Preparation of Cationic Amphiphilic Nanoparticles with Modified Chitosan Derivatives for Doxorubicin Delivery
Abstract
:1. Introduction
2. Materials and Methods
2.1. Materials
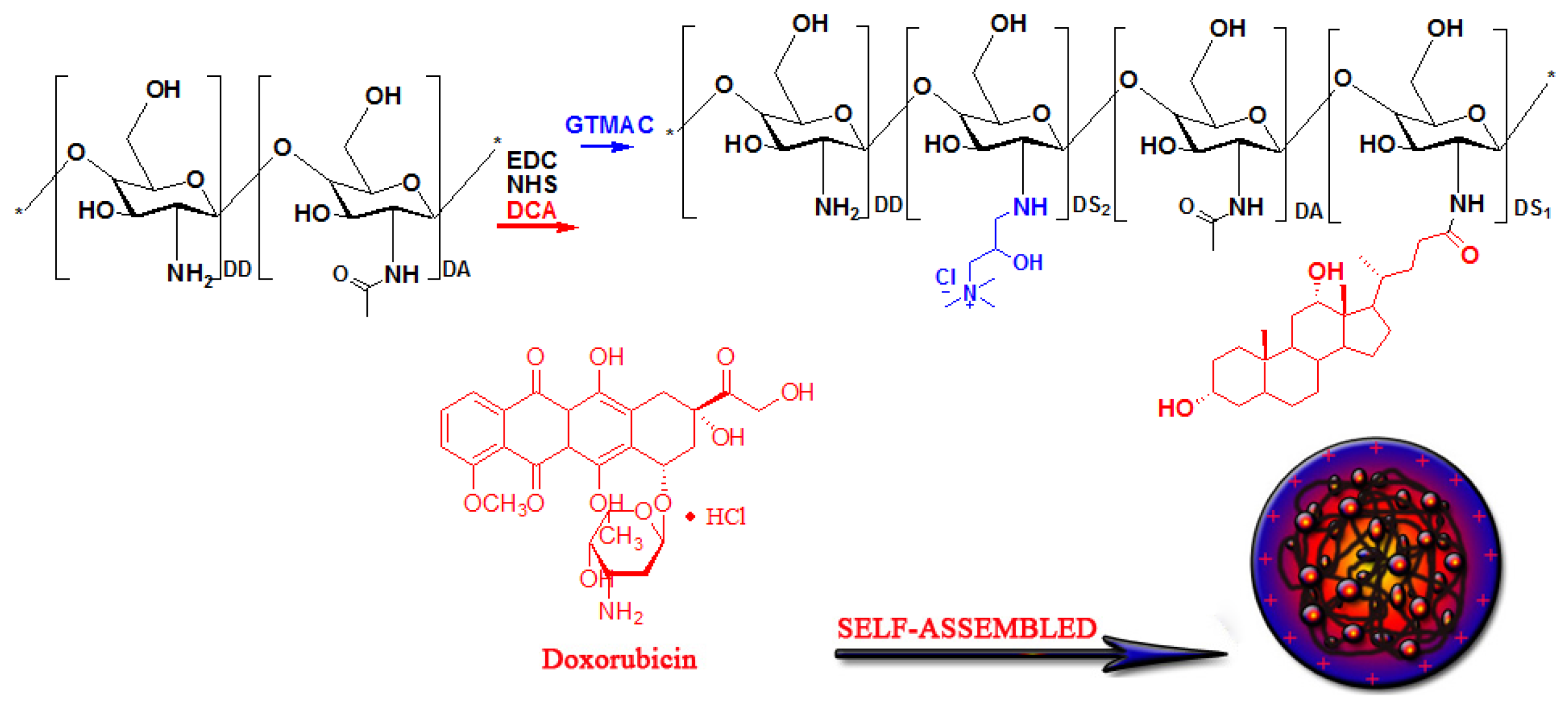
2.2. Preparation of Cationic Amphiphilic Chitosan HT-CS-DCA
2.3. Preparation HT-CS-DCA and DOX-Loaded HT-CS-DCA Nanoparticles
2.4. Measurements
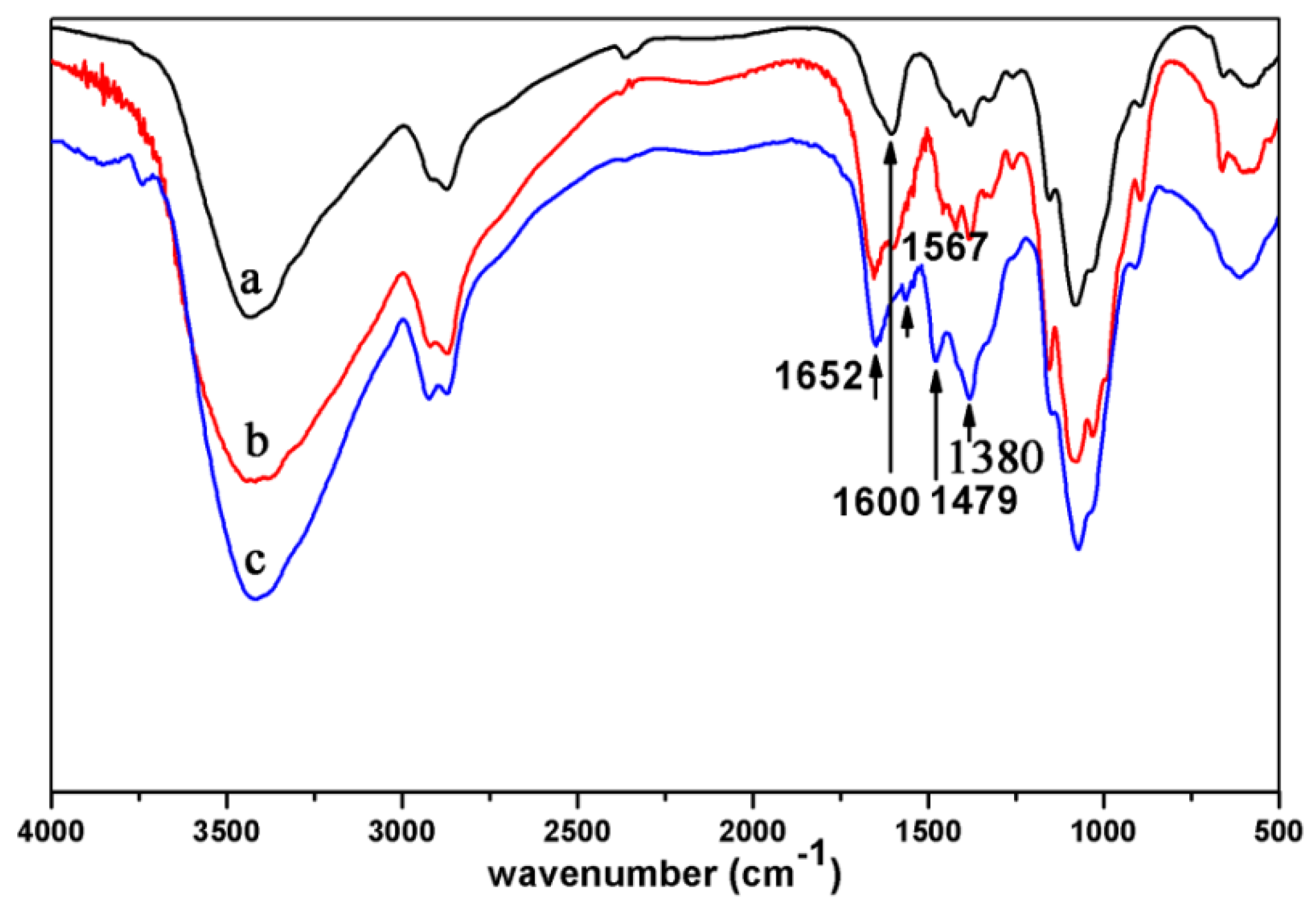
2.4.1. Characterization of Chitosan Derivatives
2.4.2. Critical Aggregation Concentration (CAC)
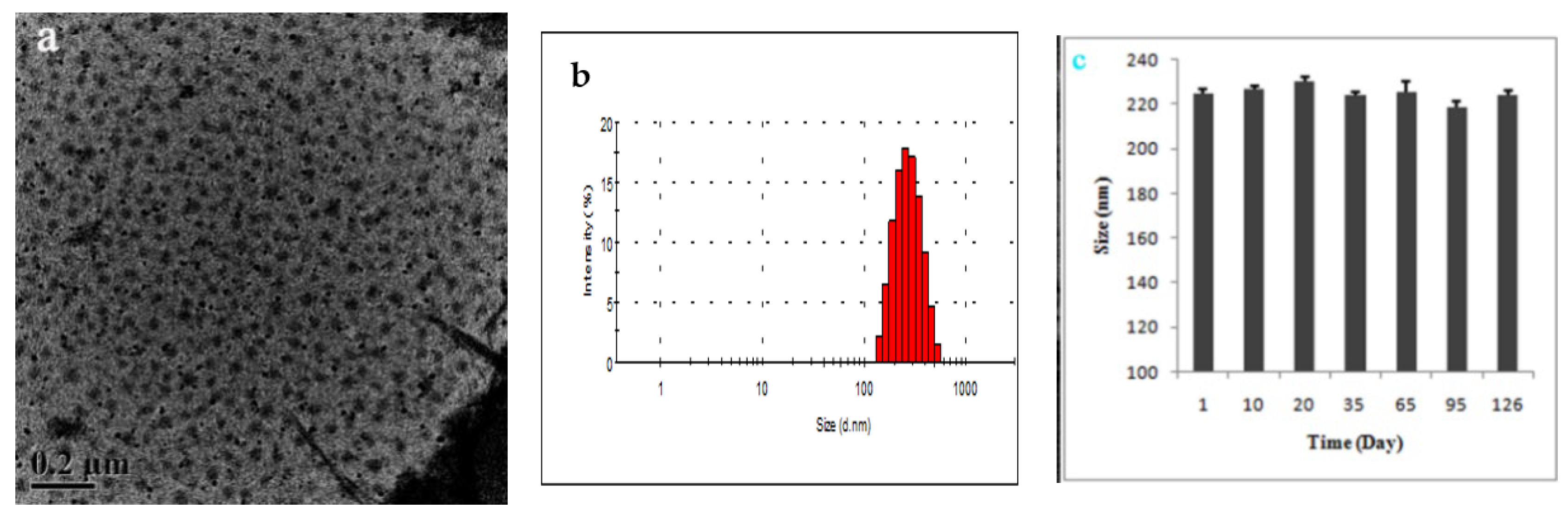
2.4.3. Morphology, Size, and Zeta Potential
2.4.4. Drug Loading
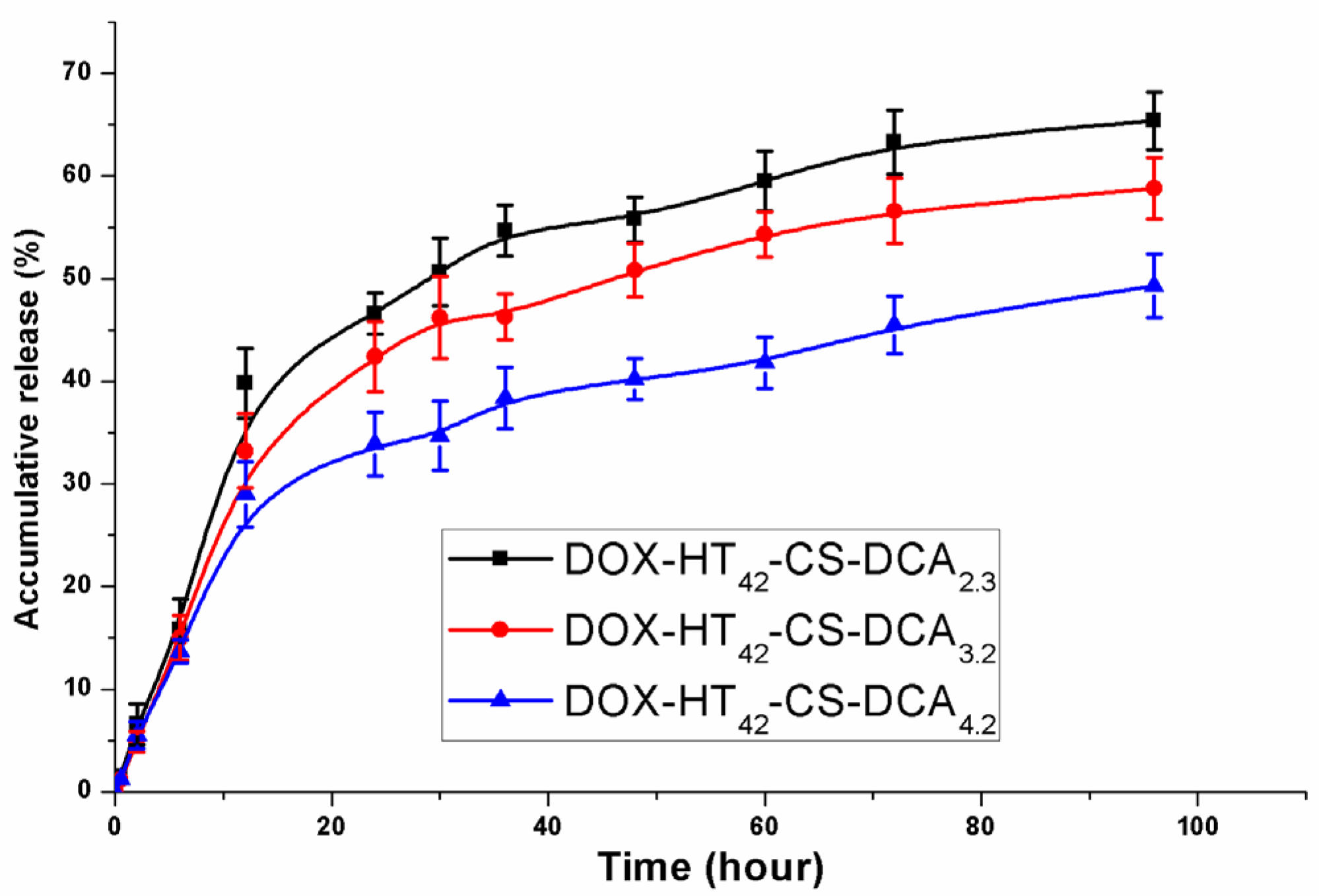
2.5. Release of DOX from HT-CS-DCA Nanoparticles In Vitro
2.6. Confocal Laser Scanning Microscopic (CLSM) Observations on Cellular Uptake
2.7. Cellular Viability Study In Vitro
3. Results and Discussion
3.1. Preparation of Cationic Amphiphilic Chitosan Derivatives HT-CS-DCA
3.2. Morphology, CAC, Size, and Zeta Potential of HT-CS-DCA Nanoparticles
3.3. Release of DOX from HT-CS-DCA Nanoparticles In Vitro
3.4. Confocal Laser Scanning Microscopic (CLSM) Observations on Cellular Uptake
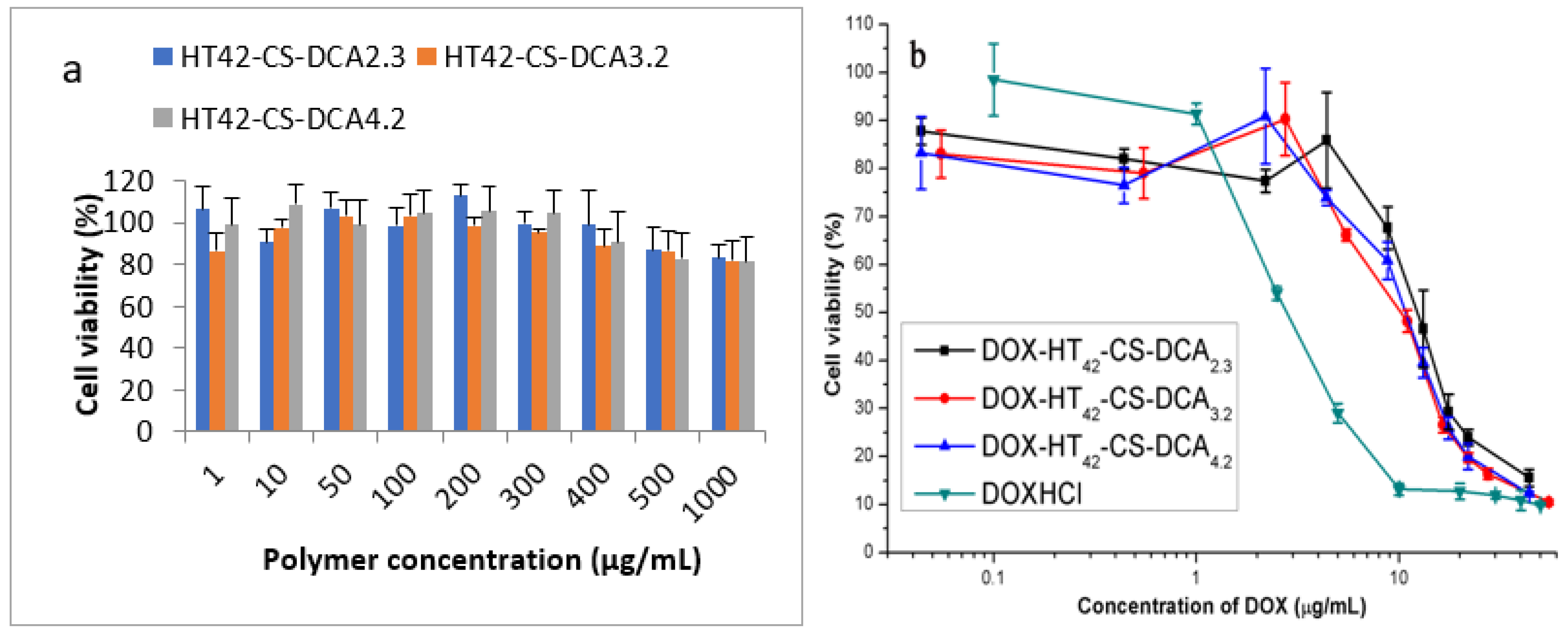
3.5. Cellular Viability Study In Vitro
4. Conclusions
Author Contributions
Funding
Conflicts of Interest
Abbreviations
| CS | Chitosan |
| CLSM | Confocal laser scanning microscopy |
| CAC | Critical aggregation concentration |
| DCA | Deoxycholic acid |
| DOX | Doxorubicin |
| EE | Encapsulation efficiency |
| EDC•HCl | 1-ethyl-3-(3-dimethylaminopropylCarbodiimide hydrochloride |
| GTMAC | Glycidyltrimethylammounium chloride |
| HT-CS-DCA | N-(2-hydroxy)propyl-3-trimethylammnonium-chitosan-deoxycholic acid |
| LC | Loading content |
| MCF-7 | Human breast cancer cells |
| MTT | Methyl tetrazolium |
| MWCO | Molecular weight cut-off |
| NHS | N-hydroxysuccimide |
| PDI | Polydispersity index |
References
- Gaucher, G.; Marchessault, R.H.; Leroux, J.C. Polyester-based micelles and nanoparticles for the parenteral delivery of taxanes. J. Control Release 2010, 143, 2–12. [Google Scholar] [CrossRef]
- Hwang, D.; Ramseya, J.D.; Kabanov, A.V. Polymeric micelles for the delivery of poorly soluble drugs: From nanoformulation to clinical approval. Adv. Drug Deliv. Rev. 2020, 156, 80–118. [Google Scholar] [CrossRef] [PubMed]
- Marinheiro, D.; Ferreira, B.J.M.L.; Oskoei, P.; Oliveira, H.; Daniel-da-Silva, A.L. Encapsulation and enhanced release of resveratrol from mesoporous silica nanoparticles for melanoma therapy. Materials 2021, 14, 1382. [Google Scholar] [CrossRef] [PubMed]
- Ding, J.X.; Chen, J.J.; Gao, L.Q.; Jiang, Z.Y.; Zhang, Y.; Li, M.Q.; Xiao, Q.C.; Lee, S.S.; Chen, X.S. Engineered nanomedicines with enhanced tumor penetration. Nanotoday 2019, 29, 100800. [Google Scholar] [CrossRef]
- Sun, H.L.; Dong, Y.Y.; Feijen, J.; Zhong, Z.Y. Peptide-decorated polymeric nanomedicines for precision cancer therapy. J. Control Release 2018, 290, 11–27. [Google Scholar] [CrossRef] [PubMed]
- Suzuki, H.; Bae, Y.H. Evaluation of drug penetration with cationic micelles and their penetration mechanism using an in vitro tumor model. Biomaterials 2016, 98, 120–130. [Google Scholar] [CrossRef] [PubMed]
- Braunová, A.; Chytil, P.; Laga, R.; Šírová, M.; Machová, D.; Parnica, J.; Říhová, B.; Janoušková, O.; Etrych, T. Polymer nanomedicines based on micelle-forming amphiphilic or water-soluble polymer-doxorubicin conjugates: Comparative study of in vitro and in vivo properties related to the polymer carrier structure, composition, and hydrodynamic properties. J. Control Release 2020, 321, 718–733. [Google Scholar] [CrossRef]
- Bobde, Y.; Patel, T.; Paul, M.; Biswas, S.; Ghosh, B. PEGylated N-(2 hydroxypropyl) methacrylamide polymeric micelles as nanocarriers for the delivery of doxorubicin in breast cancer. Colloids Surf. B Biointerfaces 2021, 204, 111833. [Google Scholar] [CrossRef]
- Pang, Y.; Zhu, Q.; Liu, J.Y.; Wu, J.L.; Wang, R.B.; Chen, S.Y.; Zhu, X.Y.; Yan, D.Y.; Huang, W.; Zhu, B.S. Design and synthesis of cationic drug carriers based on hyperbranched poly(amine-ester)s. Biomacromolecules 2010, 11, 575–582. [Google Scholar] [CrossRef] [PubMed]
- Kamra, M.; Moitra, P.; Ponnalagu, D.; Karande, A.A.; Bhattacharya, S. New water-soluble oxyamino chitosans as biocompatible vectors for efficacious anticancer therapy via co-delivery of gene and drug. ACS Appl. Mater. Interfaces 2019, 11, 37442–37460. [Google Scholar] [CrossRef]
- Li, Y.; Thambi, T.; Lee, D.S. Co-delivery of drugs and genes using polymeric nanoparticles for synergistic cancer therapeutic effects. Adv. Healthc. Mater. 2018, 7, 1700886. [Google Scholar] [CrossRef]
- Wang, Y.; van Steenbergen, M.J.; Beztsinna, N.; Shi, Y.; Lammers, T.; van Nostrum, C.F.; Hennink, W.E. Biotin-decorated all-HPMA polymeric micelles for paclitaxel delivery. J. Control Release 2020, 328, 970–984. [Google Scholar] [CrossRef] [PubMed]
- Liu, X.; Feng, Z.J.; Wang, C.R.; Su, Q.; Song, H.J.; Zhang, C.N.; Huang, P.S.; Liang, X.J.; Dong, A.J.; Kong, D.L.; et al. Co-localized delivery of nanomedicine and nanovaccine augments the postoperative cancer immunotherapy by amplifying T-cell responses. Biomaterials 2020, 230, 119649. [Google Scholar] [CrossRef] [PubMed]
- Song, Y.D.; Wu, Y.H.; Xu, L.; Jiang, T.; Tang, C.; Yin, C.H. Caveolae-mediated endocytosis drives robust siRNA delivery of polymeric nanoparticles to macrophages. ACS Nano 2021, 15, 8267–8282. [Google Scholar] [CrossRef]
- Ryu, J.H.; Yoon, H.Y.; Sun, I.; Kwon, I.C.; Kim, K. Tumor-targeting glycol chitosan nanoparticles for cancer heterogeneity. Adv. Mater. 2020, 32, 2002197. [Google Scholar] [CrossRef] [PubMed]
- Zhao, Z.M.; He, M.; Yin, L.C.; Bao, J.M.; Shi, L.L.; Wang, B.Q.; Tang, C.; Yin, C.H. Biodegradable nanoparticles based on linoleic acid and poly(beta-malic acid) double grafted chitosan derivatives as carriers of anticancer drugs. Biomacromolecules 2009, 10, 565–572. [Google Scholar] [CrossRef] [PubMed]
- Zhou, H.F.; Yu, W.T.; Guo, X.; Liu, X.D.; Li, N.; Zhang, Y.; Ma, X.J. Synthesis and characterization of amphiphilic glycidol-chitosan-deoxycholic acid nanoparticles as drug carrier for doxorubicin. Biomacromolecules 2010, 11, 3480–3486. [Google Scholar] [CrossRef] [PubMed]
- Zhang, D.M.; Song, Y.Z.; Wang, Y.; Liu, X.D.; Yu, W.T.; Ma, X.J. Insight of in vitro siRNA release from chitosan nanoparticles under enzymolysis with FRET analysis. J. Pharm. Sci. 2016, 105, 301–307. [Google Scholar] [CrossRef]
- Lu, B.; Wang, C.F.; Wu, D.Q.; Li, C.; Zhang, X.Z.; Zhuo, R.X. Chitosan based oligoamine polymers: Synthesis, characterization, and gene delivery. J. Control Release 2009, 137, 54–62. [Google Scholar] [CrossRef]
- Almeida, A.; Araújo, M.; Novoa-Carballal, R.; Andrade, F.; Gonçalves, H.; Reis, R.L.; Lúcio, M.; Schwartz, S., Jr.; Sarmento, B. Novel amphiphilic chitosan micelles as carriers for hydrophobic anticancer drugs. Mater. Sci. Eng. C 2020, 112, 110920. [Google Scholar] [CrossRef]
- Mu, Y.Z.; Fu, Y.M.; Li, J.; Yu, X.P.; Li, Y.; Wang, Y.N.; Wu, X.J.; Zhang, K.C.; Kong, M.; Feng, C.; et al. Multifunctional quercetin conjugated chitosan nano-micelles with P-gp inhibition and permeation enhancement of anticancer drug. Carbohyd. Polym. 2019, 203, 10–18. [Google Scholar] [CrossRef] [PubMed]
- Liu, X.D.; Howard, K.A.; Dong, M.D.; Andersen, M.Ø.; Rahbek, U.L.; Johnsen, M.G.; Hansen, O.C.; Besenbacher, F.; Kjems, J. The influence of polymeric properties on chitosan/siRNA nanoparticle formulation and gene silencing. Biomaterials 2007, 28, 1280–1288. [Google Scholar] [CrossRef] [PubMed]
- Zhou, H.F.; Liu, X.D.; Zhang, Y.; Ma, X.J. Preparation and characterization of nanoaggregates self-assembled by lithocholic acid and N-trimethyl modified chitosan derivatives. J. Nanosci. Nanotechnol. 2010, 10, 2304–2313. [Google Scholar] [CrossRef] [PubMed]
- Seow, W.Y.; Xue, J.M.; Yang, Y.Y. Targeted and intracellular delivery of paclitaxel using multi-functional polymeric micelles. Biomaterials 2007, 28, 1730–1740. [Google Scholar] [CrossRef]
- Bae, Y.; Fukushima, S.; Harada, A.; Kataoka, K. Design of environment-sensitive supramolecular assemblies for intracellular drug delivery: Polymeric micelles that are responsive to intracellular pH change. Angew. Chem. Int. Ed. 2003, 42, 4640–4643. [Google Scholar] [CrossRef]
- Li, Y.L.; Zhu, L.; Liu, Z.Z.; Cheng, R.; Meng, F.H.; Cui, J.H.; Ji, S.J.; Zhong, Z.Y. Reversibly stabilized multifunctional dextran nanoparticles efficiently deliver doxorubicin into the nuclei of cancer cells. Angew. Chem. Int. Ed. 2009, 48, 9914–9918. [Google Scholar] [CrossRef]
- Tseng, Y.C.; Mozumdar, S.; Huang, L. Lipid-based systemic delivery of siRNA. Adv. Drug Deliv. Rev. 2009, 61, 721–731. [Google Scholar] [CrossRef] [PubMed] [Green Version]


| Sample a | CAC (mg/mL) | Size (nm) b | Zeta Potential (mV) |
|---|---|---|---|
| HT42-CS-DCA2.3 | 0.079 | 185.8 ± 3.4 (0.18) | 14.1 ± 0.6 |
| HT42-CS-DCA3.2 | 0.035 | 224.0 ± 2.6 (0.09) | 14.6 ± 0.4 |
| HT42-CS-DCA4.2 | 0.023 | 233.6 ± 3.0 (0.08) | 15.7 ± 0.8 |
| HT61-CS-DCA3.2 | 0.045 | 229.0 ± 1.7 (0.07) | 17.1 ± 1.0 |
| HT84-CS-DCA3.2 | 0.060 | 235.2 ± 1.4 (0.08) | 23.3 ± 3.2 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Liu, X.; Zhou, H.; Yu, W.; Xiong, X.; Krastev, R.; Ma, X. Preparation of Cationic Amphiphilic Nanoparticles with Modified Chitosan Derivatives for Doxorubicin Delivery. Materials 2021, 14, 7010. https://doi.org/10.3390/ma14227010
Liu X, Zhou H, Yu W, Xiong X, Krastev R, Ma X. Preparation of Cationic Amphiphilic Nanoparticles with Modified Chitosan Derivatives for Doxorubicin Delivery. Materials. 2021; 14(22):7010. https://doi.org/10.3390/ma14227010
Chicago/Turabian StyleLiu, Xiudong, Huofei Zhou, Weiting Yu, Xin Xiong, Rumen Krastev, and Xiaojun Ma. 2021. "Preparation of Cationic Amphiphilic Nanoparticles with Modified Chitosan Derivatives for Doxorubicin Delivery" Materials 14, no. 22: 7010. https://doi.org/10.3390/ma14227010
APA StyleLiu, X., Zhou, H., Yu, W., Xiong, X., Krastev, R., & Ma, X. (2021). Preparation of Cationic Amphiphilic Nanoparticles with Modified Chitosan Derivatives for Doxorubicin Delivery. Materials, 14(22), 7010. https://doi.org/10.3390/ma14227010








