcriptome analysis reveals the molecular mechanism of hepatic fat metabolism disorder caused by Muscovy duck reovirus infection. Avian Pathol. 2017, 47, 127–139. [Google Scholar] [CrossRef] [PubMed]
- Yan, L.; Qu, S.; Liu, G.; Liu, L.; Yu, Y.; Ding, G.; Zhao, Y.; Li, Y.; Xie, Y.; Zhang, J.; et al. Comparative Transcriptomic Analysis of Primary Duck Hepatocytes Provides Insight into Differential Susceptibility to DHBV Infection. PLoS ONE 2016, 11, e0149702. [Google Scholar] [CrossRef][Green Version]
- Wang, Y.; Lupiani, B.; Reddy, S.M.; Lamont, S.J.; Zhou, H. RNA-seq analysis revealed novel genes and signaling pathway associated with disease resistance to avian influenza virus infection in chickens. Poult. Sci. 2014, 93, 485–493. [Google Scholar] [CrossRef]
- Liu, H.; Yang, X.; Zhang, Z.; Li, J.; Zou, W.; Zeng, F.; Wang, H. Comparative transcriptome analysis reveals induction of apoptosis in chicken kidney cells associated with the virulence of nephropathogenic infectious bronchitis virus. Microb. Pathog. 2017, 113, 451–459. [Google Scholar] [CrossRef]
- Ou, C.; Wang, Q.; Zhang, Y.; Kong, W.; Zhang, S.; Yu, Y.; Ma, J.; Liu, X.; Kong, X. Transcription profiles of the responses of chicken bursae of Fabricius to IBDV in different timing phases. Virol. J. 2017, 14, 1–10. [Google Scholar] [CrossRef]
- Koci, M.D.; Kelley, L.A.; Larsen, D.; Schultz-Cherry, S. Astrovirus-Induced Synthesis of Nitric Oxide Contributes to Virus Control during Infection. J. Virol. 2004, 78, 1564–1574. [Google Scholar] [CrossRef]
- Meyerhoff, R.; Nighot, P.K.; Ali, R.A.; Blikslager, A.; Koci, M.D. Characterization of turkey inducible nitric oxide synthase and identification of its expression in the intestinal epithelium following astrovirus infection. Comp. Immunol. Microbiol. Infect. Dis. 2012, 35, 63–69. [Google Scholar] [CrossRef] [PubMed]
- Olah, I.; Vervelde, L. Structure of the avian lymphoid system. In Avian Immunol; Schat, K.A., Kaspers, B., Kaiser, P., Eds.; Elsevier Academic Press Inc: Amsterdam, The Netherlands, 2014; pp. 11–44. [Google Scholar]
- Monson, M.S. Hepatotoxic and Immunomodulatory Transcriptome Responses to Aflatoxin B1 in the Turkey (Meleagris gallopavo). Ph.D. Thesis, University of Minnesota, Minneapolis, MN, USA, 2015. [Google Scholar]
- El-Diwany, R.; Soliman, M.; Sugawara, S.; Breitwieser, F.; Skaist, A.; Coggiano, C.; Sangal, N.; Chattergoon, M.; Bailey, J.R.; Siliciano, R.F.; et al. CMPK2 and BCL-G are associated with type 1 interferon–induced HIV restriction in humans. Sci. Adv. 2018, 4, eaat0843. [Google Scholar] [CrossRef] [PubMed]
- Oshiumi, H.; Miyashita, M.; Okamoto, M.; Morioka, Y.; Okabe, M.; Matsumoto, M.; Seya, T. DDX60 Is Involved in RIG-I-Dependent and Independent Antiviral Responses, and Its Function Is Attenuated by Virus-Induced EGFR Activation. Cell Rep. 2015, 11, 1193–1207. [Google Scholar] [CrossRef] [PubMed]
- Wu, X.; Liu, K.; Jia, R.; Pan, Y.; Wang, M.; Chen, S.; Liu, M.; Zhu, D.; Zhao, X.; Wu, Y.; et al. Duck IFIT5 differentially regulates Tembusu virus replication and inhibits virus-triggered innate immune response. Cytokine 2020, 133, 155161. [Google Scholar] [CrossRef]
- Rong, E.; Hu, J.; Yang, C.; Chen, H.; Wang, Z.; Liu, X.; Liu, W.; Lu, C.; He, P.; Wang, X.; et al. Broad-spectrum antiviral functions of duck interferon-induced protein with tetratricopeptide repeats (AvIFIT). Dev. Comp. Immunol. 2018, 84, 71–81. [Google Scholar] [CrossRef] [PubMed]
- Zhu, J.; Ghosh, A.; Sarkar, S.N. OASL—A new player in controlling antiviral innate immunity. Curr. Opin. Virol. 2015, 12, 15–19. [Google Scholar] [CrossRef] [PubMed]
- Ren, D.; Li, T.; Zhang, X.; Yao, X.; Gao, W.; Xie, Q.; Zhang, J.; Shao, H.; Wan, Z.; Qin, A.; et al. OASL triggered by novel goose astrovirusvia ORF2 restricts its replication. J. Virol. 2020, 94, e01767-20. [Google Scholar] [CrossRef]
- Korpela, J. Avidin, a high affinity biotin-binding protein, as a tool and subject of biological research. Med. Boil. 1984, 62, 5–26. [Google Scholar]
- Green, N.M. Avidin. Adv. Prot. Chem. 1975, 29, 85. [Google Scholar]
- Ly-Chatain, M.H.; Moussaoui, S.; Vera, A.; Rigobello, V.; Demarigny, Y. Antiviral effect of cationic compounds on bacteriophages. Front. Microbiol. 2013, 4, 46. [Google Scholar] [CrossRef]
- Villa, T.; Siota, L.F.; Rama, J.L.R.; Ageitos, J. Antivirals against animal viruses. Biochem. Pharmacol. 2016, 133, 97–116. [Google Scholar] [CrossRef]
- Schanoski, A.S.; Le, T.T.; Kaiserman, D.; Rowe, C.; Prow, N.A.; Barboza, D.D.; Santos, C.A.; Zanotto, P.M.A.; Magalhães, K.G.; Aurelio, L.; et al. Granzyme A in Chikungunya and Other Arboviral Infections. Front. Immunol. 2020, 10, 3083. [Google Scholar] [CrossRef]
- Zhong, C.; Li, C.; Wang, X.; Toyoda, T.; Gao, G.; Fan, Z. Granzyme K inhibits replication of influenza virus through cleaving the nuclear transport complex importin α1/β dimer of infected host cells. Cell Death Differ. 2012, 19, 882–890. [Google Scholar] [CrossRef]
- Cheriyath, V.; Glaser, K.B.; Waring, J.F.; Baz, R.; Hussein, M.A.; Borden, E.C. G1P3, an IFN-induced survival factor, antagonizes TRAIL-induced apoptosis in human myeloma cells. J. Clin. Investig. 2007, 117, 3107–3117. [Google Scholar] [CrossRef]
- Schoggins, J.W.; Wilson, S.J.; Panis, M.; Murphy, M.Y.; Jones, C.T.; Bieniasz, P.; Rice, C.M. A diverse range of gene products are effectors of the type I interferon antiviral response. Nature 2011, 472, 481–485. [Google Scholar] [CrossRef]
- Li, J.; Ding, S.C.; Cho, H.; Chung, B.C.; Gale, M., Jr.; Chanda, S.K.; Diamond, M.S. A short hairpin RNA screen of interfer-on-stimulated genes identifies a novel negative regulator of the cellular antiviral response. MBio 2013, 4, e00385-13. [Google Scholar] [CrossRef]
- Bitoun, E.; Micheloni, A.; Lamant, L.; Bonnart, C.; Tartaglia-Polcini, A.; Cobbold, C.; Al Saati, T.; Mariotti, F.; Mazereeuw-Hautier, J.; Boralevi, F.; et al. LEKTI proteolytic processing in human primary keratinocytes, tissue distribution and defective expression in Netherton syndrome. Hum. Mol. Genet. 2003, 12, 2417–2430. [Google Scholar] [CrossRef]
- Lee, J.Y. Host-Virus Interactions of Infectious Laryngotracheitis Virus Infection in Cultured Cells. Ph.D. Thesis, University of Arkansas, Fayetteville, AR, USA, 2011. [Google Scholar]
- Bourin, M.; Gautron, J.; Berges, M.; Attucci, S.; Le Blay, G.; Labas, V.; Nys, Y.; Rehault-Godbert, S. Antimicrobial Potential of Egg Yolk Ovoinhibitor, a Multidomain Kazal-like Inhibitor of Chicken Egg. J. Agric. Food Chem. 2011, 59, 12368–12374. [Google Scholar] [CrossRef] [PubMed]
- Beck, M.A.; Handy, J.; Levander, O.A. Host nutritional status: The neglected virulence factor. Trends Microbiol. 2004, 12, 417–423. [Google Scholar] [CrossRef] [PubMed]
- Steinbrenner, H.; Al-Quraishy, S.; Dkhil, M.; Wunderlich, F.; Sies, H. Dietary Selenium in Adjuvant Therapy of Viral and Bacterial Infections. Adv. Nutr. 2015, 6, 73–82. [Google Scholar] [CrossRef]
- Wang, Y.; Huang, J.; Sun, Y.; He, J.; Li, W.; Liu, Z.; Taylor, E.W.; Rayman, M.P.; Wan, X.; Zhang, J. SARS-CoV-2 suppresses mRNA expression of selenoproteins associated with ferroptosis, endoplasmic reticulum stress and DNA synthesis. Food Chem Toxicol. 2021, 153, 112286. [Google Scholar] [CrossRef] [PubMed]
- Murai, K.; Honda, M.; Shirasaki, T.; Shimakami, T.; Omura, H.; Misu, H.; Kita, Y.; Takeshita, Y.; Ishii, K.-A.; Takamura, T.; et al. Induction of Selenoprotein P mRNA during Hepatitis C Virus Infection Inhibits RIG-I-Mediated Antiviral Immunity. Cell Host Microbe 2019, 25, 588–601.e7. [Google Scholar] [CrossRef]
- Creagh, E.; Sheehan, D.; Cotter, T. Heat shock proteins—Modulators of apoptosis in tumour cells. Leukemia 2000, 14, 1161–1173. [Google Scholar] [CrossRef]
- Reyes-del Valle, J.; Chávez-Salinas, S.; Medina, F.; del Angel, R.M. Heat Shock Protein 90 and Heat Shock Protein 70 Are Components of Dengue Virus Receptor Complex in Human Cells. J. Virol. 2005, 79, 4557–4567. [Google Scholar] [CrossRef] [PubMed]
- Liu, J.-S.; Kuo, S.-R.; Makhov, A.M.; Cyr, D.M.; Griffith, J.D.; Broker, T.R.; Chow, L.T. Human Hsp70 and Hsp40 Chaperone Proteins Facilitate Human Papillomavirus-11 E1 Protein Binding to the Origin and Stimulate Cell-free DNA Replication. J. Biol. Chem. 1998, 273, 30704–30712. [Google Scholar] [CrossRef] [PubMed]
- Chen, Y.-J.; Chen, Y.-H.; Chow, L.-P.; Tsai, Y.-H.; Chen, P.-H.; Huang, C.-Y.F.; Chen, W.-T.; Hwang, L.-H. Heat Shock Protein 72 Is Associated with the Hepatitis C Virus Replicase Complex and Enhances Viral RNA Replication. J. Biol. Chem. 2010, 285, 28183–28190. [Google Scholar] [CrossRef]
- Weeks, S.A.; Miller, D.J. The Heat Shock Protein 70 Cochaperone YDJ1 Is Required for Efficient Membrane-Specific Flock House Virus RNA Replication Complex Assembly and Function in Saccharomyces cerevisiae. J. Virol. 2008, 82, 2004–2012. [Google Scholar] [CrossRef][Green Version]
- Livingston, C.M.; DeLuca, N.A.; Wilkinson, D.E.; Weller, S.K. Oligomerization of ICP4 and Rearrangement of Heat Shock Proteins May Be Important for Herpes Simplex Virus Type 1 Prereplicative Site Formation. J. Virol. 2008, 82, 6324–6336. [Google Scholar] [CrossRef]
- Gao, S.; Jin, L.; Liu, G.; Wang, P.; Sun, Z.; Cao, Y.; Shi, H.; Liu, X.; Shi, Q.; Zhou, X.; et al. Overexpression of RASD1 inhibits glioma cell migration/invasion and inactivates the AKT/mTOR signaling pathway. Sci. Rep. 2017, 7, 1–12. [Google Scholar] [CrossRef]
- Cheng, Z.; Guo, J.; Chen, L.; Luo, N.; Yang, W.; Qu, X. Overexpression of TMEM158 contributes to ovarian carcinogenesis. J. Exp. Clin. Cancer Res. 2015, 34, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Nieto, M.; Barradas, M.; Criado, L.M.; Flores, J.M.; Serrano, M.; Llano, E. Normal cellular senescence and cancer susceptibility in mice genetically deficient in Ras-induced senescence-1 (Ris1). Oncogene 2007, 26, 1673–1680. [Google Scholar] [CrossRef][Green Version]
- Ji, G.; Li, Y.; Tan, F.; Zhuang, J.; Li, X.; Tian, K. Complete Genome Sequence of an NADC30-Like Strain of Porcine Reproductive and Respiratory Syndrome Virus in China. Genome Announc. 2016, 4, e00303-16. [Google Scholar] [CrossRef] [PubMed]
- van Hemert, M.; Steensma, H.Y.; Van Heusden, G.P.H. 14-3-3 proteins: Key regulators of cell division, signalling and apoptosis. BioEssays 2001, 23, 936–946. [Google Scholar] [CrossRef]
- Nathan, K.G.; Lal, S.K. The Multifarious Role of 14-3-3 Family of Proteins in Viral Replication. Viruses 2020, 12, 436. [Google Scholar] [CrossRef]
- Chan, Y.K.; Gack, M.U. A phosphomimetic-based mechanism of dengue virus to antagonize innate immunity. Nat. Immunol. 2016, 17, 523–530. [Google Scholar] [CrossRef]
- Surjit, M.; Kumar, R.; Mishra, R.N.; Reddy, M.K.; Chow, V.T.K.; Lal, S.K. The Severe Acute Respiratory Syndrome Coronavirus Nucleocapsid Protein Is Phosphorylated and Localizes in the Cytoplasm by 14-3-3-Mediated Translocation. J. Virol. 2005, 79, 11476–11486. [Google Scholar] [CrossRef]
- Liu, H.M.; Loo, Y.-M.; Horner, S.M.; Zornetzer, G.A.; Katze, M.G.; Gale, M., Jr. The Mitochondrial Targeting Chaperone 14-3-3ε Regulates a RIG-I Translocon that Mediates Membrane Association and Innate Antiviral Immunity. Cell Host Microbe 2012, 11, 528–537. [Google Scholar] [CrossRef]
- Fan, Y.; Sanyal, S.; Bruzzone, R. Breaking Bad: How Viruses Subvert the Cell Cycle. Front. Cell. Infect. Microbiol. 2018, 8, 396. [Google Scholar] [CrossRef]
- Emmett, S.R.; Dove, B.; Mahoney, L.; Wurm, T.; Hiscox, J.A. The Cell Cycle and Virus Infection. Methods Mol. Biol. 2004, 296, 197–218. [Google Scholar] [CrossRef]
- Naniche, D.; Reed, S.I.; Oldstone, M.B.A. Cell Cycle Arrest during Measles Virus Infection: A G 0 -Like Block Leads to Suppression of Retinoblastoma Protein Expression. J. Virol. 1999, 73, 1894–1901. [Google Scholar] [CrossRef] [PubMed]
- Lin, G.Y.; Lamb, R.A. The Paramyxovirus Simian Virus 5 V Protein Slows Progression of the Cell Cycle. J. Virol. 2000, 74, 9152–9166. [Google Scholar] [CrossRef][Green Version]
- Chen, H.; Wurm, T.; Britton, P.; Brooks, G.; Hiscox, J.A. Interaction of the Coronavirus Nucleoprotein with Nucleolar Antigens and the Host Cell. J. Virol. 2002, 76, 5233–5250. [Google Scholar] [CrossRef]
- Song, L.; Han, X.; Jia, C.; Zhang, X.; Jiao, Y.; Du, T.; Xiao, S.; Hiscox, J.A.; Zhou, E.M.; Mu, Y. Porcine reproductive and respiratory syndrome virus inhibits MARC-145 proliferation via inducing apoptosis and G2/M arrest by activation of Chk/Cdc25C and p53/p21 pathway. Virol. J. 2018, 15, 169. [Google Scholar] [CrossRef] [PubMed]
- Sheppard, K.E.; Pearson, R.B.; Hannan, R.D. Unexpected role of CDK4 in a G2/M checkpoint. Cell Cycle 2015, 14, 1351–1352. [Google Scholar] [CrossRef] [PubMed]
- Koci, M.D.; Moser, L.A.; Kelley, L.A.; Larsen, D.; Brown, C.C.; Schultz-Cherry, S. Astrovirus Induces Diarrhea in the Absence of Inflammation and Cell Death. J. Virol. 2003, 77, 11798–11808. [Google Scholar] [CrossRef]
- Qureshi, M.A.; Yu, M.; Saif, Y.M. A Novel “Small Round Virus” Inducing Poult Enteritis and Mortality Syndrome and Associated Immune Alterations. Avian Dis. 2000, 44, 275–283. [Google Scholar] [CrossRef] [PubMed]
- Qureshi, M.A.; Saif, Y.M.; Heggen-Peay, C.L.; Edens, F.W.; Havenstein, G.B. Induction of functional defects in macrophages by a poult enteritis and mortality syndrome-associated turkey astrovirus. Avian Dis. 2001, 45, 853. [Google Scholar] [CrossRef] [PubMed]
- Xie, J.; Zhang, S.; Hu, Y.; Li, D.; Cui, J.; Xue, J.; Zhang, G.; Khachigian, L.; Wong, J.; Sun, L.; et al. Regulatory roles of c-jun in H5N1 influenza virus replication and host inflammation. Biochim. Biophys. Acta—Mol. Basis Dis. 2014, 1842, 2479–2488. [Google Scholar] [CrossRef] [PubMed]
- Leppa, S.; Bohmann, D. Diverse functions of JNK signaling and c-Jun in st6ress response and apoptosis. Oncogene 1999, 18, 6158–6162. [Google Scholar] [CrossRef]
- Ludwig, S.; Ehrhardt, C.; Neumeier, E.R.; Kracht, M.; Rapp, U.R.; Pleschka, S. Influenza Virus-induced AP-1-dependent Gene Expression Requires Activation of the JNK Signaling Pathway. J. Biol. Chem. 2001, 276, 10990–10998. [Google Scholar] [CrossRef]
- Ludwig, S. Influenza viruses and MAP kinase cascades—Novel targets for an antiviral intervention? Signal Transduct. 2007, 7, 81–88. [Google Scholar] [CrossRef]
- Koch, C.; Josephsen, J.; Nicolaisen, E.M.; Simonsen, M. Complement mediated lysis in chickens. Dev. Comp. Immunol. 1983, 6, 141–149. [Google Scholar] [CrossRef]
- Asok, K.N.; Umerali, K.; Sabu, T.; Bernet, J.J. In the Crosshairs: RNA Viruses OR Complement? Front. Immunol. 2020, 11, 2315. [Google Scholar]
- Sebire, N.J.; Malone, M.; Shah, N.; Anderson, G.; Gaspar, H.B.; Cubitt, W.D. Pathology of astrovirus associated diarrhoea in a paediatric bone marrow transplant recipient. J. Clin. Pathol. 2004, 57, 1001–1003. [Google Scholar] [CrossRef]
- Bonaparte, R.S.; Hair, P.S.; Banthia, D.; Marshall, D.M.; Cunnion, K.M.; Krishna, N.K. Human Astrovirus Coat Protein Inhibits Serum Complement Activation via C1, the First Component of the Classical Pathway. J. Virol. 2008, 82, 817–827. [Google Scholar] [CrossRef] [PubMed]
- Hair, P.S.; Gronemus, J.Q.; Crawford, K.B.; Salvi, V.P.; Cunnion, K.M.; Thielens, N.M.; Arlaud, G.J.; Rawal, N.; Krishna, N.K. Human astrovirus coat protein binds C1q and MBL and inhibits the classical and lectin pathways of complement activation. Mol. Immunol. 2010, 47, 792–798. [Google Scholar] [CrossRef] [PubMed]
- Arias, C.F.; Dubois, R.M. The Astrovirus Capsid: A Review. Viruses 2017, 9, 15. [Google Scholar] [CrossRef]
- Lachmann, P.J.; Davies, A. Complement and immunity to viruses. Immunol. Rev. 1997, 159, 69–77. [Google Scholar] [CrossRef]
- Tam, J.C.H.; Bidgood, S.R.; McEwan, W.A.; James, L.C. Intracellular sensing of complement C3 activates cell autonomous immunity. Science 2014, 345, 1256070. [Google Scholar] [CrossRef] [PubMed]
- Marvin, S.A. The Immune Response to Astrovirus Infection. Viruses 2016, 9, 1. [Google Scholar] [CrossRef] [PubMed]
- Marvin, S.A.; Huerta, C.T.; Sharp, B.; Freiden, P.; Cline, T.D.; Schultz-Cherry, S. Type I Interferon Response Limits Astrovirus Replication and Protects against Increased Barrier Permeability In Vitro and In Vivo. J. Virol. 2016, 90, 1988–1996. [Google Scholar] [CrossRef]
| Target Gene | Sequence (5′–3′) | References |
|---|---|---|
| OASL | F: AGCACTGGTACAAGGAGATGTTG | Cong et al., 2013 [44] |
| R: CCAAGCAGCTCCAGCACAG | ||
| P: CTGAAGTCCTCCCTGCCTGTGCCCT | ||
| IFIT5 | F: AAAAGAAGGCAAATCATGAGTACC | |
| R: TGATCCTCTATTGATTCTTCCAGAC | ||
| P: AATTCCTTGAAGAACTCCCTGCTGC | ||
| ACTB | F: CATCCTCACCCTGAAGTACC | Vora et al., 2004 [45] |
| R: GCTCATTGTAGAAGGTGTGG | ||
| P: CACGGCATCGTCACCAACTG | ||
| DDX60 | N/A | Thermo Fisher, Gg07198553_m1 |
| RASD1 | N/A | Thermo Fisher, Gg03359818_g1 |
| YWHAB | N/A | Thermo Fisher, Gg03369026_m1 |
| HSPA2 | N/A | Thermo Fisher, Gg03370143_s1 |
| RNA-seq Libraries | Number of Raw Reads (Millions) | Number of Processed Reads (Millions) | Number of Uniquely Mapped Reads (Millions) | Uniquely Mapped Reads (%) |
|---|---|---|---|---|
| 263CAstV4dpi | 31.6 | 27.2 | 24.8 | 91.4 |
| 264CAstV4dpi | 40.4 | 35.0 | 30.8 | 88.3 |
| 265CAstV4dpi | 41.0 | 35.0 | 30.4 | 86.7 |
| 268CAstV4dpi | 39.4 | 33.6 | 30.8 | 91.8 |
| 270CAstV4dpi | 41.2 | 35.2 | 30.8 | 87.5 |
| 276PBS4dpi | 36.2 | 30.8 | 28.0 | 90.7 |
| 277PBS4dpi | 46.6 | 38.6 | 35.6 | 91.8 |
| 278PBS4dpi | 35.4 | 31.8 | 29.2 | 91.7 |
| 279PBS4dpi | 41.4 | 35.2 | 32.0 | 90.9 |
| 280PBS4dpi | 40.6 | 36.0 | 32.8 | 91.4 |
| Description | p-Value | Negative log10 of Adjusted p-Value |
|---|---|---|
| NOD-like receptor signaling pathway | 0.023364421 | 1.631444986 |
| Influenza A | 0.025663115 | 1.590690622 |
| Cell cycle | 0.029423013 | 1.531312861 |
| NOD-like receptor signaling pathway | ENSGALG00000010870,ENSGALG00000017186,ENSGALG00000000720, ENSGALG00000007651,ENSGALG00000001619 |
| Influenza A | ENSGALG00000010870,ENSGALG00000003584,ENSGALG00000007651, ENSGALG00000041192,ENSGALG00000003144 |
| Cell cycle | ENSGALG00000004143,ENSGALG00000005769,ENSGALG00000008233, ENSGALG00000036892,ENSGALG00000010537 |
| Genes | CAstV Infected Chickens | CAstV Non-Infected Chickens | p-Value | ||
|---|---|---|---|---|---|
| RQ Mean ± SD | RQ Median | RQ Mean ± SD | RQ Median | ||
| IFIT5 | 8.9 ± 3.6 | 9.8 | 3.6 ± 2.0 | 4.3 | 0.015 |
| OASL | 5.2 ± 1.9 | 4.9 | 2.2 ± 1.1 | 2.3 | 0.015 |
| DDX60 | 17.9 ± 4.2 | 17.3 | 10.3 ± 9.1 | 6.72 | 0.01 |
| RASD1 | 1.03 ± 0.3 | 1.06 | 2.8 ± 1.3 | 2.62 | 0.09 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Sajewicz-Krukowska, J.; Jastrzębski, J.P.; Grzybek, M.; Domańska-Blicharz, K.; Tarasiuk, K.; Marzec-Kotarska, B. Transcriptome Sequencing of the Spleen Reveals Antiviral Response Genes in Chickens Infected with CAstV. Viruses 2021, 13, 2374. https://doi.org/10.3390/v13122374
Sajewicz-Krukowska J, Jastrzębski JP, Grzybek M, Domańska-Blicharz K, Tarasiuk K, Marzec-Kotarska B. Transcriptome Sequencing of the Spleen Reveals Antiviral Response Genes in Chickens Infected with CAstV. Viruses. 2021; 13(12):2374. https://doi.org/10.3390/v13122374
Chicago/Turabian StyleSajewicz-Krukowska, Joanna, Jan Paweł Jastrzębski, Maciej Grzybek, Katarzyna Domańska-Blicharz, Karolina Tarasiuk, and Barbara Marzec-Kotarska. 2021. "Transcriptome Sequencing of the Spleen Reveals Antiviral Response Genes in Chickens Infected with CAstV" Viruses 13, no. 12: 2374. https://doi.org/10.3390/v13122374
APA StyleSajewicz-Krukowska, J., Jastrzębski, J. P., Grzybek, M., Domańska-Blicharz, K., Tarasiuk, K., & Marzec-Kotarska, B. (2021). Transcriptome Sequencing of the Spleen Reveals Antiviral Response Genes in Chickens Infected with CAstV. Viruses, 13(12), 2374. https://doi.org/10.3390/v13122374








