African Swine Fever: Fast and Furious or Slow and Steady?
Abstract
1. Introduction
2. ASF and Its Spreading Speed
2.1. Basic Reproductive Number (R0)
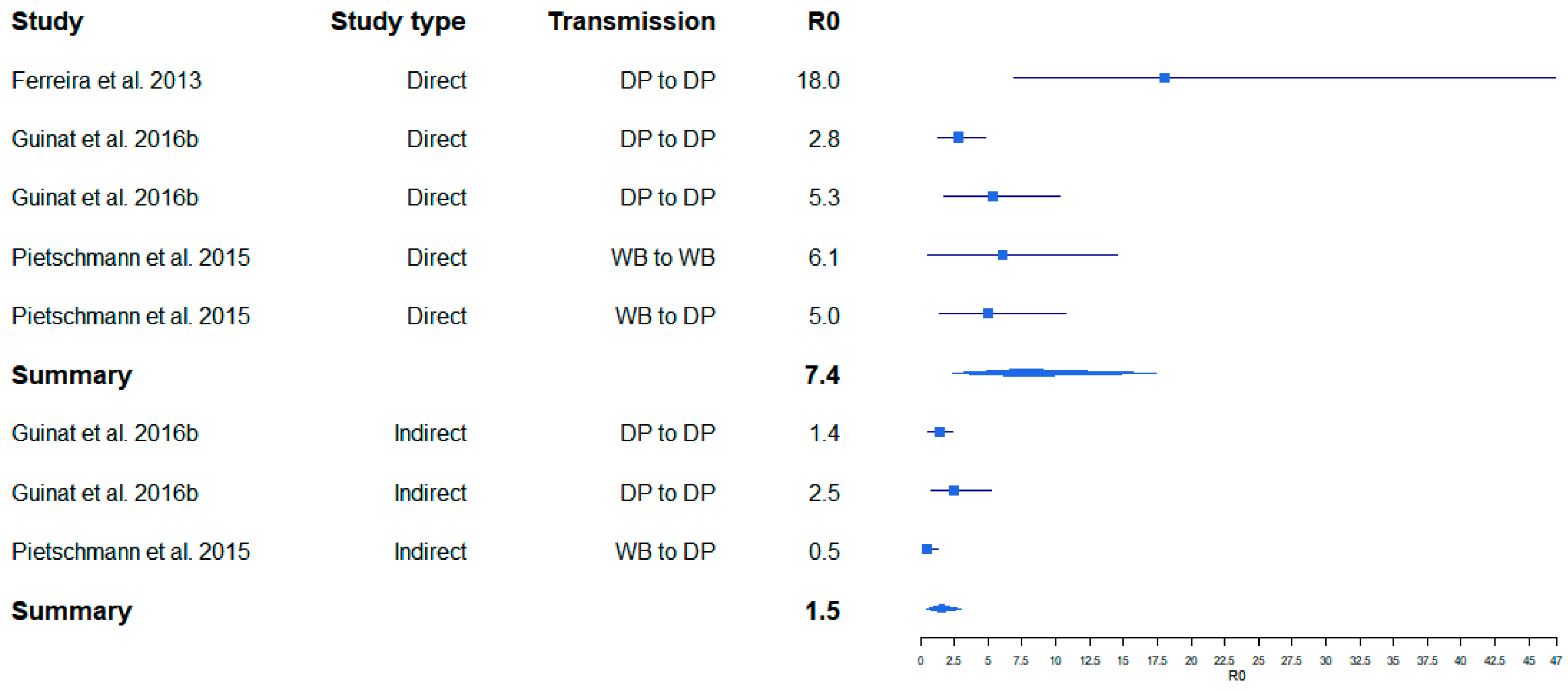
2.2. R0 in ASF Outbreak Situations
2.3. Spatio-Temporal Distribution and Disease Spread
2.4. Spatio-Temporal Distribution and Spread of ASF
2.5. Morbidity in ASF Outbreak Situations
2.6. Mortality and Case Fatality Ratio in ASF
2.7. Infectiousness and Latent Period of ASF
2.8. Infectivity of ASFV
2.9. Contagiousness of ASF
2.10. Virulence of ASFV
2.11. Tenacity or Resistance of ASFV to Environmental Factors
3. Discussion
4. Conclusions
Supplementary Materials
Funding
Conflicts of Interest
References
- Depner, K.; Staubach, C.; Probst, C.; Globig, A.; Blome, S.; Dietze, K.; Sauter-Luis, C.; Conraths, F.J. African Swine fever-epidemiological considerations and consequences for disease control. Tieraerztl. Umschau 2016, 71, 72–78. [Google Scholar]
- Oļševskis, E.; Guberti, V.; Serzants, M.; Westergaard, J.; Gallardo, C.; Rodze, I.; Depner, K. African swine fever virus introduction into the EU in 2014: Experience of Latvia. Res. Vet. Sci. 2016, 105, 28–30. [Google Scholar] [CrossRef] [PubMed]
- Khomenko, S.; Beltrán-Alcrudo, D.; Rozstalnyy, A.; Gogin, A.; Kolbasov, D.; Pinto, J.; Lubroth, J.; Martin, V. African Swine Fever in the Russian Federation: Risk Factors for Europe and Beyond. EMPRES Watch 2013, 28, 1–14. [Google Scholar]
- Chenais, E.; Ståhl, K.; Guberti, V.; Depner, K. Identification of Wild Boar–Habitat Epidemiologic Cycle in African Swine Fever Epizootic. Emerg. Infect. Dis. 2018, 24, 809–811. [Google Scholar] [CrossRef] [PubMed]
- Guinat, C.; Gogin, A.; Blome, S.; Keil, G.; Pollin, R.; Pfeiffer, D.U.; Dixon, L. Transmission routes of African swine fever virus to domestic pigs: current knowledge and future research directions. Vet. Rec. 2016, 178. [Google Scholar] [CrossRef] [PubMed]
- Guinat, C.; Porphyre, T.; Gogin, A.; Dixon, L.; Pfeiffer, D.U.; Gubbins, S. Inferring within-herd transmission parameters for African swine fever virus using mortality data from outbreaks in the Russian Federation. Transbound. Emerg. Dis. 2018, 65, e264–e271. [Google Scholar] [CrossRef] [PubMed]
- Pfeiffer, D.U.; Robinson, T.P.; Stevenson, M.; Stevens, K.B.; Rogers, D.J.; Clements, A.C.A. Spatial Analysis in Epidemiology; Oxford Universtiy Press: Oxford, UK, 2008. [Google Scholar]
- Ward, M.P.; Carpenter, T.E. Techniques for analysis of disease clustering in space and in time in veterinary epidemiology. Prev. Vet. Med. 2000, 45, 257–284. [Google Scholar] [CrossRef]
- Blome, S.; Teifke, J.P. Afrikanische Schweinepest: Was noch nicht im Lehrbuch steht. Amtstierärztlicher Dienst und Lebensmittelkontrolle 2018, 25, 27–34. [Google Scholar]
- Vergne, T.; Cao, C.F.; Li, S.; Cappelle, J.; Edwards, J.; Martin, V.; Pfeiffer, D.U.; Guo, F.S.; Roger, F.L. Pig empire under infectious threat: Risk of African swine fever introduction into the People’s Republic of China. Vet. Rec. 2017, 181. [Google Scholar] [CrossRef] [PubMed]
- Zhou, X.; Li, N.; Luo, Y.; Liu, Y.; Miao, F.; Chen, T.; Zhang, S.; Cao, P.; Li, X.; Tian, K.; et al. Emergence of African Swine Fever in China, 2018. Transbound. Emerg. Dis. 2018, 65, 1482–1484. [Google Scholar] [CrossRef] [PubMed]
- Wang, T.; Sun, Y.; Qiu, H.J. African swine fever: An unprecedented disaster and challenge to China. Infectious Diseases of Poverty 2018, 7. [Google Scholar] [CrossRef] [PubMed]
- Sur, J.-H. How far can African swine fever spread? J. Vet. Sci. 2019, 20. [Google Scholar] [CrossRef] [PubMed]
- Barongo, M.B.; Stahl, K.; Bett, B.; Bishop, R.P.; Fevre, E.M.; Aliro, T.; Okoth, E.; Masembe, C.; Knobel, D.; Ssematimba, A. Estimating the Basic Reproductive Number (R-0) for African Swine Fever Virus (ASFV) Transmission between Pig Herds in Uganda. PLoS ONE 2015, 10. [Google Scholar] [CrossRef] [PubMed]
- Costard, S.; Mur, L.; Lubroth, J.; Sanchez-Vizcaino, J.M.; Pfeiffer, D.U. Epidemiology of African swine fever virus. Virus Res. 2013, 173, 191–197. [Google Scholar] [CrossRef] [PubMed]
- European Food Safety Authority. Scientific Opinion on African swine fever. EFSA J. 2010, 8, 11–13. [Google Scholar]
- Gavier-Widen, D.; Gortazar, C.; Stahl, K.; Neimanis, A.S.; Rossi, S.; Segerstad, C.H.A.; Kuiken, T. African swine fever in wild boar in Europe: A notable challenge. Vet. Rec. 2015, 176, 199–200. [Google Scholar] [CrossRef] [PubMed]
- Gulenkin, V.M.; Korennoy, F.I.; Karaulov, A.K.; Dudnikov, S.A. Cartographical analysis of African swine fever outbreaks in the territory of the Russian Federation and computer modeling of the basic reproduction ratio. Prev. Vet. Med. 2011, 102, 167–174. [Google Scholar] [CrossRef] [PubMed]
- Galindo, I.; Alonso, C. African Swine Fever Virus: A Review. Viruses-Basel 2017, 9. [Google Scholar] [CrossRef]
- Thrusfield, M. Veterinary Epidemiology; John Wiley & Sons Ltd.: Edinburgh, UK, 2018; Volume 4. [Google Scholar]
- Diekmann, O.; Heesterbeek, J.A.P.; Metz, J.A.J. On the definition and the computation of the basic reproduction ratio R0 in models for infectious diseases in heterogeneous populations. J. Math. Biol. 1990, 28, 365–382. [Google Scholar] [CrossRef]
- Sergeant, E.; Perkins, N. Epidemiology for Field Veterinarians; CABI: Croydon, UK, 2015. [Google Scholar]
- Anderson, R.M.; May, R.M. Infectious Diseases of Humans. Dynamics and Control.; Oxford University Press: Oxford, UK, 1992. [Google Scholar]
- Thomas, J.C.; Weber, D.J. Epidemiologic Methods for the Study of Infectious Diseases; Oxford University Press: New York, NY, USA, 2001. [Google Scholar]
- Cross, P.C.; Johnson, P.L.F.; Lloyd-Smith, J.O.; Getz, W.M. Utility of R-0 as a predictor of disease invasion in structured populations. J. R. Soc. 2007, 4, 315–324. [Google Scholar] [CrossRef]
- Korennoy, F.I.; Gulenkin, V.M.; Gogin, A.E.; Vergne, T.; Karaulov, A.K. Estimating the Basic Reproductive Number for African Swine Fever Using the Ukrainian Historical Epidemic of 1977. Transbound. Emerg. Dis. 2017, 64, 1858–1866. [Google Scholar] [CrossRef] [PubMed]
- Pietschmann, J.; Guinat, C.; Beer, M.; Pronin, V.; Tauscher, K.; Petrov, A.; Keil, G.; Blome, S. Course and transmission characteristics of oral low-dose infection of domestic pigs and European wild boar with a Caucasian African swine fever virus isolate. Arch. Virol. 2015, 160, 1657–1667. [Google Scholar] [CrossRef] [PubMed]
- Ferreira, H.C.D.; Backer, J.A.; Weesendorp, E.; Klinkenberg, D.; Stegeman, J.A.; Loeffen, W.L.A. Transmission rate of African swine fever virus under experimental conditions. Vet. Microbiol. 2013, 165, 296–304. [Google Scholar] [CrossRef] [PubMed]
- Hayer, S.S.; VanderWaal, K.; Ranjan, R.; Biswal, J.K.; Subramaniam, S.; Mohapatra, J.K.; Sharma, G.K.; Rout, M.; Dash, B.B.; Das, B.; et al. Foot-and-mouth disease virus transmission dynamics and persistence in a herd of vaccinated dairy cattle in India. Transbound. Emerg. Dis. 2018, 65, e404–e415. [Google Scholar] [CrossRef] [PubMed]
- Eble, P.L.; de Koeijer, A.A.; de Jong, M.C.M.; Engel, B.; Dekker, A. A meta-analysis quantifying transmission parameters of FMDV strain O Taiwan among non-vaccinated and vaccinated pigs. Prev. Vet. Med. 2008, 83, 98–106. [Google Scholar] [CrossRef] [PubMed]
- Ster, I.C.; Dodd, P.J.; Ferguson, N.M. Within-farm transmission dynamics of foot and mouth disease as revealed by the 2001 epidemic in Great Britain. Epidemics 2012, 4, 158–169. [Google Scholar] [CrossRef] [PubMed]
- Guberti, V.; Fenati, M.; O’Flaherty, R.; Rutili, D. The epidemiology of Classical Swine Fever in the wild boar populations of Europe. In Proceedings of the STOP–CSF, International Scientific Conference, Novi Sad, Serbia, 7–8 June 2012; pp. 238–257. [Google Scholar]
- Schulz, K.; Staubach, C.; Blome, S. African and classical swine fever: Similarities, differences and epidemiological consequences. Vet. Res. 2017, 48. [Google Scholar] [CrossRef] [PubMed]
- Klinkenberg, D.; de Bree, J.; Laevens, H.; de Jong, M.C.M. Within- and between-pen transmission of Classical Swine Fever Virus: A new method to estimate the basic reproduction ratio from transmission experiments. Epidemiol. Infect. 2002, 128, 293–299. [Google Scholar] [CrossRef]
- Diggle, P.J. Statistical Analysis of Spatial and Spatio-Temporal Point Patterns; CRC Press: Boca RAton, FL, USA, 2013. [Google Scholar]
- Staubach, C.; Hoffmann, L.; Schmid, V.J.; Ziller, M.; Tackmann, K.; Conraths, F.J. Bayesian space-time analysis of Echinococcus multilocularis-infections in foxes. Vet. Parasitol. 2011, 179, 77–83. [Google Scholar] [CrossRef]
- Nurmoja, I.; Schulz, K.; Staubach, C.; Sauter-Louis, C.; Depner, K.; Conraths, F.J.; Viltrop, A. Development of African swine fever epidemic among wild boar in Estonia—Two different areas in the epidemiological focus. Sci. Rep. 2017, 7, 12562. [Google Scholar] [CrossRef]
- Denzin, N.; Borgwardt, J.; Freuling, C.; Muller, T. Spatio-temporal analysis of the progression of Aujeszky’s disease virus infection in wild boar of Saxony-Anhalt, Germany. Geospat. Health 2013, 8, 203–213. [Google Scholar] [CrossRef]
- Viet, A.F.; Jeanpierre, L.; Bouzid, M.; Mouaddib, A.I. Using Markov Decision Processes to define an adaptive strategy to control the spread of an animal disease. Comput. Electron. Agr. 2012, 80, 71–79. [Google Scholar] [CrossRef]
- Schulz, K.; Staubach, C.; Blome, S.; Viltrop, A.; Nurmoja, I.; Conraths, F.J.; Sauter-Louis, C. Analysis of Estonian surveillance in wild boar suggests a decline in the incidence of African swine fever. Sci. Rep. 2019, 9. [Google Scholar] [CrossRef] [PubMed]
- Lange, M.; Thulke, H.H. Elucidating transmission parameters of African swine fever through wild boar carcasses by combining spatio-temporal notification data and agent-based modelling. Stoch. Environ. Res. Risk Assess. 2017, 31, 379–391. [Google Scholar] [CrossRef]
- Durr, P.A.; Gatrell, A.C. GIS and Spatial Analysis in Veterinary Science; CABI Publishing: Wallingford, UK, 2004. [Google Scholar]
- Dorjee, S.; Revie, C.W.; Poljak, Z.; McNab, W.B.; Sanchez, J. One-Health Simulation Modelling: A Case Study of Influenza Spread between Human and Swine Populations using NAADSM. Transbound. Emerg. Dis. 2016, 63, 36–55. [Google Scholar] [CrossRef] [PubMed]
- Halasa, T.; Willeberg, P.; Christiansen, L.E.; Boklund, A.; AlKhamis, M.; Perez, A.; Enoe, C. Decisions on control of foot-and-mouth disease informed using model predictions. Prev. Vet. Med. 2013, 112, 194–202. [Google Scholar] [CrossRef] [PubMed]
- Schulz, J.; Boklund, A.; Toft, N.; Halasa, T. Drivers for Livestock-Associated Methicillin-Resistant Staphylococcus Aureus Spread Among Danish Pig Herds—A Simulation Study. Sci. Rep. 2018, 8. [Google Scholar] [CrossRef]
- Schulz, J.; Boklund, A.; Toft, N.; Halasa, T. Effects of control measures on the spread of LA-MRSA among Danish pig herds between 2006 and 2015-a simulation study. Sci. Rep. 2019, 9. [Google Scholar] [CrossRef]
- Ketusing, N.; Reeves, A.; Portacci, K.; Yano, T.; Olea-Popelka, F.; Keefe, T.; Salman, M. Evaluation of Strategies for the Eradication of Pseudorabies Virus (Aujeszky’s Disease) in Commercial Swine Farms in Chiang-Mai and Lampoon Provinces, Thailand, Using a Simulation Disease Spread Model. Transbound. Emerg. Dis. 2014, 61, 169–176. [Google Scholar] [CrossRef]
- Martinez-Lopez, B.; Ivorra, B.; Ramos, A.M.; Sanchez-Vizcaino, J.M. A novel spatial and stochastic model to evaluate the within- and between-farm transmission of classical swine fever virus. I. General concepts and description of the model. Vet. Microbiol. 2011, 147, 300–309. [Google Scholar] [CrossRef]
- Thulke, H.H.; Eisinger, D.; Beer, M. The role of movement restrictions and pre-emptive destruction in the emergency control strategy against CSF outbreaks in domestic pigs. Prev. Vet. Med. 2011, 99, 28–37. [Google Scholar] [CrossRef] [PubMed]
- Lange, M.; Siemen, H.; Blome, S.; Thulke, H.H. Analysis of spatio-temporal patterns of African swine fever cases in Russian wild boar does not reveal an endemic situation. Prev. Vet. Med. 2014, 117, 317–325. [Google Scholar] [CrossRef] [PubMed]
- Mur, L.; Sanchez-Vizcaino, J.M.; Fernandez-Carrion, E.; Jurado, C.; Rolesu, S.; Feliziani, F.; Laddomada, A.; Martinez-Lopez, B. Understanding African Swine Fever infection dynamics in Sardinia using a spatially explicit transmission model in domestic pig farms. Transbound. Emerg. Dis. 2018, 65, 123–134. [Google Scholar] [CrossRef] [PubMed]
- Fekede, R.J.; van Gils, H.; Huang, L.Y.; Wang, X.L. High probability areas for ASF infection in China along the Russian and Korean borders. Transbound. Emerg. Dis. 2019, 66, 852–864. [Google Scholar] [CrossRef] [PubMed]
- Pautienius, A.; Grigas, J.; Pileviciene, S.; Zagrabskaite, R.; Buitkuviene, J.; Pridotkas, G.; Stankevicius, R.; Streimikyte, Z.; Salomskas, A.; Zienius, D.; et al. Prevalence and spatiotemporal distribution of African swine fever in Lithuania, 2014–2017. Virol J. 2018, 15. [Google Scholar] [CrossRef] [PubMed]
- Iglesias, I.; Rodriguez, A.; Feliziani, F.; Rolesu, S.; de la Torre, A. Spatio-temporal Analysis of African Swine Fever in Sardinia (2012–2014): Trends in Domestic Pigs and Wild Boar. Transbound. Emerg. Dis. 2017, 64, 656–662. [Google Scholar] [CrossRef] [PubMed]
- Smietanka, K.; Wozniakowski, G.; Kozak, E.; Niemczuk, K.; Fraczyk, M.; Bocian, L.; Kowalczyk, A.; Pejsak, Z. African Swine Fever Epidemic, Poland, 2014–2015. Emerg. Infect. Dis. 2016, 22, 1201–1207. [Google Scholar] [CrossRef] [PubMed]
- Nurmoja, I.; Mõtus, K.; Kristian, M.; Niine, T.; Schulz, K.; Depner, K.; Viltrop, A. Epidemiological analysis of the 2015–2017 African swine fever outbreaks in Estonia. Prev. Vet. Med. 2018. [Google Scholar] [CrossRef] [PubMed]
- Wozniakowski, G.; Kozak, E.; Kowalczyk, A.; Lyjak, M.; Pomorska-Mol, M.; Niemczuk, K.; Pejsak, Z. Current status of African swine fever virus in a population of wild boar in eastern Poland (2014–2015). Arch. Virol. 2016, 161, 189–195. [Google Scholar] [CrossRef]
- Podgorski, T.; Apollonio, M.; Keuling, O. Contact rates in wild boar populations: Implications for disease transmission. J. Wildl. Manag. 2018, 82, 1210–1218. [Google Scholar] [CrossRef]
- Iglesias, I.; Munoz, M.J.; Montes, F.; Perez, A.; Gogin, A.; Kolbasov, D.; de la Torre, A. Reproductive Ratio for the Local Spread of African Swine Fever in Wild Boars in the Russian Federation. Transbound. Emerg. Dis. 2015, 63, E237–E245. [Google Scholar] [CrossRef] [PubMed]
- Halasa, T.; Botner, A.; Mortensen, S.; Christensen, H.; Toft, N.; Boklund, A. Simulating the epidemiological and economic effects of an African swine fever epidemic in industrialized swine populations. Vet. Microbiol. 2016, 193, 7–16. [Google Scholar] [CrossRef] [PubMed]
- Korennoy, F.I.; Gulenkin, V.M.; Malone, J.B.; Mores, C.N.; Dudnikov, S.A.; Stevenson, M.A. Spatio-temporal modeling of the African swine fever epidemic in the Russian Federation, 2007–2012. Spat. Spatio-temporal Epidemiol. 2014, 11, 135–141. [Google Scholar] [CrossRef] [PubMed]
- Blome, S.; Kramer, M.; Horeth-Bontgen, D.; Conraths, F.J.; Depner, K.; Bohle, W.; Gall, Y.; Selhorst, T.; Micklich, A.; Staubach, C.; et al. African swine fever in Eastern Europe—A threat also for German pig holdings? Tieraerztl. Umschau 2011, 66, 291–296. [Google Scholar]
- Olesen, A.S.; Lohse, L.; Boklund, A.; Halasa, T.; Gallardo, C.; Pejsak, Z.; Belsham, G.J.; Rasmussen, T.B.; Botner, A. Transmission of African swine fever virus from infected pigs by direct contact and aerosol routes. Vet. Microbiol. 2017, 211, 92–102. [Google Scholar] [CrossRef] [PubMed]
- Vlasova, N.; Varentsova, A.; Shevchenko, I.; Zhukov, I.; Remyga, S.; Gavrilova, V.; Puzankova, O.; Shevtsov, A.; Zinyakov, N.; Gruzdev, K. Comparative Analysis of Clinical and Biological Characteristics of African Swine Fever Virus Isolates from 2013 Year Russian Federation. Br. Microbiol. Res. J. 2015, 5, 203–215. [Google Scholar] [CrossRef]
- Guinat, C.; Reis, A.L.; Netherton, C.L.; Goatley, L.; Pfeiffer, D.U.; Dixon, L. Dynamics of African swine fever virus shedding and excretion in domestic pigs infected by intramuscular inoculation and contact transmission. Vet. Res. 2014, 45. [Google Scholar] [CrossRef]
- Gallardo, C.; Nurmoja, I.; Soler, A.; Delicado, V.; Simon, A.; Martin, E.; Perez, C.; Nieto, R.; Arias, M. Evolution in Europe of African swine fever genotype II viruses from highly to moderately virulent. Vet. Microbiol. 2018, 219, 70–79. [Google Scholar] [CrossRef]
- Petrov, A.; Forth, J.H.; Zani, L.; Beer, M.; Blome, S. No evidence for long-term carrier status of pigs after African swine fever virus infection. Transbound. Emerg. Dis. 2018, 65, 1318–1328. [Google Scholar] [CrossRef]
- Nurmoja, I.; Petrov, A.; Breidenstein, C.; Zani, L.; Forth, J.H.; Beer, M.; Kristian, M.; Viltrop, A.; Blome, S. Biological characterization of African swine fever virus genotype II strains from north-eastern Estonia in European wild boar. Transbound. Emerg. Dis. 2017, 64, 2034–2041. [Google Scholar] [CrossRef]
- Post, J.; Weesendorp, E.; Montoya, M.; Loeffen, W.L. Influence of Age and Dose of African Swine Fever Virus Infections on Clinical Outcome and Blood Parameters in Pigs. Viral Immunol. 2017, 30, 58–69. [Google Scholar] [CrossRef] [PubMed]
- Ferreira, H.; Weesendorp, E.; Elbers, A.R.W.; Bouma, A.; Quak, S.; Stegeman, J.A.; Loeffen, W.L.A. African swine fever virus excretion patterns in persistently infected animals: A quantitative approach. Vet. Microbiol. 2012, 160, 327–340. [Google Scholar] [CrossRef] [PubMed]
- Blome, S.; Gabriel, C.; Beer, M. Pathogenesis of African swine fever in domestic pigs and European wild boar. Virus Res. 2013, 173, 122–130. [Google Scholar] [CrossRef] [PubMed]
- Mebus, C.A. African Swine Fever. Adv. Virus Res. 1988, 35, 251–269. [Google Scholar] [PubMed]
- Montgomery, R.E. On a form of swine fever occurring in British East Africa (Kenya Colony). J. Comp. Pathol. 1921, 34, 159–191. [Google Scholar] [CrossRef]
- Guinat, C.; Vergne, T.; Jurado-Diaz, C.; Sánchez-Vizcaíno, J.M.; Dixon, L.; Pfeiffer, D.U. Effectiveness and practicality of control strategies for African swine fever: what do we really know? Vet. Rec. 2016. [Google Scholar] [CrossRef] [PubMed]
- Gallardo, C.; Soler, A.; Nieto, R.; Cano, C.; Pelayo, V.; Sanchez, M.A.; Pridotkas, G.; Fernandez-Pinero, J.; Briones, V.; Arias, M. Experimental Infection of Domestic Pigs with African Swine Fever Virus Lithuania 2014 Genotype II Field Isolate. Transbound. Emerg. Dis. 2017, 64, 300–304. [Google Scholar] [CrossRef]
- Gabriel, C.; Blome, S.; Malogolovkin, A.; Parilov, S.; Kolbasov, D.; Teifke, J.P.; Beer, M. Characterization of African Swine Fever Virus Caucasus Isolate in European Wild Boars. Emerg. Infect. Dis. 2011, 17, 2342–2345. [Google Scholar] [CrossRef]
- Blome, S.; Gabriel, C.; Dietze, K.; Breithaupt, A.; Beer, M. High Virulence of African Swine Fever Virus Caucasus Isolate in European Wild Boars of All Ages. Emerg. Infect. Dis. 2012, 18, 708. [Google Scholar] [CrossRef]
- European Food Safety Authority. Scientific opinion on African swine fever. EFSA J. 2015, 13, 4163. [Google Scholar] [CrossRef]
- Wilkinson, P.J.; Lawman, M.J.P.; Johnston, R.S. African Swine Fever in Malta, 1978. Vet. Rec. 1980, 106, 94–97. [Google Scholar] [CrossRef] [PubMed]
- Wilkinson, P.J.; Wardley, R.C.; Williams, S.M. African Swine Fever Virus (Malta-78) in pigs. J. Comp. Pathol. 1981, 91, 277–284. [Google Scholar] [CrossRef]
- Babalobi, O.O.; Olugasa, B.O.; Oluwayelu, D.O.; Ijagbone, I.F.; Ayoade, G.O.; Agbede, S.A. Analysis and evaluation of mortality losses of the 2001 African swine fever outbreak, Ibadan, Nigeria. Trop. Anim. Health Prod. 2007, 39, 533–542. [Google Scholar] [CrossRef] [PubMed]
- Wambura, P.N.; Masambu, J.; Msami, H. Molecular diagnosis and epidemiology of African swine fever outbreaks in Tanzania. Vet. Res. Commun. 2006, 30, 667–672. [Google Scholar] [CrossRef] [PubMed]
- Ekue, N.F.; Wilkinson, P.J.; Wardley, R.C. Infection of Pigs with the Cameroon Isolate (Cam/82) of African Swine Fever Virus. J. Comp. Pathol. 1989, 100, 145–154. [Google Scholar] [CrossRef]
- Haresnape, J.M.; Lungu, S.A.M.; Mamu, F.D. A 4-year survey of African Swine Fever in Malawi. J. Hyg. (Lond.) 1985, 95, 309–323. [Google Scholar] [CrossRef] [PubMed]
- Biront, P.; Castryck, F.; Leunen, J. An epizootic of African swine fever in Belgium and its eradication. Vet. Rec. 1987, 120, 432–434. [Google Scholar] [CrossRef]
- Olesen, A.S.; Lohse, L.; Boklund, A.; Halasa, T.; Belsham, G.J.; Rasmussen, T.B.; Botner, A. Short time window for transmissibility of African swine fever virus from a contaminated environment. Transbound. Emerg. Dis. 2018, 65, 1024–1032. [Google Scholar] [CrossRef] [PubMed]
- Sanchez-Vizcaino, J.M.; Mur, L.; Martinez-Lopez, B. African Swine Fever: An Epidemiological Update. Transbound. Emerg. Dis. 2012, 59, 27–35. [Google Scholar] [CrossRef] [PubMed]
- Charleston, B.; Bankowski, B.M.; Gubbins, S.; Chase-Topping, M.E.; Schley, D.; Howey, R.; Barnett, P.V.; Gibson, D.; Juleff, N.D.; Woolhouse, M.E.J. Relationship Between Clinical Signs and Transmission of an Infectious Disease and the Implications for Control. Science 2011, 332, 726–729. [Google Scholar] [CrossRef]
- Pan, I.C.; Hess, W.R. Virulence in African Swine Fever—Its measurement and implications. Am. J. Vet. Res. 1984, 45, 361–366. [Google Scholar] [PubMed]
- Boinas, F.S.; Hutchings, G.H.; Dixon, L.K.; Wilkinson, P.J. Characterization of pathogenic and non-pathogenic African swine fever virus isolates from Ornithodoros erraticus inhabiting pig premises in Portugal. J. Gen. Virol. 2004, 85, 2177–2187. [Google Scholar] [CrossRef] [PubMed]
- McVicar, J.W. Quantitative aspects of the transmission of African Swine Fever. Am. J. Vet. Res. 1984, 45, 1535–1541. [Google Scholar] [PubMed]
- European Food Safety Authority. Scientific opinion on African swine fever in wild boar. EFSA J. 2018, 16, 5344. [Google Scholar] [CrossRef]
- Schulz, K.; Olsevskis, E.; Staubach, C.; Lamberga, K.; Serzants, M.; Cvetkova, S.; Conraths, F.J.; Sauter-Louis, C. Epidemiological evaluation of Latvian control measures for African swine fever in wild boar on the basis of surveillance data. Sci. Rep. 2019, 9. [Google Scholar] [CrossRef] [PubMed]
- Lyra, T.M.D.; Freitas, T.R.P. Epizootiology, laboratory and virulence analyses during the emergency phase of the African swine fever eradication program in Brazil in 1978: a historic account. Semin-Cienc Agrar. 2015, 36, 2577–2592. [Google Scholar] [CrossRef][Green Version]
- Terpstra, C.; Wensvoort, G. African Swine Fever in the Netherlands. Tijdschr. Diergeneeskd. 1986, 111, 389–392. [Google Scholar] [PubMed]
- Gogin, A.; Gerasimov, V.; Malogolovkin, A.; Kolbasov, D. African swine fever in the North Caucasus region and the Russian Federation in years 2007–2012. Virus Res. 2013, 173, 198–203. [Google Scholar] [CrossRef] [PubMed]
- Mebus, C.A.; House, C.; Gonzalvo, F.R.; Pineda, J.M.; Tapiador, J.; Pire, J.J.; Bergada, J.; Yedloutschnig, R.J.; Sahu, S.; Becerra, V.; et al. Survival Of Foot-And-Mouth-Disease, African Swine Fever, And Hog-Cholera Viruses In Spanish Serrano Cured Hams And Iberian Cured Hams, Shoulders And Loins. Food Microbiol. 1993, 10, 133–143. [Google Scholar] [CrossRef]
- McKercher, P.D.; Yedloutschnig, R.J.; Callis, J.J.; Murphy, R.; Panina, G.F.; Civardi, A.; Bugnetti, M.; Foni, E.; Laddomada, A.; Scarano, C.; et al. Survival viruses in prosciutto-di-parma (parma ham). Can. Inst. Food Sci. Technol. J. 1987, 20, 267–272. [Google Scholar] [CrossRef]
- Dee, S.A.; Bauermann, F.V.; Niederwerder, M.C.; Singrey, A.; Clement, T.; de Lima, M.; Long, C.; Patterson, G.; Sheahan, M.A.; Stoian, A.M.M.; et al. Survival of viral pathogens in animal feed ingredients under transboundary shipping models. PLoS ONE 2018, 13. [Google Scholar] [CrossRef]
- Mebus, C.; Arias, M.; Pineda, J.M.; Tapiador, J.; House, C.; SanchezVizcaino, J.M. Survival of several porcine viruses in different Spanish dry-cured meat products. Food Chem. 1997, 59, 555–559. [Google Scholar] [CrossRef]
- Penrith, M.-L.; Bastos, A.D.; Etter, E.M.C.; Beltran-Alcrudo, D. Epidemiology of African swine fever in Africa today: Sylvatic cycle versus socio-economic imperatives. Transbound. Emerg. Dis. 2019, 66, 672–686. [Google Scholar] [CrossRef]
- Cwynar, P.; Stojkov, J.; Wlazlak, K. African Swine Fever Status in Europe. Viruses-Basel 2019, 11. [Google Scholar] [CrossRef] [PubMed]
- Dixon, L.K.; Sun, H.; Roberts, H. African swine fever. Antivir. Res. 2019, 165, 34–41. [Google Scholar] [CrossRef] [PubMed]
- Vergne, T.; Gogin, A.; Pfeiffer, D.U. Statistical Exploration of Local Transmission Routes for African Swine Fever in Pigs in the Russian Federation, 2007-2014. Transbound. Emerg. Dis. 2017, 64, 504–512. [Google Scholar] [CrossRef] [PubMed]
- Mur, L.; Martinez-Lopez, B.; Sanchez-Vizcaino, J.M. Risk of African swine fever introduction into the European Union through transport-associated routes: Returning trucks and waste from international ships and planes. BMC Vet. Res. 2012, 8. [Google Scholar] [CrossRef] [PubMed]

| ASFV Strain or Isolate | Virulence | Course of Disease | |
|---|---|---|---|
| Field Infection | Experimental Infection/Route of Infection | ||
| Malta isolate (Malta/78) | Moderate/high | Fast spread in the domestic pig population, which ended in the slaughter of all pigs in Malta within one year [79]. | Mild clinical signs in less than 50% of infected pigs, high mortality/exposure to infected donor pigs [80]. |
| Brazil’78 | Low/moderate | Mild clinical course and decreasing mortality over time in domestic pigs. Wide distribution throughout Brazil for at least eight years [94]. | High mortality/intranasally [70]. |
| Netherlands’86 | Moderate | No information found | Low mortality with a rather subclinical course of disease/oronasally and through contact [67,95]. |
| Georgia 2007/1 | High | Large scale epidemic, wild boar and domestic pigs affected [96]. | Moderate clinical signs, high mortality/intramuscularly [65]. |
| Estonian’15/WB, Tartu-14 | High | Rapid spread in the wild boar population [37]. | 100% mortality in experimentally infected domestic pigs. Two survivors in in-contact pigs/intramuscularly [66]. |
| Estonian-Ida Viru | High | Only local spread within the wild boar population [37]. | Almost 100% mortality (one survivor)/oronasally [68]. |
| Armenia’08 | High | No information found. | 100% mortality in wild boar and domestic pigs/oronasally [27]. |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Schulz, K.; Conraths, F.J.; Blome, S.; Staubach, C.; Sauter-Louis, C. African Swine Fever: Fast and Furious or Slow and Steady? Viruses 2019, 11, 866. https://doi.org/10.3390/v11090866
Schulz K, Conraths FJ, Blome S, Staubach C, Sauter-Louis C. African Swine Fever: Fast and Furious or Slow and Steady? Viruses. 2019; 11(9):866. https://doi.org/10.3390/v11090866
Chicago/Turabian StyleSchulz, Katja, Franz Josef Conraths, Sandra Blome, Christoph Staubach, and Carola Sauter-Louis. 2019. "African Swine Fever: Fast and Furious or Slow and Steady?" Viruses 11, no. 9: 866. https://doi.org/10.3390/v11090866
APA StyleSchulz, K., Conraths, F. J., Blome, S., Staubach, C., & Sauter-Louis, C. (2019). African Swine Fever: Fast and Furious or Slow and Steady? Viruses, 11(9), 866. https://doi.org/10.3390/v11090866






