Mechanical Properties of Composite Core Build-Up Materials: A Comparative Study
Abstract
1. Introduction
2. Materials and Methods
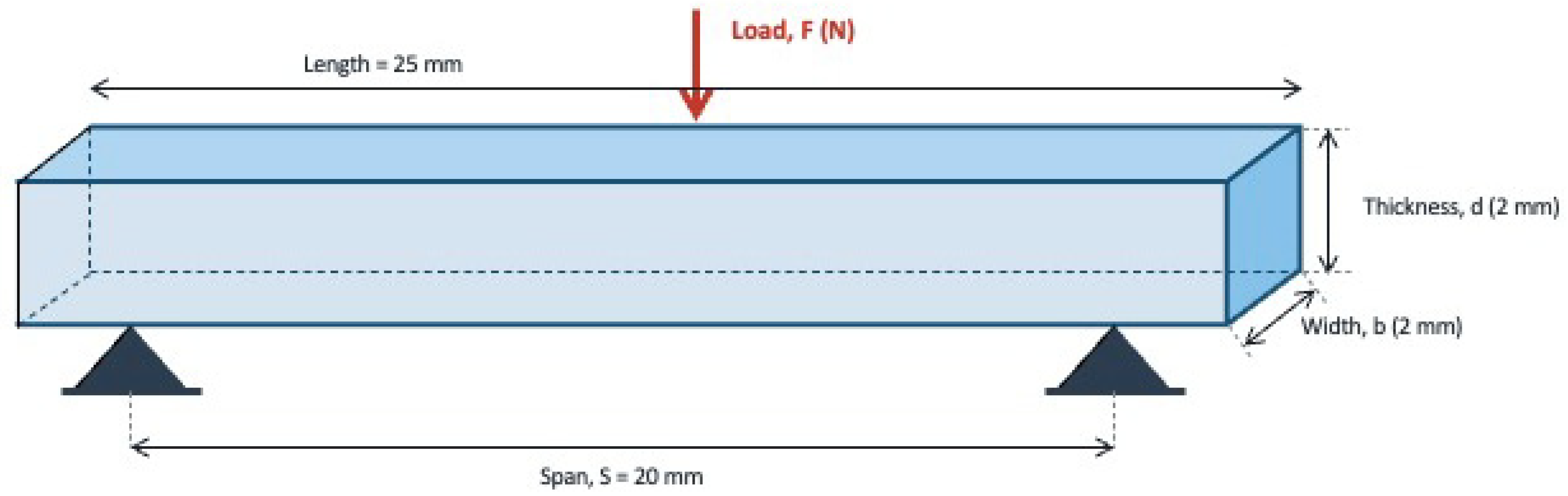
2.1. Flexural Strength and Flexural Modulus Testing
2.2. Water Sorption and Solubility Testing
2.3. Statistical Analysis
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Data Availability Statement
Conflicts of Interest
References
- Warangkulkasemkit, S.; Pumpaluk, P. Comparison of physical properties of three commercial composite core build-up materials. Dent. Mater. J. 2019, 38, 177–181. [Google Scholar] [CrossRef] [PubMed]
- Passos, S.P.; Freitas, A.P.; Jumaily, S.; Santos, M.J.; Rizkalla, A.S.; Santos, G.C. Comparison of mechanical properties of five commercial dental core build-up materials. Compend. Contin. Educ. Dent. 2013, 34, 62–68. [Google Scholar]
- Coelho Santos, M.J.; Bezerra, R.B. Fracture resistance of maxillary premolars with direct and indirect adhesive techniques. J. Can. Dent. Assoc. 2005, 71, 585. [Google Scholar]
- Mincik, J.; Urban, D.; Timkova, S.; Urban, R. Fracture resistance of endodontically treated maxillary premolars restored by various direct filling materials: An in vitro study. Int. J. Biomater. 2016, 2016, 9138945. [Google Scholar] [CrossRef]
- Rosenstiel, S.F.; Land, M.F.; Fujimoto, J. Contemporary Fixed Prosthodontics; Mosby: St. Louis, MO, USA, 2006. [Google Scholar]
- Koytchev, E.; Yamaguchi, S.; Shin-No, Y.; Suzaki, N.; Okamoto, M.; Imazato, S.; Datcheva, M.; Hayashi, M. Comprehensive micro-mechanical characterization of experimental direct core build-up resin composites with different amounts of filler contents. Dent. Mater. J. 2019, 38, 743–749. [Google Scholar] [CrossRef]
- Kim, K.H.; Ong, J.L.; Okuno, O. The effect of filler loading and morphology on the mechanical properties of contemporary composites. J. Prosthet. Dent. 2002, 87, 642–649. [Google Scholar] [CrossRef]
- Sauro, S. Bioactive and Therapeutic Dental Materials; MDPI: Basel, Switzerland, 2019. [Google Scholar]
- Hirata, R.; Kabbach, W.; De Andrade, O.S.; Bonfante, E.A.; Giannini, M.; Coelho, P.G. Bulk fill composites: An anatomic sculpting technique. J. Esthet. Restor. Dent. 2015, 27, 335–343. [Google Scholar] [CrossRef]
- Bucuta, S.; Ilie, N. Light transmittance and micro-mechanical properties of bulk fill vs. conventional resin based composites. Clin. Oral Investig. 2014, 18, 1991–2000. [Google Scholar] [CrossRef] [PubMed]
- Elshazly, T.M.; Bourauel, C.; Aboushelib, M.N.; Sherief, D.I.; El-Korashy, D.I. The polymerization efficiency of a bulk-fill composite based on matrix-modification technology. Restor. Dent. Endod. 2020, 45, e32. [Google Scholar] [CrossRef]
- Leprince, J.G.; Palin, W.M.; Vanacker, J.; Sabbagh, J.; Devaux, J.; Leloup, G. Physico-mechanical characteristics of commercially available bulk-fill composites. J. Dent. 2014, 42, 993–1000. [Google Scholar] [CrossRef] [PubMed]
- Kim, R.J.Y.; Kim, Y.J.; Choi, N.S.; Lee, I.B. Polymerization shrinkage, modulus, and shrinkage stress related to tooth-restoration interfacial debonding in bulk-fill composites. J. Dent. 2015, 43, 430–439. [Google Scholar] [CrossRef] [PubMed]
- Fugolin, A.P.P.; Pfeifer, C.S. New resins for dental composites. J. Dent. Res. 2017, 96, 1085–1091. [Google Scholar] [CrossRef]
- Kournetas, N.; Tzoutzas, I.; Eliades, G. Monomer conversion in dual-cured core buildup materials. Oper. Dent. 2011, 36, 92–97. [Google Scholar] [CrossRef]
- Taubock, T.; Oberlin, H.; Buchalla, W.; Roos, M.; Attin, T. Comparing the effectiveness of self-curing and light curing in polymerization of dual-cured core buildup materials. J. Am. Dent. Assoc. 2011, 142, 950–956. [Google Scholar] [CrossRef]
- Kim, H.J.; Kwon, J.; Kim, H.J.; Kim, R.H.; Kim, D.S.; Jang, J.H. Comparison of polymerization behaviors, microhardness and compressive strength between bulk-fill resin and dual-cured core resin. BMC Oral Health 2025, 25, 972. [Google Scholar] [CrossRef]
- Spinhayer, L.; Bui, A.T.B.; Leprince, J.G.; Hardy, C.M.F. Core build-up resin composites: An in-vitro comparative study. Biomater. Investig. Dent. 2020, 7, 159–166. [Google Scholar] [CrossRef]
- Kelch, M.; Stawarczyk, B.; Mayinger, F. Chemical and mechanical properties of dual-polymerizing core build-up materials. Clin. Oral Investig. 2022, 26, 4885–4896. [Google Scholar] [CrossRef]
- Zankuli, M.; Silikas, N.; Devlin, H. Water sorption and solubility of core build up materials. Dent. Mater. 2014, 30, 324–329. [Google Scholar] [CrossRef] [PubMed]
- Chagas Rego, H.; Butler, S.; Coelho dos Santos, M. Evaluation of the mechanical properties of three resin-modified glass ionomer cements. BioMed Res. Int. 2023, 39, 15–16. [Google Scholar]
- Kumar, G.; Shivrayan, A. Comparative study of mechanical properties of direct core build-up materials. Contemp. Clin. Dent. 2015, 6, 16–20. [Google Scholar] [CrossRef]
- Irie, M.; Maruo, Y.; Nishigawa, G.; Yoshihara, K.; Matsumoto, T. Flexural strength of resin core build-up materials: Correlation to root dentin shear bond strength and pull-out force. Polymers 2020, 12, 2947. [Google Scholar] [CrossRef]
- Beatty, M.W.; Swartz, M.L.; Moore, B.K.; Phillips, R.W.; Roberts, T.A. Effect of crosslinking agent content, monomer functionality, and repeat unit chemistry on properties of unfilled resins. J. Biomed. Mater. Res. 1993, 27, 403–413. [Google Scholar] [CrossRef]
- Ilie, N. Degradation of dental methacrylate-based composites in simulated clinical immersion media. J. Funct. Biomater. 2022, 13, 25. [Google Scholar] [CrossRef]
- Santerre, J.P.; Shajii, L.; Leung, B.W. Relation of dental composite formulations to their degradation and the release of hydrolyzed polymeric-resin-derived products. Crit. Rev. Oral Biol. Med. 2001, 12, 136–151. [Google Scholar] [CrossRef]
- Van Landuyt, K.L.; Nawrot, T.; Geebelen, B.; De Munck, J.; Snauwaert, J.; Yoshihara, K.; Scheers, H.; Godderis, L.; Hoet, P.; Van Meerbeek, B. How much do resin-based dental materials release? A meta-analytical approach. Dent. Mater. 2011, 27, 723–747. [Google Scholar] [CrossRef]
- Alshali, R.Z.; Salim, N.A.; Satterthwaite, J.D.; Silikas, N. Long-term sorption and solubility of bulk-fill and conventional resin-composites in water and artificial saliva. J. Dent. 2015, 43, 1511–1518. [Google Scholar] [CrossRef] [PubMed]
- Kazak, M.; Toz Akalin, T.; Esen, F. Comparison of water sorption and water solubility properties of current restorative materials with different contents. Eur. J. Dent. 2025, 19, 248–254. [Google Scholar] [CrossRef]
- Elmamooz, N.; Eskandarizadeh, A.; Haghani, J.; Doosty, Z.; Rahimi, F.; Shakerifar, M. Comparison of water sorption and solubility of conventional and bulk-fill composites at different depths over two time intervals. Cureus 2025, 17, e89150. [Google Scholar] [CrossRef]
- Chen, Y.; Jiang, Q.; Wei, Y. Effects of wet environment on physical, chemical and mechanical properties of four core buildup materials. Mater. Res. Express 2025, 12, 065401. [Google Scholar] [CrossRef]
- ISO 4049; Dentistry—Polymer-Based Restorative Materials. International Organization for Standardization (ISO): Geneva, Switzerland, 2019.
- Rodrigues Junior, S.A.; Zanchi, C.H.; Carvalho, R.V.D.; Demarco, F.F. Flexural strength and modulus of elasticity of different types of resin-based composites. Braz. Oral Res. 2007, 21, 16–21. [Google Scholar] [CrossRef] [PubMed]
- Alzahrani, B.; Alshabib, A.; Awliya, W. Surface hardness and flexural strength of dual-cured bulk-fill restorative materials after solvent storage. BMC Oral Health 2023, 23, 306. [Google Scholar] [CrossRef] [PubMed]
- Nakade, P.; Thaore, S.; Bangar, B.; Grover, I.; Alharethi, N.; Adsure, G.; Kulkarni, D. Comparative evaluation of fracture toughness and flexural strength of four different core build-up materials: An in vitro study. J. Contemp. Dent. Pract. 2024, 25, 191–195. [Google Scholar]
- Chang, M.; Dennison, J.; Yaman, P. Physical property evaluation of four composite materials. Oper. Dent. 2013, 38, E144–E153. [Google Scholar] [CrossRef] [PubMed]
- Eweis, A.H.; Yap, A.U.; Yahya, N.A. Comparison of flexural properties of bulk-fill restorative/flowable composites and their conventional counterparts. Oper. Dent. 2020, 45, 41–51. [Google Scholar] [CrossRef]
- Ibrahim, M.S.; AlKhalefah, A.S.; Alsaghirat, A.A.; Alburayh, R.A.; Alabdullah, N.A. Comparison between different bulk-fill and incremental composite materials used for class II restorations in primary and permanent teeth: In vitro assessments. Materials 2023, 16, 6674. [Google Scholar] [CrossRef]
- 3M Oral Care. 3M Filtek One Bulk Fill Restorative: Technical Product Profile; 3M Company: St. Paul, MN, USA, 2016. [Google Scholar]
- Balsamo, M.; Borges, A.B.; Borges, A.L.S.; Paes-Junior, T.J.A.; Lloret, P.R. Flexural strength of different composite resins. In Proceedings of the IADR/AADR/CADR 87th General Session and Exhibition, Miami, FL, USA, 1–4 April 2009. [Google Scholar]
- Kramer, N.; Reinelt, C.; Richter, G.; Petschelt, A.; Frankenberger, R. Nanohybrid vs. fine hybrid composite in class II cavities: Clinical results and margin analysis after four years. Dent. Mater. 2009, 25, 750–759. [Google Scholar] [CrossRef]
- Lassila, L.; Sailynoja, E.; Prinssi, R.; Vallittu, P.K. Characterization of a new fiber-reinforced flowable composite. Odontology 2019, 107, 342–352. [Google Scholar] [CrossRef]
- Araujo-Neto, V.G.; Sebold, M.; de Castro, E.F.; Feitosa, V.P.; Giannini, M. Evaluation of physico-mechanical properties and filler particles characterization of conventional, bulk-fill, and bioactive resin-based composites. J. Mech. Behav. Biomed. Mater. 2021, 121, 104620. [Google Scholar]
- Khan, W.; Singh, K.B.; Patil, D.; Banerjee, A.; Ahire, C.D.; Singh, V. Comparative evaluation of sorption and solubility of core buildup materials in different pH media: An in-vitro study. Cureus 2024, 16, e59432. [Google Scholar] [CrossRef]
- Bitter, K.; Schubert, A.; Neumann, K.; Blunck, U.; Sterzenbach, G.; Ruttermann, S. Are self-adhesive resin cements suitable as core build-up materials? Clin. Oral Investig. 2016, 20, 1337–1345. [Google Scholar] [CrossRef] [PubMed]
- Arbildo-Vega, H.I.; Lapinska, B.; Panda, S.; Lamas-Lara, C.; Khan, A.S.; Lukomska-Szymanska, M. Clinical effectiveness of bulk-fill and conventional resin composite restorations: Systematic review and meta-analysis. Polymers 2020, 12, 1786. [Google Scholar] [CrossRef] [PubMed]
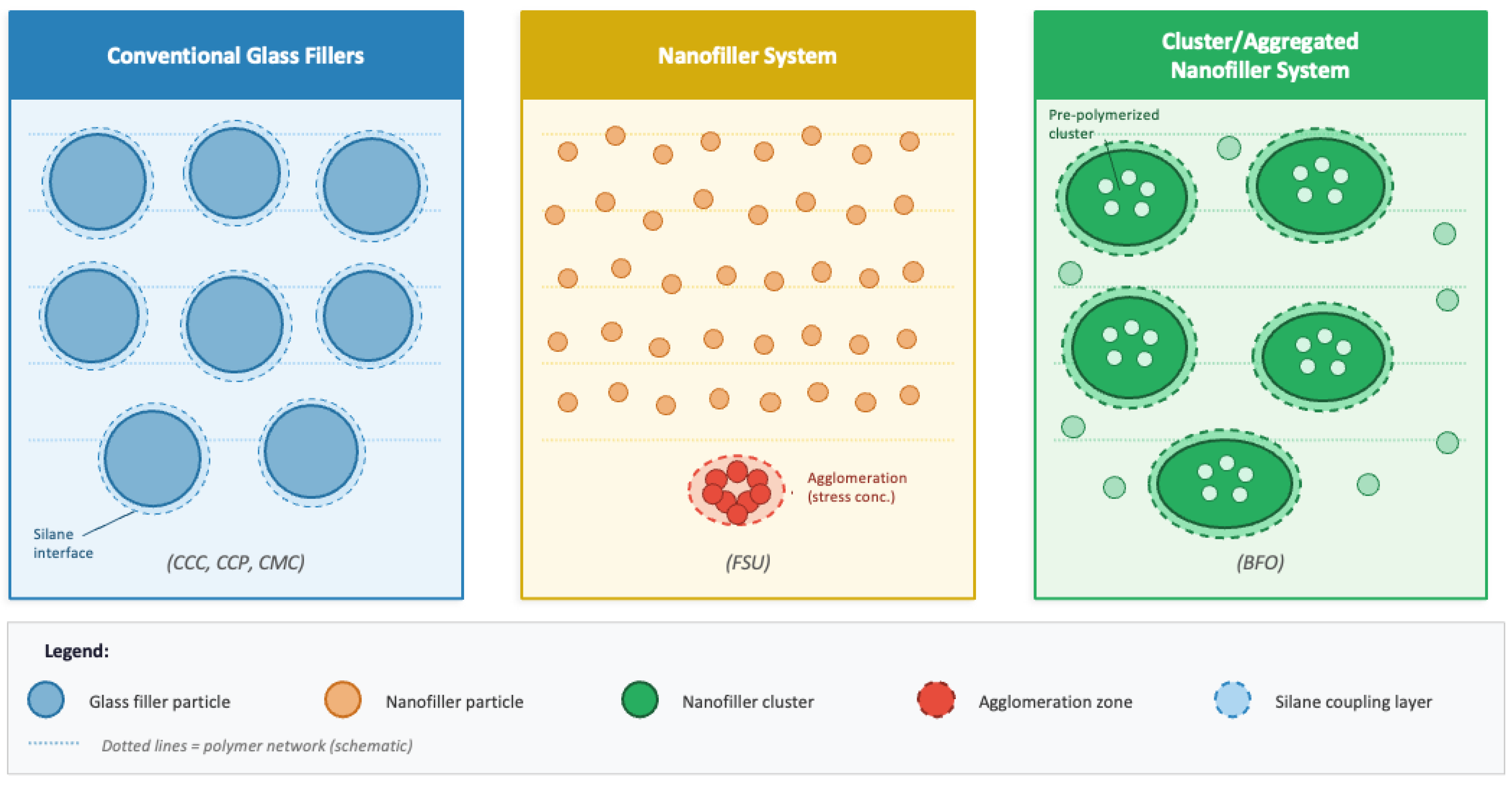
| Material | Manufacturer | Composition (Monomer System/Filler System) | Filler Content |
|---|---|---|---|
| CosmeCore DC Automix—CCC | Cosmedent, Chicago, IL, USA | Matrix: UDMA (~40%), Bis-EMA (~25%), Bis-GMA (~20%), tricyclodecanedimethanol diacrylate, 1,4-butanediol dimethacrylate. Filler: silanated barium aluminosilicate glass (1–3 μm), fumed silicon dioxide (nanosilica). 69 wt%/48 vol%. | 69 wt%, 48 vol% |
| Clearfil DC Core Plus—CCP | Kuraray, New York, NY, USA | Matrix: Bis-GMA (~55%), TEGDMA and aromatic/aliphatic dimethacrylates. Filler: silanated barium aluminosilicate glass particles (1–2 μm), colloidal silica, alumina. 74 wt%/52 vol%. | 74 wt%, 52 vol% |
| MultiCore Flow—CMC | Ivoclar Vivadent, Schaan, Liechtenstein | Matrix: Bis-GMA (~40%), UDMA (~35%), TEGDMA (~10%). Filler: silanated barium aluminosilicate glass (0.7 μm avg), ytterbium trifluoride (radiopacifier), fumed silicon dioxide. 68 wt%/47 vol%. | 68 wt%, 47 vol% |
| Filtek One Bulk Fill Restorative—BFO | 3M ESPE, St. Paul, MN, USA | Matrix: AUDMA (addition-fragmentation monomer for shrinkage stress relief), DDDMA, UDMA, 1,12-dodecanediol dimethacrylate. Filler: pre-polymerized zirconia/silica cluster fillers (0.6–10 μm) and silica nanofillers (20 nm). 76.5 wt%/58.4 vol%. | 76.5 wt%, 58.4 vol% |
| Filtek Bulk Fill Flowable—BFF | 3M ESPE, St. Paul, MN, USA | Matrix: AUDMA, DDDMA, procrylat resin (proprietary low-shrinkage monomer). Filler: zirconia/silica cluster fillers and silica nanofillers (20 nm). 64.5 wt%/42.5 vol%. | 64.5 wt%, 42.5 vol% |
| Filtek Supreme Ultra—FSU (control) | 3M ESPE, St. Paul, MN, USA | Matrix: Bis-GMA (~55%), UDMA (~15%), TEGDMA (~10%), Bis-EMA (~20%). Filler: aggregated zirconia/silica nanoclusters (0.6–1.4 μm) and discrete silica nanofillers (20 nm). 78.5 wt%/59.5 vol%. | 78.5 wt%, 59.5 vol% |
| Material | Flexural Strength—FS (MPa) | Flexural Modulus—E (GPa) | Modulus of Resilience—R (MPa) |
|---|---|---|---|
| CosmeCore DC Automix—CCC | 137.77 (11.34) c | 7.82 (0.31) a,c | 1.22 (0.20) c,d |
| Clearfil DC Core Plus—CCP | 122.12 (12.65) a,b | 7.87 (0.40) a,b | 0.96 (0.20) a,b |
| MultiCore Flow—CMC | 111.50 (11.38) b,e,f | 7.89 (0.26) b,c | 0.80 (0.17) b,f |
| Filtek One Bulk Fill Restorative—BFO | 134.57 (14.85) c | 8.53 (0.58) d | 1.09 (0.21) a,d,e |
| Filtek Bulk Fill Flowable—BFF | 109.15 (4.61) a,d,e | 4.69 (0.21) * | 1.28 (0.13) c,e |
| Filtek Supreme Ultra—FSU | 100.17 (19.91) d,f | 8.91 (0.82) d | 0.62 (0.20) f |
| Material | Water Sorption—WS (µg/mm3) | Water Solubility—SO (µg/mm3) |
|---|---|---|
| CosmeCore DC Automix—CCC | 14.92 (0.51) * | −0.45 (0.63) a |
| Clearfil DC Core Plus—CCP | 19.15 (0.90) a,b,c | −0.09 (0.92) a |
| MultiCore Flow—CMC | 20.82 (1.51) c,e,f | −1.18 (1.14) a |
| Filtek One Bulk Fill Restorative—BFO | 20.97 (1.70) b,d,f | −0.30 (1.78) a |
| Filtek Bulk Fill Flowable—BFF | 18.30 (1.95) a,d,e | −0.84 (0.95) a |
| Filtek Supreme Ultra—FSU | 28.76 (3.49) * | −0.79 (1.68) a |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license.
Share and Cite
Mundy, E.; Engineer, S.V.; Butler, S.; Rizkalla, A.; Santos Junior, G.C.; Santos, M.J.M.C. Mechanical Properties of Composite Core Build-Up Materials: A Comparative Study. Materials 2026, 19, 1487. https://doi.org/10.3390/ma19081487
Mundy E, Engineer SV, Butler S, Rizkalla A, Santos Junior GC, Santos MJMC. Mechanical Properties of Composite Core Build-Up Materials: A Comparative Study. Materials. 2026; 19(8):1487. https://doi.org/10.3390/ma19081487
Chicago/Turabian StyleMundy, Emily, Sanaya V. Engineer, Sheila Butler, Amin Rizkalla, Gildo Coelho Santos Junior, and Maria Jacinta Moraes Coelho Santos. 2026. "Mechanical Properties of Composite Core Build-Up Materials: A Comparative Study" Materials 19, no. 8: 1487. https://doi.org/10.3390/ma19081487
APA StyleMundy, E., Engineer, S. V., Butler, S., Rizkalla, A., Santos Junior, G. C., & Santos, M. J. M. C. (2026). Mechanical Properties of Composite Core Build-Up Materials: A Comparative Study. Materials, 19(8), 1487. https://doi.org/10.3390/ma19081487








